Clinical Practice Guideline on the Management of Depression in Adults
|
|
|
- Patricia Bell
- 8 years ago
- Views:
Transcription
1 Clinical Practice Guideline on the Management of Depression in Adults CLINICAL PRACTICE GUIDELINES IN THE SPANISH NHS MINISTRY OF HEALTH, SOCIAL SERVICES AND EQUALITY
2
3 Clinical Practice Guideline on the Management of Depression in Adults CLINICAL PRACTICE GUIDELINES IN THE SPANISH NHS MINISTRY OF HEALTH, SOCIAL SERVICES AND EQUALITY MINISTERIO DE ECONOMÍA Y COMPETITIVIDAD MINISTERIO DE SANIDAD, SERVICIOS SOCIALES E IGUALDAD
4 This CPG is an aid to decision-making in health care. It is not mandatory to comply with it, nor does it replace the clinical judgment of medical staff. Edition: 2014 Edited by: Galician Agency for Health Technology Assessment, avalia-t, Ministry of Health; Ministry of Health, Social Services and Equality. NIPO MSSSI: Copyright: pending Layout: Tórculo Comunicación Gráfica, SA
5 This CPG has been financed through the collaboration agreement signed by the Carlos III Health Institute, an autonomous body of the Ministry of Economy and Competitiveness, and the Profesor Novoa Santos Foundation, within the activities of the Spanish Network of Technology and Services Evaluation Agencies for the SNS, financed by the Ministry of Health, Social Services and Equality. This guideline was prepared by: Working Group of the Clinical Practice Guideline on the Management of Depression in Adults. Clinical Practice Guideline on the Management of Depression in Adults. Ministry of Health, Social Services and Equality. Galician Agency for Health Technology Assessment (avalia-t); SNS Clinical Practice Guidelines: Avalia-t 2013/06. MINISTERIO DE ECONOMÍA Y COMPETITIVIDAD MINISTERIO DE SANIDAD, SERVICIOS SOCIALES E IGUALDAD
6
7 Table of contents Presentation 9 Authorship and Collaborations 11 Questions to be answered 15 SIGN Levels of evidence and grades of recommendation 17 CPG Recommendations Introduction Scope and objectives Methodology Definition, Risk factor and Diagnosis Definition risk Factors Suicide Risk Diagnosis Diagnostic Criteria Differential Diagnosis Perspectives and experiences of patients with depression and of their relatives Evaluation and screening for depression Evaluation of depression Assessment instruments Depression Screening Treatment Depression care models and general management principles The stepped-care model Collaborative care Psychotherapeutic treatment Cognitive-behavioural therapies Behavioural activation Problem-solving therapy Couples therapy Interpersonal therapy Counselling Short-term psychodynamic psychotherapy Other psychotherapeutic interventions 76 Clinical Practice Guideline on the Management of Depression in Adults 5
8 7.3. Pharmacotherapy Adverse effects and interactions profile Safety and efficacy of antidepressant drugs Treatment dose and duration to prevent relapse Strategies for resistant depression Psychotherapeutic strategies in resistant depression Pharmacological strategies in resistant depression Increasing dose Switching to another antidepressant Combining an antidepressant with another antidepressant Augmenting an antidepressant with antipsychotics Augmenting an antidepressant with lithium Augmenting an antidepressant with anticonvulsants Augmenting an antidepressant with triiodothyronine Augmenting an antidepressant with pindolol Augmenting an antidepressant with zinc Augmenting an antidepressant with benzodiazepines Electroconvulsive therapy Vagus nerve stimulation as adjunctive treatment for resistant depression Transcranial magnetic stimulation as adjunctive treatment for resistant depression Transcranial magnetic stimulation in the treatment of depression Transcranial magnetic stimulation in treatment-resistant depression Comparison of transcranial magnetic stimulation with electroconvulsive therapy Other treatments Exercise John s Wort Diagnostic and therapeutic strategies Quality indicators CLINICAL PRACTICE GUIDELINES IN THE SNS
9 12. Diffusion and implementation Diffusion and dissemination Implementation of the CPG through integration into the electronic medical record Benefits of Clinical Decision Support Systems in depression Selection of content or recommendations to integrate into the information system National and international experiences in implementing depression guidelines via CDSS Future research lines 169 Annexes 173 Annex 1. Criteria for severity/progress specifiers according to DSM Annex 2. Validated Spanish versions of the HRSD, MADRS and PHQ-9 scale 176 Annex 3. Main antidepressant drugs: pack size and cost 181 Annex 4: Depression: information for patients, family and friends 183 Annex 5. Abbreviations 203 Annex 6. Glossary 204 Annex 7. Declaration of interest 210 Bibliography 211 Clinical Practice Guideline on the Management of Depression in Adults 7
10
11 Presentation Depression in adults is a major health problem because of its prevalence, its impact on both the quality of life of patients and the structure of their relatives and society and its role as one of the major risk factors for suicide. Therefore, depression is considered of great importance not only for the health system, but also for society. However, under-diagnosis and lack of treatment are still a challenge in the management of depression, with a significant percentage of patients not seeking medical attention for their symptoms of depression. Conversely, overdiagnosis and overtreatment of this disorder is also beginning to be mentioned. In addition to the foregoing, there is known the existence of variability in its clinical management, with different approaches to treatment, referral and follow-up and a high percentage of patients responding inadequately to therapeutic strategies or with a tendency to relapse. In 2008, the first version of the Clinical Practice Guideline on the Management of Depression in Adults was published, as part of the SNS Guidelines Programme. The length of time elapsed since then and the availability of new evidence have required an update to be prepared. This new CPG was developed by a multidisciplinary group of professionals from different areas responsible for caring for patients with depression, and the review process has received the cooperation of various scientific societies and associations directly involved with this health problem. This guideline is a result of this work and aims to be a useful tool with answers to the most important issues in the form of systematically developed recommendations using the best available evidence. In addition to the incorporation and integration of new evidence on diagnostic and therapeutic strategies, among the challenges included in this new version is the incorporation of the perspective of patients and relatives through a systematic review and a qualitative study. This approach allowed us to observe the impact of depression, understand it from a humanistic view and identify areas for improvement in the care process. Other notable contributions in relation to the previous guideline are the stepped care model approach and collaboration between primary and specialist care, which is critical for improving care for such a complex disorder as depression, based on current evidence. Finally, a section on the implementation of depression management recommendations in the electronic medical record has been included. From the Directorate General for Public Health, Quality and Innovation, we would like to thank the authors for all their hard work and hope that this guide will contribute to a higher quality of care for patients with depression and their relatives. M. MERCEDES VINUESA SEBASTIÁN General Director of Public Health, Quality and Innovation Clinical Practice Guideline on the Management of Depression in Adults 9
12
13 Authorship and Collaborations Working Group of the Clinical Practice Guideline on the Management of Depression in Adults María Álvarez Ariza, Doctor of Medicine, Psychiatry Specialist, Vigo University Hospital, Pontevedra. Gerardo Atienza Merino, Doctor of Medicine, Technical Consultant, Galicia Health Technology Assessment Agency, Department of Health, Government of Galicia. María José González Ávila, Degree in Medicine, Psychiatry Specialist, La Coruña University Hospital. Amparo González García, Mental Health Specialist Nurse, Ourense University Hospital. Delia Guitián Rodríguez, Degree in Psychology, Clinical Psychology Specialist, Lucus Augusti University Hospital, Lugo. Elena de las Heras Liñero, Doctor of Medicine, Psychiatry Specialist, Vigo University Hospital, Pontevedra. Arturo Louro González, Degree in Medicine, Family and Community Medicine Specialist, Cambre Primary Health Centre,, La Coruña. Jose Luis Rodríguez-Arias Palomo, Doctor of Psychology, Clinical Psychology Specialist, La Coruña University Hospital. Yolanda Triñanes Pego, Degree in Psychology, Technical Consultant, Galicia Health Technology Assessment Agency, Department of Health, Government of Galicia. Clinical Coordination Elena de las Heras Liñero, Doctor of Medicine, Psychiatry Specialist, Vigo University Hospital, Pontevedra. Methodical Coordination Gerardo Atienza Merino, Doctor of Medicine, Technical Consultant, Galicia Health Technology Assessment Agency, Department of Health, Government of Galicia. Collaboration Beatriz Casal Acción, Documentalist, Galicia Health Technology Assessment Agency, Department of Health, Government of Galicia. Clinical Practice Guideline on the Management of Depression in Adults 11
14 Expert Collaboration Manuel Castro Bouzas, Clinical Psychology Specialist, Ferrol Health District, La Coruña, for participation in the Psychotherapy Treatment section. Marlén Fernández Silva, Primary Care Pharmacist, O Ventorrillo Primary Health Centre, La Coruña, for her participation in the Drug Therapy section. Ernesto Ferrer Gómez del Valle, Psychiatry specialist, Ourense University Hospital, for participation in the Drug Therapy section. Diego Palao Vidal, Psychiatry specialist, Mental Health Executive Director, Taulí Park Health Corporation, Sabadell, for participation in the Electronic Health Record Integration section. Antonio Rial Boubeta, Professor at the Behavioural Sciences Methodology Department, Santiago de Compostela University, for participation in the qualitative study. External Review Enric Aragonés Benaiges, Specialist in Family and Community Medicine, Constantí Primary Care Centre, Tarragona, Catalonia Health Institute. José Angel Arbesu Prieto, Specialist in Family and Community Medicine, Mental Health Working Group Coordinator, representing SEMERGEN. Germán E. Berrios, Professor of Epistemology of Psychiatry (Emeritus), Life Fellow at Robinson College, Psychiatry Department, Cambridge University, United Kingdom. Rosendo Bugarín González, Specialist in Family and Community Medicine, Director of Outpatients and Emergency Department, Lugo, Cervo and Monforte de Lemos Health District, representing SEMERGEN. Carlos Calderón Gómez, Specialist in Family and Community Medicine, Alza Primary Health Centre, Osakidetza-Basque Health Service, REDICS-Investén, Carlos III Health Institute. Mª Consuelo Carballal Balsa, Mental Health Specialist Nurse, Naval Hospital, Ferrol, La Coruña, Vice President of ANESM. Francisco José Estupiñá Puig, Associate Professor, Faculty of Psychology, Complutense University, Madrid, representing SEPCyS. Juan L. Fernández Hierro, Psychiatry Specialist, Vigo University Hospital, Pontevedra representing SEPL. Aurora Gavino Lázaro, Associate Professor, Faculty of Psychology, Málaga University, representing SEPCyS. 12 CLINICAL PRACTICE GUIDELINES IN THE SNS
15 Marta González Pescador, Clinical Psychologist and President of the Spanish Association for Research and Development in Family Therapy. Guillermo Lahera Forteza, Assistant Professor, Faculty of Medicine, Alcalá University, Madrid, representing AEN. Raquel León Lamela, Degree in Psychology, Information and socio-family care, FEAFES-GALICIA. Germán López Cortacáns, Mental Health Specialist Nurse, Salou Primary Health Centre, Tarragona, representing FAECAP. Cristina Losada Pérez, Psychiatry Specialist, South London and Maudsley NHS Foundation Trust, London, United Kingdom. Antonio Madueño Caro, Specialist in Family and Community Medicine, La Laguna Primary Health Centre, Tenerife, representing SEMFYC. José Manuel Olivares Díez, Psychiatry Specialist, Vigo University Hospital, Pontevedra, representing SEP. Antonio Olives Alonso, Degree in Psychology, President of the Galicia Association for Family Therapy and Mediation. Manuel Portela Romero, Specialist in Family and Community Medicine, Padrón Primary Health Centre, La Coruña, representing SEMERGEN. Javier Sardiña Agra, Clinical Psychology Specialist, Oza Hospital, La Coruña. Carmen Senra Rivera, Professor, Department of Clinical Psychology and Psychobiology, Santiago de Compostela University, La Coruña. Manuel Serrano Vázquez, Psychiatry Specialist, Head of Psychiatry, La Coruña University Hospital, representing SEP. Mercé Teixido Casas, Psychiatry Specialist, Les Corts Mental Health Centre, Barcelona, representing AEN. Mikel Urretavizcaya Sarachaga, Psychiatry Specialist, Bellvitge University Hospital, Barcelona, representing SEPB. Fernando Lino Vázquez González, Professor, Department of Clinical Psychology and Psychobiology, Santiago de Compostela University, La Coruña. Acknowledgements Noemí Raña Villar, Galicia Health Technology Assessment Agency, for her administrative work and management. Isabel Pena Baliñas, for the illustrations in the section on Information for patients, family and friends. Pablo Alonso Coello, Iberoamerican Cochrane Centre, Hospital de la Santa Creu i Sant Pau, Barcelona, for his advice on the methodology of incorporation of qualitative studies. All patients and family members who participated in the qualitative study and external review of this guide. Clinical Practice Guideline on the Management of Depression in Adults 13
16 Collaborating Organisations Members of these organisations or associations participated in the external review: Spanish Association of Neuropsychiatry (AEN). Spanish Association for Clinical Psychology and Psychopathology (AEPCP). National Association of Mental Health Nursing (ANESM). Federation of Primary and Care Community Nursing Associations (FAECAP). Galicia Federation of Families and Persons with Mental Illness (Galicia FEAFES). Spanish Society of Psychiatric Epidemiology (SEEP). Spanish Society of Family and Community Medicine (SEMFYC). Spanish Society of Primary Care Physicians (SEMERGEN). Spanish Society for Family Therapy Research and Development (AEI + DTF). Spanish Society for the Advancement of Clinical Psychology and Health XXI Century (SEPCyS). Spanish Society of Psychiatry (SEP). Spanish Society of Biological Psychiatry (SEPB). Spanish Society of Legal Psychiatry (SEPL). Declaration of interest: All members of the working group, as well as those who have participated in the expert collaboration and external review, have made a declaration of interest which is presented in Annex CLINICAL PRACTICE GUIDELINES IN THE SNS
17 Questions to be answered PERSPECTIVES AND EXPERIENCES OF PATIENTS AND THEIR RELATIVES WITH DEPRESSION 1. What are the perspectives of patients and their relatives about depression and their experiences with the health care provided? EVALUATION AND SCREENING OF DEPRESSION 2. How should depression be evaluated? 3. Which scales have the best psychometric properties for the evaluation of depression in adults? 4. Does screening improve health outcomes in depression? CARE MODELS 5. How effective are stepped and collaborative care models? PSYCHOTHERAPEUTIC TREATMENT 6. How effective are different psychological interventions in patients with depression? PHARMACOLOGICAL TREATMENT 7. What is the safety and efficacy of antidepressant drugs in the treatment of depressive episodes in adults? 8. How long and at what dose should drug treatment be maintained after remission of depressive symptoms? PSYCHOTHERAPEUTIC STRATEGIES IN RESISTANT DEPRESSION 9. What is the role of psychotherapy as an enhancement or alternative in patients with resistant depression? Clinical Practice Guideline on the Management of Depression in Adults 15
18 PHARMACOLOGICAL STRATEGIES IN RESISTANT DEPRESSION 10. What pharmacological strategies are most effective in patients with treatment-resistant depression? ELECTROCONVULSIVE THERAPY 11. What is the safety and efficacy of electroconvulsive therapy as a treatment for depression? VAGUS NERVE STIMULATION 12. What is the safety and efficacy of vagus nerve stimulation as adjunctive treatment for resistant depression? TRANSCRANIAL MAGNETIC STIMULATION 13. What is the safety and efficacy of transcranial magnetic stimulation as adjunctive treatment for resistant depression? EXERCISE 14. Is physical exercise effective in patients with depression? ST JOHN S WORT 15. What is the safety and efficacy of St. John s wort in the treatment of adult depression? QUALITY INDICATORS 16. What are the indicators for monitoring quality in the management of depression? IMPLEMENTATION 17. What is the progress and impact of clinical decision support and knowledge management systems on the management of depression? 16 CLINICAL PRACTICE GUIDELINES IN THE SNS
19 SIGN Levels of evidence and grades of recommendation Levels of evidence + High quality meta-analyses, systematic reviews of clinical trials or high-quality clinical trials with very low risk of bias. Well-conducted meta-analyses, systematic reviews of clinical trials, or well-conducted clinical trials with little risk of bias. 1- Meta-analyses, systematic reviews of clinical trials or clinical trials with high risk of bias. 2++ High quality systematic reviews of case control or cohort or studies. High quality case control or cohort studies with a very low risk of confounding or bias and a high probability that the relationship is causal. Well-conducted case control or cohort studies with a low risk of confounding or bias and a moderate probability that the relationship is causal. 2+ Cohort or case-control studies with a high risk of bias and a significant risk that the relationship 2- is not causal. 3 Non-analytical studies such as case reports and case series. 4 Expert opinion. Grades of recommendation At least one meta-analysis, systematic review or clinical trial rated as 1 ++ directly applicable to A the target population of the guide; or a body of evidence consisting of studies rated as 1 + and showing overall consistency of results. A body of evidence consisting of studies rated as 2 ++, directly applicable to the target population B of the guide and showing overall consistency of results; or evidence extrapolated from studies rated as 1 ++ or 1 +. A body of evidence consisting of studies rated as 2 + directly applicable to the target population C of the guide and showing overall consistency of results; or evidence extrapolated from studies rated as D Evidence level 3 or 4; or evidence extrapolated from studies rated as 2 +. Studies classified as 1 - and 2 - must not be used in the preparation of recommendations due to their high potential for bias. The recommendations adapted from a CPG are indicated with the superscript CPG. Q 1 Evidence taken from relevant qualitative studies of appropriate quality. This category is not considered by SIGN. Good clinical practice 2 Recommended practice based on clinical experience and consensus of the editorial team. Source: Scottish Intercollegiate Guidelines Network. Forming guideline recommendations. In: SIGN 50: A guideline developers handbook: Edinburgh: SIGN; Evaluating the quality of qualitative studies was performed following the CASP (Critical Appraisal Skills Programme) 2 checklist, as proposed by Goldsmith et al. (2007) Sometimes the development group wishes to highlight an important practical aspect for which there is probably no supporting evidence. In general, these cases are related to an aspect of treatment generally accepted to be good clinical practice, and are evaluated as a point of good clinical practice. These messages are not an alternative to the recommendations based on evidence, but should be considered only when there is no other way of highlighting that aspect. Clinical Practice Guideline on the Management of Depression in Adults 17
20
21 CPG Recommendations Evaluation of depression The clinical interview is the essential procedure for the diagnosis of depression. The ICD and DSM provide a set of agreed criteria to rely on. Due to the existence of different factors that may affect the progress, course and severity of depression, it is recommended to evaluate the following areas: Features of the episode: duration, number and intensity of symptoms, comorbidity. C Psychosocial assessment (social support and interpersonal relationships). Degree of associated dysfunction and/or disabilities. Risk of suicide. Response to previous treatment. It is recommended to assess the risk of suicide in patients with depression, considering the following factors: C Q Q Q Q Q Q Presence of previous suicide attempts, other comorbid mental disorders and substance abuse. Specific symptoms such as hopelessness, anxiety, agitation or suicidal ideation. Other risk factors such as physical illness, chronicity, pain or disability, family history of suicide, social factors and a history of suicide in the environment. When assessing depression, it is recommended to consider the heterogeneity of its presentation as well as the perception patients have about their symptoms and the disorder. It is recommended to pay special attention to issues that affect the daily lives of patients with depression which may have a greater functional impact. The assessment should consider the sociodemographic and cultural factors that may affect the development or maintenance of depressive symptoms and influence treatment, such as sex, family, social network and perceived stigma. The meaning and impact of depression on the patient's family and any needs that may arise should be explored; especially regarding children, adolescents and family dependent upon the depressed patient. It is recommended to encourage the communication of feelings and emotions in an empathetic and respectful environment. When a diagnosis of depression is made, all the necessary information about the disorder and treatment options, as well as explanations to reduce the guilt and stigma attached, must be promoted and provided. Clinical Practice Guideline on the Management of Depression in Adults 19
22 Evaluation instruments D The scales provide additional information in the evaluation, but cannot replace the clinical interview. Some of the scales that may be useful in assessing depression are the Hamilton Rating Scale for Depression (HRSD), the Montgomery Asberg Depression Rating Scale (MADRS), the Brief Patient Health Questionnaire (PHQ-9) and the Beck Depression Inventory (BDI). Depression screening B B B Routine screening for depression is not recommended for the general population, as there are reasonable doubts about its effectiveness. Clinicians should be alert to the possibility of depression, especially in patients with risk factors who also have symptoms such as insomnia, low mood, anhedonia and suicidal ideation. In primary care, when an indicator for depression is observed in a routine examination, it is recommended to use two questions about mood and loss of enjoyment to assess for the presence of depressive disorders. If the response is positive, an appropriate psychopathological assessment is recommended. Care models B The management of depression in adults should be performed as a stepped care and collaboration model between primary care and mental health, so that interventions and treatments are tailored to the status and evolution of the patient. General treatment recommendations D CPG Q Q D CPG The treatment of depression in adults should be comprehensive and cover all psychotherapeutic, psychosocial and pharmacological interventions which may improve well-being and functional capacity. The management of depression should include psychoeducation, individual and family support, coordination with other professionals, care of comorbidity and regular monitoring of mental and physical status. The initial selection of the mode and scope of treatment should be based on clinical findings and other factors, such as previous history, the availability of treatment, patient preference and the ability to provide support and containment in the environment. A structured patient monitoring plan should be established. The assessment and monitoring frequency of symptoms should be according to severity, comorbidity, cooperation with treatment, social support and the frequency and severity of side effects of the prescribed treatment. With the consent of the patients, both they and their relatives and relatives should take an active role in making decisions about the treatment and care plan development. Patients and their relatives should be offered support to develop coping strategies, and should be informed of the existence of patient associations and resources which can be of help. Verbal information should be backed up with written documents whenever possible. 20 CLINICAL PRACTICE GUIDELINES IN THE SNS
23 Psychotherapeutic treatment B B B C B The availability of psychotherapeutic treatment should be ensured for patients who need it. In mild-moderate depression, a brief psychological treatment (such as cognitive behavioural therapy or problem-solving therapy) of 6-8 sessions over weeks should be considered. The psychological treatment of choice for moderate to severe depression is cognitive behavioural therapy or interpersonal therapy, of sessions over 5 months. Cognitive behavioural therapy should be considered for patients with inadequate response to other interventions or a prior history of relapses and/or residual symptoms. Other psychological interventions should be considered when addressing comorbidity or the complexity of family or marital relationships, often associated with depression. Patients with chronic and/or recurrent depression are recommended a combination of drug therapy and cognitive behavioural therapy. Pharmacotherapy A A D CPG D A D CPG Before starting antidepressant treatment, patients must be adequately informed of the expected benefits, side effects and possible delay in the therapeutic effect. The initial selection of drug therapy should be based mainly on the side effect profile and tolerability, safety and pharmacological properties, as well as other factors such as previous response to treatment, cost and patient preferences. SSRIs are antidepressants with the most evidence and better risk/benefit ratio, and should be considered as the first choice of treatment. All patients with moderate depression treated with drugs should be re-assessed within 15 days of the treatment start, and within 8 days in the case of severe depression. Benzodiazepine treatment may be considered for patients with anxiety, insomnia and/ or agitation, although they should not be used for longer than 2-3 weeks to prevent the development of dependence. Patients undergoing drug therapy must be closely monitored, at least for the first 4 weeks. Antidepressant treatment should be maintained for at least 6 months after remission of the episode, and aspects such as previous episodes, comorbidity and the presence of other risk factors should be evaluated before deciding on withdrawal of treatment. It is recommended that maintenance treatment be performed with the same dose at which the response was achieved. To avoid withdrawal symptoms, the antidepressant treatment dose should be reduced gradually, usually over a period of 4 weeks; particularly for drugs with short half-lives like paroxetine or venlafaxine. Clinical Practice Guideline on the Management of Depression in Adults 21
24 D CPG Q If withdrawal symptoms occur, a diagnostic confirmation should be performed and, if the symptoms are significant, reintroducing the original antidepressant at effective doses should be considered (or the use of another antidepressant in the same class with a long half-life) and the dose gradually reduced. When drug treatment is prescribed, the patient's perception should be explored and a positive attitude will be favoured. In addition, adequate monitoring for side effects, as well as evolution of the symptoms and functional capacity, should be performed. Moreover, after obtaining patient authorisation, any doubts the family has about the treatment must be clarified to gain their support. Psychotherapeutic strategies in resistant depression B A combined therapy of cognitive behavioural therapy and antidepressant pharmacotherapy is recommended for patients with resistant depression. Pharmacological strategies in resistant depression The following is recommended for patients who do not improve with initial antidepressant treatment for depression: Review of diagnosis. Verify compliance with taking the appropriate dosage and treatment time. Assess the existence of disease awareness, motivation to change and possible comorbidity. The following is recommended for patients with a partial response after the 3rd or 4th week: Wait for clinical evolution until the 8th week. Increase the drug dose to the maximum therapeutic dose. If the patient does not respond by the 3rd or 4th week of treatment, any of the following strategies could be attempted: B C C C Change of antidepressant to another in the same or a different family. Combination of antidepressants. Enhancement with lithium or antipsychotics. When the strategy is changing the antidepressant, a different SSRI or another secondgeneration antidepressant should initially be evaluated. If there is no response, an antidepressant with greater side effects, such as a tricyclic or MAOI, could be assessed. The combination of SSRI and mianserin or mirtazapine may be a recommendable option, bearing in mind the possibility of adverse effects. Enhancement with lithium or antipsychotics, such as olanzapine, quetiapine, aripiprazole or risperidone may also be a strategy to consider, bearing in mind the possibility of greater adverse effects. 22 CLINICAL PRACTICE GUIDELINES IN THE SNS
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Clinical Practice Guideline for the Prevention and Treatment of Suicidal Behaviour
 Clinical Practice Guideline for the Prevention and Treatment of Suicidal Behaviour CLINICAL PRACTICE GUIDELINTES IN THE NHS MINISTRY OF HEALTH, SOCIAL SERVICES AND EQUALITY MINISTERIO DE SANIDAD, POLÍTICA
Clinical Practice Guideline for the Prevention and Treatment of Suicidal Behaviour CLINICAL PRACTICE GUIDELINTES IN THE NHS MINISTRY OF HEALTH, SOCIAL SERVICES AND EQUALITY MINISTERIO DE SANIDAD, POLÍTICA
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller
 Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
MOLINA HEALTHCARE OF CALIFORNIA
 MOLINA HEALTHCARE OF CALIFORNIA MAJOR DEPRESSION IN ADULTS IN PRIMARY CARE HEALTH CARE GUIDELINE (ICSI) Health Care Guideline Twelfth Edition May 2009. The guideline was reviewed and adopted by the Molina
MOLINA HEALTHCARE OF CALIFORNIA MAJOR DEPRESSION IN ADULTS IN PRIMARY CARE HEALTH CARE GUIDELINE (ICSI) Health Care Guideline Twelfth Edition May 2009. The guideline was reviewed and adopted by the Molina
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
Depre r s e sio i n o i n i a dults Yousuf Al Farsi
 Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
See also www.thiswayup.org.au/clinic for an online treatment course.
 Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
Depression What is depression? Depression is one of the common human emotional states. It is common to experience feelings of sadness and tiredness in response to life events, such as losses or disappointments.
Authors and collaborations
 Authors and collaborations Guideline Development Group for the CPG on the Management of Major Depression in Childhood and Adolescence. María Álvarez Ariza. Doctor of Medicine. Specialist Physician in Psychiatry.
Authors and collaborations Guideline Development Group for the CPG on the Management of Major Depression in Childhood and Adolescence. María Álvarez Ariza. Doctor of Medicine. Specialist Physician in Psychiatry.
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Costing statement: Depression: the treatment and management of depression in adults. (update) and
 Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Costing statement: Depression: the treatment and management of depression in adults (update) and Depression in adults with a chronic physical health problem: treatment and management Summary It has not
Depression in Older Persons
 Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Clinical Practice Guideline on Major Depression in Childhood and Adolescence
 Clinical Practice Guideline on Major Depression in Childhood and Adolescence CLINICAL PRACTICE GUIDELINES IN THE SNS MINISTRY OF HEALTH AND SOCIAL POLICY Clinical Practice Guideline on Major Depression
Clinical Practice Guideline on Major Depression in Childhood and Adolescence CLINICAL PRACTICE GUIDELINES IN THE SNS MINISTRY OF HEALTH AND SOCIAL POLICY Clinical Practice Guideline on Major Depression
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Major Depressive Disorder (MDD) Guideline Diagnostic Nomenclature for Clinical Depressive Conditions
 Major Depressive Disorder Major Depressive Disorder (MDD) Guideline Diagnostic omenclature for Clinical Depressive Conditions Conditions Diagnostic Criteria Duration Major Depression 5 of the following
Major Depressive Disorder Major Depressive Disorder (MDD) Guideline Diagnostic omenclature for Clinical Depressive Conditions Conditions Diagnostic Criteria Duration Major Depression 5 of the following
Depression Assessment & Treatment
 Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Depressive Symptoms? Administer depression screening tool: PSC Depression Assessment & Treatment Yes Positive screen Safety Screen (see Appendix): Administer every visit Neglect/Abuse? Thoughts of hurting
Major Depressive Disorders Questions submitted for consideration by workshop participants
 Major Depressive Disorders Questions submitted for consideration by workshop participants Prioritizing Comparative Effectiveness Research Questions: PCORI Stakeholder Workshops June 9, 2015 Patient-Centered
Major Depressive Disorders Questions submitted for consideration by workshop participants Prioritizing Comparative Effectiveness Research Questions: PCORI Stakeholder Workshops June 9, 2015 Patient-Centered
Major Depression. What is major depression?
 Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Table of Contents. Preface...xv. Part I: Introduction to Mental Health Disorders and Depression
 Table of Contents Visit www.healthreferenceseries.com to view A Contents Guide to the Health Reference Series, a listing of more than 16,000 topics and the volumes in which they are covered. Preface...xv
Table of Contents Visit www.healthreferenceseries.com to view A Contents Guide to the Health Reference Series, a listing of more than 16,000 topics and the volumes in which they are covered. Preface...xv
Post-traumatic stress disorder overview
 Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression
 Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Step 2: Recognised depression in adults persistent subthreshold depressive symptoms or mild to moderate depression A NICE pathway brings together all NICE guidance, quality standards and materials to support
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Mental Health Needs Assessment Personality Disorder Prevalence and models of care
 Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Mental Health Needs Assessment Personality Disorder Prevalence and models of care Introduction and definitions Personality disorders are a complex group of conditions identified through how an individual
Recognition and Treatment of Depression in Parkinson s Disease
 Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Recognition and Treatment of Depression in Parkinson s Disease Web Ross VA Pacific Islands Health Care System What is depression? Depression is a serious medical condition that affects a person s feelings,
Depression. The treatment and management of depression in adults. This is a partial update of NICE clinical guideline 23
 Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Eating Disorder Treatment Protocol
 Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Depression & Multiple Sclerosis
 Depression & Multiple Sclerosis Managing specific issues Aaron, diagnosed in 1995. The words depressed and depression are used so casually in everyday conversation that their meaning has become murky.
Depression & Multiple Sclerosis Managing specific issues Aaron, diagnosed in 1995. The words depressed and depression are used so casually in everyday conversation that their meaning has become murky.
Understanding. Depression. The Road to Feeling Better Helping Yourself. Your Treatment Options A Note for Family Members
 TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind.
 What is depression? More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind. 1,2 The difference between clinical depression
What is depression? More than just feelings of unhappiness, clinical or major depression is a mood disorder a medical illness that involves both the body and mind. 1,2 The difference between clinical depression
Assessment of depression in adults in primary care
 Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Assessment of depression in adults in primary care Adapted from: Identification of Common Mental Disorders and Management of Depression in Primary care. New Zealand Guidelines Group 1 The questions and
Professional Reference Series Depression and Anxiety, Volume 1. Depression and Anxiety Prevention for Older Adults
 Professional Reference Series Depression and Anxiety, Volume 1 Depression and Anxiety Prevention for Older Adults TA C M I S S I O N The mission of the Older Americans Substance Abuse and Mental Health
Professional Reference Series Depression and Anxiety, Volume 1 Depression and Anxiety Prevention for Older Adults TA C M I S S I O N The mission of the Older Americans Substance Abuse and Mental Health
TREATMENT-RESISTANT DEPRESSION AND ANXIETY
 University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
What are the best treatments?
 What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90
 Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
Depression in adults: recognition and management Clinical guideline Published: 28 October 2009 nice.org.uk/guidance/cg90 NICE 2009. All rights reserved. Last updated April 2016 Your responsibility The
POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm
 E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
E-Resource March, 2014 POST-TRAUMATIC STRESS DISORDER PTSD Diagnostic Criteria PTSD Detection and Diagnosis PC-PTSD Screen PCL-C Screen PTSD Treatment Treatment Algorithm Post-traumatic Stress Disorder
Depression, Mental Health and Native American Youth
 Depression, Mental Health and Native American Youth Aisha Mays, MD UCSF Department of Family And Community Medicine Native American Health Center Oakland, CA July 8, 2015 Presenter Disclosures No relationships
Depression, Mental Health and Native American Youth Aisha Mays, MD UCSF Department of Family And Community Medicine Native American Health Center Oakland, CA July 8, 2015 Presenter Disclosures No relationships
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing
 Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing Overview Depression is significantly higher among elderly adults receiving home healthcare, particularly among
Dr. Anna M. Acee, EdD, ANP-BC, PMHNP-BC Long Island University, Heilbrunn School of Nursing Overview Depression is significantly higher among elderly adults receiving home healthcare, particularly among
Managing depression after stroke. Presented by Maree Hackett
 Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
Managing depression after stroke Presented by Maree Hackett After stroke Physical changes We can see these Depression Emotionalism Anxiety Confusion Communication problems What is depression? Category
Borderline personality disorder
 Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
Borderline personality disorder Treatment and management Issued: January 2009 NICE clinical guideline 78 guidance.nice.org.uk/cg78 NICE 2009 Contents Introduction... 3 Person-centred care... 5 Key priorities
The Priory Group. What is obsessive-compulsive disorder?
 The Priory Group What is obsessive-compulsive disorder? by Dr David Veale Dr Veale is a Consultant Psychiatrist at the Priory Hospital North London and the coauthor of Overcoming Obsessive Compulsive Disorder
The Priory Group What is obsessive-compulsive disorder? by Dr David Veale Dr Veale is a Consultant Psychiatrist at the Priory Hospital North London and the coauthor of Overcoming Obsessive Compulsive Disorder
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
Depression in the Elderly: Recognition, Diagnosis, and Treatment
 Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Depression in the Elderly: Recognition, Diagnosis, and Treatment LOUIS A. CANCELLARO, PhD, MD, EFAC Psych Professor Emeritus and Interim Chair ETSU Department of Psychiatry & Behavioral Sciences Diagnosis
Depression Overview. Symptoms
 1 of 6 6/3/2014 10:15 AM Return to Web version Depression Overview What is depression? When doctors talk about depression, they mean the medical illness called major depression. Someone who has major depression
1 of 6 6/3/2014 10:15 AM Return to Web version Depression Overview What is depression? When doctors talk about depression, they mean the medical illness called major depression. Someone who has major depression
Depression and its Treatment in Older Adults. Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City
 Depression and its Treatment in Older Adults Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City What is Depression? Everyday use of the word Clinically significant depressive symptoms : more severe,
Depression and its Treatment in Older Adults Gregory A. Hinrichsen, Ph.D. Geropsychologist New York City What is Depression? Everyday use of the word Clinically significant depressive symptoms : more severe,
Depression Screening in Primary Care
 Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Our Vision Make Greater Cleveland a healthier place to live and a better place to do business. 2
Depression Screening in Primary Care Toni Johnson, MD Kristen Palcisco, BA, MSN, APRN MetroHealth System Our Vision Make Greater Cleveland a healthier place to live and a better place to do business. 2
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
Challenges to Detection and Management of PTSD in Primary Care
 Challenges to Detection and Management of PTSD in Primary Care Karen H. Seal, MD, MPH University of California, San Francisco San Francisco VA Medical Center General Internal Medicine Section PTSD is Prevalent
Challenges to Detection and Management of PTSD in Primary Care Karen H. Seal, MD, MPH University of California, San Francisco San Francisco VA Medical Center General Internal Medicine Section PTSD is Prevalent
Depression & Multiple Sclerosis. Managing Specific Issues
 Depression & Multiple Sclerosis Managing Specific Issues Feeling blue The words depressed and depression are used so casually in everyday conversation that their meaning has become murky. True depression
Depression & Multiple Sclerosis Managing Specific Issues Feeling blue The words depressed and depression are used so casually in everyday conversation that their meaning has become murky. True depression
GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS
 GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
GUIDELINES GUIDELINES FOR USE OF PSYCHOTHERAPEUTIC MEDICATIONS IN OLDER ADULTS Preamble The American Society of Consultant Pharmacists has developed these guidelines for use of psychotherapeutic medications
DSM-5 and its use by chemical dependency professionals
 + DSM-5 and its use by chemical dependency professionals Greg Bauer Executive Director Alpine Recovery Services Inc. President Chemical Dependency Professionals Washington State (CDPWS) NAADAC 2014 Annual
+ DSM-5 and its use by chemical dependency professionals Greg Bauer Executive Director Alpine Recovery Services Inc. President Chemical Dependency Professionals Washington State (CDPWS) NAADAC 2014 Annual
Recognizing and Treating Depression in Children and Adolescents.
 Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
Depression Flow Chart
 Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13
 Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13 Screening Tools and Interventions for Common Behavioral Health Disorders Depression Depression is a potentially life-threatening
Screening Tools and Interventions for Common Behavioral Health Disorders TXPEC-0772-13 Screening Tools and Interventions for Common Behavioral Health Disorders Depression Depression is a potentially life-threatening
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Depression: Facility Assessment Checklists
 Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
Depression: Facility Assessment Checklists A facility system assessment is a starting point for a quality improvement project. The checklists included in this booklet will be most useful if you take a
Symptoms of mania can include: 3
 Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Barriers to Healthcare Services for People with Mental Disorders. Cardiovascular disorders and diabetes in people with severe mental illness
 Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
Feeling Moody? Major Depressive. Disorder. Is it just a bad mood or is it a disorder? Mood Disorders. www.seclairer.com S Eclairer 724-468-3999
 Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
There are four groups of medications most likely to be used for depression: Antidepressants Antipsychotics Mood stabilisers Augmenting agents.
 What this fact sheet covers: Physical treatments (medication, ECT and TMS) Psychological treatments Self-help & alternative therapies Key points to remember Where to get more information. Introduction
What this fact sheet covers: Physical treatments (medication, ECT and TMS) Psychological treatments Self-help & alternative therapies Key points to remember Where to get more information. Introduction
Depression in children and young people. Identification and management in primary, community and secondary care
 NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
NICE guideline May 2005 Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Objectives: Perform thorough assessment, and design and implement care plans on 12 or more seriously mentally ill addicted persons.
 Addiction Psychiatry Program Site Specific Goals and Objectives Addiction Psychiatry (ADTU) Goal: By the end of the rotation fellow will acquire the knowledge, skills and attitudes required to recognize
Addiction Psychiatry Program Site Specific Goals and Objectives Addiction Psychiatry (ADTU) Goal: By the end of the rotation fellow will acquire the knowledge, skills and attitudes required to recognize
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
Mood Disorders. What Are Mood Disorders? Unipolar vs. Bipolar
 Mood Disorders What Are Mood Disorders? In mood disorders, disturbances of mood are intense and persistent enough to be clearly maladaptive Key moods involved are mania and depression Encompasses both
Mood Disorders What Are Mood Disorders? In mood disorders, disturbances of mood are intense and persistent enough to be clearly maladaptive Key moods involved are mania and depression Encompasses both
Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too.
 The Family Library DEPRESSION What is depression? Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too. Also called
The Family Library DEPRESSION What is depression? Depression is a medical illness that causes a persistent feeling of sadness and loss of interest. Depression can cause physical symptoms, too. Also called
Mental Health, Disability and Work: Inpatient Medical Rehabilitation
 Mental Health, Disability and Work: Inpatient Medical Rehabilitation Prof. Michael Linden Head of the Rehabilitation Center Seehof of the German Pension Fund and Director of the Department of Behavioral
Mental Health, Disability and Work: Inpatient Medical Rehabilitation Prof. Michael Linden Head of the Rehabilitation Center Seehof of the German Pension Fund and Director of the Department of Behavioral
Schizoaffective disorder
 Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Schizoaffective disorder Dr.Varunee Mekareeya,M.D.,FRCPsychT Schizoaffective disorder is a psychiatric disorder that affects about 0.5 to 0.8 percent of the population. It is characterized by disordered
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
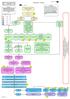 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
Alcohol Disorders in Older Adults: Common but Unrecognised. Amanda Quealy Chief Executive Officer The Hobart Clinic Association
 Alcohol Disorders in Older Adults: Common but Unrecognised Amanda Quealy Chief Executive Officer The Hobart Clinic Association The Hobart Clinic Association Not-for-profit private Mental Health Service
Alcohol Disorders in Older Adults: Common but Unrecognised Amanda Quealy Chief Executive Officer The Hobart Clinic Association The Hobart Clinic Association Not-for-profit private Mental Health Service
FACT SHEET 4. Bipolar Disorder. What Is Bipolar Disorder?
 FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Guidance on competencies for management of Cancer Pain in adults
 Guidance on competencies for management of Cancer Pain in adults Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine B: Competencies for practitioners in Pain Medicine
Guidance on competencies for management of Cancer Pain in adults Endorsed by: Contents Introduction A: Core competencies for practitioners in Pain Medicine B: Competencies for practitioners in Pain Medicine
Antidepressant Skills @ Work Dealing with Mood Problems in the Workplace
 Antidepressant Skills @ Work Dealing with Mood Problems in the Workplace Dr. Joti Samra PhD, R.Psych. Adjunct Professor & Research Scientist CARMHA www.carmha.ca Dr. Merv Gilbert PhD, R.Psych. Principal
Antidepressant Skills @ Work Dealing with Mood Problems in the Workplace Dr. Joti Samra PhD, R.Psych. Adjunct Professor & Research Scientist CARMHA www.carmha.ca Dr. Merv Gilbert PhD, R.Psych. Principal
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS
 CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
CARE MANAGEMENT FOR LATE LIFE DEPRESSION IN URBAN CHINESE PRIMARY CARE CLINICS Dept of Public Health Sciences February 6, 2015 Yeates Conwell, MD Dept of Psychiatry, University of Rochester Shulin Chen,
BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS
 BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Self-management strategies for mild to moderate depression
 Department of Epidemiology & Public Health Lunchtime seminar, 18 th Feb 2014 Self-management strategies for mild to moderate depression The internet-based ifightdepression tool Dr Celine Larkin National
Department of Epidemiology & Public Health Lunchtime seminar, 18 th Feb 2014 Self-management strategies for mild to moderate depression The internet-based ifightdepression tool Dr Celine Larkin National
CLINICAL PRACTICE GUIDELINES. Depression
 CLINICAL PRACTICE GUIDELINES Depression MOH Clinical Practice Guidelines 6/2011 3 1 Published by Ministry of Health, Singapore 16 College Road, College of Medicine Building Singapore 169854 Printed by
CLINICAL PRACTICE GUIDELINES Depression MOH Clinical Practice Guidelines 6/2011 3 1 Published by Ministry of Health, Singapore 16 College Road, College of Medicine Building Singapore 169854 Printed by
Asthma, anxiety & depression
 Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
When is psychological therapy warranted for patients with mental health problems?
 The Guidelines Advisory Committee (GAC) is empowered by the Ministry of Health and Long-Term Care and the Ontario Medical Association to promote evidence-based health care in Ontario, by encouraging physicians
The Guidelines Advisory Committee (GAC) is empowered by the Ministry of Health and Long-Term Care and the Ontario Medical Association to promote evidence-based health care in Ontario, by encouraging physicians
Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers
 SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
SUPPLEMENT 1: (Supplementary Material for online publication) Antipsychotic drug prescription for patients with dementia in long-term care. A practice guideline for physicians and caregivers About this
Depression Signs & Symptoms
 Depression Signs & Symptoms Contents What Is Depression? What Are The Signs And Symptoms Of Depression? How Do The Signs And Symptoms Of Depression Differ In Different Groups? What Are The Different Types
Depression Signs & Symptoms Contents What Is Depression? What Are The Signs And Symptoms Of Depression? How Do The Signs And Symptoms Of Depression Differ In Different Groups? What Are The Different Types
Depression in children and young people. Quick reference guide. Issue date: September 2005
 Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
Quick reference guide Issue date: September 2005 Depression in children and young people Identification and management in primary, community and secondary care Clinical Guideline 28 Developed by the National
DSM 5 SUBSTANCE USE DISORDERS. Ronald W. Kanwischer LCPC, CADC Professor Emeritus Department of Psychiatry SIU School of Medicine
 DSM 5 SUBSTANCE USE DISORDERS Ronald W. Kanwischer LCPC, CADC Professor Emeritus Department of Psychiatry SIU School of Medicine I have no financial relationships to disclose with regard to this presentation.
DSM 5 SUBSTANCE USE DISORDERS Ronald W. Kanwischer LCPC, CADC Professor Emeritus Department of Psychiatry SIU School of Medicine I have no financial relationships to disclose with regard to this presentation.
D. Clinical indicators for psychiatric evaluation are established by one or more of the following criteria. The consumer is:
 MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
MCCMH MCO Policy 2-015 Date: 4/21/11 V. Standards A. A psychiatric evaluation shall be done as an integral part of the assessment process. It serves as the guide to the identification of medical and psychiatric
Unit 4: Personality, Psychological Disorders, and Treatment
 Unit 4: Personality, Psychological Disorders, and Treatment Learning Objective 1 (pp. 131-132): Personality, The Trait Approach 1. How do psychologists generally view personality? 2. What is the focus
Unit 4: Personality, Psychological Disorders, and Treatment Learning Objective 1 (pp. 131-132): Personality, The Trait Approach 1. How do psychologists generally view personality? 2. What is the focus
