Appropriate Use Criteria for ICD/CRT Online Appendix Indications by Appropriate Use Ratings
|
|
|
- Aleesha Lucas
- 7 years ago
- Views:
Transcription
1 Appropriate Use Criteria for ICD/CRT Online Appendix Indications by Appropriate Use Ratings Table 1. Appropriate Indications (Median Score 7-9) Indication Appropriate Use Score (1-9) Section 1: Secondary Prevention CAD: VF or Hemodynamically Unstable VT Associated With Acute (<48 hours) MI (Newly Diagnosed, No Prior Assessment of LVEF) Total Revascularization Completed After Cardiac Arrest VF or polymorphic VT during acute (<48 hours) MI NSVT 4 days post MI Inducible VT/VF at EPS 4 days after revascularization VF or polymorphic VT during acute (<48 hours) MI NSVT 4 days post MI Inducible VT/VF at EPS 4 days after revascularization Obstructive CAD With Coronary Anatomy Not Amenable to Revascularization VF or polymorphic VT during acute (<48 hours) MI No EPS done CAD: VF or Hemodynamically Unstable VT <48 Hours (Acute) Post-Elective Revascularization No evidence for acute coronary occlusion, restenosis, preceding infarct, or other clearly reversible cause CAD: VF or Hemodynamically Unstable VT [No Recent MI ( 40 days) Prior to VF/VT and/or No Recent Revascularization ( 3 Months) Prior to VF/VT] No identifiable transient and completely reversible causes No need for revascularization identified by cath performed following VF/VT No identifiable transient and completely reversible causes No need for revascularization identified by cath performed following VF/VT No identifiable transient and completely reversible causes No need for revascularization identified by cath performed following VF/VT No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) Page 1
2 No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest CAD: VF or Hemodynamically Unstable VT During Exercise Testing Associated With Significant CAD No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) No revascularization performed (significant CAD present at cath performed following VF/VT, but coronary anatomy not amenable to revascularization) Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Incomplete revascularization performed after cardiac arrest Page 2
3 Dilated nonischemic cardiomyopathy Dilated nonischemic cardiomyopathy Dilated nonischemic cardiomyopathy No CAD: VF or Hemodynamically Unstable VT VF/Hemodynamically Unstable VT Associated With Other Structural Heart Disease 18. Myocardial sarcoidosis 20. Giant cell myocarditis Genetic Diseases with Sustained VT/VF 22. Congenital Long QT 23. Short QT 24. Catecholaminergic Polymorphic VT 25. Brugada syndrome 26. ARVC with successful ablation of all inducible monomorphic VTs 27. ARVC with unsuccessful attempt to ablate an inducible VT 28. ARVC without attempted ablation 29. Hypertrophic cardiomyopathy No Structural Heart Disease (LVEF 50%) or Known Genetic Causes of Sustained VT/VF Idiopathic VF With Normal Ventricular Function 32. No family history of sudden cardiac death 33. First degree relative with sudden cardiac death Syncope in Patients Without Structural Heart Disease Unexplained Syncope in a Patient With Long QT Syndrome 41. While on treatment with beta blockers 42. Not being treated with beta blockers Unexplained Syncope in a Patient With Brugada ECG Pattern 43. No EPS performed EPS performed No ventricular arrhythmias induced EPS performed Sustained VT/VF induced Unexplained Syncope in a Patient With Catecholaminergic Polymorphic VT 46. While on treatment with beta blockers Page 3
4 47. Not being treated with beta blockers Syncope in Patients With Coronary Artery Disease Unexplained Syncope With Prior MI and No Acute MI LVEF 36-49% 52. Electrophysiology study revealed inducible sustained VT/VF Unexplained Syncope With Prior MI and No Acute MI LVEF 35% 53. EPS not performed 54. Inducible VT/VF at EPS 55. Not inducible at EPS Syncope in Patients With Nonischemic Structural Heart Disease Unexplained Syncope in a Patient With Left Ventricular Hypertrophy Without Criteria for Hypertrophic Cardiomyopathy Left ventricular hypertrophy/hypertensive heart disease Unexplained Syncope in a Patient With Nonischemic Cardiomyopathy Nonischemic dilated cardiomyopathy Left ventricular non-compaction Left ventricular non-compaction 59. Hypertrophic cardiomyopathy 61. Tetralogy of Fallot with prior corrective surgery Unexplained Syncope in a Patient With Arrhythmogenic Right Ventricular Cardiomyopathy 62. No EPS performed 63. No inducible VT/VF at EPS Inducible VT/VF at EPS All inducible VTs successfully ablated Inducible VT/VF at EPS Ablation unsuccessful Sustained Hemodynamically Stable Monomorphic VT Associated With Structural Heart Disease CAD and prior MI CAD and prior MI CAD and prior MI Page 4
5 CAD and prior MI All inducible VTs successfully ablated CAD and prior MI Troponin elevation thought to be secondary to VT All inducible VTs successfully ablated CAD and prior MI Troponin elevation thought to be secondary to VT All inducible VTs successfully ablated Nonischemic dilated cardiomyopathy 69. Nonischemic dilated cardiomyopathy Nonischemic dilated cardiomyopathy Nonischemic dilated cardiomyopathy All inducible VTs successfully ablated Nonischemic dilated cardiomyopathy All inducible VTs successfully ablated Bundle branch reentry successfully ablated in a patient with nonischemic cardiomyopathy Bundle branch reentry successfully ablated in a patient with nonischemic cardiomyopathy Section 2: Primary Prevention Post Acute Myocardial Infarction ( 40 Days) LVEF 30% Revascularized After Acute MI EPS with inducible sustained VT (EPS performed after revascularization, within 30 days of MI) EPS with inducible sustained VT (EPS performed after revascularization, between 30 and 40 days after MI) Not Revascularized Obstructive CAD With Coronary Anatomy Not Amenable to Revascularization EPS with inducible sustained VT (EPS performed within 30 days of MI) EPS with inducible sustained VT (EPS performed between 30 and 40 days after MI) Post Acute Myocardial Infarction ( 40 Days) LVEF 31-40% Page 5
6 Revascularized for Acute MI EPS with inducible sustained VT (EPS performed after revascularization, within 30 days of MI) EPS with inducible sustained VT (EPS performed after revascularization, between 30 and 40 days after MI) Post Acute Myocardial Infarction ( 40 days) and Pre-Existing Chronic Cardiomyopathy ( 3 Months) LVEF 30% due to old infarction due to old infarction I-III due to nonischemic causes I-III Post Myocardial Infarction ( 40 days) and Need for Guideline-Directed Pacemaker Therapy Post MI (e.g., SSS, CHB, or Other Indications for Permanent Pacemaker) 94. Post Myocardial Infarction (>40 days) With Ischemic Cardiomyopathy No Recent PCI or CABG ( 3 Months) LVEF 30% LVEF 30% I LVEF 30% II LVEF 31-35% LVEF 31-35% I LVEF 31-35% II LVEF 36-40% Asymptomatic NSVT EPS with inducible sustained VT/VF Recent PCI or CABG ( 3 Months) Pre-existing documented cardiomyopathy on guideline-directed medical therapy >3 months prior to PCI/CABG Need for ppm post-revascularization (e.g., SSS, CHB, or other guideline-directed indications for permanent pacemaker) Page 6
7 Duration of Guideline-Directed Medical Therapy for Ischemic Cardiomyopathy Without Recent MI (Revascularization Not Indicated) On guideline-directed medical therapy <3 months NSVT EPS with inducible sustained VT On guideline-directed medical therapy 3 months LVEF 30% LVEF 30% I-III LVEF 31-35% LVEF 31-35% I-III Nonischemic Cardiomyopathy At Least 3 Months on Guideline-Directed Medical Therapy Recent Valve Surgery (i.e., Same Hospitalization or <3 Months) Which Included Incidental Bypass Graft Need for pacemaker and LV function not felt likely to improve Sarcoid heart disease Myotonic dystrophy Chagas disease Giant cell myocarditis Giant cell myocarditis LVEFF >35% Peripartum cardiomyopathy Persists >3 months postpartum Specific Etiologies Genetic Conditions (Excludes Syncope and Sustained VT, Covered in Section 1) 121. Hypertrophic cardiomyopathy with 1 or more risk factors 122. Arrhythmogenic right ventricular dysplasia/cardiomyopathy with no symptoms due to arrhythmia Congenital Long QT Syndrome With 1 or More Risk Factors Page 7
8 124. Receiving guideline-directed medical therapy Catecholaminergic Polymorphic VT With Nonsustained VT (Without Syncope) 125. Not receiving beta blockers, flecainide, or propafenone 126. Receiving beta blockers 127. Not tolerating or breakthrough nonsustained ventricular arrhythmias on beta blockers Incidentally Discovered Brugada by ECG (Type I ECG Pattern) In the Absence of Symptoms or Family History of Sudden Cardiac Death 129. Inducible VT or VF at EPS Familial Dilated/Nonischemic Cardiomyopathy (RV/LV) Associated With Sudden Cardiac Death 131. Evidence of structural cardiac disease but LVEF >35% 133. LV non-compaction with LVEF >35% Section 3: Comorbidities Special Conditions/Comorbidities in Patients for Primary Prevention (Meeting Indications of ICD Implant Related to HF Diagnosis With LVEF 30% on Guideline-Directed Medical Therapy >3 Months) Renal Disease Severe symptomatic peripheral vascular disease (e.g., peripheral interventions or clinical claudication) I Severe symptomatic peripheral vascular disease (e.g., peripheral interventions or clinical claudication) II Class IV Heart Failure 147. On waiting list for heart transplant Section 4: ICD Generator Replacement at ERI Primary Prevention ICD at Initial Implant No Clinically Relevant Ventricular Arrhythmias on ICD Since Implant Patient received primary prevention ICD when LVEF was 35% LVEF now unchanged No Clinically Relevant Ventricular Arrhythmias on ICD Since Implant (Now Has Prognosis <1 Year) Patient received primary prevention ICD Pacemaker dependent Replace with a pacemaker Clinically Relevant Ventricular Arrhythmias on ICD Since Implant Patient received primary prevention ICD when LVEF was 35% LVEF now unchanged Patient received primary prevention ICD when LVEF was 35% LVEF now 36-49% Patient received primary prevention ICD when LVEF was 35% LVEF now 50%% (normalized) Page 8
9 Patient received secondary prevention ICD No ventricular arrhythmia since initial implant Secondary Prevention ICD at Initial Implant Patient received secondary prevention ICD Had ventricular tachyarrhythmias in the monitor zone lasting >30 seconds, but no treated ventricular arrhythmias since initial implant Patient received secondary prevention ICD Had ventricular arrhythmias receiving ICD therapy since implant Primary Prevention at Initial Implant: Replacement of CRT-ICD for ERI Patient received a CRT-ICD when LVEF was 35% LVEF now unchanged (despite clinical improvement) Replace With CRT-ICD Patient received a CRT-ICD when LVEF was 35% LVEF now 36-49% Replace With CRT-ICD Patient received a CRT-ICD when LVEF was 35% LVEF now 50% (normalized) Replace With CRT-ICD Secondary Prevention at Initial Implant: Replacement of CRT-ICD for ERI Patient received a CRT-ICD when LVEF was 35% LVEF now unchanged (despite clinical improvement) Replace With CRT-ICD Patient received a CRT-ICD when LVEF was 35% LVEF now 36-49% Replace With CRT-ICD Patient received a CRT-ICD when LVEF was 35% LVEF now 50% (normalized) Replace With CRT-ICD Section 5: Dual Chamber ICD (As Opposed to Single Chamber ICD for Patients Who Meet Criteria for ICD Implantation) Conduction System Abnormalities Sinus Node Dysfunction Who Meets Criteria for ICD Sinus node dysfunction (includes sinus pauses, chronotropic incompetence, or marked sinus bradycardia that results from drug therapy required to treat other conditions) Symptomatic Resting sinus bradycardia (resting heart rate <50 bpm) Asymptomatic Conduction System Abnormalities AV Conduction Disease Who Meets Criteria for ICD (Narrow QRS <120 msec) Third degree AV block or advanced second degree AV block (Mobitz II AV block or high degree AV block) Symptomatic CRT not indicted Page 9
10 Third degree AV block or advanced second degree AV block (Mobitz II AV block or high degree AV block) Asymptomatic CRT not indicated Alternating RBBB and LBBB CRT not indicated Conduction System Abnormalities Bundle Branch Block Conduction System Abnormalities Acute MI or Ischemic Event Transient AV block thought to be secondary to ischemia Status post successful revascularization Chronic Wide QRS ( 120 msec) Transient AV block thought to be secondary to ischemia Not amenable to revascularization Chronic Wide QRS ( 120 msec) Conduction System Abnormalities Cardiac Valve Surgery 184. New LBBB and first degree AV block Tachyarrhythmias Atrial Arrhythmias or Supraventricular Tachycardia (SVT) and No Standard Pacing Indications 186. Paroxysmal atrial arrhythmias Slow Ventricular Arrhythmias Known Active patient Known slow VT that overlaps with sinus tachycardia rate Congenital Long QT Syndrome ICD for secondary prevention Congenital Long QT Syndrome ICD for primary prevention Genetic Disorders Section 6: CRT No Prior Implant Ischemic Cardiomyopathy LVEF 30% I II-amb IV Page 10
11 I II-amb IV II-amb IV Ischemic Cardiomyopathy LVEF 31-35% I II-amb IV I II-amb IV II-amb IV Nonischemic Cardiomyopathy LVEF 30% 206. I Page 11
12 II-amb IV I II-amb IV II-amb IV Nonischemic Cardiomyopathy LVEF 31-35% I II-amb IV I II-amb IV II-amb IV Pre-existing or Anticipated RV Pacing With a Clinical Indication for ICD or Pacemaker Implantation RV pacing anticipated >40% -II RV pacing anticipated >40% II-amb IV Intrinsic Narrow QRS, LVEF 35% Refractory Class III/IV CHF <3 Months Post Revascularization and/or 40 Days Post MI Page 12
13 No Other Indication for Ventricular Pacing LVEF 35% Table 2. May Be Appropriate Indications (Median Score 4-6) Indication Appropriate Use Score (1-9) Section 1: Secondary Prevention CAD: VF or Hemodynamically Unstable VT Associated With Acute (<48 hours) MI (Newly Diagnosed, No Prior Assessment of LVEF) Total Revascularization Completed After Cardiac Arrest Single episode VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI VF or polymorphic VT during acute (<48 hours) MI NSVT 4 days post MI Inducible VT/VF at EPS 4 days after revascularization No Revascularization Indicated (i.e., No Significant CAD) Single episode VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI Obstructive CAD With Coronary Anatomy Not Amenable to Revascularization VF or polymorphic VT during acute (<48 hours) MI No EPS done VF or polymorphic VT during acute (<48 hours) MI No EPS done CAD: VF or Hemodynamically Unstable VT <48 Hours (Acute) Post-Elective Revascularization No evidence for acute coronary occlusion, restenosis, preceding infarct, or other clearly reversible cause Page 13
14 No evidence for acute coronary occlusion, restenosis, preceding infarct, or other clearly reversible cause CAD: VF or Hemodynamically Unstable VT [No Recent MI ( 40 days) Prior to VF/VT and/or No Recent Revascularization ( 3 Months) Prior to VF/VT] Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest CAD: VF or Hemodynamically Unstable VT During Exercise Testing Associated With Significant CAD Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest Significant CAD identified at cath performed following VF/VT Complete revascularization performed after cardiac arrest VT/VF associated with cocaine abuse VT/VF associated with cocaine abuse No CAD: VF or Hemodynamically Unstable VT Severe Valvular Disease VT/VF <48 Hours After Surgical Repair or Replacement of Aortic or Mitral Valve No evidence of post-operative valvular dysfunction No evidence of post-operative valvular dysfunction No evidence of post-operative valvular dysfunction VF/Hemodynamically Unstable VT Associated With Other Structural Heart Disease 19. Myocarditis; not giant cell myocarditis 21. Takatsubo cardiomyopathy (stress induced cardiomyopathy, apical ballooning syndrome) 48 hours of onset of symptoms No Structural Heart Disease (LVEF 50%) or Known Genetic Causes of Sustained VT/VF Other Causes 34. Bradycardia dependent VT/VF Syncope in Patients With Coronary Artery Disease Unexplained Syncope With Prior MI and No Acute MI LVEF 36-49% 50. Electrophysiology study failed to define a cause of syncope Nonobstructive CAD; revascularization not indicated Page 14
15 51. Electrophysiology study failed to define a cause of syncope Obstructive CAD; not amenable to revascularization Syncope in Patients With Nonischemic Structural Heart Disease Unexplained Syncope in a Patient With Left Ventricular Hypertrophy Without Criteria for Hypertrophic Cardiomyopathy Left ventricular hypertrophy/hypertensive heart disease Unexplained Syncope in a Patient With Nonischemic Cardiomyopathy Nonischemic dilated cardiomyopathy Nonischemic dilated cardiomyopathy Left ventricular non-compaction 60. Cardiac amyloidosis Sustained Hemodynamically Stable Monomorphic VT Associated With Structural Heart Disease CAD and prior MI All inducible VTs successfully ablated CAD and prior MI All inducible VTs successfully ablated CAD and prior MI Troponin elevation thought to be secondary to VT All inducible VTs successfully ablated Nonischemic dilated cardiomyopathy All inducible VTs successfully ablated Bundle branch reentry successfully ablated in a patient with nonischemic cardiomyopathy Section 2: Primary Prevention Post Acute Myocardial Infarction ( 40 Days) LVEF 30% Revascularized After Acute MI EPS without inducible VT (EPS performed after revascularization, between 30 and 40 days after MI) Not Revascularized Obstructive CAD With Coronary Anatomy Not Amenable to Revascularization No EPS performed EPS without inducible VT (EPS performed within 30 days of MI) Page 15
16 84. EPS without inducible VT(EPS performed between 30 and 40 days after MI) Post Myocardial Infarction ( 40 days) and Need for Guideline-Directed Pacemaker Therapy Post MI (e.g., SSS, CHB, or Other Indications for Permanent Pacemaker) 95. LVEF 36-40% Post Myocardial Infarction (>40 days) With Ischemic Cardiomyopathy No Recent PCI or CABG ( 3 Months) LVEF 36-40% Asymptomatic NSVT No EPS LVEF 36-40% Asymptomatic NSVT EPS without inducible VT/VF No known pre-existing cardiomyopathy Recent PCI or CABG ( 3 Months) LVEF 36-40% Need for ppm post-revascularization (e.g., SSS, CHB, or other guideline-directed indications for permanent pacemaker) Duration of Guideline-Directed Medical Therapy for Ischemic Cardiomyopathy Without Recent MI (Revascularization Not Indicated) On guideline-directed medical therapy for <3 months LVEF 30% I-III Nonischemic Cardiomyopathy Treatment Since Diagnosis <3 Months Newly Diagnosed Cardiomyopathy With Narrow QRS At Least 3 Months on Guideline-Directed Medical Therapy 112. LVEF 36-40% Specific Etiologies Sarcoid heart disease LVEF >35% Myotonic dystrophy LVEF >35% Chagas disease LVEF >35% Amyloidosis with heart failure Amyloidosis with heart failure LVEF >35% Page 16
17 120. Peripartum cardiomyopathy Persists >3 months postpartum LVEF >35% Genetic Conditions (Excludes Syncope and Sustained VT, Covered in Section 1) Congenital Long QT Syndrome With 1 or More Risk Factors 123. Not receiving guideline-directed medical therapy Familial Dilated/Nonischemic Cardiomyopathy (RV/LV) Associated With Sudden Cardiac Death 132. Normal ECG and echo but carrying the implicated gene Section 3: Comorbidities Special Conditions/Comorbidities in Patients for Primary Prevention (Meeting Indications of ICD Implant Related to HF Diagnosis With LVEF 30% on Guideline-Directed Medical Therapy >3 Months) Life Expectancy 135. Noncardiac disease with life expectancy 1-2 years Elderly years old years old I years old II 90 years old I 90 years old II Cognitive Impairment Not able to understand or provide informed consent Health care proxy consents to ICD Renal Disease Severe symptomatic peripheral vascular disease (e.g., peripheral interventions or clinical claudication) Chronic kidney disease on dialysis Not a candidate for renal transplant Chronic kidney disease on dialysis Not a candidate for renal transplant I Chronic kidney disease on dialysis Not a candidate for renal transplant II Page 17
18 Chronic kidney disease with CrCl <30 cc, not yet on dialysis but candidate for dialysis Chronic kidney disease with CrCl <30 cc, not yet on dialysis but candidate for dialysis I Chronic kidney disease with CrCl <30 cc, not yet on dialysis but candidate for dialysis II Class IV Heart Failure 149. Patient with a VAD Section 4: ICD Generator Replacement at ERI No Clinically Relevant Ventricular Arrhythmias on ICD Since Implant Patient received primary prevention ICD when LVEF was 35% LVEF now 36-49% Patient received primary prevention ICD when LVEF was 35% LVEF now 50% (normalized) No Clinically Relevant Ventricular Arrhythmias on ICD Since Implant (Now Has Prognosis <1 Year) Patient received primary prevention ICD Pacemaker dependent Replace with ICD Clinically Relevant Ventricular Arrhythmias on ICD Since Implant Patient received primary prevention ICD Now has prognosis <1 year Primary Prevention at Initial Implant: Replacement of CRT-ICD for ERI Patient received a CRT-ICD when LVEF was 35% LVEF now 36-49% Replace with CRT-Pacemaker Patient received a CRT-ICD when LVEF was 35% LVEF now 50% (normalized) Replace with CRT-Pacemaker Section 5: Dual Chamber ICD (As Opposed to Single Chamber ICD for Patients Who Meet Criteria for ICD Implantation) Conduction System Abnormalities AV Conduction Disease Who Meets Criteria for ICD (Narrow QRS <120 msec) Mobitz Type I AV block Asymptomatic CRT not indicated First degree AV block (PR <300 msec) Asymptomatic First degree AV block (PR 300 msec) Asymptomatic Conduction System Abnormalities Bundle Branch Block Page 18
19 with normal PR interval CRT not indicated with first degree AV block CRT not indicated with normal PR interval Bifascicular block (RBBB/LAFB or RBBB/LPFB) CRT not indicated with first degree AV block Bifascicular block (RBBB/LAFB or RBBB /LPFB) CRT not indicated Conduction System Abnormalities Acute MI or Ischemic Event Transient AV block thought to be secondary to ischemia Status post successful revascularization Narrow QRS (<120 msec) Transient AV block thought to be secondary to ischemia Not amenable to revascularization Narrow QRS (<120 msec) Transient AV block Narrow QRS (<120 msec) with normal PR interval Asymptomatic Conduction System Abnormalities Cardiac Valve Surgery No Conduction Abnormalities Meets Criteria for ICD (Narrow QRS <120 msec) Tachyarrhythmias Atrial Arrhythmias or Supraventricular Tachycardia (SVT) and No Standard Pacing Indications Underlying structural heart disease (e.g., ischemic or nonischemic CM) No known paroxysmal atrial arrhythmias or SVT Structurally normal heart No known paroxysmal atrial arrhythmias or SVT Hypertrophic cardiomyopathy Narrow QRS (<120 msec) No standard bradycardia pacing indications Hypertrophic cardiomyopathy Wide QRS ( 120 msec) No standard bradycardia pacing indications Genetic Disorders Page 19
20 Section 6: CRT No Prior Implant Ischemic Cardiomyopathy LVEF 30% II-amb IV I Ischemic Cardiomyopathy LVEF 31-35% II-amb IV I Nonischemic Cardiomyopathy LVEF 30% 206. Page 20
21 II-amb IV I Nonischemic Cardiomyopathy LVEF 31-35% II-amb IV I LVEF >35% of Any Etiology (ICD Indicated) II-amb IV -II Page 21
22 II-amb IV II-amb IV LVEF 35% of Any Etiology NYHA Class IV On Intravenous Inotropic Support Pre-existing or Anticipated RV Pacing With a Clinical Indication for ICD or Pacemaker Implantation RV pacing anticipated 40% -II RV pacing anticipated 40% II-amb IV RV pacing anticipated 40% II-amb IV RV pacing anticipated >40% -II Intrinsic Narrow QRS, LVEF 35% Intrinsic Narrow QRS, LVEF >35% 227. RV pacing anticipated >40% II-amb IV Refractory Class III/IV CHF <3 Months Post Revascularization and/or 40 Days Post No Other Indication for Ventricular Pacing LVEF 35% No Other Indication for Ventricular Pacing LVEF 36-50% Page 22
23 Table 3. Rarely Appropriate Indications (Median Score 1-3) Indication Appropriate Use Score (1-9) Section 1: Secondary Prevention CAD: VF or Hemodynamically Unstable VT Associated With Acute (<48 hours) MI (Newly Diagnosed, No Prior Assessment of LVEF) Total Revascularization Completed After Cardiac Arrest Single episode VF or polymorphic VT during acute (<48 hours) MI Single episode VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI No Revascularization Indicated (i.e., No Significant CAD) Single episode VF or polymorphic VT during acute (<48 hours) MI Single episode VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI Recurrent VF or polymorphic VT during acute (<48 hours) MI VT/VF associated with cocaine abuse No CAD: VF or Hemodynamically Unstable VT No Structural Heart Disease (LVEF 50%) or Known Genetic Causes of Sustained VT/VF Pharmacologically Induced Sustained VT/VF R (2) R (2) R (2) 30. Non-torsades de pointes VT/VF in the setting of antiarrhythmic drug use 31. Drug induced torsades de pointes R (2) Other Causes 35. WPW syndrome with VT/VF Pathway successfully ablated Structurally normal heart Syncope in Patients Without Structural Heart Disease R (2) Unexplained Syncope With No Structural Heart Disease or Genetically Transmitted Ventricular Arrhythmias 36. Normal ECG and structurally normal heart Family history of sudden death Page 23
24 Normal ECG and structurally normal heart No known family history of sudden death Unexplained Syncope in a Patient With RV or LV Outflow Tract Tachycardia (Idiopathic VT) With Normal LV and RV Function and Anatomy Documented sustained monomorphic VT (LBBB/inferior axis) at the time of syncope Ablation not yet attempted Documented history of sustained monomorphic VT (LBBB/inferior axis) but not recorded at the time of syncope Ablation not yet attempted Documented sustained monomorphic VT (LBBB/inferior axis) at the time of syncope Ablation successful Syncope in Patients With Coronary Artery Disease Unexplained Syncope With Coronary Heart Disease and No Acute MI LVEF 50% Electrophysiology study and noninvasive investigations failed to define a cause of syncope No prior MI Nonobstructive CAD; revascularization not indicated Electrophysiology study and noninvasive investigations failed to define a cause of syncope No prior MI Obstructive CAD; not amenable to revascularization Syncope in Patients With Nonischemic Structural Heart Disease R (2) R (2) R (2) R (2) Unexplained Syncope in a Patient With Left Ventricular Hypertrophy Without Criteria for Hypertrophic Cardiomyopathy 56. Left ventricular hypertrophy/hypertensive heart disease Section 2: Primary Prevention Post Acute Myocardial Infarction ( 40 Days) LVEF 30% Plan for Revascularization (Not Yet Performed) 72. No NSVT R (2) Revascularized After Acute MI 73. No NSVT R (2) No EPS performed EPS without inducible VT (EPS performed after revascularization, within 30 days after MI) Not Revascularized Obstructive CAD With Coronary Anatomy Not Amenable to Revascularization 79. No NSVT R (2) Post Acute Myocardial Infarction ( 40 Days) LVEF 31-40% Revascularized for Acute MI 85. No NSVT R (2) Page 24
25 No EPS performed EPS without inducible VT (EPS performed after revascularization, within 30 days of MI) EPS without inducible VT (EPS performed after revascularization, between 30 and 40 days after MI) LVEF 30% LVEF 31-35% LVEF 31-35% I-III Acute lymphocytic myocarditis Newly diagnosed (<3 months ago) Acute lymphocytic myocarditis Newly diagnosed (<3 months ago) LVEF >35% Nonischemic Cardiomyopathy Treatment Since Diagnosis <3 Months Newly Diagnosed Cardiomyopathy With Narrow QRS Specific Etiologies Genetic Conditions (Excludes Syncope and Sustained VT, Covered in Section 1) Incidentally Discovered Brugada by ECG (Type I ECG Pattern) In the Absence of Symptoms or Family History of Sudden Cardiac Death 128. No EPS 130. No inducible VT or VF at EPS Section 3: Comorbidities Special Conditions/Comorbidities in Patients for Primary Prevention (Meeting Indications of ICD Implant Related to HF Diagnosis With LVEF 30% on Guideline-Directed Medical Therapy >3 Months) Life Expectancy 134. Life expectancy <1 year from cardiac or noncardiac conditions Elderly years old NHYA Class I 139. Cognitive Impairment Not able to understand or provide informed consent No health care proxy can be identified Advanced Psychiatric Impairment Page 25
26 140. Significant psychiatric illnesses that may be aggravated by device implantation or that may preclude regular follow-up Other Comorbidities 144. IV drug abuse (ongoing) R (2) 145. Unresolved infection associated with risk for hematogenous seeding R (2) 146. Non-compliance with medical therapy and follow-up Class IV Heart Failure Not candidate for cardiac transplantation, CRT, or VAD Refractory symptoms on oral therapy Not a candidate for transplant or VAD Does not meet CRT criteria Planned outpatient continuous intravenous inotropic therapy for palliation R (2) R (2) Section 4: ICD Generator Replacement at ERI Primary Prevention ICD at Initial Implant No Clinically Relevant Ventricular Arrhythmias on ICD Since Implant (Now Has Prognosis <1 Year) Patient received primary prevention ICD Not pacemaker dependent Primary Prevention at Initial Implant: Replacement of CRT-ICD for ERI Patient received a CRT-ICD when LVEF was 35% LVEF now unchanged (despite clinical improvement) Replace with CRT-Pacemaker Secondary Prevention at Initial Implant: Replacement of CRT-ICD for ERI Patient received a CRT-ICD when LVEF was 35% LVEF now 36-49% Replace with CRT-Pacemaker Patient received a CRT-ICD when LVEF was 35% LVEF now 50% (normalized) Replace with CRT-Pacemaker R (2) Section 5: Dual Chamber ICD (As Opposed to Single Chamber ICD for Patients Who Meet Criteria for ICD Implantation) Tachyarrhythmias Atrial Arrhythmias or Supraventricular Tachycardia (SVT) and No Standard Pacing Indications 189. Long-standing persistent or permanent atrial fibrillation or atrial flutter No plans for cardioversion or rhythm control Section 6: CRT No Prior Implant Ischemic Cardiomyopathy LVEF 30% 195. QRS <120 msec Page 26
27 QRS <120 msec I QRS <120 msec II-amb IV I Ischemic Cardiomyopathy LVEF 31-35% QRS <120 msec QRS <120 msec I QRS <120 msec II-amb IV I Nonischemic Cardiomyopathy LVEF 30% QRS <120 msec QRS <120 msec I QRS <120 msec II-amb IV Page 27
28 I Nonischemic Cardiomyopathy LVEF 31-35% QRS <120 msec QRS <120 msec I QRS <120 msec II-amb IV I LVEF >35% of Any Etiology (ICD Indicated) QRS <120 msec -II QRS <120 msec II-amb IV -II -II II-amb IV R (2) Page 28
29 II Pre-existing or Anticipated RV Pacing With a Clinical Indication for ICD or Pacemaker Implantation RV pacing anticipated 40% -II Intrinsic Narrow QRS, LVEF >35% Refractory Class III/IV CHF <3 Months Post Revascularization and/or 40 Days Post MI No Other Indication for Ventricular Pacing LVEF 36-50% R (2) Page 29
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
NCDR ICD Registry V2.1 Data Collection Form Generator & Leads
 A. DEMOGRAPHICS Last Name 2000 : First Name 2010 : Middle Name 2020 : SSN 2030 : - - SSN N/A 2031 Patient ID 2040 : (auto) Other ID 2045 : Birth Date 2050 : Race: B. EPISODE OF CARE (ADMISSION) Sex 2060
A. DEMOGRAPHICS Last Name 2000 : First Name 2010 : Middle Name 2020 : SSN 2030 : - - SSN N/A 2031 Patient ID 2040 : (auto) Other ID 2045 : Birth Date 2050 : Race: B. EPISODE OF CARE (ADMISSION) Sex 2060
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Appropriate Use Criteria for ICD/CRT Online Appendix Guideline Mapping and References Document
 Appropriate Use Criteria for ICD/CRT Online Appendix Guideline Mapping and References Document Section 1: Secondary Prevention Table 1.1 CAD: VF or Hemodynamically Unstable VT Associated With Acute (
Appropriate Use Criteria for ICD/CRT Online Appendix Guideline Mapping and References Document Section 1: Secondary Prevention Table 1.1 CAD: VF or Hemodynamically Unstable VT Associated With Acute (
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Premature Ventricular Contractions. Ralph Augostini, MD FACC FHRS
 Premature Ventricular Contractions Ralph Augostini, MD FACC FHRS Orlando, Florida October 7-9, 2011 Premature Ventricular Contractions: ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular
Premature Ventricular Contractions Ralph Augostini, MD FACC FHRS Orlando, Florida October 7-9, 2011 Premature Ventricular Contractions: ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Michael Hartman, CRNA, DNP, MSN, BSN, BA
 Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
Michael Hartman, CRNA, DNP, MSN, BSN, BA Intrinsic Conduction Automaticity-cardiac cells ability to spontaneously depolarize and initiate impulse Depolarization-cardiac cells go to a+ intracellular and
Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death. Management of Patients With. Learn and Live SM. ACC/AHA/ESC Pocket Guideline
 Learn and Live SM ACC/AHA/ESC Pocket Guideline Based on the ACC/AHA/ESC 2006 Guidelines Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death September 2006 Special
Learn and Live SM ACC/AHA/ESC Pocket Guideline Based on the ACC/AHA/ESC 2006 Guidelines Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death September 2006 Special
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians
 Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams
 Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC
 Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
IHE Cardiology (CARD) White Paper. Cardiac Electrophysiology Key Data Elements
 Integrating the Healthcare Enterprise IHE Cardiology (CARD) White Paper Cardiac Key Data Elements Date: August 5, 2011 Authors: IHE Cardiology Technical Committee Email: cardio@ihe.net CONTENTS Overview...
Integrating the Healthcare Enterprise IHE Cardiology (CARD) White Paper Cardiac Key Data Elements Date: August 5, 2011 Authors: IHE Cardiology Technical Committee Email: cardio@ihe.net CONTENTS Overview...
Ngaire has Palpitations
 Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Provider Checklist-Outpatient Imaging. Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469)
 Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Atrial Fibrillation Based on ESC Guidelines. Moshe Swissa MD Kaplan Medical Center
 Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect. Robert Kennedy, MD October 10, 2015
 Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services NEW product from the Medicare Learning Network (MLN) Provider Compliance Tips for Computed Tomography (CT) Scans Podcast,
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Updated Cardiac Resynchronization Therapy Guidelines
 The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
The Ohio State University Heart and Vascular Center Updated Cardiac Resynchronization Therapy Guidelines William T. Abraham, MD, FACP, FACC, FAHA, FESC Professor of Medicine, Physiology, and Cell Biology
CANADIAN COUNCIL OF MOTOR TRANSPORT ADMINISTRATORS CONSEIL CANADIEN DES ADMINISTRATEURS EN TRANSPORT MOTORISÉ CCMTA MEDICAL STANDARDS FOR DRIVERS
 ccmta! ccatm CANADIAN COUNCIL OF MOTOR TRANSPORT ADMINISTRATORS CONSEIL CANADIEN DES ADMINISTRATEURS EN TRANSPORT MOTORISÉ CCMTA MEDICAL STANDARDS FOR DRIVERS August 2011 TABLE OF CONTENTS Page INTRODUCTION...
ccmta! ccatm CANADIAN COUNCIL OF MOTOR TRANSPORT ADMINISTRATORS CONSEIL CANADIEN DES ADMINISTRATEURS EN TRANSPORT MOTORISÉ CCMTA MEDICAL STANDARDS FOR DRIVERS August 2011 TABLE OF CONTENTS Page INTRODUCTION...
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
Atrial Fibrillation The High Risk Obese Patient
 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Basics of Pacing. Ruth Hickling, RN-BSN Tasha Conley, RN-BSN
 Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
CARDIAC ELECTROPHYSIOLOGY, ARRHYTHMIAS AND PACING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Know the histology and gross anatomy of the normal sinoatrial node, atrial conduction pathways, atrioventricular (AV) junction and nod, His bundle, conduction fascicles and terminal intra-ventricular conduction
Know the histology and gross anatomy of the normal sinoatrial node, atrial conduction pathways, atrioventricular (AV) junction and nod, His bundle, conduction fascicles and terminal intra-ventricular conduction
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
PVC s / PAC s What Do They Mean? What Should You Do? Jeffrey H. Neuhauser, D.O.,F.A.C.C. BHHI Primary Care Symposium February 27, 2015
 PVC s / PAC s What Do They Mean? What Should You Do? Jeffrey H. Neuhauser, D.O.,F.A.C.C. BHHI Primary Care Symposium February 27, 2015 Financial disclosures Paid speaker for Pfizer Learning Objectives
PVC s / PAC s What Do They Mean? What Should You Do? Jeffrey H. Neuhauser, D.O.,F.A.C.C. BHHI Primary Care Symposium February 27, 2015 Financial disclosures Paid speaker for Pfizer Learning Objectives
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
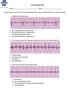 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology
 Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
2/20/2015. Cardiac Evaluation of Potential Solid Organ Transplant Recipients. Issues Specific to Transplantation. Kidney Transplantation.
 DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
NCDR ICD Registry V2.1 Coder's Data Dictionary
 A. Demographics Seq. #: 2000 Name: Last Name Indicate the patient's last name. Hyphenated names should be recorded with a hyphen. Target Value: The value on arrival at this facility Seq. #: 2010 Name:
A. Demographics Seq. #: 2000 Name: Last Name Indicate the patient's last name. Hyphenated names should be recorded with a hyphen. Target Value: The value on arrival at this facility Seq. #: 2010 Name:
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Management of Atrial Fibrillation in Heart Failure
 Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Adult Cardiac Surgery ICD9 to ICD10 Crosswalks
 164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
Atrial fibrillation. Quick reference guide. Issue date: June 2006. The management of atrial fibrillation
 Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Atrial fibrillation (AF) care pathways. for the primary care physicians
 Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99)
 CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
Preparing for ICD-10 for Physicians
 Preparing for ICD-10 for Physicians May 2011 Notices These coding suggestions and coverage guidelines do not replace seeking coding advice from the payer and/or your coding staff. The ultimate responsibility
Preparing for ICD-10 for Physicians May 2011 Notices These coding suggestions and coverage guidelines do not replace seeking coding advice from the payer and/or your coding staff. The ultimate responsibility
JAPI VOL. 52 NOVEMBER 2004 www.japi.org 883
 Review Article Wide Complex Tachycardia : Recognition and Management in the Emergency Room IB Ray Abstract Cardiac arrhythmias often present as urgent medical conditions requiring immediate care. Patient
Review Article Wide Complex Tachycardia : Recognition and Management in the Emergency Room IB Ray Abstract Cardiac arrhythmias often present as urgent medical conditions requiring immediate care. Patient
Syncope. enough to include disorders such as epileptic seizures and concussion. January 14-15, 2011 SCA Conference 1
 Syncope and Atypical Seizures Ravi Mandapati, M.D., FACC.; FHRS Director, Specialized Program for Arrhythmias in Congenital Heart Disease UCLA Cardiac Arrhythmia Center David Geffen School of Medicine
Syncope and Atypical Seizures Ravi Mandapati, M.D., FACC.; FHRS Director, Specialized Program for Arrhythmias in Congenital Heart Disease UCLA Cardiac Arrhythmia Center David Geffen School of Medicine
TABLE 1 Clinical Classification of AF. New onset AF (first detected) Paroxysmal (<7 days, mostly < 24 hours)
 Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular
 Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Karen Bain James Cook University Hospital Middlesbrough
 Karen Bain James Cook University Hospital Middlesbrough Electrophysiology Electrophysiology... Is the study of the heart s electrical system Assesses the function of each component of cardiac conduction
Karen Bain James Cook University Hospital Middlesbrough Electrophysiology Electrophysiology... Is the study of the heart s electrical system Assesses the function of each component of cardiac conduction
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
CHESHIRE EAST COUNCIL DRIVER MEDICAL
 BLOCK LETTERS PLEASE: CHESHIRE EAST COUNCIL DRIVER MEDICAL FULL NAME OF APPLICANT:.. DATE OF BIRTH.... ADDRESS:............. POST CODE... This certificate, which must be completed by a Registered Medical
BLOCK LETTERS PLEASE: CHESHIRE EAST COUNCIL DRIVER MEDICAL FULL NAME OF APPLICANT:.. DATE OF BIRTH.... ADDRESS:............. POST CODE... This certificate, which must be completed by a Registered Medical
Cardiac Implants: Morgan, Lewis & Bockius, LLP. Scott A. Memmott Albert W. Shay. The New Enforcement Priority
 Medical Necessity of Cardiac Implants: The New Enforcement Priority Morgan, Lewis & Bockius, LLP Scott A. Memmott Albert W. Shay Background Increased efforts over the last two years to combat Medicare/Medicaid
Medical Necessity of Cardiac Implants: The New Enforcement Priority Morgan, Lewis & Bockius, LLP Scott A. Memmott Albert W. Shay Background Increased efforts over the last two years to combat Medicare/Medicaid
22 Arrhythmias. C. Scharf and F. Duru. Siegenthaler, Differential Diagnosis in Internal Medicine (ISBN9783131421418), 2007 Georg Thieme Verlag
 22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
22 22 Arrhythmias C. Scharf and F. Duru 22 712 Arrhythmias 22.1 Differential Diagnosis of Arrhythmias 714 Medical History 714 Clinical Examination 714 Electrocardiogram (ECG) 715 Additional Tools for the
HYPERTROPHIC CARDIOMYOPATHY
 HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
Appendix. Costing Case Samples for OOHCA
 Appendix Costing Case Samples for OOHCA The patient (ICD-1) Treatment Codes (OPCS 4) Patient 27 Admitted to ICU following percutaneous cardiac intervention (PCI) with 2 drugeluting stents following a VF
Appendix Costing Case Samples for OOHCA The patient (ICD-1) Treatment Codes (OPCS 4) Patient 27 Admitted to ICU following percutaneous cardiac intervention (PCI) with 2 drugeluting stents following a VF
GuidePoint. Physician Reimbursement Primer for Cardiac Rhythm Management. With Clinical Case Examples. GuidePoint is simplifying reimbursement.
 GuidePoint GuidePoint is simplifying reimbursement. Physician Reimbursement Primer for Cardiac Rhythm Management With Clinical Case Examples DISCLAIMER Reimbursement information provided by Boston Scientific
GuidePoint GuidePoint is simplifying reimbursement. Physician Reimbursement Primer for Cardiac Rhythm Management With Clinical Case Examples DISCLAIMER Reimbursement information provided by Boston Scientific
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD
 92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
Managing the Patient with Atrial Fibrillation
 Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
These guidelines have been withdrawn
 These guidelines have been withdrawn MOH clinical practice guidelines are considered withdrawn five years after publication unless otherwise specified in individual guidelines. Users should keep in mind
These guidelines have been withdrawn MOH clinical practice guidelines are considered withdrawn five years after publication unless otherwise specified in individual guidelines. Users should keep in mind
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015
 Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
38 year old female with mild obesity. She is planning an exercise program to loose weight. She has no other known risk factors for CAD.
 Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Stress Testing: Wael A. Jaber, MD,FACC 38 year old female with mild obesity She is planning an exercise program to loose weight. She has no other known risk factors for CAD. You recommend: A. Exercise
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE
 SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE Summary Heart failure has a worse prognosis than many cancers with an annual mortality of 40% in the first year following diagnosis and 10% thereafter.
SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE Summary Heart failure has a worse prognosis than many cancers with an annual mortality of 40% in the first year following diagnosis and 10% thereafter.
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
LAST NAME VAT NUMBER. PHONE (Important for possible case discussion)
 Long QT Panel CUSTOMER INFORMATION FIRST NAME LAST NAME ORGANIZATION VAT NUMBER BILLING ADDRESS 1ST LINE BILLING ADDRESS 2ND LINE POST CODE CITY COUNTRY EMAIL (Required) PHONE (Important for possible case
Long QT Panel CUSTOMER INFORMATION FIRST NAME LAST NAME ORGANIZATION VAT NUMBER BILLING ADDRESS 1ST LINE BILLING ADDRESS 2ND LINE POST CODE CITY COUNTRY EMAIL (Required) PHONE (Important for possible case
Non Invasive Testing for CAD
 Non Invasive Testing for CAD Wael A. Jaber, MD Section of Cardiac Imaging Heart and Vascular Institute Cleveland Clinic 38 year old female with mild obesity She is planning an exercise program to loose
Non Invasive Testing for CAD Wael A. Jaber, MD Section of Cardiac Imaging Heart and Vascular Institute Cleveland Clinic 38 year old female with mild obesity She is planning an exercise program to loose
National CRM Database Future Directions. Francis Murgatroyd King s College Hospital, London
 National CRM Database Future Directions Francis Murgatroyd King s College Hospital, London Questions What is NICOR, and what happened to CCAD? Why are the databases changing? What changes are being made?
National CRM Database Future Directions Francis Murgatroyd King s College Hospital, London Questions What is NICOR, and what happened to CCAD? Why are the databases changing? What changes are being made?
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
2320-6691 2015; 3(3B):1132-1136 ISSN 2347-954X
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3B):1132-1136 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(3B):1132-1136 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
How to read the ECG in athletes: distinguishing normal form abnormal
 How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
Heart Failure Outpatient Clinical Pathway
 Heart Failure Outpatient Clinical Pathway PHASE 1: PHASE 2: PHASE 3: PHASE 4: Initial Consult and Treatment Optimization of Therapy Reassessment and Further Optimization Maintenance I. Provider II. Consults
Heart Failure Outpatient Clinical Pathway PHASE 1: PHASE 2: PHASE 3: PHASE 4: Initial Consult and Treatment Optimization of Therapy Reassessment and Further Optimization Maintenance I. Provider II. Consults
Life Threatening EKG s In The Office. Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium
 Life Threatening EKG s In The Office Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium January 24 th, 2015 Disclosures Speaker Honorariums: STJM, Boston Scientific Advisory role: Medtronic
Life Threatening EKG s In The Office Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium January 24 th, 2015 Disclosures Speaker Honorariums: STJM, Boston Scientific Advisory role: Medtronic
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Universitätsklinik für Kardiologie. Test. Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1
 Test Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1 Heart Failure - Definition European Heart Journal (2008) 29, 2388 2442 Akute Herzinsuffizienz Diagnostik und
Test Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1 Heart Failure - Definition European Heart Journal (2008) 29, 2388 2442 Akute Herzinsuffizienz Diagnostik und
Cardiology ARCP Decision Aid August 2014
 Cardiology ARCP Decision Aid August 2014 The table that follows includes a column for each training year which documents the targets that have to be achieved for a satisfactory ARCP outcome at the end
Cardiology ARCP Decision Aid August 2014 The table that follows includes a column for each training year which documents the targets that have to be achieved for a satisfactory ARCP outcome at the end
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
SIGN. Cardiac arrhythmias in coronary heart disease. Scottish Intercollegiate Guidelines Network. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 9 Cardiac arrhythmias in coronary heart disease A national clinical guideline 1 Introduction
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 9 Cardiac arrhythmias in coronary heart disease A national clinical guideline 1 Introduction
1p36 and the Heart. John Lynn Jefferies, MD, MPH, FACC, FAHA
 1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
