Leflunomide in rheumatoid arthritis: recommendations through a process of consensus
|
|
|
- Helen Pearson
- 8 years ago
- Views:
Transcription
1 Rheumatology 2005;44: Advance Access publication 18 January 2005 Review Leflunomide in rheumatoid arthritis: recommendations through a process of consensus P. Maddison, P. Kiely 1, B. Kirkham 2, T. Lawson 4, R. Moots 5, D. Proudfoot 6, R. Reece 7, D. Scott 3, R. Sword 8, A. Taggart 9, C. Thwaites 10 and E. Williams 11 doi: /rheumatology/keh500 Objectives. To determine, by consensus, the optimal use of in rheumatoid arthritis (RA), using a multidisciplinary panel of experts and performing meta-analyses of available data Methods. A multidisciplinary panel of experts in RA was convened. Important questions, pertinent to the use of in the treatment of RA, were defined by consensus at an initial meeting. Each question was allocated to subgroups of two or three members, who worked separately to prepare a balanced opinion, based on published literature, data from individual patients taking part in phase II and phase III clinical trials provided by Aventis, and data from a USA-based medical claims database (AETNA). The full group then reconvened to agree on an overall consensus statement. Recommendations concerning efficacy and tolerability versus comparator drugs and placebo were derived from two new meta-analyses. Results. Leflunomide was at least as effective as sulphasalazine and methotrexate, and equally well tolerated on meta-analysis of trial data. Overall withdrawal rates for all adverse events were similar for all three drugs. Avoidance of the loading dose reduces nuisance side-effects (e.g. nausea), but probably delays the onset of action. Adverse events could usually be managed by dose reduction and/or symptomatic. Conclusions. On the basis of efficacy, safety and cost, should be considered in patients with RA who have failed first-line DMARD drug. In refractory cases, may be used in combination with, for example, methotrexate before biological agents. Therapy should be initiated by a specialist, but repeat prescribing in general practice on a shared care basis is acceptable using agreed protocols. Clear mechanisms are required to monitor toxicity, with good communication between the patient and rheumatologist to manage nuisance side-effects and avoid unnecessary discontinuation of. KEY WORDS: Leflunomide, Rheumatoid arthritis, DMARDs, Combination, Adverse events. A number of agents have been introduced over recent years fulfilling the Outcomes Measures in Arthritis Clinical Trials (OMERACT) definition of a DMARD [1], retarding the progression of structural joint damage. One such drug is, an isoxazole derivative and inhibitor of de novo pyrimidine synthesis, which has been shown to provide comparable suppression of joint inflammation to methotrexate and sulphasalazine [2], thereby reducing the rate of radiologically detected joint damage and reversing disability. A number of audits on the use of in England, Wales and Northern Ireland [3; Reece R, Taggart A, personal communications] have revealed considerable variation in enthusiasm for the use of, and deviation from manufacturer recommendations on the loading and maintenance doses and drug monitoring. Therefore, to address these issues, a multidisciplinary group was convened in October 2002 to obtain rheumatologist, nurse specialist, general practice and patient views. The objective of the group was to identify important questions, pertinent to the use of in the treatment of inflammatory arthritis, and address them by systematically reviewing the available data and arriving at a consensus to inform best clinical practice. This independently written consensus statement is intended to be of help to health professionals and the general public, but is not intended for use as a practice guideline or a primary source of technical data. Department of Rheumatology, Ysbyty Gwynedd Hospital and University of Wales, Bangor, 1 Department of Rheumatology, St George s Hospital, 2 Department of Rheumatology, Guy s and St Thomas Hospital, 3 Department of Rheumatology, GKT School of Medicine, London, 4 Department of Rheumatology, Princess of Wales Hospital, Bridgend, 5 Department of Rheumatology, University Hospital Aintree, Liverpool, 6 Bognor Regis, West Sussex, 7 Department of Rheumatology, Huddersfield Royal Infirmary, Huddersfield, 8 Department of Rheumatology, Nottingham City Hospital, Nottingham, 9 Department of Rheumatology, Musgrave Park Hospital, Belfast, 10 Rheumatology Department, Haywood Hospital, Burslem, Stoke-on-Trent and 11 Department of Rheumatology, North Cheshire Hospital NHS Trust, Warrington, UK. Submitted 4 October 2004; revised version accepted 29 October Correspondence to: P. Maddison, Department of Rheumatology, Ysbyty Gwynedd Hospital, Bangor LL57 2PW, UK. peter.maddison@ nww-tr.wales.nhs.uk 280 Rheumatology Vol. 44 No. 3 ß British Society for Rheumatology 2005; all rights reserved
2 Leflunomide in RA: consensus recommendations 281 Methods A multidisciplinary panel was convened consisting of eight rheumatologists with experience of using from teaching hospitals and district general hospitals across the UK, a general practitioner (GP) with a special interest in rheumatic diseases, nurse practitioners from two additional rheumatology units and a patient with RA. At an initial meeting, eight questions pertinent to the use of in the management of inflammatory arthritis were defined. 1. How effective is? 2. How well tolerated is in comparison with other DMARDs? 3. Can be used in combination? 4. Who should prescribe? 5. How should be given? 6. How should side-effects be managed? 7. What is the ideal model of care for treatment with? 8. What does the patient need to know? Subgroups of up to three members of the panel were allocated each question to consider by systematically reviewing available data to reach a balanced opinion. New meta-analyses were also performed for questions 1 and 2. The analysis for question 1 pooled data from individual patients enrolled in three Phase III, multicentre, randomized, controlled trials reported in peer review publications [4 10], that compared the clinical efficacy of with placebo and comparator drugs. A total of 1817 patients were included. Baseline demographic data and numbers of patients available for follow-up at 12 and 24 months are given in Table 1. The trials collected swollen joint counts (28 joints), tender joint counts (28 joints), pain scores (on a 100 mm visual analogue scale), patient and physician global responses (on 100 mm visual analogue scales), ESR and CRP levels and Health Assessment Questionnaire (HAQ) scores. These data were used to determine the American College of Rheumatology (ACR) response rates (ACR20 and ACR50). Data from these trials were analysed for all drugs in all studies, for all drugs combined across studies and all cases for both the intention-to-treat and the valid compliant completer method. The safety meta-analysis for question 2 also pooled individual patient data from dose-ranging phase II studies, allowing the safety of the 25 mg daily dose regimen to be evaluated (Supplementary data, Appendix 2). Additional data were obtained from the USA-based healthcare claims database AETNA [11]. This provided useful information on the use of in over 40,000 RA patients versus comparator TABLE 1. Meta-analysis of efficacy versus comparator DMARDs: patient demographics at baseline Variable LEF (n ¼ 807) MTX (n ¼ 669) SSZ (n ¼ 132) PLC (n ¼ 209) Age (yr): mean Patients with disease for <6 months (%) Patients with disease for >24 months (%) Patients completing months treatment Patients enrolled on months extension Patients completing 24 months treatment LEF, ; MTX, methotrexate; SSZ, sulphasalazine; PLC, placebo. DMARDs in a real-life clinical setting, although there were flaws in the methodology (Supplementary data, Appendix 5). The full panel reconvened at a later date to discuss the preliminary reports of the subgroups and to produce a final set of recommendations through consensus based on dialogue, evidence where available and combined clinical experience. Recommendations 1. How effective is? Meta-analysis of published trials on. ACR response rates were better in the group than in the placebo group. At 6 months and 12 months respectively, an ACR20 (20% improvement in ACR criteria) response was seen in 60 and 53% of patients and in 27 and 26% of placebo patients. Similarly, an ACR50 response (50% improvement in ACR criteria) was seen in 29 and 34% of -treated patients and in 11 and 8% of placebotreated patients at the same time points (Supplementary data, Appendix 1). Sulphasalazine (maximum dose 2 g daily), methotrexate (maximum dose 15 mg weekly) and (maximum dose 20 mg daily) were similar in all clinical, imaging and laboratory parameters, apart from a greater lowering of erythrocyte sedimentation rate (ESR) observed with sulphasalazine and methotrexate than. Leflunomide-treated patients showed a significant improvement in disability, with mean HAQ scores decreasing at 12 months by 0.37 [95% confidence interval (CI) 0.33, 0.41] compared with an increase in placebo HAQ scores of 0.06 (95% CI 0.03, 0.16) at 12 months. Comparable results to were observed in patients taking sulphasalazine and methotrexate. The 2-yr extension studies showed that the decrease in mean HAQ scores was maintained in patients taking each of the DMARDs. Analysis of Sharp scores revealed significantly less radiological progression with than placebo ( versus placebo: 6-month study, P ¼ ; 12-month study, P ¼ ) [12]. In a subset of patients initially treated with or methotrexate for 12 months (MN302 protocol), dynamic gadolinium-enhanced magnetic resonance imaging (DEMRI) was compared at baseline and at 16 weeks. Whilst indistinguishable in terms of ACR response criteria, the DEMRI parameters (initial rate of synovial enhancement and maximal signal intensity enhancement) showed significant improvement in -treated patients and a slight deterioration in the methotrexate group at this early time point [13]. Leflunomide therefore satisfies OMERACT criteria for a DMARD, is at least as effective as sulphasalazine and methotrexate and appears to have a faster onset of action with respect to pain and reduction in synovial vascularity. 2. How well tolerated is in comparison to other DMARDs? Study withdrawals and infections. In clinical trials had a tolerability profile intermediate between that of methotrexate and sulphasalazine in terms of all-cause withdrawal rates and infections. AETNA data revealed greater withdrawal rates with in clinical practice (30 50% after 1 yr), with adverse events (especially gastrointestinal tract-related, the main reason for withdrawal). Since most patients studied received 20 mg daily and relatively few were on
3 282 P. Maddison et al. other doses, it was difficult to say whether side-effects were doserelated or idiosyncratic. However, where a dose effect was apparent this is mentioned. The most prevalent adverse events for, methotrexate and sulphasalazine were hypertension, gastrointestinal and dermatological symptoms, occurring in higher frequency in patients on any of these three drugs compared with placebo. Serious adverse events were similar to the comparator DMARDs except severe weight loss and severe dermatological toxicity, which were higher in and an increase in liver function tests (LFTs) greater than three times the upper limit of normal, which was more common with methotrexate. Nausea and diarrhoea. The prevalence of significant nausea (requiring withdrawal of treatment) was less in (1.3%)-treated patients than seen with methotrexate (2.4%) or sulphasalazine (5.3%). Diarrhoea was more prevalent than significant nausea for all three drugs, and the withdrawal rate was higher in (1.9%)-treated patients than in those on methotrexate (1.5%) or sulphasalazine (0.75%). Daily doses of 20 mg were associated with more nausea and diarrhoea than the 10 mg/day dose. The rates of diarrhoea requiring withdrawal in patients receiving loading doses of 100 or 50 mg/day were identical (2.1%) and higher than with lower doses. Hepatoxicity. The cumulative incidence of hepatic enzyme concentration elevation three times the upper limit of normal was highest with methotrexate (17%), followed by (5%), sulphasalazine (4%) and placebo (1%). This was also the case in the AETNA database; where hepatic adverse events (severe and non-severe) were lower in the group than the methotrexate and other DMARD groups. Dermatological. The prevalence of all dermatological adverse events was comparable for (28%), methotrexate (32%) and sulphasalazine (35%), but was associated with a higher incidence of serious dermatological adverse events (this higher rate was only evident with the use of the 25 mg daily dose and apparent from 3 months within the clinical trial data reviewed). The AETNA database was insufficient for comparable analysis. Hypertension. Withdrawals due to hypertension occurred rarely in the placebo-treated group (0.93%) and the (0.77%) and sulphasalazine (0.75%) groups, but these were a little higher than methotrexate (0.28%). In contrast, the AETNA data showed less hypertension in the group than all other DMARDs. The use of 100 mg/day as a loading dose for 3 days was associated with hypertension in 3.4% of 1322 study participants, but in only 1.2% of patients who received a loading dose of 50 mg/day. Confounding factors, such as NSAID use, could not be determined from this meta-analysis. Other adverse events. Neither the meta-analysis nor the AETNA database provided data to suggest that was associated with significant haematological toxicity, including cytopenias or solid or haematological malignancies. Serious adverse events therefore do not seem to be increased with compared with methotrexate or other DMARDs and anecdotal evidence that dermatological adverse events and hypertension are more common with than other DMARDs was not supported. 3. Can be used in combination? NSAIDs. Although the active metabolite of, A771726, inhibits cytochrome P450 2C9, which metabolizes many NSAIDs, published clinical trial data suggests that NSAIDs can be used effectively with [14]. There are no published data considering COX-2-specific NSAIDs and. DMARDs Methotrexate. Pharmacokinetic data have revealed no clinically significant interaction between methotrexate and [15]. A 24-week randomized, double-blind trial [16] reported that the addition of to the treatment of patients with persistently active RA on stable methotrexate resulted in a significantly better outcome than when placebo was added to the methotrexate, with acceptable toxicity (including manageable rises in transaminases). The AETNA database corroborated these findings, further supporting the efficacy and safety of and methotrexate combination. However, it is highly recommended that all patients receiving methotrexate plus are monitored closely for LFTs. Sulphasalazine. In a 12-month trial (the RELIEF study) a favourable but not significant benefit of combining and sulphasalazine vs sulphasalazine alone was reported, with between-treatment similarity in terms of safety [17]. Infliximab. To date, there are no randomized, controlled trials to assess the feasibility of a /infliximab combination. However, data from two prospective [18, 19] and two retrospective cohort studies [20, 21] have been reported. These showed that plus infliximab was an effective combination in patients failing on or intolerant to methotrexate, or those having an inadequate response to mono. However, until further evidence is available, caution is advised concerning dosing and adverse events. Adalimumab. In the Safety Trial of Adalimumab in Rheumatoid Arthritis (STAR) study [22], adalimumab or placebo injections were given to RA patients receiving DMARD polypharmacy, of whom 13.4% received alone or as combination. No relationship between adverse events and a specific DMARD was found. 4. Who should prescribe? The current Summary of Product Characteristics for (March 2001) states that only specialists experienced in the treatment of rheumatic diseases should prescribe it. The European Medicines Evaluation Agency (EMEA) [23] statement (12 March 2001), which addressed hepatic adverse events, reiterated this advice. Therefore, the initiation of in primary care is precluded in all but exceptional cases where the prescribing physician has the relevant training and experience. Repeat prescribing of on a shared care basis is acceptable under the guidance of mutually agreed protocols (Table 2). 5. How should be given? Loading dose. The use of a loading dose of 100 mg daily for 3 days results in steady-state plasma levels within 3 5 days. Omitting the loading dose delays steady-state plasma levels on a daily dose of 20 mg to approximately 2 months. It will take at least 6 months to reach therapeutic drug levels with 10 mg daily without a loading dose and sometimes a therapeutic level is not achieved. Loading doses are associated with a higher incidence of nuisance side-effects, particularly nausea and diarrhoea [3], increased discontinuation [24], and higher chance of adverse events [25]. It is now common UK (but not EU) practice to omit the loading dose (Aventis, personal communication). Whilst further research is required to determine the association between loading dose and adverse events, it may be sensible to omit the loading dose in frail or adverse event-prone patients, reserving it for patients where a rapid clinical effect is required.
4 Leflunomide in RA: consensus recommendations 283 TABLE 2. Shared care recommendations Recommendations for a shared care protocol Essential elements The provision of clearly written guidelines outlining the responsibilities of the hospital specialist and the primary care physician undertaking the shared care The availability of the necessary contact details to enable the primary care physician to gain ready access to the local on-call rheumatology service The transfer of details of the laboratory investigations undertaken by the primary care physician to the hospital specialist at each clinic visit The provision of drug information for patients outlining the benefits and risks of treatment, and the need to adhere to safety monitoring recommendations The provision for the monitoring of treatment by the hospital specialist in situations where the primary care physician is unable or unwilling to undertake shared care Responsibilities of the GP Monitoring the patient s overall health status and well-being Prescribing DMARDs and monitoring coprescribing of other drugs Ensuring safety monitoring is conducted according to the shared care protocol Adverse event monitoring and being aware of the risks involved in using each DMARD Managing minor and major adverse events Responsibilities of the hospital specialist Initiating DMARDs and monitoring patient response to treatment Evaluating the results of the community and hospital drug safety monitoring Managing minor and major adverse events Informing the primary care physician of any proposed changes to treatment Providing ready access to the primary care physician for specialist advice on the treatment Recommendations for some -related care management issues Care issue Nuisance symptoms Routine blood pressure and blood monitoring Non-compliance with monitoring Recommendation Establish a clear line of communication between the patient and the department (e.g. help-lines, , routine telephone call from the department after 1 and 2 weeks treatment) to ensure prompt action (e.g. reassurance, symptomatic treatment, dose reduction) thereby potentially facilitating treatment adherence The GP must ensure he/she takes responsibility for this to ensure blood pressure and routine blood monitoring takes place according to the agreed protocol There should be a means of identifying patients who have not complied with monitoring requirements and a strategy for repeat prescription cessation There should be an agreed clear line of communication between the department and GP regarding the interpretation of monitoring data. This may be facilitated by the production of guidelines. Efficacy should be monitored at regular intervals ideally 6-weekly until disease control is achieved. Responsibility for action taken (e.g. dose modification, discontinuation, washout, symptomatic treatment) usually lies with the consultant and must be clearly defined Daily maintenance dose. The consensus of the group is that the recommended daily dose, based on trying to achieve a balance between therapeutic benefit and the risk of side-effects, is 20 mg. This is supported by a head-to-head study [26] showing that 20 mg daily was more effective than 10 mg without compromising tolerability. However, in patients receiving other potentially hepatotoxic drugs (e.g. methotrexate) or who are renally impaired, 10 mg is recommended, although the dose can be cautiously increased to 20 mg daily if necessary. Use of in special situations. Recommendations for the use of in special populations, (such as children, the elderly, pregnancy, and hepatic dysfunction) are presented in the Supplementary data (Appendix 3). What monitoring is required? Recommendations regarding monitoring for adverse events in -treated patients are given in Appendix 3 of the Supplementary data. Since there are no data to suggest an increase in blood dyscrasias attributable to, recommendations for full blood count (FBC) monitoring are less stringent than those suggested in the Summary of Product Characteristics. 6. How should side-effects be managed? Published reports in general provide minimal detail regarding how adverse events are managed [2 8, 15, 16, 27, 28], though they indicate that most appear to be self-limiting [6 8] and in long-term studies lead to discontinuation in a minority of cases [6, 7, 16]. Detailed recommendations of how to manage adverse events are given in the Supplementary data (Appendix 4). Many adverse events can be managed simply by reducing the drug dose or by concomitant administration of symptomatic. Patients may have preferences about this and these should be incorporated in the decision-making process. A dose reduction from 20 to 10 mg is unlikely to produce a rapid diminution of adverse events, as the half life is 2 weeks. If a rapid response is required, a partial washout with cholestyramine (8 g three times daily for 1 3 days) will quickly reduce plasma levels, lead to prompt diminution of the adverse event, and allow the 10 mg dose to commence without delay. If drug dose reduction has controlled a specific adverse event, it may be possible to reintroduce the drug at the original dose if required.
5 284 P. Maddison et al. Decision to start Detailed discussion of benefits and risks/written information Start Inform GP Monitor toxicity Monitor efficacy Fixed interval blood pressure and blood test monitoring Nuisance symptoms Review data and detect non-adherence ACTION: Dose change/discontinuation/washout/ symptomatic treatment FIG. 1. Proposed model of care for treatment. 7. What is the ideal model of care for treatment with? Figure 1 illustrates a proposed model of care for. The decision to initiate treatment is usually made by a rheumatologist, although a suitably trained nurse practitioner working alongside a rheumatologist could also do so. A detailed discussion covering benefits and risks, the time to onset of action, nuisance symptoms and strategies to reduce other adverse events (e.g. low alcohol intake) may lessen the chance of premature discontinuation. A nurse practitioner may be best at providing this information, especially if he/she is subsequently the contact between the patient and department at times of crisis. This preliminary consultation may require considerable time, and written information is advocated. The responsibility for issuing repeat prescriptions should be clearly defined and shared care guidelines followed (Table 2). 8. What does the patient need to know? Educating patients about disease and therapies has been shown to facilitate long-term compliance with drug regimes [29, 30]. The degree of discussion and provision of information to patients may vary enormously and are dictated by many factors, such as the patient s desire to be involved in their treatment. A good rapport will help successful management of adverse events with. This may include allowing the patient a choice of symptomatic treatment, partial washout or dose reduction. The use of written information to reinforce verbally communicated advice is strongly advocated [31 33]. Overall conclusions What is the position of as DMARD for RA? Both the existing literature and two new meta-analyses presented here show clearly that has comparable efficacy and tolerability to methotrexate and sulphasalazine in RA. There still remains a place for other DMARDs in RA management and optimal care should be tailored to the individual patient s requirements. This group concluded by consensus that methotrexate should remain the first-line DMARD for RA because it is effective, has a low incidence of serious side-effects and is of relatively low cost [34]. For patients who fail to respond to methotrexate or who suffer intolerable adverse events [35], the available evidence suggests that sulphasalazine or may be suitable as mono [2, 36]. The meta-analyses above suggest no significant differences between these drugs with respect to efficacy or adverse effects and therefore the choice
6 Leflunomide in RA: consensus recommendations 285 RA First-line Methotrexate Intolerable AEs Ineffective Second-line Change in mono to sulfasalazine or Combination : add sulfasalazine or Treatment failure or intolerable AEs Third-line Biological FIG. 2. Proposed RA treatment pathway. of drug may depend upon factors such as sulphonamide allergy, serious co-existing hypertension or cost. Alternatively, sulphasalazine or may be successfully added to methotrexate in cases of failure of efficacy of mono with this drug [15, 37] (Fig. 2). Finally, there is as yet no firm evidence base to best inform how to place with biological in RA. There is evidence that is more cost-effective for the average RA patient who has failed methotrexate than combination with biologicals, although head-tohead trial data are not yet available [38, 39]. Some units, therefore, require failure of as well as methotrexate before starting biologicals; others treat biological failures with. Perhaps most importantly, there are many patients who cannot take biological because of chronic infection. Therapy with would allow these patients access to an effective DMARD without the risk of severe infection. Rheumatology Key messages Leflunomide has proven efficacy and safety in rheumatoid arthritis, comparable to methotrexate and sulphasalazine, offering another DMARD option. Leflunomide can be used in combination with, for example, methotrexate. Good communication between health professionals and patients, monitoring, flexibility of dosing and varying strategies to manage adverse events are key to maintaining long-term treatment adherence Acknowledgements The authors would like to thank Aventis UK for the use of their clinical data, which was necessary for the preparation of this manuscript, and The Medicus Group for their editorial support. P.M. has received research funding from Abbott, Merck, Sharp and Dohme and Wyeth and in the past acted as Medical Adviser to Aventis and Merck, Sharp and Dohme. P.K. has received departmental support for clinical rheumatology services and research from Abbott, Aventis, Schering Plough, Shire and Wyeth Pharmaceuticals. B.K. has received research funding from Abbott, Centocor, Schering Plough and Roche, and has acted as medical adviser to Abbott and Aventis. Robert Moots has received research funding from Abbott, Aventis, Merck, Sharp and Dohme, Novartis, Shire and Wyeth. He has acted as Medical Adviser to Astra-Zeneca, Aventis, Fujisawa, Merck, Sharp and Dohme, and Shire. Since 1997, R.R. has received honoraria to speak for Aventis on an international basis. D.S. has received research funding from Abbott, Aventis, Schering Plough and Wyeth. R.S. has been sponsored by Aventis to undertake a further training programme in pharmaceutical medicines (Dip Pharm Med, University of Cardiff). A.T. has acted as a Medical Adviser to Abbott Laboratories and to Merck, Sharp and Dohme Ltd. The other authors have declared no conflicts of interest. Supplementary data Supplementary data are available at Rheumatology Online.
7 286 P. Maddison et al. References 1. OMERACT IV. Outcome measures in rheumatology: Cancun, Mexico, April 16 20, J Rheumatol 1999;26: Osiri M, Shea B, Robinson V et al. Leflunomide for the treatment of rheumatoid arthritis: a systematic review and metaanalysis. J Rheumatol 2003;30: Sinha A, Amos N, Lawson TM. Leflunomide the Welsh experience. Rheumatology 2002;42: Strand V, Cohen S, Schiff M et al. Treatment of active rheumatoid arthritis with compared with placebo and methotrexate. Leflunomide Rheumatoid Arthritis Investigators Group. Arch Int Med 1999;159: Smolen JS, Kalden JR, Scott DL et al. Efficacy and safety of compared with placebo and sulfasalazine in active rheumatoid arthritis: a double blind, randomised, multicentre trial. European Leflunomide Study Group. Lancet 1999;353: Emery P, Breedfeld C, Lemmel EM et al, and the multinational study group. A comparison of the efficacy and safety of and methotrexate for the treatment of rheumatoid arthritis. Rheumatology 2000;39: Cohen S, Cannon GW, Schiff M et al. Two-year blinded randomized controlled treatment of active rheumatoid arthritis with compared with methotrexate. Utilization of Leflunomide in the Treatment of Rheumatoid Arthritis Trial Investigator Group. Arthritis Rheum 2001;44: Scott DL, Smolen JS, Kalden JR et al. Treatment of active rheumatoid arthritis with : two year follow up of a double blind, placebo controlled trial versus sulfasalazine. Ann Rheum Dis 2001;60: Kalden JR, Schattenkirchner M, Sorensen H et al. The efficacy and safety of in patients with active rheumatoid arthritis: a five-year follow up study. Arthritis Rheum 2003;48: Scott DL, Strand V. The effects of disease-modifying anti-rheumatic drugs on the Health Assessment Questionnaire score. Lessons from the clinical trials database. Rheumatology 2002;41: Emery P, Cannon G, Holden W, Smolen J, Strand V, Schiff M. Results from a cohort of over 40,000 rheumatoid arthritis (RA patients: Adverse event (AE) profiles of (LEF), methotrexate (MTX) and other disease-modifying antirheumatic drugs (DMARDs). Ann Rheum Dis 2002;61(Suppl. 1): Sharp JT, Strand V, Leung H, Hurley F, Loew-Friedrich I. Treatment with slows radiographic progression of rheumatoid arthritis. Leflunomide Rheumatoid Arthritis Investigators Group. Arthritis Rheum 2000;43: Reece RJ, Kraan MC, Radjenovic A et al. Comparative assessment of and methotrexate for the treatment of rheumatoid arthritis, by dynamic enhanced magnetic resonance imaging. Arthritis Rheum 2002;46: Cohen SB, Iqbal I. Leflunomide. Int J Clin Pract 2003;57: Weinblatt ME, Kremer JM, Coblyn JS et al. Pharmacokinetics, safety, and efficacy of combination treatment with methotrexate and in patients with active rheumatoid arthritis. Arthritis Rheum 1999;42: Kremer JM, Genovese MC, Cannon GW et al. Concomitant in patients with active rheumatoid arthritis despite stable doses of methotrexate. A randomized, double-blind, placebocontrolled trial. Ann Intern Med 2002;137: Dougados M, Emery P, Lemmel EM et al. Maintenance rate of in patients with rheumatoid arthritis: RELIEF 1-year data. Arthritis Rheum 2001;44:S Kiely PD, Johnson DM. Infliximab and combination in rheumatoid arthritis: an open-label study. Rheumatology 2002;41: Strupler CI, Thies W, Schattenkirchner M, Kellner H. Safety and efficacy of and infliximab in rheumatoid arthritis (RA) patients. Ann Rheum Dis 2002;61(Suppl.): Hansen KE, Cush J, Singhal A et al. The safety and efficacy of in combination with infliximab in rheumatoid arthritis. Arthritis Rheum 2001;44(Suppl.): Patel S, Bergen W, Kraemer A, Keena GF, Florence SC, Malvern PA. Efficacy and safety of Remicade (infliximab) plus Arava () in rheumatoid arthritis. Arthritis Rheum 2001; 44(Suppl.): Furst DE, Schiff M, Fleischmann R et al. Safety and efficacy of adalimumab (D2E7), a fully human anti-tnf- monoclonal antibody, given in combination with standard antirheumatic : Safety trial of adalimumab in rheumatoid arthritis (STAR). Arthritis Rheum 2002;46(Suppl.): The European Agency for the Evaluation of Medicinal Products. Post-authorisation evaluation of medicines for human use. EMEA public statement on (Arava) severe and serious hepatic reactions. Document reference EMEA/H/5611/01/en. London, 12 March Chokkalingam S, Shepherd R, Cunningham F, Eisen S. Leflunomide use in the first 33 months after FDA approval: Experience in a national cohort of 3325 patients. Arthritis Rheum 2002;46(Suppl.): S Erra A, Tomas C, Barcelo P, Vilardell M, Marsal S. Is the recommended dose of the best regimen to treat rheumatoid arthritis patients? Rheumatology 2003;42: Poor G, Strand V. Efficacy and safety of 10 mg versus 20mg once daily in patients with active rheumatoid arthritis: multinational double-blind, randomised trial. Rheumatology 2004;43: Rozman B. Clinical experience with in RA. J Rheumatol 1998;25(Suppl. 53): Mladenovic V, Domljan Z, Rozman B et al. Safety and effectiveness of in the treatment of patients with active rheumatoid arthritis. Results of a randomized, placebo-controlled, phase II study. Arthritis Rheum 1995;38: Fraenkel L, Bogardus S, Concato J, Felson D. Preference for disclosure of information among patients with rheumatoid arthritis. Arthritis Care Res 2001;45: Ryan S, ed. Drug in rheumatology nursing. London: Whurr, Ley P. Communicating with the patient. London: Croom Helm, Vignos PJ, Parker WT, Thompson HM. Evaluation of a clinic education program for patients with rheumatoid arthritis. J Rheumatol 1976;3: Anderson JL, Dodman S, Copelman M, Fleming A. Patient information recall in a rheumatology clinic. Rheumatol Rehabil 1979;18: Maetzel A, Strand V, Tugwell P, Wells G, Bombardier C. Economic comparison of and methotrexate in patients with rheumatoid arthritis: an evaluation based on a 1-year randomised controlled trial. Pharmacoeconomics 2002;20: Kremer JM. Methotrexate and emerging therapies. Rheum Dis Clin North Am 1998;24: van der Heijde DM, van Riel PL, Nuver-Zwart IH, Gribnau FW, vad de Putte LB. Effects of hydroxychloroquine and sulfasalazine on progression of joint damage in rheumatoid arthritis. Lancet 1989;1: Dougados M, Combe B, Cantagrel A et al. Combination in early rheumatoid arthritis: a randomised, controlled, double blind 52 week clinical trial of sulfasalazine and methotrexate compared with the single components. Ann Rheum Dis 1999;58: Yazdani C, McLaughlin T, Cummins G, Doyle J. Comparison of rheumatoid arthritis care costs in patients starting with versus etanercept. Am J Manag Care 2001;7(13 Suppl.): S Rubio-Terres C, Dominguez-Gil A. Cost-minimization analysis of the treatment of rheumatoid arthritis with in comparison with the combination of infliximab and methotrexate. Value Health 2001;4:70 8.
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC)
 BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
Rheumatoid Arthritis. Outline. Treatment Goal 4/10/2013. Clinical evaluation New treatment options Future research Discussion
 Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
New Evidence reports on presentations given at EULAR 2012. Rituximab for the Treatment of Rheumatoid Arthritis
 New Evidence reports on presentations given at EULAR 2012 Rituximab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Long-term safety of rituximab: 10-year follow-up in the
New Evidence reports on presentations given at EULAR 2012 Rituximab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Long-term safety of rituximab: 10-year follow-up in the
EMEA PUBLIC STATEMENT ON LEFLUNOMIDE (ARAVA) - SEVERE AND SERIOUS HEPATIC REACTIONS -
 The European Agency for the Evaluation of Medicinal Products Post-authorisation evaluation of medicines for human use London, 12 March 2001 Doc. Ref: EMEA/H/5611/01/en EMEA PUBLIC STATEMENT ON LEFLUNOMIDE
The European Agency for the Evaluation of Medicinal Products Post-authorisation evaluation of medicines for human use London, 12 March 2001 Doc. Ref: EMEA/H/5611/01/en EMEA PUBLIC STATEMENT ON LEFLUNOMIDE
påçííáëü=jéçáåáåéë=`çåëçêíáìã==
 påçííáëü=jéçáåáåéë=`çåëçêíáìã== adalimumab 40mg pre-filled syringe for subcutaneous injection (Humira ) No. (218/05) Abbott New indication: treatment of active and progressive psoriatic arthritis in adults
påçííáëü=jéçáåáåéë=`çåëçêíáìã== adalimumab 40mg pre-filled syringe for subcutaneous injection (Humira ) No. (218/05) Abbott New indication: treatment of active and progressive psoriatic arthritis in adults
Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy
 Media Release Basel, 6 June 2012 Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy Roche (SIX: RO, ROG; OTCQX: RHHBY) today announced
Media Release Basel, 6 June 2012 Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy Roche (SIX: RO, ROG; OTCQX: RHHBY) today announced
Shared care protocol for the management of patients with Rheumatoid Arthritis treated with disease modifying antirheumatic drugs (DMARDs)
 Tameside Hospital NHS Foundation Trust and NHS Tameside and Glossop Shared care protocol for the management of patients with Rheumatoid Arthritis treated with disease modifying antirheumatic drugs (DMARDs)
Tameside Hospital NHS Foundation Trust and NHS Tameside and Glossop Shared care protocol for the management of patients with Rheumatoid Arthritis treated with disease modifying antirheumatic drugs (DMARDs)
Immune modulation in rheumatology. Geoff McColl University of Melbourne/Australian Rheumatology Association
 Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Leflunomide Use During the First 33 Months After Food and Drug Administration Approval: Experience With a National Cohort of 3,325 Patients
 Arthritis & Rheumatism (Arthritis Care & Research) Vol. 49, No. 6, December 15, 2003, pp 745 751 DOI 10.1002/art.11452 2003, American College of Rheumatology ORIGINAL ARTICLE Leflunomide Use During the
Arthritis & Rheumatism (Arthritis Care & Research) Vol. 49, No. 6, December 15, 2003, pp 745 751 DOI 10.1002/art.11452 2003, American College of Rheumatology ORIGINAL ARTICLE Leflunomide Use During the
Etanercept (Enbrel ) in Patients with Rheumatoid Arthritis with Recent Onset Versus Established Disease: Improvement in Disability
 Etanercept (Enbrel ) in Patients with Rheumatoid Arthritis with Recent Onset Versus Established Disease: Improvement in Disability SCOTT W. BAUMGARTNER, ROY M. FLEISCHMANN, LARRY W. MORELAND, MICHAEL H.
Etanercept (Enbrel ) in Patients with Rheumatoid Arthritis with Recent Onset Versus Established Disease: Improvement in Disability SCOTT W. BAUMGARTNER, ROY M. FLEISCHMANN, LARRY W. MORELAND, MICHAEL H.
Chapter 1. Scope and objectives of the thesis
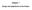 Chapter 1 Scope and objectives of the thesis Chapter 1 Observational studies: focus on leflunomide The view that randomized controlled trials are the gold standard for evaluation and that observational
Chapter 1 Scope and objectives of the thesis Chapter 1 Observational studies: focus on leflunomide The view that randomized controlled trials are the gold standard for evaluation and that observational
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists
 Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Morgan Schultz 1, Stephanie Keeling 2, Steven Katz 2, Walter Maksymowych 2, Dean Eurich 3, Jill Hall 1 1
 Morgan Schultz 1, Stephanie Keeling 2, Steven Katz 2, Walter Maksymowych 2, Dean Eurich 3, Jill Hall 1 1 Faculty of Pharmacy and Pharmaceutical Sciences, 2 Faciluty of Medicine and Dentistry, 3 School
Morgan Schultz 1, Stephanie Keeling 2, Steven Katz 2, Walter Maksymowych 2, Dean Eurich 3, Jill Hall 1 1 Faculty of Pharmacy and Pharmaceutical Sciences, 2 Faciluty of Medicine and Dentistry, 3 School
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden
 Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden Collaborators: Primary investigators Dr Lars Erik Kristensen,
Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden Collaborators: Primary investigators Dr Lars Erik Kristensen,
ABOUT RHEUMATOID ARTHRITIS
 MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
MEDIA BACKGROUNDER ABOUT RHEUMATOID ARTHRITIS Rheumatoid arthritis (RA) is a type of arthritis (chronic inflammatory polyarthritis) that typically affects hands and feet, although any joint in the body
LEFLUNOMIDE (Adults)
 Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Patient Input Information Clinical Trials Outcomes Common Drug Review
 CDEC FINAL RECOMMENDATION USTEKINUMAB (Stelara Janssen Inc.) Indication: Psoriatic Arthritis Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that ustekinumab not be listed at the submitted
CDEC FINAL RECOMMENDATION USTEKINUMAB (Stelara Janssen Inc.) Indication: Psoriatic Arthritis Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that ustekinumab not be listed at the submitted
Rheumatoid Arthritis monitoring of DMARDs
 www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
In the last decade, there have been major changes in the
 233 Promising New Treatments for Rheumatoid Arthritis The Kinase Inhibitors Yusuf Yazici, M.D., and Alexandra L. Regens, B.A. Abstract Three major advances over the last decade have impacted the way we
233 Promising New Treatments for Rheumatoid Arthritis The Kinase Inhibitors Yusuf Yazici, M.D., and Alexandra L. Regens, B.A. Abstract Three major advances over the last decade have impacted the way we
Etanercept, infliximab and adalimumab for the treatment of psoriatic arthritis
 Etanercept, infliximab and adalimumab for the treatment of Issued: August 2010 guidance.nice.org.uk/ta199 NICE has accredited the process used by the Centre for Health Technology Evaluation at NICE to
Etanercept, infliximab and adalimumab for the treatment of Issued: August 2010 guidance.nice.org.uk/ta199 NICE has accredited the process used by the Centre for Health Technology Evaluation at NICE to
Dr Sarah Levy Consultant Rheumatology Croydon University Hospital
 Dr Sarah Levy Consultant Rheumatology Croydon University Hospital Contents Definition/ epidemiology Diagnosis Importance of early diagnosis/ treatment Guidelines Evidence based treatment protocol Current
Dr Sarah Levy Consultant Rheumatology Croydon University Hospital Contents Definition/ epidemiology Diagnosis Importance of early diagnosis/ treatment Guidelines Evidence based treatment protocol Current
Evidence-based Management of Rheumatoid Arthritis (2009)
 CPLD reviews its distance learning programmes every twelve months to ensure currency. This update has been produced by an expert and should be read in conjunction with the Evidencebased Management of distance
CPLD reviews its distance learning programmes every twelve months to ensure currency. This update has been produced by an expert and should be read in conjunction with the Evidencebased Management of distance
Medication Policy Manual. Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012
 Medication Policy Manual Policy No: dru283 Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012 Committee Approval Date: December 12, 2014 Next Review Date: December 2015 Effective Date: January
Medication Policy Manual Policy No: dru283 Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012 Committee Approval Date: December 12, 2014 Next Review Date: December 2015 Effective Date: January
SYNOPSIS. 2-Year (0.5 DB + 1.5 OL) Addendum to Clinical Study Report
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier (For National Authority Use
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier (For National Authority Use
Methotrexate Is Not Disease Modifying In Psoriatic Arthritis
 Methotrexate Is Not Disease Modifying In Psoriatic Arthritis A New Treatment Paradigm Is Required Gabrielle H Kingsley*, Jonathan Packham, Neil McHugh, Diarmuid Mulherin George Kitas, Kuntal Chakravarty,
Methotrexate Is Not Disease Modifying In Psoriatic Arthritis A New Treatment Paradigm Is Required Gabrielle H Kingsley*, Jonathan Packham, Neil McHugh, Diarmuid Mulherin George Kitas, Kuntal Chakravarty,
CANADIAN RHEUMATOLOGY ASSOCIATION POSITION ON THE USE OF BIOLOGIC AGENTS FOR THE TREATMENT OF RHEUMATOID ARTHRITIS
 CANADIAN RHEUMATOLOGY ASSOCIATION POSITION ON THE USE OF BIOLOGIC AGENTS FOR THE TREATMENT OF RHEUMATOID ARTHRITIS Boulos Haraoui, MD for the CRA sub-committee on biologic agents. INTRODUCTION Rheumatoid
CANADIAN RHEUMATOLOGY ASSOCIATION POSITION ON THE USE OF BIOLOGIC AGENTS FOR THE TREATMENT OF RHEUMATOID ARTHRITIS Boulos Haraoui, MD for the CRA sub-committee on biologic agents. INTRODUCTION Rheumatoid
A Survey of Barriers to Treatment Access in Rheumatoid Arthritis. Country Annex Report: UK
 A Survey of Barriers to Treatment Access in Rheumatoid Arthritis Country Annex Report: UK October 2009 1 Interviews In the UK, five rheumatologists and one patient representative were interviewed. The
A Survey of Barriers to Treatment Access in Rheumatoid Arthritis Country Annex Report: UK October 2009 1 Interviews In the UK, five rheumatologists and one patient representative were interviewed. The
Improvement in Quality of Life of Rheumatoid Arthritis Patients on Biologic Therapy
 Improvement in Quality of Life of Rheumatoid Arthritis Patients on Biologic Therapy R Adams 1, Ct Ng 2, A Gibbs 2, L Tilson 1, D Veale 2, B Bresnihan 2, O FitzGerald 2, M Barry 1 1. National Centre for
Improvement in Quality of Life of Rheumatoid Arthritis Patients on Biologic Therapy R Adams 1, Ct Ng 2, A Gibbs 2, L Tilson 1, D Veale 2, B Bresnihan 2, O FitzGerald 2, M Barry 1 1. National Centre for
Speaking Plainly. Biologic treatment options for rheumatoid arthritis
 in association with Plain English Campaign Speaking Plainly Biologic treatment options for rheumatoid arthritis A guide to help healthcare professionals talking to patients with rheumatoid arthritis Foreword
in association with Plain English Campaign Speaking Plainly Biologic treatment options for rheumatoid arthritis A guide to help healthcare professionals talking to patients with rheumatoid arthritis Foreword
Rituximab for the treatment of rheumatoid arthritis
 DOI: 10.3310/hta13suppl2/04 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Rituximab for the treatment of rheumatoid arthritis A Bagust, A Boland, J Hockenhull, N Fleeman, J Greenhalgh, Y Dundar,
DOI: 10.3310/hta13suppl2/04 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Rituximab for the treatment of rheumatoid arthritis A Bagust, A Boland, J Hockenhull, N Fleeman, J Greenhalgh, Y Dundar,
Rheumatoid Arthritis:
 Rheumatoid Arthritis Update 2014 Mark Hulsey, MD FACR Rheumatoid Arthritis Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial
Rheumatoid Arthritis Update 2014 Mark Hulsey, MD FACR Rheumatoid Arthritis Key Features Symptoms >6 weeks duration Often lasts the remainder of the patient s life Inflammatory synovitis Palpable synovial
Benefit/risk of leflunomide in rheumatoid arthritis
 Benefit/risk of leflunomide in rheumatoid arthritis J.M. Kremer, G.W. Cannon Joel M. Kremer, MD, Director of Research, The Center for Rheumatology, Clinical Professor of Medicine, Albany Medical College,
Benefit/risk of leflunomide in rheumatoid arthritis J.M. Kremer, G.W. Cannon Joel M. Kremer, MD, Director of Research, The Center for Rheumatology, Clinical Professor of Medicine, Albany Medical College,
DAS28 criteria for initiation of biologics in early RA: a clinician s view. Dr Patrick Kiely St George s Healthcare NHS Trust, London
 DAS28 criteria for initiation of biologics in early RA: a clinician s view Dr Patrick Kiely St George s Healthcare NHS Trust, London History: NICE (E&W) guidelines for starting anti-tnf agents April 2001
DAS28 criteria for initiation of biologics in early RA: a clinician s view Dr Patrick Kiely St George s Healthcare NHS Trust, London History: NICE (E&W) guidelines for starting anti-tnf agents April 2001
Maintenance of abstinence in alcohol dependence
 Shared Care Guideline for Prescription and monitoring of Acamprosate Calcium Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist, Alcohol Services Dr Donnelly
Shared Care Guideline for Prescription and monitoring of Acamprosate Calcium Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist, Alcohol Services Dr Donnelly
Media Release. Basel, 11 June 2009. RA patients with enhanced response identified
 Media Release Basel, 11 June 2009 New data demonstrate the ability of MabThera to reduce the progression of joint damage when used as a first-line biologic treatment in rheumatoid arthritis RA patients
Media Release Basel, 11 June 2009 New data demonstrate the ability of MabThera to reduce the progression of joint damage when used as a first-line biologic treatment in rheumatoid arthritis RA patients
A patient and public guide to the National Clinical Audit for Rheumatoid and Early Inflammatory Arthritis
 A patient and public guide to the National Clinical Audit for Rheumatoid and Early Inflammatory Arthritis 1st Annual Report 2015 (Data collection: 1 February 2014 30 April 2015) 2 Contents Background Who
A patient and public guide to the National Clinical Audit for Rheumatoid and Early Inflammatory Arthritis 1st Annual Report 2015 (Data collection: 1 February 2014 30 April 2015) 2 Contents Background Who
Understanding and improving communications between people with rheumatoid arthritis and their healthcare professionals. RCUKCOMM00116w February 2014
 Understanding and improving communications between people with rheumatoid arthritis and their healthcare professionals RCUKCOMM00116w February 2014 This project has been funded by Roche Products Ltd &
Understanding and improving communications between people with rheumatoid arthritis and their healthcare professionals RCUKCOMM00116w February 2014 This project has been funded by Roche Products Ltd &
Can Rheumatoid Arthritis treatment ever be stopped?
 Can Rheumatoid Arthritis treatment ever be stopped? Robert L. DiGiovanni, DO, FACOI Program Director Largo Medical Center Rheumatology Fellowship robdsimc@tampabay.rr.com Do not pour strange medicines
Can Rheumatoid Arthritis treatment ever be stopped? Robert L. DiGiovanni, DO, FACOI Program Director Largo Medical Center Rheumatology Fellowship robdsimc@tampabay.rr.com Do not pour strange medicines
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Tight control early rheumatoid arthritis clinic in Hong Kong: a pilot study
 O R I G I N A L A R T I C L E Tight control early rheumatoid arthritis clinic in Hong Kong: a pilot study Kitty Y Kwok MH Leung 郭 殷 梁 滿 濠 Objective To evaluate disease activity in early rheumatoid arthritis
O R I G I N A L A R T I C L E Tight control early rheumatoid arthritis clinic in Hong Kong: a pilot study Kitty Y Kwok MH Leung 郭 殷 梁 滿 濠 Objective To evaluate disease activity in early rheumatoid arthritis
RHEUMATOID ARTHRITIS. Dr Bruce Kirkham Rheumatology Clinical Lead
 RHEUMATOID ARTHRITIS Dr Bruce Kirkham Rheumatology Clinical Lead RHEUMATOID ARTHRITIS (RA) RA is a common disease: 0.8 per cent of the population RA more common in females: female to male ratio 3:1 RA
RHEUMATOID ARTHRITIS Dr Bruce Kirkham Rheumatology Clinical Lead RHEUMATOID ARTHRITIS (RA) RA is a common disease: 0.8 per cent of the population RA more common in females: female to male ratio 3:1 RA
Rheumatoid Arthritis: Constantly Evolving Treatment Approaches
 Rheumatoid Arthritis: Constantly Evolving Treatment Approaches Jody Garry, Pharm.D. Primary Care Pharmacy Resident VA Medical Center - Iowa City Presentation Overview Pathophysiology & epidemiology Diagnostic
Rheumatoid Arthritis: Constantly Evolving Treatment Approaches Jody Garry, Pharm.D. Primary Care Pharmacy Resident VA Medical Center - Iowa City Presentation Overview Pathophysiology & epidemiology Diagnostic
Disease Therapy Management (DTM) Enhances Rheumatoid Arthritis Treatment
 A WHITE PAPER BY Disease Therapy Management (DTM) Enhances Rheumatoid Arthritis Treatment Increased adherence rates deliver improved outcomes for patients FALL 2010 The Benefits of DTM for Rheumatoid Arthritis
A WHITE PAPER BY Disease Therapy Management (DTM) Enhances Rheumatoid Arthritis Treatment Increased adherence rates deliver improved outcomes for patients FALL 2010 The Benefits of DTM for Rheumatoid Arthritis
ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd
 ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd 07 February 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the
ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd 07 February 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the
to Part of Dossier: Name of Active Ingredient: Title of Study: Quality of life study with adalimumab in rheumatoid arthritis. ESCALAR.
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Individual Study Table Referring to Part of Dossier: Adalimumab (HUMIRA) (For National Authority Use Only) Name of Active Ingredient: Adalimumab Title
2.0 Synopsis Abbott Laboratories Name of Study Drug: Individual Study Table Referring to Part of Dossier: Adalimumab (HUMIRA) (For National Authority Use Only) Name of Active Ingredient: Adalimumab Title
1.0 Abstract. Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA. Keywords. Rationale and Background:
 1.0 Abstract Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA Keywords Rationale and Background: This abbreviated clinical study report is based on a clinical surveillance
1.0 Abstract Title: Real Life Evaluation of Rheumatoid Arthritis in Canadians taking HUMIRA Keywords Rationale and Background: This abbreviated clinical study report is based on a clinical surveillance
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Linking biobanks to registries: Why and how? Anne Barton
 Linking biobanks to registries: Why and how? Anne Barton Biobanks why should we collect samples? Anti-TNF treatment in RA Cost approx. 8,000/person/year 30-40% RA patients do not respond Rare, serious
Linking biobanks to registries: Why and how? Anne Barton Biobanks why should we collect samples? Anti-TNF treatment in RA Cost approx. 8,000/person/year 30-40% RA patients do not respond Rare, serious
Committee Approval Date: December 12, 2014 Next Review Date: December 2015
 Medication Policy Manual Policy No: dru299 Topic: Tecfidera, dimethyl fumarate Date of Origin: May 16, 2013 Committee Approval Date: December 12, 2014 Next Review Date: December 2015 Effective Date: January
Medication Policy Manual Policy No: dru299 Topic: Tecfidera, dimethyl fumarate Date of Origin: May 16, 2013 Committee Approval Date: December 12, 2014 Next Review Date: December 2015 Effective Date: January
Key Indexing Terms: RHEUMATOID ARTHRITIS LEFLUNOMIDE METHOTREXATE OPEN-LABEL TRIAL COMBINATION DISEASE MODIFYING ANTIRHEUMATIC DRUG THERAPY
 Combination Leflunomide and Methotrexate (MTX) Therapy for Patients with Active Rheumatoid Arthritis Failing MTX Monotherapy: Open-Label Extension of a Randomized, Double-Blind, Placebo Controlled Trial
Combination Leflunomide and Methotrexate (MTX) Therapy for Patients with Active Rheumatoid Arthritis Failing MTX Monotherapy: Open-Label Extension of a Randomized, Double-Blind, Placebo Controlled Trial
Trust Guideline. for. Shared Care Guidelines for the Use of Leflunomide (Arava )
 A guideline recommended for use Trust Guideline for Shared Care Guidelines for the Use of Leflunomide (Arava ) In: By: For: East and North Herts NHS Trust (ENHT) East and North Herts PCT/ENHCCG Consultants
A guideline recommended for use Trust Guideline for Shared Care Guidelines for the Use of Leflunomide (Arava ) In: By: For: East and North Herts NHS Trust (ENHT) East and North Herts PCT/ENHCCG Consultants
The management of rheumatoid arthritis
 Medical management of rheumatoid arthritis Peter Jones Correspondence to: peter.jones@qehealth.co.nz The management of rheumatoid arthritis has changed in the last 10 years. Back then, a patient who awoke
Medical management of rheumatoid arthritis Peter Jones Correspondence to: peter.jones@qehealth.co.nz The management of rheumatoid arthritis has changed in the last 10 years. Back then, a patient who awoke
A New Era in Rheumatoid Arthritis Treatment
 A New Era in Rheumatoid Arthritis Treatment Jill C. Costello, MD; Paul B. Halverson, MD ABSTRACT Rheumatoid Arthritis (RA) is a systemic autoimmune disease that primarily manifests as a chronic symmetric
A New Era in Rheumatoid Arthritis Treatment Jill C. Costello, MD; Paul B. Halverson, MD ABSTRACT Rheumatoid Arthritis (RA) is a systemic autoimmune disease that primarily manifests as a chronic symmetric
Rheumatoid Arthritis and Treat-to-Target
 Rheumatoid Arthritis and Treat-to-Target A Case of Need Encountering Opportunity Need RA affects approximately 1.5 million adults in the United States 1 20%-30% face permanent work disability if not treated
Rheumatoid Arthritis and Treat-to-Target A Case of Need Encountering Opportunity Need RA affects approximately 1.5 million adults in the United States 1 20%-30% face permanent work disability if not treated
ACR and EULAR Improvement Criteria Have Comparable Validity in Rheumatoid Arthritis Trials
 ACR and EULAR Improvement Criteria Have Comparable Validity in Rheumatoid Arthritis Trials ANKE M. van GESTEL, JENNIFER J. ANDERSON, PIET L.C.M. van RIEL, MAARTEN BOERS, CEES J. HAAGSMA, BILL RICH, GEORGE
ACR and EULAR Improvement Criteria Have Comparable Validity in Rheumatoid Arthritis Trials ANKE M. van GESTEL, JENNIFER J. ANDERSON, PIET L.C.M. van RIEL, MAARTEN BOERS, CEES J. HAAGSMA, BILL RICH, GEORGE
Adalimumab for the treatment of psoriasis
 DOI: 10.3310/hta13suppl2/07 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Adalimumab for the treatment of psoriasis D Turner, J Picot,* K Cooper and E Loveman Southampton Health Technology Assessments
DOI: 10.3310/hta13suppl2/07 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Adalimumab for the treatment of psoriasis D Turner, J Picot,* K Cooper and E Loveman Southampton Health Technology Assessments
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 17 December 2003 CPMP/EWP/556/95 rev 1/Final COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 17 December 2003 CPMP/EWP/556/95 rev 1/Final COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
Efficacy and safety of leflunomide in psoriatic arthritis
 Original Article Efficacy and safety of leflunomide in psoriatic arthritis ATM Asaduzzaman*, Akramullah Sikder*, Md. Mostaque Mahmud**, Harashit Kumar Paul*, Md. Nazrul Islam* *Department of Dermatology
Original Article Efficacy and safety of leflunomide in psoriatic arthritis ATM Asaduzzaman*, Akramullah Sikder*, Md. Mostaque Mahmud**, Harashit Kumar Paul*, Md. Nazrul Islam* *Department of Dermatology
Rheumatoid Arthritis. GP workshop 15 January 2011
 Rheumatoid Arthritis GP workshop 15 January 2011 Case 1 A 72 year old Malay woman with RA comes for routine follow up. She feels generally unwell in the last 5 days. Appetite is fair. Her joints are fine.
Rheumatoid Arthritis GP workshop 15 January 2011 Case 1 A 72 year old Malay woman with RA comes for routine follow up. She feels generally unwell in the last 5 days. Appetite is fair. Her joints are fine.
Rheumatoid Arthritis
 Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
Rheumatoid Arthritis While rheumatoid arthritis (RA) has long been feared as one of the most disabling types of arthritis, the outlook has dramatically improved for many newly diagnosed patients. Certainly
The submission positioned dimethyl fumarate as a first-line treatment option.
 Product: Dimethyl Fumarate, capsules, 120 mg and 240 mg, Tecfidera Sponsor: Biogen Idec Australia Pty Ltd Date of PBAC Consideration: July 2013 1. Purpose of Application The major submission sought an
Product: Dimethyl Fumarate, capsules, 120 mg and 240 mg, Tecfidera Sponsor: Biogen Idec Australia Pty Ltd Date of PBAC Consideration: July 2013 1. Purpose of Application The major submission sought an
Issue date: August 2010
 Issue date: August 2010 Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure of a TNF inhibitor Part review of NICE technology appraisal
Issue date: August 2010 Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure of a TNF inhibitor Part review of NICE technology appraisal
Etanercept Versus Methotrexate in Patients With Early Rheumatoid Arthritis
 ARTHRITIS & RHEUMATISM Vol. 46, No. 6, June 2002, pp 1443 1450 DOI 10.1002/art.10308 2002, American College of Rheumatology Etanercept Versus Methotrexate in Patients With Early Rheumatoid Arthritis Two-Year
ARTHRITIS & RHEUMATISM Vol. 46, No. 6, June 2002, pp 1443 1450 DOI 10.1002/art.10308 2002, American College of Rheumatology Etanercept Versus Methotrexate in Patients With Early Rheumatoid Arthritis Two-Year
Cost-effectiveness of dimethyl fumarate (Tecfidera ) for the treatment of adult patients with relapsing remitting multiple sclerosis
 Cost-effectiveness of dimethyl fumarate (Tecfidera ) for the treatment of adult patients with relapsing remitting multiple sclerosis The NCPE has issued a recommendation regarding the cost-effectiveness
Cost-effectiveness of dimethyl fumarate (Tecfidera ) for the treatment of adult patients with relapsing remitting multiple sclerosis The NCPE has issued a recommendation regarding the cost-effectiveness
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC)
 Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Lung Pathway Group Nintedanib (Vargatef) in advanced Non-Small Cell Lung Cancer (NSCLC) Indication: In combination with docetaxel in locally advanced, metastatic or locally recurrent NSCLC of adenocarcinoma
Dose Escalation of Parenteral Methotrexate in Active Rheumatoid Arthritis That Has Been Unresponsive to Conventional Doses of Methotrexate
 ARTHRITIS & RHEUMATISM Vol. 50, No. 2, February 2004, pp 364 371 DOI 10.1002/art.20167 2004, American College of Rheumatology Dose Escalation of Parenteral Methotrexate in Active Rheumatoid Arthritis That
ARTHRITIS & RHEUMATISM Vol. 50, No. 2, February 2004, pp 364 371 DOI 10.1002/art.20167 2004, American College of Rheumatology Dose Escalation of Parenteral Methotrexate in Active Rheumatoid Arthritis That
Teriflunomide is the active metabolite of Leflunomide, a drug employed since 1994 for the treatment of rheumatoid arthritis (Baselt, 2011).
 Page 1 of 10 ANALYTE NAME AND STRUCTURE TERIFLUNOMIDE Teriflunomide TRADE NAME Aubagio CATEGORY Antimetabolite TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND sclerosis. The
Page 1 of 10 ANALYTE NAME AND STRUCTURE TERIFLUNOMIDE Teriflunomide TRADE NAME Aubagio CATEGORY Antimetabolite TEST CODE PURPOSE Therapeutic Drug Monitoring GENERAL RELEVANCY BACKGROUND sclerosis. The
The Pharmacological Management of Cancer Pain in Adults. Clinical Audit Tool
 The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
The Pharmacological Management of Cancer Pain in Adults Clinical Audit Tool 2015 This clinical audit tool accompanies the Pharmacological Management of Cancer Pain in Adults NCEC National Clinical Guideline
Cost-effectiveness of teriflunomide (Aubagio ) for the treatment of adult patients with relapsing remitting multiple sclerosis
 Cost-effectiveness of teriflunomide (Aubagio ) for the treatment of adult patients with relapsing remitting multiple sclerosis The NCPE has issued a recommendation regarding the cost-effectiveness of teriflunomide
Cost-effectiveness of teriflunomide (Aubagio ) for the treatment of adult patients with relapsing remitting multiple sclerosis The NCPE has issued a recommendation regarding the cost-effectiveness of teriflunomide
DISEASE COURSE IN EARLY RHEUMATOID ARTHRITIS: AN OBSERVATIONAL STUDY
 ORIGINAL ARTICLES DISEASE COURSE IN EARLY RHEUMATOID ARTHRITIS: AN OBSERVATIONAL STUDY Teodora Serban 1,2, Iulia Satulu 2, Oana Vutcanu 2, Mihaela Milicescu 1,2, Carina Mihai 1,2, Mihai Bojinca 1,2, Victor
ORIGINAL ARTICLES DISEASE COURSE IN EARLY RHEUMATOID ARTHRITIS: AN OBSERVATIONAL STUDY Teodora Serban 1,2, Iulia Satulu 2, Oana Vutcanu 2, Mihaela Milicescu 1,2, Carina Mihai 1,2, Mihai Bojinca 1,2, Victor
Smoking and Rheumatoid Arthritis: how to deliver brief smoking cessation advice
 Smoking and Rheumatoid Arthritis: how to deliver brief smoking cessation advice Offering brief advice to stop smoking is the most cost-effective and clinically proven preventative action a healthcare professional
Smoking and Rheumatoid Arthritis: how to deliver brief smoking cessation advice Offering brief advice to stop smoking is the most cost-effective and clinically proven preventative action a healthcare professional
11/8/2011. Administrative Definitions of Rheumatoid Arthritis: Rising Prevalence Regardless of Definition Used. No Disclosures. Background.
 Administrative Definitions of Rheumatoid Arthritis: Rising Prevalence Regardless of Definition Used Christine A. Peschken, Carol A. Hitchon, Hui Chen, Allan Garland, Hani S. El-Gabalawy, Charles N. Bernstein
Administrative Definitions of Rheumatoid Arthritis: Rising Prevalence Regardless of Definition Used Christine A. Peschken, Carol A. Hitchon, Hui Chen, Allan Garland, Hani S. El-Gabalawy, Charles N. Bernstein
Version History. Previous Versions. Drugs for MS.Drug facts box fingolimod Version 1.0 Author
 Version History Policy Title Drugs for MS.Drug facts box fingolimod Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields as required
Version History Policy Title Drugs for MS.Drug facts box fingolimod Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields as required
Rheumatoid Arthritis
 Rheumatoid Arthritis Carole Callaghan Principal Pharmacist NHS Lothian Aim To update pharmacists on the current management of rheumatoid arthritis and explore ways to implement pharmaceutical care for
Rheumatoid Arthritis Carole Callaghan Principal Pharmacist NHS Lothian Aim To update pharmacists on the current management of rheumatoid arthritis and explore ways to implement pharmaceutical care for
Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011
 Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011 Working party: Eva Baecklund, Helena Forsblad d Elia, Carl Turesson Background Our purpose
Guidelines for the Pharmaceutical Management of Rheumatoid Arthritis Swedish Society of Rheumatology, April 14, 2011 Working party: Eva Baecklund, Helena Forsblad d Elia, Carl Turesson Background Our purpose
Original paper Reumatologia 2015; 53, 4: 200 206 DOI: 10.5114/reum.2015.53997
 Original paper Reumatologia 05; 53, 4: 00 06 DOI: 0.54/reum.05.53997 Rheumatoid arthritis treatment with TNF inhibitors and alternative procedures in case of its failure results of the Polish survey in
Original paper Reumatologia 05; 53, 4: 00 06 DOI: 0.54/reum.05.53997 Rheumatoid arthritis treatment with TNF inhibitors and alternative procedures in case of its failure results of the Polish survey in
Adjunctive psychosocial intervention. Conditions requiring dose reduction. Immediate, peak plasma concentration is reached within 1 hour.
 Shared Care Guideline for Prescription and monitoring of Naltrexone Hydrochloride in alcohol dependence Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist,
Shared Care Guideline for Prescription and monitoring of Naltrexone Hydrochloride in alcohol dependence Author(s)/Originator(s): (please state author name and department) Dr Daly - Consultant Psychiatrist,
How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado
 How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado Outline 1) Brief overview of natural history of RA and how current understanding of disease
How will we prevent rheumatoid arthritis? Kevin Deane, MD/PhD Division of Rheumatology University of Colorado Outline 1) Brief overview of natural history of RA and how current understanding of disease
Version History. Previous Versions. Policy Title. Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author
 Version History Policy Title Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields
Version History Policy Title Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields
A 5 YEARS REVIEW OF RHEUMATOID ARTHRITIS PATIENTS TREATED WITH METHOTREXATE: MAXIMUM TOLERATED DOSE AND ADVERSE DRUG EVENTS
 A 5 YEARS REVIEW OF RHEUMATOID ARTHRITIS PATIENTS TREATED WITH METHOTREXATE: MAXIMUM TOLERATED DOSE AND ADVERSE DRUG EVENTS P R E S E N T E D B Y : O O I Y E E S H I N P E G A W A I F A R M A S I U 4 8
A 5 YEARS REVIEW OF RHEUMATOID ARTHRITIS PATIENTS TREATED WITH METHOTREXATE: MAXIMUM TOLERATED DOSE AND ADVERSE DRUG EVENTS P R E S E N T E D B Y : O O I Y E E S H I N P E G A W A I F A R M A S I U 4 8
Early identification and treatment - the Norwegian perspective. Till Uhlig Dept of Rheumatology Diakonhjemmet Hospital Oslo, Norway
 Early identification and treatment - the Norwegian perspective Till Uhlig Dept of Rheumatology Diakonhjemmet Hospital Oslo, Norway Oslo Rheumatoid Arthritis Registry (ORAR) Very early Arthritis Clinic
Early identification and treatment - the Norwegian perspective Till Uhlig Dept of Rheumatology Diakonhjemmet Hospital Oslo, Norway Oslo Rheumatoid Arthritis Registry (ORAR) Very early Arthritis Clinic
Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe
 Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe Chair Clinical Affairs Committee, BSR Outline The British Society for Rheumatology Challenges in improving patient outcomes
Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe Chair Clinical Affairs Committee, BSR Outline The British Society for Rheumatology Challenges in improving patient outcomes
PROVEN NON-INVASIVE TREATMENT FOR RHEUMATOID ARTHRITIS
 PROVEN NON-INVASIVE TREATMENT FOR RHEUMATOID ARTHRITIS BIONICARE HAND SYSTEM Non-drug, non-invasive Adjunctive therapy For patients symptomatic despite current therapy For patients intolerant to drug
PROVEN NON-INVASIVE TREATMENT FOR RHEUMATOID ARTHRITIS BIONICARE HAND SYSTEM Non-drug, non-invasive Adjunctive therapy For patients symptomatic despite current therapy For patients intolerant to drug
Juvenile idiopathic arthritis and its long term outcome
 Focus Juvenile idiopathic arthritis and its long term outcome Sue Rudge is a paediatric rheumatologist at the Wellington Regional Rheumatology Unit and Starship Hospital, Auckland Introduction KEY POINTS
Focus Juvenile idiopathic arthritis and its long term outcome Sue Rudge is a paediatric rheumatologist at the Wellington Regional Rheumatology Unit and Starship Hospital, Auckland Introduction KEY POINTS
Medication Policy Manual. Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012
 Medication Policy Manual Policy No: dru283 Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012 Committee Approval Date: December 11, 2015 Next Review Date: December 2016 Effective Date: January
Medication Policy Manual Policy No: dru283 Topic: Aubagio, teriflunomide Date of Origin: November 9, 2012 Committee Approval Date: December 11, 2015 Next Review Date: December 2016 Effective Date: January
A LTCI Approach to Managing Rheumatoid Arthritis
 A LTCI Approach to Managing Rheumatoid Arthritis A bit of Science, a bit of Art, a lot of Perseverance... Stephen K. Holland, MD Senior Vice President & Medical Director Long Term Care Group, Inc. Long
A LTCI Approach to Managing Rheumatoid Arthritis A bit of Science, a bit of Art, a lot of Perseverance... Stephen K. Holland, MD Senior Vice President & Medical Director Long Term Care Group, Inc. Long
5.07.09. Aubagio. Aubagio (teriflunomide) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
How To Treat Rheumatoid Arthritis
 RHEUMATOLOGY Rheumatology 2012;51:v48 v54 doi:10.1093/rheumatology/kes122 Developing an effective treatment algorithm for rheumatoid arthritis Edward C. Keystone 1, Josef Smolen 2 and Piet van Riel 3 Abstract
RHEUMATOLOGY Rheumatology 2012;51:v48 v54 doi:10.1093/rheumatology/kes122 Developing an effective treatment algorithm for rheumatoid arthritis Edward C. Keystone 1, Josef Smolen 2 and Piet van Riel 3 Abstract
1. Title 2. Background
 1. Title EARLY PsA Effectiveness of early Adalimumab therapy in psoriatic arthritis patients from Reuma.pt, the Rheumatic Diseases Portuguese Register, Portuguese RheumatoLogy SocietY (SPR) 2. Background
1. Title EARLY PsA Effectiveness of early Adalimumab therapy in psoriatic arthritis patients from Reuma.pt, the Rheumatic Diseases Portuguese Register, Portuguese RheumatoLogy SocietY (SPR) 2. Background
Rituximab (MabThera ) in rheumatoid arthritis: non-nice approved indications
 Rituximab (MabThera ) in rheumatoid arthritis: non-nice approved indications Lead author: Stephen Erhorn NHS Regional Drug & Therapeutics Centre (Newcastle) July 2011 2011 Summary NICE guidance is extensive
Rituximab (MabThera ) in rheumatoid arthritis: non-nice approved indications Lead author: Stephen Erhorn NHS Regional Drug & Therapeutics Centre (Newcastle) July 2011 2011 Summary NICE guidance is extensive
Leflunomide Leflunomide
 Drug information Leflunomide Leflunomide This leaflet provides information on leflunomide and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Drug information Leflunomide Leflunomide This leaflet provides information on leflunomide and will answer any questions you have about the treatment. Arthritis Research UK produce and print our booklets
Guidance for Industry
 Guidance for Industry Cancer Drug and Biological Products Clinical Data in Marketing Applications U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and
Guidance for Industry Cancer Drug and Biological Products Clinical Data in Marketing Applications U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation and
Not All Clinical Trials Are Created Equal Understanding the Different Phases
 Not All Clinical Trials Are Created Equal Understanding the Different Phases This chapter will help you understand the differences between the various clinical trial phases and how these differences impact
Not All Clinical Trials Are Created Equal Understanding the Different Phases This chapter will help you understand the differences between the various clinical trial phases and how these differences impact
Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice
 Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice Gu NY 1, Huang XY 2, Globe D 2, Fox KM 3 1 University of Southern California,
Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice Gu NY 1, Huang XY 2, Globe D 2, Fox KM 3 1 University of Southern California,
Guideline for the use of Biological Therapies in the Treatment of Psoriasis
 1 Date of Production: March1 st 2011 Date of 1 st review: July 10 th 2015 Date for next review: March1 st 2018 Local Contact Dermatology Consultant Shanti Ayob Patient group to which this applies: Patients
1 Date of Production: March1 st 2011 Date of 1 st review: July 10 th 2015 Date for next review: March1 st 2018 Local Contact Dermatology Consultant Shanti Ayob Patient group to which this applies: Patients
ACD 3.0 - To Evaluate the Risk Assessment System
 TOCILIZUMAB FOR THE TREATMENT OF RHEUMATOID ARTHRITIS REPORT BY THE DECISION SUPPORT UNIT Stephen Palmer, Mark Sculpher Centre for Health Economics, University of York 6 May 2010 1 CONTENTS 1. SYNOPSIS
TOCILIZUMAB FOR THE TREATMENT OF RHEUMATOID ARTHRITIS REPORT BY THE DECISION SUPPORT UNIT Stephen Palmer, Mark Sculpher Centre for Health Economics, University of York 6 May 2010 1 CONTENTS 1. SYNOPSIS
Susanne Schmitz, 1 Roisin Adams, 2 Cathal D Walsh, 1,2 Michael Barry, 2 Oliver FitzGerald 3 EXTENDED REPORT. Clinical and epidemiological research
 EXTENDED REPORT Clinical and epidemiological research A mixed treatment comparison of the effi cacy of anti-tnf agents in rheumatoid arthritis for methotrexate non-responders demonstrates differences between
EXTENDED REPORT Clinical and epidemiological research A mixed treatment comparison of the effi cacy of anti-tnf agents in rheumatoid arthritis for methotrexate non-responders demonstrates differences between
subcutaneous initially every 4 weeks then every 12 weeks Coverage Criteria: Express Scripts, Inc. monograph dated 02/24/2010
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
