Going Live: Implementing an Electronic Health Record System in the Emergency Department
|
|
|
- Bruno Lyons
- 8 years ago
- Views:
Transcription
1 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause 44 Going Live: Implementing an Electronic Health Record System in the Emergency Department Margaret Meadors, 1 Natalie Benda, 1 A. Zachary Hettinger, 1,2 Raj M. Ratwani 1,2 1 The National Center for Human Factors in Healthcare, Washington, DC 2 Department of Emergency Medicine, Georgetown University, Washington, DC This study evaluated the immediate effects of implementing an electronic health record (EHR) system on physician workflow in the emergency department. Two sets of observations were conducted in one emergency department. The first set of observations, the baseline period, was completed in the 22 days prior to the implementation of a new EHR. The second set of observations, the go-live period, was completed during the seven-day period immediately after the EHR go-live date. A comparison across four task-based categories revealed that during the go-live period there was a decrease in the proportion of time physicians spent in patient rooms and engaged with paper-based tasks, and an increase in the proportion of time physicians spent at computer stations and working with other people. In addition, physicians engaged in more information seeking behaviors during the go-live period than during the baseline period. The impact of these shifts in tasks and behaviors is discussed with a focus on the importance of fully understanding the EHR go-live process. Copyright 2014 Human Factors and Ergonomics Society. All rights reserved. DOI / As a wide range of health care settings are rapidly integrating electronic health record (EHR) systems (Office of the National Coordinator for Health Information Technology, 2013), understanding the full cycle of EHR selection, implementation, and postimplementation use is critical for current patient safety as well as for influencing the design of future EHR systems. EHRs have the potential to improve the quality of healthcare by decreasing practice variability, improving data availability and sharing, and enhancing inter-provider and patient-provider communication (Kellermann & Jones, 2013; Kern, Barrón, Dhopeshwarkar, Edwards, & Kaushal, 2013; Kuperman et al., 2007). However, the initial implementation of a new system can lead inefficiency, patient dissatisfaction, clinician frustration, and patient safety issues (Ash et al., 2007; Reed et al., 2013; Sockolow, Weiner, Bowles, & Lehmann, 2011; Spellman Kennebeck, Timm, Farrell, & Spooner, 2012). Current EHR research has primarily addressed topics related to the selection and use of EHRs, with some studies retrospectively assessing the implementation process (Laramee, Bosek, Kasprisin, & Powers-Phaneuf, 2011). The research that does address the EHR implementation cycle consists of time and motion studies and retrospective analyses aimed at calculating return on investment (Grieger, Cohen, & Krusch, 2007; Pizziferri et al., 2005; Shapiro et al., 2010). Implementing a new EHR system, whether moving from paper based records to an EHR or whether simply changing EHR systems, encompasses a range of processes. These processes include, but are not limited to: evaluation, purchase, customization, training, system go-live, and post-implementation use. Limited research investigates the details of work environment changes as the implementation cycle occurs. A great deal of emphasis has also been placed on how EHRs affect clinician workflow (Lowry, Ramaiah, Gibbons, Patterson, & Lewis, 2013). As previously mentioned, other studies have looked at workflow in terms of time and motion studies (how long it takes providers to complete certain tasks) and patient throughput (Fleming et al., 2014; Read-Brown et al., 2013). However, there has been little research looking at the day-to-day activities completed by physicians and how EHR implementation affects their workflow patterns. In a joint study by the American Medical Association and the RAND Corporation regarding physician satisfaction with their working conditions, physicians cited the short-comings of EHRs in supporting their workflow processes as a major source of frustration (Friedberg et al., 2013). In order to address and improve this issue, workflow must be studied from a cognitive, physician-driven standpoint, as opposed to using task-based approach. The early stages of EHR implementation are a critical period, where the efforts to select an appropriate system are realized and the effects of using the new system remain unknown. Implementation requires collaboration, training, and a community effort to support the EHR s successful integration into the healthcare environment (Arellano et al., 2010). There is some promise of new benefits for healthcare providers and patients, such as decreased length of hospital stay, more efficient patient throughput, and improved tracking of patient data over time (Baumlin et al., 2010; Cooper et al., 2003; Friedberg et al., 2013; Weil, 2007), and also some wariness due to the potential for serious patient safety risks (Han et al., 2005). The mixed results in the
2 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause 45 literature, in terms of workflow efficiency and patient safety findings, highlight the need for a deeper understanding of all aspects of EHR development, selection, implementation, and use. This study investigated the transition period from just before a new EHR system goes live (baseline period) to the period immediately following the EHR system go-live date (go-live period). The benefit of exploring the go-live period as a potential area of improvement along the EHR implementation cycle is that the go-live period has the potential to accommodate changes, like training, quicker than areas like EHR design where changes may take years to occur. Observations for this study were completed at one tertiary care academic emergency department (ED). This ED has more than 90,000 annual patient visits and approximately 270 patients per day. The ED environment is unique; it is fast-paced and has wide variability in the rate of patient arrivals. Emergency medicine physicians are focused on treating patients as safely and efficiently as possible, however the nature of the ED environment (e.g., frequent interruptions, and fluctuating patient volumes) increase the risk of physician error (Farley et al., 2013). The smooth and successful transition to a new EHR system is vital for these providers and the implementation process directly affects patient safety and quality of patient care (Farley et al., 2013). This paper focused on the first two phases of a threephase study aimed at understanding EHR implementation in the ED. The portion of the study reported here includes observational data gathered during the baseline period (observations completed during the 22-day period prior to the system go-live date) and the go-live period (observations completed during the first seven days following the system go-live date). A third follow-up observation phase is in progress. The EHR system being implemented at this particular hospital largely replaced a homegrown EHR system that was used for patient tracking, result viewing and limited electronic clinical documentation. Under the original EHR, physicians had the option to complete documentation on paper that was later scanned into the EHR or to type directly into the EHR. The observed go-live period consisted of the addition of a new commercially available EHR with computerized physician order entry (CPOE) system, results viewing (labs and radiology) and nursing documentation. During the go-live period the original EHR system operated in parallel and physician documentation remained the same. METHOD Data was collected by two researchers using a paperbased minute-by-minute observational template. Observational data was collected across four task-based categories based on time, and two additional categories based on frequency of occurrence. These categories were based on observational categories that have previously been used in the ED (Chisholm, Dornfeld, Nelson, & Cordell, 2001). Task-based categories included: patient room, computer, person-to-person, paper (charts/labs), and other. Patient room included any time that the physician entered a patient s room to provide direct patient care. Due to the need to provide comfort and privacy to patients, observers did not enter patient rooms. Any activities recorded (such as an interruption) during the time that a physician was in a patient room marks a moment where the physician briefly stepped out of the room (e.g., to take a call, briefly talk to another care provider). Computer tasks included reading information from the computer screen, attending to information on a computer screen, and writing or entering information on the computer. Person-to-person included interpersonal communications using any mode, including face-to-face interaction and indirect person-to-person communication such as using the telephone. Paper (charts/labs) included any time that the physician wrote on paper, and/or focused on paper-based information (e.g., charts and labs). The Other task category included personal behaviors, such as checking a personal phone or taking a break. Task-based categories were calculated as a time variable. The remaining two categories, interruptions and assistance seeking, were recorded as discrete events. Interruptions primarily included external interruptions such as phone calls or another care provider needing attention or assistance. Some interruptions prompted the physicians to switch tasks and were of longer duration, while other interruptions were either delayed or of shorter duration. Assistance seeking behaviors were classified as instances where a physician sought out guidance, not just information, from an outside source. For example, a resident asking a nurse what room the patient was in would not be counted, however a resident asking an attending physician to show them how to enter
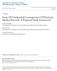
3 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause %$ Percentage)of)Total)Task)Time)) 40.0%$ 35.0%$ 30.0%$ 25.0%$ 20.0%$ 15.0%$ 10.0%$ Baseline$Period$ Go5Live$Period$ 5.0%$ 0.0%$ Computer$ Person5to5Person$ Pa7ent$Room$ Paper$(Charts/ Labs)$ Task) Figure 2. Comparison of physicians percentage of time spent on tasks across observation periods. an order would be counted. These two categories were considered events and calculated as a frequency rather than as a time period. Although they were recorded along a timeline (e.g., the interruption occurred 17 minutes into the observation) the interruption or assistance seeking would only be counted one time. Observers also took additional qualitative notes to provide information about the interruption and assistance seeking categories, such as notes regarding relevant interpersonal and environmental factors. Observations were collected in two phases, during a baseline period prior to the adoption of the new EHR system and during the go-live period. The go-live period observations were completed during the first seven days of the EHR go-live date. Overall, 14 physicians were observed for two hours each during the baseline period and 14 physicians were observed for two hours each during the go-live period. Both resident and attending physicians were observed, however none of the residents were first year residents. First year residents were excluded due to their relative inexperience in the ED environment. The total number of observation hours for each period was 28 hours for a total of 56 observational hours. The observers maintained visual contact with the physicians throughout the observation period, excluding time spent in patient rooms. Observers took care to avoid disrupting the workflow of the physician being shadowed as well as the rest of the healthcare team. Observers did not initiate conversations with the physicians in order to avoid biasing data collection. RESULTS To examine the workflow changes between the baseline period and the go-live period, each physician s time per task was converted to a percentage of their total task time. Percentages were calculated by taking the total number of minutes that a physician spent on a specific task (e.g, computer, patient room, person-toperson, or paper) and dividing that value by the cumulative number of task minutes recorded during the two hour observation period. By using this strategy, the total number of task minutes typically exceeded 120
4 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause 47 minutes because physicians often engage in more than one task per minute. A 2x4 mixed model analysis of variance (ANOVA) was performed to assess the differences in task distributions across the baseline and go-live periods. The results revealed a significant main effect between tasks, F(3, 28) = 44.60, p <.001, and a significant interaction between task and phase, F(3, 28) = 10.29, p <.001. Least Significant Difference post-hoc comparisons showed that a significantly greater percentage of time was spent on computer tasks during the go-live period (M 37.7%) than during the baseline period (M = 27.8%, p <.01). In addition, there was a significant increase in the percentage of time spent on person-to-person tasks during the go-live period (M = 35.5%) than in the baseline period (30.7%, p <.05). Conversely, a smaller percentage of time was spent on paper related tasks during the go-live period (M = 11.2%) than during the baseline period (M = 20.0%, p <.01). This was similar to the shift in task time percentage for the amount of time spent in patient rooms during the go-live period (M = 15.6%) which was significantly less than the percentage of time spent in patient rooms during the baseline period (M = 21.5%, p <.05). In summary, the average percentage of time spent on computer based tasks and engaging in person-toperson interactions increased during the go-live, while the average percentage of time spent in patient rooms and spent using paper-based charts and materials decreased during the go-live period (see Figure 1). In addition to the task-based variables, the assistance seeking data revealed a significant increase in the amount of assistance seeking between the baseline period (M =.04) and the go-live period (M =2.48, p < 0.05). This was also expected, given the nature of learning to use a new EHR system. However, the qualitative data on assistance seeking showed that physicians sought increased assistance on clinical issues in addition to computer-based issues during the go-live period. For example, the observers recorded questions including, should I do regular insulin? and is this [medication] associated with any other issues? that were not directly related to computer use. DISCUSSION This study established a comprehensive picture of workflow changes in the ED during the EHR go-live period by tracking the tasks and behaviors of emergency medicine physicians. Few studies have examined the immediate change in workflow during the go-live period. Given the implications and hazards associated with learning a new technology, this period of EHR integration needs to be better understood so that strategies may be developed to curb potential inefficiencies and patient safety risks. The results outlining changes across observation categories illustrate that the EHR go-live period immediately impacts how physicians work within their environment. While this study demonstrated anticipated changes in workflow after the introduction of the new system, such as increased time on the computer and decreased time spent working with paper records, there were also several findings that shed new light on how workflow and behavior changes in the early days of EHR implementation. Evidence of decreased time with patients and an increased amount of requested assistance by emergency medicine clinicians illustrates a shift away from direct patient care during the go-live period. This shift could potentially have real consequences in areas such as diagnostic decision-making and patient satisfaction. The increased rate of assistance seeking observed during the go-live period should be interpreted with care due to the relatively small number of assistance seeking behaviors overall. However, this finding should not be ignored. While the majority of the assistance seeking behaviors included questions that were specific to the use of the EHR system, physicians also sought out clinical input from others. Seeking clinical input from others suggests that the new EHR system introduced uncertainties related to clinical practice or information. For example, physicians using a new system may encounter pre-planned order sets with a different structure than they are accustomed to, or they may be unable to find a familiar test or treatment choice due to an unfamiliar naming system. Physicians who change their treatment protocols and preferences must adapt to increased levels of uncertainty by consulting and doublechecking with other care providers. Consulting and double-checking with peers illustrates the flexibility and resiliency of healthcare providers, but it also signals that there may be real changes to decision making strategies or patient treatment paradigms. In addition to the changes outlined in the results, this particular hospital used several strategies to mitigate the potentially adverse effects of EHR implementation on workflow and/or technology issues. During the go-live period, there were computer specialists on hand to answer questions about the EHR system and there were additional physicians present as floaters to assist with patients. These strategies, while proactive and potentially highly valuable for both the physicians using the system and the patients present in the ED during the go-live period, did not stop fluctuations in physician time allocation from occurring. One area of future research on EHR implementation should assess which strategies, such as additional floater physicians,
5 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause 48 computer specialists, training groups, are most effective in order to maximize resources. This study has several limitations, including the treatment of tasks as discrete events (versus time intervals) and the inability to enter patient rooms and record specific events, including the use of portable workstations. In addition, these findings document the implementation of a single EHR at one clinical site and results may not be generalizable across different clinical settings, healthcare organizations or other EHR systems. As more organizations implement EHRs, it is critical to patient safety that areas of the implementation process that need improvement are identified and that interventions are strategically designed to improve patient care during implementation periods. Uncovering critical periods where interventions may have a greater and more immediate impact on the process of integrating EHRs may help inform EHR developers in shaping guidelines for healthcare organizations and providers to assist them during the EHR implementation process. REFERENCES Arellano, P., Bochinski, J., Boone, E., Grayson, R., Phua, J., & Uehara, R. (2010). Selecting an EMR for your practice: Evaluating usability. HIMSS: Chicago, IL. Ash, J. S., Sittig, D. F., Poon, E. G., Guappone, K., Campbell, E., & Dykstra, R. H. (2007). The extent and importance of unintended consequences related to computerized provider order entry. Journal of the American Medical Informatics Association, 14(4), Baumlin, K. M., Shapiro, J. S., Weiner, C., Gottlieb, B., Chawla, N., & Richardson, L. D. (2010). Clinical Information System and Process Redesign Improves Emergency Department Efficiency. Joint Commission Journal on Quality and Patient Safety, 36, Chisholm, C. D., Dornfeld, A. M., Nelson, D. R., & Cordell, W. H. (2001). Work interrupted: a comparison of workplace interruptions in emergency departments and primary care offices. Annals of Emergency Medicine, 38(2), Cooper, L. A., Roter, D. L., Johnson, R. L., Ford, D. E., Steinwachs, D. M., & Powe, N. R. (2003). Patient-centered communication, ratings of care, and concordance of patient and physician race. Annals of Internal Medicine, 139(11), Farley, H. L., Baumlin, K. M., Hamedani, A. G., Cheung, D. S., Edwards, M. R., Fuller, D. C., Pines, J. M. (2013). Quality and safety implications of emergency department information systems. Annals of Emergency Medicine, 62(4), doi: /j.annemergmed Fleming, N. S., Becker, E. R., Culler, S. D., Cheng, D., McCorkle, R., Graca, B. Da, & Ballard, D. J. (2014). The impact of electronic health records on workflow and financial measures in primary care practices. Health Services Research, 49(1 Pt 2), doi: / Friedberg, M., Chen, P., Van Busum, K., Aunon, F., Pham, C., Caloyeras, J., Tutty, M. (2013). Factors affecting physician professional satisfaction and their implications for patient care, health systems, and health policy. RAND Corporation: Washington, DC. Grieger, D. L., Cohen, S. H., & Krusch, D. A. (2007). A pilot study to document the return on investment for implementing an ambulatory electronic health record at an academic medical center. Journal of the American College of Surgeons, 205(1), Han, Y. Y., Carcillo, J. A., Venkataraman, S. T., Clark, R. S., Watson, R. S., Nguyen, T. C., Orr, R. A. (2005). Unexpected increased mortality after implementation of a commercially sold computerized physician order entry system. Pediatrics, 116(6), doi:116/6/1506 [pii] /peds Kellermann, A. L., & Jones, S. S. (2013). What it will take to achieve the asyet-unfulfilled promises of health information technology. Health Affairs (Project Hope), 32(1), doi: /hlthaff Kern, L. M., Barrón, Y., Dhopeshwarkar, R. V, Edwards, A., & Kaushal, R. (2013). Electronic health records and ambulatory quality of care. Journal of General Internal Medicine, 28(4), doi: /s Kuperman, G. J., Bobb, A., Payne, T. H., Avery, A. J., Gandhi, T. K., Burns, G., Bates, D. W. (2007). Medication-related clinical decision support in computerized provider order entry systems: a review. Journal of the American Medical Informatics Association : JAMIA, 14(1), doi: /jamia.m2170 Laramee, A. S., Bosek, M., Kasprisin, C. A., & Powers-Phaneuf, T. (2011). Learning from within to ensure a successful implementation of an electronic health record. CIN: Computers, Informatics, Nursing, 29(8), doi: /ncn.0b013e3181fc3fc7 Lowry, S. Z., Ramaiah, M., Gibbons, M. C., Patterson, E. S., & Lewis, V. R. (2013). Toward a Shared Approach for Ensuring Patient Safety with Enhanced Workflow Design for Electronic Health Records Summary of the Workshop (pp. 1 15). Gaithersberg, MD. Office of the National Coordinator for Health Information Technology. (2013). Health IT Dashboard. Pizziferri, L., Kittler, A. F., Volk, L. a, Honour, M. M., Gupta, S., Wang, S., Bates, D. W. (2005). Primary care physician time utilization before and after implementation of an electronic health record: a time-motion study. Journal of Biomedical Informatics, 38(3), doi: /j.jbi Read-Brown, S., Sanders, D. S., Brown, A. S., Yackel, T. R., Choi, D., Tu, D. C., & Chiang, M. F. (2013). Time-motion analysis of clinical nursing documentation of an electronic operating room management system for ophthalmic surgery. In AMIA Annual Symposium (pp ). Washington, D.C. Reed, M., Huang, J., Brand, R., Graetz, I., Neugebauer, R., Fireman, B., Hsu, J. (2013). Implementation of an outpatient electronic health record and emergency department visits, hospitalizations, and office visits among patients with diabetes. JAMA : The Journal of the American Medical Association, 310(10), doi: /jama Shapiro, J. S., Baumlin, K. M., Chawla, N., Genes, N., Godbold, J., Ye, F., & Richardson, L. D. (2010). Emergency Department Information System Implementation and Process Redesign Result in Rapid and Sustained Financial Enhancement at a Large Academic Center. Academic Emergency Medicine, 17(5),
6 2014 International Symposium on Human Factors and Ergonomics in Health Care: Advancing the Cause 49 Sockolow, P. S., Weiner, J. P., Bowles, K. H., & Lehmann, H. P. (2011). A New Instrument for Measuring Clinician Satisfaction With Electronic Health Records. Computers, Informatics, Nursing : CIN, 29(10), doi: /ncn.0b013e31821a1568 Spellman Kennebeck, S., Timm, N., Farrell, M. K., & Spooner, S. A. (2012). Impact of electronic health record implementation on patient flow metrics in a pediatric emergency department. Journal of the American Medical Informatics Association : JAMIA, 19(3), doi: /amiajnl Weil, N. (2007). Hospital emergency departments find relief in IT. InfoWorld. Retrieved from
The Health IT Patient Safety Journey in the United States
 The Health IT Patient Safety Journey in the United States Patricia P. Sengstack DNP, RN-BC, CPHIMS Chief Nursing Informatics Officer Bon Secours Health System Marriottsville, Maryland, USA 1 To Err is
The Health IT Patient Safety Journey in the United States Patricia P. Sengstack DNP, RN-BC, CPHIMS Chief Nursing Informatics Officer Bon Secours Health System Marriottsville, Maryland, USA 1 To Err is
5/29/2015. Stephen Adams, M.D. Professor of Family Medicine CMIO Erlanger Health Systems
 Stephen Adams, M.D. Professor of Family Medicine CMIO Erlanger Health Systems Discuss benefits of EHR use. Discuss negative aspects of EHRs. List situations where EHR usage results in cost savings. Review
Stephen Adams, M.D. Professor of Family Medicine CMIO Erlanger Health Systems Discuss benefits of EHR use. Discuss negative aspects of EHRs. List situations where EHR usage results in cost savings. Review
The Economic Effect of Implementing an EMR in an Outpatient Clinical Setting
 Reprinted from Volume 18, Number 1 Winter 2004 Original Contributions The Economic Effect of Implementing an EMR in an Outpatient Clinical Setting Scott Barlow, MBA, Jeffrey Johnson, MD, Jamie Steck, MBA
Reprinted from Volume 18, Number 1 Winter 2004 Original Contributions The Economic Effect of Implementing an EMR in an Outpatient Clinical Setting Scott Barlow, MBA, Jeffrey Johnson, MD, Jamie Steck, MBA
Presented by Kevin Tolin Scheper
 The information presented in this Webinar is current as of date of live airing April 12, 2012. Presented by Kevin Tolin Scheper Vice President, Professional Services Now is the time to switch Meaningful
The information presented in this Webinar is current as of date of live airing April 12, 2012. Presented by Kevin Tolin Scheper Vice President, Professional Services Now is the time to switch Meaningful
IL-HITREC P.O. Box 755 Sycamore, IL 60178 Phone 815-753-1136 Fax 815-753-2460 email info@ilhitrec.org www.ilhitrec.org
 IL-HITREC P.O. Box 755 Sycamore, IL 60178 Phone 815-753-1136 Fax 815-753-2460 email info@ilhitrec.org www.ilhitrec.org INTRODUCTION BENEFITS CHALLENGES WHY NOW? HOW WE HELP SUMMARY Better patient care
IL-HITREC P.O. Box 755 Sycamore, IL 60178 Phone 815-753-1136 Fax 815-753-2460 email info@ilhitrec.org www.ilhitrec.org INTRODUCTION BENEFITS CHALLENGES WHY NOW? HOW WE HELP SUMMARY Better patient care
Streamline Your Radiology Workflow. With Radiology Information Systems (RIS) and EHR
 Streamline Your Radiology Workflow With Radiology Information Systems (RIS) and EHR 2 Practicing medicine effectively requires transferring large amounts of information quickly, accurately, and securely.
Streamline Your Radiology Workflow With Radiology Information Systems (RIS) and EHR 2 Practicing medicine effectively requires transferring large amounts of information quickly, accurately, and securely.
Harnessing the Untapped Potential of EHR Systems
 CASE STUDY Harnessing the Untapped Potential of EHR Systems TalkChart Transforms the Documentation Efficiency of the Child & Adolescent Psychiatry Department of a Large Academic Institution Electronic
CASE STUDY Harnessing the Untapped Potential of EHR Systems TalkChart Transforms the Documentation Efficiency of the Child & Adolescent Psychiatry Department of a Large Academic Institution Electronic
Electronic Health Record Impact on Eye Clinic Efficiency: A Time and Revenue Study
 Electronic Health Record Impact on Eye Clinic Efficiency: A Time and Revenue Study Matthew Recko, MD Derrick Fung, MD, Kyle Smith, MD, Robert H. Rosa, Jr., MD May 16, 2014 Financial Disclosures Kyle Smith,
Electronic Health Record Impact on Eye Clinic Efficiency: A Time and Revenue Study Matthew Recko, MD Derrick Fung, MD, Kyle Smith, MD, Robert H. Rosa, Jr., MD May 16, 2014 Financial Disclosures Kyle Smith,
Conflict of Interest Disclosure
 Leveraging Clinical Decision Support for Optimal Medication Management Anne M Bobb, BS Pharm., Director Quality Informatics Children s Memorial Hospital, Chicago IL, February 20, 2012 DISCLAIMER: The views
Leveraging Clinical Decision Support for Optimal Medication Management Anne M Bobb, BS Pharm., Director Quality Informatics Children s Memorial Hospital, Chicago IL, February 20, 2012 DISCLAIMER: The views
Electronic Medical Record Position Paper December 2014
 Electronic Medical Record Position Paper December 2014 Purpose: The purpose of this Electronic Medical Record (EMR) position paper is to present an overview of the electronic medical record along with
Electronic Medical Record Position Paper December 2014 Purpose: The purpose of this Electronic Medical Record (EMR) position paper is to present an overview of the electronic medical record along with
Electronic Prescribing at the Point of Care: A Time Motion Study in the Primary Care Setting
 Health Services Research r Health Research and Educational Trust DOI: 10.1111/j.1475-6773.2009.01063.x RESEARCH ARTICLE Electronic Prescribing at the Point of Care: A Time Motion Study in the Primary Care
Health Services Research r Health Research and Educational Trust DOI: 10.1111/j.1475-6773.2009.01063.x RESEARCH ARTICLE Electronic Prescribing at the Point of Care: A Time Motion Study in the Primary Care
Transforming Healthcare in Emerging Markets with EMR adoption
 Transforming Healthcare in Emerging Markets with EMR adoption Author Ann Geo Thekkel User Experience. Accenture, India Ann.geothekkel@accenture.com Abstract Compromising 24 countries, 35 percent of the
Transforming Healthcare in Emerging Markets with EMR adoption Author Ann Geo Thekkel User Experience. Accenture, India Ann.geothekkel@accenture.com Abstract Compromising 24 countries, 35 percent of the
How To Study The Unintended Consequences Of Emit
 Association for Information Systems AIS Electronic Library (AISeL) PACIS 2012 Proceedings Pacific Asia Conference on Information Systems (PACIS) 7-15-2012 Issues Of Unintended Consequences Of Electronic
Association for Information Systems AIS Electronic Library (AISeL) PACIS 2012 Proceedings Pacific Asia Conference on Information Systems (PACIS) 7-15-2012 Issues Of Unintended Consequences Of Electronic
How does your EHR tie into Patient Safety?
 How does your EHR tie into Patient Safety? 2 nd Annual Wyoming Patient Safety Summit Casper, Wyoming November 15, 2013 David S Hanekom, M.D., F.A.C.P., C.M.P.E Chief Medical Officer MDdatacor, Inc. The
How does your EHR tie into Patient Safety? 2 nd Annual Wyoming Patient Safety Summit Casper, Wyoming November 15, 2013 David S Hanekom, M.D., F.A.C.P., C.M.P.E Chief Medical Officer MDdatacor, Inc. The
Better patient care and better practice management
 www.hitecla.org INTRODUCTION BENEFITS CHALLENGES WHY NOW? INCENTIVES FOR PROVIDERS HOW WE HELP SUMMARY Better patient care and better practice management Using Electronic Health Records in a meaningful
www.hitecla.org INTRODUCTION BENEFITS CHALLENGES WHY NOW? INCENTIVES FOR PROVIDERS HOW WE HELP SUMMARY Better patient care and better practice management Using Electronic Health Records in a meaningful
Sentara Healthcare EMR: Our Journey. Bert Reese, CIO and Senior Vice President
 Sentara Healthcare EMR: Our Journey Bert Reese, CIO and Senior Vice President Sentara Healthcare 123-year not-for-profit mission 10 hospitals; 2,349 beds; 3,700 physicians on staff 10 long term care/assisted
Sentara Healthcare EMR: Our Journey Bert Reese, CIO and Senior Vice President Sentara Healthcare 123-year not-for-profit mission 10 hospitals; 2,349 beds; 3,700 physicians on staff 10 long term care/assisted
Post-Implementation EMR Evaluation for the Beta Ambulatory Care Clinic Proposed Plan Jul 6/2012, Version 2.0
 1. Purpose and Scope Post-Implementation EMR Evaluation for the Beta Ambulatory Care Clinic Proposed Plan Jul 6/2012, Version 2.0 This document describes our proposed plan to conduct a formative evaluation
1. Purpose and Scope Post-Implementation EMR Evaluation for the Beta Ambulatory Care Clinic Proposed Plan Jul 6/2012, Version 2.0 This document describes our proposed plan to conduct a formative evaluation
Health Information Technology and the National Quality Agenda. Daphne Ayn Bascom, MD PhD Chief Clinical Systems Officer Medical Operations
 Health Information Technology and the National Quality Agenda Daphne Ayn Bascom, MD PhD Chief Clinical Systems Officer Medical Operations Institute of Medicine Definition of Quality "The degree to which
Health Information Technology and the National Quality Agenda Daphne Ayn Bascom, MD PhD Chief Clinical Systems Officer Medical Operations Institute of Medicine Definition of Quality "The degree to which
Successful EHR Usage. It s not about the bits and the bytes, nor the size of the practice. Practice culture drives EHR success.
 Successful EHR Usage It s not about the bits and the bytes, nor the size of the practice. Practice culture drives EHR success. WHITE PAPER Successful EHR Usage It s not about the bits and the bytes, nor
Successful EHR Usage It s not about the bits and the bytes, nor the size of the practice. Practice culture drives EHR success. WHITE PAPER Successful EHR Usage It s not about the bits and the bytes, nor
Using Public Health Evaluation Models to Assess Health IT Implementations
 Using Public Health Evaluation Models to Assess Health IT Implementations September 2011 White Paper Prepared for Healthcare Information and Management Systems Society 33 West Monroe Street Suite 1700
Using Public Health Evaluation Models to Assess Health IT Implementations September 2011 White Paper Prepared for Healthcare Information and Management Systems Society 33 West Monroe Street Suite 1700
Hospital IT Expenses and Budgets Related to Clinical Sophistication. Market Findings from HIMSS Analytics
 Hospital IT Expenses and Budgets Related to Clinical Sophistication Market Findings from HIMSS Analytics Table of Contents 2 3 4 8 13 14 Executive Summary Expense Metrics Used for this Research Operating
Hospital IT Expenses and Budgets Related to Clinical Sophistication Market Findings from HIMSS Analytics Table of Contents 2 3 4 8 13 14 Executive Summary Expense Metrics Used for this Research Operating
Workflow Analysis and Redesign for Electronic Health Records (EHRs) Tools, Examples, and Discussion for RHITND Grantees
 600 East Superior Street, Suite 404 I Duluth, MN 55802 I Ph. 800.997.6685 or 218.727.9390 I www.ruralcenter.org Workflow Analysis and Redesign for Electronic Health Records (EHRs) Tools, Examples, and
600 East Superior Street, Suite 404 I Duluth, MN 55802 I Ph. 800.997.6685 or 218.727.9390 I www.ruralcenter.org Workflow Analysis and Redesign for Electronic Health Records (EHRs) Tools, Examples, and
Addressing the State of the Electronic Health Record (EHR)
 Addressing the State of the Electronic Health Record (EHR) Agenda Definitions Attributes Differences Adoption Model Current State Challenges Implementation considerations What is it? EMR CMR EHR EPR PHR
Addressing the State of the Electronic Health Record (EHR) Agenda Definitions Attributes Differences Adoption Model Current State Challenges Implementation considerations What is it? EMR CMR EHR EPR PHR
A Review on Usability Features for Designing Electronic Health Records. Luis Bernardo Villa Ivan Cabezas
 A Review on Usability Features for Designing Electronic Health Records Luis Bernardo Villa Ivan Cabezas 1 UNIVERSIDAD DE SAN BUENAVENTURA CALI 2 Content Introduction Problem Statement Usability Standards
A Review on Usability Features for Designing Electronic Health Records Luis Bernardo Villa Ivan Cabezas 1 UNIVERSIDAD DE SAN BUENAVENTURA CALI 2 Content Introduction Problem Statement Usability Standards
Electronic Health Record Use: Health Care Providers Perception at a Community Health Center
 Electronic Health Record Use: Health Care Providers Perception at a Community Health Center Gina Robinson D.O. Candidate 2017 Arizona College of Osteopathic Medicine at Midwestern University GE-National
Electronic Health Record Use: Health Care Providers Perception at a Community Health Center Gina Robinson D.O. Candidate 2017 Arizona College of Osteopathic Medicine at Midwestern University GE-National
EHRs and Contexts of Use
 2 EHRs and Contexts of Use A Providers Perspective on EHR User Experience Presented by March 2013 1 EHRs and Contexts of Use It s not a new concept. Most modern EHRs, descending from products designed
2 EHRs and Contexts of Use A Providers Perspective on EHR User Experience Presented by March 2013 1 EHRs and Contexts of Use It s not a new concept. Most modern EHRs, descending from products designed
EMR Physician Planning Guide. Version 1.2
 Version 1.2 About this Guide OntarioMD has created the Physician EMR Planning Guide to assist physicians who are in the process of planning and implementing an EMR. The Guide provides high level advice
Version 1.2 About this Guide OntarioMD has created the Physician EMR Planning Guide to assist physicians who are in the process of planning and implementing an EMR. The Guide provides high level advice
SUMMARY OF AAO MEMBERSHIP SURVEY ON ELECTRONIC HEALTH RECORDS
 SUMMARY OF AAO MEMBERSHIP SURVEY ON ELECTRONIC HEALTH RECORDS EXECUTIVE SUMMARY: The Academy and its contractor, Medical Group Management Association (MGMA), conducted a survey of the membership on the
SUMMARY OF AAO MEMBERSHIP SURVEY ON ELECTRONIC HEALTH RECORDS EXECUTIVE SUMMARY: The Academy and its contractor, Medical Group Management Association (MGMA), conducted a survey of the membership on the
A Long Way to Go for EMR Usability By: Jessica Green
 Topic Overview & Introduction: A Long Way to Go for EMR Usability By: Jessica Green With the ever increasing implementation of Electronic Medical and Health Records (EMR and EHR) systems into hospitals,
Topic Overview & Introduction: A Long Way to Go for EMR Usability By: Jessica Green With the ever increasing implementation of Electronic Medical and Health Records (EMR and EHR) systems into hospitals,
Electronic Medical Record Adoption: Does usability help? Nicole Bammel. Med Info 409. Northwestern University
 Electronic Medical Record Adoption: Does usability help? Nicole Bammel Med Info 409 Northwestern University November 23, 2014 Introduction Macomb Hospital is a 100 bed hospital with 150 health care workers
Electronic Medical Record Adoption: Does usability help? Nicole Bammel Med Info 409 Northwestern University November 23, 2014 Introduction Macomb Hospital is a 100 bed hospital with 150 health care workers
ehealth, HIS, etc ehealth All information about health HMIS mhealth HIS Statistical IS Credited: Karl Brown, Rockefeller Foundation
 ehealth, HIS, etc Statistical IS Health Informatics: Formal discipline that studies use of information in health All information about health HIS HMIS ehealth mhealth Tele-medicine Enterprise architecture:
ehealth, HIS, etc Statistical IS Health Informatics: Formal discipline that studies use of information in health All information about health HIS HMIS ehealth mhealth Tele-medicine Enterprise architecture:
Accountable Care: Implications for Managing Health Information. Quality Healthcare Through Quality Information
 Accountable Care: Implications for Managing Health Information Quality Healthcare Through Quality Information Introduction Healthcare is currently experiencing a critical shift: away from the current the
Accountable Care: Implications for Managing Health Information Quality Healthcare Through Quality Information Introduction Healthcare is currently experiencing a critical shift: away from the current the
Building More Usable Electronic Health Records (EHRs) Supporting the Needs of Developers Focus on Faster & Usable Clinical Documentation
 Building More Usable Electronic Health Records (EHRs) Supporting the Needs of Developers Focus on Faster & Usable Clinical Documentation Jorge A. Ferrer, M.D., M.B.A. Medical Informaticist Chief Health
Building More Usable Electronic Health Records (EHRs) Supporting the Needs of Developers Focus on Faster & Usable Clinical Documentation Jorge A. Ferrer, M.D., M.B.A. Medical Informaticist Chief Health
How To Understand The Barriers And Facilitators To The Effective Use Of An Ehr
 Barriers and Facilitators to the Effective Use of Electronic Health Records A case study of barriers and facilitators to the effective use of the electronic health records as measured by providers ability
Barriers and Facilitators to the Effective Use of Electronic Health Records A case study of barriers and facilitators to the effective use of the electronic health records as measured by providers ability
EHR: Pearls and Pitfalls. Sue Wolver, MD FACP Associate Professor, General Internal Medicine Assistant CMIO Virginia ACP March 7, 2015
 EHR: Pearls and Pitfalls Sue Wolver, MD FACP Associate Professor, General Internal Medicine Assistant CMIO Virginia ACP March 7, 2015 1 Conflict of interest None 2 Objectives The Why Pearls: What has the
EHR: Pearls and Pitfalls Sue Wolver, MD FACP Associate Professor, General Internal Medicine Assistant CMIO Virginia ACP March 7, 2015 1 Conflict of interest None 2 Objectives The Why Pearls: What has the
Electronic Medical Record Customization and the Impact Upon Chart Completion Rates
 338 May 2010 Family Medicine Improving Workflow Electronic Medical Record Customization and the Impact Upon Chart Completion Rates Kevin J. Bennett, PhD; Christian Steen, MD Objective: The study s objctive
338 May 2010 Family Medicine Improving Workflow Electronic Medical Record Customization and the Impact Upon Chart Completion Rates Kevin J. Bennett, PhD; Christian Steen, MD Objective: The study s objctive
A National Web Conference on Managing Change to Achieve Successful Health IT Implementation. July 15, 2014 2:30pm 4:00pm ET
 A National Web Conference on Managing Change to Achieve Successful Health IT Implementation July 15, 2014 2:30pm 4:00pm ET Moderator and Presenters Disclosures Moderator: Teresa Zayas Cabán, Ph.D.* Agency
A National Web Conference on Managing Change to Achieve Successful Health IT Implementation July 15, 2014 2:30pm 4:00pm ET Moderator and Presenters Disclosures Moderator: Teresa Zayas Cabán, Ph.D.* Agency
Return on Investment Potential EHRs and Iowa s HIE
 Return on Investment Potential EHRs and Iowa s HIE Health information technology (health IT) holds the potential to increase the efficiency, cost effectiveness, quality, and safety of our health care system.
Return on Investment Potential EHRs and Iowa s HIE Health information technology (health IT) holds the potential to increase the efficiency, cost effectiveness, quality, and safety of our health care system.
Clintegrity 360 QualityAnalytics
 WHITE PAPER Clintegrity 360 QualityAnalytics Bridging Clinical Documentation and Quality of Care HEALTHCARE EXECUTIVE SUMMARY The US Healthcare system is undergoing a gradual, but steady transformation.
WHITE PAPER Clintegrity 360 QualityAnalytics Bridging Clinical Documentation and Quality of Care HEALTHCARE EXECUTIVE SUMMARY The US Healthcare system is undergoing a gradual, but steady transformation.
Certificate Course in Electronic Medical Records Administration
 Course Name Certificate Course in Electronic Medical Records Administration Contact Hours: 45 Course Description This course is approved by the Association for Healthcare Documentation Integrity (AHDI)
Course Name Certificate Course in Electronic Medical Records Administration Contact Hours: 45 Course Description This course is approved by the Association for Healthcare Documentation Integrity (AHDI)
WHITE PAPER. QualityAnalytics. Bridging Clinical Documentation and Quality of Care
 WHITE PAPER QualityAnalytics Bridging Clinical Documentation and Quality of Care 2 EXECUTIVE SUMMARY The US Healthcare system is undergoing a gradual, but steady transformation. At the center of this transformation
WHITE PAPER QualityAnalytics Bridging Clinical Documentation and Quality of Care 2 EXECUTIVE SUMMARY The US Healthcare system is undergoing a gradual, but steady transformation. At the center of this transformation
The Paperless Project - A Practical Paper
 IS CPOE SAFE FOR PATIENTS? An early experience. Leah Brown MSN, RN and James Frye MBA Abstract In a 1999 report from the Committee on Quality Healthcare in America, To Err is Human [1], indicated that
IS CPOE SAFE FOR PATIENTS? An early experience. Leah Brown MSN, RN and James Frye MBA Abstract In a 1999 report from the Committee on Quality Healthcare in America, To Err is Human [1], indicated that
EHR IMPLEMENTATION SURVEY: Proactive Consideration and Planning Lead to Successful EHR Implementation
 TEKsystems Healthcare Services is dedicated to providing workforce planning, human capital management and professional IT services to the healthcare industry. Utilizing our suite of services, including
TEKsystems Healthcare Services is dedicated to providing workforce planning, human capital management and professional IT services to the healthcare industry. Utilizing our suite of services, including
Implementation of Electronic Patient Records Lessons Learned from the Literature (05/23/04)
 In association with Simon Fraser University & the Vancouver Coastal Health Research Institute FOR CIRCULATION X NOT FOR CIRCULATION Implementation of Electronic Patient Records Lessons Learned from the
In association with Simon Fraser University & the Vancouver Coastal Health Research Institute FOR CIRCULATION X NOT FOR CIRCULATION Implementation of Electronic Patient Records Lessons Learned from the
Experiences Implementing Ambulatory EMRs and Early Benefits
 Experiences Implementing Ambulatory EMRs and Early Benefits Colleen Rogers, Chad Leaver and Simon Hagens ehealth 2015 Today s Presentation Infoway and Investment in Ambulatory EMR Adoption Progress Emerging
Experiences Implementing Ambulatory EMRs and Early Benefits Colleen Rogers, Chad Leaver and Simon Hagens ehealth 2015 Today s Presentation Infoway and Investment in Ambulatory EMR Adoption Progress Emerging
Executive Checklist: Four ways to leverage EMR to improve patient outcomes, increase satisfaction and control costs.
 White Paper Executive Checklist: Four ways to leverage EMR to improve patient outcomes, increase satisfaction and control costs. Brendon Buckley Healthcare Enterprise Solutions Manager Lorrie LiBrizzi
White Paper Executive Checklist: Four ways to leverage EMR to improve patient outcomes, increase satisfaction and control costs. Brendon Buckley Healthcare Enterprise Solutions Manager Lorrie LiBrizzi
Tips and Strategies on Handoffs
 Tips and Strategies on Handoffs In 2007, the Handoffs & Transitions Learning Network (H&T) was established to support the mid-atlantic healthcare community in tackling the complex problem of handoffs and
Tips and Strategies on Handoffs In 2007, the Handoffs & Transitions Learning Network (H&T) was established to support the mid-atlantic healthcare community in tackling the complex problem of handoffs and
Known Pitfalls and Proven Methods for a Successful EMR Implementation
 Known Pitfalls and Proven Methods for a Successful EMR Implementation Deciding to adopt an EMR is one of the most important decisions made by any practice. The transition to an EMR from a paper system
Known Pitfalls and Proven Methods for a Successful EMR Implementation Deciding to adopt an EMR is one of the most important decisions made by any practice. The transition to an EMR from a paper system
Effectively Managing EHR Projects: Guidelines for Successful Implementation
 Phoenix Health Systems Effectively Managing EHR Projects: Guidelines for Successful Implementation Introduction Effectively managing any EHR (Electronic Health Record) implementation can be challenging.
Phoenix Health Systems Effectively Managing EHR Projects: Guidelines for Successful Implementation Introduction Effectively managing any EHR (Electronic Health Record) implementation can be challenging.
CNPE DRAFT POSITION STATEMENT (04-25-2011) Nurses Involvement With the EHR: Advocating Patient Safety
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 CNPE DRAFT POSITION STATEMENT (04-25-2011) Nurses Involvement With the EHR:
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 CNPE DRAFT POSITION STATEMENT (04-25-2011) Nurses Involvement With the EHR:
Testimony to the Meaningful Use Workgroup, ONC. Panel 1: Current HIT Support of Care Coordination
 Testimony to the Meaningful Use Workgroup, ONC Panel 1: Current HIT Support of Care Coordination August 5, 2010 Dr. Bates, Dr. Tang, Dr. Hripcsak, and Members of the Meaningful Use Workgroup: Thank you
Testimony to the Meaningful Use Workgroup, ONC Panel 1: Current HIT Support of Care Coordination August 5, 2010 Dr. Bates, Dr. Tang, Dr. Hripcsak, and Members of the Meaningful Use Workgroup: Thank you
THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION. 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams
 THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams Agenda Overview Impact of HIT on Patient-Centered Care (PCC)
THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams Agenda Overview Impact of HIT on Patient-Centered Care (PCC)
The Computer Will See You Now: How IT
 The Computer Will See You Now: How IT Affects Doctor-Patient Communication Clinicians Patients Exam Room Computers Richard M. Frankel, PhD Research Scientist Center for Implementing Evidence Based Practice
The Computer Will See You Now: How IT Affects Doctor-Patient Communication Clinicians Patients Exam Room Computers Richard M. Frankel, PhD Research Scientist Center for Implementing Evidence Based Practice
EMR BIG BOX DISSATISFACTION Pushes Demand for Specialty Specific Systems
 WHITE PAPER EMR BIG BOX DISSATISFACTION Pushes Demand for Specialty Specific Systems ONE SIZE DOES NOT FIT ALL General Practice EMR Dissatisfaction Pushes ONE SIZE DOES NOT FIT ALL Due to the unique needs
WHITE PAPER EMR BIG BOX DISSATISFACTION Pushes Demand for Specialty Specific Systems ONE SIZE DOES NOT FIT ALL General Practice EMR Dissatisfaction Pushes ONE SIZE DOES NOT FIT ALL Due to the unique needs
The Crucial Role of the Nurse in EHR Implementation
 MED3OOO White Paper The Crucial Role of the Nurse in EHR Implementation By Jay Anders, M.D., Chief Medical Information Officer, and Terry Daly, R.N., Vice President of Clinical Systems As residents coming
MED3OOO White Paper The Crucial Role of the Nurse in EHR Implementation By Jay Anders, M.D., Chief Medical Information Officer, and Terry Daly, R.N., Vice President of Clinical Systems As residents coming
The Physician Productivity Hit
 WHITE PAPER The Physician Productivity Hit Addressing the Efficiency Failures and Design Flaws of EHR Systems in Medical Practices Abstract Immediate and dramatic loss of productivity is one of the most
WHITE PAPER The Physician Productivity Hit Addressing the Efficiency Failures and Design Flaws of EHR Systems in Medical Practices Abstract Immediate and dramatic loss of productivity is one of the most
Medweb Telemedicine 667 Folsom Street, San Francisco, CA 94107 Phone: 415.541.9980 Fax: 415.541.9984 www.medweb.com
 Medweb Telemedicine 667 Folsom Street, San Francisco, CA 94107 Phone: 415.541.9980 Fax: 415.541.9984 www.medweb.com Meaningful Use On July 16 2009, the ONC Policy Committee unanimously approved a revised
Medweb Telemedicine 667 Folsom Street, San Francisco, CA 94107 Phone: 415.541.9980 Fax: 415.541.9984 www.medweb.com Meaningful Use On July 16 2009, the ONC Policy Committee unanimously approved a revised
HIMSS EMR Usability Evaluation Guide For Clinicians Practices
 HIMSS EMR Usability Evaluation Guide For Clinicians Practices Goal of this Guide This document has been prepared as an aid to practices engaged in selection of an electronic medical record (EMR) system.
HIMSS EMR Usability Evaluation Guide For Clinicians Practices Goal of this Guide This document has been prepared as an aid to practices engaged in selection of an electronic medical record (EMR) system.
Electronic Medical Records vs. Electronic Health Records: Yes, There Is a Difference. A HIMSS Analytics TM White Paper. By Dave Garets and Mike Davis
 Electronic Medical Records vs. Electronic Health Records: Yes, There Is a Difference A HIMSS Analytics TM White Paper By Dave Garets and Mike Davis Updated January 26, 2006 HIMSS Analytics, LLC 230 E.
Electronic Medical Records vs. Electronic Health Records: Yes, There Is a Difference A HIMSS Analytics TM White Paper By Dave Garets and Mike Davis Updated January 26, 2006 HIMSS Analytics, LLC 230 E.
New Self-Assessment Guides Help Ensure Safer Electronic Health Records Dean F. Sittig, PhD
 New Self-Assessment Guides Help Ensure Safer Electronic Health Records Dean F. Sittig, PhD DISCLAIMER: The views and opinions expressed in this presentation are those of the author and do not necessarily
New Self-Assessment Guides Help Ensure Safer Electronic Health Records Dean F. Sittig, PhD DISCLAIMER: The views and opinions expressed in this presentation are those of the author and do not necessarily
Evaluating the AMIA-OHSU 10x10 Program to Train Healthcare Professionals in Medical Informatics Sue S. Feldman, RN, MEd 1, William Hersh, MD 2
 Evaluating the AMIA-OHSU 10x10 Program to Train Healthcare Professionals in Medical Informatics Sue S. Feldman, RN, MEd 1, William Hersh, MD 2 1 Claremont Graduate University, Claremont, CA; 2 Oregon Health
Evaluating the AMIA-OHSU 10x10 Program to Train Healthcare Professionals in Medical Informatics Sue S. Feldman, RN, MEd 1, William Hersh, MD 2 1 Claremont Graduate University, Claremont, CA; 2 Oregon Health
The MARYLAND HEALTH CARE COMMISSION
 The MARYLAND HEALTH CARE COMMISSION February 2012 The main goal of using technology in the health care arena is to improve the quality of patient care Adopting EHRs can enhance patient safety through:
The MARYLAND HEALTH CARE COMMISSION February 2012 The main goal of using technology in the health care arena is to improve the quality of patient care Adopting EHRs can enhance patient safety through:
Medical Device Integration with an Ambulatory Electronic Health Record System
 Medical Device Integration with an Ambulatory Electronic Health Record System Alliance of Chicago Community Health Services Welch Allyn INTRODUCTION A fully functional electronic health record (EHR) system
Medical Device Integration with an Ambulatory Electronic Health Record System Alliance of Chicago Community Health Services Welch Allyn INTRODUCTION A fully functional electronic health record (EHR) system
Implementation of EMR
 Implementation of EMR Paul Steven Collins MD FACS RPVI Assistant Clinical Professor of Surgery University of South Florida Bay Surgical Specialists St Petersburg, Fl No Magic Formula However, Fail to Plan,
Implementation of EMR Paul Steven Collins MD FACS RPVI Assistant Clinical Professor of Surgery University of South Florida Bay Surgical Specialists St Petersburg, Fl No Magic Formula However, Fail to Plan,
Where to Begin? Auditing the Current EHR System
 Chapter 1 Where to Begin? Auditing the Current EHR System After implementation, allow for a period of stabilization, so physicians and employees can gain more comfort using the electronic health record
Chapter 1 Where to Begin? Auditing the Current EHR System After implementation, allow for a period of stabilization, so physicians and employees can gain more comfort using the electronic health record
Variation in Use of Informatics Tools Among Providers in a Diabetes Clinic
 Variation in Use of Informatics Tools Among Providers in a Diabetes Clinic Kim M. Unertl MS, Matthew Weinger MD, Kevin Johnson MD MS Dept. of Biomedical Informatics, Vanderbilt University Medical Center,
Variation in Use of Informatics Tools Among Providers in a Diabetes Clinic Kim M. Unertl MS, Matthew Weinger MD, Kevin Johnson MD MS Dept. of Biomedical Informatics, Vanderbilt University Medical Center,
Health Information Technology Toolkit for Family Physicians
 Health Information Technology Toolkit for Family Physicians Health Information Technology in Primary Care: A Bibliography "Crossing the Quality Chasm: A New Health System for the 21st Century." Washington,
Health Information Technology Toolkit for Family Physicians Health Information Technology in Primary Care: A Bibliography "Crossing the Quality Chasm: A New Health System for the 21st Century." Washington,
AN ANALYSIS OF ELECTRONIC HEALTH RECORD-RELATED PATIENT SAFETY CONCERNS
 AN ANALYSIS OF ELECTRONIC HEALTH RECORD-RELATED PATIENT SAFETY CONCERNS 1 HARDEEP SINGH, MD, MPH MICHAEL E. DEBAKEY VA MEDICAL CENTER BAYLOR COLLEGE OF MEDICINE DEAN SITTIG, PHD UNIVERSITY OF TEXAS HEALTH
AN ANALYSIS OF ELECTRONIC HEALTH RECORD-RELATED PATIENT SAFETY CONCERNS 1 HARDEEP SINGH, MD, MPH MICHAEL E. DEBAKEY VA MEDICAL CENTER BAYLOR COLLEGE OF MEDICINE DEAN SITTIG, PHD UNIVERSITY OF TEXAS HEALTH
EHR 101. A Guide to Successfully Implementing Electronic Health Records
 EHR 101 A Guide to Successfully Implementing Electronic Health Records Electronic health records are the inevitable next step in the continued progress of U.S. healthcare. Medicine may be the most information-intensive
EHR 101 A Guide to Successfully Implementing Electronic Health Records Electronic health records are the inevitable next step in the continued progress of U.S. healthcare. Medicine may be the most information-intensive
Evidenced Based Nursing: Electronic Medical Charting and Patient Safety
 Evidenced Based Nursing: Electronic Medical Charting and Patient Safety Presented By Nicole Chambers, Sharon Herring, Sheila Lucas, and Shelley Meyerholtz Introduction In the 1999 publication of To Err
Evidenced Based Nursing: Electronic Medical Charting and Patient Safety Presented By Nicole Chambers, Sharon Herring, Sheila Lucas, and Shelley Meyerholtz Introduction In the 1999 publication of To Err
Enabling Healthcare in Out-Patient Settings and The Patient Centered Medical Home of the Future
 Enabling Healthcare in Out-Patient Settings and The Patient Centered Medical Home of the Future Gregory J. Raglow, MD, FAAFP Group Health Informatics Officer Abu Dhabi Health Services SEHA Objectives List
Enabling Healthcare in Out-Patient Settings and The Patient Centered Medical Home of the Future Gregory J. Raglow, MD, FAAFP Group Health Informatics Officer Abu Dhabi Health Services SEHA Objectives List
A Pilot Study to Document the Return on Investment for Implementing an Ambulatory Electronic Health Record at an Academic Medical Center
 A Pilot Study to Document the Return on Investment for Implementing an Ambulatory Electronic Health Record at an Academic Medical Center Dara L Grieger, MD, Stephen H Cohen, MD, CPE, David A Krusch, MD,
A Pilot Study to Document the Return on Investment for Implementing an Ambulatory Electronic Health Record at an Academic Medical Center Dara L Grieger, MD, Stephen H Cohen, MD, CPE, David A Krusch, MD,
Improving Government Websites and Surveys With Usability Testing and User Experience Research
 Introduction Improving Government Websites and Surveys With Usability Testing and User Experience Research Jennifer Romano Bergstrom, Jonathan Strohl Fors Marsh Group 1010 N Glebe Rd., Suite 510, Arlington,
Introduction Improving Government Websites and Surveys With Usability Testing and User Experience Research Jennifer Romano Bergstrom, Jonathan Strohl Fors Marsh Group 1010 N Glebe Rd., Suite 510, Arlington,
UAB HEALTH SYSTEM AMBULATORY EHR IMPLEMENTATION
 UAB HEALTH SYSTEM AMBULATORY EHR IMPLEMENTATION Richard Rosenthal, MD Associate Chief of Staff Ambulatory Services Associate Professor of Medicine Department of Medicine Endocrinology Agenda About UAB
UAB HEALTH SYSTEM AMBULATORY EHR IMPLEMENTATION Richard Rosenthal, MD Associate Chief of Staff Ambulatory Services Associate Professor of Medicine Department of Medicine Endocrinology Agenda About UAB
Integrating A3 Reports and the House of Quality: Improving Workflow in the Recovery Room Using Information Technology
 416 Medical Informatics in a United and Healthy Europe K.-P. Adlassnig et al. (Eds.) IOS Press, 2009 2009 European Federation for Medical Informatics. All rights reserved. doi:10.3233/978-1-60750-044-5-416
416 Medical Informatics in a United and Healthy Europe K.-P. Adlassnig et al. (Eds.) IOS Press, 2009 2009 European Federation for Medical Informatics. All rights reserved. doi:10.3233/978-1-60750-044-5-416
Mona Osman MD, MPH, MBA
 Mona Osman MD, MPH, MBA Objectives To define an Electronic Medical Record (EMR) To demonstrate the benefits of EMR To introduce the Lebanese Society of Family Medicine- EMR Reality Check The healthcare
Mona Osman MD, MPH, MBA Objectives To define an Electronic Medical Record (EMR) To demonstrate the benefits of EMR To introduce the Lebanese Society of Family Medicine- EMR Reality Check The healthcare
Using Document Imaging to Make Healthcare Better Business
 Using Document Imaging to Make Healthcare Better Business A Canon White Paper 2005 Canon U.S.A., Inc. No part of the publication may be reproduced, stored in a retrieval system, or transmitted in any form
Using Document Imaging to Make Healthcare Better Business A Canon White Paper 2005 Canon U.S.A., Inc. No part of the publication may be reproduced, stored in a retrieval system, or transmitted in any form
OPTIMIZING THE USE OF YOUR ELECTRONIC HEALTH RECORD. A collaborative training offered by Highmark and the Pittsburgh Regional Health Initiative
 OPTIMIZING THE USE OF YOUR ELECTRONIC HEALTH RECORD A collaborative training offered by Highmark and the Pittsburgh Regional Health Initiative Introductions Disclosures Successful completion of training
OPTIMIZING THE USE OF YOUR ELECTRONIC HEALTH RECORD A collaborative training offered by Highmark and the Pittsburgh Regional Health Initiative Introductions Disclosures Successful completion of training
Introduction. Our world has been radically transformed by digital technology We live in an age of information where everything is a click away.
 Introduction Our world has been radically transformed by digital technology We live in an age of information where everything is a click away. Medicine is an area full of information that has yet to fully
Introduction Our world has been radically transformed by digital technology We live in an age of information where everything is a click away. Medicine is an area full of information that has yet to fully
Prospective EHR-based clinical trials: The challenge of missing data
 MS #16180 Prospective EHR-based clinical trials: The challenge of missing data Hadi Kharrazi MHI, MD, PhD*, Chenguang Wang, PhD** and Daniel Scharfstein, ScD*** Johns Hopkins University * Department of
MS #16180 Prospective EHR-based clinical trials: The challenge of missing data Hadi Kharrazi MHI, MD, PhD*, Chenguang Wang, PhD** and Daniel Scharfstein, ScD*** Johns Hopkins University * Department of
Microsoft Amalga HIS Electronic Medical Record
 m Microsoft Amalga HIS Electronic Medical Record The Microsoft Amalga Hospital Information System (HIS) revolves around an electronic medical record (EMR) providing a comprehensive view into a patient
m Microsoft Amalga HIS Electronic Medical Record The Microsoft Amalga Hospital Information System (HIS) revolves around an electronic medical record (EMR) providing a comprehensive view into a patient
Online Supplement to Clinical Peer Review Programs Impact on Quality and Safety in U.S. Hospitals, by Marc T. Edwards, MD
 Online Supplement to Clinical Peer Review Programs Impact on Quality and Safety in U.S. Hospitals, by Marc T. Edwards, MD Journal of Healthcare Management 58(5), September/October 2013 Tabulated Survey
Online Supplement to Clinical Peer Review Programs Impact on Quality and Safety in U.S. Hospitals, by Marc T. Edwards, MD Journal of Healthcare Management 58(5), September/October 2013 Tabulated Survey
SAFER Guides: Safety Assurance Factors for EHR Resilience
 SAFER Guides: Safety Assurance Factors for EHR Resilience Kathy Kenyon, JD MA, Office of the National Coordinator Joan Ash, PhD MLS, MS, MBA, Oregon Health & Science University Hardeep Singh, MD MPH, Houston
SAFER Guides: Safety Assurance Factors for EHR Resilience Kathy Kenyon, JD MA, Office of the National Coordinator Joan Ash, PhD MLS, MS, MBA, Oregon Health & Science University Hardeep Singh, MD MPH, Houston
Special Topics in Vendor- Specific Systems. Outline. Results Review. Unit 4 EHR Functionality. EHR functionality. Results Review
 Special Topics in Vendor- Specific Systems Unit 4 EHR Functionality EHR functionality Results Review Outline Computerized Provider Order Entry (CPOE) Documentation Billing Messaging 2 Results Review Laboratory
Special Topics in Vendor- Specific Systems Unit 4 EHR Functionality EHR functionality Results Review Outline Computerized Provider Order Entry (CPOE) Documentation Billing Messaging 2 Results Review Laboratory
Errors Associated with the Use of E-PrescribingE
 Errors Associated with the Use of E-PrescribingE Eric Poon MD, MPH IS Director of Clinical Informatics, Associate Physician, Brigham and Women s s Hospital, Boston, MA Assistant Professor, Harvard Medical
Errors Associated with the Use of E-PrescribingE Eric Poon MD, MPH IS Director of Clinical Informatics, Associate Physician, Brigham and Women s s Hospital, Boston, MA Assistant Professor, Harvard Medical
Understanding the Role of Physician-Focused At-The-Elbow Support During EMR Go-Live
 Understanding the Role of Physician-Focused At-The-Elbow Support During EMR Go-Live Learnings from a mid-sized hospital Epic EMR Implementation. Contents Data Collection... 1 Results... 2...2 Support Events
Understanding the Role of Physician-Focused At-The-Elbow Support During EMR Go-Live Learnings from a mid-sized hospital Epic EMR Implementation. Contents Data Collection... 1 Results... 2...2 Support Events
Attitudes of Academic-based and Community-based Physicians Regarding EMR Use During Outpatient Encounters
 Attitudes of Academic-based and Community-based Physicians Regarding EMR Use During Outpatient Encounters Louis E. Penrod, MD' and Cynthia S. Gadd, PhD2 'Departnent ofphysical Medicine and Rehabilitation,
Attitudes of Academic-based and Community-based Physicians Regarding EMR Use During Outpatient Encounters Louis E. Penrod, MD' and Cynthia S. Gadd, PhD2 'Departnent ofphysical Medicine and Rehabilitation,
EHR Implementation Best Practices: An EHR implementation that increases efficiencies versus an EHR that is under utilized, abandoned or replaced.
 EHR Implementation Best Practices: An EHR implementation that increases efficiencies versus an EHR that is under utilized, abandoned or replaced. By Tana Goering, M.D. EHR Implementation Best Practices:
EHR Implementation Best Practices: An EHR implementation that increases efficiencies versus an EHR that is under utilized, abandoned or replaced. By Tana Goering, M.D. EHR Implementation Best Practices:
Darice M. Grzybowski, MA, RHIA, FAHIMA President, H.I.Mentors, LLC
 Darice M. Grzybowski, MA, RHIA, FAHIMA President, H.I.Mentors, LLC Paper and electronic health records (EHR), or a combination of both, provide supporting documentation and records information about a
Darice M. Grzybowski, MA, RHIA, FAHIMA President, H.I.Mentors, LLC Paper and electronic health records (EHR), or a combination of both, provide supporting documentation and records information about a
Benefits and Risks of Electronic Health Records
 Benefits and Risks of Electronic Health Records Rainu Kaushal, MD, MPH Director, Center for Informatics and Health Systems Improvement Weill Cornell Medical College and Graduate School Chief, Division
Benefits and Risks of Electronic Health Records Rainu Kaushal, MD, MPH Director, Center for Informatics and Health Systems Improvement Weill Cornell Medical College and Graduate School Chief, Division
Technology Mediated Translation Clinical Decision Support. Marisa L. Wilson, DNSc, MHSc, CPHIMS, RN-BC. January 23, 2015.
 Technology Mediated Translation Clinical Decision Support Marisa L. Wilson, DNSc, MHSc, CPHIMS, RN-BC January 23, 2015 Background Presidents Bush, President Obama American Recovery and Reinvestment Act
Technology Mediated Translation Clinical Decision Support Marisa L. Wilson, DNSc, MHSc, CPHIMS, RN-BC January 23, 2015 Background Presidents Bush, President Obama American Recovery and Reinvestment Act
The Future of Technology in Long Term Care
 The Future of Technology in Long Term Care Lisa Mitchelson and Scott White, TEF Traci Jersen, 6N Systems Ellen Flaherty, VCNY David Finkelstein, VCNY In today s workshop. Introduction Overview Electronic
The Future of Technology in Long Term Care Lisa Mitchelson and Scott White, TEF Traci Jersen, 6N Systems Ellen Flaherty, VCNY David Finkelstein, VCNY In today s workshop. Introduction Overview Electronic
Adopting Clinical Decision Support Systems: A Best Practice Snapshot for Ophthalmology
 Adopting Clinical Decision Support Systems: A Best Practice Snapshot for Ophthalmology Electronic Health Records Practice Management Clinical Decision Support Seeing the Forest through the Trees: Clinical
Adopting Clinical Decision Support Systems: A Best Practice Snapshot for Ophthalmology Electronic Health Records Practice Management Clinical Decision Support Seeing the Forest through the Trees: Clinical
Electronic health records: underused in the ICU?
 Electronic health records: underused in the ICU? Christopher W. Seymour, MD MSc Assistant Professor of Critical Care Medicine Core Faculty Member, CRISMA Center University of Pittsburgh School of Medicine
Electronic health records: underused in the ICU? Christopher W. Seymour, MD MSc Assistant Professor of Critical Care Medicine Core Faculty Member, CRISMA Center University of Pittsburgh School of Medicine
Evaluating the Effectiveness of Electronic Medical Records in a Long Term Care Facility Using Process Analysis
 Journal of Healthcare Engineering Vol. 2 No. 1 2011 Page 75 86 75 Evaluating the Effectiveness of Electronic Medical Records in a Long Term Care Facility Using Process Analysis Barbara Cherry 1, *, DNSc,
Journal of Healthcare Engineering Vol. 2 No. 1 2011 Page 75 86 75 Evaluating the Effectiveness of Electronic Medical Records in a Long Term Care Facility Using Process Analysis Barbara Cherry 1, *, DNSc,
EMR Cost-Benefit Analysis: Managing ROI into Reality
 EMR Cost-Benefit Analysis: Managing ROI into Reality Michael H. Zaroukian, MD, PhD, FACP EMR Medical Director, MSU HealthTeam President, Centricity Healthcare User Group Arlotto & Oakes No Free Lunch for
EMR Cost-Benefit Analysis: Managing ROI into Reality Michael H. Zaroukian, MD, PhD, FACP EMR Medical Director, MSU HealthTeam President, Centricity Healthcare User Group Arlotto & Oakes No Free Lunch for
Implementation of an Open Access Scheduling System in a Residency Training Program
 666 October 2003 Family Medicine Practice Managemen t Implementation of an Open Access Scheduling System in a Residency Training Program James G. Kennedy, MD, MBA; Julian T. Hsu, MD Background and Objectives:
666 October 2003 Family Medicine Practice Managemen t Implementation of an Open Access Scheduling System in a Residency Training Program James G. Kennedy, MD, MBA; Julian T. Hsu, MD Background and Objectives:
Successful EHR Change Management
 Successful EHR Change Management Roles and responsibilities White paper Table of contents Executive summary... 2 Introduction... 3 Never underestimate the power of the people... 3 People... 4 From resisting
Successful EHR Change Management Roles and responsibilities White paper Table of contents Executive summary... 2 Introduction... 3 Never underestimate the power of the people... 3 People... 4 From resisting
EHR Implementation Best Practices. EHR White Paper
 EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
Mastering emeasures - Charting a Course To Align Quality And Payment
 Mastering emeasures - Charting a Course To Align Quality And Payment a complimentary webinar from healthsystemcio.com, sponsored by Encore Health Resources Housekeeping To ensure you enjoy all the functionality
Mastering emeasures - Charting a Course To Align Quality And Payment a complimentary webinar from healthsystemcio.com, sponsored by Encore Health Resources Housekeeping To ensure you enjoy all the functionality
