Technology Assessment
|
|
|
- Belinda Goodman
- 8 years ago
- Views:
Transcription
1 Technology Assessment Use of Cardiac Resynchronization Therapy in the Medicare Population Technology Assessment Program Prepared for: Agency for Healthcare Research and Quality 540 Gaither Road Rockville, Maryland March 24, 2015 Final Report
2 Use of Cardiac Resynchronization Therapy in the Medicare Population Technology Assessment Report Project ID: CRDT1013 March 24, 2015 Johns Hopkins University Evidence-based Practice Center John Rickard, M.D.,M.P.H. Henry Michtalik, M.D., M.P.H., M.H.S. Ritu Sharma, B.Sc. Zackary Berger, M.D., Ph.D. Emmanuel Iyoha, M.B.Ch.B., M.P.H. Ariel R. Green, M.D., M.P.H. Nowreen Haq, M.D., M.P.H. Karen A. Robinson, Ph.D. This report is based on research conducted by the Johns Hopkins University Evidence-based Practice Center under contract to the Agency for Healthcare Research and Quality (AHRQ), Rockville, MD HHSA ). The findings and conclusions in this document are those of the author (s) who are responsible for its contents; the findings and conclusions do not necessarily represent the views of AHRQ. No statement in this article should be construed as an official position of the Agency for Healthcare Research and Quality or of the U.S. Department of Health and Human Services. The information in this report is intended to help health care decision-makers; patients and clinicians, health system leaders, and policymakers, make wellinformed decisions and thereby improve the quality of health care services. This report is not intended to be a substitute for the application of clinical judgment. Decisions concerning the provision of clinical care should consider this report in the same way as any medical reference and in conjunction with all other pertinent information, i.e., in the context of available resources and circumstances presented by individual patients. ii
3 This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or as a basis for reimbursement and coverage policies. AHRQ or U.S. Department of Health and Human Services endorsement of such derivative products may not be stated or implied. None of the investigators has any affiliations or financial involvement related to the material presented in this report. This document is in the public domain and may be used and reprinted without special permission. Citation of the source is appreciated. Persons using assistive technology may not be able to fully access information in this report. For assistance contact TAP@ahrq.hhs.gov. Suggested citation: Rickard J, Michtalik H, Sharma R, Berger Z, Iyoha E, Green AR, Haq N, Robinson KA. Use of Cardiac Resynchronization Therapy in the Medicare Population. (Prepared by the Prepared by the Johns Hopkins University Evidence-based Practice Center under Contract No. HHSA ) Rockville, MD: Agency for Healthcare Research and Quality. March 24, iii
4 Acknowledgments We would like to thank Allen Zhang and Elisabeth Haberl Nannes for their assistance in data abstraction, Lisa Wilson for conducting meta-analysis and Eric Vohr for copy editing. We would also like to thank the Peer Reviewers, the Task Order Officers, and representatives from CMS. Peer Reviewers We wish to acknowledge individuals listed below for their review of this report. This report was reviewed in draft form by individuals chosen for their expertise and diverse perspectives. The purpose of the review was to provide candid, objective, and critical comments for consideration by the EPC in preparation of the final report. Synthesis of the scientific literature presented here does not necessarily represent the views of individual reviewers. Sana M. Al-Khatib, M.D., M.H.S. Heart Rhythm Specialist and Associate Professor of Medicine Division of Medicine Cardiology, Department of Medicine Duke University Medical Center Durham, NC Daniel B. Kramer, MD, MPH Cardiac Electrophysiology Cardiac Arrhythmias Specialist Beth Israel Deaconess Medical Center Boston, MA Michael Lauer, M.D. Director, Division of Cardiovascular Sciences National Heart, Lung, and Blood Institute (NHLBI) National Institutes of Health (NIH) Bethesda, MD Win-Kuang Shen, M.D. Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Arizona Scottsdale, AZ Lynne Stevenson, M.D. Director, Cardiomyopathy and Heart Failure Program Harvard Medical School Boston, MA iv
5 Structured Abstract Objectives: To assess the benefits and harms of cardiac resynchronization with (CRT-D) and compared to an ICD alone, CRT without a defibrillator (CRT-P) compared with optimal medical therapy and CRT-D compared with CRT-P in patients with an EF 35% and a QRS duration 120 ms. We also sought to assess predictors of response to CRT-D and CRT-P. Data Sources: We searched MEDLINE, Embase, and the Cochrane Central Register of Controlled Trials (CENTRAL) from January 1, 1995, as this is the date of first article reporting use of CRT through October 20 th, Review Methods: Paired investigators independently screened search results to assess eligibility. Investigators abstracted data sequentially and assessed risk of bias independently. Investigators graded the strength of evidence as a group. Results: CRT-D was found to be effective in reducing heart failure hospitalizations, inducing ventricular reverse remodeling, improving quality of life, and increasing six-minute hall walk distances compared to an ICD alone with a high strength of evidence. In a meta-analysis of minimally symptomatic patients, CRT-D reduced LVESV (ml) (mean difference , 95% CI to -9.56). This analysis was comprised primarily on NYHA class II patients; therefore, the applicability to NYHA class I patients is unclear. In a meta-analysis of patients with advanced heart failure (NYHA class III-IV), CRT-D improved quality of life scores (as measured by the Minnesota Living with Heart Failure Questionnaire) (mean difference , 95% CI to ) compared to an ICD alone. CRT-P was found to be effective in improving all-cause survival and reducing heart failure hospitalizations compared to optimal medal therapy alone with a moderate level of evidence. CRT-P was also found to induce reverse ventricular remodeling and increase six-minute hall walk distances compared to optimal medical therapy alone. These findings were primarily noted in NYHA class III-IV patients. The applicability of these findings to NYHA class I-II patients is unclear. Determining predictors of response to CRT was limited by the likely presence of reporting bias. Nevertheless, a left bundle branch (LBBB) morphology, non-ischemic cardiomyopathy (NICM), and female gender were generally associated with improved outcomes following CRT-D. Sinus rhythm (as compared to atrial fibrillation) and a wider QRS duration were associated with improved outcomes following CRT- D albeit with a lower strength of evidence. There is insufficient evidence to determine predictors of outcomes in patients undergoing CRT-P. There is insufficient evidence to determine the effectiveness of CRT-D versus CRT-P. Compared to CRT-P, device infection was slightly more common in patients receiving CRT-D. Conclusions: There is convincing evidence that CRT-D is effective with regard to improvements in multiple clinical outcomes compared to an ICD alone in patients with an LVEF 35% and a QRS duration 120ms. Similarly, there is convincing evidence that CRT-P is effective in improving multiple clinical endpoints compared to optimal medical therapy alone in the same population. The certainty of these findings varies based on NYHA class. Female gender, LBBB, a wider QRS duration, sinus rhythm, and non-ischemic cardiomyopathy are associated with improved outcomes following CRT although the likely presence of reporting bias qualifies these results. More data are needed for several questions including the efficacy of CRT in patients with a non-lbbb morphology or atrial fibrillation and the comparison of outcomes in patients receiving a CRT-D vs. CRT-P device. v
6 Contents Executive summary... ES1 Introduction...1 Scope and Key Questions... 2 Methods...6 Protocol Development... 6 Search Strategy... 6 Study Selection... 6 Data Abstraction and Data Management... 6 Risk of Bias Assessment Data Synthesis Strength of the Body of Evidence Applicability Results...12 Results of the Search...12 Overview of included studies by outcomes...14 Organization of Results Chapter...16 Effectiveness of Cardiac Resynchronization Therapy with Defibrillator (CRT-D)...17 Harms of Cardiac Resynchronization Therapy with Defibrillator (CRT-D)...40 Effectiveness of Cardiac Resynchronization Therapy with Pacemaker (CRT-P)...56 Harms of Cardiac Resynchronization Therapy with Pacemaker (CRT-P)...73 Effectiveness of Cardiac Resynchronization Therapy with Pacemaker versus Defibrillator (CRT-P vs CRT-D)...83 Harms of Cardiac Resynchronization Therapy with Pacemaker versus Defibrillator (CRT- P vs CRT-D)...90 Predictors of Response to Cardiac Resynchronization Therapy with Defibrillator (CRT-D).105 Predictors of Response to Cardiac Resynchronization Therapy with Pacemaker (CRT-P) Discussion Key Findings and the Strength of Evidence Relationship of Findings to Existing Literature Applicability Limitations of the Comparative Effectiveness Review Process Limitations of the Evidence Base Research Gaps Conclusion References List of Abbreviations Tables Table 1. PICOTS (population, interventions, comparators, outcomes, timing, setting) for each Key Question...7 Table 2. List of exclusion criteria at the abstract and article screening level...8 Table 3. List of device manufacturers...9 Table 4. Strength of evidence grades and definitions...11 Table 5. List of included studies by outcomes...14 Table 6. List of trials included in the review...15 vi
7 Table 7. Evidence addressing effectiveness and harms of CRT-D...17 Table 8. Study characteristics of trials assessing effectiveness of CRT-D...19 Table 9. Summary of risk of bias for trials assessing effectiveness of CRT-D...22 Table 10. Outcomes reported in the trials assessing effectiveness of CRT-D...25 Table 11. Summary of CRT-D effectiveness outcomes reported by subgroup...37 Table 12. Strength of evidence for key effectiveness outcomes of CRT-D...38 Table 13. Summary of risk of bias for trials assessing harms of CRT-D...42 Table 14. Summary of risk of bias for cohort studies assessing harms of CRT-D...44 Table 15. List of harms reported in studies assessing harms of CRT-D...46 Table 16.Characteristics of studies of CRT-D reporting on the incidence of pneumothorax...49 Table 17. Characteristics of studies of CRT-D reporting on the incidence of pocket hematoma.50 Table 18. Characteristics of studies of CRT-D reporting on the incidence of cardiac device infection...51 Table 19. Characteristics of studies of CRT-D reporting on the incidence of cardiac perforation/tamponade...52 Table 20. Characteristics of studies of CRT-D reporting on the incidence of lead dislodgement 53 Table 21. Characteristics of studies of CRT-D reporting inappropriate ICD shocks...55 Table 22. Evidence addressing effectiveness and harms of CRT-P...57 Table 23. Study characteristics of trials assessing effectiveness of CRT-P...59 Table 24. Summary of risk of bias for trials assessing effectiveness of CRT-P...63 Table 25. Outcomes reported in the trials assessing effectiveness of CRT-P...65 Table 26. Summary of CRT-P effectiveness outcomes reported by subgroup...72 Table 27. Strength of evidence for key effectiveness outcomes of CRT-P...73 Table 28. Summary of risk of bias for trials assessing harms of CRT-P...75 Table 29. Summary of risk of bias for cohort studies assessing harms of CRT-P...77 Table 30. List of harms reported in the studies assessing harms of CRT-P...78 Table 31. Characteristics of studies of CRT-P reporting on the procedure-related complications80 Table 32. Characteristics of studies of CRT-P reporting on the incidence of pneumothorax...80 Table 33. Characteristics of studies of CRT-P reporting on the incidence of pocket hematoma..81 Table 34. Characteristics of studies of CRT-P reporting on the incidence of cardiac device infection...81 Table 35. Characteristics of studies of CRT-P reporting on the incidence of cardiac perforation/tamponade...82 Table 36. Characteristics of studies of CRT-P reporting on the incidence of lead dislodgement.82 Table 37. Characteristics of studies of CRT-P reporting on the death within one week...83 Table 38. Evidence addressing effectiveness and harms of CRT-P vs CRT-D...84 Table 39. Study characteristics of trials assessing effectiveness of CRT-P vs CRT-D...85 Table 40. Summary of risk of bias for trials assessing effectiveness of CRT-P vs CRT-D...87 Table 41. Summary of effectiveness outcomes reported in the trial of CRT-P vs CRT-D, by subgroup...90 Table 42. Strength of evidence for key effectiveness outcomes of CRT-P vs CRT-D...90 Table 43. Summary of risk of bias for trials assessing harms of CRT-P vs CRT-D...93 Table 44. Summary of risk of bias for cohort studies assessing harms of CRT-P vs CRT-D...94 Table 45. List of harms reported in the studies assessing harms of CRT-P vs CRT-D...96 Table 46. Summary of effectiveness outcomes by comparator Table 47. Summary of harms by comparator Table 48. Study characteristics of studies assessing predictors of response to CRT-D Table 49. Summary of risk of bias for studies assessing predictor of response to CRT-D vii
8 Table 50. Included predictors of response for CRT-D Table 51. Definitions of response for CRT-D predictors Table 52. Evidence addressing predictors of response to CRT-D, by predictor Table 53. Summary of findings of predictors of response to CRT-D, by outcome Table 54. Study characteristics of studies assessing predictor of response to CRT-P Table 55. Summary of risk of bias for studies assessing predictor of response to CRT-P Table 56. Included predictors of response for CRT-P Table 57. Definitions of response for CRT-P predictors Table 58. Evidence addressing predictors of response to CRT-P, by predictor Table 59. Summary of findings of predictors of response to CRT-P, by outcome Table 60. Summary of the strength of evidence for key effectiveness outcomes Table 61. Prior systematic reviews of cardiac resynchronization therapy Table 62. Characteristics of an ideal study to compare the effectiveness of CRT-D vs. CRT-P 147 Table 63. Characteristics of an ideal study to compare the effectiveness of CRT-D in Patients with a non-left Bundle Branch Block morphology Table 64. Characteristics of an ideal study to compare the effectiveness of CRT-D in Patients with Atrial Fibrillation Figures Figure 1. Analytic framework for use of cardiac resynchronization therapy with defibrillator (CRT-D) in the Medicare population...3 Figure 2. Analytic framework for use of cardiac resynchronization therapy without defibrillator capacity (CRT-P) in the Medicare population...4 Figure 3. Analytic framework for use of cardiac resynchronization therapy with defibrillator capacity (CRT-D) versus cardiac resynchronization therapy without defibrillator capacity (CRT- P) in the Medicare population...5 Figure 4. Summary of the literature search and screen...13 Figure 5. Summary of risk of bias for trials assessing effectiveness of CRT-D...23 Figure 6. Meta-analysis of left ventricular end-diastolic volume in trials including minimally symptomatic patients CRT- D Effectiveness...30 Figure 7a and b. Meta-analysis of trials including minimally symptomatic patients in terms of improvement in quality of scores via the Minnesota Living with Heart Failure Questionnaire CRT- D Effectiveness...32 Figure 8. Meta-analysis of trials including minimally symptomatic patients in terms of left ventricular ejection fraction improvement CRT- D Effectiveness...34 Figure 9. Meta-analysis of patients with NYHA class I-II heart failure in terms of improvement in 6-minute hall walk distance CRT- D Effectiveness...36 Figure 10. Summary of risk of bias for trials assessing harms of CRT-D...43 Figure 11. Summary of risk of bias for cohort studies assessing harms of CRT-D...45 Figure 12. Summary of risk of bias for trials assessing effectiveness of CRT-P...64 Figure 13. Summary of risk of bias for trials assessing harms of CRT-P...75 Figure 14. Summary of risk of bias for cohort studies assessing harms of CRT-P...78 Figure 15. Summary of risk of bias for cohort studies assessing harms of CRT-P vs CRT-D...95 Figure 16. Summary of risk of bias for studies assessing predictor of response to CRT-D viii
9 Appendixes Appendix A. Detailed Electronic Database Search Strategies Appendix B. Forms Appendix C. List of Excluded Studies Appendix D. Evidence Tables Appendix E. SIP ix
10 Executive Summary Background Chronic heart failure (CHF) is a major public health problem in the United States affecting an estimated 4.9 million Americans, causing high rates of hospitalization, poor quality of life, and 300,000 deaths each year. 1 Cardiac resynchronization (CRT) is a pacing modality utilizing a left ventricular (LV) pacing lead with the goal of re-synchronizing myocardial contraction in patients with CHF. CRT was originally indicated in patients with significant LV dysfunction, defined as a left ventricular ejection fraction (LVEF) 35%, New York Heart Association (NYHA) class III-IV heart failure symptoms, and a QRS duration 120ms on optimal medical therapy. 2-4 More recently, the indications for CRT expanded to include patients with minimally symptomatic heart failure (NYHA class II). 5,6 The appropriateness of CRT in patients with NYHA class I symptoms is unclear. 1 The vast majority of candidates for CRT devices also have an indication for an implantable cardiac defibrillator (ICD), therefore, the large majority of patients receiving CRT in the United States receive a CRT device with a defibrillator (CRT-D) as opposed to a CRT pacemaker (CRT-P). CRT-P devices are occasionally placed in patients who wish to avoid ICD shocks or in patients with an indication for frequent ventricular pacing due to conduction disease who have an LVEF between percent. Scope and Key Questions We conducted a systematic review on the efficacy for both CRT-D and CRT-P. The questions were nominated by the Centers for Medicare and Medicaid (CMS).We sought to address the following questions for patients with an LVEF 35% and a QRS duration 120ms: What is the effectiveness and safety of CRT-D compared to an ICD alone? What is the effectiveness and safety of CRT-P compared to optimal medical therapy alone? What is the comparative effectiveness and safety of CRT-D versus CRT-P? What are the clinical predictors of response in patients deemed appropriate candidates for CRT-D devices? What are the clinical predictors of response in patients deemed appropriate candidates for CRT-P devices? ES-1
11 Methods With input from key informants, we refined the questions, including eligibility criteria, and developed a protocol (PROSPERO registration CRD ). We searched MEDLINE, Embase, and the Cochrane Central Register of Controlled Trials (CENTRAL) from January 1, 1995, as this is the date of first article reporting use of CRT through October 20th, We also reviewed the reference lists of all included articles, requested information from device manufacturers and searched Clinicaltrials.gov. Citations were screened independently by two reviewers using predefined eligibility criteria. One reviewer completed data abstraction and a second reviewer checked abstraction for completeness and accuracy. Data when available by subgroups (females, QRS duration >150 ms, left bundle branch block, atrial fibrillation and non-ischemic cardiac conditions) were also abstracted. Two reviewers independently assessed risk of bias for individual studies. We used the Cochrane Collaboration s tool for assessing the risk of bias of controlled studies. 7 For nonrandomized studies, we used the Newcastle Ottawa Scale 8 and for predictor studies, we used Quality In Prognosis Studies (QUIPS) tool. 9 Differences between reviewers were resolved through consensus. All studies were summarized qualitatively. We conducted meta-analyses for an outcome when there were sufficient data (at least 3 studies of the same design) and studies were sufficiently homogenous with respect to key variables (population characteristics, intervention, and outcome measurement) using profile likelihood estimate for random effects model. We identified substantial statistical heterogeneity in the trials as an I-squared statistic with a value greater than 50 percent. All meta-analyses were conducted using STATA 12.1 (College Station, TX). We graded the strength of evidence using the scheme recommended by the AHRQ EPC Methods Guide for Conducting Comparative Effectiveness Reviews. 10 For this report, we graded the strength of evidence for the outcomes we classified during protocol development as the most important or critical outcomes, including quality of life as assessed by the Minnesota Living with Heart Failure Inventory Score (MLHFQ), left ventricular end systolic volume, hospitalizations for heart failure and, all- cause mortality. ES-2
12 Results We included 60 studies, reported in 86 articles (see Figure A). Eight trials assessed the effectiveness of CRT-D with 7 providing data about all-cause mortality. We found moderate evidence of a benefit with CRT-D compared with ICD alone for survival in minimally symptomatic patients. There is insufficient evidence about the effect of CRT-D on all-cause mortality in patients with NYHA III-IV. CRT-D was noted to reduce heart failure hospitalizations, an effect seen primarily in patients with left bundle branch block (LBBB) morphology (6 trials; n=4736; high strength of evidence). There was also a high strength of evidence for CRT-D inducing ventricular reverse remodeling compared to ICD alone (5 trials; n=2936). A meta-analysis of three trials found a mean difference in mean change from baseline in left ventricular end systolic volume (LVESV) of favoring CRT-D (95% CI to -9.56). Quality of life, as measured by MLHFQ, was not different for minimally symptomatic patients (NYHA I-II) ( % CI to 5.30) but showed improvement with CRT-D compared to ICD alone in those with NYHA class III-IV symptoms ( % CI to -7.27) (high strength of evidence). CRT-D also increased six-minute hall walk distances compared to an ICD alone and improved clinical composite score. The prevalence of harms associated with CRT-D devices were as follows: cardiac perforation/tamponade ( %), pocket hematoma ( %), pneumothorax ( %), device infection ( %), and lead dislodgement (2.4% to 9.8%). No conclusions could be drawn about the association between CRT-D implant and subsequent ventricular arrhythmias or inappropriate shocks. We identified six trials, which assessed the efficacy of cardiac resynchronization therapy with a pacemaker (CRT-P) compared to optimal medical therapy alone (OMT). Three trials with longer followup showed improved survival (all-cause mortality) with CRT-P but those with shorter duration did not find an effect (moderate strength of evidence).there was moderate strength of evidence that CRT-P reduced heart failure hospitalizations and low strength of evidence that CRT-P, compared with OMT, induced ventricular reverse remodeling. Evidence about MLHFQ was insufficient to draw conclusions, and the effect of CRT-P on six-minute hall walk distances compared to optimal medical alone was similarly unclear. Harms associated with CRT-P were as follows: cardiac perforation/tamponade (0-1.6%), pocket hematoma ( %), pneumothorax ( %), device infection ( %), and lead dislodgement (1.7-17%). Determining predictors of response to CRT was limited by the likely presence of reporting bias. Nevertheless, a left bundle branch block (LBBB) morphology, non-ischemic cardiomyopathy (NICM), and female gender were generally associated with improved outcomes following CRT-D. Sinus rhythm (as compared to atrial fibrillation) and a wider QRS duration were associated with improved outcomes following CRT-D albeit with a lower strength of evidence. There is insufficient evidence to determine predictors of outcomes in patients undergoing CRT-P. However, of the outcomes that were assessed, the ICD function would impact only the mortality endpoint. Therefore similar conclusions as to those noted for CRT-D can be drawn for CRT-P devices for the other, non-mortality endpoints. The availability of only one trial, with methodological limitations, means that there is insufficient evidence to determine the effectiveness of CRT-D vs. CRT-P. Compared to CRT-P, device infection was slightly more common in patients receiving CRT-D. There was insufficient evidence to draw conclusions on any other harms comparing the two devices. ES-3
13 Figure A. Summary of the literature search and screen Electronic Databases MEDLINE (7421) EMBASE (10876) Cochrane (885) Clinicaltrials.gov (133) Hand Searching (30) Retrieved (19345) Duplicates (6330) Abstract Screening (13015) Excluded (11897) Reasons for Exclusion at Abstract Screening* Does not evaluate CRT: 9393 Study published before 1995: 10 No original data: 1769 Not conducted in humans: 273 Not in English: 2 No full report (e.g. conference or meeting abstract):25 Study of children only: 506 Not relevant to key questions: 4021 Full-Text Screening (1118) Included Articles (86) 60 studies (86 articles) Excluded (1032) Reasons for Exclusion at Full-Text Screening* Does not evaluate CRT: 70 Study published before 1995: 0 No original data: 25 Not conducted in humans: 0 Not in English: 2 No full report (e.g. conference or meeting abstract): 6 Study of children only: 0 Not relevant to key questions: 498 Single case study: 21 Addresses effectiveness questions and is not RCT: 200 Population inclusion criteria do not fall within the QRS>/=120ms range and LVEF</=35%: 289 Address remodeling outcomes but response definition not within range of LVESV 10%, LVEDV 10% or EF 5%: 200 Study addresses predictors questions but did not adjust through the model or via selection of participants for at least two predictors: 510 Contacted authors but did not receive the requested information: 22 Other: 283 * Total number of reasons for exclusion exceeds the number of citations excluded, because citations could be excluded for more than one reason ES-4
14 Discussion Key Findings and the Strength of Evidence Efficacy and Safety of CRT-D (KQ1a, KQ2) There is convincing evidence that CRT-D devices are effective in reducing heart failure symptoms, improving myocardial function, and reducing hospitalizations for heart failure in patients with an LVEF 35% and a QRS duration 120 ms compared to therapy with an ICD alone. Specifically, we found moderate strength of evidence for benefit of CRT-D versus ICD alone for all-cause mortality in minimally symptomatic patients. This statement is derived from data looking primarily at NYHA class II patients. The applicability of this finding to NYHA class I patients, a population significantly under-represented in studies, is unclear. There is insufficient evidence to determine whether CRT-D devices are effective in improving survival compared to an ICD alone in an advanced heart failure population (NYHA III-IV). In terms of pre-specified subgroups, there is generally strong evidence that in CRT-D patients (compared to an ICD alone), female gender, a left bundle branch block, and nonischemic cardiomyopathy are associated with superior outcomes. Sinus rhythm (as opposed to a history of atrial fibrillation) and a wider QRS complex and also associated with superior outcomes in patients undergoing CRT-D implant compared to an ICD alone although the data for this are less compelling. (Table A.) Efficacy and Safety of CRT-P (KQ3a, KQ4) There is moderate evidence that CRT-P, compared to optimal medical therapy, is effective in improving survival, reducing LVESV, and reducing hospitalizations for heart failure in patients with an LVEF 35% and a QRS duration 120 ms compared to optimal medical therapy alone. These data are largely derived from patients with NYHA class III-IV heart failure. The applicability of these findings to patient with NYHA class I-II heart failure is unclear. We found insufficient evidence about the effect of CRT-P on quality of life, as measured with the MLHFQ, compared to optimal medical therapy alone. Efficacy and Safety of CRT-D versus CRT-P (KQ5, KQ6) Only one included trial contained both CRT-D and CRT-P arms, and direct comparisons between those arms were lacking. Therefore, there is insufficient evidence to determine the effectiveness of CRT-D compared to CRT-P. In comparing harms between CRT-D and CRT-P devices, there was also insufficient evidence to draw any conclusions except for device infections, which appear to be slightly more common for CRT-D devices. Predictors of Response: CRT-D and CRT-P (KQ1b, KQ3b) The evidence regarding predictors of a favorable response following CRT varied considerably based on outcome. In addition, the high likelihood of reporting bias qualifies these results. Age was not an important predictor of outcomes in patients receiving CRT-D devices. However, data for very elderly patients (> 75 years of age) were limited. Non-ischemic cardiomyopathy, female gender, and a left bundle branch block morphology were strongly associated with improved outcomes. A history of atrial fibrillation and a narrower QRS duration were predictive of poorer outcomes although the evidence for this was less robust. There was inadequate evidence to determine the predictive nature of chronic kidney disease, left atrial volume, baseline LVEF, body mass index, and left ventricular end-diastolic volume on outcomes following CRT-D implant. There was also insufficient evidence to draw conclusions as to the predictive nature of baseline characteristics in patients receiving a CRT-P device. However, of ES-5
15 the outcomes that were assessed, the ICD function would impact only the mortality endpoint. Therefore similar conclusions as to those noted for CRT-D can likely be drawn for CRT-P devices for the other, non-mortality endpoints. ES-6
16 Table A. Summary of the strength of evidence for key effectiveness outcomes Comparisons All-cause mortality Hospitalizations for heart failure Cardiac resynchronization therapy with defibrillator vs. ICD alone Cardiac resynchronization therapy with pacemaker vs. optimal medical therapy Cardiac resynchronization therapy with pacemaker or with defibrillator Moderate In patients with minimally symptomatic CHF (primarily class NYHA class II), data from the RAFT trial (a larger, slightly more symptomatic population, with a longer followup) demonstrates a mortality benefit, The MADIT-CRT trial did not report a mortality benefit with CRT-D in primarily NYHA class II patients. Longterm followup of a subset of patients demonstrated a mortality benefit in patients with LBBB but not with a non- LBBB and did not report a mortality comparison for the group as a whole. The other trials assessing mortality in minimally symptomatic patients were either too small in size or followup to add significant additional evidence. The trials assessing mortality in patients with NYHA class III-IV symptoms were limited in terms of followup and size, therefore there is insufficient evidence to determine the effect of CRT-D on mortality compared to an ICD alone. Moderate Studies showed statistically significant differences in mortality favoring CRT-P. Insufficient High The large RAFT and MADIT- CRT trials showed a reduction in CHF events for CRT-D compared to an ICD alone. Subgroup analyses from both trials demonstrate the effect to be primarily in patients with LBBB morphology. Moderate Studies showed fewer hospitalizations in the CRT-P group Low Compared with optimal medical therapy, CRT-P and CRT-D were associated with 44% and 41% reduction in heart failure hospitalizations (not significantly different). ES-7 Left ventricular end systolic volume (or index) High The trials were consistent in demonstrating a reduction in LVESV with CRT-D compared to an ICD alone. Meta-analysis of trials in patients with NYHA I-II (primarily NYHA class II patients), mean difference (95% CI, to -9.56). Low CRT-P significantly reduced LVESV compared with optimal medical therapy alone. Insufficient Minnesota Living with Heart Failure Questionnaire High The current data suggest that CRT-D does not improve QOL in minimally symptomatic patients compared to an ICD alone. The data does suggest a significant improvement in QOL in patients with NYHA class III-IV CHF (mean difference (95% CI to 7.27). Insufficient Insufficient
17 Relationship of Findings to Existing Literature Our current review differs from prior reviews in that only studies with patients with an LVEF 35% and a baseline QRS duration 120 ms undergoing biventricular pacing were included. These criteria were developed in consultation with our key informants and largely mirror the current appropriate use criteria for CRT from United States guidelines. 1 This eliminated the REVERSE, BLOCK CHF, and HOBIPACE trials which included patients with an LVEF>35% The criteria also excluded all trials looking at the effects of CRT in a narrow QRS duration population, and studies of LV only pacing. 17,18 We considered the appropriate control for the CRT-D effectiveness question to be an ICD alone given the compelling data demonstrating improvements in mortality with an ICD that evolved concomitantly with studies of CRT effectiveness. We considered the appropriate control for CRT-P to be optimal medical therapy alone to assess the impact of cardiac resynchronization. We did not assess the comparison of CRT-D to optimal medical therapy as we determined this to be an inappropriate comparison, given the known improvements in mortality by defibrillation. Also, in contrast to several previous reviews, we included only RCTs to assess the questions regarding effectiveness. In terms of minimally symptomatic patients, the results of our review largely agree with those of prior reviews, which focused on the same population. Similarly, the current review is in agreement with the systematic review performed in 2007 by Mcallister et al., which included studies primarily involving an advanced heart failure population. 19 Our review arrived at somewhat different conclusions in terms of the efficacy of CRT-D vs. CRT-P compared to that by Jiang et. al. 20 Given that we considered only RCTs for determination of effectiveness, only the COMPANION trial was included in our review, which likely explains the discrepancy in conclusions. 3 In our systematic analysis of predictors of outcomes following CRT, many studies assessing the capacity for baseline characteristics to predict responses (defined in many different ways) were identified. The large majority of studies were small (<100 patients) and not properly controlled. At a minimum, we pre-specified that a cohort study addressing our questions about predictors of response to CRT had to include at least gender and either QRS duration or morphology in a multivariate model to address confounding factors. Such criteria eliminated many studies. Despite this, the positive predictive effect noted with LBBB, female gender, nonischemic cardiomyopathy, a wider QRS duration, and normal sinus rhythm on multiple outcomes was supportive of the similar findings noted from the pre-specified subgroup analyses of the RCTs. There are other potential predictors we did not consider (e.g. lead position). Given the large number of potential predictors in the literature, a review of all predictors was not practical. Our predictors were chosen based on prevailing knowledge of the most important predictors, identified in consultation with our key informants. Finally, we did not conduct individual patient data meta-analysis to assess predictors meaning that our analyses may suggest that clinically relevant subgroup effects exist, but we are unable to quantify the effects reliably or precisely. Applicability The generalizability of these results is slightly limited. Race was reported very infrequently, prohibiting an assessment of applicability based on racial differences. The majority of patients included in the RCTs were male, although a large focus in sub-studies has been given to the role of CRT in women, given the heightened response to therapy seen in this population. The average age in the RCTs and cohort studies was in the mid 60s although many patients included were in ES-8
18 the age range of the elderly Medicare population. There has not been an RCT that specifically enrolled Medicare eligible patients. Also, data for very elderly patients (> 75 years of age) are limited. In cohort studies and subgroup analyses from the RCTs, age was not found to be an important predictor of outcomes. Taken together, the results of our review are generalizable to the Medicare population although given the absence of dedicated RCTs, a definitive statement of generalizability to this population is not possible. Limitations of the Comparative Effectiveness Review Process In addressing the questions of efficacy of CRT-D and CRT-P, several studies potentially of interest were excluded since they were non-randomized. For the questions about the predictors of response to CRT, many retrospective cohort studies were excluded because of a mixed population of CRT-D and CRT-P devices. Attempts were made to contact the authors of such studies to obtain the device-specific data but, in many cases, this was unsuccessful. In addition, many cohorts that contained outcomes of interest were excluded due to failure to control for gender and QRS duration and/or morphology, important baseline confounders. Finally, we did not include prior or conduct new individual patient data meta-analyses to assess predictors. Therefore, our analyses may suggest that clinically relevant subgroup effects exist, but we are unable to quantify the effects reliably or precisely. Limitations of the Evidence Base Multiple, well-conducted RCTs were identified addressing the questions about the efficacy of CRT-D and CRT-P. The majority of patients enrolled in the clinical trials had NYHA class II-IV heart failure symptoms. The applicability of the current findings to class I patients is less clear. In contrast, only the COMPANION trial contained both CRT-D and CRT-P arms. 3 However, a direct comparison of the CRT-D to CRT-P arms was not reported for several outcomes. For the questions examining predictors of response to CRT many of the included cohort studies were relatively small. While all studies controlled for gender and either QRS duration or morphology based on our pre-specified inclusion criteria, the remaining variables in the model varied widely between studies. Similarly, many studies used statistical criteria to create their multivariate adjustments, rather than pre-specifying clinical factors known to be important. Research Gaps There is convincing evidence that CRT-D results in reverse ventricular remodeling and improvements in quality of life compared to an ICD alone. However, only two trials showed a mortality benefit of CRT-D over ICD alone. The RAFT trial primarily contained patients with NYHA class II symptoms. 6 Long term follow up of the MADIT-CRT trial suggested a mortality benefit in the LBBB subgroup alone but did not report mortality for the cohort as a whole. 21 Whether CRT-D results in improved survival compared to an ICD alone in patients with advanced heart failure is unclear. Several subgroup analyses from RCTs as well as cohort studies demonstrate superior outcomes in patients with a native LBBB compared to a non-lbbb. Subgroup analysis from the MADIT-CRT trial suggested possible harm for CRT-D versus an ICD alone in non-lbbb patients. 5,21 Subgroup analyses from other RCTs suggested little benefit of CRT in non-lbbb patients (but no convincing trend towards harm). 6 One important issue with the assessment of CRT efficacy according to QRS morphology is the interaction between QRS duration, another ES-9
19 variable with impact on outcome, and morphology. Patients with a LBBB tend to have wider QRS durations than patients with non-lbbbs. Several retrospective studies have attempted to determine the relative impact on outcomes of QRS duration within various QRS morphology groups in patients receiving a CRT device with mixed results. 22,23 There has not been an RCT, which compares CRT to a control in patients with a non-lbbb morphology. Given the lack of such a trial, the ability to conclude definitively that CRT is ineffective or, in fact harmful, in patients with non-lbbb morphology is limited. Similarly, subgroup analyses from RCTs suggest limited benefit of CRT in patients with atrial fibrillation. Outside the small MUSTIC-AF study, data focused on the AF population are lacking. 24 Therefore, the ability to definitively conclude a lack of benefit in patients with AF receiving CRT is not possible. The effectiveness of CRT-D versus CRT-P in patients with an LVEF 35% has not been adequately addressed. The COMPANION trial, which included both arms, did not directly compare the CRT types and is therefore inadequate to answer this question definitively. 3 Conclusion We performed a systematic review to evaluate the efficacy and safety of CRT-D and CRT-P devices as well as predictors of outcomes following implant of such devices. There is convincing evidence that CRT-D is effective with regard to improvements in multiple outcomes compared to an ICD alone in patients with an LVEF 35% and a QRS duration 120ms. These findings are based on patients primarily with NYHA class II-IV heart failure. The applicability of these findings to patients with NYHA class I symptoms is unclear. Similarly, there is convincing evidence that CRT-P is effective in improving multiple endpoints compared to optimal medical therapy alone in the same population. These data are primarily derived from NYHA class III-IV and the applicability to patients with NYHA class I and II is less clear. Female gender, LBBB, a widened QRS duration, sinus rhythm, and non-ischemic cardiomyopathy are associated with improved outcomes following CRT. ES-10
20 Reference List 1. Heart Failure Society of America (HFSA) practice guidelines. HFSA guidelines for management of patients with heart failure caused by left ventricular systolic dysfunction-- pharmacological approaches. J Card Fail 1999; 5(4): PMID: Abraham WT, Fisher WG, Smith AL et al. Cardiac resynchronization in chronic heart failure. N Engl J Med 2002; 346(24): PMID: Bristow MR, Saxon LA, Boehmer J et al. Cardiac-resynchronization therapy with or without an implantable defibrillator in advanced chronic heart failure. N Engl J Med 2004; 350(21): PMID: Cleland JG, Daubert JC, Erdmann E et al. The effect of cardiac resynchronization on morbidity and mortality in heart failure. N Engl J Med 2005; 352(15): PMID: Moss AJ, Hall WJ, Cannom DS et al. Cardiacresynchronization therapy for the prevention of heart-failure events. N Engl J Med 2009; 361(14): PMID: Tang AS, Wells GA, Talajic M et al. Cardiacresynchronization therapy for mild-to-moderate heart failure. N Engl J Med 2010; 363(25): PMID: Higgins JPT. Cochrane handbook for systemic reviews of interventions Version The Cochrane Collaboration. 2011;Oxford, England. Available at: PMID: 8. Wells GA. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses ford.asp Hayden JA. Assessing bias in studies of prognostic factors. Ann Intern Med. 2013; 158(4): PMID: Agency for Healthcare Research and Quality. Grading the Strength of a Body of Evidence When Assessing Health Care Interventions - AHRQ and the Effective Health Care Program: An Update. Rockville, MD: Agency for Healthcare Research and Quality. 2013: Available at: 457/1163/GradingTheStrengthofEvidence_Draft MethodsChapter_ pdf PMID: 11. Daubert C, Gold MR, Abraham WT et al. Prevention of disease progression by cardiac resynchronization therapy in patients with asymptomatic or mildly symptomatic left ventricular dysfunction: insights from the European cohort of the REVERSE (Resynchronization Reverses Remodeling in Systolic Left Ventricular Dysfunction) trial. J Am Coll Cardiol 2009; 54(20): PMID: Kindermann M, Hennen B, Jung J, Geisel J, Bohm M, Frohlig G. Biventricular versus conventional right ventricular stimulation for patients with standard pacing indication and left ventricular dysfunction: the Homburg Biventricular Pacing Evaluation (HOBIPACE). J Am Coll Cardiol 2006; 47(10): PMID: Curtis AB, Worley SJ, Adamson PB et al. Biventricular pacing for atrioventricular block and systolic dysfunction. N Engl J Med 2013; 368(17): PMID: Beshai JF, Grimm RA, Nagueh SF et al. Cardiac-resynchronization therapy in heart failure with narrow QRS complexes. N Engl J Med 2007; 357(24): PMID: Thibault B, Harel F, Ducharme A et al. Cardiac resynchronization therapy in patients with heart failure and a QRS complex <120 milliseconds: the Evaluation of Resynchronization Therapy for Heart Failure (LESSER-EARTH) trial. Circulation 2013; 127(8): PMID: Ruschitzka F, Abraham WT, Singh JP et al. Cardiac-resynchronization therapy in heart failure with a narrow QRS complex. N Engl J Med 2013; 369(15): PMID: Boriani G, Kranig W, Donal E et al. A randomized double-blind comparison of biventricular versus left ventricular stimulation ES-11
Updated Cardiac Resynchronization Therapy Guidelines
 The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): November 25, 2014 Effective Date: February 1, 2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): November 25, 2014 Effective Date: February 1, 2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Department of Veterans Affairs Health Services Research and Development - A Systematic Review
 Department of Veterans Affairs Health Services Research & Development Service Effects of Health Plan-Sponsored Fitness Center Benefits on Physical Activity, Health Outcomes, and Health Care Costs and Utilization:
Department of Veterans Affairs Health Services Research & Development Service Effects of Health Plan-Sponsored Fitness Center Benefits on Physical Activity, Health Outcomes, and Health Care Costs and Utilization:
How do you decide on rate versus rhythm control?
 Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Noves Indicacions de la Resincronització
 INSUFICIÈNCIA CARDÍACA. TRACTAMENT DE RESINCRONITZACIÓ EN MALALTS COMPLICATS Noves Indicacions de la Resincronització Dr Xavier Viñolas Director Unitat d Aritmies Hospital de Sant Pau Societat Catalana
INSUFICIÈNCIA CARDÍACA. TRACTAMENT DE RESINCRONITZACIÓ EN MALALTS COMPLICATS Noves Indicacions de la Resincronització Dr Xavier Viñolas Director Unitat d Aritmies Hospital de Sant Pau Societat Catalana
on behalf of the AUGMENT-HF Investigators
 One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
One Year Follow-Up Results from AUGMENT-HF: A Multicenter Randomized Controlled Clinical Trial of the Efficacy of Left Ventricular Augmentation with Algisyl-LVR in the Treatment of Heart Failure* Douglas
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS
 65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
How should we treat atrial fibrillation in heart failure
 Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
Echocardiography Guided Cardiac Resynchronization Therapy in Patients with Symptomatic Heart Failure and Narrow QRS Complex
 Echocardiography Guided Cardiac Resynchronization Therapy in Patients with Symptomatic Heart Failure and Narrow QRS Complex Johannes Holzmeister, M.D. University of Zurich, Zurich, Switzerland on behalf
Echocardiography Guided Cardiac Resynchronization Therapy in Patients with Symptomatic Heart Failure and Narrow QRS Complex Johannes Holzmeister, M.D. University of Zurich, Zurich, Switzerland on behalf
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
SEX INCLUSION in CLINICAL TRIALS
 SEX INCLUSION in CLINICAL TRIALS MARJORIE R. JENKINS, MD MEHP FACP PROFESSOR OF MEDICINE CHIEF SCIENTIFIC OFFICER RUSH ENDOWED CHAIR FOR EXCELLENCE IN RESEARCH LAURA W. BUSH INSTITUTE FOR WOMEN S HEALTH
SEX INCLUSION in CLINICAL TRIALS MARJORIE R. JENKINS, MD MEHP FACP PROFESSOR OF MEDICINE CHIEF SCIENTIFIC OFFICER RUSH ENDOWED CHAIR FOR EXCELLENCE IN RESEARCH LAURA W. BUSH INSTITUTE FOR WOMEN S HEALTH
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Stakeholder Guide 2014 www.effectivehealthcare.ahrq.gov
 Stakeholder Guide 2014 www.effectivehealthcare.ahrq.gov AHRQ Publication No. 14-EHC010-EF Replaces Publication No. 11-EHC069-EF February 2014 Effective Health Care Program Stakeholder Guide Contents Introduction...1
Stakeholder Guide 2014 www.effectivehealthcare.ahrq.gov AHRQ Publication No. 14-EHC010-EF Replaces Publication No. 11-EHC069-EF February 2014 Effective Health Care Program Stakeholder Guide Contents Introduction...1
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
If several different trials are mentioned in one publication, the data of each should be extracted in a separate data extraction form.
 General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
When to Implant an ICD and Which One. Brad Suprenant DO, FACC, FACOI
 When to Implant an ICD and Which One Brad Suprenant DO, FACC, FACOI Major Implantable Cardioverter-Defibrillator Trials for Secondary Prevention of Sudden Cardiac Death Trial Year Patients (n) Inclusion
When to Implant an ICD and Which One Brad Suprenant DO, FACC, FACOI Major Implantable Cardioverter-Defibrillator Trials for Secondary Prevention of Sudden Cardiac Death Trial Year Patients (n) Inclusion
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation. Michael Acker, MD For the CTSN Investigators AHA November 2013
 Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
Mitral Valve Repair versus Replacement for Severe Ischemic Mitral Regurgitation Michael Acker, MD For the CTSN Investigators AHA November 2013 Acknowledgements Supported by U01 HL088942 Cardiothoracic
How To Write A Systematic Review
 Formulating the Review Question & Writing a Protocol Madhukar Pai, MD, PhD Associate Professor Department of Epidemiology & Biostatistics McGill University, Montreal, Canada Email: madhukar.pai@mcgill.ca
Formulating the Review Question & Writing a Protocol Madhukar Pai, MD, PhD Associate Professor Department of Epidemiology & Biostatistics McGill University, Montreal, Canada Email: madhukar.pai@mcgill.ca
Clinical Trials In Cardiac Rhythm Management
 Clinical Trials In Cardiac Rhythm Management Stuart Allen Principal Cardiac Physiologist Manchester Heart Centre HRUK Council Physiologist Representative stuart.allen@cmft.nhs.uk Clinical Trials Pacemakers
Clinical Trials In Cardiac Rhythm Management Stuart Allen Principal Cardiac Physiologist Manchester Heart Centre HRUK Council Physiologist Representative stuart.allen@cmft.nhs.uk Clinical Trials Pacemakers
Technology Assessment
 Technology Assessment Catheter Ablation for Treatment of Atrial Fibrillation Technology Assessment Program Prepared for: Agency for Healthcare Research and Quality 540 Gaither Road Rockville, Maryland
Technology Assessment Catheter Ablation for Treatment of Atrial Fibrillation Technology Assessment Program Prepared for: Agency for Healthcare Research and Quality 540 Gaither Road Rockville, Maryland
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
PCORI Methodology Standards: Academic Curriculum. 2016 Patient-Centered Outcomes Research Institute. All Rights Reserved.
 PCORI Methodology Standards: Academic Curriculum 2016 Patient-Centered Outcomes Research Institute. All Rights Reserved. Module 5: Step 3 Search the Literature Category 11: Systematic Reviews Prepared
PCORI Methodology Standards: Academic Curriculum 2016 Patient-Centered Outcomes Research Institute. All Rights Reserved. Module 5: Step 3 Search the Literature Category 11: Systematic Reviews Prepared
Steven J. Yakubov, MD FACC For the CoreValve US Clinical Investigators
 Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Main Effect of Screening for Coronary Artery Disease Using CT
 Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
CCAD Training Manual. Cardiac Rhythm Management (CRM)
 CCAD Training Manual Cardiac Rhythm Management (CRM) Version 1.0 A D Cunningham 19/3/2008 Introduction This manual is intended to assist users of the Notes Client version of the CCAD Cardiac Rhythm Management
CCAD Training Manual Cardiac Rhythm Management (CRM) Version 1.0 A D Cunningham 19/3/2008 Introduction This manual is intended to assist users of the Notes Client version of the CCAD Cardiac Rhythm Management
4/7/2015. Cardiac Rehabilitation: From the other side of the glass door. Chicago, circa 1999. Objectives. No disclosures, no conflicts
 Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
Cardiac Rehabilitation: From the other side of the glass door No disclosures, no conflicts Charles X. Kim, MD, FACC, ABVM Objectives 1. Illustrate common CV benefits of CV rehab in real world practice.
DEVICE RECALLS: The Era of Regulation and Outcome Metrics: Optimizing Benefits and Managing Risks
 DEVICE RECALLS: The Era of Regulation and Outcome Metrics: Optimizing Benefits and Managing Risks Kenneth A. Ellenbogen, MD Kontos Professor & Chairman Virginia Commonwealth University School of Medicine
DEVICE RECALLS: The Era of Regulation and Outcome Metrics: Optimizing Benefits and Managing Risks Kenneth A. Ellenbogen, MD Kontos Professor & Chairman Virginia Commonwealth University School of Medicine
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
Telemedicine in the Prevention and Monitoring of Heart Disease
 Telemedicine in the Prevention and Monitoring of Heart Disease Prof. Dr. med. Friedrich Köhler 26. April 2012 Charité-Universitätsmedizin Berlin Facts Founded in 1710 11 Nobel laureates 12.922 employees
Telemedicine in the Prevention and Monitoring of Heart Disease Prof. Dr. med. Friedrich Köhler 26. April 2012 Charité-Universitätsmedizin Berlin Facts Founded in 1710 11 Nobel laureates 12.922 employees
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation
 A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION
 Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Guidance for Industry
 Guidance for Industry Cancer Drug and Biological Products Clinical Data in Marketing Applications U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and
Guidance for Industry Cancer Drug and Biological Products Clinical Data in Marketing Applications U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and
Improving Outcomes and Saving Lives in Real Time: How Hospitals Can Use Predictive Analytics Across the Care Continuum Essential Hospitals Engagement
 Improving Outcomes and Saving Lives in Real Time: How Hospitals Can Use Predictive Analytics Across the Care Continuum Essential Hospitals Engagement Network February 18, 2015 CHAT FEATURE The chat tool
Improving Outcomes and Saving Lives in Real Time: How Hospitals Can Use Predictive Analytics Across the Care Continuum Essential Hospitals Engagement Network February 18, 2015 CHAT FEATURE The chat tool
Technology Assessment
 Technology Assessment Lifestyle Interventions for Four Conditions: Type 2 Diabetes, Metabolic Syndrome, Breast Cancer, and Prostate Cancer Technology Assessment Program Prepared for: Agency for Healthcare
Technology Assessment Lifestyle Interventions for Four Conditions: Type 2 Diabetes, Metabolic Syndrome, Breast Cancer, and Prostate Cancer Technology Assessment Program Prepared for: Agency for Healthcare
Secondary Uses of Data for Comparative Effectiveness Research
 Secondary Uses of Data for Comparative Effectiveness Research Paul Wallace MD Director, Center for Comparative Effectiveness Research The Lewin Group Paul.Wallace@lewin.com Disclosure/Perspectives Training:
Secondary Uses of Data for Comparative Effectiveness Research Paul Wallace MD Director, Center for Comparative Effectiveness Research The Lewin Group Paul.Wallace@lewin.com Disclosure/Perspectives Training:
Cardiac Rehabilitation An Underutilized Class I Treatment for Cardiovascular Disease
 Cardiac Rehabilitation An Underutilized Class I Treatment for Cardiovascular Disease What is Cardiac Rehabilitation? Cardiac rehabilitation is a comprehensive exercise, education, and behavior modification
Cardiac Rehabilitation An Underutilized Class I Treatment for Cardiovascular Disease What is Cardiac Rehabilitation? Cardiac rehabilitation is a comprehensive exercise, education, and behavior modification
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity
 Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Tufts-New England Medical Center Evidence-based Practice Center Boston, MA
 Tufts-New England Medical Center Evidence-based Practice Center Boston, MA Joseph Lau, MD, Director Ethan Balk, MD, MPH, Associate Director Thomas Trikalinos, MD, PhD, Assistant Director Stanley Ip, MD,
Tufts-New England Medical Center Evidence-based Practice Center Boston, MA Joseph Lau, MD, Director Ethan Balk, MD, MPH, Associate Director Thomas Trikalinos, MD, PhD, Assistant Director Stanley Ip, MD,
Measure #257 (NQF 1519): Statin Therapy at Discharge after Lower Extremity Bypass (LEB) National Quality Strategy Domain: Effective Clinical Care
 Measure #257 (NQF 1519): Statin Therapy at Discharge after Lower Extremity Bypass (LEB) National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #257 (NQF 1519): Statin Therapy at Discharge after Lower Extremity Bypass (LEB) National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Establishing a Remote Monitoring Program. Martha Ferrara, FNP
 Establishing a Remote Monitoring Program Martha Ferrara, FNP Establishing a Remote Monitoring Program What is Remote Monitoring? Martha Ferrara, FNP, CCDS November 2012 CIED Timeline: Cardiovascular Implantable
Establishing a Remote Monitoring Program Martha Ferrara, FNP Establishing a Remote Monitoring Program What is Remote Monitoring? Martha Ferrara, FNP, CCDS November 2012 CIED Timeline: Cardiovascular Implantable
Evidence-based Practice Center Comparative Effectiveness Review Protocol
 Evidence-based Practice Center Comparative Effectiveness Review Protocol Project Title: Comparative Effectiveness of Case Management for Adults With Medical Illness and Complex Care Needs I. Background
Evidence-based Practice Center Comparative Effectiveness Review Protocol Project Title: Comparative Effectiveness of Case Management for Adults With Medical Illness and Complex Care Needs I. Background
Breast cancer treatment for elderly women: a systematic review
 Breast cancer treatment for elderly women: a systematic review Gerlinde Pilkington Rumona Dickson Anna Sanniti Funded by the NCEI and POI Elderly people less likely to receive chemotherapy than younger
Breast cancer treatment for elderly women: a systematic review Gerlinde Pilkington Rumona Dickson Anna Sanniti Funded by the NCEI and POI Elderly people less likely to receive chemotherapy than younger
FY2015 Final Hospital Inpatient Rule Summary
 FY2015 Final Hospital Inpatient Rule Summary Interventional Cardiology (IC) Peripheral Interventions (PI) Rhythm Management (RM) On August 4, 2014, the Centers for Medicare & Medicaid Services (CMS) released
FY2015 Final Hospital Inpatient Rule Summary Interventional Cardiology (IC) Peripheral Interventions (PI) Rhythm Management (RM) On August 4, 2014, the Centers for Medicare & Medicaid Services (CMS) released
Management of Symptomatic Atrial Fibrillation
 Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
DISCLOSURES. I am a consultant for Biosense Webster St Jude Medical
 Ablation vs. Amiodarone for Treatment of Atrial Fibrillation in Patients with Congestive Heart Failure and an Implanted ICD/CRTD (AATAC-AF in Heart Failure) ClinicalTrials.gov Identifier: NCT00729911/
Ablation vs. Amiodarone for Treatment of Atrial Fibrillation in Patients with Congestive Heart Failure and an Implanted ICD/CRTD (AATAC-AF in Heart Failure) ClinicalTrials.gov Identifier: NCT00729911/
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013. Reference: NHSCB/A09/PS/b
 Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry
 Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry Results published in European Heart Journal (March 2014) Pier D. Lambiase, Craig Barr, Dominic A.M.J. Theuns, Reinoud Knops,
Worldwide Experience with S-ICD: Early results from the EFFORTLESS Registry Results published in European Heart Journal (March 2014) Pier D. Lambiase, Craig Barr, Dominic A.M.J. Theuns, Reinoud Knops,
Current reporting in published research
 Current reporting in published research Doug Altman Centre for Statistics in Medicine, Oxford, UK and EQUATOR Network Research article A published research article is a permanent record that will be used
Current reporting in published research Doug Altman Centre for Statistics in Medicine, Oxford, UK and EQUATOR Network Research article A published research article is a permanent record that will be used
Alexandra Bargiota Assist. Prof. in Endocrinology University Hopsital of Larissa Thessaly, Greece. www.united4health.eu
 Applying Evidence-Based Medicine with Telehealth the clinician view Assessing the impact of telehealth/telemedicine either via an RCT or an observational study the voice of a clinician Alexandra Bargiota
Applying Evidence-Based Medicine with Telehealth the clinician view Assessing the impact of telehealth/telemedicine either via an RCT or an observational study the voice of a clinician Alexandra Bargiota
November 15, 2013. Ann Laramee MS ANP-BC ACNS-BC CHFN FletcherAllen.org
 Advance Care Planning with Heart Failure: Results of a Primary Care Practitioners Needs Survey 5 th Annual Nursing Research and Evidence Based Practice Symposium November 15, 2013 Ann Laramee MS ANP-BC
Advance Care Planning with Heart Failure: Results of a Primary Care Practitioners Needs Survey 5 th Annual Nursing Research and Evidence Based Practice Symposium November 15, 2013 Ann Laramee MS ANP-BC
Submitted Electronically to AdvanceNotice2016@cms.hhs.gov
 March 6, 2015 Marilyn Tavenner, RN, BSN, MHA Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services 200 Independence Avenue, SW Washington, D.C. 20201 Submitted
March 6, 2015 Marilyn Tavenner, RN, BSN, MHA Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services 200 Independence Avenue, SW Washington, D.C. 20201 Submitted
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
Benefits and Harms of Femtosecond Laser Assisted Cataract Surgery: A Systematic Review
 4 Department of Veterans Affairs Health Services Research & Development Service Benefits and Harms of Femtosecond Laser Assisted Cataract Surgery: A Systematic Review December 2013 Prepared for: Department
4 Department of Veterans Affairs Health Services Research & Development Service Benefits and Harms of Femtosecond Laser Assisted Cataract Surgery: A Systematic Review December 2013 Prepared for: Department
Management of Atrial Fibrillation in Heart Failure
 Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014
 ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
Cardiac Resynchronization Therapy in Patients with and without Atrial Fibrillation
 Original Article CRT in Patients with and without AF Acta Cardiol Sin 2011;27:46 51 Electrophysiology Cardiac Resynchronization Therapy in Patients with and without Atrial Fibrillation Hung-Ta Wo, Po-Cheng
Original Article CRT in Patients with and without AF Acta Cardiol Sin 2011;27:46 51 Electrophysiology Cardiac Resynchronization Therapy in Patients with and without Atrial Fibrillation Hung-Ta Wo, Po-Cheng
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Neal Rouzier responds to the JAMA article on Men and Testosterone
 Neal Rouzier responds to the JAMA article on Men and Testosterone On the first day the JAMA article was released I received 500 emails from physicians and patients requesting my opinion of the article
Neal Rouzier responds to the JAMA article on Men and Testosterone On the first day the JAMA article was released I received 500 emails from physicians and patients requesting my opinion of the article
Treatment of Low Risk MDS. Overview. Myelodysplastic Syndromes (MDS)
 Overview Amy Davidoff, Ph.D., M.S. Associate Professor Pharmaceutical Health Services Research Department, Peter Lamy Center on Drug Therapy and Aging University of Maryland School of Pharmacy Clinical
Overview Amy Davidoff, Ph.D., M.S. Associate Professor Pharmaceutical Health Services Research Department, Peter Lamy Center on Drug Therapy and Aging University of Maryland School of Pharmacy Clinical
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
MIND-BODY THERAPIES FOR HYPERTENSION
 MIND-BODY THERAPIES FOR HYPERTENSION Systematic Review and Meta-Analysis Ather Ali, ND, MPH (1), David L. Katz, MD, MPH (1,2), Michael B. Bracken, PhD, MPH (2). (1)Yale-Griffin Prevention Research Center
MIND-BODY THERAPIES FOR HYPERTENSION Systematic Review and Meta-Analysis Ather Ali, ND, MPH (1), David L. Katz, MD, MPH (1,2), Michael B. Bracken, PhD, MPH (2). (1)Yale-Griffin Prevention Research Center
STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013
 1. INTRODUCTION STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013 This document replaces the previous Heart Rhythm UK documents Clinical Guidance by Consensus
1. INTRODUCTION STANDARDS FOR IMPLANTATION AND FOLLOW-UP OF CARDIAC RHYTHM MANAGEMENT DEVICES IN ADULTS January 2013 This document replaces the previous Heart Rhythm UK documents Clinical Guidance by Consensus
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular
 Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
What factors determine poor functional outcome following Total Knee Replacement (TKR)?
 Specific Question: What factors determine poor functional outcome following Total Knee Replacement ()? Clinical bottom line All groups derived benefit from undergoing a, reviews suggests that the decision
Specific Question: What factors determine poor functional outcome following Total Knee Replacement ()? Clinical bottom line All groups derived benefit from undergoing a, reviews suggests that the decision
Identifying and Prioritizing Research Gaps. Tim Carey, M.D., M.P.H. Amica Yon, Pharm.D. Chris Beadles, M.D. Roberta Wines, M.P.H.
 Identifying and Prioritizing Research Gaps Tim Carey, M.D., M.P.H. Amica Yon, Pharm.D. Chris Beadles, M.D. Roberta Wines, M.P.H. 1 Importance: Why We Need to Identify and Prioritize Research Gaps from
Identifying and Prioritizing Research Gaps Tim Carey, M.D., M.P.H. Amica Yon, Pharm.D. Chris Beadles, M.D. Roberta Wines, M.P.H. 1 Importance: Why We Need to Identify and Prioritize Research Gaps from
Marcus Wilson, PharmD. First Plenary Session
 Moderator First Plenary Session THE USE OF "BIG DATA" - WHERE ARE WE AND WHAT DOES THE FUTURE HOLD? Marcus Wilson, PharmD HealthCore Wilmington, DE, USA Speakers First Plenary Session THE USE OF "BIG DATA"
Moderator First Plenary Session THE USE OF "BIG DATA" - WHERE ARE WE AND WHAT DOES THE FUTURE HOLD? Marcus Wilson, PharmD HealthCore Wilmington, DE, USA Speakers First Plenary Session THE USE OF "BIG DATA"
Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease
 Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
MISSING DATA ANALYSIS AMONG PATIENTS IN THE PINNACLE REGISTRY
 MISSING DATA ANALYSIS AMONG PATIENTS IN THE PINNACLE REGISTRY In order to improve the efficiency of PINNACLE Registry data analytics, a missing data analysis has been conducted on PINNACLE Registry data
MISSING DATA ANALYSIS AMONG PATIENTS IN THE PINNACLE REGISTRY In order to improve the efficiency of PINNACLE Registry data analytics, a missing data analysis has been conducted on PINNACLE Registry data
Electrophysiology. The AFFIRM Investigators*
 Electrophysiology Clinical factors that influence response to treatment strategies in atrial fibrillation: The Atrial Fibrillation Follow-up Investigation of Rhythm Management (AFFIRM) Study The AFFIRM
Electrophysiology Clinical factors that influence response to treatment strategies in atrial fibrillation: The Atrial Fibrillation Follow-up Investigation of Rhythm Management (AFFIRM) Study The AFFIRM
How To Improve Health Care For Remote Workers
 CRM Devices and Telemonitoring Where the industry stands today Annette Brüls VP CRDM Marketing CareLink Status worldwide More than 450.000000 patients in > 4000 clinics > 30 countries 9 years of experience
CRM Devices and Telemonitoring Where the industry stands today Annette Brüls VP CRDM Marketing CareLink Status worldwide More than 450.000000 patients in > 4000 clinics > 30 countries 9 years of experience
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Objectives. Preoperative Cardiac Risk Stratification for Noncardiac Surgery. History
 Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Preoperative Cardiac Risk Stratification for Noncardiac Surgery Kimberly Boddicker, MD FACC Essentia Health Heart and Vascular Center 27 th Heart and Vascular Conference May 13, 2011 Objectives Summarize
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Cloud Computing / Tele- Health in a Novel Integrated CHF Disease Management Program: The Israeli Experience
 Cloud Computing / Tele- Health in a Novel Integrated CHF Disease Management Program: The Israeli Experience Haim Silber MD Programs Initiator Maccabi Health Care services and Gertner Institute, ISRAEL
Cloud Computing / Tele- Health in a Novel Integrated CHF Disease Management Program: The Israeli Experience Haim Silber MD Programs Initiator Maccabi Health Care services and Gertner Institute, ISRAEL
Committee Approval Date: September 12, 2014 Next Review Date: September 2015
 Medication Policy Manual Policy No: dru361 Topic: Pradaxa, dabigatran Date of Origin: September 12, 2014 Committee Approval Date: September 12, 2014 Next Review Date: September 2015 Effective Date: November
Medication Policy Manual Policy No: dru361 Topic: Pradaxa, dabigatran Date of Origin: September 12, 2014 Committee Approval Date: September 12, 2014 Next Review Date: September 2015 Effective Date: November
How To Calculate The Cost Of Diabetic Foot Ulcers
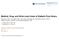 Medical, Drug, and Work-Loss Costs of Diabetic Foot Ulcers Brad Rice, PhD; 1 Urvi Desai, PhD; 1 Alice Kate Cummings, BA; 1 Michelle Skornicki, MPH; 2 Nathan Parsons, RN BSN; 2 and Howard Birnbaum, PhD
Medical, Drug, and Work-Loss Costs of Diabetic Foot Ulcers Brad Rice, PhD; 1 Urvi Desai, PhD; 1 Alice Kate Cummings, BA; 1 Michelle Skornicki, MPH; 2 Nathan Parsons, RN BSN; 2 and Howard Birnbaum, PhD
Taming Of The Queue VI. Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute
 Taming Of The Queue VI Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute March 2009 The Heart Failure Continuum 2 Leadership. Knowledge. Community. HF Readmissions Hospital
Taming Of The Queue VI Christine Struthers APN Cardiac Telehealth University of Ottawa Heart Institute March 2009 The Heart Failure Continuum 2 Leadership. Knowledge. Community. HF Readmissions Hospital
Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial
 Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial Connie N. Hess, MD, MHS, Stefan James, MD, PhD, Renato D. Lopes, MD, PhD, Daniel M. Wojdyla,
Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial Connie N. Hess, MD, MHS, Stefan James, MD, PhD, Renato D. Lopes, MD, PhD, Daniel M. Wojdyla,
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness
 Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure
 Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure Gaetano M. De Ferrari, MD Dept. of Cardiology, Fondazione IRCCS Policlinico S. Matteo, Pavia, Italy for the CardioFit
Chronic Vagus Nerve Stimulation: A New Treatment Modality for Congestive Heart Failure Gaetano M. De Ferrari, MD Dept. of Cardiology, Fondazione IRCCS Policlinico S. Matteo, Pavia, Italy for the CardioFit
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery
 The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
Executive Summary: Diabetes and Commercial Motor Vehicle Driver Safety. September 8, 2006
 Executive Summary: Diabetes and Commercial Motor Vehicle Driver Safety Presented to Federal Motor Carrier Safety Administration September 8, 2006 Prepared for Prepared by MANILA Consulting Group, Inc.
Executive Summary: Diabetes and Commercial Motor Vehicle Driver Safety Presented to Federal Motor Carrier Safety Administration September 8, 2006 Prepared for Prepared by MANILA Consulting Group, Inc.
Cardiac Rhythm Device Summit:
 Division of Cardiovascular Diseases Cardiac Rhythm Device Summit: Implantation, Management, and Follow Up June 17-19, 2016 Swissotel Chicago Course Directors: LEARN. ADVANCE. CONNECT. celinks.mayo.edu/cardiacdevice2016
Division of Cardiovascular Diseases Cardiac Rhythm Device Summit: Implantation, Management, and Follow Up June 17-19, 2016 Swissotel Chicago Course Directors: LEARN. ADVANCE. CONNECT. celinks.mayo.edu/cardiacdevice2016
Telecardiology Technical Innovations and Challegenes in Clinical Practice
 Telecardiology Technical Innovations and Challegenes in Clinical Practice Axel Müller Clinic of Internal Medicine I (Head of Department: Prof. Dr. med. J. Schweizer) Klinikum Chemnitz ggmbh June 24, 2015
Telecardiology Technical Innovations and Challegenes in Clinical Practice Axel Müller Clinic of Internal Medicine I (Head of Department: Prof. Dr. med. J. Schweizer) Klinikum Chemnitz ggmbh June 24, 2015
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Mortality Assessment Technology: A New Tool for Life Insurance Underwriting
 Mortality Assessment Technology: A New Tool for Life Insurance Underwriting Guizhou Hu, MD, PhD BioSignia, Inc, Durham, North Carolina Abstract The ability to more accurately predict chronic disease morbidity
Mortality Assessment Technology: A New Tool for Life Insurance Underwriting Guizhou Hu, MD, PhD BioSignia, Inc, Durham, North Carolina Abstract The ability to more accurately predict chronic disease morbidity
Research Skills for Non-Researchers: Using Electronic Health Data and Other Existing Data Resources
 Research Skills for Non-Researchers: Using Electronic Health Data and Other Existing Data Resources James Floyd, MD, MS Sep 17, 2015 UW Hospital Medicine Faculty Development Program Objectives Become more
Research Skills for Non-Researchers: Using Electronic Health Data and Other Existing Data Resources James Floyd, MD, MS Sep 17, 2015 UW Hospital Medicine Faculty Development Program Objectives Become more
