Quad/Patella Tendon Repair
|
|
|
- Kellie Dickerson
- 9 years ago
- Views:
Transcription
1 Quad/Patella Tendon Repair Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap) and the groove of cartilage on the femur in which it sits. The purpose of the patella and the patellofemoral joint is to allow for greater force development through the quadriceps muscle by creating a fulcrum mechanism as the knee is extended (straightened). Normally the knee cap slides up and down following the track of the groove in the middle of the femur. This joint is subject to tremendous forces when the knee is repetitively loaded in flexion and extension during sports and physical activity. The Quadriceps muscle is anchored to the patella via the Quadriceps tendon. The patella, in turn is anchored to the shin bone via the patellar tendon (see picture above). When the tensile load through the tendon is greater than the tissue can bear it will tear. These tears often come in the form of one single traumatic event, but the the events leading up to the tear may be a culmination of a series of actions (repetitive microtrauma), or a medical predisposition for breakdown. Typically, a strong force such as an explosive jump, is required to rupture the tendon. However, with a history of chronic tendon inflammation (tendinitis), the tendon may be weakened and could tear with less force. Some medical conditions can also weaken the tendons and make a tear more likely. These include, but are not limited to: aging and degenerative changes, diabetes, kidney disease, and rheumatoid arthritis. Regardless, when the Patellar or Quadriceps tendon tears there is often a tearing or popping sensation, followed by pain and swelling. Additional symptoms include: An indentation above or below the patella where the tendon is torn Bruising Tenderness Muscle cramping The kneecap may move up into the thigh because it is no longer anchored Inability to straighten the knee Knee buckling or giving way Treatment Options The severity, and resulting dysfunction, of Patella/Quadriceps tendon tears, varies greatly. In each case the physician and his or her staff evaluates the individual case and determines the best plan of care for each patient. A period of rest and modified activity, including the use of knee brace for 3 6 weeks, may be enough to =A00512 Page 1
2 manage some cases (usually minor partial tears). Use of anti inflammatory medication and ice may also be recommended. The physician and his or her staff may also ask the patient to undergo a course of physical therapy to address the underlying mechanical causes of patella femoral joint stress. In most cases surgery is required to reattach the torn tendon to its attachment point =A Surgery Surgical repair reattaches the torn tendon to the bone. Patients who require surgery often do better if the repair is performed early after the injury. Early repair may prevent the tendon from scarring and retracting in a shortened position. The surgical technique and specific procedure can vary from case to case. The goal of the procedure is always to restore the correct tension and positioning of the patella so that the fulcrum mechanism can be maintained. The most common complications of patellar tendon repair include weakness and loss of motion. Your doctor will likely require you to have physical therapy, so as to minimize loss of strength and mobility. In most cases a full return to pre injury activity levels is expected. Recovery/Time off Work Recovering from Patellar/Quadriceps tendon repair surgery is not easy. It is very important that the patient knows the recovery process is difficult and time consuming. He or she must be an active participant during this process, performing daily exercises to ensure there is proper return of range of motion and strength. There is a large amount of variability in the time it takes to fully recover from this procedure. It is usually estimated that it will take at least 6 months for the patient to feel as though he or she has completely returned to a pre injury level of activity. Some cases may take as long as a year to make a full recovery. People with desk jobs should plan to take at least 1 week off from work. Manual laborers will likely be out of work for at least 4 6 months. Recovery is different in each case. Your individual time table for return to activities and work will be discussed by your surgeon during post operative office visits. Hospital Stay/Post Operative Visits After having surgery to repair the Patellar/Quadriceps tendon you may be required to stay in the hospital for a few days. You will be discharged home as soon as it is safe for you to be so. Your first post op visit to the doctor s office will be approximately two weeks after the operation. At this visit your stitches will be removed and you will review the procedure with the surgeon or his/her assistant. At this time you will most likely be cleared to make an appointment to begin Physical Therapy. Your surgeon will determine the frequency of subsequent follow up visits. Page 2
3 At Home You should replace your post op dressing daily and inspect your incision for signs of infection. If you have staples closing your incision they will likely be scheduled to be removed around two weeks after the operation. If your surgeon used stitches to close the wound do not remove the strips of tape (steristrips) that are across your incision. Allow them to fall off on their own or to be removed at your doctor s office visit. Medication Your surgeon will prescribe pain medicine for you after the operation. Please call the doctor s office if you have any questions regarding medication. Ice You must use ice on your knee after the operation for management of pain and swelling. Ice should be applied 3 5 times a day for minutes at a time. Always maintain one layer of protection between ice and the skin. Putting a pillow case or towel over your ice pack works well for this. Walking It is very important for you to use crutches (or a walker) after the surgery. Putting too much weight on your knee in the early phases of recovery can create excessive and persistent swelling, poor gait mechanics and may cause undue stress on the healing repair. You will be instructed on how much weight you can bear on your leg while using your crutches (walker) right away after surgery. With your doctor s permission your therapist will instruct you on how to safely wean from using your crutches (walker) after 2 weeks post op. Brace After surgery your doctor will require you to wear a hinged knee brace. If your doctor has specific instructions regarding the use of this brace then he or she will go over them with you and your family after the operation, or at your first post operative appointment. Generally, it is recommended that you keep the brace locked in extension while walking at all times. The doctor will inform you when you may walk with the brace unlocked. You may be allowed to unlock the brace to allow some bending when sitting. Your doctor will tell you exactly how much you are allowed to bend your knee after the operation. Generally, patients are not allowed to bend the knee past 90 degrees for the first six weeks after surgery. You will need to use this knee brace for at least six weeks after the operation. Driving After surgery you will not be allowed to drive as long as you are taking narcotic pain medicine. If you had surgery on your left leg you may drive an automatic transmission car, if your doctor allows you, as soon as you are no longer taking narcotics. If you had surgery on your right leg your doctor will let you know when you are clear to drive. Driving is generally not permitted when your leg is weak enough that you still need to use the post operative brace. Page 3
4 Rehabilitation **The following is an outlined progression for rehab. Advancement from phase to phase as well as specific exercises performed should be based on each individual patient s case and sound clinical judgment by the rehab professional. ** Phase 1: Inpatient Phase (Surgery Hospital Discharge) Control Pain and Swelling Protect Healing Tissue Restore independent functional mobility Work with Case Management to Develop Appropriate Discharge Plan WBAT with Crutches/Walker, unless otherwise ordered Brace locked in extension at all times unless otherwise ordered Range of Motion Ankle pumps Heel Prop (passive extension) Contralateral leg exercise Functional Mobility Gait training on level surfaces Stair training Transfer training ADL s with adaptive equip as needed Positioning (when in bed) Use a towel roll under ankle to promote knee extension Never place anything under the operative knee. This can cause difficulty reaching the goal of full extension. Inpatient Plan of Care Day of Surgery Out of bed to chair PT Evaluation Post Op Day 1 PT service and OT Evaluation Therapeutic Exercise including ROM,, and Functional Mobility as appropriate ADL Training as appropriate Post Op Day 2 Discharge Progression of Therapeutic Exercise and Functional Mobility Continued ADL Training Page 4
5 Phase 2 (Immediate Post Operative Phase Hospital Discharge 2 Weeks) Control Pain and Swelling Protect Healing Tissue Begin to Restore Range of Motion (ROM) Especially Full Extension Establish Good Quadriceps Activation WBAT with Crutches or walker (unless otherwise specified) Brace locked in extension with ambulation and while sleeping Brace unlocked when sitting (flexion angle per order) Range of Motion Heel Slides (with in flexion limitations) 2 Sets of 20 Repetitions Assisted Knee Flexion/Extension in Sitting (within flexion limitations) 2 Sets of 20 Repetitions Heel Prop (passive extension) 5 Minutes Belt Stretch (Calf/Hamstring) Hold 30 Seconds 3 5 Repetitions Ankle Pumps without resistance at least 2 Sets of 20 Repetitions Strength Quad Sets 2 3 Sets of 20 Repetitions Guidelines Perform Range of Motion and exercises 3 5 times a day as tolerated. Phase 3 (Protected ROM Phase 2 6 Weeks) Continued protection of healing tissue Continue to improve ROM (continue guided restrictions for flexion) Continue to establish quad activation WBAT with progressive weaning of crutches or walker as able Continue limited knee flexion (0 90 degrees) Brace locked with ambulation Range of Motion Continue ROM exercises from Phase 1 (slowly progress flexion to 90 degrees) Continue Quad Sets (as needed for VMO activation) Open chain hip abduction, extension, adduction (add ankle weight or resistance band as appropriate) Active Knee Flexion (0 90 degrees only) Page 5
6 Heel Raises *No SLR or Open Chain Active Knee Extension Until 6 Wks* Guidelines Perform all ROM and strengthening exercises once a day. Do 2 3 sets of repetitions. Phase 4 (Early Phase 6 12 Weeks) Progressive Restoration of Normal Knee Flexion Wean from Brace and establish proper gait pattern Begin closed chain strength and proprioceptive training (0 30 degrees of flexion) Stress proper gait as wean from brace Must avoid painful patella femoral stress and excessive loading No running or ballistic movements Range of Motion and Flexibility Continue ROM exercises from phase 1 and 2 (slowly progress to full knee flexion) Add Lower Extremity stretching (Hamstring, Calf, Glutes, Adductors, ITB, etc) *No Quadriceps Stretching until 12 wks Cycle with minimal resistance Continue Progression of Open chain hip abduction, extension, adduction and Hamstring Curls Squats to 30⁰ Low Load, Low Flexion Angle Leg Press Closed Chain Terminal Knee Extension Single Leg Stance Static Balance on Bosu/Wobble Board/Foam/Etc Guidelines Perform ROM and stretching exercises once a day until normal ROM is achieved. Hold stretches for 30 seconds and perform 2 3 repetitions of each. exercise is recommended 3 5 times a week for minutes. Perform strengthening exercises 3 5 times a week. Do 2 3 sets of Reps. Strict attention must be paid to form and minimal patella femoral pain with exercises. Page 6
7 Phase 5 (Advanced Phase Weeks) Continue to avoid patella femoral and extensor mechanism pain Progress to single leg strengthening with progressive increase in flexion angle No Running, Jumping, Plyometric Progressions until Wks (per ) No sports (gradual return to sports after 6 months) ROM and Stretching Continue daily stretching Add gentle Quadriceps stretching Continue cycle with increased resistance Add elliptical, swimming Continue SLR Program Slow Progression to gym Equipment (Leg Press, Ham Curl, Multi Hip) Begin Step Up Progressions (lateral step ups, cross over step ups) *Forward Step Downs are not recommended due to increased patella femoral load* Lunge progression (static to dynamic) Lateral Lunge Progressive Single Leg late in phase (single leg squat, split squat, single leg dead lift) Dynamic Balance (Bosu/Foam/Etc) Dynamic Progressions May begin slow progression of jogging and agility training with approval at 20 Wks Work with PT or to create patient specific plan Jumping Progressions after 24 Wks with approval Guidelines Perform stretching program daily. Hold stretches for 30 seconds and perform 2 3 repetitions of each. program is recommended 3 5 times a week for minutes Perform strengthening/proprioception exercises 3 times a week. Do 2 3 sets of Reps. Perform dynamic progression exercises 2 times a week Phase 6 (Return to Sport/Activity Phase 24 Weeks and Beyond) Maintain adequate ROM, flexibility and strength Continue progressive/dynamic strengthening, proprioceptive, plyometric and agility training Achieve adequate strength to begin return to sport progressions (pending surgeon s clearance) Page 7
8 Limited and controlled plyometric/ballistic movements Gradual return to sport pending surgeon s clearance (6 9 months or greater) Work with surgeon or Physical Therapist to develop specific return to sport progression Stretching Continue daily lower extremity stretching Continue cardio program and progress intensity and duration Continue strengthening program from phase 4 (increase load and decrease volume) Continue and advance proprioceptive training (increase difficulty of drills) Dynamic Progressions Progress plyometric/jumping program as outlined by PT or Outline specific return to sport/activity program with PT and/or Guidelines Perform stretching program daily. Hold stretches for 30 seconds and perform 2 3 repetitions of each. program is recommended 3 5 times a week for minutes Perform strengthening/proprioception exercises 3 times a week. Do 2 3 sets of Reps. Perform plyometric/jumping/agility exercises 2 times a week Perform return to sport activities as directed by P.T. or Page 8
9 Time Weight Bearing and Gait Focus Range of Motion Recommended Exercises Phase 1 Surgery to Discharge Phase Weeks *WBAT with crutches and brace locked at 0⁰ *WBAT with crutches and brace locked at 0⁰ *Control Pain and Swelling *Protect Repair *Restore independent functional mobility *Develop Appropriate Discharge Plan *Wound Healing *Protect Repair *Establish Early ROM in Extension and limited Flexion *Establish Good Quadriceps Contraction with Quad Set *Emphasize 0⁰ Extension *Limit Flexion per order *May Have Specific ROM Instructions per *Emphasize 0⁰ Extension *Limit Flexion per order *May Have Specific ROM Instructions per ROM Ankle pumps Heel Prop (passive extension) Contralateral leg exercise Functional Mobility Gait training on level surfaces Stair training Transfer training ADL s with adaptive equip as needed Positioning (when in bed) Use a towel roll under ankle to promote knee extension ROM Heel Slides, Seated Assisted Knee Flexion/Extension, heel prop, Quad Sets, Hip Abd/Add/Extension, Standing or Prone Hamstring Curl *Protect Repair *Limit Flexion per order *Lock Brace with Weight Bearing *Limit Flexion per order *Minimize Joint Effusion and Edema Phase Weeks *Progress WBAT and wean crutches as tolerated *Continue Brace locked at 0⁰ for ambulations *Continue to Protect Repair *Progress ROM slowly to 90⁰ of flexion over 6 Wks *Continue isometric Quadriceps *Continue Emphasis on 0⁰ of Extension *Slowly progress ROM to 90⁰ of flexion over 6 Wks *May Have Specific ROM Instructions per based on operative findings ROM Continue Phase 1 Exercises: slowly progress flexion to 90 degrees Quad Sets, Hip Abd/Add/Extension, Standing or Prone Hamstring Curl *Still protective of repair so progress flexion slowly *Minimize Joint Effusion and Edema * Stress Locked Brace with Gait *Avoid Patella Femoral Joint Stress Phase Weeks *Unlock Brace with Gait. * Wean From Brace as Gait Improves and Quad gets stronger *Normalize Gait Mechanics *Initiate Active Knee Extension and Isotonic Quad in OKC and CKC *Slowly progress to full flexion *Begin Lower Extremity Stretching Program for uninvolved muscle groups. ROM/Stretching Continue ROM work as needed. Start Lower Extremity Stretching Program of Hamstring, Calf, Hip Muscle Groups Introduce Cycle with minimal resistance Progress Open Chain Hip Program, Add SLR and Active Low Load Open Chain Knee Extension Squats or Wall Slides to 30⁰ Low Load, Low Flexion Angle *Continue to Take Care Not to Overload Patella Femoral Joint Page 9
10 Leg Press Closed Chain Terminal Knee Ext Phase Weeks Phase 6 24 Weeks and Beyond *Straight Ahead Jogging per Approval *Return to Sport per Approval *Focus on regaining strength *Progress from Double leg to single leg CKC strengthening through phase *Continue Preparation for Return to Sport and Physical Activity *Progressive and Jumping *Continue Lower Extremity Stretching Daily *Initiate gentle Quad Stretching * Continue Lower Extremity Stretching Daily Single Leg Stance, Static Balance on Bosu/Wobble Board/Etc ROM/Stretching *Continue Daily Stretching *Add Gentle Quad Stretch *Continue cycle with increased resistance *Add elliptical, swimming *Continue SLR and Low Load Open Chain Program * Slow Progression to gym Equipment (Leg Press, Ham Curl, Multi Hip) Begin Step Up Progressions (lateral step ups, cross over step ups) *Lunge progression (static to dynamic) Lateral Lunge Progressive Single Leg late in phase (single leg squat, split squat, single leg dead lift, etc) Dynamic Balance with Bosu/Foam/Etc Dynamic Progressions *Jogging, agility, jumping all per Stretching Continue daily Continue cardio program and progress intensity and duration Continue strengthening program from phase 4 (increase load and decrease volume) Continue and advance proprioceptive training Dynamic Progressions Progress plyometric/jumping program as outlined by PT or Outline specific return to sport/activity program with PT and/or * Continue to Take Care Not to Overload Patella Femoral Joint *Jogging generally held until 20 Wks *Agility generally held until 20 Wks *Jumping generally held until 24 Wks * Must Have Full ROM, 90% Return of Strength and No Patella Femoral Pain to Begin Return to Sport Progressions * Gradual return to sport/activity pending surgeon s clearance (6 9 months or greater) *Reviewed by Michael Geary, Page 10
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
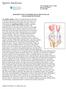 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
Strength Training for the Knee
 Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Strength Training for the Knee This handout is to help you rebuild the strength of the muscles surrounding the knee after injury. It is intended as a guideline to help you organize a structured approach
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
HIPABDUCTOR REPAIR PROTOCOL (Gluteus Medius/Minimus Repair)
 R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Medial Collateral Ligament (MCL) Rehabilitation Protocol
 Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Dr. O Meara s. Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com
 Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
Dr. O Meara s Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol www.palomarortho.com Anterior Knee Pain (PatelloFemoral Syndrome) Rehabilitation Protocol Hamstring Stretching & Strengthening
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol Phase I: Healing Phase (0-2 Weeks) Goal: Protect Incision, Reduce Inflammation, Allow Tissues to Heal, and Rest Wound Care: Keep Incision covered with sealed dressing
Hip Arthroscopy Rehabilitation Protocol Phase I: Healing Phase (0-2 Weeks) Goal: Protect Incision, Reduce Inflammation, Allow Tissues to Heal, and Rest Wound Care: Keep Incision covered with sealed dressing
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
ACL Rehabilitation Protocol
 ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
ACL Rehabilitation Protocol Mark Clatworthy, Orthopaedic Surgeon, Knee Specialist This guideline has been prepared to help guide you through your recovery following your anterior cruciate ligament reconstruction.
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty. Richard M. Wilk, M.D. Michael Kain, M.D.
 Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty Richard M. Wilk, M.D. Michael Kain, M.D. Department of Orthopaedic Surgery Lahey Hospital & Medical
Rehabilitation Protocol: Hip Arthroscopy Femoral Acetabular Impingement Debridement/Osteochondroplasty Richard M. Wilk, M.D. Michael Kain, M.D. Department of Orthopaedic Surgery Lahey Hospital & Medical
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Hip Arthroscopy Labral Repair Rehabilitation Protocol
 Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
Hip Arthroscopy Labral Repair Rehabilitation Protocol PHASE 1: INITIAL Diminish pain and inflammation Protect integrity of repaired tissue Prevent muscular inhibition Restore ROM within the restrictions
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella)
 EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Rehabilitation After Your Total Knee Replacement
 1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
ACL Reconstruction Rehabilitation Protocol
 Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
Peter J. Millett, MD, MSc The Steadman Clinic Vail, CO www.drmillett.com Table of Contents Preoperative Rehabilitation Phase...3 Understanding Surgery...7 Postoperative Days 1-7...8 Postoperative Days
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Inland Orthopaedic Surgery & Sports Medicine
 Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Vanderbilt Orthopaedic Institute
 Total Knee Arthroplasty (TKA) and Unicondylar Rehabilitation Guideline Pre-operative Phase Recommendations Attend pre-operative group education class Maintain and/or increase strength and ROM Education
Total Knee Arthroplasty (TKA) and Unicondylar Rehabilitation Guideline Pre-operative Phase Recommendations Attend pre-operative group education class Maintain and/or increase strength and ROM Education
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Most Common Running Injuries
 Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY
 PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
PHYSIOTHERAPY REHAB AFTER HIP ARTHROSCOPY Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction This leaflet has been compiled by the Physiotherapy Team to help you understand the hip
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
