16 Pharmacological treatments
|
|
|
- Nickolas West
- 8 years ago
- Views:
Transcription
1 Pharmacological treatments Pharmacological treatments Robert Baldwin and Alistair Burns Pharmacokinetics l Pharmacodynamics l Dementia l Delirium l Depressive illness l Mania l Schizophrenia l Sleep disorders l Rapid tranquillisation l Conclusion Pharmacokinetics The pharmacological treatment of the elderly differs from that of younger patients, mainly because of altered pharmacokinetics and the higher proportion of patients with organic disorders. Pharmacokinetics describes the way in which drugs reach their target tissues. Absorption Absorption is not grossly affected in the elderly although there are reductions in gastric ph, area of absorptive surface, mesenteric blood flow and transport enzymes (Lader, 1994). Distribution Changes in distribution in the elderly include: reduction in lean body mass and increase in body fat (fat acts as a reservoir for psychotropics, increasing their half-lives); reduction in body water (increased concentration of water soluble compounds, e.g. alcohol); reduction in plasma proteins such as albumin (increased levels of free drug); and reduction in cerebral blood flow. Metabolism This is reduced and is particularly important with polypharmacy. Liver blood flow decreases (by up to a third in over 65-year-olds (Bender, 1965)) and liver microsomes are less efficient (with some exceptions). Excretion Excretion is decreased. Glomerular filtration reduces by up to a half by the age of 70 (Papper, 1978). Plasma creatinine may be unreliable, so creatinine clearance is the preferred test of renal function. 247
2 248 Baldwin & Burns Pharmacodynamics Pharmacodynamics describes the effects of drugs on body tissues. It is more difficult to study and is less well understood than pharmacokinetics. However, knowledge is increasing with the use of new technology such as positron emission tomography (see Chapter 12). Results about receptor numbers and characteristics do not always explain what is seen clinically, and these discrepancies may result from more complex changes (e.g. post-synaptic changes or receptor effector system coupling). Narcotics and sedative hypnotics Generally there is an increased sensitivity to sedatives in the elderly. Fewer available receptors may mean that the same drug concentration results in increased receptor occupancy (Lader, 1994). The elderly are less sensitive to some drugs (e.g. isoprenaline). Dopaminergic system There are less dopaminergic cells in the basal ganglia. This contributes to an increased sensitivity to the extrapyramidal side-effects (excluding dystonias) of neuroleptics. Cholinergic system There are less cholinergic receptors. A cholinergic deficit is well established in Alzheimer s disease, and a number of medications (donepezil, rivastigmine, metritonate) have been developed to increase the availability of acetylcholine. Noradrenergic system Noradrenaline levels decrease with age. This may make the elderly more vulnerable to affective disorders. Practical implications of these changes Start low, go slow changes in pharmacokinetics and pharmacodynamics mean that the elderly are generally two to three times more sensitive to many medications, including psychotropic drugs. It is important to reduce the dose and frequency of medications because a longer half-life means that it takes longer to reach a steady state.
3 Dementia Pharmacological treatments 249 Pharmacological therapy is aimed at two areas in dementia: cognitive deficits and non-cognitive features (psychiatric symptoms and behavioural disturbances). Cognitive deficits Alzheimer s disease Donepezil and rivastigmine, acetylcholinesterase inhibitors, are the first drugs aimed at improving cognitive function to be licensed in the UK, and others are likely to follow. Most medications targeted at cognitive function are based on the cholinergic hypothesis, with the common goal of increasing available acetylcholine. Three approaches have been described as: (a) Loading with acetylcholine precursors. (b) Cholinesterase inhibitors (i.e. inhibiting the enzyme which degrades acetylcholine). (c) Direct stimulation of the receptors. Studies with precursors such as lethicin were initially successful but inconsistent results and a lack of efficacy have followed. Anticholinesterases have been the most studied group of drugs with the most promising results. Donepezil appears to be less hepatotoxic and better tolerated than its predecessor tetrahydroaminoacridine. Trials have shown the drug to lead to an approximate six months delay in the course of the dementia, more evidence is required (Kelly et al, 1997). Co-dergocrine mesylate is regularly prescribed in continental Europe and has been shown, in double-blind trials, to be effective at reducing symptoms of anxiety, depression, confusion and impaired social care (effects which can be of practical benefit to patients and carers). There is little evidence that it improves cognitive function. Negative results have been found in trials with thiamine and piracetam. Improvements in cognition have been described with desferrioxamine, indomethacin and N-acetylcarnitine (Burns, 1992). Vascular dementia There is some evidence that treating risk factors for stroke improves cognitive impairment. Reducing systolic blood pressure to between 135 and 150 mmhg improved cognitive function, but further reduction led to a deterioration (Meyer et al, 1986). Stopping smoking in normotensive patients with multi-infarct dementia was also beneficial. Prescribing 325 mg of aspirin per day can produce an improvement in cognitive function
4 250 Baldwin & Burns and cerebral perfusion (Meyer et al, 1989). Low dose aspirin (75 mg per day) reduces the risk of stroke and death in patients with pre-existing vascular disease (SALT Collaborative Group, 1991). Dementia with Lewy bodies The clinical features of dementia with Lewy bodies include episodic confusion, hallucinations and cognitive deterioration. Patients with dementia with Lewy bodies may have profound cholinergic losses. McKeith et al (1992) reported high mortality when prescribed neuroleptics. Furthermore, patients with Alzheimer s disease who respond to tetrahydroaminoacridine have Lewy bodies at post-mortem (Levy, 1993). In view of the fluctuation in cognitive state there are difficulties in attributing improvement to specific medication. Behavioural disturbances can be controlled with chlormethiazole and benzodiazepines. Non-cognitive features This term is generally applied to psychiatric symptoms and behavioural disturbances (for a review see Burns, 1993) (see Chapter 6). It is important to define accurately what features are being targeted. Neuroleptics Neuroleptics are moderately effective at reducing agitation and aggression. Schneider et al (1992) in a meta-analysis, found that 18% of patients with dementia and agitation may benefit from neuroleptics. Individual studies showed no significant change, but together there was a small effect in favour of neuroleptics. Also behaviour deteriorated when neuroleptics were stopped. There is no established difference between thioridazine and haloperidol. Lower doses are required than for treating psychoses in younger patients. In fact very low doses, such as 5 mg of thioridazine, or mg of haloperidol, may be effective. There is a concern that the anticholinergic effects of neuroleptics may contribute to cognitive decline in some patients with dementia. Choice of neuroleptic This depends upon individual preference and experience. Thioridazine is often prescribed but has marked anticholinergic effects. Haloperidol is another common choice but can cause extrapyramidal signs and symptoms. Sulpiride is useful when avoiding parkinsonian side-effects. Chlorpromazine is not recommended because of hypotension, and promazine may be too weak. Regarding the newer agents, there are good theoretical reasons why clozapine may benefit patients with dementia
5 Pharmacological treatments 251 with Lewy bodies. Risperidone and olanzapine may also be useful because of their side-effect profiles. Both clozapine and risperidone have been shown to be reasonably well tolerated and efficacious in psychosis in the elderly, and in the psychosis of Parkinson s disease (Kumar, 1997). The newer neuroleptics tend to be more expensive. Depot neuroleptics have been tried with some success and have the obvious advantage of improved compliance. Other medications A number of other medications have been used to control behavioural symptoms in dementia (Schneider & Sobin, 1994) (Box 16.1). Box 16.1 Medications (other than neuroleptics) used for behaviour symptoms in dementia Antidepressants have consistently been shown to be effective in alleviating affective symptoms in dementia. Monoamine oxidase inhibitors (type A and type B) are successful in improving memory and concentration, possibly by alleviating depressive symptoms. Selective serotonin reuptake inhibitors reduce aggression and irritability. They may be particularly effective in vascular dementia Lithium has been shown in a few reports to control agitation, often dramatically, but the side-effect profile of the drug and the proven benefit of other drugs make it unlikely to become an agent of choice Beta-blockers have been used in younger patients to control aggression, usually after brain damage Carbamazepine has been reported to control aggression, although there has been no placebo controlled study that has shown any benefit Benzodiazepines have a significant propensity to cause confusional states in the elderly, so their use is limited. However, from three recent studies, two have shown benzodiazepines to be more efficacious than thioridazine or haloperidol Psychostimulants such as methylphenidate have only been shown to benefit patients in open trials. It is likely with the invention of newer drugs that these older agents will no longer be used Buspirone have been reported, in two out of three cases of dementia, to have shown an improvement Trazodone has been highlighted by the attention given to the serotonergic deficit in Alzheimer s disease. It has been shown to help with aggression, not just in dementia
6 252 Baldwin & Burns Delirium Delirium is caused by physical disease, and treatment is aimed at the underlying condition such as a urinary tract infection (see Chapter 3). Appropriate nursing and medical care are important, and include reassurance, the presence of familiar people and a quiet, well lit environment. Prominent behavioural disturbance may be managed with psychotropic medication. Haloperidol and thioridazine remain the drugs of choice. Conditions such as delirium tremens require detoxification regimes along conventional lines, with a corresponding dose reduction of around a half. Rapid tranquillisation may be required for serious behavioural problems which put the patient or others at risk. Antidepressants Depressive illness Antidepressants can be classified into: (a) Tricyclics: subdivided into traditional agents (amitriptyline, imipramine, dothiepin, doxepin, clomipramine, nortriptyline) and newer agents (lofepramine). (b) Atypical antidepressants (trazodone, mianserin). (c) The selective serotonin reuptake inhibitors (SSRIs) (fluoxetine, fluvoxamine, paroxetine, sertraline). (d) Monoamine oxidase inhibitors (MAOIs), subdivided into traditional agents (phenelzine, tranylcypromine) and the newer reversible inhibitors of monoamine oxidase A enzyme (RIMA agents) (moclobemide). Choice of antidepressant Efficacy The recovery rate of adult patients with depressive illness treated with an antidepressant is similar at any age, around 60 70%. There is no evidence that any drug or class of drugs is superior in terms of response rate to another (Katona, 1993). Some concern has been expressed that SSRIs may be less effective in severe depression, but there is no evidence supporting this in older patients. Safety There is little doubt that the newer agents are safer than traditional tricyclics in over dosage. However, the use of the newer medications should not lead to a complacent approach to managing suicide risk, which is high in the elderly.
7 Contraindications Pharmacological treatments 253 Contraindications for tricyclics include a history of acute (but not necessarily chronic) glaucoma; prostatism; a myocardial infarct within the preceding three months; a tachy- or brady-arrhythmia; poorly controlled (but not necessarily stable) heart failure; or a clinically relevant cardiac conduction disorder (for example bi- or tri-fascicular block). Severe renal or hepatic insufficiency are contraindications to using an SSRI. Side-effects There are important differences in side-effects (Table 16.1). For the traditional tricyclics, anticholinergic effects are prominent and frequently troublesome, but are less marked with lofepramine. Postural hypotension is arguably the most troublesome and dangerous side-effect of the tricyclics. They commonly cause sedation, as does trazodone. Tricyclics may provoke delirium, especially in the setting of acute physical illness or dementia; amitriptyline is the worst offender. With relatively minor variations, all the SSRIs cause nausea (5 15%), diarrhoea (10%), insomnia (5 15%), agitation or anxiety (2 15%), headache and weight loss. Many of these are transient and early phenomena. Also, dosages of SSRIs were originally too high, possibly exaggerating this profile. However, studies in the elderly have not found a lower rate of side-effects in SSRIs than the older tricyclics, but a different pattern (Katona, 1993). Sedation is least likely with fluoxetine and more likely with paroxetine, while fluoxetine may lead to anxiety and agitation. Fluvoxamine causes nausea, but has a lower incidence of insomnia. Paroxetine has a specific indication for the treatment of anxiety in association with depression. Table 16.1 Side-effects of antidepressants (numbered 0 to 5 by increasing intensity of effect) Anticholinergic effects Orthostatic effects Sedation Amitriptyline Imipramine Dothiepin Mianserin 0/1 0/1 4 Lofepramine 1/2 1 1 Trazodone Fluvoxamine 0/1 0 0 Sertraline 0/1 0 0 Fluoxetine 0/1 0 0 Paroxetine 0/1 0 1/2 Moclobemide 1 1 1/2
8 254 Baldwin & Burns Moclobemide appears to be of equal efficacy to tricyclics and SSRIs in late-life depression. It has a low risk of the cheese effect, a short duration of action and half-life and is safe and seems well tolerated. Adverse effects include agitation, anxiety and insomnia. Interactions All antidepressants may antagonise anticonvulsant medication. Concomitant antipsychotics lead to increased levels of tricyclic drugs, and the plasma concentration of haloperidol may be increased by fluoxetine. There is an increased risk of lithium central nervous system toxicity if combined with SSRIs. Two SSRIs, fluvoxamine and paroxetine, may enhance the effects of warfarin. Plasma concentrations of lipophilic betablockers may be increased by fluvoxamine. Imipramine and possibly other tricyclics may lead to increased levels of diltiazem and verapamil. Anxiolytics and hypnotics may enhance the sedative effects of tricyclics. Cimetidine may raise plasma levels of moclobemide and the tricyclics. Although the risk of a hypertensive crisis is low, drugs with sympathomimetic effect and opiate-based drugs should be avoided with moclobemide. If changing to a MAOI from fluoxetine five weeks must elapse, two weeks for paroxetine and a week for sertraline. Mixing an SSRI with a MAOI may cause the serotonergic syndrome characterised by excitement, confusion, rigidity, tremor, hyperthermia, tachycardia, hypotension and convulsions. Lastly, although rare, there have been a number of reports of SSRIs leading to, or exacerbating, parkinsonism or akathisia. Compliance Lack of compliance correlates with the number of other drugs prescribed and polypharmacy is frequent among older depressed patients. Memory is less efficient in depression and may impair compliance. The once daily dosage regime of most of the SSRIs is an advantage over tricyclics. Cost Costs are generally much higher for the newer medications. While arguments have been put forward that cost-benefit analysis favours the newer agents because of increased compliance, there is no relevant data with older, depressed patients. Comorbidity Tricyclics are less well tolerated by elderly medically ill patients (Koenig et al, 1989) than SSRIs (Evans, 1993). There is little evidence about the best way of treating depression comorbid with dementia. In a double-
9 Pharmacological treatments 255 blind placebo controlled trial, using imipramine, Reifler et al (1989) found a significant improvement in mood in an elderly group of patients with Alzheimer s disease and depression. The mean dose was 80 mg daily, but it was noted that cognitive function remained stable only within a fairly narrow dose range. Other agents have been inadequately assessed in dementia. In one small open study, patients reported improvement in depression comorbid with dementia using mg of moclobemide (Postma & Vranesic, 1985). Treatment-resistant depression This is defined as failure to respond to eight weeks of an adequate single agent therapy. There has been considerable interest in augmentation regimes, but little data about older depressives. Finch & Katona (1989) reported improvement and good tolerance with lithium augmentation in two-thirds of a small sample of patients resistant to either first line treatment or electroconvulsive therapy. Van Marwijk et al (1990) reported a similar improvement rate in a larger series, but encountered more side-effects, especially of lithium toxicity. Seth et al (1992), in an open study of eight refractory, mainly elderly, cases, reported improvement in all when given nortriptyline plus an SSRI. However, this combination may cause toxic plasma levels of the tricyclic. Continuation therapy Response to treatment often occurs later than in younger patients (Flint, 1992; National Insistute of Health Consensus Development Panel on Depression in Late Life, 1992). A minimum trial is six weeks, although a significant minority of patients respond up to eight or nine weeks after starting therapy (NIH Consensus Development Panel on Depression in Late Life, 1992). The standard six months of continuation therapy after resolution of depressive symptoms is probably too short for elderly patients (Flint, 1992); a year is more realistic. The main risk period for recurrence and relapse is the first two years (Flint, 1992). Prophylaxis Some clinicians argue for the long-term treatment of all patients who have had a major depression in later life. Few elderly patients remain symptom free during extended periods of follow-up (Baldwin & Jolley, 1986) and even one further episode of depressive illness occurring to an older person is time lost from an already short life expectancy. However, this is controversial. Clinicians are faced with the choice of either maintaining patients on antidepressants indefinitely, or attempting to wean them off after about
10 256 Baldwin & Burns a year. As a guide, those patients who do best are characterised by having good health and an uncomplicated recovery from depression (Baldwin & Jolley, 1986). Both lithium (Abou-Saleh & Coppen, 1983) and dothiepin (Old Age Depression Interest Group, 1993) are reported to significantly reduce relapse rates in the medium term. For antidepressants the prophylactic dose should be as close as possible to the therapeutic one (Reynolds et al, 1993). However, weight gain associated with long-term tricyclic usage may be problematic; more work is needed on the role of the newer agents in prophylaxis. Which antidepressant? A meta-analysis of the efficacy and acceptability of SSRIs (Song et al, 1993) concluded that their routine use as first line agents in depressive illness was unwarranted. Tricyclic antidepressants can be recommended as a well-tried, effective and cheap treatment for depression in old age, provided the patient has no contraindications and is tolerant of sideeffects. In practice, the newer agents constitute an important advance in the treatment of those elderly patients, not inconsiderable in number, who do not fulfil these conditions, especially the physically frail. Mania Acute treatment Neuroleptic drugs are the mainstay of treatment in the acute phase. Haloperidol, which has an extremely wide dose range, is popular. Drugs with lower potency such as thioridazine or promazine can be prescribed to reduce the risk of extrapyramidal side-effects. Practical problems include falls caused by a mixture of parkinsonism and sedation in an overactive patient and anticholinergic delirium caused by prescribing neuroleptics and anticholinergic agents (benzhexol, orphenadrine, benztropine). Mania may then be erroneously diagnosed. Lithium is an option for the less disturbed patient but serum levels should be lower than for younger patients, on average mmol/l (Shulman et al, 1992). There is a little evidence that valproate or carbamazepine may be effective, but much further work is required, including research to produce definitive guidelines for lithium treatment in older people (Shulman et al, 1992). Prophylaxis Lithium is also used for prophylaxis. As with acute treatment, dosages will generally be half that of younger adults. Lithium toxicity is a risk and is associated as much with poor monitoring as with the presence of organic
11 Pharmacological treatments 257 Box 16.2 Key learning points Non-cognitive features in dementia are amenable to treatment with neuroleptics and non-neuroleptic drugs In vascular dementia, removing risk factors and aspirin improve cognitive function Patients with Lewy body dementia are particularly sensitive to neuroleptics Remember inter-individual variation in drugs metabolism is much greater in elderly than younger patients All antidepressant and antipsychotic agents are equally effective so prescribing decisions are largely based on side-effect profiles The principles of prescribing to older patients are not different but are complicated by issues of comorbidity, poorer compliance and higher risk of side-effects Suicide risk is not dealt with simply by prescribing a safer drug (not infrequently cerebral) pathology. Regular checks of renal and thyroid function and concurrent medication, particularly the inadvertent prescription of a diuretic, are essential. Acute treatment Schizophrenia The principles of treating schizophrenia are similar at any age. Ageing results in reduced levels of dopamine and tyrolase hydroxylase, as well as lower counts of dopamine-rich neurons in the midbrain (Morgan et al, 1987). This raises susceptibility to neuroleptic-induced extrapyramidal symptoms. Antipsychotic drugs can be classified into: (a) Phenothiazines, aminoalkyl compounds (chlorpromazine), piperazines (trifluoperazine) and piperidines (thioridazine). (b) Thioxanthenes (flupenthixol). (c) Butyrophenones (haloperidol and pimozide, a butyrophenone derivative). (d) Dibenzapines (clozapine). (e) Other newer agents: sulpiride (a substituted 0-anisomide), risperidone (a benzisoxazole), sertindole and olanzapine. The first three groups have similar pharmacokinetics and are metabolised in the liver and excreted by the kidney. Their elimination half-lives are in the order of hours, although pimozide is much
12 258 Baldwin & Burns longer and clozapine and sulpiride somewhat shorter (5 15 hours). Clinical experience with clozapine, risperidone and olanzapine in the elderly is limited. However, the fact that these newer compounds may cause less extrapyramidal symptoms or tardive dyskinesia is of great significance to older patients. Choice of neuroleptic Effectiveness All current antipsychotics are effective in late-onset schizophrenia. Contraindications Caution is necessary in patients with a history of myocardial disease (in particular with pimozide), hepatic disorder, prostatism and Parkinson s disease, but apart from agranulocytosis most contraindications are relative. Side-effects Choosing a neuroleptic depends largely on the anticipated side-effects. These are best understood by reference to neurotransmitter systems (Table 16.2): (a) Antidopaminergic effects cause parkinsonism and akathisia. The former is a particular hazard in elderly patients. Lowering the dose, if practicable, is the first move; otherwise changing to a lower potency neuroleptic may help. Routine prescribing of anticholinergic agents to suppress such symptoms is not recommended as it may increase the risk of tardive dyskinesia in older patients (World Health Organization, 1990). Age is a major risk factor for tardive dyskinesia so that drug treatment should be reviewed regularly. Drug holidays can make the problem worse. Treatment of tardive dyskinesia is difficult, but sulpiride benefits some patients (Schwartz et al, 1990). (b) Anticholinergic effects cause similar problems to those of the tricyclic antidepressants. (c) Antihistaminic effects may lead to oversedation, especially when combined with other centrally active drugs, including antidepressants and hypnotics. Weight gain may occur with long-term use. (d) Antiadrenergic effects may cause dangerous postural hypotension. Chlorpromazine is the worst culprit, it is not a drug of first choice for the frail elderly. In addition, there are a number of idiosyncratic reactions of which the most important are the neuroleptic malignant syndrome, adverse liver effects (which are not confined to chlorpromazine) and agranulocytosis.
13 Pharmacological treatments 259 Table 16.2 Side-effects of antipsychotic drugs (+++ marked, ++ moderate, + mild, + minimal, 0 none) Anti- Anti- Anti- Anti-alphadopaminergic muscarinic histaminic adrenergic Chlorpromazine Thioridazine Perphenazine Trifluoperazine Haloperidol Pimozide Sulpiride Clozapine Promazine Risperidone Olanzapine Long-term use is associated with corneal particulate material which could carelessly be attributed to cataract in the elderly. Interactions Interactions which alter plasma antipsychotic levels may occur with: lithium, phenobarbitol, carbamazepine, phenyldantoin, cimetidine, propranolol and antidepressant drugs. Cost is a major issue with the newer agents such as risperidone and clozapine. Many clinicians have locally produced protocols for their use. Treatment-resistant schizophrenia Clozapine is reserved for refractory schizophrenia and is not contraindicated in older patients, although dosages are typically half that of younger adults, and hypotension can be problematic. Surprisingly, age has not been identified as a risk factor for agranulocytosis (Ball, 1992). Maintenance therapy Post s seminal work (1966) suggested that only a third of patients with late paraphrenia, followed over 14 to 21 months, remained symptom free. Regrettably, the advent of the newer antipsychotics and specialised services have not convincingly altered this prognosis (Howard & Levy, 1992). They suggested that compliance, and therefore outcome, may be improved by the use of depot neuroleptics and the deployment of community psychiatric nurses. All the current depot neuroleptics have been used in
14 260 Baldwin & Burns Box 16.3 Good practice points Start low, go slow when prescribing to elderly patients to start in very low doses, syrups are sometimes available Exclude Lewy body dementia, as far as possible, before prescribing neuroleptics to a patient with dementia Examine a patient with dementia to exclude vascular disease treatment of risk factors and/or aspirin may help Gain experience with prescribing at least one of the tricyclics and one of the newer agents; become familiar with their dose ranges and side-effect profiles Take a good drug and alcohol history polypharmacy accounts for much iatrogenic morbidity A therapeutic antidepressant trial in older patients should last at least six to eight weeks A reasonable period for continuation treatment is 12 months. Lithium dose ranges are lower in the elderly, generally mol/l elderly patients and there is little to suggest that one is superior to another, or that any is less likely to precipitate parkinsonism. Dosages will generally be half that of younger adults. Parkinsonism may occur quite suddenly after weeks of treatment and may take months to wear off, or may expose latent Parkinson s disease. Many clinicians avoid the longer acting depot agents (haloperidol decanoate, pipothiazine palmitate) in elderly patients. Sleep disorders Disturbed sleep in the elderly is a common complaint and often results in a request for sedative medication. It is important to recognise that sleep disturbances are very often secondary to a physical disorder (obvious symptomatic culprits being pain, dysuria and nocturia) or a psychiatric disturbance (such as depression or delirium). Attention to the primary problem often leads to restoration of the normal sleep pattern. It is important to be aware of iatrogenic causes of sleep disturbance, notably steroids, theophyllines and psychoactive medication, as well as alcohol. Specific sleep disturbances of snoring, sleep apnoea and neuromuscular disorders such akathisia may be responsible. Specific agents to treat sleep disorders include chlormethiazole, which is effective and widely used; the only side-effect being nasal stuffiness. Benzodiazepines are still the most commonly used drugs for sleep disturbance and the shorter acting the drug the better, temazepam being the best. Chlordiazepoxide and diazepam are longer acting and newer
15 Pharmacological treatments 261 Table 16.3 Medications prescribed for sleep disorders Starting Maximum Side-effects dose dose Chloral hydrate 1 2 tabs (as Up to 5 Gastric irritation 414 mg per tablet) nocte Triclofos sodium 1 2g nocte Same Fewer gastrointestinal effects Chlormethiazole 1 2 caps nocte Up to 3 Nasal congestion Zopiclone 1/2 tab nocte Up to 2 tabs New drug, caution in elderly Temazepam 5 15 mg nocte Up to 30 mg As with other benzodiazepines agents such as zopiclone require more research. Medications are summarised in Table Rapid tranquillisation The elderly, in common with their younger counterparts, can become aggressive and agitated requiring emergency sedation. One has to exercise more caution with sedation as coexisting physical illness may interact detrimentally with prescribed medication. For example, heavy sedation in a person with a confusional state secondary to cerebral hypoxia could be fatal. Bearing this in mind, the principles of rapid tranquillisation are the same as in younger patients, although doses need adjusting accordingly. Intravenous treatment is rarely required and intramuscular injections usually suffice. Prolonged and sustained aggression is not as often a management problem and hence long-term treatment is rarely necessary. Haloperidol is particularly effective at controlling aggression Box 16.4 Controversial issues Donepezil may be helpful in alleviating the cognitive deficit in Alzheimer s disease. A careful diagnostic assessment and follow-up is necessary The newer antidepressants are regarded by some, but by no means all, old age psychiatrists as drugs of first choice when prescribing to elderly depressives There is a trend to life-long maintenance therapy in major depression of later life, but not all agree with this
16 262 Baldwin & Burns and a suggested regime for management is: (a) haloperidol 1 mg orally every hour (1 5 mg intramuscularly in an emergency); (b) continue with 0.5 to 2.0 mg, eight hourly; when settled for 48 hours, reduce dose by 25%, continue with this until signs of aggression break through ; (d) aim to discontinue drug after a maximum of four weeks. Conclusion Care must be exercised when prescribing for the elderly. Changes in pharmacokinetics and pharmacodynamics mean that doses often need to be reduced and side-effects are more common. Good prescribing behaviour is summed up by the adage start low, go slow. However, consideration must be taken not to treat mental illnesses in the elderly inadequately. In recent years, new treatments have become available for dementia, depression and schizophrenia. More studies, in the elderly, will be necessary to gain the maximum benefits for patients. References Abou-Saleh, M. T. & Coppen, A. (1993) The prognosis of depression in old age: the case for lithium therapy. British Journal of Psychiatry, 143, Baldwin, R. C. & Jolley, D. J. (1986) The prognosis of depression in old age. British Journal of Psychiatry, 149, Ball, C. J. (1992) The use of clozapine in older people. International Journal of Geriatric Psychiatry, 7, Bender, A. D. (1965) The effect of increasing age on the distribution of peripheral blood flow in man. Journal of the American Geriatrics Society, 13, Burns, A. (1992) Treatment by physical methods: medication. Current Opinion in Psychiatry, 5, (1993) Treatment of non-cognitive features of dementia. In Treatment and Care in Old Age Psychiatry (eds R. Levy, R. Howard & A. Burns), pp Petersfield: Wrightson Biomedical Publishing. Evans, M. E. (1993) Depression in elderly physically ill inpatients: a 12 month prospective study. International Journal of Geriatric Psychiatry, 8, Finch, E. J. L. & Katona, C. L. E. (1989) Lithium augmentation in the treatment of refractory depression in old age. International Journal of Geriatric Psychiatry, 4, Flint, A. J. (1992) The optimum duration of antidepressant treatment in the elderly. International Journal of Geriatric Psychiatry, 7, Howard, R. & Levy, R. (1992) Which factors affect treatment response in late paraphrenia. International Journal of Geriatric Psychiatry, 7, Katona, C. L. E. (1993) Optimising treatment for the elderly depressive: new antidepressants in the elderly. Journal of Psychopharmacology, 7 (suppl. 1), Kelly, C., Harvey, R. & Cayton, H. (1997) Therapies for Alzheimer s disease. British Medical Journal, 314,
17 Pharmacological treatments 263 Koenig, H. G., Goli, V., Shelp, F., et al (1989) Antidepressant use in elderly medical inpatients: lessons from an attempted clinical trial. Journal of General Internal Medicine, 4, Kumar, V. (1997) Use of atypical antipsychotic agents in geriatric patients: a review. International Journal of Geriatric Psychopharmacology, 1, Lader, M. (1994) Neuropharmacology and pharmacokinetics of psychotropic drugs in old age. In Principles and Practice of Geriatric Psychiatry (eds J. Copeland, M. Abou-Saleh & D. Blazer), pp Chichester: John Wiley. Levy, R. (1993) Is there life in the neuro-transmitter approach to the treatment of Alzheimer s disease? In Treatment and Care in Old Age Psychiatry (eds R. Levy, R. Howard & A. Burns), pp Petersfield: Wrightson Biomedical Publishing. McKeith, I., Fairburn, A., Perry, R., et al (1992) Neuroleptic sensitivity in patients with senile dementia of Lewy body type. British Medical Journal, 305, Meyer, J., Judd, B., Tawaklna, T., et al (1986) Improved cognition after control of risk factors for multi-infarct dementia. Journal of the American Medical Association, 256, Meyer, J. S., Rogers, R., McClintic, K., et al (1989). Randomised clinical trial of daily aspirin therapy and multi-infarct dementia. Journal of the American Geriatrics Society, 37, Morgan, D. G., May, P. C. & Fich, C. E. (1987) Dopamine and serotonin system in human and rodent brain: effects of age and neurodegenerative disease. Journal of the American Geriatric Society, 35, National Institute of Health Consensus Development Panel on Depression in Late Life (1992) Diagnosis and treatment of depression in late life. Journal of the American Medical Association, 268, Old Age Depression Interest Group (1993) How long should the elderly take antidepressants? A double-blind placebo-controlled study of continuation/ prophylaxis therapy with dothiepin. British Journal of Psychiatry, 162, Papper, S. (1978) Clinical Nephrology. Boston, MA: Little Brown. Post, F. (1966) Persistent Persecutory States of the Elderly. Oxford: Pergamon. Postma, J. U. & Vranesic, D. (1985) Moclobemide in the treatment of depression in demented geriatric patients. Acta Therapeutica, 11, 1 4. Reifler, B. V., Teri, L., Raskind, M., et al (1989) Double-blind trial of imipramine in Alzheimer s disease patients with and without depression. American Journal of Psychiatry, 146, Reynolds, C. F., Schneider, L. S., Lebowitz, B. D., et al (1993) Treatment of depression in the elderly: guidelines for primary care. In Diagnosis and Treatment of Depression in the Elderly: Proceedings of the NIH Consensus Development Panel Conference (eds L. S. Schneider, C. F. Reynolds, B. Lebowitz, et al). Washington, DC: American Psychiatric Press. SALT Collaborative Group (1991) Swedish aspirin low dose trial of 75 mg aspirin as secondary prophylaxis after cerebrovascular ischaemic events. Lancet, 338, Schneider, L., Pollock, D. & Lyness, S. (1990) A meta-analysis of controlled trials of neuroleptic treatment in dementia. Journal of the American Geriatrics Society, 38, & Sobin, P. (1994) Treatment for psychiatric symptoms and behavioural disturbances. In Dementia (eds A. Burns & R. Levy), pp London: Chapman and Hall Medical.
18 264 Baldwin & Burns Schwartz, M., Moquillansky, L., Lanyi, G., et al (1990) Sulpiride in tardive dyskinesia. Journal of Neurology, Neurosurgery and Psychiatry, 53, Seth, R., Jennings, A. L., Bindman, J., et al (1992) Combination treatment with noradrenaline and serotonin reuptake inhibitors in resistant depression. British Journal of Psychiatry, 161, Shulman, K., Tohen, M. & Satlin, A. (1992) The significance of mania in old age. Reviews in Clinical Gerontology, 2, Song, F., Freemantle, N., Sheldon, T. A., et al (1993) Selective serotonin reuptake inhibitors: a meta-analysis of efficacy and acceptability. British Medical Journal, 306, Van Marwijk, H. W. J., Beeker, F. M., Nolan, W. A., et al (1990) Lithium augmentation in geriatric depression. Journal of Affective Disorders, 20, World Health Organization (1990) Heads of centres collaborating in WHO coordinated studies in biological aspects of mental illness. Prophylactic use of anticholinergics in patients on long-term neuroleptic treatment: a consensus statement. British Journal of Psychiatry, 156, 412.
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of
 Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of antipsychotic agents Identify common adverse effects
Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of antipsychotic agents Identify common adverse effects
Psychopharmacology. Psychopharmacology. Hamish McAllister-Williams Reader in Clinical. Department of Psychiatry, RVI
 Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Treatments for Major Depression. Drug Treatments The two (2) classes of drugs that are typical antidepressants are:
 Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services
 Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA
 COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
Depression in Older Persons
 Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Background. Population/Intervention(s)/Comparator/Outcome(s) (PICO)
 updated 2012 Role of anticholinergic medications in patients requiring long-term antipsychotic treatment for psychotic disorders Q6: In individuals with psychotic disorders (including schizophrenia) who
updated 2012 Role of anticholinergic medications in patients requiring long-term antipsychotic treatment for psychotic disorders Q6: In individuals with psychotic disorders (including schizophrenia) who
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
DEMENTIA EDUCATION & TRAINING PROGRAM
 The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
Recognition and Treatment of Depression in Parkinson s Disease
 Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
**Form 1: - Consultant Copy** Telephone Number: Fax Number: Email: Author: Dr Bernard Udeze Pharmacist: Claire Ault Date of issue July 2011
 Effective Shared Care Agreement for the treatment of Dementia in Alzheimer s Disease Donepezil tablets / orodispersible tablets (Aricept / Aricept Evess ) These forms (1 and 2) are to be completed by both
Effective Shared Care Agreement for the treatment of Dementia in Alzheimer s Disease Donepezil tablets / orodispersible tablets (Aricept / Aricept Evess ) These forms (1 and 2) are to be completed by both
Medications for bipolar disorder
 Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Dementa Formulary Guidance [v1.0]
![Dementa Formulary Guidance [v1.0] Dementa Formulary Guidance [v1.0]](/thumbs/29/13622067.jpg) Dementa Formulary Guidance [v1.0] 1. Introduction These Guidelines are intended for routine use. However there will be instances where they are not suitable for the patient you are managing, where more
Dementa Formulary Guidance [v1.0] 1. Introduction These Guidelines are intended for routine use. However there will be instances where they are not suitable for the patient you are managing, where more
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers
 SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
ATYPICALS ANTIPSYCHOTIC MEDICATIONS
 The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
Major Depression. What is major depression?
 Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Disclosure Statement. Nursing Facility Regulations and Psychotropic Medication Use. Learning Objectives (Cont) Learning Objectives
 Nursing Facility Regulations and Psychotropic Medication Use Jeffrey C. Reist PharmD, BCPS College of Pharmacy The University of Iowa December 2010 Disclosure Statement I, Jeffrey Reist, PharmD, BCPS do
Nursing Facility Regulations and Psychotropic Medication Use Jeffrey C. Reist PharmD, BCPS College of Pharmacy The University of Iowa December 2010 Disclosure Statement I, Jeffrey Reist, PharmD, BCPS do
A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES
 INTRODUCTION A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES Individuals with intellectual disabilities are not uncommonly prescribed psychotropic medications.
INTRODUCTION A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES Individuals with intellectual disabilities are not uncommonly prescribed psychotropic medications.
A Manic Episode is defined by a distinct period during which there is an abnormally and persistently elevated, expansive, or irritable mood.
 Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Understanding Antipsychotic Medications
 Understanding Antipsychotic Medications NARSAD RESEARCH National Alliance for Research on Schizophrenia and Depression 60 Cutter Mill Road, Suite 404 Great Neck, NY 11021 516-829-0091 1-800-829-8289 516-487-6930
Understanding Antipsychotic Medications NARSAD RESEARCH National Alliance for Research on Schizophrenia and Depression 60 Cutter Mill Road, Suite 404 Great Neck, NY 11021 516-829-0091 1-800-829-8289 516-487-6930
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Obsessive Compulsive Disorder: a pharmacological treatment approach
 Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale.
![Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale. Below, this letter outlines [patient name] s medical history, prognosis, and treatment rationale.](/thumbs/25/5563775.jpg) [Date] [Name of Contact] [Title] [Name of Health Insurance Company] [Address] [City, State, Zip Code] Insured: [Patient Name] Policy Number: [Number] Group Number: [Number] Diagnosis: [Diagnosis and ICD-9-CM
[Date] [Name of Contact] [Title] [Name of Health Insurance Company] [Address] [City, State, Zip Code] Insured: [Patient Name] Policy Number: [Number] Group Number: [Number] Diagnosis: [Diagnosis and ICD-9-CM
4 Clinical Particulars
 SUMMARY OF PRODUCT CHARACTERISTICS 1 Name of the Medicinal Product Procyclidine Syrup 5mg/5ml 2. Qualitative and Quantitative Composition Each 5ml dose contains 5mg Procyclidine Hydrochloride BP. 3. Pharmaceutical
SUMMARY OF PRODUCT CHARACTERISTICS 1 Name of the Medicinal Product Procyclidine Syrup 5mg/5ml 2. Qualitative and Quantitative Composition Each 5ml dose contains 5mg Procyclidine Hydrochloride BP. 3. Pharmaceutical
GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS
 GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
Depression in the Elderly: Recognition, Diagnosis, and Treatment
 Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
ASSESSMENT AND MANAGEMENT OF PSYCHOSIS IN PERSONS WITH DEMENTIA
 ASSESSMENT AND MANAGEMENT OF PSYCHOSIS IN PERSONS WITH DEMENTIA Overview: Psychosis is a common clinical feature of dementia. Hallucinations and delusions are the two most common types of psychotic symptoms
ASSESSMENT AND MANAGEMENT OF PSYCHOSIS IN PERSONS WITH DEMENTIA Overview: Psychosis is a common clinical feature of dementia. Hallucinations and delusions are the two most common types of psychotic symptoms
Benzodiazepines: A Model for Central Nervous System (CNS) Depressants
 Benzodiazepines: A Model for Central Nervous System (CNS) Depressants Objectives Summarize the basic mechanism by which benzodiazepines work in the brain. Describe two strategies for reducing and/or eliminating
Benzodiazepines: A Model for Central Nervous System (CNS) Depressants Objectives Summarize the basic mechanism by which benzodiazepines work in the brain. Describe two strategies for reducing and/or eliminating
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS. Juanaelena Garcia, MD Psychiatry Director Institute for Family Health
 PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
Contemporary Psychiatric-Mental Health Nursing. Assessing the Effectiveness of Medications. Administering Medications
 Contemporary Psychiatric-Mental Health Nursing Chapter 32 Psychopharmacologic Nursing Interventions Assessing the Effectiveness of Medications Include how well the medications are helping the client to
Contemporary Psychiatric-Mental Health Nursing Chapter 32 Psychopharmacologic Nursing Interventions Assessing the Effectiveness of Medications Include how well the medications are helping the client to
Pharmacotherapy of BPSD. Pharmacological interventions. Anti-dementia drugs. Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence
 Pharmacotherapy of BPSD Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Pharmacological interventions Reducing medication errors. Reducing potentially inappropriate medication prescription.
Pharmacotherapy of BPSD Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Pharmacological interventions Reducing medication errors. Reducing potentially inappropriate medication prescription.
What are the best treatments?
 What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
Clinical Audit: Prescribing antipsychotic medication for people with dementia
 Clinical Audit: Prescribing antipsychotic medication for people with dementia Trust, team and patient information Q1. Patient's DIS number... Q2. Patient s residence: Home Residential Home Nursing Home
Clinical Audit: Prescribing antipsychotic medication for people with dementia Trust, team and patient information Q1. Patient's DIS number... Q2. Patient s residence: Home Residential Home Nursing Home
Dementia & Movement Disorders
 Dementia & Movement Disorders A/Prof Michael Davis Geriatrician ACT Health & GSAHS ANU Medical School Eastern Dementia Network Aged and Dementia Care Symposium Bateman s Bay, 22 October 2010 Types of Dementia
Dementia & Movement Disorders A/Prof Michael Davis Geriatrician ACT Health & GSAHS ANU Medical School Eastern Dementia Network Aged and Dementia Care Symposium Bateman s Bay, 22 October 2010 Types of Dementia
TREATMENT-RESISTANT DEPRESSION AND ANXIETY
 University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Depression in elderly people
 www.bpac.org.nz keyword: elderlydepression Depression in elderly people DECISION TO PRESCRIBE Have I identified the cause of the depression? Treat any underlying causes as well as the depression. What
www.bpac.org.nz keyword: elderlydepression Depression in elderly people DECISION TO PRESCRIBE Have I identified the cause of the depression? Treat any underlying causes as well as the depression. What
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Shared Care Guideline-Use of Donepezil, Galantamine, Rivastigmine and Memantine in Dementia
 Shared Care Guideline-Use of Donepezil, Galantamine, Rivastigmine and Memantine in Dementia Version: 3.0 Ratified by: Medicines Committee Date ratified: 16 th November 2011 Name of originator/author: James
Shared Care Guideline-Use of Donepezil, Galantamine, Rivastigmine and Memantine in Dementia Version: 3.0 Ratified by: Medicines Committee Date ratified: 16 th November 2011 Name of originator/author: James
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 26 April 2001 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 26 April 2001 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
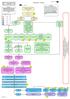 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
North of Tyne Area Prescribing Committee
 North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
Psychotic Disorder. Psychosis. Psychoses may be caused by: Examples of Hallucinations and Delusions 12/12/2012
 Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: info@psywellness.com.sg Web: www.psywellness.com.sg A condition
Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: info@psywellness.com.sg Web: www.psywellness.com.sg A condition
Antipsychotics in people with dementia an update and reminder
 www.bpac.org.nz keyword: dementia Antipsychotics in people with dementia an update and reminder Key concepts: Non-pharmacological treatments for the behavioural and psychological symptoms of dementia (BPSD)
www.bpac.org.nz keyword: dementia Antipsychotics in people with dementia an update and reminder Key concepts: Non-pharmacological treatments for the behavioural and psychological symptoms of dementia (BPSD)
Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole)
 EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
Overview of Mental Health Medication Trends
 America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
1. Which of the following SSRIs requires up to a 5-week washout period because of the
 1 Chapter 38. Major Depressive Disorders, Self-Assessment Questions 1. Which of the following SSRIs requires up to a 5-week washout period because of the long half-life of its potent active metabolite?
1 Chapter 38. Major Depressive Disorders, Self-Assessment Questions 1. Which of the following SSRIs requires up to a 5-week washout period because of the long half-life of its potent active metabolite?
Systematic Review of Treatment for Alcohol Dependence
 Systematic Review of Treatment for Alcohol Dependence ALCOHOL ARCUATE NUCLEUS in Hypothalamus, pituitary Beta-endorphin Dynorphin Kappa receptor Nucleus Enkephalins accumbens Delta receptor (+) Mu receptor
Systematic Review of Treatment for Alcohol Dependence ALCOHOL ARCUATE NUCLEUS in Hypothalamus, pituitary Beta-endorphin Dynorphin Kappa receptor Nucleus Enkephalins accumbens Delta receptor (+) Mu receptor
Disclosures Christer Allgulander
 How Patients With Generalized Anxiety Disorder (GAD) Are Treated in Specialized Care: A Pharmacoepidemiological Case Register Study in Sweden Christer Allgulander MD, Karolinska Institutet, Sweden Jan
How Patients With Generalized Anxiety Disorder (GAD) Are Treated in Specialized Care: A Pharmacoepidemiological Case Register Study in Sweden Christer Allgulander MD, Karolinska Institutet, Sweden Jan
Pharmacokinetics: Do we know what we are doing? Prof Dana Niehaus Department of Psychiatry University of Stellenbosch
 Pharmacokinetics: Do we know what we are doing? Prof Dana Niehaus Department of Psychiatry University of Stellenbosch Content Pharmacokinetics (What the body does to the drug) Absorption Distribution Metabolism
Pharmacokinetics: Do we know what we are doing? Prof Dana Niehaus Department of Psychiatry University of Stellenbosch Content Pharmacokinetics (What the body does to the drug) Absorption Distribution Metabolism
The Road to Rehabilitation, Part 6: Mapping the Way: Drug Therapy & Brain Injury Written by Gregory O Shanick, MD
 The Road to Rehabilitation, Part 6: Mapping the Way: Drug Therapy & Brain Injury Written by Gregory O Shanick, MD Introduction The basic unit of the nervous system is the neuron or nerve cell. Billions
The Road to Rehabilitation, Part 6: Mapping the Way: Drug Therapy & Brain Injury Written by Gregory O Shanick, MD Introduction The basic unit of the nervous system is the neuron or nerve cell. Billions
BENZODIAZEPINE CONSIDERATIONS IN WORKERS COMPENSATION: IMPLICATIONS FOR WORK DISABILITY AND CLAIM COSTS By: Michael Erdil MD, FACOEM
 3 rd Quarter 2015 BENZODIAZEPINE CONSIDERATIONS IN WORKERS COMPENSATION: IMPLICATIONS FOR WORK DISABILITY AND CLAIM COSTS By: Michael Erdil MD, FACOEM Introduction Benzodiazepines, sometimes called "benzos",
3 rd Quarter 2015 BENZODIAZEPINE CONSIDERATIONS IN WORKERS COMPENSATION: IMPLICATIONS FOR WORK DISABILITY AND CLAIM COSTS By: Michael Erdil MD, FACOEM Introduction Benzodiazepines, sometimes called "benzos",
Chapter 28. Drug Treatment of Parkinson s Disease
 Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Update and Review of Medication Assisted Treatments
 Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
An Introduction to Lewy Body Dementia
 An Introduction to Lewy Body Dementia A special publication for people newly diagnosed with Lewy body dementia and those still seeking answers. You don t have to face LBD alone. Increasing Knowledge Sharing
An Introduction to Lewy Body Dementia A special publication for people newly diagnosed with Lewy body dementia and those still seeking answers. You don t have to face LBD alone. Increasing Knowledge Sharing
White, circular, biconvex, uncoated tablets with a score line on one side, plain on the other.
 Nausicalm Cyclizine hydrochloride Ph. Eur. 50 mg Presentation White, circular, biconvex, uncoated tablets with a score line on one side, plain on the other. Uses Actions The active ingredient-cyclizine
Nausicalm Cyclizine hydrochloride Ph. Eur. 50 mg Presentation White, circular, biconvex, uncoated tablets with a score line on one side, plain on the other. Uses Actions The active ingredient-cyclizine
Psychotropic PRN: A model for best practice management of acute psychotic behavioural disturbance in inpatient psychiatric settings
 International Journal of Mental Health Nursing (2004) 13, 18 21 FEATURE ARTICLE Psychotropic PRN: A model for best practice management of acute psychotic behavioural disturbance in inpatient psychiatric
International Journal of Mental Health Nursing (2004) 13, 18 21 FEATURE ARTICLE Psychotropic PRN: A model for best practice management of acute psychotic behavioural disturbance in inpatient psychiatric
Drug Treatment Considerations In The Elderly
 Drug Treatment Considerations In The Elderly by Gordon Mallarkey Download Drug Treatment Considerations In The Elderly online in pdf Here you can see related and other interesting book : Pharmacotherapy
Drug Treatment Considerations In The Elderly by Gordon Mallarkey Download Drug Treatment Considerations In The Elderly online in pdf Here you can see related and other interesting book : Pharmacotherapy
ALZHEIMER DISEASE: TREATMENT OF NONCOGNITIVE BEHAVIORAL ABNORMALITIES
 88 ALZHEIMER DISEASE: TREATMENT OF NONCOGNITIVE BEHAVIORAL ABNORMALITIES MURRAY A. RASKIND ROBERT F. BARNES The original patient described by Dr. Alois Alzheimer in suggest directions for future investigation
88 ALZHEIMER DISEASE: TREATMENT OF NONCOGNITIVE BEHAVIORAL ABNORMALITIES MURRAY A. RASKIND ROBERT F. BARNES The original patient described by Dr. Alois Alzheimer in suggest directions for future investigation
Alcohol Withdrawal Syndrome & CIWA Assessment
 Alcohol Withdrawal Syndrome & CIWA Assessment Alcohol Withdrawal Syndrome is a set of symptoms that can occur when an individual reduces or stops alcoholic consumption after long periods of use. Prolonged
Alcohol Withdrawal Syndrome & CIWA Assessment Alcohol Withdrawal Syndrome is a set of symptoms that can occur when an individual reduces or stops alcoholic consumption after long periods of use. Prolonged
Essential Shared Care Agreement Drugs for Dementia
 Ref No. E040 Essential Shared Care Agreement Drugs for Dementia Please complete the following details: Patient s name, address, date of birth Consultant s contact details (p.3) And send One copy to: 1.
Ref No. E040 Essential Shared Care Agreement Drugs for Dementia Please complete the following details: Patient s name, address, date of birth Consultant s contact details (p.3) And send One copy to: 1.
adaptations whenever possible, to prevent or reduce the occurrence of challenging behaviours.
 POSITION STATEMENT on Management of Challenging Behaviours in People with Dementia 1. AIM OF THE POSITION STATEMENT This position statement applies to people living in supported accommodation and those
POSITION STATEMENT on Management of Challenging Behaviours in People with Dementia 1. AIM OF THE POSITION STATEMENT This position statement applies to people living in supported accommodation and those
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
I. The Positive Symptoms...Page 2. The Negative Symptoms...Page 2. Primary Psychiatric Conditions...Page 2
 SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
GMMMG Interface Prescribing Subgroup. Shared Care Template
 GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
Psychopharmacotherapy for Children and Adolescents
 TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
Treatment Modalities As in younger patients, the goals of treating depression in elderly patients include alleviating
 Iranian Rehabilitation Journal, Vol. 10, No. 16, Oct. 2012 Reviews/Short communication Treatment of Depression in the Elderly: A systematic review Arash Mirabzadeh, MD. University of Social Welfare and
Iranian Rehabilitation Journal, Vol. 10, No. 16, Oct. 2012 Reviews/Short communication Treatment of Depression in the Elderly: A systematic review Arash Mirabzadeh, MD. University of Social Welfare and
Summary of the risk management plan (RMP) for Rasagiline ratiopharm (rasagiline)
 EMA/744222/2014 Summary of the risk management plan (RMP) for Rasagiline ratiopharm (rasagiline) This is a summary of the risk management plan (RMP) for Rasagiline ratiopharm, which details the measures
EMA/744222/2014 Summary of the risk management plan (RMP) for Rasagiline ratiopharm (rasagiline) This is a summary of the risk management plan (RMP) for Rasagiline ratiopharm, which details the measures
Guidelines for the Diagnosis and Management of Acute Confusion (delirium) in the Elderly
 Guidelines for the Diagnosis and Management of Acute Confusion (delirium) in the Elderly Author: Madeleine Purchas (SpR Care of the Elderly) Consultant Supervisor: Dr Neil Pollard Date: 16 th Dec 2005
Guidelines for the Diagnosis and Management of Acute Confusion (delirium) in the Elderly Author: Madeleine Purchas (SpR Care of the Elderly) Consultant Supervisor: Dr Neil Pollard Date: 16 th Dec 2005
Trends in Prescribing of Antipsychotic Drugs in General Practice in England (Chart 1) 2.0. Other second generation antipsychotics (SGA)
 Antipsychotic drugs Antipsychotics can be broadly classified into first generation antipsychotics (FGAs, formerly known as typical antipsychotics) and second generation antipsychotics (SGAs, formerly known
Antipsychotic drugs Antipsychotics can be broadly classified into first generation antipsychotics (FGAs, formerly known as typical antipsychotics) and second generation antipsychotics (SGAs, formerly known
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller
 Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Data Based Medicine Paper: Dependence and Withdrawal
 Data Based Medicine Paper: Dependence and Withdrawal Author: Dr. David Healy Date Last Revised: 7 June 2012 Contents TREATMENT GROUPS... 2 DRUG GROUPS... 2 ALL DRUGS ACT ON EVERYTHING... 3 DRUG WITHDRAWAL
Data Based Medicine Paper: Dependence and Withdrawal Author: Dr. David Healy Date Last Revised: 7 June 2012 Contents TREATMENT GROUPS... 2 DRUG GROUPS... 2 ALL DRUGS ACT ON EVERYTHING... 3 DRUG WITHDRAWAL
Anti-Parkinsonism Drugs
 Anti-Parkinsonism Drugs Pharma Team 429 Fahad Alrumaih Ibrahim Alshiddi Sultan Alsalem Ismail Raslan Suhail Asiri Parkinsonism - Could be: primary [idiopathic] or secondary [viral infection or drug induced
Anti-Parkinsonism Drugs Pharma Team 429 Fahad Alrumaih Ibrahim Alshiddi Sultan Alsalem Ismail Raslan Suhail Asiri Parkinsonism - Could be: primary [idiopathic] or secondary [viral infection or drug induced
Paxil/Paxil-CR (paroxetine)
 Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
PSYCHOTROPIC MEDICATIONS
 PSYCHOTROPIC MEDICATIONS 644.3 Bipolar Disorder This Instructor s Guide contains: Brief Description, Objectives, Discussion Questions, Pretest, Post-test, Answer Keys and Glossary for this program, Psychotropic
PSYCHOTROPIC MEDICATIONS 644.3 Bipolar Disorder This Instructor s Guide contains: Brief Description, Objectives, Discussion Questions, Pretest, Post-test, Answer Keys and Glossary for this program, Psychotropic
Update on Treatment of the Dementias
 Update on Treatment of the Dementias Mark Pippenger, MD Behavioral Neurology Associate Clinical Professor of Neurology University of Arkansas for Medical Sciences Disclosures I will be discussing off-label
Update on Treatment of the Dementias Mark Pippenger, MD Behavioral Neurology Associate Clinical Professor of Neurology University of Arkansas for Medical Sciences Disclosures I will be discussing off-label
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL INVESTIGATION OF MEDICINAL PRODUCTS IN THE TREATMENT OF DEPRESSION
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 25 April 2002 CPMP/EWP/518/97, Rev. 1 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 25 April 2002 CPMP/EWP/518/97, Rev. 1 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE
Depre r s e sio i n o i n i a dults Yousuf Al Farsi
 Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
N-methyl-D-aspartate (NMDA) Receptor Antagonist Memantine (CWM TAF ONLY)
 Bro Taf Localities Drugs & Therapeutics Committee SHARED CARE Drugs: Acetylcholinesterase inhibitors - Donepezil, Rivastigmine and Galantamine (Cardiff and Vale and Cwm Taf) Protocol No. CV 52 N-methyl-D-aspartate
Bro Taf Localities Drugs & Therapeutics Committee SHARED CARE Drugs: Acetylcholinesterase inhibitors - Donepezil, Rivastigmine and Galantamine (Cardiff and Vale and Cwm Taf) Protocol No. CV 52 N-methyl-D-aspartate
Treating Mental Disorders. Types of Biological Treatment. Drug Treatments for Psychological Disorders
 Treating Mental Disorders Biological Treatments for Psychological Disorders Aims: Describe and Assess Biological Treatments Objectives By the end of this session you should be able to: Describe the use
Treating Mental Disorders Biological Treatments for Psychological Disorders Aims: Describe and Assess Biological Treatments Objectives By the end of this session you should be able to: Describe the use
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
