Bipolar disorder. Understanding NICE guidance
|
|
|
- Augusta Gardner
- 10 years ago
- Views:
Transcription
1 Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments they should receive. This booklet is about the care and treatment of people with bipolar disorder in the NHS in England and Wales. It explains guidance (advice) from NICE (the National Institute for Health and Clinical Excellence). It is written for adults, children and adolescents with bipolar disorder but it may also be useful for their families or carers or for anyone with an interest in the condition. The booklet aims to help you understand the care and treatment options that should be available in the NHS. It does not describe bipolar disorder or the tests or treatments for it in detail. A member of your healthcare team should discuss these with you. There are examples of questions you could ask throughout this booklet to help you with this. Some sources of further information and support are on page 25. Medical terms printed in bold type are explained on pages Information about NICE clinical guideline 38 Issue date: July 2006
2 Contents Your care 3 Bipolar disorder 4 What should happen when I am first diagnosed? 4 What support can I expect from healthcare professionals? 5 Who can I expect to treat me? 6 What treatments are helpful for people with bipolar disorder? 6 Can I expect treatment in the long-term? 12 How do I stay healthy? 18 Will I be offered any further support? 18 Special issues for women who are pregnant or planning a 19 pregnancy Special issues for children and young people with bipolar 22 disorder Help for families and carers of people with bipolar disorder 24 More information about bipolar disorder 25 Glossary 26 About NICE 28 The advice in the NICE clinical guideline covers: what treatment people with bipolar disorder can expect to be offered, including medication and psychological therapies advice on self-help the services that may help people with bipolar disorder, including psychiatric or specialist mental health services how families and carers may be able to support people with bipolar disorder, and get support for themselves. 2 Information about NICE clinical guideline 38
3 Your care Your treatment and care should take into account your personal needs and preferences, and you have the right to be fully informed and to make decisions in partnership with your healthcare team. To help with this, your healthcare team should give you information you can understand and that is relevant to your circumstances. All healthcare professionals should treat you with respect, sensitivity and understanding and explain bipolar disorder and the treatments for it simply and clearly. The information you get from your healthcare team should include details of the possible benefits and risks of particular treatments. You can ask any questions you want to and can always change your mind as your treatment progresses or your condition or circumstances change. Your own preference for a particular treatment is important and your healthcare team should support your choice of treatment wherever possible, but this does depend on your age. If you are over 16 you can give your own agreement; if you are under 16 and you fully understand all the information you may also be able to give your own agreement; but if you are too young, your parents or carers may also need to agree to treatment. Your treatment and care, and the information you are given about it, should take account of any religious, ethnic or cultural needs you may have. It should also take into account any additional factors, such as physical or learning disabilities, sight or hearing problems, or difficulties with reading or speaking English. Your doctor or nurse should be able to arrange an interpreter or an advocate (someone who supports you in asking for what you want) if needed. If you think that your care does not match what is described in this booklet, please talk to your doctor or nurse. If you agree, your carers and relatives should have the chance to be involved in decisions about your care. Carers and relatives also have the right to the information and support they need in their roles as carers. If people are unable to understand a particular issue or are not able to make decisions for themselves, doctors should follow the advice that the Department of Health has produced about this. You can find this by going to the Department of Health website ( and searching for information on consent. Information about NICE clinical guideline 38 3
4 Bipolar disorder People with bipolar disorder have periods (or episodes ) of what is called mania and periods of depression. For this reason, it was once known as manic depression. It can affect people of any age, from children to older adults (people over 65). During a manic episode, people usually have feelings of elation (extreme happiness or feeling high ), or irritability, or both. They may also feel overconfident, sleep less than usual, and be driven to take unnecessary risks. People with depression feel low and lose pleasure in things they used to enjoy. They may also have other symptoms such as feeling tired all the time, sleep problems and thoughts of suicide or harming themselves. People with bipolar disorder may also have symptoms of psychosis (seeing or believing things that are not real). Episodes of mania and depression may alternate with one another. Some people have no more than one episode a year and feel well otherwise, while others do not get better fully between episodes. Some people may have a less severe type of mania (called hypomania). People who have hypomania and depression are said to have bipolar II disorder. What should happen when I am first diagnosed? If you see your GP about your symptoms, you should usually be offered an appointment with a mental health specialist (usually a doctor called a psychiatrist) if the GP thinks you may have bipolar disorder. If you have mania or severe depression, and there is a risk you could harm yourself or others, your GP should arrange for you to see a specialist immediately. The specialist should ask you a number of questions that will help him or her decide if you have bipolar disorder, and work out what treatments could help you best (called an assessment). The questions will cover events or feelings leading up to your illness, whether other members of your family have bipolar disorder, and whether you have had thoughts of harming yourself or other people. The specialist may talk to a member of your family as well, but should ask for your agreement first. Depending on your symptoms, you may also have tests to see whether you have a physical problem such as thyroid disease. If there is a risk you could harm yourself or others, your healthcare professional should develop a plan with you of what should happen if there is a crisis. 4 Information about NICE clinical guideline 38
5 Questions you could ask healthcare professionals about bipolar disorder What makes you think I have bipolar disorder? What do you think causes bipolar disorder? Are all of my symptoms caused by bipolar disorder? How might bipolar disorder affect my everyday life and what might it mean for my physical health? How can I recognise the early warning signs of an episode of mania or depression? What support can I expect from healthcare professionals? Good information, informed consent and mutual support With the right kind of information you can make informed decisions about your care. However, if you experience very severe symptoms you may no longer be able to make an informed decision or communicate your needs. In case this happens, you can draw up a set of written instructions (called advance directives) saying what treatments and other help you do and do not want. Healthcare professionals can help you write these instructions. Your healthcare professional should give you general advice about coping with your symptoms, such as how to spot the early warning signs of an episode and how to sleep well and have a regular lifestyle. They should also tell you about self-help groups and support groups. Many people find it helpful to meet other people with bipolar disorder and share their experiences as a way of learning how to manage the condition. See page 25 for a list of organisations that can provide more information and support. An equal right to care If you have bipolar disorder and also have a learning difficulty or a personality disorder, you should receive the same level of care as other people with bipolar disorder. Your doctor should take account of any other medication you may be taking when considering what might help you. Information about NICE clinical guideline 38 5
6 Who can I expect to treat me? Most people with bipolar disorder receive most of their treatment from a psychiatrist and other specialist mental health professionals, although your GP will also play an important part in your treatment. If your GP is or has been responsible for your treatment for bipolar disorder, you may be offered an appointment with a psychiatrist or other specialist if you move to a new practice. You should also be offered an appointment if your symptoms become a lot worse, if you are thought to be a risk to yourself or others, if treatment has not helped you, or if you have drug or alcohol problems. Some treatments may not be suitable for you, depending on your exact circumstances. If you have questions about the specific treatments and options covered in this booklet, please talk to your doctor or nurse. Where possible, your care should be provided by the same healthcare professional(s) and you should have regular appointments. If you are being treated by a number of different healthcare professionals, there should be a clear plan about what each of them does to help you. Will I have to stay in hospital or have treatment against my will? You should receive most of your treatment without having to stay in hospital. However, if your symptoms are very severe, or you are being treated under the Mental Health Act, you can be admitted to hospital. As an alternative, you may be offered treatment in a day hospital, where you spend most of the day but return home at night. What treatments are helpful for people with bipolar disorder? There are a number of treatments for adults with bipolar disorder, including: drugs for an episode of mania antidepressants psychological treatments long-term treatment to stabilise your mood and prevent episodes. Some of the drugs used for long-term treatment are the same as those used for treating an episode of mania. When planning your treatment, your doctor should discuss with you any treatment you have had before and your own preference for treatment. He or she should take into account how severe your symptoms are, what treatments have helped you in the past, and be aware of any other drugs you might be taking. 6 Information about NICE clinical guideline 38
7 If you are a woman at an age where you could get pregnant, your doctor should talk to you about the risks involved and about contraception (see the section Special issues for women who are pregnant or planning a pregnancy, page 19). If you have had a manic episode or severe depression, your healthcare professional should meet with you again within 1 week of your first assessment. After that they should see you regularly, for example every 2 4 weeks in the first 3 months and then at longer intervals if the treatment is helping. If you are over 65, you may be cared for by special services for older people. You should be given low doses of medication and your healthcare professional should ask you about any other illnesses or problems. Questions you could ask healthcare professionals about treatment in general What treatment will I need? What choices do I have about treatment? How long will I need treatment? How will having treatment for bipolar disorder affect my daily life and work (for example, can I drive or work machinery)? Physical health checks People with bipolar disorder should have some physical health checks too. This is because they often have other health problems, and because the medication used to treat bipolar disorder can affect their physical health (for example, people often put on weight). At your first check-up, your doctor should ask whether you smoke and how much alcohol you drink. You should also have blood tests, and your blood pressure, weight and height checked. You may be asked to have other tests, such as a chest X-ray and an electrocardiogram (ECG). These tests might need to be repeated if you have long-term treatment; there is more information about this on pages You should then be offered a yearly check-up, which will include questions about smoking and drinking, and a blood pressure test. Your healthcare professional should talk to you about the results and tell other professionals involved in your care. Information about NICE clinical guideline 38 7
8 Treatments for episodes of mania or hypomania If you are taking an antidepressant at the time that a manic episode starts, your doctor should stop the medication. The main drugs used to treat mania are summarised in the tables below. If you are not already taking a drug for mania Medicines you may be offered An antipsychotic (such as olanzapine, quetiapine and risperidone) What you need to know Can be particularly helpful if symptoms are severe or your behaviour is disturbed. You will need checks for side effects (particularly if you have diabetes or are at risk of developing it) and should start on a low dose. If your symptoms do not improve, you may be offered valproate or lithium as well. Lithium Valproate A benzodiazepine Normally offered only if you have relatively mild symptoms and it has helped you before. May be offered if it has helped you before, but not usually offered to women who could get pregnant because it could harm the baby. May be offered in addition to an antipsychotic, lithium or valproate, to help you calm down and sleep better. If you are already taking a drug for mania Medicine that you are already taking An antipsychotic What you need to know The dose should be checked and increased if needed. If symptoms do not improve you may be offered lithium or valproate as well. Lithium The amount in your blood should be checked and the dose increased. If symptoms do not improve or are severe, you may be offered an antipsychotic as well. Valproate The dose should be increased if possible. If symptoms do not improve or are severe, you may be offered an antipsychotic as well. Carbamazepine The dose should not usually be increased. You may be offered an antipsychotic as well. 8 Information about NICE clinical guideline 38
9 Healthcare professionals may give you advice about coping with manic feelings. This may include avoiding situations that make you over-excited; doing things that help you to feel calm; and getting into a good routine, especially making sure you regularly get enough sleep. Treatments for depression If you develop depression when you are already taking medication for mania, your doctor should first check that you are taking the right dose of medication and change it if necessary. You will probably not be offered treatment with an antidepressant right away if your symptoms are relatively mild. But your healthcare professional should arrange to see you again, usually within 2 weeks. If your symptoms are more severe or have become worse you may be offered an antidepressant (a type called a selective serotonin reuptake inhibitor or SSRI). If you are already taking medication for mania that is not an antipsychotic, you may be offered quetiapine. If you are not already taking medication for mania, you should be offered one in addition to the antidepressant because there is a risk that antidepressants can start a manic episode (this is often called switching ). However, if you decide not to take medication for mania your doctor should make sure you know the risks, arrange to see you regularly, and give you a low dose of the antidepressant at first. If drug treatment does not help you, you may be offered a psychological treatment that should help you deal with your depressive thoughts and symptoms and any problems you have, and improve your relationships. Your healthcare professional may also give you advice about helping to reduce symptoms of depression. This may include doing exercise regularly, planning activities, doing things that you enjoy and give you a sense of achievement, and making sure you have a good diet and sleep well. Information about NICE clinical guideline 38 9
10 What you should know about antidepressants If you are offered an antidepressant, you should be given full information about it, including how long it takes to work, the importance of taking the medication as advised, any side effects and advice on what to do if you have them. You and your doctor should be able to discuss any worries you have. Your doctor should see you regularly, particularly when you first start taking an SSRI. If you are under 30 you should usually be seen within 1 week of starting treatment. Your doctor should be aware of any other drugs you may be taking, such as non-steroidal anti-inflammatory drugs (for example, ibuprofen). You may be offered an additional drug to take with it, to prevent a very small risk of bleeding from the stomach. When your symptoms have gone, or improved significantly, your doctor should gradually reduce the dose of the antidepressant over several weeks until you stop taking it. But you should carry on taking medication for mania. Treatment for depression and psychosis If you have depression and psychosis, your doctor may offer you antipsychotic medication in addition to any other treatment you are having. Treatments for episodes of both mania and depression Sometimes people have an episode of both mania and depression the symptoms can be mixed or can alternate very quickly, usually within a few hours. If this happens you may be offered medication for mania, but not usually an antidepressant. Your doctor should see you at least weekly. 10 Information about NICE clinical guideline 38
11 Treatments for rapid-cycling bipolar disorder and hypomania If you have rapid-cycling bipolar disorder, have had a recent episode of hypomania, or your mood has recently been up and down, your doctor should not usually offer you an antidepressant. Your current medication dose for mania may be increased, or you may be offered another drug for mania (such as lamotrigine) in addition to your current medication. For rapid-cycling bipolar disorder, treatment will otherwise be similar to that described on pages 8 10, but your doctor should also: treat your illness as a whole (the wider pattern of ups and downs) rather than one particular episode or symptom encourage you to keep a diary of your moods to help your doctor look at how different treatments have affected your symptoms. What if the treatment I am started on does not help me? In general, if your treatment is not working, your doctor will look at it again and may make changes to it, offer you other treatments, or arrange for you to see a psychiatrist who has more experience of treating bipolar disorder. Very rarely, a treatment called electroconvulsive therapy (ECT) may be offered to you if you have very severe symptoms (including psychosis) or if several other treatments have not improved your symptoms. If you are offered ECT, it should only be after all the disadvantages and advantages of the treatment have been discussed with you. Questions you could ask healthcare professionals if you do not feel better after treatment I had expected to feel differently from how I m feeling now. Can we discuss how I m getting on? I feel worse, not better. Can we discuss my treatment? Do we need to look at different types of treatment? Information about NICE clinical guideline 38 11
12 What happens if I behave in a disturbed or violent way when having an episode? If you show signs of behaving violently or in a way that might seriously disturb others, your healthcare professional should start by looking at your lifestyle and surroundings and anything else that might help to reduce your stress. Your healthcare professional should make sure that you are in a place where you feel safe and supported, check on your physical health, and may help you to do activities that help calm you down. If a treatment described in this booklet appears suitable for you, but it is not available, you should talk to your local Patient Advice and Liaison Service (PALS) in the first instance. If they are not able to help you, they should refer you to your local Independent Complaints Advocacy Service. If you are given medication to control your behaviour it should usually be one such as lorazepam or an antipsychotic, or a combination of an antipsychotic and a benzodiazepine, in tablet form. If this does not calm you down, then you may be given an injection of olanzapine, lorazepam or haloperidol. Can I expect treatment in the long-term? Your doctor may offer you long-term treatment (to help reduce the risk of symptoms coming back) in the following circumstances: after a severe manic episode if you have had two or more episodes of mania, depression or both if you have bipolar II disorder and your daily life is severely affected by your symptoms, you have had thoughts of suicide, or you have frequent episodes if you have had repeated periods of depression, or you have had depression for a long time. What are long-term treatments for bipolar disorder? Long-term treatment consists mainly of the same types of medication as are used for manic episodes (usually lithium, olanzapine or valproate). If these do not help you (either on their own or in combination), then your doctor may offer you: an appointment with a psychiatrist who has more experience of bipolar disorder lamotrigine (especially if you have bipolar II disorder) carbamazepine. If your symptoms are relatively stable but have not gone away completely, you may be offered psychological treatment in addition to medication. This should include education about the illness, and advice on coping with it. 12 Information about NICE clinical guideline 38
13 If you live with your family or see them regularly, your doctor may offer you a psychological treatment that involves you and your family. When you have recovered from depression, you should normally be advised to stop taking the antidepressants because you could develop mania. But if you have had repeated or long periods of depression, you are not taking medication for mania as a long-term treatment, and you have not recently had a manic episode, your healthcare professional should consider whether any of the following treatments would help you: long-term treatment with a low dose of an antidepressant (an SSRI) together with medication for mania cognitive behavioural therapy (also known as CBT) in addition to medication for mania as a long-term treatment quetiapine, or lamotrigine. If your depression has lasted a long time you may be offered a befriending service, where a trained volunteer visits you once a week for a few months, to talk with you and offer practical advice and support. If you have problems with alcohol or drugs, you may be offered psychological treatment such as education about alcohol and drugs and encouraged to develop a plan for changing your behaviour. If you have an anxiety disorder, you may be offered psychological treatment or an antipsychotic. How long is long-term treatment for bipolar disorder? Long-term treatment varies from person to person, but it usually continues for at least 2 years after an episode and sometimes up to 5 years. During this time your doctor should see you regularly. If you wish to stop taking medication within this time, you should discuss this with your doctor. If, after discussing the advantages and disadvantages with your doctor, you decide not to take medication long-term, you should still be offered regular appointments. Information about NICE clinical guideline 38 13
14 What should I know about long-term treatment with medication? What you need to know Antipsychotics You may gain weight while taking the drug. If you are diabetic your condition could get worse. You should normally be given tablets, not injections. If you are offered quetiapine, you should start on a low dose and gradually increase it. Lithium Do not miss doses or stop taking the drug suddenly. See a doctor if you have diarrhoea or are vomiting. Drink water regularly, particularly after sweating and especially if you are over 65, have a chest infection or pneumonia or are immobile for long periods. You should not usually take non-steroidal anti-inflammatory drugs (such as ibuprofen), but if your doctor prescribes them you will need regular checks. Tests You should have: your weight and height measured when you start and at least every 3 months for the first year blood tests for glucose and cholesterol when you start and after 3 months (and possibly more often) a blood test for the hormone prolactin when you start and then occasionally (if you are taking risperidone). You may need: an electrocardiogram (ECG) when you start if you have, or are at risk of, heart disease. You should have: blood tests to check thyroid and kidneys when you start, then at least every 6 months your weight and height measured when you start, then regularly if you put on a lot of weight a test for the amount of lithium in your blood 1 week after you start, 1 week after every dose change, and every 3 months. You may need: an ECG when you start if you have, or are at risk of, heart disease a blood count when you start and then once during the first 6 months. You should normally take lithium for at least 6 months before trying a different drug. 14 Information about NICE clinical guideline 38
15 What you need to know Valproate Not normally offered to women at an age where they could get pregnant. If there is no alternative, your doctor should make sure you are using a very reliable form of contraception because there may be risks to an unborn child. Tests You should have: a blood test to check your liver and a blood count when you start and 6 months later your weight and height measured when you start, then regularly if you put on a lot of weight. Your doctor should tell you how to spot signs of blood or liver problems and what to do if these develop. Your doctor should be careful if you are also taking a drug for epilepsy, and see you more often if you are over 65. Lamotrigine Your doctor should start You will have a yearly health check (see page 7), you on a low dose and but will not need any other tests. increase it gradually, especially if you are also taking valproate. Seek medical help urgently if you develop a rash. If you are taking the contraceptive pill, your doctor should talk to you about changing to a different contraceptive. Carbamazepine You should start taking carbamazepine only after an expert in bipolar disorder has been consulted. Your doctor should start you on a low dose and increase it gradually. Carbamazepine can cause problems if you are taking other drugs (including the contraceptive pill), so you will need careful checks. Tests you will need: blood tests to check your liver when you start and after 6 months a blood count when you start and after 6 months your weight and height measured, when you start and then regularly if you put on a lot of weight blood tests to check your kidneys and the amount of drug in your blood when you start and every 6 months. Information about NICE clinical guideline 38 15
16 When taken as long-term treatment, some drugs for mania (particularly olanzapine) can cause weight gain. If you put on weight during treatment, your doctor should look closely at your medication and may offer extra support, advice on diet or exercise, or an appointment with a dietitian. If you are advised to stop taking medication If you are advised to stop taking medication, the dose should usually be reduced gradually over at least 4 weeks, and up to 3 months if you are taking an antipsychotic or lithium. If for any reason you stop taking lithium suddenly, your doctor should talk to you about taking an antipsychotic or valproate instead. Your doctor should see you regularly. Long-term treatment of rapid-cycling bipolar disorder If you have rapid-cycling bipolar disorder, your doctor may first offer you a combination of lithium and valproate. If this does not suit you or does not help, you may be offered lithium on its own, or lithium or valproate together with lamotrigine. You should not usually be offered an antidepressant unless it has been advised by an expert in bipolar disorder. Your doctor should check your thyroid every 6 months if you have thyroid problems. 16 Information about NICE clinical guideline 38
17 Questions you could ask about medication If you are offered medication, you might want to know more about it, so you could ask one or more of these questions. How will medication help me? What are the advantages and disadvantages of the different medications available? How long will it take before I start to feel better? Does it matter if I miss a dose? How can I be sure that I am taking the correct dose? Can I stop taking the medication if I feel better? Is there a leaflet or other written material about the medication that I can read? How much water should I be drinking if I am taking lithium? You should be informed about the side effects associated with any medication you are taking. If you are unsure, you might consider asking the following questions. Does this medication have any side effects? What should I do if I get any of these side effects? How long do these side effects last? Are there any long-term side effects of taking this medication? What are the alternatives to this medication? Information about NICE clinical guideline 38 17
18 How do I stay healthy? Your healthcare professional should give you written information about staying healthy, and ways to cope with bipolar disorder. This should include the importance of sleeping well and having a regular lifestyle. They should also discuss giving you extra help and support at particularly difficult periods in your life. This may include checking on your mood and general health and encouraging you to talk through difficulties with family and friends. You and your healthcare professional should develop a plan that looks at things that can start your symptoms off and make them worse, and what to do if this happens. Will I be offered any further support? There are different kinds of support that may be offered to you depending on your circumstances, including: telephone support a community mental health team assertive community treatment a crisis resolution and home treatment team an early intervention service support in getting a job or going back to work (this may involve training or attending a workshop, or helping you to go straight back to work) or support in starting or re-starting a programme of education or other similar activity specialist clinics (such as a lithium clinic). 18 Information about NICE clinical guideline 38
19 Special issues for women who are pregnant or planning a pregnancy If you are a woman who could get pregnant, you should be given information about contraception and the possible risks both to you and to an unborn child if you get pregnant. Taking medication in pregnancy does entail risks for the baby. But if you stop treatment there is also a risk that you could become seriously unwell again. So the decision about taking medication can be very difficult and will depend partly on the drug you are taking, and how likely you are to become unwell if you stop taking it. Usually, doctors should advise women taking an antipsychotic to carry on taking the drug throughout pregnancy if they are relatively well but likely to become ill again without the medication. If you are taking lithium, you may be advised to stop gradually, or change to an antipsychotic. If you continue to take lithium during your pregnancy, the amount of lithium in your blood should be checked every 4 weeks at first, then every week from the 36th week and within 24 hours of giving birth. You should be advised to drink enough water while taking lithium. The following medications should not usually be offered during pregnancy: valproate carbamazepine benzodiazepines as long-term treatment lamotrigine. During pregnancy your doctor should see you more frequently and should develop with you a plan of your treatment and care for the pregnancy, and during and after birth, which should include information about any medication you are taking. This plan should be shown to your obstetrician, midwife, GP and health visitor. Information about NICE clinical guideline 38 19
20 Planning a pregnancy If you are planning a pregnancy you are encouraged to discuss this with your doctor. If he or she thinks you may have a manic episode during your pregnancy, you may be offered an antipsychotic because it is associated with less risk to the baby than other drugs. However, some antipsychotics can cause difficulties in becoming pregnant. If you have increased levels of the hormone prolactin, you may be offered a different drug. If you are taking valproate, lithium, carbamazepine, or lamotrigine, your doctor should normally advise you to stop taking it. However, if you have had manic episodes that have made previous pregnancies very difficult, and lithium has helped you in the past, your doctor might advise you to carry on taking it while you are trying to conceive and throughout pregnancy. But your doctor should fully discuss with you the risks of doing so. If you are depressed and not on long-term medication, your doctor may offer you cognitive behavioural therapy rather than an antidepressant. If you are offered an antidepressant, it should be an SSRI (not paroxetine because there may be a risk to the unborn child). Unplanned pregnancies If you have an unplanned pregnancy, your doctor should confirm your pregnancy as soon as possible. They should arrange counselling if you are unsure about continuing with the pregnancy and should offer to screen your unborn child for problems. If you decide to continue with the pregnancy and you are taking valproate, carbamazepine or lamotrigine, your doctor should usually advise you to stop taking it. If you are taking lithium and your pregnancy is confirmed in the first trimester, you should be advised to stop taking the lithium gradually over 4 weeks if you are feeling reasonably well. But even if you do this there might still be a risk to your unborn child. You may be offered another medication such as an antipsychotic. If you continue to take lithium during your pregnancy, the amount in your blood should be checked every 4 weeks at first, then every week from the 36th week and within 24 hours of giving birth. You should drink plenty of water while taking lithium. Your newborn baby should be thoroughly assessed. 20 Information about NICE clinical guideline 38
21 Manic episodes during pregnancy If you are not already taking medication for mania, you may be offered a low dose of an antipsychotic. If you are already taking medication, your doctor should check how much you are taking or may offer you an antipsychotic if you are not already taking one. If your symptoms do not improve, and your episode is very severe, you may be offered electroconvulsive therapy or lithium. You will be offered valproate only if there is no helpful alternative. You should have the chance to discuss the risks and be given the lowest possible dose. You may also be offered another drug for mania (not carbamazepine). Depression during pregnancy If you have mild depression, you should be offered a self-help treatment such as guided self-help or computerised cognitive behavioural therapy, other psychological treatments, or antidepressant medication. If you have moderate depression you may be offered cognitive behavioural therapy. If your depression is severe you may be offered medication together with a psychological treatment. Medication could be quetiapine on its own, or an SSRI (not paroxetine) together with medication for mania. Your doctor should see you often, and if you develop mania you should be advised to stop the antidepressant. If you are offered an antidepressant during pregnancy or immediately after birth, your doctor should warn you that it may cause short-term problems for your newborn child. What should happen during and after giving birth? If you are taking lithium, you should be advised to have your baby in hospital. If there is a risk you could have a manic episode soon after the baby is born, you may be offered an antipsychotic as well. If you are not taking medication but there is a risk that you could have a manic episode or develop depression, your doctor should start or restart your medication as soon as possible. If you develop severe mania or psychosis during labour, you may be given an injection of an antipsychotic. You should be advised not to breastfeed if you are taking lithium, benzodiazepines or lamotrigine. If you wish to breastfeed, you should be offered other medication for mania, such as an antipsychotic (but not clozapine), and an SSRI for depression if needed (but not fluoxetine or citalopram). If you have taken medication during pregnancy, your doctor should see your baby regularly in the first few weeks after birth to check for any problems. These might include muscle weakness, constant crying, shivering, shakes, restlessness, stiffness, feeding and sleeping problems and, very rarely, seizures. Information about NICE clinical guideline 38 21
22 Special issues for children and young people with bipolar disorder Can I choose what treatments I get? You will be able to talk about the treatments you get with your doctor. If you are over 16 you can give your own agreement; if you are under 16 but you fully understand the information you may also be able to give your own agreement. If there are treatments that you do not want, tell your doctor. If you are too young or you have not fully understood the information about treatments, your parents or carers may also need to agree to treatment. Sometimes parents and doctors may go against your decision if they think it is best for you. Your doctor should usually tell your parents and carers about treatments that have been offered to you. This is because if you are not able to agree to treatment yourself, your parents need to have the right information to be able to make a decision. It is usually helpful for young people if their parents and other members of the family are involved in their treatment, but this will depend on how things are at home. But your doctor should offer you a chance to have appointments on your own, without your parents or carers. What treatments can help me? Treatments for children and young people are similar to those for adults but with some differences. When planning your treatment doctors should ask you about: anything at home or school that makes you anxious or unhappy whether you have any other problems or illnesses, such as attention deficit hyperactivity disorder (ADHD) or anxiety how far bipolar disorder affects your education and how you get on with your friends your behaviour when you have an episode. 22 Information about NICE clinical guideline 38
23 Treatments for mania If you have mania your treatment should be similar to treatment for adults and will involve taking medicine. Your doctor should measure your height and weight when you first start treatment and regularly afterwards and you should have some blood tests. If you have mania you may first be offered a medicine called an antipsychotic. If this does not help you, you may be offered another medicine as well (one called lithium if you are a girl, and lithium or valproate if you are a boy). Girls should not be offered valproate because there are risks both to them and to their baby if they get pregnant. Treatments for depression If you have mild depression, your doctor should see you once a week and should help if you have any problems at home or school. If you have more severe depression, your treatment should be similar to treatment for adults and may involve psychological treatment and taking medicine (usually the same as for mania, see above). Your doctor should see you once a week. If this does not help you after about 4 weeks, you may be offered a medicine for depression called fluoxetine. If this does not help you, you may be offered another medicine (sertraline or citalopram). If you are an older teenager and you have moderate or severe depression, you may be offered the same treatment as adults (see pages 9 10). Long-term treatment After you have had treatment for mania or depression you should feel better again. It is important that your doctor continues to see you and offer you treatment to try to stop the feelings and moods coming back. This treatment will be similar to long-term treatment for adults (see pages 12 16) and will involve medicine (usually an antipsychotic) and psychological treatment. Will I need to stay in hospital? If you need special care that you cannot get anywhere else, or your doctor is concerned that you may harm yourself, they may suggest a stay in a hospital that looks after young people with bipolar disorder. You might be able to have the treatment in hospital during the day and go home at night, or to have the extra treatment or support in your home. If your behaviour is very disturbed, treatment will be similar to treatment for adults (see page 12) and will involve medicine to help calm you down. Information about NICE clinical guideline 38 23
24 Help for families and carers of people with bipolar disorder If someone in your family has bipolar disorder, healthcare professionals should give you information about bipolar disorder and treatments that can help and they should be available in times of crisis. Doctors should also consider your needs, especially if you are under 18, and if you have your own problems and difficulties. You should be offered a regular assessment of your circumstances, needs and physical and mental health, and you may be offered treatment and support. You should also be told about any support groups for families and carers. Questions for families and carers to ask healthcare professionals If you are unsure about how you can help someone with bipolar disorder, you could ask some of these questions. What can I/we do to help someone with bipolar disorder? Is there anywhere I/we can get extra support? I/we feel stressed and are not sleeping well. Can you give me advice on how I/we can cope with this? Are there any ways I/we can reduce stress while trying to live a relatively normal life? How can I/we help our children cope with living with someone with bipolar disorder? Can our child s school get help and advice on dealing with the effects of their bipolar disorder? 24 Information about NICE clinical guideline 38
25 More information about bipolar disorder The organisations below can provide more information and support for people with bipolar disorder. Please note that NICE is not responsible for the quality or accuracy of any information or advice provided by these organisations. Depression Alliance, , MDF The BiPolar Organisation, , Mind, (MindinfoLine, 9.15am 5.15pm), Rethink, , SANE, (SANELINE, 1pm 11pm), NHS Direct online ( may also be a good starting point for finding out more. Your local Patient Advice and Liaison Service (PALS) may also be able to give you further information and support. Information about NICE clinical guideline 38 25
26 Glossary Antidepressant: medicines that help symptoms of depression. Anxiety: feelings of worry or fear that can be difficult to control. Assertive community treatment: a type of care given outside hospital, for people who have very severe symptoms or are homeless or living in seriously inadequate conditions. Assessment: a meeting with a healthcare professional, who will ask a person questions, and arrange medical tests if needed, so that he or she can work out what treatment and care would suit the person best. Attention deficit hyperactivity disorder (ADHD): a problem usually affecting children and young people. People with ADHD are overactive and have difficulty concentrating. Bipolar II disorder: a type of bipolar disorder where people have periods of hypomania and periods of depression. Blood count: a common blood test to check the cells in the blood. Cognitive behavioural therapy (CBT): a psychological treatment in which people work with a therapist to look at how their problems, feelings and behaviour all fit together. CBT can help people to challenge negative thoughts and change behaviour that may have developed since they became ill. Community mental health team: a group of professionals that includes nurses who may visit people in their own homes, psychiatrists, psychologists, occupational therapists and support workers. Computerised cognitive behavioural therapy: a psychological treatment which is delivered by a computer program, with support from a healthcare professional. See cognitive behavioural therapy. Crisis resolution and home treatment team: a team of healthcare professionals that can help you cope with a crisis in your own home, so that you do not need to go to hospital. This team may also help if you are leaving hospital. Depression: a mental disorder that causes a loss of pleasure in things that were once enjoyable, withdrawal from family and friends, negative and self-critical thoughts, and other symptoms, such as feeling tearful, irritable or tired, poor appetite, and sleep problems. Early intervention service: a team of healthcare professionals who can help people who have symptoms of psychosis. As well as providing treatments, the service can help people recognise early warning signs of an episode or crisis. The service is usually for people under 35 who are experiencing their first or second episode. 26 Information about NICE clinical guideline 38
27 Electrocardiogram (ECG): a test that can measure the rate and regularity of the heartbeats and detect heart problems. Electroconvulsive therapy (ECT): a procedure sometimes used to treat severe mental health problems. ECT is always given in hospital and it involves passing a small electric current through the brain. Guided self-help: a kind of psychological treatment in which the patient works through books, often called self-help manuals, with the support of a healthcare professional. Hypomania: a less severe type of mania. Mania or manic episode: symptoms of bipolar disorder including elation (extreme happiness or feeling high ), irritability and over-confidence. A person having a manic episode may not need as much sleep as usual, and may take unnecessary risks, have racing thoughts, fidget, gesture, or talk a lot, and have poor concentration. If the episode is severe they might behave in an inappropriate way and upset others. Mental Health Act: a law that allows a person with a mental disorder to be treated against their will, or without their agreement, if they are judged to be at serious risk to themselves or others. This is sometimes called being sectioned. Psychological treatment: a broad term used to describe meeting with a therapist to talk about feelings and moods. This might be a simple treatment such as getting advice on how to cope with symptoms and other problems; or it might be a longer treatment such as one called cognitive behavioural therapy. Psychosis: a severe mental disorder in which a person has hallucinations (seeing things that are not really there) and delusions (believing things that are not real). Rapid-cycling bipolar disorder: a form of bipolar disorder in which a person has more than four episodes a year. Selective serotonin reuptake inhibitor (SSRI): a type of antidepressant medication (such as fluoxetine). Telephone support: help from a healthcare professional over the telephone, for example advice about taking medication. Information about NICE clinical guideline 38 27
28 About NICE NICE produces advice (guidance) for the NHS about preventing, diagnosing and treating different medical conditions. The guidance is written by independent experts including healthcare professionals and people representing patients and carers. They consider the best available evidence on the condition and treatments, the views of patients and carers and the experiences of doctors, nurses and other healthcare professionals working in the field. Staff working in the NHS are expected to follow this guidance. To find out more about NICE, its work and how it reaches decisions, see This booklet and other versions of this guideline aimed at healthcare professionals are available at You can order printed copies of this booklet from the NHS Response Line (phone and quote reference N1077). National Institute for Health and Clinical Excellence MidCity Place, 71 High Holborn, London, WC1V 6NA, ISBN N k 1P Jul 06 National Institute for Health and Clinical Excellence, July All rights reserved. This material may be freely reproduced for educational and not-for-profit purposes. No reproduction by or for commercial organisations, or for commercial purposes, is allowed without the express written permission of the Institute.
Borderline personality disorder
 Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Borderline personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Antisocial personality disorder
 Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Antisocial personality disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Symptoms of mania can include: 3
 Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Treatments for drug misuse
 Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
and body dysmorphic disorder (BDD) in adults, children and young people Issue date: November 2005
 Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
This factsheet covers:
 Depression This factsheet might be useful to you if you have depression or if you think you might have depression. It gives information on the symptoms and causes of depression, as well as the treatments
Depression This factsheet might be useful to you if you have depression or if you think you might have depression. It gives information on the symptoms and causes of depression, as well as the treatments
A Guide to Bipolar Disorder
 A Guide to Bipolar Disorder Bipolar disorder is a serious, chronic (long-term) condition where you have periods of depression ( lows ) and periods of mania or hypomania ( highs ). Treatment with mood
A Guide to Bipolar Disorder Bipolar disorder is a serious, chronic (long-term) condition where you have periods of depression ( lows ) and periods of mania or hypomania ( highs ). Treatment with mood
Drug treatments for neuropathic pain
 Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Understanding NICE guidance Information for people who use NHS services Drug treatments for neuropathic pain NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children
 Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Post-traumatic stress disorder (PTSD): the treatment of PTSD in adults and children Understanding NICE guidance information for people with PTSD, their advocates and carers, and the public March 2005 Information
Understanding Bipolar Disorder
 Barnet, Enfield and Haringey Mental Health NHS Trust Understanding Bipolar Disorder Information for patients and carers Page What is bipolar disorder? Bipolar disorder is a serious mental illness involving
Barnet, Enfield and Haringey Mental Health NHS Trust Understanding Bipolar Disorder Information for patients and carers Page What is bipolar disorder? Bipolar disorder is a serious mental illness involving
Postnatal depression is an illness. It is not a sign that you don't love your baby or can't look after your baby properly.
 Patient information from the BMJ Group Postnatal depression Postnatal depression is an illness that women can get after having a baby. If you have it, you may feel sad and anxious, and find it hard to
Patient information from the BMJ Group Postnatal depression Postnatal depression is an illness that women can get after having a baby. If you have it, you may feel sad and anxious, and find it hard to
making sense of psychiatric medication making sense psychiatric medication
 making sense of psychiatric medication making sense psychiatric medication Making sense of psychiatric medication This booklet is for anyone who wants to know more about psychiatric medication. It explains
making sense of psychiatric medication making sense psychiatric medication Making sense of psychiatric medication This booklet is for anyone who wants to know more about psychiatric medication. It explains
Understanding mania and hypomania
 Understanding mania and hypomania 1 Contents What are mania and hypomania? 3 How are mania and hypomania diagnosed? 4 What causes mania and hypomania? 5 What treatments are available? 5 How can I help
Understanding mania and hypomania 1 Contents What are mania and hypomania? 3 How are mania and hypomania diagnosed? 4 What causes mania and hypomania? 5 What treatments are available? 5 How can I help
Rheumatoid arthritis inadults
 Understanding NICE guidance Information for people who use NHS services Rheumatoid arthritis inadults NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Understanding NICE guidance Information for people who use NHS services Rheumatoid arthritis inadults NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Bipolar disorder, Pregnancy and Childbirth
 Bipolar disorder, Pregnancy and Childbirth Having a baby is a major event in the life of any woman. For those with bipolar disorder (manic depression) there are a number of additional issues. Women with
Bipolar disorder, Pregnancy and Childbirth Having a baby is a major event in the life of any woman. For those with bipolar disorder (manic depression) there are a number of additional issues. Women with
Lithium Therapy. Important information for patients COLLEGE CENTRE FOR QUALITY IMPROVEMENT
 Lithium Therapy Important information for patients COLLEGE CENTRE FOR QUALITY IMPROVEMENT National Patient Safety Agency National Patient Safety Agency Your information Your name: Address: Postcode: Home
Lithium Therapy Important information for patients COLLEGE CENTRE FOR QUALITY IMPROVEMENT National Patient Safety Agency National Patient Safety Agency Your information Your name: Address: Postcode: Home
MEDGUIDE SECTION. What is the most important information I should know about SEROQUEL? SEROQUEL may cause serious side effects, including:
 MEDGUIDE SECTION Medication Guide SEROQUEL (SER-oh-kwell) (quetiapine fumarate) Tablets Read this Medication Guide before you start taking SEROQUEL and each time you get a refill. There may be new information.
MEDGUIDE SECTION Medication Guide SEROQUEL (SER-oh-kwell) (quetiapine fumarate) Tablets Read this Medication Guide before you start taking SEROQUEL and each time you get a refill. There may be new information.
Understanding. Depression. The Road to Feeling Better Helping Yourself. Your Treatment Options A Note for Family Members
 TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
Depression in children and adolescents
 Patient information from the BMJ Group Depression in children and adolescents Depression is an illness that affects people of all ages, including children and teenagers. It can stop a child or teenager
Patient information from the BMJ Group Depression in children and adolescents Depression is an illness that affects people of all ages, including children and teenagers. It can stop a child or teenager
Identifying and treating long-term kidney problems (chronic kidney disease)
 Understanding NICE guidance Information for people who use NHS services Identifying and treating long-term kidney problems (chronic kidney disease) NICE clinical guidelines advise the NHS on caring for
Understanding NICE guidance Information for people who use NHS services Identifying and treating long-term kidney problems (chronic kidney disease) NICE clinical guidelines advise the NHS on caring for
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
Treating harmful drinking and alcohol dependence
 Understanding NICE guidance Information for people who use NHS services Treating harmful drinking and alcohol dependence NICE clinical guidelines advise the NHS on caring for people with specific conditions
Understanding NICE guidance Information for people who use NHS services Treating harmful drinking and alcohol dependence NICE clinical guidelines advise the NHS on caring for people with specific conditions
MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families
 MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lee S. Cohen, MD, and Lori L. Altshuler, MD www.womensmentalhealth.org
MAJOR DEPRESSION DURING CONCEPTION AND PREGNANCY: A Guide for Patients and Families David A. Kahn, MD, Margaret L. Moline, PhD, Ruth W. Ross, MA, Lee S. Cohen, MD, and Lori L. Altshuler, MD www.womensmentalhealth.org
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression
 Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease
 Understanding NICE guidance Information for people who use NHS services Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease NICE technology appraisal guidance advises on when and
Understanding NICE guidance Information for people who use NHS services Donepezil, galantamine, rivastigmine and memantine for Alzheimer s disease NICE technology appraisal guidance advises on when and
Mid Essex. Specialist Psychosis Service
 Mid Essex Specialist Psychosis Service What is psychosis? Why have you been referred to us? Psychosis is general term used to describe a number of symptoms. Some of the symptoms of psychosis include: False
Mid Essex Specialist Psychosis Service What is psychosis? Why have you been referred to us? Psychosis is general term used to describe a number of symptoms. Some of the symptoms of psychosis include: False
Treatment for people who are overweight or obese
 Understanding NICE guidance Information for people who use NHS services Treatment for people who are overweight or obese NICE advises the NHS on caring for people with specific conditions or diseases.
Understanding NICE guidance Information for people who use NHS services Treatment for people who are overweight or obese NICE advises the NHS on caring for people with specific conditions or diseases.
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS
 BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
Depression Overview. Symptoms
 1 of 6 6/3/2014 10:15 AM Return to Web version Depression Overview What is depression? When doctors talk about depression, they mean the medical illness called major depression. Someone who has major depression
1 of 6 6/3/2014 10:15 AM Return to Web version Depression Overview What is depression? When doctors talk about depression, they mean the medical illness called major depression. Someone who has major depression
Dealing with depression
 Dealing with depression 1 Dealing with depression Every year, one person in ten will suffer from some form of depression. That s about 10% of the population. Depression is different from feeling down or
Dealing with depression 1 Dealing with depression Every year, one person in ten will suffer from some form of depression. That s about 10% of the population. Depression is different from feeling down or
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Care Programme Approach (CPA)
 Care Programme Approach (CPA) The Care Programme Approach (CPA) is the system that is used to organise many people s care from 'secondary mental health services'. This factsheet explains what you should
Care Programme Approach (CPA) The Care Programme Approach (CPA) is the system that is used to organise many people s care from 'secondary mental health services'. This factsheet explains what you should
Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders
 Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders Understanding NICE guidance: a guide for people with eating disorders, their advocates and carers, and the public January
Eating disorders: anorexia nervosa, bulimia nervosa and related eating disorders Understanding NICE guidance: a guide for people with eating disorders, their advocates and carers, and the public January
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
1. What are anti-epileptic drugs? Anti-epileptic drugs (AEDs) are prescribed to control seizures. They do not cure epilepsy.
 14 FREQUENTLY ASKED QUESTIONS ON ANTI- EPILEPTIC DRUGS 1. What are anti-epileptic drugs? Anti-epileptic drugs (AEDs) are prescribed to control seizures. They do not cure epilepsy. 2. When should treatment
14 FREQUENTLY ASKED QUESTIONS ON ANTI- EPILEPTIC DRUGS 1. What are anti-epileptic drugs? Anti-epileptic drugs (AEDs) are prescribed to control seizures. They do not cure epilepsy. 2. When should treatment
Asenapine (Saphris) for bipolar I disorder
 Asenapine (Saphris) for bipolar I disorder This Medicine Update is for people with bipolar I disorder who are taking, or thinking about taking, asenapine. Summary Asenapine is an antipsychotic medicine.
Asenapine (Saphris) for bipolar I disorder This Medicine Update is for people with bipolar I disorder who are taking, or thinking about taking, asenapine. Summary Asenapine is an antipsychotic medicine.
Treatments for Depression
 Treatments for Depression This leaflet contains information about depression and how it can be treated Children and Families Community Services Mental Health Secure Services Specialist Services Adult Mental
Treatments for Depression This leaflet contains information about depression and how it can be treated Children and Families Community Services Mental Health Secure Services Specialist Services Adult Mental
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets
![MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets MEDICATION GUIDE. TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets](/thumbs/40/21035524.jpg) MEDICATION GUIDE TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets Read this Medication Guide before you start taking TRINTELLIX and each time you get a refill. There may be new information. This information
MEDICATION GUIDE TRINTELLIX [trin -tel-ix] (vortioxetine) Tablets Read this Medication Guide before you start taking TRINTELLIX and each time you get a refill. There may be new information. This information
Postnatal Depression. A guide for mothers, family and friends
 Postnatal Depression A guide for mothers, family and friends What is it? What is it? After giving birth, most mothers experience some degree of mood swings. There are three main kinds of postnatal mood
Postnatal Depression A guide for mothers, family and friends What is it? What is it? After giving birth, most mothers experience some degree of mood swings. There are three main kinds of postnatal mood
Care Programme Approach (CPA)
 Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
Care Programme Approach (CPA) The Care Programme Approach (CPA) is used to plan many people s mental health care. This factsheet explains what it is, when you should get and when it might stop. The Care
Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders
 Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders A guide for people with eating disorders, their advocates and carers,
Eating disorders: core interventions in the treatment and management of anorexia nervosa, bulimia nervosa, and related eating disorders A guide for people with eating disorders, their advocates and carers,
Asthma, anxiety & depression
 Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets
 MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets Read this Medication Guide carefully before you start using WELLBUTRIN and each time you get a refill. There may be new information.
MEDICATION GUIDE WELLBUTRIN (WELL byu-trin) (bupropion hydrochloride) Tablets Read this Medication Guide carefully before you start using WELLBUTRIN and each time you get a refill. There may be new information.
Post-traumatic stress disorder overview
 Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Alcohol. Problems with drinking alcohol
 Alcohol Alcoholism is a word which many people use to mean alcohol dependence (alcohol addiction). Some people are problem drinkers without being dependent on alcohol. If you are alcohol- dependent then
Alcohol Alcoholism is a word which many people use to mean alcohol dependence (alcohol addiction). Some people are problem drinkers without being dependent on alcohol. If you are alcohol- dependent then
Bipolar Disorder. When people with bipolar disorder feel very happy and "up," they are also much more active than usual. This is called mania.
 Bipolar Disorder Introduction Bipolar disorder is a serious mental disorder. People who have bipolar disorder feel very happy and energized some days, and very sad and depressed on other days. Abnormal
Bipolar Disorder Introduction Bipolar disorder is a serious mental disorder. People who have bipolar disorder feel very happy and energized some days, and very sad and depressed on other days. Abnormal
Medication Guide LATUDA (luh-too-duh) (lurasidone hydrochloride) Tablets
 Medication Guide LATUDA (luh-too-duh) (lurasidone hydrochloride) Tablets What is the most important information I should know about LATUDA? LATUDA may cause serious side effects, including: 1. Increased
Medication Guide LATUDA (luh-too-duh) (lurasidone hydrochloride) Tablets What is the most important information I should know about LATUDA? LATUDA may cause serious side effects, including: 1. Increased
Medications for bipolar disorder
 Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
The sooner a person with depression seeks support, the sooner they can recover.
 Depression Summary Depression is a constant feeling of dejection and loss, which stops you doing your normal activities. Different types of depression exist, with symptoms ranging from relatively minor
Depression Summary Depression is a constant feeling of dejection and loss, which stops you doing your normal activities. Different types of depression exist, with symptoms ranging from relatively minor
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
This information explains the advice about type 2 diabetes in adults that is set out in NICE guideline NG28.
 Information for the public Published: 2 December 2015 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care
Information for the public Published: 2 December 2015 nice.org.uk About this information NICE guidelines provide advice on the care and support that should be offered to people who use health and care
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Leukapheresis for inflammatory bowel disease
 Issue date: June 2005 Leukapheresis for inflammatory bowel disease Understanding NICE guidance information for people considering the procedure, and for the public Information about NICE Interventional
Issue date: June 2005 Leukapheresis for inflammatory bowel disease Understanding NICE guidance information for people considering the procedure, and for the public Information about NICE Interventional
Deciding whether to become a parent
 Deciding whether to become a parent This information is an extract from the booklet, Relationships, sex and fertility for young people affected by cancer. You may find the full booklet helpful. We can
Deciding whether to become a parent This information is an extract from the booklet, Relationships, sex and fertility for young people affected by cancer. You may find the full booklet helpful. We can
Methadone treatment Information for service users Page
 South London and Maudsley NHS Foundation Trust Methadone treatment Information for service users Page What can happen if I stop using heroin? If you are addicted to or dependent on heroin, you develop
South London and Maudsley NHS Foundation Trust Methadone treatment Information for service users Page What can happen if I stop using heroin? If you are addicted to or dependent on heroin, you develop
Medication Guide KLONOPIN (KLON-oh-pin) (clonazepam) Tablets
 Medication Guide KLONOPIN (KLON-oh-pin) (clonazepam) Tablets Read this Medication Guide before you start taking KLONOPIN and each time you get a refill. There may be new information. This information does
Medication Guide KLONOPIN (KLON-oh-pin) (clonazepam) Tablets Read this Medication Guide before you start taking KLONOPIN and each time you get a refill. There may be new information. This information does
Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic hepatitis B. Issue date: February 2006
 Issue date: February 2006 Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic Understanding NICE guidance information for people with chronic, their families and carers, and the public
Issue date: February 2006 Adefovir dipivoxil and peginterferon alfa-2a for the treatment of chronic Understanding NICE guidance information for people with chronic, their families and carers, and the public
Alcohol and Dependence
 The facts about... Alcohol and Dependence Five key things you need to know A glass of wine with dinner, a beer after work, a cocktail in the sunshine on holiday. Alcohol makes an appearance in so many
The facts about... Alcohol and Dependence Five key things you need to know A glass of wine with dinner, a beer after work, a cocktail in the sunshine on holiday. Alcohol makes an appearance in so many
Bipolar Disorder. in Children and Teens. Does your child go through intense mood changes? Does your child have
 Bipolar Disorder in Children and Teens Does your child go through intense mood changes? Does your child have extreme behavior changes too? Does your child get too excited or silly sometimes? Do you notice
Bipolar Disorder in Children and Teens Does your child go through intense mood changes? Does your child have extreme behavior changes too? Does your child get too excited or silly sometimes? Do you notice
BIPOLAR DISORDER IN PRIMARY CARE
 E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
Cognitive and behavioural therapy (CBT) for people with depression and anxiety What skills can service users expect their therapists to have?
 Cognitive and behavioural therapy (CBT) for people with depression and anxiety What skills can service users expect their therapists to have? Cognitive and behavioural therapy (CBT) for people with depression
Cognitive and behavioural therapy (CBT) for people with depression and anxiety What skills can service users expect their therapists to have? Cognitive and behavioural therapy (CBT) for people with depression
Going to a Mental Health Tribunal hearing
 June 2015 Going to a Mental Health Tribunal hearing Includes: information about compulsory treatment and treatment orders information about Mental Health Tribunal hearings worksheets to help you represent
June 2015 Going to a Mental Health Tribunal hearing Includes: information about compulsory treatment and treatment orders information about Mental Health Tribunal hearings worksheets to help you represent
MEDICATION GUIDE Savella (Sa-vel-la) (milnacipran HCl) Tablets
 MEDICATION GUIDE Savella (Sa-vel-la) (milnacipran HCl) Tablets Savella is not used to treat depression, but it acts like medicines that are used to treat depression (antidepressants) and other psychiatric
MEDICATION GUIDE Savella (Sa-vel-la) (milnacipran HCl) Tablets Savella is not used to treat depression, but it acts like medicines that are used to treat depression (antidepressants) and other psychiatric
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
F r e q u e n t l y As k e d Qu e s t i o n s
 Depression Q: What is depression? A: Life is full of ups and downs. But when the down times last for weeks or months at a time or keep you from your regular activities, you may be suffering from depression.
Depression Q: What is depression? A: Life is full of ups and downs. But when the down times last for weeks or months at a time or keep you from your regular activities, you may be suffering from depression.
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
MEDICATION GUIDE. Bupropion Hydrochloride (bue-proe-pee-on HYE-droe-KLOR-ide) Extended-Release Tablets, USP (SR)
 MEDICATION GUIDE Bupropion Hydrochloride (bue-proe-pee-on HYE-droe-KLOR-ide) Extended-Release Tablets, USP (SR) Read this Medication Guide carefully before you start taking bupropion hydrochloride extendedrelease
MEDICATION GUIDE Bupropion Hydrochloride (bue-proe-pee-on HYE-droe-KLOR-ide) Extended-Release Tablets, USP (SR) Read this Medication Guide carefully before you start taking bupropion hydrochloride extendedrelease
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
WHICH talking therapy for depression?
 WHICH talking therapy for depression? A guide to understanding the different psychological therapies you may be offered to treat your depression 1 Contents Introduction 3 Cognitive Behavioural Therapy
WHICH talking therapy for depression? A guide to understanding the different psychological therapies you may be offered to treat your depression 1 Contents Introduction 3 Cognitive Behavioural Therapy
Detention under the Mental Health Act
 Detention under the Mental Health Act This factsheet gives information about detention under the Mental Health Act. This is also known as being sectioned. It explains what the Mental Health Act is, why
Detention under the Mental Health Act This factsheet gives information about detention under the Mental Health Act. This is also known as being sectioned. It explains what the Mental Health Act is, why
Bipolar Disorder UHN. Information for patients and families. Read this booklet to learn:
 Bipolar Disorder UHN Information for patients and families Read this booklet to learn: what bipolar disorder is what causes it the signs or symptoms of bipolar disorder what treatments can help Please
Bipolar Disorder UHN Information for patients and families Read this booklet to learn: what bipolar disorder is what causes it the signs or symptoms of bipolar disorder what treatments can help Please
Bipolar Disorder. Some people with these symptoms have bipolar disorder, a serious mental illness. Read this brochure to find out more.
 Bipolar Disorder Do you go through intense moods? Do you feel very happy and energized some days, and very sad and depressed on other days? Do these moods last for a week or more? Do your mood changes
Bipolar Disorder Do you go through intense moods? Do you feel very happy and energized some days, and very sad and depressed on other days? Do these moods last for a week or more? Do your mood changes
A Carer s Guide to Depression in People with a Learning Disability
 A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
A Carer s Guide to Depression in People with a Learning Disability Fife Clinical Psychology Department Lynebank Hospital Halbeath Road Dunfermline Fife KY11 4UW Tel: 01383 565 210 December 2009 This booklet
Understanding bipolar disorder. understanding. bipolar disorder
 Understanding bipolar disorder understanding bipolar disorder Understanding bipolar disorder This booklet is for anyone experiencing bipolar disorder. It explains what bipolar disorder is, and how you
Understanding bipolar disorder understanding bipolar disorder Understanding bipolar disorder This booklet is for anyone experiencing bipolar disorder. It explains what bipolar disorder is, and how you
More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind.
 What is depression? More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind. 1,2 The difference between clinical depression
What is depression? More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind. 1,2 The difference between clinical depression
Schizophrenia. This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available.
 This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a commonly misunderstood condition,
This factsheet provides a basic description of schizophrenia, its symptoms and the treatments and support options available. What is schizophrenia? Schizophrenia is a commonly misunderstood condition,
Making sense of cognitive behaviour therapy (CBT)
 Making sense of cognitive behaviour therapy (CBT) Making sense of cognitive behaviour therapy What is cognitive behaviour therapy? 4 How does negative thinking start? 6 What type of problems can CBT help
Making sense of cognitive behaviour therapy (CBT) Making sense of cognitive behaviour therapy What is cognitive behaviour therapy? 4 How does negative thinking start? 6 What type of problems can CBT help
Heart information. Cardiac rehabilitation
 Heart information Cardiac rehabilitation Contents 2 What is cardiac rehabilitation? 3 What are the benefits of cardiac rehabilitation? 4 Who should take part in cardiac rehabilitation? 4 When does cardiac
Heart information Cardiac rehabilitation Contents 2 What is cardiac rehabilitation? 3 What are the benefits of cardiac rehabilitation? 4 Who should take part in cardiac rehabilitation? 4 When does cardiac
ADHD: what treatments work?
 Patient information from the BMJ Group ADHD: what treatments work? Caring for a child who has attention deficit hyperactivity disorder (ADHD) can put a strain on you and your family. If your child has
Patient information from the BMJ Group ADHD: what treatments work? Caring for a child who has attention deficit hyperactivity disorder (ADHD) can put a strain on you and your family. If your child has
Caring for depression
 Caring for depression Aetna Health Connections SM Disease Management Program Get information. Get help. Get better. 21.05.300.1 B (6/08) Get back to being you How this guide can help you Having an ongoing
Caring for depression Aetna Health Connections SM Disease Management Program Get information. Get help. Get better. 21.05.300.1 B (6/08) Get back to being you How this guide can help you Having an ongoing
Obstetric Cholestasis (itching liver disorder) Information for parents-to-be
 Oxford University Hospitals NHS Trust Obstetric Cholestasis (itching liver disorder) Information for parents-to-be page 2 You have been given this leaflet because you have been diagnosed with (or are suspected
Oxford University Hospitals NHS Trust Obstetric Cholestasis (itching liver disorder) Information for parents-to-be page 2 You have been given this leaflet because you have been diagnosed with (or are suspected
Rethink 2008 www.rethink.org. the mental health act. essential information for parents and carers
 Rethink 2008 www.rethink.org the mental health act essential information for parents and carers 1 About Rethink Rethink, the leading national mental health membership charity, works to help everyone affected
Rethink 2008 www.rethink.org the mental health act essential information for parents and carers 1 About Rethink Rethink, the leading national mental health membership charity, works to help everyone affected
Understanding bipolar disorder. understanding. bipolar disorder. understanding bipolar disorder 1
 Understanding bipolar disorder understanding bipolar disorder understanding bipolar disorder 1 Understanding bipolar disorder This booklet describes the symptoms of bipolar disorder and what treatments
Understanding bipolar disorder understanding bipolar disorder understanding bipolar disorder 1 Understanding bipolar disorder This booklet describes the symptoms of bipolar disorder and what treatments
Memantine (Ebixa) Drug treatment for Alzheimer s disease
 IS 20 October 2011 Information sheet Memantine (Ebixa) Drug treatment for Alzheimer s disease Introduction... 1 How does Ebixa work?... 1 Who might benefit?... 2 What effect might Ebixa have?... 2 How
IS 20 October 2011 Information sheet Memantine (Ebixa) Drug treatment for Alzheimer s disease Introduction... 1 How does Ebixa work?... 1 Who might benefit?... 2 What effect might Ebixa have?... 2 How
Costing statement: Depression: the treatment and management of depression in adults. (update) and
 Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
A story of bipolar disorder
 A story of bipolar disorder (manic-depressive illness) Does this sound like you? D E P A R T M E N T O F H E A L T H A N D H U M A N S E R V I C E S P U B L I C H E A L T H S E R V I C E N A T I O N A
A story of bipolar disorder (manic-depressive illness) Does this sound like you? D E P A R T M E N T O F H E A L T H A N D H U M A N S E R V I C E S P U B L I C H E A L T H S E R V I C E N A T I O N A
Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP. Primary Care Provider:
 Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP Primary Care Provider: If you are considering hepatitis C treatment, please read this treatment
Liver Disease & Hepatitis Program Providers: Brian McMahon, MD, Steve Livingston, MD, Lisa Townshend, ANP Primary Care Provider: If you are considering hepatitis C treatment, please read this treatment
Understanding anxiety and depression
 Understanding anxiety and depression www.beyondblue.org.au 1300 22 4636 Anxiety Over two million people in Australia experience anxiety each year. On average, one in three women and one in fve men will
Understanding anxiety and depression www.beyondblue.org.au 1300 22 4636 Anxiety Over two million people in Australia experience anxiety each year. On average, one in three women and one in fve men will
Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too.
 The Family Library DEPRESSION What is depression? Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too. Also called
The Family Library DEPRESSION What is depression? Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too. Also called
Cancer Pain. Relief from PALLIATIVE CARE
 PALLIATIVE CARE Relief from Cancer Pain National Clinical Programme for Palliative Care For more information on the National Clinical Programme for Palliative Care, go to www.hse.ie/palliativecareprogramme
PALLIATIVE CARE Relief from Cancer Pain National Clinical Programme for Palliative Care For more information on the National Clinical Programme for Palliative Care, go to www.hse.ie/palliativecareprogramme
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
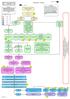 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
