Pulmonary Vein İsolation with the Cryoballoon: Simpler, Faster But Equally Effective?
|
|
|
- Jasmin Stevens
- 8 years ago
- Views:
Transcription
1 Pulmonary Vein İsolation with the Cryoballoon: Simpler, Faster But Equally Effective? Gian Battista Chierchia M.D., Antonio Sorgente M.D., Fatih Bayrak M.D., Andrea Sarkozy M.D., Carlo De Asmundis M.D., Pedro Brugada M.D. Heart Rhythm Management Centre, Uz Brussel-vub, Brussels, Belgium ABSTRACT Atrial Fibrillation (AF) is the most frequently encountered arrhythmia in clinical practice that represents an enormous burden for our current health care systems. Since the demonstration of pulmonary vein (PV) ectopic activity as the main trigger of paroxysmal AF, radiofrequency ablation (RF) of this arrhythmia has become an increasingly popular procedure in many electrophysiology laboratories. Nowadays creation of circumferential lesions around the PVs is certainly the most widespread technique to achieve PV isolation. Recently, novel balloon shaped ablation catheters have proven very effective in producing PV isolation with the added potential ability of achieving complete circular lesions with a single application. However, the cryoballoons currently available do not always adapt themselves well to the anatomical variants and do not systematically isolate the PVs in one application. Ideally, a more compliant balloon which would fit into most PVs might lead to a more effective procedure. Future technological improvements might lead a larger number of electrophysiologists to adopt such a technique. KEYWORDS Ablation, atrial fibrillation, catheter, cryoballoon, isolation, pulmonary vein
2 62 Türk Aritmi, Pacemaker ve Elektrofizyoloji Dergisi Kriyobalon ile Pulmoner Ven İzolasyonu: Basit, Hızlı... Fakat Eşit Etkili mi? ÖZET Atriyal fibrilasyon klinik uygulamada en sık karşılaşılan aritmidir ve sağlık sistemi üzerine önemli bir yük getirmektedir. Pulmoner venlerdeki (PV) ektopik aktivitenin paroksizmal AF için ana tetikleyici olduğu gösterilmesiyle bu aritminin radyofrekans (RF) ablasyonu birçok elektrofizyoloji laboratuvarında popüler bir işlem haline gelmiştir. Günümüzde PV izolasyonunda dairesel lezyonların PV etrafında oluşturulması en yaygın tekniktir. Son zamanlarda yeni balon şeklindeki ablasyon kateterlerinin etkili PV izolasyonunda tek uygulama ile tam dairesel lezyon oluşturma başarıları kanıtlanmıştır. Bununla birlikte halen kullanılan kriyobalonlar anatomik çeşitliliğe tam uyum göstermemekte ve tek uygulama ile sistematik olarak PV ler izole edilememektedir. PV lere daha iyi uyum sağlayan balonlar daha etkili olabilir. Gelecek teknolojik ilerlemeler çok sayıda elektrofizyologun böyle tekniklere uyum sağlamasına neden olabilir. ANAHTAR KELİMELER Ablasyon, atriyal fibrilasyon, kateter, kriyobalon, izolasyon, pulmoner ven İLETİŞİM ADRESİ Gian Battista Chierchia MD Heart Rhythm Management Centre UZ Brussel-VUB Laarbeeklaan 101, 1090 Brussels, Belgium Introduction Atrial Fibrillation (AF) is the most frequently encountered arrhythmia in clinical practice that represents an enormous burden for our current health care systems. Since the demonstration of pulmonary vein (PV) ectopic activity as the main trigger of paroxysmal AF (1,2), radiofrequency ablation (RF) of this arrhythmia has become an increasingly popular procedure in many electrophysiology laboratories. Nowadays creation of circumferential lesions around the PVs is certainly the most widespread technique to achieve PV isolation. In most centers, this procedure is achieved by performing a point by point lesion that renders the creation of continuous lines difficult and permits the formation of electrical gaps which may lead to arrhythmic recurrence (3). Additionally even in experienced hands this approach is still too cumbersome (4). Furthermore, AF ablation using RF is associated with a certain number of serious complications such as PV stenosis, thrombo-embolism, pericardial tamponade, and atrio-oesophageal fistula (4). Recently, novel balloon shaped ablation catheters have proven very effective in producing PV isolation with the added potential ability of achieving complete circular lesions with a single application (5). Among the latter, the Cryo-
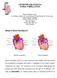
3 Pulmonary Vein İsolation with the Cryoballoon: Simpler, Faster But Equally Effective? 63 balloon (Arctic Front, Medtronic, USA) using cryothermal energy ablation, is certainly the one that has awoken the most interest in the Electrophysiologist Community (5). Not only does it reliably achieve the ultimate goal of PV isolation but, by the fact of using cryothermal energy, the procedure might be safer due to less thrombogenic lesions and potentially associated with a lower risk of PV stenosis than RF energy (6,7,8). Due to its relatively uncomplicated procedure, an increasing number of electrophysiology laboratories might choose the cryoballoon as the standard tool ablation for PV isolation in the near future. The Cryothermal Balloon Device This tool (Fig 1) represents a very appealing system to perform PV isolation being able to produce electrical isolation with virtually one single application. Mainly designed to approach drug resistant paroxysmal AF, the cryoballoon therapy apparatus include the Arctic Front doubled-walled cryoballoon catheter, which inflates and fills with coolant (N 2 O) to ablate between the pulmonary veins and the left atrium; the FlexCath Steerable Sheath, which helps deliver and position the cryocatheter in the left atrium (LA) and the CryoConsole, which houses the coolant, electrical and mechanical components that run the catheter during a cryotherapy procedure. The refrigerant N 2 O is delivered into the balloon where it undergoes a liquid-togas phase change, resulting in cooling temperature of approximately -80 C. As other cryothermal tools the endocardial lesion created by the cryoballoon occurs in three main phases. The first phase is characterized by the immediate effect of freezing on the cardiac tissue by the formation of ice crystals in both the extracellular and intracellular space. When reaching temperatures lower than -20/-25 C ice cristal formation occurs in the extracellular space. Further ablation reaching temperatures lower than -40 C leads to cellular damage by the means of intracellular ice cristal formation. This phenomenon provokes destruction of cytoplasmic organels and architectural subversion of the cell membrane. Irreversible cellular death will occur when temperatures reach values lower than -70 C. When cryothermal energy is stopped, a rapid vasodilatation and a state of augmented vascular permeability lead to hemorrage and edema with further tissue injury. During this hyperemic response endothelial damage results in platelet aggregation and microthrombus formation with microcirculation stagnation for roughly 30 to 45 min. The third phase is characterized by scar formation. During the latter, tissue repairment occurs by collagen deposits, fatty infiltrations and neovascularisation. The fibrotic scar will first develop from the peripheric areas of the lesion eventually reaching the centre (9,10). The cryoballoon catheter has a central lumen, which can be used for different scopes such as the insertion of the guide wire, the injection of contrast medium (diluted 1:1 ratio FİGURE 1 The cryoballoon catheter
4 64 Türk Aritmi, Pacemaker ve Elektrofizyoloji Dergisi FİGURE 2 The Achieve inner lumen mapping catheter(black arrow) permits real time recordings of PV potentials when inserted into the veins ostia through the cryoballoon (white arrow) lumen. with 0.9% saline) for PV angiograms and eventually the insertion of a circular mapping catheter to evaluate PV isolation during cryothermal energy application (8). Navigation of the balloon inside the LA is simplified using the overthe-wire technique in addition to the steerable sheath (12 F, FlexCath, Medtronic Cryocath TM, USA). In addition, the cryoballoon itself is steerable thanks to a pull wire mechanism integrated in the handle of the catheter itself. catheter (Achieve, Medtronic, USA) is positioned in the PV ostium to gather real time recordings (Fig 2). The balloon is then inflated and advanced over the circular mapping catheter in the PV ostium of each vein. Optimal vessel occlusion is considered to have been achieved when selective contrast injection shows total contrast retention with no flow to the atrium. If occlusion is not possible using the circular mapping catheter, the latter can be exchanged with a guide wire that might offer better stability. For each vein, cryoablation usually consists of a minimum of 2 applications lasting 5 minutes each. Whenever possible, the operator tries to engage with the guide-wire 2 different branches of the same vein and to orient the balloon differently, in the attempt of covering a wider ostial surface. However, if successful occlusion could only be obtained in one branch, both applications are delivered by leaving the guide-wire in the same branch. Usually, the left superior PV (LSPV) (Fig 3) is The Procedure Usually a single transseptal puncture is then performed using the right femoral venous approach. In some centers, a double transseptal puncture is achieved in order to have simultaneous electrical information during the freezing phase. After gaining the LA access, a 70 IU/Kg heparin iv bolus is given and afterwards repeated to maintain the activated clotting time over 300 s. Selective PV angiograms are then performed. Immediately after, a steerable 15 F over-the-wire sheath (FlexCath, Cryocath, Medtronic, USA) is positioned in the LA. Through the latter, a 23 or 28 mm double walled cryoballoon (Arctic Front, Medtronic, USA) is up to the LA. An inner lumen circular mapping FİGURE 3 Successful occlusion of the LSPV with the cryoballoon demonstrated by total retention of contrast inside the vein.
5 Pulmonary Vein İsolation with the Cryoballoon: Simpler, Faster But Equally Effective? 65 treated first, followed by the left inferior PV (LIPV), right superior PV (RSPV) and right inferior PV (RIPV). During ablation, the circular mapping catheter offers real time information of the electrical activity in the vein. Usually, PV isolation can be observed real-time during energy delivery. In order to avoid phrenic nerve palsy, a complication observed during cryoballoon ablation in the RSPV and RIPV, a bipolar catheter is inserted in the superior vena cava in order to pace phrenic nerve with a 1000 ms cycle and a 20 ma pulse output. Diaphragmatic contraction during pacing will indicate correct phrenic capture. If this contraction suddenly stops or weakens, the cryoablation should be immediately interrupted. The reason of pacing at such a slow rate is to prevent catheter displacement in the early phases of application due to diaphragmatic contraction. In case of persistence of PV potentials extra cryoballoon applications were performed until complete PV isolation. In case of failure of the cryoballoon, a focal RF or cryothermal energy catheter is used to complete PV isolation. In clinical practice isolating the inferior PVs can be particularly challenging in comparison to the superior ones (11). Specifically, occluding and isolating the RIPV is often quite tricky due to the proximity of this vein to the site of transatrial access and its posterior orientation, especially in patients with relatively small LA (LA diameter < 35 mm). Various ablation techniques aiming at overcoming these anatomical obstacles have been reported : the hockey stick technique, the pull-down technique. The hockey stick technique is applied in patients with an early branching inferior PV and consists of a maximal bending of the sheath towards the superior-posterior LA, allowing the cryoballoon to be pushed and to adhere to inferior part of the PV ostium. The RIPV can be addressed using the pull-down technique. This procedure consists in starting the freeze at the ostium of the PV, regardless of the incomplete occlusion and when the latter adheres to the interpulmonary carina (typically at -20 C) to pull down all the cryoballoon apparatus, in order to close the inferior gap. Pulmonary Vein İsolation: Acute Results According to recent publications about PV isolation can be demonstrated in more than 90% of veins following cryoballoon ablation. Successful PV isolation with the cryoballoon is highly dependent on a perfect contact to the atrial wall at the level of the PV ostia Indeed, lack of blood back-flow allows the cryoballoon to obtain lower temperatures with the result of achieving more deeper lesions (12). Anatomical difficulties seem to represents the main obstacle to complete PV isolation when using the cryoballoon; Van Belle et al. reported that oval shaped PV ostia or veins inserting into the LA with a sharp angulation are the most difficult to occlude (12). However like in all other techniques, the learning curve and the level of the operator s experience will condition the efficacy of cryoballoon ablation. Our group analyzed the degree of adenosine induced LA-PV isolation following cryoballoon ablation (13). Adenosine is known to induce transient reconduction in isolated PVs, due to incomplete lesions after RF ablation (14,15). In our series of patients, transient PV-LA reconnection occurred only in 4,6% PVs compared to a mean 30% of veins following PV isolation with RF. A possible explanation of this discrepancy is that a balloon strategy might lead to more continuous lesions than point by point circumferential PV isolation.
6 66 Türk Aritmi, Pacemaker ve Elektrofizyoloji Dergisi Pulmonary Vein İsolation: Chronic Results Fürnkranz and colleagues (16) analyzed the sites of PV reconnection in 26 patients undergoing repeat ablation for recurrent symptomatic AF or atrial tachycardia after initial cryoballoon ablation for paroxysmal AF. They found a high rate of PV reconnection (around 50%) at a median follow-up of about 6 months. Reconnection mostly occurred in the inferior segments of the inferior PVs and on the LA appendix -LSPV ridge. They postulated, in accordance to the previous findings described by others (12) that a straighter alignment of the balloon with the superior PVs as compared with the inferior ones provides more contact force on the LA wall and lower temperatures. Accordingly to these findings, Ahmed and coworkers evidenced at 8-12 weeks months follow up that 88% of PVs previously ablated with the cryoablation therapy were still isolated and that reconnections occurred mainly in the LIPV and in the inferior aspects of each vein (17). Both groups of authors underlined the importance of full PV occlusion during cryoablation. Follow-Up Unfortunately, data on follow-up of patients having undergone AF ablation is extremely heterogeneous and varies immensely from center to center. The success rates following AF ablation on the long-term should thus be interpreted with extreme caution. However, data available in the literature reports promising results. Klein et al (18) first reported the success rate of cryoballoon ablation at 6 months. In their study up to 86% of patients were AF free on a short term follow-up. Neumann et al, rounding up the biggest series up to now, obtained at 1 year a success rate of 74% (5). Kühne et al.(19) reported a success rate of 71% at 1 year follow up too. Linhart and colleagues, which compared cryoballoon ablation to RF in a small series of patients (20), found a deceiving success rate of about 50% at 1 year of follow-up. However as the authors explained this finding with the fact that the blanking period in their study was of only 4 weeks. Additionally, many AF recurrences following the cryoballoon ablation occurred immediately after the procedure and decreasingly lowered in the following observational period. Adverse Events Phrenic Nerve Palsy (PNP) Cryoablation is historically known as a safe ablative energy source. However, it is also the procedure known to be mostly associated with PNP among all the PV isolation techniques. Although mostly associated with the 23 mm balloon, PNP has been demonstrated during ablation with the bigger balloon as well. Luckily, it is in nearly all cases a transient phenomenon that reverts spontaneously. According to the recently presented STOP AF data at the American College of Cardiology 2010, this complication occurred in 11% of the 228 patients studied (21). Fortunately in 98,2% of patients the complication spontaneously resolved. A recent publication, (20) comparing cryoballoon technology with RF ablation in a group of patients affected by paroxysmal AF, right PNP occurred in about 11% of patients undergoing cryoballoon ablation and all these cases resolved spontaneously. Interestingly, all of them were associated with the use of a 23 mm cryoballoon. This could be explained by the fact that the smaller cryoballoon might achieve a more distal lesion occurring closer to the phrenic nerve s anatomical course.
7 Pulmonary Vein İsolation with the Cryoballoon: Simpler, Faster But Equally Effective? 67 PV Stenosis Only the data presented on the STOP AF (21) reported PV stenosis as a possible collateral effect of cryoballoon ablation. In fact, the rate of PV stenosis was 3.1% versus a complete absence of this complication in the already published reports. This difference might be explained by the fact that in the STOP AF trial the PV stenosis was intensively investigated during the follow-up and that the definition of PV stenosis was quite strict. Esophageal Lesions More interestingly, atrio-esophageal fistula has never been described among procedural complications of cryoballoon ablation. Esophageal lesions following cryoballoon ablation is another matter of debate. In fact, whereas Fürnkranz et al.(22) demonstrated that PV isolation with the cryoballoon was not associated with thermal esophageal lesions in any of 38 studied patients, Ahmed et al.(23) on the contrary showed appearance of transient esophageal ulcerations in 17% of the patients following this procedure. Interestingly, a correlation with temperature changes inside the esophageal lumen was found by the authors. Pericardial Effusion Pericardial effusion is another potentially life threatening complication observed associated to AF ablation. Our group (24) compared the incidence and clinical outcome of pericardial effusion following cryoballoon ablation and RF ablation. A total of 133 consecutive patients with paroxysmal AF were included in this study. Pericardial effusion was detected in 14.2% of the 133 patients. Sixteen patients presented mild effusion, one moderate effusion, and 2 pericardial tamponades(related to transseptal puncture). Interestingly, there was no significant difference in the incidence of pericardial effusion between the cryoballoon and the RF group (11 vs. 16%). Fortunately, pericardial effusion was mostly mild and asymptomatic, with benign clinical outcome not requiring additional hospitalization days. Cerebral Embolisation Cryoablation is known to be associated to less thrombus formation. However the recent MEDAFI study (25), not only reported a 14% of new cerebral lesions following ablation but, more importantly showed no significant difference in this event between patients undergoing ablation with RF or Cryoballoon. Luckily, all these neurological lesions proved to be asymptomatic. However, it does proove that the anticoagulation strategy when working in the LA with any tool is of utmost importance. Conclusion Cryoballoon ablation is a very promising technique to treat AF. However, the cryoballoons currently available do not always adapt themselves well to the anatomical variants and do not systematically isolate the PVs in one application. Ideally, a more compliant balloon which would fit into most PVs might lead to a more effective procedure. Future technological improvements will certainly overcome some of the abovementioned issues and might lead a larger number of electrophysiologists to adopt such a technique. The future randomized trials such as the ongoing Freeze AF trial (26) will certainly provide valuable answers to the most important issue: can cryoballoon reach the goal of becoming the gold standard for PV isolation? For the moment, this role is still played by point by point RF circumferential PV isolati-
8 68 Türk Aritmi, Pacemaker ve Elektrofizyoloji Dergisi on in most Electrohysiology Laboratories. Conflicts of interests: Dr GB Chierchia has received compensation as a proctor for AF Solutions Medtronic. REFERENCES 1. Natale A, Raviele A, Arentz T, et al. Venice Chart international consensus document on atrial fibrillation ablation. J Cardiovasc Electrophysiol 2007;18: Haissaguerre M, Jaı s P, Shah DC, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med 1998;339: Ouyang F, Bansch D, Ernst S, et al. Complete isolation of left atrium surrounding the pulmonary veins: new insights from the double-lasso technique in paroxysmal atrial fibrillation. Circulation 2004;110: Cappato R, Calkins H, Chen SA, et al. Updated worldwide survey on the methods, efficacy, and safety of catheter ablation for human atrial fibrillation. Circ Arrhythm Electrophysiol. 2010;3: Neumann T, Vogt J, Schumacher B, et al. Circumferential pulmonary vein isolation with the cryoballoon technique results from a prospective 3-center study. J Am Coll Cardiol ;52: Khairy P, Chauvet P, Lehmann J, et al. Lower incidence of thrombus formation with cryoenergy versus radiofrequency catheter ablation. Circulation 2003;107: Tse HF, Reek S, Timmermans C, et al. Pulmonary vein isolation using transvenous catheter cryoablation for treatment of atrial fibrillation without risk of pulmonary vein stenosis. J Am Coll Cardiol 2003;42: Chun KR, Fürnkranz A, Metzner A, et al. Cryoballoon pulmonary vein isolation with realtime recordings from the pulmonary veinsj Cardiovasc Electrophysiol. 2009;20: Atienza F, Almendral J, Sanchez-Quintana D, et al. Cryoablation time-dependent dose-response effect at minimal temperatures(_8à degrees C): an experimental study. Europce.2009;11: Dubuc M, Roy D, Thibault B, Ducharme A, et al. Transvenous catheter ice mapping and cryoablationof the atrioventricular node in dogs. Pacing Clin Electrophysiol.1999;22: Chun KR, Schmidt B, Metzner A, et al. The single big cryoballoon technique for acute pulmonary vein isolation in patients with paroxysmal atrial fibrillation: a prospective observational single centre study. Eur Heart J. 2009;30: Van Belle Y, Janse P, Rivero-Ayerza MJ, et al. Pulmonary vein isolation using an occluding cryoballoon for circumferential ablation: feasibility, complications, and short-term outcome. Eur Heart J. 2007;28: Chierchia GB, Yazaki Y, Sorgente A, et al. Transient atriovenous reconnection induced by adenosine after successful pulmonary vein isolation with the cryothermal energy balloon. Europace. 2009;11: Arentz T, Macle L, Kalusche D, et al. Dormant pulmonary vein conduction revealed by adenosine after ostial radiofrequency catheter ablation. J Cardiovasc Electrophysiol 2004;15: Tritto M, De Ponti R, Salerno-Uriarte JA, et al. Adenosine restores atrio-venous conduction after apparently successful ostial isolation of the pulmonary veins. Eur Heart J 2004;25: Fürnkranz A, Chun KR, Nuyens D, et al. Characterization of conduction recovery after pulmonary vein isolation using the single big cryoballoon technique. Heart Rhythm. 2010;7: Ahmed H, Neuzil P, Skoda J, et al.the Permanency of Pulmonary Vein Isolation Using a Balloon Cryoablation Catheter. J Cardiovasc Electrophysiol in press. 18. Klein G, Oswald H, Gardiwal A, et al. Efficacy of pulmonary vein isolation by cryoballoon ablation in patients with paroxysmal atrial fibrillation. Heart Rhythm. 2008;5: Kühne M, Schaer B, Ammann P, Suter Y, Osswald S, Sticherling C. Cryoballoon ablation for pulmonary vein isolation in patients with paroxysmal atrial fibrillation. Swiss Med Wkly. 2010;140: Linhart M, Bellmann B, Mittmann-Braun E, et al. Comparison of cryoballoon and radiofrequency ablation of pulmonary veins in 40 patients with paroxysmal atrial fibrillation: a case-control study. J Cardiovasc Electrophysiol. 2009;20: Packer D. Abstract presented at ACC Fürnkranz A, Chun KR, Metzner A, et al. Esophageal endoscopy results after pulmonary vein isolation using a single big cryoballoon technique. J Cardiovasc Electrophysiol. 2010;21: Ahmed H, Neuzil P, d Avila A, et al. The esophageal effects of cryoenergy during cryoablation for atrial fibrillation. Heart Rhythm 2009;6: Chierchia GB, Capulzini L, Droogmans S, et al. Pericardial effusion in atrial fibrillation ablation: a comparison between cryoballoon and radiofrequency pulmonary vein isolation. Europace. 2010;12: Neumann T, Kuniss M, Conradi G, et al. MEDAFI-Trial (Micro-embolization during ablation of atrial fibrillation): comparison of pulmonary vein isolation using cryoballoon technique vs. radiofrequency energy. Europace. 2011;13: Luik A, Merkel M, Hoeren D, Riexinger T, Kieser M, Schmitt C. Rationale and design of the FreezeAF trial: a randomized controlled noninferiority trial comparing isolation of the pulmonary veins with the cryoballoon catheter versus open irrigated radiofrequency ablation in patients with paroxysmal atrial fibrillation. Am Heart J 2010;159:
Ablation For Atrial Fibrillation. Bill Petrellis Electrophysiologist
 Ablation For Atrial Fibrillation Bill Petrellis Electrophysiologist AF is the most common arrhythmia in the Western world Prevalence 1.1% in Australia conservative estimate - 240,000 June 2009 AF is an
Ablation For Atrial Fibrillation Bill Petrellis Electrophysiologist AF is the most common arrhythmia in the Western world Prevalence 1.1% in Australia conservative estimate - 240,000 June 2009 AF is an
DIU de rythmologie et stimulation cardiaque. Orateur : Serge BOVEDA Le 25 janvier 2012
 DIU de rythmologie et stimulation cardiaque Titre : Fibrillation atriale paroxystique : ablation, résultats, complications Orateur : Serge BOVEDA Le 25 janvier 2012 Fibrillation Atriale Paroxystique :
DIU de rythmologie et stimulation cardiaque Titre : Fibrillation atriale paroxystique : ablation, résultats, complications Orateur : Serge BOVEDA Le 25 janvier 2012 Fibrillation Atriale Paroxystique :
DISCLOSURE. Atrial Fibrillation Management An Evidence-based Approach OBJECTIVES BACKGROUND AFFIRM 9/16/2015
 Death (%) Mortality (%) 9/16/2015 DISCLOSURE Atrial Fibrillation Management An Evidence-based Approach Jonathon Adams, MD, FHRS Relevant Financial Relationship(s) None Off Label Usage None OBJECTIVES What
Death (%) Mortality (%) 9/16/2015 DISCLOSURE Atrial Fibrillation Management An Evidence-based Approach Jonathon Adams, MD, FHRS Relevant Financial Relationship(s) None Off Label Usage None OBJECTIVES What
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
 The Decision Tree for Ablation Therapy in Atrial Fibrillation Colin Movsowitz, MD, FACC Cardiology Consultants of Philadelphia Director of Electrophysiology Einstein Medical Center Montgomery Co-Director
The Decision Tree for Ablation Therapy in Atrial Fibrillation Colin Movsowitz, MD, FACC Cardiology Consultants of Philadelphia Director of Electrophysiology Einstein Medical Center Montgomery Co-Director
Combined Epicardial and Endocardial Ablation for Treatment of Atrial Fibrillation. Ashkan Babaie MD Providence Portland Medical Center
 Combined Epicardial and Endocardial Ablation for Treatment of Atrial Fibrillation Ashkan Babaie MD Providence Portland Medical Center 1 Disclosures None 2 Cox-Maze III The Godfather Cure rates > 95% in
Combined Epicardial and Endocardial Ablation for Treatment of Atrial Fibrillation Ashkan Babaie MD Providence Portland Medical Center 1 Disclosures None 2 Cox-Maze III The Godfather Cure rates > 95% in
Management of Symptomatic Atrial Fibrillation
 Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
Management of Symptomatic Atrial Fibrillation John F. MacGregor, MD, FHRS Associate Medical Director, Cardiac Electrophysiology PeaceHealth St. Joseph Medical Center, Bellingham, WA September 18, 2015
Corporate Medical Policy
 Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
CATHETER ABLATION for ATRIAL FIBRILLATION
 CATHETER ABLATION for ATRIAL FIBRILLATION Atrial Fibrillation Clinic Dr. Richard Leather, Dr. Larry Sterns, Dr Paul Novak, Dr. Chris Lane Royal Jubilee Hospital Block 3 rd floor, Rm 343 1952 Bay Street
CATHETER ABLATION for ATRIAL FIBRILLATION Atrial Fibrillation Clinic Dr. Richard Leather, Dr. Larry Sterns, Dr Paul Novak, Dr. Chris Lane Royal Jubilee Hospital Block 3 rd floor, Rm 343 1952 Bay Street
Techniques of Mapping and Isolation of the Pulmonary Veins in Patients with Atrial Fibrillation
 Aus dem Deutschen Herzzentrum Berlin Klinik für Innere Medizin/Kardiologie DISSERTATION Techniques of Mapping and Isolation of the Pulmonary Veins in Patients with Atrial Fibrillation zur Erlangung des
Aus dem Deutschen Herzzentrum Berlin Klinik für Innere Medizin/Kardiologie DISSERTATION Techniques of Mapping and Isolation of the Pulmonary Veins in Patients with Atrial Fibrillation zur Erlangung des
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Current ablation techniques for persistent atrial fibrillation: results of the European Heart Rhythm Association Survey
 Europace (215) 17, 1596 16 doi:1.19/europace/euv2 EP WIRE Current techniques for persistent atrial fibrillation: results of the European Heart Rhythm Association Survey Nikolaos Dagres 1 *, Maria Grazia
Europace (215) 17, 1596 16 doi:1.19/europace/euv2 EP WIRE Current techniques for persistent atrial fibrillation: results of the European Heart Rhythm Association Survey Nikolaos Dagres 1 *, Maria Grazia
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Catheter Ablation as Treatment Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Catheter Ablation as Treatment Professional Institutional Original Effective
Catheter Ablation as Treatment Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Catheter Ablation as Treatment Professional Institutional Original Effective
Catheter Ablation of Arrhythmogenic Foci as Treatment for Atrial Fibrillation
 Catheter Ablation of Arrhythmogenic Foci as Treatment for Atrial Fibrillation Policy Number: Original Effective Date: MM.06.011 09/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Catheter Ablation of Arrhythmogenic Foci as Treatment for Atrial Fibrillation Policy Number: Original Effective Date: MM.06.011 09/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
How do you decide on rate versus rhythm control?
 Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Heart Rhythm Congress 2014 How do you decide on rate versus rhythm control? Dr Ed Duncan Consultant Cardiologist & Electrophysiologist Define Rhythm Control DC Cardioversion Pharmacological AFFIRM study
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Name of Policy: Transcatheter Ablation of Arrhythmogenic Foci as a Treatment of Atrial Fibrillation
 Name of Policy: Transcatheter Ablation of Arrhythmogenic Foci as a Treatment of Atrial Fibrillation Policy #: 283 Latest Review Date: June 2015 Category: Medical Policy Grade: A Background/Definitions:
Name of Policy: Transcatheter Ablation of Arrhythmogenic Foci as a Treatment of Atrial Fibrillation Policy #: 283 Latest Review Date: June 2015 Category: Medical Policy Grade: A Background/Definitions:
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy
 How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
How to control atrial fibrillation in 2013 The ideal patient for a rate control strategy L. Pison, MD Advances in Cardiac Arrhythmias and Great Innovations in Cardiology - Torino, September 28 th 2013
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): January 27, 2015 Effective Date: April 1, 2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): January 27, 2015 Effective Date: April 1, 2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Rome, Italy December 4-7, 2012 Rome Cavalieri TIMETABLE
 Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Rome, Italy December 4-7, 2012 Rome Cavalieri Monday, December 3 ROOM Terrazza Monte Mario PATIENT MANAGEMENT CONCEPTS AND CONTROVERSIES IN ELECTROPHYSIOLOGY BIOTRONIK International Fellows Program (IFP)
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI
 Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation and Cardiac Device Therapy RAKESH LATCHAMSETTY, MD DIVISION OF ELECTROPHYSIOLOGY UNIVERSITY OF MICHIGAN HOSPITAL ANN ARBOR, MI Outline Atrial Fibrillation What is it? What are the associated
Atrial Fibrillation Catheter Ablation versus Surgical Ablation Treatment: FAST A Two-Center Randomized Clinical Trial
 Atrial Fibrillation Catheter Ablation versus Surgical Ablation Treatment: FAST A Two-Center Randomized Clinical Trial Lucas Boersma, WimJan van Boven, Alaaddin Yilmaz, Johannes Kelder, Maurits Wijffels
Atrial Fibrillation Catheter Ablation versus Surgical Ablation Treatment: FAST A Two-Center Randomized Clinical Trial Lucas Boersma, WimJan van Boven, Alaaddin Yilmaz, Johannes Kelder, Maurits Wijffels
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY. Charles Jazra
 RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
RATE VERSUS RHYTHM CONTROL OF ATRIAL FIBRILLATION: SPECIAL CONSIDERATION IN ELDERLY Charles Jazra NO CONFLICT OF INTEREST TO DECLARE Relationship Between Atrial Fibrillation and Age Prevalence, percent
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Atrial Fibrillation and Ablation Therapy: A Patient s Guide
 Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
How should we treat atrial fibrillation in heart failure
 Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Advances in Cardiac Arrhhythmias and Great Innovations in Cardiology Torino, 23/24 Ottobre 2015 How should we treat atrial fibrillation in heart failure Matteo Anselmino Dipartimento Scienze Mediche Città
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Atrial Fibrillation (AF) Explained
 James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
Atrial fibrillation How is treatment changing? Charles Henrikson, MD Director, Electrophysiology Service 1 February 2014
 Atrial fibrillation How is treatment changing? Charles Henrikson, MD Director, Electrophysiology Service 1 February 2014 Outline Introduction Natural history of afib and stroke Current risk stratification
Atrial fibrillation How is treatment changing? Charles Henrikson, MD Director, Electrophysiology Service 1 February 2014 Outline Introduction Natural history of afib and stroke Current risk stratification
Surgeons Role in Atrial Fibrillation
 Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Atrial Fibrillation Surgeons Role in Atrial Fibrillation Steven J Feldhaus, MD, FACS 2015 Cardiac Symposium September 18, 2015 Stages of Atrial Fibrillation Paroxysmal (Intermittent) Persistent (Continuous)
Radiofrequency Ablation for Atrial Fibrillation. A Guide for Adults
 Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Advances in the Treatment of Atrial Fibrillation At VCU Medical Center
 Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
Contact Us For additional information or to schedule an appointment with one of our specialists, please call: Ken Ellenbogen, M.D. Cardiology/Electrophysiology 804-828-7565 or 804-628-0147 You can also
III. Cell destruction by freezing and cryoprobe development
 III. Cell destruction by freezing and cryoprobe development 1 WHAT IS CRYOSURGERY? Cryoprobe Surface iceball formation Ice-ball Cryoprobe Cryosurgery of liver (Angular insertion) Cryosurgery of liver (Vertical
III. Cell destruction by freezing and cryoprobe development 1 WHAT IS CRYOSURGERY? Cryoprobe Surface iceball formation Ice-ball Cryoprobe Cryosurgery of liver (Angular insertion) Cryosurgery of liver (Vertical
SECTION I: Request. SECTION II: Need. Program Description
 SECTION I: Request This is a formal request for the Utah CARMA Center to be formally recognized by the University of Utah as a large, collaborative medical and academic center whose focus is on comprehensive
SECTION I: Request This is a formal request for the Utah CARMA Center to be formally recognized by the University of Utah as a large, collaborative medical and academic center whose focus is on comprehensive
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect. Robert Kennedy, MD October 10, 2015
 Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION. Department of Arrhythmology, Villa Maria Cecilia Hospital, Cotignola, Ravenna, ITALY
 COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION Carlo PAPPONE, MD, PhD, FACC Vincenzo SANTINELLI, MD Department of Arrhythmology, Villa Maria Cecilia Hospital, Cotignola, Ravenna, ITALY Address for correspondence
COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION Carlo PAPPONE, MD, PhD, FACC Vincenzo SANTINELLI, MD Department of Arrhythmology, Villa Maria Cecilia Hospital, Cotignola, Ravenna, ITALY Address for correspondence
Hot Line Session at European Society of Cardiology (ESC) Congress 2014:
 Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Hot Line Session at European Society of Cardiology (ESC) Congress 2014: Once-Daily
Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Hot Line Session at European Society of Cardiology (ESC) Congress 2014: Once-Daily
A Patient Guide to Atrial Fibrillation and Catheter Ablation
 A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
A Patient Guide to Atrial Fibrillation and Catheter Ablation Al-Sabah Arrhythmia Institute 1111 Amsterdam Avenue New York, NY 10025 Phone: 212-523-2400 Fax: 212-523-2571 www.stlukescardiology.org Printed
How do you decide on rate versus rhythm control?
 How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
How do you decide on rate versus rhythm control? Dr. Mark O Neill Consultant Cardiologist & Electrophysiologist Assumptions Camm et al. EHJ 2010;Sept 25 epub Choice of strategy: Criteria for consideration
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
Cryoballoon or Radiofrequency Ablation for Paroxysmal Atrial Fibrillation
 Original Article or Radiofrequency Ablation for Paroxysmal Atrial Fibrillation Karl-Heinz Kuck, M.D., Josep Brugada, M.D., Alexander Fürnkranz, M.D., Andreas Metzner, M.D., Feifan Ouyang, M.D., K.R. Julian
Original Article or Radiofrequency Ablation for Paroxysmal Atrial Fibrillation Karl-Heinz Kuck, M.D., Josep Brugada, M.D., Alexander Fürnkranz, M.D., Andreas Metzner, M.D., Feifan Ouyang, M.D., K.R. Julian
Vorhofflimmern und Schlaganfall Ablation, Antikoagulation, Vorhofohrverschluß was wann für wen? B. Keweloh Unfallkrankenhaus Berlin
 Vorhofflimmern und Schlaganfall Ablation, Antikoagulation, Vorhofohrverschluß was wann für wen? B. Keweloh Unfallkrankenhaus Berlin B. Keweloh 16.11.2013 Incidence of Atrial Fibrillation, Standard population
Vorhofflimmern und Schlaganfall Ablation, Antikoagulation, Vorhofohrverschluß was wann für wen? B. Keweloh Unfallkrankenhaus Berlin B. Keweloh 16.11.2013 Incidence of Atrial Fibrillation, Standard population
Ostial LAD: Single stent approach is the best. Antonio A. Pocoví, MD, FSCAI, MTSAC, Advisory Council Member, CACI
 Ostial LAD: Single stent approach is the best Antonio A. Pocoví, MD, FSCAI, MTSAC, Advisory Council Member, CACI Chair, Interventional Cardiology Sanatorio San Lucas Instituto Alexander Fleming Buenos
Ostial LAD: Single stent approach is the best Antonio A. Pocoví, MD, FSCAI, MTSAC, Advisory Council Member, CACI Chair, Interventional Cardiology Sanatorio San Lucas Instituto Alexander Fleming Buenos
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Protocol. Catheter Ablation as Treatment for Atrial Fibrillation
 Protocol Catheter Ablation as Treatment for Atrial Fibrillation (20219) (Formerly Catheter Ablation of the Pulmonary Veins as Treatment for Atrial Fibrillation) Medical Benefit Effective Date: 10/01/15
Protocol Catheter Ablation as Treatment for Atrial Fibrillation (20219) (Formerly Catheter Ablation of the Pulmonary Veins as Treatment for Atrial Fibrillation) Medical Benefit Effective Date: 10/01/15
Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects
 Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects Halon Alternatives Technical Working Conference 1993 Reva Rubenstein, Ph.D. U.S.Environmenta1 Protection Agency
Short Duration High-Level Exposure to Halon Substitutes: Potential Cardiovascular Effects Halon Alternatives Technical Working Conference 1993 Reva Rubenstein, Ph.D. U.S.Environmenta1 Protection Agency
Radiofrequency ablation of atrial tachycardia from no man s land
 CASE REPORT 103 A case of atrial tachycardia originating between the His region and the non-coronary cusp Radiofrequency ablation of atrial tachycardia from no man s land Nikola Pavlović a,b, Sven Knecht
CASE REPORT 103 A case of atrial tachycardia originating between the His region and the non-coronary cusp Radiofrequency ablation of atrial tachycardia from no man s land Nikola Pavlović a,b, Sven Knecht
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Tunneled Hemodialysis Catheters: Placement and complications
 Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
1547-5271/$ -see front matter 2007 by the Heart Rhythm Society and the European Heart Rhythm Association,
 HRS/EHRA/ECAS Expert Consensus Statement on Catheter and Surgical Ablation of Atrial Fibrillation: Recommendations for Personnel, Policy, Procedures and Follow-Up A report of the Heart Rhythm Society (HRS)
HRS/EHRA/ECAS Expert Consensus Statement on Catheter and Surgical Ablation of Atrial Fibrillation: Recommendations for Personnel, Policy, Procedures and Follow-Up A report of the Heart Rhythm Society (HRS)
Contact force technology in catheter ablation of atrial fibrillation
 Contact force technology in catheter ablation of atrial fibrillation Anna Wysocka 1, Maciej Wójcik 2 1 Chair of Internal Medicine and Department of Internal Medicine in Nursing, Medical University, Lublin,
Contact force technology in catheter ablation of atrial fibrillation Anna Wysocka 1, Maciej Wójcik 2 1 Chair of Internal Medicine and Department of Internal Medicine in Nursing, Medical University, Lublin,
PRACTICAL APPROACH TO SVT. Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia
 PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
brussels Postgraduate in Cardiac Electrophysiology and Pacing
 brussels Postgraduate in Cardiac Electrophysiology and Pacing the Postgraduate Course This Postgraduate in Cardiac Electrophysiology and Pacing - is offered within the Faculty of Medicine and Pharmacy
brussels Postgraduate in Cardiac Electrophysiology and Pacing the Postgraduate Course This Postgraduate in Cardiac Electrophysiology and Pacing - is offered within the Faculty of Medicine and Pharmacy
SUBMISSION ACCC Report to the Senate on Private Health Insurance
 SUBMISSION ACCC Report to the Senate on Private Health Insurance Medtronic Australasia welcomes the opportunity to contribute to the preparation of the Australian Competition and Consumer Commission (ACCC)
SUBMISSION ACCC Report to the Senate on Private Health Insurance Medtronic Australasia welcomes the opportunity to contribute to the preparation of the Australian Competition and Consumer Commission (ACCC)
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them?
 2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them? Gaetano Senatore DIVISION OF CARDIOLOGY HOSPITAL OF CIRIE
2014: nowadays the one shot technologies and the injectable monitor allow a wide and complete AF patient management. Why shouldn t we use them? Gaetano Senatore DIVISION OF CARDIOLOGY HOSPITAL OF CIRIE
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015
 Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
Point of view: Thromboembolic risks associated with catheter ablation for atrial fibrillation
 Point of view: Thromboembolic risks associated with catheter ablation for atrial fibrillation Shah, Dipen 1. What is the background of thromboembolic complications in the setting of catheter ablation of
Point of view: Thromboembolic risks associated with catheter ablation for atrial fibrillation Shah, Dipen 1. What is the background of thromboembolic complications in the setting of catheter ablation of
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE?
 TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
Cilostazol versus Clopidogrel after Coronary Stenting
 Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014
 Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014 Atrial Fibrillation 2 Atrial Fibrillation The most common arrhythmia encountered
Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014 Atrial Fibrillation 2 Atrial Fibrillation The most common arrhythmia encountered
Listen to Your Heart. What Everyone Needs To Know About Atrial Fibrillation & Stroke. The S-ICD System. The protection you need
 Listen to Your Heart The S-ICD System What Everyone Needs To Know About Atrial Fibrillation & Stroke The protection you need without Stroke. touching Are you your at heart risk? Increase your knowledge.
Listen to Your Heart The S-ICD System What Everyone Needs To Know About Atrial Fibrillation & Stroke The protection you need without Stroke. touching Are you your at heart risk? Increase your knowledge.
PATIENT INFORMATION BOOKLET
 PATIENT INFORMATION BOOKLET Wingspan Stent System with Gateway PTA Balloon Catheter TABLE OF CONTENTS Definitions... 2 What is the Purpose of This Booklet?... 3 What is an Intracranial Lesion?... 3 Who
PATIENT INFORMATION BOOKLET Wingspan Stent System with Gateway PTA Balloon Catheter TABLE OF CONTENTS Definitions... 2 What is the Purpose of This Booklet?... 3 What is an Intracranial Lesion?... 3 Who
Your Atrial Fibrillation Catheter Ablation
 UW MEDICINE PATIENT EDUCATION Your Atrial Fibrillation Catheter Ablation How to prepare and what to expect This handout explains how to prepare for your catheter ablation to treat atrial fibrillation.
UW MEDICINE PATIENT EDUCATION Your Atrial Fibrillation Catheter Ablation How to prepare and what to expect This handout explains how to prepare for your catheter ablation to treat atrial fibrillation.
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
What Can I Do about Atrial Fibrillation (AF)?
 Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
New in Atrial Fibrillation
 New in Atrial Fibrillation September 2011 Stroke prevention more options Rhythm Control -drugs - alternatives to drugs; ablation Rate Control - pace + ablate A-FIB Dell Stroke Risk AFib Two Principles
New in Atrial Fibrillation September 2011 Stroke prevention more options Rhythm Control -drugs - alternatives to drugs; ablation Rate Control - pace + ablate A-FIB Dell Stroke Risk AFib Two Principles
COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION Is catheter ablation safe?
 Providing information, support and access to established, new or innovative treatments for Atrial Fibrillation COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION Is catheter ablation safe? Registered Charity
Providing information, support and access to established, new or innovative treatments for Atrial Fibrillation COMPLICATIONS OF ATRIAL FIBRILLATION ABLATION Is catheter ablation safe? Registered Charity
Talent Thoracic Stent Graft with THE Xcelerant Delivery System. Expanding the Indications for TEVAR
 Talent Thoracic with THE Xcelerant Delivery System Expanding the Indications for TEVAR Talent Thoracic Precise placement 1 Broad patient applicability 1 Excellent clinical outcomes 1, a + Xcelerant Delivery
Talent Thoracic with THE Xcelerant Delivery System Expanding the Indications for TEVAR Talent Thoracic Precise placement 1 Broad patient applicability 1 Excellent clinical outcomes 1, a + Xcelerant Delivery
Managing the Patient with Atrial Fibrillation
 Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
National Medical Policy
 National Medical Policy Subject: Policy Number: Catheter Ablation for Atrial Fibrillation NMP175 Effective Date*: May 2010 Update: July 2015 This National Medical Policy is subject to the terms in the
National Medical Policy Subject: Policy Number: Catheter Ablation for Atrial Fibrillation NMP175 Effective Date*: May 2010 Update: July 2015 This National Medical Policy is subject to the terms in the
How to manage a patient who needs thrombolysis in acute stroke, ablation or angioplasty/stenting? Janet M McComb Freeman Hospital Newcastle upon Tyne
 How to manage a patient who needs thrombolysis in acute stroke, ablation or angioplasty/stenting? Janet M McComb Freeman Hospital Newcastle upon Tyne What do the guidelines say? What happens with warfarin
How to manage a patient who needs thrombolysis in acute stroke, ablation or angioplasty/stenting? Janet M McComb Freeman Hospital Newcastle upon Tyne What do the guidelines say? What happens with warfarin
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
How To Get A Dose Of Bayer Healthcare'S Oral Anticoagulant, Xarelto
 News Release FOR UK HEALTHCARE MEDIA ONLY Bayer HealthCare Bayer plc Bayer House Strawberry Hill Newbury Berkshire, RG14 1JA www.bayer.co.uk Bayer s Xarelto (rivaroxaban) Recommended by CHMP for EU Approval
News Release FOR UK HEALTHCARE MEDIA ONLY Bayer HealthCare Bayer plc Bayer House Strawberry Hill Newbury Berkshire, RG14 1JA www.bayer.co.uk Bayer s Xarelto (rivaroxaban) Recommended by CHMP for EU Approval
How To Use An Ekosonic Endovascular System
 EkoSonic Endovascular System Nursing Presentation Imagine where we can go. Imagine where we can go. Forward-looking statement This presentation and information communicated verbally to you may contain
EkoSonic Endovascular System Nursing Presentation Imagine where we can go. Imagine where we can go. Forward-looking statement This presentation and information communicated verbally to you may contain
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
2013 Medicare Physician Coding and Reimbursement Changes
 2013 Medicare Physician Coding and Reimbursement Changes Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent of Medtronic s Economic Strategies
2013 Medicare Physician Coding and Reimbursement Changes Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent of Medtronic s Economic Strategies
The largest clinical study of Bayer's Xarelto (rivaroxaban) Wednesday, 14 November 2012 07:38
 Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
Complete Guide for Interventional Radiology
 2013 Complete Guide for Interventional Radiology Contents Introduction... 1 CPT Codes and Descriptions...1 Procedure Codes...2 Chapter 1: The Basics... 5 APC Basics Why Is This Important?...5 CCI Edits
2013 Complete Guide for Interventional Radiology Contents Introduction... 1 CPT Codes and Descriptions...1 Procedure Codes...2 Chapter 1: The Basics... 5 APC Basics Why Is This Important?...5 CCI Edits
