Has This Prepubertal Girl Been Sexually Abused?
|
|
|
- Sheena Jennings
- 8 years ago
- Views:
Transcription
1 THE RATIONAL CLINICAL EXAMINATION CLINICIAN S CORNER Has This Prepubertal Girl Been Sexually Abused? Molly Curtin Berkoff, MD, MPH Adam J. Zolotor, MD, MPH Kathi L. Makoroff, MD Jonathan D. Thackeray, MD Robert A. Shapiro, MD Desmond K. Runyan, MD, DrPH CLINICAL SCENARIOS Case 1 A 6-year-old girl is brought to the emergency department by her mother. The mother states her child said a male babysitter touched her in the genital area. The mother reported the case to the police and was advised to bring the child to the emergency department for a medical examination. No behavioral problems were reported. The emergency department nurse asked the child why she thought her mother brought her to the hospital, and the child reported because of what happened with the babysitter. No further details were obtained. On physical examination she is sexual maturity rating 1. You note mild erythema of the inner aspect of the labia minora. The hymen is well visualized and appears normal. There is no bleeding, discharge, or lesions seen around the genitalia or anus. There are no other concerning examination findings. Is the lack of findings reassuring? See also CME available online at and questions on p Context The legal and social sequelae of interpreting genital findings as indicative of sexual abuse are significant. While the absence of genital trauma does not rule out sexual abuse, the physical examination can identify genital findings compatible with sexual abuse. Objectives To determine the diagnostic utility of the genital examination in prepubertal girls for identifying nonacute sexual abuse. Data Sources Published articles (1966-October 2008) that appeared in the MEDLINE database and were indexed under the search terms of child abuse, sexual or child abuse and either physical examination; genitalia; female, diagnosis; orsensitivity and specificity; and bibliographies of retrieved articles and textbooks. Study Selection Three of the authors independently reviewed titles of articles obtained from MEDLINE and selected articles for full-text review. Data Extraction Two authors independently abstracted data to calculate sensitivity, specificity, and likelihood ratios for the diagnosis of nonacute genital trauma caused by sexual abuse in prepubertal girls. Results Data were not pooled due to study heterogeneity. The presence of vaginal discharge (positive likelihood ratio, 2.7; 95% confidence interval, ) indicates an increased likelihood of sexual abuse. In the posterior hymen, hymenal transections, deep notches, and perforations prompt concerns for genital trauma from sexual abuse, but the sensitivity is unknown. Without a history of genital trauma from sexual abuse, the majority of prepubertal girls will not have a hymenal transection (specificity close to 100%). Conclusions Vaginal discharge as well as posterior hymenal transections, deep notches, and perforations raise the suspicion for sexual abuse in a prepubertal girl, but the findings do not independently confirm the diagnosis. Given the broad 95% confidence intervals around the likelihood ratios for the presence of findings along with the low or unknown sensitivity of all physical examination findings evaluated, the physical examination cannot independently confirm or exclude nonacute sexual abuse as the cause of genital trauma in prepubertal girls. JAMA. 2008;300(23): Case 2 An 18-month-old girl is brought to her pediatrician s office. Her family has noted blood in her diaper 1 week prior to the appointment. There is no history of trauma and no known explanation for the bleeding. On physical examination the child is crying but is easily calmed by her mother after the examination. The only significant finding is a separation or interruption (pos- Author Affiliations: Division of General Pediatrics (Drs Berkoff and Runyan) and Department of Family Medicine (Dr Zolotor), University of North Carolina, Chapel Hill; Center for Safe and Healthy Children, Cincinnati Children s Hospital Medical Center, Cincinnati, Ohio (Drs Makoroff and Shapiro); and Center for Child and Family Advocacy, Nationwide Children s Hospital, Columbus, Ohio (Dr Thackeray). Corresponding Author: Molly Curtin Berkoff, MD, MPH, Division of General Pediatrics, University of North Carolina, 231 MacNider, CB #7225, Chapel Hill, NC (molly_berkoff@med.unc.edu). The Rational Clinical Examination Section Editors: David L. Simel, MD, MHS, Durham Veterans Affairs Medical Center and Duke University Medical Center, Durham, NC; Drummond Rennie, MD, Deputy Editor, JAMA American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
2 Box 1. Suggested Behavioral Questions 19 Does your child have difficulty with the following symptoms? Headaches Stomachaches Sleeping (falling asleep, staying asleep, nightmares) Appetite School performance Anger or aggression Sexualized behaviors (this can include masturbating frequently, acting out sexually with their peers, touching other people s genitalia, showing their own genitalia) Unusual fears Depression (such as crying easily) Unusual behaviors Changes in bowel or bladder habits sible transection) of the posterior hymen that appears to extend to the base of the hymen. The source of the bleeding is not apparent. What is the chance that this is a normal finding? WHY PERFORM A PHYSICAL EXAMINATION FOR SEXUAL ABUSE ACUTELY? In 2005, more than children in the United States were sexually abused and their cases were confirmed (substantiated) by child protective services. 1 This number likely underestimates the problem because it includes only incidents of sexual abuse brought to the attention of a mandated reporter, those determined to have enough evidence for substantiation, and because most states only include abuse by caregivers. A population survey of North Carolina and South Carolina mothers suggests that official statistics may grossly underestimate the true incidence. 2 In this computerassisted, anonymous, telephone survey of 1435 mothers, while no mother reported her child had been forced to have sex with an adult or older child in the previous year, the prevalence throughout childhood was 11/1000 (1.1%). Within the year prior to the survey, the same frequency (1.1%) of children had been touched in a sexual way or had been made to touch an adult or an older child. These results were similar to those obtained in a Gallup poll of child discipline and thus serve as an anchor for estimating the pretest probability (1%) that a child has been sexually abused. 3 However, it is important to note that some surveys of adult women indicate a history of sexual abuse approaching 25%. 4 The evaluation of children for sexual abuse involves a careful and timeconsuming assessment. Each case requires a thorough history with particular attention to recent behavioral problems and a complete physical examination. Families may present with concerns that need immediate evaluation or concerns for sexual abuse may arise during an examination for a seemingly unrelated issue. However, for complicated cases it may be useful to identify the local or regional child abuse specialist; in 2009, the first child abuse pediatrics specialty examination is to be administered by the American Board of Pediatrics. Among children who recently have been sexually abused ( 72 hours) and have had forensic evidence collected, up to 25% may have evidence of acute anogenital injury. 5 A referral for an immediate examination should be made when (1) there is the possibility of acute trauma, (2) the child needs an evaluation for a symptom or illness, (3) emergency prophylaxis against infection is indicated, or (4) forensic evidence must be collected, typically within 72 hours of an acute event of sexual abuse. 6 When looking at the prevalence of significant physical findings in nonacute examinations, case-series reports note that 95% of children with a history of sexual abuse will have unremarkable physical examinations. 7,8 For some children, sexual abuse may not have involved complete penetration; for example, it may have only involved fondling or genital-genital contact. Furthermore, many children do not disclose a history of sexual abuse until long after the abuse; the hymen and surrounding tissues heal rapidly, often leaving no signs of healed trauma Finally, penetration may have occurred without causing physical injury. The legal and social sequelae of interpreting a physical examination finding as indicative or suggestive of sexual abuse are significant. Children with findings indicating sexual abuse may be removed from their family, the suspected abuser may be incarcerated, and/or the children may be stigmatized by their family and community. Therefore, it is extremely important that the examiner correctly identify abnormalities on the physical examination and relay the interpretation of these findings as well as their significance to the appropriate authorities (department of social services or child protection services, law enforcement, and clinicians). Correctly interpreting the significance of a normal examination in the presence of a history of sexual abuse also is important. A completely normal examination does not exclude abuse and is the most frequent examination finding in children who have been sexually abused. 7,8,13,14 Sexually abused children with an unremarkable physical examination may be left to suffer ongoing abuse or judged to be lying if the normal examination is incorrectly interpreted as having ruled out sexual abuse. The misinterpretation of examination findings may have significant consequences for the child s mental health, relationships with family and friends, and protection against ongoing abuse. Recent publications describe the necessary components of a sexual abuse evaluation in children and recommend an approach to interpreting physical findings in suspected child sexual abuse. 6,15,16 These guidelines suggest there are few nonacute physical examination findings that support a disclosure of child sexual abuse. However, the diagnostic utility of these nonacute findings is not well described. We conducted a systematic review of the literature on the diagnostic utility of nonacute physical examination findings for identifying sexual abuse in prepubertal girls JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
3 Our review focused solely on genital findings; it did not include anal or oral findings or review the precision and accuracy of history or laboratory tests (such as tests for sexually transmitted infections [STIs] or seminal fluid). Taking a History A clinician may have concerns from the clinical history that a child has been sexually abused. Clinicians who care for children must have a strategy for approaching both the patient and adults accompanying the child. When obtaining a history for possible child sexual abuse, the clinician should attempt to interview the caregiver and the child separately. This is especially important if the caregiver reports the child has made a disclosure of sexual abuse and/or assault. The focus should be a brief assessment with good documentation, which should include quotes of what was said. For examiners not skilled with the interviewing of young children, a limited set of questions should be used including open-ended questions (such as Tell me more or I understand someone is worried about you, can you tell me about that ). The examiner should avoid the use of yes or no questions. 6,17 Extended interviews of children younger than 3 years are not likely to be useful. Care should be made to avoid multiple interviews by different medical personnel. Consideration should be made to refer a child for an interview by a professional experienced in the evaluation of child sexual abuse. Further specifics of the interview of young children are detailed in experts recommendations. 18 The caregiver should be asked to describe the context of the child s disclosure, including if the disclosure was spontaneous or was facilitated by the caregiver. As with any medical history, a complete history and review of systems should be included. The history should include questions focusing on any new behavioral symptoms and any new medical symptoms of the child, including questions about genitourinary and gastrointestinal tract symptoms. Suggested behavioral questions are listed in BOX 1. These questions are not meant to be used as a general screening for child sexual abuse. Instead, they are questions that may assist with formulating a review of systems when con- Figure 1. Positions and Techniques for Examination of Genitalia in Prepubertal Girls A Supine frog-leg or butterfly position B Knee-chest position Labial separation Labial traction Two examination positions commonly used are the supine frog-leg or butterfly position and the knee-chest position. When findings are abnormal or concerning in the supine position, the examination should be repeated in the knee-chest position to provide additional certainty or clarification. The knee-chest position provides greater visibility of genital structures because gravity may unfold the hymenal tissue. The positions in which findings are observed should be recorded. A, In supine position, the child is examined supine on the examination table or alternatively, sitting on the lap of a trusted adult. Labial separation (performed first) helps the examiner get an initial view of the genital structures. Labial traction permits a complete view of the genital structures. B, To view the genital structures in the knee-chest position, the examiner holds the buttocks apart by pressing laterally and upward American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
4 cerns of child sexual abuse have been raised. It is important to try to establish a history of onset for any positive responses because they may help formulate a differential diagnosis. A positive response should be explored to obtain details of symptoms and associated findings. At present there are no screening tools for making a diagnosis of child sexual abuse. However, specific screenings exist to assess children s sexualized behaviors, language skills, and unusual behaviors. 20 These specific screenings may be helpful to support a diagnosis of sexual abuse. While not typically recommended for use in the general patient population, they are tools that can be used by an examiner specifically trained in interviewing children. In the clinical setting of child sexual abuse diagnosis, the screenings augment the information obtained from the caregiver interview (including an exploration of behavioral problems), child interview, and the physical examination of the child. 6,20 Performing a Physical Examination A complete physical examination is encouraged for many reasons. Sexual abuse may involve oral penetration or trauma in addition to genital and anal contact. Because a child who is sexually abused Figure 2. Female Prepubertal Genital Anatomy A Normal prepubertal female genitalia B Normal anatomical variations in hymenal openings Crescentic Annular Prepuce Clitoris Labia majora Urethral opening Labia minora Hymenal opening Hymenal membrane Fossa navicularis (vestibular fossa) Posterior fourchette (frenulum of labia) Anus Posterior hymenal rim C Comparison between clinical appearance of normal prepubertal and pubertal hymenal membranes Prepubertal Pubertal Hymenal membrane Hymenal membrane Hymenal membrane A, Inset, The region defined as the posterior hymenal rim, between 4 and 8 o clock, is shaded blue. B, There is a range of normal anatomical variations in hymenal openings. Crescentic and annular are 2 of the most common shapes. C, The photographs illustrate the range of normal prepubertal hymenal membranes. In most children, the hymen becomes thicker and more redundant during puberty JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
5 Figure 3. Hymenal Membrane Characteristics Measurements 28 Horizontal diameter of hymenal opening Clock-face diagram 12 Width of hymenal tissue from edge of the hymen to the muscular portion of the vaginal introitus at 3, 6, and 9 o clock Clinical signs Notch Superficial Deep Definition Indentation on the edge of the hymenal membrane. A notch may be angular (v-shaped) or curved (u-shaped). Notch extending <50% of width of hymen Notch extending >50% of width of hymen Deep notch Superficial notch Deep notch Photo obtained in knee-chest position Transection A tear (separation or interruption) through the entire width of the hymenal membrane extending to or through its attachment to the vaginal wall Transection Transection Transection Perforation a A hole or opening in the hymenal membrane that is separate from the hymenal opening Perforation When considering the possibility of sexual abuse during an examination, the examiner should document pertinent positive and negative findings. In addition to the clinical signs depicted in the figure, other possible findings include prominent hymenal vessels, bumps, tags, longitudinal intravaginal ridge, external ridge, periurethral bands, or vestibular bands. a Perforation is a finding reported from Berenson et al. 28 Perforation of the hymen is not a finding commonly discussed in the literature American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
6 Figure 4. Study Selection Process 1121 Excluded (no original data on evaluation of physical examination findings in prepubertal girls) 1525 Articles identified in MEDLINE searches 404 Potentially eligible also may experience other forms of trauma such as physical abuse and neglect, a complete physical examination may reveal bite marks, burns, bruises, or patterned injuries. Studies have suggested that children who experience maltreatment may have unmet medical needs such as untreated dental caries, 21 which will be recognized only after a complete physical examination. A complete physical examination also helps to deemphasize the genital examination, which may be an awkward examination for the child. Finally, a genital examination may be viewed by some children as therapeutic. 22 Examination Positions There are 2 examination positions commonly used in child sexual abuse. The first position is referred to as the supine, frog-leg or butterfly position (FIGURE 1A). In this position, the child is asked to bend her knees and place the bottoms of her feet together while abducting her legs. Neither a speculum nor stirrups are 502 Full-text articles and book chapters reviewed 72 Met inclusion criteria 11 Studies included in analysis 98 Articles identified in alternative search strategies 92 Reference lists of included articles 6 Textbook references 430 Excluded (did not meet inclusion criteria) 61 Excluded 44 Reference standard not used or physical finding used in reference standard 9 Unable to determine examination methods or definition of findings 6 Unable to separate by pubertal status 2 Study only available in abstract form used in the prepubertal female genital examination. The examiner should inspect the genitalia (FIGURE 2) for any signs of lesions, discharge, trauma (such as bruising), or scarring. The child s sexual maturity rating also should be noted. 23 To examine the hymen, the examiner separates the labia majora by applying traction. By gently grasping the labia bilaterally between the thumb and forefinger and then pulling gently outward and downward, the hymenal tissue and vaginal opening should be completely visualized without causing discomfort. If findings appear concerning or abnormal, the examination should be repeated in the knee-chest position (Figure 1B) to provide additional certainty to the findings noted in the standard, supine position. The knee-chest position permits far greater visibility of the vagina because gravity may unfold hymenaltissuetoclarifyconcerningfindings from the supine view. 24 The child kneels in a prone position on the examination table and places her head and chest onto the examination table. 6 Many studies have demonstrated poor correlation in genital examination interpretation between experienced and inexperienced examiners. 25,26 Inexperienced examiners should have abnormal findings confirmed by an experienced examiner. When possible, all genital findings should be photodocumented. Before photodocumenting, the examiner must be mindful of the specific allegations because child pornography is a form of child sexual abuse, which some children may have been experienced. Examiners performing photodocumentation for evidentiary purposes might need to obtain consent from caregivers and assent from children. Testing for STIs The US Centers for Disease Control and Prevention has guidelines for STI testing in cases of suspected sexual abuse, which include when to test for human immunodeficiency virus, hepatitis B and C, and syphilis. 27 In addition, the American Academy of Pediatrics has recommendations for when to test prepubertal children for STIs. 6 When considering the diagnosis of sexual abuse, if vaginal discharge is present the evaluation should include tests for Neisseria gonorrhoeae, Chlamydia trachomatis, and Trichomonas vaginalis from the vagina and not the cervix because vaginal samples are adequate for STI testing in prepubertal girls. 6 Infection in prepubertal girls causes vaginitis, not cervicitis. Specimens therefore are obtained from the vaginal vault or just proximal to the hymen. Avoiding direct contact with the hymenal tissue is important because this is an area very sensitive to touch in most prepubertal girls. Confirmatory testing is almost always indicated to exclude falsepositive test results. Current studies are evaluating the characteristics of nucleic amplification tests in prepubertal girls, but cultures are considered the current criterion standard. Presumptive treatment for gonorrhea and chlamydia is not recommended for the prepubertal patient due to the low incidence in these patients, the low risk of ascending infection, and the frequent 2784 JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
7 need for confirmatory testing. Human immunodeficiency virus and hepatitis B prophylaxis, when indicated, are both exceptions to this recommendation. The presence of an STI does not always mean a child was sexually abused. For some STIs, the clinician must carefully evaluate whether the child could have obtained these infections from a nonsexual mechanism such as acquisition at the time of birth or autoinoculation. 6 Referral to or consultation with a child abuse specialist is highly recommended if an STI is diagnosed. A discussion of the interpretation of STIs is beyond the scope of this article. Documentation of the Genital Examination A complete description of findings should be noted, including the child s position during the examination and whether labial traction was used. Documentation should include a notation of the sexual maturity rating. Additional items to document include the presence of erythema, lesions, abrasions, bruising, lacerations, scarring, or discharge with reference to the anatomic location of each finding (Figure 2). Current convention uses a clock-face analogy to indicate locations of the hymen; 12 o clock describes the area of the hymen closest to the urethra. The examiner should describe and document the hymenal characteristics and whether the hymenal edges contain irregularities such as notches, bumps, or complete transections (FIGURE 3). Significant findings and their location should be recorded. The examiner also should record pertinent negatives. If photos of the examination are obtained, this should be documented. METHODS Search Strategy Articles in the MEDLINE database were identified using the PubMed search engine from 1966-October The Cochrane database did not contain relevant articles. There were 2 searches using different main Medical Subject Headings of child abuse (used from ) and child abuse, sexual Box 2. Criteria for Determining Quality Score Level 1 Independent, blind comparison of physical examination findings with a reference standard among a large number of consecutive patients Level 2 Independent, blind comparison of physical examination findings with a reference standard among a small number of consecutive patients Level 3 Independent, blind comparison of physical examination findings with a reference standard among nonconsecutive patients Level 4 Nonindependent comparison of the physical examination findings with a reference standard among nonconsecutive patients (added beginning in 1987). These main Medical Subject Headings were combined with the following terms: sensitivity and specificity; genitalia, female; physical examination; and diagnosis. Both searches were limited to articles published in the English language and containing human participants. Together, the searches produced a total of 1525 articles (FIGURE 4). Three of the authors (M.C.B., K.L.M., J.D.T.) reviewed the titles and available abstracts for the 1525 articles, selecting for further review the articles that appeared to address the evaluation of prepubertal girls for signs of sexual abuse and/or hymenal trauma. Articles were selected for full-text review if they included prepubertal girls (defined as 10 years if pubertal status not mentioned) and contained original research. When there was disagreement between the reviewers, the article was pulled for fulltext review. Full-text review was performed by 2 of the authors (M.C.B., A.J.Z.). Reference sections of all 404 articles selected for full-text review were scanned for materials not available on PubMed and those not included in the original search. An additional 98 articles and book chapters were identified from the reference sections of the original articles. Thus, 502 articles and book chapters were considered. To be included in this analysis, articles had to (1) contain data permitting calculation of test characteristics by pubertal status and/or age, (2) provide sufficient data for statistical analysis, (3) use a well described or reproducible examination technique, and (4) include a reference standard to determine whether a child had been sexually abused. Acceptable reference standards included information about the child s court disposition, perpetrator confession, substantiation by the department of social services or child protection services, or diagnosis by a community or hospital-based child protection team when physical findings were not used to determine level of suspicion of sexual abuse. When articles were limited to only children without a history of sexual abuse, inclusion criteria needed to clearly outline reasons for how the authors excluded the possibility of sexual abuse. Eleven studies met all criteria and were included in this review. Information regarding quality score is included in BOX 2. A summary of these articles is presented in TABLE 1 and TABLE 2. Statistical Analysis Data were abstracted from the articles and entered into 2 2 tables to calculate the point estimates and 95% confidence intervals (CIs) for the likelihood ratios (LRs). When studies reported only the specificity, the 95% CIs for the specificity are shown with 0.5 added to the numerator and denominator when the specificity is 100% (rounded down to provide larger, more conservative 95% CIs). Test characteristics of all physical findings that would be easily recognized by a clinician who is not considered a specialist in child sexual abuse examinations are presented. Results were not mathematically pooled due to the varying methods and definitions used by each article. Instead, a range is reported where a summary value is warranted American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
8 RESULTS Eleven articles met the inclusion criteria. Only 2 of these articles included prepubertal girls with and without a history of sexual abuse, 28,29 allowing us to calculate LRs. None of these articles included information allowing for the interpretation of physical examination findings acutely ( 72 hours of the event). The remaining 9 articles only included prepubertal girls without a history of sexual abuse, permitting estimation only of the specificity of the findings. Table 1. Accuracy Studies a Source Berenson et al, Study Quality b No. of Participants No. Abused Age Range, y Reference Standard Child protection team; History of sexual abuse was based on a clinic interview including administration of a nonvalidated 8-item scale (Digital/Penile Vulvar Penetration Rating Scale); scale did not include physical examination findings as a measure Berenson et al, Child protection team; History of sexual abuse was based on a clinic interview including administration of a nonvalidated 8-item scale (Digital/Penile Vulvar Penetration Rating Scale); scale did not include physical examination findings as a measure a Children specifically evaluated to determine physical examination findings related to a history of child sexual abuse. b See Box 2 for explanation of study quality. Diagnostic Value of Physical Examination Findings Sensitivity, specificity, and positive and negative LRs derived from the 2 articles that included both populations of prepubertal girls are included in TABLE 3. The signs of vaginal discharge or the diameter of the hymenal opening were the only findings where the 95% CIs for both the positive and negative LRs excluded 1.0. The presence of vaginal discharge (LR, 2.7; 95% CI, ) or a diameter of the hymenal opening of greater than 6.5 mm in the knee-chest position (LR, 2.0; 95% CI, ) are the findings with the highest positive LRs for sexual abuse. Diagnostic characteristics of vaginal discharge were limited to the presence or absence of the finding. Diagnostic characteristics of the diameter of the hymenal opening included children examined in supine and knee-chest position with traction. Despite the higher positive LR for vaginal discharge, it is present in only 11% of prepubertal children with a history of sexual abuse. A diameter of the hymenal opening greater than 6.5 mm in the knee-chest position was present in 29% of prepubertal girls with a history of sexual abuse. The absence of either of these findings has an LR that is statistically less than 1.0, but the point estimate is so close to 1.0 that it lacks diagnostic utility. Transections in the posterior hymen are consistent with genital trauma from sexual abuse with a positive LR of 3.1, but the presence of transections has a large CI so that the diagnostic impact is uncertain (95% CI, ). The wide 95% CI is a reflection of the small number of children included in the study. The absence of a transection has little impact on the likelihood that a child has been abused (negative LR, 0.99; 95% CI, ) (Table 3). While this LR data comes from only 1 study, 4 studies Table 2. Studies of Prepubertal Girls to Establish Normal Physical Examination Findings a Source Study Quality b No. of Participants Age Range Inclusion Criteria Berenson and Grady, y Separate parent and child interviews; parent interview included administration of structured questionnaire, Child Sexual Behavior Inventory Heger et al, Prepubertal Separate parent and child interviews Myhre et al, y Parent interview and physical examination findings Berenson, Newborn-3 y Parent interview and medical record review Berenson, Newborn-1 y Parent interview and medical record review Berenson et al, Newborn-7 y Parent interview and medical record review Gardner, mo-11 y Parent history by clinician Berenson et al, Newborn None; examinations conducted prior to discharge examination after delivery McCann et al, Newborn-10 y Parent history by clinician including administration of a structured interview to determine sexual abuse (possible physical, behavioral, or emotional symptoms); review of physical examination findings by physicians experienced in child sexual abuse examinations; and high incidence of other examination findings not used to determine normality a Studies that included only girls without a history of sexual abuse permitted for calculation of specificity of physical examination findings. b See Box 2 for explanation of study quality JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
9 Table 3. Accuracy of Signs for Genital Trauma Resulting From Sexual Abuse a LR (95% CI) Sensitivity, % b Specificity, % c Positive Negative Signs From Berenson et al 29 Vulvar Ecchymosis ( ) 0.99 ( ) Laceration ( ) 0.99 ( ) Vaginal discharge d ( ) 0.93 ( ) Labial adhesion ( ) 0.94 ( ) Erythema ( ) 0.93 ( ) Linea vestibularis ( ) 1.0 ( ) Perineal depression ( ) 1.0 ( ) Friability ( ) 1.03 ( ) Prominent vessels in hymen ( ) 0.99 ( ) Superior/anterior hymen Tags ( ) 0.99 ( ) Superficial notch ( ) 0.99 ( ) Bumps ( ) 0.95 ( ) Longitudinal intravaginal ridge ( ) 0.79 ( ) Deep notch ( ) 1.0 ( ) External ridge ( ) 1.0 ( ) Periurethral bands ( ) 1.1 ( ) Vestibular bands ( ) 1.0 ( ) Inferior/posterior hymen Deep notch ( ) 0.99 ( ) Perforation ( ) 0.99 ( ) Transection ( ) 0.99 ( ) Superficial notch ( ) 0.98 ( ) External ridge ( ) 1.0 ( ) Bumps ( ) 1.0 ( ) Longitudinal intravaginal ridge ( ) 1.5 ( ) Tags ( ) 1.0 ( ) Signs From Berenson et al 28 Difference in hymenal tissue width at 3 and 9 o clock Supine position during examination, mm asymmetry ( ) 0.98 ( ) ( ) 0.91 ( ) ( ) 1.0 ( ) Knee-chest position during examination, mm asymmetry ( ) 0.95 ( ) ( ) 0.9 ( ) ( ) 0.92 ( ) Horizontal hymenal diameter 6.5 mm Supine position during examination ( ) 0.93 ( ) Knee-chest position during examination d ( ) 0.83 ( ) Amount of hymenal tissue 1.0 mm Supine position during examination 6 o clock ( ) 0.99 ( ) 3 o clock ( ) 0.99 ( ) 9 o clock ( ) 1.0 ( ) Knee-chest position during examination 6 o clock ( ) 0.98 ( ) 3 o clock ( ) 1.0 ( ) 9 o clock ( ) 0.97 ( ) Abbreviations: CI, confidence interval; LR, likelihood ratio. a Values were rounded to the nearest whole number percentage. b Sensitivity values less than 1% were rounded to 1%. c Specificity values greater than 99% were rounded to 100%. d The 95% CIs for both the positive and negative LRs do not include American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
10 Table 4. Vulvar Findings in Nonabused Population Finding No. of Participants Specificity, % (95% CI) a Erythema Heger et al, (43-59) McCann et al, (34-54) Labial adhesion Myhre et al, (89-96) Heger et al, (78-90) McCann et al, (51-71) Linea vestibularis Myhre et al, (95-100) Heger et al, (75-87) Posterior fourchette Increased vascularity Gardner, (77-93) Ragged Myhre et al, (95-99) Gardner, (74-91) McCann et al, (95-100) Urethral dilation Gardner, (62-82) McCann et al, (77-92) Vaginal discharge Myhre et al, (97-100) Gardner, (90-100) McCann et al, (94-100) Abbreviation: CI, confidence interval. a Frequency of findings in these studies that only involved nonabused children is equal to 1 minus specificity. Table 5. Hymenal Findings in Nonabused Population Finding No. of Participants Specificity, % (95% CI or Range) a Asymmetric hymen Gardner, (85-97) Bumps or mounds Myhre et al, (70-83) Berenson and Grady, b (37-58); (13-32); (20-43) Heger et al, (58-74) Berenson, (89-100) Berenson et al, (89-96) Gardner, (82-96) McCann et al, (67-86) Erythema Myhre et al, (98-100) Heger et al, (43-59) External ridge Myhre et al, (96-100) Berenson and Grady, b (93-100); (96-100); (98-100) Berenson et al, (10-16) Berenson, (92-99) Berenson, (77-95) Berenson et al, (80-90) Large hymenal opening Myhre et al, (76-87) Heger et al, (62-77) Gardner, (82-96) Longitudinal intravaginal ridge Berenson and Grady, b (7-21); (3-17); (1-15) Heger et al, (2-10) Berenson, (35-44) (continued) including only prepubertal girls without a history of genital trauma from sexual abuse report the specificity of transections based on their location within the hymen. Deep notches of the posterior hymen are consistent with genital trauma from sexual abuse (positive LR of 5.2). Similar to transections, the small number of children in the study explains the wide 95% CIs, making the diagnostic impact uncertain (95% CI, ). Additionally, the absence of a deep notch in the posterior hymen has little impact on the likelihood that a child has been abused (negative LR, 0.99; 95% CI, ). Perforations of the posterior hymen are associated with genital trauma from sexual abuse (positive LR, 3.1; 95% CI, ). Like transections and deep notches, the diagnostic impact of this finding is unclear and the absence of this finding has limited utility in determining whether a child has been abused (negative LR, 0.99; 95% CI, ). TABLE4, TABLE5, TABLE6, andtable7 listthespecificityoffindingsfromthenonabusedpopulation. Vulvarfindingsarereported in Table 4. An infrequent finding in nonabused population is vaginal discharge ( 95% specificity in all studies); inotherwords,amonggirlswhohavenot experienced sexual abuse, less than 5% have vaginal discharge. Table 5 presents the specificity of hymenal findings in the nonabused population. Possibly because of the examiner s subjective interpretation, there is wide variation in the specificity of children with findings such as bumps, tags, and notches. Table 6 and Table 7 summarize hymenal findings in the anterior or superior and posterior or inferior locations. It is difficult to comment on the specificity of these findings in the different locations because few of the studies permitted abstraction of data in this format. For example, only 1 study permitted calculation of the specificity of posterior and inferior superficial and deep notches. Four studies permitted for the calculation of specificity of transections; the specificity was 99% to 100%. Only 1 nonabused prepubertal girl among all 4 study 2788 JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
11 populations was noted to have a transection at 3 o clock. There were no transections noted in the posterior hymen between 4 and 8 o clock. Limitations This study has several significant limitations. First, most of the findings are uncommon in the nonacute population. Second, the test characteristics reported can only be applied to prepubertal girls with a nonacute history of sexual abuse. Third, many studies were excluded either because they lacked an acceptable reference standard or because they combined findings of prepubertal and postpubertal girls; therefore, the calculation of test characteristics was either not possible or was based on few participants. Test characteristics were based on the results of only 2 studies. Fourth, most eligible studies in this review included only prepubertal girls who were not sexually abused so that the sensitivity of findings was not determined. Fifth, the lack of standard definitions made it impossible to combine findings. The large ranges in specificity for some findings may have resulted from the lack of standard definitions and examination techniques. For example, the specificity of hymenal notches ranged from 27% to 100%. Studies included defined ventral or anterior notches as either 12 o clock in annular hymens 31 or as a disruption of the hymenal membrane at 11 or 1 o clock in crescent-shaped hymens. 38 Different examination techniques may be responsible for some of the variation. For example, if an examiner did not use labial traction he/she may not be able to visualize the entire hymen and therefore may not be able to accurately determine if there is a notch or bump. Additionally, if a child is only examined in the supine and not the knee-chest position, the findings may be missed or mischaracterized. For example, an examiner may be convinced they are seeing a notch of the posterior hymen in a child in the supine position while the examination in the kneechest position demonstrates that the finding is more consistent with an uninterrupted portion of the hymen. Table 5. Hymenal Findings in Nonabused Population (continued) Finding No. of Participants Specificity, % (95% CI or Range) a Longitudinal intravaginal ridge Berenson, (34-60) Berenson et al, (69-81) Berenson, (40-49) McCann et al, (2-18) Notches Berenson and Grady, b (88-99); (85-97); (81-97) Heger et al, c (20-34); (75-88) Berenson, (86-96) Berenson, (66-88) Berenson et al, (88-96) Gardner, (94-100) Berenson, (68-76) McCann et al, (91-100) Periurethral bands Berenson and Grady, b (0.1-1); (0.01-1); (0-5) McCann et al, (39-60) Prominent vessels Myhre et al, (76-87) Heger et al, (55-70) Gardner, (53-74) McCann et al, (58-80) Tags Myhre et al, (99-100) Heger et al, (94-100) Berenson and Grady, b (80-94); (83-97); (83-98) Berenson, (88-97) Berenson, (82-97) Berenson et al, (95-99) Gardner, (95-100) Berenson, (84-90) McCann et al, (66-85) Thickened hymen Heger et al, (46-62) McCann et al, (35-57) Vestibular bands Berenson and Grady, b (44-65); (26-47); (33-58) Abbreviation: CI, confidence interval. a Some studies had repeat examinations so ranges are shown. b Study includes repeat examinations on the same children at different age. c Study includes discussion of anterior and posterior notches. Table 6. Superior and Anterior Hymenal Findings in Nonabused Population Finding No. of Participants Specificity, % (95% CI) Bumps Berenson et al, (89-96) Longitudinal intravaginal ridge Berenson, (88-97) Berenson et al, (95-100) Ventral or anterior notch Heger et al, (20-34) Berenson, (92-99) Berenson et al, (90-97) Berenson et al, a (72-81); (99-100) McCann et al, (96-100) Tags Berenson, (94-100) Berenson et al, (97-100) Abbreviation: CI, confidence interval. a This study includes repeat examinations on the same children at different age so ranges are shown American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
12 Table 7. Inferior and Posterior Hymenal Findings in Nonabused Population Finding No. of Participants Specificity, % (95% CI) Bumps Berenson et al, (93-99) Longitudinal intravaginal ridge Berenson, (73-87) Berenson et al, (88-96) Notch Heger et al, (75-88) Berenson, (99-100) Berenson et al, (99-100) Berenson et al, a (99-100) Deep notch Myhre et al, (99-100) Superficial notch Myhre et al, (98-100) Transection Myhre et al, (99-100) Berenson and Grady, (99-100) Heger et al, (99-100) Berenson et al, (99-100) Width (narrowed hymen) Heger et al, (71-84) Berenson et al, (93-99) Abbreviation: CI, confidence interval. a This study includes repeat examinations on the same children at different age so ranges are shown. Take-Home Message This study focused on the test characteristics of nonacute genital findings in prepubertal girls to assist in the diagnosis of sexual abuse. Findings are limited to 2 case-control studies that included both sexually abused and nonabused girls. Nine other studies included in the review only included nonabused prepubertal girls. The diagnostic utility of the presence or absence of genital findings on the probability of genital trauma or maltreatment requires an understanding of the pretest probability. While population surveys suggest a starting pretest probability of 1%, this estimate applies only to the population of children at large. Once a family member expresses concern for maltreatment, the probability of maltreatment likely increases much higher than the general population. No population data exist to estimate the probability once a parent expresses suspicion of maltreatment. Physicians who evaluate at-risk children must assess the probability of maltreatment and must perform an objective physical examination unbiased by their pretest probability. We caution that the findings for the diameter of the hymenal opening may lack precision and therefore are not clinically useful. The ability to adequately measure the diameter of the hymenal opening is limited by a child s ability to relax. It also is limited by the examiner s technique and tools. The diameter of the hymenal opening may be measured from photographs or by using tools such as a tape measure or by a grid on the viewfinder of a colposcope. The diameter of the hymenal opening varies with a patient s weight, age, amount of traction applied, and by the amount of hymenal tissue present. Measuring the diameter of the hymenal opening is not easily replicated and therefore this finding is not useful for helping to determine whether a prepubertal girl has been sexually abused. A transection of the posterior hymen between 4 and 8 o clock in prepubertal girls suggests genital penetrating trauma; however, the presence of this finding is not confirmatory of sexual abuse. Posterior hymenal findings including transections between 4 and 8 o clock, deep notches, and perforations were not seen in studies of prepubertal girls without a history of genital trauma from sexual abuse included in this systematic review. Therefore, one can conclude that the posterior hymenal findings of transections, deep notches, and perforations are extremely infrequent findings among children without a history of genital trauma from sexual abuse or other means. Current guidelines suggest deep notches are supportive of a disclosure of sexual abuse. Without a disclosure of sexual abuse, interpretation of deep notches is considered an indeterminate finding that may require further evaluation. 15,16 While deep notches of the posterior hymen were not found in prepubertal girls without a history of sexual abuse, the finding also is uncommon among sexually abused children (positive LR, 5.2; 95% CI, ). Similarly, while some authors list hymenal transections as indicating penetrating trauma to the hymen, the finding also has a wide 95% CI (positive LR, 3.1; 95% CI, ). 15,16 However, because the prevalence of posterior hymenal findings (between 4 and 8 o clock) such as transections, deep notches, and perforations are near zero in nonabused prepubertal girls, the presence of these examination findings suggests genital trauma from sexual abuse. In the absence of known genital trauma from accidental means, the possibility for sexual abuse must be strongly considered. In a prepubertal girl with a posterior hymenal finding of a transection (between 4 and 8 o clock), a deep notch (between 4 and 8 o clock), or a perforation, a report to child protective services should be strongly considered. At a minimum, an examination by a child abuse specialist should occur to confirm these findings and to help provide a careful interpretation regarding the likelihood of sexual abuse. While identifying trauma and infectious diseases is extremely important and may require specific treatment, it also is important to reassure a child and her family that she is healthy and that her genital examination is normal. A clinician s assurance of a genital exami JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
13 nation without evidence of trauma, and hence normal findings helps begin a process of healing. This review should not be interpreted to mean that the physical examination of a prepubertal girl with a suspicion of sexual abuse has limited value. This review did not focus on the test characteristics of acute findings nor the usefulness of testing for STIs when indicated. Previous research has stated that the majority of girls who provide a history of sexual abuse will have a normal or unremarkable examination. 39 Therefore, the fact that a child has an unremarkable genital examination should not dispute a child s allegations and a careful investigation by child protective services and/or law enforcement should continue. In summary, results of this review suggest the accuracy of most genital findings used in isolation to predict nonacute sexual abuse among prepubertal girls is poor. In addition, this review suggests that the presence of vaginal discharge in a prepubertal girl should raise the suspicion of sexual abuse. Other findings that support a suspicion of sexual abuse in a prepubertal girl include deep notches and transections in the posterior hymen between 4 and 8 o clock as well as a perforation of the hymen. It is important to note that a perforation of the hymen is not a finding commonly discussed in the literature and is not part of what is typically used to assist in the interpretation of physical examination findings for children suspected of being sexually abused. 16 Transections, deep notches, and perforations of the hymen as described above raise the suspicion of sexual abuse and therefore should trigger a thoughtful investigation by the appropriate agency (social services and/or law enforcement) for the possibility of sexual abuse. The rarity of these findings in the studies included limits the ability of transections, deep notches, and perforations to be used alone in the diagnosis of sexual abuse among prepubertal girls. Research in this area continues to be challenging and likely accounts for why only 2 studies met criteria to provide data regarding diagnostic accuracy. Recruitment of nonsexually abused children for thorough genital examinations is difficult. The definition of a criterion standard for child sexual abuse is lacking given the context of providing a medical diagnosis that requires a forensic interpretation, and the veracity of information provided to the physician in arriving at a diagnosis. The department of social services or child protection services and court decisions of abuse can by influenced by the interpretation of physical examination findings. Additionally, it can be difficult to determine the type of abuse a child has experienced, whether it is fondling or hymenal penetration. However, despite these limitations it is important to try to further the field with larger studies with a strict reference standard and definitions; these studies should include both sexually abused and nonsexually abused girls. They also should include standardized definitions of findings, standardized examination techniques of children in the supine position as well as knee-chest position when possible, and a description of the type of abuse experienced. This review illustrates that more data are needed to determine the test characteristics of physical examination findings in prepubertal girls with a suspicion of sexual abuse. Reporting Concerns to the Appropriate Agency All physicians in the United States are required by state law to report suspected cases of child sexual abuse. 6 To determine the level of suspicion a physician should use the history, physical examination, and laboratory evaluation together. In general, when there is a history of possible sexual abuse because a child has made a concerning statement, if there is a concerning finding, or if there is a presence of an STI that is suggestive of sexual transmission, a report should be made to the appropriate agency according to local guidelines. SCENARIO RESOLUTION Case 1 The finding of erythema on the labia minora is a nonspecific finding (positive LR of 1.1) and therefore does not assist with determining whether the child has been sexually abused or the type of sexual contact the child has experienced. The fact that the child has an unremarkable examination of the hymen also does not assist with determining if the child has been sexually abused or with determining if the child has experienced some form of penetration (negative LR of most findings approximates to 1.0). The objective findings do not support or refute the mother s suspicion. Because the patient is a verbal child, a formal interview should be conducted with the child in a controlled atmosphere by a trained expert or a report made to the appropriate authorities. In many areas, specialized centers exist that assist in comprehensive evaluations for suspected sexual abuse cases. The physician should be reminded that his/her role is to help with coordinating follow-up services for many of these cases and to stress the importance of a comprehensive interview of the child by a skilled examiner that focuses on the concern for sexual abuse. Case 2 It is difficult to determine a history of sexual abuse in a child before he/she is verbal. Hymenal injury, especially a transection (positive LR for transection of 3.1), without any other known history of trauma supports a suspicion of sexual abuse. An evaluation for sexual abuse should be completed and an immediate referral to the appropriate agency should be made. Author Contributions: Dr Berkoff had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Berkoff, Makoroff, Thackeray, Shapiro, Runyan. Acquisition of data: Berkoff, Zolotor, Makoroff, Thackeray. Analysis and interpretation of data: Berkoff, Zolotor, Makoroff, Shapiro, Runyan American Medical Association. All rights reserved. (Reprinted) JAMA, December 17, 2008 Vol 300, No
14 Drafting of the manuscript: Berkoff, Zolotor. Critical revision of the manuscript for important intellectual content: Berkoff, Zolotor, Makoroff, Thackeray, Shapiro, Runyan. Statistical analysis: Berkoff, Zolotor. Administrative, technical, or material support: Makoroff, Thackeray, Shapiro, Runyan. Study supervision: Runyan. Financial Disclosures: None reported. Funding/Support: Dr Berkoff was supported in part by the Robert Wood Johnson Clinical Scholars Program. Role of the Sponsor: The funding source had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. Additional Contributions: We thank David Simel, MD, for his guidance and careful review of the manuscript as well as Janet Serwint, MD, and Philip V. Scribano, DO, for their thoughtful review of this article. None of the persons listed were compensated for their contribution. REFERENCES 1. US Department of Health and Human Services, Administration on Children, Youth, and Families. Child Maltreatment Washington, DC: US Government Printing Office; Theodore AD, Chang JJ, Runyan DK, Hunter WM, Bangdiwala SI, Agans R. Epidemiologic features of the physical and sexual maltreatment of children in the Carolinas. Pediatrics. 2005;115(3):e331-e Gallup Poll Organization. Disciplining Children in America: A Gallup Poll Report. Princeton, NJ: Gallup Poll Organization; Dube SR, Anda RF, Felitti VJ, Chapman DP, Williamson DF, Giles WH. Childhood abuse, household dysfunction, and the risk of attempted suicide throughout the life span: findings from the Adverse Childhood Experiences Study. JAMA. 2001;286 (24): Christian CW, Lavelle JM, De Jong AR, Loiselle J, Brenner L, Joffe M. Forensic evidence findings in prepubertal victims of sexual assault. Pediatrics. 2000; 106(1 pt 1): Kellogg N. The evaluation of sexual abuse in children. Pediatrics. 2005;116(2): Adams JA. Normal studies are essential for objective medical evaluations of children who may have been sexually abused. Acta Paediatr. 2003;92(12): Heger A, Ticson L, Velasquez O, Bernier R. Children referred for possible sexual abuse: medical findings in 2384 children. Child Abuse Negl. 2002; 26(6-7): McCann J, Voris J, Simon M. Genital injuries resulting from sexual abuse: a longitudinal study. Pediatrics. 1992;89(2): McCann J, Voris J. Perianal injuries resulting from sexual abuse: a longitudinal study. Pediatrics. 1993; 91(2): McCann J, Miyamoto S, Boyle C, Rogers K. Healing of hymenal injuries in prepubertal and adolescent girls: a descriptive study. Pediatrics. 2007;119(5): e1094-e McCann J, Miyamoto S, Boyle C, Rogers K. Healing of nonhymenal genital injuries in prepubertal and adolescent girls: a descriptive study. Pediatrics. 2007; 120(5): Kellogg ND, Menard SW, Santos A. Genital anatomy in pregnant adolescents: normal does not mean nothing happened. Pediatrics. 2004;113 (1 pt 1):e67-e AdamsJA,HarperK,KnudsonS,RevillaJ.Examination findings in legally confirmed child sexual abuse: it s normal to be normal. Pediatrics. 1994;94(3): Adams JA, Kaplan RA, Starling SP, et al. Guidelines for medical care of children who may have been sexually abused. J Pediatr Adolesc Gynecol. 2007; 20(3): Adams JA. Guidelines for medical care of children evaluated for suspected sexual abuse: an update for Curr Opin Obstet Gynecol. 2008; 20(5): Bernet W; American Academy of Child and Adolescent Psychiatry. Practice parameters for the forensic evaluation of children and adolescents who may have been physically or sexually abused. J Am Acad Child Adolesc Psychiatry. 1997;36(10)(suppl): 37S-56S. 18. American Professional Society on the Abuse of Children. Psychosocial Evaluation of Suspected Sexual Abuse in Children. 2nd ed. Elmhurst, IL: American Professional Society on the Abuse of Children; 1997: Child Medical Evaluation Program. North Carolina Child Medical Evaluation Program Tool. http: // Accessed July 29, Friedrich WN, Fisher JL, Dittner CA, et al. Child Sexual Behavior Inventory: normative, psychiatric, and sexual abuse comparisons. Child Maltreat. 2001; 6(1): Simms MD, Dubowitz H, Szilagyi MA. Health care needs of children in the foster care system. Pediatrics. 2000;106(4)(suppl): De Jong AR. Impact of child sexual abuse medical examinations on the dependency and criminal systems. Child Abuse Negl. 1998;22(6): Rosen DS. Physiologic growth and development during adolescence. Pediatr Rev. 2004;25(6): McCann J, Voris J, Simon M, Wells R. Comparison of genital examination techniques in prepubertal girls. Pediatrics. 1990;85(2): Makoroff KL, Brauley JL, Brandner AM, Myers PA, Shapiro RA. Genital examinations for alleged sexual abuse of prepubertal girls: findings by pediatric emergency medicine physicians compared with child abuse trained physicians. Child Abuse Negl. 2002;26 (12): Sinal SH, Lawless MR, Rainey DY, et al. Clinician agreement on physical findings in child sexual abuse cases. Arch Pediatr Adolesc Med. 1997;151(5): Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines Accessed March 6, Berenson AB, Chacko MR, Wiemann CM, Mishaw CO, Friedrich WN, Grady JJ. Use of hymenal measurements in the diagnosis of previous penetration. Pediatrics. 2002;109(2): Berenson AB, Chacko MR, Wiemann CM, Mishaw CO, Friedrich WN, Grady JJ. A case-control study of anatomic changes resulting from sexual abuse. Am J Obstet Gynecol. 2000;182(4): Berenson AB, Grady JJ. A longitudinal study of hymenal development from 3 to 9 years of age. J Pediatr. 2002;140(5): Heger AH, Ticson L, Guerra L, et al. Appearance of the genitalia in girls selected for nonabuse: review of hymenal morphology and nonspecific findings. J Pediatr Adolesc Gynecol. 2002;15(1): Myhre AK, Berntzen K, Bratlid D. Genital anatomy in non-abused preschool girls. Acta Paediatr. 2003; 92(12): Berenson AB. A longitudinal study of hymenal morphology in the first 3 years of life. Pediatrics. 1995; 95(4): Berenson AB. Appearance of the hymen at birth and one year of age: a longitudinal study. Pediatrics. 1993;91(4): Berenson AB, Heger AH, Hayes JM, Bailey RK, Emans SJ. Appearance of the hymen in prepubertal girls. Pediatrics. 1992;89(3): Gardner JJ. Descriptive study of genital variation in healthy, nonabused premenarchal girls. J Pediatr. 1992;120(2 pt 1): Berenson A, Heger A, Andrews S. Appearance of the hymen in newborns. Pediatrics. 1991;87(4): McCann J, Wells R, Simon M, Voris J. Genital findings in prepubertal girls selected for nonabuse: a descriptive study. Pediatrics. 1990;86(3): Adams JA. Medical evaluation of suspected child sexual abuse. J Pediatr Adolesc Gynecol. 2004; 17(3): JAMA, December 17, 2008 Vol 300, No. 23 (Reprinted) 2008 American Medical Association. All rights reserved.
Child Maltreatment Medical Consultation - Referral Guidelines
 Child Maltreatment Medical Consultation - Referral Guidelines These guidelines are intended to help CPS and law enforcement decide when to seek medical consultation for suspected child abuse and neglect.
Child Maltreatment Medical Consultation - Referral Guidelines These guidelines are intended to help CPS and law enforcement decide when to seek medical consultation for suspected child abuse and neglect.
Child Medical Evaluations. Molly Curtin Berkoff MD, MPH Medical Director, NC CMEP
 Child Medical Evaluations Molly Curtin Berkoff MD, MPH Medical Director, NC CMEP Objectives Introduce the Child Medical Evaluation Program (CMEP) Describe the program Discuss components of program Child
Child Medical Evaluations Molly Curtin Berkoff MD, MPH Medical Director, NC CMEP Objectives Introduce the Child Medical Evaluation Program (CMEP) Describe the program Discuss components of program Child
Medical Evaluation for Child Sexual Abuse. What Is Normal & How Do We Know? What do we know about exam findings? 12/4/2008
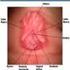 Medical Evaluation for Child Sexual Abuse Cathy Baldwin-Johnson MD FAAFP Marg Volz RN CPNP Alaska CARES Providence Health Services Alaska What Is Normal & How Do We Know? What do we know about exam findings?
Medical Evaluation for Child Sexual Abuse Cathy Baldwin-Johnson MD FAAFP Marg Volz RN CPNP Alaska CARES Providence Health Services Alaska What Is Normal & How Do We Know? What do we know about exam findings?
Child Abuse and Neglect AAP Policy Recommendations
 Child Abuse and Neglect AAP Policy Recommendations When Inflicted Skin Injuries Constitute Child Abuse Committee on Child Abuse and Neglect PEDIATRICS Vol. 110 No. 3 September 2002, pp. 644-645 Recommendations
Child Abuse and Neglect AAP Policy Recommendations When Inflicted Skin Injuries Constitute Child Abuse Committee on Child Abuse and Neglect PEDIATRICS Vol. 110 No. 3 September 2002, pp. 644-645 Recommendations
Forensic Examination
 Forensic Examination _ _ 4 purposes of forensic evidence To identify the assailant To confirm recent sexual contact To establish force or threat To corroborate the victim s story When to obtain a forensic
Forensic Examination _ _ 4 purposes of forensic evidence To identify the assailant To confirm recent sexual contact To establish force or threat To corroborate the victim s story When to obtain a forensic
Recognising and Managing Child Abuse DCH Lectures 2015. Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital
 Recognising and Managing Child Abuse DCH Lectures 2015 Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common presentations
Recognising and Managing Child Abuse DCH Lectures 2015 Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common presentations
OHIO ATTORNEY GENERAL SEXUAL ASSAULT FORENSIC EXAMINATION (SAFE) PROGRAM INSTRUCTIONS FOR REIMBURSEMENT FORM
 OHIO ATTORNEY GENERAL SEXUAL ASSAULT FORENSIC EXAMINATION (SAFE) PROGRAM INSTRUCTIONS FOR REIMBURSEMENT FORM All exams must be conducted using the 2011 Ohio Sexual Assault Protocol for Sexual Assault Forensic
OHIO ATTORNEY GENERAL SEXUAL ASSAULT FORENSIC EXAMINATION (SAFE) PROGRAM INSTRUCTIONS FOR REIMBURSEMENT FORM All exams must be conducted using the 2011 Ohio Sexual Assault Protocol for Sexual Assault Forensic
YOU are a mandated reporter.
 Nurses Guide for Reporting Suspected Child Abuse and Neglect YOU are a mandated reporter. The Michigan Child Protection Law requires that certain persons report any case of suspected child abuse or child
Nurses Guide for Reporting Suspected Child Abuse and Neglect YOU are a mandated reporter. The Michigan Child Protection Law requires that certain persons report any case of suspected child abuse or child
7 Child sexual abuse SUMMARY. 7.1 Definition of child sexual abuse
 BIBLIOGRAPHY 7 Child sexual abuse SUMMARY The dynamics of child sexual abuse differ from those of adult sexual abuse. In particular, children rarely disclose sexual abuse immediately after the event. Moreover,
BIBLIOGRAPHY 7 Child sexual abuse SUMMARY The dynamics of child sexual abuse differ from those of adult sexual abuse. In particular, children rarely disclose sexual abuse immediately after the event. Moreover,
36 Interviewing the Patient, Taking a History, and Documentation
 CHAPTER 36 Interviewing the Patient, Taking a History, and Documentation Learning Outcomes 36.1 Identify the skills necessary to conduct a patient interview. 36.2 Implement the procedure for conducting
CHAPTER 36 Interviewing the Patient, Taking a History, and Documentation Learning Outcomes 36.1 Identify the skills necessary to conduct a patient interview. 36.2 Implement the procedure for conducting
SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION. Assaults on Clients: Suspected or Reported
 SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION DATE: March 22, 2001 MENTAL HEALTH POLICY: MH 01-03 SUBJECT: Assaults on Clients: Suspected or Reported AUTHORITY: California Welfare and Institution Codes
SAN MATEO COUNTY MENTAL HEALTH SERVICES DIVISION DATE: March 22, 2001 MENTAL HEALTH POLICY: MH 01-03 SUBJECT: Assaults on Clients: Suspected or Reported AUTHORITY: California Welfare and Institution Codes
Frequently Asked Questions: Reporting Child Abuse and Neglect in the University System of Maryland
 Frequently Asked Questions: Reporting Child Abuse and Neglect in the University System of Maryland I. What Constitutes Child Abuse and Neglect A. What is Child Abuse? Abuse is defined in Maryland law as
Frequently Asked Questions: Reporting Child Abuse and Neglect in the University System of Maryland I. What Constitutes Child Abuse and Neglect A. What is Child Abuse? Abuse is defined in Maryland law as
The challenge of herpes
 The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
The challenge of herpes Herpes is a common and personally challenging disease Herpes is very common. One out of four adults has genital herpes. When people first hear that they are infected, many become
Frequently Asked Questions
 Frequently Asked Questions Testing for Gonorrhea Q1: What test should be completed for accurately diagnosing gonorrhea? A1: Testing is done with either a culture or a NAAT (nucleic acid amplification test).
Frequently Asked Questions Testing for Gonorrhea Q1: What test should be completed for accurately diagnosing gonorrhea? A1: Testing is done with either a culture or a NAAT (nucleic acid amplification test).
Government of Western Australia Department for Child Protection and Family Support. How do I recognise when a child is at risk of abuse or neglect?
 Government of Western Australia Department for Child Protection and Family Support How do I recognise when a child is at risk of abuse or neglect? Physical abuse Physical abuse is when someone is deliberately
Government of Western Australia Department for Child Protection and Family Support How do I recognise when a child is at risk of abuse or neglect? Physical abuse Physical abuse is when someone is deliberately
Child Advocacy. Medical Staff: Administrative Staff: Children s Access Center. Outpatient Referral. Child Advocacy Office Numbers
 Child Advocacy Children s Access Center 24/7 access for referring physicians (866) 353-KIDS (5437) Outpatient Referral Referral forms online at: www.childrenscentralcal.org/services/medicaloffice/refer
Child Advocacy Children s Access Center 24/7 access for referring physicians (866) 353-KIDS (5437) Outpatient Referral Referral forms online at: www.childrenscentralcal.org/services/medicaloffice/refer
CHILDHOOD SEXUAL ABUSE FACT SHEET
 CHILDHOOD SEXUAL ABUSE FACT SHEET Emily M. Douglas and David Finkelhor PART 1: HOW MANY CHILDREN ARE THE VICTIMS OF CHILD SEXUAL ABUSE? There are many estimates of the number of children who are the victims
CHILDHOOD SEXUAL ABUSE FACT SHEET Emily M. Douglas and David Finkelhor PART 1: HOW MANY CHILDREN ARE THE VICTIMS OF CHILD SEXUAL ABUSE? There are many estimates of the number of children who are the victims
Accent on Health Obgyn, PC HERPES Frequently Asked Questions
 1. What is herpes? 2. How common is herpes? 3. Is there a cure for herpes? 4. What is oral herpes (cold sores)? 5. How is oral herpes spread? 6. What is genital herpes? 7. How is genital herpes spread?
1. What is herpes? 2. How common is herpes? 3. Is there a cure for herpes? 4. What is oral herpes (cold sores)? 5. How is oral herpes spread? 6. What is genital herpes? 7. How is genital herpes spread?
Sexual Assault of People in Aged Care Settings: Towards a Better Understanding and Response
 Northern Sydney Sexual Assault Service J Blyth, L Kelly Sexual Assault of People in Aged Care Settings: Towards a Better Understanding and Response In the past 25 years there has been widespread focus
Northern Sydney Sexual Assault Service J Blyth, L Kelly Sexual Assault of People in Aged Care Settings: Towards a Better Understanding and Response In the past 25 years there has been widespread focus
How To Write A Medical Report
 State of California Governor s Office of Emergency Services MEDICAL REPORT: SUSPECTED CHILD PHYSICAL ABUSE AND NEGLECT EXAMINATION OES 900 For more information or assistance in completing the OES 900,
State of California Governor s Office of Emergency Services MEDICAL REPORT: SUSPECTED CHILD PHYSICAL ABUSE AND NEGLECT EXAMINATION OES 900 For more information or assistance in completing the OES 900,
Additional Information for Community Partners Activity
 Additional Information for Community Partners Activity Law Enforcement Sexual abuse referrals are referred to police on the CY-104 (Report to Law Enforcement Officials). Note that referrals which do not
Additional Information for Community Partners Activity Law Enforcement Sexual abuse referrals are referred to police on the CY-104 (Report to Law Enforcement Officials). Note that referrals which do not
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Developed by: California Department of Public Health (CDPH) Sexually Transmitted Diseases (STD) Control Branch. In collaboration with:
 Best Practices for the Prevention and Early Detection of Repeat Chlamydial and Gonococcal Infections: Effective Partner Treatment and Patient Retesting Strategies for Implementation in California Health
Best Practices for the Prevention and Early Detection of Repeat Chlamydial and Gonococcal Infections: Effective Partner Treatment and Patient Retesting Strategies for Implementation in California Health
Assessing capacity to consent and to give evidence
 Assessing capacity to consent and to give evidence Dr Theresa Joyce Estia Centre; South London & Maudsley NHS Trust, London, UK This presentation will consider 4 topics Assessing capacity to consent to
Assessing capacity to consent and to give evidence Dr Theresa Joyce Estia Centre; South London & Maudsley NHS Trust, London, UK This presentation will consider 4 topics Assessing capacity to consent to
Examination Content Blueprint
 Examination Content Blueprint Overview The material on NCCPA s certification and recertification exams can be organized in two dimensions: (1) organ systems and the diseases, disorders and medical assessments
Examination Content Blueprint Overview The material on NCCPA s certification and recertification exams can be organized in two dimensions: (1) organ systems and the diseases, disorders and medical assessments
Female Genitalia Surgery. Individual Funding Request Policy. Date Adopted: 09 December 2015. VERSION: 1516.v4
 Female Genitalia Surgery Individual Funding Request Policy Date Adopted: 09 December 2015 VERSION: 1516.v4 Document Control Title of document Female Genitalia Surgery Individual Funding Request Policy
Female Genitalia Surgery Individual Funding Request Policy Date Adopted: 09 December 2015 VERSION: 1516.v4 Document Control Title of document Female Genitalia Surgery Individual Funding Request Policy
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT SUSPECTED VICTIMS OF ABUSE AND NEGLECT (PATIENTS PRESENTING TO LSUHSC)
 LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT SUSPECTED VICTIMS OF ABUSE AND NEGLECT (PATIENTS PRESENTING TO LSUHSC) Purpose: To establish guidelines for all hospital personnel to follow
LOUISIANA STATE UNIVERSITY HEALTH SCIENCES CENTER - SHREVEPORT SUSPECTED VICTIMS OF ABUSE AND NEGLECT (PATIENTS PRESENTING TO LSUHSC) Purpose: To establish guidelines for all hospital personnel to follow
Technical Assistance Document 5
 Technical Assistance Document 5 Information Sharing with Family Members of Adult Behavioral Health Recipients Developed by the Arizona Department of Health Services Division of Behavioral Health Services
Technical Assistance Document 5 Information Sharing with Family Members of Adult Behavioral Health Recipients Developed by the Arizona Department of Health Services Division of Behavioral Health Services
OSTEOPATHIC CARE OF CHILDREN
 OSTEOPATHIC CARE OF CHILDREN OSTEOPATHIC HEALTHCARE OF MAINE OSTEOPATHIC CARE OF CHILDREN Donald V. Hankinson, D.O. Childhood is a time when the potential for mental, physical and spiritual growth is profound.
OSTEOPATHIC CARE OF CHILDREN OSTEOPATHIC HEALTHCARE OF MAINE OSTEOPATHIC CARE OF CHILDREN Donald V. Hankinson, D.O. Childhood is a time when the potential for mental, physical and spiritual growth is profound.
Yes, I know I have genital herpes:
 Counseling Messages for Herpes Simplex Type II (HSV-II) Genital herpes Always take the time to attend to the participant s feelings and emotional state; for some people, this is the most devastating news
Counseling Messages for Herpes Simplex Type II (HSV-II) Genital herpes Always take the time to attend to the participant s feelings and emotional state; for some people, this is the most devastating news
Child Abuse/Neglect Intake, Investigation and Assessment Diane Carver, Program Administrator DCF Prevention and Protection Services
 Child Abuse/Neglect Intake, Investigation and Assessment Diane Carver, Program Administrator DCF Prevention and Protection Services Strong Families Make a Strong Kansas Child Abuse Prevention and Treatment
Child Abuse/Neglect Intake, Investigation and Assessment Diane Carver, Program Administrator DCF Prevention and Protection Services Strong Families Make a Strong Kansas Child Abuse Prevention and Treatment
HIV/AIDS: General Information & Testing in the Emergency Department
 What Is HIV? HIV/AIDS: General Information & Testing in the Emergency Department HIV is the common name for the Human Immunodeficiency Virus. HIV is a retrovirus. This means it can enter the body s own
What Is HIV? HIV/AIDS: General Information & Testing in the Emergency Department HIV is the common name for the Human Immunodeficiency Virus. HIV is a retrovirus. This means it can enter the body s own
Understanding Abuse and Neglect. A Collaborative Training Module by the John H. Stroger Hospital Medical, Nursing and Social Work Staffs
 Understanding Abuse and Neglect A Collaborative Training Module by the John H. Stroger Hospital Medical, Nursing and Social Work Staffs Training Outline Review of definitions and general facts Outline
Understanding Abuse and Neglect A Collaborative Training Module by the John H. Stroger Hospital Medical, Nursing and Social Work Staffs Training Outline Review of definitions and general facts Outline
A Guide for Larimer County Parents
 Services Child Protection A Guide for Larimer County Parents This booklet was prepared by the Program Committee of the Larimer County Child Advocacy Center in consultation with the Larimer County Department
Services Child Protection A Guide for Larimer County Parents This booklet was prepared by the Program Committee of the Larimer County Child Advocacy Center in consultation with the Larimer County Department
Elder and Dependent Adult Abuse. Adult Protective Services Contra Costa County
 Elder and Dependent Adult Abuse Adult Protective Services Contra Costa County Objectives As a result of this training, participants will be able to: Define elder and dependent adult abuse Define the responsibilities
Elder and Dependent Adult Abuse Adult Protective Services Contra Costa County Objectives As a result of this training, participants will be able to: Define elder and dependent adult abuse Define the responsibilities
CHALLENGES IN IDENTIFYING NON- ACCIDENTAL INJURY. Graham Vimpani Senior Clinical Advisor Child Protection and Wellbeing NSW Kids and Families
 CHALLENGES IN IDENTIFYING NON- ACCIDENTAL INJURY Graham Vimpani Senior Clinical Advisor Child Protection and Wellbeing NSW Kids and Families Possible presentations of Physical abuse and neglect Cutaneous
CHALLENGES IN IDENTIFYING NON- ACCIDENTAL INJURY Graham Vimpani Senior Clinical Advisor Child Protection and Wellbeing NSW Kids and Families Possible presentations of Physical abuse and neglect Cutaneous
Identifying Victims of Abuse and Neglect
 Wesley Medical Center Wichita, Kansas Identifying Victims of Abuse and Neglect Department of Staff Development August, 2008 Identifying Victims of Abuse and Neglect Objectives Define the major types of
Wesley Medical Center Wichita, Kansas Identifying Victims of Abuse and Neglect Department of Staff Development August, 2008 Identifying Victims of Abuse and Neglect Objectives Define the major types of
Information for you Abortion care
 Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
CERVICAL CANCER What every woman should know What is a cervix?
 CERVICAL CANCER What every woman should know What is a cervix? The cervix is the entrance to the womb from the vagina. It is the narrow, lower part of the uterus that is the passageway connecting the uterus
CERVICAL CANCER What every woman should know What is a cervix? The cervix is the entrance to the womb from the vagina. It is the narrow, lower part of the uterus that is the passageway connecting the uterus
Sarasota Personal Medicine 1250 S. Tamiami Trail, Suite 202 Sarasota, FL 34239 Phone 941.954.9990 Fax 941.954.9995
 Sarasota Personal Medicine 1250 S. Tamiami Trail, Suite 202 Sarasota, FL 34239 Phone 941.954.9990 Fax 941.954.9995 NOTICE OF PRIVACY PRACTICES THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY
Sarasota Personal Medicine 1250 S. Tamiami Trail, Suite 202 Sarasota, FL 34239 Phone 941.954.9990 Fax 941.954.9995 NOTICE OF PRIVACY PRACTICES THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
#3: SAMPLE CONSENT FORM
 #3: SAMPLE CONSENT FORM [Key Element #3: Who is conducting the study] UPMC University of Pittsburgh Medical Center Western Psychiatric Institute and Clinic CONSENT TO ACT AS A PARTICIPANT IN A RESEARCH
#3: SAMPLE CONSENT FORM [Key Element #3: Who is conducting the study] UPMC University of Pittsburgh Medical Center Western Psychiatric Institute and Clinic CONSENT TO ACT AS A PARTICIPANT IN A RESEARCH
Sexual Assault. Sexual battery. Most Frequently Committed & Underreported Violent Crime
 Sexual Assault Columbia University School of Nursing Interpersonal Violence: for Health Care Providers M 6930 Rula Btoush, RN, MSN www. columbia.edu/itc/hs/nursing/m6930 Most Frequently Committed & Underreported
Sexual Assault Columbia University School of Nursing Interpersonal Violence: for Health Care Providers M 6930 Rula Btoush, RN, MSN www. columbia.edu/itc/hs/nursing/m6930 Most Frequently Committed & Underreported
MODEL POLICY REPORTING CHILD ABUSE AND NEGLECT FOR SCHOOL OFFICIALS IN DUPAGE COUNTY
 MODEL POLICY REPORTING CHILD ABUSE AND NEGLECT FOR SCHOOL OFFICIALS IN DUPAGE COUNTY The DuPage County State s Attorney s Office, the DuPage Regional Superintendent of Schools, the School District, the
MODEL POLICY REPORTING CHILD ABUSE AND NEGLECT FOR SCHOOL OFFICIALS IN DUPAGE COUNTY The DuPage County State s Attorney s Office, the DuPage Regional Superintendent of Schools, the School District, the
DISCLAIMER THIS DOCUMENT CONTAINS A SCREENING TOOL. IT IS NOT INTENDED TO BE USED AS A MENTAL HEALTH DIAGNOSTIC TOOL.
 MENTAL HEALTH ASSESSMENT TOOL FORWARD The Mental Health Assessment Tool was developed to bring awareness to behaviors that may potentially disrupt the TB treatment regimen. Substance abuse and mental illness
MENTAL HEALTH ASSESSMENT TOOL FORWARD The Mental Health Assessment Tool was developed to bring awareness to behaviors that may potentially disrupt the TB treatment regimen. Substance abuse and mental illness
Legal Issues for People with HIV
 Legal Issues for People with HIV Duke Legal Project Box 90360 Durham, NC 27708-0360 (919) 613-7169 (888) 600-7274 Duke Legal Project is a clinical legal education program of Duke Law School. Legal Representation
Legal Issues for People with HIV Duke Legal Project Box 90360 Durham, NC 27708-0360 (919) 613-7169 (888) 600-7274 Duke Legal Project is a clinical legal education program of Duke Law School. Legal Representation
CODE OF GEORGIA TITLE 19. DOMESTIC RELATIONS CHAPTER 7. PARENT AND CHILD RELATIONSHIP GENERALLY ARTICLE 1. GENERAL PROVISIONS
 CODE OF GEORGIA TITLE 19. DOMESTIC RELATIONS CHAPTER 7. PARENT AND CHILD RELATIONSHIP GENERALLY ARTICLE 1. GENERAL PROVISIONS 19-7-5 Reporting of child abuse; when mandated or authorized; content of report;
CODE OF GEORGIA TITLE 19. DOMESTIC RELATIONS CHAPTER 7. PARENT AND CHILD RELATIONSHIP GENERALLY ARTICLE 1. GENERAL PROVISIONS 19-7-5 Reporting of child abuse; when mandated or authorized; content of report;
CHAPTER 245C HUMAN SERVICES BACKGROUND STUDIES
 1 MINNESOTA STATUTES 2014 245C.02 CHAPTER 245C HUMAN SERVICES BACKGROUND STUDIES 245C.01 TITLE. 245C.02 DEFINITIONS. 245C.03 BACKGROUND STUDY; INDIVIDUALS TO BE STUDIED. 245C.04 WHEN BACKGROUND STUDY MUST
1 MINNESOTA STATUTES 2014 245C.02 CHAPTER 245C HUMAN SERVICES BACKGROUND STUDIES 245C.01 TITLE. 245C.02 DEFINITIONS. 245C.03 BACKGROUND STUDY; INDIVIDUALS TO BE STUDIED. 245C.04 WHEN BACKGROUND STUDY MUST
Floyd Healthcare Management, Inc. Notice of Privacy Practices
 Floyd Healthcare Management, Inc. Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW
Floyd Healthcare Management, Inc. Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG
 TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
OFFICE OF MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES BULLETIN
 OFFICE OF MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES BULLETIN ISSUE DATE April 15, 2015 EFFECTIVE DATE: April 1, 2015 NUMBER: OMHSAS-15-01 SUBJECT: BY: Community Incident Management & Reporting System
OFFICE OF MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES BULLETIN ISSUE DATE April 15, 2015 EFFECTIVE DATE: April 1, 2015 NUMBER: OMHSAS-15-01 SUBJECT: BY: Community Incident Management & Reporting System
Foley Catheter Placement
 Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
E arly C hildhood E ducation
 Child's Last Name, First Name: Grade: The Seven Hills School E arly C hildhood E ducation State Mandated Documentation Instructions and Forms Dear Parents: Enclosed you will find the paperwork required
Child's Last Name, First Name: Grade: The Seven Hills School E arly C hildhood E ducation State Mandated Documentation Instructions and Forms Dear Parents: Enclosed you will find the paperwork required
Summary Guide for MANDATED REPORTERS in New York State
 Summary Guide for MANDATED REPORTERS in New York State Table of Contents Who Are Mandated Reporters?... 2 When Am I Mandated to Report?... 3 What Is Abuse and Maltreatment?... 4 How Do I Recognize Child
Summary Guide for MANDATED REPORTERS in New York State Table of Contents Who Are Mandated Reporters?... 2 When Am I Mandated to Report?... 3 What Is Abuse and Maltreatment?... 4 How Do I Recognize Child
Epilepsy 101: Getting Started
 American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
Polk Medical Center Notice of Privacy Practices
 Polk Medical Center Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW IT CAREFULLY.
Polk Medical Center Notice of Privacy Practices THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW IT CAREFULLY.
Glossary. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty.
 Glossary amenorrhea - absence or cessation of menstrual periods. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty. A amenorrhea, secondary - due to some physical
Glossary amenorrhea - absence or cessation of menstrual periods. amenorrhea, primary - from the beginning and lifelong; menstruation never begins at puberty. A amenorrhea, secondary - due to some physical
SURGICAL CENTER FOR EXCELLENCE PATIENT INFORMATION
 As a person with pain, you have the right to: SURGICAL CENTER FOR EXCELLENCE PATIENT INFORMATION PAIN CARE BILL OF RIGHTS Have your report of pain taken seriously and to be treated with dignity and respect
As a person with pain, you have the right to: SURGICAL CENTER FOR EXCELLENCE PATIENT INFORMATION PAIN CARE BILL OF RIGHTS Have your report of pain taken seriously and to be treated with dignity and respect
Suicide, PTSD, and Substance Use Among OEF/OIF Veterans Using VA Health Care: Facts and Figures
 Suicide, PTSD, and Substance Use Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy July 18, 2011 Congressional Research Service CRS Report for Congress
Suicide, PTSD, and Substance Use Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy July 18, 2011 Congressional Research Service CRS Report for Congress
SCREENING FOR INTIMATE PARTNER VIOLENCE IN THE PRIMARY CARE SETTING
 SCREENING FOR INTIMATE PARTNER VIOLENCE IN THE PRIMARY CARE SETTING Partner violence can affect one third of the patients cared for in the primary care setting. The primary care setting offers an opportunity
SCREENING FOR INTIMATE PARTNER VIOLENCE IN THE PRIMARY CARE SETTING Partner violence can affect one third of the patients cared for in the primary care setting. The primary care setting offers an opportunity
IOWA DEPARTMENT OF JUSTICE ATTORNEY GENERAL'S OFFICE CRIME VICTIM ASSISTANCE DIVISION SEXUAL ABUSE EXAMINATION PAYMENT PROGRAM
 IOWA DEPARTMENT OF JUSTICE ATTORNEY GENERAL'S OFFICE CRIME VICTIM ASSISTANCE DIVISION SEXUAL ABUSE EXAMINATION PAYMENT PROGRAM The Attorney General's Crime Victim Assistance Division administers the Sexual
IOWA DEPARTMENT OF JUSTICE ATTORNEY GENERAL'S OFFICE CRIME VICTIM ASSISTANCE DIVISION SEXUAL ABUSE EXAMINATION PAYMENT PROGRAM The Attorney General's Crime Victim Assistance Division administers the Sexual
Additional Questions to Intake Interview Questions
 Additional Questions to Intake Interview Questions Contents ADDITIONAL QUESTIONS TO INTAKE INTERVIEW QUESTIONS... 3 Neglect... 3 Abandonment... 3 Clothing... 3 Drug Labs... 3 Food... 4 Home Environment...
Additional Questions to Intake Interview Questions Contents ADDITIONAL QUESTIONS TO INTAKE INTERVIEW QUESTIONS... 3 Neglect... 3 Abandonment... 3 Clothing... 3 Drug Labs... 3 Food... 4 Home Environment...
SUSPECTED CHILD ABUSE AND NEGLECT
 13.1 SUSPECTED CHILD ABUSE AND NEGLECT This summary is intended to provide only minimal information. For detailed procedures and information see the Family Violence Policy and Procedures; Suspected Child
13.1 SUSPECTED CHILD ABUSE AND NEGLECT This summary is intended to provide only minimal information. For detailed procedures and information see the Family Violence Policy and Procedures; Suspected Child
DARKNESS to LIGHT S 5 STEPS TO PROTECTING OUR CHILDREN. A guide for responsible adults
 DARKNESS to LIGHT S 5 STEPS TO PROTECTING OUR CHILDREN A guide for responsible adults DARKNESS TO LIGHT We are a national nonprofit organization that seeks to empower adults to prevent child sexual abuse.
DARKNESS to LIGHT S 5 STEPS TO PROTECTING OUR CHILDREN A guide for responsible adults DARKNESS TO LIGHT We are a national nonprofit organization that seeks to empower adults to prevent child sexual abuse.
ILLINOIS DEPARTMENT OF CENTRAL MANAGEMENT SERVICES CLASS SPECIFICATION
 ILLINOIS DEPARTMENT OF CENTRAL MANAGEMENT SERVICES CLASS SPECIFICATION CLASS TITLE POSITION CODE EFFECTIVE CHILD PROTECTION ASSOCIATE SPECIALIST 07162 09-01-2007 CHILD PROTECTION SPECIALIST 07163 09-01-2007
ILLINOIS DEPARTMENT OF CENTRAL MANAGEMENT SERVICES CLASS SPECIFICATION CLASS TITLE POSITION CODE EFFECTIVE CHILD PROTECTION ASSOCIATE SPECIALIST 07162 09-01-2007 CHILD PROTECTION SPECIALIST 07163 09-01-2007
2013 Key Survey Findings
 2013 Key Survey Findings National Multi-Site Survey of Children s Advocacy Centers The Midwest Regional Children s Advocacy Center is funded through a grant from the Department of Justice, Office of Juvenile
2013 Key Survey Findings National Multi-Site Survey of Children s Advocacy Centers The Midwest Regional Children s Advocacy Center is funded through a grant from the Department of Justice, Office of Juvenile
ICD-10-CM Official Guidelines for Coding and Reporting
 2013 Narrative changes appear in bold text Items underlined have been moved within the guidelines since the 2012 version Italics are used to indicate revisions to heading changes The Centers for Medicare
2013 Narrative changes appear in bold text Items underlined have been moved within the guidelines since the 2012 version Italics are used to indicate revisions to heading changes The Centers for Medicare
National Child Protection Alert System Management Policy
 National Child Protection Alert System Management Policy 1. Purpose To ensure that safe and consistent practices are followed by West Coast District Health Board (WCDHB) staff when placing, responding
National Child Protection Alert System Management Policy 1. Purpose To ensure that safe and consistent practices are followed by West Coast District Health Board (WCDHB) staff when placing, responding
New Brunswick Health Indicators
 New Brunswick Health Indicators Issue 8, July 2013 A population health bulletin published by the Office of the Chief Medical Officer of Health Youth Sexual Health Sexual health is an important aspect of
New Brunswick Health Indicators Issue 8, July 2013 A population health bulletin published by the Office of the Chief Medical Officer of Health Youth Sexual Health Sexual health is an important aspect of
WHAT HAPPENS NEXT? A guide to the NORTH DAKOTA CHILD PROTECTION SERVICES. This guide is made available by
 WHAT HAPPENS NEXT? A guide to the NORTH DAKOTA CHILD PROTECTION SERVICES This guide is made available by NORTH DAKOTA CHILD PROTECTION SERVICES CHILDREN AND FAMILY SERVICES North Dakota Department of Human
WHAT HAPPENS NEXT? A guide to the NORTH DAKOTA CHILD PROTECTION SERVICES This guide is made available by NORTH DAKOTA CHILD PROTECTION SERVICES CHILDREN AND FAMILY SERVICES North Dakota Department of Human
Illinois DCFS Flowchart How to Report Suspected Child Abuse or Neglect
 Illinois DCFS Flowchart How to Report Suspected Child Abuse or Neglect Organize the Information for your report. Gather ONLY the information you need to make the report of abuse/neglect to the Hotline.
Illinois DCFS Flowchart How to Report Suspected Child Abuse or Neglect Organize the Information for your report. Gather ONLY the information you need to make the report of abuse/neglect to the Hotline.
Debbie Beach, LCSW Debbiebeach4@gmail.com 202-415-6242
 Debbie Beach, LCSW Debbiebeach4@gmail.com 202-415-6242 COLLABORATIVE ENGAGEMENT AGREEMENT DIVORCE COACH Debbie Beach, LCSW 405 N. Washington St, #104 Falls Church, VA 22046 Date: Name of party: Dear Party:
Debbie Beach, LCSW Debbiebeach4@gmail.com 202-415-6242 COLLABORATIVE ENGAGEMENT AGREEMENT DIVORCE COACH Debbie Beach, LCSW 405 N. Washington St, #104 Falls Church, VA 22046 Date: Name of party: Dear Party:
CHILD PROTECTION POLICY
 THE BARCLAY SCHOOL CHILD PROTECTION POLICY Senior Designated Person : Nat Baker (Assistant Head) Deputy Designated Senior Person: Jill Marshall (Pastoral Support Leader) Chair of Governors: Andrew Boakes
THE BARCLAY SCHOOL CHILD PROTECTION POLICY Senior Designated Person : Nat Baker (Assistant Head) Deputy Designated Senior Person: Jill Marshall (Pastoral Support Leader) Chair of Governors: Andrew Boakes
Specimen collection and transport for Chlamydia trachomatis and Neisseria gonorrhoeae testing
 Specimen collection and transport for Chlamydia trachomatis and Neisseria gonorrhoeae testing Overview Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) infections are two of the most common sexually
Specimen collection and transport for Chlamydia trachomatis and Neisseria gonorrhoeae testing Overview Chlamydia trachomatis (CT) and Neisseria gonorrhoeae (NG) infections are two of the most common sexually
Working Together HEALTH SERVICES FOR CHILDREN IN FOSTER CARE
 Chapter Eight Maintaining Health Records Maintaining the health records of children in foster care is critical to providing and monitoring health care on an ongoing basis. When health records are maintained
Chapter Eight Maintaining Health Records Maintaining the health records of children in foster care is critical to providing and monitoring health care on an ongoing basis. When health records are maintained
Antenatal perineal massage. Information for women
 Antenatal perineal massage Information for women Research has shown that antenatal perineal massage from approximately 35 weeks gestation reduces the likelihood of perineal trauma that needs stitching.
Antenatal perineal massage Information for women Research has shown that antenatal perineal massage from approximately 35 weeks gestation reduces the likelihood of perineal trauma that needs stitching.
Parent s Guide. to Child Protective Services (CPS) Children s. Administration. Division. of Children. and Family. Services
 Parent s Guide to Child Protective Services (CPS) Children s Administration Division of Children and Family Services Table Of Contents Topic Page What Is Child Protective Services (CPS)?... What Is Child
Parent s Guide to Child Protective Services (CPS) Children s Administration Division of Children and Family Services Table Of Contents Topic Page What Is Child Protective Services (CPS)?... What Is Child
DOMESTIC VIOLENCE AND CHILDREN. A Children s Health Fund Report. January, 2001
 DOMESTIC VIOLENCE AND CHILDREN A Children s Health Fund Report January, 2001 Peter A. Sherman, MD Division of Community Pediatrics The Children s Hospital at Montefiore -1- Introduction Domestic violence
DOMESTIC VIOLENCE AND CHILDREN A Children s Health Fund Report January, 2001 Peter A. Sherman, MD Division of Community Pediatrics The Children s Hospital at Montefiore -1- Introduction Domestic violence
FLORIDA VIRTUAL SCHOOL MISCONDUCT AND ABUSE REPORTING POLICY
 FLORIDA VIRTUAL SCHOOL MISCONDUCT AND ABUSE REPORTING POLICY Florida legislation mandates that all school staff know the signs and symptoms of abuse, how to report it, and how to follow-up with a child
FLORIDA VIRTUAL SCHOOL MISCONDUCT AND ABUSE REPORTING POLICY Florida legislation mandates that all school staff know the signs and symptoms of abuse, how to report it, and how to follow-up with a child
NOTICE OF PRIVACY PRACTICES. The University of North Carolina at Chapel Hill. UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates
 NOTICE OF PRIVACY PRACTICES The University of North Carolina at Chapel Hill UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU
NOTICE OF PRIVACY PRACTICES The University of North Carolina at Chapel Hill UNC-CH School of Nursing Faculty Practice Carolina Nursing Associates THIS NOTICE DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU
Acute pelvic inflammatory disease: tests and treatment
 Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
PARTNERS IN PEDIATRIC CARE. Intake and History for Mental Health Referral
 PARTNERS IN PEDIATRIC CARE Intake and History for Mental Health Referral This form is designed to give you an opportunity to provide us with background information that will help us help you. Please read
PARTNERS IN PEDIATRIC CARE Intake and History for Mental Health Referral This form is designed to give you an opportunity to provide us with background information that will help us help you. Please read
Oral Health Coding Fact Sheet for Primary Care Physicians
 2015 Oral Health Coding Fact Sheet for Primary Care Physicians CPT Codes: Current Procedural Terminology (CPT) codes are developed and maintained by the American Medical Association. The codes consist
2015 Oral Health Coding Fact Sheet for Primary Care Physicians CPT Codes: Current Procedural Terminology (CPT) codes are developed and maintained by the American Medical Association. The codes consist
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
Diseases that can be spread during sex
 Diseases that can be spread during sex Did you know... over 65 million people in the United States have a chronic, incurable sexually transmitted disease (STD)? and that every year another 19 million persons
Diseases that can be spread during sex Did you know... over 65 million people in the United States have a chronic, incurable sexually transmitted disease (STD)? and that every year another 19 million persons
The University of Texas Southwestern Medical Center at Dallas Retina Foundation of the Southwest CONSENT TO PARTICIPATE IN RESEARCH
 The University of Texas Southwestern Medical Center at Dallas Retina Foundation of the Southwest CONSENT TO PARTICIPATE IN RESEARCH Title of Research: Funding Agency/Sponsor: Study Doctors: Research Personnel:
The University of Texas Southwestern Medical Center at Dallas Retina Foundation of the Southwest CONSENT TO PARTICIPATE IN RESEARCH Title of Research: Funding Agency/Sponsor: Study Doctors: Research Personnel:
STATE OF OHIO. DEPARTMENT OF REHABILITATION RELATED ACA STANDARDS: EFFECTIVE DATE: AND CORRECTION February 19, 2011 I. AUTHORITY
 STATE OF OHIO SUBJECT: PAGE 1 OF 7. Specialized Assessments and Screenings NUMBER: 67-MNH-16 RULE/CODE REFERENCE: SUPERSEDES: AR 5120-11-03, 07, 21 67-MNH-16 dated 01/13/10 ORC 5120.031; 5120.032; 5120.033
STATE OF OHIO SUBJECT: PAGE 1 OF 7. Specialized Assessments and Screenings NUMBER: 67-MNH-16 RULE/CODE REFERENCE: SUPERSEDES: AR 5120-11-03, 07, 21 67-MNH-16 dated 01/13/10 ORC 5120.031; 5120.032; 5120.033
CHAPTER 2015-177. Committee Substitute for Committee Substitute for House Bill No. 1055
 CHAPTER 2015-177 Committee Substitute for Committee Substitute for House Bill No. 1055 An act relating to child protection; amending s. 39.2015, F.S.; providing requirements for the representation of Children
CHAPTER 2015-177 Committee Substitute for Committee Substitute for House Bill No. 1055 An act relating to child protection; amending s. 39.2015, F.S.; providing requirements for the representation of Children
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
HIPAA Notice of Privacy Practices
 This notice describes how medical information about you may be used and disclosed and how you can get access to this information. Please review this notice carefully. This practice is required by law to
This notice describes how medical information about you may be used and disclosed and how you can get access to this information. Please review this notice carefully. This practice is required by law to
CURRENT ISSUES IN CHILD MALTREATMENT
 CURRENT ISSUES IN CHILD MALTREATMENT MULTIDISCIPLINARY PERSPECTIVES & 5 th ANNUAL CANADIAN SYMPOSIUM ON ADVANCED PRACTICES IN CHILD MALTREATMENT PEDIATRICS Nov. 17, 18 & 19, 2014 MONTREAL UNIVERSITY CLUB
CURRENT ISSUES IN CHILD MALTREATMENT MULTIDISCIPLINARY PERSPECTIVES & 5 th ANNUAL CANADIAN SYMPOSIUM ON ADVANCED PRACTICES IN CHILD MALTREATMENT PEDIATRICS Nov. 17, 18 & 19, 2014 MONTREAL UNIVERSITY CLUB
Washington State Mandated Reporter v2.1 (Child Abuse and Neglect)
 Washington State Mandated Reporter v2.1 (Child Abuse and Neglect) Identification and Management of Concerns at Seattle Children s Click to navigate through this course. During this course you will review:
Washington State Mandated Reporter v2.1 (Child Abuse and Neglect) Identification and Management of Concerns at Seattle Children s Click to navigate through this course. During this course you will review:
Medical Records Analysis
 Medical Records Analysis Karen A. Mulroy, Partner Evans & Dixon, L.L.C. The analysis of medical legal issues posed in any case can be complicated, requiring some close reading and detective work to both
Medical Records Analysis Karen A. Mulroy, Partner Evans & Dixon, L.L.C. The analysis of medical legal issues posed in any case can be complicated, requiring some close reading and detective work to both
Child Protection. Be vigilant, report child abuse
 Child Protection Be vigilant, report child abuse Introduction All children have the right to live free of abuse. Most children grow up in families where they are safe and secure. Others may be abused
Child Protection Be vigilant, report child abuse Introduction All children have the right to live free of abuse. Most children grow up in families where they are safe and secure. Others may be abused
Health Science Career Field Allied Health and Nursing Pathway (JM)
 Health Science Career Field Allied Health and Nursing Pathway (JM) ODE Courses Possible Sinclair Courses CTAG Courses for approved programs Health Science and Technology 1 st course in the Career Field
Health Science Career Field Allied Health and Nursing Pathway (JM) ODE Courses Possible Sinclair Courses CTAG Courses for approved programs Health Science and Technology 1 st course in the Career Field
SCREENING FOR SEXUALLY TRANSMITTED INFECTIONS
 SCREENING FOR SEXUALLY TRANSMITTED INFECTIONS Take history:- History of presenting problem Full sexual history (refer to guideline on sexual history taking) Relevant past medical history, including previous
SCREENING FOR SEXUALLY TRANSMITTED INFECTIONS Take history:- History of presenting problem Full sexual history (refer to guideline on sexual history taking) Relevant past medical history, including previous
Pediatric and Adolescent Medical Record Review Tool
 Pediatric and Adolescent Medical Record Review Tool Primary Care Provider: Member Name: DOB: Provider Name: Provider ID #: Product: Date of Review: Initials of Reviewer: The Medical Record contains the
Pediatric and Adolescent Medical Record Review Tool Primary Care Provider: Member Name: DOB: Provider Name: Provider ID #: Product: Date of Review: Initials of Reviewer: The Medical Record contains the
Paediatrica Indonesiana. Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation
 Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Paediatrica Indonesiana VOLUME 51 November NUMBER 6 Original Article Limitations of the Indonesian Pediatric Tuberculosis Scoring System in the context of child contact investigation Rina Triasih 1,2,
Garland s Christian Counseling Center
 Garland s Christian Counseling Center : PERSONAL DATA Name: Email: Home Phone: Address: Cell Phone: Work Phone: (Street, City, Zip Code) DL #, ST & Exp : SS#: DOB: Sex: Please circle where we may leave
Garland s Christian Counseling Center : PERSONAL DATA Name: Email: Home Phone: Address: Cell Phone: Work Phone: (Street, City, Zip Code) DL #, ST & Exp : SS#: DOB: Sex: Please circle where we may leave
Providing support to vulnerable children and families. An information sharing guide for registered school teachers and principals in Victoria
 Providing support to vulnerable children and families An information sharing guide for registered school teachers and principals in Victoria Service Coordination Tool Templates 2006 reference guide Providing
Providing support to vulnerable children and families An information sharing guide for registered school teachers and principals in Victoria Service Coordination Tool Templates 2006 reference guide Providing
