IN UTERO FETAL SURGERY
|
|
|
- Kerry Griffith
- 9 years ago
- Views:
Transcription
1 MEDICAL POLICY IN UTERO FETAL SURGERY Policy Number: 2015T0035N Effective Date: May 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES.. DESCRIPTION OF SERVICES... CLINICAL EVIDENCE.. U.S. FOOD AND DRUG ADMINISTRATION CENTERS FOR MEDICARE AND MEDICAID SERVICES (CMS). REFERENCES.. POLICY HISTORY/REVISION INFORMATION.. Policy History Revision Information INSTRUCTIONS FOR USE This Medical Policy provides assistance in interpreting UnitedHealthcare benefit plans. When deciding coverage, the enrollee specific document must be referenced. The terms of an enrollee's document (e.g., Certificate of Coverage (COC) or Summary Plan Description (SPD) and Medicaid State Contracts) may differ greatly from the standard benefit plans upon which this Medical Policy is based. In the event of a conflict, the enrollee's specific benefit document supersedes this Medical Policy. All reviewers must first identify enrollee eligibility, any federal or state regulatory requirements and the enrollee specific plan benefit coverage prior to use of this Medical Policy. Other Policies and Coverage Determination Guidelines may apply. UnitedHealthcare reserves the right, in its sole discretion, to modify its Policies and Guidelines as necessary. This Medical Policy is provided for informational purposes. It does not constitute medical advice. UnitedHealthcare may also use tools developed by third parties, such as the MCG Care Guidelines, to assist us in administering health benefits. The MCG Care Guidelines are intended to be used in connection with the independent professional medical judgment of a qualified health care provider and do not constitute the practice of medicine or medical advice. BENEFIT CONSIDERATIONS Page Related Policies: None Essential Health Benefits for Individual and Small Group: For plan years beginning on or after January 1, 2014, the Affordable Care Act of 2010 (ACA) requires fully insured non-grandfathered individual and small group plans (inside and outside of Exchanges) to provide coverage for ten categories of Essential Health Benefits ( EHBs ). Large group plans (both self-funded and fully insured), and small group ASO plans, are not subject to the requirement to offer coverage for EHBs. However, if such plans choose to provide coverage for benefits which are deemed EHBs (such as maternity benefits), the ACA requires all dollar limits on those benefits to be removed on all Grandfathered and Non-Grandfathered plans. The determination of which benefits constitute EHBs is made on a state by state basis. As such, when using this guideline, it is important to refer to the enrollee specific benefit document to determine benefit coverage. When deciding coverage for in utero fetal surgery, refer to the enrollee-specific benefit document language for further information on benefit coverage for treatment of life-threatening conditions. In
2 some benefit documents, coverage exists for unproven services for persons with life-threatening conditions, under certain circumstances. COVERAGE RATIONALE Intrauterine fetal surgery is proven and medically necessary for the following diagnoses and procedures: 1. Congenital cystic adenomatoid malformation (CCAM) and extralobar pulmonary sequestration (EPS): fetal lobectomy or thoracoamniotic shunt placement for CCAM and thoracoamniotic shunt placement for EPS 2. Sacrococcygeal teratoma (SCT): SCT resection 3. Urinary tract obstruction (UTO): urinary decompression via vesicoamniotic shunt placement 4. Twin-twin transfusion syndrome: fetoscopic laser surgery 5. Twin reversed arterial perfusion (TRAP): ablation or occlusion of anastomotic vessels (e.g., laser coagulation or radiofrequency ablation) 6. Myelomeningocele (MMC) repair Intrauterine fetal surgery is unproven and not medically necessary for the following: 1. Congenital diaphragmatic hernia (CDH) There is insufficient evidence that in utero correction of CDH improves health outcomes for fetuses with CDH compared with standard postnatal surgery. Consistent improvements in survival following in utero fetal surgery have not been observed. 2. Congenital heart disease (CHD) There is insufficient evidence that in utero fetal surgery for complex heart disease improves health outcomes or survival. APPLICABLE CODES The Current Procedural Terminology (CPT ) codes and Healthcare Common Procedure Coding System (HCPCS) codes listed in this policy are for reference purposes only. Listing of a service code in this policy does not imply that the service described by this code is a covered or noncovered health service. Coverage is determined by the enrollee specific benefit document and applicable laws that may require coverage for a specific service. The inclusion of a code does not imply any right to reimbursement or guarantee claims payment. Other policies and coverage determination guidelines may apply. This list of codes may not be all inclusive. Proven Description CPT Code Transabdominal amnioinfusion, including ultrasound guidance Fetal umbilical cord occlusion, including ultrasound guidance Fetal fluid drainage (e.g., vesicocentesis, thoracocentesis, paracentesis), including ultrasound guidance Fetal shunt placement, including ultrasound guidance Unproven Description CPT Code Unlisted fetal invasive procedure, including ultrasound guidance 2
3 CPT is a registered trademark of the American Medical Association. Proven HCPCS Code S2401 S2402 S2403 S2404 S2405 S2411 Unproven HCPCS Code S2400 S2409 Description Repair, urinary tract obstruction in the fetus, procedure performed in utero Repair, congenital cystic adenomatoid malformation in the fetus, procedure performed in utero Repair, extralobar pulmonary sequestration in the fetus, procedure performed in utero Repair, myelomeningocele in the fetus, procedure performed in utero Repair of sacrococcygeal teratoma in the fetus, procedure performed in utero Fetoscopic laser therapy for treatment of twin-to-twin transfusion syndrome Description Repair, congenital diaphragmatic hernia in the fetus using temporary tracheal occlusion, procedure performed in utero Repair, congenital malformation of fetus, procedure performed in utero, not otherwise classified DESCRIPTION OF SERVICES This policy addresses the use of in utero fetal surgery, an open surgical treatment of fetuses with specific life-threatening conditions that involve a fetal malformation. During in utero fetal surgery, a hysterotomy is performed, and the fetus is partially removed to correct a fetal malformation. In utero fetal surgery uses minimally invasive techniques (i.e, small incisions) and instruments to correct the fetal malformation. The primary medical conditions indicated for in utero fetal surgery include the following: Congenital cystic adenomatoid malformation Extralobar pulmonary sequestration Sacrococcygeal teratoma Urinary tract obstruction Twin-twin transfusion syndrome Twin reversed arterial perfusion syndrome Myelomeningocele repair Congenital diaphragmatic hernia Congenital heart disease. Thoracic Lesions Congenital cystic adenomatoid malformation (CCAM) and bronchopulmonary sequestration (BPS) are congenital anomalies of the lung. Appropriate candidates for in utero treatment include a small subset of patients with congenital pulmonary airway malformations. In this subset,the fetal mediastinum is compressed, leading to impaired venous return with resulting fetal hydrops, secondary to cardiac failure (Walsh et al., 2011). Sacrococcygeal Teratoma Fetuses with large, vascular sacrococcygeal teratomas (SCT) have a high incidence of prenatal mortality from high-output cardiac failure or spontaneous hemorrhage of the growing tumor. Fetal surgical procedures for SCT have focused on the small subgroup of fetuses with SCT and hydrops because untreated cases are expected to die in utero or at birth. In severe cases, SCT with hydrops is associated with a maternal risk of developing mirror syndrome, a severe form of preeclampsia (Walsh et al., 2011). 3
4 Urinary Tract Obstruction Fetal urinary tract obstruction (UTO) interferes with normal development of the kidneys and lungs, particularly when involving the lower urinary tract. Goals of fetal surgery have emphasized decompression procedures, such as percutaneous shunting, rather than repair of the specific lesion. The goal of decompression of the distended portion of the urinary tract is to protect function of the remaining kidney and to promote lung development (Walsh et al., 2011). Twin-twin Transfusion Syndrome In twin-twin transfusion syndrome (TTTS), twins share a single chorionic membrane and a single placenta, but have separate amniotic sacs. Women with severe TTTS, who have not undergone treatment before 26 weeks, will usually experience loss of both fetuses. However, if both twins survive, they often experience severe neurologic compromise and organ failure. Treatment options include amnioreduction to relieve pressure and uterine size, termination of the sicker twin, or fetoscopic laser ablation of the communicating vessels. In nonselective ablation, all vessels crossing the dividing membrane are ablated, whereas selective ablation is limited to certain vessels connecting the two fetuses (Walsh et al., 2011). Twin Reversed Arterial Perfusion Twin reversed arterial perfusion (TRAP) sequence is a condition in which an acardiac/acephalic twin receives all of its blood supply from a normal twin, the so-called "pump" twin. Blood enters the acardiac twin through a retrograde flow via the umbilical artery and exits via the umbilical vein. The extra work places an increased demand on the heart of the pump twin, resulting in cardiac failure. Twin death occurs more frequently when the size of the acardiac twin is greater than half that of the pump twin. The goal of fetal surgery is to interrupt blood supply to the nonviable twin. Myelomeningocele Myelomeningocele (MMC) or spinal bifida is a neural tube defect in which the spinal cord forms but remains open. Although MMC is rarely fatal, individuals affected with it have a range of disabilities, including paraplegia, hydrocephalus, skeletal deformities, bowel and bladder incontinence and cognitive impairment. Standard therapy is postnatal surgical closure of the MMC followed by shunting for hydrocephalus if needed (Walsh et al., 2011). Congenital Diaphragmatic Hernia Congenital diaphragmatic hernia (CDH) results from abnormal development of the diaphragm, which allows abdominal organs like the bowel, stomach, and liver to protrude into the chest cavity. Fetuses diagnosed in utero as a result of maternal symptoms have a high mortality risk. Less invasive fetal procedures are being developed that focus on methods to accomplish tracheal occlusion (Walsh et al., 2011). Congenital Heart Disease In utero procedures are performed for cardiac conditions such as pulmonary atresia with intact ventricular septum, critical aortic stenosis with impending hypoplastic left heart syndrome, and hypoplastic left heart syndrome with intact atrial septum. All of these conditions, if untreated either in utero or soon after birth, are fatal (Walsh et al., 2011). CLINICAL EVIDENCE In a Technical Brief, the Agency for Healthcare Research and Quality (AHRQ) presented an overview of the current state of practice and research regarding in utero fetal surgical procedures for the following conditions: congenital diaphragmatic hernia, cardiac malformations, myelomeningocele, obstructive uropathy, sacrococcygeal teratoma, twin-twin transfusion syndrome and thoracic lesions (Walsh et al., 2011). 4
5 Congenital Cystic Adenomatoid Malformation (CCAM) and Extralobar Pulmonary Sequestration (EPS) A prospective study evaluating 58 fetuses with CCAM found that 29% were at risk for hydrops and required fetal intervention. The overall survival rate was 71% after fetal surgery; however, the survival rate for hysterotomy and open fetal lobectomy was 29% compared with 100% for fetoscopic shunting or cyst aspiration. The perinatal mortality rate was 29% in those fetuses who were considered unlikely to survive (Crombleholme et al., 2002). Sacrococcygeal Teratoma (SCT) Fetal surgery is not considered appropriate in the presence of the maternal mirror syndrome or in cases of advanced high-output cardiac failure (Hedrick et al., 2004). Urinary Tract Obstruction (UTO) In utero fetal surgery for UTO improves perinatal survival in selected fetuses and children, who are at high risk for mortality due to renal failure and pulmonary complications. Perinatal survival rates ranged from approximately 57% to 80%. The prognosis appears to be worse for fetuses with elevated urinary electrolytes or prolonged anhydramnios at the time of surgery. Despite initial surgical success and improved survival, more than 25% of children have residual renal disease that require subsequent transplantation, urinary tract surgery, or other medical interventions. Most children also demonstrate growth retardation, and many void spontaneously. Pulmonary dysfunction is apparent, despite fetal surgery, and has been reported to result in death in 18% to 25% of children followed for a period up to 114 months. A meta-analysis evaluated the efficacy and safety of prenatal bladder drainage. Results showed significantly improved perinatal survival among 195 fetuses in controlled trials that received the intervention compared with those who did not (Clark et al., 2003; Freedman et al., 1999; McLorie et al, 2001; Welsh et al., 2003). Twin-Twin Transfusion Syndrome (TTTS) A total of 120 infants with twin-to-twin transfusion syndrome (TTTS) were enrolled in a randomized clinical trial (RCT) of laser photocoagulation versus amnioreduction. Investigators assessed long-term neurological and developmental outcomes. The primary outcome was a composite of death and major neurological impairment. The authors found that, at 6 years of age, 82% of the children in the laser group and 70% of the children in the amnioreduction group had a normal neurological evaluation; the differences between the grops was not significant.. Laser therapy was associated with a 40% reduction in the risk of fetal death or long-term neurologic impairment when compared with amnioreduction (Salomon et al., 2010). Roberts et al. (2008) assessed which treatments for twin-twin transfusion syndrome (TTTS) improved fetal, childhood and maternal outcomes. The authors compared outcomes from 3 (253 women) randomized and quasi-randomized studies of amnioreduction, laser coagulation, and septostomy. Laser coagulation resulted in reduced overall mortality and neonatal mortality when compared with amnioreduction. There was no difference in perinatal outcome between amnioreduction and septostomy. The results suggest that endoscopic laser coagulation of anastomotic vessels should be considered for treatment of all stages of TTTS to improve perinatal and neonatal outcome. In a later publication, Roberts et al. (2014) concluded that endoscopic laser coagulation of anastomotic vessels should be considered in the treatment of all stages of twin-twin transfusion syndrome to improve neurodevelopmental outcomes. Further research to assess the effect of treatment on milder and more severe forms of twin-twin transfusion syndrome and long-term survival outcomes are still required. There is some evidence that fetoscopic laser surgery to ablate placental vascular anastomoses is relatively efficacious for treating clinically and ultrasonographically confirmed, severe TTTS, in monozygotic and monochorionic twin pregnancies, less than 26 weeks gestation.. The surgery improves fetal and neonatal survival rates and perinatal outcomes compared with conservative management and serial amnioreduction; however, serial amnioreduction or delivery is more appropriate for TTTS diagnosed at 26 weeks gestation or more. Serial amnioreduction, which reduces polyhydramnios and prevents premature rupture of the membranes (PROM) and pre- 5
6 term delivery (PTD), may be more appropriate for TTTS diagnosed at 26 weeks or more since it is less likely to result in intrauterine fetal death than laser surgery. As a result, serial amnioreduction may be more beneficial for pregnancies that are closer to viability and delivery (Berghella et al., 2001; van Gemert et al., 2001). Senat et al. (2007) conducted a RCT and evaluated pregnant women with severe TTTS before 26 weeks of gestation, who were randomly assigned to laser therapy (n=72) or amnioreduction (n=70). The study concluded early because an interim analysis demonstrated a significant survival benefit in the laser group. Compared to the amnioreduction group, the laser group had a higher likelihood of survival (of at least 1 twin) to 28 days of age (76% in laser group and 56% in amnioreduction group). The laser group also had a lower incidence of cystic periventricular leukomalacia, and were more likely to have no neurological complications at 6 months of age (52% in laser group and 31% in amnioreduction group). Graef et al. (2006) evaluated 167 children (median age 3 years, 2 months) to investigate longterm neurodevelopment after intrauterine laser coagulation for TTTS. A total of 145 children (86.8%) demonstrated normal development, 12 children (7.2%) showed minor neurological abnormalities, and 10 children (6%) demonstrated major neurological abnormalities. The investigators concluded that intrauterine laser coagulation was the relatively best treatment option for severe TTTS (Graef et al., 2006). Professional Societies Society for Maternal-Fetal Medicine (SMFM) A SMFM clinical guideline reviewed the natural history, pathophysiology, diagnosis, and treatment options for TTTS. The guideline recommends that extensive counseling be provided to patients with pregnancies complicated by TTTS, including natural history of the disease, as well as management options, and their risks and benefits. More than three-fourths of stage I TTTS cases remain stable or regress without invasive intervention, with perinatal survival of about 86%. Therefore, many patients with stage I TTTS can often be managed expectantly. Fetoscopic laser photocoagulation of placental anastomoses is considered by most experts to be the best available approach for stages II, III and IV TTTS in continuing pregnancies at <26 weeks, but published meta-analysis data have demonstrated no significant survival benefit. In addition, longterm neurologic outcomes reported in the Eurofetus trial were not significantly different between treatment and control group. Laser-treated TTTS has been shown to be associated with a perinatal mortality rate of 30-50%, and a 5-20% chance of long-term neurologic handicap. Steroids for fetal maturation should be considered at 24 0/7 to 33 6/7 weeks, particularly in pregnancies complicated by stage III TTTS, and those undergoing invasive interventions (SMFM, 2013). Twin Reversed Arterial Perfusion (TRAP) Lee et al. (2013) reported the North American Fetal Therapy Network (NAFTNet) Registry data on the outcomes of using radiofrequency ablation to treat twin reversed arterial perfusion (TRAP). This was a retrospective review of all patients who underwent percutaneous radiofrequency ablation of an acardiac twin after referral to a NAFTNet institution. The primary outcome was neonatal survival to 30 days of age. Of the 98 patients identified, there were no maternal deaths. Mean gestational age at delivery was 33.4 weeks overall and 36.0 weeks for survivors. Median gestational age at delivery was 37 weeks. Survival of the pump twin to 30 days was 80% in the overall cohort. The authors concluded that this data suggests that radiofrequency ablation of the acardiac twin is an effective treatment for TRAP sequence. Pagani et al. (2013) conducted a retrospective cohort study and meta-analysis of intrafetal laser treatment for twin reversed arterial perfusion (TRAP) sequence. A total of 23 cases of TRAP were identified during the study period. Of these, 6 were managed conservatively and 17 were treated with laser therapy. All cases managed conservatively were complicated by intrauterine death (IUD) at a median gestational age of 14 weeks. Among the treated cases, 14 (82%) delivered a healthy twin at a median gestational age of 37 weeks. The overall neonatal survival was 80%. 6
7 Adverse pregnancy outcome was significantly lower when the treatment was performed before 16 weeks' gestation. Cabassa et al. (2013) evaluated the treatment of monochorionic twin pregnancies complicated by twin reversed arterial perfusion sequence (TRAP) using radiofrequency ablation (RFA). Between July 2007 and October 2010, 11 monochorionic twin pregnancies complicated by TRAP were identified. A total of 7 patients underwent intrafetal ablation of the acardiac twin with RFA. Median gestational age at the intervention was 17 weeks. A total of 5 fetuses (71%) were delivered at a median gestational age of 33 weeks; all were alive and had a normal examination at 6 months of age. The overall neonatal survival was 85%. The authors noted that further research is needed to define the best timing of the procedure. The results of some studies demonstrate improved outcomes for umbilical cord laser photocoagulation. A prospective multicenter study evaluated the outcome of laser coagulation of placental anastomoses (n=18) or the umbilical cord of the acardiac twin (n=42). The overall survival rate of the pump twin was 80% (Hecher et al., 2006). Another approach is to use radiofrequency ablation to obliterate blood supply to an acardiac twin. Tsao et al. (2002) evaluated 13 monochorionic twin gestations with twin reversed arterial perfusion sequence who underwent selective reduction of the abnormal twin with the use of radiofrequency ablation. All 13 pump fetuses were delivered. At the time of the study, 12 of 13 infants were alive and well. The first patient in this series was delivered at 24.4 weeks and the infant subsequently died from complications of prematurity. Average gestational age at intervention was 20.7 weeks, and the average gestational age at delivery was 36.2 weeks. The investigators concluded that radiofrequency ablation is a minimally invasive, percutaneous technique that can effectively obliterate blood supply to an acardiac twin to preserve and protect the pump twin. Tan et al. (2003) identified 32 reports involving 74 cases of acardiac twin treated by minimally invasive techniques. Seventy-one cases were included for analysis including 40 treated by cord occlusion and 31 by intrafetal ablation. Cord occlusion was first attempted by embolization (n = 5), cord ligation (n = 15), laser coagulation (n = 10), bipolar diathermy (n = 7) and monopolar diathermy (n = 3). Intrafetal ablation was performed by alcohol (n = 5), monopolar diathermy (n = 9), interstitial laser (n = 4) and radiofrequency (n = 13). The overall pump twin survival rate was 76% (n = 54). Intrafetal ablation was associated with later median gestational age at delivery (37 vs. 32 weeks) and higher median treatment-delivery interval (16 vs. 9.5 weeks) compared with cord occlusion techniques. It was also associated with a lower technical failure rate (13% vs. 35%), lower rate of premature delivery or rupture of membranes before 32 weeks (23% vs. 58%) and higher rate of clinical success (77% vs. 50%) than cord occlusion techniques. This review suggests that intrafetal ablation is the treatment of choice for acardiac twins because it is simpler, safer and more effective when compared with the cord occlusion techniques. Lee et al. (2007) evaluated the treatment of 29 patients with twin reversed arterial perfusion (TRAP) sequence using radiofrequency ablation to stop perfusion to the acardiac twin and protect the pump twin. The investigators concluded that radiofrequency ablation of the acardiac twin effectively protects the pump twin from high-output cardiac failure and death. Greater than 90% survival can be achieved in monochorionic-diamniotic pregnancies complicated by TRAP sequence with a mean gestation age at time of delivery close to term. Myelomeningocele (MMC) A Hayes report concluded that there is moderate quality evidence that in utero fetal surgery (IUFS) for myelomeningocele (MMC) is associated with improved motor function, excretory function and neuroanatomical outcomes, as well as reduced need for shunt placement. However, IUFS did not influence cognitive outcomes and did result in lower gestational age at birth (premature birth) relative to postnatal controls. One randomized controlled trial and ten nonrandomized controlled studies compared in utero fetal surgery (IUFS) with standard postnatal 7
8 surgery. Most of the studies were retrospective and did not follow up on the developmental outcomes of IUFS past 3 years of age. As a consequence, the relationship between many of the findings and longer-term clinical outcomes is not clear at this time (Hayes, 2012a; updated 2013). The Management of Myelomeningocele Study (MOMS) compared outcomes of prenatal versus postnatal repair of myelomeningocele. Patients (n=183) were randomized to undergo either prenatal surgery before 26 weeks of gestation or standard postnatal repair. Primary outcomes were fetal or neonatal death, the need for a cerebrospinal shunt by the age of 12 months and mental development and motor function at 30 months. The children of 158 patients were available for evaluation at 12 months. The children of 134 patients were available for evaluation at 30 months. The trial was stopped after recruiting 183 of the planned 200 patients due to demonstrated efficacy of prenatal versus postnatal repair. Despite having more severe lesions and an increased risk of preterm delivery, the study found that the prenatal surgery group had significantly better outcomes than the postnatal surgery group. Prenatal surgery for myelomeningocele decreased the risk of death or need for shunting by the age of 12 months. Prenatal surgery also improved scores on a composite measure of mental and motor function at 30 months. However, prenatal surgery was associated with an increased risk of preterm delivery and uterine dehiscence at delivery. The authors noted that the potential benefits of prenatal surgery must be balanced against the risks of prematurity and maternal morbidity (Adzick, 2011). Danzer et al. (2009) evaluated lower extremity neuromotor function (LENF) and short-term ambulatory potential following fetal myelomeningocele (fmmc) closure in a retrospective chart review of 54 children. Neonatal LENF was compared to predicted function based on spinal lesion level assigned by prenatal ultrasound. A total of 31 out of 54 of fmmc children (57.4%) had better than predicted, 13/54 (24.1%) same as predicted and 10/54 (18.5%) worse than predicted LENF at birth. At a median follow-up age of 66 months, 37/54 (69%) walk independently, 13/54 (24%) are assisted walkers, and 4/54 (7%) are wheelchair dependent. Despite the observed improved ambulatory status, structured evaluation of coordinative skills revealed that the majority of independent walkers and all children that require assistive devices to walk experience significant deficits in lower extremity coordination. The investigators concluded that fmmc surgery results in better than predicted LENF at birth and short-term ambulatory status. However, fmmc children continue to demonstrate deficits in movement coordination that are characteristic for children with spina bifida. Danzer et al. (2008) evaluated the incidence and clinical implications of the development of cutaneously derived intradural inclusion cysts (ICs) following fetal myelomeningocele (fmmc) closure in retrospective databases and responses to a parental questionnaire. The investigators found that cutaneously derived intradural ICs can develop following fmmc surgery. Deterioration of bladder function, risk of recurrence, and loss of lower-extremity function appear to be the most important long-term complications of IC in children with fmmcs. Koh et al. (2006) compared urodynamic findings in patients who underwent prenatal closure of myelomeningocele with those of patients who underwent postnatal closure. Urodynamic studies of 5 patients who underwent prenatal closure of myelomeningocele were compared to those of 88 patients with similar level lesions who underwent postnatal repair. All 5 prenatally treated patients had lower lumbosacral lesions on neurological examination. In comparison, 34 of the 88 patients in the postnatal cohort (39%) lacked sphincter activity at newborn examination, with similar findings noted at 1-year evaluation. In terms of bladder function, all 5 patients in the prenatal cohort showed detrusor overactivity, compared to 33 of the 88 patients (38%) in the postnatal cohort at the newborn examination, with similar findings at 1-year evaluation. The investigators concluded that fetal closure of myelomeningocele is associated with a higher incidence of complete denervation of the external urethral sphincter and detrusor overactivity compared to postnatal closure. In a comparative study, pre- and postnatal head biometry and cerebrospinal fluid (CSF) space data were obtained from in utero repaired MMC fetuses (n=22) and were compared to 8
9 measurement of MMC patients that underwent standard MMC repair after birth (n=16) and a cohort of age-matched control patients. No differences in postnatal CSF spaces were found between controls and prenatally repaired MMC patients. In patients with postnatal repair, CSF spaces remained significantly reduced. In utero repair fetuses showed a significant reversal of hindbrain herniation and normalization of the CSF spaces compared to postnatally repaired patients (Danzer 2007). Another study followed 51 patients who underwent MMC closure. Fortyeight patients survived and passed their second birthday. Neuro-developmental testing indicated that 67% of the patients had cognitive language and social skills in the normal range, 20% with mild delays, and 13% with significant delays. The investigators concluded that children who have undergone fetal MMC surgery have characteristic neuro-developmental deficits that may not be worsened by fetal surgery (Johnson, 2006). Professional Societies American College of Obstetricians and Gynecologists (ACOG) In 2014, ACOG s Maternal-Fetal Management Task Force published a position statement (Cohen et al., 2014) regarding fetal myelomeningocele repair to develop optimal practice criteria for medical and surgical leadership. Members of the task force report the following: Fetal MMC repairs should be performed in established fetal therapy centers using a multidisciplinary team approach. The fetal surgery team must have experience working together and individual members have a level of expertise in their field. The level of fetal surgical technical expertise demanded requires an adequate annual volume of open fetal and EXIT procedures to maintain competency. The level of technical expertise in fetal MMC repair requires an initial experience of at least 5 cases and an ongoing adequate annual volume of cases evaluated for fetal surgery to maintain competency. Centers developing new programs must receive guidance and training from established programs and experienced individuals. The MOMS protocol should be followed for preoperative, intraoperative, and immediate postoperative care. This applies to inclusion and exclusion criteria for in utero MMC repair. Modification of the long-term postoperative and delivery care is acceptable in certain circumstances. Modifications to the perioperative protocol are only permissible after the results of fetal MMC repair performed by an expanded number of centers have been shown to be consistent with the results obtained in the MOMS trial. Such modifications would, ideally, be developed by means of a series of cooperative trials. Ongoing neonatal and pediatric care should be performed in multidisciplinary spina bifida clinics. This can be done at outside centers but must be standardized. Counseling should be full disclosure and nondirective in nature. It should also include reproductive implications for future pregnancies. A reflective period of at least 24 hours is recommended. 9
10 Short-term and long-term outcomes data from all centers should be kept in a national registry with periodic review. Centers performing open MMC repair must maintain a collaborative approach to outcomes reporting and future research, including participating in the long-term outcomes data collection and evaluation. Close links between fetal centers throughout the country and community providers are essential. An ACOG practice bulletin addresses the role of fetal surgery in treating neural tube defects but makes no specific recommendations (ACOG, 2003; reaffirmed 2013). An ACOG committee opinion states that maternal-fetal surgery is a major procedure for the woman and her fetus, and it has significant implications and complications that occur acutely, postoperatively, for the duration of the pregnancy and in subsequent pregnancies. Therefore, it should only be offered at facilities with the expertise, multidisciplinary teams, services and facilities to provide the intensive care required for these patients (ACOG, 2013). Congenital Diaphragmatic Hernia (CDH) There is some low quality evidence that survival rates may be increased by in utero fetal surgery (IUFS) as a treatment for congenital diaphragmatic hernia; however, findings were not consistent across studies. Several studies included randomization, however most had small sample sizes, limited follow-up periods, and heterogeneous outcomes. There were seven studies representing three separate data sets; of these, two stu provided descriptive findings only and lacked statistical analyses (Hayes, 2012b; updated 2013). Ruano et al. (2012) conducted a RCT to determine whether fetal endoscopic tracheal occlusion (FETO) improved survival in cases of congenital diaphragmatic hernia (CDH). Patients whose fetuses had severe isolated CDH (lung-to-head ratio < 1.0, liver herniation into the thoracic cavity and no other detectable anomalies) were randomly assigned to FETO (n=20) or to standard postnatal management (n=21). Tracheal balloon placement was achieved with ultrasound guidance and fetoscopy between 26 and 30 weeks of gestation. Postnatal therapy was the same for both treated fetuses and controls. The primary outcome was survival to 6 months of age. Delivery occurred at 35.6 ± 2.4 weeks in the FETO group and at 37.4 ± 1.9 weeks in the control group. In the intention-to-treat analysis, 10/20 (50.0%) infants in the FETO group survived, while 1/21 (4.8%) controls survived. In the received-treatment analysis, 10/19 (52.6%) infants in the FETO group and 1/19 (5.3%) controls survived. The authors concluded that FETO improved infant survival in isolated severe CDH; however, the risk of prematurity and preterm premature rupture of membranes was high. Runao et al. (2011) treated 16 fetuses with severe congenital diaphragmatic hernia (CDH) with fetal endoscopic tracheal occlusion (FETO) and compared their outcome to 18 similar cases treated with standard neonatal therapy. The primary outcome was neonatal survival (up to 28 days after birth). Survival in the FETO group was 53% compared to 6% in the standard therapy group. This study is limited by small sample size and lack of randomization. Two uncontrolled studies showed that in carefully selected fetuses, in utero tracheal occlusion can promote lung growth and improve the likelihood of neonatal survival compared with standard postnatal surgery (Flake 2000; Harrision 2003a). However, questions about treatment efficacy have been raised by a recent RCT that found no significant improvement in survival rates or health outcomes among fetuses treated with in utero tracheal occlusion compared with standard postnatal surgery (Harrison, 2003b). Fetendo appears to promote fetal lung growth as shown by fetal and postnatal US. Despite observations of enhanced lung growth, in utero tracheal occlusion has limitations, including the occurrence of pulmonary complications, the need for postnatal interventions, prematurity, and a lack of correlation of lung maturation with improved postnatal outcomes, including survival. 10
11 Preterm labor was common and virtually all infants were born prematurely (i.e., at less than 37 weeks). In utero tracheal occlusion was associated with numerous complications. Postnatal complications included the need for extracorporeal membrane oxygenation (ECMO) (a form of long-term heart-lung bypass) and mechanical ventilation as well as barotrauma, chylothorax, and renal failure. Tracheal injury is common and some patients require permanent tracheostomies. Survivors displayed significant morbidity including gastroesophageal reflux (some required surgery), respiratory problems, problems with the operative site, and neurological disabilities. However, one study found no significant neurologic abnormalities among the survivors (Harrison 2003b). Perinatal mortality rates ranged from 36% to 67%. Causes of death included prematurity (at less than 37 weeks), lung immaturity at birth, multiorgan failure, and sepsis. Mortality is higher when the procedure is performed via maternal hysterotomy than by fetoscopy. No maternal deaths were reported; however, maternal complications included preterm labor, pulmonary edema, vaginal bleeding, premature rupture of the membrane (PROM), and chorioamniotic membrane separation (Flake, 2000; Harrision, 2003a; Harrison, 2003b; Sydorak, 2003). A case series reported the results of 24 fetuses with severe CDH who underwent percutaneous fetal endoluminal tracheal occlusion (FETO) with a balloon. Premature prelabor rupture of the membrane occurred in 16.7% and 33.3% at 28 and 32 weeks respectively. Seven-day, 28-day, and survival at discharge were 75%, 58.3%, and 50%, respectively. The investigators concluded that FETO may improve survival in highly selected CDH cases (Deprest et al., 2006). Hirose et al. (2004) conducted a retrospective review of 52 patients who underwent an EXIT procedure. Fifty-one of 52 patients were born alive. At the time of the study, 27 of 52 patients (52%) were alive. All deaths have been in patients with congenital diaphragmatic hernia. The investigators concluded that the EXIT procedures can be performed with minimal maternal morbidity and with good outcomes. Saura et al. (2007) reported their experience in the postnatal management of congenital diaphragmatic hernia (CDH) in 19 fetuses after fetal endoluminal balloon tracheal occlusion (FETO). The investigators found that CDH patients with a poor prognosis undergoing FETO had postnatal outcomes similar to non-prenatally studied cases and good prognosis cases. Kunisaki et al. (2007) evaluated whether ex utero intrapartum treatment with extracorporeal membrane oxygenation (EXIT to ECMO) is a reasonable approach for managing patients antenatally diagnosed with severe congenital diaphragmatic hernia Fourteen patients underwent EXIT with a trial of ventilation. Fetuses with poor preductal oxygen saturations despite mechanical ventilation received ECMO before their delivery. Three babies passed the ventilation trial and survived, but 2 of them required ECMO within 48 hours. The remaining 11 fetuses received ECMO before their delivery. Overall survival after EXIT-to-ECMO was 64%. At 1-year follow-up, all survivors had weaned off supplemental oxygen, but 57% required diuretics and/or bronchodilators. The investigators concluded that the EXIT-to-ECMO procedure is associated with favorable survival rates and acceptable pulmonary morbidity in fetuses expected to have a poor prognosis under conventional management. There are several ongoing clinical trials evaluating various types of fetal surgery, including tracheal occlusion for fetal surgery. Congenital Heart Disease (CHD) Pedra et al. (2014) reported results of a small case series of fetal cardiac procedures for various cardiac conditions (21 fetuses; 22 procedures). The procedures included artrial septostomy, aortic valvuloplasty, pulmonary valvuloplasty, or a combination of aortic septostomy and aortic valvuloplasty. The fetal clinical conditions consisted of critical aortic stenosis (n=13), hypoplastic left heart syndrome and intact interatrial septum or small patent foramen ovale (n=4), pulmonary atresia with intact ventricular septum (n=1), and critical pulmonary stenosis (n=3). A total of 91% of procedures (20 of 22) were considered successful. Two procedures, aortic valvuloplasty and 11
12 pulmonary valvuloplasty, failed. One fetus died and no maternal complications were reported. Long-term morbidity was frequent, and 12 fetal deaths eventually occurred. Kalish et al. (2014) reported that prenatal atrial septal stent placement was technically feasible in 4 of 9 fetuses. There was one fetal death. Although eight fetuses survived to delivery, four died during the neonatal period. Chaturvedi et al. (2013) conducted a small retrospective review (2000 to 2012) in 10 fetusus. A total of four fetuses underwent percutaneous ultrasound-guided stenting of the atrial septum to decompress fetal left atrial (LA) hypertension. Two neonatal deaths occurred, and there were no maternal complications or deaths. At up to 20 months of follow up, 2 children were alive. A total of 70 fetuses underwent attempted aortic valvuloplasty for critical aortic stenosis with evolving hypoplastic left heart syndrome. The procedure was technically successful (increased flow across the valve) in 52 fetuses (74%). Forty-five of these resulted in a viable live birth. Relative to 21 untreated comparison fetuses, subsequent prenatal growth of the aortic and mitral valves, but not the left ventricle, was improved after intervention. Nine pregnancies (13%) did not reach a viable term or preterm birth. Seventeen patients had biventricular circulation postnatally, 15 from birth. Larger left heart structures and higher left ventricular pressure at the time of intervention were associated with biventricular outcome. Technically successful aortic valvuloplasty alters left heart valvar growth in fetuses with aortic stenosis and evolving hypoplastic left heart syndrome and, in a subset of cases, appeared to contribute to a biventricular outcome after birth. The authors note that fetal aortic valvuloplasty carries a risk of fetal demise. Further studies from well-designed clinical trials are needed to confirm these results (McElhinney et al., 2009). Marshall et al. (2008) reviewed the medical records and imaging of 21 fetuses undergoing intervention for atrial septal defect creation for hypoplastic left heart syndrome and intact atrial septum. Of the 21 procedures attempted between 24 and 34 weeks' gestation, 19 were technically successful. Fetal demise occurred in two cases. Selamet et al. (2007) evaluated the effects of mid-gestation fetal balloon aortic valvuloplasty in 30 fetuses with aortic stenosis. In 26 fetuses, aortic valvuloplasty was technically successful and improved left ventricular systolic function and left heart Doppler characteristics. Vida et al. (2007) retrospectively identified 32 neonates with a diagnosis of hypoplastic left heart syndrome (HLHS) and intact or highly restrictive atrial septum (I/HRAS) who underwent left atrial decompression in utero or postnatally before surgery. Fourteen patients (44%) underwent fetal intervention, either atrial septoplasty (n = 9) or aortic valvuloplasty (n = 5). The investigators concluded that prenatal decompression of the left atrium may be associated with greater hospital survival. Proposed effects of fetal intervention on lung pathology and longer-term survival require further study. An international retrospective study evaluated the efficacy and safety of percutaneous US-guided balloon valvuloplasty for treatment of severe aortic valve obstruction in 12 fetuses. Technically successful valvuloplasties were achieved in 7 (58%) fetuses, none of which had atresias. There was 1 (8%) long-term survivor following fetal surgery who remained alive with near-normal recovery of cardiac contractility and ejection fraction at 4 years of age. A second survivor failed fetal valvuloplasty but survived postnatal surgery. Twenty-five percent of the mothers required emergency cesarean section deliveries for sustained fetal bradycardia or chorioamnionitis (Kohl et al., 2000). Tulzer and colleagues (2002) described 2 cases of fetal pulmonary valvuloplasty for critical pulmonary stenosis or atresia with intact septum associated with imminent hydrops. Both children survived to delivery and had repeat valvuloplasty after birth. At last follow-up, one child was alive at 12 months of age and another at 18 months of age. In utero balloon dilation of severe aortic stenosis was attempted in 20 fetuses with technical success in 14 of the fetuses. Of the 14 fetuses with technically successful interventions, 3 had two-ventricle circulation at 1 month of age and 2 infants underwent surgical repair and maintained two-ventricle circulation. Of the remaining 9 fetuses, two died after the technically successful intervention and the remaining 7 12
13 fetuses developed hypoplastic left heart syndrome (Tworetzky et al., 2004). U.S. FOOD AND DRUG ADMINISTRATION (FDA) The fetal interventions described in this policy are surgical procedures and are not subject to FDA approval. CENTERS FOR MEDICARE AND MEDICAID SERVICES (CMS) Medicare does not have a National Coverage Determination (NCD) for intrauterine fetal surgery. Local Coverage Determinations (LCDs) do not exist at this time. (Accessed January 27, 2015). REFERENCES Adzick NS, Thom EA, Spong CY, et al. A randomized trial of prenatal versus postnatal repair of myelomeningocele. N Engl J Med. 2011;364(11): American College of Obstetricians and Gynecologists (ACOG). ACOG Committee opinion no. #44. Neural tube defects. Int J Gynaecol Obstet Oct;83(1): American College of Obstetricians and Gynecologists (ACOG). ACOG Committee opinion no. 550: Maternal-fetal surgery for myelomeningocele. Obstet Gynecol. 2013; Jan;121(1): American College of Obstetricians and Gynecologists (ACOG). ACOG committee opinion #501: Maternal-fetal intervention and fetal care centers. Obstet Gynecol Aug;118(2 Pt 1): Berghella V, Kaufmann M. Natural history of twin-twin transfusion syndrome. J Reprod Med May;46(5): Biard JM, Johnson MP, Carr MC,et al. Long-term outcomes in children treated by prenatal vesicoamniotic shunting for lower urinary tract obstruction. Obstet Gynecol. 2005; Sep;106(3): Cabassa P, Fichera A, Prefumo F, et al. The use of radiofrequency in the treatment of twin reversed arterial perfusion sequence: a case series and review of the literature. Eur J Obstet Gynecol Reprod Biol. 2013; Feb;166(2): Chaturvedi RR, Ryan G, Seed M, et al. Fetal stenting of the atrial septum: technique and initial results in cardiac lesions with left atrial hypertension. Int J Cardiol. Oct; 168(3): Clark TJ, Martin WL, Divakaran TG, et al. Prenatal bladder drainage in the management of fetal lower urinary tract obstruction: a systematic review and meta-analysis. Obstet Gynecol. 2003;102(2): Cohen AR, Couto J, Cummings JJ, et al. Position statement on fetal myelomeningocele repair. Am J Obstet Gynecol. 2014; 210(2): Crombleholme T, Coleman B, Hedrick H, et al. Cystic adenomatoid malformation volume ratio predicts outcome in prenatally diagnosed cystic adenomatoid malformation of the lung. J Pediatr Surg. 2002;37(3): Danzer E, Adzick NS, Rintoul NE, et al. Intradural inclusion cysts following in utero closure of myelomeningocele: clinical implications and follow-up findings. J Neurosurg Pediatr. 2008; Dec;2(6):
14 Danzer E, Gerdes M, Bebbington MW, et al. Lower extremity neuromotor function and short-term ambulatory potential following in utero myelomeningocele surgery. Fetal Diagn Ther. 2009; Jan 28;25(1): Danzer E, Johnson MP, Bebbington M, et al. Fetal head biometry assessed by fetal magnetic resonance imaging following in utero myelomeningocele repair. Fetal Diagn Ther. 2007;22(1):1-6. Deprest J, Jani J, Van Schoubroeck D, et al. Current consequences of prenatal diagnosis of congenital diaphragmatic hernia. J Pediatr Surg Feb;41(2): ECRI Institute. Hotline Service. Fetal surgery for correcting myelomeningocele. June Flake AW, Crombleholme TM, Johnson MP, et al. Treatment of severe congenital diaphragmatic hernia by fetal tracheal occlusion: clinical experience with fifteen cases. Am J Obstet Gynecol. 2000;183(5): Freedman AL, Johnson MP, Smith CA, et al. Long-term outcome in children after antenatal intervention for obstructive uropathies. Lancet. 1999;354(9176): Graef C, Ellenrieder B, Hecher K, et al. Long-term neurodevelopmental outcome of 167 children after intrauterine laser treatment for severe twin-twin transfusion syndrome. Am J Obstet Gynecol Feb;194(2): Grivell Rm Andersen C, Dodd JM. Prenatal versus postnatal repair procedures for spina bifida for improving infant and maternal outcomes. Cochrane Database Syst Rev. 2014; CD Harrison M, Keller R, Hawgood S, et al. A randomized trial of fetal endoscopic tracheal occlusion for severe fetal congenital diaphragmatic hernia. N Engl J Med. 2003b;349(20): Harrison M, Sydorak R, Farrell J, et al. Fetoscopic temporary tracheal occlusion for congenital diaphragmatic hernia: prelude to a randomized, controlled trial. J Pediatr Surg. 2003a;38(7): Hayes, Inc. Directory. In utero fetal surgery for myelomeningocele. October 2012a. Updated October Hayes, Inc. Directory. In utero fetal surgery for congenital diaphragmatic hernia. October 2012b. Updated October Hecher K, Lewi L, Gratacos E, et al. Twin reversed arterial perfusion: fetoscopic laser coagulation of placental anastomoses or the umbilical cord. Ultrasound Obstet Gynecol. 2006; Oct;28(5): Hedrick HL, Flake AW, Crombleholme TM, et al. Sacrococcygeal teratoma: prenatal assessment, fetal intervention, and outcome. J Pediatr Surg. 2004;39(3): Hirose S, Farmer DL, Lee H, et al. The ex utero intrapartum treatment procedure: Looking back at the EXIT. J Pediatr Surg Mar;39(3): Johnson MP, Gerdes M, Rintoul N, et al. Maternal-fetal surgery for myelomeningocele: neurodevelopmental outcomes at 2 years of age. Am J Obstet Gynecol. 2006; Apr;194(4): ; discussion Kalish BT, Tworetzky W, Benson CB, et al. Technical challenges of atrial septal stent placement in fetuses with hypoplastic left heart syndrome and intact arterial septum. Catheter Cardiovasc 14
15 Interv. 2014; Jul; 84(1): Koh CJ, DeFilippo RE, Borer JG, et al. Bladder and external urethral sphincter function after prenatal closure of myelomeningocele. J Urol. 2006;176(5): Kohl T, Sharland G, Allan LD, et al. World experience of percutaneous ultrasound-guided balloon valvuloplasty in human fetuses with severe aortic valve obstruction. Am J Cardiol. 2000;85(10): Kunisaki SM, Barnewolt CE, Estroff JA, et al. Ex utero intrapartum treatment with extracorporeal membrane oxygenation for severe congenital diaphragmatic hernia. J Pediatr Surg Jan;42(1): Lee H, Bebbington M, Crombleholme TM; North American Fetal Therapy Network. The North American Fetal Therapy Network Registry data on outcomes of radiofrequency ablation for twinreversed arterial perfusion sequence. Fetal Diagn Ther. 2013;33(4): Lee H, Wagner AJ, Sy E, et al. Efficacy of radiofrequency ablation for twin-reversed arterial perfusion sequence. Am J Obstet Gynecol May;196(5):459.e1-4. Marshall AC, Levine J, Morash D, et al. Results of in utero atrial septoplasty in fetuses with hypoplastic left heart syndrome. Prenat Diagn. 2008; Nov;28(11): McElhinney DB, Marshall AC, Wilkins-Haug LE, et al. Predictors of technical success and postnatal biventricular outcome after in utero aortic valvuloplasty for aortic stenosis with evolving hypoplastic left heart syndrome. Circulation. 2009; Oct 13;120(15): McLorie G, Farhat W, Khoury A, et al. Outcome analysis of vesicoamniotic shunting in a comprehensive population. J Urol. 2001;166(3): Pagani G, D'Antonio F, Khalil A, et al. Intrafetal laser treatment for twin reversed arterial perfusion sequence: cohort study and meta-analysis. Ultrasound Obstet Gynecol Jul;42(1):6-14. Pedra SR, Peralta CF, Crema L, et al. Fetal interventions for congenital heart disease in Brazil. Pediatr Cardiol. Mar 2014; 35(3): Roberts D, Neilson JP, Kilby MD, Gates S. Interventions for the treatment of twin-twin transfusion syndrome. Cochrane Database Syst Rev Jan 30;1:CD Roberts D, Gates S, Kilby M, Neilson JP. Interventions for twin-twin transfusion syndrome: a Cochrane review. Ultrasound Obstet Gynecol Jun;31(6): Ruano R, Duarte SA, Pimenta EJ, et al. Comparison between fetal endoscopic tracheal occlusion using a 1.0-mm fetoscope and prenatal expectant management in severe congenital diaphragmatic hernia. Fetal Diagn Ther. 2011;29(1): Ruano R, Yoshisaki CT, da Silva MM, et al. A randomized controlled trial of fetal endoscopic tracheal occlusion versus postnatal management of severe isolated congenital diaphragmatic hernia. Ultrasound Obstet Gynecol Jan;39(1):20-7. Salomon LJ, Ortqvist L, Aegerter P, et al. Long-term developmental follow-up of infants who participated in a randomized clinical trial of amniocentesis vs laser photocoagulation for the treatment of twin-to-twin transfusion syndrome. Am J Obstet Gynecol Nov;203(5):444.e1-7. Saura L, Castanon M, Prat J, et al. Impact of fetal intervention on postnatal management of 15
16 congenital diaphragmatic hernia. Eur J Pediatr Surg Dec;17(6): Selamet Tierney ES, Wald RM, et al. Changes in left heart hemodynamics after technically successful in-utero aortic valvuloplasty. Ultrasound Obstet Gynecol Oct;30(5): Senat MV, Deprest J, Boulvain M, et al. Endoscopic laser surgery versus serial amnioreduction for severe twin-to-twin transfusion syndrome. N Engl J Med. 2004; Jul;351(2): Society for Maternal-Fetal Medicine (SMFM), Simpson LL. Twin-twin transfusion syndrome. Am J Obstet Gynecol. 2013; Jan;208(1):3-18. Sydorak R, Harrison M. Congenital diaphragmatic hernia: advances in prenatal therapy. Clin Perinatol. 2003;30(3): Tan TY, Sepulveda W. Acardiac twin: a systematic review of minimally invasive treatment modalities. Ultrasound Obstet Gynecol. 2003; Oct;22(4): Tsao K, Feldstein VA, Albanese CT, et al. Selective reduction of acardiac twin by radiofrequency ablation. Am J Obstet Gynecol Sep;187(3): Tulzer G, Arzt W, Franklin R, et al. Fetal pulmonary valvuloplasty for critical pulmonary stenosis or atresia with intact septum. Lancet. 2002;360(9345): Tworetzky W, Wilkins-Haug L, et al. Balloon dilation of severe aortic stenosis in the fetus: potential for prevention of hypoplastic left heart syndrome: candidate selection, technique, and results of successful intervention. Circulation. 2004; Oct ;110(15): van Gemert MJ, Umur A, Tijssen JG, Ross MG. Twin-twin transfusion syndrome: etiology, severity and rational management. Curr Opin Obstet Gynecol. 2001; Apr;13(2): Vida VL, Bacha EA, Larrazabal A, et al. Hypoplastic left heart syndrome with intact or highly restrictive atrial septum: surgical experience from a single center. Ann Thorac Surg. 2007; Aug;84(2): Walsh WF, Chescheir NC, Gillam-Krakauer M, et al. Maternal-fetal surgical procedures. Technical Brief No. 5. (Prepared by the Vanderbilt Evidence-based Practice Center under Contract No ) AHRQ Publication No. 10(11)-EHC059-EF. Rockville, MD: Agency for Healthcare Research and Quality. April WAPM Consensus Group on Twin-to-Twin Transfusion, Baschat A, Chmait RH, Deprest J, Gratacós E, et al. Twin-to-twin transfusion syndrome (TTTS). J Perinat Med. 2011;39(2): Welsh A, Agarwal S, Kumar S, et al. Fetal cystoscopy in the management of fetal obstructive uropathy: experience in a single European centre. Prenat Diagn. 2003(13): POLICY HISTORY/REVISION INFORMATION Date 05/01/2015 Action/Description Updated supporting information to reflect the most current description of services, clinical evidence, and references; no change to coverage rationale or lists of applicable codes Archived previous policy version 2014T0035M 16
Clinical Policy Title: Home uterine activity monitoring
 Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being
 Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. [email protected]
Universal Fetal Cardiac Ultrasound At the Heart of Newborn Well-being Optimizes detection of congenital heart disease (chd) in the general low risk obstetrical population Daniel J. Cohen, M.D. [email protected]
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Feeding in Infants with Complex Congenital Heart Disease. Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014
 Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
Feeding in Infants with Complex Congenital Heart Disease Rachel Torok, MD Southeastern Pediatric Cardiology Society Conference September 6, 2014 Objectives Discuss common feeding issues in patients with
Neural tube defects: open spina bifida (also called spina bifida cystica)
 Screening Programmes Fetal Anomaly Neural tube defects: open spina bifida (also called spina bifida cystica) Information for health professionals Publication date: April 2012 Review date: April 2013 Version
Screening Programmes Fetal Anomaly Neural tube defects: open spina bifida (also called spina bifida cystica) Information for health professionals Publication date: April 2012 Review date: April 2013 Version
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Fetal Prognosis in Varix of the Intrafetal Umbilical Vein
 Fetal Prognosis in Varix of the Intrafetal Umbilical Vein Waldo Sepulveda, MD, Antonio Mackenna, MD, Jorge Sanchez, MD, Edgardo Corral, MD, Eduardo Carstens, MD To assess the clinical significance of varix
Fetal Prognosis in Varix of the Intrafetal Umbilical Vein Waldo Sepulveda, MD, Antonio Mackenna, MD, Jorge Sanchez, MD, Edgardo Corral, MD, Eduardo Carstens, MD To assess the clinical significance of varix
Delivery Planning for the Fetus with Congenital Heart Disease
 Delivery Planning for the Fetus with Congenital Heart Disease Mar y T. Donofrio MD, FAAP, FACC, FASE Director of the Fetal Heart Program Children s National Medical Center Washington DC Objectives Review
Delivery Planning for the Fetus with Congenital Heart Disease Mar y T. Donofrio MD, FAAP, FACC, FASE Director of the Fetal Heart Program Children s National Medical Center Washington DC Objectives Review
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS
 ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
ELSO GUIDELINES FOR TRAINING AND CONTINUING EDUCATION OF ECMO SPECIALISTS PURPOSE The "" is a document developed by the Extracorporeal Life Support Organization (ELSO) as a reference for current and future
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Provider Notification Obstetrical Billing
 Provider Notification Obstetrical Billing Date of Notification September 1, 20 Revision Date September 17, 2015 Plans Affected Mercy Care Plan and Mercy Care Long Term Care Plan Referrals As outlined in
Provider Notification Obstetrical Billing Date of Notification September 1, 20 Revision Date September 17, 2015 Plans Affected Mercy Care Plan and Mercy Care Long Term Care Plan Referrals As outlined in
UMBILICAL CORD BLOOD HARVESTING & STORAGE
 Protocol: TRP009 Effective Date: October 14, 2013 UMBILICAL CORD BLOOD HARVESTING & STORAGE Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 BACKGROUND... 2 CLINICAL EVIDENCE...
Protocol: TRP009 Effective Date: October 14, 2013 UMBILICAL CORD BLOOD HARVESTING & STORAGE Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE... 1 BACKGROUND... 2 CLINICAL EVIDENCE...
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Epidemiology 521. Epidemiology of Maternal and Child Health Problems. Winter / Spring, 2010
 Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Extended MPH Degree Program School of Public Health Department of Epidemiology University of Washington Epidemiology 521 Epidemiology of Maternal and Child Health Problems Winter / Spring, 2010 Instructor:
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Neural Tube Defects - NTDs
 Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
Neural Tube Defects - NTDs Introduction Neural tube defects are also known as NTDs. They happen when the spine and brain do not fully develop while the fetus is forming in the uterus. Worldwide, there
OBSTETRICAL POLICY. Page
 OBSTETRICAL POLICY REIMBURSEMENT POLICY Policy Number: ADMINISTRATIVE 200.14 T0 Effective Date: April 1, 2016 Table of Contents APPLICABLE LINES OF BUSINESS/PRODUCTS... APPLICATION... OVERVIEW... REIMBURSEMENT
OBSTETRICAL POLICY REIMBURSEMENT POLICY Policy Number: ADMINISTRATIVE 200.14 T0 Effective Date: April 1, 2016 Table of Contents APPLICABLE LINES OF BUSINESS/PRODUCTS... APPLICATION... OVERVIEW... REIMBURSEMENT
1-1 THE NERVOUS SYSTEM
 C A S E S T U D Y 1 : N e w b o r n Adapted from Thomson Delmar Learning s Case Study Series: Pediatrics, by Bonita E. Broyles, RN, BSN, MA, PhD. Copyright 2006 Thomson Delmar Learning, Clifton Park, NY.
C A S E S T U D Y 1 : N e w b o r n Adapted from Thomson Delmar Learning s Case Study Series: Pediatrics, by Bonita E. Broyles, RN, BSN, MA, PhD. Copyright 2006 Thomson Delmar Learning, Clifton Park, NY.
Prenatal screening and diagnostic tests
 Prenatal screening and diagnostic tests Contents Introduction 3 First trimester routine tests in the mother 3 Testing for health conditions in the baby 4 Why would you have a prenatal test? 6 What are
Prenatal screening and diagnostic tests Contents Introduction 3 First trimester routine tests in the mother 3 Testing for health conditions in the baby 4 Why would you have a prenatal test? 6 What are
AMBULANCE SERVICES. Page
 AMBULANCE SERVICES COVERAGE DETERMINATION GUIDELINE Guideline Number: CDG.001.03 Effective Date: June 1, 2015 Table of Contents COVERAGE RATIONALE... DEFINITIONS. APPLICABLE CODES... REFERENCES... HISTORY/REVISION
AMBULANCE SERVICES COVERAGE DETERMINATION GUIDELINE Guideline Number: CDG.001.03 Effective Date: June 1, 2015 Table of Contents COVERAGE RATIONALE... DEFINITIONS. APPLICABLE CODES... REFERENCES... HISTORY/REVISION
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
Prenatal Diagnosis of Congenital Heart Disease
 Prenatal Diagnosis of Congenital Heart Disease Pei-NiJone, MD a, Kenneth O. Schowengerdt, Jr., MD b, * KEYWORDS Fetal echocardiography Prenatal diagnosis Neonatal heart disease Fetal echocardiography,
Prenatal Diagnosis of Congenital Heart Disease Pei-NiJone, MD a, Kenneth O. Schowengerdt, Jr., MD b, * KEYWORDS Fetal echocardiography Prenatal diagnosis Neonatal heart disease Fetal echocardiography,
Priya Rajan, MD Northwestern University September 13, 2013
 Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Maj Alison Baum. R3, Nellis FMR
 Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
SWISS SOCIETY OF NEONATOLOGY. Umbilical cord complications in two subsequent pregnancies
 SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
echocardiography practice and try to determine the ability of each primary indication to identify congenital heart disease. Patients and Methods
 29 ABNORMAL CARDIAC FINDINGS IN PRENATAL SONOGRAPHIC EXAMINATION: AN IMPORTANT INDICATION FOR FETAL ECHOCARDIOGRAPHY? RIMA SAMI BADER Aim: The present study was conducted to evaluate the most common indications
29 ABNORMAL CARDIAC FINDINGS IN PRENATAL SONOGRAPHIC EXAMINATION: AN IMPORTANT INDICATION FOR FETAL ECHOCARDIOGRAPHY? RIMA SAMI BADER Aim: The present study was conducted to evaluate the most common indications
8/13/2014. Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature. Delayed Cord Clamping
 8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
Pregnancy and Substance Abuse
 Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Specialty Excellence Award and America s 100 Best Hospitals for Specialty Care 2013-2014 Methodology Contents
 Specialty Excellence Award and America s 100 Best Hospitals for Specialty Care 2013-2014 Methodology Contents Introduction... 2 Specialty Excellence Award Determination... 3 America s 100 Best Hospitals
Specialty Excellence Award and America s 100 Best Hospitals for Specialty Care 2013-2014 Methodology Contents Introduction... 2 Specialty Excellence Award Determination... 3 America s 100 Best Hospitals
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Optional Tests Offered Before and During Pregnancy
 Plano Women s Healthcare Optional Tests Offered Before and During Pregnancy Alpha-Fetoprotein Test (AFP) and Quad Screen These are screening tests that can assess your baby s risk of having such birth
Plano Women s Healthcare Optional Tests Offered Before and During Pregnancy Alpha-Fetoprotein Test (AFP) and Quad Screen These are screening tests that can assess your baby s risk of having such birth
REHABILITATION SERVICES (OUTPATIENT)
 REHABILITATION SERVICES (OUTPATIENT) Protocol: MSC028 Effective Date: March 1, 2016 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 2 APPLICABLE CODES... 4 REFERENCES... 7 POLICY
REHABILITATION SERVICES (OUTPATIENT) Protocol: MSC028 Effective Date: March 1, 2016 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 2 APPLICABLE CODES... 4 REFERENCES... 7 POLICY
British Association of Perinatal Medicine. The Management of Babies born Extremely Preterm at less than 26 weeks of gestation
 Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
Arch Dis Child - FNN Online First:Published on October 6, 2008 as 10.1136/adc.2008.143321 British Association of Perinatal Medicine The Management of Babies born Extremely Preterm at less than 26 weeks
ELSO GUIDELINES FOR ECMO CENTERS
 ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
ELSO GUIDELINES FOR ECMO CENTERS PURPOSE These guidelines developed by the Extracorporeal Life Support Organization, outline the ideal institutional requirements needed for effective use of extracorporeal
Evaluation and Follow-up of Fetal Hydronephrosis
 Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
Congenital heart defects
 CONGENITAL ANOMALY REGISTER & INFORMATION SERVICE COFRESTR ANOMALEDDAU CYNHENID Congenital heart defects Cardiovascular defects are by far the commonest major group of congenital anomalies. Development
CONGENITAL ANOMALY REGISTER & INFORMATION SERVICE COFRESTR ANOMALEDDAU CYNHENID Congenital heart defects Cardiovascular defects are by far the commonest major group of congenital anomalies. Development
Facts about Congenital Heart Defects
 Facts about Congenital Heart Defects Joseph A. Sweatlock, Ph.D., DABT New Jersey Department of Health Early Identification & Monitoring Program Congenital heart defects are conditions that are present
Facts about Congenital Heart Defects Joseph A. Sweatlock, Ph.D., DABT New Jersey Department of Health Early Identification & Monitoring Program Congenital heart defects are conditions that are present
CHLAMYDIA SCREENING IN WOMEN
 CHLAMYDIA SCREENING IN WOMEN APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE What screening should be done? NCQA ACCEPTED CODES DOCUMENTATION
CHLAMYDIA SCREENING IN WOMEN APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE What screening should be done? NCQA ACCEPTED CODES DOCUMENTATION
Preconception Clinical Care for Women Medical Conditions
 Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Non-surgical treatment of severe varicose veins
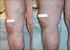 Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Long-Term Prognosis of Pregnancies Complicated by Slow Embryonic Heart Rates in the Early First Trimester
 Long-Term Prognosis of Pregnancies Complicated by Slow Embryonic Heart Rates in the Early First Trimester Peter M. Doubilet, MD, PhD, Carol B. Benson, MD, Jeanne S. Chow, MD Slow embryonic heart rates
Long-Term Prognosis of Pregnancies Complicated by Slow Embryonic Heart Rates in the Early First Trimester Peter M. Doubilet, MD, PhD, Carol B. Benson, MD, Jeanne S. Chow, MD Slow embryonic heart rates
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
The Patterns and Public Health Impact of Heart Defects in Texas Pediatric Cardiac Care Conference VI Dell Children s Medical Center, Feb.
 The Patterns and Public Health Impact of Heart Defects in Texas Pediatric Cardiac Care Conference VI Dell Children s Medical Center, Feb. 7-8, 2013 Mark Canfield, Ph.D. Manager, Birth Defects Epidemiology
The Patterns and Public Health Impact of Heart Defects in Texas Pediatric Cardiac Care Conference VI Dell Children s Medical Center, Feb. 7-8, 2013 Mark Canfield, Ph.D. Manager, Birth Defects Epidemiology
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Cardiac Rehabilitation (Outpatient Phase II) Corporate Medical Policy. Medical Policy
 Cardiac Rehabilitation (Outpatient Phase II) Corporate Medical Policy File name: Cardiac Rehabilitation (Outpatient Phase II) File code: UM.REHAB.04 Origination: 08/1994 Last Review: 08/2011 Next Review:
Cardiac Rehabilitation (Outpatient Phase II) Corporate Medical Policy File name: Cardiac Rehabilitation (Outpatient Phase II) File code: UM.REHAB.04 Origination: 08/1994 Last Review: 08/2011 Next Review:
Fetal Therapy Center. Phone: 305-585-6636 Fax: 305-325-1282 www.uhealthobgyn.com www.jhsmiami.org AMNIOPATCH INFORMATION PACKET
 Fetal Therapy Center Phone: 305-585-6636 Fax: 305-325-1282 www.uhealthobgyn.com www.jhsmiami.org AMNIOPATCH INFORMATION PACKET 2 AMNIOPATCH FOR TREATMENT OF PREVIABLE PREMATURE RUPTURE OF MEMBRANES Premature
Fetal Therapy Center Phone: 305-585-6636 Fax: 305-325-1282 www.uhealthobgyn.com www.jhsmiami.org AMNIOPATCH INFORMATION PACKET 2 AMNIOPATCH FOR TREATMENT OF PREVIABLE PREMATURE RUPTURE OF MEMBRANES Premature
FAMILY PLANNING AND PREGNANCY
 FAMILY PLANNING AND PREGNANCY Decisions about family planning can be difficult and very emotional when one of the prospective parents has a genetic disorder, such as Marfan syndrome. Before making any
FAMILY PLANNING AND PREGNANCY Decisions about family planning can be difficult and very emotional when one of the prospective parents has a genetic disorder, such as Marfan syndrome. Before making any
Applications of Doppler Ultrasound in Fetal Growth Assessment. David Cole
 Applications of Doppler Ultrasound in Fetal Growth Assessment David Cole Aims The aim of this presentation is to consider the use of Doppler ultrasound to investigate and monitor those pregnancies at risk
Applications of Doppler Ultrasound in Fetal Growth Assessment David Cole Aims The aim of this presentation is to consider the use of Doppler ultrasound to investigate and monitor those pregnancies at risk
PANNICULECTOMY & BODY CONTOURING PROCEDURES
 COVERAGE DETERMINATION GUIDELINE PANNICULECTOMY & BODY CONTOURING PROCEDURES Guideline Number: CDG.014.05 Effective Date: December 1, 2015 Table of Contents COVERAGE RATIONALE... DEFINITIONS. APPLICABLE
COVERAGE DETERMINATION GUIDELINE PANNICULECTOMY & BODY CONTOURING PROCEDURES Guideline Number: CDG.014.05 Effective Date: December 1, 2015 Table of Contents COVERAGE RATIONALE... DEFINITIONS. APPLICABLE
Corporate Reimbursement Policy
 Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Cerebral Palsy. In order to function, the brain needs a continuous supply of oxygen.
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Patient information on soft markers
 Patient information on soft markers Before you read this section remember the following important points. The vast majority of babies with soft markers are normal. Soft markers are frequently seen in healthy
Patient information on soft markers Before you read this section remember the following important points. The vast majority of babies with soft markers are normal. Soft markers are frequently seen in healthy
CONGENITAL HEART DISEASE
 CONGENITAL HEART DISEASE Introduction Congenital heart disease (CHD) is the most common congenital disorder in newborns [1]. Due to definitional issues, there are large variations in prevalence estimates.
CONGENITAL HEART DISEASE Introduction Congenital heart disease (CHD) is the most common congenital disorder in newborns [1]. Due to definitional issues, there are large variations in prevalence estimates.
Cerebral Palsy An Expensive Enigma
 Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Safe and Effective Surgery for Endometriosis Including Detection and Intervention for Ovarian Cancer
 Safe and Effective Surgery for Endometriosis Including Detection and Intervention for Ovarian Cancer Camran Nezhat,, MD, FACOG, FACS Stanford University Medical Center Center for Special Minimally Invasive
Safe and Effective Surgery for Endometriosis Including Detection and Intervention for Ovarian Cancer Camran Nezhat,, MD, FACOG, FACS Stanford University Medical Center Center for Special Minimally Invasive
Certified Professional Midwives Caring for Mothers and Babies in Virginia
 Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Cerebral Palsy. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com nr200105 Last reviewed: 06/17/2014 1
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Cerebral palsy, neonatal death and stillbirth rates Victoria, 1973-1999
 Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal. Drugs for the treatment of pulmonary arterial hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Drugs for the treatment of Remit / Appraisal objective: Final scope To appraise the clinical and cost effectiveness of
Ultrasound Billing CPT Codes Summary and Notes
 Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
The position of hysteroscopy in current fertility practice is under debate.
 The position of hysteroscopy in current fertility practice is under debate. The procedure is well tolerated. No consensus on effectiveness of HSC in improving prognosis of subfertile women. systematic
The position of hysteroscopy in current fertility practice is under debate. The procedure is well tolerated. No consensus on effectiveness of HSC in improving prognosis of subfertile women. systematic
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
Steven J. Yakubov, MD FACC For the CoreValve US Clinical Investigators
 Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
Long-Term Outcomes Using a Self- Expanding Bioprosthesis in Patients With Severe Aortic Stenosis Deemed Extreme Risk for Surgery: Two-Year Results From the CoreValve US Pivotal Trial Steven J. Yakubov,
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
Chapter 3: Healthy Start Risk Screening
 Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
Introduction Healthy Start legislation requires that all pregnant women and infants be offered screening for risk factors that may affect their pregnancy, health, or development. The prenatal and infant
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014
 CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE
 CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
CROSS HEALTH CARE BOUNDARIES MATERNITY CLINICAL GUIDELINE Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Obstetric Early Warning Score Guideline Implementation
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates
 Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Diagnosis Codes for Pregnancy and Complications of Pregnancy
 This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions?
 Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions? AFSHAN HAMEED, MD, FACOG, FACC Associate Clinical Professor Maternal Fetal Medicine and Cardiology University
Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions? AFSHAN HAMEED, MD, FACOG, FACC Associate Clinical Professor Maternal Fetal Medicine and Cardiology University
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013. Reference: NHSCB/A09/PS/b
 Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Clinical Commissioning Policy Statement: Percutaneous mitral valve leaflet repair for mitral regurgitation April 2013 Reference: NHS Commissioning Board Clinical Commissioning Policy Statement: Percutaneous
Prognosis of Very Large First-Trimester Hematomas
 Case Series Prognosis of Very Large First-Trimester Hematomas Juliana Leite, MD, Pamela Ross, RDMS, RDCS, A. Cristina Rossi, MD, Philippe Jeanty, MD, PhD Objective. The aim of this study was to evaluate
Case Series Prognosis of Very Large First-Trimester Hematomas Juliana Leite, MD, Pamela Ross, RDMS, RDCS, A. Cristina Rossi, MD, Philippe Jeanty, MD, PhD Objective. The aim of this study was to evaluate
Effective Date: March 2, 2016
 Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
ABSTRACT LABOR AND DELIVERY
 ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
Alcohol and drugs Be proactive
 Alcohol and drugs Be proactive PREGNANCY: a critical time to take care of yourself and your future baby Pregnant women must often change certain daily habits and are bombarded with recommendations from
Alcohol and drugs Be proactive PREGNANCY: a critical time to take care of yourself and your future baby Pregnant women must often change certain daily habits and are bombarded with recommendations from
surg urin Surgery: Urinary System 1
 Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
