INITIAL MANAGEMENT OF ABDOMINAL INJURY
|
|
|
- Kelly Stafford
- 7 years ago
- Views:
Transcription
1 INITIAL MANAGEMENT OF ABDOMINAL INJURY The intra-abdominal contents may extend anteriorly from the nipples to the groin creases and posteriorly from the tips of the scapulae to the gluteal folds. Consequently, intraabdominal injury frequently co-exists with injuries within the chest and to the pelvis Within West Yorkshire most patients are injured through blunt forces such as motor vehicle collisions, falls and assaults. A much smaller proportion of patients are injured through penetrating mechanisms. The management guidance differs between blunt and penetrating mechanisms of injury so these will be considered separately. Network Referrals Emergency transfers to the Major Trauma Centre should follow the standard pathway. Stabilise, arrange immediate transfer, inform ED consultant at LGI ( or ). When time permits contact relevant specialty / ies. The vascular trauma surgeon is the first point of call for all abdominal trauma advice. Between , the case should be discussed with the on call Consultant Vascular Trauma Surgeon at Leeds General Infirmary (switch board ). From the case should be discussed with the oncall resident Vascular Registrar or Vascular Consultant (switch board ).
2 BLUNT INJURY Clinical assessment The patient will be assessed by the trauma team in line with ATLS principles. Abdominal examination should be included within C as a potential site of bleeding. Patients in shock and suspected to have intra-abdominal injury (including at time of pre-alert) need to be discussed at a very early stage with: o MTC: the on call Vascular Trauma Consultant (switch board ). o TU: the on call General Surgical Consultant o Simultaneously ensure O -ve blood will be available MTC: In all cases of massive transfusion protocol activation ensure the interventional radiologist on-call is alerted. Inspection: abdominal wall bruising e.g. from the seat belt, confirms that the abdomen has been subjected to significant forces and should raise the index of suspicion for injury. New and progressive abdominal distension in a shocked patient clearly suggests exsanguinating intra-abdominal bleeding but a significant volume of intra peritoneal blood can collect without undue distension. Palpation: Tenderness to palpation is often difficult to interpret. It may be the result of intra-abdominal organ injury. However, the tenderness elicited may be from local bony injury e.g. fractured lower ribs and / or pelvic fracture. However, both intra-abdominal and bony injury may be present as these fractures are frequently present in patients who also have intra-abdominal injury. Conversely, patients who do have intraabdominal injury may have little tenderness due to remote but distracting injuries, reduced consciousness (head injury, intoxication, sedating medication, spinal cord injury) or the fact that a haemoperitoneum causes no signs in about 40% of patients. Percussion and auscultation add little to the examination. The presence or absence of bowel sounds has no diagnostic value. As clinical assessment may not be reliable, further imaging is justified in most patients.
3 Investigation Bloods: A FBC, U&E, clotting, venous gas sample and cross-match (with activation of major transfusion protocol if appropriate) should be taken for all significantly injured patients. A pregnancy test should be taken if relevant. Early amylase measurement does little to guide early management. Ultrasound: A FAST scan should be performed in all patients with suspected intraabdominal injury. A FAST scan aims to detect fluid in the peritoneal cavity. It cannot distinguish between blood, ascites or spilt intestinal fluid. However, in the context of trauma this is blood until proven otherwise. It is not designed to look directly for solid organ (liver, spleen, kidney) or hollow viscus injury. A normal scan does not rule out significant intra-abdominal injury and bleeding. A positive scan must be interpreted in the context of the hemodynamic status of the patient and is not in itself an indication for invasive radiological or surgical intervention. It is most useful as a confirmation of the abdomen as a significant source of bleeding in a patient with deteriorating shock. If a decision has been made to proceed to CT, performance of the FAST scan should not delay patient transfer. CT scan: Unless there is rapid hemodynamic deterioration that requires immediate transfer to theatre, all patients where there is concern for significant injury should undergo a CT scan. An arterial phase CT scan has a high sensitivity and specificity for detecting haemoperitoneum and solid organ (liver, spleen, kidney) injury. The presence and site of active bleeding may be identified and so provide a target for embolization treatment. However, this early scan is performed before the inflammatory effects of a viscus perforation have occurred and surprisingly little free gas or fluid may be released. As a result, the initial trauma CT has a much lower diagnostic accuracy for hollow viscus injury. Similarly, fresh pancreatic injury can be difficult to detect on the initial trauma CT.
4 Management (see Figure 1) The guidance below covers expected management at the Major Trauma Centre. At a Trauma Unit management may be limited by the available resources. When the treatment necessary exceeds the TUs capabilities the patient will require transfer to the MTC. Patients with unresponsive or transiently responding shock and considered to have on going intra-abdominal bleeding require rapid transfer to theatre for laparotomy and any other surgery required to control bleeding e.g. pelvic stabilization, thoracotomy etc. Evidence for an intra-abdominal source includes mechanism of injury, progressive abdominal distension and grossly positive FAST scan. Other causes of severe shock need to be considered e.g. bleeding (chest, pelvis, limbs, bleeding from wounds), tension pneumothorax, cardiac tamponade and cardiac contusion or infarction (rare). Patients whose shock is not rapidly deteriorating should have a trauma CT scan. Patients with radiological evidence of ongoing bleeding from solid organs (spleen, kidney, liver) must be discussed with the consultant vascular trauma surgeon and consultant interventional radiologist. These senior decision makers must then decide, based on the patient s hemodynamic status, constellation of injuries and physiological reserve, whether the patient would benefit from minimally invasive embolization after some delay to mobilize personnel compared with proceeding immediately to theatre for more rapid but more invasive surgical hemorrhage control. o Patients with radiological evidence of pseudoaneurysm rather than free, active bleeding from the spleen, liver or kidney must be discussed with the consultant vascular trauma surgeon and Consultant Interventional Radiologist with a view to angio-embolisation. Angio-embolisation of splenic pseudoaneurysms is particularly associated with an increased success of non-operative management. o Patients with solid organ (spleen, liver, kidney) injury but no evidence of ongoing bleeding or pseudoaneurysm must be discussed with the consultant vascular trauma surgeon. A trial of non-operative management can usually be
5 commenced. The patient must be adequately resuscitated to correct hypoperfusion. In a minority of patients with the expected increase in perfusion pressure, bleeding may recur. o During a trial of non-operative treatment regular clinical examinations and hemoglobin measurements must be undertaken. If re-bleeding is suspected (progressive shock and / or falling hemoglobin) transfer to theatre or further CT angiography is required. If confirmed, then angio-embolisation or operative control of bleeding is required. Increasing abdominal pain, tenderness, inflammatory markers or deranged liver function tests may be the result of a missed hollow viscus injury, pancreatic injury or a local complication of solid organ injury e.g. biliary peritonitis. Further CT imaging is indicated to attempt to identify the underlying problem. o Patients with Grade IV or more splenic or hepatic injuries undergoing a trial of non-operative management should be considered for angiography as a proportion will reveal significant vascular injury which if treated should reduce the risk of re-bleeding (see Appendix 1 & 2 for injury grading). o Patients with evidence of hollow viscus injury, mesenteric injury (and so likely ischemic gut) or diaphragmatic injury on the initial trauma CT will almost certainly require laparotomy and should be discussed with the vascular trauma surgeon. o Pancreatic injury occurs in 4% of patients with abdominal injury. It is associated with other intra-abdominal injuries in over 90% of cases & with significant morbidity & mortality because of the close anatomical relation to major vasculature. Damage to the main pancreatic duct occurs in 15%. Identification of such an injury is crucial as it requires reconstruction by an HPB surgeon. Delay in recognition of duct injuries increases morbidity. Serum amylase is not reliable for ruling out significant injury. Early CT will miss pancreatic injuries: there must be a low threshold for re-imaging if there is clinical concern. If there is concern for pancreatic injury then discussion with the Upper GI or pancreatic surgeon on call at SJUH (adults) or Paediatric Surgery (LGI) is mandatory.
6 Figure 1: Management algorithm for blunt abdominal injury Blunt force injury Trauma team ATLS assessment A Yes Unresponsive / transiently responsive shock B No Evaluate for C : Bleeding chest, abdomen, pelvis, limbs & external Tension pneumothorax Cardiac tamponade CT scan Evidence of abdominal bleeding? High energy mechanism / direct force to abdomen / bruising Increasing abdominal distension Positive FAST scan Hollow organ rupture or infarction ACTIVE bleeding or blush e.g. splenic or liver injury D Splenic, liver or kidney injury - NO active bleeding Trial of nonoperative management Laparotomy Percutaneous intervention Embolization Deterioration E (Rebleeding, missed hollow viscus or pancreatic injury, complication of solid organ injury)
7 Figure 1 Key A Abdominal examination should be included within assessment of C as a potential source of bleeding B Senior decision makers (Consultant Vascular Trauma Surgeon (or equivalent in TU) / Consultant in Emergency Medicine/Consultant Interventional radiologist) to assess and decide if patient s hemodynamic status is deteriorating too fast to proceed to CT. C Unresponsive or transiently responsive shock is usually due to bleeding. Potential sites (chest, abdomen, pelvis, limbs and external loss) of bleeding should be evaluated. Obstructive / mechanical causes of shock (tension pneumothorax and cardiac tamponade) should also be considered. Rarer causes of shock include myocardial contusion, neurogenic shock, myocardial infarction and air embolus. Non abdominal sources of shock will need intervention in parallel with intra-abdominal assessment and intervention e.g. chest drain, pelvic binder, wound compression etc. D If bleeding or blush reported on CT scan a discussion between vascular trauma team and radiological team is required to clarify precise nature of abnormality detected. Evidence of bleeding in to peritoneal cavity will almost certainly require intervention. Contained blush within a solid organ may not. If evidence of active bleeding and hemodynamic deterioration requires discussion between Consultant Vascular Trauma Surgeon (or equivalent in TU) and Interventional Radiologist to determine suitability for embolization or laparotomy. Factors to consider include rate of hemodynamic deterioration, constellation of injuries and physiological reserve. E Patients undergoing a trial of non-operative management require regular clinical assessment and hemoglobin measurements ideally initially within a critical care environment. Evidence of hemodynamic deterioration, falling hemoglobin, increasing abdominal pain or tenderness or rising inflammatory markers requires discussion with the Consultant Vascular Trauma Surgeon. Depending on the rate of deterioration and clinical suspicion, the patient should undergo CT imaging or more rarely emergency transfer to theatre. The CT scan may reveal re-bleeding, missed hollow viscus injury, pancreatic injury or complication of known solid organ injury. Further bleeding may be treated with embolization or surgery determined by hemodynamic deterioration, constellation of injuries and physiological reserve. Missed injuries or complications may require a combination of radiological or surgical intervention depending on the exact diagnosis.
8 PENETRATING INJURY Background Within the trauma network, gunshot wounds are rare but stabbing and impalements are not uncommon. The mechanism of wounding needs to be established as it strongly influences management decisions. Patients suffering stab injury are less likely to require laparotomy (25-33%) than those suffering gunshot injury (80-95%) 1. Note, 55-60% of patients with any stab wound that has entered the peritoneum have hypovolemic shock, peritonitis or bowel / omental evisceration and require a laparotomy. In the remainder, 50% will eventually require operation if observed. The majority of patients with abdominal gunshot wounds have significant intraperitoneal injury and therefore justify laparotomy. Clinicians have a responsibility to inform the police if a patient attends the Emergency Department with a knife or gunshot wound after an assault but demographic information should, in the first instance, only be shared with the patient s consent. Reporting is the responsibility of the ED consultant in charge. Further information can be found: reporting_gunshot.pdf_ pdf Clinical assessment The patient must be assessed by the trauma team in line with ATLS principles. Abdominal examination should be included within C as a potential site of bleeding. As with blunt injury, patients in shock with penetrating chest and / or abdominal injury need to be discussed at a very early stage with: o MTC: the on call vascular trauma consultant (switch board ). o TU: the on call general surgical consultant o Simultaneously ensure O -ve blood will be available o MTC: In all cases of massive transfusion protocol activation ensure the Interventional Radiologist oncall is alerted.
9 o This includes at time of pre-alert from Ambulance Control - Inspection: Anatomically, the intra-abdominal contents may extend anteriorly from the nipples to the groin creases and posteriorly from the scapulae tips to the gluteal folds. Any penetrating wound within this area may produce an intra-peritoneal injury and must be identified. Unless the patient requires an emergency department thoracotomy, the patient must be log rolled to identify all injuries. Particular care should be taken to inspect the axillae and perineum as wounds in these sites can be missed. Skin wounds should be marked with radio opaque markers e.g. closed paper clip taped to anterior wounds and opened paper clip to posterior wounds. Any protruding knife / foreign body must not be removed. Remember, new and progressive abdominal distension in a shocked patient clearly suggests exsanguinating intra-abdominal bleeding but a significant volume of intra peritoneal blood can collect without undue distension. - Palpation: Tenderness around the wound is to be expected but progressive pain and tenderness remote from the initial wound suggests intra peritoneal hollow viscus injury. As with blunt injury, the reliability of clinical examination will be reduced with there are remote but distracting injuries or reduced consciousness (head injury, intoxication, sedating medication, spinal cord injury). - Percussion and auscultation: add little to the examination. The presence or absence of bowel sounds has no diagnostic value. Management of penetrating injuries. The guidance below covers expected management at the Major Trauma Centre. At a Trauma Unit management may be limited by the available resources. When the treatment necessary exceeds the TUs capabilities the patient will require transfer to the MTC.
10 Management of stab wounds (see Figure 2) For patients with penetrating injury balanced resuscitation should be utilized unless contraindicated (head injury) and used with caution in the elderly. Patients with unresponsive or transiently responding shock and considered to have on going intra-abdominal bleeding require rapid transfer to theatre for laparotomy and any other surgery required to control bleeding e.g. thoracotomy. Other causes of severe shock need to be considered e.g. bleeding (chest, limbs, bleeding from wounds), tension pneumothorax and cardiac tamponade. Clearly, patients with multiple wounds can have life threatening pathology in more than one body cavity. Patients with foreign bodies e.g. knives, protruding from the abdomen require these to be removed in the operating theatre with the abdomen open if there is any concern that they may have entered the peritoneum. Preoperative CT scan is likely to be degraded by artefact but may be considered if findings would influence surgical approach. Patients without overt shock but with clinical signs of peritonitis or bowel / omental evisceration require a laparotomy (bowel evisceration is associated with a 75% risk of bowel perforation). A FAST scan has no role in the exclusion of hollow viscus injury. A preoperative CT scan may be undertaken but the trauma scan is poor at detecting fresh hollow organ injury. Patients without overt shock but with an unreliable examination e.g. brain injury, spinal cord injury, intoxication or sedating medication, should have further investigation with a CT scan or undergo exploratory laparotomy / laparoscopy.
11 Patients who are conscious, cooperative and can concentrate and with no signs of peritonitis or diffuse abdominal tenderness (away from the wounding site) may be initially managed non-operatively. A CT scan should be performed to help quantify the depth of injury. Repeated / serial examination preferably by the same experienced surgeon should be undertaken. At hand over, ideally both surgeons should examine the patient together and agree on the clinical findings. Any injury is likely to reveal itself within 24 hours so after this time, if diet can be reintroduced and abdominal findings are minimal, the patient can be discharged. Stab wounds can be classified as anterior (between the anterior axillary lines), flank (between anterior and posterior axillary lines) and posterior (posterior to posterior axillary line). In general, one third of anterior wounds do not penetrate the peritoneum. One third, penetrate the peritoneum but no not require intervention and the remaining third penetrate the peritoneum and require surgical repair. Anterior abdominal wounds may be explored under local anesthetic within the emergency department or within theatre. If the wound extends deep to the anterior fascia then the chance of intraperitoneal hollow viscus perforation is increased although not definite. Patients with posterior fascial penetration proceed to theatre for laparotomy / laparoscopy. Hollow viscus injury can be difficult to detect even at laparotomy. Laparoscopic examination to exclude injury is practiced in some high volume centers. Within the Trauma Network exclusion of visceral injury by laparoscopy should only be performed by those with appropriate skills and experience. Exploration of flank and posterior wounds is rarely indicated. In the absence of a need for immediate laparotomy (shock or generalized peritonitis), a CT scan helps to determine depth of injury. Oral / rectal / IV contrast enhanced CT may help to exclude retroperitoneal organ injury e.g. colon and should be discussed with the on call radiologist. Thoraco-Abdominal injuries can present a diagnostic dilemma as penetrating wounds between the nipples and costal margin may damage structures within the chest cavity, within the peritoneal cavity and make a hole in the intervening diaphragm.
12 o As indicated above, patients with unresponsive or transiently responding shock and considered to have ongoing abdominal or thoracic bleeding require rapid chest drain insertion and transfer to theatre for laparotomy and any other surgery required to control bleeding e.g. thoracotomy. o For patients without overt shock, a CT scan will give some indication of the trajectory of the wound although may not detect incised wounds of the diaphragm. If concern regarding diaphragmatic injury persists, then a laparoscopy should be performed. If an injury is detected then laparotomy is indicated to repair the defect and exclude visceral injury. Both diaphragmatic repair and exclusion of visceral injury are possible laparoscopically but only by those with appropriate skills and experience. Management of low velocity (hand gun / shotgun) gunshot wounds (see Figure 3) Patients with abdominal gunshot wounds have a very high chance of intraperitoneal injury and nearly always justify laparotomy. A few patients suffer tangential wounds where the path of the bullet is subcutaneous and does not penetrate the peritoneum. Plain radiographs (chest & abdo/pelvis) after marking of skin wounds (see above) helps to determine trajectory and is helpful in injury identification and planning the surgical approach. Patients with unresponsive or transiently responding shock require immediate laparotomy. Those without overt shock may undergo a CT scan to guide surgical planning and identify those few patients with tangential injuries. Close range shot gun injuries are locally destructive and likely to penetrate the peritoneum mandating laparotomy. For those delivered at distance, CT scanning may demonstrate pellet penetration deep to peritoneum although scatter may limit image quality.
13 Figure 2: Management algorithm for penetrating stab injury Stab wound potentially involving abdominal cavity Trauma team ATLS assessment Unresponsive / transiently responsive shock Consider also bleeding within chest, limbs & external Tension pneumothorax Cardiac tamponade Protruding knife Peritonitis or omental/gut evisceration No peritonitis & patient co-operative CT scan Close observation & serial examination Progressive pain & tenderness Discharge at 24 hours if improved Laparotomy
14 Figure 3: Management algorithm for penetrating gunshot wound Gunshot wound potentially involving abdominal cavity Trauma team ATLS assessment Unresponsive / transiently responsive shock Consider also bleeding within chest, limbs & external Tension pneumothorax Cardiac tamponade Yes No Mark wounds & plain radiographs if time allows trajectory helps predict injuries Mark wounds & CT scan Laparotomy
15 Related issues Patient advice regarding return to normal activity and return to contact sports Advice regarding mobility must also take into account any musculoskeletal injuries. There is little data to guide return of activity and the following is a probably a conservative recommendation based on injury grade (see Appendix 1-3). However, with regard to solid organ injury (spleen, liver, kidney) recommend o Rest at home = 1 week per grade of injury o Avoid contact sports (including horse riding) = 1 month per grade of injury For example, a patient with a grade III splenic laceration should be advised to o Rest at home for 3 weeks (specifically not to be advised to stay in bed, normal gentle activities of daily living should be fine, do not do anything that gets them out of breath) o No contact sport for 3 months. Venous Thromboembolic (VTE) prophylaxis in patients with abdominal injury Mechanical prophylaxis e.g. calf pumps can be used for all patients unless precluded by lower limb injury. Pharmacological prophylaxis with a fractionated heparin should be commenced when the risk of further bleeding becomes less than the risk of VTE. o Typically, for a patient who has required a laparotomy to arrest bleeding, pharmacological prophylaxis is commenced at of the following day as long as the clotting (APTT & INR) has returned to normal.
16 o There is no evidence that pharmacological prophylaxis reduces the success of non-operative management of blunt liver and splenic injuries. Similarly, pharmacological prophylaxis is commenced at of the following day as long as the clotting (APTT & INR) has returned to normal. o Patients requiring laparotomy for hollow viscus injury rather than bleeding can usually commence post-operative pharmacological prophylaxis at on the day of surgery unless there is evidence of coagulopathy.
17 APPENDIX 1 Liver Injury Scale The American Association for the Surgery of Trauma (AAST) liver injury grading system for liver trauma is as follows: Grade I Haematoma: sub capsular, < 10% surface area Laceration: capsular tear, < 1cm depth Grade II Haematoma: sub capsular, 10-50% surface area Haematoma: intra-parenchymal < 10cm diameter Laceration: capsular tear, 1-3cm depth, < 10cm length Grade III Haematoma: sub capsular, > 50% surface area, or ruptured with active bleeding Haematoma: intra-parenchymal > 10 cm diameter Laceration: capsular tear, > 3 cm depth Grade IV Haematoma: ruptured intra-parenchymal with active bleeding Laceration: parenchymal disruption involving 25-75% hepatic lobes or involves 1-3 Couinaud segments (within one lobe) Grade V Laceration: parenchymal disruption involving >75% hepatic lobe or involves > 3 Couinaud segments (within one lobe) Vascular: juxta-hepatic venous injuries (IVC, major hepatic vein) Grade VI Vascular: hepatic avulsion
18 APPENDIX 2 Splenic injury scale The American Association for the Surgery of Trauma (AAST) splenic injury grading system is as follows: Grade I Subcapsular haematoma <10% of surface area Capsular laceration <1 cm depth Grade II Subcapsular haematoma 10-50% of surface area Intra-parenchymal haematoma <5 cm in diameter Laceration 1-3 cm depth not involving trabecular vessels Grade III Subcapsular haematoma >50% of surface area or expanding Intra-parenchymal haematoma >5 cm or expanding Laceration >3 cm depth or involving trabecular vessels Ruptured subcapsular or parenchymal haematoma Grade IV Laceration involving segmental or hilar vessels with major devascularization (>25% of spleen) Grade V Shattered spleen Hilar vascular injury with devascularised spleen
19 APPENDIX 3 Renal injury scale The American Association for the Surgery of Trauma (AAST) renal injury grading system is as follows: Grade I: Contusion or non-enlarging sub-capsular haematoma, but no laceration. Grade II Superficial laceration <1cm depth and does not involve the collecting system; non expanding peri-renal haematoma. Grade III Laceration >1cm, without extension into the renal pelvis or collecting system and with no evidence of urine extravasation. Grade IV Laceration extends to renal pelvis or urinary extravasation. Vascular: injury to main renal artery or vein with contained haemorrhage. Grade V Shattered kidney. Avulsion of renal hilum: devascularisation of kidney due to hilar injury.
United States Department of Transportation National Highway Traffic Safety Administration Paramedic: National Standard Curriculum 1
 UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
BLUNT TORSO INJURY FROM IMPACT OR DECELERATION HAS ABDOMINAL SOLID ORGAN TRAUMA UNTIL PROVEN OTHERWISE
 Abdominal and Pelvic Trauma In the primary survey, the circulation part includes thinking about the abdomen as a source of occult hemorrhage The OBVIOUS THING is a penetrating abdominal injury Generally
Abdominal and Pelvic Trauma In the primary survey, the circulation part includes thinking about the abdomen as a source of occult hemorrhage The OBVIOUS THING is a penetrating abdominal injury Generally
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma
 Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4
 ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
Emergency Ultrasound Course
 Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
Retrospective Review of Intra Abdominal Injuries Sustained in a Tertiary Teaching Hospital
 American Journal of Medicine and Medical Sciences 2015, 5(1): 26-30 DOI: 10.5923/j.ajmms.20150501.06 Retrospective Review of Intra Abdominal Injuries Sustained in a Tertiary Teaching Hospital Azhar Amir
American Journal of Medicine and Medical Sciences 2015, 5(1): 26-30 DOI: 10.5923/j.ajmms.20150501.06 Retrospective Review of Intra Abdominal Injuries Sustained in a Tertiary Teaching Hospital Azhar Amir
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Chapter 6. Hemorrhage Control UNDER FIRE KEEP YOUR HEAD DOWN
 Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
INJURY SEVERITY SCORING
 INJURY SEVERITY SCORING Injury Severity Scoring is a process by which complex and variable patient data is reduced to a single number. This value is intended to accurately represent the patient's degree
INJURY SEVERITY SCORING Injury Severity Scoring is a process by which complex and variable patient data is reduced to a single number. This value is intended to accurately represent the patient's degree
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
Chapter 7. Expose the Injured Area
 Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
The Abbreviated Injury Scale (AIS) A brief introduction
 The Abbreviated Injury Scale (AIS) A brief introduction Abbreviated Injury Scale 1990 Revision Update 98 The Abbreviated Injury Scale produced by: Association for the Advancement of Automotive Medicine
The Abbreviated Injury Scale (AIS) A brief introduction Abbreviated Injury Scale 1990 Revision Update 98 The Abbreviated Injury Scale produced by: Association for the Advancement of Automotive Medicine
Focused assessment of sonography in trauma
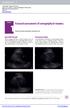 Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
Chapter1 Focused assessment of sonography in trauma Patricia Fermin and John Christian Fox Epicardial fat pad When imaging the heart, careful attention must be made in identifying any surrounding fluid.
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary
 X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
Injury Law Center OTHER INJURIES
 Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. OTHER INJURIES
Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. OTHER INJURIES
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Biliary Stone Disease
 Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Cardiac and Pulmonary Issues in the Elite Athlete. Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015
 Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Guideline for Emergency CT scanning Tony Bleetman Aidan Macnamara October 2008. June annually Emergency Department guidelines
 Meta Data Guideline Title: Guideline Author: Guideline Sponsor: Date of Ratification (CSC): Review Date: Related Policies/Topic/Driver Stored Centrally: Guideline for Emergency CT scanning Tony Bleetman
Meta Data Guideline Title: Guideline Author: Guideline Sponsor: Date of Ratification (CSC): Review Date: Related Policies/Topic/Driver Stored Centrally: Guideline for Emergency CT scanning Tony Bleetman
CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113
 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113 CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder
PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113 CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Mesenteric Angiography
 Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
Information for patients Mesenteric Angiography Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as a Mesenteric Angiogram. This
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients
 Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Oxford Centre for Respiratory Medicine Bronchial-Artery Embolisation Information for patients This leaflet tells you about the bronchial-artery embolisation procedure. It explains what is involved and
Red Flags. Whether you handle malpractice. in General Surgical Malpractice Cases
 10 Red Flags in General Surgical Malpractice Cases Whether you handle malpractice cases regularly or you have a general personal injury practice, at some point you likely will need to evaluate a general
10 Red Flags in General Surgical Malpractice Cases Whether you handle malpractice cases regularly or you have a general personal injury practice, at some point you likely will need to evaluate a general
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Seven steps to patient safety The full reference guide. Second print August 2004
 Seven steps to patient safety The full reference guide Second print August 2004 National Patient Safety Agency Seven steps to patient safety 113 Appendix Four F Examples of events according to severity
Seven steps to patient safety The full reference guide Second print August 2004 National Patient Safety Agency Seven steps to patient safety 113 Appendix Four F Examples of events according to severity
School of Diagnostic Medical Sonography Course Catalog
 School of Diagnostic Medical Sonography Course Catalog 2 School of Diagnostic Medical Sonography Course Schedule Our program provides a broad base of education and performance- based clinical experience
School of Diagnostic Medical Sonography Course Catalog 2 School of Diagnostic Medical Sonography Course Schedule Our program provides a broad base of education and performance- based clinical experience
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES
 Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Damage Control in Abdominal Trauma
 Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Damage Control in Abdominal Trauma Steven Stylianos, MD Surgeon-in-Chief, Morgan Stanley Children s Hospital Rudolph Schullinger Professor of Surgery, Columbia University College of Physicians & Surgeons
Gunshot wounds. Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P
 Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY
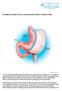 INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
Confirmed Deep Vein Thrombosis (DVT)
 Confirmed Deep Vein Thrombosis (DVT) Information for patients What is deep vein thrombosis? Blood clotting provides us with essential protection against severe loss of blood from an injury to a vein or
Confirmed Deep Vein Thrombosis (DVT) Information for patients What is deep vein thrombosis? Blood clotting provides us with essential protection against severe loss of blood from an injury to a vein or
4.2 Spinal Cord Compression
 4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
Basic ATLS. The Primary Survey. Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon
 Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
School of Diagnostic Medical Sonography Course Catalog
 School of Diagnostic Medical Sonography Course Catalog 2 School of Diagnostic Medical Sonography Course Schedule Our program provides a broad base of education and performance- based clinical experience
School of Diagnostic Medical Sonography Course Catalog 2 School of Diagnostic Medical Sonography Course Schedule Our program provides a broad base of education and performance- based clinical experience
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Uterine fibroids (Leiomyoma)
 Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy. Case Series
 ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Ultrasound Billing CPT Codes Summary and Notes
 Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Peritoneal Carcinosis
 Peritoneal Carcinosis What is it and how to cure it Peritoneum Peritoneum is a thin and transparent membrane that covers the internal part of the abdominal and pelvic cavity and all the viscera contained
Peritoneal Carcinosis What is it and how to cure it Peritoneum Peritoneum is a thin and transparent membrane that covers the internal part of the abdominal and pelvic cavity and all the viscera contained
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON. Director of surgical department of Lefkos Stavros of Athens
 Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
ITLS Basic Pre-Test 7 th Edition
 1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
Introduction. Advantages of minimally invasive surgery (MIS) in pediatric trauma:
 Introduction Purpose of Study: To validate the use of laparoscopic and thoracoscopic surgery for diagnostic and therapeutic modalities in the treatment of pediatric trauma Advantages of minimally invasive
Introduction Purpose of Study: To validate the use of laparoscopic and thoracoscopic surgery for diagnostic and therapeutic modalities in the treatment of pediatric trauma Advantages of minimally invasive
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
LEADING CAUSE OF DEATH FOR PERSONS UNDER 39 YEARS OLD RESPONSIBLE FOR MORE THAN 150,000 DEATHS EACH YEAR, NEIGHBORHOOD OF 50,000000 ON HIGHWAYS
 THE KINETICS OF T MAX BORNSTEIN, NREMTP OLD DOMINION OMINION EMS A EMS ALLIANCE DIRECTOR PRINCE GEORGE FIRE (RETIRED) OF TRAUMA IRE/EMS BASIC TRAUMA F RAUMA FACTS LEADING CAUSE OF DEATH FOR PERSONS UNDER
THE KINETICS OF T MAX BORNSTEIN, NREMTP OLD DOMINION OMINION EMS A EMS ALLIANCE DIRECTOR PRINCE GEORGE FIRE (RETIRED) OF TRAUMA IRE/EMS BASIC TRAUMA F RAUMA FACTS LEADING CAUSE OF DEATH FOR PERSONS UNDER
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
The Acute Abdomen. Dr. Ed Snyder Dr. Melanie Walker Huntington Memorial Hospital
 The Acute Abdomen Dr. Ed Snyder Dr. Melanie Walker Huntington Memorial Hospital Causes of the Acute Abdomen Hemorrhage in the GI tract Blood vessel GU tract Perforation of the GI tract Ulcer Infection
The Acute Abdomen Dr. Ed Snyder Dr. Melanie Walker Huntington Memorial Hospital Causes of the Acute Abdomen Hemorrhage in the GI tract Blood vessel GU tract Perforation of the GI tract Ulcer Infection
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
INFORMATION FOR PATIENTS CONSIDERING LAPAROSCOPIC INGUINAL HERNIA REPAIR
 INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
Vascular Technology (VT) Content Outline Anatomy & physiology 20% Cerebrovascular Cerebrovascular normal anatomy Evaluate the cerebrovascular vessels
 Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
Coding Companion for Urology/Nephrology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
Pennsylvania Trauma Nursing Core Curriculum. Posted to PTSF Website: 10/30/2014
 Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Bile Leaks After Laparoscopic Cholecystectomy. Kings County Hospital Center Eliana A. Soto, MD
 Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi
 Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Laparoscopic Cholecystectomy (Removal of the Gallbladder)
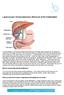 Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Abdomen X-Ray (AXR) Collimation is ideally from diaphragms to lower border of the symphysis pubis and the lateral skin margins.
 Abdomen X-Ray (AXR) Collimation is ideally from diaphragms to lower border of the symphysis pubis and the lateral skin margins. LMP of child-bearing age female patients should be checked. 1. Acute abdomen
Abdomen X-Ray (AXR) Collimation is ideally from diaphragms to lower border of the symphysis pubis and the lateral skin margins. LMP of child-bearing age female patients should be checked. 1. Acute abdomen
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
School of Diagnostic Medical Sonography
 Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care. Clinical Management Guideline: Standard Trauma Resuscitation
 Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
KEYHOLE HERNIA SURGERY
 Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Pathway for the Management of Acute Gallstone Diseases
 Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
LAPAROSCOPIC OVARIAN CYSTECTOMY
 LAPAROSCOPIC OVARIAN CYSTECTOMY Information Leaflet Your Health. Our Priority. Page 2 of 5 About this information This leaflet is for you if you have a cyst on one or both ovaries and are considering surgery.
LAPAROSCOPIC OVARIAN CYSTECTOMY Information Leaflet Your Health. Our Priority. Page 2 of 5 About this information This leaflet is for you if you have a cyst on one or both ovaries and are considering surgery.
Catheter Embolization and YOU
 Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report
 Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report 1. Background Information 1.1. Initial review of the tool in November 2006, and subsequent queries in January
Clinical Governance Development Committee October 2007 Dr Foster RTM Alerts Progress Report 1. Background Information 1.1. Initial review of the tool in November 2006, and subsequent queries in January
Women s Health Laparoscopy Information for patients
 Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
Electrical Burns 新 光 急 診 張 志 華
 Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Complications of Femoral Catheterization. Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005
 Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
