Bipolar Disorder BPD 1
|
|
|
- Julie McDonald
- 7 years ago
- Views:
Transcription
1 Bipolar Disorder BPD Bipolar disorder is characterized by episodes in which the person s mood and activity levels are significantly disturbed. This disturbance consists on some occasions of an elevation of mood and increased energy and activity (mania), and on others of a lowering of mood and decreased energy and activity (depression). Characteristically, recovery is complete between episodes. People who experience only manic episodes are also classified as having bipolar disorder.
2 Bipolar Disorder BPD 1 Assessment and Management Guide 1. Is the person in a manic state? look for:» Elevated, expansive or irritable mood» Increased activity, restlessness, excitement» Increased talkativeness» Loss of normal social inhibitions» Decreased need for sleep» Inflated self-esteem» Distractibility» Elevated sexual energy or sexual indiscretion Ask about:» Symptom duration» Whether symptoms interfered with usual responsibilities related to work, school, domestic or social activities» Whether hospitalization was required if the person has:» multiple symptoms» lasting for at least 1 week» severe enough to interfere significantly with work and social activities or requiring hospitalization mania is likely if manic symptoms are associated with drug intoxication, refer to Drug use Disorders Module» DRu» Begin treatment of acute mania with lithium, valproate, carbamazepine or with antipsychotics.» BPD 3.1» Consider a short-term benzodiazepine (such as diazepam) for behavioural disturbance or agitation.» BPD 3.2» Discontinue any antidepressants.» BPD 3.3» Advise the person to modify lifestyle; provide information about bipolar disorder and its treatment.» BPD 2.1» Provide regular follow-up.» BPD 2.4» Begin treatment with a mood-stabilizer.» BPD 4» Consider antidepressant combined with mood stabilizer for moderate / severe depression according to suggestions in Depression Module.» DEP 2. Does the person have a known prior episode of mania but now has depression? (Assess according to Depression Module» DEP ) if YES, then bipolar depression is likely. inform the person about the risk of switching to mania before starting antidepressant medication» Advise the person to modify lifestyle; provide information about bipolar disorder and its treatment.» BPD 2.1» Reactivate social networks.» BPD 2.2» If available, consider psychological interventions.» int» Pursue rehabilitation, including appropriate economic and educational activities, using formal and informal systems.» BPD 2.3» Provide regular follow-up.» BPD 2.4 Bipolar Disorder» Assessment and Management Guide 24
3 25 Bipolar Disorder BPD 1 Assessment and Management Guide 3. Look for presence of concurrent conditions if YES» Manage both the bipolar disorder and the concurrent condition.» Alcohol use or drug use disorders» Dementia» Suicide / self-harm» Concurrent medical illness, especially hyper- or hypothyroidism, renal or cardiovascular disease 4. Is the person not currently manic or depressed but has a history of mania? This person most likely has bipolar disorder and is currently between episodes. Relapse prevention is needed if the person has had:» 2 or more acute episodes (e.g. 2 episodes of mania, or one episode of mania and one episode of depression) or» a single manic episode involving significant risk and adverse consequences» If the person is not on a mood stabilizer then begin one.» BPD 4» Advise person to modify lifestyle; provide information about bipolar disorder and its treatment.» BPD 2.1» Reactivate social networks.» BPD 2.2» Pursue rehabilitation, including appropriate economic and educational activities, using formal and informal systems.» BPD 2.3» Provide regular follow-up; monitor side-effects and adherence.» BPD 2.4
4 Bipolar Disorder BPD 1 Assessment and Management Guide 5. Is the person in a special group?» Pregnant or breast-feeding» consult A SPEciAliSt, if available.» Avoid starting treatment with a mood stabilizer.» Consider low-dose haloperidol (with caution).» If a pregnant woman develops acute mania while taking a mood stabilizer, consider changing to low-dose haloperidol.» Elderly» Use lower doses of medication.» Anticipate increased risk of drug interactions.» Adolescent» Presenting symptoms may be atypical.» Take special care to ensure adherence to treatment.» consult A SPEciAliSt, if available. Bipolar Disorder» Assessment and Management Guide 26
5 27 Bipolar Disorder BPD 2 Intervention Details Psychosocial interventions 2.1 Psychoeducation Messages to people with bipolar disorder (not currently in acute manic state) and to family members of people with bipolar disorder» Explanation: Bipolar disorder is a mental health condition that tends to involve extreme moods, which may go from feeling very depressed and fatigued to feeling extremely energetic, irritated and overly excited.» There needs to be some method for monitoring mood, such as keeping a daily mood log in which irritability, anger or euphoria are recorded.» It is important to maintain a regular sleep cycle (e.g. going to bed at the same time every night, trying to sleep the same amount as before illness, avoiding sleeping much less than usual).» Relapses need to be prevented, by recognizing when symptoms return, such as sleeping less, spending more money or feeling much more energetic than usual, and coming back for treatment when these occur.» A person in a manic state lacks insight into the illness and may even enjoy the euphoria and improved energy, so carers must be part of relapse prevention.» Alcohol and other psychoactive substances should be avoided.» Since lifestyle changes should be continued as long as needed, potentially indefinitely, they should be planned and developed for sustainability.» The person should be encouraged to seek support after significant life events (e.g. bereavement) and to talk to family and friends.» General coping strategies, such as planning a regular work or school schedule that avoids sleep deprivation, improving social support systems, discussing and soliciting advice about major decisions (especially ones involving money or major commitments) need to be enhanced.» The family s physical, social and mental health needs should be considered.» Build rapport: Mutual trust between the person and the health-care staff is critical for a person with bipolar disorder, since a positive therapeutic alliance may improve the longterm outcome, especially by improving treatment adherence. 2.2 Reactivate social networks» Identify the person s prior social activities that, if reinitiated, would have the potential for providing direct or indirect psychosocial support (e.g. family gatherings, outings with friends, visiting neighbours, social activities at work sites, sports, community activities).» Actively encourage the person to resume these social activities and advise family members about this. 2.3 Rehabilitation» Facilitate opportunities for people and their carers to be included in economic, educational and cultural activities appropriate to their cultural environment, using available formal and informal systems.» Consider supported employment for those who have difficulty obtaining or retaining normal employment. 2.4 Follow-up» Regular follow-up is required. The relapse rate is high and those in a manic state are often unable to see the need for treatment, so treatment non-adherence is common and involvement of carers is critical during such periods.» At each follow-up, assess symptoms, side-effects of medications, adherence and the need for psychosocial interventions.» A person with mania should return for evaluation as frequently as warranted. The evaluation should be more frequent until the manic episode is over.» Provide information about the illness and treatment to the person and their carers, particularly regarding the signs and symptoms of mania, the importance of regular adherence to medication, even in the absence of symptoms, and the characteristic difficulty the person may sometimes have in understanding the need for treatment. If a person has no carer or person at least to check on them periodically, encourage recruiting someone from the person s community, ideally someone from their network of friends and family.
6 Bipolar Disorder BPD 3 Intervention Details Treatment of acute mania 3.1 Lithium, valproate, carbamazepine or antipsychotics Consider lithium, valproate, carbamazepine or antipsychotics for treatment of acute mania. Lithium may be considered only if clinical and laboratory monitoring are available. If symptoms are severe, consider using an antipsychotic, since onset of effectiveness is more rapid than with mood stabilizers. For details regarding dose, monitoring, adverse effects, etc, see the section on mood stabilizers in the maintenance treatment of bipolar disorders and the table on mood stabilizers.» BPD 4 For details of the use of antipsychotics, refer to the Psychosis Module, pharmacological interventions.» PSY Benzodiazepines Person in a manic state who is experiencing agitation may benefit from short-term use of a benzodiazepine such as diazepam. Benzodiazepines should be discontinued gradually as soon as symptoms improve, as tolerance can develop. 3.3 Antidepressants If mania develops in a person on antidepressants, stop the antidepressants as soon as possible, abruptly or gradually, weighing the risk of discontinuation symptoms (refer to Depression Module, pharmacological interventions, see» DEP) against the risk of the antidepressant worsening the mania. People with bipolar disorder should not receive antidepressants alone because of the risk of inducing mania, particularly with tricyclic antidepressants. Antidepressants are less likely to induce mania when prescribed in conjunction with lithium, antipsychotic therapy or valproate. 3.4 Monitoring Treatment should be regularly monitored and its effect assessed after 3 and 6 weeks. If the person has not improved after 6 weeks, consider switching to a medication that has not been tried, or adding another medication in combination therapy, such as an antipsychotic plus a mood stabilizer. If combination therapy proves ineffective, consult A SPEciAliSt. Bipolar Disorder» Intervention Details 28
7 29 Bipolar Disorder BPD 4 Intervention Details Maintenance treatment of bipolar disorders Choosing a mood stabilizer (lithium, valproate, carbamazepine) 4.1 Lithium» Consider lithium only if clinical and laboratory monitoring is available.» Lithium monotherapy is effective against the relapse of both mania and depression, although it is most effective as an antimanic agent.» Before beginning lithium therapy, obtain renal function tests, thyroid function tests, complete blood count, electrocardiogram and a pregnancy test, if possible. note: Lithium treatment requires close monitoring of serum level, since the medication has a narrow therapeutic range. In addition, thyroid function must be checked every 6 12 months. If laboratory examinations are not available or feasible, lithium should be avoided. Erratic compliance or stopping lithium treatment suddenly may increase the risk of relapse. Do not prescribe lithium where the lithium supply may be frequently interrupted.» Start with a low dose (300 mg at night) increasing gradually while monitoring the blood concentration every 7 days until it is meq / litre. Once therapeutic blood levels have been achieved, check the blood levels every 2 3 months.» It takes at least 6 months to determine lithium s full effectiveness as maintenance treatment in bipolar disorder.» Advise the person to maintain fluid intake, particularly after sweating, or if immobile for long periods or febrile.» Seek medical attention if the person develops diarrhoea or vomiting.» A person taking lithium should avoid over-the-counter nonsteroidal anti-inflammatory drugs.» If a severe metabolic or respiratory disturbance occurs, consider stopping lithium treatment for up to 7 days. 4.2 Valproate» Before beginning valproate treatment, take a history of cardiovascular, renal or hepatic disease.» Start with a low dose (500 mg / day), increasing (as tolerated) to the target dose.» Monitor closely for response, side-effects and adherence. Explain the signs and symptoms of blood and liver disorders, and advise the person to seek immediate help if these develop.» Reduce the dose of medication if intolerable side-effects persist. If reduction in dose does not help, consider switching to another antimanic agent. 4.3 Carbamazepine» If lithium and valproate are ineffective or poorly tolerated, or if therapy with one of these agents is not feasible, consider carbamazepine.» Before and during carbamazepine therapy, take a history of cardiovascular, renal or hepatic disease.» Start with a low dose (200 mg / day at bedtime) and slowly increase until a dose of mg / day is achieved.» Health-care providers should consider that the dose may need to be adjusted after 2 weeks due to hepatic enzyme induction.» Reduce the dose of medication if intolerable side-effects persist. If reduction in dose does not help, consider switching to another antimanic agent. Avoid lithium, valproate and carbamazepine in pregnant women, and weigh the risks and benefits in women of childbearing age. If the person has frequent relapses or continuing functional impairment, consider switching to a different mood stabilizer or adding a second mood stabilizer. consult A SPEciAliSt.
8 Bipolar Disorder BPD 4 Intervention Details Maintenance treatment of bipolar disorders 4.4 Discontinuation of mood stabilizers» In a person not currently in a manic or depressed state (bipolar disorder between episodes), follow up every 3 months. Continue treatment and monitor closely for relapse.» Continue maintenance treatment with the mood stabilizer for at least 2 years after the last bipolar episode.» However, if a person has had severe episodes with psychotic symptoms or frequent relapses, consult A SPEciAliSt regarding the decision to discontinue maintenance treatment after 2 years.» When discontinuing medications, reduce gradually over a period of weeks or months.» If switching to another medication, begin that medication first and treat with both medications for 2 weeks before tapering off the first medication. Table: Mood Stabilizers This table is for quick reference only and is not intended to be an exhaustive guide to the medications, their dosing and side-effects. Additional details are given in Pharmacological Treatment of Mental Disorders in Primary Health Care (WHO, 2009) ( Medication: Lithium Valproate Carbamazepine Starting dose (mg): typical effective dose (mg): Route: oral oral oral target blood level: noteworthy side effects: meq / litre mania: meq / litre; maintenance: meq / litre. Regular serum level monitoring is critical. Impaired coordination, polyuria, polydypsia, cognitive problems, cardiac arrhythmias, diabetes insipidus, hypothyroidism Not routinely recommended Caution if there is underlying hepatic disease. Hair loss and, rarely, pancreatitis are possible. Not routinely recommended Diplopia, impaired coordination, rash, liver enzyme elevations; Rarely: Stevens-Johnson syndrome, aplastic anaemia. Sedation: Tremor: Weight gain: Hepatotoxicity: Thrombocytopenia: Leucopoenia, mild asymptomatic: Bipolar Disorder» Intervention Details 30
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Quick reference guide Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care Developed by the National Collaborating
Quick reference guide Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care Developed by the National Collaborating
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
A Manic Episode is defined by a distinct period during which there is an abnormally and persistently elevated, expansive, or irritable mood.
 Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Symptoms of mania can include: 3
 Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR. 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014
 COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Bipolar disorder. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA
 COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING BIPOLAR DISORDER
 TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. 1 For Continuing Medical
TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. 1 For Continuing Medical
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
B i p o l a r D i s o r d e r
 B i p o l a r D i s o r d e r Professor Ian Jones Director National Centre for Mental Health www.ncmh.info @ncmh_wales /WalesMentalHealth 029 2074 4392 info@ncmh.info Robert Schumann 1810-1856 Schumann's
B i p o l a r D i s o r d e r Professor Ian Jones Director National Centre for Mental Health www.ncmh.info @ncmh_wales /WalesMentalHealth 029 2074 4392 info@ncmh.info Robert Schumann 1810-1856 Schumann's
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Medications for bipolar disorder
 Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Adjunctive psychosocial intervention. Conditions requiring dose reduction. Immediate, peak plasma concentration is reached within 1 hour.
 Shared Care Guideline for Prescription and monitoring of Naltrexone Hydrochloride in alcohol dependence Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist,
Shared Care Guideline for Prescription and monitoring of Naltrexone Hydrochloride in alcohol dependence Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist,
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
THE BASICS. Community Based Medically Assisted Alcohol Withdrawal. World Health Organisation 2011. The Issues 5/18/2011. RCGP Conference May 2011
 RCGP Conference May 2011 Community Based Medically Assisted Alcohol Withdrawal THE BASICS An option for consideration World Health Organisation 2011 Alcohol is the world s third largest risk factor for
RCGP Conference May 2011 Community Based Medically Assisted Alcohol Withdrawal THE BASICS An option for consideration World Health Organisation 2011 Alcohol is the world s third largest risk factor for
Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole)
 EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
DEMENTIA EDUCATION & TRAINING PROGRAM
 The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers
 SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
FACT SHEET 4. Bipolar Disorder. What Is Bipolar Disorder?
 FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance
 Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance Introduction Indication/Licensing information: Naltrexone is licensed for use as an additional therapy, within
Naltrexone Shared Care Guideline for the treatment of alcohol dependence and opioid dependance Introduction Indication/Licensing information: Naltrexone is licensed for use as an additional therapy, within
Remeron (mirtazapine)
 Remeron (mirtazapine) FDA ALERT [07/2005] Suicidal Thoughts or Actions in Children and Adults Patients with depression or other mental illnesses often think about or attempt suicide. Closely watch anyone
Remeron (mirtazapine) FDA ALERT [07/2005] Suicidal Thoughts or Actions in Children and Adults Patients with depression or other mental illnesses often think about or attempt suicide. Closely watch anyone
Treatments for Major Depression. Drug Treatments The two (2) classes of drugs that are typical antidepressants are:
 Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
See also www.thiswayup.org.au/clinic for an online treatment course.
 Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS
 BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
Dementa Formulary Guidance [v1.0]
![Dementa Formulary Guidance [v1.0] Dementa Formulary Guidance [v1.0]](/thumbs/29/13622067.jpg) Dementa Formulary Guidance [v1.0] 1. Introduction These Guidelines are intended for routine use. However there will be instances where they are not suitable for the patient you are managing, where more
Dementa Formulary Guidance [v1.0] 1. Introduction These Guidelines are intended for routine use. However there will be instances where they are not suitable for the patient you are managing, where more
Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome
 Dr. May Lam Assistant Professor, Department of Psychiatry, The University of Hong Kong Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome a mental state in
Dr. May Lam Assistant Professor, Department of Psychiatry, The University of Hong Kong Psychosis Psychosis-substance use Bipolar Affective Disorder Programmes EASY JCEP EPISO Prodrome a mental state in
This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC.
 This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC. Indiana University School of Medicine and CME Outfitters, LLC, gratefully acknowledge
This continuing education activity is co-sponsored by Indiana University School of Medicine and by CME Outfitters, LLC. Indiana University School of Medicine and CME Outfitters, LLC, gratefully acknowledge
Paxil/Paxil-CR (paroxetine)
 Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
Generic name: Paroxetine Available strengths: 10 mg, 20 mg, 30 mg, 40 mg tablets; 10 mg/5 ml oral suspension; 12.5 mg, 25 mg, 37.5 mg controlled-release tablets (Paxil-CR) Available in generic: Yes, except
North of Tyne Area Prescribing Committee
 North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
ADVANCED BEHAVIORAL HEALTH, INC. Clinical Level of Care Guidelines - 2015
 The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
Drugs for Alcohol Dependence: Clinical Guidance and Three Way Agreement
 Drugs for Alcohol Dependence: Clinical Guidance and Three Way Agreement for County Durham In partnership with the GP, the client, and the County Durham Drug and Alcohol Service December 2015 Version 1.0
Drugs for Alcohol Dependence: Clinical Guidance and Three Way Agreement for County Durham In partnership with the GP, the client, and the County Durham Drug and Alcohol Service December 2015 Version 1.0
Trileptal (Oxcarbazepine)
 Brand and Generic Names: Trileptal Tablets: 150mg, 300mg, 600mg Liquid Suspension: 300mg/5mL Generic name: oxcarbazepine What is Trileptal and what does it treat? Trileptal (Oxcarbazepine) Oxcarbazepine
Brand and Generic Names: Trileptal Tablets: 150mg, 300mg, 600mg Liquid Suspension: 300mg/5mL Generic name: oxcarbazepine What is Trileptal and what does it treat? Trileptal (Oxcarbazepine) Oxcarbazepine
Recognition and Treatment of Depression in Parkinson s Disease
 Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Alcohol information. A standard drink contains about 10g of alcohol takes a healthy liver about 1 hour to remove alcohol from the body.
 Alcohol information Facts about alcohol use Alcohol (grog) is the most widely used recreational drug in Australia NT drinks 70% more and WA 25% more than the rest of Australia Alcohol related deaths for
Alcohol information Facts about alcohol use Alcohol (grog) is the most widely used recreational drug in Australia NT drinks 70% more and WA 25% more than the rest of Australia Alcohol related deaths for
Clinical Audit: Prescribing antipsychotic medication for people with dementia
 Clinical Audit: Prescribing antipsychotic medication for people with dementia Trust, team and patient information Q1. Patient's DIS number... Q2. Patient s residence: Home Residential Home Nursing Home
Clinical Audit: Prescribing antipsychotic medication for people with dementia Trust, team and patient information Q1. Patient's DIS number... Q2. Patient s residence: Home Residential Home Nursing Home
TREATING BIPOLAR DISORDER
 TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. A guideline watch,
TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. A guideline watch,
Feeling Moody? Major Depressive. Disorder. Is it just a bad mood or is it a disorder? Mood Disorders. www.seclairer.com S Eclairer 724-468-3999
 Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
BIPOLAR DISORDER BIPOLAR I DISORDER 4/4/14
 BIPOLAR DISORDER Jason Tentinger PA-C 1. Bipolar I Disorder 2. Bipolar II Disorder 3. Bipolar vs Unipolar Depression 4. Cyclothymic Disorder 5. Treatment Epidemiology BIPOLAR I DISORDER Affects around
BIPOLAR DISORDER Jason Tentinger PA-C 1. Bipolar I Disorder 2. Bipolar II Disorder 3. Bipolar vs Unipolar Depression 4. Cyclothymic Disorder 5. Treatment Epidemiology BIPOLAR I DISORDER Affects around
Postpartum Depression and Post-Traumatic Stress Disorder
 Postpartum Depression and Post-Traumatic Stress Disorder Emotional Recovery: Postpartum Depression and Post-Traumatic Stress Disorder By: Lisa Houchins Published: July 23, 2013 Emotions vary widely after
Postpartum Depression and Post-Traumatic Stress Disorder Emotional Recovery: Postpartum Depression and Post-Traumatic Stress Disorder By: Lisa Houchins Published: July 23, 2013 Emotions vary widely after
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
BIPOLAR DISORDER IN PRIMARY CARE
 E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
Schizoaffective Disorder
 FACT SHEET 10 What Is? Schizoaffective disorder is a psychiatric disorder that affects about 0.5 percent of the population (one person in every two hundred). Similar to schizophrenia, this disorder is
FACT SHEET 10 What Is? Schizoaffective disorder is a psychiatric disorder that affects about 0.5 percent of the population (one person in every two hundred). Similar to schizophrenia, this disorder is
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery
 New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery USING THE 48 HOUR OBSERVATION BED USING THE 48 HOUR OBSERVATION BED Detoxification
New York State Office of Alcoholism & Substance Abuse Services Addiction Services for Prevention, Treatment, Recovery USING THE 48 HOUR OBSERVATION BED USING THE 48 HOUR OBSERVATION BED Detoxification
Schizoaffective disorder
 Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Depression Flow Chart
 Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Review of Pharmacological Pain Management
 Review of Pharmacological Pain Management CHAMP Activities are possible with generous support from The Atlantic Philanthropies and The John A. Hartford Foundation The WHO Pain Ladder The World Health Organization
Review of Pharmacological Pain Management CHAMP Activities are possible with generous support from The Atlantic Philanthropies and The John A. Hartford Foundation The WHO Pain Ladder The World Health Organization
Preconception Clinical Care for Women Medical Conditions
 Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
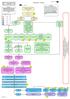 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Diagnosis: Appropriate diagnosis is made according to diagnostic criteria in the current Diagnostic and Statistical Manual of Mental Disorders.
 Page 1 of 6 Approved: Mary Engrav, MD Date: 05/27/2015 Description: Eating disorders are illnesses having to do with disturbances in eating behaviors, especially the consuming of food in inappropriate
Page 1 of 6 Approved: Mary Engrav, MD Date: 05/27/2015 Description: Eating disorders are illnesses having to do with disturbances in eating behaviors, especially the consuming of food in inappropriate
Major Depressive Disorder (MDD) Guideline Diagnostic Nomenclature for Clinical Depressive Conditions
 Major Depressive Disorder Major Depressive Disorder (MDD) Guideline Diagnostic omenclature for Clinical Depressive Conditions Conditions Diagnostic Criteria Duration Major Depression 5 of the following
Major Depressive Disorder Major Depressive Disorder (MDD) Guideline Diagnostic omenclature for Clinical Depressive Conditions Conditions Diagnostic Criteria Duration Major Depression 5 of the following
Guide for family and friends of people affected by bipolar disorders. www.douglas.qc.ca
 Guide for family and friends of people affected by bipolar disorders www.douglas.qc.ca This guide is intended for families, friends and other people who are interested in understanding the different aspects
Guide for family and friends of people affected by bipolar disorders www.douglas.qc.ca This guide is intended for families, friends and other people who are interested in understanding the different aspects
INTOXICATED PATIENTS AND DETOXIFICATION
 VAMC Detoxification Decision Tree Updated May 2006 INTOXICATED PATIENTS AND DETOXIFICATION Patients often present for evaluation of substance use and possible detoxification. There are certain decisions
VAMC Detoxification Decision Tree Updated May 2006 INTOXICATED PATIENTS AND DETOXIFICATION Patients often present for evaluation of substance use and possible detoxification. There are certain decisions
Opioid Prescribing for Chronic Pain: Guidelines for Marin County Clinicians
 Opioid Prescribing for Chronic Pain: Guidelines for Marin County Clinicians Although prescription pain medications are intended to improve the lives of people with pain, their increased use and misuse
Opioid Prescribing for Chronic Pain: Guidelines for Marin County Clinicians Although prescription pain medications are intended to improve the lives of people with pain, their increased use and misuse
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of benzodiazepine misuse
 York Service Management of benzodiazepine misuse Version 2 JT July 2013 page 1 background Note: not all those who use benzodiazepines are dependent, and not all those who are dependent will benefit from
York Service Management of benzodiazepine misuse Version 2 JT July 2013 page 1 background Note: not all those who use benzodiazepines are dependent, and not all those who are dependent will benefit from
MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets
![MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets](/thumbs/40/21035524.jpg) MEDICATION GUIDE TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets Read this Medication Guide before you start taking TRINTELLIX and each time you get a refill. There may be new information. This information
MEDICATION GUIDE TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets Read this Medication Guide before you start taking TRINTELLIX and each time you get a refill. There may be new information. This information
A Carer s Guide to Depression in People with a Learning Disability
 A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
Depression Assessment & Treatment
 Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS
 E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
E-Resource December, 2013 SLEEP DISTURBANCE AND PSYCHIATRIC DISORDERS Between 10-18% of adults in the general population and up to 50% of adults in the primary care setting have difficulty sleeping. Sleep
Topics In Addictions and Mental Health: Concurrent disorders and Community resources. Laurence Bosley, MD, FRCPC
 Topics In Addictions and Mental Health: Concurrent disorders and Community resources Laurence Bosley, MD, FRCPC Overview Understanding concurrent disorders. Developing approaches to treatment Definitions
Topics In Addictions and Mental Health: Concurrent disorders and Community resources Laurence Bosley, MD, FRCPC Overview Understanding concurrent disorders. Developing approaches to treatment Definitions
Update and Review of Medication Assisted Treatments
 Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
Update and Review of Medication Assisted Treatments for Opiate and Alcohol Use Disorders Richard N. Whitney, MD Medical Director Addiction Services Shepherd Hill Newark, Ohio Medication Assisted Treatment
GUIDELINES FOR COMMUNITY ALCOHOL DETOXIFICATION IN SHARED CARE
 GUIDELINES FOR COMMUNITY ALCOHOL DETOXIFICATION IN SHARED CARE Dr Millicent Chikoore MBBS MRCPsych Dr O Lagundoye MBBS MRCPsych Community based alcohol detoxification is a safe and effective option for
GUIDELINES FOR COMMUNITY ALCOHOL DETOXIFICATION IN SHARED CARE Dr Millicent Chikoore MBBS MRCPsych Dr O Lagundoye MBBS MRCPsych Community based alcohol detoxification is a safe and effective option for
Opioid Treatment Services, Office-Based Opioid Treatment
 Optum 1 By United Behavioral Health U.S. Behavioral Health Plan, California Doing Business as OptumHealth Behavioral Solutions of California ( OHBS-CA ) 2015 Level of Care Guidelines Opioid Treatment Services,
Optum 1 By United Behavioral Health U.S. Behavioral Health Plan, California Doing Business as OptumHealth Behavioral Solutions of California ( OHBS-CA ) 2015 Level of Care Guidelines Opioid Treatment Services,
ALCOHOL AND OTHER DRUG WITHDRAWAL: PRACTICE GUIDELINES
 ALCOHOL AND OTHER DRUG WITHDRAWAL: PRACTICE GUIDELINES 2009 Pauline Kenny Amy Swan Lynda Berends Linda Jenner Barbara Hunter Janette Mugavin CHAPTER 12: BENZODIAZEPINE WITHDRAWAL 12 BENZODIAZEPINES These
ALCOHOL AND OTHER DRUG WITHDRAWAL: PRACTICE GUIDELINES 2009 Pauline Kenny Amy Swan Lynda Berends Linda Jenner Barbara Hunter Janette Mugavin CHAPTER 12: BENZODIAZEPINE WITHDRAWAL 12 BENZODIAZEPINES These
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 26 April 2001 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 26 April 2001 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) NOTE FOR GUIDANCE ON CLINICAL
SECTION N: MEDICATIONS. N0300: Injections. Item Rationale Health-related Quality of Life. Planning for Care. Steps for Assessment. Coding Instructions
 SECTION N: MEDICATIONS Intent: The intent of the items in this section is to record the number of days, during the last 7 days (or since admission/reentry if less than 7 days) that any type of injection,
SECTION N: MEDICATIONS Intent: The intent of the items in this section is to record the number of days, during the last 7 days (or since admission/reentry if less than 7 days) that any type of injection,
Lamictal (lamotrigine)
 Lamictal (lamotrigine) Important Warning : Serious skin rashes requiring medical hospitalization and discontinuation of treatment have been associated with Lamictal. Although rare, this rash (also known
Lamictal (lamotrigine) Important Warning : Serious skin rashes requiring medical hospitalization and discontinuation of treatment have been associated with Lamictal. Although rare, this rash (also known
Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31
 Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
Obsessive-compulsive e disorder and body dysmorphic disorder: treatment Clinical guideline Published: 29 November 2005 nice.org.uk/guidance/cg31 NICE 2005. All rights reserved. Contents Introduction...
Smoking Cessation and Mental Health: A briefing for front-line staff
 Smoking Cessation and Mental Health: A briefing for front-line staff 2014 National Centre for Smoking Cessation and Training (NCSCT) Authors: Deborah Robson and Jennifer Potts Editors: Andy McEwen and
Smoking Cessation and Mental Health: A briefing for front-line staff 2014 National Centre for Smoking Cessation and Training (NCSCT) Authors: Deborah Robson and Jennifer Potts Editors: Andy McEwen and
MOOD DISORDERS PART II BIPOLAR AFFECTIVE DISORDER (BAD) Todd Stull, M.D. James Sorrell, M.D.
 MOOD DISORDERS PART II BIPOLAR AFFECTIVE DISORDER (BAD) Todd Stull, M.D. James Sorrell, M.D. BIPOLAR AFFECTIVE DISORDER (BAD) General Assessment is challenging Input important Change in level of functioning
MOOD DISORDERS PART II BIPOLAR AFFECTIVE DISORDER (BAD) Todd Stull, M.D. James Sorrell, M.D. BIPOLAR AFFECTIVE DISORDER (BAD) General Assessment is challenging Input important Change in level of functioning
GMMMG Interface Prescribing Subgroup. Shared Care Template
 GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Ways to support the person with bipolar disorder
 Ways to support the person with bipolar disorder People differ in what help they need and want from caregivers. Caregivers differ in how involved they are in providing support. Finding ways to provide
Ways to support the person with bipolar disorder People differ in what help they need and want from caregivers. Caregivers differ in how involved they are in providing support. Finding ways to provide
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
MEDGUIDE SECTION. What is the most important information I should know about SEROQUEL? SEROQUEL may cause serious side effects, including:
 MEDGUIDE SECTION Medication Guide SEROQUEL (SER-oh-kwell) (quetiapine fumarate) Tablets Read this Medication Guide before you start taking SEROQUEL and each time you get a refill. There may be new information.
MEDGUIDE SECTION Medication Guide SEROQUEL (SER-oh-kwell) (quetiapine fumarate) Tablets Read this Medication Guide before you start taking SEROQUEL and each time you get a refill. There may be new information.
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT ALCOHOL MISUSE
 SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
Depakote (divalproex sodium) - Valproic Acid
 Depakote (divalproex sodium) - Valproic Acid Brand and Generic Names Depakene (Valproic acid) Immediate release Syrup: 250 mg/5ml (there is 250 mg in one teaspoonful) Capsules: 250 mg Depakote /Depakote
Depakote (divalproex sodium) - Valproic Acid Brand and Generic Names Depakene (Valproic acid) Immediate release Syrup: 250 mg/5ml (there is 250 mg in one teaspoonful) Capsules: 250 mg Depakote /Depakote
How to Recognize Depression and Its Related Mood and Emotional Disorders
 How to Recognize Depression and Its Related Mood and Emotional Disorders Dr. David H. Brendel Depression s Devastating Toll on the Individual Reduces or eliminates pleasure and jo Compromises and destroys
How to Recognize Depression and Its Related Mood and Emotional Disorders Dr. David H. Brendel Depression s Devastating Toll on the Individual Reduces or eliminates pleasure and jo Compromises and destroys
Antipsychotics in people with dementia an update and reminder
 www.bpac.org.nz keyword: dementia Antipsychotics in people with dementia an update and reminder Key concepts: Non-pharmacological treatments for the behavioural and psychological symptoms of dementia (BPSD)
www.bpac.org.nz keyword: dementia Antipsychotics in people with dementia an update and reminder Key concepts: Non-pharmacological treatments for the behavioural and psychological symptoms of dementia (BPSD)
Appendix to Tennessee Department of Health: Tennessee Clinical Practice Guidelines for Outpatient Management of Chronic Non- Malignant Pain
 Appendix to Tennessee Department of Health: Tennessee Clinical Practice Guidelines for Outpatient Management of Chronic Non- Malignant Pain Division of Workers Compensation 04.01.2015 Background Opioids
Appendix to Tennessee Department of Health: Tennessee Clinical Practice Guidelines for Outpatient Management of Chronic Non- Malignant Pain Division of Workers Compensation 04.01.2015 Background Opioids
Prescribing Framework for Donepezil in the Treatment and Management of Dementia
 Hull & East Riding Prescribing Committee Prescribing Framework for Donepezil in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker) GP
Hull & East Riding Prescribing Committee Prescribing Framework for Donepezil in the Treatment and Management of Dementia Patients Name:.. NHS Number: Patients Address:... (Use addressograph sticker) GP
information for service providers Schizophrenia & Substance Use
 information for service providers Schizophrenia & Substance Use Schizophrenia and Substance Use Index 2 2 3 5 6 7 8 9 How prevalent are substance use disorders among people with schizophrenia? How prevalent
information for service providers Schizophrenia & Substance Use Schizophrenia and Substance Use Index 2 2 3 5 6 7 8 9 How prevalent are substance use disorders among people with schizophrenia? How prevalent
