ADEA Clinical Recommendations. Subcutaneous Injection Technique for Insulin and Glucagon-like Peptide 1
|
|
|
- Elizabeth Simpson
- 8 years ago
- Views:
Transcription
1 ADEA Clinical Recommendations Subcutaneous Injection Technique for Insulin and Glucagon-like Peptide 1
2 Published 2011 by the Australian Diabetes Educators Association ABN Chifley Health and Wellbeing Hub Unit 6/70 Maclaurin Cres Chifley ACT 2606 ISBN Agency Thorpe & Bowker Australian Diabetes Educators Association ADEA Clinical Recommendations Subcutaneous Injection Technique for Insulin and Glucagon-Like Peptide 1 ISBN Australian Diabetes Educators Association All Rights Reserved. No part of this publication may be reproduced, stored or transmitted, except as permitted by the Australian Copyright Act 1968, without the prior permission of the publisher. Although the publisher has taken every care to ensure the accuracy of the professional, clinical and technical components of this publication, it accepts no responsibility for any loss or damage suffered by any person as a result of following the procedures described or acting upon information set out in this publication. The publisher reminds readers that the information in this publication is no substitute for individual, medical and/or nursing assessment and treatment by professional staff.
3 Foreword Correct injection technique is paramount for optimal control of diabetes, and the following recommendations are based on the latest research in the delivery of injected diabetes medicines, especially insulin. There is always a fear associated with injections, and the ultimate aim is to improve the ease, comfort, and accuracy of insulin delivery. Diabetes educators are very aware of these fears and concerns when teaching clients, their families, carers and other health professionals how to inject insulin or glucagon-like peptide-1. Some 20 years ago insulin pen devices were first made available in Australia and have since revolutionized the way insulin is injected. Since that time, many new and innovative devices have been developed, which has assisted many people with diabetes to become more receptive and confident to self-inject. Insulin syringes and pen needles are available in different dimensions and lengths, and research has been carried out to identify which needle size, technique and site, would result in optimal absorption of injectable diabetes medicines. Expert panels throughout the world have reviewed such studies and developed best practice clinical guidelines that address the many components of education and assessment required to teach and support people injecting diabetes medicines. As with any process of clinical review, changes to established practice occur. The ADEA Clinical Recommendations for Subcutaneous Injection Technique for Insulin and Glucagon-like Peptide-1 identifies a number of broad clinical issues including optimal needle length and angle of needle insertion for children/adolescents and adults of varying anatomical size. These clinical recommendations reinforce the importance of documenting the process of teaching and reviewing injection technique. Correct injection technique using the appropriate size needle is not only important for glycaemic control, it has a direct impact on client self confidence and acceptance of injectable medicines. On behalf of the ADEA Clinical Practice Committee who was pivotal in their development, I hope these clinical recommendations become a useful working document assisting all diabetes educators to reflect on their current practice and promote the use of evidence based practice when using injectable diabetes medicines. Nuala Harkin ADEA President 2
4 Definition of Terms GLP-1 Mimetic At the time of this report only one GLP-1 mimetic agent is available in Australia, exenatide. This GLP-1 mimetic can only be administrated using a disposable pen device which requires a subcutaneous injection technique using the same principles of subcutaneous insulin injection technique. Lipoatrophy Lipoatrophy is the breakdown of subcutaneous fat tissue resulting from repeated insulin injections at the same anatomical site. A depression or sunken look to the affected can be observed. Lipohypertrophy Lipohypertrophy is an area of thickened subcutaneous tissue resulting from repeated injections of insulin using syringes and pen devices into an area of tissue where a nonrotation technique of injection sites is not employed. Lipohypertrophy may not be detected by visual inspection. However, when palpated the affected area cannot be pinched together. Lipohypertrophy can further exacerbate the problems associated with insulin absorption. Insulin injected into areas of lipohypertrophy may cause delayed insulin absorption and could thus contribute to erratic blood glucose levels. Skin fold lift A skin fold lift is made using the thumb and index or middle finger to gently lift subcutaneous tissue away from the muscle layer to reduce the risk of administering the medicine intramuscularly. With shorter needles, often the creation of a skin fold lift is not required. 3
5 Acknowledgments The development of the ADEA Clinical Recommendations for Subcutaneous Injection Technique for Insulin and Glucagon-like Peptide 1 has been undertaken by the Australian Diabetes Educators Association Clinical Practice Committee. The support of Becton, Dickinson and Company in the production is gratefully acknowledged. This project was undertaken by the ADEA Clinical Practice Committee. Committee Michelle Robins (Chair) Carol De Groot Denise Smith Lyndon Homeming Mark Coles Melissa Armstrong Wendy Bryant The ADEA wishes to acknowledge the work of The Third Injection Technique Workshop in Athens (TITAN) for its published guidelines titled New injection recommendations for patients with diabetes. In addition, a literature search, review and grading was undertaken to identify any additional studies since the publication of the TITAN recommendations in September We would like to thank Lhawang Ugyel from ADEA National Office for this contribution. 4
6 Contents The ADEA recommends:... 7 Purpose of clinical recommendations... 8 Background... 8 Clinical recommendations... 9 Children Very slim adults Adults of normal weight Adults who are overweight or obese Additional considerations References
7 ADEA Clinical Recommendations for Subcutaneous Injection Technique for Insulin and Glucagon-Like Peptide 1 The Australian Diabetes Educators Association (ADEA) promotes the use of evidence and consensus based practice within all aspects of diabetes education and care, including when using injectable diabetes medicines. The ADEA recognises that incomplete and/or inaccurate instruction and education on injectable medicines and injection technique can result in diabetes medicines designed to be administered into subcutaneous tissue, being injected intramuscularly. This may cause an alteration in the action of the medication and an increased risk of pain or discomfort, bruising or bleeding at the injection site, as well as the person with diabetes being at risk of experiencing a serious adverse event from an alteration in the onset and action of the medicine. These clinical recommendations address the injection technique for pen devices and syringes for insulin and glucagon-like 1 peptide (GLP-1) mimetic. This document does not address the administration of glucagon which is normally administered intramuscularly except in children aged less than 5 years of age, 1 nor does it focus on technical issues associated with continuous subcutaneous insulin infusion devices (CSII). The ADEA wishes to acknowledge the work of The Third Injection Technique Workshop in Athens (TITAN) for its published guidelines titled new injection recommendations for patients with diabetes. 2 In addition, a literature search, review and grading was undertaken to identify any additional studies since the publication of the TITAN recommendations in September
8 The ADEA recommends: People with diabetes, their relevant family members, carers and health care providers receive quality education and instruction that encompasses contemporary evidence and consensus based principles of injection technique from diabetes educators. Diabetes educators should document all components of assessment and education for the administration of injectable diabetes medicines including the psychological status of the patient when initiating insulin therapy, site of delivery, site rotation, whether using a skin fold lift technique is required, the size and angle of insertion of the needle used, pen device assembly and priming as per individual manufacturers instructions, duration injecting device is kept insitu following the administration of the medicine and safe disposal of sharps and injecting materials. Shorter length needles 4, 5 and 6mm are generally recommended for both children/adolescents and adults including obese patients and have been shown to provide equivalent glycaemic control as needles of 8 and 12.7mm length. A 45 degree angle should be used when administering insulin with a syringe when using a needle length 8mm. Injectable diabetes medicines should not be administered in areas of scarring or hypertrophy or through clothing and diabetes educators need to be aware of the factors that can affect efficacy of injected medicines. Different diabetes injectable medicines have specific recommendations in relation to the preferred site of injection. The size and angle of insertion of the needle used to inject a diabetes medicine is consonant to the age and size of the person with diabetes, the amount of subcutaneous and muscle tissue mass available at the injection site and use of a lifted skin fold where appropriate. All people receiving education and instruction about injectable diabetes medicines are taught the correct technique for lifting a skin fold. Regular reviewing of injection technique and injection site inspection are undertaken and documented by diabetes educators and are considered as integral to the assessment for all people with diabetes requiring injectable diabetes medicines. As part of quality improvement, management activities and risk reduction strategies, regular review of health care providers knowledge and skills pertaining to injecting diabetes medicines is undertaken by diabetes educators. Appropriate policies and procedures should be developed for health care facilities and education strategies and programs implemented and evaluated to ensure compliance. Additional consideration should be afforded to issues that include the priming of pen devices, re-suspension of cloudy insulin, duration pen devices are left insitu following delivery of medicine, disinfection of skin and the washing of hands prior to injecting, injection location in pregnancy, insulin leakage, when to remove pen needles and where additional information can be sought. 7
9 Purpose of clinical recommendations The purpose of these clinical recommendations is to: Outline the considerations required when determining the site for injecting a diabetes medicine, the size and insertion angle of needles to be used, and whether the technique of lifting a skin fold lift as part of injecting is required. Identify factors that can affect the efficacy of the medicine injected and the degree of discomfort experienced by the person with diabetes. Highlight that the review of injection technique and injection site inspections are integral to the assessment of the diabetes self-management skills for the person with diabetes. Focus on the need to teach and evaluate the understanding and application of the principles that underpin correct injection techniques and factors that effect the efficacy of pharmacological actions to all people: the person with diabetes, family members, carers and health care providers directly engaged in the administration of injectable diabetes medicines. Reinforce the importance of documentation of assessment and teaching activities involved with injectable diabetes medicines. Minimise adverse outcomes. Background The instruction of correct injection technique is a core function for diabetes educators. Education in correct injection technique undertaken by diabetes educators is provided to people with diabetes, their family members, carers and to other health care providers. People with diabetes requiring insulin therapy may require four or more injections each day. For the purpose of this document, injectable diabetes medicines include insulin and glucagon-like peptide 1 (GLP-1) mimetic. In the future, other classes of agents to treat diabetes may also be administered subcutaneously or intramuscularly. With an increase in the number of new medicines and pen devices released, a number of key overarching principles exist. These principles address issues such as the amount of subcutaneous or muscle tissue available at a potential injection site, the length and angle of needle to be inserted and the use of a skin fold lift as part of the injection process. Incomplete and/or inaccurate instruction on injection technique can result in diabetes medicines administered incorrectly and may cause an alteration in the action of the medication and an increased risk of pain or discomfort, bruising or bleeding at the site to the person with diabetes. Fundamentally, insulin and GLP-1 mimetic agents are designed to be administered subcutaneously in order to attain the most consistent efficacy of their pharmacological actions. Glucagon has been developed to be injected into muscle tissue to maximise its effects on blood glucose levels, and although it can be administered in children under the age of 5 years subcutaneously, will not be addressed by these clinical recommendations. 2 8
10 Studies identified by the TITAN recommendations highlight that people with diabetes may not receive essential information pertaining to administration of diabetes medicines that include 2 : The injecting regimen. The choice and management of the devices used. The choice, care and self-examination of injection sites. Proper injection techniques (including site rotation, injection angle and use of skin fold lifting). Injection complications and how to avoid them. Optimal needle lengths. Safe disposal of sharps. Clinical recommendations People with diabetes, their relevant family members, carers and health care providers receive quality education and instruction that encompasses contemporary evidence and consensus based principles of injection technique from diabetes educators. Educating the person with diabetes, family members, carers or health care providers is a dynamic process. A number of issues need to be identified, addressed and evaluated including: The person s readiness and ability to learn. The person s understanding of the diabetes disease process. Physical or psychosocial factors affecting the ability to inject. Type of device best suited to the individual. The level of mastery and confidence. Willingness to undertake other aspects of diabetes self-management related to injectable diabetes medicines. Diabetes educators should document all components of assessment and education for the administration of injectable diabetes medicines including the psychological status of the patient when initiating insulin therapy, site of delivery, site rotation, whether using a skin fold lift technique is required, the size and angle of insertion of the needle used, pen device assembly and priming as per individual manufacturers instructions, duration injecting device is kept insitu following the administration of the medicine and safe disposal of sharps and injecting materials. The entire process of education must be documented. Formal and regular review of any preexisting injection knowledge and self-care practices should also be undertaken and documented where the person is already using injectable medicines. Knowledge and competency are assessed against education outcomes and documented. Traditionally pen needles have been recommended to be used at a 90 degree angle. In cases where there is insufficient adipose tissue for the needle length to ensure that a subcutaneous injection will occur, administration using a 45 degree angle maybe required and therefore will need to be documented by the diabetes educator. Shorter-length needles may be used at a 90 degree angle. 9
11 Shorter length needles 4, 5 and 6mm are generally recommended for both children/adolescents and adults including obese patients and have been shown to provide equivalent glycaemic control as needles of 8 and 12.7mm length. A 45 degree angle should be used when administering insulin with a syringe when using a needle length 8mm. Insulin syringes currently available in Australia range in needle length of 8mm, 12mm, 12.7mm and 13mm. 3 To ensure that insulin is not inadvertently administered intramuscularly, the use of a 45 degree to inject should be adopted for all syringes. There are additional considerations with the use of syringes when drawing up insulin and removing air bubbles. Unlike pen devices, a syringe can be removed following the completion of injecting without waiting ten seconds. 4 Different manufacturers produce syringe needles with varying widths; 29 gauge, 30 gauge and 31 gauge. The finer the gauge (higher the number), the smaller the diameter which may be helpful for patients experiencing discomfort during injecting. 5 Injectable diabetes medicines should not be administered in areas of scarring or hypertrophy or through clothing and diabetes educators need to be aware of the factors than can effect efficacy of injected medicines. Lipohypertrophy and lipoatrophy can occur when older and less purified insulin preparations are used, not rotating the sites of injecting by either repeatedly injecting in the same spot or using an area that is too small for effective rotation, or reusing needles. Such areas of tissue can be detected both visually and by palpation and can affect the absorption of insulin, which in turn can affect glycaemic control. 2 Any area of lipohypertrophy, inflammation, oedema or infection should be avoided as an injection site until resolved. 5 People with diabetes, their carers and health care providers should be taught an easy-tofollow rotation regimen with successive injections should be spaced at least 1cm from each other. The rotation regimen used by individual person with diabetes should be documented by the diabetes educator. When switching from previously used areas of lipohypertrophy to non-affected areas, a reduced insulin dose may need to be considered in conjunction with increased blood glucose testing. 5 Injecting through clothing means that neither the person injecting cannot see the injection process fully nor employ a skin fold lift if required, increasing the risk of a transdermal (intramuscular) injection and therefore is not recommended. 6 Patients should be instructed on how to self-examine their injection sites. 5 Different diabetes injectable medicines have specific recommendations in relation to the preferred site of injection. Rapid-acting insulin analogues can be given at any recommended injection site without significant effect on absorption rates. 7 Long-acting insulin analogues may also be injected at any recommended injection site, but should not be injected intramuscularly due to risk of severe hypoglycaemia. 8 The thigh and buttocks are the preferred site for NPH due to a slower absorption rate (and reduced risk of nocturnal hypoglycaemia), 9 and the abdomen 10
12 preferred for faster absorbing of regular human insulin. 10 Basal analogue insulin injected subcutaneously into the thigh followed by vigorous exercise has not shown any increased rate of absorption. 11 In elderly people with diabetes, the absorption rate of regular human insulin is slower and therefore will not produce a rapid post prandial effect. 12 Pending further studies, long-acting insulin analogues and GLP-1 mimetic agents should be administered in current established locations such as the abdomen or where sufficient fatty tissue is available the outer thighs. 13 When injecting rapid and long-acting analogue insulin, each injection should be administered within a different site, even if injected at different times during the day. 5 Massaging the injection site either before or after injecting could increase the rate of absorption of insulin and therefore is not generally recommended. 14 The size and insertion angle of the needle used to inject a diabetes medicine is consonant to the age and size of the person with diabetes, the amount of subcutaneous and muscle tissue mass available at the injection site and use of a lifted skin fold where appropriate. Several studies have identified that the thickness of subcutaneous tissue varies considerably according to age, body site, gender and body mass index (BMI). The thickness of the skin (epidermis and dermis), however does not vary greatly and is usually mm in thickness regardless of site, age, ethnic background, gender or BMI and rarely more than 3.0mm. 15, 16 Therefore people with a larger BMI do not necessarily need to use a longer needle. The absorption of regular insulin has been shown to be the same whether injected deep into subcutaneous fat with a long needle, or superficially with a short needle. 17 There is no medical reason for the use of needles greater than 8mm in length for any adult with diabetes regardless of their BMI; for children, needles longer than 6mm are generally not recommended, unless using a syringe with an 8mm needle. 2 If a person with diabetes wishes to continue using needles greater than 8mm in length, they should lift a skin fold or inject at a 45 degree angle to avoid inadvertently injecting into muscle. 18 Adults should use 4, 5 or 6mm needles using a 90 degree angle (especially the 4mm length), and rarely require the use of a skin fold lift Very slim people with diabetes and children should use 4 or 5mm needles, may require a skin fold lift, especially with 5mm needles. Further research is needed with respect to 4mm needles. Very slim people using 6mm needles should use 19, 23 either a skin fold lift or inject on a 45 degree angle. 11
13 Children Needle size Degree of injection angle Use of skinfold 4mm 90 May 5mm 45 or 90 Yes 6mm 45 or 90 Yes 8mm* 45 Yes >12mm^ 45 Yes * use for syringe only, preferable to use shorter needles when using pen needles ^ needle length discouraged in children Very slim adults Needle size Degree of injection angle Use of skinfold 4mm 90 May 5mm 45 or 90 Yes 6mm 45 or 90 Yes 8mm 45 Yes >12mm* 45 Yes *use of syringe only and discouraged August Review Date: August 2014
14 Adults of normal weight Needle size Degree of injection angle Use of skinfold 4mm 90 Rarely 5mm 90 Yes 6mm 90 Yes 8mm 45 Yes >12mm* 45 Yes *not generally recommended Adults who are overweight or obese Needle size Degree of injection angle Use of skinfold 4mm 90 No 5mm 90 No 6mm 90 No 8mm No >12mm* No May *not generally recommended All people receiving education and instruction about injectable diabetes medicines are taught the correct technique for lifting a skin fold. Prior to injecting, the injection site should be examined to determine whether lifting a skin fold is required in terms of the needle length employed. A skin fold lift is made using the thumb and index or middle finger that lifts subcutaneous tissue away from the muscle layer and reduces the risk of administering medicines intramuscularly. 18 This process should be done gently to avoid harsh handling of the area to minimise potential cause for skin blanching or pain, or inadvertently also lifting up muscle tissue. All people with diabetes, 13
15 their family members, carers and health care providers should be taught the correct technique for lifting a skin fold. Regular reviewing of injection technique and injection sites is undertaken and documented by diabetes educators and is considered as integral to the assessment for all people with diabetes requiring injectable diabetes medicines. This review should include the visual assessment and palpation of injection sites. Signs of bleeding and bruising maybe due to intramuscular administration. TITAN recommends review of injection sites and technique with each visit if possible and at the very least annually. 24 If blood glucose results recorded indicate a high variability without obvious explanation, review of injection sites and technique should form the basis of clinical enquiry. As part of quality improvement, management activities and risk reduction strategies, regular review of health care providers knowledge and skills pertaining to injecting diabetes medicines is undertaken by diabetes educators. Appropriate policies and procedures should be developed for health care facilities and education strategies and programs implemented and evaluated to ensure compliance. Syringes and pen needles are single use only. Recapping of needles should only be undertaken by the person with diabetes administering their own medicine. Needle stick injuries are common among health care providers, particularly when infection prevention procedures are not adhered to. Family members, carers and health care providers should not recap needles. Organisations should protect the person with diabetes, the public and staff from blood-borne pathogens by ensuring their specific infection prevention policies reflect best-practice and their employees receive the training and have access to the equipment to practice in accordance with these policies. 25 If the person with diabetes is unable to remove the pen needle from their injecting device (regardless of whether they are able to self-administer), health care providers should instead administer insulin using a syringe (note there is no provision to use a syringe for exenatide). 26 Retractable pen needles and syringes are available, with only one syringe manufacturer with National Diabetes Services Scheme subsidy at the time this document was developed. 3 Some health care facilities use specific sharps disposal containers that allow the safe unscrewing of a pen device needle to occur within the defines of the container. Under no circumstance should pen device needles and syringes be directly disposed into public rubbish. Rather all injectable diabetes medicines sharps must be discarded into an approved sharps container and taken to an approved sharps waste disposal agency, for example, the local council or shire. Pen devices and cartridges are for single person use only and should never be shared due to the risk of cross contamination, even if a fresh pen needle is used for each injection
16 Additional considerations Differences in pen devices pertaining to priming Manufacturers of pen devices for insulin and GLP-1 mimetics differ with respect to whether a priming process is required at the commencement of a new device or as part of every injection. Diabetes educators need to be cognisant of these individual differences in manufacturers instructions for the preparations of injection devices. Re-suspension of insulin Cloudy insulin (NPH and pre-mixed insulins) must be resuspended according to individual manufacturers instructions prior to every injection: this generally means gently tipping of the vial or pen 10 to 20 times. Time pen device is left insitu following injection As with priming of pen devices, the duration of time a pen device is left insitu following injecting varies between different manufacturers, but is usually at least 10 seconds. However counting past ten seconds maybe necessary for higher doses of insulin to minimise insulin backflow/leakage. 4 Disinfection of skin prior to injection Use of alcohol swabs to prepare the skin prior to injection is usually not required, however the application of soap and water to an injection site if unclean should occur. 2 Washing of hands prior to injecting Hands should be clean prior to injecting a diabetes medicine. 5 Injection location during pregnancy Pregnant women with diabetes should administer all injections into the abdomen using a raised skin fold, but avoiding areas close to the umbilicus during the third trimester is recommended. 28 Insulin leakage Studies in people with type 1 and type 2 diabetes using 4, 5, and 6mm needles indicate that needle length size does not impact on insulin leakage at the injection site and measured 4, 18, 21,22 leakage is very small as a percentage of the injected dose. Removal of the pen needle When using a pen device, the pen needle should be removed from the device immediately after administering the diabetes medicine. Pen needles left attached can allow for the contents of the pen device to leak out or allow air bubbles to enter the cartridge chamber leading to inaccurate dosing of subsequent injections. 4, 29 An additional consideration to 15
17 remove the pen needle after use is microbe contamination, present after a single use and amplified after repeated use. 30 Awareness of risk of using incorrect injection needle length occur at NDSS outlets and sub-agents Two documents currently exist on line to assist NDSS outlets and sub-agents in the 31, 32 awareness and risk of incorrect needle length. 16
18 References 1. Australian Medicines Handbook, Adelaide Frid A, Hirsch L, Gaspar R, Hicks D, Kreugel G, Liersch J, Letondeur C, Sauvanet J, Tubiana-Rufi N, Strauss K, et al. New injection recommendations for patients with diabetes. Diabetes and Metabolism. Special issue 2 September 2010;36:s3-s National Diabetes Services Scheme Order Form Annersten M, Frid A. Insulin pens dribble from the tip of the needle after injection. Practical Diabetes International. 2000;17: Diabetes Care in the UK. The First UK Injection Technique Recommendations October Flemming D, Jacover S, Vanderberg M, Fitzgerald J, Grunberger G. The safety of injecting insulin through clothing. Diabetes Care. 1997;20: Mudaliar S, Lindberg F, Joyce M, Beersden P, Strange P, Lin A, Henry R. Insulin aspart B28 asp-insulin: a fast-acting analog of human insulin: absorption kinetics and action profile compared with regular human insulin in healthy nondiabetic subjects. Diabetes Care. 1999;22: Vaag A, Handberg A, Lauritzen M, Henriksen J, Pedersen K, Beck-Nielsen H. Variation in absorption of NPH insulin due to intramuscular injection. Diabetes Care. 1990; 13: Henriksen J, Vaag A, Hansen I, Lauritzen M, Djurhuus M, Beck-Nielsen H. Absorption of NPH isophane insulin in resting diabetic patients; evidence for subcutaneous injection in the thigh as preferred site. Diabetic Medicine. 1991;8: Henriksen J, Djurhuus M, Vaag A, Thye-Ronn P, Knudsen D, Hother-Nielsen O, et al. Impact of injection sites for soluble insulin on glycemic control in type 1 (insulindependent) diabetic patient treated with a multiple insulin injection regimen. Diabetologica. 1993;36: Rajesh P, Luzio S, Dunseath G, Miles A, Hare B, Backx K, Pauvaday V, Owens D, et al. Effects of exercise on the absorption of insulin glargine in patients with type 1 diabetes. Diabetes Care. 2005;28(3): Clauson P, Linde B. Absorption of rapid-acting insulin in obese and non obese NIDDM patients. Diabetes Care. 1995;18: Byetta. Pen User Manual. Eli Lilly and Company, Danish Nurses Organization. Evidence-based Clinical Guidelines for Injection of Insulin for Adults with diabetes Mellitus 2 nd edition, December Gibney M, Arce C, Byron K, Hirsch L. Skin and subcutaneous adipose layer thickness in adults with diabetes at sites used for insulin injections: implications for needle length recommendations. Current Medical Research and Opinion. 2010;26: Thow J, Coulthard A, Home P. Insulin injection site tissue depths and localization of a simulated insulin bolus using a novel air contrast ultrasonographic technique in insulin treated diabetic subjects. Diabetic Medicine. 1992;9:
19 17. Frid A, Linde B. Intraregional differences in the absorption of unmodified insulin form the abdominal wall. Diabetic Medicine. 1992;9: Schwartz S, Hassman D, Shelmet J, Sieverw R, Weinstein R, Liang J, Lyness W. A multicentre, open-label, randomized, two-period crossover trial comparing glycemic control, satisfaction, and preference achieved with a 31 gauge x 6mm needle versus a 29 gauge x 12.7mm needle in obese patients with diabetes mellitus. Clinical Therapeutics. 2004;26: Birkebaek N, Solvig J, Hansen B, Jorgensen C, Smedegaard J, Christiansen J, et al. 4mm needle reduces the risk of intramuscular injections without increasing backflow to skin surface in lean diabetic children and adults. Diabetes Care. 2008;22;e Kreugel G, Keers J, Jongbloed A, Verweij-Gjaltema A, Wolffenbuttel B. The influence of needle length on glycemic control and patient preference in obese diabetic patients. Diabetes. 2009; 58:A Hirsch L, Gibney M, Albanese J, Qu S, Kassler-Taub K, Klaff L, Bailey T, et al. Comparative glycemic control, safety and patient ratings for a new 4mm x 32G insulin pen needle in adults with diabetes. Current Medical Research & Opinion. 2010;26: Wittman A, Kover J, Kralj N, Gasthaus K, Lerch H, Rommel M, Moses S, Hofmann F, et al. Insulin leakage value in relation to pen needle length and administered dose after subcutaneous injection. Diabetes Technology and Therapeutics. 2010;12: Strauss K. Insulin injection techniques. Practical Diabetes International. 1998;15: Seyoum B, Abdulkadir J. Systematic inspection of insulin injection sites for local complications related to incorrect injection technique. Tropical Doctor. 1996;26: National Health and Medical Research Council and Australian Commission on Safety and Quality in Healthcare. Australian Guidelines for the Prevention and Control of Infection in Healthcare trolguidelines2010.pdf 26. Centre for Healthcare Related Infection Surveillance and Prevention Le Floch J, Herbreteau C, Lange F, Perlemuter L. Biologic material in needles and cartridges after injection with a pen in diabetic people with diabetes. Diabetes Care. 1998;21: Engstrom L, Jinnerot H, Jonasson E. Thickness of subcutaneous fat tissue where pregnant diabetics inject their insulin an ultrasound study. IDF Meeting Mexico City, Chantelau E, Heinemann L, Roos D. Air bubbles in insulin pens. Lancet. 1989; 334: Misnikova I, Dreval A, Gubkina V, Rusanova E. The risk of repeated use of insulin pen needles in patients with Diabetes Mellitus. Journal of Diabetology. 2011;1: NDSS Fact Sheet For NDSS Sub-Agents: Risk of using the incorrect needle length November NDSS Fact Sheet: Risk of using the incorrect needle length cited research articles November
20 ADEA National Office: PO Box 163 Woden ACT 2606 Phone: Fax: inquiries@adea.com.au Proudly sponsored by
INSULIN INJECTION KNOW-HOW
 0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
UW MEDICINE PATIENT EDUCATION. Using Insulin. Basic facts about insulin and self-injection. What is insulin? How does diabetes affect the body?
 UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
INSULIN INJECTION KNOW-HOW
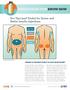 0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
PHARMACOTHERAPY HOW TO INJECT INSULIN. Living your life as normal as possible. www.lilly-pharma.de www.lilly-diabetes.de
 PHARMACOTHERAPY HOW TO INJECT INSULIN Living your life as normal as possible www.lilly-pharma.de www.lilly-diabetes.de In Germany about 1.9 million people with diabetes are being treated with insulin.
PHARMACOTHERAPY HOW TO INJECT INSULIN Living your life as normal as possible www.lilly-pharma.de www.lilly-diabetes.de In Germany about 1.9 million people with diabetes are being treated with insulin.
Gentle and safe injections. Tips and tricks for injecting insulin.
 Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Gentle and safe injections. Tips and tricks for injecting insulin. More freedom. More confidence. With mylife. Gentle and safe injections The correct injection technique The insulin is injected into the
Gentle and safe injections Tips and tricks for injecting insulin
 Gentle and safe injections Tips and tricks for injecting insulin More freedom. More confidence. With mylife. Tip 1 The pen needle that fits For achieving a good insulin dose effect it is essential to inject
Gentle and safe injections Tips and tricks for injecting insulin More freedom. More confidence. With mylife. Tip 1 The pen needle that fits For achieving a good insulin dose effect it is essential to inject
Updates in Insulin Injection Technique: Data and Recommendations
 Updates in Insulin Injection Technique: Data and Recommendations Maureen Mo Bressett, RPh, MSHA Senior Medical Science Liaison BD Medical Affairs: Diabetes Care Disclosures Maureen Bressett is an employee
Updates in Insulin Injection Technique: Data and Recommendations Maureen Mo Bressett, RPh, MSHA Senior Medical Science Liaison BD Medical Affairs: Diabetes Care Disclosures Maureen Bressett is an employee
Insulin Pens. Basic facts. What is insulin? What are the different types of insulin?
 UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
PATIENT INFORMATION. Medicine To Treat: D iabetes. What You Need to Know About. Insulin
 PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
Guidelines for Education and Training
 Aim These protocols aim to provide the necessary guidance to enable insulin to be initiated safely and effectively Objectives 1. To provide the suggested procedure for the initiation of insulin for people
Aim These protocols aim to provide the necessary guidance to enable insulin to be initiated safely and effectively Objectives 1. To provide the suggested procedure for the initiation of insulin for people
Guideline for the Administration of Insulin by Nursing Staff
 Guideline for the Administration of Insulin by Nursing Staff Aims and objectives In Lanarkshire the number of people with Diabetes on insulin treatment is growing, as both the population ages and people
Guideline for the Administration of Insulin by Nursing Staff Aims and objectives In Lanarkshire the number of people with Diabetes on insulin treatment is growing, as both the population ages and people
Getting started with Insulin Injections
 Getting started with Insulin Injections Table of Contents Introduction........................2 Insulin Injection Devices...............3 Blood Glucose Levels Hyperglycemia.....................15 Table
Getting started with Insulin Injections Table of Contents Introduction........................2 Insulin Injection Devices...............3 Blood Glucose Levels Hyperglycemia.....................15 Table
HED\ED:NS-BL 037-3rd
 HED\ED:NS-BL 037-3rd Insulin Insulin is produced by the beta cells in the islets of Langerhans in the pancreas. When glucose enters our blood, the pancreas should automatically excrete the right amount
HED\ED:NS-BL 037-3rd Insulin Insulin is produced by the beta cells in the islets of Langerhans in the pancreas. When glucose enters our blood, the pancreas should automatically excrete the right amount
Step-by-Step Patient Injection Guide
 Step-by-Step Patient Injection Guide 1 Your step-by-step guide to injection. 3 Table of Contents How your insulin works... 1 o Definitions to review Insulin action curves... 2 o Rapid-acting insulin o
Step-by-Step Patient Injection Guide 1 Your step-by-step guide to injection. 3 Table of Contents How your insulin works... 1 o Definitions to review Insulin action curves... 2 o Rapid-acting insulin o
Insulin Administration: What You Don t Know May Hurt Your Patient
 Insulin Administration: What You Don t Know May Hurt Your Patient Jaime A. Davidson, MD, FACP, MACE Clinical Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Jaime A. Davidson,
Insulin Administration: What You Don t Know May Hurt Your Patient Jaime A. Davidson, MD, FACP, MACE Clinical Professor of Internal Medicine UT Southwestern Medical Center Dallas, Texas Jaime A. Davidson,
Subcutaneous insulin. injection technique. Injection management CONTINUING PROFESSIONAL DEVELOPMENT
 By reading this article and writing a practice profile, you can gain ten continuing education points (CEPs). You have up to a year to send in your practice profile. Guidelines on how to write and submit
By reading this article and writing a practice profile, you can gain ten continuing education points (CEPs). You have up to a year to send in your practice profile. Guidelines on how to write and submit
Insulin. and diabetes. What is insulin? Who needs to inject insulin? Why must it be injected? What if I have to go on to insulin?
 Insulin What is insulin? and diabetes Insulin is a hormone made by special cells, called beta cells, in the pancreas. When we eat, insulin is released into the blood stream where it helps to move glucose
Insulin What is insulin? and diabetes Insulin is a hormone made by special cells, called beta cells, in the pancreas. When we eat, insulin is released into the blood stream where it helps to move glucose
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
An estimated 280 Australians develop diabetes every day. It is Australia s fastest-growing chronic disease.
 Diabetes and insulin Summary Even with the help of your doctor and diabetes nurse educator, it may take a while to find the right insulin dose to reduce your blood glucose to your target levels. Insulin
Diabetes and insulin Summary Even with the help of your doctor and diabetes nurse educator, it may take a while to find the right insulin dose to reduce your blood glucose to your target levels. Insulin
ON PENS AND NEEDLES A PRIMER ON INSULIN PENS AND PROPER INJECTION TECHNIQUES PETE KRECKEL, RPH
 ON PENS AND NEEDLES A PRIMER ON INSULIN PENS AND PROPER INJECTION TECHNIQUES PETE KRECKEL, RPH ON PENS AND NEEDLES - A PRIMER ON INSULIN PENS AND PROPER INJECTION TECHNIQUES ACTIVITY DESCRIPTION Insulin
ON PENS AND NEEDLES A PRIMER ON INSULIN PENS AND PROPER INJECTION TECHNIQUES PETE KRECKEL, RPH ON PENS AND NEEDLES - A PRIMER ON INSULIN PENS AND PROPER INJECTION TECHNIQUES ACTIVITY DESCRIPTION Insulin
Department of Health Commencing insulin therapy
 Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Lipohypertrophy - The Neglected Area of Concern in the much Talked about Diabetes
 International Journal of Diabetes Research 2015, 4(2): 38-42 DOI: 10.5923/j.diabetes.20150402.03 Lipohypertrophy - The Neglected Area of Concern in the much Talked about Diabetes Salahuddin Farooq Mohammed
International Journal of Diabetes Research 2015, 4(2): 38-42 DOI: 10.5923/j.diabetes.20150402.03 Lipohypertrophy - The Neglected Area of Concern in the much Talked about Diabetes Salahuddin Farooq Mohammed
Instructions for Use HUMALOG KwikPen insulin lispro injection (rdna origin)
 1 Instructions for Use HUMALOG KwikPen insulin lispro injection (rdna origin) Read the Instructions for Use before you start taking HUMALOG and each time you get a refill. There may be new information.
1 Instructions for Use HUMALOG KwikPen insulin lispro injection (rdna origin) Read the Instructions for Use before you start taking HUMALOG and each time you get a refill. There may be new information.
Insulin Administration by Syringe 10/24/2012 1
 Insulin Administration by Syringe 10/24/2012 1 This PowerPoint and test will satisfy the knowledge portion of medication training for High Alert/High Risk Medication - Insulin. This PowerPoint covers basic
Insulin Administration by Syringe 10/24/2012 1 This PowerPoint and test will satisfy the knowledge portion of medication training for High Alert/High Risk Medication - Insulin. This PowerPoint covers basic
SHORT CLINICAL GUIDELINE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SHORT CLINICAL GUIDELINE SCOPE 1 Guideline title Type 2 diabetes: newer agents for blood glucose control in type 2 diabetes 1.1 Short title Type 2
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SHORT CLINICAL GUIDELINE SCOPE 1 Guideline title Type 2 diabetes: newer agents for blood glucose control in type 2 diabetes 1.1 Short title Type 2
Insulin pen start checklist
 Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Safe use of insulin e- learning module
 Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
insulin & diabetes What is insulin? Why must it be injected? What if I have to go on to insulin? Are there different types of insulin?
 Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Instructions for Use
 1 Instructions for Use HUMULIN R U-500 KwikPen insulin human injection U-500 (500 units/ml, 3 ml pen) Important: Know your dose of HUMULIN R U-500 insulin. The Pen delivers your dose in insulin units.
1 Instructions for Use HUMULIN R U-500 KwikPen insulin human injection U-500 (500 units/ml, 3 ml pen) Important: Know your dose of HUMULIN R U-500 insulin. The Pen delivers your dose in insulin units.
Why is Insulin so Important?
 Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
INTRODUCTION TO INSULIN
 INTRODUCTION TO INSULIN This section will give you some practical advice about using insulin. Your diabetes team will answer any particular questions that you may have e.g. dose of insulin. TYPES OF INSULIN
INTRODUCTION TO INSULIN This section will give you some practical advice about using insulin. Your diabetes team will answer any particular questions that you may have e.g. dose of insulin. TYPES OF INSULIN
Insulin and Diabetes
 Insulin What is Insulin? Insulin is a hormone produced by special cells in the pancreas These cells that are produced are called beta cells Insulin allows the glucose from food we eat to enter the cells
Insulin What is Insulin? Insulin is a hormone produced by special cells in the pancreas These cells that are produced are called beta cells Insulin allows the glucose from food we eat to enter the cells
Scottish Medicines Consortium
 Scottish Medicines Consortium insulin glulisine for subcutaneous injection 100 units/ml (Apidra ) No. (298/06) Sanofi Aventis 4 August 2006 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium insulin glulisine for subcutaneous injection 100 units/ml (Apidra ) No. (298/06) Sanofi Aventis 4 August 2006 The Scottish Medicines Consortium (SMC) has completed its assessment
My Doctor Says I Need to Mix Insulins... How Do I Begin? BD Getting Started. Mixing Insulins
 My Doctor Says I Need to Mix Insulins... How Do I Begin? BD Getting Started Mixing Insulins When your doctor tells you to use two types of insulin for an injection, they can be mixed in the same insulin
My Doctor Says I Need to Mix Insulins... How Do I Begin? BD Getting Started Mixing Insulins When your doctor tells you to use two types of insulin for an injection, they can be mixed in the same insulin
The OmniPod Insulin Management System
 Caregiver GUIDE The OmniPod Insulin Management System The OmniPod is an easy-to-use, two-part insulin delivery system. If you are a school nurse, daycare provider, or other secondary caregiver for someone
Caregiver GUIDE The OmniPod Insulin Management System The OmniPod is an easy-to-use, two-part insulin delivery system. If you are a school nurse, daycare provider, or other secondary caregiver for someone
ClikSTAR - Important facts about your new insulin delivery device.
 ClikSTAR - Important facts about your new insulin delivery device. Instruction for Use ClikSTAR Insulin delivery device Before you start: Read these instructions and follow them completely each time you
ClikSTAR - Important facts about your new insulin delivery device. Instruction for Use ClikSTAR Insulin delivery device Before you start: Read these instructions and follow them completely each time you
YOUR GUIDE TO THE LANTUS SOLOSTAR INSULIN PEN
 Important Safety Information for Lantus You must test your blood sugar levels while using insulin, such as Lantus. Do not make any changes to your dose or type of insulin without talking to your healthcare
Important Safety Information for Lantus You must test your blood sugar levels while using insulin, such as Lantus. Do not make any changes to your dose or type of insulin without talking to your healthcare
An introduction to the principles and practice of safe and effective administration of injections
 An introduction to the principles and practice of safe and effective administration of injections Introduction Giving an injection safely is considered to be a routine nursing activity. However it requires
An introduction to the principles and practice of safe and effective administration of injections Introduction Giving an injection safely is considered to be a routine nursing activity. However it requires
Effect of insulin needle reuse, size and site of injection on the risk of bending and breaking
 Effect of insulin needle reuse, size and site of injection on the risk of bending and breaking Theresa Torrance A retrospective study was conducted using a questionnaire sent to DSNs in the UK to assess
Effect of insulin needle reuse, size and site of injection on the risk of bending and breaking Theresa Torrance A retrospective study was conducted using a questionnaire sent to DSNs in the UK to assess
HUMULIN 70/30 KwikPen
 1 Instructions for Use HUMULIN 70/30 KwikPen (70% human insulin isophane suspension 30% human insulin injection [rdna origin]) Read the Instructions for Use before you start taking HUMULIN 70/30 and each
1 Instructions for Use HUMULIN 70/30 KwikPen (70% human insulin isophane suspension 30% human insulin injection [rdna origin]) Read the Instructions for Use before you start taking HUMULIN 70/30 and each
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org
 written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
INJECTION TECHNIQUE. IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole
 IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
P A T I E N T I N F O R M A T I O N. Apidra
 P A T I E N T I N F O R M A T I O N Apidra We have written this leaflet for those of you with diabetes who have been prescribed Apidra by your doctor. The primary goal of all diabetes treatment is to achieve
P A T I E N T I N F O R M A T I O N Apidra We have written this leaflet for those of you with diabetes who have been prescribed Apidra by your doctor. The primary goal of all diabetes treatment is to achieve
Intensive Insulin Therapy in Diabetes Management
 Intensive Insulin Therapy in Diabetes Management Lillian F. Lien, MD Medical Director, Duke Inpatient Diabetes Management Assistant Professor of Medicine Division of Endocrinology, Metabolism, & Nutrition
Intensive Insulin Therapy in Diabetes Management Lillian F. Lien, MD Medical Director, Duke Inpatient Diabetes Management Assistant Professor of Medicine Division of Endocrinology, Metabolism, & Nutrition
insulin & diabetes Talking diabetes No.24 Revised 2012
 Talking diabetes No.24 Revised 2012 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with
Talking diabetes No.24 Revised 2012 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with
Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm
 Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm Why might my Doctor ask me to inject Methotrexate? Methotrexate comes in two forms:
Learning to Self Inject Methotrexate at Home Developed by Andy Thompson MD FRCPC and Marie J Craig-Chambers B.Sc.Phm Why might my Doctor ask me to inject Methotrexate? Methotrexate comes in two forms:
A patient guide to the use of insulin for diabetes
 A patient guide to the use of insulin for diabetes Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A patient guide to the use of insulin for diabetes Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Using Insulin Pens and Pen Needles
 My Doctor Says I Should Begin Using an Insulin Pen... How Do I Use Them? BD Getting Started Using Insulin Pens and Pen Needles Insulin Pens and Dosers easy to carry, dose and use An insulin pen is a convenient
My Doctor Says I Should Begin Using an Insulin Pen... How Do I Use Them? BD Getting Started Using Insulin Pens and Pen Needles Insulin Pens and Dosers easy to carry, dose and use An insulin pen is a convenient
insulin & diabetes What is insulin? Why must it be injected? What if I have to go on to insulin? Are there different types of insulin?
 Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Insulin Pens & Improving Patient Adherence
 Insulin Pens & Improving Patient Adherence Bonnie Pepon, RN, BSN, CDE Certified Diabetes Educator Conemaugh Diabetes Institute Kip Benko, MD FACEP Asst Clinical Professor University of Pittsburgh School
Insulin Pens & Improving Patient Adherence Bonnie Pepon, RN, BSN, CDE Certified Diabetes Educator Conemaugh Diabetes Institute Kip Benko, MD FACEP Asst Clinical Professor University of Pittsburgh School
Educational Objectives. Type 2 Diabetes: a progressive condition. Insulin Delivery Devices. Insulin we may wait too long
 Educational Objectives Insulin Delivery Devices James Bennett RPh, FACA, CDE Director of Clinical Services at James Bennett Apothecary Corinth Mississippi After viewing this program, participants should
Educational Objectives Insulin Delivery Devices James Bennett RPh, FACA, CDE Director of Clinical Services at James Bennett Apothecary Corinth Mississippi After viewing this program, participants should
10 to 30 minutes ½ to 3 hours 3 to 5 hours. 30 60 minutes 1 to 5 hours 8 hours. 1 to 4 hours
 Insulin Action There are several types of insulin. They are classified by how long they act: very fast, fast, slow and very slow acting. Each type of insulin has a certain time period in which it works.
Insulin Action There are several types of insulin. They are classified by how long they act: very fast, fast, slow and very slow acting. Each type of insulin has a certain time period in which it works.
Oral Therapy for Type 2 Diabetes
 Oral Therapy for Type 2 Diabetes Diabetes pills can help to manage your blood sugar. These pills are not insulin. They work to manage your blood sugar in several ways. You may be given a combination of
Oral Therapy for Type 2 Diabetes Diabetes pills can help to manage your blood sugar. These pills are not insulin. They work to manage your blood sugar in several ways. You may be given a combination of
DAFNE Session Learning Outcome (SLO) Form: Session content
 DAFNE Session Learning Outcome (SLO) Form: Session content Session No: 7 Session Title: Insulin action and injection technique Expected minimum timing for session: 75 minutes Insulin Regimen Day: Time
DAFNE Session Learning Outcome (SLO) Form: Session content Session No: 7 Session Title: Insulin action and injection technique Expected minimum timing for session: 75 minutes Insulin Regimen Day: Time
Onset Peak Duration Comments
 Rapid- Acting 5-15 minutes 0.5-3 hours 3-5 hours Meal should be available before administering, ideally taking within 10 minutes of eating). Good in refrigerator (36-46 F) until expiration date. Protect
Rapid- Acting 5-15 minutes 0.5-3 hours 3-5 hours Meal should be available before administering, ideally taking within 10 minutes of eating). Good in refrigerator (36-46 F) until expiration date. Protect
Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes
 Diabetes Sans Frontières Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes 1. Introduction This guideline has been developed in order to support practices to undertake insulin therapeutic
Diabetes Sans Frontières Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes 1. Introduction This guideline has been developed in order to support practices to undertake insulin therapeutic
HUMULIN (HU-mu-lin) N
 Instructions for Use HUMULIN (HU-mu-lin) N (human insulin [rdna origin] isophane suspension) vial (100 Units/mL, U-100) Read the Instructions for Use before you start taking HUMULIN N and each time you
Instructions for Use HUMULIN (HU-mu-lin) N (human insulin [rdna origin] isophane suspension) vial (100 Units/mL, U-100) Read the Instructions for Use before you start taking HUMULIN N and each time you
My Doctor Says I Should Learn To Use Insulin... What Do I Do Next? BD Getting Started. Drawing and Injecting Insulin
 My Doctor Says I Should Learn To Use Insulin... What Do I Do Next? BD Getting Started Drawing and Injecting Insulin It is important to know how to draw and inject insulin so that you can give your injection
My Doctor Says I Should Learn To Use Insulin... What Do I Do Next? BD Getting Started Drawing and Injecting Insulin It is important to know how to draw and inject insulin so that you can give your injection
Cochrane Quality and Productivity topics
 Long-acting insulin analogues versus NPH insulin (human isophane insulin) for type 2 diabetes mellitus NICE has developed the Cochrane Quality and Productivity (QP) topics to help the NHS identify practices
Long-acting insulin analogues versus NPH insulin (human isophane insulin) for type 2 diabetes mellitus NICE has developed the Cochrane Quality and Productivity (QP) topics to help the NHS identify practices
KwikPen Insulin delivery device
 USER MANUAL KwikPen Insulin delivery device PLEASE READ THESE INSTRUCTIONS BEFORE USE Lilly Introduction The KwikPen is designed for ease of use. It is a disposable pen containing 3 ml (300 units) of U-
USER MANUAL KwikPen Insulin delivery device PLEASE READ THESE INSTRUCTIONS BEFORE USE Lilly Introduction The KwikPen is designed for ease of use. It is a disposable pen containing 3 ml (300 units) of U-
Methotrexate. What is methotrexate?
 Methotrexate What is methotrexate? Methotrexate is a mild immunosuppressant that also exhibits antiinflammatory activity. Methotrexate is commonly used for the treatment of certain cancers including but
Methotrexate What is methotrexate? Methotrexate is a mild immunosuppressant that also exhibits antiinflammatory activity. Methotrexate is commonly used for the treatment of certain cancers including but
by Rodney Lorenz, MD and Janet Silverstein, MD
 Managing Insulin Requirements at School by Rodney Lorenz, MD and Janet Silverstein, MD Introduction Multiple advances over the past decade have revolutionized treatment of diabetes in youth. Two fundamental
Managing Insulin Requirements at School by Rodney Lorenz, MD and Janet Silverstein, MD Introduction Multiple advances over the past decade have revolutionized treatment of diabetes in youth. Two fundamental
Tell your doctor about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements.
 SOMAVERT pegvisomant for injection PATIENT INFORMATION SOMAVERT (SOM-ah-vert) (pegvisomant for injection) Read the patient information that comes with SOMAVERT before you start using it and each time you
SOMAVERT pegvisomant for injection PATIENT INFORMATION SOMAVERT (SOM-ah-vert) (pegvisomant for injection) Read the patient information that comes with SOMAVERT before you start using it and each time you
Insulin Pump Therapy
 CHILDREN S SERVICES Insulin Pump Therapy These guidelines are not intended for starting a patient on an insulin pump. They are intended to give staff not part of the diabetic team information regarding
CHILDREN S SERVICES Insulin Pump Therapy These guidelines are not intended for starting a patient on an insulin pump. They are intended to give staff not part of the diabetic team information regarding
INSTRUCTIONS FOR USE. Read this information before you start. Important things to know about your SmartJect autoinjector. Important things to remember
 INSTRUCTIONS FOR USE SIMPONI (SIM-po-nee) (golimumab) SmartJect autoinjector If your doctor decides that you or a caregiver may be able to give your injections of SIMPONI at home, you should receive training
INSTRUCTIONS FOR USE SIMPONI (SIM-po-nee) (golimumab) SmartJect autoinjector If your doctor decides that you or a caregiver may be able to give your injections of SIMPONI at home, you should receive training
PA 9114 FSAMP. Lilly Disposable Insulin Delivery Device User Manual
 1 Lilly Disposable Insulin Delivery Device User Manual PA 9114 FSAMP Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may
1 Lilly Disposable Insulin Delivery Device User Manual PA 9114 FSAMP Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may
Insulin initiation in type 2 diabetes: Experience and insights
 Insulin initiation in type 2 diabetes: Experience and insights Joan Everett A diagnosis of type 2 diabetes can be devastating for the individual and their family. Furthermore, many people with diabetes
Insulin initiation in type 2 diabetes: Experience and insights Joan Everett A diagnosis of type 2 diabetes can be devastating for the individual and their family. Furthermore, many people with diabetes
Disposable Insulin Delivery Device User Manual
 PV 3734 AMP Disposable Insulin Delivery Device User Manual Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may get too
PV 3734 AMP Disposable Insulin Delivery Device User Manual Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may get too
THE INS AND OUTS OF INSULIN. Mary Beth Wald, RN,BSN,CDE
 THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
IVF CLASS. IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.
 IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.mil PLEASE NOTE: If you do not have medications for the next
IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, darshana.naik.ctr@health.mil Nicole 301-400-2146, nicole.l.sobers.ctr@health.mil PLEASE NOTE: If you do not have medications for the next
California SB-486 Plan Revision Date: July 1, 2014. Plan for Supporting Safe Collection and Proper Disposal of Home Generated Sharps
 Plan for Supporting Safe Collection and Proper Disposal of Home Generated Sharps Background: The State of California recently enacted two laws to address home generated sharps disposal. The first law (SB
Plan for Supporting Safe Collection and Proper Disposal of Home Generated Sharps Background: The State of California recently enacted two laws to address home generated sharps disposal. The first law (SB
How To Prepare and Give a Prefilled Syringe Injection
 Diablo Valley Onc&Hem Med Grp, Inc Phone Number: (925)6775041 How To Prepare and Give a Prefilled Syringe Injection Patient Education Quick Reference Guide The following are instructions for use of prefilled
Diablo Valley Onc&Hem Med Grp, Inc Phone Number: (925)6775041 How To Prepare and Give a Prefilled Syringe Injection Patient Education Quick Reference Guide The following are instructions for use of prefilled
Skin and subcutaneous thickness at injecting sites in children with diabetes: ultrasound findings and recommendations for giving injection
 Pediatric Diabetes 2012 doi: 101111/j1399-5448201200865x All rights reserved 2012 John Wiley & Sons A/S Pediatric Diabetes Original Article Skin and subcutaneous thickness at injecting sites in children
Pediatric Diabetes 2012 doi: 101111/j1399-5448201200865x All rights reserved 2012 John Wiley & Sons A/S Pediatric Diabetes Original Article Skin and subcutaneous thickness at injecting sites in children
Information for Starting Insulin Basal-Bolus Regime
 Information for Starting Insulin Basal-Bolus Regime Department of Diabetes Page 12 Patient Information Insulin Instructions for Basal Bolus Regimen Two types of insulin are used in this insulin regimen.
Information for Starting Insulin Basal-Bolus Regime Department of Diabetes Page 12 Patient Information Insulin Instructions for Basal Bolus Regimen Two types of insulin are used in this insulin regimen.
Emma Jenkins BSc, RD, CEDT Diabetes Specialist Dietitian Royal Bournemouth Hospital Dorset, UK. Pens & calculators at the ready?!...
 Emma Jenkins BSc, RD, CEDT Diabetes Specialist Dietitian Royal Bournemouth Hospital Dorset, UK Pens & calculators at the ready?!... Robert, age 42. Type 1 diabetes for 26yrs. HbA1c 76mmols/mol 2 recent
Emma Jenkins BSc, RD, CEDT Diabetes Specialist Dietitian Royal Bournemouth Hospital Dorset, UK Pens & calculators at the ready?!... Robert, age 42. Type 1 diabetes for 26yrs. HbA1c 76mmols/mol 2 recent
Insulin - Jet Administration System. instructions for use
 Insulin - Jet Administration System instructions for use INTRODUCTION Thank you for choosing the InsuJet, a European-designed insulin-jet administration system, developed with your comfort and convenience
Insulin - Jet Administration System instructions for use INTRODUCTION Thank you for choosing the InsuJet, a European-designed insulin-jet administration system, developed with your comfort and convenience
Injectable Insulin During Pregnancy
 Injectable Insulin During Pregnancy What is insulin? Insulin is a hormone made by the pancreas. The pancreas is a small organ that lies behind and below the stomach. Insulin allows the food you eat to
Injectable Insulin During Pregnancy What is insulin? Insulin is a hormone made by the pancreas. The pancreas is a small organ that lies behind and below the stomach. Insulin allows the food you eat to
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
Introduction to Insulin. Your guide to taking insulin
 Introduction to Insulin Your guide to taking insulin Introduction Insulin helps control the level of blood glucose in the body. Everyone with type 1 diabetes must take insulin, and many people with type
Introduction to Insulin Your guide to taking insulin Introduction Insulin helps control the level of blood glucose in the body. Everyone with type 1 diabetes must take insulin, and many people with type
PA 9117 FSAMP. Lilly. Prefilled Insulin Delivery Device User Manual
 1 Lilly PA 9117 FSAMP Prefilled Insulin Delivery Device User Manual Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may
1 Lilly PA 9117 FSAMP Prefilled Insulin Delivery Device User Manual Instructions for Use Read and follow all of these instructions carefully. If you do not follow these instructions completely, you may
HOW TO USE YOUR LANTUS SOLOSTAR PEN
 What is Lantus (insulin glargine injection) 100 Units/mL? Prescription Lantus is a long-acting insulin used to treat adults with type 2 diabetes and adults and pediatric patients (children 6 years and
What is Lantus (insulin glargine injection) 100 Units/mL? Prescription Lantus is a long-acting insulin used to treat adults with type 2 diabetes and adults and pediatric patients (children 6 years and
Giving Yourself Dalteparin (Fragmin) or Heparin
 Contents www.bcwomens.ca What is Dalteparin (Fragmin)...1 Where do I get this medication from?...1 How often do I give myself this medication?...1 Side effects...1 Steps to Giving Yourself Dalteparin (Fragmin)..1
Contents www.bcwomens.ca What is Dalteparin (Fragmin)...1 Where do I get this medication from?...1 How often do I give myself this medication?...1 Side effects...1 Steps to Giving Yourself Dalteparin (Fragmin)..1
Basal and Bolus Insulin 7/16/2014. Jackie Aday RN, BSN, CDE Jeni Neighbors RN, BSN, CDE. BASAL: Small amount of insulin infused every few minutes
 Jackie Aday RN, BSN, CDE Jeni Neighbors RN, BSN, CDE Insulin Pump Therapy Open looped system in which a small amount of insulin is continuously infused through a cannula or needle (basal rate) Larger doses
Jackie Aday RN, BSN, CDE Jeni Neighbors RN, BSN, CDE Insulin Pump Therapy Open looped system in which a small amount of insulin is continuously infused through a cannula or needle (basal rate) Larger doses
Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes.
 PROTOCOL Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes. A. This the revised protocol (April 2002) B. Review team Contact for correspondence: Dr Jill Colquitt
PROTOCOL Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes. A. This the revised protocol (April 2002) B. Review team Contact for correspondence: Dr Jill Colquitt
Shared Care Agreement Insulin Degludec (Tresiba )
 Licensed Indication Shared Care Agreement Insulin Degludec (Tresiba ) Insulin Degludec is licensed for the treatment of diabetes mellitus in adults. Countess of Chester prescribing guidelines Restricting
Licensed Indication Shared Care Agreement Insulin Degludec (Tresiba ) Insulin Degludec is licensed for the treatment of diabetes mellitus in adults. Countess of Chester prescribing guidelines Restricting
DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358. www.nj.gov/health
 CHRIS CHRISTIE Governor KIM GUADAGNO Lt. Governor Dear Administrator: DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358 www.nj.gov/health January, 2013 MARY E. O DOWD, M.P.H. Commissioner Since
CHRIS CHRISTIE Governor KIM GUADAGNO Lt. Governor Dear Administrator: DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358 www.nj.gov/health January, 2013 MARY E. O DOWD, M.P.H. Commissioner Since
User Manual Important: First read the Medication Guide that comes inside your FORTEO carton.
 1 RA082FSAM02 User Manual Important: First read the Medication Guide that comes inside your FORTEO carton. Before you use your new FORTEO delivery device, please read the entire front and back of this
1 RA082FSAM02 User Manual Important: First read the Medication Guide that comes inside your FORTEO carton. Before you use your new FORTEO delivery device, please read the entire front and back of this
by Rodney Lorenz, MD and Janet Silverstein, MD
 Managing Insulin Requirements at School by Rodney Lorenz, MD and Janet Silverstein, MD Introduction Multiple advances over the past decade have revolutionized treatment of diabetes in youth. Two fundamental
Managing Insulin Requirements at School by Rodney Lorenz, MD and Janet Silverstein, MD Introduction Multiple advances over the past decade have revolutionized treatment of diabetes in youth. Two fundamental
A pictorial guide to diabetes care, supplies, and devices
 A pictorial guide to diabetes care, supplies, and devices Caution: This publication contains depictions of blood, needles and medical procedures related to diabetes care. This publication may be reproduced
A pictorial guide to diabetes care, supplies, and devices Caution: This publication contains depictions of blood, needles and medical procedures related to diabetes care. This publication may be reproduced
INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE
 INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE We welcome feedback on this policy and the way it operates. We are interested to know of any possible or actual adverse impact that this policy/procedure
INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE We welcome feedback on this policy and the way it operates. We are interested to know of any possible or actual adverse impact that this policy/procedure
Insulin Delivery Devices
 My Doctor Says I Need Insulin to Control My Diabetes... How Should I Take It? BD Getting Started Insulin Delivery Devices Why is Insulin So Important? Insulin is a life-saving drug for people with diabetes.
My Doctor Says I Need Insulin to Control My Diabetes... How Should I Take It? BD Getting Started Insulin Delivery Devices Why is Insulin So Important? Insulin is a life-saving drug for people with diabetes.
FRAGMIN Please bring this booklet the day of your surgery.
 FRAGMIN Please bring this booklet the day of your surgery. QHC#72 Fragmin (dalteparin sodium injection); an anticoagulant (blood thinner) is used to help prevent blood clots after surgery. While on Fragmin,
FRAGMIN Please bring this booklet the day of your surgery. QHC#72 Fragmin (dalteparin sodium injection); an anticoagulant (blood thinner) is used to help prevent blood clots after surgery. While on Fragmin,
Glycaemic Control in Adults with Type 1 Diabetes
 Glycaemic Control in Adults with Type 1 Diabetes Aim(s) and objective(s) This document aims to provide guidance on good clinical practice in managing glycaemic control in adult patients with Type 1 Diabetes
Glycaemic Control in Adults with Type 1 Diabetes Aim(s) and objective(s) This document aims to provide guidance on good clinical practice in managing glycaemic control in adult patients with Type 1 Diabetes
Insulin delivery using pen devices
 Insulin delivery using pen devices Simple-to-use tools may help young and old alike Nancy J. V. Bohannon, MD Preview: Clinical trials have convincingly demonstrated that improved glycemic control significantly
Insulin delivery using pen devices Simple-to-use tools may help young and old alike Nancy J. V. Bohannon, MD Preview: Clinical trials have convincingly demonstrated that improved glycemic control significantly
Insulin Pump Therapy during Pregnancy and Birth
 Approvals: Specialist Group: Miss F Ashworth, Dr I Gallen, Dr J Ahmed Maternity Guidelines Group: V1 Dec 2012 Directorate Board: V1 Jan 2013 Clinical Guidelines Subgroup: July 2011 MSLC: V1 Nov 2012 Equality
Approvals: Specialist Group: Miss F Ashworth, Dr I Gallen, Dr J Ahmed Maternity Guidelines Group: V1 Dec 2012 Directorate Board: V1 Jan 2013 Clinical Guidelines Subgroup: July 2011 MSLC: V1 Nov 2012 Equality
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS
 PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
Owner Manual. Diabetes in Dogs. www.pet-diabetes.com. Simplifying small animal diabetes
 Owner Manual www.pet-diabetes.com Diabetes in Dogs Simplifying small animal diabetes D i a b e t e s i n D o g s What is Diabetes? Glucose ( blood sugar ) provides the cells in the body with the energy
Owner Manual www.pet-diabetes.com Diabetes in Dogs Simplifying small animal diabetes D i a b e t e s i n D o g s What is Diabetes? Glucose ( blood sugar ) provides the cells in the body with the energy
Chapter 9 Drawing Up and Giving Insulin
 Chapter 9 Drawing Up and Giving Insulin H. Peter Chase, MD Catherine Suffoletta, RN WHERE TO INJECT THE INSULIN Insulin is injected into the fat layer beneath the skin. Proper techniques must be learned
Chapter 9 Drawing Up and Giving Insulin H. Peter Chase, MD Catherine Suffoletta, RN WHERE TO INJECT THE INSULIN Insulin is injected into the fat layer beneath the skin. Proper techniques must be learned
IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL
 464 IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL PRACTICE STEPHAN A SCHREIBER AND ANIKA RUßMAN ABSTRACT
464 IMPROVED METABOLIC CONTROL WITH A FAVORABLE WEIGHT PROFILE IN PATIENTS WITH TYPE 2 DIABETES TREATED WITH INSULIN GLARGINE (LANTUS ) IN CLINICAL PRACTICE STEPHAN A SCHREIBER AND ANIKA RUßMAN ABSTRACT
