The results for all specimens sent for TB culture are filed in the TB Office between the main entrance and the Staff Health clinic.
|
|
|
- Alan Tate
- 7 years ago
- Views:
Transcription
1 DIAGNOSIS AND MANAGEMENT OF TUBERCULOSIS The HIV epidemic has greatly increased the incidence of tuberculosis (TB) and complicated TB diagnosis: smear-negative pulmonary TB and extrapulmonary TB account for 60% of total case load. The aim of this policy is to standardize the diagnosis and management of TB. A. Diagnosis of TB 1. Patients who require admission and who are coughing productively should have 2 or more sputum specimens sent for AFB smears within 24 hours of admission. 2. Sputum induction using hypertonic saline and ultrasonic nebulization should be performed within 24 hours of admission for all TB suspects with a non-productive cough [See Policy: Sputum collection and ultrasonic sputum induction]. 3. Ambulant patients who do not require admission and who have been coughing for >2 weeks should be referred to their nearest Primary Health clinic for sputum smears for AFB, according to national guidelines. The Cough Warriors The Cough Warriors are clinical auxiliaries who assist with delivery of TB specimens for AFB to the laboratory and return the results to the patients file. TB Cultures The results for all specimens sent for TB culture are filed in the TB Office between the main entrance and the Staff Health clinic. Note: All TB suspects should be offered testing for HIV infection using the VCT service. I. Sputum smear-positive pulmonary TB (PTB) Note: Mark AFB microscopy ONLY on the sputum form Sputum AFB results should be available in the ward within 48 hours of the sample being sent. Patients with at least one positive smear should be notified with smear-positive TB (note scanty positive result is accepted as positive). II. Sputum smear-negative PTB See Annexures 1 and 2 for the WHO algorithms. Patients can be diagnosed with smear-negative PTB if ALL of the following criteria are met: 1. Cough >2 weeks 2. Two or more sputa smear-negative OR non-productive cough 3. Pulmonary infiltrate compatible with TB present on current CXR (including micronodular OR nodular infiltrates) 4. No clinical response to oral antibiotics after 2 weeks OR intravenous antibiotics after 3 days 5. Pneumocystis pneumonia excluded clinically 6. Decision by a clinician at the level of Senior Medical Officer or above to commit the patient to a full course of antituberculous therapy Patients meeting all criteria should be notified with smear-negative PTB
2 Requesting TB culture and sensitivities TB culture should be requested if: 1. A patient is being re-treated for TB 2. If the patient is diagnosed with smear-negative TB, pleural TB, extrapulmonary TB 3. A patient is sputum smear-positive after 7-11 weeks of TB therapy (failure to convert) 4. A patient is referred for failure to thrive ( non-responder ) after 2-8 weeks of TB therapy (see definition below) 5. A patient is an MDRTB suspect (see definition below) Sputum culture has the highest yield - ask for an induced specimen for patients with nonproductive cough or prescribe nebulised saline. Pleural aspirate, ascites aspirate, cold abscess aspirate can be inoculated into a myco-f-lytic culture bottle. Note: Mark AFB microscopy, culture and sensitivity and indication for request (e.g. retreatment case, failure to thrive on TB treatment) III. Pleural TB Diagnose pleural TB if: 1. A pleural aspirate returns fluid 2. Fluid clinically has a high protein content (straw colour, 4+ protein on dipstick) OR protein clot forms on standing. 3. Empyema excluded on clinical examination of aspirated fluid (i.e. fluid not cloudy or purulent and ph >5 on dipstick) If pleural malignancy suspected (age 45 years, blood-stained effusion): 1. Assess smoking history, and other features of malignancy (e.g. breast mass; hard, enlarged lymph nodes; hoarseness; chest pain) 2. Send fluid for cytology (half fluid, half alcohol solution [kept in schedule 6 cupboard]) Note: in equivocal cases send fluid total protein, serum total protein and bacterial culture; pleural biopsy can be subsequently performed. IV Extrapulmonary TB (EPTB) EPTB should be diagnosed in patients with constitutional symptoms (fever, weight loss, night sweats, fatigue) by a specialist, CMO, PMO or registrar based on: 1. Mediastinal or intra-abdominal lymphadenopathy 2. Peripheral lymphadenopathy asymmetric lymphadenopathy with caseating granuloma or giant cells seen on cytology or histology 3. Pericardial effusion >10mm in diameter 4. Ascitic exudates (serum albumin to fluid albumin gradient <11) send specimen for cytology in alcohol if malignancy suspected Note: 1. TB arthritis is diagnosed on arthoscopic synovial biopsy; TB spine should be diagnosed on MRI. These cases are managed by the Department of Orthopaedic Surgery 2. TB peritionitis is diagnosed on imaging, with or without laparoscopy. These cases are managed by the Department of General Surgery contact Dr Islam, Department of Surgery. V TB meningitis (TBM) TBM should be diagnosed by a specialist, CMO, PMO or registrar based on CSF analysis showing: 1. Duration of symptoms >5 days 2. Pleiocytosis (usually with lymphocytic predominance) 3. Elevated protein and low glucose (gradient <0.5 calculated using blood glucose or finger prick glucose OR glucose <1.9)
3 B. Management of TB TB should be treated according to national guidelines with fixed dosed combination therapy according to weight. Streptomycin should be added for patients receiving retreatment for TB. Doses are calculated according to weight - see below. [Reference: South African Medicines Formulary 7 th Edition 2005 page ] TB pericarditis and miliary TB: Prednisone should be added: 80 mg daily for 7 days, then 60 mg daily for 7 days, then 40 mg daily for 7 days, then 20 mg daily for 7 days, then 10 mg daily 7 days, then 5 mg daily for 7 days TBM: Dexamethazone intravenously should be added (0.4 mg per kilogram per day for week 1, 0.3 mg per kilogram per day for week 2, 0.2 mg per kilogram per day for week 3, and 0.1 mg per kilogram per day for week 4) and then oral treatment for four weeks, starting at a total of 4 mg per day and decreasing by 1 mg each week. Usual therapy would be 8 mg tds for 7 days, then 6 mg tds for 7 days, then 4 mg tds for 7 days, then 2 mg tds for 7 days, then 2 mg bd for 28 days, decreasing by 1 mg per week. If oral dexamethazone is not available prednisone or dexamethazone can be substituted, at a starting dose of prednisone 80 mg bid or betamethazone 10 mg bid. Note: Iron supplementation should not be given to patients with TB unless iron deficiency has been diagnosed using iron studies Record keeping The details of all TB suspects should be entered in the TB suspect register, and the final diagnosis documented. Referral to the TB clinic Patients referred to the TB clinic should have: 1. Discharge summary (if inpatient) 2. TB referral form (pink) 3. Seven days of TB medication from the pharmacy 4. Counselling from the TB team on how to access TB therapy from the Primary Health Care Clinics 5. A Zulu TB information pamphlet giving details of the District TB control system First-line antituberculous drugs Drugs Mode of Potency Recommended dose for action (mg/kg of body weight) Isoniazid (H) bactericidal high 5 Rifampicin (R) bactericidal high 10 Pyrazinamide (Z) bactericidal low 25 Streptomycin (S) bactericidal low 15 Ethambutol (E) bacteriostatic low 15 Rifafour e-275 (each tablet contains): Rifampicin 150 mg Isoniazid 75 mg Pyrazinamide 400 mg Ethambutol 275 mg
4 Example of recommended treatment dosages, kg 2 tablets kg 3 tablets kg 4 tablets 71 kg and over 5 tablets RIFINAH-150: RIFINAH-300: Patients weighing less than 50 kg: 3 tablets (450 mg rifampicin and 300 mg isoniazid). Patients weighing 50 kg or greater: 2 tablets (600 mg rifampicin and 300 mg isoniazid). All TB medications given 5 times per week Duration of treatment at the clinic New case regimen: Months 1-2: H / R / Z / E Months 3-6: H/R Re-treatment regimen: Months 1-2: H / R / Z / E / S (40 doses of S IM) Month 3: H / R / Z / E Months 4-8: H / R / E Reasons for structure of re-treatment regimen Aim is to achieve relapse-free cure Prolonged therapy needed due to presence of dormant / latent organisms (persisters) Combination therapy to prevent development of drug resistance Single drug resistant mutations may be present at initiation of therapy due to high number of organisms present Three bactericidal drugs given in intensive phase will rapidly reduce number of organisms and reduce the risk of resistance developing Inclusion of Z allows duration of treatment to be shortened E included for duration of treatment to cover for H resistance present Common side-effects of TB treatment Severe Jaundice due to drug-induced hepatitis Z most likely cause stop all drugs and refer for re-introduction under specialist supervision E and S not hepatotoxic Skin rash can be caused by all drugs stop all drugs and refer for re-introduction under specialist supervision Hearing loss, vertigo, renal impairment due to S Visual loss due to prolonged use of E stop E - assessment of colour vision and ophthalmologist review Sensory peripheral neuropathy common caused by H can be prevented / treated by pyridoxine HIV neuropathy identical presentation Minor Nausea, vomiting Itch Athralgia Other medications: Pyridoxine mg daily (to prevent INH neurotoxicity) Co-trimoxazole 480 mg 1-2 tabs daily (for PLWH to prevent opportunistic infections, shown to improve survival in RCT)
5 Operational: Notification and registration with TB clinic, cough hygiene Directly observed therapy if possible for entire duration of treatment Completion of Green Card to record adherence to therapy Application for disability grant for duration of therapy (if needed) Nutritional assessment Monitoring New smear-positive case: Repeat sputum smears at the end of month 2 and month 5 - if positive at month 5 register as treatment failure send sputum for culture and DST - review in 6 weeks Re-treatment smear-positive case: Follow-up initial smear and culture status Review culture and DST results at 6 weeks refer if drug resistance present Repeat two sputum smears sent at the end of month 3 and month 7 If smear positive at 3 months - repeat culture If smear positive at 7 month register as treatment failure and refer Weigh regularly, adjust drug doses Smear-negative cases: Smear-negative PTB and pleural TB: Duration as for smear-positive PTB (new case and retreatment) - clinical reassessment at weeks 2 and 4, with clinical and culture review at week 8. Repeat cultures if necessary. Final clinical review at months 3 and 4. At clinical review assess symptoms and level of functioning.* EPTB excluding TBM and TB lymphadenitis: as for smear-positive TB TBM and TB lymphadenitis: New case as for smear + PTB, with continuation phase extended by 3 months for total of 9 months Rx (with option of extending to 12 months). Re-treatment case as for smear-negative PTB with continuation phase extended for 4 months to give total of 12 months Rx. Clinical review as for smear negative PTB, with visual acuity checks at months 3, 6, 9, (12 for re-treatments). *Focal symptoms (including cough), fever, fatigue, weight loss, should have resolved after 8 weeks of treatment. Weight gain implies successful treatment. Level of functioning is determined clinically - successful treatment implies that the patient should be able to return to normal way of life. Untreated HIV infection or post-tb lung disease can make response to treatment more difficult to assess. HIV-positive patients: Repeat CD4 count six monthly after initial count Initiate antiretroviral training if CD4 <200 or AIDS-defining diagnosis develops Follow-up of TB cases at MOPD The following patients should be seen at MOPD at 4 weeks and 8 weeks if not responding well to treatment. 1. TBM: to review neurological status and assess need for ventriculoperitoneal shunt. 2. Pericardial TB: to assess for features of pericardial tamponade or constriction. 3. Pleural TB: to exclude empyema or malignancy TB clinic nurses should refer patients in for review if there is failure to thrive after 8 weeks of TB treatment based on: 1. Weight loss 2. Fatigue 3. Persisting focal symptoms (e.g. cough, lymph node enlargement, pleural effusion) Note: Patients with smear-negative TB should not be referred back to MOPD for chest X-ray at treatment completion UNLESS there are symptoms suggestive of persisting TB (see above).
6 C. Multidrug Resistant TB (MDRTB) MDRTB is becoming increasingly common in KwaZulu-Natal. The severity of this problem and its public health implications should not be underestimated. Definitions of TB drug resistance Mono-resistance: Resistance to one of the first line TB drugs Poly-resistance: Resistance to two or more first line TB drugs Multi-drug resistance: Resistance to isoniazid and rifampicin XDRTB: Resistance to most or all first line and second line TB drugs including isoniazid and rifampicin Note: Patients with mono-resistance or poly-resistance other than multi-drug resistance or XDRTB are frequently cured by standard four-drug therapy. Patients with multi-drug resistance or XDRTB are never cured by standard four drug therapy. Definitions of MDRTB suspect 1. Any patient who is sputum smear positive after 2 months of TB therapy AND culture/sensitivity tests have been sent 2. Any patient who is failing to thrive after 2 months of TB therapy and has signs of a deteriorating focal disease process compatible with tuberculosis AND culture/sensitivity tests have been sent 3. Any TB suspect who has been in contact with a patient known to have MDRTB AND culture/sensitivity tests have been sent Management of MDRTB suspects: Admission: MDRTB cases or suspects should preferably be managed at home. Rationale: fewer people will come into contact with the patient at home than in a crowded hospital ward. Please ensure that outpatients have a good sputum specimen sent for culture and DST - label the form very clearly MDRTB suspect or MDRTB case. MDRTB cases or suspects can only be admitted if: There is an intercurrent illness (e.g. pneumonia) that needs inpatient treatment Advanced TB alone is not an indication for admission (infection control risks outweigh benefit to patient). MDRTB suspects who need admission should be admitted to the isolation cubicle after a Consultant has assessed the case. The Consultant should sign the transfer on the front of the case sheet. Note: It is compulsory that all Healthcare Workers who enter the MDRTB isolation cubicles wear a closely fitted N95 mask. Only two designated family members can visit the patient in the cubicle wearing compulsory N95 masks (each patient is assigned two N95 masks for visitors) All suspected MDRTB cases on admission should be taught cough hygiene, taught how to wear a surgical mask and presented to a consultant within 24 hours of admission. If the diagnosis of MRTB suspect is confirmed by the consultant the patient should remain in the isolation ward or cubicle.
7 Day 1: Enter the patient s name onto the TB suspect register. The patient is started on intravenous coamoxyclav 1,2 g IV 8 hourly with erythromycin 500 mg 6 hourly and TWO sputum specimens are sent for AFB smear. A THIRD specimen is sent for TB culture and DST. All forms must include the patient s national ID number and contact details. Day 3: The patient s case and sputum smear results is reviewed with an infectious diseases consultant. Day 5-7: The patient s case is reviewed again with in infectious diseases consultant, response to antibiotic therapy is assessed, and a decision whether or not to start empiric MDRTB therapy is made (usually it is NOT started). Safe arrival of the specimen at IALH TB lab must be confirmed by the registrar. ARV therapy is initiated if needed. Further: If empiric MDRTB therapy is started the patient is kept in the isolation cubicle until the DST becomes available. If empiric MDRTB therapy is not started the patient can be discharged home and asked to return for DST results within 4 to 6 weeks or immediately if deterioration occurs. Family members must receive education and counselling by the TB Coordinator, Infection Control or an appropriately trained person under their supervision: Infection risks in the home, details of MDRTB treatment, duration and side-effects The patient sleeps alone in room with open window; Family members who HIV-infected, diabetic, very young or very old should move out of the house The patient follows cough hygiene (coughs into cupped hands that are frequently washed, or a tissue which is thrown away) and wears a surgical mask when in other rooms of the house. Definition of MDRTB 1. Any patient with a TB culture resistant to both isoniazid and rifampicin Management of MDRTB 1. All MDRTB suspects should have full traceable (including two active cellphone numbers) contact details in MDRTB suspect register entered by the TB Coordinator (or a designated supervised staff member) 2. All MDRTB suspects or MDRTB cases should be discussed with the doctor on call at King George Hospital, or a medical specialist or infectious diseases specialist. 3. MDRTB suspects or cases should be nursed in the side cubicles of 5B1 and 5F 4. All staff in contact with MDRTB suspects or cases should use fitted N95 masks that can be obtained from the Unit Manager 5. The minimum amount of time an N95 mask can be used for is 7 days of continuous use, the maximum amount of time an N95 mask can be used for is 14 days 6. Less ill patients can be managed as outpatients while waiting for sensitivity results 7. If the decision is made to treat for MDRTB at least three to four effective drugs should be prescribed in consultation with an MDRTB specialist 8. Patients being treated for MDRTB should be transferred to the Doris Goodwin TB Hospital, Richmond Chest or King George V Hospital for ongoing therapy. Management of poly-resistance other than MDRTB Treatment of poly-resistance other than MDRTB should be individualized after discussion with a specialist. Note: A single drug should never be added to a failing regimen
GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA
 GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA 2010 1 TB prophylaxis GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS Background
GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS IN SOUTH AFRICA 2010 1 TB prophylaxis GUIDELINES FOR TUBERCULOSIS PREVENTIVE THERAPY AMONG HIV INFECTED INDIVIDUALS Background
TB Prevention, Diagnosis and Treatment. Accelerating advocacy on TB/HIV 15th July, Vienna
 TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
TB Prevention, Diagnosis and Treatment Accelerating advocacy on TB/HIV 15th July, Vienna Diagnosis Microscopy of specially stained sputum is the main test for diagnosing TB (1 2 days) TB bacilli seen in
2011 NTP Paediatric guidelines update- final draft
 Childhood TB Investigation and management of children suspected to have tuberculosis (TB) or who are close contacts of a TB case (sputum smear positive or negative) Key facts Children who are close contacts
Childhood TB Investigation and management of children suspected to have tuberculosis (TB) or who are close contacts of a TB case (sputum smear positive or negative) Key facts Children who are close contacts
TB preventive therapy in children. Introduction
 TB preventive therapy in children H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg Children s Hospital Introduction Children are
TB preventive therapy in children H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg Children s Hospital Introduction Children are
Management of Tuberculosis (TB)
 for Professional Health Care Providers Management of Tuberculosis (TB) USAID UNITED STATES AGENCY INTERNATIONAL DEVELOPMENT USAID FROM THE AMERICAN PEOPLE SOUTHERN AFRICA WHAT IS TB? Tuberculosis (TB)
for Professional Health Care Providers Management of Tuberculosis (TB) USAID UNITED STATES AGENCY INTERNATIONAL DEVELOPMENT USAID FROM THE AMERICAN PEOPLE SOUTHERN AFRICA WHAT IS TB? Tuberculosis (TB)
TB CARE EARLY DETECTION AND PREVENTION OF TUBERCULOSIS (TB) IN CHILDREN. Risk factors in children acquiring TB:
 EARLY DETECTION AND PREVENTION OF TUBERCULOSIS (TB) IN CHILDREN Risk factors in children acquiring TB: Children living in the same household as a lung TB patient (especially children under 5) Children
EARLY DETECTION AND PREVENTION OF TUBERCULOSIS (TB) IN CHILDREN Risk factors in children acquiring TB: Children living in the same household as a lung TB patient (especially children under 5) Children
Treatment of Tuberculosis
 Treatment of Tuberculosis 1a Taking TB Treatment 2 Learning outcomes Describe the use of TB case definitions & the management of TB patients Successfully treat TB using the appropriate regimen for the
Treatment of Tuberculosis 1a Taking TB Treatment 2 Learning outcomes Describe the use of TB case definitions & the management of TB patients Successfully treat TB using the appropriate regimen for the
MANAGEMENT OF TUBERCULOSIS
 MANAGEMENT OF TUBERCULOSIS Dean B. Ellithorpe, M.D. Clinical Professor of Medicine Section of Pulmonary Diseases, Critical Care and Environmental Medicine Tulane University School of Medicine INTRODUCTION
MANAGEMENT OF TUBERCULOSIS Dean B. Ellithorpe, M.D. Clinical Professor of Medicine Section of Pulmonary Diseases, Critical Care and Environmental Medicine Tulane University School of Medicine INTRODUCTION
LEARNING OUTCOMES. Identify children at risk of developing TB disease. Correctly manage and refer children suspected of TB. Manage child contacts
 TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
TB in Children 1a TB IN CHILDREN 2 LEARNING OUTCOMES Identify children at risk of developing TB disease Correctly manage and refer children suspected of TB Manage child contacts 3 TB Infection and Disease
Tuberculosis Care with TB-HIV Co-management
 WHO/HTM/HIV/2007.01 WHO/HTM/TB/2007.380 April 2007 Tuberculosis Care with TB-HIV Co-management INTEGRATED MANAGEMENT OF ADOLESCENT AND ADULT ILLNESS (IMAI) T B HIV WHO Library Cataloguing-in-Publication
WHO/HTM/HIV/2007.01 WHO/HTM/TB/2007.380 April 2007 Tuberculosis Care with TB-HIV Co-management INTEGRATED MANAGEMENT OF ADOLESCENT AND ADULT ILLNESS (IMAI) T B HIV WHO Library Cataloguing-in-Publication
Tuberculosis and You A Guide to Tuberculosis Treatment and Services
 Tuberculosis and You A Guide to Tuberculosis Treatment and Services Tuberculosis (TB) is a serious disease that can damage the lungs or other parts of the body like the brain, kidneys or spine. There are
Tuberculosis and You A Guide to Tuberculosis Treatment and Services Tuberculosis (TB) is a serious disease that can damage the lungs or other parts of the body like the brain, kidneys or spine. There are
Clinical description 2 Laboratory test for diagnosis 3. Incubation period 4 Mode of transmission 4 Period of communicability 4
 Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
Tuberculosis Contents Epidemiology in New Zealand 2 Case definition 2 Clinical description 2 Laboratory test for diagnosis 3 Case classification 3 Spread of infection 4 Incubation period 4 Mode of transmission
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS
 AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS (UPDATE 2004) Internal guidelines of the Tuberculosis & Chest Service of the Department of Health
AMBULATORY TREATMENT AND PUBLIC HEALTH MEASURES FOR A PATIENT WITH UNCOMPLICATED PULMONARY TUBERCULOSIS (UPDATE 2004) Internal guidelines of the Tuberculosis & Chest Service of the Department of Health
12 Points of Tuberculosis (TB) Patient Education
 12 Points of Tuberculosis (TB) Patient Education Transmission of TB TB is a disease caused by the TB germ. The disease is mainly in the lungs (pulmonary TB), but the germ can travel to other parts of the
12 Points of Tuberculosis (TB) Patient Education Transmission of TB TB is a disease caused by the TB germ. The disease is mainly in the lungs (pulmonary TB), but the germ can travel to other parts of the
Management of Tuberculosis: Indian Guidelines
 Chapter 105 Management of Tuberculosis: Indian Guidelines Kuldeep Singh Sachdeva INTRODUCTION Tuberculosis (TB) is an infectious disease caused predominantly by Mycobacterium tuberculosis and among the
Chapter 105 Management of Tuberculosis: Indian Guidelines Kuldeep Singh Sachdeva INTRODUCTION Tuberculosis (TB) is an infectious disease caused predominantly by Mycobacterium tuberculosis and among the
TB at Edendale Hospital: Operational Guidelines for Doctors and Nurses. Dr. Michael Clark Medical Officer Edendale Hospital
 TB at Edendale Hospital: Operational Guidelines for Doctors and Nurses Dr. Michael Clark Medical Officer Edendale Hospital The Burden What? Tuberculosis (TB) HIV/TB co-infection Drug resistance Where?
TB at Edendale Hospital: Operational Guidelines for Doctors and Nurses Dr. Michael Clark Medical Officer Edendale Hospital The Burden What? Tuberculosis (TB) HIV/TB co-infection Drug resistance Where?
Self-Study Modules on Tuberculosis
 Self-Study Modules on Tuberculosis Treatment of Latent Tuberculosis Infection and Tube rc ulos is Disease U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National
Self-Study Modules on Tuberculosis Treatment of Latent Tuberculosis Infection and Tube rc ulos is Disease U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Disease Control and Prevention National
Desk-guide for diagnosis and management of TB in children
 Desk-guide for diagnosis and management of TB in children 2 Desk-guide for diagnosis and management of TB in children 2010 3 International Union Against Tuberculosis and Lung Disease (The Union) 68 Boulevard
Desk-guide for diagnosis and management of TB in children 2 Desk-guide for diagnosis and management of TB in children 2010 3 International Union Against Tuberculosis and Lung Disease (The Union) 68 Boulevard
Pediatric Latent TB Diagnosis and Treatment
 Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Date Updated: April 2015 Guidelines Reviewed: 1. CDC Latent TB Guidelines 2. Harborview Pediatric Clinic Latent TB Management, 2010 3. Pediatric Associates Latent TB Guidelines, 2013 4. Seattle Children
Pregnancy and Tuberculosis. Information for clinicians
 Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Pregnancy and Tuberculosis Information for clinicians When to suspect Tuberculosis (TB)? Who is at risk of TB during pregnancy? Recent research suggests that new mothers are at an increased risk of TB
Tuberculosis: FAQs. What is the difference between latent TB infection and TB disease?
 Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY. Stephanie N. Lin MD 2/12/2016
 TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
TUBERCULOSIS SCREENING AND TREATMENT IN PREGNANCY Stephanie N. Lin MD 2/12/2016 Epidemiology of TB 9.6 million new cases in 2014 12% of them are in HIV positive patients 1.5 million deaths in 2014 ~646
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams
 MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams Document control Title Type Author/s Management of tuberculosis in prisons: Guidance for prison healthcare teams Operational
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015
 Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Treatment of tuberculosis. guidelines. Fourth edition
 Treatment of tuberculosis guidelines Fourth edition Treatment of tuberculosis Guidelines Fourth edition WHO Library Cataloguing-in-Publication Data: Treatment of tuberculosis: guidelines 4th ed. WHO/HTM/TB/2009.420
Treatment of tuberculosis guidelines Fourth edition Treatment of tuberculosis Guidelines Fourth edition WHO Library Cataloguing-in-Publication Data: Treatment of tuberculosis: guidelines 4th ed. WHO/HTM/TB/2009.420
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention
 U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention National Center for HIV, STD, and TB Prevention Division of Tuberculosis Elimination Public
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service Centers for Disease Control and Prevention National Center for HIV, STD, and TB Prevention Division of Tuberculosis Elimination Public
Gaps in the diagnosis and management of severe TB in children Red Flags
 This presentation is provided on the South African Child Health Priorities Website as presented at the 5 th Child Health Priorities Conference except that potential patient identifying content has been
This presentation is provided on the South African Child Health Priorities Website as presented at the 5 th Child Health Priorities Conference except that potential patient identifying content has been
Tuberculousmeningitis: what is the best treatment regimen?
 Tuberculousmeningitis: what is the best treatment regimen? H S Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Faculty of Medicine and Health Sciences, Stellenbosch University
Tuberculousmeningitis: what is the best treatment regimen? H S Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Faculty of Medicine and Health Sciences, Stellenbosch University
New York City Department of Health Protocols for Latent TB Infection Treatment
 New York City Department of Health Protocols for Latent TB Infection Treatment CONTENT A. Medical evaluation for latent TB infection (LTBI) treatment 1. Medical history and physical examination 2. Chest
New York City Department of Health Protocols for Latent TB Infection Treatment CONTENT A. Medical evaluation for latent TB infection (LTBI) treatment 1. Medical history and physical examination 2. Chest
Clinical Scenarios In Childhood TB. Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C
 Clinical Scenarios In Childhood TB Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C Objectives: To present different commonly encountered clinical scenarios
Clinical Scenarios In Childhood TB Josefina Cadorna Carlos M.D., FPPS, FPIDSP, FSMID Associate Professor of Pediatrics U E R M M M C Objectives: To present different commonly encountered clinical scenarios
You. guide to tuberculosis treatment and services
 Adapted from TB and You: A Guide to Tuberculosis Treatment and Services with permission from Division of Public Health TB Control Program State of North Carolina Department of Health and Human Services
Adapted from TB and You: A Guide to Tuberculosis Treatment and Services with permission from Division of Public Health TB Control Program State of North Carolina Department of Health and Human Services
Tuberculosis And Diabetes. Dr. hanan abuelrus Prof.of internal medicine Assiut University
 Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Tuberculosis And Diabetes Dr. hanan abuelrus Prof.of internal medicine Assiut University TUBERCULOSIS FACTS More than 9 million people fall sick with tuberculosis (TB) every year. Over 1.5 million die
Tuberculosis Case Management in Prisoners
 Tuberculosis Case Management in Prisoners Joint Protocol for Corrections Facilities and TB Treatment Supervising Services (Regional Public Health Services and/or Clinical TB Services) in New Zealand Ministry
Tuberculosis Case Management in Prisoners Joint Protocol for Corrections Facilities and TB Treatment Supervising Services (Regional Public Health Services and/or Clinical TB Services) in New Zealand Ministry
Tuberculosis. Subject. Goal/Objective. Instructions. Rationale. Operations Directorate, Health Branch Immigration Medical Examination Instructions
 Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Subject Instructions for the screening of clients to detect tuberculosis (TB) in the context of the Canadian immigration medical examination (IME). Goal/Objective These instructions are provided to ensure
Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults)
 Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults) H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg
Screening and preventive therapy for MDR/XDR-TB exposed/infected children (and adults) H S Schaaf Department of Paediatrics and Child Health, and Desmond Tutu TB Centre Stellenbosch University, and Tygerberg
Chapter 6 Treatment of Tuberculosis Disease
 Chapter 6 Treatment of Tuberculosis Disease Table of Contents Chapter Objectives.... 139 Introduction.... 141 Treatment and Monitoring Plan.... 143 Adherence Strategies... 143 TB Disease Treatment Regimens....
Chapter 6 Treatment of Tuberculosis Disease Table of Contents Chapter Objectives.... 139 Introduction.... 141 Treatment and Monitoring Plan.... 143 Adherence Strategies... 143 TB Disease Treatment Regimens....
QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS Ministry of Health Malaysia Academy of Medicine Malaysia Malaysian Thoracic Society KEY MESSAGES 1. Tuberculosis (TB) is a notifiable infectious disease. Timely
QUICK REFERENCE FOR HEALTHCARE PROVIDERS Ministry of Health Malaysia Academy of Medicine Malaysia Malaysian Thoracic Society KEY MESSAGES 1. Tuberculosis (TB) is a notifiable infectious disease. Timely
Patient Education CONTENTS. Introduction... 12.2
 CONTENTS Introduction... 12.2 Purpose... 12.2 General Guidelines... 12.3 Language and Comprehension Barriers... 12.4 Education Topics... 12.5 Medical Diagnosis... 12.5 Contact Investigation... 12.6 Isolation...
CONTENTS Introduction... 12.2 Purpose... 12.2 General Guidelines... 12.3 Language and Comprehension Barriers... 12.4 Education Topics... 12.5 Medical Diagnosis... 12.5 Contact Investigation... 12.6 Isolation...
X-Plain Pediatric Tuberculosis Reference Summary
 X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
X-Plain Pediatric Tuberculosis Reference Summary Introduction Tuberculosis, or TB, is a bacterial infection that causes more deaths in the world than any other infectious disease. When a child gets TB,
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT
 TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
TUBERCULOSIS PLEURAL EFFUSION - MANAGEMENT Introduction : ETB 15-20% Pleural effusion 20% in non HIV Under reporting because of AFB negative in fluid In HIV patients: EPTB 20% PTB + EPTB 50% Pleural Effusion
MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol)
 MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol) 1. Hepatotoxicity: In Active TB Disease a. Background: 1. Among the 4 standard anti-tb drugs,
MANAGEMENT OF COMMON SIDE EFFECTS of INH (Isoniazid), RIF (Rifampin), PZA (Pyrazinamide), and EMB (Ethambutol) 1. Hepatotoxicity: In Active TB Disease a. Background: 1. Among the 4 standard anti-tb drugs,
Guideline. Treatment of tuberculosis in adults and children Version 2.1 July 2015
 Guideline Treatment of tuberculosis in adults and children Version 2.1 July 2015 Contents What this guideline covers:... 1 What this guideline does not cover:... 1 Standard regimens for pulmonary tuberculosis...
Guideline Treatment of tuberculosis in adults and children Version 2.1 July 2015 Contents What this guideline covers:... 1 What this guideline does not cover:... 1 Standard regimens for pulmonary tuberculosis...
Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB).
 Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB). Author: Responsible Lead Executive Director: Endorsing Body: Governance or Assurance Committee
Policy for the control and management of Tuberculosis (TB) including multi-drug resistant Tuberculosis (MDR-TB). Author: Responsible Lead Executive Director: Endorsing Body: Governance or Assurance Committee
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG
 TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
TUBERCULOSIS (TB) SCREENING GUIDELINES FOR RESIDENTIAL FACILITIES AND DRUG Tx CENTERS Tuberculosis Control Program Health and Human Services Agency San Diego County INTRODUCTION Reducing TB disease requires
In Tanzania, ARVs were introduced free-of-charge by the government in 2004 and, by July 2008, almost 170,000 people were receiving the drugs.
 ANTIRETROVIRAL TREATMENT What is ART and ARV? ART is a short form for Antiretroviral Therapy (or Treatment). Antiretroviral therapy is a treatment consisting of a combination of drugs which work against
ANTIRETROVIRAL TREATMENT What is ART and ARV? ART is a short form for Antiretroviral Therapy (or Treatment). Antiretroviral therapy is a treatment consisting of a combination of drugs which work against
DIRECTLY OBSERVED TREATMENT SHORT-COURSE (DOTS)
 DIRECTLY OBSERVED TREATMENT SHORT-COURSE (DOTS) Protocol for Tuberculosis Demonstration Projects in Russia U.S. Centers for Disease Control and Prevention and U.S. Agency for International Development
DIRECTLY OBSERVED TREATMENT SHORT-COURSE (DOTS) Protocol for Tuberculosis Demonstration Projects in Russia U.S. Centers for Disease Control and Prevention and U.S. Agency for International Development
Referral Guidelines for TB/HIV co-management. (First Edition)
 Referral Guidelines for TB/HIV co-management (First Edition) Government of Lesotho April 2011 1 REFERRAL GUIDELINES FOR TB/HIV CO-MANAGEMENT INTRODUCTION Many TB patients are infected with HIV. Many people
Referral Guidelines for TB/HIV co-management (First Edition) Government of Lesotho April 2011 1 REFERRAL GUIDELINES FOR TB/HIV CO-MANAGEMENT INTRODUCTION Many TB patients are infected with HIV. Many people
PEOSH Model Tuberculosis Infection Control Program
 PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
PEOSH Model Tuberculosis Infection Control Program Revised November, 2004 NOTE: The information in this document is not considered to be a substitute for any provision of the PEOSH Act or for any standards
Management of HIV and TB Co-infection in South Africa
 Management of HIV and TB Co-infection in South Africa Halima Dawood Department of Medicine Case Report 39 yr old female Referred to clinic on 14/06/2006 for consideration to commence antiretroviral therapy
Management of HIV and TB Co-infection in South Africa Halima Dawood Department of Medicine Case Report 39 yr old female Referred to clinic on 14/06/2006 for consideration to commence antiretroviral therapy
Guideline. Treatment of tuberculosis in pregnant women and newborn infants. Version 3.0
 Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Guideline Treatment of tuberculosis in pregnant women and newborn infants Version 3.0 Key critical points The decision to treat tuberculosis (TB) in pregnancy must consider the potential risks to mother
Appendix B: Provincial Case Definitions for Reportable Diseases
 Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Tuberculosis Revised August 2015 Tuberculosis 1.0 Provincial Reporting Confirmed and suspect cases
Substance misuse and TB: Information for families affected
 Substance misuse and TB: Information for families affected What is TB? TB is the short name for an infectious disease called tuberculosis. You can get TB by prolonged and close contact with someone who
Substance misuse and TB: Information for families affected What is TB? TB is the short name for an infectious disease called tuberculosis. You can get TB by prolonged and close contact with someone who
San Francisco Treatment Guidelines for Latent Tuberculosis Infection
 City and County of San Francisco Department of Public Health Tuberculosis Control Unit Julie Higashi, MD, PhD Director Population Health Division Edwin M. Lee Mayor Disease Prevention and Control Branch
City and County of San Francisco Department of Public Health Tuberculosis Control Unit Julie Higashi, MD, PhD Director Population Health Division Edwin M. Lee Mayor Disease Prevention and Control Branch
Tuberculosis in Children and Adolescents
 Tuberculosis in Children and Adolescents Ritu Banerjee, MD, Ph.D TB Clinical Intensive April 8, 2015 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Describe the epidemiology of pediatric
Tuberculosis in Children and Adolescents Ritu Banerjee, MD, Ph.D TB Clinical Intensive April 8, 2015 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Describe the epidemiology of pediatric
GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN
 GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 health Department: Health REPUBLIC OF SOUTH AFRICA GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 Published by the Department
GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 health Department: Health REPUBLIC OF SOUTH AFRICA GUIDELINES FOR THE MANAGEMENT OF TUBERCULOSIS IN CHILDREN 2013 Published by the Department
Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children
 Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children Celia DC Christie-Samuels Professor of Paediatrics (Infectious Diseases, Epidemiology and Public Health) University
Childhood Tuberculosis: Diagnosis, Treatment and Prevention of TB in HIV-infected Children Celia DC Christie-Samuels Professor of Paediatrics (Infectious Diseases, Epidemiology and Public Health) University
Recent Advances in The Treatment of Mycobacterium Tuberculosis
 Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Recent Advances in The Treatment of Mycobacterium Tuberculosis Dr Mohd Arif Mohd Zim Senior Lecturer & Respiratory Physician Faculty of Medicine, Universiti Teknologi MARA mohdarif035@salam.uitm.edu.my
Cryptococcal Screening Program Case Studies
 Slide 1 Cryptococcal Screening Program Case Studies Image courtesy of World Health Organization National Center for Emerging and Zoonotic Infectious Diseases Mycotic Diseases Branch Slide 2 Note to trainers
Slide 1 Cryptococcal Screening Program Case Studies Image courtesy of World Health Organization National Center for Emerging and Zoonotic Infectious Diseases Mycotic Diseases Branch Slide 2 Note to trainers
Guideline. Treatment of tuberculosis in patients with HIV co-infection. Version 3.0
 Guideline Treatment of tuberculosis in patients with HIV co-infection Version 3.0 Key critical points Co-infection with Tuberculosis (TB) and HIV is common in many parts of the world, especially sub-saharan
Guideline Treatment of tuberculosis in patients with HIV co-infection Version 3.0 Key critical points Co-infection with Tuberculosis (TB) and HIV is common in many parts of the world, especially sub-saharan
Tuberculosis. Clinical diagnosis and management of tuberculosis, and measures for its prevention and control
 Issue date: March 2011 Tuberculosis Clinical diagnosis and management of tuberculosis, and measures for its prevention and control This updates and replaces NICE clinical guideline 33 NICE clinical guideline
Issue date: March 2011 Tuberculosis Clinical diagnosis and management of tuberculosis, and measures for its prevention and control This updates and replaces NICE clinical guideline 33 NICE clinical guideline
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Chapter Four: Treatment of Tuberculosis Disease
 Chapter Four: Treatment of Tuberculosis Disease The standard of tuberculosis (TB) treatment in Los Angeles County (LAC) is to initiate an appropriate chemotherapeutic regimen along with Directly Observed
Chapter Four: Treatment of Tuberculosis Disease The standard of tuberculosis (TB) treatment in Los Angeles County (LAC) is to initiate an appropriate chemotherapeutic regimen along with Directly Observed
BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC
 BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC HIV What are HIV and AIDS? HIV stands for Human Immunodeficiency Virus. This is the virus that causes AIDS. HIV is
BASIC INFORMATION ABOUT HIV, HEPATITIS B and C, and TUBERCULOSIS Adapted from the CDC HIV What are HIV and AIDS? HIV stands for Human Immunodeficiency Virus. This is the virus that causes AIDS. HIV is
Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015
 Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015 Completion of Treatment: Case Studies or A Little Bit of Everything Presented by Cherie Fulk February 25, 2015 Cherie Fulk
Introduction to TB Nurse Case Management Online February 4, 11, 18 and 25, 2015 Completion of Treatment: Case Studies or A Little Bit of Everything Presented by Cherie Fulk February 25, 2015 Cherie Fulk
Main objectives in TB Rx
 Treatment of Tuberculosis in Children HS Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health Stellenbosch University Main objectives in TB Rx To rapidly kill most bacilli in order
Treatment of Tuberculosis in Children HS Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health Stellenbosch University Main objectives in TB Rx To rapidly kill most bacilli in order
Chapter 5 Treatment for Latent Tuberculosis Infection
 Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI.... 112 LTBI Treatment Regimens.... 118 LTBI
Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI.... 112 LTBI Treatment Regimens.... 118 LTBI
GENERAL MANNUAL FOR TUBERCULOSIS CONTROL
 GENERAL MANNUAL FOR TUBERCULOSIS CONTROL National programme for Tuberculosis Control and Chest Diseases Ministry of Health Sri Lanka January 2005 GENERAL MANUAL FOR TUBERCULOSIS CONTROL Second Edition
GENERAL MANNUAL FOR TUBERCULOSIS CONTROL National programme for Tuberculosis Control and Chest Diseases Ministry of Health Sri Lanka January 2005 GENERAL MANUAL FOR TUBERCULOSIS CONTROL Second Edition
TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION
 ersnet.org/school TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION 23-26 May 2012 - Bucharest, Romania SCHOOL COURSE 2012 Educational Material Thank you for viewing this document. We
ersnet.org/school TB AND M/XDR-TB: FROM CLINICAL MANAGEMENT TO CONTROL AND ELIMINATION 23-26 May 2012 - Bucharest, Romania SCHOOL COURSE 2012 Educational Material Thank you for viewing this document. We
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams
 MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams 1 Original document control by Public Health England Title Type Author/s Management of tuberculosis in prisons: Guidance for
MANAGEMENT OF TUBERCULOSIS IN PRISONS: Guidance for prison healthcare teams 1 Original document control by Public Health England Title Type Author/s Management of tuberculosis in prisons: Guidance for
Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges
 Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges John B. Kaneene, DVM, MPH, PhD University Distinguished Professor of Epidemiology Director, Center for Comparative Epidemiology
Tuberculosis and HIV/AIDS Co-Infection: Epidemiology and Public Health Challenges John B. Kaneene, DVM, MPH, PhD University Distinguished Professor of Epidemiology Director, Center for Comparative Epidemiology
SARCOIDOSIS. Signs and symptoms associated with specific organ involvement can include the following:
 SARCOIDOSIS Sarcoidosis is a disease that occurs when areas of inflammation develop in different organs of the body. Very small clusters of inflammation, called granulomas, are seen with sarcoidosis. They
SARCOIDOSIS Sarcoidosis is a disease that occurs when areas of inflammation develop in different organs of the body. Very small clusters of inflammation, called granulomas, are seen with sarcoidosis. They
Yes, Tuberculosis is a serious problem all over the world. Between 6 and 10 million in South Africa are infected by the TB germ.
 What is TB? Do many people get tuberculosis (TB)? Yes, Tuberculosis is a serious problem all over the world. Between 6 and 10 million in South Africa are infected by the TB germ. It is infectious, so it
What is TB? Do many people get tuberculosis (TB)? Yes, Tuberculosis is a serious problem all over the world. Between 6 and 10 million in South Africa are infected by the TB germ. It is infectious, so it
PEDIATRIC TUBERCULOSIS. Hot topics / Unresolved issues in Clinical Practice
 PEDIATRIC TUBERCULOSIS Hot topics / Unresolved issues in Clinical Practice Ann M. Loeffler, M.D. Legacy Emanuel Children s Hospital Portland, OR Faculty Consultant Francis J. Curry National TB Center February
PEDIATRIC TUBERCULOSIS Hot topics / Unresolved issues in Clinical Practice Ann M. Loeffler, M.D. Legacy Emanuel Children s Hospital Portland, OR Faculty Consultant Francis J. Curry National TB Center February
Table. Positive Purified Protein Derivative Results (Pediatrics In Review Apr 2008)
 PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
PPD and TB Sreening COMPETENCY- The resident should know the risk factors for TB exposure, when to screen, and the appropriate criteria for recognizing a positive PPD in children of different age groups
DISCLAIMER. www.health.gov.fj
 DISCLAIMER The authors do not warrant the accuracy of the information contained in the TB Technical Guideline and do not take responsibility for any death, loss, damage or injury caused by using the information
DISCLAIMER The authors do not warrant the accuracy of the information contained in the TB Technical Guideline and do not take responsibility for any death, loss, damage or injury caused by using the information
Revised National Tuberculosis Control Programme (RNTCP) Dr. NAVPREET
 Revised National Tuberculosis Control Programme (RNTCP) Dr. NAVPREET Assistant Prof., Deptt. of Community Medicine GMCH Chandigarh Problem Statement of TB in India India accounts for nearly 1/4 th of global
Revised National Tuberculosis Control Programme (RNTCP) Dr. NAVPREET Assistant Prof., Deptt. of Community Medicine GMCH Chandigarh Problem Statement of TB in India India accounts for nearly 1/4 th of global
Papua New Guinea. National Tuberculosis Management Protocol. Department of Health Disease Control Branch National Tuberculosis Program
 2011 Papua New Guinea National Tuberculosis Management Protocol Department of Health Disease Control Branch National Tuberculosis Program P.O. Box 807, Waigini, Port Moresby, Papua New Guinea Telephones:
2011 Papua New Guinea National Tuberculosis Management Protocol Department of Health Disease Control Branch National Tuberculosis Program P.O. Box 807, Waigini, Port Moresby, Papua New Guinea Telephones:
CHAPTER 9: TREATMENT OF ACTIVE TB DISEASE
 CHAPTER 9: TREATMENT OF ACTIVE TB DISEASE 9.1 Treatment Regimens....... 2 9.1.1 Standard TB Treatment Regimen......2 9.1.2 Alternate TB Treatment Regimens.3 9.2 Phases of TB Treatment....3 9.3 TB Medications
CHAPTER 9: TREATMENT OF ACTIVE TB DISEASE 9.1 Treatment Regimens....... 2 9.1.1 Standard TB Treatment Regimen......2 9.1.2 Alternate TB Treatment Regimens.3 9.2 Phases of TB Treatment....3 9.3 TB Medications
Get the Facts About Tuberculosis Disease
 TB Get the Facts About Tuberculosis Disease What s Inside: Read this brochure today to learn how to protect your family and friends from TB. Then share it with people in your life. 2 Contents Get the facts,
TB Get the Facts About Tuberculosis Disease What s Inside: Read this brochure today to learn how to protect your family and friends from TB. Then share it with people in your life. 2 Contents Get the facts,
Tuberculosis Prevention and Control Protocol, 2008
 Tuberculosis Prevention and Control Protocol, 2008 Preamble The Ontario Public Health Standards (OPHS) are published by the Minister of Health and Long- Term Care under the authority of the Health Protection
Tuberculosis Prevention and Control Protocol, 2008 Preamble The Ontario Public Health Standards (OPHS) are published by the Minister of Health and Long- Term Care under the authority of the Health Protection
 You can get more information about TB from the following: Local Public Health Nurse Community Clinic Nurse Communicable Disease Control Nurse Your Family or Community Doctor Your Infection Control Practitioner
You can get more information about TB from the following: Local Public Health Nurse Community Clinic Nurse Communicable Disease Control Nurse Your Family or Community Doctor Your Infection Control Practitioner
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
Assisted Living - TB Risk Assessment
 Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Montana DPHHS Tuberculosis Program Assisted Living - TB Risk Assessment Assisted Living, Adult Day Care, Adult Foster Care & Transitional Living Centers Today s Date Facility Address Phone County Completed
Pneumonia Education and Discharge Instructions
 Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
MODULE THREE TB Treatment. Treatment Action Group TB/HIV Advocacy Toolkit
 MODULE THREE TB Treatment Treatment Action Group TB/HIV Advocacy Toolkit 1 Topics to be covered TB treatment fundamentals Treatment of TB infection and disease TB treatment research Advocacy issues 2 Section
MODULE THREE TB Treatment Treatment Action Group TB/HIV Advocacy Toolkit 1 Topics to be covered TB treatment fundamentals Treatment of TB infection and disease TB treatment research Advocacy issues 2 Section
Staying on Track with TUBERCULOSIS. Medicine
 Staying on Track with TB TUBERCULOSIS Medicine What s Inside: Read this brochure to learn about TB and what you can do to get healthy. Put it in a familiar place to pull out and read when you have questions.
Staying on Track with TB TUBERCULOSIS Medicine What s Inside: Read this brochure to learn about TB and what you can do to get healthy. Put it in a familiar place to pull out and read when you have questions.
General Information on Tuberculosis
 General Information on Tuberculosis ON THE MOVE AGAINST TUBERCULOSIS: Transforming the fi ght towards elimination World TB Day 2011 SAARC Tuberculosis & HIV/AIDS Centre GPO Box No 9517, Kathmandu, Nepal
General Information on Tuberculosis ON THE MOVE AGAINST TUBERCULOSIS: Transforming the fi ght towards elimination World TB Day 2011 SAARC Tuberculosis & HIV/AIDS Centre GPO Box No 9517, Kathmandu, Nepal
Peripheral Neuropathy (painful feet)
 Peripheral Neuropathy (painful feet) What does it feel like? Peripheral neuropathy is a long lasting pain that usually occurs in the lower legs. Often it is a burning sensation of the foot soles, sometimes
Peripheral Neuropathy (painful feet) What does it feel like? Peripheral neuropathy is a long lasting pain that usually occurs in the lower legs. Often it is a burning sensation of the foot soles, sometimes
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Tuberculosis: Clinical diagnosis and management of tuberculosis, and measures for its prevention and control in Scotland
 5 Tuberculosis: Clinical diagnosis and management of tuberculosis, and measures for its prevention and control in Scotland Health Protection Network Scottish Guidance Adapted from NICE guidelines for Scottish
5 Tuberculosis: Clinical diagnosis and management of tuberculosis, and measures for its prevention and control in Scotland Health Protection Network Scottish Guidance Adapted from NICE guidelines for Scottish
TB Intensive San Antonio, Texas November 11 14, 2014
 TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
TB Intensive San Antonio, Texas November 11 14, 2014 TB in the HIV Patient Lisa Armitige, MD, PhD November 13, 2014 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
MEDICAL REPORT MEDICAL HISTORY QUESTIONS
 MEDICAL HISTORY QUESTIONS PAGE 1 OF 7 IF YOUR ANSWER IS YES TO ANY OF THE FOLLOWING QUESTIONS, PLEASE PROVIDE ADDITIONAL INFORMATION INCLUDING: DIAGNOSIS, DATE, AND TREATMENT (INCLUDING MEDICATIONS AND/OR
MEDICAL HISTORY QUESTIONS PAGE 1 OF 7 IF YOUR ANSWER IS YES TO ANY OF THE FOLLOWING QUESTIONS, PLEASE PROVIDE ADDITIONAL INFORMATION INCLUDING: DIAGNOSIS, DATE, AND TREATMENT (INCLUDING MEDICATIONS AND/OR
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
Tuberculosis (TB) remains the leading cause of mortality from infectious. Tuberculosis (TB)
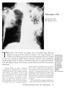 Tuberculosis (TB) John Bernardo, MD Jill S. Roncarati, PA-C Tuberculosis (TB) remains the leading cause of mortality from infectious diseases in humans in the world. In contrast to the world situation,
Tuberculosis (TB) John Bernardo, MD Jill S. Roncarati, PA-C Tuberculosis (TB) remains the leading cause of mortality from infectious diseases in humans in the world. In contrast to the world situation,
Definitions and reporting framework for tuberculosis 2013 revision (updated December 2014)
 Definitions and reporting framework for tuberculosis 2013 revision (updated December 2014) Cover photos: WHO Photo Library Top, Nepal (C. Black); middle, Afghanistan (C. Black); bottom, China (S. Lim)
Definitions and reporting framework for tuberculosis 2013 revision (updated December 2014) Cover photos: WHO Photo Library Top, Nepal (C. Black); middle, Afghanistan (C. Black); bottom, China (S. Lim)
Hinds Community College Nursing and Allied Health Programs Health Record Packet
 Health Record Packet All Clinical Requirements (including the NAH Health Record Packet) must be submitted by the health profession program s designated date. For students admitted to a new program, failure
Health Record Packet All Clinical Requirements (including the NAH Health Record Packet) must be submitted by the health profession program s designated date. For students admitted to a new program, failure
NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33
 Tuberculosis NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33 NICE 2016. All rights reserved. Last updated May 2016 Your responsibility The recommendations in this guideline represent
Tuberculosis NICE guideline Published: 13 January 2016 nice.org.uk/guidance/ng33 NICE 2016. All rights reserved. Last updated May 2016 Your responsibility The recommendations in this guideline represent
National Chlamydia Screening Programme September 2012 PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF AZITHROMYCIN FOR CHLAMYDIA TRACHOMATIS
 PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF AZITHROMYCIN FOR CHLAMYDIA TRACHOMATIS Below is a template that can be used to produce a local patient group direction (PGD) for the administration of
PATIENT GROUP DIRECTION FOR THE ADMINISTRATION OF AZITHROMYCIN FOR CHLAMYDIA TRACHOMATIS Below is a template that can be used to produce a local patient group direction (PGD) for the administration of
