Regional Anesthesia Fellowship at Wake Forest University
|
|
|
- Pamela McGee
- 7 years ago
- Views:
Transcription
1 Regional Anesthesia Fellowship at Wake Forest University Fellowship Director: Douglas Jaffe, DO Assistant Professor and Member - Section of Regional Anesthesia & Acute Pain Management (RAAPM) Department of Anesthesiology, Wake Forest University Baptist Medical Center Mission Statement: The purpose of the fellowship in regional anesthesia at Wake Forest University is to educate individuals who become qualified and committed to enhancing and promoting the specialty of regional anesthesia and acute pain management. Research activities, the development of educational methods, and advanced clinical care will be emphasized to achieve this Mission. The fellowship is also designed to enhance the clinical experience of Wake Forest University residents in regional anesthesia and to contribute to the ongoing development of the specialty of regional anesthesia at Wake Forest University. Eligible Applicants The ideal candidate for the fellowship will have a strong clinical base in regional anesthesia and a professional commitment to build skills and competency suitable for the development of a regional anesthesia program at an academic institution. Fellowship Training in Regional Anesthesia at Wake Forest University: Outline: I. Scope of Training II. Duration of Training III. Institutional Organization IV. Program Director and Faculty V. Facilities and Resources VI. Competency-Based Goals and Objectives VII. Evaluation and Advising I. Scope of Training:
2 II. III. Regional anesthesia fellowship training is concentrated on the perioperative management of patients receiving neuraxial or peripheral neural blockade for anesthesia or analgesia. The program is designed to develop a base of expertise in the practice and theory of regional anesthesia, the organization of a consultant service, and the acquisition of operating room management skills as they relate to regional anesthesia. In addition, the fellow is expected to enhance their teaching abilities and their comprehension and incorporation of practice guidelines and research in the specialty. Duration of Training The time required for fellowship training in regional anesthesia is twelve months. Institutional Organization: A) The fellow functions in close relationship with our ACGME-accredited residency in anesthesiology which includes specific rotations in regional anesthesia and acute pain management. B) There is no ACGME designation or certification for regional anesthesia fellowships to date, but the fellowship is recognized by the Wake Forest University Office of Graduate Medical Education. C) The fellowship stipend would be supported in part by the fellow s activity as a junior faculty anesthesiologist, one day per week, in the Inpatient OR at North Carolina Baptist Hospital. IV. Program Director and Faculty: A) The Director of the fellowship training program is a Board-Certified anesthesiologist who has completed a fellowship in regional anesthesia. B) All faculty are Board-Certified or in the examination system in Anesthesiology. The number of faculty supervising fellowship training in regional anesthesia is five to seven. V. Resources: A) A dedicated area adjacent to the operating rooms and specific to the provision of regional anesthesia techniques is provided for the education of residents and fellows. This area provides all the necessary elements as listed below for such education: 1. Separate patient care beds with full monitoring facilities and computerized electronic record-keeping 2. Dedicated nurses responsible for care of patients receiving regional anesthetics 2
3 3. Computer access to the Institutional Patient Information System for laboratory data, progress notes and consultations, and computerized order entry 4. Equipment necessary for the performance of current regional anesthesia techniques including nerve simulators, neuraxial and peripheral block and catheter supplies, and ultrasound machines. 5. Pharmacy supplies using an AcuDose system 6. Conference area for educational activities and the use of regional anesthesia teaching material and models. 7. A library dedicated to anesthesiology with literature specific to the practice of regional anesthesia is also maintained in the Department. VI. Competency-Based Goals and Objectives Program Goals: Over the course of the 12 month fellowship, the fellow will enhance his or her cognitive, psychomotor, and affective skills to safely and effectively administer and teach regional anesthesia as a consultant in anesthesiology. The fellow will be responsible for decisions related to case and block selection to facilitate the smooth flow of OR cases and to enhance patient recovery. The fellow will be expected to have the skills needed to establish regional anesthesia and acute pain management as a primary component of his or her future practice in anesthesiology. A.) Medical Knowledge Upon completion of the program, the fellow should be able to: 1. Match specific patient and surgical procedure requirements to appropriate regional anesthesia selection. Debate the advantages/disadvantages of regional vs. general anesthesia for various procedures and patients in regard to patient recovery, patient outcome, operating room efficiency, and cost of care. 2. Use evidence-based medicine to select local anesthetics and adjuncts for neural blockade Local Anesthetics A. Discuss the pharmacokinetics of local anesthetics: absorption, distribution, metabolism, and excretion. B. Discuss the site and mechanism of action of local anesthetics. C. Discuss the chemical structure of amino-amides and amino-esters. D. Describe the concept of minimum effective concentration 3
4 of local anesthetic (Cm.) E. Discuss effective concentrations, toxic dosage, influence of site of injection, and vasoconstrictor use in regard to clinical practice. F. Compare attributes of various local anesthetics: motor vs. sensory blocking discrimination and relative toxicity. G. Discuss lipid solubility, protein binding, pka and their influence on onset, potency, and duration of block. H. Describe signs, symptoms and treatment of local anesthetic toxicity 3. Make sound clinical decisions in the administration of systemic and neuraxial opioids, NSAIDs, and non-opioid adjuncts for analgesia. Neuraxial Opioids A. Discuss available drugs, effective dose, and duration of action. B. Compare and contrast extended release epidural morphine with standard preservative-free opioids. C. Discuss the incidence of complications and side effects, monitoring, prevention and therapy. D. Describe the indications/contraindications for the use of neuraxial narcotics for acute pain management. E. Describe the mechanism of action of neuraxial narcotics. F. Differentiate intrathecal vs. epidural administration relative to dose, effect and side effects. G. Differentiate between hydrophilic and hydrophobic drugs to include advantages/disadvantages. Systemic Opioids A. Discuss the pharmacokinetics of opioid analgesics: bioavailability, absorption, distribution, metabolism, and excretion. B. Discuss the site and mechanism of action of opioids. C. Discuss the differences of chemical structure of the various opioids. D. Describe challenges of post-procedure analgesic management in the patient with chronic pain and/or opioid tolerance Non-Opioid Adjuncts A. Describe the concept of multimodal analgesia and its impact on functional restoration after surgery. B. Discuss the pharmacology of NSAIDs, COX-2 inhibitors, NMDA antagonists, alpha-2 agonists, GABA-ergic agents with respect to optimizing postoperative analgesia. 4
5 4. Skillfully and efficiently describe and perform a wide variety of modern regional anesthesia techniques including single-shot and continuous peripheral nerve block, spinal and combined spinalepidural anesthesia, thoracic epidural, and nerve stimulator- and ultrasound-guided approaches (See detailed list below). Spinal Anesthesia A. Discuss the cardiovascular and pulmonary physiologic effects of spinal anesthesia. B. Discuss local anesthetics for intrathecal use: agents, dosage, surgical and total duration of action, and adjuvants. C. Describe baricity of spinal local anesthetic solutions, and the effect on block level. D. Describe the indications and contraindications for spinal anesthesia. E. Discuss side effects, complications and management: inadequate anesthesia, hypotension, and ventilatory insufficiency. F. Define post-dural puncture headache, and describe symptoms, etiology, risk factors and treatment. G. Discuss the use of spinal anesthesia in an ambulatory surgery setting. H. Explain the relative importance of factors affecting intensity, extent and duration of block such as dose, volume, and baricity of injectate. I. Describe differential blockade during neuraxial blockade. J. Describe advantages and disadvantages of continuous spinal anesthesia. Epidural Anesthesia (Lumbar, Thoracic, Caudal) A. Discuss the physiology of epidural anesthesia. B. Describe the contents of the epidural space. C. Discuss the local anesthetics available for epidural use: agents, dosage, adjuncts, and duration of action. D. Differentiate between spinal and epidural anesthesia with regards to reliability, latency, duration, and segmental limitations. C. Describe the indications and contraindications for epidural anesthesia. D. Discuss side effects, complications and management: inadequate anesthesia, hypotension, total spinal, accidental dural puncture, systemic toxicity, and the use 5
6 of appropriate test dosing to minimize some of these complications. F. Describe the volume-segment relationship and the effect of patient age, pregnancy, position, and site of injection on resultant block. G. Discuss combined spinal-epidural anesthesia as distinguished from lumbar epidural anesthesia, including advantages/disadvantages, dose requirements, complications, indications and contraindications. H. Discuss caudal epidural and thoracic epidural anesthesia as distinguished from lumbar epidural anesthesia, including advantages/disadvantages, dose requirements, complications, indications and contraindications. Nerve Localization Techniques A. Understand principles, operation, advantages and limitations of the peripheral nerve stimulator to identify and anesthetize peripheral nerves B. Understand principles, operation, advantages and limitations of ultrasound to identify and anesthetize peripheral nerves Subcategories of knowledge in ultrasound include: 1. Physics and technical aspects of image generation 2. Machine controls for image optimization 3. Transducer manipulation for image optimization 4. Sonoanatomic appearance of nerves and other tissues 5. Needle guidance approaches 6. Injectate appearance and optimization Upper Extremity Nerve Block A. Describe the anatomy of the brachial plexus in relation to sensory and motor innervation. B. Discuss local anesthetics for brachial plexus block: agents, dosage, duration of action, and adjuvants. C. Discuss side effects, complications, and management: inadequate anesthesia, systemic toxicity, blockade of adjacent neural structures (phrenic, sympathetic chain and neuraxis), neuropathy. D. Describe the various approaches to brachial plexus blockade, along with the indications/contraindications, advantages/disadvantages, and complications specific to each. 6
7 E. Describe peripheral nerve block in the upper extremity of the median, ulnar and radial nerves, with indications, contraindications, and complications. F. Discuss the use and advantages/disadvantages nerve localizing techniques including transarterial, perivascular, nerve stimulator and paresthesiaseeking techniques. G. Discuss the use and advantages/disadvantages specific to continuous brachial plexus anesthesia. Lower Extremity Nerve Block A. Describe anatomy of the lower extremity: sciatic, femoral, lateral femoral cutaneous, obturator nerves in relation to sensory and motor innervation. B. Discuss local anesthetics for lower extremity block: agents, dosage, duration of action, and adjuvants. C. Describe the various approaches to lower extremity blockade, along with the indications/contraindications, advantages/disadvantages, and complications specific to each. D. Discuss side effects, complications, and management of lower extremity blockade: inadequate analgesia, systemic toxicity, blockade of adjacent neural structures, and post-operative neuropathy. E. Differentiate individual blockade of the femoral, lateral femoral cutaneous, and obturator nerves from the anterior and posterior approaches to the lumbar plexus. F. Differentiate individual blockade of the tibial and peroneal nerves from the classic and popliteal approaches to the sciatic nerve. Truncal Blockade A. Discuss the anatomy of intercostal, paravertebral, rectus sheath and transversus abdominus plane (TAP) blockade. B. Discuss local anesthetics for truncal blockade: agents, dosage, and duration of action. C. Discuss the indications and contraindications for truncal blockade. D. Discuss the side effects, complications, and management: inadequate anesthesia, systemic toxicity, and pneumothorax. 7
8 Intravenous Regional Anesthesia A. Discuss the mechanism of action of IVRA. B. Discuss agents for IVRA: local anesthetic choice, dosage, and use of adjuvants. C. Describe the indications and contraindications, advantages and disadvantages of IVRA. D. Discuss the complications and management: systemic toxicity, inadequate anesthesia, and phlebitis. B) Patient Care Upon completion of the program, the fellow should be able to: A) Demonstrate rational selection of regional anesthesia for specific clinical situations. B) Recognize and intervene to manage inadequate regional anesthetic techniques with supplemental blockade or alternate anesthetic approaches C) Properly prepare to manage rare but serious complications of regional anesthesia including local anesthetic toxicity and total spinal anesthesia. D) Properly perform and teach correct technique for many of the following listed regional blocks to achieve a high success and low complication rate: 1) Basic Techniques and Approaches: Superficial cervical plexus block Axillary brachial plexus block Intercostobrachial nerve block Wrist Block Intravenous regional anesthesia (Bier block) Saphenous nerve block Ankle block Spinal anesthesia Lumbar epidural anesthesia Combined spinal-epidural anesthesia Femoral nerve block 2) Intermediate Techniques and Approaches: Deep cervical plexus block Interscalene block Supraclavicular block Infraclavicular block 8
9 Sciatic nerve block: posterior approaches Lumbar plexus block Popliteal block Suprascapular nerve block Intercostal nerve block Thoracic epidural anesthesia 3) Advanced Techniques and Approaches: Continuous interscalene block Continuous infraclavicular block Continuous axillary block Thoraco-lumbar paravertebral block: single or continuous Continuous femoral nerve block Sciatic nerve block: anterior approaches Obturator nerve block Continuous sciatic nerve block Continuous popliteal block: all approaches E) Demonstrate the ability to lead acute pain rounds with attending supervision, while managing patients at the level of a consultant. Management will include multi-modal analgesic techniques such as neuraxial and peripheral nerve catheters, local anesthetics and narcotic infusions, and non-narcotic analgesic adjuvants. Indications, contraindications, side effects, potential complications, and daily management of patients on the acute pain service will be stressed. C. Scholarly Activities / Practice-Based Learning Upon completion of the program, the fellow should: A) Academic Activities: 1) Participate in clinical research as a major activity of the year long fellowship. 2) Maintain the goal of publication of two clinical studies during the year. 3) Expect to guest review manuscripts for the faculty who serve as editors of peer-reviewed journals to gain knowledge of manuscript preparation. To accomplish these objectives, The RAAPM faculty will be committed to mentoring the fellow in the production of research, co-author papers as appropriate, and preparation of clinical research proposals with IRB approval prior to the start of the fellowship year. 9
10 B) Teaching Activities: 1) Present once during the second half of the fellowship year at Anesthesia Grand Rounds covering a topic or case relevant to regional anesthesia. 2) Prepare resident education lectures or journal reviews for the regional anesthesia subspecialty conference. 3) Participate and direct portions of the fresh cadaver anatomy labs organized for anesthesia residents as part of their annual curriculum. 4) Participate at the Annual American Society of Regional Anesthesia and Pain Medicine Meeting with poster, lecture, or problem-based learning presentations. 5) Learn teaching techniques by instructing residents at the bedside in the Regional Anesthesia Area under the supervision of faculty. 6) Learn teaching techniques by directing the APS during the last week of every month under the supervision of faculty. 7) Participate in the education of residents and student nurse anesthetists as part of the fellow s one-day per week clinical commitment in the general OR. 8) Review and enhance web-based teaching resources including the resident handbook, curriculum document, and self study and testing materials. C) Practice-Based Learning: 1) Evaluate and apply evidence from scientific studies, and expert guidelines and practice pathways to their patient s health problems. 2) Use information technology to obtain and record patient information, access institutional and national policies and guidelines, and participate in self education. 3) Evaluate their own practice with respect to patient outcomes (esp. success and complications from regional block) and compare to available literature. D) Interpersonal and Communication Skills: Upon completion of the program, the fellow should be able to: 10
11 A) Provide information to the patient and family with respect to the options, alternatives, risks and benefits of regional anesthesia in a manner that is clear, understandable, ethical and appropriate. B) Employ effective listening skills and answer questions appropriately in the process of obtaining informed consent. C) Work effectively in a team environment, communicating and cooperating with surgeons, nurses, pharmacists, physical therapists and other members of the perioperative team. This requires the fellow to: 1) appreciate the roles of other members of the team 2) communicate clearly in a collegial manner that facilitates the achievement of care goals 3) help other members of the team to enhance the sharing of important information 4) formulate care plans that utilize the multidisciplinary team skills, such as a plan for facilitated recovery. E) Professionalism Upon completion of the program, the fellow should be able to: A) Continuously conduct the practice of medicine with integrity, honesty, and accountability. B) Demonstrate a commitment to life-long learning and excellence in practice. C) Show consistent subjugation of self-interest to the good of the patient and the health care needs of society. D) Show a commitment to ethical principles in providing care, obtaining informed consent, and maintaining patient confidentiality. F) Systems-Based Practice Upon completion of the program, the fellow should be able to: A) Effectively balance the need for operating room efficiency with a high quality of patient care in the setting of a residency teaching program. The fellow will effectively choose surgeons, patients, techniques and 11
12 approaches to achieve the best balance possible in order to use regional anesthesia to improve recovery. B) Understand the interaction of the Acute Pain Management Service with other elements of the health care system including primary surgical and medical teams, other consultant services, nursing, pharmacy, and physical therapy. C) Demonstrate awareness of health care costs and resource allocation, and the impact of their choices on those costs and resources. D) Advocate for the patient and their family within the health care system, and assist them in understanding and negotiating complexities in that system. VII.) Evaluation and Advising: A) As per ACGME Residency Guidelines, the attending faculty will be evaluated by the fellows twice annually. B) Written web-based evaluations of fellows by all faculty with whom they have worked shall occur monthly. Evaluation in the areas of the six competency categories as related to regional anesthesia will be evaluated and reported to the clinical competence committee. The results of these evaluations shall be recorded and reviewed with the fellows by the program director no less often than every three months. C) The Fellowship Director will meet with the Fellow at regular intervals to review performance, scholarly activity, and achievement of personal and program objectives. 12
Department of Anesthesiology and Perioperative Medicine Acute Pain Service Resident Goals and Objectives
 Department of Anesthesiology and Perioperative Medicine Acute Pain Service Resident Goals and Objectives GOAL: SUPERVISION: OBJECTIVES: The Pain Medicine Resident will develop the knowledge and skills
Department of Anesthesiology and Perioperative Medicine Acute Pain Service Resident Goals and Objectives GOAL: SUPERVISION: OBJECTIVES: The Pain Medicine Resident will develop the knowledge and skills
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011
 Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Geisinger Health System Anesthesiology Residency Program. Obstetric Anesthesia
 Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
Geisinger Health System Anesthesiology Residency Program Obstetric Anesthesia INTRODUCTION Education and training in obstetric anesthesia will consist of attending-supervised rotations for four weeks during
Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines for the Management of Major Regional Analgesia
 PS03 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Faculty of Pain Medicine Guidelines for the Management of Major Regional Analgesia 1. OVERVIEW This document is intended to apply to
PS03 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Faculty of Pain Medicine Guidelines for the Management of Major Regional Analgesia 1. OVERVIEW This document is intended to apply to
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson
 The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Collaboration Anesthesia
 HPC hpcconnection.ca Nursing Neuro - axial Analgesia cross sector Pharmacists Intractable patient centered Opioids Interventional Consensus Collaboration Anesthesia Physicians epidural evidence based Intraspinal
HPC hpcconnection.ca Nursing Neuro - axial Analgesia cross sector Pharmacists Intractable patient centered Opioids Interventional Consensus Collaboration Anesthesia Physicians epidural evidence based Intraspinal
Laser Treatment Policy
 Laser Treatment Policy Pursuant to federal law 21 CFR 812.2(c)7 and 812.3(b), physician(s) at this pain center may advise and use unapproved laser s on patients under one or more of the following conditions:
Laser Treatment Policy Pursuant to federal law 21 CFR 812.2(c)7 and 812.3(b), physician(s) at this pain center may advise and use unapproved laser s on patients under one or more of the following conditions:
How To Treat Anesthetic With Local Anesthesia
 3. LOCAL ANESTHETICS INTRODUCTION Compared to general anesthesia with opioidbased perioperative pain management, regional anesthesia can provide benefits of superior pain control, improved patient satisfaction,
3. LOCAL ANESTHETICS INTRODUCTION Compared to general anesthesia with opioidbased perioperative pain management, regional anesthesia can provide benefits of superior pain control, improved patient satisfaction,
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
Department of Anesthesia & Perioperative Medicine 5-Year Strategic Plan FY 2012-2016. Contents
 Anesthesia & Perioperative Medicine 167 Ashley Avenue, Suite 301 MSC 912 Charleston, SC 29425-9120 Tel 843 792 2322 Fax 843 792 9314 Department of Anesthesia & Perioperative Medicine 5-Year Strategic Plan
Anesthesia & Perioperative Medicine 167 Ashley Avenue, Suite 301 MSC 912 Charleston, SC 29425-9120 Tel 843 792 2322 Fax 843 792 9314 Department of Anesthesia & Perioperative Medicine 5-Year Strategic Plan
GRADUATE PROGRAM IN NURSE ANESTHESIA. Course Descriptions and Student Learning Objectives
 GRADUATE PROGRAM IN NURSE ANESTHESIA Course Descriptions and NA640 Chemistry & Physics for Nurse Anesthesia - 4 Credits This course examines the principles of inorganic chemistry, organic chemistry, biochemistry
GRADUATE PROGRAM IN NURSE ANESTHESIA Course Descriptions and NA640 Chemistry & Physics for Nurse Anesthesia - 4 Credits This course examines the principles of inorganic chemistry, organic chemistry, biochemistry
Updated Guide to Billing for Regional Anesthesia (United States)
 Updated Guide to Billing for Regional Anesthesia (United States) Tae-Wu Edward Kim, MD* w Stanford University School of Medicine, Palo Alto, California Veterans Affairs Palo Alto Health Care System, Palo
Updated Guide to Billing for Regional Anesthesia (United States) Tae-Wu Edward Kim, MD* w Stanford University School of Medicine, Palo Alto, California Veterans Affairs Palo Alto Health Care System, Palo
OB PBLD L117 Labor and Delivery in the Age of Ebola Upper 20B-20C. PI PBLD L120 He's 15, Needs This Operation, and He's DNR!
 ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists
 Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
I) Rotation Goals. Teaching Methods
 I) Rotation Goals UNMC Anesthesia Rotation Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Revised: 3/2016 A) To manage patients
I) Rotation Goals UNMC Anesthesia Rotation Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Revised: 3/2016 A) To manage patients
30. BASIC PEDIATRIC REGIONAL ANESTHESIA
 30. BASIC PEDIATRIC REGIONAL ANESTHESIA INTRODUCTION Military anesthesia providers often encounter pediatric patients while delivering medical care in the field. The application of regional anesthesia
30. BASIC PEDIATRIC REGIONAL ANESTHESIA INTRODUCTION Military anesthesia providers often encounter pediatric patients while delivering medical care in the field. The application of regional anesthesia
Clinical Site Resource Manual. Northport Medical Center- DCH
 Clinical Site Resource Manual Northport Medical Center- DCH Nurse Anesthesia Program School of Health Related Professions The University of Alabama at Birmingham TABLE OF CONTENTS Section 1 CLINICAL SITE
Clinical Site Resource Manual Northport Medical Center- DCH Nurse Anesthesia Program School of Health Related Professions The University of Alabama at Birmingham TABLE OF CONTENTS Section 1 CLINICAL SITE
BEFORE THE ALABAMA BOARD OF NURSING IN THE MATTER OF: ) PETITION FOR ) DECLARATORY RULING STEVE SYKES, M.D., ) ) ) Petitioner. ) DECLARATORY RULING
 BEFORE THE ALABAMA BOARD OF NURSING IN THE MATTER OF: ) PETITION FOR ) DECLARATORY RULING STEVE SYKES, M.D., ) ) ) Petitioner. ) DECLARATORY RULING COMES NOW the Alabama Board of Nursing, by and through
BEFORE THE ALABAMA BOARD OF NURSING IN THE MATTER OF: ) PETITION FOR ) DECLARATORY RULING STEVE SYKES, M.D., ) ) ) Petitioner. ) DECLARATORY RULING COMES NOW the Alabama Board of Nursing, by and through
Basic Standards for Fellowship Training in Pain Medicine
 Basic Standards for Fellowship Training in Pain Medicine American Osteopathic Association and American Academy of Osteopathy (AAO) American College of Osteopathic Family Physicians (ACOFP) American College
Basic Standards for Fellowship Training in Pain Medicine American Osteopathic Association and American Academy of Osteopathy (AAO) American College of Osteopathic Family Physicians (ACOFP) American College
International Training Program for Nurse Anesthetist The program: International training program for nurse anesthetist Name of certificate:
 International Training Program for Nurse Anesthetist Department of Anesthesiology Faculty of Medicine Siriraj Hospital Mahidol University, Bangkok, Thailand The program: International training program
International Training Program for Nurse Anesthetist Department of Anesthesiology Faculty of Medicine Siriraj Hospital Mahidol University, Bangkok, Thailand The program: International training program
Acute Pain Management in the Opioid Dependent Patient. Maripat Welz-Bosna MSN, CRNP-BC
 Acute Pain Management in the Opioid Dependent Patient Maripat Welz-Bosna MSN, CRNP-BC Relieving Pain in America (IOM) More then 116 Million Americans have pain the persists for weeks to years $560-635
Acute Pain Management in the Opioid Dependent Patient Maripat Welz-Bosna MSN, CRNP-BC Relieving Pain in America (IOM) More then 116 Million Americans have pain the persists for weeks to years $560-635
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
devoted physicians. collaborative partners. metrics-driven quality.
 Regional Anesthesia and Multimodal Pain Management Improves Outcomes, Reduces Costs and Boosts Patient Satisfaction devoted physicians. collaborative partners. metrics-driven quality. usap.com jlrmedicalgroup.com
Regional Anesthesia and Multimodal Pain Management Improves Outcomes, Reduces Costs and Boosts Patient Satisfaction devoted physicians. collaborative partners. metrics-driven quality. usap.com jlrmedicalgroup.com
Advanced Heart Failure & Transplantation Fellowship Program
 Advanced Heart Failure & Transplantation Fellowship Program Curriculum I. Patient Care When on the inpatient Heart Failure and Transplant Cardiology service, the cardiology fellow will hold primary responsibility
Advanced Heart Failure & Transplantation Fellowship Program Curriculum I. Patient Care When on the inpatient Heart Failure and Transplant Cardiology service, the cardiology fellow will hold primary responsibility
Local Anesthetics Used for Spinal Anesthesia
 Local Anesthetics Used for Spinal Anesthesia Several local anesthetics are used for spinal anesthesia. These include procaine, lidocaine, tetracaine, levobupivacaine, and bupivacaine. Local anesthetics
Local Anesthetics Used for Spinal Anesthesia Several local anesthetics are used for spinal anesthesia. These include procaine, lidocaine, tetracaine, levobupivacaine, and bupivacaine. Local anesthetics
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Anatomical Consideration and Brachial Plexus Anesthesia. Anatomy
 Brachial Plexus Anesthesia There are four approaches to the brachial plexus. These include the interscalene, supraclavicular, infraclavicular, and axillary approach. For the purposes of this lecture we
Brachial Plexus Anesthesia There are four approaches to the brachial plexus. These include the interscalene, supraclavicular, infraclavicular, and axillary approach. For the purposes of this lecture we
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form
 Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Fellowship in Multiple Sclerosis and Neuroinflammatory Disorders Type of Fellowship: Clinical Research
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Fellowship in Multiple Sclerosis and Neuroinflammatory Disorders Type of Fellowship: Clinical Research
Military Advanced Regional Anesthesia and Analgesia handbook
 Military Advanced Regional Anesthesia and Analgesia handbook Published by the Office of The Surgeon General Department of the Army, United States of America US Army Medical Center and School Fort Sam Houston,
Military Advanced Regional Anesthesia and Analgesia handbook Published by the Office of The Surgeon General Department of the Army, United States of America US Army Medical Center and School Fort Sam Houston,
ELECTRODIAGNOSTIC MEDICINE
 ELECTRODIAGNOSTIC MEDICINE OBJECTIVES BEGINNER Patient Care Perform a comprehensive electrodiagnostic evaluation of each patient and to provide a concise diagnosis and plan for further treatment Describe
ELECTRODIAGNOSTIC MEDICINE OBJECTIVES BEGINNER Patient Care Perform a comprehensive electrodiagnostic evaluation of each patient and to provide a concise diagnosis and plan for further treatment Describe
Why would we want to change a practice with a track record that has proven safe and that works well?
 Good morning, Mr. Chairman and distinguished members of the House Professional Licensure Committee. My name is Dr. Erin Sullivan. I am president of the Pennsylvania Society of Anesthesiologists and a board
Good morning, Mr. Chairman and distinguished members of the House Professional Licensure Committee. My name is Dr. Erin Sullivan. I am president of the Pennsylvania Society of Anesthesiologists and a board
OHIP BILLING for ANESTHESIOLOGY. (Updated September 13, 2011)
 OHIP BILLING for ANESTHESIOLOGY (Updated September 13, 2011) Introduction Review the SOB (Schedule of Benefits) on line at either the OMA website or the MOHLTC website http://www.health.gov.on.ca/english/providers/program/ohip/sob/physserv/physserv_mn.html.
OHIP BILLING for ANESTHESIOLOGY (Updated September 13, 2011) Introduction Review the SOB (Schedule of Benefits) on line at either the OMA website or the MOHLTC website http://www.health.gov.on.ca/english/providers/program/ohip/sob/physserv/physserv_mn.html.
Prerequisites. Authorization, Notification and Referral. Limitations ANESTHESIA SERVICES
 ANESTHESIA SERVICES Policy NHP reimburses participating providers for the administration of general and regional anesthesia, and supportive services performed in conjunction with covered obstetrical, surgical,
ANESTHESIA SERVICES Policy NHP reimburses participating providers for the administration of general and regional anesthesia, and supportive services performed in conjunction with covered obstetrical, surgical,
Ultrasound Guided / Cadaver Course in Regional Anesthesia and Central Vascular Access
 Fifth Annual Ultrasound Guided / Cadaver Course in Regional Anesthesia and Central Vascular Access Best value for your CME dollars... Register today! May 30 31, 2015 An exciting opportunity to acquire
Fifth Annual Ultrasound Guided / Cadaver Course in Regional Anesthesia and Central Vascular Access Best value for your CME dollars... Register today! May 30 31, 2015 An exciting opportunity to acquire
ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284
 ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284 15 TH APRIL 2013 Dr Suresh Kumar Jeyaraj, Specialty Doctor Dr Tim Pepall, Consultant Anaesthetist Frimley Park Hospital NHS foundation
ULTRASOUND GUIDED FEMORAL NERVE BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 284 15 TH APRIL 2013 Dr Suresh Kumar Jeyaraj, Specialty Doctor Dr Tim Pepall, Consultant Anaesthetist Frimley Park Hospital NHS foundation
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
Best practice in the management of epidural analgesia in the hospital setting
 Best practice in the management of epidural analgesia in the hospital setting FACULTY OF PAIN MEDICINE of The Royal College of Anaesthetists Royal College of Anaesthetists Royal College of Nursing Association
Best practice in the management of epidural analgesia in the hospital setting FACULTY OF PAIN MEDICINE of The Royal College of Anaesthetists Royal College of Anaesthetists Royal College of Nursing Association
Neuromuscular Medicine Fellowship Curriculum
 Neuromuscular Medicine Fellowship Curriculum General Review Goals and Objectives Attend weekly EMG sessions as assigned Take a Directed History and Exam of each EMG patient Attend every other week Muscle
Neuromuscular Medicine Fellowship Curriculum General Review Goals and Objectives Attend weekly EMG sessions as assigned Take a Directed History and Exam of each EMG patient Attend every other week Muscle
Mississippi Board of Nursing
 Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Medicine in Osteopathic Family Practice and Manipulative Treatment
 0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
Goals and Objectives Pediatric Surgery PGY 1 MCVH
 Goals and Objectives Pediatric Surgery PGY 1 MCVH PGY-1 Clinical Duties and Privileges Lines of Supervision During the PGY-1 each resident begins his/her clinical experience in the General Surgery Residency
Goals and Objectives Pediatric Surgery PGY 1 MCVH PGY-1 Clinical Duties and Privileges Lines of Supervision During the PGY-1 each resident begins his/her clinical experience in the General Surgery Residency
First Year. PT7040- Clinical Skills and Examination II
 First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
The ACGME and the American Board of Anesthesiology accredit the Pain Management Fellowship Program at M. D. Anderson Cancer Center.
 Pain Management Fellowship Facts The Fellowship Program in Pain Management is a fifth-year level program of one-year duration that prepares a fellow in all aspects of pain management. Each year, four new
Pain Management Fellowship Facts The Fellowship Program in Pain Management is a fifth-year level program of one-year duration that prepares a fellow in all aspects of pain management. Each year, four new
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine
 Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
Basic Standards for Residency Training in Physical Medicine and Rehabilitation
 Basic Standards for Residency Training in Physical Medicine and Rehabilitation American Osteopathic Association and American Osteopathic College of Physical Medicine and Rehabilitation COPT/R-88 Rev. BOT,
Basic Standards for Residency Training in Physical Medicine and Rehabilitation American Osteopathic Association and American Osteopathic College of Physical Medicine and Rehabilitation COPT/R-88 Rev. BOT,
Who Should Participate*
 earn 25 contact hours! For as little as $49. 95 Announcing: Sedation Clinical Competency Program Finally A practical solution to satisfy formal training, credentialing, and competency-based educational
earn 25 contact hours! For as little as $49. 95 Announcing: Sedation Clinical Competency Program Finally A practical solution to satisfy formal training, credentialing, and competency-based educational
ANAESTHESIOLOGY, PAIN AND INTENSIVE CARE MEDICINE
 ANAESTHESIOLOGY, PAIN AND INTENSIVE CARE MEDICINE UEMS/EBA GUIDELINES POSTGRADUATE TRAINING PROGRAM FROM THE STANDING COMMITTEE ON EDUCATION AND TRAINING OF THE SECTION AND BOARD OF ANAESTHESIOLOGY 1 Summary
ANAESTHESIOLOGY, PAIN AND INTENSIVE CARE MEDICINE UEMS/EBA GUIDELINES POSTGRADUATE TRAINING PROGRAM FROM THE STANDING COMMITTEE ON EDUCATION AND TRAINING OF THE SECTION AND BOARD OF ANAESTHESIOLOGY 1 Summary
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Test Content Outline Effective Date: June 9, 2014. Pain Management Nursing Board Certification Examination
 Pain Management Nursing Board Certification Examination There are 175 questions on this examination. Of these, 150 are scored questions and 25 are pretest questions that are not scored. Pretest questions
Pain Management Nursing Board Certification Examination There are 175 questions on this examination. Of these, 150 are scored questions and 25 are pretest questions that are not scored. Pretest questions
INTERNATIONAL FEDERATION OF NURSE ANESTHETISTS. Standards of Education, Practice, Monitoring and Code of Ethics
 INTERNATIONAL FEDERATION OF NURSE ANESTHETISTS Standards of Education, Practice, Monitoring and Code of Ethics Revised 25 May 2012 All rights reserved IFNA, 2012 1 Standards and Code of Ethics INTERNATIONAL
INTERNATIONAL FEDERATION OF NURSE ANESTHETISTS Standards of Education, Practice, Monitoring and Code of Ethics Revised 25 May 2012 All rights reserved IFNA, 2012 1 Standards and Code of Ethics INTERNATIONAL
Board encourages physicians to treat patients pain responsibly
 STATE OF IOWA TERRY BRANSTAD, GOVERNOR KIM REYNOLDS, LT. GOVERNOR IOW A BO ARD OF MEDICINE MARK BOW DEN, E XECUTIVE DIRECTO R FOR IMMEDIATE RELEASE: June 10, 2014 CONTACT: Mark Bowden, ( 515) 242-3268
STATE OF IOWA TERRY BRANSTAD, GOVERNOR KIM REYNOLDS, LT. GOVERNOR IOW A BO ARD OF MEDICINE MARK BOW DEN, E XECUTIVE DIRECTO R FOR IMMEDIATE RELEASE: June 10, 2014 CONTACT: Mark Bowden, ( 515) 242-3268
Nurse Anesthesia History and Practice in the United States. Debra Maloy CRNA, EdD Director Graduate Programs of Nurse Anesthesia
 Nurse Anesthesia History and Practice in the United States 1 Hospital Based Training Hospital based, Sisters 1873 3 schools 3 years of service Little education Laundry Housekeeping 55-75 hour/week Few
Nurse Anesthesia History and Practice in the United States 1 Hospital Based Training Hospital based, Sisters 1873 3 schools 3 years of service Little education Laundry Housekeeping 55-75 hour/week Few
Epidural Anesthesia. Advantages of Epidural Anesthesia
 Epidural Anesthesia Epidural anesthesia involves the use of local anesthetics injected into the epidural space to produce a reversible loss of sensation and motor function. Epidural anesthesia requires
Epidural Anesthesia Epidural anesthesia involves the use of local anesthetics injected into the epidural space to produce a reversible loss of sensation and motor function. Epidural anesthesia requires
Wake Forest University Physician Assistant Program Curriculum Description Class of 2015
 Wake Forest University Physician Assistant Program Curriculum Description Class of 2015 The Wake Forest University Physician Assistant Program has a unique history of innovation in medical education. From
Wake Forest University Physician Assistant Program Curriculum Description Class of 2015 The Wake Forest University Physician Assistant Program has a unique history of innovation in medical education. From
Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009
 Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009 I. Overview of Training in Cardiac Catheterization Cardiac catheterization
Cardiac Catheterization Curriculum for Fellows in Cardiology Dartmouth-Hitchcock Medical Center Level 1 and Level 2 Training 2008-2009 I. Overview of Training in Cardiac Catheterization Cardiac catheterization
Spinal Anesthesia. Contraindications Please review Chapter 2 for contraindications.
 Spinal Anesthesia Spinal anesthesia involves the use of small amounts of local anesthetic injected into the subarachnoid space to produce a reversible loss of sensation and motor function. The anesthesia
Spinal Anesthesia Spinal anesthesia involves the use of small amounts of local anesthetic injected into the subarachnoid space to produce a reversible loss of sensation and motor function. The anesthesia
Post-operative Pain Management
 Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
LUMBAR PARAVERTEBRAL (PSOAS COMPARTMENT) BLOCK BY ANDRÉ P BOEZAART MD, PHD
 BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION When evaluating the efficacy of centrally performed nerve blocks one must think
BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION When evaluating the efficacy of centrally performed nerve blocks one must think
CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving
 CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral)
CURRICULUM ON MEDICAL KNOWLEDGE I. Educational Purpose and Goals Physicians must demonstrate knowledge about both established and evolving biomedical, clinical, and cognate (e.g. epidemiological and social-behavioral)
Submitted via email to chronic_care@finance.senate.gov. June 22, 2015
 Submitted via email to chronic_care@finance.senate.gov June 22, 2015 Chronic Care Working Group Senate Finance Committee United States Senate 219 Dirksen Senate Office Building Washington, D.C. 20510 Re:
Submitted via email to chronic_care@finance.senate.gov June 22, 2015 Chronic Care Working Group Senate Finance Committee United States Senate 219 Dirksen Senate Office Building Washington, D.C. 20510 Re:
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
The Pharmacological Management of Cancer Pain in Adults. Clinical Audit Tool
 The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
 American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
American Association of Nurse Anesthetists 222 South Prospect Avenue Park Ridge, IL 60068 www.aana.com Guidelines for the Management of the Obstetrical Patient for the Certified Registered Nurse Anesthetist
Richard C. Clarke, M.D. Texas Tech University Health Science Center. Anesthesiology Residency March 1999- March 2001 Lubbock Texas.
 Curriculum Vitae Richard C. Clarke, M.D. Education Texas Tech University Health Science Center. Anesthesiology Residency March 1999- March 2001 Lubbock Texas. Tulane University Hospital. New Orleans, Louisiana.
Curriculum Vitae Richard C. Clarke, M.D. Education Texas Tech University Health Science Center. Anesthesiology Residency March 1999- March 2001 Lubbock Texas. Tulane University Hospital. New Orleans, Louisiana.
Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients
 ORIGINAL RESEARCH Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients Edward R. Mariano, MD, MAS, Jay B. Brodsky, MD Article includes CME test
ORIGINAL RESEARCH Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients Edward R. Mariano, MD, MAS, Jay B. Brodsky, MD Article includes CME test
PERI-OPERATIVE MANAGEMENT OF PATIENTS ON STRONG OPIOIDS ANAESTHESIA TUTORIAL OF THE WEEK 260 21 ST MAY 2012 QUESTIONS
 PERI-OPERATIVE MANAGEMENT OF PATIENTS ON STRONG OPIOIDS ANAESTHESIA TUTORIAL OF THE WEEK 260 21 ST MAY 2012 Dr Michael J.E. Neil. South West School of Anaesthesia Correspondence to mneil@nhs.net QUESTIONS
PERI-OPERATIVE MANAGEMENT OF PATIENTS ON STRONG OPIOIDS ANAESTHESIA TUTORIAL OF THE WEEK 260 21 ST MAY 2012 Dr Michael J.E. Neil. South West School of Anaesthesia Correspondence to mneil@nhs.net QUESTIONS
Specific Standards of Accreditation for Residency Programs in General Surgery
 Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Preface to Practice Standards
 0 0 0 0 Preface to Practice Standards A profession s practice standards serve as a guide for appropriate practice. The practice standards define the practice and establish general criteria to determine
0 0 0 0 Preface to Practice Standards A profession s practice standards serve as a guide for appropriate practice. The practice standards define the practice and establish general criteria to determine
How To Manage A Pediatric Inpatient Rotation At American University Of Britain
 Pediatric Residency Program American University of Beirut In patients Experience Goals and Objectives The in patient rotation at AUB MC is based on a general pediatric ward in a tertiary care setting with
Pediatric Residency Program American University of Beirut In patients Experience Goals and Objectives The in patient rotation at AUB MC is based on a general pediatric ward in a tertiary care setting with
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES
 02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
02 DEPARTMENT OF PROFESSIONAL AND FINANCIAL REGULATION 380 BOARD OF NURSING Chapter 10: REGULATIONS RELATING TO ADMINISTRATION OF INTRAVENOUS THERAPY BY LICENSED NURSES SUMMARY: This chapter identifies
Course Curriculum for Master Degree in Clinical Pharmacy
 Course Curriculum for Master Degree in Clinical Pharmacy The Master Degree in Clinical Pharmacy is awarded by the Faculty of Graduate studies at Jordan University of Science and Technology (JUST) upon
Course Curriculum for Master Degree in Clinical Pharmacy The Master Degree in Clinical Pharmacy is awarded by the Faculty of Graduate studies at Jordan University of Science and Technology (JUST) upon
INTRODUCTION BY ANDRÉ P BOEZAART MD, PHD
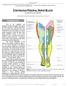 BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION Due to the multiplicity and divergence of the nerve supply to the joints of the
BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION Due to the multiplicity and divergence of the nerve supply to the joints of the
Kidney and Pancreas Transplant Evaluation Clinics and Committee: Inpatient Nephrology Transplant Consult Service
 Care of Renal Transplant Patients takes place in five distinct practice settings at the University of Michigan: a) Kidney and Pancreas Pre-transplant evaluation clinics (five half-day clinics per week)
Care of Renal Transplant Patients takes place in five distinct practice settings at the University of Michigan: a) Kidney and Pancreas Pre-transplant evaluation clinics (five half-day clinics per week)
Registered Nurse (RN) and Nursing Careers, Jobs, and Employment Information
 www.careersinghana.com Email : info@careersinghana.com Tel: +233 245649846 Registered Nurse (RN) and Nursing Careers, Jobs, and Employment Information Registered Nurse and Nursing Career Overview Registered
www.careersinghana.com Email : info@careersinghana.com Tel: +233 245649846 Registered Nurse (RN) and Nursing Careers, Jobs, and Employment Information Registered Nurse and Nursing Career Overview Registered
Cardiovascular Fellowship Goals and Objectives
 Cardiovascular Fellowship Goals and Objectives I. GOALS OF THE PROGRAM The objective of the Fellowship Training Program in Cardiovascular Disease is to provide an academically and clinically rigorous training
Cardiovascular Fellowship Goals and Objectives I. GOALS OF THE PROGRAM The objective of the Fellowship Training Program in Cardiovascular Disease is to provide an academically and clinically rigorous training
Our faculty has been hand-picked for their knowledge, experience, and enthusiasm for teaching
 We welcome your interest in Advocate Lutheran General Hospital s Psychiatry Residency Program. ALGH is a 638-bed teaching hospital located adjacent to Chicago on the northwest side. We proudly provide
We welcome your interest in Advocate Lutheran General Hospital s Psychiatry Residency Program. ALGH is a 638-bed teaching hospital located adjacent to Chicago on the northwest side. We proudly provide
CALIFORNIA ASSOCIATION OF NURSE ANESTHETISTS CRNA SCOPE OF PRACTICE GUIDELINES
 CALIFORNIA ASSOCIATION OF NURSE ANESTHETISTS CRNA SCOPE OF PRACTICE GUIDELINES The following offers guidance on the scope of practice for Certified Registered Nurse Anesthetists (CRNAs) in California.
CALIFORNIA ASSOCIATION OF NURSE ANESTHETISTS CRNA SCOPE OF PRACTICE GUIDELINES The following offers guidance on the scope of practice for Certified Registered Nurse Anesthetists (CRNAs) in California.
Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website.
 Local Coverage Determination (LCD): NERVE Blockade for Treatment of Chronic Pain and Neuropathy (L35457) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website.
Local Coverage Determination (LCD): NERVE Blockade for Treatment of Chronic Pain and Neuropathy (L35457) Links in PDF documents are not guaranteed to work. To follow a web link, please use the MCD Website.
Passionate concerns about welfare and ethics have created an environment where discussions about
 M e d i c a t i o n s P A I N M A N A G E M E N T Lysa Pam Posner, DVM, Diplomate ACVA North Carolina State University Analgesia for Declaw Patients Onychectomy in cats is controversial both within and
M e d i c a t i o n s P A I N M A N A G E M E N T Lysa Pam Posner, DVM, Diplomate ACVA North Carolina State University Analgesia for Declaw Patients Onychectomy in cats is controversial both within and
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Core Competencies for Addiction Medicine, Version 2
 Core Competencies for Addiction Medicine, Version 2 Core Competencies, Version 2, was approved by the Directors of the American Board of Addiction Medicine (ABAM) Foundation March 6, 2012 Core Competencies
Core Competencies for Addiction Medicine, Version 2 Core Competencies, Version 2, was approved by the Directors of the American Board of Addiction Medicine (ABAM) Foundation March 6, 2012 Core Competencies
CLINICAL PRIVILEGES- NURSE ANESTHETIST
 Name: Page 1 Initial Appointment Reappointment All new applicants must meet the following requirements as approved by the governing body effective: 8/5/2015. Applicant: Check off the Requested box for
Name: Page 1 Initial Appointment Reappointment All new applicants must meet the following requirements as approved by the governing body effective: 8/5/2015. Applicant: Check off the Requested box for
1. ANESTHESIA. Intensity/Complexity Fee $ (per 15 minutes Level Code or part thereof)
 1. ANESTHESIA Anesthesia Preamble The tariff is for all types of anesthetic service. This includes general and regional anesthesia, resuscitation and critical care, monitored anesthesia care, and any other
1. ANESTHESIA Anesthesia Preamble The tariff is for all types of anesthetic service. This includes general and regional anesthesia, resuscitation and critical care, monitored anesthesia care, and any other
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice
 PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
Complications Associated With Eye Blocks and Peripheral Nerve Blocks: An American Society of Anesthesiologists Closed Claims Analysis
 Complications Associated With Eye Blocks and Peripheral Nerve Blocks: An American Society of Anesthesiologists Closed Claims Analysis Lorri A. Lee, M.D., Karen L. Posner, Ph.D., Frederick W. Cheney, M.D.,
Complications Associated With Eye Blocks and Peripheral Nerve Blocks: An American Society of Anesthesiologists Closed Claims Analysis Lorri A. Lee, M.D., Karen L. Posner, Ph.D., Frederick W. Cheney, M.D.,
The Emergency Medical Services Milestone Project
 The Emergency Medical Services Milestone Project A Joint Initiative of The Accreditation Council for Graduate Medical Education and The American Board of Emergency Medicine July 2015 The Emergency Medical
The Emergency Medical Services Milestone Project A Joint Initiative of The Accreditation Council for Graduate Medical Education and The American Board of Emergency Medicine July 2015 The Emergency Medical
Home Dialysis Benchmarks Workgroup. Peritoneal Dialysis (PD)
 Home Dialysis Benchmarks Workgroup Peritoneal Dialysis (PD) Medical Knowledge Fellows must demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social behavioral
Home Dialysis Benchmarks Workgroup Peritoneal Dialysis (PD) Medical Knowledge Fellows must demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social behavioral
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
NORTHSIDE ANESTHESIOLOGY CONSULTANTS AND PAIN MANAGEMENT SERVICES
 NORTHSIDE ANESTHESIOLOGY CONSULTANTS AND PAIN MANAGEMENT SERVICES K. Douglas Smith, M.D. Chairman John B. Neeld, Jr., M.D. Sheryl S. Dickman, M.D. Alan R. Kaplan, M.D. Thomas B. West, M.D. Michael E. Maffett,
NORTHSIDE ANESTHESIOLOGY CONSULTANTS AND PAIN MANAGEMENT SERVICES K. Douglas Smith, M.D. Chairman John B. Neeld, Jr., M.D. Sheryl S. Dickman, M.D. Alan R. Kaplan, M.D. Thomas B. West, M.D. Michael E. Maffett,
Pediatric Anesthesia/Pediatric Cardiac Anesthesia/ Pain Management Elective
 Pediatric Anesthesia/Pediatric Cardiac Anesthesia/ Pain Management Elective Introduction: This elective may be undertaken as a full-time elective in pediatric anesthesia, pediatric cardiac anesthesia,
Pediatric Anesthesia/Pediatric Cardiac Anesthesia/ Pain Management Elective Introduction: This elective may be undertaken as a full-time elective in pediatric anesthesia, pediatric cardiac anesthesia,
Occupational Outlook Handbook, 2004-05 Edition
 Occupational Outlook Handbook, 2004-05 Edition U.S. Department of Labor Bureau of Labor Statistics Bulletin 2540 Registered Nurses + Chris is pleased with the favorable job outlook. Job security is important
Occupational Outlook Handbook, 2004-05 Edition U.S. Department of Labor Bureau of Labor Statistics Bulletin 2540 Registered Nurses + Chris is pleased with the favorable job outlook. Job security is important
Neurocritical Care Program Requirements
 Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS
 I. INTRODUCTION CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS Advance registered nurse practitioners (ARNPs) and clinical nurse practitioners (CNPs) have their scope
I. INTRODUCTION CHAPTER 27 THE SCOPE OF PROFESSIONAL NURSING PRACTICE AND ARNP AND CNM PROTOCOLS Advance registered nurse practitioners (ARNPs) and clinical nurse practitioners (CNPs) have their scope
MANAGEMENT OF CHRONIC NON MALIGNANT PAIN
 MANAGEMENT OF CHRONIC NON MALIGNANT PAIN Introduction The Manitoba Prescribing Practices Program (MPPP) recognizes the important role served by physicians in relieving pain and suffering and acknowledges
MANAGEMENT OF CHRONIC NON MALIGNANT PAIN Introduction The Manitoba Prescribing Practices Program (MPPP) recognizes the important role served by physicians in relieving pain and suffering and acknowledges
Medical Coverage Policy Monitored Anesthesia Care (MAC)
 Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
Postgraduate 2-years studies Pain Medicine supported by IASP
 Postgraduate 2-years studies Pain Medicine supported by IASP Jan Dobrogowski President of Polish Pain Society Head of Department of Pain Research and Therapy Chair of Anaesthesiology and Intensive Care
Postgraduate 2-years studies Pain Medicine supported by IASP Jan Dobrogowski President of Polish Pain Society Head of Department of Pain Research and Therapy Chair of Anaesthesiology and Intensive Care
