Long-term Effectiveness of Sorbie- QUESTOR Elbow Arthroplasty: Single Surgeon s Series of 15 Years
|
|
|
- Valentine McCoy
- 8 years ago
- Views:
Transcription
1 Long-term Effectiveness of Sorbie- QUESTOR Elbow Arthroplasty: Single Surgeon s Series of 15 Years CHARLES SORBIE, MB, CHB, FRCS(E), FRSC(C) ; GERALD SAUNDERS; PATRICIA CARSON, BSC(HON), BED; WILMA M. HOPMAN, MA; SANDRA J. OLNEY, PHD; JANET SORBIE, MD, FCFP abstract Full article available online at ORTHOSuperSite.com. Search: With increasing usage of many types of total elbow replacements, there is a continuing need for clinical series that report survivorship, complications and revisions, and performance of single types of implants over extended time periods. The purpose of this study was to assess the long-term effectiveness of all implants of the Sorbie-QUESTOR (SQ) unlinked surface arthroplasty conducted by a single surgeon (C.S.) over 15 years at a single site, and to determine whether there were diagnostic group differences. Between 1995 and 2002, 51 S-Q prosthetic elbows were implanted into 44 patients. The patient groups were hemophilia, rheumatoid arthritis, and other, which included osteoarthritis, traumatic arthritis, psoriatic arthritis, and reactive arthritis. Annual evaluations included scores of pain, range of motion, and function. The most recent annual evaluation was included in the data set. Details of complications and revisions were recorded. The hemophiliac group had the best survival outcomes at 87.5%. Eighteen prostheses required revision or removal with all but 3 retained or replaced. Postoperatively, 73% rated their pain as slight or none. The hemophilia and rheumatoid arthritis groups made very large total flexion/extension gains. The rheumatoid arthritis group made significant forearm motion gains. Average functional assessment gains were nearly 2 grades of 5 functional levels and were significant for all groups. The S-Q surface arthroplasty has demonstrated long-term effectiveness in patients with a variety of elbow joint pathologies showing reduction in pain, large gains in joint range and function, and good long-term survival. Dr Sorbie (Charles) was from Division of Orthopaedic Surgery and Clinical Mechanics Group, Mr Saunders, Ms Carson, and Dr Olney are from the Division of Orthopaedic Surgery and Clinical Mechanics Group, Queen s University and Kingston General Hospital, Ms Hopman is from Clinical Research Centre, Kingston General Hospital and Department of Community Health and Epidemiology, and Dr Sorbie (Janet) is from Department of Family Medicine, Queen s University, Kingston, Ontario, Canada. Canada. Died March 29, Drs Sorbie (Charles), Olney, and Sorbie (Janet), Mr Saunders, and Mss Carson and Hopman have no relevant fi nancial relationships to disclose. The authors thank Carolyn Heymans for her extensive technical assistance, Dr Derek Cooke for editorial assistance, and the many patients who contributed to this study. Correspondence should be addressed to: Sandra J. Olney PhD, 154 Albert St, Queen s University, Kingston, Ontario, Canada K7L 3N6 (sandra.olney@queensu.ca). doi: / e561
2 Arthritis of the elbow joint may cause chronic, often unremitting pain, joint instability, or stiffness, and results in serious functional loss. A good elbow is essential for placing the hand in space, for personal care, and for the use of canes and crutches. Before the development of replacement arthroplasty, synovectomy of the elbow joint, 1 resection arthroplasty, 2 cheilectomy, 3 radial head resection, 4 and arthrodesis 3 were the surgical techniques available for the treatment of elbow arthritis. With modern technology and improved implant design, it is now possible to achieve a stable joint and a pain-free range of movement. The complexity of the surface geometry, 5,6 and the kinematics of the joint 7 have challenged surgeons and engineers in the design of elbow implant prostheses for successful arthroplasty. The evolution of design has progressed from a rough approximation metal hinge, to linked or semi-constrained hinges and finally to unlinked prostheses, 8,9 including one mirroring normal surface geometry, 10 the joint being stabilized by surface shape and soft tissues. This is the basis of the design of the Sorbie- QUESTOR (S-Q) (Wright Medical Technology, Mississauga, ON, Canada) surface arthroplasty reported in this study. Clinical and survivorship performance of an implant are important in device selection. Findings to date are by no means uniform or conclusive. Survivorship reporting has rarely involved the use of a survival analysis, making the data unreliable. 11 Complication rates have varied from 14% to 80% with little insight into differences. With respect to function, constrained implants have shown a better range of movement than unlinked, although overall outcomes have been marginally better with semi-constrained than either unlinked or constrained devices. 11 Unlinked devices have been reported to have higher rates of loosening, instability, and dislocation than other types. 11 The average reporting time for follow-up has been 60 months, making reports of 5 years of considerable value. The provision of systematic information on a 15-year clinical series of 1 type of unlinked implant would complement current information and assist in clinical decision-making. Between 1995 and 2002, fifty-one S-Q prosthetic elbows were implanted into 44 patients by a single surgeon (C.S.). The purpose of this study was to assess the long-term effectiveness, including pain relief, range of motion, stability, and function of total elbow arthroplasty using the unlinked S-Q surface arthroplasty 12 in the treatment of a variety of arthritic conditions. A secondary purpose was to determine if there were any apparent differences between major diagnostic groups that might affect clinical decision-making. MATERIALS AND METHODS This research was approved by the Queen s University Health Sciences and Affiliated Teaching Hospitals Research Ethics Board. The protocol, consisting of questions about pain and function, as well as direct observations and measurements made by the surgeon, was administered to each patient returning for annual follow-up visits. For the purpose of this analysis, the most recent complete data set available for each patient was included in the data set. Patients who retained the prosthesis but were unable to attend clinic due to distance or health constraints were interviewed by the Research Associate (P.C). over the telephone. The outcome protocol, based on the Mayo Elbow Performance Score with modification 13,14 was completed prior to surgery and at follow-up. The assessment of pain (0 complete disability, 5 none) included elbow, shoulder, and wrist joints. Measurements included elbow range of motion (flexion and extension), forearm movement (supination, pronation), shoulder movement (flexion, extension, abduction, adduction, internal rotation, external rotation), and wrist movement (flexion and extension). Only data for the elbow and forearm is presented in this article. Functional assessment was based on 11 items (cup to mouth, eating with spoon, cutting with knife, lifting 1-liter kettle, pouring kettle to glass, telephone to ear, grasp opposite earlobe, wash opposite axilla, rise from chair with arms, turn door knob and push door open, pull door open), with each item scored from 0 (impossible) to 4 (no difficulty); total scores ranged from 0 to 44. Additional information including age, gender, diagnosis, dominant side, and time since symptoms started, was also collected. Statistical Analysis Data was entered into an Excel spreadsheet and imported into SPSS 18.0 for Windows 15 for statistical analysis. Following descriptive analyses (frequencies for the categorical variables, means, standard deviations, and medians for the linear variables), improvements in range of motion and functional activity were assessed by calculating change scores; the 95% confidence intervals of the change scores indicate whether the changes within the groups were statistically significant. Chi-square tests were used to compare the 3 diagnostic groups on categorical data such as sex, and 1-way analysis of variance was used to compare continuous data such as the change within each of the 3 diagnostic groups. A Kaplan-Meier curve was generated to assess the survival time of the prosthesis; cases were censored at the last known time that they had a functional S-Q prosthesis. If the patient died with a functional prosthesis, the date of death was used as the last time of known functional prosthesis. Implant Design The design philosophy for the S-Q unlinked arthroplasty had the objective of transferring load more naturally from the forearm to the arm through synthetic joint surfaces and the soft tissues around the joint. It was assumed that surface arthroplasty implants using soft tissue to transfer a significant amount of load, would be less likely to wear or loosen with the passage of time. For successful function and survival of unlinked forms of arthroplasty, there would have to be sufficient ligament and capsule integrity for joint stability. An arthroplasty faithfully e562 ORTHOPEDICS ORTHOSuperSite.com
3 ELBOW ARTHROPLASTY EFFECTIVENESS SORBIE ET AL reproducing the natural surface geometry of the 3 elbow joint bones, correctly placed, would allow the forearm to move along normal kinematic axes and allow muscles to restore normal strength. Such an arthroplasty would require instruments to ensure precise bone preparation and firm fixation of implants to host bone in the correct original axes of motion. In 1980, the morphometry of the elbow joint was determined. Overall dimensions were obtained by statistical analysis of distances between 11 identifiable bony points in the distal humerus and upper ulna obtained on radiographs of 60 normal left/right, male/female adult elbow joints. 16 Cartilage thickness was added to bone surface measurements using cadaveric data. A biostatistical analysis 17 determined ideal dimensions for 1 to 6 sizes for humeral and ulnar components. Using 3 average sizes, small, medium, and large, the maximum dimensions are within 2 mm of correct fit tolerance in the greatest dimension (medial-lateral width) for normal patients. The kinematics of the elbow joint were studied to determine axes of motion, carrying angle, and the distribution of forces across the trochlea, olecranon, and capitello-radial head surfaces described in full in previous publications. 10 To determine the surface geometry, cadaver elbow bones fixed on standard, definable axes were sliced on a milling machine in the sagittal plane. Slices of.76 mm thickness were shaved from each distal humerus and upper ulna specimen. The cut surfaces, cartilage stained red, were photographed and digitized, yielding 5000 coordinates, which described the outer limits of the slices. A software program was written for analysis of the data using Cartesian mathematical assumptions. Reproduction of the virtual slices by computer graphics visually displayed their amassed coordinates, their joint surface geometry, and the location of their centers. The centroidal axis of flexion/ extension of the humerus was determined by joining the centers of the humeral slices. The axes of rotation of the olecranon and coronoid facets were similarly determined. The data showed that the elbow does not move in flexion and extension on a simple, single axis of motion, but one described as a sloppy hinge. Instant centers of motion are defined when major contact is between the posterior surface of the trochlea and the olecranon facet (force applied with the joint in extension) and between the anterior surface of the trochlea and the coronoid facet (force applied with the joint in flexion). The data was also used to create software that allowed computer numeric contouring in steel of implant prototypes for the humerus, radius, and ulna. Instruments were developed that, when attached to bone, guide precision cutting tools to remove damaged joint surfaces. The ulnar implant was made to hold modular polyethylene inserts of 2 thicknesses, which reproduce the ulnar surfaces. The contact surface of the radial head component is polyethylene covered. Stabilizing stems are present on all components. Surgical Technique The S-Q elbow arthroplasty is inserted with the patient supine, elevated on the affected side so that the weight of the arm across the front of the chest maintains its position. While a posterior midline incision is possible, a modification of the Kocher 18 approach has been used in this series. Before lifting the anconeus and triceps insertion, Methylene Blue or a colored pen is used to mark its area of insertion on the triceps posterior surface. This facilitates the tendon s accurate repositioning and fixation at the end of the procedure. Steel templates are used on the sides of the trochlea and capitellum to locate the centroidal axis of flexion/extension, which extends between the center points of their surface contours (Figure 1). One-eighth inch (3.175 mm) drills are inserted to a depth of 1 cm at these points to accept pins protruding from the first cutting guide, which directs the saw at the correct angle to remove the central part of the trochlea and open the distal medullary canal of the humerus. The elbow is dislocated to allow this. The canal is broached and a second block-cutting guide attached with side bars and pins that use the same drill holes in the centroidal axis of flexion/extension to fix the block in place. An attached rod engages the medullary canal at the correct angle for the humeral implant stem. Five osteotomy cuts are made in the subchondral bone of the distal humerus, excluding the non-cartilage covered area on the posterior surface of the capitellum, which is the origin of the anconeus (Figure 2). These cuts shape the end of the humerus to accept the implant. A trial humeral implant is inserted and then removed. Using an oscillating saw, a minimum amount of radial joint surface is removed at 90 to the long axis of the neck, making sure that the cut is below the cartilage boundary. The neck is broached with a trifin instrument to take the radial implant stem. A jig is attached to the ulna, and a side-cutting router, directed by a cam, is used to remove the surface of the sigmoid fossa of the ulna in a precise curve, retaining the maximum amount of subchondral bone. The upper part of the ulna is broached to take a trial implant. When all 3 trial implants are in po- Figure 1: Sizing of the humerus. (Reprinted with permission from Wright Medical.) 1 e563
4 3 Figure 2: Distal, anterior, and bevel cuts. (Reprinted with permission from Wright Medical.) Figure 3: Insertion of medullary cement restrictor. (Reprinted with permission from Wright Medical.) sition, the elbow is reduced, and depending on the laxity of the joint space when flexed, a decision is made on the thickness of the polyethylene modular bearing surface on the ulnar component. Because the thickness increments are very small, there is Figure 4: Mediolateral radiograph of completed Sorbie-QUESTOR elbow arthroplasty. Figure 5: AP radiograph of completed Sorbie-QUESTOR elbow arthroplasty. minimum impact on the kinematics of the elbow. The appropriate medullary insert size is selected and placed in the humeral canal to the designated depth (Figure 3). The permanent implants are then inserted and fastened with PMMA cement. The tendon of triceps is reattached using the stained blue area to ensure accurate repositioning. Four holes are drilled through the upper end of the ulna starting near the 4 corners of the area of triceps attachment and exiting on the posterior surface of the ulna approximately 3 cm from the tip of the olecranon. With the help of doubled-over wires, non-absorbable sutures are drawn through these holes, crossing the posterior border of the ulna. Free curved cutting needles lead the doubled suture threads through the peripheral limits of the stained area on the tendon over which the sutures are firmly tied. This process of attachment of the triceps allows early mobilization of the joint. The raised common extensor origin is reattached to the lateral epicondyle and secured with non-absorbable sutures through a drill hole in the epicondyle. The wound is closed in layers and in the skin, subdermal polyglycolic acid sutures with buried knots, draw the wound edges together and ensure that no sutures track through the skin. Radiographs of a completed arthroplasty are shown in Figures 4 and 5. RESULTS Pain was the overarching reason for elbow replacement, with stiffness being the second most common complaint. Patient characteristics appear in Table 1. The groups differed in age, gender, and occurrence of previous surgeries at surgery. Average follow-up was 7 years or more for all groups. For many patients, the joint replacement followed many years of interventions, reflecting the 28 years of average duration of their conditions. Six patients had received prior same-side surgeries before receiving the S-Q prosthesis, 1 having had a single procedure, 2 patients with between 2 and 4 operations, and 3 having had 5 surgeries before elbow arthroplasty. Four patients had prior elbow surface replacements for rheumatoid arthritis (n 3) or trauma (n 1). Two elbows were completely ankylosed prior to surgery, 1 the result of juvenile rheumatoid arthritis, the other, hemophilia. Although patients with gross distortion of the elbow bones were excluded, 2 patients had significant distal humeral deformity as a result of supracondylar fracture in childhood. Five patients had prior radial head excision after injury or in association with synovectomy for the treatment of rheumatoid arthritis and had insufficient remaining radial neck to support a radial implant. The humero-ulna relationship nonetheless remained intact in 4 and functioned well. One patient with humeral deformity and a permanently displaced radial head after supracondylar fracture as a child had the radial head removed. Her ulna now tracks on the groove between trochlea and capitellum, but she has a painless elbow with a stable functional range of 45 to 140. Survivorship Analysis The Kaplan-Meier curve (Figure 6) shows that the hemophiliac group had the best outcomes overall, with all 8 lasting at least 60 months, and only 1 of 8 experiencing a failure for a functional rate of 87.5% at study end. The rheumatoid arthritis group and the other group showed a similar pattern, although 23/32 (72%) of the rheumatoid arthritis replacements were still functional at the time of censoring while 6/11 (55%) of the other group were functional. However, these e564 ORTHOPEDICS ORTHOSuperSite.com
5 ELBOW ARTHROPLASTY EFFECTIVENESS SORBIE ET AL group differences fell short of statistical significance (Mantel-Cox Chi-square 2.22, P.14). Complications, Revisions, and Removals of S-Q A total of 18 implants were revised or replaced once, and of these, 4 were revised twice. Of these, 15 implants were removed, 12 of which were replaced (Table 2). Seven were likely due to nosocomial infection (discussed below), 4 occurred due to traumatic loosening in non-rheumatoid arthritis patients, 2 patients with rheumatoid arthritis had aseptic loosening, and 2 were removed or revised due to infection and complex health problems. Although group differences were not statistically significant, there may be clinical importance to the fact that these involved 13.5% of the hemophilia group, 27% of the rheumatoid arthritis group, and 50% of the other group. The final status of the 15 removals was 10 received Coonrad- Morrey, 2 received new S-Qs, and 3 were flail. Three patients, all with rheumatoid arthritis, had revisions that required ulnar stabilization, triceps plication, or a change of polyethylene insert. All retained their original S-Q prostheses. Seven patients developed infection at some time after the operative procedure, with the shortest time between surgery and recorded infection being 3 weeks, and the longest, 9 years. Five of the patients with infections had rheumatoid arthritis and were immunocompromised by the disease and their treatment with steroids and/or methotrexate. One infected case with posttraumatic osteoarthritis had 7 previous operative procedures before presenting for replacement. The remaining patient who had the shortest postoperative time to infection, 3 weeks, had psoriatic arthropathy, previous splenectomy, was hepatitis C positive, had chronic liver failure, and had serious drug addictions. Three of 8 arthroplasties in patients with hemophilia showed some evidence of osteolysis between the host bone and bone cement around both the humeral and ulnar components. One arthroplasty required complete Table 1 Characteristics of 44 Patients and 51 Elbows Mean SD (Range) Rheumatoid Characteristic Hemophilia (N 7) Arthritis (N 27) Other a (N 10) P value Age at surgery, y 43 9 (28-54) (24-77) 48 8 (34-62).033 Years affected at (9-46) (10-57) (7-69).62 surgery Follow-up, mo (66-120) (2-148) (5-144).78 Frequency, % Men 7 (100) 9 (33) 6 (60).006 Prior elbow surgery 0 (0) 9 (33) 7 (70).011 Follow-up status Lost to follow-up 1 (14) 1 (4) 1 (10).86 Seen at clinic (2009) 2 (29) 6 (22) 2 (20) By telephone (2009) 3 (43) 13 (48) 6 (60) Died 1 (14) 7 (26) 1 (10) Abbreviation: SD, standard deviation. a Includes osteoarthritis (3), traumatic arthritis (5), psoriatic arthritis (1) and reactive arthritis (1). b If the patient died with a functional S-Q, this was included as functional. c P values are based on independent samples t tests (continuous data) or chi-square tests (categorical data). Figure 6: Kaplan-Meier curve comparing prosthetic survival time for the 3 groups. Log rank test for differences between groups: X , P.136. e565
6 Table 2 Characteristics and Final Status of S-Q Elbow Arthroplasty Removals/Replacements (N=15) and Revisions (N=3) Reason for Removal/Replacement Final Status Diagnosis Months to S-Q Revision/Removal Likely nosocomial infection (N=7) 4 Coonrad-Morrey, 2 new S-Q, 1 flail 5 RA, 1 OA, 1O 2-12 Traumatic loosening (N=4) 4 Coonrad-Morrey 3 OA, 1 H Aseptic loosening (N=2) 1 Coonrad-Morrey, 1 flail 2 RA 27, 78 Infection, trauma, multiple comorbidities (N=2) 1 Coonrad-Morrey, 1 flail 1 RA, 1 O 7, 9 Reason for Revision Without Removal Stabilize ulnar component (N=2) Original S-Q 2 RA 8, 3 Triceps plication, change polyethylene insert (N=1) Original S-Q 1 RA 10 Abbreviations: H, hemophiliac; OA, osteoarthritis; O, other; RA, rheumatoid arthritis. revision, and 1 other may need revision in the future. This radiological appearance has been assumed to result from hemorrhage around the implant, as the individuals have all been young, hardworking men who did not stay strictly to Factor 8 protocol. The joint proved to be very stable. In this series, only 2 patients subluxed early, 1 with 7 previous operations, and the other with tissues badly weakened by rheumatoid arthritis. The second, a patient with a deformity from childhood and no radial head, tracks her ulna in the groove between trochlea and capitellum of the humeral component. There were 2 cases of prolonged ulnar nerve injury (4%) from the time of surgery. Three cases of temporary ulnar neuritis (6%) occurred in patients with rheumatoid arthritis, all of which cleared. Table 3 Number of Patients and Percentage of Group in Each Pain Category Pre- and Postoperative a N (%) Hemophilia (N=8) Rheumatoid Arthritis (N=32) Other (N=11) Pre Post Pre Post Pre Post Complete disability 3 (38) 0 (0) 5 (17) 0 (0) 2 (20) 0 (0) Severe 2 (25) 0 (0) 10 (35) 0 (0) 6 (60) 1 (10) Moderate/severe 2 (25) 0 (0) 8 (28) 1 (3) 0 (0) 0 (0) Moderate on activity 0 (0) 3 (38) 2 (7) 3 (10) 2 (20) 2 (20) Slight 1 (13) 2 (25) 2 (7) 14 (48) 0 (0) 4 (40) None 0 (0) 3 (38) 2 (7) 11 (38) 0 (0) 3 (30) Abbreviations: Post, postoperative; Pre, preoperative. a Percentages do not always equal 100 due to rounding. Pain and Functional Outcomes The numbers of patients and percentages of groups in each pain category pre- and postoperative appear in Table 3. Means and confidence intervals for ranges of motion and functional outcomes pre- and postoperative appear in Table 4. Changes in range of motion and functional outcomes are shown in Table 5. There were no statistically significant differences between groups in pain, range of motion or function before surgery. Pain data (Table 3) shows that 55% rated their pain as complete disability or severe preoperatively, whereas 73% rated their pain as slight or none postoperatively. The hemophilia and rheumatoid arthritis groups made total range of motion gains of 59 and 40 respectively, with the other group s changes not reaching significance (Table 5). Gains in forearm motion were significant only for the rheumatoid arthritis group, with 49 improvement derived from nearly equal increases in pronation and supination. Average functional assessment gains, ranging from 17 to 21 points, were significant for all groups, and not different between groups. This represented an average of nearly 2 grades (eg, from with much difficulty to no difficulty or from with aid to with little difficulty ). All patients who were employed prior to their elbow replacement returned to their previous occupations, some of which required significant elbow muscle strength and stability. The occupations included working at a supermarket checkout counter, computer programming, horse breeding, cattle breeding, farming, and other forms of intensive e566 ORTHOPEDICS ORTHOSuperSite.com
7 ELBOW ARTHROPLASTY EFFECTIVENESS SORBIE ET AL physical work. One patient, within 1 year of surface replacement, won 2 golf championships and a longest drive competition (315 yards). The golfer continues, 12 years after his replacement, to play competitive golf. DISCUSSION Survivorship The hemophiliac group had the best outcomes overall with a functional rate of 87.5% at study end, which was a mean of 100 months. In the rheumatoid arthritis group, 72% of the replacements were still functional at the time of censoring (mean, 89 months), while this was true for 55% of the other group (mean, 84 months). Although survivorship has been seldom reported, for the unlinked Souter-Strathclyde prosthesis, authors have reported average 5-year survivals to be 96%, year 89%, year 76%, 20 and 15-year to be 83%. 19 For rheumatoid arthritis patients, the unlinked Kudo 5 has shown its estimated 12-year survival to be 74%. 21 For the semi-constrained Coonrad-Morrey, Prasad and Dent 20 reported 100% surviving at 60 months; Throckmorton et al, 22 using end points of revision or resection, have reported the 5-year survival rate to be 92%, 10-year survival 78%, and 15-year survival to be 70%. The results of the present series are considered satisfactory considering the length of follow-up. Consistent with previous observations, total elbow arthroplasty appears not as durable for the treatment of posttraumatic arthritis as it is for the treatment of the hemophiliac 23 or rheumatoid elbow. 22 Complications A complication rate of 35% in this study, which included removals, replacements, and revisions, compares favorably with literature values, which vary from 14% to 80%. 11,24 One factor influencing this number in all studies is the condition of the patients at the time of surgery. In this series, in many instances, surgery was seen as a final opportunity to alleviate pain and/or to improve elbow function. Table 4 Mean and 95% Confidence Intervals for Pre- and Postoperative Range of Motion and Functional Outcomes a,b Preoperative Hemophilia (N 8) The infection rate of approximately 16% is higher than post-1989 reports, which has reached a low of approximately 4%. 11 Two factors may account for this. First, many patients had pre-existing conditions and prior surgery that added to the occurrence of complications. Cheung et al 25 reported that a third of total elbow arthroplasties that became infected had previous elbow surgery. Second, 1 simple procedural change was found to be of importance in reducing infections in the current series. In the early part of this clinical trial, standard, multi-use, clean, but non-sterile tourniquets were being applied to the arm and could have been a source of infection, Rheumatoid Arthritis (N 32) Other (N 11) P Value c Elbow ROM flexion 96 (62, 131) 98 (87, 109) 117 (105, ) Elbow ROM extension 48 (19, 78) 42 (31, 52) 41 (20, 62).84 Elbow ROM total 48 (4, 92) 57 (44, 69) 76 (51, 100).26 Forearm pronation 46 (15, 77) 41 (30, 53) 62 (39, 84).23 Forearm supination 60 (26, 94) 40 (27, 54) 68 (47, 89).08 Forearm ROM total 106 (45, 167) 87 (64, 111) 129 (98, 159).18 Functional total d 21 (14, 28) 15 (11, 19) 13 (4, 21).28 Postoperative Elbow ROM flexion 129 (108, 151) 129 (121, 137) 135 (125, ) Elbow ROM extension 23 (0, 45) 33 (26, 40) 40 (27, 53).19 Elbow ROM total 107 (67, 147) 96 (85, 107) 92 (77, 107).62 Forearm pronation 60 (28, 92) 71 (63, 79) 55 (32, 77).18 Forearm supination 63 (30, 97) 68 (60, 77) 63 (42, 83).77 Forearm ROM total 123 (69, 178) 138 (125, 152) 117 (81, 153).34 Functional total d 40 (37, 44) 32 (29, 36) 34 (20, 47).14 Abbreviation: ROM, range of motion. a All joint angles and range of motion in degrees, with full extension equal to 0. b Confi dence Intervals indicate whether the between-group differences are signifi cant. If the confi dence intervals of 2 groups overlap, the differences between them are not statistically signifi cant. c P value is based on the one-way ANOVA for between-group differences. d Function total is based on 11 items (eating, telephone use, turning knobs, etc); each item is scored from 4 (no diffi culty) to 0 (impossible); scores range from 0 to 44. especially in the rheumatoid arthritis patients. After changing to sterile, disposable, singleuse tourniquets, no infections occurred. The group that had nonsterile tourniquets accounted for 14% of the 16% of infections. The rate of loosening in this study was 12%. As a comparison, in Little s review, 11 the loosening across all prosthetic types was reported to be about 9%, with sloppy hinge devices showing the lowest rates and fixed hinges the highest, and values appearing to be the highest for rheumatoid arthritis patients. 20 However, others 26 have reported that 14% of the Kudo type 5 unlinked prostheses required revision at 6 years because e567
8 Table 5 Mean and 95% Confidence Intervals for Changes in Range of Motion and Functional Outcomes a,b Hemophilia (N=8) of loosening of the ulnar component, and another 27 reported a revision rate of 29% at 10 years for Kudo Type III prostheses. The results of the current study are therefore considered satisfactory. The complications of prolonged nerve injury (4%) and temporary ulnar neuritis (6%), all of which cleared, compare favorably with those of Rispoli et al, 28 who reported ulnar neuropathy in 5% to 10% of total elbow replacements. Pain and Function Pain showed marked improvement after surgery. Because pain was a primary reason for seeking the surgery, the improvement was gratifying, though not unexpected. In the few studies that report pain separately, good results have generally been found. 29 The hemophilia and rheumatoid arthritis groups, with flexion/extension range of motion gains of 59 and 40, exceeded greatly the average improvement of only 20 reported in 46 studies of unlinked prostheses. 11 Other studies do not report Mean (95% CI) Rheumatoid Arthritis (N=32) Other (N=11) P value c Elbow ROM flexion 33 (6, 60) 31 (18, 45) 18 (2, 35).54 Elbow ROM extension 25 ( 47, 4) 8 ( 19, 3) 1 ( 19, 17).18 Elbow ROM total 59 (21, 96) 40 (26, 53) 17 ( 12, 46).09 Forearm pronation 14 ( 18, 45) 28 (16, 40) 9 ( 42, 25).029 Forearm supination 1 ( 8, 10) 26 (13, 40) 3 ( 23, 17).033 Forearm ROM total 15 ( 24, 54) 49 (26, 72) 9 ( 46, 28).026 Functional total d 20 (12, 27) 17 (12, 22) 21 (10, 32).68 Abbreviations: CI, confi dence intervals; ROM, range of motion. a All joint angles and range of motion in degrees, with full extension equal to 0. b Confi dence intervals indicate whether or not the between-group differences are signifi cant. They can also be used to assess the signifi cance of within-group change. For example, if the range crosses 0, as it does for rheumatoid arthritis elbow ROM extension, the change is not signifi cant. However, all 3 groups saw signifi cant gains in function. c P value is based on the one-way ANOVA for between-group differences. d Function total is based on 11 items (eating, telephone use, turning knobs, etc); each item is scored from 4 (no diffi culty) to 0 (impossible); scores range from 0 to 44. forearm gains, which were high for the rheumatoid arthritis group (49 ). Differences Between Diagnostic Groups Because numbers of patients in 2 groups were small and variances large, limited interpretations can be made. Preoperatively, the rheumatoid arthritis group was older, though years affected at surgery and follow-up times were not substantially different. Also, 70% of the other group had received prior elbow surgery, whereas only 33% of the rheumatoid arthritis group had, and the hemophiliac group had none. With respect to elbow range gains, the other group was the only one not making significant range of motion total gains, though the average gain was 17. Examining for preoperative differences that might explain this finding, there was a trend for this group to have more flexion (average 21 and 19 ) and a greater total range (27 and 19 ) at baseline than the hemophilia and rheumatoid arthritis groups respectively. Their modest gains resulted in similar average flexion ranges as the other 2 groups but substantially less extension than the other 2 groups (17 and 7 ), although the values did not reach significance. The function gains were as large as those of the other groups and placed them, on average, in the performance with little difficulty category. Because half of this other group had posttraumatic arthritis, these are encouraging results. 30 The positive results of the rheumatoid group suggest more optimistic outcomes and less guarded approaches than previously advised. 7 Despite small variations in outcomes, the minor differences between groups do not suggest any group preference for implantation of the S-Q prosthesis. Importance of Design and Surgical Method We believe the postoperative joint stability and increases in joint range and function, combined with satisfactory survival and complication rates, are due to the unique design of the S-Q prosthesis, which was directed to restoring normal elbow kinematics, and to surgical procedures directed to achieving normal joint kinematics and early postoperative movement. The human elbow joint is inherently stable in its natural state, and the S-Q prosthesis was designed to reproduce normal geometry. This included replication of the trochlear flanges on the humeral surface of the S-Q prosthesis, which ensures that joint forces can be applied with no unnatural stresses. Using simulated loads and a full range of motion, Inagaki et al 31 concluded that the unconstrained S-Q elbow replacement simulated the geometry of the normal articular surface and demonstrated normal motion patterns under conditions of medium and high muscle loading. They showed that the radial head component enhanced the dynamic contribution to stability of muscle loading, particularly in extension. Any relative laxity, as exists in the normal elbow, was reduced with increased muscle loading. Similarly, in his 2002 series, Inagaki et al 32 showed the inherent stability of the S-Q implants when precisely placed because of their reproduction of the normal surface geometry. e568 ORTHOPEDICS ORTHOSuperSite.com
9 ELBOW ARTHROPLASTY EFFECTIVENESS SORBIE ET AL The design and surgical method insures that the components be placed exactly on the natural axis of motion, which is important for recovery of normal joint function and avoidance of abnormal stresses. 33,34 Having located the position of the axis of flexion and extension by the slicing technique, metal templates used in surgery ensured that the humeral component of the S-Q implant was correctly located. Because loads during simple activities of daily living can be very large, the triceps tendon was carefully preserved and firmly replaced on its original position on the olecranon. Failure to do so can lead to weak fixation of the tendon or complete loss of attachment. 35 Furthermore, because the triceps tendon was secured to its original location with such firm reattachment, the patients were able to begin extending the elbow on postoperative day 1, which may have facilitated early gains in range of motion. The S-Q surface arthroplasty has demonstrated long-term effectiveness in patients with a variety of elbow joint pathologies showing good stability, reduction in pain, large gains in joint range and function, and good long-term survival. REFERENCES 1. Laine V, Vainio K. Synovectomy of the elbow. In: Hijmans W, Paul WD, Herschel H, eds Early Synovectomy in Rheumatoid Arthritis. Amsterdam: Excerpta Medica; 1969: Hurri L, Pulkki T, Vainio K. Arthroplasty of the elbow in rheumatoid arthritis. Acta Chir Scand. 1964; 127: Savoie FH III, Nunley PD, Field LD. Arthroscopic management of the arthritic elbow: indications, techniques, and results. J Shoulder Elbow Surg. 1999; 8(3): van der Lugt JC, Rozing PM. Systematic review of primary total elbow prostheses used for the rheumatoid elbow [published online ahead of print April 16, 2004]. Clin Rheumatol. 2004; 23(4): Shiba R, Sorbie C, Siu DW, Bryant JT, Cooke TD, Wevers HW. Geometry of the humeroulnar joint. J Orthop Res. 1988; 6(6): Waide DV, Lawlor GJ, McCormack BA, Carr AJ. The relationship between surface topography and contact in the elbow joint: development of a two-dimensional geometrical model in the coronal plane. Proc Inst Mech Eng H. 2000; 214(4): Bernstein AD, Jazrawi LM, Rokito AS, Zuckerman JD. Elbow joint biomechanics: basic science and clinical applications. Orthopedics. 2000; 23(12): Goldberg SH, Urban RM, Jacobs JJ, King GJ, O Driscoll SW, Cohen MS. Modes of wear after semiconstrained total elbow arthroplasty. J Bone Joint Surg Am. 2008; 90(3): Goldberg VM, Figgie HE III, Inglis AE, Figgie MP. Total elbow arthroplasty. J Bone Joint Surg Am. 1988; 70(5): Shiba R, Siu DW, Sorbie C, Bryant JT. Geometric analysis of the elbow joint. In: Orthopaedic Research Society; 1983; 8: Little CP, Graham AJ, Carr AJ. Total elbow arthroplasty: a systematic review of the literature in the English language until the end of J Bone Joint Surg Br. 2005; 87(4): Sorbie C, Shiba R, Siu D, Saunders G, Wevers H. The development of a surface arthroplasty for the elbow. Clin Orthop Relat Res. 1986; (208): Morrey BF, Adams RA. Semiconstrained arthroplasty for the treatment of rheumatoid arthritis of the elbow. J Bone Joint Surg Am. 1992; 74(4): Packer TL, Peat M, Wyss U, Sorbie C. Examining the elbow during functional activities. Am J Occup Ther. 1990; 10: SPSS (for Windows) [computer program]. Version Chicago, IL; Harrison D, Chaychowski TA. A prosthesis to replace the human elbow joint. Queen s University Project Report. Mech. 1980; Wevers HW, Siu DW, Broekhoven LH, Sorbie C. Resurfacing elbow prosthesis: shape and sizing of the humeral component. J Biomed Eng. 1985; 7(3): Kocher T, Stiles HJ, Paul CB, trans. Textbook of Operative Surgery. 3rd ed. London: Adam & Charles Black; Ikävalko M, Tiihonen R, Skyttä ET, Belt EA. Long-term survival of the Souter-Strathclyde total elbow replacement in patients with rheumatoid arthritis. J Bone Joint Surg Br. 2010; 92(5): Prasad N, Dent C. Outcome of total elbow replacement for rheumatoid arthritis: single surgeon s series with Souter-Strathclyde and Coonrad-Morrey prosthesis [published online ahead of print January 13, 2010]. J Shoulder Elbow Surg. 2010; 19(3): Qureshi F, Draviaraj KP, Stanley D. The Kudo 5 total elbow replacement in the treatment of the rheumatoid elbow: results at a minimum of ten years. J Bone Joint Surg Br. 2010; 92(10): Throckmorton T, Zarkadas P, Sanchez-Sotelo J, Morrey B. Failure patterns after linked semiconstrained total elbow arthroplasty for posttraumatic arthritis. J Bone Joint Surg Am. 2010; 92(6): Marshall Brooks M, Tobase P, Karp S, Francis D, Fogarty PF. Outcomes in total elbow arthroplasty in patients with haemophilia at the University of California, San Francisco: a retrospective review. Haemophilia. 2011; 17(1): Krenek L, Farng E, Zingmond D, SooHoo NF. Complication and revision rates following total elbow arthroplasty. J Hand Surg Am. 2011; 36(1): Cheung EV, Adams RA, Morrey BF. Reimplantation of a total elbow prosthesis following resection arthroplasty for infection. J Bone Joint Surg Am. 2008; 90(3): Brinkman JM, de Vos MJ, Eygendaal D. Failure mechanisms in uncemented Kudo type 5 elbow prosthesis in patients with rheumatoid arthritis: 7 of 49 ulnar components revised because of loosening after 2-10 years. Acta Orthop. 2007; 78(2): Thillemann TM, Olsen BS, Johannsen HV, Sojbjerg JO. Long-term results with the Kudo type 3 total elbow arthroplasty. J Shoulder Elbow Surg. 2006; 15(4): Rispoli DM, Athwal GS, Morrey BF. Neurolysis of the ulnar nerve for neuropathy following total ebow replacement. J Bone Joint Surg Br. 2008; 90(20): Little CP, Graham AJ, Karatzas G, Woods DA, Carr AJ. Outcomes of total elbow arthroplasty for rheumatoid arthritis: comparative study of three implants. J Bone Joint Surg Am. 2005; 87(11): Patil N, Cheung EV, Mow CS. High revision rate after total elbow arthroplasty with a linked semiconstrained device. Orthopedics. 2009; 32(5): Inagaki K, O Driscoll SW, Morrey BF, et al. Kinematics of the Sorbie-QUESTOR total elbow arthroplasty. In: Orthopaedic Research Society (abs); February,1-4, 1999; Ahaheim, CA. 32. Inagaki K, O Driscoll SW, Neale PC, Uchiyama E, Morrey BF, An KN. Importance of a radial head component in the Sorbie unlinked total elbow arthroplasty. Clin Orthop Relat Res. 2002; (400): Gramstad GD, King GJ, O Driscoll SW, Yamaguchi K. Elbow arthroplasty using a convertible implant. Tech Hand Up Extrem Surg. 2005; 9(3): Kamineni S, O Driscoll SW, Urban M, et al. Intrinsic constraint of unlinked total elbow replacements--the ulnotrochlear joint. J Bone Joint Surg Am. 2005; 87(9): Guerroudj JM, de Longueville JC, Rooze M, Hinsenkamp M, Feipel V, Schuind F. Biomechanical properties of triceps brachii tendon after in vitro simulation of different posterior surgical approaches. J Shoulder Elbow Surg. 2007; 16(6): e569
Total Elbow Arthroplasty and Rehabilitation
 Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
Total Elbow Arthroplasty and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: There are three bones and four joint articulations that have a high degree of congruence in
How To Perform An Elbow Operation
 Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Elbow Arthroplasty
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Indications... 3 7.2 Types of
THE ARTHROPLASTICAL POSSIBILITIES OF ELBOW JOINT IN RHEUMATOID ARTHRITIS. Miklós Farkasházi M.D.
 Abstract of the Ph.D. Thesis THE ARTHROPLASTICAL POSSIBILITIES OF ELBOW JOINT IN RHEUMATOID ARTHRITIS by Miklós Farkasházi M.D. Doctoral School of Semmelweis University Faculty of Physical Education and
Abstract of the Ph.D. Thesis THE ARTHROPLASTICAL POSSIBILITIES OF ELBOW JOINT IN RHEUMATOID ARTHRITIS by Miklós Farkasházi M.D. Doctoral School of Semmelweis University Faculty of Physical Education and
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Semi-constrained total elbow arthroplasty for the treatment of rheumatoid arthritis of the elbow
 O r i g i n a l A r t i c l e Singapore Med J 2005; 46(12) : 718 Semi-constrained total elbow arthroplasty for the treatment of rheumatoid arthritis of the elbow K T Lee, S Singh, C H Lai ABSTRACT Introduction:
O r i g i n a l A r t i c l e Singapore Med J 2005; 46(12) : 718 Semi-constrained total elbow arthroplasty for the treatment of rheumatoid arthritis of the elbow K T Lee, S Singh, C H Lai ABSTRACT Introduction:
Elbow Examination. Haroon Majeed
 Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Valgus deformity and proximal subluxation of the rheumatoid elbow: a radiographic 15 year follow up study of 148 elbows
 Ann Rheum Dis 2001;60:765 769 765 Valgus deformity and proximal subluxation of the rheumatoid elbow: a radiographic 15 year follow up study of 148 elbows J T Lehtinen, K Kaarela, M J Kauppi, E A Belt,
Ann Rheum Dis 2001;60:765 769 765 Valgus deformity and proximal subluxation of the rheumatoid elbow: a radiographic 15 year follow up study of 148 elbows J T Lehtinen, K Kaarela, M J Kauppi, E A Belt,
Radial Head Fracture Repair and Rehabilitation
 1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
The most common complaint associated with elbow. Elbow Arthritis. Michael G. Soojian, M.D., and Young W. Kwon, M.D., Ph.D. Anatomy
 61 Elbow Arthritis Michael G. Soojian, M.D., and Young W. Kwon, M.D., Ph.D. Abstract Patients with elbow arthritis typically present with complaints of pain and stiffness. Rheumatoid arthritis is the most
61 Elbow Arthritis Michael G. Soojian, M.D., and Young W. Kwon, M.D., Ph.D. Abstract Patients with elbow arthritis typically present with complaints of pain and stiffness. Rheumatoid arthritis is the most
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Total Hip Joint Replacement. A Patient s Guide
 Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
ELBOW REPLACEMENT SURGERY (ARTHROPLASTY)
 Protocol: ORT014 Effective Date: August 1, 2015 ELBOW REPLACEMENT SURGERY (ARTHROPLASTY) Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 U.S. FOOD AND DRUG ADMINISTRATION
Protocol: ORT014 Effective Date: August 1, 2015 ELBOW REPLACEMENT SURGERY (ARTHROPLASTY) Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 U.S. FOOD AND DRUG ADMINISTRATION
Rheumatoid arthritis of the elbow
 Ann. rheum. Dis. (1975), 34, 403 Rheumatoid arthritis of the elbow Pattern of joint involvement, and results of synovectomy with excision of the radial head H. STEIN, R. A. DICKSON, AND G. BENTLEY From
Ann. rheum. Dis. (1975), 34, 403 Rheumatoid arthritis of the elbow Pattern of joint involvement, and results of synovectomy with excision of the radial head H. STEIN, R. A. DICKSON, AND G. BENTLEY From
Arthroscopy of the Hand and Wrist
 Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
Arthroscopy of the Hand and Wrist Arthroscopy is a minimally invasive procedure whereby a small camera is inserted through small incisions of a few millimeters each around a joint to view the joint directly.
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
High-Flex Solutions for the MIS Era. Zimmer Unicompartmental High Flex Knee System
 High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014
 THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014 ELBOW FUNCTION 1. Required to provide stability for power and precision tasks for both open and closed kinetic chain
THE THERAPIST S MANAGEMENT OF THE STIFF ELBOW MARK PISCHKE, OTR/L, CHT NOV, 17, 2014 ELBOW FUNCTION 1. Required to provide stability for power and precision tasks for both open and closed kinetic chain
Arthroscopic Shoulder Procedures. David C. Neuschwander MD. Shoulder Instability. Allegheny Health Network Orthopedic Associates of Pittsburgh
 Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
.org. Distal Radius Fracture (Broken Wrist) Description. Cause
 Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S?
 Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S? Clarification of Terms The elbow includes: 3 bones (humerus, radius, and ulna) 2 joints (humeroulnar and humeroradial)
Elbow & Forearm H O W V I T A L I S T H E E L B O W T O O U R D A I L Y L I V E S? Clarification of Terms The elbow includes: 3 bones (humerus, radius, and ulna) 2 joints (humeroulnar and humeroradial)
.org. Tennis Elbow (Lateral Epicondylitis) Anatomy. Cause
 Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Position Statement: The Use of Total Ankle Replacement for the Treatment of Arthritic Conditions of the Ankle
 Position Statement: The Use of Total Ankle Replacement for the Treatment of Arthritic Conditions of the Ankle Position Statement The (AOFAS) endorses the use of total ankle replacement surgery for treatment
Position Statement: The Use of Total Ankle Replacement for the Treatment of Arthritic Conditions of the Ankle Position Statement The (AOFAS) endorses the use of total ankle replacement surgery for treatment
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Joint Replacement A guide for patients
 Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Why an Exactech Hip is Right for You
 Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
National Joint Replacement Registry. Demographics and Outcome of Elbow & Wrist Arthroplasty
 National Joint Replacement Registry Demographics and Outcome of Elbow & Wrist Arthroplasty SUPPLEMENTARY REPORT 2015 CONTENTS INTRODUCTION... 1 ELBOW REPLACEMENT... 2 Categories of Elbow Replacement...
National Joint Replacement Registry Demographics and Outcome of Elbow & Wrist Arthroplasty SUPPLEMENTARY REPORT 2015 CONTENTS INTRODUCTION... 1 ELBOW REPLACEMENT... 2 Categories of Elbow Replacement...
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT
 1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
1 FEMORAL NECK FRACTURE FOLLOWING TOTAL KNEE REPLACEMENT László Sólyom ( ), András Vajda & József Lakatos Orthopaedic Department, Semmelweis University, Medical Faculty, Budapest, Hungary Correspondence:
Total Elbow Arthroplasty as Primary Treatment for Distal Humeral Fractures in Elderly Patients*
 Copyright 199 by The Journal of Bone and Joint Surgery, Incorporated Total Elbow Arthroplasty as Primary Treatment for Distal Humeral Fractures in Elderly Patients* BY TYSON K. COBB, M.D.f, AND BERNARD
Copyright 199 by The Journal of Bone and Joint Surgery, Incorporated Total Elbow Arthroplasty as Primary Treatment for Distal Humeral Fractures in Elderly Patients* BY TYSON K. COBB, M.D.f, AND BERNARD
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Integra. MCP Joint Replacement PATIENT INFORMATION
 Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
LONG-TERM EFFECTS OF EXCISION OF THE RADIAL HEAD IN RHEUMATOID ARTHRITIS
 LONG-TERM EFFECTS OF EXCISION OF THE RADIAL HEAD IN RHEUMATOID ARTHRITIS L. A. RYMASZEWSKI, I. MACKAY, A. A. AMIS. J. H. MILLER From the Accident and Orthopaedic Department, Glasgow Royal Infirmary The
LONG-TERM EFFECTS OF EXCISION OF THE RADIAL HEAD IN RHEUMATOID ARTHRITIS L. A. RYMASZEWSKI, I. MACKAY, A. A. AMIS. J. H. MILLER From the Accident and Orthopaedic Department, Glasgow Royal Infirmary The
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Copeland Surface Replacement Arthroplasty (Hannan Mullett)
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Mini Medical School _ Focus on Orthopaedics
 from The Cleveland Clinic Mini Medical School _ Focus on Orthopaedics Arthritis of the Shoulder: Treatment Options Joseph P. Iannotti MD, PhD Professor and Chairman, Department of Orthopaedic Surgery The
from The Cleveland Clinic Mini Medical School _ Focus on Orthopaedics Arthritis of the Shoulder: Treatment Options Joseph P. Iannotti MD, PhD Professor and Chairman, Department of Orthopaedic Surgery The
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Rotator Cuff Repair
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
The Coonrad-Morrey Total Elbow Arthroplasty in Patients Who Have Rheumatoid Arthritis
 Copyright 1998 by The Journal of Bone and Joint Surgery, Incorporated The Coonrad-Morrey Total Elbow Arthroplasty in Patients Who Have Rheumatoid Arthritis A TEN TO FIFTEEN-YEAR FOLLOW-UP STUDY* BY DAVID
Copyright 1998 by The Journal of Bone and Joint Surgery, Incorporated The Coonrad-Morrey Total Elbow Arthroplasty in Patients Who Have Rheumatoid Arthritis A TEN TO FIFTEEN-YEAR FOLLOW-UP STUDY* BY DAVID
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Get Rid of Elbow Pain
 Get Rid of Elbow Pain Self Regional Healthcare Optimum Life Center 115 Academy Avenue Greenwood, SC 29646 Office: (864) 725-7088 Self Regional Healthcare Physical Therapy Savannah Lakes 207 Holiday Road
Get Rid of Elbow Pain Self Regional Healthcare Optimum Life Center 115 Academy Avenue Greenwood, SC 29646 Office: (864) 725-7088 Self Regional Healthcare Physical Therapy Savannah Lakes 207 Holiday Road
Robotic-Arm Assisted Surgery
 Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
J F de Beer, K van Rooyen, D Bhatia. Rotator Cuff Tears
 1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
1 J F de Beer, K van Rooyen, D Bhatia Rotator Cuff Tears Anatomy The shoulder consists of a ball (humeral head) and a socket (glenoid). The muscles around the shoulder act to elevate the arm. The large
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma. Magee, 2008. pg.
 PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
Shoulder Pain and Weakness
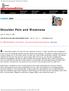 Shoulder Pain and Weakness John D. Kelly IV, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 11 - NOVEMBER 2004 For CME accreditation information, instructions and learning objectives, click here. A
Shoulder Pain and Weakness John D. Kelly IV, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 11 - NOVEMBER 2004 For CME accreditation information, instructions and learning objectives, click here. A
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Treatment Guide Understanding Elbow Pain. Using this Guide. Choosing Your Care. Table of Contents:
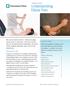 Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Total Shoulder Arthroplasty
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Exeter. Surgical Technique. V40 Stem Cement-in-Cement. Orthopaedics
 Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Systemic condition affecting synovial tissue Hypertrohied synovium destroys. Synovectomy. Tenosynovectomy Tendon Surgery Arthroplasty Arthrodesis
 Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
Surgical Options for Rheumatoid Arthritis of the Wrist Raj Bhatia Consultant Hand & Orthopaedic Surgeon Bristol Royal Infirmary & Avon Orthopaedic Centre Rheumatoid Arthritis Systemic condition affecting
LIST OF PUBLICATIONS
 LIST OF PUBLICATIONS List of publications 166 List of publications Papers van der Lugt JC, Valstar ER, Witvoet-Braam SW, Nelissen, RG. Migration of the humeral component of the Souter-Strathclyde elbow
LIST OF PUBLICATIONS List of publications 166 List of publications Papers van der Lugt JC, Valstar ER, Witvoet-Braam SW, Nelissen, RG. Migration of the humeral component of the Souter-Strathclyde elbow
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM
 INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Wrist Fusion and Back to Work
 Wrist Fusion and Back to Work Marc J. Richard, M.D. Associate Professor Department of Orthopaedic Surgery Durham, North Carolina 42 yo Ironworker, Failed Scope Debridement FUSION ARTHROPLASTY FUSION ARTHROPLASTY
Wrist Fusion and Back to Work Marc J. Richard, M.D. Associate Professor Department of Orthopaedic Surgery Durham, North Carolina 42 yo Ironworker, Failed Scope Debridement FUSION ARTHROPLASTY FUSION ARTHROPLASTY
Elbow arthroplasty: design, indications and results
 UPDATES IN ORTHOPEDICS Elbow arthroplasty: design, indications and results S. Antuña a,b y V. Vallina a a Orthopaedic Surgery Service. Hospital Valle del Nalón. Principado de Asturias, Spain. b Departament
UPDATES IN ORTHOPEDICS Elbow arthroplasty: design, indications and results S. Antuña a,b y V. Vallina a a Orthopaedic Surgery Service. Hospital Valle del Nalón. Principado de Asturias, Spain. b Departament
frequently asked questions Knee and Hip Joint Replacement Technology
 frequently asked questions Knee and Hip Joint Replacement Technology frequently asked questions Knee and Hip Joint Replacement Technology Recently, you may have seen advertisements from legal companies
frequently asked questions Knee and Hip Joint Replacement Technology frequently asked questions Knee and Hip Joint Replacement Technology Recently, you may have seen advertisements from legal companies
Ankle Arthritis Treatment in Worker Compensation The New Gold Standard ~ Total Ankle Replacement
 Ankle Arthritis Treatment in Worker Compensation The New Gold Standard ~ Total Ankle Replacement Aprajita Nakra, DPM, FACFAS Board Certified, Reconstructive Foot & Ankle Surgery Past President, Arizona
Ankle Arthritis Treatment in Worker Compensation The New Gold Standard ~ Total Ankle Replacement Aprajita Nakra, DPM, FACFAS Board Certified, Reconstructive Foot & Ankle Surgery Past President, Arizona
International Standards for the Classification of Spinal Cord Injury Motor Exam Guide
 C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
Elbow & Forearm. Notes. Notes. Lecture Slides - A.D.A.M. Lab Pics. Bones & Joints: Elbow & Forearm
 Elbow & Forearm Elbow & Forearm Notes Lecture Slides - A.D.A.M. Lab Pics Notes Bones & Joints: The elbow joint is a combination of joints but common reference is usually to the articulation of the distal
Elbow & Forearm Elbow & Forearm Notes Lecture Slides - A.D.A.M. Lab Pics Notes Bones & Joints: The elbow joint is a combination of joints but common reference is usually to the articulation of the distal
METAL HEMI. Great Toe Implant SURGICAL TECHNIQUE
 METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
Scaphoid Fracture of the Wrist
 Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Clinical performance of endoprosthetic and total hip replacement systems
 Veterans Administration Journal of Rehabilitation Research and Development Vol. 24 No. 3 Pages 49 56 Clinical performance of endoprosthetic and total hip replacement systems P. M. SANDBORN, B.S. ; S. D.
Veterans Administration Journal of Rehabilitation Research and Development Vol. 24 No. 3 Pages 49 56 Clinical performance of endoprosthetic and total hip replacement systems P. M. SANDBORN, B.S. ; S. D.
.org. Shoulder Joint Replacement. Anatomy
 Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Biceps Tenodesis Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Titanium Wire with Barb and Needle. For canthal tendon procedures.
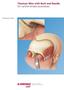 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Musculoskeletal Ultrasound Technical Guidelines. II. Elbow
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines II. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines II. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
Subspecialty: Shoulder and Elbow
 Complications of Total Elbow Arthroplasty Subspecialty: Shoulder and Elbow x Jaehon M. Kim MD, xxx Chaitanya S. Mudgal MD, MS (Orth.) MCh (Orth.), xx Joseph Konopka BA MSc, xxx Jesse B. Jupiter MD x Harvard
Complications of Total Elbow Arthroplasty Subspecialty: Shoulder and Elbow x Jaehon M. Kim MD, xxx Chaitanya S. Mudgal MD, MS (Orth.) MCh (Orth.), xx Joseph Konopka BA MSc, xxx Jesse B. Jupiter MD x Harvard
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329
 ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329 Consultant Orthopaedic Surgeon London Bridge Hospital Medico-Legal Secretary:
ASSOCIATE PROFESSOR BO POVLSEN Emeritus Consultant Orthopaedic Surgeon Guy s & St Thomas Hospitals NHS Trust GMC no. 3579329 Consultant Orthopaedic Surgeon London Bridge Hospital Medico-Legal Secretary:
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Total elbow arthroplasty in rheumatoid arthritis
 472 Acta Orthopaedica 2009; 80 (4): 472 477 Total elbow arthroplasty in rheumatoid arthritis A population-based study from the Finnish Arthroplasty Register Eerik T Skyttä 1,2, Antti Eskelinen 1,2, Pekka
472 Acta Orthopaedica 2009; 80 (4): 472 477 Total elbow arthroplasty in rheumatoid arthritis A population-based study from the Finnish Arthroplasty Register Eerik T Skyttä 1,2, Antti Eskelinen 1,2, Pekka
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
