BlueCross BlueShield of Illinois
|
|
|
- Opal Warner
- 7 years ago
- Views:
Transcription
1 â â BlueCross BlueShield of Illinois OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This is not the insurance contract, and only the actual Policy provisions will control. The Policy itself sets forth in detail the rights and obligations of both you and your insurance company. It is, therefore, important that you READ YOUR POLICY CAREFULLY! 2. Blue Choice Preferred PPO Coverage Coverage is designed to provide you with economic incentives for using designated health care providers. It provides, to persons insured, coverage for major Hospital, medical, and surgical expenses incurred as a result of a covered accident or sickness. Coverage is provided for daily Hospital room and board, miscellaneous Hospital MAJOR MEDICAL EXPENSE COVERAGE Blue Choice Preferred Bronze PPO 106 Blue Choice Preferred PPO Network services, surgical services, anesthesia services, In-Hospital medical services, and Out-of-Hospital care, subject to any s, Copayment provisions, or other limitations which may be set forth in the Policy. Although you can go to the Hospitals and Physicians of your choice, your benefits under the Policy will be greater when you use the services of designated Hospitals and Physicians. 3. Each benefit period you must satisfy the calendar year before your benefits will begin, except for Preventive Care Services and other Covered Services not subject to a. Expenses incurred by you for Covered Services will also be applied towards the calendar year. Refer to the Policy for more information. Changes in some state or federal law or regulations or interpretations thereof may change the terms and conditions of coverage. BASIC PROVISIONS Blue Choice Preferred Bronze PPO 106 YOUR COST Hospitals Benefits Daily bed, board and general nursing care, and ancillary services (i.e., operating rooms, drugs, surgical dressings, and lab work). Inpatient Hospital Covered Services Participating 50% of the Eligible Charge
2 Outpatient Hospital Covered Services Surgery, diagnostic services, radiation, therapy, chemotherapy, electroconvulsive therapy, renal dialysis treatments and continuous ambulatory peritoneal dialysis treatment, coordinated home care program, pre-admission testing, partial hospitalization treatment program, autism spectrum disorders, habilitative services, surgical implants, maternity services, and urgent care. Participating Hospital Emergency Care 50% of the Eligible Charge Emergency Accident Care from either a Participating or Provider Emergency Medical Care from either a Participating or Provider Emergency Room (waived if admitted to the Hospital as an Inpatient immediately following emergency treatment) Physician Benefits Surgery, anesthesia, assistant surgeon, medical care, treatment of illness, consultations, mammograms, outpatient periodic health examinations, routine pediatric care, diagnostic services, injected medicines, amino acid-based elemental formulas, electroconvulsive therapy, radiation therapy, chemotherapy, cancer medications, outpatient rehabilitative therapy, autism spectrum disorders, habilitative services, outpatient respiratory therapy, chiropractic and osteopathic manipulation, hearing screening, diabetes self-management training and education, pediatric vision care, dental accident care, family planning services, outpatient contraceptive services, bone mass measurement and osteoporosis, investigational cancer treatment, infertility treatment, pediatric dental services, mastectomy related services, maternity services, and urgent care. Payment level for Surgical/Medical Covered Services Outpatient office visits (Participating Providers) (except for Outpatient periodic health examinations, routine pediatric care, pediatric routine vision examinations, Physical Therapy, Occupational Therapy, Speech Therapy, chiropractic and osteopathic manipulation, Surgery, Diagnostic Services (including, x-rays, lab services, CT, PET, MRI) and Maternity Services after the first pre-natal visit) Outpatient Specialist office visits (Participating Providers) Participating 50% of the Maximum Allowance Chiropractic and Osteopathic Manipulation Naprapathic Services 25 Visit Maximum per Benefit Period 15 Visit Maximum per Benefit Period
3 Emergency Accident Care from either a Participating or Provider Emergency Medical Care from either a Participating or Provider Other (Miscellaneous) Covered Services Blood and blood components; medical and surgical dressings, supplies, casts and splints, prosthetic devices, orthotic devices and durable medical equipment. Individual Per individual, per calendar year. (If you have Family Coverage, each member of your family must satisfy his/her own individual deductible.) Family If you have Family Coverage and your family has satisfied the family amount specified, it will not be necessary for anyone else in your family to meet a calendar year in the benefit period. That is, for the remainder of that benefit period, no other family members will be required to meet the calendar year before receiving benefits. Participating $6,000* $15,000* Participating $13,100* $45,000* Participating $6,000* Individual Out-of-Pocket Expense Limit* No limit* Participating $13,100* Family Out-of-Pocket Expense Limit* No limit* Participating * Inpatient Hospital *
4 Participating * Outpatient Surgical * Preventive Care Services Benefits will be provided for the following Covered Services and will not be subject to Coinsurance,, Copayment or dollar maximum: Evidence-based items or services that have in effect a rating of A or B in the current recommendations of the United States Preventive Services Task Force (USPSTF); immunizations recommended by the Advisory Committee on Immunization Practices of the Centers for Disease Control and prevention with respect to the individual involved; evidenced-informed preventive care and screenings provided for in the comprehensive guidelines supported by the Health Resources and Services Administration (HRSA) for infants, children, and adolescents; and additional preventive care and screenings provided for in comprehensive guidelines supported by the HRSA. For purposes of this benefit, the current recommendations of the USPSTF regarding breast cancer screening and mammography and prevention will be considered the most current (other than those issued in or around November 2009). Outpatient Prescription Drug Program Drugs, diabetic supplies, insulin and syringes *The calendar year, Copayment amount, Out-of-Pocket Expense Limit and Covered Service Expense Limitation amounts may be subject to change or increase as permitted by applicable law.
5 Schedule of Pediatric Vision Coverage Vision Care Services In-network Covered Person Cost or Discount (When a fixed-dollar Copayment is due from the Covered Person, the remainder is payable under this Policy up to the covered charge*) Out-of-network Allowance (Maximum amount payable under this Policy, not to exceed the retail costs)** Exam (with dilation as necessary): No Copayment Up to $30 Frames: Collection frame Frames covered under this Policy are limited to the Pediatric Frame Selection of covered frames. The Pediatric Frame Selection includes a selection of frame sizes (including adult sizes) for children up to age 19. The network provider will show you the selection of frames covered under this Policy. If you select a frame that is not included in the Pediatric Frame Selection covered under this Policy, you are responsible for the difference in cost between the In network provider reimbursement amount for covered frames from the Pediatric Frame Selection and the retail price of the frame selected. If frames are provided by an out-ofnetwork Provider, benefits are limited to the amount shown above. Any amount 1) paid to the in network provider for the difference in cost of a non-pediatric Frame Selection frame or 2) that exceeds the Maximum Covered Fee for an out-of-network provider supplied frame will not apply to any applicable, Coinsurance, or out-of-pocket maximum/outof-pocket Coinsurance maximum. Up to $150, after Up to $30, after Frequency: Examination, Lenses or Contact Lenses Frame Once every 12-month benefit period Once every 12-month benefit period Standards Plastic, Glass or Poly Spectacle Lenses: Single Vision Covered, after Up to $25, after Lined Bifocal Covered, after Up to $35, after Lined Trifocal Covered, after Up to $45, after Lenticular Covered, after Up to $45, after Note: All lenses include scratch resistant coating with no additional copayment. There
6 may be an additional charge at Walmart and Sam s Club Lens Options (add to lens costs above): Ultraviolet Protective Coating Polycarbonate Lenses Blended Segment Lenses Intermediate vision Lenses Standard Progressives Premium Progressives (Varilux, etc.) Photochromic Glass Lenses Plastic Photosensitive Lenses (Transitions ) Polarized Lenses Standard Anti-Reflective (AR) Coating Premium AR Coating Ultra AR Coating High Index Lenses Progressive Lens Options Members may receive a discount on additional progressive lens options: Select Progressive Lenses Ultra Progressive Lenses Scratch Protection Plan Single Vision Lens Multifocal Lens Contact Lenses: covered once every calendar year in lieu of eyeglasses No Copayment No Copayment $20 Copayment $30 Copayment No Copayment $90 Copayment $20 Copayment No Copayment $75 Copayment $35 Copayment $48 Copayment $60 Copayment $55 Copayment $70 Copayment $140 Copayment $20 Copayment $40 Copayment Not covered Elective Up to $150, after Up to $75, after Medically Necessary contact lenses Preauthorization is required to be considered for benefits (see details below) Contact lenses covered under this Policy are limited to the Pediatric Lens Selection. The Network Provider will inform you of the contact lens selection covered under this Policy. If you select a frame that is not included in the pediatric lens selection covered under this Policy, you are responsible for the difference in cost between the network provider reimbursement amount for covered contact lenses available from the Pediatric Contact Lens Selection and the retail price of the contact lenses selected. Any amount 1) paid to the network provider for the difference in cost of a non-pediatric Contact Lens Selection contact lens or 2) that exceeds the Maximum Covered Fee for Provider supplied contacts will not apply to any applicable, Coinsurance, or out-ofpocket maximum/out-of-pocket limit/out-ofpocket coinsurance maximum. Up to $600, after Up to $225, after
7 Note: Additional benefits over allowance are available from participating providers except Walmart and Sam s Club Routine eye exams do not include professional services for contact lens evaluations. Any applicable fees are the responsibility of the patient. Value-added features: Laser vision correction: You will receive a discount for traditional LASIK and custom LASIK from Participating Physicians and contracted laser centers. You must obtain Preauthorization for this service in order to receive coverage. Prices/discounts may vary by state and are subject to change without notice. Mail-order contact lens replacement: Lens Program (visit the Lens website: Additional Benefits Medically Necessary contact lenses: Contact lenses may be determined to be medically necessary and appropriate in the treatment of patients affected by certain conditions. In general, contact lenses may be medically necessary and appropriate when the use of contact lenses, in lieu of eyeglasses, will result in significantly better visual and/or improved binocular function, including avoidance of diplopia or suppression. Contact lenses may be determined to be medically necessary in the treatment of the following conditions: keratoconus, pathological myopia, aphakia, anisometropia, aniseikonia, aniridia, corneal disorders, post-traumatic disorders, irregular astigmatism. Medically necessary contact lenses are covered in lieu of other eyewear. Participating providers will obtain the necessary preauthorization for these services. Low Vision: Low vision is a significant loss of vision but not total blindness. Ophthalmologists and optometrists specializing in low vision care can evaluate and prescribe optical devices, and provide training and instruction to maximize the remaining usable vision for our members with low vision. With prior approval from Blue Cross and Blue Shield of Illinois, covered persons who required low-vision services and optical devices are entitled to the following coverage, both In- and Out-of Network: Low Vision Evaluation: One comprehensive evaluation every five years (Out-of-Network Maximum Allowance of $300). This examination, sometimes called a functional vision assessment, can determine distance and clarity of vision, the size of readable print, the existence of blind spots or tunnel vision, depth perception, eye-hand coordination, problems perceiving contrast and lighting requirements for optimum vision. Low Vision Aid: Covered for one device per year such as high-power spectacles, magnifiers and telescopes (Outof-Network Maximum Allowance of $600 per device and $1200 lifetime). These devices are utilized to maximize use of available vision, reduce problems of glare or increase contrast perception, based on the individual s vision goals and lifestyle needs. Follow-up care: Four visits in any five-year period (Out-of-Network Maximum Allowance of $100 per visit). Warranty: Warranty limitations may apply to Provider or retailer supplied frames and/or eyeglass lenses. Please ask your Provider for details of the warranty that is available to you. * The covered charge is the rate negotiated with network providers for a particular Covered Service. ** THE PLAN PAYS THE LESSER OF THE MAXIMUM ALLOWANCE NOTED OR THE RETAIL COST. RETAIL PRICES VARY BY LOCATION.
8 EXCLUSIONS AND LIMITATIONS: Services or supplies that are not specifically mentioned in this Policy. Services or supplies for any illness or injury arising out of or in the course of employment for which benefits are available under any Workers Compensation Law or other similar laws whether or not you make a claim for such compensation or receive such benefits. However, this exclusion shall not apply if you are a corporate officer of any domestic or foreign corporation and are employed by the corporation and elect to withdraw yourself from the operation of the Illinois Workers Compensation Act according to the provisions of the Act. Services or supplies that are furnished to you by the local, state or federal government and for any services or supplies to the extent payment or benefits are provided or available from the local, state or federal government (for example, Medicare) whether or not that payment or benefits are received, except however, this exclusion shall not be applicable to medical assistance benefits under Article V, VI or VII of the Illinois Public Aid Code (Ill. Rev. Stat. ch et seq.) or similar legislation of any state, benefits provided in compliance with the Tax Equity and Fiscal Responsibility Act or as otherwise provided by law. Services and supplies for any illness or injury occurring on or after your Coverage Date as a result of war or an act of war. Services or supplies that do not meet accepted standards of medical and/or dental practice. Experimental/Investigational Services and Supplies and all related services and supplies, except as may be provided under this Policy for a) Routine Patient Costs associated with Experimental/Investigational cancer treatment, if you are a qualified individual participating in a qualified clinical cancer trial, if those services or supplies would otherwise be covered under this Policy if not provided in connection with a qualified cancer trial program and b) applied behavior analysis used for the treatment of Autism Spectrum Disorder(s). Custodial Care Service. Long Term Care Service. Respite Care Service, except as specifically mentioned under the Hospice Care Program section of this Policy. Inpatient Private Duty Nursing. Services or supplies received during an Inpatient stay when the stay is solely related to behavioral, social maladjustment, lack of discipline or other antisocial actions which are not specifically the result of Mental Illness. This does not include services or supplies provided for the treatment of an injury resulting from an act of domestic violence or a medical condition (including both physical and mental health conditions.). Cosmetic Surgery and related services and supplies, except for the correction of congenital deformities or for conditions resulting from accidental injuries, scars, tumors or diseases. Services or supplies for which you are not required to make payment or would have no legal obligation to pay if you did not have this or similar coverage. Charges for failure to keep a scheduled visit or charges for completion of a Claim form. Personal hygiene, comfort or convenience items commonly used for other than medical purposes, such as air conditioners, humidifiers, physical fitness equipment, televisions and telephones. Special braces, specialized equipment, appliances, or ambulatory apparatus, except as specifically mentioned in this Policy. Blood derivatives which are not classified as drugs in the official formularies. Eyeglasses, contact lenses or cataract lenses and the examinations for prescribing or fitting of glasses or contact lenses or for determining the refractive state of the eye, except as specifically mentioned in this Policy. This is exclusion is not applicable to children. Treatment of flat foot conditions and the prescription of supportive devices for such conditions and the treatment of subluxations of the foot or routine foot care. Routine foot care, except for persons diagnosed with diabetes.
9 Maintenance Occupational Therapy, Maintenance Physical Therapy and Maintenance Speech Therapy, except as specifically mentioned in this Policy. Acupuncture, whether for medical or anesthesia purposes. Maintenance Care. Hearing aids, except for bone anchored hearing aids (osseointegrated auditory implants), or examinations for the prescription or fitting of hearing aids, unless otherwise specified in this Policy. This exclusion is not applicable to children as described in this Policy. Diagnostic Service as part of determination of the refractive errors of the eyes, auditory problems, surveys, case finding, research studies, screening, or similar procedures and studies, or tests which are Investigational, unless otherwise specified in this Policy. Procurement or use of prosthetic devices, special appliances and surgical implants which are for cosmetic purposes, for the comfort and convenience of the patient, or unrelated to the treatment of a disease or injury. Wigs (also referred to as cranial prostheses). Prescription antiseptic or fluoride mouthwashes, mouth rinses or topical oral solutions or preparations, Retin-A or pharmacological similar topical drugs. Abortions for which Federal funding is not allowed in accordance with Affordable Care Act section 1303(b)(1)(B)(i), namely all abortions except in the case of rape or incest, or for a pregnancy which, as certified by a physician, places the woman in danger of death unless an abortion is performed. Repair and replacement for appliances and/or devices due to misuse or loss, except as specifically mentioned in this Policy. Habilitative Services that are solely educational in nature or otherwise paid under State or Federal law for purely educational services. Not withstanding any provision in the Policy to the contrary, any services and/or supplies provided to you outside the United States, unless you receive Emergency Accident Care or Emergency Medical Care. Services and supplies rendered or provided for human organ or tissue transplants other than those specifically mentioned in this Policy. Reversals of vasectomies. Residential Treatment Centers, except for Inpatient Substance Use Disorder Rehabilitation Treatment or Inpatient Mental Illness except as specifically mentioned under this Policy. Any drugs and medicines, except as may be provided under Outpatient Prescription Drugs, that are: Dispensed by a Pharmacy and received by you while covered under this Policy, Dispensed in a Provider s office or during confinement in a Hospital or other acute care institution or facility and received by you for use on an Outpatient basis, Over-the-counter drugs and medicines; or drugs for which no charge is made,
10 GUARANTEED RENEWABILITY Coverage under the Policy will be terminated for nonpayment of premiums. Blue Cross and Blue Shield may terminate or refuse to renew the Policy only for the following reasons: 1. If every Policy that bears the Policy form number, is not renewed. If every Policy that bears the same Group Number, is not renewed or if Blue Cross and Blue Shield ceases to offer a particular type of coverage in the individual market. If this should occur: a. Blue Cross and Blue Shield will give you at least 90 days prior written notice. b. You may convert to any other individual policy Blue Cross and Blue Shield offers to the individual market. c. If Blue Cross and Blue Shield should terminate or refuse to terminate the Policy, it must do so uniformly without regard to any health status-related factor of covered individuals or dependents of covered individuals who may become eligible for coverage. 2. If Blue Cross and Blue Shield discontinue all health care coverage and does not renew all health insurance Policies it issues or delivers for issuance in the individual market in the state. If this should occur, Blue Cross and Blue Shield will give you at least 180 days prior written notice. 3. In the event of fraud or an intentional misrepresentation of material fact under the terms of the Policy. In this case, Blue Cross and Blue Shield will give you at least 30 days prior written notice. 4. You no longer reside, live or work in the Blue Cross and Blue Shield s service area. 5. Failure to pay your premium in accordance with the terms of the Policy, including any timeliness requirements. Blue Cross and Blue Shield will never terminate or refuse to renew the Policy because of the condition of your health.
OUTLINE OF COVERAGE. BASIC PROVISIONS Blue Choice Gold PPO 001. MAJOR MEDICAL EXPENSE COVERAGE Blue Choice Gold PPO 001 Blue Choice PPO Network
 OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This is not the insurance contract, and only the actual
OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your Policy. This is not the insurance contract, and only the actual
BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network
 BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
Health Choice Essential Gold Standard Gold Off Exchange Plan Network: Health Choice Essential Type of Coverage: HMO
 Subscriber ID: [XXXXXXX] Health Choice Essential Gold Standard Gold Off Exchange Plan Network: Health Choice Essential Type of Coverage: HMO EOC Effective Date: [XX/XX/XXXX] Subscriber: [Subscriber Name]
Subscriber ID: [XXXXXXX] Health Choice Essential Gold Standard Gold Off Exchange Plan Network: Health Choice Essential Type of Coverage: HMO EOC Effective Date: [XX/XX/XXXX] Subscriber: [Subscriber Name]
Blue Cross Premier Bronze Extra
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
Group Hospitalization and Medical Services, Inc.
 Group Hospitalization and Medical, Inc. doing business as CareFirst BlueCross BlueShield [840 First Street, NE] [Washington, DC 20065] [202-479-8000] An independent licensee of the Blue Cross and Blue
Group Hospitalization and Medical, Inc. doing business as CareFirst BlueCross BlueShield [840 First Street, NE] [Washington, DC 20065] [202-479-8000] An independent licensee of the Blue Cross and Blue
BlueCare Direct Bronze SM HMO 103 BlueCare Direct SM HMO Network
 BlueCare Direct Bronze SM HMO 103 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
BlueCare Direct Bronze SM HMO 103 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
Summary of Services and Cost Shares
 Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Coventry Health & Life Insurance Company Small Group PPO Schedule of Benefits:
 Coventry Health & Life Insurance Company Small Group PPO Schedule of Benefits: Plan ID#: Silver Traditional 3000 90-14 (# ) This Schedule of Benefits summarizes Your obligation towards the cost of certain
Coventry Health & Life Insurance Company Small Group PPO Schedule of Benefits: Plan ID#: Silver Traditional 3000 90-14 (# ) This Schedule of Benefits summarizes Your obligation towards the cost of certain
Benefit Summary - A, G, C, E, Y, J and M
 Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Coventry Health Care of Missouri
 Small Group PPO Schedule of Benefits: Coventry Health Care of Missouri Plan ID#: Platinum Carelink from Coventry A000-14 (# ) This Schedule of Benefits summarizes Your obligation towards the cost of certain
Small Group PPO Schedule of Benefits: Coventry Health Care of Missouri Plan ID#: Platinum Carelink from Coventry A000-14 (# ) This Schedule of Benefits summarizes Your obligation towards the cost of certain
CareFirst BlueChoice, Inc.
 CareFirst BlueChoice, Inc. [840 First Street, NE] [Washington, DC 20065] [(202) 479-8000] An independent licensee of the BlueCross and Blue Shield Association ATTACHMENT [C] IN-NETWORK SCHEDULE OF BENEFITS
CareFirst BlueChoice, Inc. [840 First Street, NE] [Washington, DC 20065] [(202) 479-8000] An independent licensee of the BlueCross and Blue Shield Association ATTACHMENT [C] IN-NETWORK SCHEDULE OF BENEFITS
International Student Health Insurance Program (ISHIP) 2014-2015
 2014 2015 Medical Plan Summary for International Students Translation Services If you need an interpreter to help with oral translation services, you may contact the LifeWise Customer Service team at 1-800-971-1491
2014 2015 Medical Plan Summary for International Students Translation Services If you need an interpreter to help with oral translation services, you may contact the LifeWise Customer Service team at 1-800-971-1491
Commercial. Individual & Family Plan. Health Net California Farm Bureau and PPO. Insurance Plans. Outline of Coverage and Exclusions and Limitations
 Commercial Individual & Family Plan Health Net California Farm Bureau and PPO Insurance Plans Outline of Coverage and Exclusions and Limitations Table of Contents Health Plans Outline of coverage 1 Read
Commercial Individual & Family Plan Health Net California Farm Bureau and PPO Insurance Plans Outline of Coverage and Exclusions and Limitations Table of Contents Health Plans Outline of coverage 1 Read
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective 7/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
National PPO 1000. PPO Schedule of Payments (Maryland Small Group)
 PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
APPENDIX C Description of CHIP Benefits
 Inpatient General Acute and Inpatient Rehabilitation Hospital Unlimited. Includes: Hospital-provided physician services Semi-private room and board (or private if medically necessary as certified by attending)
Inpatient General Acute and Inpatient Rehabilitation Hospital Unlimited. Includes: Hospital-provided physician services Semi-private room and board (or private if medically necessary as certified by attending)
UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits
 UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits Please refer to your Provider Directory for listings of Participating Physicians, Hospitals, and other Providers.
UnitedHealthcare Insurance Company of the River Valley Attachment D - Schedule of Benefits Please refer to your Provider Directory for listings of Participating Physicians, Hospitals, and other Providers.
Member s responsibility (deductibles, copays, coinsurance and dollar maximums)
 MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective 1/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
SERVICES IN-NETWORK COVERAGE OUT-OF-NETWORK COVERAGE
 COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
Preauthorization Requirements * (as of January 1, 2016)
 OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
General Cost Sharing Features In-Network Out-of-Network
 SECTION A. Summary of Benefits 9-RCF, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
SECTION A. Summary of Benefits 9-RCF, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
Benefits At A Glance Plan C
 Benefits At A Glance Plan C HIGHLIGHTS OF WELFARE FUND BENEFITS WELFARE FUND BENEFITS IN BRIEF Medical and Hospital Benefits Empire BlueCross BlueShield Plan C-1 Empire BlueCross BlueShield Plan C-2 All
Benefits At A Glance Plan C HIGHLIGHTS OF WELFARE FUND BENEFITS WELFARE FUND BENEFITS IN BRIEF Medical and Hospital Benefits Empire BlueCross BlueShield Plan C-1 Empire BlueCross BlueShield Plan C-2 All
THE EPIC LIFE INSURANCE COMPANY
 THE EPIC LIFE INSURANCE COMPANY VISION BENEFITS ENDORSEMENT FOR WSE SUPPLEMENTAL DENTAL, HOSPITAL INDEMNITY AND ACCIDENTAL DEATH AND DISMEMBERMENT CERTIFICATE In consideration of the premiums charged by
THE EPIC LIFE INSURANCE COMPANY VISION BENEFITS ENDORSEMENT FOR WSE SUPPLEMENTAL DENTAL, HOSPITAL INDEMNITY AND ACCIDENTAL DEATH AND DISMEMBERMENT CERTIFICATE In consideration of the premiums charged by
California Ironworkers Field Welfare Plan 1/1/2014 Open Enrollment Benefit Plan Comparison Non-Medicare Retired Participants Residing in Nevada
 Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
LOCKHEED MARTIN AERONAUTICS COMPANY PALMDALE 2011 IAM NEGOTIATIONS UNDER AGE 65 LM HEALTHWORKS SUMMARY
 Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
SCHEDULE OF BENEFITS. Group Access Care Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix)
 Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
MyHPN Solutions HMO Silver 4
 MyHPN Solutions HMO Silver 4 Attachment A Schedule Calendar Year Deductible (CYD): $2,250 of EME per Member and $4,500 of EME per family. The Calendar Year Out of Pocket Maximum includes the CYD and is
MyHPN Solutions HMO Silver 4 Attachment A Schedule Calendar Year Deductible (CYD): $2,250 of EME per Member and $4,500 of EME per family. The Calendar Year Out of Pocket Maximum includes the CYD and is
SCHEDULE OF BENEFITS. Group Access Care Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
Important Questions Answers Why this Matters:
 Bronze 60 EPO - Network Name: EPO Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: EPO
Bronze 60 EPO - Network Name: EPO Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: EPO
CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance
 CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview
CENTRAL MICHIGAN UNIVERSITY - Premier Plan (PPO1) 007000285-0002 0004 Effective Date: July 1, 2015 Benefits-at-a-Glance This is intended as an easy-to-read summary and provides only a general overview
Personal Blue PPO QHDHP $5,000/$10,000
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-962-2242. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-962-2242. Important
I want a health care plan with all the options.
 I want a health care plan with all the options. PERSONAL BLUEPLANS SE These are my plans. Personal BluePlans SM SE PLAN FEATURES Personal Blue BluePlans SE let you build the plan that works for you. The
I want a health care plan with all the options. PERSONAL BLUEPLANS SE These are my plans. Personal BluePlans SM SE PLAN FEATURES Personal Blue BluePlans SE let you build the plan that works for you. The
Independence Blue Cross Plan Summary PPO Core Medical Plan
 TO: FROM: SUBJECT: MLH Medical Plan Participants MLH Human Resources Benefits Team Independence Blue Cross Plan Summary PPO Core Medical Plan Attached you will find the Independence Blue Cross (IBC) Plan
TO: FROM: SUBJECT: MLH Medical Plan Participants MLH Human Resources Benefits Team Independence Blue Cross Plan Summary PPO Core Medical Plan Attached you will find the Independence Blue Cross (IBC) Plan
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 Blue Cross Blue Shield Solution 102, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Blue Cross Blue Shield Solution 102, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueShield: Regence Direct Gold with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What
Regence BlueShield: Regence Direct Gold with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What
SCHEDULE OF BENEFITS (continued) Group LINK Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68 ] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68 ] Family Coverage [$1,210.66]] Benefit
SECTION A. Summary of Benefits LW-V, 10/09
 SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
US Airways Medicare Options US Trust 2015 Benefits Guide
 US Airways Medicare Options US Trust 2015 Benefits Guide Welcome to the 2015 Medicare Options US Trust Retiree Benefit Plans This guide includes detailed information regarding the benefit options available
US Airways Medicare Options US Trust 2015 Benefits Guide Welcome to the 2015 Medicare Options US Trust Retiree Benefit Plans This guide includes detailed information regarding the benefit options available
Greater Tompkins County Municipal Health Insurance Consortium
 WHO IS COVERED Requires both Medicare A & B enrollment. Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement None None Medical Benefit Management Program Not
WHO IS COVERED Requires both Medicare A & B enrollment. Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement None None Medical Benefit Management Program Not
Schedule of Benefits HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS MEMBER COST SHARING
 Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
SCHEDULE OF BENEFITS. Group Access Care Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SUMMARY!OF!BENEFITS!
 SUMMARY!OF!BENEFITS!! BASIC!PLAN! COMPREHENSIVE! Policy Year Maximum Unlimited Unlimited Out-of-Pocket Limit OUTPATIENT!BENEFITS! Doctor s Visits Most Primary Care office visits at SHC are provided at
SUMMARY!OF!BENEFITS!! BASIC!PLAN! COMPREHENSIVE! Policy Year Maximum Unlimited Unlimited Out-of-Pocket Limit OUTPATIENT!BENEFITS! Doctor s Visits Most Primary Care office visits at SHC are provided at
Important Questions Answers Why this Matters:
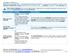 Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Schedule of Benefits Summary. Health Plan. Out-of-network Provider
 Schedule of Benefits Summary University Name: University of Nebraska - Student Plan Health Plan : 2014/2015 Academic Year (see attached) Payment for Services Covered Services are reimbursed based on the
Schedule of Benefits Summary University Name: University of Nebraska - Student Plan Health Plan : 2014/2015 Academic Year (see attached) Payment for Services Covered Services are reimbursed based on the
Blue Choice Silver PPO 004 Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com/member/policy-forms/ or by calling 1-800-538-8833.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcbsil.com/member/policy-forms/ or by calling 1-800-538-8833.
Coventry Health and Life Insurance Company PPO Schedule of Benefits
 State(s) of Issue: Oklahoma PPO Plan: OI08C30050 30 Coventry Health and Life Insurance Company PPO Schedule of Benefits Covered Services Contract Year Deductible For All Eligible Expenses (unless otherwise
State(s) of Issue: Oklahoma PPO Plan: OI08C30050 30 Coventry Health and Life Insurance Company PPO Schedule of Benefits Covered Services Contract Year Deductible For All Eligible Expenses (unless otherwise
How To Pay For Health Care With A Health Care Plan With A Premium Rate Of $1,000 A Year
 Regence BlueCross BlueShield of Utah: Regence Direct Silver HSA Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual &
Regence BlueCross BlueShield of Utah: Regence Direct Silver HSA Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual &
Your Out-of-Pocket Type of Service
 Calendar Year Deductible (CYD) 1 $5,000 single/ 2x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,000 single/ 2x family maximum. With respect to family plans,
Calendar Year Deductible (CYD) 1 $5,000 single/ 2x family Out-of-Pocket Maximum - Deductibles and copays all accrue towards the out-of-pocket $6,000 single/ 2x family maximum. With respect to family plans,
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 Blue Cross Blue Shield Basic 103, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
Blue Cross Blue Shield Basic 103, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan
Alternate PPO/Alternate Rx
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-866-802-4761. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-866-802-4761. Important
What is the overall deductible? Are there other deductibles for specific services?
 : MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
: MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
PLAN DESIGN AND BENEFITS - New York Open Access EPO 1-10/10
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $3,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
Regence BlueCross BlueShield of Oregon: Regence Oregon Standard Bronze Plan Coverage Period: Beginning on or after 01/01/2014
 Regence BlueCross BlueShield of Oregon: Regence Oregon Standard Bronze Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 01/01/2014 Coverage
Regence BlueCross BlueShield of Oregon: Regence Oregon Standard Bronze Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: Beginning on or after 01/01/2014 Coverage
SCHEDULE OF BENEFITS. Group LINK Comprehensive Health Insurance Policy
 SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
SCHEDULE OF BENEFITS Classes of Employees Insured: [Class 1 All Active Full-Time Indian Employees] [Monthly Premium Rates: Individual - [$ 398.34] Two-Person [$796.68] Family Coverage [$1,210.66]] Benefit
Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016
 Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016 This Schedule of Benefits summarizes your obligation towards the cost of certain covered services. Refer to
Schedule of Benefits for the MoDOT/MSHP Medical Plan Medicare ASO PPO 20088 Effective 1/1/2016 This Schedule of Benefits summarizes your obligation towards the cost of certain covered services. Refer to
Greater Tompkins County Municipal Health Insurance Consortium
 WHO IS COVERED Requires Covered Member to be Enrolled in Both Medicare Parts A & B Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement Not Applicable Not Applicable
WHO IS COVERED Requires Covered Member to be Enrolled in Both Medicare Parts A & B Type of Coverage Offered Single only Single only MEDICAL NECESSITY Pre-Certification Requirement Not Applicable Not Applicable
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE
 ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
SCHEDULE OF BENEFITS
 SCHEDULE OF BENEFITS Premier HealthOne Bronze 5500 Health Maintenance Organization (HMO) Individual Certificate of Coverage This schedule of benefits (SOB) is part of your Certificate of Coverage (COC)
SCHEDULE OF BENEFITS Premier HealthOne Bronze 5500 Health Maintenance Organization (HMO) Individual Certificate of Coverage This schedule of benefits (SOB) is part of your Certificate of Coverage (COC)
StudentBlue University of Nebraska
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO What is the overall deductible? This is only a summary. If you want more details about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO What is the overall deductible? This is only a summary. If you want more details about
HIGHMARK VISION COVERAGE MAKES IT EASY TO GET VISION CARE
 HIGHMARK VISION COVERAGE MAKES IT EASY TO GET VISION CARE You know the importance of vision care. Regular eye exams are an important part of overall preventive health care. According to the Vision Council
HIGHMARK VISION COVERAGE MAKES IT EASY TO GET VISION CARE You know the importance of vision care. Regular eye exams are an important part of overall preventive health care. According to the Vision Council
TempCare Health Plan BENEFITS BROCHURE. Short-Term Health Plan for Individuals and Families
 TempCare Health Plan BENEFITS BROCHURE Short-Term Health Plan for Individuals and Families Blue Cross and Blue Shield of Nebraska is an independent licensee of the Blue Cross and Blue Shield Association.
TempCare Health Plan BENEFITS BROCHURE Short-Term Health Plan for Individuals and Families Blue Cross and Blue Shield of Nebraska is an independent licensee of the Blue Cross and Blue Shield Association.
2015 Medical Plan Summary
 2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
Services and supplies required by Health Care Reform Age and frequency guidelines apply to covered preventive care Not subject to deductible if PPO
 Page 1 of 5 Individual Deductible Calendar year $400 COMBINED Individual / Family OOP Calendar year $4,800 Individual $12,700 per family UNLIMITED Annual Maximum July 1 st to June 30 th UNLIMITED UNLIMITED
Page 1 of 5 Individual Deductible Calendar year $400 COMBINED Individual / Family OOP Calendar year $4,800 Individual $12,700 per family UNLIMITED Annual Maximum July 1 st to June 30 th UNLIMITED UNLIMITED
Blue Cross of NEPA: Custom PPO Option 10014 Coverage Period: 03/01/2015-02/29/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcnepa.com or by calling 1-888-345-2346. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.bcnepa.com or by calling 1-888-345-2346. Important Questions
Coventry Health & Life Insurance Company
 Coventry Health & Life Insurance Company (Benefits underwritten by Coventry Health & Life Insurance Company and Administered by Coventry Health Care of Missouri, Inc.) Small Group PPO Schedule of Benefits:
Coventry Health & Life Insurance Company (Benefits underwritten by Coventry Health & Life Insurance Company and Administered by Coventry Health Care of Missouri, Inc.) Small Group PPO Schedule of Benefits:
Your Plan: Anthem Bronze PPO 5500/30%/6450 w/hsa Your Network: Prudent Buyer PPO
 Your Plan: Anthem Bronze PPO 5500/30%/6450 w/hsa Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Your Plan: Anthem Bronze PPO 5500/30%/6450 w/hsa Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-445-7490. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-445-7490. Important Questions
ROCHESTER INSTITUTE OF TECHNOLOGY 2014 Medical Benefits Comparison Chart Medicare-Eligible Retirees in the Rochester Area
 Contacting the Carrier Voice: (877) 883-9577 TTY: (585) 454-2845 Website: Voice: (800) 665-7924 TTY: (800) 252-2452 Website: www.excellusbcbs.com www.mvphealthcare.com Deductible Carry Over None None Deductible,
Contacting the Carrier Voice: (877) 883-9577 TTY: (585) 454-2845 Website: Voice: (800) 665-7924 TTY: (800) 252-2452 Website: www.excellusbcbs.com www.mvphealthcare.com Deductible Carry Over None None Deductible,
Vision Care Rider. Premier Option. Definitions
 Vision Care Rider Premier Option This Vision Care Rider is made part of, and is in addition to any information you may have in your Blue Cross and Blue Shield of New Mexico (BCBSNM) member benefit booklet
Vision Care Rider Premier Option This Vision Care Rider is made part of, and is in addition to any information you may have in your Blue Cross and Blue Shield of New Mexico (BCBSNM) member benefit booklet
Additional Information Provided by Aetna Life Insurance Company
 Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
Additional Information Provided by Aetna Life Insurance Company Inquiry Procedure The plan of benefits described in the Booklet-Certificate is underwritten by: Aetna Life Insurance Company (Aetna) 151
In-Network: $5,000 self-only / $10,000 family, not to exceed $6,450 from any one person. Does not apply to preventive care or vision hardware.
 Personal Alliance 5000 Bronze ON Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Self Only / Family Plan Type: HMO HSA This
Personal Alliance 5000 Bronze ON Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Self Only / Family Plan Type: HMO HSA This
AVMED POS PLAN. Allergy Injections No charge 30% co-insurance after deductible Allergy Skin Testing $30 per visit 30% co-insurance after deductible
 AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
Important Questions Answers Why this Matters: In-network: $0/Individual; $0/Family Out-of-network: $500/Individual; $1,000/Family
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-445-7490. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com or by calling 1-800-445-7490. Important Questions
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 4X8 of Southern State Community College Enrolling Group Number: 755032
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 4X8 of Southern State Community College Enrolling Group Number: 755032
Personal Alliance 4500 Bronze ON
 Personal Alliance 4500 Bronze ON Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual / Family Plan Type: HMO This is
Personal Alliance 4500 Bronze ON Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2016-12/31/2016 Coverage for: Individual / Family Plan Type: HMO This is
New York Small Group Indemnity Aetna Life Insurance Company Plan Effective Date: 10/01/2010. PLAN DESIGN AND BENEFITS - NY Indemnity 1-10/10*
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
Nationwide Life Insurance Co.: University of Phoenix NJ Coverage Period: 9/24/13-8/23/14
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.chpstudent.com or by calling 1-800-633-7867. Important
Regence BluePoint 20/40 Plan Highlights For Groups of 51+ 1/1/2015
 Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In Network providers. If a member chooses an Out of Network provider, the member
Plan Features Provider choice: Members have direct access to their choice of providers. Coinsurance levels are lowest for In Network providers. If a member chooses an Out of Network provider, the member
Land of Lincoln Health : Family Health Network LLH 3-Tier Bronze PPO Coverage Period: 01/01/2016 12/31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-FHN-4YOU.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-FHN-4YOU.
Highmark Delaware: Shared Cost Blue EPO 3000 Coverage Period: 01/01/2016-12/31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbsde.com or by calling 1-888-601-2242. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.highmarkbcbsde.com or by calling 1-888-601-2242. Important
Important Questions Answers Why this Matters:
 BridgeSpan Health Company: Exchange Silver Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
BridgeSpan Health Company: Exchange Silver Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Summary of Benefits Community Advantage (HMO)
 Summary of Benefits Community Advantage (HMO) January 1, 2015 - December 31, 2015 This booklet gives you a summary of what we cover and what you pay. It doesn't list every service that we cover or list
Summary of Benefits Community Advantage (HMO) January 1, 2015 - December 31, 2015 This booklet gives you a summary of what we cover and what you pay. It doesn't list every service that we cover or list
Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO
 Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
SUMMARY OF BENEFITS. Out-of-Network Care: $10,000 per policy year
 OUTPATIENT BENEFITS Most Primary Care office visits at SHC are provided at no charge. This is not an insured benefit but is provided by NYU to all matriculated students including students who waive the
OUTPATIENT BENEFITS Most Primary Care office visits at SHC are provided at no charge. This is not an insured benefit but is provided by NYU to all matriculated students including students who waive the
Summary of PNM Resources Health Care Benefits Active Employees 2011
 of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
OUTLINE OF COVERAGE. Individual Engage Comprehensive Health Insurance Policy
 OUTLINE OF COVERAGE Individual Engage Comprehensive Health Insurance Policy Policy Number: [123456] Policy Effective Date: [January 1, 2016] Policyowner: [John Doe] Policy Anniversary Date: [January 1
OUTLINE OF COVERAGE Individual Engage Comprehensive Health Insurance Policy Policy Number: [123456] Policy Effective Date: [January 1, 2016] Policyowner: [John Doe] Policy Anniversary Date: [January 1
$0 See the chart starting on page 2 for your costs for services this plan covers. Are there other. deductibles for specific No.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
PPO Schedule of Payments (Maryland Large Group) Qualified High Deductible Health Plan National QA2000-20
 PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
Healthy Benefits PPO 6000.0 - Zero Cost Sharing Plan Variation Coverage Period: Beginning on or after 1/1/2014 Summary of Benefits and Coverage:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
2015 Medicare Advantage Summary of Benefits
 2015 Medicare Advantage Summary of Benefits HNE Medicare Premium No Rx and HNE Medicare Basic No Rx January 1, 2015 - December 31, 2015 H8578_2015_034 Accepted HNE MEDICARE ADVANTAGE ENROLLMENT KIT 2015
2015 Medicare Advantage Summary of Benefits HNE Medicare Premium No Rx and HNE Medicare Basic No Rx January 1, 2015 - December 31, 2015 H8578_2015_034 Accepted HNE MEDICARE ADVANTAGE ENROLLMENT KIT 2015
What is the overall deductible? Are there other deductibles for specific services? Is there an out-of-pocket limit on my expenses?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at capbluecross.com or by calling 1-800-730-7219. Important
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary
 CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
LEGACY PLAN Medical In-Ntwk Out-of-Ntwk
 Preventive Services Age, gender and frequency criteria Adult physical/immunizations Well child visits/immunizations Screenings 0 Co-Insurance (after deductible) Out-of-Pocket Maximums Office Visit (copays)
Preventive Services Age, gender and frequency criteria Adult physical/immunizations Well child visits/immunizations Screenings 0 Co-Insurance (after deductible) Out-of-Pocket Maximums Office Visit (copays)
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.cs.ny.gov/employee-benefits or by calling 1-877-7-NYSHIP
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at https://www.cs.ny.gov/employee-benefits or by calling 1-877-7-NYSHIP
: Blue Cross Blue Shield Silver 1, a Multi-State Plan
 : Blue Cross Blue Shield Silver 1, a Multi-State Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2014 12/31/14 Coverage for: Single Plan Type: EPO This
: Blue Cross Blue Shield Silver 1, a Multi-State Plan Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 1/1/2014 12/31/14 Coverage for: Single Plan Type: EPO This
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Appendix A. Prepared Exclusively for The Dow Chemical Company
 Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
