AMERICAN PUBLIC UNIVERSITY SYSTEM. Charles Town, West Virginia JAIL DIVERSION BENEFITS THE CRIMINAL JUSTICE SYSTEM AND STAKEHOLDERS IN THE COMMUNITY
|
|
|
- Clarence Patterson
- 8 years ago
- Views:
Transcription
1 1 AMERICAN PUBLIC UNIVERSITY SYSTEM Charles Town, West Virginia JAIL DIVERSION BENEFITS THE CRIMINAL JUSTICE SYSTEM AND STAKEHOLDERS IN THE COMMUNITY A thesis submitted in partial fulfillment of the requirements for the degree of MASTER OF ARTS In CRIMINAL JUSTICE By Christine Jones Department Approval Date: The author hereby grants the American Public University System the right to display these contents for educational purposes. The author assumes total responsibility for meeting the requirements set by United States Copyright Law for the inclusion of any materials that are not the author s creation or in the public domain.
2 Copyright 2011 by Christine Jones All rights reserved. 2
3 3 DEDICATION This body of work is dedicated to my husband Kenny, who patiently supported me while I spent hours at work on the computer. I also thank my sons Aaron and Dylan and granddaughters, Katelyn and Jaden, just because you make me happy. Mom, Dad, and Erika, thanks for believing in me and cheering me on.
4 4 ACKNOWLEDGEMENTS My gratitude to the staff at American Military University, I was always challenged to do my best and my work was held to the highest standards. The course work was a challenge and I am proud to be a graduate of the university. For this work I acknowledge Professor Muehlenbeck, her guidance throughout the course was invaluable and her assistance timely and friendly, thank you so much.
5 5 ABSTRACT OF THE THESIS JAIL DIVERSION BENEFITS THE CRIMINAL JUSTICE SYSTEM AND STAKEHOLDERS IN THE COMMUNITY By Christine Jones American Public University System, September 21, 2011 Charles Town, West Virginia Dr. Kerry L. Muehlenbeck, Thesis Professor The purpose of this research is to show that jail diversion for offenders with mental illness benefits both the criminal justice system and the stakeholders that provide for individuals with mental illness. Jail diversion seeks to divert mentally ill individuals from the criminal justice system and provide them with appropriate treatment of the disease and save taxpayer resources. The study makes use of peer reviewed journals, criminal justice and mental health system web sites, legislation, and personal conversation confirming that jail diversion reduces costs within the criminal justice system. The stakeholders in the community are mental and medical health care professionals, social service providers, and community support centers within the mental health system that treat and support individuals with mental illness. The stakeholders benefit by early intervention, providing treatment, and by providing support services that help mentally ill individuals return to the community. Providing these services are more difficult, if not impossible, to provide for mentally ill individuals wedged in the criminal justice system. In closing, the study will show that both the criminal justice and mental health systems benefit through jail diversion.
6 6 TABLE OF CONTENTS: CHAPTER PAGE I. Introduction.7 II. The Criminal Justice System 10 Law Enforcement.10 Corrections Courts...23 Probation and Parole 28 III. Mental Health Care History.. 35 Mental Health Care in Early America.35 Foundation for Institutionalization..36 Community Mental Health Movement...40 IV. The Mental Health System 40 Jail Diversion.42 Pre-Booking...43 Post-Booking...47 The Bexar County Jail Diversion Program..52 V. Conclusion.57 VI. References 60
7 7 Chapter I: Introduction In the early 1950 s and 60 s states began to close their public mental health hospitals in a process known as deinstitutionalization (Rivera, 2004). The idea to liberate persons from mental hospitals was a noble idea and part of the social changes of the times. The care and treatment of people that were institutionalized was questionable and forced institutionalization was seen as incomprehensible. This was the era of rapid change in mental health treatment and the heyday of the community health movement, which set in motion the closure of impersonal state hospitals and the return of the mentally ill to their families and communities (Marsh, 1994). However, the anticipated treatment in community health centers was not realized and resulted in the shift of many of the mentally ill from mental hospitals into the criminal justice system. The question of what to do with the mentally ill, especially those who violate laws, is not new as is evident in this statement recorded in the American Journal of Insanity in 1817, But the insane criminal has nowhere any home; no age or nation has provided a place for him, he is everywhere unwelcome and objectionable (Marsh, 1994, p. 1). The dilemma remains today as mentally ill persons, through their behavior, are often unwelcome in their home or community and subsequently find themselves arrested and in jail. This is not to oversimplify the plight of persons with mental illness, as it is a complicated social and medical issue with each individual and their families having their own personal experience. However, one can deduce from the definition of mental illness that a brain disorder may lead to behavior that can be criminalized. Mental illnesses are medical conditions that disrupt a person s thinking, feeling, mood, ability to relate to others and a diminished capacity for coping with the ordinary demands of life (National Alliance on Mental Illness [NAMI], 2011). Coping with the demands of ordinary life is challenging for those of sound mind and even more difficult for a person with mental illness especially those with serious mental illness. The number of Americans that have some degree of
8 8 mental illness is quite large. The National Institute of Mental Health (NIMH) reports that one in four adults or approximately 57.7 million Americans experience some type of mental health disorder in any given year; however, the main burden of illness is concentrated in those diagnosed with serious mental illness which occurs in about 6 percent, or 1 in 17 Americans (NAMI, 2011). The disruption in life caused by untreated mental illness may lead to a downward spiral of unemployment, homelessness, and self-medicating with alcohol and drugs. These circumstances leave the mentally ill, especially those with untreated serious mental illness, prone to involvement with the criminal justice system. It is acknowledged that there are thousands of persons in America diagnosed with varying degrees of mental illness and many of them end up in the criminal justice system. An estimated 11.4 million people are admitted to local jails every year in the United States and two million people are incarcerated in jails and prisons. Estimates indicate that 45 to 64 percent of those incarcerated in jails or prisons have some type of mental health problem (Mental Health America, 2001). These numbers represent persons who are taken to jail or sentenced to jail or prison; however, the criminal justice system involves much more than going to the county jail or prison. Mental health advocates posit that persons with mental illness are overrepresented in all parts of the criminal justice system; in their contact with law enforcement, in the courts, in jails and prisons, and in probation and parole caseloads across the country (Council of State Governments Justice Center [CSG Justice Center], 2006). This observation made by mental health advocates is shared with those in the criminal justice system as increasing numbers of mentally ill persons enter their system. Police arrest people with serious mental illness because few other options are available to handle their disruptive public behavior. Jail and prison administrators often struggle to treat and protect the mentally ill, judges grapple with limited sentencing alternatives for the mentally ill
9 9 who fall outside specific forensic categories, and probation and parole officers scramble to obtain scarce community services and treatment and struggle to monitor them with traditional case management strategies (Lurigio & Snowden, 2009). Advocates in the mental health system suggest that criminalization of the mentally ill is a consequence of a brain disorder and recommend treatment and care and the criminal justice system must accept into their system the mentally ill offender when no alternative is available (Torrey et al., 1992). The two systems have different agendas but share the commonality of dealing with the mentally ill and the collaboration between the systems would be beneficial, albeit the benefits would differ for each system. The benefits to the mental health system are incurred through treating the mentally ill and improving their place in the community and the benefits to the criminal justice system are public safety and cost savings. According to the CSG Justice Center (2006), there is no one solution to the problem of mentally ill persons involved in the criminal justice system; however, at each juncture of the criminal justice process, from before arrests to after release from jail, there are steps that criminal justice and mental health systems can take to improve their response to people with mental illness. The steps that are suggested are collaborations broadly referred to as jail diversion. According to Torrey (as cited in Steadman et al.), jail diversion programs should be set up to minimize the number of individuals with serious mental illness who end up in jail (p.1630). There are no identical jail diversion programs as each are created and developed specific to communities and their needs; however, one definition gives a general description of what jail diversion is. According to Florida Partners in Crisis (2010), the term "jail diversion" refers to programs that divert individuals with serious mental illness (and often co-occurring substance use disorders) away from jail and provide linkages to community-based treatment and
10 10 support services. Therefore, the individual avoids arrest or spends a significantly reduced time period in jail on the current charge or on violations of probation resulting from previous charges. Chapter II: The Criminal Justice System Criminal justice in the United States involves three interdependent agencies: law enforcement, courts, and corrections (jail and prison), operating at the federal, state, and local levels. Together, these agencies represent the criminal justice system (Caputo, 2004). The criminal justice system as a whole is costly to taxpayers at every level of government. Pustilnik (2005) states that responding to problems of mental illness principally through the criminal justice system imposes billions of dollars in costs annually to the public, estimating the annual incarceration costs alone of nonviolent offenders are approximately $5.95 billion. The amount of money spent goes up significantly when law enforcement and the courts are added into the cost. According to Bohm and Haley (2003), in 1999, local, state, and federal governments spent a total of $146 billion in direct expenditures for the civil and criminal justice systems. Collectively, law enforcement, corrections, and courts are each enormous systems, independent of one another, but interconnected just the same. Law Enforcement According to Steadman (1991), police involvement with the mentally ill is based on two legal principles; the police power function is to protect the safety and welfare of the public and parens patriae which involves protection for the disabled citizen. Police officers make contact with all citizens to include those with mental health problems and often time s individuals that are in a mental health crisis. Lamb, Weinberger, and DeCuir (2002) state that law enforcement agencies have played an increasingly important role in the management of persons who are experiencing psychiatric crises and police are often the first to be called to deal with persons with mental emergencies.
11 11 Police officers are tasked with responding to calls from the community, protecting citizens from harm, and upholding the law. Using their expertise and discretion they must decide if the circumstances warrant treatment or detention. It is clear that detention for minor disruptive behavior resulting from mental illness should not be a cause for detention in local jail; it is equally clear that very serious criminal behavior committed by persons who are seriously mentally ill warrants detention to accommodate criminal justice processing and community safety concerns (Steadman, 1991). Police officers that do not believe the person s behavior warrants arrest but recognize that some action must be taken are afforded another option through legislation provided in the health and safety code s written into states criminal code of procedures. States health and safety codes are relatively similar in all states and primarily guide law enforcement officers in emergency detention of individuals exhibiting harmful behavior. The Texas Health and Safety Code (2011) authorizes peace officers to take a person into custody if the officer believes the person is mentally ill and because of that illness there is a substantial risk of serious harm to the person or to others. If emergency detention is necessary, the person must then be taken immediately to the nearest mental health facility. The facilities that are intended to accept the citizens brought in by police officers are often unable to accommodate them because they are overcrowded and are forced to turn them away. Funding is always an issue with public amenities and mental health facilities are no exception. Budgets are being cut nationwide and many states are cutting budgets that fund mental health facilities. According to Torres (2011), in Texas, the Department of State Health Services has proposed an $80 million cut that could affect the state s 39 publicly supported community mental health centers. Many Texas cities may be affected and one that could see cuts include El Paso Mental Health and Mental Retardation (MHMR) which serves about 7,000 people and relies on $26 million in state money; without this funding, local leaders fear that a funding gap will crowd
12 12 El Paso s jails with the mentally ill (Torres, 2011). Budget cuts to mental health centers exasperate an already strained program. When community mental health centers are full it forces the police officer to take their detainee to a hospital for treatment and in some instances to jail. El Paso County Sheriff s Deputy A. Becerra is a member of the El Paso Inter Facility Task Force, a committee comprised of local law enforcement and mental health professionals and associates that is tasked with creating a jail diversion program in El Paso, Texas. Deputy Becerra stated that when the mental health facilities don t have room available they take emergency detention detainees to one of the six local hospital emergency rooms. The problem with this is that emergency rooms are already overloaded with patients with physical injuries and other medical conditions. Persons in a mental health crisis just do not fit in and usually have to sit there and wait to be seen. Deputy Becerra said that the hospital will contact MHMR and a representative will go to the hospital to evaluate the person. Sometimes the person will be referred to get additional treatment and sometimes they will be released after a few hours, it just depends (personal communication, October 26, 2011). This practice burdens already crowded emergency rooms and does not provide immediate care to the detainee. Based on the two legal principles of public safety and protecting the disabled citizen, police officers have a duty to act whether it is through emergency detention or jail. K. G. Jones, a detective and 23-year veteran with the El Paso Police Department, recalls emergency room doctors refusing to accept mentally ill detainees because nothing was wrong with them. This, he said, left me no other choice but to book them into jail on misdemeanor charges, because at least it would get them off the street and get them some kind of help (personal communication, October 29, 2011). Police officers may find the mental health option to be problematic. The problems associated with the mental health option for police are the long waiting periods in emergency rooms during which officers cannot attend to other duties. Health professionals may
13 13 question the judgment of police and refuse admission, or they may admit for only a brief hospital stay a person that just a short time before constituted a clear menace to the community (Lamb & Weinberger, 1998). The two scenarios provided by Deputy Becerra and Detective Jones indicate how a jail diversion facility specifically designated to accept emergency detainees brought in by police officers, staffed with mental health professionals and security, would be most advantageous. According to Steadman (as cited in Reuland, 2004), the best diversion model is one that has a single point of entry, a no refusal policy, and streamlined intake for police, all of these features make the service police-friendly and improves service delivery to the mentally ill. The diversion facility would ensure swift assessment and treatment, maintain public safety, and divert the detainee from the criminal justice system. Cost savings to law enforcement is translated in personnel and service. As stated, patrol officers are responsible for public safety and upholding the law. However, law enforcement administrators are tasked with the fiscal responsibilities and managing their agencies. According to Bennett and Hess (2004), in most law enforcement agencies budgets, salaries and wages account for the largest expenditure, typically 80 to 85 percent. A factor that is relative to law enforcement and cost savings is the concept that police are most effective when they are out in the community and available to take calls. Efficient use of personnel and providing timely service to the community are essential to law enforcement agencies. Costs must be managed if law enforcement agencies are to provide the services citizens expect and require (Bennett & Hess, 2004). Detective Jones time-consuming trip to the emergency room and subsequent trip to the jail, and Deputy Becerra s time in emergency waiting rooms were costly in time and in service to the community.
14 14 Corrections Marcia K. Goin, M.D., Ph.D., and president of the American Psychiatric Association, stated, Our jails and prisons have become the primary mental health care facilities in the United States today, this is a function these institutions are neither designed nor equipped to handle (The American Psychiatric Association, 2004, p. 1). Quietly but steadily, jails and prisons are replacing public mental hospitals as the primary purveyors of public psychiatric services for individuals with serious mental illness in the United States (Torrey, 1995). These bold statements are presented by professionals representing the mental health community and are shared by jail administrators. Reports from jail administrators from various county jails concur with the sentiment of the mental health professionals. E. Fuller Torrey, a research psychiatrist with NIMH, Neuropsychiatric Research Hospital in Washington, DC, conducted research and found that American county jails nationwide report that jails are overburdened with mentally ill inmates. Torrey (1995) found that county jail representatives from coast to coast shared a common theme: San Diego County jail assistant sheriff stated that his jail has become the bottom-line mental health provider in the county; Seattle s King County jail reported the jail has become King County s largest institution for the mentally ill; Travis County jail in Austin, Texas reported the jails psychiatric population rivals that of Austin State Hospital; Miami s Dade County reported, the jail usually houses more people with mental illness, more than any single institution or hospital in the county; and the Los Angeles County jail system stated that 3,300 of its 21,000 inmates require mental health services on a daily basis,; the basis for the claim that the
15 15 county jail has become de facto, the largest mental institution in the country. (pp ) Jail administrators have accepted that mentally ill inmates are a part of the jail population and have implemented systems to address their role as quasi-mental health facilities. There are three basic types of corrections agencies: jails which are run locally and are used to detain people while they await trial or for short sentences; prisons, run by states that provide long term incarceration; and community corrections agencies, such as probation and parole that supervise people in the community either in lieu of or in addition to jail and prison time (CSG Justice Center, 2006). By this definition all persons entering into this phase of the criminal justice system will be incarcerated in jail but not all of them will enter prison or be placed on probation or parole. According to Steadman (1991), when an apprehended person is transferred from the custody of law enforcement personnel to the custody of an officer in a jail, a significant criminal justice system boundary is crossed. The significance for the person being booked into jail is that at this point the options for the person are to post bail and be released with the promise to appear in court or wait in jail until they are scheduled for a court appearance. The significance for the jail is once the prisoner is booked into jail the county jail becomes responsible for their well-being and care and all the costs incurred with incarceration. The concerns of jail administration are the additional financial costs associated with housing mentally ill inmates by way of mental and medical health care, violent and destructive behavior, suicide watches, and the litigation concerns that present with each of these issues. Additionally, mentally ill inmates usually stay in jail longer than the general population adding to the cost of housing and opportunity for transgression to occur on the part of the inmate or jail staff.
16 16 When police bring their prisoners to jail the transfer of custody transpires through a process referred to as intake or booking. Once this process is complete, the prisoner is now referred to as an inmate and in the care of jail staff. It is at this point that jail staff screen for mental and medical health problems and suicidal tendencies. This was not always the case but experience, education, and litigation have established the screening process that specifically questions the inmate s medical condition, mental health history and suicidal tendencies. Borne through lawsuits costing taxpayers millions of dollars in punitive damages screening incoming inmates and subsequent care have become high priority for jail administrators. Both class action lawsuits on behalf of groups of mentally ill prisoners and lawsuits by individuals suffering from mental illness have resulted in large liability awards in specific cases (Farber, 2009). Jails are rife with potential lawsuits; excessive use of force and deprivation of rights are common jail lawsuits. However, lawsuits stemming from inadequate mental health screening and subsequent care are all too common and very costly. In addition to monetary awards for the plaintiff, facilities were ordered to write policies that would improve intake procedures and follow up care for the mentally ill. In the case of D. M. v. Terhune (1999), the state of New Jersey reached a wide-ranging $16 million settlement in a lawsuit over alleged inadequate treatment of mentally-ill prisoners and disability discrimination against them, it also ordered that all new prisoners were to receive a mental health assessment within 72 hours of their incarceration. This settlement is one of many that have spearheaded improvements in screening, assessment and treatment of mentally ill inmates. According to Ford et al. (2007), jails and prisons have a substantial legal obligation to provide mental health care for inmates although case law and statues have not provided a clear definition of what constitutes adequate mental health care.
17 17 To help guide jail administrators, mental health advocates have suggested minimum criteria to improve their intake procedure and continuity of care throughout their incarceration. The American Psychiatric Association (APA) has recommended that all jails provide at minimum mental health screening, referral, and evaluation: crisis intervention and short term treatment (most often medication); and discharge and pre-release planning (Steadman, Scott, Osher, Angnese, & Robbins, 2005). This recommendation requires cooperation between jail administrators and clinic staff and would ensure that care is given at multiple phases of incarceration. El Paso Sheriff s Office Jail Annex Director of Nursing, A. Pina, stated: We are obligated by law to conduct mental health screening covering aspects of mental health such as history of bipolar, schizophrenia, history of suicide and victimization. All inmates with any mental health disorder will be evaluated within 14 days of admission to the jail. After diagnosis a follow up is conducted within two months or sooner if the inmate requests one. In a crisis, most events of psychosis are treated with an injection and may be forced as applicable by Texas law. Short-term treatment is given by prescribing medication. Discharge planning is discussed and a form is given to them upon release that provides them with local clinics in the event that medical treatment is needed. We also provide a 3- day supply of medication when the inmate is released. The jail clinic and MHMR communicate about pre-release planning and share lists of clients to ensure continuity of care after discharge from the jail system (personal communication, November 3, 2011). Pina s assertion of care from intake and throughout incarceration is a testament to the jail s willingness to provide care and is commendable. It should be noted that providing these services is expensive. To achieve this level of care jails must invest in retaining
18 18 specially trained mental health care personnel and provide costly psychotropic medication during and after release. Some states have mandated jail standards that specifically address mental health screening and assessment to ensure the best practices and policies are in place to avoid lawsuits and to protect the mentally ill inmate. Texas is one state that has mandatory standards to which all county jails must adhere. The Texas Legislature created the Texas Commission on Jail Standards (TCJS, n.d.) in 1975 to implement a declared state policy that all county jail facilities conform to minimum standards of construction, maintenance and operation. The standards are general in language and allow each jail administrator to write policy and procedure to meet the minimum standards of operation. The commission dedicated a chapter to the standards that must be met regarding mental disabilities and suicide prevention. TCJS (n.d.) approved a plan, dated March 31, 1997, that ordered each sheriff to develop and implement disabilities/suicide prevention plan, in coordination with available medical and mental health officials. The plan requires provisions for staff training, intake screening, communication, special housing, adequate supervision, intervention and emergency treatment, reporting procedures for completed suicides, follow-up on policies following attempted or completed suicides, and screening instruments. In addition, it requires that during intake inmates will be checked against the Department of State Health Services system to determine if the inmate has previously received state mental healthcare. Not all jails are mandated by law to provide screening or care, but jail administrators that fail to implement the most basic care resulting in egregious neglect face costly law suits. Dona Ana County, New Mexico faced a lawsuit that was filed on behalf of jail inmates who alleged the county jail failed to provide mental health care. Dona Ana County officials settled a class action lawsuit with 14 jail inmates, who alleged the county routinely failed to
19 19 provide adequate mental health care to its detainees in 2006 and 2007, costing the county $400,000, and forced the jail to make a number of changes to polices including new mental health care staffing and monitoring of inmates mental condition (Alba, 2010). The Las Cruces Police Department, in Dona Ana County, was also named in the lawsuit. According to Alba (2010), the plaintiffs claimed the police departments practice was to use the jail as a de facto mental health care holding facility for mentally ill residents who had not committed a serious crime, the lawsuit ordered the department to provide police officers training in crisis intervention and asked that officers seek options other than arrest for people who seem to have a mental disability. Police departments and jails should not ignore the need for police training or the care of inmates with mental illness that are in jail; however, the community at large should be aware of how their tax dollars are being spent by city and county run departments. Dona Ana County spokesman Jess Williams said, Counties are obligated by law to run jails and recognize the reality of the increased responsibilities and costs of providing social services, but the public should know that the funds required to provide these services are funds that cannot be used for other county programs and services (Alba, 2010, p. 1). The lawsuit resulted in training for police officers and suggested that officers seek options other than arrest and jail but did not provide the officers with any other options. Jail diversion is an option that would provide an alternative facility for the trained police officer to take a mentally ill person in crisis and reduce the number of mentally ill inmates needing costly care in the jail. It is clear from the Dona Ana County Jail and the City of Las Cruces Police Department lawsuit that although they are separate agencies and their missions are different they are a part of the criminal justice system and costly lawsuits are not conducive to either agency or the taxpaying citizens. It is evident that jail administrators consider their jails as miniature
20 20 psychiatric hospitals and many jail administrators have accepted that mentally ill inmates are and will be a part of their population. In 2000, nearly 95 % of all state adult correctional facilities screened inmates for mental health problems, and of the nation s 1,558 state, public and private adult facilities, 1,394 reported that they provided mental health services to their inmates (Rivera, 2004). With the majority of jails and prisons participating in mental health services they do so at an exaggerated cost. Research indicates that it costs less to house a person in a jail diversion facility than to house a person in a jail or prison. According to Steverman and Lubin (2007), community mental health care can be costly, but it is far cheaper than incarceration, it costs around $26 a day to treat someone in a community mental health program, but it can cost more than $65 a day to keep them in jail. Cost shifting between mental health care and criminal justice systems is problematic. It is accepted that social services must be provided but deciding which system will fund the care and where the care is provided is challenging. Texas representative, John E. Davis explained, You can pay now or you are going to pay later and stated, we have to spend money up front for prevention, community services and support for people with mental health needs or you ll end up housing them in the prison system (Steverman & Lubin, 2007, p.20). There is credible research that attest to the higher costs associated with housing mentally ill inmates and the view that jail is not conducive to treating the mentally ill making compelling arguments for implementing jail diversion in communities. Care for mentally ill inmates costs the criminal justice system far more than caring for inmates without mental illness. Studies show that it costs approximately 75 % more to incarcerate individuals with mental illness than other inmates with the same charge (Cowell, Aldridge, Broner, & Hinde 2008). The cost of housing inmates is expensive in itself and the cost of housing mentally ill inmates drive that cost up even more. The American Psychiatric
Austin Travis County Integral Care Jail Diversion Programs and Strategies
 Jail Diversion Diversion programs serve as critical strategies in preventing people with mental illness who commit crimes from entering or unnecessarily remaining in the criminal justice system. Interception
Jail Diversion Diversion programs serve as critical strategies in preventing people with mental illness who commit crimes from entering or unnecessarily remaining in the criminal justice system. Interception
WHAT IS THE ILLINOIS CENTER OF EXCELLENCE AND HOW DID IT START? MISSION STATEMENT
 WHAT IS THE ILLINOIS CENTER OF EXCELLENCE AND HOW DID IT START? MISSION STATEMENT The mission of the Illinois Center of Excellence for Behavioral Health and Justice is to equip communities to appropriately
WHAT IS THE ILLINOIS CENTER OF EXCELLENCE AND HOW DID IT START? MISSION STATEMENT The mission of the Illinois Center of Excellence for Behavioral Health and Justice is to equip communities to appropriately
How To Run A Diversion Program In Connecticut
 Connecticut's Criminal Justice Diversion Program: A Comprehensive Community Forensic Mental Health Model By Linda Frisman, Gail Sturges, Madelon Baranoski, and Michael Levinson, Contributing Writers Connecticut,
Connecticut's Criminal Justice Diversion Program: A Comprehensive Community Forensic Mental Health Model By Linda Frisman, Gail Sturges, Madelon Baranoski, and Michael Levinson, Contributing Writers Connecticut,
CORRELATES AND COSTS
 ANOTHER LOOK AT MENTAL ILLNESS AND CRIMINAL JUSTICE INVOLVEMENT IN TEXAS: CORRELATES AND COSTS Decision Support Unit Mental Health and Substance Abuse Services Another Look at Mental Illness and Criminal
ANOTHER LOOK AT MENTAL ILLNESS AND CRIMINAL JUSTICE INVOLVEMENT IN TEXAS: CORRELATES AND COSTS Decision Support Unit Mental Health and Substance Abuse Services Another Look at Mental Illness and Criminal
GETTING THROUGH THE CRIMINAL JUSTICE SYSTEM
 GETTING THROUGH THE CRIMINAL JUSTICE SYSTEM ARREST An ARREST starts the criminal justice process. It is called an arrest whether the police officer hands you a summons or puts handcuffs on you and takes
GETTING THROUGH THE CRIMINAL JUSTICE SYSTEM ARREST An ARREST starts the criminal justice process. It is called an arrest whether the police officer hands you a summons or puts handcuffs on you and takes
Criminal Justice 101. The Criminal Justice System in Colorado and the Impact on Individuals with Mental Illness. April 2009
 Criminal Justice 101 The Criminal Justice System in Colorado and the Impact on Individuals with Mental Illness April 2009 Acronyms DOC = Department of Corrections DYC = Division of Youth Corrections DCJ
Criminal Justice 101 The Criminal Justice System in Colorado and the Impact on Individuals with Mental Illness April 2009 Acronyms DOC = Department of Corrections DYC = Division of Youth Corrections DCJ
(2) If you have no other information regarding his mental illness, you might contact the county mental health coordinator at 214 875 2323
 CHECKLIST FOR DEFENDANTS WITH MENTAL HEALTH ISSUES IN DALLAS (see below for more information and for defense attorneys outside Dallas County) (1) What is the diagnosed mental illness? The defense attorney
CHECKLIST FOR DEFENDANTS WITH MENTAL HEALTH ISSUES IN DALLAS (see below for more information and for defense attorneys outside Dallas County) (1) What is the diagnosed mental illness? The defense attorney
court. However, without your testimony the defendant might go unpunished.
 Office of State Attorney Michael J. Satz VICTIM RIGHTS BROCHURE YOUR RIGHTS AS A VICTIM OR WITNESS: CRIMINAL JUSTICE PROCESS The stages of the criminal justice system are as follows: We realize that for
Office of State Attorney Michael J. Satz VICTIM RIGHTS BROCHURE YOUR RIGHTS AS A VICTIM OR WITNESS: CRIMINAL JUSTICE PROCESS The stages of the criminal justice system are as follows: We realize that for
Jail Diversion & Behavioral Health
 Jail Diversion & Behavioral Health Correctional Health Reentry Meeting Mandy Gilman, Director of Public Policy & Research Association for Behavioral Healthcare Association for Behavioral Healthcare Statewide
Jail Diversion & Behavioral Health Correctional Health Reentry Meeting Mandy Gilman, Director of Public Policy & Research Association for Behavioral Healthcare Association for Behavioral Healthcare Statewide
Maricopa County Attorney s Office Adult Criminal Case Process
 The following is a brief description of the process to prosecute an adult accused of committing a felony offense. Most misdemeanor offenses are handled by municipal prosecutors; cases involving minors
The following is a brief description of the process to prosecute an adult accused of committing a felony offense. Most misdemeanor offenses are handled by municipal prosecutors; cases involving minors
Proposition 5. Nonviolent Offenders. Sentencing, Parole and Rehabilitation. Statute.
 Proposition 5 Nonviolent Offenders. Sentencing, Parole and Rehabilitation. Statute. SUMMARY This measure (1) expands drug treatment diversion programs for criminal offenders, (2) modifies parole supervision
Proposition 5 Nonviolent Offenders. Sentencing, Parole and Rehabilitation. Statute. SUMMARY This measure (1) expands drug treatment diversion programs for criminal offenders, (2) modifies parole supervision
Criminal Justice System Commonly Used Terms & Definitions
 Criminal Justice System Commonly Used Terms & Definitions A B C D E F G H I J K L M N O P Q R S T U V W X Y Z Accused: Acquittal: Adjudication: Admissible Evidence: Affidavit: Alford Doctrine: Appeal:
Criminal Justice System Commonly Used Terms & Definitions A B C D E F G H I J K L M N O P Q R S T U V W X Y Z Accused: Acquittal: Adjudication: Admissible Evidence: Affidavit: Alford Doctrine: Appeal:
Mental Health Needs of Juvenile Offenders. Mental Health Needs of Juvenile Offenders. Juvenile Justice Guide Book for Legislators
 Mental Health Needs of Juvenile Offenders Mental Health Needs of Juvenile Offenders Juvenile Justice Guide Book for Legislators Mental Health Needs of Juvenile Offenders Introduction Children with mental
Mental Health Needs of Juvenile Offenders Mental Health Needs of Juvenile Offenders Juvenile Justice Guide Book for Legislators Mental Health Needs of Juvenile Offenders Introduction Children with mental
AN ACT. The goals of the alcohol and drug treatment divisions created under this Chapter include the following:
 ENROLLED Regular Session, 1997 HOUSE BILL NO. 2412 BY REPRESENTATIVE JACK SMITH AN ACT To enact Chapter 33 of Title 13 of the Louisiana Revised Statutes of 1950, comprised of R.S. 13:5301 through 5304,
ENROLLED Regular Session, 1997 HOUSE BILL NO. 2412 BY REPRESENTATIVE JACK SMITH AN ACT To enact Chapter 33 of Title 13 of the Louisiana Revised Statutes of 1950, comprised of R.S. 13:5301 through 5304,
FLORIDA STATE UNIVERSITY POLICE DEPARTMENT Chief David L. Perry
 FLORIDA STATE UNIVERSITY POLICE DEPARTMENT Chief David L. Perry 830 West Jefferson Street 850-644-1234 VICTIMS' RIGHTS BROCHURE YOUR RIGHTS AS A VICTIM OR WITNESS: ------- We realize that for many persons,
FLORIDA STATE UNIVERSITY POLICE DEPARTMENT Chief David L. Perry 830 West Jefferson Street 850-644-1234 VICTIMS' RIGHTS BROCHURE YOUR RIGHTS AS A VICTIM OR WITNESS: ------- We realize that for many persons,
AB 109 is DANGEROUS. Governor Brown signed AB 109 the Criminal Justice Realignment Bill into law on April 5, 2011.
 AB 109 is DANGEROUS Governor Brown signed AB 109 the Criminal Justice Realignment Bill into law on April 5, 2011. Governor Brown stated in his signing message on AB 109 - "For too long, the state s prison
AB 109 is DANGEROUS Governor Brown signed AB 109 the Criminal Justice Realignment Bill into law on April 5, 2011. Governor Brown stated in his signing message on AB 109 - "For too long, the state s prison
Mental Health Court 101
 Mental Health Court 101 2007 Georgia Drug & DUI Court Conference Peachtree City, GA Honorable Kathlene Gosselin, Hall County Superior Court & H.E.L.P. Program Team While the number of patients in psychiatric
Mental Health Court 101 2007 Georgia Drug & DUI Court Conference Peachtree City, GA Honorable Kathlene Gosselin, Hall County Superior Court & H.E.L.P. Program Team While the number of patients in psychiatric
ELEVENTH JUDICIAL CRIMINAL MENTAL HEALTH PROJECT Program Summary. Impact to the Community
 ELEVENTH JUDICIAL CRIMINAL MENTAL HEALTH PROJECT Program Summary The Eleventh Judicial Circuit Criminal Mental Health Project (CMHP) was established in 2000 to divert individuals with serious mental illnesses
ELEVENTH JUDICIAL CRIMINAL MENTAL HEALTH PROJECT Program Summary The Eleventh Judicial Circuit Criminal Mental Health Project (CMHP) was established in 2000 to divert individuals with serious mental illnesses
Glossary of Terms Acquittal Affidavit Allegation Appeal Arraignment Arrest Warrant Assistant District Attorney General Attachment Bail Bailiff Bench
 Glossary of Terms The Glossary of Terms defines some of the most common legal terms in easy-tounderstand language. Terms are listed in alphabetical order. A B C D E F G H I J K L M N O P Q R S T U V W
Glossary of Terms The Glossary of Terms defines some of the most common legal terms in easy-tounderstand language. Terms are listed in alphabetical order. A B C D E F G H I J K L M N O P Q R S T U V W
Mental Health Courts: Solving Criminal Justice Problems or Perpetuating Criminal Justice Involvement?
 Mental Health Courts: Solving Criminal Justice Problems or Perpetuating Criminal Justice Involvement? Monday, September 21 st, 2015 3 PM EDT Mental Health America Regional Policy Council Mental Health
Mental Health Courts: Solving Criminal Justice Problems or Perpetuating Criminal Justice Involvement? Monday, September 21 st, 2015 3 PM EDT Mental Health America Regional Policy Council Mental Health
Information for Crime Victims and Witnesses
 Office of the Attorney General Information for Crime Victims and Witnesses MARCH 2009 LAWRENCE WASDEN Attorney General Criminal Law Division Special Prosecutions Unit Telephone: (208) 332-3096 Fax: (208)
Office of the Attorney General Information for Crime Victims and Witnesses MARCH 2009 LAWRENCE WASDEN Attorney General Criminal Law Division Special Prosecutions Unit Telephone: (208) 332-3096 Fax: (208)
How To Fund A Mental Health Court
 Mental Health Courts: A New Tool By Stephanie Yu, Fiscal Analyst For fiscal year (FY) 2008-09, appropriations for the Judiciary and the Department of Community Health (DCH) include funding for a mental
Mental Health Courts: A New Tool By Stephanie Yu, Fiscal Analyst For fiscal year (FY) 2008-09, appropriations for the Judiciary and the Department of Community Health (DCH) include funding for a mental
Mental Illness, Addiction and the Whatcom County Jail
 March 1, 015 Mental Illness, Addiction and the Whatcom County Jail Bill Elfo, Sheriff Whatcom County America is experiencing a disturbing and increasing trend in the number of offenders housed in its county
March 1, 015 Mental Illness, Addiction and the Whatcom County Jail Bill Elfo, Sheriff Whatcom County America is experiencing a disturbing and increasing trend in the number of offenders housed in its county
Morgan County Prosecuting Attorney Debra MH McLaughlin
 Morgan County Prosecuting Attorney Debra MH McLaughlin Directions: From Fairfax Street Entrance, Enter Main Door, turn Right through door, up the narrow staircase. Office is at top of steps. (Old Circuit
Morgan County Prosecuting Attorney Debra MH McLaughlin Directions: From Fairfax Street Entrance, Enter Main Door, turn Right through door, up the narrow staircase. Office is at top of steps. (Old Circuit
Glossary of Court-related Terms
 Glossary of Court-related Terms Acquittal Adjudication Appeal Arraignment Arrest Bail Bailiff Beyond a reasonable doubt Burden of proof Capital offense Certification Charge Circumstantial evidence Citation
Glossary of Court-related Terms Acquittal Adjudication Appeal Arraignment Arrest Bail Bailiff Beyond a reasonable doubt Burden of proof Capital offense Certification Charge Circumstantial evidence Citation
IAC 7/2/08 Parole Board[205] Ch 11, p.1. CHAPTER 11 PAROLE REVOCATION [Prior to 2/22/89, Parole, Board of[615] Ch 7]
![IAC 7/2/08 Parole Board[205] Ch 11, p.1. CHAPTER 11 PAROLE REVOCATION [Prior to 2/22/89, Parole, Board of[615] Ch 7] IAC 7/2/08 Parole Board[205] Ch 11, p.1. CHAPTER 11 PAROLE REVOCATION [Prior to 2/22/89, Parole, Board of[615] Ch 7]](/thumbs/30/14732577.jpg) IAC 7/2/08 Parole Board[205] Ch 11, p.1 CHAPTER 11 PAROLE REVOCATION [Prior to 2/22/89, Parole, Board of[615] Ch 7] 205 11.1(906) Voluntary termination of parole. Any voluntary termination of parole should
IAC 7/2/08 Parole Board[205] Ch 11, p.1 CHAPTER 11 PAROLE REVOCATION [Prior to 2/22/89, Parole, Board of[615] Ch 7] 205 11.1(906) Voluntary termination of parole. Any voluntary termination of parole should
JUDICIAL ORIENTATION NEW COUNTY JUDGES: MENTAL HEALTH. Topics. Hypothetical Scenarios
 JUDICIAL ORIENTATION NEW COUNTY JUDGES: MENTAL HEALTH February 6, 2015 Professor Brian Shannon Texas Tech University School of Law Topics Serious mental illnesses Emergency Detention Civil Commitment Process
JUDICIAL ORIENTATION NEW COUNTY JUDGES: MENTAL HEALTH February 6, 2015 Professor Brian Shannon Texas Tech University School of Law Topics Serious mental illnesses Emergency Detention Civil Commitment Process
Issue Brief. State and County Collaboration: Mental Health and the Criminal Justice System
 Issue Brief State and County Collaboration: Mental Health and the Criminal Justice System December 2008 Issue Brief State and County Collaboration: Mental Health and the Criminal Justice System Produced
Issue Brief State and County Collaboration: Mental Health and the Criminal Justice System December 2008 Issue Brief State and County Collaboration: Mental Health and the Criminal Justice System Produced
Written statement of the American Psychological Association. Hearing before the United States Senate Committee on the Judiciary
 Written statement of the American Psychological Association Hearing before the United States Senate Committee on the Judiciary Breaking the Cycle: Mental Health and the Justice System February 10, 2016
Written statement of the American Psychological Association Hearing before the United States Senate Committee on the Judiciary Breaking the Cycle: Mental Health and the Justice System February 10, 2016
httpjlceo.lacounty.gov
 WILLIAM T FUJIOKA Chief Executive Offcer County of Los Angeles CHIEF EXECUTIVE OFFICE Kenneth Hahn Hall of Administration 500 West Temple Street, Room 713, Los Angeles, California 90012 (213) 974-1101
WILLIAM T FUJIOKA Chief Executive Offcer County of Los Angeles CHIEF EXECUTIVE OFFICE Kenneth Hahn Hall of Administration 500 West Temple Street, Room 713, Los Angeles, California 90012 (213) 974-1101
Marin County s STAR Program: Support and Treatment for Mentally Ill Offenders
 Marin County s STAR Program: Support and Treatment for Mentally Ill Offenders Marcella Velasquez EXECUTIVE SUMMARY Overrepresentation of the mentally ill in prisons and jails and limited mental health
Marin County s STAR Program: Support and Treatment for Mentally Ill Offenders Marcella Velasquez EXECUTIVE SUMMARY Overrepresentation of the mentally ill in prisons and jails and limited mental health
It s time to shift gears on criminal justice VOTER
 It s time to shift gears on criminal justice VOTER TOOLKIT 2014 Who are the most powerful elected officials most voters have never voted for? ANSWER: Your District Attorney & Sheriff THE POWER OF THE DISTRICT
It s time to shift gears on criminal justice VOTER TOOLKIT 2014 Who are the most powerful elected officials most voters have never voted for? ANSWER: Your District Attorney & Sheriff THE POWER OF THE DISTRICT
An Introduction to the Federal Public Defender=s Office and the Federal Court System
 Some Things You Should Know An Introduction to the Federal Public Defender=s Office and the Federal Court System Office of the Federal Public Defender Southern District of West Virginia 300 Virginia Street
Some Things You Should Know An Introduction to the Federal Public Defender=s Office and the Federal Court System Office of the Federal Public Defender Southern District of West Virginia 300 Virginia Street
Community Supervision Texas Association of Counties October 2015
 10/26/2015 Community Supervision Texas Association of Counties October 2015 Presented by District Judge Todd Blomerth, 421 st Judicial District Court of Caldwell County 1 10/26/2015 2 10/26/2015 Your Possible
10/26/2015 Community Supervision Texas Association of Counties October 2015 Presented by District Judge Todd Blomerth, 421 st Judicial District Court of Caldwell County 1 10/26/2015 2 10/26/2015 Your Possible
Chapter 3. Justice Process at the County Level. Brooks County Courthouse
 Chapter 3 Justice Process at the County Level Brooks County Courthouse Chapter Three: Judice Process at the County Level Developmental Assets: Life Skills: TEKS: Objectives: 10. Safety 30. Responsibility
Chapter 3 Justice Process at the County Level Brooks County Courthouse Chapter Three: Judice Process at the County Level Developmental Assets: Life Skills: TEKS: Objectives: 10. Safety 30. Responsibility
Pretrial Diversion Programs
 Pretrial Diversion Programs Research Summary Prepared by: Catherine Camilletti, Ph.D. CSR, Incorporated 2107 Wilson Boulevard, Suite 1000 Arlington, VA 20001 www.csrincorporated.com Under Contract No.
Pretrial Diversion Programs Research Summary Prepared by: Catherine Camilletti, Ph.D. CSR, Incorporated 2107 Wilson Boulevard, Suite 1000 Arlington, VA 20001 www.csrincorporated.com Under Contract No.
External Advisory Group Meeting June 2, 2015
 External Advisory Group Meeting June 2, 2015 1. There seems to be an extended wait from disposition to sentence where defendants are in jail awaiting the completion of the pre-sentence report. How many
External Advisory Group Meeting June 2, 2015 1. There seems to be an extended wait from disposition to sentence where defendants are in jail awaiting the completion of the pre-sentence report. How many
Frequently Asked Questions (FAQ)
 The Affordable Care Act (ACA) and Justice-Involved Populations 1. Can Medicaid pay for any health care services provided within jails or prisons? No. Under the ACA (and prior to the ACA), no health care
The Affordable Care Act (ACA) and Justice-Involved Populations 1. Can Medicaid pay for any health care services provided within jails or prisons? No. Under the ACA (and prior to the ACA), no health care
COPE Collaborative Opportunities for Positive Experiences
 COPE Collaborative Opportunities for Positive Experiences The Deferred Prosecution Program of the Travis County Juvenile Mental Health Court Project COPE PROGRAM DESCRIPTION An Introduction The Travis
COPE Collaborative Opportunities for Positive Experiences The Deferred Prosecution Program of the Travis County Juvenile Mental Health Court Project COPE PROGRAM DESCRIPTION An Introduction The Travis
Reentry on Steroids! NADCP 2013
 Reentry on Steroids! NADCP 2013 Panel Introductions Judge Keith Starrett Moderator Judge Robert Francis Panelist Judge Stephen Manley Panelist Charles Robinson - Panelist Dallas SAFPF 4-C Reentry Court
Reentry on Steroids! NADCP 2013 Panel Introductions Judge Keith Starrett Moderator Judge Robert Francis Panelist Judge Stephen Manley Panelist Charles Robinson - Panelist Dallas SAFPF 4-C Reentry Court
PROPOSAL. Expansion of Drug Treatment Diversion Programs. December 18, 2007
 December 18, 2007 Hon. Edmund G. Brown Jr. Attorney General 1300 I Street, 17 th Floor Sacramento, California 95814 Attention: Ms. Krystal Paris Initiative Coordinator Dear Attorney General Brown: Pursuant
December 18, 2007 Hon. Edmund G. Brown Jr. Attorney General 1300 I Street, 17 th Floor Sacramento, California 95814 Attention: Ms. Krystal Paris Initiative Coordinator Dear Attorney General Brown: Pursuant
Involuntary Admissions & Treatment Facts and Procedures
 Involuntary Admissions & Treatment Facts and Procedures Marcia Horan Assistant State s Attorney, Cook County Seniors and Persons with Disabilities Division WHEN IS INVOLUNTARY ADMISSION APPROPRIATE? The
Involuntary Admissions & Treatment Facts and Procedures Marcia Horan Assistant State s Attorney, Cook County Seniors and Persons with Disabilities Division WHEN IS INVOLUNTARY ADMISSION APPROPRIATE? The
(1) Sex offenders who have been convicted of: * * * an attempt to commit any offense listed in this subdivision. (a)(1). * * *
 House Proposal of Amendment S. 292 An act relating to term probation, the right to bail, medical care of inmates, and a reduction in the number of nonviolent prisoners, probationers, and detainees. The
House Proposal of Amendment S. 292 An act relating to term probation, the right to bail, medical care of inmates, and a reduction in the number of nonviolent prisoners, probationers, and detainees. The
Purpose of the Victim/Witness Unit
 Purpose of the Victim/Witness Unit The Victim/Witness Assistance Division of the Lake County State s Attorney s Office was formed to serve the needs of people like you. The division is meant to ensure
Purpose of the Victim/Witness Unit The Victim/Witness Assistance Division of the Lake County State s Attorney s Office was formed to serve the needs of people like you. The division is meant to ensure
SENTENCING REFORM FOR NONVIOLENT OFFENSES: BENEFITS AND ESTIMATED SAVINGS FOR ILLINOIS
 SENTENCING REFORM FOR NONVIOLENT OFFENSES: BENEFITS AND ESTIMATED SAVINGS FOR ILLINOIS LISE MCKEAN, PH.D. SUSAN K. SHAPIRO CENTER FOR IMPACT RESEARCH OCTOBER 2004 ACKNOWLEDGEMENTS PROJECT FUNDER Chicago
SENTENCING REFORM FOR NONVIOLENT OFFENSES: BENEFITS AND ESTIMATED SAVINGS FOR ILLINOIS LISE MCKEAN, PH.D. SUSAN K. SHAPIRO CENTER FOR IMPACT RESEARCH OCTOBER 2004 ACKNOWLEDGEMENTS PROJECT FUNDER Chicago
Orange County, Texas Adult Criminal Justice Data Sheet
 Orange County, Texas Adult Criminal Justice Data Sheet For more information, contact Dr. Ana Yáñez- Correa at acorrea@texascjc.org, or (512) 587-7010. The Texas Criminal Justice Coalition seeks the implementation
Orange County, Texas Adult Criminal Justice Data Sheet For more information, contact Dr. Ana Yáñez- Correa at acorrea@texascjc.org, or (512) 587-7010. The Texas Criminal Justice Coalition seeks the implementation
Best Practices in Mental Health at Corrections Facilities
 POLICY BRIEF November 2011 Best Practices in Mental Health at Corrections Facilities Sahil Jain Introduction Police, court personnel, and correctional staff interact with, stabilize, and treat more persons
POLICY BRIEF November 2011 Best Practices in Mental Health at Corrections Facilities Sahil Jain Introduction Police, court personnel, and correctional staff interact with, stabilize, and treat more persons
State Policy Implementation Project
 State Policy Implementation Project CIVIL CITATIONS FOR MINOR OFFENSES Explosive growth in the number of misdemeanor cases has placed a significant burden on local and state court systems. Throughout the
State Policy Implementation Project CIVIL CITATIONS FOR MINOR OFFENSES Explosive growth in the number of misdemeanor cases has placed a significant burden on local and state court systems. Throughout the
SHORT TITLE: Criminal procedure; creating the Oklahoma Drug Court Act; codification; emergency.
 SHORT TITLE: Criminal procedure; creating the Oklahoma Drug Court Act; codification; emergency. STATE OF OKLAHOMA 2nd Session of the 45th Legislature (1996) SENATE BILL NO. 1153 By: Hobson AS INTRODUCED
SHORT TITLE: Criminal procedure; creating the Oklahoma Drug Court Act; codification; emergency. STATE OF OKLAHOMA 2nd Session of the 45th Legislature (1996) SENATE BILL NO. 1153 By: Hobson AS INTRODUCED
INFORMATION FOR CRIME VICTIMS AND WITNESSES CHARLES I. WADAMS PROSECUTING ATTORNEY
 INFORMATION FOR CRIME VICTIMS AND WITNESSES CHARLES I. WADAMS PROSECUTING ATTORNEY Garden City, Idaho 6015 Glenwood St., Garden City, ID 83714 (208) 472-2900 www.gardencityidaho.org A MESSAGE Garden City
INFORMATION FOR CRIME VICTIMS AND WITNESSES CHARLES I. WADAMS PROSECUTING ATTORNEY Garden City, Idaho 6015 Glenwood St., Garden City, ID 83714 (208) 472-2900 www.gardencityidaho.org A MESSAGE Garden City
MEDINA COUNTY COMMON PLEAS COURT EARLY INTERVENTION PRE-TRIAL PROGRAM
 MEDINA COUNTY COMMON PLEAS COURT EARLY INTERVENTION PRE-TRIAL PROGRAM JUDGE CHRISTOPHER J. COLLIER Courtroom #1 Christine Demlow, Program Coordinator (330) 725-9131 Starting January 1, 2014, Judge Collier
MEDINA COUNTY COMMON PLEAS COURT EARLY INTERVENTION PRE-TRIAL PROGRAM JUDGE CHRISTOPHER J. COLLIER Courtroom #1 Christine Demlow, Program Coordinator (330) 725-9131 Starting January 1, 2014, Judge Collier
JUVENILE JUSTICE SYSTEM
 JUVENILE JUSTICE SYSTEM A delinquency petition is a court document alleging that a juvenile, between ages 10-16, has violated a law which would be a criminal offense if committed by an adult. Disposition
JUVENILE JUSTICE SYSTEM A delinquency petition is a court document alleging that a juvenile, between ages 10-16, has violated a law which would be a criminal offense if committed by an adult. Disposition
7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ
 7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ 7.1 Victim of a crime What are my rights if I have been the victim of a crime? As a victim of crime, you have the right to report that crime to
7. MY RIGHTS IN DEALING WITH CRIMINAL LAW AND THE GARDAÍ 7.1 Victim of a crime What are my rights if I have been the victim of a crime? As a victim of crime, you have the right to report that crime to
A Better Model: Ensuring Equal Justice for Persons With Mental Illness & Mental Retardation
 A Better Model: Ensuring Equal Justice for Persons With Mental Illness & Mental Retardation The central issue today is the same as it was at the time of Dorothea Dix when insane paupers were warehoused
A Better Model: Ensuring Equal Justice for Persons With Mental Illness & Mental Retardation The central issue today is the same as it was at the time of Dorothea Dix when insane paupers were warehoused
Understanding the Civil Involuntary Commitment Process
 Understanding the Civil Involuntary Commitment Process About the Author By D. Renée Hildebrant http://www.okbar.org/obj/articles_05/021205.htm Oklahoma Bar Journal D. Renée Hildebrant is the trial court
Understanding the Civil Involuntary Commitment Process About the Author By D. Renée Hildebrant http://www.okbar.org/obj/articles_05/021205.htm Oklahoma Bar Journal D. Renée Hildebrant is the trial court
Fairfax-Falls Church Community Services Board
 LOB #267: ADULT RESIDENTIAL TREATMENT SERVICES Purpose Adult Residential Treatment Services provides residential treatment programs for adults with severe substance use disorders and/or co occurring mental
LOB #267: ADULT RESIDENTIAL TREATMENT SERVICES Purpose Adult Residential Treatment Services provides residential treatment programs for adults with severe substance use disorders and/or co occurring mental
MENTAL HEALTH AND SUBSTANCE ABUSE
 MENTAL HEALTH AND SUBSTANCE ABUSE Perhaps no state government function has experienced such a profound change in its mission over the past 40 years than the mental health system. As late as the 1960s,
MENTAL HEALTH AND SUBSTANCE ABUSE Perhaps no state government function has experienced such a profound change in its mission over the past 40 years than the mental health system. As late as the 1960s,
CHILD ABUSE REPORTING PROCEDURES
 CHILD ABUSE REPORTING PROCEDURES REASON FOR INVESTIGATION The Grand Jury received a citizen s complaint concerning the possible mishandling of a Suspected Child Abuse Report (SCAR) by the Nevada County
CHILD ABUSE REPORTING PROCEDURES REASON FOR INVESTIGATION The Grand Jury received a citizen s complaint concerning the possible mishandling of a Suspected Child Abuse Report (SCAR) by the Nevada County
Youth and the Law. Presented by The Crime Prevention Unit
 Youth and the Law Presented by The Crime Prevention Unit Objectives Explaining the juvenile justice system and the differences between it and the adult system. Discussing juveniles rights and responsibilities
Youth and the Law Presented by The Crime Prevention Unit Objectives Explaining the juvenile justice system and the differences between it and the adult system. Discussing juveniles rights and responsibilities
Minnesota County Attorneys Association Policy Positions on Drug Control and Enforcement
 T H E M I N N E S O T A C O U N T Y A T T O R N E Y S A S S O C I A T I O N Minnesota County Attorneys Association Policy Positions on Drug Control and Enforcement Adopted: September 17, 2004 Introduction
T H E M I N N E S O T A C O U N T Y A T T O R N E Y S A S S O C I A T I O N Minnesota County Attorneys Association Policy Positions on Drug Control and Enforcement Adopted: September 17, 2004 Introduction
Title 15 CRIMINAL PROCEDURE -Chapter 23 ALABAMA CRIME VICTIMS Article 3 Crime Victims' Rights
 Section 15-23-60 Definitions. As used in this article, the following words shall have the following meanings: (1) ACCUSED. A person who has been arrested for committing a criminal offense and who is held
Section 15-23-60 Definitions. As used in this article, the following words shall have the following meanings: (1) ACCUSED. A person who has been arrested for committing a criminal offense and who is held
The Legal System in the United States
 The Legal System in the United States At the conclusion of this chapter, students will be able to: 1. Understand how the legal system works; 2. Explain why laws are necessary; 3. Discuss how cases proceed
The Legal System in the United States At the conclusion of this chapter, students will be able to: 1. Understand how the legal system works; 2. Explain why laws are necessary; 3. Discuss how cases proceed
STUDENT STUDY GUIDE CHAPTER NINE
 Multiple Choice Questions STUDENT STUDY GUIDE CHAPTER NINE 1. Which of the following is a type of case that is often heard by lower level courts? a. Breach of contract b. Federal appeals c. Maritime claims
Multiple Choice Questions STUDENT STUDY GUIDE CHAPTER NINE 1. Which of the following is a type of case that is often heard by lower level courts? a. Breach of contract b. Federal appeals c. Maritime claims
BASIC CRIMINAL LAW. Joe Bodiford. Overview of a criminal case Presented by: Board Certified Criminal Trial Lawyer
 BASIC CRIMINAL LAW Overview of a criminal case Presented by: Joe Bodiford Board Certified Criminal Trial Lawyer www.floridacriminaldefense.com www.blawgger.com THE FLORIDA CRIMINAL PROCESS Source: http://www.fsu.edu/~crimdo/cj-flowchart.html
BASIC CRIMINAL LAW Overview of a criminal case Presented by: Joe Bodiford Board Certified Criminal Trial Lawyer www.floridacriminaldefense.com www.blawgger.com THE FLORIDA CRIMINAL PROCESS Source: http://www.fsu.edu/~crimdo/cj-flowchart.html
The Juvenile and Domestic Relations District Court
 The Juvenile and Domestic Relations District Court I. General Information The juvenile and domestic relations district court handles cases involving: Juveniles accused of delinquent acts, traffic infractions
The Juvenile and Domestic Relations District Court I. General Information The juvenile and domestic relations district court handles cases involving: Juveniles accused of delinquent acts, traffic infractions
HOW A TYPICAL CRIMINAL CASE IS PROSECUTED IN ALASKA
 HOW A TYPICAL CRIMINAL CASE IS PROSECUTED IN ALASKA The Office of Victims Rights receives many inquiries from victims about how a criminal case in Alaska is investigated by police and then prosecuted by
HOW A TYPICAL CRIMINAL CASE IS PROSECUTED IN ALASKA The Office of Victims Rights receives many inquiries from victims about how a criminal case in Alaska is investigated by police and then prosecuted by
Your Criminal Justice System
 Your Criminal Justice System Helpful Information for the Victims and Witnesses of Crime Provided by Kansas Attorney General Derek Schmidt Victims Services Division 120 SW 10th Ave, 2nd Floor Topeka, KS
Your Criminal Justice System Helpful Information for the Victims and Witnesses of Crime Provided by Kansas Attorney General Derek Schmidt Victims Services Division 120 SW 10th Ave, 2nd Floor Topeka, KS
General District Courts
 General District Courts To Understand Your Visit to Court You Should Know: It is the courts wish that you know your rights and duties. We want every person who comes here to receive fair treatment in accordance
General District Courts To Understand Your Visit to Court You Should Know: It is the courts wish that you know your rights and duties. We want every person who comes here to receive fair treatment in accordance
A Brief Overview of Promising Jail Diversion Programs in Florida
 EFFECTIVE ALTERNATIVES A Brief Overview of Promising Jail Diversion Programs in Florida By the Florida Substance Abuse and Mental Health Corporation and Florida Partners in Crisis January 2009 EFFECTIVE
EFFECTIVE ALTERNATIVES A Brief Overview of Promising Jail Diversion Programs in Florida By the Florida Substance Abuse and Mental Health Corporation and Florida Partners in Crisis January 2009 EFFECTIVE
Adult Plea Negotiation Guidelines
 From the office of the Rice County Attorney: Adult Plea Negotiation Guidelines Revision June, 2004 1. These guidelines apply to any adult felony defendant case prosecuted by this office, which is not disposed
From the office of the Rice County Attorney: Adult Plea Negotiation Guidelines Revision June, 2004 1. These guidelines apply to any adult felony defendant case prosecuted by this office, which is not disposed
Mental Health Fact Sheet
 Mental Health Fact Sheet Substance Abuse and Treatment Branch (SATB), Community Supervision Services Re-Entry and Sanctions Center (RSC), Office of Community Justice Programs Adult Probationers / Parolees
Mental Health Fact Sheet Substance Abuse and Treatment Branch (SATB), Community Supervision Services Re-Entry and Sanctions Center (RSC), Office of Community Justice Programs Adult Probationers / Parolees
DESCRIPTION OF FORENSIC POPULATION
 SERVICES FOR FORENSIC CLIENTS GENERAL LEGAL RIGHTS CHAPTER 13 DESCRIPTION OF FORENSIC POPULATION The forensic program for the State of Missouri is designed to provide services to all circuit courtordered
SERVICES FOR FORENSIC CLIENTS GENERAL LEGAL RIGHTS CHAPTER 13 DESCRIPTION OF FORENSIC POPULATION The forensic program for the State of Missouri is designed to provide services to all circuit courtordered
Case 3:15-cv-04959 Document 1 Filed 10/28/15 Page 1 of 13
 Case 3:15-cv-04959 Document 1 Filed 10/28/15 Page 1 of 13 Phil Telfeyan California Bar No. 258270 Attorney, Equal Justice Under Law 601 Pennsylvania Avenue NW South Building Suite 900 Washington, D.C.
Case 3:15-cv-04959 Document 1 Filed 10/28/15 Page 1 of 13 Phil Telfeyan California Bar No. 258270 Attorney, Equal Justice Under Law 601 Pennsylvania Avenue NW South Building Suite 900 Washington, D.C.
UNITED STATES DISTRICT COURT DISTRICT OF MINNESOTA CRIMINAL JUSTICE ACT PLAN
 UNITED STATES DISTRICT COURT DISTRICT OF MINNESOTA CRIMINAL JUSTICE ACT PLAN I. AUTHORITY Under the Criminal Justice Act of 1964, as amended, (CJA), 18 U.S.C. 3006A and the Guidelines for Administering
UNITED STATES DISTRICT COURT DISTRICT OF MINNESOTA CRIMINAL JUSTICE ACT PLAN I. AUTHORITY Under the Criminal Justice Act of 1964, as amended, (CJA), 18 U.S.C. 3006A and the Guidelines for Administering
ARREST! What Happens Now?
 Personal Injury Wrongful Death Slip & Fall Automobile Accidents Trucking Accidents Motorcycle Accidents Medical Malpractice Criminal Defense You re Under ARREST! What Happens Now? Do NOT Speak to Police
Personal Injury Wrongful Death Slip & Fall Automobile Accidents Trucking Accidents Motorcycle Accidents Medical Malpractice Criminal Defense You re Under ARREST! What Happens Now? Do NOT Speak to Police
CRIMINAL LAW AND VICTIMS RIGHTS
 Chapter Five CRIMINAL LAW AND VICTIMS RIGHTS In a criminal case, a prosecuting attorney (working for the city, state, or federal government) decides if charges should be brought against the perpetrator.
Chapter Five CRIMINAL LAW AND VICTIMS RIGHTS In a criminal case, a prosecuting attorney (working for the city, state, or federal government) decides if charges should be brought against the perpetrator.
How To Help Mentally Ill Offenders In The Criminal Justice System
 Mentally Ill Offenders in the Criminal Justice System Webinar Panelists: Hon. Michael Finkle King County District Court Judge Seattle, WA Bradley Jacobs Deputy Director, Adult Behavioral Health Services
Mentally Ill Offenders in the Criminal Justice System Webinar Panelists: Hon. Michael Finkle King County District Court Judge Seattle, WA Bradley Jacobs Deputy Director, Adult Behavioral Health Services
CHAPTER 23. BE IT ENACTED by the Senate and General Assembly of the State of New Jersey:
 CHAPTER 23 AN ACT concerning treatment for drug and alcohol dependent persons, amending N.J.S.2C:35-14 and N.J.S.2C:44-6, and supplementing Title 2C of the New Jersey Statutes. BE IT ENACTED by the Senate
CHAPTER 23 AN ACT concerning treatment for drug and alcohol dependent persons, amending N.J.S.2C:35-14 and N.J.S.2C:44-6, and supplementing Title 2C of the New Jersey Statutes. BE IT ENACTED by the Senate
DESCRIPTION OF THE FEDERAL CRIMINAL JUSTICE SYSTEM FOR DEFENDANTS
 DESCRIPTION OF THE FEDERAL CRIMINAL JUSTICE SYSTEM FOR DEFENDANTS DESCRIPTION OF THE FEDERAL CRIMINAL JUSTICE SYSTEM FOR DEFENDANTS This pamphlet has been provided to help you better understand the federal
DESCRIPTION OF THE FEDERAL CRIMINAL JUSTICE SYSTEM FOR DEFENDANTS DESCRIPTION OF THE FEDERAL CRIMINAL JUSTICE SYSTEM FOR DEFENDANTS This pamphlet has been provided to help you better understand the federal
DeKalb County Drug Court: C.L.E.A.N. Program (Choosing Life and Ending Abuse Now)
 DeKalb County Drug Court: C.L.E.A.N. Program (Choosing Life and Ending Abuse Now) MISSION STATEMENT The mission of the DeKalb County Drug Court:.C.L.E.A.N. Program (Choosing Life and Ending Abuse Now)
DeKalb County Drug Court: C.L.E.A.N. Program (Choosing Life and Ending Abuse Now) MISSION STATEMENT The mission of the DeKalb County Drug Court:.C.L.E.A.N. Program (Choosing Life and Ending Abuse Now)
Building A Reformed Criminal Justice System: The Sequential Intercept Model
 Building A Reformed Criminal Justice System: The Sequential Intercept Model Mark Gale Criminal Justice Chair, NAMI Los Angeles County Council markgale510@gmail.com Ratan Bhavnani Board Member, NAMI California
Building A Reformed Criminal Justice System: The Sequential Intercept Model Mark Gale Criminal Justice Chair, NAMI Los Angeles County Council markgale510@gmail.com Ratan Bhavnani Board Member, NAMI California
Issues Contributing to the Overcrowding in the Santa Cruz County Main Jail
 Issues Contributing to the Overcrowding in the Santa Cruz County Main Jail Synopsis Since it opened in 1981, the Santa Cruz main jail has been overcrowded. Potential causes of this overcrowding are reviewed
Issues Contributing to the Overcrowding in the Santa Cruz County Main Jail Synopsis Since it opened in 1981, the Santa Cruz main jail has been overcrowded. Potential causes of this overcrowding are reviewed
UNDERSTANDING THE CRIMINAL JUSTICE SYSTEM Anne Benson
 UNDERSTANDING THE CRIMINAL JUSTICE SYSTEM Anne Benson What is the Criminal Justice System? The criminal justice system is the system we have in the United States for addressing situations where it is believed
UNDERSTANDING THE CRIMINAL JUSTICE SYSTEM Anne Benson What is the Criminal Justice System? The criminal justice system is the system we have in the United States for addressing situations where it is believed
Stearns County, MN Repeat Felony Domestic Violence Court
 Stearns County, MN Repeat Felony Domestic Violence Court Planning and Implementation Best Practice Guide How can a community come together to change its response to domestic violence crimes? Can a court
Stearns County, MN Repeat Felony Domestic Violence Court Planning and Implementation Best Practice Guide How can a community come together to change its response to domestic violence crimes? Can a court
APPEARANCE, PLEA AND WAIVER
 Guide to Municipal Court What Types of Cases Are Heard in Municipal Court? Cases heard in municipal court are divided into four general categories: Violations of motor vehicle and traffic laws Violations
Guide to Municipal Court What Types of Cases Are Heard in Municipal Court? Cases heard in municipal court are divided into four general categories: Violations of motor vehicle and traffic laws Violations
What you don t know can hurt you.
 What you don t know can hurt you. Why you need a defense lawyer if you are charged with a misdemeanor. A misdemeanor conviction is SERIOUS A misdemeanor is not a minor crime. If you are convicted of a
What you don t know can hurt you. Why you need a defense lawyer if you are charged with a misdemeanor. A misdemeanor conviction is SERIOUS A misdemeanor is not a minor crime. If you are convicted of a
New Developments in Supported Employment San Francisco Behavioral Health Court
 New Developments in Supported Employment San Francisco Behavioral Health Court NADCP National Conference May 27, 2014 Lisa Lightman Kathleen Connolly Lacey, LCSW Gregory Jarasitis, MOT, OTR/L Goals of
New Developments in Supported Employment San Francisco Behavioral Health Court NADCP National Conference May 27, 2014 Lisa Lightman Kathleen Connolly Lacey, LCSW Gregory Jarasitis, MOT, OTR/L Goals of
Crime. What is the sequence of events in the criminal justice system? Prosecution and pretrial services Refusal to indict.
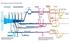 What is the sequence of events in the criminal justice system? Entry into the system Prosecution and pretrial services Refusal to indict Grand jury Charge dismissed Acquitted Sentencing and sanctions Appeal
What is the sequence of events in the criminal justice system? Entry into the system Prosecution and pretrial services Refusal to indict Grand jury Charge dismissed Acquitted Sentencing and sanctions Appeal
SPECIAL OPTIONS SERVICES PROGRAM UNITED STATES PRETRIAL SERVICES AGENCY EASTERN DISTRICT OF NEW YORK
 SPECIAL OPTIONS SERVICES PROGRAM UNITED STATES PRETRIAL SERVICES AGENCY EASTERN DISTRICT OF NEW YORK February 4, 2013 1 I. Introduction The Special Options Services (SOS) Program was established in the
SPECIAL OPTIONS SERVICES PROGRAM UNITED STATES PRETRIAL SERVICES AGENCY EASTERN DISTRICT OF NEW YORK February 4, 2013 1 I. Introduction The Special Options Services (SOS) Program was established in the
Tarrant County College Police Department
 Tarrant County College Police Department VICTIM ASSISTANCE An Assistance Program for Victims and Family Survivors of Violent Crimes Tarrant County College The Tarrant County College District Police Department
Tarrant County College Police Department VICTIM ASSISTANCE An Assistance Program for Victims and Family Survivors of Violent Crimes Tarrant County College The Tarrant County College District Police Department
HANDOUT 1: Purpose and Principles of Sentencing in Canada
 HANDOUT 1: Purpose and Principles of Sentencing in Canada Principles of Sentencing The Criminal Code of Canada outlines the principles and purpose of sentencing in s. 718. These principles are placed in
HANDOUT 1: Purpose and Principles of Sentencing in Canada Principles of Sentencing The Criminal Code of Canada outlines the principles and purpose of sentencing in s. 718. These principles are placed in
Title 34-A: CORRECTIONS
 Title 34-A: CORRECTIONS Chapter 5: PROBATION AND PAROLE Table of Contents Subchapter 1. GENERAL PROVISIONS... 3 Section 5001. DEFINITIONS... 3 Section 5002. PARDONS BY THE GOVERNOR... 4 Section 5003. PROHIBITED
Title 34-A: CORRECTIONS Chapter 5: PROBATION AND PAROLE Table of Contents Subchapter 1. GENERAL PROVISIONS... 3 Section 5001. DEFINITIONS... 3 Section 5002. PARDONS BY THE GOVERNOR... 4 Section 5003. PROHIBITED
COMMUNITY SAFETY VICTIM RESPECT OFFENDER ACCOUNTABILITY
 COMMUNITY SAFETY VICTIM RESPECT OFFENDER ACCOUNTABILITY OUR MISSION The mission of the New Hampshire Department of Corrections is to provide a safe, secure, and humane correctional system through effective
COMMUNITY SAFETY VICTIM RESPECT OFFENDER ACCOUNTABILITY OUR MISSION The mission of the New Hampshire Department of Corrections is to provide a safe, secure, and humane correctional system through effective
The Rights of Crime Victims in Texas
 The Rights of Crime Victims in Texas 1 Housekeeping Please turn off cell phones and pagers or place in a silent mode. Questions can be answered in presentations or during break. 2 Constitutional Rights
The Rights of Crime Victims in Texas 1 Housekeeping Please turn off cell phones and pagers or place in a silent mode. Questions can be answered in presentations or during break. 2 Constitutional Rights
Arizona Constitution: Article II, Section 2.1 Victims Bill of Rights. Arizona Revised Statutes:
 Arizona Laws Arizona Constitution: Article II, Section 2.1 Victims Bill of Rights Arizona Revised Statutes: Title 13, Chapter 40 Crime Victims Rights Title 8, Chapter 3, Article 7 Victims Rights for Juvenile
Arizona Laws Arizona Constitution: Article II, Section 2.1 Victims Bill of Rights Arizona Revised Statutes: Title 13, Chapter 40 Crime Victims Rights Title 8, Chapter 3, Article 7 Victims Rights for Juvenile
A Victim s Guide to Understanding the Criminal Justice System
 A Victim s Guide to Understanding the Criminal Justice System The Bartholomew County Prosecutor s Office Victim Assistance Program Prosecutor: William Nash 234 Washington Street Columbus, IN 47201 Telephone:
A Victim s Guide to Understanding the Criminal Justice System The Bartholomew County Prosecutor s Office Victim Assistance Program Prosecutor: William Nash 234 Washington Street Columbus, IN 47201 Telephone:
The Public Mental Health System in Texas And Its Relation to Criminal Justice
 The Public Mental Health System in Texas And Its Relation to Criminal Justice Criminal Justice Policy Council February 2000 Tony Fabelo, Ph.D. Executive Director The Public Mental Health System in Texas
The Public Mental Health System in Texas And Its Relation to Criminal Justice Criminal Justice Policy Council February 2000 Tony Fabelo, Ph.D. Executive Director The Public Mental Health System in Texas
The Substance Abuse Felony Punishment Program: Evaluation and Recommendations
 The Substance Abuse Felony Punishment Program: Evaluation and Recommendations Criminal Justice Policy Council Prepared for the 77 th Texas Legislature, 2001 Tony Fabelo, Ph.D. Executive Director The Substance
The Substance Abuse Felony Punishment Program: Evaluation and Recommendations Criminal Justice Policy Council Prepared for the 77 th Texas Legislature, 2001 Tony Fabelo, Ph.D. Executive Director The Substance
Removal of Youth in the Adult Criminal Justice System: A State Trends Update. Rebecca Gasca on behalf of Campaign for Youth Justice
 Removal of Youth in the Adult Criminal Justice System: A State Trends Update Rebecca Gasca on behalf of Campaign for Youth Justice Juvenile Court founded in 1899 to create a separate justice system for
Removal of Youth in the Adult Criminal Justice System: A State Trends Update Rebecca Gasca on behalf of Campaign for Youth Justice Juvenile Court founded in 1899 to create a separate justice system for
Restructuring Proposal for the Criminal Division of the Circuit Court of Cook County
 Chicago-Kent College of Law From the SelectedWorks of Daniel T. Coyne 2010 Restructuring Proposal for the Criminal Division of the Circuit Court of Cook County Daniel T. Coyne, Chicago-Kent College of
Chicago-Kent College of Law From the SelectedWorks of Daniel T. Coyne 2010 Restructuring Proposal for the Criminal Division of the Circuit Court of Cook County Daniel T. Coyne, Chicago-Kent College of
