Kinematic Alignment in Total Knee Arthroplasty
|
|
|
- Darleen Morgan
- 9 years ago
- Views:
Transcription
1 Chapter 121 Kinematic lignment in Total Knee rthroplasty Stephen M. Howell and Maury L. Hull The most important predictor of clinical outcome in total knee arthroplasty (TK) is placement of the femoral and tibial components. Prior to the advent of kinematic alignment, the placement of components was based on the widely accepted principles of classic mechanical alignment, as follows: (1) aligning the femoral component perpendicular to the mechanical axis of the femur; (2) aligning the tibial component perpendicular to the mechanical axis of the tibia; (3) adjusting the anterior-posterior and internal-external rotation positions of the femoral component so that the extension and flexion gaps are equal; and (4) releasing ligaments when necessary to restore motion and balance the knee. In kinematic alignment, the principles for placing the components are different from those of classic mechanical alignment, as follows: (1) coaligning the transverse axis of the best-fitting femoral component with the primary transverse axis in the femur about which the tibia flexes and extends; (2) removing osteophytes to restore ligament length motion and stability; and (3) placing the tibial component so that the longitudinal axis of the tibia is perpendicular to the transverse axis in the femur, about which the tibia flexes and extends. Kinematic alignment can prevent the loss of flexion and extension, stiffness, instability, pain, and prolonged recovery associated with mechanical alignment. 16,17 Kinematic alignment of the femoral component is confirmed intraoperatively by comparing the symmetry of the thickness of the distal medial, distal lateral, posterior medial, and posterior lateral femoral bone resections after measuring the thickness of the resections with calipers and after correcting for cartilage wear, bone wear, and kerf (i.e., the bone removed by the saw blade). Once kinematic alignment of the femoral component is confirmed, restoring motion and balancing the total knee arthroplasty is simplified by following a stepwise algorithm. The algorithm consists of four steps removing osteophytes, adjusting the plane of the tibial cut, releasing the posterior capsule from the femur, and medializing or lateralizing the tibial component. This chapter reviews the history and definition of kinematic alignment with patient-specific guides, highlights the inherent disadvantages of mechanical alignment that kinematic alignment strives to avoid, describes the planning, outlines the algorithm for restoring motion and balancing the kinematically aligned TK, provides an overview of the surgical technique of kinematic alignment with patient-specific cutting guides and unconventional use of conventional instruments, addresses theoretical concerns of kinematic alignment, and reviews clinical studies showing the early benefits of kinematically aligning the TK. History and Definition of Kinematic lignment The biomechanical rationale for kinematic alignment is traced to Hollister and colleagues classic research on the kinematics of the knee. 12 Kinematics refers to the relative relationship of the femur, patella, and tibia at any angle of flexion, without force applied to the knee. The joint surface, menisci, and ligament structures determine the normal kinematic relationship among the femur, patella, and tibia. The center of the femoral head and center of the ankle, which are used by conventional and computer-assisted instruments to align a TK mechanically, have no bearing on the kinematics of the knee. 10,11,14,15 Three axes govern the movement of the patella and tibia with respect to the femur, and understanding how the placement of the femoral and tibial components affects the interrelationship of these axes is the key to kinematically aligning a TK (Fig ). The primary axis is a transverse axis in the femur about which the tibia flexes and extends. It passes through the center of a circle fit to the articular surface of the femoral condyles from 10 to 160 degrees of flexion. 7,10-12 There is a second transverse axis in the femur about which the patella flexes and extends that is parallel, proximal, and anterior to the transverse axis in the femur about which the tibia flexes and extends. The third axis is a longitudinal axis in the tibia about which the tibia internally and externally rotates on the femur that is perpendicular to each of the two transverse axes in the femur. lthough each of the three axes is aligned parallel or perpendicular to one another, none are aligned orthogonally to the three anatomic planes, which means that the axis cannot be found with imaging studies performed in the sagittal, coronal, and axial planes. 15 The goal for kinematically aligning the femoral component is to coalign the transverse axis of a symmetrical femoral component with the primary transverse axis in the femur about which the tibia flexes and extends (Fig ). 7,10-12,14 ecause there is no clinically important asymmetry between the medial and lateral femoral condyles in the varus and valgus knee with end-stage osteoarthritis, a symmetrical, single-radius femoral component is an optimal design for replicating knee kinematics. The principle for kinematically aligning the femoral component to the femur is the simple step of shape-matching the femoral component to the articular surface of the femur on a three-dimensional model of the knee that has been restored to normal by filling in the worn articular surface. Shape matching the femoral component to the femur coaligns the transverse axis of the femoral component with the primary transverse axis in the femur about which the tibia flexes and extends, which is requisite to restoring the normal interrelationships among the three axes. 13,16 In contrast to the simplicity of kinematically aligning the femoral component, kinematically aligning the tibial component involves several steps. The first step is to align the anterior-posterior axis of the tibial component perpendicular to the transverse axis in the femoral component, which has previously been coaligned to the primary transverse axis in 1255 main.indd /3/2011 2:15:14 PM
2 1256 Section 12 Joint Replacement and Its lternatives Figure Interrelationship of the three kinematic axes in a right knee., Coronal projection with the knee in extension., xial projection of the femur with the knee in 90 degrees of flexion. C, Lateral projection with the knee in extension. The primary transverse axis in the femur about which the tibia flexes and extends passes through the center point of the best-fit circles of the medial and lateral femoral condyles (green line and circle), which is equidistant from the articular surface of the condyles (double-headed black arrows). second transverse axis in the femur about which the patella flexes and extends axis (magenta line and circle) is oriented parallel, proximally, and anteriorly to the transverse axis in the femur about which the tibia flexes and extends. third longitudinal axis in the tibia (vertical orange line) about which the tibia rotates on the femur internally and externally is oriented perpendicular to both transverse axes in the femur. Figure Single-radius femoral component of a right knee (silver) shape-matched to the femur of a normal knee model (pink). Shape matching the femoral component to the femur is the critical step in kinematically aligning the knee and in reestablishing the orthogonal interrelationships among the three kinematic axes. kinematically aligned femoral component greatly simplifies the stepwise algorithm for identifying the correct options for restoring motion and balance to the knee before cementation of the components. The principle for kinematically aligning the tibial component to the femoral component is to align the anterior-posterior axis of the tibial component perpendicular to the transverse axis in the femur and femoral component. The principle for kinematically aligning the tibia to the tibial component is to accept the assumption that the internal-external rotational relationship between the femur and tibia is normal in a non weight-bearing MRI scan and then center the tibia under the center of the tibial component. the femur about which the tibia flexes and extends by the shape-matching step. 1,7 The second step is to align the tibia to the tibial component kinematically, which is based on the assumption that the internal-external rotational relationship between the femur and tibia is normal in a magnetic resonance imaging (MRI) scan of the non weight-bearing knee with end-stage osteoarthritis. The assumption that the internal-external rotational relationship is normal in the non weight-bearing knee with end-stage osteoarthritis is inferred from the layer of joint fluid that is consistently seen separating the worn articular surface between the femur and tibia on the MRI scan of the knee. oth the layer of joint fluid and the image of a non weight-bearing knee indicate that there is no contact between the worn femur and tibia and no transmission of force across the knee to malrotate the tibia on the femur. The final step is aligning the center of the tibia under the center of the tibial component. With a goal of improving on the 20% prevalence of patient dissatisfaction from mechanically aligned TK with conventional and computer-assisted instruments, 3,5 we began developing the method for performing kinematic alignment with patient-specific femoral and tibial cutting guides in We developed software that creates a threedimensional model of the arthritic knee from a non weightbearing MRI or computed tomography (CT) arthrogram of the knee (OtisKnee, OtisMed, lameda, Calif; dditional software transforms the arthritic knee model to a normal knee model and then kinematically aligns the components by shape-matching the best-fitting femoral and tibial components to the normal main.indd /3/2011 2:15:16 PM
3 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1257 Femoral guide Tibial guide Figure Femoral () and tibial () patient-specific cutting guides (orange) on the arthritic knee model (right knee). The saw slot (black arrow) in each guide sets the proximal-distal, flexion-extension, and varus-valgus degrees of freedom of each component. The two holes (white arrows) in each guide set the internal-external rotation, anterior-posterior, and medial-lateral degrees of freedom of each component. knee model. The three-dimensional position of each component is then transferred from the normal knee to the arthritic knee model. Patient-specific cutting guides that incorporate the cut planes of each component and that reference the arthritic knee model are made to fit the patient s femur and tibia (Fig ). The cutting guides are used intraoperatively to transfer the six degrees of freedom (6DOF) positions of the femoral and tibial components from the computer to the patient varus-valgus, internal-external rotation, flexion-extension, anterior-posterior, proximaldistal, and medial-lateral. 13,14,16,25 The first use of patient-specific cutting guides to align a TK kinematically was in January s of ugust 2009, 23,000 kinematically aligned TKs had been implanted with patient-specific cutting guides nationwide with the lead author (SMH) implanting over 700. From September through December 2009, he implanted 116 kinematically aligned TKs with unconventional use of conventional instruments instead of patient-specific cutting guides. This 4-year developmental and clinical experience, which is admittedly limited in terms of long-term follow-up, forms the basis for the concepts shared in this chapter with the primary goals of stimulating debate and advancing the understanding of kinematic alignment of total knee arthroplasty. dvantages of Kinematic lignment Over Mechanical lignment Studies from the United Kingdom and Canada that reviewed more than 10,000 patients at 1 year following mechanically aligned TK with conventional instruments and contemporary components have shown that one of five patients are not satisfied because of continued pain and poor function in activities of daily living (DLs). 3,5 The use of computerassisted surgery has improved the mechanical alignment compared with conventional surgery, but has not improved the clinical outcome (much to the dismay of proponents of computer-assisted surgery). 2,9,21,26 Therefore, a mechanically aligned TK, whether performed with conventional instruments or computer assistance, has an unacceptably high prevalence of continued pain, poor function in DLs, and patient dissatisfaction, which means that there is ample room for improvement. For the kinematics of a TK to be the same as a normal knee, the three-dimensional placements of the femoral and tibial components have to be chosen so that the orientation of the three kinematic axes is unchanged from that of the normal knee. None of these axes can be found by referencing the transepicondylar axis, center of the femoral head, and center of the ankle with the use of conventional or computer-assisted instruments. 1,10,15 There is a 5-degree average difference (range, 2 to 11 degrees) between the transepicondylar and primary transverse axes in the femur about which the tibia flexes and extends, which means that referencing the transepicondylar axis substantially changes the joint line from normal in the axial plane. 11 Of normal subjects, 98% do not have a neutral hip-knee-ankle axis because the longitudinal shape of the femur and tibia are unrelated and variable among subjects, which means that referencing the center of the femoral head and of the ankle changes the joint line in the coronal plane. 12 Changing the joint line of the femur from normal in the axial and/or coronal planes using instruments that align components to the transepicondylar axis, center of the femoral head, and center of the ankle kinematically malalign the knee and may explain the midrange instability reported in TK (Fig ). 7 ecause mechanical alignment kinematically malaligns the knee, we hypothesized that kinematic alignment would reduce the high prevalence of persistent pain, poor function in DLs, and patient dissatisfaction after mechanically aligned TK with conventional and computer-assisted instruments. 16,25 Planning Kinematic lignment With Patient-Specific Cutting Guides Protocol for ligning and Performing Magnetic Resonance Imaging of the Knee For kinematic alignment, the projection of the knee in the MRI scan has to be customized to the patient s knee position in the MRI scanner so that the oblique sagittal image plane main.indd /3/2011 2:15:17 PM
4 1258 Section 12 Joint Replacement and Its lternatives is perpendicular to the primary axis in the femur about which the tibia flexes and extends. patient that has a painful osteoarthritic knee should be allowed to choose a position for the leg that is comfortable so that he or she does not inadvertently move the knee during image acquisition and cause Femoral component in valgus Figure Illustration of how a femoral component not shapematched to the articular surface of the normal knee in the coronal plane () or the axial plane () kinematically malaligns the knee. Placing the femoral component in more valgus (or varus) than normal () tilts the transverse axis in the femoral component (green line) so that it is no longer parallel to the primary transverse axis in the femur about which the patella flexes and extends (magenta line), nor is it perpendicular to the longitudinal axis in the tibia (orange), which kinematically malaligns the movement of the patella on the femur and the tibia on the femur. Placing the femoral component in more external rotation (or internal rotation) than normal () tilts the transverse axis in the femoral component (green line) so that it is no longer parallel to the transverse axis in the femur nor is it perpendicular to the longitudinal axis in the tibia (orange), which kinematically malaligns the movement of the patella on the femur and the tibia on the femur. Tilting the femoral component in just one plane or in opposite directions in the coronal and axial planes creates an uncorrectable ligament imbalance (white arrows). In this right knee, valgus positioning of the femoral component loosens the lateral side in extension () and external rotation of the femoral component worsens the ligament balance by tightening the lateral side in flexion (). The only way to maintain ligament balance throughout the motion arc is to shape-match the femoral component to the femur. Femoral component in external rotation a motion artifact. The knee with a severe varus or valgus deformity or flexion contracture can be successfully imaged without forcing the knee into extension or an uncomfortable rotation by customizing the projection of the knee in the coronal and axial planes. The following are contraindications for MRI of the knee for patient-specific cutting guides: (1) presence of a pacemaker; (2) movement of the knee during image acquisition because of inability to follow instructions, tremor, and claustrophobia; (3) obese knee that prevents the use of a dedicated knee coil; (4) hardware about the knee that distorts the image and subsequent three-dimensional model; and (5) metal in the body that might move in the magnetic field (e.g., brain aneurysm clips, metal in the eye, shrapnel near vital structures). The following is a description of the suggested MRI technique, which relies on the use of coronal and axial locator images to obtain nonorthogonal, oblique, sagittal images perpendicular to the primary transverse axis in the femur about which the tibia flexes and extends (Fig ). 14 nonorthogonal, oblique, sagittal MRI scan of the treated knee is obtained using a 1.5- or 3.0-T scanner and dedicated knee coil. The plane for the nonorthogonal, oblique, sagittal scan is based on the use of coronal and axial locator images. These images are used to align the image plane perpendicular to the primary transverse axis in the femur about which the tibia flexes and extends, which projects the femoral condyles approximately in the same plane that the tibia flexes and extends about the femur. Coronal, axial, and sagittal highresolution locator images are obtained using a 4-mm slice thickness, 1-mm spacing/gap, matrix, one number of excitations (NEX), and 24-cm field of view (FOV), which yield nine slices in all three planes. The locator image in the coronal plane that shows the largest projection of the distal femoral condyles is used to adjust the varus-valgus orientation of the plane of the nonorthogonal, oblique, sagittal scan. The nonorthogonal, oblique, sagittal scan plane is aligned perpendicular to a line connecting the cortical-cancellous bone interface of the distal femoral condyles on the locator image in the coronal plane. The locator image in the axial plane that shows the largest projection of the posterior femoral condyles is used to adjust the axial rotation of the plane of the nonorthogonal, oblique, sagittal scan. The nonorthogonal, oblique, sagittal Figure Illustration of the coronal () and axial () localizers, femoral joint line (thick white line), transverse axis in the femur about which the tibia flexes and extends (green line), and plane for the nonorthogonal, oblique, sagittal scan (thin parallel lines). ligning the nonorthogonal, oblique, sagittal scan perpendicular to the distal femoral joint line (thick white line) in the coronal localizer and the posterior femoral joint line (thick white line) in the axial localizer aligns the nonorthogonal, oblique, sagittal scan perpendicular to the transverse axis in the femur about which the tibia flexes and extends (green line), which projects the femoral condyles as a circle in the same plane that the tibia flexes and extends about the femur. main.indd /3/2011 2:15:18 PM
5 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1259 scan plane is aligned perpendicular to a line connecting the cortical-cancellous bone interface of the posterior femoral condyles in the locator image in the axial plane. ecause the contour of the posterior femoral condyles from 10 to 160 degrees forms a single radius of curvature, and because the primary transverse axis in the femur about which the tibia flexes and extends is equidistant from the distal and posterior articular surfaces of the femoral condyles, the femoral condyles are projected as circular in the nonorthogonal, oblique, sagittal imaging plane and perpendicular to the primary transverse axis in the femur about which the tibia flexes and extends. 10,11,14 nonorthogonal, oblique, sagittal scan is then acquired of the knee, which is subsequently processed with software to generate a three-dimensional model of the knee. The scanning parameters are selected to provide contrast among fat, joint fluid, cartilage, degenerative and normal menisci, and subchondral, cancellous, and cortical bone. For a 1.5-T scanner and a dedicated knee coil (General Electric Medical Systems, Milwaukee, Wisc), we use these parameters: FRFSE PD, 30 to 35 TE, 2800 to 3400 TR, Hz bandwidth, and minimum of two excitations using a 16-cm field of view centered at the joint line of the knee, matrix, 2-mm slice thickness, with no spacing or gap. The length of each side of a pixel in the oblique sagittal image is 0.31 mm. 14 Generation of Three-Dimensional rthritic and Normal Knee Models Kinematic alignment of the femoral and tibial components begins with a three-dimensional arthritic knee model generated from the MRI scans, from 44 to 60 slices, depending on the width of the knee (Fig ). Proprietary software segments the femur, tibia, articular cartilage, and osteophytes from each image and meshes the images together to form a rthritic knee model Figure Illustration of the arthritic knee model () and normal knee model () created with software from an MRI scan of the knee. The software creates the normal knee model from the arthritic knee model by removing osteophytes, filling in worn joint surfaces, centering the tibia under the femur, and reestablishing an equal medial and lateral joint space (white arrows). Normal knee model three-dimensional model of the arthritic knee (OtisMed). series of steps is applied to the arthritic knee model to create a normal knee model. The articular surface of the arthritic knee model is transformed into a knee with a normal articular surface by filling articular defects. Osteophytes are removed to restore ligament length and restore a normal shape to the knee. The normal knee model is then aligned in the coronal plane by adjusting the varus-valgus rotation and proximaldistal position of the tibia until the distance between the femoral and tibial articular surfaces is equal medially and laterally. 13,16 This process of creating a normal knee from an arthritic knee by filling defects, removing osteophytes to restore ligament length, and reestablishing a symmetrical medial-lateral joint space borrows from the well-established principles used to align the mobile-bearing unicompartmental knee replacement (i.e., Oxford Knee). Shape-Matching Femoral and Tibial Components The three-dimensional model of the femoral and tibial component that best fits the normal knee model is selected by proprietary software (see Fig ). lgorithms shapematch the femoral component to the restored articular surface of the femur in the normal knee model from 10 to 160 degrees, which kinematically aligns the femoral component by coaligning the transverse axis of the femoral component with the primary transverse axis in the femur about which the tibia flexes and extends. The internal-external rotation of the anterior-posterior axis of the tibial component is set perpendicular to the transverse axis of the femur and femoral component, which kinematically aligns the tibial component to the femoral component. The tibia is centered under the tibial component, which kinematically aligns the tibia to the tibial component. 1,7,10,12 In theory, kinematic alignment restores the normal parallel and perpendicular interrelationship among the three kinematic axes of the prearthritic knee. 14 Function, Design, and Machining of Patient-Specific Cutting Guides common function of all patient-specific cutting femoral and tibial cutting guides, whether they are made to align the TK kinematically or mechanically, is to transfer the position of each component in three-dimensional space accurately from the computer to the operating room (see Fig ). Each cutting guide sets 6DOF positions of the component in three-dimensional space, which is comprised of three rotations flexion-extension, varus-valgus, and internal-external and three translations (proximaldistal, anterior-posterior, and medial-lateral). When osteophyte removal changes the dimensions of the femur and tibia, the surgeon has the option to adjust the medial-lateral position of the femoral and tibial components visually. The patient-specific cutting guides are designed to be small enough to fit in the knee using minimally invasive incisions, yet large enough to register enough knee topography so that the surgeon accurately seats the guide in the intended position. In the event that a cutting guide is inadvertently dropped on the floor, the guide must be sturdy enough to avoid breakage and retain its cavitary shape during resterilization with heat. Rapid manufacturing is required to make the main.indd /3/2011 2:15:19 PM
6 1260 Section 12 Joint Replacement and Its lternatives production of patient-specific cutting guides cost-effective and to limit the turnaround time between receiving the MRI scan and shipping the finished guides. Currently, the turnaround time varies from 10 to 20 business days, depending on the manufacturer, but with future technologic improvements, might only be 1 day. Patient-specific femoral and tibial cutting guides are machined to fit the arthritic knee model using a biocompatible plastic (polyoxymethylene [POM], Delrin). The cut planes corresponding to the positions of the femoral and tibial components in the normal knee model are transferred to the arthritic knee model. There is one saw slot and four holes for fixation pins in each guide (see Fig ). The saw slot sets the proximal-distal, flexion-extension, and varusvalgus degrees of freedom of each of the femoral and tibial components. The two pinholes on the articular surface of each guide set the anterior-posterior and internal-external rotation degrees of freedom of each of the femoral and tibial components. The two pinholes on the articular surface of each guide are used to pin the guide to the knee and also reference the conventional chamfer block and tibial component alignment instrument. The two pinholes on the anterior surface of each guide are used to pin the guide to the knee; they also accept the conventional distal femoral and proximal tibial cutting guides for the surgeon who prefers to use the conventional cutting block instead of the saw slot in the patient-specific guide. Hence, each guide provides the surgeon with the size and position of the femoral and tibial components and efficiently and accurately transfers the 6DOF position of each component from the computer to the patient.* *References 1, 2, 6, 7, 9, and 13. lgorithm for Restoring Motion and alancing the Kinematically ligned Total Knee rthroplasty The algorithm for determining the stepwise corrections to restore motion and balance to the knee before cementation of the components is greatly simplified by first aligning the femoral component kinematically (Fig ). Kinematic alignment of the femoral component is confirmed intraoperatively by comparing the symmetry of the thickness of the distal medial, distal lateral, posterior medial, and posterior lateral femoral bone resections after measuring the thickness of the resections with calipers and after correcting for cartilage wear, bone wear, and saw blade kerf. fter correction, the thickness of each bone resection should equal the thickness of the condyle of the femoral component. For example, if a femoral component 8 mm thick and a saw blade 1.25 to 1.37 mm thick are used, then each bone resection should be 6.5 mm thick when there is no cartilage wear or bone wear. Predicting the thickness of each bone resection is more complicated in the arthritic femur in which there is preexisting focal cartilage wear (typically, 1 to 2 mm) and occasionally bone wear (usually no more than 1 mm). The resection thickness can be predicted preoperatively from a biplanar, rotationally controlled MRI scan, which is carefully viewed to reveal the location and amount of wear (Fig ). 14 fter selecting the image that projects the largest radius of each femoral condyle using image analysis software (OsiriX DICOM Viewer, Dicom Solutions, Irvine, Calif; the thickness of the cartilage on the distal and posterior surface of the unworn and worn condyles is measured in millimeters. The difference in thickness between the worn and unworn condyle is computed in millimeters and Is femoral component kinematically aligned? (Measure distal and femoral bone resection thickness with calipers) Yes Distal and posterior femoral bone resections equal thickness of femoral component (after factoring wear and kerf) No Distal and posterior femoral bone resections DO NOT equal thickness of femoral component (after factoring wear and kerf). Recut Tight in extension and flexion? Tight in extension? Tight in flexion? Tight medially? Tight laterally? 1. Remove more tibia 1. Remove posterior osteophytes 2. Strip posterior capsule off femur 3. Decrease posterior tibial slope 1. Increase 1. Remove posterior medial slope osteophytes 2. Cut tibia in more varus 1. Remove lateral osteophytes 2. Cut tibia in more valgus Figure lgorithm for restoring motion and balancing the kinematically aligned TK. main.indd /3/2011 2:15:19 PM
7 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1261 Figure Illustration of a circle fit to the unworn lateral femoral condyle () and worn medial femoral condyle (). On the medial side, the wear on the distal medial femoral condyle measures 1.5 mm and there is no wear on the posterior medial femoral condyle. For an 8-mm-thick femoral condyle, the thickness of the distal medial resection should be 5 mm and the thickness of the posterior medial, distal lateral, and posterior lateral resection should be 6.5 mm. The femoral component is kinematically aligned when the thicknesses of each femoral resection are equal and equal to the thickness of the femoral component, after correcting for cartilage wear, bone wear, and saw blade kerf. Distal medial resection 4 mm Posterior medial resection 5 mm used to determine the location and amount of correction needed for the worn condyle. In a varus osteoarthritic knee, which typically has 2 mm of distal and 1 mm of posterior cartilage wear, the distal medial resection should be 4.5 mm thick and the distal lateral resection should be 6.5 mm, which give a 2-degree correction in the coronal plane (Fig ). The posterior medial resection should be 5.5 mm thick and the posterior lateral resection should be 6.5 mm thick, which gives a 1-degree correction in the axial plane. If the planned and executed cuts do not match, fine adjustments in the varus-valgus, internal-external rotation, proximal-distal, and anterior-posterior positions of the femoral component should be made. ccounting for cartilage wear, bone wear, and saw blade kerf when selecting the distal and posterior cut planes is needed to correct coronal and axial malrotation. This is also needed to set the varus-valgus and internal-external rotation and flexion-extension, proximal-distal, anteriorposterior, and medial-lateral positions of the femoral component so that the femoral component is shape-matched to a restored articular surface. When a single-radius femoral component is used, shape-matching the femoral component to a restored articular surface on the femur coaligns the transverse axis of the femoral component with the primary transverse axis of the femur about which the tibia flexes and extends and kinematically aligns the knee. 16,17 Once the femoral component is kinematically aligned, all subsequent steps to restore motion and balance the knee are limited to just four options removing osteophytes, adjusting the plane of the tibial cut, releasing the posterior capsule from the femur, and medializing or lateralizing the tibial component. To determine which options are needed to restore motion and balance the knee, the knee is examined with trial components with the aim of deciding whether the knee fully flexes and extends and whether anterior-posterior and varusvalgus stability are acceptable at 30-degree intervals, from full extension to flexion. If the knee lacks extension and lacks flexion but has anterior-posterior and varus-valgus stability throughout the motion arc, then remove more tibia. If the knee lacks extension but fully flexes and has anterior-posterior and varus-valgus stability throughout the motion arc, then Distal lateral resection 6.5 mm Posterior lateral resection 7 mm Figure Illustration of a weight-bearing anteroposterior and lateral radiograph of a right knee with varus osteoarthritis (top) and the distal medial, posterior medial, distal lateral, and posterior lateral bone resections with their measured thickness in millimeters (mm; bottom). The distal medial resection is 4.5 mm thick and the distal lateral resection is 6.5 mm, which gives a 2-degree correction in the coronal plane. The posterior medial resection is 5 mm thick and the posterior lateral resection is 7 mm thick, which gives a 2-degree correction in the axial plane. To align an 8-mm-thick femoral component kinematically, each resection should be 6.5 mm thick after accounting for cartilage and bone wear and saw blade kerf, which is 1.25 to 1.5 mm thick, depending on the thickness of the saw blade. remove posterior osteophytes and release the posterior capsule. If removal of the posterior osteophytes and releasing the posterior capsule are ineffective, decrease the posterior slope on the tibia. We do not recommend additional resection of bone from the distal femur to restore extension unless the distal bone resection is 2 mm or more thinner than the posterior bone resection. The penalty from additional resection of bone from the distal femur is proximal movement of the femoral component, primary transverse axis of the femur, and joint line, which kinematically malaligns the knee and limits flexion. 24 If the knee lacks flexion but fully extends and has anteriorposterior and varus-valgus stability throughout the motion arc, then increase the posterior slope on the tibia. We have not found the need to recess or release the posterior cruciate ligament (PCL) to increase flexion. If the knee is tight medially throughout the motion arc, then remove all medial osteophytes. If the medial tightness persists after removing medial osteophytes from the tibia and femur, recut the tibia in 1 to 2 degrees more varus as long as the overall alignment of the limb will be acceptable. If the medial tightness persists after recutting, medialize the tibia on the tibial component and remove any bone from the tibia that extends beyond the tibial component 19 (Fig ). If the knee is tight laterally main.indd /3/2011 2:15:21 PM
8 1262 Section 12 Joint Replacement and Its lternatives Figure Intraoperative photograph of a right knee showing the tibia medialized on the trial base plate and a saw-trimming bone extending beyond the component to reduce medial tightness. The decision to medialize the tibia on the tibial component was made because of medial tightness that persisted after removing osteophytes from the medial femur and tibia, and after verifying that the plane of the varus-varus cut of the tibia was correct. This sequence of steps restores motion, stability, and alignment without releasing the medial collateral ligament in the knee with varus deformity caused by osteoarthritis. throughout the motion arc, remove all lateral osteophytes. If the lateral tightness persists after removing lateral osteophytes from the tibia and femur, recut the tibia in 1 to 2 degrees more valgus as long as the overall alignment of the limb will be acceptable. If the PCL ligament is insufficient because of inadvertent release or incompetency and there is anterior-posterior and varus-valgus instability in 90 degrees of flexion but not in full extension, resect 2 mm of bone from the distal femur and use a 2-mm thicker liner. If the knee still has anterior-posterior and varus-valgus instability in 90 degrees of flexion, use a liner with an increased anterior slope or a posterior-stabilized component. Surgical Techniques Patient-Specific Cutting Guides The range of motion and magnitude of varus-valgus deformity are assessed under anesthesia. knee with a varus or valgus deformity is typically corrected by a thorough removal of medial or lateral femoral and tibial osteophytes, respectively. 16,25 knee with a flexion contracture of 10 degrees or more is typically corrected by removal of posterior osteophytes and posterior capsule release from the femur; this rarely requires additional resection of bone from the femur. 24 The operating room technician, circulating nurse, and surgeon should each cross-check the information etched on the patient-specific femoral and tibial cutting guides before anesthetizing the patient. Each guide has the name of the surgeon, patient initials and date of birth, component size, and an inscription of R or L, which indicates the side of the knee being operated on. The operating room technician and circulating nurse should also verify that they have sterilized the patient-specific cutting guides, correct subset of conventional instruments, and trial components that match the size determined by computer planning (Fig ). The use of Figure Photograph of the scrub table shows that one tray of instruments is needed to perform a kinematic TK with patientspecific cutting guides. The patient-specific femoral guide (FG) and tibial guide (TG) are sterilized with the instruments and trial components that match the size of the components to be used, as determined by computer planning. patient-specific cutting guides reduces the number of instrument trays from eight to one, which decreases operating time, room turnover time, and cost of processing instruments. 16 midvastus approach without patellar eversion gives an adequate exposure for using the patient-specific cutting guides. Fat is removed from the anterior surface of the femur proximal to the trochlear groove, as are any prominent osteophytes extending from the proximal trochlea. The patientspecific femoral guide is seated on the anterior cortex and trochlear groove, and centered mediolaterally on the distal femur (Fig ). The guide is secured with two articular and two anterior pins. The saw slot sets the varus-valgus, flexion-extension, and proximal-distal positions of the femoral component. The medial and the lateral distal pins are sequentially removed as the distal cut is made. lternatively, the patient-specific femoral guide can be removed and the conventional distal femoral cutting guide can be placed over the two anterior pins, which allows visual assessment of the thickness of the distal resections before the cuts are made. The thickness of each distal femoral resection is measured with a caliper. The symmetry between the distal resections is assessed using the stepwise algorithm and minor corrections are made when the symmetry is not correct. The chamfer guide from the conventional set of instruments that corresponds to the size of the femoral component determined by preoperative planning is inserted into the two articular pinholes. The chamfer guide sets the internal-external rotation, anterior-posterior, and medial-lateral positions of the femoral component. The two posterior femoral resections are made before the anterior and chamfer cuts, and the thickness of each resection is measured with calipers. The symmetry between the two posterior resections and between the two posterior and two distal resections is assessed using the algorithm, and minor corrections are made when the symmetry is not correct. n intramedullary alignment rod is not used because the wide variability in the longitudinal shape of the femur makes use of the center of the femoral head an unreliable landmark, and because referencing the center of the femoral head kinematically malaligns the knee. 10,11,15 The tibia is exposed by preserving the insertion of the PCL and by removing both menisci. With the tibia dislocated anteromedially, the patient-specific tibial guide is seated on the articular surface and anteromedial cortex of the tibia. The main.indd /3/2011 2:15:21 PM
9 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1263 Saw slot xial view nterior view Lateral view Figure Illustration of the right knee showing axial, anterior, and lateral views of the patient-specific femoral guide on the normal knee model. The saw slot sets the varus-valgus, flexion-extension, and proximal-distal degrees of freedom of the femoral component. The axial view shows two articular pinholes through which pins are drilled to fix the femoral guide. fter making the distal femoral resections, these two holes are used to position the conventional chamfer block, which sets the internal-external rotation, anteriorposterior, and medial-lateral positions of the femoral component. The anterior view shows two pinholes through which pins are drilled to fix the femoral guide. conventional distal femoral cutting guide can be placed over these two pins to make the distal cut for the surgeon who wants to assess the thickness of each distal resection before making the cut. Saw slot xial view nterior view Medial view Figure Illustration of a right knee showing axial, anterior, and medial views of the patient-specific tibial guide on the normal knee model. The saw slot sets the varus-valgus, flexion-extension, and proximal-distal position of the tibial component. The axial view shows two articular pinholes through which pins are drilled to fix the tibial guide. fter making the tibial resection, these two holes are used to align the tibial positioning guide, which sets the internal-external rotation, anterior-posterior, and medial lateral positions of the tibial component. The anterior view shows two pinholes through which pins are drilled to fix the tibial guide. conventional tibial cutting guide can be placed over these two pins for the surgeon who wants to assess the thickness and slope of the tibial resection before making the cut. guide is secured with two articular and two anterior pins (Fig ). The medial and lateral articular pins are sequentially removed as the tibial cut is made. lternatively, the patient-specific tibial guide can be removed and the conventional tibial guide can be placed over the two anterior pins to assess the thickness and slope of the tibial resection before making the cut. The medial-lateral thickness and anteriorposterior slope of the resected portion of the tibia are examined. The thickness of the worn side should be thinner than the unworn side by the amount of wear. fter removing the resected portion of the tibia, the anterior-posterior slope of the proximal tibia should be neutral and conservative, which helps preserve the insertion of the PCL and tibial bone. long-alignment rod is not used to check the varus-valgus orientation of the tibial cut because the wide variability in the longitudinal shape of the tibia makes the use of the center of the ankle an unreliable landmark, and because referencing the center of the ankle kinematically malaligns the knee. 15 The trial reduction is used to assess the range of motion and anterior-posterior and varus-valgus stability at 30-degree intervals, from full extension to flexion. ny loss of motion, instability, or tightness is noted and corrected using the algorithm. Correction of a flexion contracture rarely requires additional resection of distal femur as long as the sequence of removing posterior osteophytes, stripping the posterior capsule from the femur, and ensuring that the tibial cut is neutral and not sloped posteriorly is followed. 24 The sequence of complete removal of medial osteophytes, moving the tibia main.indd /3/2011 2:15:23 PM
10 1264 Section 12 Joint Replacement and Its lternatives medially on the tibial component and removing more medial tibia, 22 and cutting the tibia in 1 to 2 degrees of varus corrects almost all knees with varus deformity and medial tightness without releasing the medial ligaments. The sequence of complete removal of lateral osteophytes (and, if necessary, then recutting the tibia in 1 to 2 degrees of valgus) corrects almost all knees with valgus deformity and lateral tightness without releasing the medial ligaments. 16 The step of ensuring that the tibial cut is neutral and not anteriorly sloped corrects most knees with loss of flexion. The articular pinholes made by drilling through the tibial guide are used to set the internal-external rotation of the tibial component on the tibia. We prefer to use the articular pinholes to set internal-external rotation because of the following factors: (1) medial-lateral location of the tibial tubercle is an inconsistent landmark (ranges 32 to 47 mm from the medial tibia); (2) the range of movement or floating trial technique, which allows the tibial component to orient itself in the best position relative to the femoral component gives widely variable results; and (3) registration of anatomic landmarks with conventional and computer-assisted techniques is not repeatable. 18,23 The tibial template, corresponding to the size of the tibial component, is aligned with the articular pinholes. Small, 1- to 2-mm medial-lateral and anteriorposterior translation adjustments may be required to center the tibia on the tibial component. In the varus knee, moving the tibia medially on the tibial component and removing more medial tibia is effective for restoring coronal alignment and eliminating medial tightness. 22 Unconventional Use of Conventional Instruments In September 2009, the OtisMed patient-specific cutting guides became unavailable in the United States because of a U.S. Food and Drug dministration (FD) classification issue. ccordingly, the senior author (SMH) developed a method to align the knee kinematically using a preoperative rotationally controlled MRI scan and using conventional total knee arthroplasty instruments unconventionally. We term this procedure manual kinematic alignment because the cut planes are selected and assessed manually without using patient-specific cutting guides. Manual kinematic alignment requires preoperative planning to determine the location and amount of cartilage and bone wear on the femur. The thickness of each femoral bone resection is predicted by measuring the amount of cartilage and bone wear in millimeters from a nonorthogonal, oblique, sagittal MRI scan (see Fig ). knee with end-stage varus osteoarthritis typically has 2 mm of distal wear and 1 mm of posterior wear confined to the medial femoral condyle; a knee with end-stage valgus osteoarthritis typically has 2 mm of distal wear and 2 mm of posterior wear confined to the lateral femoral condyle. The surgical technique for manual kinematic alignment is the same as the surgical technique for kinematic alignment with patient-specific guides, regarding exposure, assessing and correcting motion, and addressing tightness and instability. The principle for kinematically aligning the femoral component is to remove the correct amount of bone and cartilage from the distal and posterior femur after accounting for wear and saw blade kerf, so that the total thickness of the missing and removed tissue matches the thickness of the femoral component. The location for the distal femoral cut is selected by manually positioning the conventional femoral guide on the distal surface of the femur, just posterior to the apex of the notch, without using an intramedullary rod (Fig ). The intramedullary rod is not used because it can kinematically malalign the femoral component because of the longitudinal shape of the femur being variable among subjects. 7 The conventional femoral guide is placed flush on the unworn side and pinned, and then the guide is manually raised away from the worn side according to the thickness of the wear (typically, 2 mm) and pinned. The proximal-distal C Figure Photographs of a right knee showing the distal femur with the anterior boundary of the notch marked by blue lines (), the conventional distal femoral guide pinned to the femur posterior to the anterior boundary of the notch (), and the cutting guide attached to the conventional distal femoral guide (C). The conventional femoral guide is placed flush on the unworn side and manually raised away from the worn side according to the thickness of the wear (typically, 2 mm) and pinned. main.indd /3/2011 2:15:26 PM
11 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1265 Figure Photographs of a right knee showing the distal medial resection () and the caliper measurement of the thickness of the resection (). The thickness of each distal femoral resection should be 6.5 ± 1 mm thick after correcting for cartilage wear, bone wear, and saw blade kerf. Figure Photographs of a right knee showing the positioning of the conventional posterior referencing guide set at 0 degrees of rotation () and the caliper measurement of the posteromedial resection (). Each posterior femoral resection should be 6.5 ± 1 mm thick after correcting for cartilage wear, bone wear, and saw blade kerf. Small internal-external rotational adjustments can be made without compromising the fit of the femoral component if the posterior resections are made and measured before making the anterior and chamfer resections. setting on the proximal extension of the conventional femoral guide is set to match the thickness of the femoral component and the cutting block portion is pinned to the anterior surface of the femur. The distal femoral resection is made, and each distal bone resection is measured with calipers (Fig ). The worn side should be 4 to 5 mm thick and the unworn side should be 6 to 7 mm thick when an 8-mm thick femoral component is used. parallel cutting guide is used to adjust the thickness of the distal femoral cut when the difference between the predicted and actual thickness of each distal resection is 2 mm or more. The location for the posterior femoral cut is selected with the conventional posterior referencing guide set at neutral rotation. The conventional posterior referencing guide is placed flush on the unworn side and pinned. The guide is then manually raised away from the worn condyle equal to the amount of wear (typically, 1 to 2 mm) and pinned (Fig ). The chamfer block matching the size of the best-fitting femoral component is placed in the pinholes. The posterior cuts are made before making the anterior and chamfer cuts, and each posterior resection is measured with calipers. The worn side should be 4 to 5 mm thick and the unworn side 6 to 7 mm thick. If the difference between the predicted and actual thickness of each distal resection is 2 mm or more, the internal-external rotation and anterior-posterior positions of the chamfer guide are adjusted to correct the posterior femoral cut. The principle for kinematically aligning the tibial component is to set the tibial cut plane so that the worn side of the main.indd /3/2011 2:15:28 PM
12 1266 Section 12 Joint Replacement and Its lternatives Figure Photographs of a right knee showing the positioning of the conventional tibial cutting guide with an angel wing placed in the slot to assess the proximal-distal and anterior-posterior slopes of the tibial cut (). The plane of the conventional tibial cutting guide is manually positioned so that the proximal-distal location of the tibial cut plane is conservative and the anterior-posterior slope of the tibial cut plane is neutral. The varus-valgus orientation of the tibial cut plane is adjusted until the worn side of the resected portion of the tibia is thinner than the unworn side by the amount of wear., The conservative tibial resection shows that more anterior bone is removed than posterior bone, which places the tibial component in neutral slope and preserves the insertion of the posterior cruciate ligament. resected portion of the tibia is thinner than the unworn side by the amount of wear, and the anterior-posterior slope is neutral and conservative, which helps preserve the insertion of the posterior cruciate ligament. n angel wing is placed in the slot of the conventional tibial cutting guide (Fig ). The plane of the conventional tibial cutting guide is manually positioned so that the proximal-distal location of the tibial cut plane is conservative and the anterior-posterior slope of the tibial cut plane is neutral. One pin is placed in the conventional tibial cutting guide, which sets the proximaldistal and anterior-posterior slopes. The varus-valgus orientation of the tibial cut plane is adjusted by rotating the conventional tibial cutting guide until the worn side of the resected portion of the tibia is thinner than the unworn side by the amount of wear. The conventional tibial cutting guide is pinned to the tibia and the tibial cut is made. longalignment rod is not used to check the varus-valgus orientation of the tibial cut because the wide variability in the longitudinal shape of the tibia makes the use of the center of the ankle an unreliable landmark, and because referencing the center of the ankle kinematically malaligns the knee. 7 The alignment of the limb is visually inspected during the trial reduction and varus-valgus adjustments of the tibial resection are made if the limb appears malaligned. Theoretical Concerns One theoretical concern is whether the hip-knee-ankle axis of the kinematically aligned TK is different from a TK mechanically aligned with conventional and computerassisted instrumentation. source of this concern was a pilot study, in September 2006, of four knees treated with patientspecific cutting guides at the request of an implant company to evaluate the first-time use of their knee component before commercial release. The authors of this pilot study suggested that kinematically aligned knees were malaligned in the coronal plane. 20 lthough the primary goal of kinematic alignment is to restore knee kinematics and not to restore a neutral or 0-degree hip-knee-ankle axis, two other studies have shown that kinematic alignment does not malalign the limb in the coronal plane, as suggested by Klatt and associates 20 in their study of four subjects. 16 One level III study, consisting of 21 subjects, found an average hip-knee-ankle axis of 1.2 degree varus, 25 which was closer to the 0-degree mechanical axis and had less fewer outliers outside the range of 0 ± 3 degrees than many previously reported results using conventional and computer-assisted techniques. 25 second level III study, consisting of 48 subjects, found an average hip-knee-ankle axis of 1.4 degrees valgus, which is within the range of 0 ± 3 degrees. level I prospective, double-blinded, randomized clinical trial is underway to further clarify the differences in limb alignment between the kinematically aligned knee with patient-specific cutting guides and mechanical alignment with conventional instruments. 8 However, on the basis of these level III studies, the hip-knee-ankle axis of the kinematically aligned TK is similar to that of conventional and computer-assisted techniques. lthough there is a widely held opinion that a neutral hip-knee-ankle axis will result in better TK survivorship, the mid- or long-term scientific support for this contention is surprisingly weak. Every study that has been considered evidence to support this contention is limited for various reasons. Six of seven published studies used short-leg radiographs, which cannot accurately assess the hip-knee-ankle axis. 15,27 In the one study that used long-leg radiographs, a rudimentary implant design consisted of a noncondylar roller and trough design that was implanted with primitive instrumentation (Denham Knee). 2,23a recent study of the survivorship of a modern implant design with better instrumentation in 395 knees has shown that factors other than the mechanical axis are more important for determining survivorship at 15 years, which suggests that the surgical goal of restoring a 0-degree hip-knee-ankle axis should be revisited. The study indicated that the group with a hip-knee-ankle axis outside the range of 0 ± 3 degrees, which consisted of 25% of the knees, had a threefold better survivorship at 15 years than the group with a hip-knee-ankle axis inside the range of 0 ± 3 degrees, which consisted of 75% of the knees, a finding that starkly contrasts with the study of the Denham main.indd /3/2011 2:15:29 PM
13 Chapter 121 Kinematic lignment in Total Knee rthroplasty 1267 Knee. 2 The better survivorship of so-called outliers, with modern implant design and modern instrumentation, might be the result of better balancing of the knee and restoration of normal kinematics. Studies have shown that release of the collateral ligaments is not needed with kinematic alignment, 17,25 which may explain why kinematic alignment restores more normal contact kinematics than mechanical alignment, with the potential for better mid- and long-term survivorship. 13 second theoretical concern is whether the process of kinematic alignment that begins with performing MRI of the knee and ends with surgical implantation of the components consistently aligns the knee kinematically. There are many sources of error in the process, including the quality of the MRI image (i.e., proper biplanar alignment, high signalto-noise ratio, no motion artifact), generation of the arthritic and normal knee models, shape fitting of the components, manufacturing the patient-specific cutting guides, and the surgeon using the guides in the operating room. lthough some studies have shown that the process is reliable, 16,17,25 we believe that there is still a need to follow the algorithm intraoperatively to verify that the actual and predicted thickness of each bone resection is correct and, when necessary, to make adjustments in component position before cementing. Early Clinical enefits s of December 2009, the clinical experience with kinematic alignment spanned 4 years and comprised 23,000 knees, which is sufficient to determine whether there are any early clinical benefits or failures associated with kinematic alignment. We have prospectively used a handheld computer (OrthoSight, Conshohocken, Pa; to eliminate interviewer bias that patients self-administer to respond to a survey of queries consisting of custom questions, Oxford score, Short Form Health Survey (12 items; SF-12), and Knee Society score. Patients spend an average of 8 to 10 minutes preoperatively and postoperatively filling out the survey in the waiting room, which has improved our office efficiency. The handheld computer is used intraoperatively to record operative time, ligament releases, bone recuts, guide fit, and whether the implanted component matches the size of the planned component. 16,17 The perioperative data suggest that kinematic alignment may lessen the surgical stress experienced by the patient, shorten the recovery time, and increase the rate of return to DLs. The average operative duration of 53 minutes is less than the average reported operative times for conventional (73 minutes) and computer-assisted (90 minutes) approaches. 16,25,26 Currently, our average operative duration is 30 minutes with patient-specific cutting guides and 36 minutes with the unconventional use of conventional instruments. Transfusions are infrequent, which is attributed to not releasing collateral and retinacular soft tissue releases. Fat emboli have not occurred because intramedullary rods are not used with either kinematic alignment technique. The hospital stay of 2 nights is short, with 98% of patients discharged to home rather than to a rehabilitation facility. t 4 to 5 weeks postoperatively, 80% of patients walk without a cane, 54% drive a car, 88% notice that their knee functions better than before surgery, 94% judge the treated knee as normal or almost normal, and 98% judge the alignment of their limb as just right. In terms of patient response to standardized questionnaires, by 4 to 5 weeks patients experience less pain than before surgery and show significant improvements in 11 of 12 activities evaluated by the Oxford score, SF-12 physical score, knee function score, and Knee Society score. 17 level I prospective, double-blinded, randomized clinical trial is underway to clarify further the differences in early recovery between the kinematically aligned knee with patient-specific cutting guides and mechanical alignment with conventional instruments. 8 Summary The primary goals of this chapter were to stimulate debate and advance the understanding of kinematic alignment of TK. Kinematic alignment offers a much-needed alternative to mechanical alignment because mechanical alignment with conventional and computer-assisted techniques has a prevalence of patient dissatisfaction (20%) because of continued pain and poor function in DLs. Kinematic alignment does not malalign the hip-knee-ankle axis. The early success of the kinematically aligned TK (OtisKnee) has been recognized by the implant manufacturing industry. Most major implant manufacturers have since developed patient-specific cutting guides, but these guides align the limb mechanically and do not align the knee kinematically. s of the end of 2009, the available patient-specific cutting guides that mechanically align the limb are Signature (iomet, Warsaw Ind), Visionaire (Smith & Nephew, Memphis, Tenn), Prophecy (Wright Medical Technology, rlington, Tenn), and Tru Match (DePuy Orthopaedics, Warsaw, Ind). We have recognized that there is a need for level I studies to clarify differences in limb alignment and early recovery between the kinematically aligned knee with patient-specific cutting guides and mechanical alignment with conventional and computer-assisted instruments, and we await the publication of the registered level I study that is currently underway. 8 We also want to emphasize that level I studies are also needed to determine whether patient-specific cutting guides that mechanically align the limb improve on the high prevalence of patient dissatisfaction with mechanically aligned TKs implanted with conventional and computer-assisted instruments. Key References lden KJ, Pagnano MW: Computer-assisted surgery: a wine before its time. Orthopedics 31: , aker PN, van der Meulen JH, Lewsey J, Gregg PJ: The role of pain and function in determining patient satisfaction after total knee replacement. Data from the National Joint Registry for England and Wales. J one Joint Surg r 89: , Coughlin KM, Incavo SJ, Churchill DL, eynnon D: Tibial axis and patellar position relative to the femoral epicondylar axis during squatting. J rthroplasty 18: , Dossett GH: Total knee replacement study using standard cutting guide vs. Otismed MRI generated cutting guide, Phoenix, riz, 2010, Department of Veterans ffairs. Eckhoff D, Hogan C, DiMatteo L, et al: Difference between the epicondylar and cylindrical axis of the knee. Clin Orthop Relat Res 461: , Eckhoff DG, ach JM, Spitzer VM, et al: Three-dimensional mechanics, kinematics, and morphology of the knee viewed in virtual reality. J one Joint Surg m 87(Suppl 2):71 80, main.indd /3/2011 2:15:29 PM
14 1268 Section 12 Joint Replacement and Its lternatives Hollister M, Jatana S, Singh K, et al: The axes of rotation of the knee. Clin Orthop Relat Res 290: , Howell SM, Hodapp EE, Kuznik K, Hull ML: In vivo adduction and reverse axial rotation (external) of the tibial component can be minimized. Orthopedics 32:319, Howell SM, Howell SJ, Hull ML: ssessment of the radii of the medial and lateral femoral condyles in varus and valgus knees with osteoarthritis. J one Joint Surg m 92:98 104, Howell SM, Kuznik K, Hull ML, Siston R: Results of an initial experience with custom-fit positioning total knee arthroplasty in a series of 48 patients. Orthopedics 31: , Howell SM, Kuznik K, Hull ML, Siston R: Longitudinal shapes of the tibia and femur are unrelated and variable. Clin Orthop Relat Res 468: , Howell SM, Rogers SL: Method for quantifying patient expectations and early recovery after total knee arthroplasty. Orthopedics 32: , Matziolis G, Krocker D, Weiss U, et al: prospective, randomized study of computer-assisted and conventional total knee arthroplasty. Threedimensional evaluation of implant alignment and rotation. J one Joint Surg m 89: , Smith C, Chen J, Howell SM, Hull ML: n in vivo study of the effect of distal femoral resection on passive knee extension. J rthroplasty 25: , Spencer, Mont M, McGrath MS, et al: Initial experience with customfit total knee replacement: intra-operative events and long-leg coronal alignment. Int Orthop 33: , Full references for this chapter can be found on main.indd /3/2011 2:15:29 PM
15 Chapter 121 Kinematic lignment in Total Knee rthroplasty e121-1 References 1. kagi M, Oh M, Nonaka T, et al: n anteroposterior axis of the tibia for total knee arthroplasty. Clin Orthop Relat Res 420: , lden KJ, Pagnano MW: Computer-assisted surgery: a wine before its time. Orthopedics 31: , aker PN, van der Meulen JH, Lewsey J, Gregg PJ: The role of pain and function in determining patient satisfaction after total knee replacement. Data from the National Joint Registry for England and Wales. J one Joint Surg r 89: , arrack RL, Schrader T, ertot J, et al: Component rotation and anterior knee pain after total knee arthroplasty. Clin Orthop Relat Res 392:46 55, ourne R, Chesworth M, Davis M, et al: Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 468:57 63, urnett RS, oone JL, Rosenzweig SD, et al: Patellar resurfacing compared with nonresurfacing in total knee arthroplasty. concise follow-up of a randomized trial. J one Joint Surg m 91: , Coughlin KM, Incavo SJ, Churchill DL, eynnon D: Tibial axis and patellar position relative to the femoral epicondylar axis during squatting. J rthroplasty 18: , Dossett GH: Total knee replacement study using standard cutting guide vs. Otismed MRI generated cutting guide, Phoenix, riz, 2010, Department of Veterans ffairs. 9. Dutton, Yeo SJ, Yang KY, et al: Computer-assisted minimally invasive total knee arthroplasty compared with standard total knee arthroplasty. prospective, randomized study. J one Joint Surg m 90:2 9, Eckhoff DG, ach JM, Spitzer VM, et al: Three-dimensional mechanics, kinematics, and morphology of the knee viewed in virtual reality. J one Joint Surg m 87(Suppl 2):71 80, Eckhoff D, Hogan C, DiMatteo L, et al: Difference between the epicondylar and cylindrical axis of the knee. Clin Orthop Relat Res 461: , Hollister M, Jatana S, Singh K, et al: The axes of rotation of the knee. Clin Orthop Relat Res 290: , Howell SM, Hodapp EE, Kuznik K, Hull ML: In vivo adduction and reverse axial rotation (external) of the tibial component can be minimized. Orthopedics 32:319, Howell SM, Howell SJ, Hull ML: ssessment of the radii of the medial and lateral femoral condyles in varus and valgus knees with osteoarthritis. J one Joint Surg m 92:98 104, Howell SM, Kuznik K, Hull ML, Siston R: Longitudinal shapes of the tibia and femur are unrelated and variable. Clin Orthop Relat Res 468: , Howell SM, Kuznik K, Hull ML, Siston R: Results of an initial experience with custom-fit positioning total knee arthroplasty in a series of 48 patients. Orthopedics 31: , Howell SM, Rogers SL: Method for quantifying patient expectations and early recovery after total knee arthroplasty. Orthopedics 32: , Ikeuchi M, Yamanaka N, Okanoue Y, et al: Determining the rotational alignment of the tibial component at total knee replacement: a comparison of two techniques. J one Joint Surg r 89:45 49, Jeffery RS, Morris RW, Denham R: Coronal alignment after total knee replacement. J one Joint Surg r 73: , Klatt, Goyal N, ustin MS, Hozack WJ: Custom-fit total knee arthroplasty (OtisKnee) results in malalignment. J rthroplasty 23:26 29, Matziolis G, Krocker D, Weiss U, et al: prospective, randomized study of computer-assisted and conventional total knee arthroplasty. Threedimensional evaluation of implant alignment and rotation. J one Joint Surg m 89: , Mihalko WM, Saleh KJ, Krackow K, Whiteside L: Soft tissue balancing during total knee arthroplasty in the varus knee. J m cad Orthop Surg 17: , Siston R, Goodman S, Patel JJ, et al: The high variability of tibial rotational alignment in total knee arthroplasty. Clin Orthop Relat Res 452:65 69, a. Parratte S, Pagnano MW, Trousdale RT, et al: Effect of postoperative mechanical axis alignment on the fifteen-year survival of modern, cemented total knee replacements. J one Joint Surg 92(12):2143, Smith C, Chen J, Howell SM, Hull ML: n in vivo study of the effect of distal femoral resection on passive knee extension. J rthroplasty 25: , Spencer, Mont M, McGrath MS, et al: Initial experience with custom-fit total knee replacement: intra-operative events and long-leg coronal alignment. Int Orthop 33: , Stulberg SD, Yaffe M, Koo SS: Computer-assisted surgery versus manual total knee arthroplasty: a case-controlled study. J one Joint Surg m 88(Suppl 4):47 54, van Raaij TM, rouwer RW, Reijman M, et al: Conventional knee films hamper accurate knee alignment determination in patients with varus osteoarthritis of the knee. Knee 16: , main.indd 1 8/3/2011 2:15:29 PM
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
NEXGEN COMPLETE KNEE SOLUTION. Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees
 NEXGEN COMPLETE KNEE SOLUTION Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees INTRODUCTION Successful total knee arthroplasty is directly dependent on reestablishment
NEXGEN COMPLETE KNEE SOLUTION Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees INTRODUCTION Successful total knee arthroplasty is directly dependent on reestablishment
Kinematic Alignment in Total Knee Arthroplasty
 Kinematic Alignment in Total Knee Arthroplasty Definition, History, Principle, Surgical Technique, and Results of an Alignment Option for TKA Stephen M Howell, MD 1,2 Joshua D Roth, BS 1 Maury L Hull,
Kinematic Alignment in Total Knee Arthroplasty Definition, History, Principle, Surgical Technique, and Results of an Alignment Option for TKA Stephen M Howell, MD 1,2 Joshua D Roth, BS 1 Maury L Hull,
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique
 Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer NexGen CR-Flex and LPS-Flex Knees. Surgical Technique with Posterior Referencing Instrumentation
 Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation INTRO Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation
Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation INTRO Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation
Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique
 Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique
 NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique For the NexGen Cruciate Retaining & Legacy Posterior Stabilized Knee INTRODUCTION Successful total knee arthroplasty is directly
NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique For the NexGen Cruciate Retaining & Legacy Posterior Stabilized Knee INTRODUCTION Successful total knee arthroplasty is directly
Scorpio NRG CR & PS. Single Radius Primary Knee System Surgical Protocol. Anterior Referencing
 Scorpio NRG CR & PS Single Radius Primary Knee System Surgical Protocol AR Anterior Referencing This document is intended to be used by healthcare professionals only. Scorpio NRG AR Single Radius Primary
Scorpio NRG CR & PS Single Radius Primary Knee System Surgical Protocol AR Anterior Referencing This document is intended to be used by healthcare professionals only. Scorpio NRG AR Single Radius Primary
High-Flex Solutions for the MIS Era. Zimmer Unicompartmental High Flex Knee System
 High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
Simplified surgery. Personalized performance.
 Simplified surgery. Personalized performance. VISIONAIRE Patient Matched Technology Accuracy Advanced surgical precision, resulting in reproducible outcomes Efficiency Simplifying surgery, reducing costs,
Simplified surgery. Personalized performance. VISIONAIRE Patient Matched Technology Accuracy Advanced surgical precision, resulting in reproducible outcomes Efficiency Simplifying surgery, reducing costs,
Zimmer NexGen LCCK. Surgical Technique for use with LCCK 4-in-1 Instrumentation. Contact your Zimmer representative or visit us at www.zimmer.
 Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System family of knee implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System family of knee implants with the INTUITION Instrumentation.
Trabecular Metal Femoral Component. Surgical Technique
 Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
PRIMARY KNEE SYSTEM SIGMA SURGICAL TECHNIQUE. Balanced Surgical Technique INSTRUMENTS
 SIGMA PRIMARY KNEE SYSTEM Balanced Surgical Technique SURGICAL TECHNIQUE INSTRUMENTS Contemporary total knee arthoplasty demands high performance instrumentation that provides enhanced efficiency, precision
SIGMA PRIMARY KNEE SYSTEM Balanced Surgical Technique SURGICAL TECHNIQUE INSTRUMENTS Contemporary total knee arthoplasty demands high performance instrumentation that provides enhanced efficiency, precision
Rotational alignment of the femoral component in total knee arthroplasty
 Review Article on Primary Total Knee Arthroplasty Page 1 of 9 Rotational alignment of the femoral component in total knee arthroplasty Claudio Carlo Castelli, Daniele Antonio Falvo, Mario Luigi Iapicca,
Review Article on Primary Total Knee Arthroplasty Page 1 of 9 Rotational alignment of the femoral component in total knee arthroplasty Claudio Carlo Castelli, Daniele Antonio Falvo, Mario Luigi Iapicca,
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Patellofemoral Chondrosis
 Patellofemoral Chondrosis What is PF chondrosis? PF chondrosis (cartilage deterioration) is the softening or loss of smooth cartilage, most frequently that which covers the back of the kneecap, but the
Patellofemoral Chondrosis What is PF chondrosis? PF chondrosis (cartilage deterioration) is the softening or loss of smooth cartilage, most frequently that which covers the back of the kneecap, but the
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
ROTATING PLATFORM TOTAL KNEE REPLACEMENT BRIGHAM AND WOMEN S HOSPITAL, BOSTON, MA Broadcast May 20, 2004
 NARRATOR ROTATING PLATFORM TOTAL KNEE REPLACEMENT BRIGHAM AND WOMEN S HOSPITAL, BOSTON, MA Broadcast May 20, 2004 Thank you for joining us from Brigham and Women s Hospital in Boston, MA, to view the minimally
NARRATOR ROTATING PLATFORM TOTAL KNEE REPLACEMENT BRIGHAM AND WOMEN S HOSPITAL, BOSTON, MA Broadcast May 20, 2004 Thank you for joining us from Brigham and Women s Hospital in Boston, MA, to view the minimally
iassist Knee Surgical Technique 2-Pod Version Instruments
 iassist Knee Surgical Technique 2-Pod Version Instruments Table of Contents Page 1. Overview 4 1.1 Indication for Use 4 1.2 Training 4 1.3 Implant Indications 4 1.4 Contraindications 4 1.5 Complications
iassist Knee Surgical Technique 2-Pod Version Instruments Table of Contents Page 1. Overview 4 1.1 Indication for Use 4 1.2 Training 4 1.3 Implant Indications 4 1.4 Contraindications 4 1.5 Complications
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Zimmer MOST Options System
 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
DRAFT. Triathlon TS Knee System. Surgical Protocol. Version 1
 DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
METAL HEMI. Great Toe Implant SURGICAL TECHNIQUE
 METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
The patellofemoral joint and the total knee replacement
 Applied and Computational Mechanics 1 (2007) The patellofemoral joint and the total knee replacement J. Pokorný a,, J. Křen a a Faculty of AppliedSciences, UWB inpilsen, Univerzitní 22, 306 14Plzeň, CzechRepublic
Applied and Computational Mechanics 1 (2007) The patellofemoral joint and the total knee replacement J. Pokorný a,, J. Křen a a Faculty of AppliedSciences, UWB inpilsen, Univerzitní 22, 306 14Plzeň, CzechRepublic
Zimmer Persona Adverse Events Reported to FDA Through 3/27/2015
 Event Description: IT IS REPORTED THAT THE PATIENT WAS REVISED DUE TO GROSS ASEPTIC LOOSENING. Manufacturer 1822565-2015- 00224 PERSONA STEMMED CEMENTED TIBIAL COMPONENT 2/23/15 1/21/15 Injury Narrative:
Event Description: IT IS REPORTED THAT THE PATIENT WAS REVISED DUE TO GROSS ASEPTIC LOOSENING. Manufacturer 1822565-2015- 00224 PERSONA STEMMED CEMENTED TIBIAL COMPONENT 2/23/15 1/21/15 Injury Narrative:
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM
 INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic Procedures
 Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: computer_assisted_surgical_navigational_orthopedic_procedures
Corporate Medical Policy Computer Assisted Surgical Navigational Orthopedic File Name: Origination: Last CAP Review: Next CAP Review: Last Review: computer_assisted_surgical_navigational_orthopedic_procedures
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Michael Ries, MD Chief of Arthroplasty UCSF Medical Center San Francisco, CA. Jan Victor, MD Orthopaedic Department AZ Sint-Lucas Brugge, Belgium
 Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Fred D Cushner, MD Insall Scott Kelly Institute for
Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Fred D Cushner, MD Insall Scott Kelly Institute for
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
The Knee: Problems and Solutions
 The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
Exeter X3 RimFit. Acetabular Cup Surgical Protocol
 Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Zimmer M/L Taper Hip Prosthesis. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
S-ROM NOILES. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
 S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
Malrotation Causing Patellofemoral Complications After Total Knee Arthroplasty
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 356, pp 144-153 1998 Lippincott Williams 8 Wilkins Malrotation Causing Patellofemoral Complications After Total Knee Arthroplasty R.A. Berger, MD *; L.S.
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 356, pp 144-153 1998 Lippincott Williams 8 Wilkins Malrotation Causing Patellofemoral Complications After Total Knee Arthroplasty R.A. Berger, MD *; L.S.
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Surgical Technique and Reference Guide
 Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
Goals. Our Real Goals. Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas. Perform a basic, logical, history and physical exam
 Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Know-how brings motion back to life. SM. Solution UC-PLUS. Unicompartmental Knee Prosthesis. Surgical Technique
 Know-how brings motion back to life. SM TM UC-PLUS Solution Unicompartmental Knee Prosthesis Surgical Technique Table of Contents 1 Introduction 3 2 Characteristics and Advantages of the System 4 3 Indications
Know-how brings motion back to life. SM TM UC-PLUS Solution Unicompartmental Knee Prosthesis Surgical Technique Table of Contents 1 Introduction 3 2 Characteristics and Advantages of the System 4 3 Indications
Post Surgical Care of Patella Luxation Repair
 Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Sports Radiology : Making a diagnosis or solving a problem
 Sports Radiology : Making a diagnosis or solving a problem Professor Dr John George University of Malaya Research Imaging Centre University of Malaya Medical Centre Kuala Lumpur, Malaysia. Abstract: Aim:
Sports Radiology : Making a diagnosis or solving a problem Professor Dr John George University of Malaya Research Imaging Centre University of Malaya Medical Centre Kuala Lumpur, Malaysia. Abstract: Aim:
THE MEASUREMENT AND ANALYSIS OF AXIAL DEFORMITY AT THE KNEE
 THE MEASUREMENT AND ANALYSIS OF AXIAL DEFORMITY AT THE KNEE Kenneth A. Krackow, M.D. Clinical Director, Department of Orthopaedic Surgery Kaleida Health System Buffalo General Hospital Professor and Full
THE MEASUREMENT AND ANALYSIS OF AXIAL DEFORMITY AT THE KNEE Kenneth A. Krackow, M.D. Clinical Director, Department of Orthopaedic Surgery Kaleida Health System Buffalo General Hospital Professor and Full
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Musculoskeletal MRI Technical Considerations
 Musculoskeletal MRI Technical Considerations Garry E. Gold, M.D. Professor of Radiology, Bioengineering and Orthopaedic Surgery Stanford University Outline Joint Structure Image Contrast Protocols: 3.0T
Musculoskeletal MRI Technical Considerations Garry E. Gold, M.D. Professor of Radiology, Bioengineering and Orthopaedic Surgery Stanford University Outline Joint Structure Image Contrast Protocols: 3.0T
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
DIAGNOSING SCAPHOID FRACTURES. Anthony Hewitt
 DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Patellofemoral Joint: Superior Glide of the Patella
 Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Biomechanics of Knee Replacement. Ryan Keyfitz Rohinton Richard
 Biomechanics of Knee Replacement Ryan Keyfitz Rohinton Richard Biomechanics of the Knee Knee Joint Provide mobility Provide stability to the lower extremity Allow flexion and rotation 2 Anatomy of the
Biomechanics of Knee Replacement Ryan Keyfitz Rohinton Richard Biomechanics of the Knee Knee Joint Provide mobility Provide stability to the lower extremity Allow flexion and rotation 2 Anatomy of the
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Twelve. Figure 12.1: 3D Curved MPR Viewer Window
 Twelve The 3D Curved MPR Viewer This Chapter describes how to visualize and reformat a 3D dataset in a Curved MPR plane: Curved Planar Reformation (CPR). The 3D Curved MPR Viewer is a window opened from
Twelve The 3D Curved MPR Viewer This Chapter describes how to visualize and reformat a 3D dataset in a Curved MPR plane: Curved Planar Reformation (CPR). The 3D Curved MPR Viewer is a window opened from
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
OptiLock Periarticular Plating System For Proximal Tibial Fractures. Pre-Launch Surgical Technique
 OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
How To Perform An Elbow Operation
 Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report KNEE INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Knee Injury Cases The Petrylaw Lawsuits Settlements and Injury
The Petrylaw Lawsuits Settlements and Injury Settlement Report KNEE INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Knee Injury Cases The Petrylaw Lawsuits Settlements and Injury
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
This week. CENG 732 Computer Animation. Challenges in Human Modeling. Basic Arm Model
 CENG 732 Computer Animation Spring 2006-2007 Week 8 Modeling and Animating Articulated Figures: Modeling the Arm, Walking, Facial Animation This week Modeling the arm Different joint structures Walking
CENG 732 Computer Animation Spring 2006-2007 Week 8 Modeling and Animating Articulated Figures: Modeling the Arm, Walking, Facial Animation This week Modeling the arm Different joint structures Walking
Technique Guide. VersiTomic. Michael A. Rauh, MD. Anterior Cruciate Ligament Reconstruction
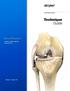 Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Affected Product: Polyethylene Implants from Gender Solutions Natural-Knee Flex, Natural-Knee, Natural-Knee II, MOST Options, and Apollo Systems
 March 19, 2014 To: Surgeons Subject: URGENT MEDICAL DEVICE RECALL NOTIFICATION Zimmer reference: 1822565-02-07-2014-001-R Affected Product: Polyethylene Implants from Gender Solutions Natural-Knee Flex,
March 19, 2014 To: Surgeons Subject: URGENT MEDICAL DEVICE RECALL NOTIFICATION Zimmer reference: 1822565-02-07-2014-001-R Affected Product: Polyethylene Implants from Gender Solutions Natural-Knee Flex,
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Zimmer Gender Solutions NexGen High-Flex Implants
 Zimmer Gender Solutions NexGen High-Flex Implants Because Women and Men are Different Something new is taking shape It s all about shape. Women and men are different. That s not news to the medical establishment.
Zimmer Gender Solutions NexGen High-Flex Implants Because Women and Men are Different Something new is taking shape It s all about shape. Women and men are different. That s not news to the medical establishment.
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Evaluating Knee Pain
 Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
How To Treat A Patella Dislocation
 Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Total Hip Joint Replacement. A Patient s Guide
 Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Terminology of Human Walking From North American Society for Gait and Human Movement 1993 and AAOP Gait Society 1994
 Gait Cycle: The period of time from one event (usually initial contact) of one foot to the following occurrence of the same event with the same foot. Abbreviated GC. Gait Stride: The distance from initial
Gait Cycle: The period of time from one event (usually initial contact) of one foot to the following occurrence of the same event with the same foot. Abbreviated GC. Gait Stride: The distance from initial
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
Configuration and Use of the MR Knee Dot Engine
 Configuration and Use of the MR Knee Dot Engine Kai Reiter (RT); Sebastian Auer (RT) Radiology Herne, Herne, Germany 1 42 MAGNETOM Flash 3/2011 www.siemens.com/magnetom-world We are a radiological joint
Configuration and Use of the MR Knee Dot Engine Kai Reiter (RT); Sebastian Auer (RT) Radiology Herne, Herne, Germany 1 42 MAGNETOM Flash 3/2011 www.siemens.com/magnetom-world We are a radiological joint
INFORMATION SOCIETIES TECHNOLOGY (IST) PROGRAMME
 INFORMATION SOCIETIES TECHNOLOGY (IST) PROGRAMME Project Number IST-1999-10954 Project Title: Virtual Animation of the Kinematics of the Human for Industrial, Educational and Research Purposes Title of
INFORMATION SOCIETIES TECHNOLOGY (IST) PROGRAMME Project Number IST-1999-10954 Project Title: Virtual Animation of the Kinematics of the Human for Industrial, Educational and Research Purposes Title of
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty
 Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts
 Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts Advancing ACL Reconstruction with implant absorption and ossification of the Implant site 2,3,5 The MILAGRO BR Interference Screw
Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts Advancing ACL Reconstruction with implant absorption and ossification of the Implant site 2,3,5 The MILAGRO BR Interference Screw
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE
 TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so
TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System
 Knee Series Technique Guide ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System Stuart Fromm, M.D. As described by: Stuart Fromm, M.D. Black Hills Orthopedic
Knee Series Technique Guide ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System Stuart Fromm, M.D. As described by: Stuart Fromm, M.D. Black Hills Orthopedic
External Fixation Systems IMPORTANT MEDICAL INFORMATION
 External Fixation Systems IMPORTANT MEDICAL INFORMATION EN SPECIAL NOTE External fixation should be used only under the directions of physicians who have a thorough knowledge of the anatomy, physiology
External Fixation Systems IMPORTANT MEDICAL INFORMATION EN SPECIAL NOTE External fixation should be used only under the directions of physicians who have a thorough knowledge of the anatomy, physiology
Surgical procedure. METS Modular Distal Femur
 Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
