Building Healthy Lifestyles. Chronic Respiratory COPD. Clinical Guide. Building. Healthy. Lifestyles
|
|
|
- Tyler Owen
- 7 years ago
- Views:
Transcription
1 Chronic Respiratory Clinical Guide Building Healthy Lifestyles
2 We would like to acknowledge the contribution of the following groups: Chronic Respiratory Interdisciplinary Working Groups Chronic Disease Physician Advisory Group Chronic Disease Clinical Leadership Group Specialist Consultants Chronic Respiratory Clinical Champions Utilizing the Chronic Care model, these groups developed the Chronic Respiratory: Clinical Guide as a decision-support tool for improved functional and clinical outcomes. This Guide supports primary care interdisciplinary team-based practice with a strong focus on self-management. Please use and reproduce with acknowledgements to the Chinook Health Region. Chronic Disease Management and Prevention Network: An Alberta Health Capacity Building Initiative Chinook Health Region Lethbridge, Alberta April 2006 Chinook Health Region 2
3 Table of Contents 1. Diagnosis a. Definition...5 b. Risk Factors...5 c. Screening...5 d. Signs and Symptoms...5 e. Testing and Evaluation...5 f. Further Testing...6 g. Algorithm Classification/Type/Staging a. Stages/Types of Disease Patient Care Flow Sheet for Health Teams a. Patient Care Flow Sheet...11 b. Key Clinical Summary Management Strategies for Health Teams a. Goals of Management...13 b. Key Clinical Targets...13 c. Non-Pharmacologic Strategies...15 d. Pharmacologic Strategies Management Strategies for Patients/Clients a. Self-Care Support Information/Handouts/Tools...21 b. Supplementary Handouts Available...23 c. Patient/Client Checklist for Evidence-Based Care Referral to Specialists/Specialty Programs a. Indications for Referral to Medical Specialists...35 b. Indications for Referral to Specialty Programs...35 c. Local Contacts References a. Evidence...37 b. On-line Resources...37 Chinook Health Region 3
4 Chinook Health Region 4
5 1. Diagnosis BUILDING HEALTHY LIFESTYLES CHRONIC RESPIRATORY-ASTHMA 1. Diagnosis a. Definitions (Chronic Obstructive Pulmonary Disease): is a respiratory disorder largely caused by smoking and is characterized by progressive, partially reversible airway obstruction, systemic manifestations and increasing frequency and severity of exacerbations. Chronic Bronchitis: is characterized by expectoration of sputum on most days during at least 3 consecutive months for more than 2 successive years, for which other causes, such as infection with Mycobacterium tuberculosis, carcinoma of the lung or chronic heart failure have been excluded. Emphysema: is characterized by abnormal, permanent enlargement of the airspaces distal to the terminal bronchioles with destruction of their walls and without obvious fibrosis. Destruction is defined as irregular enlargement of respiratory airspaces; the orderly appearance of the acinus and its components is disturbed and may be lost. b. Risk Factors Tobacco Smoke: The most important risk factor for is cigarette smoking. Pipe, cigar and other types of tobacco smoking popular in many countries are also risk factors for. Other documented causes of include: Occupational dusts and chemicals (vapors, irritants and fumes when the exposures are sufficiently intense or prolonged) Alpha-1 antitrypsin deficiency syndrome c. Screening 1. Smokers or ex-smokers 40 years of age and older 2. Individuals with persistent cough and sputum production 3. Individuals with frequent respiratory tract infections 4. Individuals with progressive activity-related shortness of breath d. Signs and Symptoms Cardinal symptoms experienced by people with are: 1. Shortness of breath 2. Exercise intolerance 3. Cough & sputum production These symptoms are usually insidious in onset, typically progressive and characterized by frequent exacerbations. Although initially confined to the lungs this chronic, inflammatory process, which is the pathological basis for, is accompanied by systemic manifestations. Systemic manifestations of 1. Skeletal muscle dysfunction 2. Right heart failure 3. Secondary polycythemia 4. Altered nutritional status 5. Depression e. Testing and Evaluation Diagnosing Objective demonstration of air flow obstruction by Spirometry is mandatory for the diagnosis of. If is suspected, the patient should have a pre and post spirometry test performed by someone properly trained in this procedure. In order to establish a diagnosis of both of the following criteria must be met on the spirometry test: 1. Post-bronchodilator Forced Expiratory Volume in 1 second (FEV1.0) of less than 80% of predicted 2. Post-bronchodilator FEV1.0/FVC (Forced Vital Capacity) ratio of less than 0.7 Physical Examination Physical examination of patients with, although important, is not usually diagnostic and even careful physical examination can underestimate the presence of significant airflow limitation. With more advanced, clinical signs such as lung hyperinflation, right heart failure and generalized muscle wasting may be evident. Assessing Tobacco Consumption Total pack years = Number of cigarettes smoked/day 20 X number of years smoking Chinook Health Region 5
6 1. Diagnosis f. Further Testing Chest x-ray (rule out other respiratory co-morbidities) Arterial blood gas measurements or oximetry** Formal assessment of exercise capacity (six-minute walk test)** Body mass index (nutritional status) Full pulmonary function testing including lung volumes and diffusing capacity if spirometry shows a restrictive defect (if FVC from spirometry is below 80% of predicted normal) Sputum Gram Stain and culture should be considered for patients with very poor lung function, frequent exacerbations (> 3/year) or those who have been on antibiotics in the preceding 3 months **Indicated in more severe Chinook Health Region 6
7 1. Diagnosis g. Algorithm: MAKING A DIAGNOSIS OF Consider a Diagnosis of for patients who are: Smokers or ex-smokers more than 40 years old Patients with a persistent cough & sputum production Patients who experience frequent respiratory tract infections Patients who report progressive activity-related dyspnea And have no clinical features of asthma (See table A) Book for Pre & Post Spirometry Testing with adequately trained personnel Post Bronchodilator FEV1.0/FVC ratio less than 0.7 and Post Bronchodilator FEV1.0 is less than 80% predicted value YES NO Clinical features of are present (Listed in table A) Diagnosis of can be made Initiate treatment and education; refer to section 4 of Clinical Guide Clinical features of are present (Listed in table A) Diagnosis of cannot be made Patient at risk for development of ; regular follow-up with serial spirometry on an annual basis may be required TABLE A - CLINICAL DIFFERENCES BETWEEN ASTHMA AND Asthma Age of onset Usually < 40 years Usually > 40 years Smoking history Not causal Usually > 10 pack-years Sputum Production Infrequent Often Allergies Often Infrequent Disease course Stable (with exacerbations) Progressive worsening (with exacerbations) Spirometry Often normalizes Never Normalizes Clinical symptoms Intermittent and Variable Persistent - Differential diagnosis of chronic breathlessness: Other conditions included in the diagnosis of older patients presenting with progressive breathlessness include: cardiovascular conditions pulmonary vascular disease (pulmonary embolus) severe deconditioning obesity anemia interstitial lung disease rarely, neuromuscular disease ** In a small proportion of patients (e.g., those with chronic asthma who are smokers) diagnostic differentiation may be challenging and may require specialist assistance. Chinook Health Region 7
8 Chinook Health Region 8
9 2. Classification/Type/Staging 2. Classification/Type/Staging Determining the Severity of Most existing paradigms for the stratification of severity use the FEV1.0. None of these have been validated and there is no consensus as to which stratification system should be used. FEV1.0 measurement, while necessary for diagnosis and followup of, correlates poorly with symptom intensity, exercise capacity and quality of life. Moreover, physicians rarely rely on FEV1.0 thresholds to make therapeutic decisions. The Canadian Thoracic Society (CTS) panel believes that an ideal stratification system would use a composite index with evaluation in the domains of impairment, disability and handicap. The CTS panel believes that management decisions should be based on an assessment of dyspnea and disability on an individual basis, rather than spirometry alone. The panel encourages the use of the Medical Research Council (MRC) scale for dyspnea and disability assessment. A simple stratification system where severity is based on the MRC grade is provided below: MEDICAL RESEARCH COUNCIL DYSPNEA SCALE None Severe Grade 1 Grade 2 Grade 3 Grade 4 Grade 5 Breathlessness with strenuous exercise Short of breath when hurrying on the level or walking up a slight hill Walks slower than people of the same age on the level or stops for breath while walking at own pace on the level Stops to breathe after walking 100 yards Too breathless to leave the house or breathless when dressing Grade 0 refers to asymptomatic smokers/patients who have chronic productive cough, but who do not yet meet spirometric criteria for diagnosis. These patients are at risk for developing overt in the future. Such patients should receive regular follow-up with annual spirometry. Grade 2 or greater have significant disability and will benefit from effective treatment. Grade 5 are greatly disabled and require a more intensive, comprehensive management strategy to optimize outcomes. Therapy would be expected to escalate from MRC grade 2 through to grade 5. Canadian Thoracic Society Classification by Symptoms/Disability (MRC scale) Stage At Risk (does not meet criteria) Mild Moderate Severe Symptoms Asymptomatic smoker, ex-smoker or chronic cough/sputum, but most post-bronchodilator FEV1.0/FVC ratio 0.70 and / or FEV1.0 80% of predicted Shortness of breath from when hurrying on the level or walking up a slight hill (MRC 1-2) Shortness of breath from causing the client to stop after walking about 100m (or after a few minutes) on the level (MRC 3-4) Shortness of breath from resulting in the client too breathless to leave the house, or breathless after dressing/undressing or the presence of chronic respiratory failure or clinical signs of right heart failure (MRC 5) In the presence of non- conditions that may cause shortness of breath (e.g., cardiac dysfunction, anemia, muscle weakness, metabolic disorders), symptoms may not appropriately reflect disease severity. Classification of severity should be undertaken with care in patients with comorbid diseases or other possible contributors to shortness of breath. classification by lung function Stage At Risk Mild Moderate Severe Spirometry Normal spirometry, chronic symptoms FEV1.0/ FVC ratio 0.7 &/or FEV1.0 80% predicted FEV1.0/FVC ratio < 0.7, FEV1.0 60% - 79% of predicted FEV1.0/FVC ratio < 0.7, FEV1.0 40% - 59% of predicted FEV1.0/FVC ratio < 0.7, FEV1.0 < 40% of predicted FEV1.0= Forced expiratory volume in 1 second; FVC= Forced Vital Capacity Chinook Health Region 9
10 Chinook Health Region 10
11 3. Patient Care Flow Sheet for Health Terms 3. Chronic Disease Patient Care Flowsheet Patient Care Flowsheet Comorbid Conditions Patient Name: DOB: PHN: Year of diagnosis Ensure diagnosis of was made with Pre & Post Spirometry testing and meets both the following Canadian Thoracic Societies criteria to establish a diagnosis of : Post bronchodilator FEV1.0/FVC ratio < 0.7, and a post bronchodilator FEV1.0 < 80% predicted REVIEW ITEMS DATE: Too SOB to leave the house, or SOB when dressing (If yes, MRC score of grade 5= severe stage of ) FOR VISITS OFFICE REGULAR NEEDED ANNUALLY OR AS SEVERITY PHYSICAL EXAM MANAGEMENT TESTS OTHER Stops for breath after walking about 100 yards (If yes, MRC score of grade 4= moderate stage of ) Walks slower than people of same age on the level, or stops for breath while walking at own pace on the level (If yes, MRC score of grade 3 = moderate stage of ) SOB when hurrying on a level surface or walking up slight hill (If yes, MRC score of grade 2 = mild stage of ) SOB with strenuous exercise (If yes, MRC score of grade 1 = very mild stage of ) MRC = medical research council dyspnea scale, which is recommended by the CTS for assessment of disability from Temperature, pulse, respirations, blood pressure (PRN) Auscultation q visit O 2 sat (if in clinic) if < 90%, order blood gas Signs of right heart failure (If yes, is severe) Signs of lung hyperinflation Generalized muscle wasting Poor nutritional status (BMI, low <18.5 or high > 24.9) (Note: if over 65 years BMI, low < 24.0 or high > 29.0) Clinical signs of depression/anxiety Atypical features of : Early onset of (< 40 years) Family Hx of Disabled in 40s or 50s from If present, arrange screening for AAT deficiency Smoking Cessation, if still smoking 4 A model (Ask, Advise, Assist, Arrange) Short-acting bronchodilators: Long-acting bronchodilators: Long-acting anticholinergic: Inhaled corticosteroids: Review proper inhaler technique with client Devise or review a written CHR action plan for client Pre & Post Spirometry testing FEV1.0 Blood work Atypical features of present, write the following on a CHR lab req: Alpha-1 antitrypsin Pi phenotype test If using oral steroids, frequent Fasting Blood Sugar (FBS) Sputum gram stain & culture when purulent AE if: very poor lung function, AE > 3/year or has been on antibiotics in last 3 months Bone Mineral Density (BMD) for osteoporosis (If on ICS/oral steroids and has risk factors) Referrals: educator/program for education & pulmonary Rehab Pulmonary Medical Specialist- as needed Vaccinations: Annual influenza vaccine Pneumococcal vaccine (once in lifetime, repeat in 5-10 years in high risk patients) Revised as of June 16, 2005 developed by the BHL/ chronic respiratory/ Chinook Health Region Chinook Health Region 11
12 3. Patient Care Flow Sheet for Health Terms Stepwise Approach to the Classification and Management of General Characteristics & Symptoms Ensure early diagnosis with spirometry Treat AE as they occur and classify as: purulent or non-purulent Provide medical follow-up Advanced end of life care issues Consider Lung reduction Surgery Add long-term oxygen if an ABG shows a PaO2 of < 55 mmhg With frequent AE (> 3/year) add in ICSs to a long acting bronchodilators in a combination product + a long acting anticholinergic medication Without frequent AE ( < 3/year) long-acting bronchodilators + long-acting anticholinergic medications Add long-acting bronchodilator or a long-acting anticholinergic medication and refer to a pulmonary rehabilitation program Add Short-acting Bronchodilator as needed Smoking cessation, encourage healthy lifestyle, activity & Patient education Annual Influenza vaccination, Pneumococcal vaccination (If diagnosed with once in lifetime) Over 40 years Smoker or an ex-smoker Asymptomatic or chronic cough or SOB with exertion SOB from when hurrying on the level or walking up a slight hill SOB from causing the patient to stop walking after a few minutes on the level SOB from resulting in the client too breathless to leave the house, or breathless after dressing/undressing or the presence of chronic respiratory failure or clinical signs of right heart failure. MRC dyspnea Scale score Grade 0 Grade 1-2 Grade 3 4 Grade 5 Spirometry- post Bronchodilator Results FEV1.0 > 80% of predicted and FEV1.0/FVC > 0.7 FEV % of Predicted and FEV1.0/FVC < 0.7 FEV % of predicted and FEV1.0/FVC < 0.7 FEV1.0 < 40% of predicted and FEV1.0/FVC < 0.7 Stages of AT RISK MILD MODERATE SEVERE THERAPY AT EACH STAGE OF Adapted from the Global Initiative for Chronic Obstructive Lung Disease Executive Summary, and the Canadian Thoracic Society s Recommendations for Management of 2003 Executive Summary Short-acting Bronchodilators For symptomatic or rescue treatment Salbutamol (Ventolin) MDI/spacer 100 mcg per dose 1 or 2 inhalations QID and prn Salbutamol (Ventolin) Diskus 200 mcg per dose 1 inhalation QID and prn Combivent (salbutamol 120 mcg/ipratropium 20 mcg per dose) MDI/spacer 2 inhalations QID and prn Ipratropium (Atrovent) MDI/spacer 20 mcg per dose 2 inhalations QID and prn Terbutaline (Bricanyl) turbuhaler 0.5 mg per dose 1 inhalation QID and prn Salbutamol (Airomir) MDI/spacer 100 mcg per dose 1 or 2 inhalations QID and prn Long-acting Beta agonist Bronchodilators (LABA) Can be used alone or in a combination product Salmeterol (Serevent) MDI/spacer 25 mcg per dose 1 or 2 inhalations BID Salmeterol (Serevent) Diskus 50 mcg per dose 1 inhalation BID Formoterol (Oxeze) Turbuhaler 6 or 12 mcg per dose 1 to 2 inhalations BID of 6 mcg dose 1 inhalation BID of 12 mcg dose Long-acting Anti-cholinergic Bronchodilators Tiotropium (Spiriva) Handihaler 18 mcg per dose 1 inhalation QD*** Acute Exacerbations of (AE) Inhaled bronchodilators to treat dyspnea in AE consider combination therapy (Combivent MDI/spacer) No role for the initiation of methylxanthines during AE, possible drug interactions with antibiotics. Oral/parenteral steroids for 14 days in most moderate to severe clients with, limited data on benefits of clients with mild (FEV1.0 > 60% of predicted). Dosages of 25 to 50 mg per day are recommended. Antibiotic therapy is recommended only for those clients with purulent exacerbations, refer to chart below: Combination products with Inhaled Corticosteroids (ICS) Recommended for severe with > than 3 exacerbations per year, use LABA and ICS in combination form: Symbicort (Oxeze 6 mcg/pulmicort 100 or 200 mcg per dose) Turbuhaler 1 or 2 inhalations BID Advair (Serevent 25 mcg/flovent 125 or 250 mcg per dose) MDI/spacer 1 or 2 inhalations BID Advair (Serevent 50 mcg/flovent 100, 200 or 500 mcg per dose) Diskus 1 inhalation BID *** Spiriva is not to be used in conjunction with Atrovent or Combivent inhalers. Treatment options from the 2003 Canadian Thoracic Society Recommendations for Management of Medication information updated as of May 9, 2005 Chinook Health Region 12
13 4. Management Strategies for Health Teams 4. Management Strategies for Health Teams a & b. Goals of Management & Key Clinical Targets The goals of management of Chronic Obstructive Pulmonary Disease are as follows: 1. To prevent disease progression (smoking cessation) 2. To alleviate breathlessness and other respiratory symptoms 3. To improve exercise tolerance 4. To prevent and treat exacerbations 5. To improve health status 6. To reduce mortality It is essential once the diagnosis has been made that continuous follow-up of patients occurs with prompt and effective treatment of acute exacerbations. Patients with advanced symptomatic disease require a comprehensive management plan that includes effective end-of-life care. Chinook Health Region 13
14 4. Management Strategies for Health Teams Stepwise Approach to the Classification and Management of Consider Lung reduction Surgery Add long-term oxygen if an ABG shows a PaO2 of < 55 mmhg Ensure early diagnosis with spirometry Treat AE as they occur and classify as: purulent or non-purulent Provide medical follow-up Advanced end of life care issues With frequent AE (> 3/year) add in ICSs to a long acting bronchodilators in a combination product + a long acting anticholinergic medication Without frequent AE ( < 3/year) long-acting bronchodilators + long-acting anticholinergic medications Add long-acting bronchodilator or a long-acting anticholinergic medication and refer to a pulmonary rehabilitation program General Characteristics & Symptoms Add Short-acting Bronchodilator as needed Smoking cessation, encourage healthy lifestyle, activity & Patient education Annual Influenza vaccination, Pneumococcal vaccination (If diagnosed with once in lifetime) Over 40 years Smoker or an ex-smoker Asymptomatic or chronic cough or SOB with exertion SOB from when hurrying on the level or walking up a slight hill SOB from causing the patient to stop walking after a few minutes on the level SOB from resulting in the client too breathless to leave the house, or breathless after dressing/undressing or the presence of chronic respiratory failure or clinical signs of right heart failure. MRC dyspnea Scale score Grade 0 Grade 1-2 Grade 3 4 Grade 5 Spirometry- post Bronchodilator Results FEV1.0 > 80% of predicted and FEV1.0/FVC > 0.7 FEV % of Predicted and FEV1.0/FVC < 0.7 FEV % of predicted and FEV1.0/FVC < 0.7 FEV1.0 < 40% of predicted and FEV1.0/FVC < 0.7 Stages of AT RISK MILD MODERATE SEVERE THERAPY AT EACH STAGE OF Adapted from the Global Initiative for Chronic Obstructive Lung Disease Executive Summary, and the Canadian Thoracic Society s Recommendations for Management of 2003 Executive Summary Chinook Health Region 14
15 4. Management Strategies for Health Teams c. Non-Pharmacologic Strategies for Smoking Cessation: Smoking cessation interventions (4A model) should be offered to patients with who are still smoking, or to spouses or other persons living with patient who smoke. Physical Activity & Pulmonary Rehabilitation: Encourage patients with to maintain physical activity to prevent deconditioning that results in increased dyspnea. Refer to a formal pulmonary rehabilitation program if patient has clinically stable, symptomatic ; reduced activity levels and increased dyspnea despite pharmacological treatment; no evidence of active ischemic, musculoskeletal, psychiatric or other systemic disease; sufficient motivation for participation. Self-Management Plan & Education: Provide disease specific education individually or through a pulmonary rehab program; refer to Section 5, Subsection a for the Chinook Health Region Action Plan. Influenza & Pneumococcal Vaccinations: Encourage patients with to receive an annual influenza vaccination. A pneumococcal vaccination is recommended for patients once in a lifetime. Nutrition: Assess patients with to ensure adequate and proper nutrition (BMI). Alpha 1 Antitrypsin (AAT) Deficiency: It is recommended that any patient with atypical features of, including the following: a. Patients with early onset of disease < 40 years of age b. A positive family history of c. Patients who become disabled in their 40s or 50s be screened for AAT deficiency and AAT phenotype (Pi type); all provincial health plans should cover the cost of screening. The guidelines strongly recommend participation in the Alpha-1 Canadian registry at The guidelines recommend restricting the option for AAT replacement therapy to AAT deficient patients with an FEV1.0 > 35% and less than 50% predicted who have quit smoking and are on optimal medical therapy, yet continue to show a rapid decline in FEV1.0 (> 80 ml/year). Lung Volume Reduction Surgery (LVRS) or Lung Transplantation for : Referral to a respiratory specialist for evaluation of inclusion criteria Indications Selection criteria for Lung Volume Reduction Surgery Disability from emphysema (not from bronchitis or asthma) despite maximal medial treatment Age is less than years Abstinence from smoking > 4 months FEV1.0 < 40% predicted TLC > 120% of predicted RV > 175% of predicted Hyperinflation, preferably with upper lobe dominance by CT scan (heterogeneous distribution) Contraindications Comorbid disease (i.e., operation prohibitive risk or life expectancy < 2 years) Severe obesity or cachexia Severe coronary artery disease Active smoker Alpha-1 antitrypsin deficiency Extensive pleural symphysis Chest wall deformity PaCO2 > 50 to 60 mmhg PAP > 35 mmhg (mean) FEV1.0 < 20% predicted and homogenous distribution or DLCO < 20% predicted DLCO = Diffusing Capacity from Carbon Monoxide FEV1.0 = Forced Expiratory Volume in 1 second PaCO2 = Partial Pressure of Arterial CO2 (ABGs) PAP = Pulmonary Arterial Pressure RV = Residual Volume TLC = Total Lung Capacity End-of-life issues: Encourage patients to articulate to their physicians and caregivers a desire for information about their disease, prognosis and the possible circumstances of their death. End of life communication skills are an integral component for all physicians who care for patients. Consider a referral to palliative care services to assist the patient and their family. Supplemental Oxygen Therapy: See Pharmacologic Strategies for Asthma Chinook Health Region 15
16 4. Management Strategies for Health Teams Brief Primary Care Smoking Cessation Intervention Tool Place patient label here ASK about smoking (at every opportunity/visit) Tobacco Use: Smoking Status: (circle number corresponding to visit) Cigarettes Current smoker Visit # Cigars Non-smoker Visit # Pipe tobacco Recent ex-smoker Visit # Other If patient is a current smoker ask the following question to assess their interest in quitting smoking: Visit # Have you ever tried to stop smoking? Y N Y N Y N Y N ADVISE about smoking (clear, firm, personalized advice to quit) Have you thought about quitting smoking? NO Not thinking of quitting in the next 6 months (precontemplation) YES Thinking of quitting in the next 6 months (contemplation) YES Plans to quit within in next 30 days (preparation) YES Quit smoking within the past 6 months (action) YES Has not smoked for more than 6 months (maintenance) Visit # Visit # Visit # Visit # Visit # PRECONTEMPLATION Do you believe your smoking is a cause for concern? Who would benefit if you quit smoking? Are you aware of all of the risks of smoking? CONTEMPLATION What do you like about smoking? What are some good things about quitting smoking? What are some bad things about quitting smoking? PREPARATION What is your plan of action for quitting? What do you need to know to handle quitting smoking? Tell your family & friends you re going to quit smoking and ask for their help. ACTION What strategies are you using to cope with quitting? What situations tempt you to want to smoke? Are you able to avoid these situations? CLEAR- My best advice for you is to quit smoking FIRM- As your physician/clinician, I need you to know that quitting smoking is the most important thing you can do to protect your health. PERSONALIZED- emphasize the impact of smoking on patient & family ASSIST If patient is not yet ready to quit: Offer to help patient quit when they are ready. Refer to the Smoker s Help line If patient is ready to quit: Set a quit date with patient: Visit # 1 #2 #3 #4 dd/mm/yy dd/mm/yy dd/mm/yy dd/mm/yy **smokers make an average of 3-4 quit attempts before they achieve long-term maintenance MAINTENANCE Are you aware of any things that could tempt you to start smoking again? Could you tell if you were at risk for a slip? What would you do if you were at risk for a slip? Discuss pharmacotherapy support: Nicotine replacement therapies (NRT): Gum Patch Bupropion (Zyban) Provide resources: Smoker s help line Provide brochures Your smoking stage- What kind of smoker are you? Withdrawal..And Beyond The benefits of quitting smoking Quit-Smoking aids compared Stop smoking resources ARRANGE Follow-up consultation on: Visit # 1 #2 #3 #4 dd/mm/yy dd/mm/yy dd/mm/yy dd/mm/yy Completed by Signature (Adapted from the Calgary Health Region Tobacco assessment form, 2000) Chinook Health Region 16
17 4. Management Strategies for Health Teams d. Pharmacologic Strategies for I. Short-acting Bronchodilators first line therapy: For patients with symptoms that are only noticeable with exertion and who have relatively little disability, initiation of therapy with either a short acting beta-2 agonist as needed (or a regular anticholinergic or combination anticholinergic and/or beta-2 agonist) is acceptable. Short-acting beta-2 agonists (SABA): Salbutamol (Ventolin) MDI/spacer 100 mcg per dose 1 or 2 inhalations PRN Salbutamol (Ventolin) Diskus 200 mcg per dose 1 inhalation PRN Terbutaline (Bricanyl) Turbuhaler 0.5 mg per dose 1 inhalation PRN Salbutamol (Airomir) MDI/spacer 100 mcg per dose 1 or 2 inhalations PRN Short-acting anticholinergic bronchodilators: Ipratropium (Atrovent) MDI/spacer 20 mcg per dose 2 inhalations QID and PRN Combination short-acting bronchodilators: (Combivent 120 mcg/ipratropium 20 mcg) per dose MDI/spacer 2 inhalations QID and PRN II. Long-acting Beta-2 Bronchodilators (LABA) second line therapy: Use a long-acting bronchodilator for patients whose symptoms persist despite reasonable short-acting bronchodilator therapy. Short acting beta-2 agonists may be used as needed for immediate symptom relief. For patients with moderate to severe, persistent symptoms and exercise intolerance, a combination of Tiotropium once daily and a LABA is recommended to maximize bronchodilation, although it should be noted that results of ongoing studies on the effect of this combination on various health outcomes are not yet available. Short-acting beta-2 agonists may be used as needed for immediate symptom relief. In patients with severe symptoms, despite the use of both Tiotropium and LABA, a long-acting preparation of oral theophylline may be tried, although monitoring of blood levels, side effects and potential drug interactions is necessary. Long-acting Beta-2 agonist Bronchodilators (LABA): Can be used alone or in a combination product Salmeterol (Serevent) MDI/spacer 25 mcg per dose 1 or 2 inhalations BID Salmeterol (Serevent) Diskus 50 mcg per dose 1 inhalation BID Formoterol (Oxeze) Turbuhaler 6 or 12 mcg per dose 1 to 2 inhalations BID of 6 mcg dose 1 inhalation BID of 12 mcg dose Long-acting Anti-cholinergic Bronchodilators: Tiotropium (Spiriva) Handihaler 18 mcg 1 inhalation QD Spiriva is not to be used in conjunction with Atrovent or Combivent inhalers III. Inhaled Corticosteroids (ICSs) third line therapy In contrast to asthma, ICSs should NOT be used as first line medication in because no consistent effects have been demonstrated on airway inflammatory cells, related inflammatory cells and related inflammatory mediators Regular use of high doses of ICSs alone should only be considered in patients with moderate to severe who have recurrent, acute exacerbations (3 or more exacerbations per year, especially in those requiring the use of an oral steroid) The guidelines suggest that the potential for limited benefits in many patients contrasted sharply with the likelihood of adverse effects when ICSs are used in high doses for prolonged periods of time, particularly in the elderly Combination products with Inhaled Corticosteroids (ICSs) Recommended for severe with > than 3 exacerbations per year; use LABA and ICSs in combination form: Symbicort (Oxeze 6 mcg/pulmicort 100 or 200 mcg per dose) Turbuhaler 1 or 2 inhalations BID Advair (Serevent 25 mcg/flovent 125 or 250 mcg per dose) MDI/spacer 1 or 2 inhalations BID Advair (Serevent 50 mcg/flovent 100, 200 or 500 mcg per dose) Diskus 1 inhalation BID Supplemental Oxygen Therapy: For patients with with resting hypoxemia, defined as a PO 2 on an ABG 55 mmhg, or when the PaO 2 on an ABG is less than 60 mmhg with the presence of bilateral ankle edema, cor pulmonale or a hematocrit greater than 56%. Chinook Health Region 17
18 4. Management Strategies for Health Teams Dose Equivalencies for Inhaled Corticosteroids (All ages) Daily Dose (mcg/day) Product Low Moderate High BUD turbuhaler < > 800 FP pmdi and spacer < > 500 FP Diskus < > 500 BDP pmdi (HFA) < > 500 BUD wet nebulization < > 2000 BDP= Beclomethasone dipropionate (Q-var) BUD= Budesonide (pulmicort) FP= Fluticasone propionate (Flovent) Chinook Health Region 18
19 4. Management Strategies for Health Teams Management of Acute Exacerbations of (AE) AE: is a sustained worsening of dyspnea, cough or sputum production leading to an increased use of maintenance medications and/or supplementation with additional medicine. The term, sustained, implies a change from baseline lasting 48 hours or more Exacerbations should be defined as either purulent (characterized by change in sputum color) or non-purulent, because this is helpful in predicting the need for antibiotic therapy Testing and Evaluation Arterial blood gases on those patients who present with low (< 90%) oxygen saturations on oximetry Chest x-rays are recommended for patients presenting to the ER or for admission to hospital because they have been shown to reveal abnormalities that lead to a change in management in 16% to 21% of patients Sputum Gram Stain and culture should be considered for patients with very poor lung function, frequent exacerbations (> 3/year) or those who have been on antibiotics in the preceding 3 months Non-Pharmacologic Strategies: Avoid smoking including 2nd hand smoke Reduce activity Refer to personalized, written Action Plan as to how to temporarily modify medications Pulmonary function tests should be performed in patients suspected of having following recovery if they have not previously had spirometry to diagnose II. Oral Steroid therapy: There is good evidence to support the use of oral or parenteral steroids for 14 days with most AE in patients who have moderate to severe. The exact dose and duration of therapy should be individualized, but treatment periods of between 7 to 14 days are recommended. Dosages of 25 mg to 50 mg of prednisone equivalent per day are suggested. No Prednisone dose tapering required if less than 2 weeks. The role for oral steroid therapy in outpatients with milder (FEV1.0 > than 60% predicted) remains unclear at this time. The role of high dose ICS therapy during an AE warrants further investigation before recommendations can be made. III. Antibiotic therapy: The guidelines recommend that antibiotics only be considered for use in patients with purulent exacerbations Then, divide patients into two groups: simple or complicated exacerbations, based on the presence of risk factors that either increase the likelihood of treatment failure or more likely to be associated with more virulent or resistant microbial pathogens Pharmacologic Strategies: I. Bronchodilators Inhaled bronchodilators should be used to treat dyspnea in AE. While most studies do not reveal any additional benefit from combining an inhaled beta-2 agonist with an inhaled anti-cholinergic drug, there are some patients who clearly benefit from combination therapy. Therefore, combination therapy is still recommended in the acute situation. There is no difference in the objective outcomes between the use of nebulized bronchodilators or bronchodilators given through an MDI with spacer. Due to the lower cost of using MDIs with spacer, this route is preferred in most situations. There is no role for the initiation of therapy with methylxanthines during an AE. For patients already on an oral methylxanthine product, it is reasonable to continue the medication during an AE. However, in this circumstance one must consider the possibility of drug interactions with antibiotics and monitor the dose accordingly. Chinook Health Region 19
20 4. Management Strategies for Health Teams Antibiotic Treatment Recommendations for Purulent AE Group State Basic Clinical Symptoms and Risk Factors Probable Pathogens First Choice Alternative for treatment Simple without risk factors Increased cough & sputum Sputum purulence & increased dyspnea Haemophilus Influenzae Haemophilus species Moraxella catarrhalis Streptococcus pneumoniae Amoxicillin, doxycycline, trimethoprim/ sulfamethoxazole, 2 nd or 3 rd generation cephalsporins, extended spectrum macrolides Beta-lactam/beta-lactamase inhibitor; fluoroquinolone Complicated with risk factors As in simple, plus (at least one of): FEV1.0 < 50% predicted > 4 exacerbations/year Ischemic heart disease Use of home oxygen Chronic oral Steroid use As in simple, plus: Klebsiella species & other gram negatives Increased probability of beta lactam reistance Beta-lactum/beta-lactamase inhibitor, fluoroquinolone (Antibiotics for uncomplicated patients when combined with oral steroids may suffice) May require parenteral therapy Consider referral to a specialist or hospital Antibiotic use in past 3 months FEV1.0 = forced expiratory volume in 1 second Chinook Health Region 20
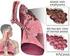
21 5. Management Strategies for Patients / Clients 5. Management Strategies for Patients/Clients YOU HAVE JUST BEEN TOLD THAT YOU HAVE, NOW WHAT? WHAT IS? C CHRONIC or long term O OBSTRUCTIVE, the air passages are partially blocked or occluded P PULMONARY, which refers to the lungs D DISEASE is a condition that makes breathing more difficult because the air passages and air sacs in the lungs have been damaged. The air passages become partly blocked and the air sacs (like balloons at the end of the air passages) have lost their ability to contract down, making it more difficult to push the stale air out of the lungs and breathe fresh air into the lungs. It is a condition that has developed and worsened over a period of time. WHAT ARE THE SYMPTOMS OF? The most common symptoms of are as follows: Shortness of breath as well as increased phlegm production Decreased ability to perform exercise or daily activities due to shortness of breath IS THERE A CURE FOR? No. Once you have it will never go away and may worsen over time. However, if you take good care of the lung capacity you still have, you can preserve and improve your ability to be active without getting winded. WHAT CAN I DO TO STOP FROM GETTING WORSE? If you smoke, then you must quit! breath with activity and because of this they may avoid activity. Avoiding activity results in a downward cycle of less and less activity which leads to more and more shortness of breath. Shortness of breath with activity More shortness of breath than before Even less activity Be sure to get a flu shot once per year Be sure to get a pneumonia shot once in a lifetime Less activity to avoid feeling short of breath Muscles become weaker from lack of exercise and need more oxygen than normal to do work ASK YOUR DOCTOR TO REFER YOU TO THE CHINOOK HEALTH REGION PROGRAM At the program you will meet with educators who will provide you with information about and how to live well with. They will work with your doctor to reduce the impact of and improve your quality of life. The program provides a supervised exercise program to help people with get fit, improve shortness of breath and ability to exercise. You will also receive a home exercise program to help keep you fit. Revised as of June 21, 2005 developed by the BHL/chronic respiratory/chinook Health Region Smoking is the major cause of. By quitting smoking you can slow the progression of significantly. The sooner you quit the better! If you need help to quit smoking, talk to your doctor or phone toll free the smokers help line: Remember: It is never too late to quit smoking! WHAT CAN BE DONE NOW THAT I HAVE? Breathing medications ( puffers ) that act to open up the air passages can be used to help relieve shortness of breath. Your doctor will prescribe the right combination of breathing medications for you. Exercising and getting in good shape will improve breathlessness. People with commonly become short of Chinook Health Region 21 Reproduced with permission from Boehringer Ingelheim
22 Chinook Health Region 22
23 5. Management Strategies for Patients / Clients Chinook Health Region 23
24 5. Management Strategies for Patients / Clients Chinook Health Region 24
25 5. Management Strategies for Patients / Clients Chinook Health Region 25
26 5. Management Strategies for Patients / Clients Chinook Health Region 26
27 5. Management Strategies for Patients / Clients Chinook Health Region 27
28 5. Management Strategies for Patients / Clients Chinook Health Region 28
29 5. Management Strategies for Patients / Clients Chinook Health Region 29
30 Chinook Health Region 30
31 5. Management Strategies for Patients / Clients 33 Chinook Health Region 31
32 Chinook Health Region 32
33 5. Management Strategies for Patients / Clients Client Checklist for What to expect at each office visit with your family physician: Discuss symptoms such as shortness of breath Discuss current medications and if they are helping symptoms Physical exam (listening to lungs with stethoscope) Checking oxygen levels (if oximeter is available) Discuss smoking (if still smoking) Review proper inhaler technique Make or review a written action plan Tests & Measurements that should be done or discussed on a yearly basis, or as recommended by your family physician: Lung function testing (spirometry) Height and weight measurements Screening for osteoporosis if using inhaled steroids and you have the following risk factors: Age > 60 years Postmenopausal state without hormone replacement therapy Male impotence or infertility Previous fractures with minor trauma Family history of fractures (parental) Past or current chronic glucocorticoid therapy Smoking or alcoholism Physical inactivity Referral to program for education and pulmonary rehabilitation Vaccinations Annual influenza vaccine Pneumonia vaccine (once in a lifetime, or every 10 years) Ensure immunizations are up to date Chinook Health Region 33
34 Chinook Health Region 34
35 6. Referral to Specialists/Specialty Programs 6. Referral to Specialists/Speciality Program a. Indications for Referral to Medical Specialists The symptoms/stages/circumstances that warrant a referral to a medical specialist are: Uncertainty over the diagnosis Symptoms are severe or disproportionate to the level of obstruction on lung function tests There is an accelerated decline in lung function (FEV1.0 decline of 80 ml or more per year over a two year period) The onset of symptoms occurs at a young age (less than 40 years of age) b. Indications for Referral to Speciality Programs Who to refer to a pulmonary rehabilitation program: Clinically stable, symptomatic Reduced activity levels and increased dyspnea despite pharmacological treatment No evidence of active ischemic, musculoskeletal, psychiatric or other systemic disease Sufficient motivation for participation c. Local Contacts For a medical specialist, the primary care physician would have to refer their patient to the medical specialist. An appointment would be made with the medical specialist and the patient would follow up with the specialist at their clinic. To refer to the Lethbridge rehab program: The referral form is completed, signed by a physician and mailed or faxed to Respiratory Therapy Services at LRH, Fax # If the client is accepted into the program, the client will be contacted and required to attend a structured pulmonary rehab program. Rural Educators Taber Telephone Cardston Telephone Magrath Telephone Pincher Creek, Telephone Crowsnest Pass, Telephone Fort Macleod, Telephone Raymond, Telephone Milk River, Telephone Picture Butte, Telephone By contacting or an appointment can be booked for the patient and BHL will notify the appropriate chronic respiratory educator. Clinical Guides are available on-line at: Medical Specialists in the CHR who deal with : Dr. Eric Wilde Dr. Stanley Benke Dr. Chi- Cheong Au Dr. Dave Holland Dr. Gordon Hunt Dr. Ernest Janzen Dr. David Koegler Dr. Richard Schuld Dr. Morley Wong Telephone Fax Respirologist (403) (403) Internal Medicine Internal Medicine Internal Medicine Internal Medicine Internal Medicine Internal Medicine (403) (403) (403) (403) (403) (403) (403) (403) (403) (403) (403) (403) (403) Chinook Health Region 35
36 Chinook Health Region 36
37 7. References 7. References a. Evidence 1. Fletcher, C., & Peto, R. (1977). The Natural History of Chronic Airflow Obstruction. British Medical Journal, 1(16), Lenfant, C., & Khaltaev, N. (1998). MD on behalf of the Global initiative for chronic obstructive lung disease: Global Strategy for the Diagnosis, Management and Prevention of. NHLBI/WHO workshop report, Executive Summary 3. O Donnell, D. E., Aaron, S., Bourbeau, J., et.al. (2003). Canadian Thoracic Society Recommendations for the Management of Chronic Obstructive Pulmonary Disease. Canadian Respiratory Journal, 10 (supplement A): 11A-33A 4. O Donnell, D. S., Hernandez, P., Aaron, S., Bourbeau, J., Marciniuk, D., Hodder, R., Balter, M., Ford, G., Maltais, F., Road, J., McKay, V., & Schenket, J. (2003). Canadian Thoracic Society Guidelines: Summary of Highlights for Family Doctors. Canadian Respiratory Journal, 10(4) 5. West, R., McNeill, A., & Raw, M. (2000). Smoking cessation guidelines for Health Professionals an update. Thorax; 55: b. On-line resources The Lung Association Canadian Thoracic Society & Asthma Network of Alberta National Institute of Health Global Initiative for professional Chinook Health Region 37
Pathway for Diagnosing COPD
 Pathway for Diagnosing Visit 1 Registry Clients at Risk Patient presents with symptoms suggestive of Exertional breathlessness Chronic cough Regular sputum production Frequent bronchitis ; wheeze Occupational
Pathway for Diagnosing Visit 1 Registry Clients at Risk Patient presents with symptoms suggestive of Exertional breathlessness Chronic cough Regular sputum production Frequent bronchitis ; wheeze Occupational
Understanding COPD. Carolinas Healthcare System
 Understanding COPD Carolinas Healthcare System 2013 This self-directed learning module contains information about the pathophysiology, diagnosis, and treatment of COPD. Target Audience: All RNs and LPNs
Understanding COPD Carolinas Healthcare System 2013 This self-directed learning module contains information about the pathophysiology, diagnosis, and treatment of COPD. Target Audience: All RNs and LPNs
Chronic obstructive pulmonary disease (COPD)
 Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
PLAN OF ACTION FOR. Physician Name Signature License Date
 PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
COPD and Asthma Differential Diagnosis
 COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
COPD PROTOCOL CELLO. Leiden
 COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
COPD PROTOCOL CELLO Leiden May 2011 1 Introduction This protocol includes an explanation of the clinical picture, diagnosis, objectives and medication of COPD. The Cello way of working can be viewed on
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
CLINICAL PATHWAY. Acute Medicine. Chronic Obstructive Pulmonary Disease
 CLINICAL PATHWAY Acute Medicine Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of this Pathway 1 Pathway Contacts
CLINICAL PATHWAY Acute Medicine Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease Table of Contents (tap to jump to page) INTRODUCTION 1 Scope of this Pathway 1 Pathway Contacts
medicineupdate to find out more about this medicine
 medicineupdate Asking the right questions about new medicines Seretide for chronic obstructive pulmonary disease What this medicine is 1 What this medicine treats 2 Other medicines available for this condition
medicineupdate Asking the right questions about new medicines Seretide for chronic obstructive pulmonary disease What this medicine is 1 What this medicine treats 2 Other medicines available for this condition
COPD MANAGEMENT PROTOCOL STANFORD COORDINATED CARE
 I. PURPOSE To establish guidelines f the collabative management of patients with a diagnosis of chronic obstructive pulmonary disease (COPD) who are not adequately controlled and to define the roles and
I. PURPOSE To establish guidelines f the collabative management of patients with a diagnosis of chronic obstructive pulmonary disease (COPD) who are not adequately controlled and to define the roles and
Prevention of Acute COPD exacerbations
 December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
COPD. What is COPD? How many people have COPD in Canada? Who gets COPD?
 What is COPD? COPD stands for Chronic Obstructive Pulmonary Disease. It is a long-term lung disease that makes it difficult for air to move into and out of the lungs. COPD is used to describe a few lung
What is COPD? COPD stands for Chronic Obstructive Pulmonary Disease. It is a long-term lung disease that makes it difficult for air to move into and out of the lungs. COPD is used to describe a few lung
Pulmonary Rehabilitation in Newark and Sherwood
 Pulmonary Rehabilitation in Newark and Sherwood With exception of smoking cessation pulmonary rehabilitation is the single most effective intervention for any patient with COPD. A Cochrane review published
Pulmonary Rehabilitation in Newark and Sherwood With exception of smoking cessation pulmonary rehabilitation is the single most effective intervention for any patient with COPD. A Cochrane review published
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Management of exacerbations in chronic obstructive pulmonary disease in Primary Care
 Management of exacerbations in chronic obstructive pulmonary disease in Primary Care Acute exacerbations of chronic obstructive pulmonary disease (COPD) are associated with significant morbidity and mortality.
Management of exacerbations in chronic obstructive pulmonary disease in Primary Care Acute exacerbations of chronic obstructive pulmonary disease (COPD) are associated with significant morbidity and mortality.
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd
 written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are two major diseases included in
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org/copd What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are two major diseases included in
Waterloo Wellington Rehabilitative Care System Integrated Care Pathway for COPD Stream of Care (short version)
 Waterloo Wellington Rehabilitative Care System Integrated Care Pathway for COPD Stream of Care (short version) Care Setting ACUTE Activity Confirmation of COPD diagnoses: If time and the patient s condition
Waterloo Wellington Rehabilitative Care System Integrated Care Pathway for COPD Stream of Care (short version) Care Setting ACUTE Activity Confirmation of COPD diagnoses: If time and the patient s condition
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST...
 YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST... ...HERE S WHAT TO EXPECT You have been referred to an allergist because you have or may have asthma. The health professional who referred you wants you to
YOU VE BEEN REFERRED TO AN ASTHMA SPECIALIST... ...HERE S WHAT TO EXPECT You have been referred to an allergist because you have or may have asthma. The health professional who referred you wants you to
COPD Prescribing Guidelines
 South Staffordshire Area Prescribing Group COPD Prescribing Guidelines Inhaler choices in this guideline are different from previous versions produced by the APG. It is not expected patients controlled
South Staffordshire Area Prescribing Group COPD Prescribing Guidelines Inhaler choices in this guideline are different from previous versions produced by the APG. It is not expected patients controlled
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
RES/006/APR16/AR. Speaker : Dr. Pither Sandy Tulak SpP
 RES/006/APR16/AR Speaker : Dr. Pither Sandy Tulak SpP Definition of Asthma (GINA 2015) Asthma is a common and potentially serious chronic disease that imposes a substantial burden on patients, their families
RES/006/APR16/AR Speaker : Dr. Pither Sandy Tulak SpP Definition of Asthma (GINA 2015) Asthma is a common and potentially serious chronic disease that imposes a substantial burden on patients, their families
Emphysema. Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
COPD. (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community
 COPD (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community Chronic Obstructive Pulmonary Disease (COPD) Definition Chronic obstructive pulmonary disease (COPD)
COPD (Chronic Obstructive Pulmonary Disease) (Emphysema) (Chronic Bronchitis) Education For Our Community Chronic Obstructive Pulmonary Disease (COPD) Definition Chronic obstructive pulmonary disease (COPD)
An Overview of Asthma - Diagnosis and Treatment
 An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
COPD It Can Take Your Breath Away www.patientedu.org
 written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are 2 major diseases included in COPD:
written by Harvard Medical School COPD It Can Take Your Breath Away www.patientedu.org What Is COPD? COPD stands for chronic obstructive pulmonary disease. There are 2 major diseases included in COPD:
These factors increase your chance of developing emphysema. Tell your doctor if you have any of these risk factors:
 Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Medications for Managing COPD in Hospice Patients. Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources
 Medications for Managing COPD in Hospice Patients Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources Goal of medications in COPD Decrease symptoms and/or complications Reduce frequency
Medications for Managing COPD in Hospice Patients Jim Joyner, PharmD, CGP Director of Clinical Operations Outcome Resources Goal of medications in COPD Decrease symptoms and/or complications Reduce frequency
National Learning Objectives for COPD Educators
 National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
National Learning Objectives for COPD Educators National Learning Objectives for COPD Educators The COPD Educator will be able to achieve the following objectives. Performance objectives, denoted by the
The patient s response to therapy within the first hour in the Emergency Room is one of the most reliable ways to predict need for hospitalization.
 Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
COPD. Information brochure for chronic obstructive pulmonary disease.
 COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
FIBROGENIC DUST EXPOSURE
 FIBROGENIC DUST EXPOSURE (ASBESTOS & SILICA) WORKER S MEDICAL SCREENING GUIDELINE Prepared By Dr. T. D. Redekop Chief Occupational Medical Officer Workplace Safety & Health Division Manitoba Labour & Immigration
FIBROGENIC DUST EXPOSURE (ASBESTOS & SILICA) WORKER S MEDICAL SCREENING GUIDELINE Prepared By Dr. T. D. Redekop Chief Occupational Medical Officer Workplace Safety & Health Division Manitoba Labour & Immigration
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Your Go-to COPD Guide
 Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Chronic Obstructive Pulmonary Disease (COPD) Admission Order Set
 Patient Name: PHN: Page 1/1 Admit to Dr: Notified Consult: Dr: Family Dr: Precautions: Contact Droplet Enhanced Droplet Airborne - Reason: _ Code Status: Full Resuscitation or Consults: Reason: Dietician
Patient Name: PHN: Page 1/1 Admit to Dr: Notified Consult: Dr: Family Dr: Precautions: Contact Droplet Enhanced Droplet Airborne - Reason: _ Code Status: Full Resuscitation or Consults: Reason: Dietician
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
IN-HOME QUALITY IMPROVEMENT. BEST PRACTICE: DISEASE MANAGEMENT Chronic Obstructive Pulmonary Disease NURSE TRACK
 IN-HOME QUALITY IMPROVEMENT BEST PRACTICE: DISEASE MANAGEMENT Chronic Obstructive Pulmonary Disease NURSE TRACK Best Practice Intervention Packages were designed for use by any In-Home Provider Agency
IN-HOME QUALITY IMPROVEMENT BEST PRACTICE: DISEASE MANAGEMENT Chronic Obstructive Pulmonary Disease NURSE TRACK Best Practice Intervention Packages were designed for use by any In-Home Provider Agency
COPD Intervention. Components:
 COPD Intervention 1. Primary disease education Member will have an increased understanding of chronic obstructive pulmonary disease, the causes, risks and complications. Explain COPD Explain how COPD is
COPD Intervention 1. Primary disease education Member will have an increased understanding of chronic obstructive pulmonary disease, the causes, risks and complications. Explain COPD Explain how COPD is
COPD RESOURCE PACK SECTION 11. Fife Integrated COPD Care Pathways
 COPD RESOURCE PCK SECTION 11 Fife Integrated COPD Care Pathways In this section: 1. COPD Guidance treatment at each stage of the disease 2. Overview of Respiratory (COPD) Integrated Pathway 3. Chronic
COPD RESOURCE PCK SECTION 11 Fife Integrated COPD Care Pathways In this section: 1. COPD Guidance treatment at each stage of the disease 2. Overview of Respiratory (COPD) Integrated Pathway 3. Chronic
Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD)
 Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD) Development of disability in COPD The decline in airway function may initially go unnoticed as people adapt their lives to avoid
Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD) Development of disability in COPD The decline in airway function may initially go unnoticed as people adapt their lives to avoid
Chronic Obstructive Pulmonary Disease Patient Guidebook
 Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD)
 Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma
 Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
Guidance to support the stepwise review of combination inhaled corticosteroid therapy for adults ( 18yrs) in asthma Important Complete asthma control needs to be achieved for at least 12 weeks before attempting
Idiopathic Pulmonary Fibrosis
 Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops
 PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY
 GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
Clinical Guideline. Recommendation 3: For stable COPD patients with respiratory symptoms
 Clinical Guideline Diagnosis and Management of Stable Chronic Obstructive Pulmonary Disease: A Clinical Practice Guideline Update from the American College of Physicians, American College of Chest Physicians,
Clinical Guideline Diagnosis and Management of Stable Chronic Obstructive Pulmonary Disease: A Clinical Practice Guideline Update from the American College of Physicians, American College of Chest Physicians,
Exploring the Chronic Obstructive Pulmonary Disease (COPD) Clinical Pathway. Health Quality Ontario s integrated episode of care for COPD
 Exploring the Chronic Obstructive Pulmonary Disease (COPD) Clinical Pathway Health Quality Ontario s integrated episode of care for COPD Dr. Charlie Chan Health Quality Ontario Expert Panel Co-Chair May/June
Exploring the Chronic Obstructive Pulmonary Disease (COPD) Clinical Pathway Health Quality Ontario s integrated episode of care for COPD Dr. Charlie Chan Health Quality Ontario Expert Panel Co-Chair May/June
Understanding COPD. An educational health series from
 Understanding COPD An educational health series from Our Mission since 1899 is to heal, to discover, and to educate as a preeminent healthcare institution. We serve by providing the best integrated and
Understanding COPD An educational health series from Our Mission since 1899 is to heal, to discover, and to educate as a preeminent healthcare institution. We serve by providing the best integrated and
Clinical Guideline. Recommendation 3: For stable COPD patients with respiratory symptoms
 Clinical Guideline Diagnosis and Management of Stable Chronic Obstructive Pulmonary Disease: A Clinical Practice Guideline Update from the American College of Physicians, American College of Chest Physicians,
Clinical Guideline Diagnosis and Management of Stable Chronic Obstructive Pulmonary Disease: A Clinical Practice Guideline Update from the American College of Physicians, American College of Chest Physicians,
COPD - Education for Patients and Carers Integrated Care Pathway
 Patient NHS COPD - Education for Patients and Carers Integrated Care Pathway Date ICP completed:. Is the patient following another Integrated Care Pathway[s].. / If yes, record which other Integrated Care
Patient NHS COPD - Education for Patients and Carers Integrated Care Pathway Date ICP completed:. Is the patient following another Integrated Care Pathway[s].. / If yes, record which other Integrated Care
Pharmacology of the Respiratory Tract: COPD and Steroids
 Pharmacology of the Respiratory Tract: COPD and Steroids Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Pharmacology of the Respiratory Tract: COPD and Steroids Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
AECOPD: Management and Prevention
 AECOPD: Management and Prevention Neil MacIntyre MD Duke University Medical Center Durham NC AECOPD: Management and Prevention AECOPD: Definitions and impact Acute management of AECOPD Preventing AECOPD.
AECOPD: Management and Prevention Neil MacIntyre MD Duke University Medical Center Durham NC AECOPD: Management and Prevention AECOPD: Definitions and impact Acute management of AECOPD Preventing AECOPD.
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Documenting & Coding. Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC
 Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Chronic Obstructive Pulmonary Disease
 COPD Guideline Team Team Leader Davoren A Chick, MD General Medicine Team Members Paul J Grant, MD General Medicine Meilan K Han, MD, MS Pulmonary Medicine R Van Harrison, PhD Medical Education Elisa B
COPD Guideline Team Team Leader Davoren A Chick, MD General Medicine Team Members Paul J Grant, MD General Medicine Meilan K Han, MD, MS Pulmonary Medicine R Van Harrison, PhD Medical Education Elisa B
PTE Pediatric Asthma Metrics Reporting Updated January 2015
 PTE Pediatric Asthma Metrics Reporting Updated January 20 Introduction: The Maine Health Management Coalition s (MHMC) Pathways to Excellence (PTE) Program is preparing for its next round of PTE Pediatric
PTE Pediatric Asthma Metrics Reporting Updated January 20 Introduction: The Maine Health Management Coalition s (MHMC) Pathways to Excellence (PTE) Program is preparing for its next round of PTE Pediatric
Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines.
 Formulary Guidance for Management of COPD patients Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines. For inhaler
Formulary Guidance for Management of COPD patients Before prescribing for COPD management, the patient should have had appropriate assessment, including spirometry, as per NICE guidelines. For inhaler
Pulmonary Disorders. Chronic Obstructive Pulmonary Disease (COPD) Chronic Obstructive Pulmonary Disease (COPD)
 RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Pulmonary Disorders Chronic Obstructive Pulmonary Disease (COPD) Characterized by decreased expiratory airflow Reduction in expiratory
RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Pulmonary Disorders Chronic Obstructive Pulmonary Disease (COPD) Characterized by decreased expiratory airflow Reduction in expiratory
Global Initiative for Chronic Obstructive Lung Disease
 Global Initiative for Chronic Obstructive Lung Disease POCKET GUIDE TO COPD DIAGNOSIS, MANAGEMENT, AND PREVENTION A Guide for Health Care Professionals REVISED 2011 Global Initiative for Chronic Obstructive
Global Initiative for Chronic Obstructive Lung Disease POCKET GUIDE TO COPD DIAGNOSIS, MANAGEMENT, AND PREVENTION A Guide for Health Care Professionals REVISED 2011 Global Initiative for Chronic Obstructive
Pre-Operative Services Teaching Rounds 2 Jan 2011
 Pre-Operative Services Teaching Rounds 2 Jan 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Pre-Operative Services Teaching Rounds 2 Jan 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
understanding the professional guidelines
 SEVERE ASTHMA understanding the professional guidelines This guide includes information on what the European Respiratory Society (ERS) and the American Thoracic Society (ATS) have said about severe asthma.
SEVERE ASTHMA understanding the professional guidelines This guide includes information on what the European Respiratory Society (ERS) and the American Thoracic Society (ATS) have said about severe asthma.
Clinical guideline Published: 23 June 2010 nice.org.uk/guidance/cg101
 Chronic obstructive pulmonary disease in over 16s: diagnosis and management Clinical guideline Published: 23 June 2010 nice.org.uk/guidance/cg101 NICE 2010. All rights reserved. Your responsibility The
Chronic obstructive pulmonary disease in over 16s: diagnosis and management Clinical guideline Published: 23 June 2010 nice.org.uk/guidance/cg101 NICE 2010. All rights reserved. Your responsibility The
Understanding and Controlling Asthma Attacks. Information for parents
 Understanding and Controlling Asthma Attacks Information for parents Your child was recently seen by a doctor for asthma. This guide will help you gain a better understanding about your child's recent
Understanding and Controlling Asthma Attacks Information for parents Your child was recently seen by a doctor for asthma. This guide will help you gain a better understanding about your child's recent
NEWS NP S. Inside. Defining COPD. Is it COPD? National Prescribing Service Newsletter
 NP S NEWS National Prescribing Service Newsletter 5 1999 ISSN 1441-7421 Aug 99 Inside Bronchodilators and corticosteroids: Their use in COPD Give it up the best advice for COPD patients: NRT can help This
NP S NEWS National Prescribing Service Newsletter 5 1999 ISSN 1441-7421 Aug 99 Inside Bronchodilators and corticosteroids: Their use in COPD Give it up the best advice for COPD patients: NRT can help This
Tests. Pulmonary Functions
 Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Bronchodilators in COPD
 TSANZSRS Gold Coast 2015 Can average outcomes in COPD clinical trials guide treatment strategies? Long live the FEV1? Christine McDonald Dept of Respiratory and Sleep Medicine Austin Health Institute for
TSANZSRS Gold Coast 2015 Can average outcomes in COPD clinical trials guide treatment strategies? Long live the FEV1? Christine McDonald Dept of Respiratory and Sleep Medicine Austin Health Institute for
Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age
 Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age Components of Severity Symptoms Intermittent 2 days/week Classification of Asthma Severity (0 4 years of age) Persistent
Classifying Asthma Severity and Initiating Treatment in Children 0 4 Years of Age Components of Severity Symptoms Intermittent 2 days/week Classification of Asthma Severity (0 4 years of age) Persistent
Sponsor Novartis Pharmaceuticals
 Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Generic Drug Name Indacaterol Therapeutic Area of Trial Chronic Obstructive Pulmonary Disease (COPD) Indication studied: COPD Study
Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Generic Drug Name Indacaterol Therapeutic Area of Trial Chronic Obstructive Pulmonary Disease (COPD) Indication studied: COPD Study
Objectives COPD. Chronic Obstructive Pulmonary Disease (COPD) 4/19/2011
 Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Interpretation of Pulmonary Function Tests
 Interpretation of Pulmonary Function Tests Dr. Sally Osborne Cellular & Physiological Sciences University of British Columbia Room 3602, D.H Copp building 604 822-3421 sally.osborne@ubc.ca www.sallyosborne.com
Interpretation of Pulmonary Function Tests Dr. Sally Osborne Cellular & Physiological Sciences University of British Columbia Room 3602, D.H Copp building 604 822-3421 sally.osborne@ubc.ca www.sallyosborne.com
Global Strategy for the Diagnosis, Management and Prevention of Chronic Obstructive Pulmonary Disease
 Page 1 of 67 AJRCCM Articles in Press. Published on August 9, 2012 as doi:10.1164/rccm.201204-0596pp GOLD Executive Summary Global Strategy for the Diagnosis, Management and Prevention of Chronic Obstructive
Page 1 of 67 AJRCCM Articles in Press. Published on August 9, 2012 as doi:10.1164/rccm.201204-0596pp GOLD Executive Summary Global Strategy for the Diagnosis, Management and Prevention of Chronic Obstructive
David J. Lederer, MD, MS
 COPD: Definition Chronic Obstructive Pulmonary Disease Chronic airflow obstruction due to chronic bronchitis and/or pulmonary emphysema David J. Lederer, MD, MS Associate Medical Director, Lung Transplant
COPD: Definition Chronic Obstructive Pulmonary Disease Chronic airflow obstruction due to chronic bronchitis and/or pulmonary emphysema David J. Lederer, MD, MS Associate Medical Director, Lung Transplant
HEALTH CARE FOR EXPOSURE TO ASBESTOS. 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.
 HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
Asthma Intervention. An Independent Licensee of the Blue Cross and Blue Shield Association.
 Asthma Intervention 1. Primary disease education Member will have an increased understanding of asthma and the classification by severity, the risks and the complications. Define asthma Explain how lungs
Asthma Intervention 1. Primary disease education Member will have an increased understanding of asthma and the classification by severity, the risks and the complications. Define asthma Explain how lungs
Insights for Improvement: Advancing COPD Care Through Quality Measurement. An NCQA Insights for Improvement Publication
 2009 Insights for Improvement: Advancing COPD Care Through Quality Measurement An NCQA Insights for Improvement Publication Chronic obstructive pulmonary disease (COPD) includes chronic bronchitis, emphysema,
2009 Insights for Improvement: Advancing COPD Care Through Quality Measurement An NCQA Insights for Improvement Publication Chronic obstructive pulmonary disease (COPD) includes chronic bronchitis, emphysema,
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD
 Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Irish Association for Emergency Medicine (IAEM) submission to the National COPD Strategy
 31 st Irish Association for Emergency Medicine (IAEM) submission to the National COPD Strategy 1 Introduction Chronic obstructive pulmonary disease (COPD) is an important disease for patients, the health
31 st Irish Association for Emergency Medicine (IAEM) submission to the National COPD Strategy 1 Introduction Chronic obstructive pulmonary disease (COPD) is an important disease for patients, the health
To provide standardized Supervised Exercise Programs across the province.
 TITLE ALBERTA HEALTHY LIVING PROGRAM SUPERVISED EXERCISE PROGRAM DOCUMENT # HCS-67-01 APPROVAL LEVEL Executive Director Primary Health Care SPONSOR Senior Consultant Central Zone, Primary Health Care CATEGORY
TITLE ALBERTA HEALTHY LIVING PROGRAM SUPERVISED EXERCISE PROGRAM DOCUMENT # HCS-67-01 APPROVAL LEVEL Executive Director Primary Health Care SPONSOR Senior Consultant Central Zone, Primary Health Care CATEGORY
Drug therapy SHORT-ACTING BETA AGONISTS SHORT-ACTING ANTICHOLINERGICS LONG-ACTING BETA AGONISTS LONG-ACTING ANTICHOLINERGICS
 Drug therapy 6 6.1 What is the role of bronchodilators in COPD? 52 SHORT-ACTING BETA AGONISTS 6.2 How do short-acting beta agonists work? 52 6.3 What are the indications for their use? 52 6.4 What is the
Drug therapy 6 6.1 What is the role of bronchodilators in COPD? 52 SHORT-ACTING BETA AGONISTS 6.2 How do short-acting beta agonists work? 52 6.3 What are the indications for their use? 52 6.4 What is the
EMPHYSEMA THERAPY. Information brochure for valve therapy in the treatment of emphysema.
 EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
Respiratory Concerns in Children with Down Syndrome
 Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Coding Guidelines for Certain Respiratory Care Services July 2014
 Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Population Health Management Program
 Population Health Management Program Program (formerly Disease Management) is dedicated to improving our members health and quality of life. Our Population Health Management Programs aim to improve care
Population Health Management Program Program (formerly Disease Management) is dedicated to improving our members health and quality of life. Our Population Health Management Programs aim to improve care
Breathe With Ease. Asthma Disease Management Program
 Breathe With Ease Asthma Disease Management Program MOLINA Breathe With Ease Pediatric and Adult Asthma Disease Management Program Background According to the National Asthma Education and Prevention Program
Breathe With Ease Asthma Disease Management Program MOLINA Breathe With Ease Pediatric and Adult Asthma Disease Management Program Background According to the National Asthma Education and Prevention Program
KIH Cardiac Rehabilitation Program
 KIH Cardiac Rehabilitation Program For any further information Contact: +92-51-2870361-3, 2271154 Feedback@kih.com.pk What is Cardiac Rehabilitation Cardiac rehabilitation describes all measures used to
KIH Cardiac Rehabilitation Program For any further information Contact: +92-51-2870361-3, 2271154 Feedback@kih.com.pk What is Cardiac Rehabilitation Cardiac rehabilitation describes all measures used to
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
1 ALPHA-1. What is Alpha-1? A family history... of lung disease? of liver disease? FOUNDATION
 What is Alpha-1? A family history... of lung disease? of liver disease? What you need to know about Alpha-1 Antitrypsin Deficiency 1 ALPHA-1 FOUNDATION What is Alpha-1? Alpha-1 Antitrypsin Deficiency (Alpha-1)
What is Alpha-1? A family history... of lung disease? of liver disease? What you need to know about Alpha-1 Antitrypsin Deficiency 1 ALPHA-1 FOUNDATION What is Alpha-1? Alpha-1 Antitrypsin Deficiency (Alpha-1)
Background information
 Background information Asthma Asthma is a complex disease affecting the lungs that can be managed but cannot be cured. 1 Asthma can be controlled well in most people most of the time, although some people
Background information Asthma Asthma is a complex disease affecting the lungs that can be managed but cannot be cured. 1 Asthma can be controlled well in most people most of the time, although some people
Understanding Pulmonary Function Testing. PFTs, Blood Gases and Oximetry Skinny Little Reference Guide
 Understanding Pulmonary Function Testing PFTs, Blood Gases and Oximetry Skinny Little Reference Guide INTRODUCTION This brochure is intended to help you understand the meaning of Pulmonary Function Testing,
Understanding Pulmonary Function Testing PFTs, Blood Gases and Oximetry Skinny Little Reference Guide INTRODUCTION This brochure is intended to help you understand the meaning of Pulmonary Function Testing,
COPD with Respiratory Failure Case Study #21. Molly McDonough
 COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
Prof. Florian Gantner. Vice President Respiratory Diseases Research Boehringer Ingelheim
 Prof. Florian Gantner Vice President Respiratory Diseases Research Boehringer Ingelheim Research and Development in Practice: COPD Chronic Obstructive Pulmonary Disease (COPD) Facts Main cause of COPD
Prof. Florian Gantner Vice President Respiratory Diseases Research Boehringer Ingelheim Research and Development in Practice: COPD Chronic Obstructive Pulmonary Disease (COPD) Facts Main cause of COPD
Chronic obstructive pulmonary disease: Management of adults with chronic obstructive pulmonary disease in primary and secondary care
 Chronic obstructive pulmonary disease: Management of adults with chronic obstructive pulmonary disease in primary and secondary care NICE guideline First draft for consultation, September 2003 If you wish
Chronic obstructive pulmonary disease: Management of adults with chronic obstructive pulmonary disease in primary and secondary care NICE guideline First draft for consultation, September 2003 If you wish
Breathless The Whys and Wherefores Living with Alpha-1-Antitrypsin Deficiency
 Breathless The Whys and Wherefores Living with Deficiency Patient Information Program Breathlessness Short of breath after running the marathon? Short of breath after climbing a flight of stairs? Short
Breathless The Whys and Wherefores Living with Deficiency Patient Information Program Breathlessness Short of breath after running the marathon? Short of breath after climbing a flight of stairs? Short
Smoking Cessation Program
 Smoking Cessation Program UHN Information for people who are ready to quit smoking Read this information to learn: why you should quit smoking how the Smoking Cessation Program works treatments to help
Smoking Cessation Program UHN Information for people who are ready to quit smoking Read this information to learn: why you should quit smoking how the Smoking Cessation Program works treatments to help
F r e q u e n t l y As k e d Qu e s t i o n s. Lung Disease
 Lung Disease page 1 Q: What is lung disease? A: Lung disease refers to disorders that affect the lungs, the organs that allow us to breathe. Breathing problems caused by lung disease may prevent the body
Lung Disease page 1 Q: What is lung disease? A: Lung disease refers to disorders that affect the lungs, the organs that allow us to breathe. Breathing problems caused by lung disease may prevent the body
Chronic obstructive pulmonary disease
 12 Chronic obstructive pulmonary disease Anna Murphy Case study and questions Day 1 Mr LT, a 68-year-old man, attended his general practitioner s (GP s) surgery for a routine check-up. He had been diagnosed
12 Chronic obstructive pulmonary disease Anna Murphy Case study and questions Day 1 Mr LT, a 68-year-old man, attended his general practitioner s (GP s) surgery for a routine check-up. He had been diagnosed
Living Well With COPD Chronic Bronchitis and Emphysema
 Living Well With COPD Chronic Bronchitis and Emphysema Your Patient workbook AMERICAN COLLEGE OF CHEST PHYSICIANS AND THE CHEST FOUNDATION Living Well With COPD Chronic Bronchitis and Emphysema your patient
Living Well With COPD Chronic Bronchitis and Emphysema Your Patient workbook AMERICAN COLLEGE OF CHEST PHYSICIANS AND THE CHEST FOUNDATION Living Well With COPD Chronic Bronchitis and Emphysema your patient
Asthma. Micah Long, MD
 Asthma Micah Long, MD Goals Define the two components of asthma. Describe the method of action and uses for: Steroids (inhaled and IV) Quick Beta Agonists (Nebs and MDIs) The "Others" Magnesium, Epi IM,
Asthma Micah Long, MD Goals Define the two components of asthma. Describe the method of action and uses for: Steroids (inhaled and IV) Quick Beta Agonists (Nebs and MDIs) The "Others" Magnesium, Epi IM,
