Furcation defects present difficult treatment problems,
|
|
|
- Eleanore Flynn
- 7 years ago
- Views:
Transcription
1 Volume 75 Number 9 A Randomized Clinical Trial Comparing Enamel Matrix Derivative and Membrane Treatment of Buccal Class II Furcation Involvement in Mandibular Molars. Part II: Secondary Outcomes Jörg Meyle,* José R. Gonzales,* Rolf H. Bödeker, Thomas Hoffmann, Steffen Richter, Bernd Heinz, Mehrdad Arjomand, Elmar Reich, Anton Sculean, Karin Jepsen, and Søren Jepsen Background: This multicenter, randomized trial compared enamel matrix derivative (EMD) with barrier membranes for the treatment of Class II mandibular furcations with regard to secondary outcomes. The influence of furcation morphology on the effectiveness of either treatment was also evaluated. Methods: Forty-eight patients (age range 28 to 73 years; 22 females, 26 males) with buccal Class II furcation involvements in both contralateral lower first or second molars were included. After initial periodontal treatment, defects were randomized to either EMD or bioabsorbable guided tissue regeneration (GTR) barrier. Study design and the results for the primary parameter were previously described. Results of the following secondary outcome variables are reported here: changes of the hard tissue boundaries describing the anatomical situation of the furcation defect and changes in the following clinical parameters between baseline and 14 months: plaque, level of gingival margin, probing depth, bleeding on probing, attachment level, and bone sounding at five sites/tooth at the buccal side. Descriptive statistics were applied for changes in clinical parameters and measurements of hard tissue boundaries. The differences observed under treatment with EMD or membrane were analyzed by means of the Wilcoxon two-sample test. The difference between the effect of the EMD and membrane treatment was estimated by means of the Hodges-Lehmann estimator. Results: Overall, similar healing results were observed for both treatments. However, there was slightly more recession in the mid-furcation site following membrane treatment (P = 0.04). Additionally, different treatment effects could be detected for the distances from the stent or cemento-enamel junction (CEJ) to the buccal bone crest, mid-distal root (P stent = 0.01; P CEJ = 0.07) and for the distance from the stent or CEJ to the buccal bone crest, mid-mesial root (P stent = 0.01; P CEJ = 0.01). There was no measurable bone resorption in EMD sites, whereas a slight resorption occurred with membrane treatment. Furcation morphology at the time of surgery was not associated with clinical outcome, irrespective of the treatment. Conclusion: With regard to secondary outcome parameters, enamel matrix derivative treatment led to a similar regenerative result as the membrane procedure. J Periodontol 2004;75: KEY WORDS Comparison studies; furcation/surgery; furcation/therapy; guided tissue regeneration; membranes, barrier; proteins, enamel matrix; statistical distribution. * Department of Periodontology, University of Giessen, Giessen, Germany. Department of Statistics, University of Giessen. Department of Periodontology, University of Dresden, Dresden, Germany. Private practice, Hamburg, Germany. Department of Periodontology, University of Homburg, Homburg, Germany. Department of Periodontology, University of Bonn, Bonn, Germany. 1188
2 J Periodontol September 2004 Meyle, Gonzales, Bödeker, et al. Furcation defects present difficult treatment problems, mostly due to the complexity of the furcation morphology. Specifically, in Class II mandibular furcations, several treatment approaches to obtain furcation fill have been used with varying success. They include coronally repositioned flaps, bone replacement grafts, guided tissue regeneration (GTR), or a combination of therapies. 1-7 To date, there is consensus that GTR procedures have resulted in significant gains in clinical attachment levels (AL) both horizontally and vertically in mandibular Class II furcations. 8 Initially, GTR was carried out using a non-resorbable expanded polytetraflouroethylene membrane, alone or in combination with bone grafts In order to remove non-resorbable membranes, though, a second surgery is necessary. Therefore, bioabsorbable barriers have been introduced, either alone or in combination with bone grafts or other graft materials. 13 However, the great variability of clinical outcomes that has been shown for regenerative procedures for furcation defects remains a problem in periodontal therapy. The available scientific information does not clearly indicate the real impact of these therapeutic procedures on the final outcome and prognosis of the affected tooth and patient. 14 The identification of the role of enamel matrix derivatives # (EMD) in the formation of the cementum led to the development of a biological concept for periodontal regeneration. 15 Subsequently, clinical studies in humans and animals, as well as histological research, have shown that the application of EMD leads to the formation of a new connective tissue attachment and new alveolar bone Predominantly, 1- and 2-wall intrabony defects treated with EMD have been reported in the literature. Different mean values for clinical AL gain have been demonstrated, ranging between 1.5 mm and approximately 6 mm, and similar results have been shown for radiographic bone gains. 22,23 Additionally, periodontal regeneration of angular bony defects using EMD has proved to be at least equally effective in terms of probing depth (PD) reduction and AL gain in comparison with different regenerative modalities using barrier membranes. 24 Thus, EMD has been used as an alternative to bone grafts and barrier membranes in the treatment of intrabony defects. 16,25,26 More recently, EMD has been combined with other graft materials, such as bovine-derived bone mineral and bioactive glass. 27,28 There is a lack of data on the effects of EMD in the treatment of periodontal furcation defects. Recently, a multi-center study was conducted to assess the effectiveness of EMD treatment in buccal Class II furcation defects in mandibular molars, and to compare the efficacies of treatment with EMD and a bioabsorbable GTR barrier.** 29 The authors reported a significant clinical improvement obtained with both treatments in the perprotocol (PP) population. The median of the reduction of open horizontal furcation depth was 2.8 mm (interquartile interval: 1.5 mm, 3.5 mm) at sites treated with EMD, compared with 1.8 mm (interquartile interval: 1.0 mm, 2.8 mm) at sites treated with bioabsorbable membrane. Thus, treatment with EMD resulted in more horizontal depth reduction than with the membrane treatment (Hodges-Lehmann estimator: 0.75 mm; 95% confidence interval [CI]: to mm; P = 0.033, Wilcoxon). In addition, secondary outcomes, i.e., hard tissue boundaries and clinical parameters for evaluation of the regeneration of the furcation defects, were studied. Here we report the changes in these parameters. An additional aim was the analysis of the influence of furcation morphology on the effectiveness of either treatment. MATERIALS AND METHODS Study Design The present randomized, examiner-masked, multicenter study had a split-mouth design. Five independent centers participated. The study design included a previous calibration of all investigators and examiners. The examiners, who performed all the clinical assessments at the treated sites, were treatment-masked. Details of the study design have previously been described. 29 Briefly, having met the criteria for inclusion and after giving informed consent, a total of 48 patients (22 females, 26 males) with buccal Class II furcation involvements in both contralateral lower first or second molars were included (horizontal probing depth >3 mm, measured with the Nabers probe). Initial periodontal treatment was performed, to ensure that all patients presented full-mouth plaque and gingival bleeding scores of <25% at the beginning of the active treatment phase. Subsequently, patients were randomized to receive one of two surgical procedures, either EMD or bioabsorbable GTR barrier in the first surgery. Surgeries started with the left side, and continued with the alternative treatment on the right side within 2 to 6 weeks. Assignment of treatment with EMD or membrane was not revealed to the surgeon until the flap was reflected and the root surfaces were debrided. The clinical study was completed after a reentry surgery 14 months later. Clinical Parameters The primary outcome of the study was the change in horizontal furcation depth, determined by measuring the depth of the furcation defect at the deepest point (Fig. 1, parameter h) during the first surgery (baseline) and during the reentry surgery. Additionally, several secondary parameters were recorded. These included # Emdogain, Straumann Biologics Division, Waltham, MA (formerly Biora AB, Malmö, Sweden). ** Resolut, W.L. Gore & Associates, Inc., Flagstaff, AZ. 1189
3 Comparison of Enamel Matrix Derivative and Membranes for Furcation Therapy Volume 75 Number 9 measurements of the hard tissue boundaries describing the anatomical situation of the furcation defect and the following clinical parameters: level of gingival margin (GM), probing depth (PD), attachment level (AL), and bone sounding (BS) at five sites/tooth on the buccal side: mesio-buccal, mid-mesial root, mid-furcation, middistal root and disto-buccal. Bleeding on probing (BOP) observed during PD measurement was also reported. In order to assess oral hygiene status, modified fullmouth plaque and site plaque indices were determined. Both indices were based on determination of the presence or absence of disclosed plaque. The hard tissue boundaries in the furcation defects and the clinical parameters were measured twice, using as reference the cemento-enamel junction (CEJ) and an individually manufactured acrylic stent with grooves at five sites, as previously described. 29 Measurements were recorded using a standard periodontal probe (UNC-15) and rounded to the nearest 0.5 mm. Some of these parameters were measured during follow-up appointments at 1, 3, 6, and 8 to 12 weeks and at 3, 6, and 8 months. Additionally, parameters describing adverse reactions during the study were recorded using special questionnaires (objective and subjective adverse events). Smoking status was also assessed; however, smokers were not excluded from the study. Data Analysis The study was designed both to assess the effectiveness of EMD treatment and to compare the effectiveness of EMD treatment with membrane treatment. As 1190 Figure 1. Intrasurgical measurements of hard tissue boundaries: a = interproximal bone crest, distal; b = buccal bone crest, mid-distal root; c = bone crest of defect, mid-furcation; d = buccal bone crest, mid-mesial root; e = interproximal bone crest, mesial; f = fornix to bone crest of defect; g = width of defect at the bottom of the defect; h = horizontal depth of furcation; i = bottom of the defect. All measurements were made twice, from the cemento-enamel junction and the stent, with the exception of parameters h and i. 29 explained in detail by Jepsen et al., three populations were determined for the analyses: the safety population, the intention-to-treat (ITT) population, and the PP population. 29 The number and characteristics of the patients included in each group, as well as the results of the primary parameter h have been described. 29 In the current paper, the results of the secondary parameters are reported, using the ITT population. Descriptive statistical methods were applied to the parameters of interest and the results were tabulated separately for sequence and/or treatment. First, the homogeneity of the clinical parameters was tested. The Wilcoxon two-sample test was used for the continuous variables and Fisher s exact test was used for the discrete variables. According to the study protocol, the statistical analysis was designed with the objective of demonstrating the effectiveness of each therapy, i.e., the difference or change in the measurements of the clinical parameters (GM, PD, AL, BS) and the measurements of the hard tissue boundaries (shown in Figure 1) between the baseline and the reentry surgeries. For the continuous parameters, the assumption of normal distribution could not be held. The distribution was described by minimum, first quartile, median, third quartile, and maximum and particular sizes were computed for the different locations (mesio-buccal, mid-mesial root, mid-furcation, middistal root and disto-buccal). In accordance with the study design, statistical tests were also performed. Thus, the differences in the distributions of the parameters either under treatment with EMD or membrane were analyzed by means of the Wilcoxon two-sample test. However, the computed P value is only a measure of the distance of the observed value to that expected under the assumption that both samples were drawn from the same population. This means that the greater the P value, the more likely the assumption that both samples were drawn from the same population. Additionally, in order to estimate the difference between the effects of the EMD and membrane treatments, an estimator (Hodges-Lehmann) associated with Wilcoxon s rank sum statistics and the related distribution-free confidence interval, also based on Wilcoxon s rank sum statistics, was computed. The computed P values of the statistical tests, however, have to be interpreted in a descriptive manner. They are a measure of how the observed data differ from that expected under the assumption of no different treatment effect.
4 J Periodontol September 2004 Meyle, Gonzales, Bödeker, et al. Additionally, the influence of furcation morphology on the effectiveness of either treatment was determined. This was performed by analyzing the possible associations between the baseline measurements of the hard tissue boundaries that assessed the alveolar bone levels (Fig. 1, parameters a, c, and e), the morphology of the furcation (parameters f and g) and depth (parameter i) with the parameters describing the effectiveness of treatment based on the changes in clinical outcomes, such as PD reduction and AL gains (in the mid-furcation site), and change in horizontal and vertical furcation depth (parameters h and i). As the assumption of normal distribution could not be made, a non-parametric Spearman s correlation coefficient test was used. Analysis was carried out using a statistical software program. In order to obtain exact estimators for the treatment effects, a second software program was also used. Figure 2. Frequency of BOP in mid-furcation sites. Percentages refer to total number of patients (N = 47). Figure 3. Mean reduction of full-mouth plaque index. Percentages refer to total number of patients (N = 47). RESULTS The results presented here are those relating to the secondary clinical parameters (GM, PD, AL, BS, and BOP) and the hard tissue boundaries (Fig. 1). The ITT population consisted of 48 patients (22 females, 26 males) with a median age of 54 years (range 28 to 73 years). As a result of missing values, the sample size may differ slightly for the various analyses of secondary variables. The patients were randomly assigned to one of two treatment sequences: left EMD right membrane (LE RM; N = 21) and left membrane right EMD (LM RE; N = 27). Ten patients were active smokers: six in the LE RM group and four in the LM RE group. No indication for the rejection of the assumption of homogeneity could be found for the parameters measured before or during surgery. The median reduction of PD in the mid-furcation site changed from 3.5 mm at baseline to 3.0 mm after 14 months in sites treated with EMD, and in membrane treated sites from 3.25 mm to 3.0 mm. The median reduction of AL in the mid-furcation site changed from 7.5 mm at baseline to 7.0 mm after 14 months with EMD treatment, and from 7.38 mm to 7.0 mm with membrane treatment. A reduction in the frequency of BOP in the midfurcation site was determined with both treatments, changing from approximately 40% at the beginning of treatment to 21.3% (EMD) and 23.4% (membrane) after 8 months (Fig. 2). However, after 14 months, a further reduction of BOP was shown only with EMD treatment (10.6%) and not with membrane treatment (25.5%). A reduction in the full-mouth plaque index was also demonstrated with both treatments, changing from approximately 16% after 2 months to 12% after 14 months (Fig. 3). In contrast, a slight increase in the frequency of site plaque in the mid-furcation site was registered for both treatments during the study, from 14.9% (EMD) and 10.4% (membrane) in the second month, to 17% and 25.5%, respectively, after 8 months. However, after 14 months, a slight reduction of site plaque (12.8%) was shown only for the teeth treated with EMD (Fig. 4). The results of the changes in the clinical parameters between treatments are summarized in Table 1. No significant differences after 14 months between treatment with EMD and with membrane at the mesio-buccal, mid-mesial root, mid-distal root, and disto-buccal sites SAS Version 8.01, SAS Institute Inc., Cary, NC. StatXact Version for Windows, CYTEL Software Corporation, Cambridge, MA. 1191
5 Comparison of Enamel Matrix Derivative and Membranes for Furcation Therapy Volume 75 Number 9 Figure 4. Frequency of site plaque in the mid-furcation site. Percentages refer to total number of patients (N = 47). Figure 5. Distribution of the change in the level of gingival margin (GM) measured from the stent to the mid-furcation site, separated by treatment and side.the box contains 50% of the data around the median.the vertical lines extending from the box mark the lowest and the highest value except the outliers. Negative values indicate gingival recession. Table 1. Estimators of the Differences in Changes in Clinical Parameters With EMD or Membrane Hodges-Lehmann Variable Location Estimator* 95% CI P Value Level of gingival margin Mesio-buccal to Mid-mesial root to Mid-furcation to Mid-distal root to Disto-buccal to Probing depth Mesio-buccal to Mid-mesial root to Mid-furcation to Mid-distal root to Disto-buccal to Attachment level Mesio-buccal to Mid-mesial root to Mid-furcation to Mid-distal root to Distobuccal to Bone sounding Mesiobuccal to Mid-mesial root to Mid-furcation to Mid-distal root to Distobuccal to *Estimator of (X EMD,surgery X EMD,reentry ) (X Membrane,surgery X Membrane,reentry ). Wilcoxon two-sample test. Measured from the stent. Clinical and statistically relevant differences. were found. However, an indication of different effects could be detected for the distance from the stent to the GM level in the mid-furcation site (P = 0.04). Figure 5 illustrates the distribution of change in this parameter in the form of box plots. The median change was 0.13 mm and 0 mm (left and right sides, respectively) with EMD treatment, and 0.5 mm with the membrane (both sides). The results of the changes in the hard tissue boundaries between treatments are summarized in Table 2. Different treatment effects were found for the distance from the stent or CEJ to the buccal bone crest, mid-distal root (Figure 1, parameter b) (P stent = 0.01; P CEJ = 0.07). The median change was 0 mm (both sides) with EMD treatment, and 0.5 mm and 0.25 mm (left and right sides, respectively) with the membrane (Fig. 6). Similar results were found for the distance from the stent or CEJ to the buccal bone crest, mid-mesial root (Figure 1, parameter d) (P stent = 0.01; P CEJ = 0.01). In this case, the median change was 0.25 mm and 0 mm (left and right sides, respectively) with EMD, and 0.63 mm and 0.75 mm (left and right sides, respectively) with the membrane (Fig. 7). This demonstrates that the differences between both materials tested were similar, independent from the treatment sequence. Furthermore, the possible influence of furcation morphology on the effectiveness of the treatment was analyzed in this study. No 1192
6 J Periodontol September 2004 Meyle, Gonzales, Bödeker, et al. Table 2. Estimators of the Differences in Changes of Measurements of Hard Tissue Boundaries With EMD or Membrane Hodges-Lehmann Variable* Estimator 95% CI P Value Interproximal bone crest, distal (a) Stent to CEJ to Buccal bone crest, mid-distal root (b) Stent to CEJ to Bone crest of defect, mid-furcation (c) Stent to CEJ to Buccal bone crest, mid-mesial root (d) Stent to CEJ to Interproximal bone crest, mesial (e) Stent to CEJ to Fornix to bone crest of defect (f) to Width of defect at the bottom to of the defect (g) Bottom of the defect (i) Stent to CEJ to * Letters in parentheses refer to parameters in Figure 1. Estimator of (X EMD,surgery X EMD,reentry ) (X Membrane,surgery X Membrane,reentry ). Wilcoxon two-sample test. Clinical and statistically relevant differences. indication of an association between those parameters describing the furcation morphology (Fig. 1, parameters f, g, and i) and the change in the primary parameter h, or parameter f could be demonstrated. Also, no association was found for the parameters a, c, e, f, and g with the change of parameter i, and for the parameters a, c, and e with the changes of PD and AL measured in the mid-furcation site. DISCUSSION In the treatment of mandibular Class II furcations, many comparative studies using diverse materials and therapies have been performed. While some reports demonstrated significant clinical attachment and bone gains, other studies did not show a significant clinical improvement. 14 Similar results have been shown for GTR furcation therapy when bioabsorbable and nonresorbable barriers were compared. 30 Moreover, few studies using bioabsorbable membranes have demonstrated that the furcation defects were filled with bone to more than 50% of the lesion. 31 Thus, the results obtained from most of the GTR procedures, regardless of the barrier membrane used, clearly showed the limitations of this therapy in this type of defect. Figure 6. Distribution of the change in the distance from the stent to the buccal bone crest, mid-distal root (Fig. 1, parameter b), separated by treatment and side. Figure 7. Distribution of the change in the distance from the stent to the buccal bone crest, mid-mesial root (Fig. 1, parameter d), separated by treatment and side. 1193
7 Comparison of Enamel Matrix Derivative and Membranes for Furcation Therapy Volume 75 Number 9 Periodontal regeneration of intrabony defects using EMD is well documented in clinical trials and case reports. 16,32,33 Recently, a multicenter, randomized, controlled clinical study was conducted on 172 patients, evaluating the effect of EMD in deep intrabony defects. The results after 1 year showed greater gains of clinical AL (3.1 ± 1.5 mm) and PD reduction (3.9 ± 1.5 mm) with the use of EMD than with only root debridement and conditioning (clinical AL: 2.5 ± 1.5 mm; PD: 3.3 ± 1.7 mm). 19 Studies comparing EMD and GTR with either bioabsorbable or non-resorbable membranes for the treatments of intrabony defects have been also performed. 24,34,35 These clinical studies indicated that a similar therapeutic effect was achieved by using either EMD or GTR procedures, irrespective of the type of membrane used. In addition, a histological study demonstrated the formation of new connective tissue attachment in human intrabony defects, either with EMD or GTR procedures. 36 There is a lack of data with regard to the effectiveness of EMD for the treatment of Class II furcation defects. Therefore, the present study was designed as a multicenter, randomized clinical study for evaluating and comparing the effects of EMD treatment with GTR using a bioabsorbable membrane in human mandibular buccal Class II furcation defects. In this type of study, the null hypothesis is that there is no different treatment effect between the two treatments. Secondary parameters comprised all the anatomical measurements of hard tissue boundaries in the furcation defect and the clinical parameters assessing the GM level, PD, BOP, AL, and bone level. Under the conditions of this study, treatment with EMD was equally effective with membrane treatment. This result is supported by published data on the clinical gains after treatment of intrabony defects with EMD. 35 However, different effects could be found for the distance from the stent to the GM level at the mid-furcation site (P = 0.04). This indicates that a modest gingival recession occurred in both treatments; however, the level of recession was less in the EMD-treated sites. There is a sparsity of data on gingival recession following regenerative periodontal surgery with EMD. The percentage of BOP was reduced throughout the study, irrespective of the treatment. In addition to clinical outcomes, oral hygiene was monitored throughout the study assessing full-mouth and site plaque indices. Overall, patients showed a good level of compliance. However, whereas full-mouth plaque was reduced, a slight increase in site plaque in the mid-furcation of the tooth after 8 to 14 months was observed. This percentage was higher in membrane-treated teeth than in those treated with EMD. With respect to the hard tissue boundaries, different treatment effects were found for the distance from the stent and the CEJ to the buccal bone crest, in the mid-buccal of the distal root (P stent = 0.01; P CEJ = 0.07), and in the mid-buccal of the mesial root (P stent = 0.01; P CEJ = 0.01). However, the values of these bone level changes were slightly negative in the sites treated with membrane, whereas no changes were found in sites treated with EMD. This means that no measurable bone resorption occurred in the EMD treated sites, whereas a slight resorption resulted in those sites treated with membrane. This is the first time that such an effect of EMD versus membrane treatment on hard tissue margins has been reported. This might be the reason for the minimal recession observed with EMD treatment in the present study. Some variability in outcomes following the GTR technique was expected; however, in the case of EMD it has been reported that clinical improvements were better at sites with deep, rather than shallow, defects. 24 In the present study, no influence of furcation morphology on the effectiveness of the treatment could be demonstrated. In summary, this study demonstrates equivalent clinical results when treatment with EMD was compared with GTR with bioabsorbable membrane in treating mandibular Class II furcations. Evaluation of clinical and osseous changes associated with this study indicated that treatment with EMD led to similar regenerative outcomes as the GTR procedure. ACKNOWLEDGMENT This study was supported by Biora AB, Malmö, Sweden (now Straumann Biologics Division, Waltham, Massachusetts). REFERENCES 1. Lekovic V, Kenney EB, Kovacevic K, Carranza FA Jr. Evaluation of guided tissue regeneration in Class II furcation defects. A clinical re-entry study. J Periodontol 1989;60: Kenney EB, Lekovic V, Elbaz JJ, Kovacevic K, Carranza FA Jr, Takei HH. The use of a porous hydroxylapatite implant in periodontal defects. II. Treatment of Class II furcation lesions in lower molars. J Periodontol 1988;59: Gottlow J, Nyman S, Lindhe J, Karring T, Wennström J. New attachment formation in the human periodontium by guided tissue regeneration. Case reports. J Clin Periodontol 1986;13: Caffesse RG, Smith BA, Duff B, Morrison EC, Merrill D, Becker W. Class II furcations treated by guided tissue regeneration in humans: Case reports. J Periodontol 1990; 61: Gantes B, Martin M, Garrett S, Egelberg J. Treatment of periodontal furcation defects. (II). Bone regeneration in mandibular class II defects. J Clin Periodontol 1988;15: Andersson B, Bratthall G, Kullendorff B, Grondahl K, Rohlin M, Attstrom R. Treatment of furcation defects. Guided tissue regeneration versus coronally positioned flap in mandibular molars; a pilot study. J Clin Periodontol 1994;21: Wallace SC, Gellin RG, Miller MC, Mishkin DJ. Guided tissue regeneration with and without decalcified freeze-dried 1194
8 J Periodontol September 2004 Meyle, Gonzales, Bödeker, et al. bone in mandibular Class II furcation invasions. J Periodontol 1994;65: Jepsen S, Eberhard J, Herrera D, Needleman I. A systematic review of guided tissue regeneration for periodontal furcation defects. What is the effect of guided tissue regeneration compared with surgical debridement in the treatment of furcation defects? J Clin Periodontol 2002;29: Yukna RA. Clinical human comparison of expanded polytetrafluoroethylene barrier membrane and freeze-dried dura mater allografts for guided tissue regeneration of lost periodontal support. I. Mandibular molar Class II furcations. J Periodontol 1992;63: Bouchard P, Ouhayoun JP, Nilveus RE. Expanded polytetrafluoroethylene membranes and connective tissue grafts support bone regeneration for closing mandibular Class II furcations. J Periodontol 1993;64: Machtei EE, Grossi SG, Dunford R, Zambon JJ, Genco RJ. Long-term stability of Class II furcation defects treated with barrier membranes. J Periodontol 1996;67: Camelo MC, Nevins ML, Nevins M. Treatment of Class II furcations with autogenous bone grafts and e-ptfe membranes. Int J Periodontics Restorative Dent 2000;20: Garrett S, Polson AM, Stoller NH, et al. Comparison of a bioabsorbable GTR barrier to a non-absorbable barrier in treating human Class II furcation defects. A multicenter parallel design randomized single-blind trial. J Periodontol 1997;68: Sanz M, Giovannoli JL. Focus on furcation defects: Guided tissue regeneration. Periodontol ;22: Hammarstrom L. Enamel matrix, cementum development and regeneration. J Clin Periodontol 1997;24: Heijl L, Heden G, Svardstrom G, Ostgren A. Enamel matrix derivative (EMDOGAIN) in the treatment of intrabony periodontal defects. J Clin Periodontol 1997;24: Hammarstrom L, Heijl L, Gestrelius S. Periodontal regeneration in a buccal dehiscence model in monkeys after application of enamel matrix proteins. J Clin Periodontol 1997;24: Mellonig JT. Enamel matrix derivative for periodontal reconstructive surgery: Technique and clinical and histologic case report. Int J Periodontics Restorative Dent 1999;19: Tonetti MS, Lang NP, Cortellini P, et al. Enamel matrix proteins in the regenerative therapy of deep intrabony defects. J Clin Periodontol 2002;29: Froum SJ, Weinberg MA, Rosenberg E, Tarnow D. A comparative study utilizing open flap debridement with and without enamel matrix derivative in the treatment of periodontal intrabony defects: A 12-month re-entry study. J Periodontol 2001;72: Okuda K, Momose M, Miyazaki A, et al. Enamel matrix derivative in the treatment of human intrabony osseous defects. J Periodontol 2000;71: Cardaropoli G, Leonhardt AS. Enamel matrix proteins in the treatment of deep intrabony defects. J Periodontol 2002;73: Bratthall G, Lindberg P, Havemose-Poulsen A, et al. Comparison of ready-to-use EMDOGAIN-gel and EMDO- GAIN in patients with chronic adult periodontitis. J Clin Periodontol 2001;28: Pontoriero R, Wennstrom J, Lindhe J. The use of barrier membranes and enamel matrix proteins in the treatment of angular bone defects. A prospective controlled clinical study. J Clin Periodontol 1999;26: Heden G. A case report study of 72 consecutive Emdogain-treated intrabony periodontal defects: Clinical and radiographic findings after 1 year. Int J Periodontics Restorative Dent 2000;20: Sculean A, Reich E, Chiantella GC, Brecx M. Treatment of intrabony periodontal defects with an enamel matrix protein derivative (Emdogain): A report of 32 cases. Int J Periodontics Restorative Dent 1999;19: Velasquez-Plata D, Scheyer ET, Mellonig JT. Clinical comparison of an enamel matrix derivative used alone or in combination with a bovine-derived xenograft for the treatment of periodontal osseous defects in humans. J Periodontol 2002;73: Sculean A, Barbe G, Chiantella GC, Arweiler NB, Berakdar M, Brecx M. Clinical evaluation of an enamel matrix protein derivative combined with a bioactive glass for the treatment of intrabony periodontal defects in humans. J Periodontol 2002;73: Jepsen S, Heinz B, Jepsen K, et al. A randomized clinical trial comparing enamel matrix derivative and membrane treatment of buccal Class II furcation involvement in mandibular molars. Part 1: Study design and results for primary outcomes. J Periodontol 2004;75: Hugoson A, Ravald N, Fornell J, Johard G, Teiwik A, Gottlow J. Treatment of Class II furcation involvements in humans with bioresorbable and nonresorbable guided tissue regeneration barriers. A randomized multi-center study. J Periodontol 1995;66: Wang HL, O Neal RB, Thomas CL, Shyr Y, MacNeil RL. Evaluation of an absorbable collagen membrane in treating Class II furcation defects. J Periodontol 1994;65: Parashis A, Tsiklakis K. Clinical and radiographic findings following application of enamel matrix derivative in the treatment of intrabony defects. A series of case reports. J Clin Periodontol 2000;27: Heden G, Wennstrom J, Lindhe J. Periodontal tissue alterations following Emdogain treatment of periodontal sites with angular bone defects. A series of case reports. J Clin Periodontol 1999;26: Silvestri M, Ricci G, Rasperini G, Sartori S, Cattaneo V. Comparison of treatments of infrabony defects with enamel matrix derivative, guided tissue regeneration with a nonresorbable membrane and Widman modified flap. A pilot study. J Clin Periodontol 2000;27: Sculean A, Windisch P, Chiantella GC, Donos N, Brecx M, Reich E. Treatment of intrabony defects with enamel matrix proteins and guided tissue regeneration. A prospective controlled clinical study. J Clin Periodontol 2001;28: Sculean A, Donos N, Windisch P, et al. Healing of human intrabony defects following treatment with enamel matrix proteins or guided tissue regeneration. J Periodontal Res 1999;34: Correspondence: Dr. Jörg Meyle and Dr. José R. Gonzales, University of Giessen, Department of Periodontology, Schlangenzahl 14, Giessen, Germany. joerg. meyle@dentist.med.uni-giessen.de; jose.gonzales@dentist. med.uni-giessen.de. Accepted for publication January 5,
Emdogain. The reliable solution for periodontal treatment.
 Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
Emdogain The reliable solution for periodontal treatment. Straumann is the exclusive industrial partner of the ITI (International Team for Implantology) in the areas of research, development, and education.
vitality meets bone volume around dental implants Straumann BoneCeramic
 vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
Endodontic-periodontal lesion is a clinical manifestation of the pathologic/inflammatory
 Treatment Strategy for Guided Tissue Regeneration in Combined Endodontic-Periodontal Lesions: Case Report and Review Se-Lim Oh, DMD MS,* Ashraf F. Fouad, BDS, DDS, MS, and Sang-Hoon Park, DDS, MS Abstract
Treatment Strategy for Guided Tissue Regeneration in Combined Endodontic-Periodontal Lesions: Case Report and Review Se-Lim Oh, DMD MS,* Ashraf F. Fouad, BDS, DDS, MS, and Sang-Hoon Park, DDS, MS Abstract
MUCOGINGIVAL SURGERY WITH FREE GINGIVAL GRAFT (STRIP TECHNIQUE) FOR AUGMENTATION OF THE ATTACHED GINGIVAL TISSUES: REPORT OF THREE CASES
 Journal of IMAB - Annual Proceeding (Scientific Papers) 2007, vol. 13, book 2 MUCOGINGIVAL SURGERY WITH FREE GINGIVAL GRAFT (STRIP TECHNIQUE) FOR AUGMENTATION OF THE ATTACHED GINGIVAL TISSUES: REPORT OF
Journal of IMAB - Annual Proceeding (Scientific Papers) 2007, vol. 13, book 2 MUCOGINGIVAL SURGERY WITH FREE GINGIVAL GRAFT (STRIP TECHNIQUE) FOR AUGMENTATION OF THE ATTACHED GINGIVAL TISSUES: REPORT OF
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
PARTIAL CURRICULUM VITAE. Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012
 PARTIAL CURRICULUM VITAE Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012 Professional Education: D.D.S. Marquette University 1952-1956 Certificate
PARTIAL CURRICULUM VITAE Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012 Professional Education: D.D.S. Marquette University 1952-1956 Certificate
SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW
 Review Article International Journal of Dental and Health Sciences Volume 02,Issue 06 SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW Deepak Kumar 1, Manvi Chandra agarwal 2, Ellora
Review Article International Journal of Dental and Health Sciences Volume 02,Issue 06 SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW Deepak Kumar 1, Manvi Chandra agarwal 2, Ellora
Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW
 Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW Presented by: Dr. Syeda Mahvash Hussain Resident Operative Dentistry Aga Khan University Hospital Karachi Contributors: Drs. Maham
Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW Presented by: Dr. Syeda Mahvash Hussain Resident Operative Dentistry Aga Khan University Hospital Karachi Contributors: Drs. Maham
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
Papilla Preservation Flap : Revisited
 REVIEW ARTICLE Papilla Preservation Flap : Revisited Lisa N. Chacko*, Sathish Abraham**, Nilima Landge***, Fareedi Mukram Ali**** Abstract An ideal periodontal therapy should establish a state of periodontal
REVIEW ARTICLE Papilla Preservation Flap : Revisited Lisa N. Chacko*, Sathish Abraham**, Nilima Landge***, Fareedi Mukram Ali**** Abstract An ideal periodontal therapy should establish a state of periodontal
Removal of epithelium in periodontal pockets after diode (980nm) laser application in the animal model
 Removal of epithelium in periodontal pockets after diode (980nm) laser application in the animal model G.E. Romanos, M. Henze, S. Banihashemi, H. Parsanejad, G.H. Nentwig Dept. of Oral Surgery and Implantology,
Removal of epithelium in periodontal pockets after diode (980nm) laser application in the animal model G.E. Romanos, M. Henze, S. Banihashemi, H. Parsanejad, G.H. Nentwig Dept. of Oral Surgery and Implantology,
Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on Periodontology
 J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
BRITISH DENTAL JOURNAL
 IN BRIEF The most important step in treatment planning is determining the prognosis of the remaining dentition. There is some evidence that placement of foreign materials into extraction sockets will interfere
IN BRIEF The most important step in treatment planning is determining the prognosis of the remaining dentition. There is some evidence that placement of foreign materials into extraction sockets will interfere
Guided bone regeneration (GBR) has made the
 Case Report 684 Guided Bone Regeneration for Fenestration Defects in Dental Implants Hwey-Chin Yeh, DDS, MS; Kuang-Wei Hsu 1, DDS has been applied in implant dentistry for increasing the width and height
Case Report 684 Guided Bone Regeneration for Fenestration Defects in Dental Implants Hwey-Chin Yeh, DDS, MS; Kuang-Wei Hsu 1, DDS has been applied in implant dentistry for increasing the width and height
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Periodontal Screening and Recording: Early Detection of Periodontal Diseases
 Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Current Advances in the Use of Lasers in Periodontal Therapy: A LANAP Case Series
 Current Advances in the Use of Lasers in Periodontal Therapy: A LANAP Case Series I. Stephen Brown, DDS, FACD, FICD Professor of Periodontics, University of Pennsylvania School of Dental Medicine Professor
Current Advances in the Use of Lasers in Periodontal Therapy: A LANAP Case Series I. Stephen Brown, DDS, FACD, FICD Professor of Periodontics, University of Pennsylvania School of Dental Medicine Professor
REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS
 CONTINUING EDUCATION X X REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS Nicolas Elian, DDS* Ziad N. Jalbout, DDS Sang-Choon Cho, DDS Stuart
CONTINUING EDUCATION X X REALITIES AND LIMITATIONS IN THE MANAGEMENT OF THE INTERDENTAL PAPILLA BETWEEN IMPLANTS: THREE CASE REPORTS Nicolas Elian, DDS* Ziad N. Jalbout, DDS Sang-Choon Cho, DDS Stuart
The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis
 [ continuing [ education 1 ] 1 ] The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis Paul S. Rosen, DMD, MS Abstract Practitioners who are knowledgeable
[ continuing [ education 1 ] 1 ] The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis Paul S. Rosen, DMD, MS Abstract Practitioners who are knowledgeable
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Calibrated Periodontal Probes and Basic Probing Technique
 Module 11 Calibrated Periodontal Probes and Basic Probing Technique MODULE OVERVIEW This module presents the (1) design characteristics of calibrated periodontal probes and (2) step-by-step instructions
Module 11 Calibrated Periodontal Probes and Basic Probing Technique MODULE OVERVIEW This module presents the (1) design characteristics of calibrated periodontal probes and (2) step-by-step instructions
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
(Traitement des furcations à l aide d une membrane en collagène bioabsorbable : essai clinique)
 R E C H E R C H E A P P L I Q U É E Furcation Therapy with Bioabsorbable Collagen Membrane: A Clinical Trial (Traitement des furcations à l aide d une membrane en collagène bioabsorbable : essai clinique)
R E C H E R C H E A P P L I Q U É E Furcation Therapy with Bioabsorbable Collagen Membrane: A Clinical Trial (Traitement des furcations à l aide d une membrane en collagène bioabsorbable : essai clinique)
The management of traumatic tooth loss with dental implants: Part 2. Severe trauma
 The management of traumatic tooth loss with dental implants: Part 2. Severe trauma D. W. Seymour,* 1 M. Patel, 2 L. Carter 3 and M. Chan 2 IN BRIEF Discusses the challenges associated with the provision
The management of traumatic tooth loss with dental implants: Part 2. Severe trauma D. W. Seymour,* 1 M. Patel, 2 L. Carter 3 and M. Chan 2 IN BRIEF Discusses the challenges associated with the provision
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery. Consequences of tooth loss.
 Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Molar Uprighting Dr. Margherita Santoro Division of Orthodontics School of Dental and Oral surgery Molars The wide occlusal surface is designed for food grinding. The surface needs to be aligned with the
Single anterior tooth replacement: clinical approaches
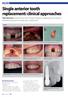 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
One way to attempt periodontal regeneration
 PERIODONTAL REGENERATIVE POTENTIAL VETENSKAP Periodontal regenerative potential using enamel matrix proteins (EMDOGAIN ) Lars Heijl Med Emdogain har man för första gången möjlighet att återskapa ett förlorat
PERIODONTAL REGENERATIVE POTENTIAL VETENSKAP Periodontal regenerative potential using enamel matrix proteins (EMDOGAIN ) Lars Heijl Med Emdogain har man för första gången möjlighet att återskapa ett förlorat
Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF)
 Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF) 309 Of the numerous periodontal surgical techniques, the oft-modified Widman flap ( Modified Widman Flap, MWF) remains the standard
Access Flap Surgery, Open Flap Debridement (OFD) Modified Widman Flap (MWF) 309 Of the numerous periodontal surgical techniques, the oft-modified Widman flap ( Modified Widman Flap, MWF) remains the standard
Prevention and Treatment of Periodontal Diseases in Primary Care Dental Clinical Guidance
 Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Dental Clinical Guidance June 2014 Scottish Dental Clinical Effectiveness Programme
Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Dental Clinical Guidance June 2014 Scottish Dental Clinical Effectiveness Programme
Scottish Dental Clinical Effectiveness Programme SDcep. Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief
 Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D.
 Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D. 1 Potential periodontal problems Before Orthodontic Treatment During Orthodontic Treatment After Orthodontic
Periodontal Consideration Before and After Orthodontic Treatment Tsung-Ju Hsieh, D.D.S., M.S.D. 1 Potential periodontal problems Before Orthodontic Treatment During Orthodontic Treatment After Orthodontic
SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION. Ph.D. thesis. Dr. med. dent.
 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION Ph.D. thesis Dr. med. dent. Sofia Aroca Szeged, Hungary 2010 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL
SURGICAL TREATMENTS OF MULTIPLE GINGIVAL RECESSIONS: STATE OF THE ART and WOUND HEALING MODULATION Ph.D. thesis Dr. med. dent. Sofia Aroca Szeged, Hungary 2010 SURGICAL TREATMENTS OF MULTIPLE GINGIVAL
Many factors must be considered when
 + CASE STUDY 1 Loss of the Interdental Papilla Prevention and management of dental implant-related complications in the esthetic zone + Stephen J. Chu DMD, MSD, CDT + Mark N. Hochman DDS + Dennis P. Tarnow
+ CASE STUDY 1 Loss of the Interdental Papilla Prevention and management of dental implant-related complications in the esthetic zone + Stephen J. Chu DMD, MSD, CDT + Mark N. Hochman DDS + Dennis P. Tarnow
Comparison of Peri-Implant Bone Loss
 Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Guideline for Periodontal Therapy
 Guideline for Periodontal Therapy Originating Group American Academy of Periodontology Endorsed by the American Academy of Pediatric Dentistry 2003 Research has provided evidence that chronic inflammatory
Guideline for Periodontal Therapy Originating Group American Academy of Periodontology Endorsed by the American Academy of Pediatric Dentistry 2003 Research has provided evidence that chronic inflammatory
Prosthodontist s Perspective
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Periodontal Re-treatment in Patients on Maintenance Following Pocket Reduction Surgery
 Periodontal Re-treatment in Patients on Maintenance Following Pocket Reduction Surgery Roberto Galindo 1, Paul Levi 2, Andres Pascual LaRocca 1, José Nart 1 1 Periodontics Department, Universitat Internacional
Periodontal Re-treatment in Patients on Maintenance Following Pocket Reduction Surgery Roberto Galindo 1, Paul Levi 2, Andres Pascual LaRocca 1, José Nart 1 1 Periodontics Department, Universitat Internacional
RESTORATIVE DENTISTRY ORAL DIAGNOSIS TOOTH WHITENING/BLEACHING IMPLANT RESTORATIONS WWW.AGD.ORG. 6t952. Academy of Geucml Dentistry
 RESTORATIVE DENTISTRY ORAL DIAGNOSIS TOOTH WHITENING/BLEACHING IMPLANT RESTORATIONS WWW.AGD.ORG 6t952 Academy of Geucml Dentistry 20120 II LASERS IN PERIODONTICS 1111 --------------------------------------------------------------------------------
RESTORATIVE DENTISTRY ORAL DIAGNOSIS TOOTH WHITENING/BLEACHING IMPLANT RESTORATIONS WWW.AGD.ORG 6t952 Academy of Geucml Dentistry 20120 II LASERS IN PERIODONTICS 1111 --------------------------------------------------------------------------------
Complications with excess cement & dental implants: Diagnosis, recommendations & treatment of 7 clinical cases.
 Robert A. Levine DDS, FCPP, Diplomate, American Board of Periodontology Clinical Professor, Temple University Kornberg School of Dentistry Fellow International Team for Implantology Pennsylvania Center
Robert A. Levine DDS, FCPP, Diplomate, American Board of Periodontology Clinical Professor, Temple University Kornberg School of Dentistry Fellow International Team for Implantology Pennsylvania Center
Electronic Oral Health Risk Assessment Tools
 SCDI White Paper No. 1074 Approved by ADA Council on Dental Practice May 2013 ADA SCDI White Paper No. 1074 Electronic Oral Health Risk Assessment Tools 2013 Copyright 2013 American Dental Association.
SCDI White Paper No. 1074 Approved by ADA Council on Dental Practice May 2013 ADA SCDI White Paper No. 1074 Electronic Oral Health Risk Assessment Tools 2013 Copyright 2013 American Dental Association.
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Insurance Coding: Teaching Our Periodontics Residents
 Charleston, SC Insurance Coding: Teaching Our Periodontics Residents Joe W. Krayer, D.D.S., M.S. Associate Professor & Director Post-Doctoral Periodontics Program Robert G. Gellin, D.M.D., M.H.S. Professor
Charleston, SC Insurance Coding: Teaching Our Periodontics Residents Joe W. Krayer, D.D.S., M.S. Associate Professor & Director Post-Doctoral Periodontics Program Robert G. Gellin, D.M.D., M.H.S. Professor
Oral Plastic Surgery
 20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
In many instances where a tooth is no longer
 Management of the extraction socket: Site preservation prior to implant placement By Michael Danesh-Meyer, BDS, MDS (Perio) Site preservation through socket grafting will help to optimise bony fill within
Management of the extraction socket: Site preservation prior to implant placement By Michael Danesh-Meyer, BDS, MDS (Perio) Site preservation through socket grafting will help to optimise bony fill within
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
HEALTH SERVICES POLICY & PROCEDURE MANUAL. SUBJECT: Types of Dental Treatments Provided EFFECTIVE DATE: July 2014 SUPERCEDES DATE: January 2014
 PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up
 Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 375 Use of a Combination Epithelized- Subepithelial Connective Tissue Graft for Closure and Soft Tissue Augmentation of an Extraction Site
The International Journal of Periodontics & Restorative Dentistry 375 Use of a Combination Epithelized- Subepithelial Connective Tissue Graft for Closure and Soft Tissue Augmentation of an Extraction Site
Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies
 Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies Jason M. Mailhot, DMD, MS, FACD; Spencer L. Fried, DDS, MS Continuing
Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies Jason M. Mailhot, DMD, MS, FACD; Spencer L. Fried, DDS, MS Continuing
Straumann Dental Implant System. Implant Selection Guide.
 Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
Straumann Dental Implant System. Implant Selection Guide. STRAUMANN's IMPLANT PORTFOLIO The Straumann Dental Implant System offers two implant lines with diverse body and neck designs ranging from the
CURRICULUM VITAE Donald S. Clem, D.D.S., F.A.C.D. 130 Laguna Rd., Suite B Fullerton, California 92835 Business Telephone: (714) 441-0436
 Business Address: CURRICULUM VITAE Donald S. Clem, D.D.S., F.A.C.D. Donald S. Clem, III, D.D.S., Inc. 130 Laguna Rd., Suite B 92835 Business Telephone: (714) 441-0436 EDUCATION Loyola University of Chicago
Business Address: CURRICULUM VITAE Donald S. Clem, D.D.S., F.A.C.D. Donald S. Clem, III, D.D.S., Inc. 130 Laguna Rd., Suite B 92835 Business Telephone: (714) 441-0436 EDUCATION Loyola University of Chicago
Boston College, BS in Biology 1980-1984. University of Southern California, Doctor of Dental Surgery, DDS, 1990.
 CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
Periodontal surgery report for crown lengthening of tooth number 24,25
 411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
Communication Task - Scenario 1 CANDIDATE COPY
 Communication Task - Scenario 1 Your patient is 30 years old, and has presented today complaining of pain from the lower right posterior side. The tooth had been cold sensitive for several weeks, but the
Communication Task - Scenario 1 Your patient is 30 years old, and has presented today complaining of pain from the lower right posterior side. The tooth had been cold sensitive for several weeks, but the
Treatment of Plaque-induced Gingivitis, Chronic Periodontitis, and Other Clinical Conditions
 REFERENCE MANUAL V 37 / NO 6 15 / 16 Treatment of Plaque-induced Gingivitis, Chronic Periodontitis, and Other Clinical Conditions Originating Group American Academy of Periodontology - Research, Science,
REFERENCE MANUAL V 37 / NO 6 15 / 16 Treatment of Plaque-induced Gingivitis, Chronic Periodontitis, and Other Clinical Conditions Originating Group American Academy of Periodontology - Research, Science,
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Immediate provisional restoration of a single-tooth implant in the esthetic zone: A case report
 Kaohsiung Journal of Medical Sciences (2011) 27, 80e84 available at www.sciencedirect.com journal homepage: http://www.kjms-online.com CASE REPORT Immediate provisional restoration of a single-tooth implant
Kaohsiung Journal of Medical Sciences (2011) 27, 80e84 available at www.sciencedirect.com journal homepage: http://www.kjms-online.com CASE REPORT Immediate provisional restoration of a single-tooth implant
Tissue alterations at implant-supported single-tooth replacements: a 1-year prospective clinical study
 Giuseppe Cardaropoli Ulf Lekholm Jan L. Wennström Tissue alterations at implant-supported single-tooth res: a 1-year prospective clinical study Authors affiliations: Giuseppe Cardaropoli, Jan L. Wennström,
Giuseppe Cardaropoli Ulf Lekholm Jan L. Wennström Tissue alterations at implant-supported single-tooth res: a 1-year prospective clinical study Authors affiliations: Giuseppe Cardaropoli, Jan L. Wennström,
The saddle connective tissue graft: a periodontal plastic surgery technique to obtain soft tissue coronal gain on immediate implants.
 CASE REPORT The saddle connective tissue graft: a periodontal plastic surgery technique to obtain soft tissue coronal gain on immediate implants. A case report David González, DMD, PhD Periodontology,
CASE REPORT The saddle connective tissue graft: a periodontal plastic surgery technique to obtain soft tissue coronal gain on immediate implants. A case report David González, DMD, PhD Periodontology,
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Chronic periodontitis is initiated
 J Periodontol November 2008 Review The Effect of Laser Therapy as an Adjunct to Non-Surgical Periodontal Treatment in Subjects With Chronic Periodontitis: A Systematic Review Marcus R. Karlsson,* Christina
J Periodontol November 2008 Review The Effect of Laser Therapy as an Adjunct to Non-Surgical Periodontal Treatment in Subjects With Chronic Periodontitis: A Systematic Review Marcus R. Karlsson,* Christina
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice.
 32 News No. 32 May 2013 Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice. MAKE IT SIMPLE 2 Using BONDBONE as a composite in post extraction sockets
32 News No. 32 May 2013 Using BONDBONE as a composite in post extraction sockets with immediate implant placement everyday practice. MAKE IT SIMPLE 2 Using BONDBONE as a composite in post extraction sockets
Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry
 REVIEW 193 Guy Huynh-Ba, Urs Brägger, Niklaus P Lang Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry KEY WORDS crown lengthening, surgery Guy Huynh-Ba Department
REVIEW 193 Guy Huynh-Ba, Urs Brägger, Niklaus P Lang Surgical lengthening of the clinical crown: a periodontal concept for reconstructive dentistry KEY WORDS crown lengthening, surgery Guy Huynh-Ba Department
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
1.0 Abstract. Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA. Keywords. Rationale and Background:
 1.0 Abstract Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA Keywords Rationale and Background: This abbreviated clinical study report is based on a clinical surveillance
1.0 Abstract Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA Keywords Rationale and Background: This abbreviated clinical study report is based on a clinical surveillance
Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report
 Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Effects of 980 Diode Laser Treatment Combined with Scaling and. Root Planing on Periodontal Pockets in Chronic Periodontitis.
 Effects of 980 Diode Laser Treatment Combined with Scaling and Root Planing on Periodontal Pockets in Chronic Periodontitis Abstract: Patients Alireza Fallah, DDS, M.Sc., PhD Candidate Aachen Institute
Effects of 980 Diode Laser Treatment Combined with Scaling and Root Planing on Periodontal Pockets in Chronic Periodontitis Abstract: Patients Alireza Fallah, DDS, M.Sc., PhD Candidate Aachen Institute
Immediate Dental Implant Placement: Technique, Part 2
 Course Number: 170 Immediate Dental Implant Placement: Technique, Part 2 Authored by John Cavallaro, DDS, and Gary Greenstein, DDS, MS Upon successful completion of this CE activity 2 CE credit hours may
Course Number: 170 Immediate Dental Implant Placement: Technique, Part 2 Authored by John Cavallaro, DDS, and Gary Greenstein, DDS, MS Upon successful completion of this CE activity 2 CE credit hours may
Dental Bone Grafting Options. A review of bone grafting options for patients needing more bone to place dental implants
 Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Periodontal Surgery. What Can I Expect? The word "periodontal" literally means around the tooth. Many factors, such as oral hygiene habits, genetics,
 The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
Clinical Study Report. Clinical Efficacy of the e-bright Tooth Whitening Accelerator Home Edition: a randomized placebo controlled clinical trial
 Clinical Study Report Clinical Efficacy of the e-bright Tooth Whitening Accelerator Home Edition: a randomized placebo controlled clinical trial (Clinical Study Protocol Number: EBRIGHT-2007-01) Study
Clinical Study Report Clinical Efficacy of the e-bright Tooth Whitening Accelerator Home Edition: a randomized placebo controlled clinical trial (Clinical Study Protocol Number: EBRIGHT-2007-01) Study
Cairo Dental Journal (25) Number (1), 61:67 Janurary, 2009. Tamer N. Mohamed; 1 Abd El Salam B. Younis 2 and Basma G. Moussa 3.
 Cairo Dental Journal (25) Number (1), 61:67 Janurary, 2009 IMMEDIATE IMPLANTS IN LOWER POSTERIOR TEETH WITH BONE SUBISTITUTE AND GUIDED TISSUE MEMBRANE Tamer N. Mohamed; 1 Abd El Salam B. Younis 2 and
Cairo Dental Journal (25) Number (1), 61:67 Janurary, 2009 IMMEDIATE IMPLANTS IN LOWER POSTERIOR TEETH WITH BONE SUBISTITUTE AND GUIDED TISSUE MEMBRANE Tamer N. Mohamed; 1 Abd El Salam B. Younis 2 and
Periodontal Risk Assessment (PRA) for Patients in Supportive Periodontal Therapy (SPT)
 Oral Health & Preventive Dentisty 1/2003, S. 7-16 Periodontal Risk Assessment (PRA) for Patients in Supportive Periodontal Therapy (SPT) Niklaus P. Lang a / Maurizio S. Tonetti b Abstract Summary: The
Oral Health & Preventive Dentisty 1/2003, S. 7-16 Periodontal Risk Assessment (PRA) for Patients in Supportive Periodontal Therapy (SPT) Niklaus P. Lang a / Maurizio S. Tonetti b Abstract Summary: The
INFUSE Bone Graft (rhbmp-2/acs)
 1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
Chapter 6 Aesthetical improvement Use of one-piece type implants
 Chapter 6 Aesthetical improvement Use of one-piece type implants 1. Improving esthetics with one-piece implant Director of Kinebuchi Dental Clinic Takao Kinebuchi Aesthetics of two-piece two-stage type
Chapter 6 Aesthetical improvement Use of one-piece type implants 1. Improving esthetics with one-piece implant Director of Kinebuchi Dental Clinic Takao Kinebuchi Aesthetics of two-piece two-stage type
The principal objective
 Volume 74 Number 5 Periodontal Treatment with an Er:YAG Laser or Scaling and Root Planing. A 2-Year Follow-Up Split-Mouth Study Frank Schwarz,* Anton Sculean, Mohammad Berakdar, Thomas Georg, Elmar Reich,
Volume 74 Number 5 Periodontal Treatment with an Er:YAG Laser or Scaling and Root Planing. A 2-Year Follow-Up Split-Mouth Study Frank Schwarz,* Anton Sculean, Mohammad Berakdar, Thomas Georg, Elmar Reich,
www.drcolinrichman.com - (404)784/7272 Agenda 9/14/2014 Questions?
 Altering Alveolar Bone Volume and Biotype Periodontally Accelerated Osteogenic Orthodontics TM Colin Richman DMD Questions? 1 Why are orthodontic problems and gingival recession so prevalent in the USA
Altering Alveolar Bone Volume and Biotype Periodontally Accelerated Osteogenic Orthodontics TM Colin Richman DMD Questions? 1 Why are orthodontic problems and gingival recession so prevalent in the USA
Implants Placed in Immediate Extraction Sites: A Report of Histologic and Histometric Analyses of Human Biopsies
 Implants Placed in Immediate Extraction Sites: A Report of Histologic and Histometric Analyses of Human Biopsies Thomas G. Wilson, Jr, DDS*/Robert Schenk, MD, Prof Dr Med**/ Daniel Buser, DMD, Prof Dr
Implants Placed in Immediate Extraction Sites: A Report of Histologic and Histometric Analyses of Human Biopsies Thomas G. Wilson, Jr, DDS*/Robert Schenk, MD, Prof Dr Med**/ Daniel Buser, DMD, Prof Dr
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
Cross-sectional. Translate Lp3 after. Translate Lp3 after. Tipping Up3 after. ext Up2. ext Lp2. ext Lp2. Bur buc-ling with flap
 Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
Table 2.1 Tooth movement following alveolar decortication injury is represented by 10 evidence-based, refereed, professional journal articles through to May 2013. All investigations include measurements
To save or to extract, that is the question. Natural teeth or dental implants in periodontitissusceptible
 Periodontology 2000, Vol. 47, 2008, 27 50 Printed in Singapore. All rights reserved Ó 2008 The Authors. Journal compilation Ó 2008 Blackwell Munksgaard PERIODONTOLOGY 2000 To save or to extract, that is
Periodontology 2000, Vol. 47, 2008, 27 50 Printed in Singapore. All rights reserved Ó 2008 The Authors. Journal compilation Ó 2008 Blackwell Munksgaard PERIODONTOLOGY 2000 To save or to extract, that is
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 14 ORDINAL MEASURES OF CORRELATION: SPEARMAN'S RHO AND GAMMA
 CHAPTER 14 ORDINAL MEASURES OF CORRELATION: SPEARMAN'S RHO AND GAMMA Chapter 13 introduced the concept of correlation statistics and explained the use of Pearson's Correlation Coefficient when working
CHAPTER 14 ORDINAL MEASURES OF CORRELATION: SPEARMAN'S RHO AND GAMMA Chapter 13 introduced the concept of correlation statistics and explained the use of Pearson's Correlation Coefficient when working
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation
 Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
1 st International Symposium. Regeneration and Esthetics in Periodontology and Implant Dentistry. Chairmen: Prof. Daniel Buser and Prof.
 1 st International Symposium Regeneration and Esthetics in Periodontology and Implant Dentistry Chairmen: Prof. Daniel Buser and Prof. Anton Sculean Welcome We have been able to attract an excellent faculty
1 st International Symposium Regeneration and Esthetics in Periodontology and Implant Dentistry Chairmen: Prof. Daniel Buser and Prof. Anton Sculean Welcome We have been able to attract an excellent faculty
Immediate Dental Implant Placement: Technique, Part 1
 Course Number: 169 Immediate Dental Implant Placement: Technique, Part 1 Authored by Gary Greenstein, DDS, MS, and John Cavallaro, DDS Upon successful completion of this CE activity 2 CE credit hours may
Course Number: 169 Immediate Dental Implant Placement: Technique, Part 1 Authored by Gary Greenstein, DDS, MS, and John Cavallaro, DDS Upon successful completion of this CE activity 2 CE credit hours may
Vertical augmentation using the mandibular body bone for repair of failed implants: a case report
 Vol. 34 No. 2, September 2015 Vertical augmentation using the mandibular body bone for repair of failed implants: a case report Da-Nee Jeon, Han-Kyul Park, Yong-Deok Kim* Department of Oral and Maxillofacial
Vol. 34 No. 2, September 2015 Vertical augmentation using the mandibular body bone for repair of failed implants: a case report Da-Nee Jeon, Han-Kyul Park, Yong-Deok Kim* Department of Oral and Maxillofacial
Immediate Implant Placement After Extraction of Mandibular molars : Report of 3 cases
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 5, Issue 6 (Mar.- Apr. 2013), PP 46-53 Immediate Implant Placement After Extraction of Mandibular s
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 5, Issue 6 (Mar.- Apr. 2013), PP 46-53 Immediate Implant Placement After Extraction of Mandibular s
