Concise Guide to the Management of Heart Failure
|
|
|
- Priscilla May
- 7 years ago
- Views:
Transcription
1 Concise Guide to the Management of Heart Failure WORLD HEALTH ORGANIZATION/COUNCIL ON GERIATRIC CARDIOLOGY TASK FORCE ON HEART FAILURE EDUCATION
2 CONTENTS WHO/CGC TASK FORCE ON Heart Failure EDUCATION...4 objective OF GUIDELINE...5 DefinitionS OF HEART FAILURE...5 Pathophysiological Definition...5 Clinical Definition...5 Clinical Diagnosis OF HEART FAILURE...6 Diagnostic Algorithm...6 Clinical History and Examination...7 Investigations lead ECG...8 Chest Radiograph...9 Echocardiogram...9 DIAGNOSIS AS THE BASIS OF TREATMENT...10 SUMMARY OF THE Types of Heart Failure and THEIR Treatment...10 Aetiology and Pathophysiology...10 Treatments in Common Practice...10 Treatment of Heart Failure DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION...12 Treatment Algorithm...12 Nonpharmacological Treatment/Lifestyle Modification...13 Diuretics...14 Angiotensin Converting Enzyme (ACE) Inhibitors...15 Digoxin...19 Other Vasodilators...19 Other Drugs...20 Aspirin...20 Warfarin...20 Beta adrenoceptor antagonists...20 Apparently Intractable Heart Failure
3 OTHER ASPECTS OF Management...21 Co-Prescribing...21 Non-adherence...22 Management of Concomitant Problems...22 Prevention of Heart Failure...24 Conclusion...25 Bibliography...25 FIGURES Figure 1 Diagnostic Algorithm...6 Figure 2 Treatment Algorithm...12 Figure 3 Initiation of an ACE inhibitor in Heart Failure...16 TABLES Table I Table II Table III ECG findings in patients with suspected heart failure...8 Summary of the types of heart failure and their treatments...10 High-risk conditions for which specialist assessment is desirable...17 Principal Author: John McMurray, Consultant, Department of Cardiology, Western General Hospital, Edinburgh, Scotland 3
4 WHO/CGC TASK FORCE ON HEART FAILURE EDUCATION Representing every continent except Antarctica Co-Chairs Dr. Ivan Gyárfás Chief, Cardiovascular Disease Unit, WHO Geneva, Switzerland Professor Nanette K. Wenger Professor of Medicine (Cardiology) Emory University School of Medicine Atlanta, Georgia, USA M e m b e r s Dr. M. M. Al Nozha Professor of Medicine, Consultant Cardiologist King Saud University Rlyadh, Saudi Arabia Professor Dr. Bernardo Boskis Professor Dr., Cardiology Institute Favaloro Foundation Buenos Aires, Argentina Dr. Michael Bristow Professor, Medicine University of Colorado Health Sciences Center Denver, Colorado, USA Dr. Mireille Brochier Emeritus Prof. University of Cardiology Residence du Lac, Tours, France Professsor Jean Paul Broustet Chief, Cardiology Service Cardiology Hospital, Haut Leveque, Pessac France Dr. Oon Chong Hau Consultant Physician Mount Elizabeth Medical Center Singapore Dr. Jay N. Cohn Head, Cardiovascular Division Professor of Medicine University of Minnesota Medical School, USA Professor Azhar M. A. Faruqui Professor of Cardiology National Institute of Cardiovascular Diseases Karachi, Pakistan Dr. Alan Goble Heart Research Centre Melbourne, Australia Dr. Ivan Gyárfás Chief, Cardiovascular Disease Unit WHO, Geneva, Switzerland Professor Peter Mathes Professor of Cardiology Hoehenried Clinic for Cardiovascular Diseases Bernried, Germany Dr. John McMurray Consultant, Department of Cardiology Western General Hospital Edinburgh, Scotland Professor Walinjom F. T. Muna Acting Director, Chief of Medicine General Hospital Yaounde, Cameroon Professor Rodolfo Paoletti President, Italian Heart Foundation University di Milano Milan, Italy Dr. J. Papp President, Hungarian Society of Cardiology Szeged, Hungary Dr. Marc A. Pfeffer Cardiology Department Brigham & Women s Hospital Harvard Medical School Boston, Massachusetts, USA Professor Philip Poole-Wilson Royal Brompton Hospital National Heart & Lung Institute London, UK Professor Luigi Tavazzi Fondazione Clinica del Lavoro Pavia, Italy Professor Nanette K. Wenger Professor of Medicine (Cardiology) Emory University School of Medicine Atlanta, Georgia, USA 4
5 OBJECTIVE OF GUIDELINE Heart failure is a major and growing public health problem worldwide. It is common, costly, disabling and deadly. Early diagnosis and effective treatment reduce morbidity, mortality, and cost. The aim of these guidelines is to provide a concise summary, for primary care physicians (general practitioners), of the modern diagnostic and therapeutic approach to a patient with suspected heart failure. DEFINITIONS OF HEART FAILURE Pathophysiological Definition Cardiac failure is an inability of the heart to deliver blood (and therefore oxygen) at a rate commensurate with the requirements of the metabolising tissues at rest or during light exercise. This leads to characteristic systemic pathophysiological responses (neural, hormonal, renal and others), symptoms and signs. Clinical Definition Clinically the term heart failure is applied to the syndrome of breathlessness and fatigue associated with cardiac disease. It is often accompanied by fluid retention ( congestion ), as indicated by an elevated jugular venous pressure and oedema. Conditions leading to a mismatch between tissue oxygen delivery and demand (eg. anemia) may mimic the clinical signs of heart failure as may conditions causing fluid retention (eg. renal and hepatic failure). The clinical diagnosis of heart failure, therefore, necessitates both the presence of significant cardiac disease and typical symptoms and signs. 5
6 Clinical Diagnosis OF HEART FAILURE The clinical assessment of the patient with suspected heart failure seeks to answer two questions: (Figure 1; Diagnostic Algorithm) Are the patient s symptoms cardiac or non-cardiac in origin, i.e. is heart disease present? Where there is cardiac disease, what is the precise nature of the cardiac problem? FIGURE 1: Diagnostic Algorithm Suspected Heart failure? dyspnoea fatigue oedema Seek Evidence of Underlying Heart Disease 1. Clinical History previous myocardial infarction (MI) angina hypertension valvular disease/ rheumatic fever palpitations 2. Clinical Examination tachycardia raised jugular venous pressure (JVP) displaced apex beat 3rd heart sound murmur pulmonary crackles dependent oedema 3. Investigation electrocardiogram (ECG) chest X-ray (CXR) echocardiogram haemoglobin blood chemistry thyroid function tests Heart Failure Confirmed and Aetiology Determined (see table II, page 10) Systolic left ventricular (LV) dysfunction (the most frequent cause for heart failure) Diastolic LV dysfunction Valvular disease Congenital heart disease Pericardial disease Endocardial disease Rhythm/conduction disturbance 6
7 1. Clinical history Although dyspnoea and fatigue are the hallmarks of heart failure, they are also common in other conditions (eg. respiratory disease, obesity). Knowledge of a pre-existing myocardial (eg. past myocardial infarction) or valvular problem increases the probability that the patient s symptoms are due to heart failure. A history of angina, hypertension, rheumatic fever or previous cardiac surgery is also helpful. Palpitations may indicate a cardiac rhythm or conduction disorder that may be the cause (or result) of heart failure. Conversely, a history of other relevant medical problems (eg. anaemia, pulmonary, renal or hepatic disease) may reduce the probability of heart failure. 2. Clinical examination Many patients with heart failure have few and/or subtle clinical signs. Conversely, some physical signs, such as ankle oedema, are very nonspecific and may be seen in patients without cardiac disease. A raised jugular venous pressure (in the absence of anaemia, pulmonary, renal or hepatic disease), a rapid low amplitude pulse, a third heart sound and displacement of the apex beat are specific signs of cardiac disease. Blood pressure is usually normal or low for the patient s age provided that hypertensive heart disease is not the cause of the heart failure. Pulmonary crackles are non-specific in the absence of other signs of cardiac disease. Conversely, dyspnoea in the absence of cardiac signs as mentioned above is more suggestive of pulmonary or other disease. 3. Investigations The purpose of investigation is to: 1.) Confirm the diagnosis of heart failure by demonstrating underlying cardiac disease 2.) Define the cause of heart failure by characterizing the underlying cardiac problem 3.) Assist in the choice of optimal therapy (and avoid inappropriate treatment) by defining the precise cause of heart failure 4.) Obtain prognostic information 5.) Provide a reference point from which to measure the effects of treatment Blood tests help exclude anaemia, thyroid, hepatic and renal disease. The most commonly used cardiac investigations are the 12 lead electrocardiogram (ECG), the chest radiograph ( X-ray ) and, where available, the echocardiogram. 7
8 Clinical Diagnosis OF HEART FAILURE 12 lead ECG A completely normal 12 lead ECG is uncommon in a patient with heart failure. Even in pericardial disease the QRS complexes are usually of low voltage and the patient often has atrial fibrillation. However, a breathless patient with an abnormal ECG may not necessarily have heart failure. Table I shows how the ECG can help in defining the cause of heart failure. TABLE I: ECG Findings In Patients With Suspected Heart Failure Finding Q-waves; poor R wave progression Left ventricular hypertrophy (LVH) Left bundle-branch block (LBBB) Right bundle-branch block (RBBB) Atrial fibrillation Bradyarrhythmias Atrioventricular block Low voltage QRS complexes Significance Indicates previous MI; LV systolic dysfunction probable. May be due to hypertension, aortic stenosis, hypertrophic or dilated cardiomyopathy. May have either systolic or diastolic LV dysfunction. Usually indicates underlying heart disease May not denote underlying heart disease. Incomplete RBBB may indicate an atrial septal defect. RBBB and left anterior hemiblock (LAHB) are common in Chagas disease. Common in old age. May be caused by any cardiac disease. Should specifically consider mitral stenosis, pulmonary embolism, and thyrotoxicosis. If ventricular rate is very rapid may have rate related heart failure despite normal myocardial and valve function. Heart failure may be rate related Heart failure may be rate related. May be present in Chagas disease. May indicate pericardial constriction or effusion, infiltrative disease. 8
9 Chest radiograph In acute, or decompensated chronic, heart failure the chest x-ray may show florid alveolar pulmonary oedema, interstitial pulmonary oedema, basal pleural effusions or pulmonary venous engorgement. In older patients the most common finding is cardiac enlargement. Cardiomegaly is indicative of significant cardiac disease though it does not define the precise cardiac problem. For example, conditions as diverse as pericardial effusion, cor pulmonale, left ventricular aneurysm and mitral stenosis all cause radiographic cardiomegaly. It is important to realise, however, that significant left ventricular dysfunction can occur in the absence of radiographic cardiomegaly. Echocardiogram An important investigation in a patient with suspected heart failure is the echocardiogram. This ultrasonic examination visualises the cardiac chambers and valves. Systolic and diastolic ventricular contractile function can be measured, as can chamber size and wall thickness. Similarly, Doppler ultrasound enables valvular stenosis and regurgitation to be detected and quantified. Congenital heart defects, valvular vegetations, intracardiac tumours and intracavitary thrombus can also be detected. Ideally all patients with suspected heart failure should have an echocardiogram though this investigation is often not available. If a definite diagnosis of heart failure can be made clinically, eg. in a patient who has had a large myocardial infarction in the past or who has the characteristic auscultatory findings of mitral stenosis, echocardiography is not essential if access is limited. On the other hand echocardiography is strongly recommended where there is diagnostic uncertainty on clinical grounds (see pages 10-11). 9
10 DIAGNOSIS AS THE BASIS OF TREATMENT Optimal treatment is based on accurate diagnosis. Enough diagnostic information to enable appropriate treatment may be available from the history, examination and simple investigations. For example, a patient presenting with breathlessness for a number of months or years after myocardial infarction, and who has Q waves on the ECG, will almost certainly have heart failure due to left ventricular systolic dysfunction. The probability is even TABLE II: SUMMARY OF THE TYPES OF HEART FAILURE AND AETIOLOGY AND PATHOPHYSIOLOGY Myocardial Systolic Failure Heart failure is most commonly due to systolic dysfunction where the myocardium fails to contract normally; the left ventricle is usually dilated. Previous myocardial infarction, chronic hypertension, dilated cardiomyopthy, viral myocardits, Chagas disease and alcoholic heart disease are common causes of this type of heart failure. Myocardial Diastolic Failure Heart failure is sometimes due to diastolic ventricular dysfunction, where the myocardium is stiff, often because of hypertrophy, and fails to relax normally. This problem seems to be more common in the elderly and may have a better prognosis than systolic heart failure. Hypertension can cause this type of heart failure. Valvular Disease Valvular disease remains a common cause of heart failure in areas of the world where rheumatic fever is prevalent. Calcific aortic stenosis is also a frequent problem in elderly patients. TREATMENTS IN COMMON PRACTICE It is important to identify these patients, because prognosis in systolic heart failure is improved if an angiotensin converting enzyme (ACE) inhibitor is given in addition to diuretic and/or digoxin. Heart failure in patients with alcoholic cardiomyopathy often improves or resolves if they stop drinking. The optimal treatment for diastolic heart failure has yet to be determined. Underlying problems should be treated appropriately, eg., antihypertensive therapy should be given to lower elevated blood pressure, aiming to induce regression of left ventricular hypertrophy. Congestion should be relieved with diuretics. Surgery and other interventional procedures such as balloon valvuloplasty are of potentially great benefit. Inoperable regurgitant valvular disease may be helped by vasodilators. 10
11 greater if the chest x-ray shows cardiomegaly and/or pulmonary congestion. Other patients may need more thorough investigation, possibly necessitating referral to a cardiologist. Ultimately the precise cause of each patient s heart failure should be ascertained as different causes of heart failure require different treatments (Table II pages 10,11 and Figures 2 and 3, pages 12 and 16). THEIR TREATMENTS AETIOLOGY AND PATHOPHYSIOLOGY Pericardial Disease Pericardial constriction and effusion, for example, due to tuberculosis or viral disease may compromise pump function. Cardiac tamponade should be considered. Endocardial Disease Endocardial or endomyocardial fibrosis and its variant, Löffler s disease (endocarditis parietalis fibroplastica), cause a form of diastolic, or restrictive, heart failure. Congenital Heart Disease Many forms of congenital heart disease may cause heart failure in infancy or childhood. Some types (eg. atrial septal defect and aortic stenosis) may not present until late in life as heart failure. Metabolic Heart Disease Thyroid disease causes heart failure. Thiamine deficiency (beri beri) may cause heart failure in specific populations. Iron overload (haemochromatosis and haemosiderosis) may also cause myocardial injury. TREATMENTS IN COMMON PRACTICE If conservative treatment fails, pericardiocentesis, balloon pericardiotomy and surgical pericardiectomy may be of benefit. The pathophysiology of heart failure due to these conditions is poorly understood and its treatment is not well studied. Diuretics and digoxin are commonly given for symptomatic relief. Surgical as well as medical treatment is often required. Replacement or removal of the relevant nutritional, hormonal or metabolic factor is usually curative. 11
12 TREATMENT OF HEART FAILURE DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION FIGURE 2: Treatment Algorithm Heart Failure Standard Treatment Non-pharmacological Therapy low salt diet avoid alcohol avoid smoking regular moderate physical activity Pharmacological Therapy diuretic ACE inhibitor digoxin* ACE Inhibitor Not Tolerated Consider: hydralazine and isosorbide dinitrate Symptoms Persist Persisting Fluid Retention Consider: combination of oral diuretics such as loop diuretic with: thiazide or metolazone spironolactone Consider: Intravenous diuretic No Fluid Retention Consider: digoxin hydralazine and isosorbide dinitrate May require hospital admission and additional treatment * Some physicians use digoxin as first line therapy for heart failure, with diuretics and ACE inhibitors, whereas others reserve its use to those patients with atrial fibrillation or those patients whose symptoms persist. 12
13 NON-PHARMACOLOGICAL TREATMENT/LIFE-STYLE MODIFICATION Diet All patients need support and dietary advice regarding maintenance of optimal weight. Obesity increases the workload on the heart, especially during physical activity. Weight reduction, through restriction of dietary fat and calories is imperative for those who are obese, and is advised for those who are overweight. In patients with coronary heart disease and raised lipids, a low fat diet may delay recurrence of significant cardiovascular events. Conversely, maintenance or improvement of the nutritional status in wasted, undernourished or alcoholic patients is also important. Salt intake should be restricted as this may aggravate a patient s condition. Salt should not be added during cooking or at the table. Fluid intake Patients with heart failure often have an intense thirst, which can lead to excessive fluid intake and hyponatraemia. Fluid intake should be limited where possible, to about 2 liters a day for most patients. During periods of hot weather, diarrhoea, vomiting or fever, fluid intake may be increased or the dose of diuretic reduced. Alcohol intake Alcohol can damage the myocardium and precipitate arrhythmias. It should be avoided or used only in moderation. Smoking Smoking increases the risk of many cardiovascular, pulmonary and other problems, including cancers, and must be avoided at all costs. Exercise Bed rest is an important part of the treatment of acute heart failure or decompensated chronic heart failure, though early mobilization is important. Otherwise regular, and moderate physical activity for the condition of the patient, should be encouraged. This has significant symptomatic and 13
14 TREATMENT OF HEART FAILURE DUE TO LEFT VENTRICULAR SYSTOLIC DYSFUNCTION other benefits in patients with heart failure. Dynamic exercise activities such as walking, cycling, swimming, bowling, gardening, etc. should be continued at a pace that is comfortable for the patient. Vaccination Heart failure may predispose to and be exacerbated by pulmonary infection, which is a common cause of hospitalization. Therefore, influenza and pneumococcal vaccinations are recommended. DIURETICS For the patient with heart failure and fluid retention there is no more effective symptomatic treatment than a diuretic. Normally diuretics are used in combination with an ACE inhibitor and/or digoxin (see footnote, page 12). Four main principles underlie the use of diuretics in heart failure (see below). Loop diuretics are commonly used though in mild heart failure thiazide diuretics may suffice. The effective daily dose of frusemide is 40 mg (equivalent to 1 mg of bumetanide), but a reduced response may lead to a need for 80 to 120 mg daily. Overtreatment can cause hypovolaemia, hypotension and renal impairment. Principles of using diuretics for heart failure Use in moderation; avoid excessive doses of any single drug Make use of synergy between different classes of drugs, especially in cases of diuretic resistance (the principle of sequential nephron blockade) Monitoring of blood chemistry may help to avoid uraemia, hypokalaemia, and hyponatraemia Use in combination with an angiotensin converting enzyme (ACE) inhibitor and/or digoxin (see footnote, page 12), unless this is not tolerated 14
15 Patient Guidelines for Use All diuretics cause inconvenience for patients who usually have to organize their daily activities around the period of most intense diuresis. Thiazide diuretics cause a prolonged mild diuresis whereas loop diuretics cause a shorter, more vigorous diuresis. The effect of loop diuretics usually diminishes four hours after dosage. Patients should be informed that there is generally no fixed time of day that diuretics must be taken and, according to individual circumstances, the dose may be taken in the morning, afternoon or evening (but not too late as the diuresis may interrupt sleep). The patient may also be flexible with the diuretic dose according to need. Patients can be instructed to record their daily weight (on rising, after voiding, before breakfast) and, if there is a consistent (more than three consecutive days) increase in weight of more than 0.5 kg., they are advised to increase the diuretic dose until dry weight is regained. If the weight gain or symptoms worsen, the patient should be instructed to seek medical help. ANGIOTENSIN CONVERTING ENZYME (ACE) INHIBITORS (see figure 3 and table III) ACE inhibitors have been shown to be of benefit in all symptomatic classes of heart failure due to left ventricular systolic dysfunction. ACE inhibitors reduce vasoconstriction, improve pump function, and increase renal and skeletal muscle blood flow in heart failure. When given with diuretics, ACE inhibitors improve the symptoms and signs of all classes of heart failure and improve exercise tolerance. Increased severity of heart failure and need for hospital admission are reduced. Survival is improved in all classes of heart failure with ACE inhibitor treatment. The risk of myocardial infarction may also be reduced. 15
16 FIGURE 3: Initiation of an ACE Inhibitor in Heart Failure Heart failure confirmed BP 90 mm Hg systolic No contraindications to ACE inhibitor Blood chemistry normal Use with caution in high risk conditions (see table III) Stop K + supplements/k + sparing diuretics Advise patient/care-giver regarding dizziness Start with low dose of ACE inhibitor and titrate up Use test dose, then start dose titration after 1st dose Continue dose titration over next month Where possible, review within one week and check blood chemistry, then at three months and six months. Earlier monitoring is advised if chemistry is abnormal or in very elderly patients Guidelines for use Certain precautions should be taken before treatment is started. Potassium supplements and potassium sparing diuretics should be withdrawn. It is desirable that a baseline measurement of blood chemistry is made. The patient should be observed for two to four hours after the first dose. A low dose should be given initially - for example, enalapril 2.5 mg or captopril 6.25 mg - and regular treatment can then usually be started at an intermediate dose - enalapril 2.5 mg twice daily or captopril 12.5 mg three times daily. It is desirable that the patient should be reviewed after one or two weeks to check blood chemistry and for symptoms of hypotension; the drug dose should be modified accordingly. Provided the patient has not experienced significant hypotensive symptoms or a significant rise in serum creatinine or potassium concentration (>200 mmol/l or 5.5 mmol/l respectively), the dose of ACE inhibitor should be increased as tolerated. Larger doses such as enalapril 10 mg given twice daily or captopril 50 mg three times daily are recommended as these dosages have been shown to be ben- 16
17 eficial in clinical trials. The correct dose of ACE inhibitors in heart failure should be guided by clinical trials and individual patient response. For certain patients at high risk (Table III), specialist assessment is desirable and hospital admission may be advisable. TABLE III High-risk conditions for which specialist assessment is desirable Severe heart failure (New York Heart Association class III or IV shortness of breath on slight effort or at rest); patients with a dose of 80 mg of frusemide or equivalent Low systolic blood pressure (<90 mmhg) Low serum concentration of sodium (<130 mmol/l) or high potassium concentration >5.5 mmol/l Existing renal dysfunction (serum creatinine concentration [2.26 mg%] >200µmol/L) Severe generalized atherosclerosis (especially if intermittent claudication and arterial bruits are present) ie., risk of renal artery stenosis Severe chronic obstructive airways disease and pulmonary heart disease (cor pulmonale) ie., risk of fixed pulmonary hypertension Adverse effects of angiotensin converting enzyme inhibitors Hypotension Some reduction in blood pressure is expected but it usually induces no symptoms. However symptomatic hypotension may occur in a small percentage of patients. If it does occur, the patient may be hypovolemic, in which case treatment can often be restarted after correction of dehydration.ensure that obstructive valve disease is not present, and that the patient does not have diastolic rather than systolic left ventricular dysfunction. Renal dysfunction In patients with mild and moderate heart failure in clinical trials only small changes in serum creatinine and urea concentration (8.8 µmol/l [0.10 mg%] and 1.2 mmol/l [3.2 mg%] respectively) occurred after treatment. Among patients with severe heart failure, many of whom had abnormal baseline blood chemistry, serum creatinine concentration was as likely to fall as it was to increase after starting ACE inhibitor treatment. As with symptomatic hypotension, renal dysfunction is often exacerbated by dehydration. Non-steroidal anti-inflammatory drugs (NSAIDs) may also cause 17
18 renal dysfunction and should be avoided if possible in patients receiving ACE inhibitors. Patients should be advised not to purchase and use over the counter NSAIDs. See co-prescribing, page 21. Hyperkalaemia Few patients with mild and moderate heart failure develop worrisome hyperkalaemia ie., K + > 5.5 mmol/l. This has rarely been a cause of withdrawal in the large trials using an ACE inhibitor. Dehydration, NSAIDs, and potassium-sparing diuretics increase the risk of hyperkalaemia. If these are not responsible the dose of ACE inhibitor should be reduced and K + monitored carefully. Cough Cough is common in patients with heart failure and pulmonary oedema/congestion should always be excluded. ACE inhibitors can also cause cough, though this was only troublesome enough to cause treatment withdrawal in a very small percentage of patients in the large ACE inhibitor clinical trials. Advice to the patient and care-givers Symptomatic patients should be informed that they are likely to notice a gradual improvement in their symptoms, and that this may take some weeks to develop fully. Patients who become asymptomatic should be informed that their treatment is being continued to keep them well. Patients can also be advised that future hospitalization is less likely and that life expectancy is improved by treatment with an ACE inhibitor. Patients should be warned that dizziness may occur initially, after starting treatment, though this is usually transient and resolves with lying down. If it is persistent and troublesome, a doctor should be notified before further doses are taken. If patients become dehydrated (eg, due to diarrhoea and vomiting or a hot climate), dizziness may occur. A temporary increase in fluid intake and/or reduction in diuretic dose usually results in resolution. Cough and, less commonly, taste disturbance may occur within the first few weeks of starting treatment. If the adverse effect is not particularly troublesome, patients may be willing to accept it in light of the substantial benefits of ACE inhibitor therapy. 18
19 DIGOXIN Digoxin should be used to control the ventricular rate, where necessary,in patients with heart failure and atrial fibrillation. Digoxin is also of benefit in patients with heart failure who are in sinus rhythm. Although usually considered a positive inotropic agent, digoxin is known to have other important effects in heart failure. These include neuroendocrine suppression, especially sympathetic nervous system inhibition, and arterial vasodilatation. Digoxin also has complex direct and indirect electrophysiological effects. Digoxin is of symptomatic benefit in patients with heart failure in sinus rhythm though survival data will not be available until the DIG (Digitalis Investigation Group) Trial reports in Digoxin is also of symptomatic benefit when given with an ACE inhibitor and diuretic and this is its main indication in patients with heart failure who are in sinus rhythm. Most trials showing clinical benefit have used daily doses between and mg, though a lower dose may be required in elderly patients and those with impaired renal function. The incidence of digoxin toxicity in outpatients appears to be low, about one episode for every 20 years of treatment. This is supported by the recent large digoxin trials where the incidence of adverse effects with digoxin has been no different from that with placebo. However, the presence of renal insufficiency augments the risk of toxicity. Some potential drug interactions are relevant to heart failure. Hypokalaemia (caused by diuretics) increases the risk of digoxin toxicity. Amiodarone and quinidine increase serum digoxin concentrations due to a pharmacokinetic interaction. OTHER VASODILATORS Hydralazine and isosorbide dinitrate This combination improves symptoms, exercise tolerance, and survival in patients with heart failure. The combination is not as widely used as ACE inhibitors because it has more side effects and less survival benefit. It is, however, indicated where ACE inhibitors are not tolerated. Hydralazine - isosorbide dinitrate may also be used in addition to ACE inhibitors in the patient who remains symptomatic. The target daily dose in divided doses should be 300 mg hydralazine and mg isosorbide dinitrate. 19
20 OTHER DRUGS Aspirin Patients with heart failure due to coronary artery disease or who have concomitant peripheral or cerebrovascular disease may benefit from low dose (75mg -325 mg) aspirin, because of its platelet antiaggregant property. Warfarin Patients with atrial fibrillation and heart failure should always be considered for warfarin treatment. Any other patient who has had a thromboembolic episode or who has been shown to have intracardiac thrombus should be considered for treatment with warfarin. The place of anticoagulation in patients with heart failure who are in sinus rhythm and who do not have intracardiac thrombus or a history of thromboembolism is uncertain. Beta Adrenoreceptor Antagonists Initiation of conventional doses of beta blockers in patients with heart failure can cause profound haemodynamic and clinical deterioration. There is, however, some evidence that cautious introduction of a very low dose of beta blocker, under careful observation, followed by gradual dose titration may lead to symptomatic and, possibly, survival benefit. At present the precise role of beta blockers in the treatment of heart failure is uncertain and the results of ongoing trials are awaited. APPARENTLY INTRACTABLE HEART FAILURE (also see Figure 2 page 12) Patients who do not respond to standard therapy with a diuretic and ACE inhibitor should be referred for specialist assessment. Adding digoxin and/or the combination of hydralazine and isosorbide dinitrate may help. If there is persisting fluid retention, the addition of a thiazide diuretic or metolazone may induce diuresis. The addition of spironolactone may also initiate a diuresis. Each of these strategies merits careful 20
21 monitoring of the blood chemistry. Short term use (a few days to a week) of additional diuretic therapy is usually all that is required. Intravenous diuretic may be necessary in the patient with very resistant oedema or persistent symptoms. Many patients who do not respond to standard treatment are best referred to a cardiologist for hospital admission and some combination of bed rest, fluid restriction, intravenous diuretic, dobutamine, sodium nitroprusside or dopamine. Invasive haemodynamic monitoring is often helpful in establishing treatment goals and efficacy. Cardiac transplantation may be considered in selected cases. In patients with severe diuretic resistant heart failure, careful nursing attention is important. Sleeping with the head elevated in bed or in a comfortable chair may prevent distressing nocturnal breathlessness. OTHER ASPECTS OF MANAGEMENT CO-PRESCRIBING Care in co-prescribing cannot be over-emphasized. The following drugs should be used with caution and usually avoided: NSAIDs Calcium channel blockers (except possibly amlodipine) Antiarrhythmics (except amiodarone) Beta blockers (see page 20) Corticosteroids Tricyclic antidepressants Lithium Carbenoloxone 21
22 NON-ADHERENCE Careful advice about the rationale behind treatment, especially diuretic treatment, and an explanation about flexible timing of doses may help to prevent non-compliance. When ACE inhibitors are prescribed for patients rendered asymptomatic by diuretics the patient should be told of their prophylactic benefit in maintaining stability, preventing hospitalisation and improving survival. MANAGEMENT OF CONCOMITANT PROBLEMS Many patients with heart failure have concomitant problems which either reflect the underlying cause of their heart failure (e.g., angina) or are a consequence of it (e.g., ventricular arrhythmias). The management of these concomitant problems in patients with heart failure is often different from that in patients who do not have heart failure. This section briefly highlights the concomitant problems typically present in patients with heart failure. ATRIAL FIBRILLATION Up to 30 percent of patients with heart failure have concomitant atrial fibrillation. Five questions should be asked before management is started (see below). Control of ventricular rate is usually achieved with digoxin; if there is difficulty, consider amiodarone but remember that digitalis toxicity may develop. Thromboembolism should be prevented, and recent trials have shown substantial benefit from treatment with warfarin. Cardioversion, possibly preceded and followed by treatment with amiodarone, should be considered as, ideally, sinus rhythm should be restored. Issues affecting management of atrial fibrillation in patients with heart failure Is atrial fibrillation the cause or consequence of heart failure? Could the patient have mitral valve disease? Could the patient have thyrotoxicosis? Is atrial fibrillation part of sick sinus syndrome? (Bradycardia may aggravate heart failure, and digoxin may aggravate bradycardia.) Are there any contraindications to the use of warfarin? 22
23 ANGINA As the commonest cause of heart failure is coronary artery disease, many patients also have angina. Coronary artery bypass grafting should be considered if the patient is otherwise suitable for surgery. Coronary angioplasty or other transcatheter revascularization procedure may also be appropriate. Prognosis may be improved by surgery in patients with extensive coronary artery disease and left ventricular dysfunction. Advanced age (>75 years) and severe left ventricular dysfunction (left ventricular ejection fraction <20%) are relative contraindications. The only antiischaemic drugs available that do not exacerbate pump dysfunction are the nitrates and possibly amlodipine (see beta blockers, page 20). VENTRICULAR ARRHYTHMIA Patients with symptoms of palpitations, dizziness, and blackouts should be investigated for arrhythmias, since symptomatic ventricular arrhythmia requires treatment. Before an antiarrhythmic drug is given, possible precipitating or aggravating factors must be excluded. (see below). The drug to consider is amiodarone; others are likely to worsen a patient's overall condition and even the arrhythmia. Beta blockers may be useful, if tolerated. The role of implantable pacemaker and defibrillator devices in patients with heart failure is not yet clear. Possible precipitating or aggravating factors for ventricular arrhythmia Electrolyte disturbance, eg. hypokalaemia, hypomagnesaemia, hyperkalaemia Digoxin toxicity Drugs exacerbating pump dysfunction, eg. most antiarrhythmic drugs and some calcium channel blockers Drugs causing electrical instability, eg. most antiarrhythmic drugs (except amiodarone) and antidepressants Recurrent myocardial ischaemia Respiratory disease, infection, hypoxaemia, hyperthyroidism 23
24 Prevention of heart failure Prevention of heart failure is a major aim of modern cardiological practice because the burden of symptoms is so high and prognosis is so poor once overt cardiac failure is established. This aim can be achieved by a) preventing the development of causal heart disease, eg. myocardial infarction, hypertensive heart disease and b) preventing the progression of established cardiac disease to heart failure. The role of smoking, cholesterol, sedentary lifestyle and other factors in promoting the development of coronary heart disease (CHD) are well recognised and can be altered. Hypertension also increases the risk of developing CHD and the risk of developing heart failure through direct, chronic, myocardial damage. Antihypertensive therapy has been clearly shown to reduce the risk of developing heart failure. Improved socioeconomic conditions and antimicrobial therapy have reduced the incidence of rheumatic heart disease in many societies. Once cardiac disease is established its progression to heart failure can also be reduced. Infarct size can be limited by thrombolytic therapy and reinfarction reduced by aspirin, beta blockers, and, possibly, ACE inhibitors. In asymptomatic patients with substantial impairment of left ventricular function prophylactic ACE inhibitor therapy has been shown to reduce the risk of developing heart failure and to improve survival. 24
25 Conclusion In a patient with suspected heart failure, precise diagnosis of the underlying cardiac problem is the basis of optimal treatment. Non-pharmacological, pharmacological, and surgical treatments are available. With modern treatment, both morbidity and mortality from heart failure can be substantially reduced. Bibliography 1. Cohn JN, Archibald DG, Ziesche S, Franciosa JA, Harston WE, Tristani FE,et al. Effect of vasodilator therapy on mortality in chronic congestive heart failure. Results of a Veterans Affairs Administration Cooperative study. N Engl J Med 1986;314: CONSENSUS Trial Study Group. Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandinavian Enalapril Survival Study. N Engl J Med 1987;316: The SOLVD Investigators. Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med 1991;325: Cohn JN, Johnson G, Ziesche S, Cobb F, Francis G, Tristani F, et al. A comparison of enalapril with hydralazine-isosorbide dinitrate in the treatment of chronic congestive heart failure. N Engl J Med 1991;325: The SOLVD Investigators. Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. N Engl J Med 1992;327: Pfeffer MA, Braunwald E, Moye LA, Basta L, Brown EJ Jr, Cuddy TE, et al for the SAVE investigators. Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infraction. Results of the Survival and Ventricular Enlargement trial. N Engl J Med 1992;327: The Captopril-digoxin Multicenter Research Group. Comparative effects of therapy with captopril and digoxin in patients with mild to moderate heart failure. JAMA 1988;259: Kleber FX, Niemöller L, Doering W. Impact of converting enzyme inhibition on progression of chronic heart failure: results of the Munich mild heart failure trial. Br Heart J 1992;67: Mujais SK, Nora NA, Levin ML. Principles and clinical uses of diuretic therapy. Prog Cardiovasc Dis 1992;35: Smith TW. Digoxin in heart failure. N Engl J Med 1993;329: Packer M, Gheorghiade M, Young JB, Constantini PJ, Adams KF, Cody RJ, et al for the RADIANCE study. Withdrawal of digoxin from patients with chronic heart failure treated with angiotensin-converting enzyme-inhibitors. N Engl J Med 1993;329:
26 WORLD HEALTH ORGANIZATION/COUNCIL ON GERIATRIC CARDIOLOGY TASK FORCE ON HEART FAILURE EDUCATION 8-00-RNT-95-W G-SBI
27 Concise Guide to the Management of Heart Failure WORLD HEALTH ORGANIZATION/COUNCIL ON GERIATRIC CARDIOLOGY TASK FORCE ON HEART FAILURE EDUCATION
SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE
 SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE Summary Heart failure has a worse prognosis than many cancers with an annual mortality of 40% in the first year following diagnosis and 10% thereafter.
SPECIALTY : CARDIOLOGY CLINICAL PROBLEM: HEART FAILURE Summary Heart failure has a worse prognosis than many cancers with an annual mortality of 40% in the first year following diagnosis and 10% thereafter.
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
The new Heart Failure pathway
 The new Heart Failure pathway An integrated and seamless Strategy Dr Sunil Balani Definition of Heart Failure The inability of the heart to pump blood at a rate commensurate with the requirements of metabolising
The new Heart Failure pathway An integrated and seamless Strategy Dr Sunil Balani Definition of Heart Failure The inability of the heart to pump blood at a rate commensurate with the requirements of metabolising
1 Congestive Heart Failure & its Pharmacological Management
 Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
HYPERTENSION ASSOCIATED WITH RENAL DISEASES
 RENAL DISEASE v Patients with renal insufficiency should be encouraged to reduce dietary salt and protein intake. v Target blood pressure is less than 135-130/85 mmhg. If patients have urinary protein
RENAL DISEASE v Patients with renal insufficiency should be encouraged to reduce dietary salt and protein intake. v Target blood pressure is less than 135-130/85 mmhg. If patients have urinary protein
Cardiovascular System & Its Diseases. Lecture #4 Heart Failure & Cardiac Arrhythmias
 Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
Cardiovascular System & Its Diseases Lecture #4 Heart Failure & Cardiac Arrhythmias Dr. Derek Bowie, Department of Pharmacology & Therapeutics, Room 1317, McIntyre Bldg, McGill University derek.bowie@mcgill.ca
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
A Patients Guide to Heart Failure
 A Patients Guide to Heart Failure Exceptional healthcare, personally delivered Heart Failure The term heart failure means that your heart is weakened and is having difficulty in pumping as hard as it would
A Patients Guide to Heart Failure Exceptional healthcare, personally delivered Heart Failure The term heart failure means that your heart is weakened and is having difficulty in pumping as hard as it would
Heart Disease: Diagnosis & Treatment
 How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
Cardiovascular Risk in Diabetes
 Cardiovascular Risk in Diabetes Lipids Hypercholesterolaemia is an important reversible risk factor for cardiovascular disease and should be tackled aggressively in all diabetic patients. In Type 1 patients,
Cardiovascular Risk in Diabetes Lipids Hypercholesterolaemia is an important reversible risk factor for cardiovascular disease and should be tackled aggressively in all diabetic patients. In Type 1 patients,
Case Study 8: Heart Failure
 Case Study 8: Heart Failure April 2000 Scenario Mr James is a 68 year old man who presents to you for the first time complaining of increasing shortness of breath on exertion. He was prescribed frusemide
Case Study 8: Heart Failure April 2000 Scenario Mr James is a 68 year old man who presents to you for the first time complaining of increasing shortness of breath on exertion. He was prescribed frusemide
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Atrial fibrillation. Quick reference guide. Issue date: June 2006. The management of atrial fibrillation
 Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Atrial Fibrillation Based on ESC Guidelines. Moshe Swissa MD Kaplan Medical Center
 Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
Atrial Fibrillation The High Risk Obese Patient
 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Hypertension Guidelines
 Overview Hypertension Guidelines Aim to reduce Blood Pressure to 140/90 or less (140/80 for diabetics), adding drugs as needed until further treatment is inappropriate or declined. N.B. patients do not
Overview Hypertension Guidelines Aim to reduce Blood Pressure to 140/90 or less (140/80 for diabetics), adding drugs as needed until further treatment is inappropriate or declined. N.B. patients do not
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
Protocol for the management of atrial fibrillation in primary care
 Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
5. Management of rheumatic heart disease
 5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
Adult Cardiac Surgery ICD9 to ICD10 Crosswalks
 164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal. Drugs for the treatment of pulmonary arterial hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
National Medicines Information Centre
 National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 www.nmic.ie THE CONTEMPORARY MANAGEMENT OF ATRIAL FIBRILLATION VOLUME 12 NUMBER 3 2006
National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 www.nmic.ie THE CONTEMPORARY MANAGEMENT OF ATRIAL FIBRILLATION VOLUME 12 NUMBER 3 2006
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
The development of a pathway to support the management of patients requiring palliative care are ongoing.
 South East Wales Cardiac Network Model Pathway for Heart Failure CHD NSF Key Action 25 Introductory statement This pathway has been developed in line with the document 'Tackling CHD in Wales: Implementing
South East Wales Cardiac Network Model Pathway for Heart Failure CHD NSF Key Action 25 Introductory statement This pathway has been developed in line with the document 'Tackling CHD in Wales: Implementing
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Universitätsklinik für Kardiologie. Test. Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1
 Test Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1 Heart Failure - Definition European Heart Journal (2008) 29, 2388 2442 Akute Herzinsuffizienz Diagnostik und
Test Thomas M. Suter Akute Herzinsuffizienz Diagnostik und Therapie thomas.suter@insel.ch 1 Heart Failure - Definition European Heart Journal (2008) 29, 2388 2442 Akute Herzinsuffizienz Diagnostik und
Department of Cardiology Royal Berkshire Hospital. Heart Failure. Information for patients
 Department of Cardiology Royal Berkshire Hospital Heart Failure Information for patients Introduction Heart failure can be caused by various heart conditions, which can be treated in different ways, to
Department of Cardiology Royal Berkshire Hospital Heart Failure Information for patients Introduction Heart failure can be caused by various heart conditions, which can be treated in different ways, to
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
DISCLOSURES RISK ASSESSMENT. Stroke and Heart Disease -Is there a Link Beyond Risk Factors? Daniel Lackland, MD
 STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
Hypertension and Heart Failure Medications. Dr William Dooley
 Hypertension and Heart Failure Medications Dr William Dooley Plan Heart Failure Acute vs. chronic Mx Hypertension Common drugs used Method of action Choice of medications Heart Failure Aims; Short term:
Hypertension and Heart Failure Medications Dr William Dooley Plan Heart Failure Acute vs. chronic Mx Hypertension Common drugs used Method of action Choice of medications Heart Failure Aims; Short term:
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Case Study 6: Management of Hypertension
 Case Study 6: Management of Hypertension 2000 Scenario Mr Ellis is a fit 61-year-old, semi-retired market gardener. He is a moderate (10/day) smoker with minimal alcohol intake and there are no other cardiovascular
Case Study 6: Management of Hypertension 2000 Scenario Mr Ellis is a fit 61-year-old, semi-retired market gardener. He is a moderate (10/day) smoker with minimal alcohol intake and there are no other cardiovascular
HYPERTROPHIC CARDIOMYOPATHY
 HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
SYMPTOMS Heart failure symptoms may vary and can be hard to detect. Symptoms may include:
 Heart Failure Heart failure is a condition in which the heart has trouble pumping blood. This means your heart does not pump blood efficiently for your body to work well. In some cases of heart failure,
Heart Failure Heart failure is a condition in which the heart has trouble pumping blood. This means your heart does not pump blood efficiently for your body to work well. In some cases of heart failure,
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
MINISTRY OF HEALTH AND LONG-TERM CARE Primary Health Care Team FACT SHEET
 Title: Date: April 2008 MINISTRY OF HEALTH AND LONG-TERM CARE Primary Health Care Team FACT SHEET HEART FAILURE MANAGEMENT INCENTIVE Eligible Patient Enrolment Models (PEMs): Family Health Networks (FHNs)
Title: Date: April 2008 MINISTRY OF HEALTH AND LONG-TERM CARE Primary Health Care Team FACT SHEET HEART FAILURE MANAGEMENT INCENTIVE Eligible Patient Enrolment Models (PEMs): Family Health Networks (FHNs)
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
Inpatient Heart Failure Management: Risks & Benefits
 Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Inpatient Heart Failure Management: Risks & Benefits Dr. Kenneth L. Baughman Professor of Medicine Harvard Medical School Director, Advanced Heart Disease Section Brigham & Women's Hospital Harvard Medical
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology
 Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
Cardiology ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Cardiology Chapter 4: Endocrine, Nutritional, and Metabolic Diseases (E00-E89) The diabetes mellitus codes are combination codes
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Congestive Heart Failure
 Healthy People 2010 Conference Health Education on the Internet Welcome Mr. System Administrator Congestive Heart Failure What is congestive heart failure? How does it occur? What are the symptoms? How
Healthy People 2010 Conference Health Education on the Internet Welcome Mr. System Administrator Congestive Heart Failure What is congestive heart failure? How does it occur? What are the symptoms? How
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
How To Treat Dilated Cardiomyopathy
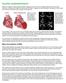 DILATED CARDIOMYOPATHY Dilated or congestive cardiomyopathy (DCM) is diagnosed when the heart is enlarged (dilated) and the pumping chambers contract poorly (usually left side worse than right). A diagram
DILATED CARDIOMYOPATHY Dilated or congestive cardiomyopathy (DCM) is diagnosed when the heart is enlarged (dilated) and the pumping chambers contract poorly (usually left side worse than right). A diagram
1p36 and the Heart. John Lynn Jefferies, MD, MPH, FACC, FAHA
 1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation
 A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
HEART FAILURE ROBERT SOUFER, M.D.
 CHAPTER 14 HEART FAILURE ROBERT SOUFER, M.D. The heart s primary function is to pump blood to all parts of the body, bringing nutrients and oxygen to the tissues and removing waste products. When the body
CHAPTER 14 HEART FAILURE ROBERT SOUFER, M.D. The heart s primary function is to pump blood to all parts of the body, bringing nutrients and oxygen to the tissues and removing waste products. When the body
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
SIGN. Management of chronic heart failure. Scottish Intercollegiate Guidelines Network. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 95 Management of chronic heart failure A national clinical guideline 1 Introduction
SIGN Scottish Intercollegiate Guidelines Network Help us to improve SIGN guidelines - click here to complete our survey 95 Management of chronic heart failure A national clinical guideline 1 Introduction
Anaesthesia and Heart Failure
 Anaesthesia and Heart Failure Andrew Baldock, Specialist Registrar, Southampton University Hospitals NHS Trust E mail: ajbaldock@doctors.org.uk Self-assessment The following true/false questions may be
Anaesthesia and Heart Failure Andrew Baldock, Specialist Registrar, Southampton University Hospitals NHS Trust E mail: ajbaldock@doctors.org.uk Self-assessment The following true/false questions may be
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Congestive heart failure (CHF) is a. Diastolic Heart Failure. By Michel D Astous, MD, FRCPC
 Diastolic Heart Failure The evaluation of both systolic and diastolic functions is of great importance among patients presenting with signs of CHF, as the treatment may be quite different depending on
Diastolic Heart Failure The evaluation of both systolic and diastolic functions is of great importance among patients presenting with signs of CHF, as the treatment may be quite different depending on
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
CorCap Cardiac Support Device Patient Information Booklet
 What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
HEART DISEASE IN THE ELDERLY
 CHAPTER 21 HEART DISEASE IN THE ELDERLY LAWRENCE H. YOUNG, M.D. INTRODUCTION The elderly represent the fastest-growing segment of the American population. By the year 2000, it is estimated that people
CHAPTER 21 HEART DISEASE IN THE ELDERLY LAWRENCE H. YOUNG, M.D. INTRODUCTION The elderly represent the fastest-growing segment of the American population. By the year 2000, it is estimated that people
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Atrial Fibrillation (AF) Explained
 James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
Heart Failure: Diagnosis and Treatment
 Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Heart Failure: Diagnosis and Treatment Approximately 5 million people about 2 percent of the U.S. population are affected by heart failure. Diabetes affects 20.8 million Americans and 65 million Americans
Diabetic nephropathy is detected clinically by the presence of persistent microalbuminuria or proteinuria.
 Kidney Complications Diabetic Nephropathy Diabetic nephropathy is detected clinically by the presence of persistent microalbuminuria or proteinuria. The peak incidence of nephropathy is usually 15-25 years
Kidney Complications Diabetic Nephropathy Diabetic nephropathy is detected clinically by the presence of persistent microalbuminuria or proteinuria. The peak incidence of nephropathy is usually 15-25 years
Heart Failure Outpatient Clinical Pathway
 Heart Failure Outpatient Clinical Pathway PHASE 1: PHASE 2: PHASE 3: PHASE 4: Initial Consult and Treatment Optimization of Therapy Reassessment and Further Optimization Maintenance I. Provider II. Consults
Heart Failure Outpatient Clinical Pathway PHASE 1: PHASE 2: PHASE 3: PHASE 4: Initial Consult and Treatment Optimization of Therapy Reassessment and Further Optimization Maintenance I. Provider II. Consults
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT
 RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
Cardiology Fact Sheet. ACVIM Fact Sheet: Myxomatous Mitral Valve Degeneration
 Cardiology Fact Sheet ACVIM Fact Sheet: Myxomatous Mitral Valve Degeneration Overview Myxomatous mitral valve degeneration (MMVD) is the most common acquired type of heart disease and new murmurs in older
Cardiology Fact Sheet ACVIM Fact Sheet: Myxomatous Mitral Valve Degeneration Overview Myxomatous mitral valve degeneration (MMVD) is the most common acquired type of heart disease and new murmurs in older
Drug Treatment in Type 2 Diabetes with Hypertension
 Hypertension is 1.5 2 times more prevalent in Type 2 diabetes (prevalence up to 80 % in diabetic subjects). This exacerbates the risk of cardiovascular disease by ~ two-fold. Drug therapy reduces the risk
Hypertension is 1.5 2 times more prevalent in Type 2 diabetes (prevalence up to 80 % in diabetic subjects). This exacerbates the risk of cardiovascular disease by ~ two-fold. Drug therapy reduces the risk
Sign up to receive ATOTW weekly - email wfsahq@anaesthesiologists.org
 ATRIAL FIBRILLATION (AF). PERI-OPERATIVE MANAGEMENT FOR NON-CARDIAC SURGERY ANAESTHESIA TUTORIAL OF THE WEEK 307 28 th APRIL 2014 Dr J Sokhi Southend University Hospital, UK Professor J Kinnear Southend
ATRIAL FIBRILLATION (AF). PERI-OPERATIVE MANAGEMENT FOR NON-CARDIAC SURGERY ANAESTHESIA TUTORIAL OF THE WEEK 307 28 th APRIL 2014 Dr J Sokhi Southend University Hospital, UK Professor J Kinnear Southend
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below
 Name: generic (trade) Rivaroxaban (Xarelto ) HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below What it is Indications
Name: generic (trade) Rivaroxaban (Xarelto ) HERTFORDSHIRE MEDICINES MANAGEMENT COMMITTEE (HMMC) RIVAROXABAN RECOMMENDED see specific recommendations for licensed indications below What it is Indications
INTRODUCTION TO EECP THERAPY
 INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
Acquired, Drug-Induced Long QT Syndrome
 Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Tackling the Semantic Interoperability challenge
 European Patient Summaries: What is next? Tackling the Semantic Interoperability challenge Dipak Kalra Cross-border health care The context for sharing health summaries Also useful for within-border health
European Patient Summaries: What is next? Tackling the Semantic Interoperability challenge Dipak Kalra Cross-border health care The context for sharing health summaries Also useful for within-border health
Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease
 Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
PULMONARY HYPERTENSION. Charles A. Thompson, M.D., FACC, FSCAI Cardiovascular Institute of the South Zachary, Louisiana
 PULMONARY HYPERTENSION Charles A. Thompson, M.D., FACC, FSCAI Cardiovascular Institute of the South Zachary, Louisiana What is Pulmonary Hypertension? What is normal? Pulmonary artery systolic pressure
PULMONARY HYPERTENSION Charles A. Thompson, M.D., FACC, FSCAI Cardiovascular Institute of the South Zachary, Louisiana What is Pulmonary Hypertension? What is normal? Pulmonary artery systolic pressure
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation
 INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
CONGESTIVE HEART FAILURE PATIENT TEACHING
 CONGESTIVE HEART FAILURE PATIENT TEACHING What is Heart Failure? Congestive Heart Failure occurs when the heart loses its ability to pump enough blood to meet the body s needs. Because the heart is not
CONGESTIVE HEART FAILURE PATIENT TEACHING What is Heart Failure? Congestive Heart Failure occurs when the heart loses its ability to pump enough blood to meet the body s needs. Because the heart is not
Atrial Fibrillation. Information for you, and your family, whänau and friends. Published by the New Zealand Guidelines Group
 Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
