PERIODONTAL FLAPS DR JEBIN,MDS.,D.ICOI
|
|
|
- Betty Richardson
- 9 years ago
- Views:
Transcription
1 PERIODONTAL FLAPS DR JEBIN,MDS.,D.ICOI
2 DEF: A periodontal flap is a section of gingiva and/or mucosa surgically separated from the underlying tissues to provide visibility and access to the bone and root surface.
3 INDICATIONS: Irregular bony contours Deep craters Pockets on teeth in which a complete removal of root irritants is not clinically possible Grade II or III furcation involvement Root resection / hemisection Intrabony pockets on distal areas of last molars Persistent inflammation in areas with moderate to deep pockets. CONTRAINDICATIONS: Uncontrolled medical conditions such as unstable angina uncontrolled diabetes uncontrolled hypertension myocardial infarction / stroke within 6 months Poor plaque control High caries rate Unrealistic patient expectations or desires
4 CLASSIFICATION OF FLAPS Classified based on: Bone exposure after flap reflection Full thickness (mucoperiosteal) Partial thickness (mucosal) Placement of the flap after surgery Nondisplaced flaps Displaced flaps Management of the papilla Conventional flaps Papilla preservation flaps
5 BASED ON BONE EXPOSURE AFTER REFLECTION FULL THICKNESS FLAP Periosteum is reflected to expose the underlying bone. Indicated in resective osseous surgery. Contraindications : Area where treatment for osseous defect with mucogingival problem is not required. Thin periodontal tissue with probable osseous dehiscence and osseous fenestration. Area where alveolar bone is thin.
6 PARTIAL THICKNESS FLAP Split thickness flap. Periosteum covers the bone. Indicated when the flap has to be positioned apically. When the operator does not desire to expose the bone.
7 BASED ON FLAP PLACEMENT AFTER SURGERY Non displaced flaps: When the flap is returned and sutured in its original position. Displaced flaps: When the flap is placed apically, coronally or laterally to their original position
8 DESIGN OF THE FLAP Split the papilla (conventional flap) or Preserve it (papilla preservation flap).
9 BASED ON MANAGEMENT OF THE PAPILLA CONVENTIONAL FLAP The interdental papilla is split beneath the contact point of the two approximating teeth to allow reflection of buccal and lingual flaps.
10 The conventional flap is used when The interdental spaces are too narrow When the flap is to be displaced. Conventional flaps include the The Modified Widman flap, The undisplaced flap, The apically displaced flap, and The flap for regenerative procedures.
11 PAPILLA PRESERVATION FLAP The papilla preservation flap incorporates the entire papilla in one of the flaps
12 Two basic flap designs, those with and those without vertical releasing incisions: Envelope Flap: A flap that is released in a linear fashion at the gingival margin but has no vertical releasing incision(s). Pedicle Flap: If two vertical releasing incisions are included in the flap design. Triangular Flap: If one vertical releasing incision is included in the flap design. Envelope Flap Pedicle Flap Triangular Flap
13 The major blood supply to a flap is at its base and travels in an apical to coronal direction. Recommended flap length (height) to base ratio should be no greater than 2:1
14 INCISIONS Horizontal incisions. Vertical incisions.
15 HORIZONTAL INCISIONS Horizontal incisions are directed along the margin of the gingiva in a mesial or a distal direction. Two types of horizontal incisions have been recommended: A) The internal bevel incision, which starts at a distance from the gingival margin and is aimed at the bone crest, and B) The crevicular incision, which starts at the bottom of the pocket and is directed to the bone margin. C) In addition, the interdental incision is performed after the flap is elevated.
16 INTERNAL BEVEL INCISION 1st incision 1º incision Reverse bevel incision 11 or 15 surgical scalpel used Starts at a distance from the gingival margin aiming at the bone crest.
17 Removes pocket lining. Produces a sharp thin flap margin. Starts from a designated area on the gingiva and is directed to an area at or near the crest of the bone.
18 Various locations and angles of internal bevel incision
19 CREVICULAR INCISION Also known as second incision Made from the base of the pocket to the crest of the bone This incision, together with the initial reverse bevel incision, forms a V-shaped wedge ending at or near the crest of bone
20 PROCEDURE: 1) Beak-shaped #12D blade is used 2) Periosteal elevator inserted into the initial internal bevel incision 3) Flap separated from the bone
21 INTERDENTAL INCISION Also known as third incision To separate the collar of gingiva that is left around the tooth Incision made facially lingually & interdentally connecting the 2 segments. Orbans knife is used
22 VERTICAL INCISIONS Can be used on one or both ends of the horizontal incision Must extend beyond the mucogingival line, reaching the alveolar mucosa, to allow for the release of the flap to be displaced Vertical incisions in the lingual and palatal areas are avoided
23 This incision should be made at the line angles to prevent splitting of a papilla or incising directly over a radicular surface.
24 ELEVATION OF THE FLAP Blunt dissection with periosteal elevator For reflection of full thickness flap
25 Sharp dissection with surgical scalpel (#11 or #15) For reflection of partial thickness flap
26 A flap that includes only gingival tissue is referred to as a GINGIVAL FLAP. A flap that extends beyond the mucogingival junction to include alveolar mucosa, is a MUCOGINGIVAL FLAP.
27 FLAP RETRACTION Retraction should be passive without any tension. Force should not be necessary to keep the flap retracted. The edge of the retractor always be kept on bone.
28 Continuous flap retraction for long periods is also is not advised. Such a practice will desiccate the soft tissue and bone causing a delay in wound healing. When the flap is retracted, the surgical assistant should frequently irrigate the surgical field with sterile saline, to keep the tissues moistened, to reduce contamination, and to improve visibility.
29 OPEN FLAP DEBRIDEMENT provide access to root surfaces and marginal alveolar bone.
30 FLAP POSITIONING surgical flaps may be repositioned, apically positioned, coronally positioned or laterally positioned An apically positioned flap is one that is apically displaced from its original position to the level of the alveolar crest or about 1mm coronal to the crest. The coronally positioned flap is advanced coronal to its original position.
31 FLAP TECHNIQES FOR POCKET THERAPY Increase accessibility to root deposits Eliminate or reduce pocket depth by resection of the pocket wall Expose the area to perform regenerative methods FLAP TECHNIQUES The modified widman flap The undisplaced flap The palatal flap The apically displaced flap Flaps for regenerative surgery The papilla preservation flap Conventional flap for regenerative surgery Distal molar surgery
32 THE ORIGINAL WIDMAN FLAP By Leonard Widman (1918) Widman described a mucoperiosteal flap designed to remove the pocket epithelium and the inflamed connective tissue, there by facilitating optimal cleaning of the root surfaces. ADVANTAGES: Less discomfort for the patient, since healing occurred by primary intention. It was possible to reestablish a proper contour of the alveolar bone in sites with angular bony defects.
33 STEP 1 STEP 2 STEP 3 STEP 4
34 THE MODIFIED WIDMAN F LAP Ramfjord and Nissle (1974) The modified Widman flap. planing with direct vision. The main goals of the procedure include optimum mechanical sub gingival root
35 INDICATIONS: Especially effective with pocket depths of 5 7 mm. CONTRAINDICATIONS: Lack of or very thin and narrow attached gingiva can render the technique difficult, because a narrow band of attached gingiva does not permit the initial scalloped incision (internal gingivectomy).. osseous surgical procedure
36 ADVANTAGES: Root cleaning with direct vision. Tissue friendly. Healing by primary intention. Minimal crestal bone resorption. Lack of post operative discomfort. STEP 1 STEP 2
37 STEP 3 STEP 4 STEP 5 STEP 6
38 THE UNDISPLACED FLAP Currently, it is the most commonly performed type of periodontal surgery. It differs from the modified Widman flap in that the soft tissue pocket wall is removed with the initial incision; thus it may be considered an internal bevel gingivectomy.
39 Pre-operative Facial & Lingual Views Internal Bevel Incisions Facial & Palatal Aspects Flap Elevated Showing Osseous Defects
40 Osseous surgery has been performed Flaps Placed In Their Original Site And Sutured Post Operative Results
41 PARTIAL THICKNESS PALATAL FLAP SURGERY Developed by Staffileno and improved by Corn et al. elimination of periodontal pockets where thick palatal tissues occur. ADVANTAGES: Flap thickness may be adjusted. Palatal flap may be adapted to the proper position. Better postoperative gingival morphology is possible with a thin flap design. Treatments may be combined (osseous resection and wedge procedure). Rapid healing. Easy management of palatal tissue. Minimal damage to palatal tissue.
42 Outline of primary incision
43 . Primary incision Thin primary flap preparation.
44 . Secondary incision Secondary flap removal Suture
45 THE APICALLY DISPLACED FLAP It can be used for both pocket eradication as well as widening the zone of attached gingiva. It can be a full thickness (mucoperiosteal) or a split thickness (mucosal) flap. ADVANTAGES: Eliminates periodontal pocket. Preserves attached gingiva and increases its width. Establishes gingival morphology facilitating good hygiene. Ensures healthy root surface necessary for the biologic width on alveolar margin and lengthened clinical crown.
46 DISADVANTAGES: May cause esthetic problems due to root exposure. May cause attachment loss due to surgery. May cause hypersensitivity. May increase the risk of root caries. Unsuitable for treatment of deep periodontal pockets. Possibility of exposure of furcations and roots, which complicates post operative supragingival plaque control. CONTRAINDICATIONS: Periodontal pockets in severe periodontal disease. Periodontal pockets in areas where esthetics is critical. Deep intrabony defects. Patient at high risk for caries. Severe hypersensitivity. Tooth with marked mobility and severe attachment loss. Tooth with extremely unfavourable clinical crown / Root ratio.
47 Facial And Lingual Preoperative Views Facial And Lingual Flaps Elevated After Debridement Of The Areas
48 Sutures In Place Healing After 1 Week Healing After 2 Months Preoperative Postoperative
49 PRE-TREATMENT BEFORE OSSEOUS RESECTION AFTER OSSEOUS RESECTION FLAP APICALLY POSITIONED AND SUTURED POST-TREATMENT
50 FLAPS FOR REGENERATIVE SURGERY Two flap designs are available for regenerative surgery: The papilla preservation flap & The conventional flap with only crevicular incisions. Adequate interdental space Interdental space is very narrow Papilla preservation flap Conventional flap with only crevicular incisions
51 THE PAPILLA PRESERVATION FLAP Entire papilla is incorporated into one of the flaps. INDICATIONS: Where esthetics is of concern. Where bone regeneration techniques are attempted.
52
53 CONVENTIONAL FLAP FOR REGENERATIVE SURGERY In the conventional flap operation, the incisions for the facial and the lingual or palatal flap reach the tip of the interdental papilla, thereby splitting the papilla into a facial half and a lingual or palatal half. INDICATIONS: When the interdental areas are too narrow to permit the preservation of flap. When there is a need for displasing flaps.
54 DISTAL MOLAR SURGERY Treatment of periodontal pockets on the distal surface of terminal molars is often complicated by the presence of bulbous fibrous tissue over the maxillary tuberosity or prominent retromolar pads in the mandible. Operations for this purpose were described by Robinson and Braden Impaction Of A Third Molar Distal To A Second Molar Little Or No Bone Distal To The Second Molar. Often Leads To A Vertical Osseous Defect Distal To The Second Molar.
55 A typical incision design for a surgical procedure distal to the maxillary second molar.
56 Incision designs for surgical procedures distal to the mandibular second molar. The incision should follow the areas of greatest attached gingiva and underlying bone.
57 TRIANGULAR DISTAL WEDGE: Triangular wedge incisions are placed creating the apex of the triangle close to the hamular notch and the base of the triangle next to the distal surface of the terminal tooth.
58 LINEAR DISTAL WEDGE: The linear distal wedge incorporates two parallel incisions over the crest of the tuberosity that extend from the proximal surface of the terminal molar to the hamular notch area. The distance between the two linear incisions is determined by the thickness of the tissues
59 DISTAL POCKET ERADICATION PROCEDURE WITH THE INCISION DISTAL TO THE MOLAR SCALLOPED INCISION AROUND THE REMAINING TEETH FLAP REFLECTED AND THINNED AROUND THE DISTAL INCISION
60 FLAP IN POSITION BEFORE SUTURING. IT SHOULD BE CLOSELY APPROXIMATED FLAP SUTURED BOTH DISTALLY AND OVER THE REMAINING SURGICAL AREA
61
62
63 HEALING AFTER FLAP SURGERY Immediately after suturing (0 to 24 hours), established by a blood clot, which consists of a fibrin reticulum with many polymorphonuclear leukocytes, erythrocytes, debris of injured cells, and capillaries at the edge of the wound. One to 3 days after flap surgery, the space between the flap and the tooth or bone is thinner, and epithelial cells migrate over the border of the flap One week after surgery The blood clot is replaced by granulation tissue derived from the gingival connective tissue, the bone marrow, and the periodontal ligament.
64 Two weeks after surgery, collagen fibers begin to appear parallel to the tooth surface. Union of the flap to the tooth is still weak, owing to the presence of immature collagen fibers, although the clinical aspect may be almost normal. One month after surgery, a fully epithelialized gingival crevice with a well defined epithelial attachment is present. There is a beginning functional arrangement of the supracrestal fibers.
65 THANK U
Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF)
 Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF) 309 Of the numerous periodontal surgical techniques, the oft-modified Widman flap ( Modified Widman Flap, MWF) remains the standard
Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF) 309 Of the numerous periodontal surgical techniques, the oft-modified Widman flap ( Modified Widman Flap, MWF) remains the standard
Periodontal surgery report for crown lengthening of tooth number 24,25
 411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
SURGICAL EXTRACTIONS: TECHNIQUE AND CAUTIONS By Tony M. Woodward, DVM, AVDC
 SURGICAL EXTRACTIONS: TECHNIQUE AND CAUTIONS By Tony M. Woodward, DVM, AVDC We continue describing the five basic dental services that all general practitioners should be able to provide for their patients.
SURGICAL EXTRACTIONS: TECHNIQUE AND CAUTIONS By Tony M. Woodward, DVM, AVDC We continue describing the five basic dental services that all general practitioners should be able to provide for their patients.
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Papilla Preservation Flap : Revisited
 REVIEW ARTICLE Papilla Preservation Flap : Revisited Lisa N. Chacko*, Sathish Abraham**, Nilima Landge***, Fareedi Mukram Ali**** Abstract An ideal periodontal therapy should establish a state of periodontal
REVIEW ARTICLE Papilla Preservation Flap : Revisited Lisa N. Chacko*, Sathish Abraham**, Nilima Landge***, Fareedi Mukram Ali**** Abstract An ideal periodontal therapy should establish a state of periodontal
Calibrated Periodontal Probes and Basic Probing Technique
 Module 11 Calibrated Periodontal Probes and Basic Probing Technique MODULE OVERVIEW This module presents the (1) design characteristics of calibrated periodontal probes and (2) step-by-step instructions
Module 11 Calibrated Periodontal Probes and Basic Probing Technique MODULE OVERVIEW This module presents the (1) design characteristics of calibrated periodontal probes and (2) step-by-step instructions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION
 MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D.
 Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D. 1 Potential periodontal problems Before Orthodontic Treatment During Orthodontic Treatment After Orthodontic
Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D. 1 Potential periodontal problems Before Orthodontic Treatment During Orthodontic Treatment After Orthodontic
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery. Consequences of tooth loss.
 Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Periodontal plastic surgery
 Periodontology 2000, Vol. 68, 2015, 333 368 2015 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Periodontal plastic surgery GIOVANNI
Periodontology 2000, Vol. 68, 2015, 333 368 2015 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Periodontal plastic surgery GIOVANNI
porcelain fused to metal crown
 Lectur.5 Dr.Adel F.Ibraheem porcelain fused to metal crown the most widely used fixed restoration,it is full metal crown having facial surface (or all surfaces) covered by ceramic material. It consist
Lectur.5 Dr.Adel F.Ibraheem porcelain fused to metal crown the most widely used fixed restoration,it is full metal crown having facial surface (or all surfaces) covered by ceramic material. It consist
The gingival flap technique,
 Ban0108_034-041.qxd 2/1/08 4:47 PM Page 34 Creating effective dental flaps Practitioners can use this surgery to visualize and treat dental problems. By Beatriz Woodall, DVM Contributing Author The gingival
Ban0108_034-041.qxd 2/1/08 4:47 PM Page 34 Creating effective dental flaps Practitioners can use this surgery to visualize and treat dental problems. By Beatriz Woodall, DVM Contributing Author The gingival
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 375 Use of a Combination Epithelized- Subepithelial Connective Tissue Graft for Closure and Soft Tissue Augmentation of an Extraction Site
The International Journal of Periodontics & Restorative Dentistry 375 Use of a Combination Epithelized- Subepithelial Connective Tissue Graft for Closure and Soft Tissue Augmentation of an Extraction Site
TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS.
 TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS. The attached is a list of dental procedures for which benefits are payable under
TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS. The attached is a list of dental procedures for which benefits are payable under
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Dentistry has undergone a significant evolution in the last 2 decades.
 Esthetic Crown Lengthening for Maxillary Anterior Teeth CE 5 Abstract: In the maxillary anterior region, the gingival labial margin position is an important parameter in the achievement of an ideal smile.
Esthetic Crown Lengthening for Maxillary Anterior Teeth CE 5 Abstract: In the maxillary anterior region, the gingival labial margin position is an important parameter in the achievement of an ideal smile.
SURGICAL MANUAL. Step By Step Techniques
 SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
Full Crown Module: Learner Level 1
 Full Crown Module Restoration / Tooth # Full Gold Crown (FGC) / 30 Extensions: Porcelain Fused to Metal (PFM) / 12 All Ceramic / 8 Learner Level 1 Mastery of Tooth Preparation Estimated Set Up Time: 30
Full Crown Module Restoration / Tooth # Full Gold Crown (FGC) / 30 Extensions: Porcelain Fused to Metal (PFM) / 12 All Ceramic / 8 Learner Level 1 Mastery of Tooth Preparation Estimated Set Up Time: 30
Prosthodontist s Perspective
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Single anterior tooth replacement: clinical approaches
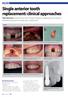 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
General Technique of Third Molar Removal
 Oral Maxillofacial Surg Clin N Am 19 (2007) 23 43 General Technique of Third Molar Removal Sam E. Farish, DMD a,b, *, Gary F. Bouloux, MD, BDS, MDSc, FRACDS, FRACDS(OMS) b a Division of Oral and Maxillofacial
Oral Maxillofacial Surg Clin N Am 19 (2007) 23 43 General Technique of Third Molar Removal Sam E. Farish, DMD a,b, *, Gary F. Bouloux, MD, BDS, MDSc, FRACDS, FRACDS(OMS) b a Division of Oral and Maxillofacial
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS
 CONTINUING EDUCATION X X REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS Nicolas Elian, DDS* Ziad N. Jalbout, DDS Sang-Choon Cho, DDS Stuart
CONTINUING EDUCATION X X REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS Nicolas Elian, DDS* Ziad N. Jalbout, DDS Sang-Choon Cho, DDS Stuart
DEVELOPMENT AND GROWTH OF THE MANDIBLE
 2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
Tissue alterations at implant-supported single-tooth replacements: a 1-year prospective clinical study
 Giuseppe Cardaropoli Ulf Lekholm Jan L. Wennström Tissue alterations at implant-supported single-tooth res: a 1-year prospective clinical study Authors affiliations: Giuseppe Cardaropoli, Jan L. Wennström,
Giuseppe Cardaropoli Ulf Lekholm Jan L. Wennström Tissue alterations at implant-supported single-tooth res: a 1-year prospective clinical study Authors affiliations: Giuseppe Cardaropoli, Jan L. Wennström,
Denture Trouble Shooting Guide
 Denture Trouble Shooting Guide Comfort Sore spot in vestibuleupper or lower denture 1. Overextended borders 2. Rough spot in base 1. Shorten borders and polish. 2. Refinish borders. Sore spot in upper
Denture Trouble Shooting Guide Comfort Sore spot in vestibuleupper or lower denture 1. Overextended borders 2. Rough spot in base 1. Shorten borders and polish. 2. Refinish borders. Sore spot in upper
Failures in periodontal therapy
 Bangladesh Journal of Medical Science Vol.09 No.4 Jul 10 Review article Failures in periodontal therapy Abstract KD Jithendra 1, Bansali A 2, Ramachandra SS 3 Studies have shown that modern periodontal
Bangladesh Journal of Medical Science Vol.09 No.4 Jul 10 Review article Failures in periodontal therapy Abstract KD Jithendra 1, Bansali A 2, Ramachandra SS 3 Studies have shown that modern periodontal
Universal Screw Removal System (USR)
 Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
Craniomaxillofacial Surgery 3 Universal Screw Removal System (USR) Craniomaxillofacial rigid fixation systems are available from a variety of manufacturers. The USR system is a complete screwdriver array
Complications Associated with Tooth Extraction
 1 Complications Associated with Tooth Extraction Mark M. Smith, VMD, DACVS, DAVDC Center for Veterinary Dentistry and Oral Surgery 9041 Gaither Road Gaithersburg, MD 20877 Introduction Tooth extraction
1 Complications Associated with Tooth Extraction Mark M. Smith, VMD, DACVS, DAVDC Center for Veterinary Dentistry and Oral Surgery 9041 Gaither Road Gaithersburg, MD 20877 Introduction Tooth extraction
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Boston College, BS in Biology 1980-1984. University of Southern California, Doctor of Dental Surgery, DDS, 1990.
 CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
The Obvious and the Obscure:Diagnostic Steps for Crack Confirmation
 Cracking the Cracked Tooth Code In response to your requests... At the end of each issue of ENDODONTICS: Colleagues for Excellence, the American Association of Endodontists (AAE) asks readers to send in
Cracking the Cracked Tooth Code In response to your requests... At the end of each issue of ENDODONTICS: Colleagues for Excellence, the American Association of Endodontists (AAE) asks readers to send in
Emdogain. The reliable solution for periodontal treatment.
 Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Anterior Esthetic Gingival Depigmentation and Crown Lengthening: Report of a Case
 Anterior Esthetic Gingival Depigmentation and Crown Lengthening: Report of a Case Abstract Excessive gingival display space and gingival hyperpigmentation are major concerns for a large number of patients
Anterior Esthetic Gingival Depigmentation and Crown Lengthening: Report of a Case Abstract Excessive gingival display space and gingival hyperpigmentation are major concerns for a large number of patients
TREATMENT REFUSAL FORMS
 TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
Dental Implants and Esthetics
 Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry
 REVIEW 193 Guy Huynh-Ba, Urs Brägger, Niklaus P Lang Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry KEY WORDS crown lengthening, surgery Guy Huynh-Ba Department
REVIEW 193 Guy Huynh-Ba, Urs Brägger, Niklaus P Lang Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry KEY WORDS crown lengthening, surgery Guy Huynh-Ba Department
The Treatment of Traumatic Dental Injuries
 The Recommended Guidelines of the American Association of Endodontists for The Treatment of Traumatic Dental Injuries 2013 American Association of Endodontists Revised 9/13 The Recommended Guidelines of
The Recommended Guidelines of the American Association of Endodontists for The Treatment of Traumatic Dental Injuries 2013 American Association of Endodontists Revised 9/13 The Recommended Guidelines of
Guidelines for Flapless Surgery
 BASI AND PATIENT-IENTED ESEAH ATIE IN PESS J ral Maxillofac Surg xx:xxx, 2007 Guidelines for Flapless Surgery Anthony G. Sclar, DMD* With the introduction ofi n-office cone beam computed tomography (T),
BASI AND PATIENT-IENTED ESEAH ATIE IN PESS J ral Maxillofac Surg xx:xxx, 2007 Guidelines for Flapless Surgery Anthony G. Sclar, DMD* With the introduction ofi n-office cone beam computed tomography (T),
Managing worn teeth with composites
 6 Managing worn teeth with composites Clinical details A 50-year-old man presents to you complaining about his worn teeth and would like the appearance improved (Fig. 6.1). He complains of regurgitation
6 Managing worn teeth with composites Clinical details A 50-year-old man presents to you complaining about his worn teeth and would like the appearance improved (Fig. 6.1). He complains of regurgitation
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Fast and Predictable Tooth Extraction Technique
 Fast and Predictable Tooth Extraction Technique When I first saw the ads for Physics Forceps, I did not believe the claims could be true. At first glance, I didn t see how this strange looking instrument
Fast and Predictable Tooth Extraction Technique When I first saw the ads for Physics Forceps, I did not believe the claims could be true. At first glance, I didn t see how this strange looking instrument
The Attractive Glass Abutment System (ZX-27) HANDOUT
 The Attractive Glass Abutment System () HANDOUT! " " # $ % $ # & ' ( ) FAQs New Solutions Pharmaceuticals Tel.: +971 6 7460661 Fax : +971 6 7460771 P.O.Box. 18161 Ajman - UAE e-mail : [email protected]
The Attractive Glass Abutment System () HANDOUT! " " # $ % $ # & ' ( ) FAQs New Solutions Pharmaceuticals Tel.: +971 6 7460661 Fax : +971 6 7460771 P.O.Box. 18161 Ajman - UAE e-mail : [email protected]
SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION. Ph.D. thesis. Dr. med. dent.
 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION Ph.D. thesis Dr. med. dent. Sofia Aroca Szeged, Hungary 2010 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL
SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION Ph.D. thesis Dr. med. dent. Sofia Aroca Szeged, Hungary 2010 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL
deltadentalins.com/usc
 Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
Tooth Supported Overdentures
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Universal Crown and Bridge Preparation
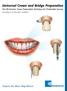 Universal Crown and Bridge Preparation The All-Ceramic Crown Preparation Technique for Predictable Success According to Dr. Ronald E. Goldstein Expect the Best. Buy Direct. The Universal * Crown and Bridge
Universal Crown and Bridge Preparation The All-Ceramic Crown Preparation Technique for Predictable Success According to Dr. Ronald E. Goldstein Expect the Best. Buy Direct. The Universal * Crown and Bridge
Classification of Malocclusion
 Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
ATLANTIS abutments design guide CAD/CAM patient-specific abutments
 ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
Relative position of gingival zenith in maxillary anterior teeth- a clinical appraisal
 Original article: Relative position of gingival zenith in maxillary anterior teeth- a clinical appraisal 1Dr Dipti Shah, 2 Dr Kalpesh Vaishnav, 3 Dr Sareen Duseja, 4 Dr Pankti Agrawal 1HOD, Dept of Prosthodontics,
Original article: Relative position of gingival zenith in maxillary anterior teeth- a clinical appraisal 1Dr Dipti Shah, 2 Dr Kalpesh Vaishnav, 3 Dr Sareen Duseja, 4 Dr Pankti Agrawal 1HOD, Dept of Prosthodontics,
SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE?
 CONTINUING EDUCATION X X SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE? André P. Saadoun, DDS, MS* Bernard Touati, DDS, MS SAADOUN 19 1 JANUARY/FEBRUARY When treatment with dental implants
CONTINUING EDUCATION X X SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE? André P. Saadoun, DDS, MS* Bernard Touati, DDS, MS SAADOUN 19 1 JANUARY/FEBRUARY When treatment with dental implants
Provide chairside support during the extraction of teeth and minor oral surgery
 About this workforce competence This workforce competence is intended for those who provide close support during the extraction of erupted teeth, the extraction of unerupted teeth or roots, and bone removal.
About this workforce competence This workforce competence is intended for those who provide close support during the extraction of erupted teeth, the extraction of unerupted teeth or roots, and bone removal.
The Mandibular Two-Implant Overdenture First-Choice. Standard of Care for the Edentulous Denture Patient
 The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Foundation Revolutionary Bone Augmentation Material. Thinking ahead. Focused on life. Regional Partner
 Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
Eliminating a Gummy Smile with Surgical Lip Repositioning
 Eliminating a Gummy Smile with Surgical Lip Repositioning by Ziv Simon, D.M.D., M.Sc., Ari Rosenblatt, D.D.S., D.M.D., William Dorfman, D.D.S., F.A.A.C.D. Dr. Simon is a periodontist who completed his
Eliminating a Gummy Smile with Surgical Lip Repositioning by Ziv Simon, D.M.D., M.Sc., Ari Rosenblatt, D.D.S., D.M.D., William Dorfman, D.D.S., F.A.A.C.D. Dr. Simon is a periodontist who completed his
Preventive Pediatric Dental Care. Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203
 Preventive Pediatric Dental Care Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203 Patient comfort and safety 1. All children are treated using the
Preventive Pediatric Dental Care Lawrence A. Kotlow DDS Practice Limited to Pediatric Dental Care 340 Fuller Road Albany, New York 12203 Patient comfort and safety 1. All children are treated using the
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
LESSON ASSIGNMENT. Topography of the Mouth and Tooth Structure. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Topography of the Mouth and Tooth Structure. LESSON ASSIGNMENT Paragraphs 3-1 through 3-9. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify
LESSON ASSIGNMENT LESSON 3 Topography of the Mouth and Tooth Structure. LESSON ASSIGNMENT Paragraphs 3-1 through 3-9. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Identify
Mucosal dehiscence coverage for dental implant using sprit pouch technique: a two-stage approach
 ase Report J Periodontal Implant Sci 2012;42:105-109 http://dx.doi.org/10.5051/jpis.2012.42.3.105 Mucosal dehiscence coverage for dental implant using sprit pouch technique: a two-stage approach Toyohiko
ase Report J Periodontal Implant Sci 2012;42:105-109 http://dx.doi.org/10.5051/jpis.2012.42.3.105 Mucosal dehiscence coverage for dental implant using sprit pouch technique: a two-stage approach Toyohiko
Page 1 of 10 BDS FINAL PROFESSIONAL EXAMINATION 2007 Prosthodontics (MCQs) Model Paper SECTION I
 Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
Page 1 of 10 COMPLETE DENTURES ANATOMICAL LANDMARKS SECTION I 1. There are many landmarks in the oral cavity which helps in designing complete dentures. One of the important landmarks is fovea palatini.
Chapter 21: Extraction
 Chapter 21: Extraction This chapter is near the end of the book as extraction is typically the last resort. I want you to think of other options before leaping to extract. Tooth extraction, or exodontia,
Chapter 21: Extraction This chapter is near the end of the book as extraction is typically the last resort. I want you to think of other options before leaping to extract. Tooth extraction, or exodontia,
Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice.
 32 News No. 32 May 2013 Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice. MAKE IT SIMPLE 2 Using BONDBONE as a composite in post extraction sockets
32 News No. 32 May 2013 Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice. MAKE IT SIMPLE 2 Using BONDBONE as a composite in post extraction sockets
ORAL SURGERY: MADE FUN AND EASY
 Paul Q. Mitchell, DVM, Diplomate AVDC Senior Veterinary Specialist Dentistry Veterinary Specialty Team Zoetis ORAL SURGERY: MADE FUN AND EASY Oral surgery is in many ways plastic and reconstructive surgery
Paul Q. Mitchell, DVM, Diplomate AVDC Senior Veterinary Specialist Dentistry Veterinary Specialty Team Zoetis ORAL SURGERY: MADE FUN AND EASY Oral surgery is in many ways plastic and reconstructive surgery
!Financial agreement COST / RISK / BENEFIT
 COMPLETE DENTURES 1 2 Oral Examination, Diagnosis and Treatment Planning Initial Appointment! Get to know your patient! Personally, experiences, expectations! Past medical history! Past dental history!
COMPLETE DENTURES 1 2 Oral Examination, Diagnosis and Treatment Planning Initial Appointment! Get to know your patient! Personally, experiences, expectations! Past medical history! Past dental history!
Periapical radiography
 8 Periapical radiography Periapical radiography describes intraoral techniques designed to show individual teeth and the tissues around the apices. Each film usually shows two to four teeth and provides
8 Periapical radiography Periapical radiography describes intraoral techniques designed to show individual teeth and the tissues around the apices. Each film usually shows two to four teeth and provides
Teeth and Dental Implants: When to save, and when to extract.
 Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
The extraction of teeth in Pets
 Ban0108_043-050 2/1/08 8:51 AM Page 43 Techniques for dental extractions Refined techniques allow practitioners to perform successful extractions and enhance a Pet s well-being. The extraction of teeth
Ban0108_043-050 2/1/08 8:51 AM Page 43 Techniques for dental extractions Refined techniques allow practitioners to perform successful extractions and enhance a Pet s well-being. The extraction of teeth
Many factors must be considered when
 + CASE STUDY 1 Loss of the Interdental Papilla Prevention and management of dental implant-related complications in the esthetic zone + Stephen J. Chu DMD, MSD, CDT + Mark N. Hochman DDS + Dennis P. Tarnow
+ CASE STUDY 1 Loss of the Interdental Papilla Prevention and management of dental implant-related complications in the esthetic zone + Stephen J. Chu DMD, MSD, CDT + Mark N. Hochman DDS + Dennis P. Tarnow
LIST OF DENTAL PROCEDURES (LOW PLAN) PREVENTIVE PROCEDURES
 LIST OF DENTAL PROCEDURES (LOW PLAN) The following is a complete list of the dental procedures for which benefits are payable under this section. No benefits are payable for a procedure that is not listed.
LIST OF DENTAL PROCEDURES (LOW PLAN) The following is a complete list of the dental procedures for which benefits are payable under this section. No benefits are payable for a procedure that is not listed.
Secondary dentition permanent teeth - 32. Primary dentition deciduous teeth - 20
 Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
Scottish Dental Clinical Effectiveness Programme SDcep. Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief
 Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
SCHEDULE OF BENEFITS DIRECT REFERRAL DENTAL PLAN*
 SCHEDULE OF BENEFITS DIRECT REFERRAL DENTAL PLAN* Nexus 150 This document describes the Covered Services of this dental plan, as well as Copayment requirements, Limitations of Benefits and Exclusions.
SCHEDULE OF BENEFITS DIRECT REFERRAL DENTAL PLAN* Nexus 150 This document describes the Covered Services of this dental plan, as well as Copayment requirements, Limitations of Benefits and Exclusions.
CRACKED TOOTH SYNDROME
 CRACKED TOOTH SYNDROME Dr Vijay Salvi We all come across apparently healthy teeth eliciting complex and often bizarre symptoms. The patient will give a long history of undiagnosed but severe pain, and
CRACKED TOOTH SYNDROME Dr Vijay Salvi We all come across apparently healthy teeth eliciting complex and often bizarre symptoms. The patient will give a long history of undiagnosed but severe pain, and
Humana Health Plans of Florida. Important:
 Humana Health Plans of Florida Important: Dental discount membership in Florida is determined by viewing the member s ID card and verifying that the Humana Logo and Medicare name is listed with an effective
Humana Health Plans of Florida Important: Dental discount membership in Florida is determined by viewing the member s ID card and verifying that the Humana Logo and Medicare name is listed with an effective
EQUINE ODONTOCLASTIC TOOTH RESORPTION AND HYPERCEMENTOSIS: TECHNIQUES FOR EXTRACTION OF CANINE AND INCISOR TEETH
 EQUINE ODONTOCLASTIC TOOTH RESORPTION AND HYPERCEMENTOSIS: TECHNIQUES FOR EXTRACTION OF CANINE AND INCISOR TEETH Jennifer E. Rawlinson, DVM, DAVDC Cornell University College of Veterinary Medicine, Ithaca,
EQUINE ODONTOCLASTIC TOOTH RESORPTION AND HYPERCEMENTOSIS: TECHNIQUES FOR EXTRACTION OF CANINE AND INCISOR TEETH Jennifer E. Rawlinson, DVM, DAVDC Cornell University College of Veterinary Medicine, Ithaca,
Dental Updates. Excerpted Article e-mail: [email protected]. Why Implant Screws Loosen Part 1. Richard Erickson, MS, DDS
 ¼ ½ ¾ µ mw/cm 2 Volume 17; 2007 Dental Updates "CUTTING EDGE INFORMATION FOR THE DENTAL PROFESSIONAL " 200 SEMINARS AND 30 JOURNALS REVIEWED YEARLY FOR THE LATEST, CUTTING EDGE INFORMATION Excerpted Article
¼ ½ ¾ µ mw/cm 2 Volume 17; 2007 Dental Updates "CUTTING EDGE INFORMATION FOR THE DENTAL PROFESSIONAL " 200 SEMINARS AND 30 JOURNALS REVIEWED YEARLY FOR THE LATEST, CUTTING EDGE INFORMATION Excerpted Article
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Straumann Dental Implant System. Implant Selection Guide.
 Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
Periodontal Surgery. What Can I Expect? The word "periodontal" literally means around the tooth. Many factors, such as oral hygiene habits, genetics,
 The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
