Alameda Alliance for Health SPECIALTY PHARMACY PROGRAM FOR ALLIANCE MEDI-CAL AND GROUP CARE MEMBERS PROGRAM DESCRIPTION
|
|
|
- Mercy Austin
- 8 years ago
- Views:
Transcription
1 Alameda Alliance for Health SPECIALTY PHARMACY PROGRAM FOR ALLIANCE MEDI-CAL AND GROUP CARE MEMBERS PROGRAM DESCRIPTION Contents Page Program Overview 1 Process for Obtaining Authorization 2 Contacts 2 Medication Request Form 3 Specialty Pharmacy Program Drug List 4 Alliance Specialty Pharmacy Program Overview: Effective September 1, 2010, Diplomat Specialty Pharmacy (Diplomat) is the Alliance s specialty pharmacy for Alliance Medi-Cal and Group Care programs. (Specialty drug orders for Alliance CompleteCare members can be filled by Diplomat, or any other Alliance-contracted pharmacy.) Attached to this program description is the list of drugs that Diplomat is providing under this program. Diplomat is the only pharmacy that can fill the drugs on this list for Alliance Medi-Cal and Group Care members. Retail pharmacies may not dispense these drugs. Providers (including physicians, hospitals, infusion centers, and dialysis centers) can, however, continue to purchase specialty drugs directly from manufactures and wholesalers. The benefits of using Diplomat Specialty Pharmacy include: There are no up-front costs for specialty drugs or medication supplies, such as needles. Convenient FREE delivery of specialty drugs to your patients homes or to your office. Diplomat offers proactive renewal on all medications. You can continue to bill the Alliance your administration fee.
2 Process for Obtaining Specialty Drugs from Diplomat for Alliance Medi-Cal and Group Care Members: Starting September 1, 2010, prior authorization is required for new specialty drug orders and for renewals. The same review process is used for specialty drug orders as is used for other drugs that require prior authorization. Please fax the attached Medication Request Form to PerformRx at or call PerformRx at PerformRx will process the request within 72 hours (for urgent requests) or 14 days (for routine requests) and notify your office and Diplomat of the decision. Upon PerformRx s approval, Diplomat will call your office to obtain the prescription and dispense the drug by mail. Diplomat can be reached at Contacts for Additional Information: Call Diplomat toll-free at for: o A complete list of specialty drugs provided by Diplomat o Questions related to dispensing of the drugs Call PerformRx toll-free at for prior authorization-related questions Call Alliance Pharmacy Services at for any other specialty pharmacy related questions Alameda Alliance for Health - Specialty Pharmacy Program Description Last Updated: January
3 Alameda Alliance for Health Medication Request Form Attn: Prior Authorization Department 200 Stevens Drive Philadelphia, PA Phone (Medi-Cal/Group Care): Phone (AllianceSELECT): Fax: Instructions: This form is to be used by participating providers to obtain coverage for a formulary drug with PA guideline, other restrictions, or a nonformulary drug for which there is no suitable alternative available. Please complete this form and fax it to PerformRx at or call with this information. If you have any questions regarding this process, please contact PerformRx s Provider Service Line at for Medi-Cal/Group Care and for AllianceSELECT. Urgent Request (Must be reserved for requests that, in the provider s best professional judgment, are potentially life threatening or pose a significant risk to the continuous care of the patient.) Patient Name Patient DOB Patient ID Number Prescriber Name Specialty Prescriber Phone Prescriber Fax NPI# Prescriber Address Pharmacy Name Pharmacy Phone Pharmacy Fax Medication Name and Strength Requested: Brand Medically Necessary request (Rationale required below) Directions: Quantity Requested: Anticipated Length of Therapy: Days 3 Months 6 Months 12 Months Diagnosis: Preferred Medications tried/previous therapy, please include strength, frequency and duration: Rationale and/or additional information, which may be relevant to the review of this prior authorization request: Prescriber Signature Date Please Fax Completed Form to Alameda Alliance for Health Medication Request Form Revised
4 Alliance Medi-Cal and Group Care Specialty Pharmacy Program Drug List Effective: January 1, 2014 The following list reflects drugs that are a part of the Alameda Alliance for Health Specialty Pharmacy Program. This program applies to Alliance Medi-Cal and Group Care only. Providers (including physicians, hospitals, dialysis centers, and infusion centers) can order the drugs on this list from a drug distributor or from Diplomat Specialty Pharmacy (Diplomat). Retail pharmacies may not dispense these drugs. Diplomat is the only pharmacy that can dispense these drugs. Prior authorization is required for the drugs on this list. Please submit a Prior Authorization Form to PerformRx via fax at or call PerformRx at Upon approval, Diplomat will contact the ordering physicians office for prescription. The list is sorted by drug class and most common brand name. This list is subject to change. Please visit to for updates. Antibacterials Colistimethate Coly-Mycin M Coly-Mycin S Antiemetics Aloxi Anzemet Antifungals Cancidas Vfend Antithrombotic Agents Activase Cathflo Activase Integrilin Blood Cell Deficiency Leukine Neulasta Neumega Neupogen Bones Resorption Inhibitors Prolia Xgeva Zoledronic Acid Zometa CMV Cidofovir Cytovene Valcyte Growth Hormone Genotropin Humatrope CRT Increlex Nordiflex Norditropin Nutropin Nutropin AQ Omnitrope Serostim Tev-Tropin Hemophilia Alphanate AlphaNine SD Bebulin VH BeneFix Feiba NF Hemofil Humate-P Koate DVI Kogenate FS Bio Set Kogenate FS Monoclate-P Mononine NovoSeven RT Profilnine SD Recombinate Recombinate w/baxjet Wilate Xyntha AHF Xyntha Intravenous Kit Xyntha Solofuse Intravenous Hepatitis B Tyzeka Viread Hepatitis C Incivek Infergen Intron A Pegasys Pegasys Proclick PegIntron RediPEN Rebetol RibaPak Ribasphere Ribavirin Victrelis Hormonal Therapy Danazol Delestrogen Immune Deficiencies Carimune NF Flebogamma DIF Gammagard LIQ Gammagard S/D less IgA Gammagard SD Gammaked Gammaplex Gamunex-C Hizentra Octagam Privigen WinRho SDF Liquid Lysosomal Storage Disorders Aldurazyme Elaprase Fabrazyme Multiple Sclerosis (MS) Ampyra Aubagio Avonex Pen Avonex PFS Avonex SDV Celestone Soluspan Copaxone Extavia Gilenya Rebif Rebidose Rebif titration pack Rebif Tecfidera Oncology Abraxane Adcetris Adriamycin Adrucil Alimta Alkeran Amifostine IV Arimidex Aromasin Arranon Arzerra Avastin Bicnu Bleomycin Bosulif Busulfex Camptosar Carboplatin CeeNU Cerubidine Cisplatin Cladribine Clolar Cometriq Cosmegen Cyclophosphamide Cytarabine Dacarbazine Dactinomycin Daunorubicin Dexrazoxane Diplomat is able to provide other drugs that are not listed here. For a complete list of drugs, contact Diplomat at To check the status of prior authorization requests, contact PerformRx at For questions about the specialty pharmacy program, please contact Alliance Pharmacy Services at Pg 1 of 2
5 Alliance Medi-Cal and Group Care Specialty Pharmacy Program Drug List Effective: January 1, 2014 The following list reflects drugs that are a part of the Alameda Alliance for Health's Specialty Pharmacy Program. This program applies to Alliance Medi-Cal and Group Care plans only. Providers (including physicians, hospitals, dialysis centers, and infusion centers) can order the drugs on this list from a drug distributor or from Diplomat Specialty Pharmacy (Diplomat). Retail pharmacies may not dispense these drugs. Diplomat is the only pharmacy that can dispense these drugs. Prior authorization is required for the drugs on this list. Please submit a Prior Authorization Form to PerformRx via fax at or call PerformRx at Upon approval, Diplomat will contact the ordering physicians office for prescription. The list is sorted by drug class and most common brand name. This list is subject to change. Please visit to for updates. Oncology continued Docefrez DOCEtaxel Doxil Doxorubicin Eligard Ellence Eloxatin Elspar Emcyt Epirubicin Erbitux Erivedge Etopophos Etoposide Fareston Faslodex Floxuridine Fludarabine Fluorouracil IV Flutamide Folotyn Gemcitabine HCL Gemzar Gleevec Halaven Idamycin Ifex Irinotecan Jakafi Leukeran Leuprolide Lysodren Melphalan HCL Mercaptopurine Tabs Methotrexate IV Mitomycin Myleran Nexavar Nipent Octreotide Paclitaxel Pamidronate Pentostatin Pomalyst Revlimid Rituxan Sprycel Stivarga Sutent Sylatron Tarceva Temodar Thalomid Oncology continued TheraCys Topotecan Tretinoin Caps Tykerb Xeloda Yervoy Zaltrap Zanosar Zinecard Zolinza Zytiga Other Aminocaproic Acid Syr Aminocaproic Acid Tab Berinert Botox Buphenyl Decavac Deferoxamine Desmopressin Droperidol Elitek Euflexxa Exjade Eylea Hyalgan Kepivance Leucovorin Mannitol Marcaine Mesalamine Pentam RhoGam Ultra Filtered Plus Rhophylac PFS RiaSTAP Supartz Synvisc Zemplar Parenteral Iron Dexferrum Feraheme Infed Venofer Pulmonary Hypertension Adcirca Alprostadil Sildenafil Rheumatoid Arthritis (RA) Actemra Arava Cimzia Enbrel Gengraf Humira Kineret Leflunomide Neoral Orencia Remicade Xeljanz Transplant Atgam Cellcept IV Cyclosporine Inj Mycophenolate Diplomat is able to provide other drugs that are not listed here. Please contact Diplomat at for a complete list of drugs. To check the status of prior authorization requests, contact PerformRx at For questions about the specialty pharmacy program, please contact Alliance Pharmacy Services at Pg 2 of 2
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE August 20, 2015 SUBJECT EFFECTIVE DATE September 28, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER 99-15-08 BY Specialty Pharmacy Drug Program Pharmacy Services Leesa M. Allen, Deputy Secretary Office
ISSUE DATE August 20, 2015 SUBJECT EFFECTIVE DATE September 28, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER 99-15-08 BY Specialty Pharmacy Drug Program Pharmacy Services Leesa M. Allen, Deputy Secretary Office
Pain management for cancer patients Acute Ischemic Stroke. Hemophilia, Von willebrand disease & Bleeding disorders. Infectious Disease
 Cigna Specialty Pharmacy Services Limited Distribution and Risk Evaluation Mitigation (RE) Drug List Last updated on 04/06/2015 Medication Brand Name Condition Actemra Rheumatroid Arthritis Acthar Seizure
Cigna Specialty Pharmacy Services Limited Distribution and Risk Evaluation Mitigation (RE) Drug List Last updated on 04/06/2015 Medication Brand Name Condition Actemra Rheumatroid Arthritis Acthar Seizure
Specialty Drug Program RX Benefit Member Guide
 Specialty Drug Program RX Benefit Member Guide bcbsm.com Enrollment Form for Walgreens Specialty Pharmacy, LLC. How to place your initial order with Walgreens Specialty Pharmacy: 1) Print and complete
Specialty Drug Program RX Benefit Member Guide bcbsm.com Enrollment Form for Walgreens Specialty Pharmacy, LLC. How to place your initial order with Walgreens Specialty Pharmacy: 1) Print and complete
Specialty Pharmacy: Understanding the Market and Solution. Your Goals. Presented by Chris Brown November 2009
 Specialty Pharmacy: Understanding the Market and Solution Presented by Chris Brown November 2009 Your Goals What What is a Specialty is a specialty Medication? medication? Specialty drugs are injectable,
Specialty Pharmacy: Understanding the Market and Solution Presented by Chris Brown November 2009 Your Goals What What is a Specialty is a specialty Medication? medication? Specialty drugs are injectable,
N/A N/A N/A. Supporting statement of diagnosis from the N/A. physician and documented trial of 1 generic. formulary alternative
 Actimmune Amlodipine Androderm Anticonvulsant Antidepressants Antineoplastics Antipsychotics Arcalyst Butalbital Colony Stimulating Factors ESRD Therapy Actimmune Norvasc Androderm Banzel Keppra Mysoline
Actimmune Amlodipine Androderm Anticonvulsant Antidepressants Antineoplastics Antipsychotics Arcalyst Butalbital Colony Stimulating Factors ESRD Therapy Actimmune Norvasc Androderm Banzel Keppra Mysoline
Self-injectable, infused and oral specialty drugs 2014 Aetna Specialty CareRx SM Benefits Plan Drug List
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Self-injectable, infused and oral specialty drugs 2014 Aetna Specialty CareRx SM Benefits Plan Drug List 05.03.382.1
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Self-injectable, infused and oral specialty drugs 2014 Aetna Specialty CareRx SM Benefits Plan Drug List 05.03.382.1
ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers. May 1, 2012
 ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers May 1, 2012 Agenda Topics for Today 1. Program Summary Specialty Injectable Drugs in scope EmblemHealth
ICORE Healthcare: Injectable Drug Utilization Management Program Overview for EmblemHealth Providers May 1, 2012 Agenda Topics for Today 1. Program Summary Specialty Injectable Drugs in scope EmblemHealth
Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment
 A Patient s Guide Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment Recommendations of the American Society of Clinical Oncology The American Society of Clinical Oncology (ASCO) is
A Patient s Guide Preventing and Treating Nausea and Vomiting Caused by Cancer Treatment Recommendations of the American Society of Clinical Oncology The American Society of Clinical Oncology (ASCO) is
STAT Bulletin. Drug Therapy Guideline Updates. May 11, 2012 Volume: 18 Issue: 12
 STAT Bulletin May 11, 2012 Volume: 18 Issue: 12 To: All primary care physicians and specialists Contracts Affected: All Lines of Business Drug Therapy Guideline Updates Why you re receiving this Stat What
STAT Bulletin May 11, 2012 Volume: 18 Issue: 12 To: All primary care physicians and specialists Contracts Affected: All Lines of Business Drug Therapy Guideline Updates Why you re receiving this Stat What
Prescription Drug Utilization and Cost Trends, 2009-2013
 Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services
 scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
REVISING SPECIALTY TIERS
 WHITE PAPER REVISING SPECIALTY TIERS PROTECTING MEDICARE PART D BENEFICIARIES FROM BURDENSOME COST SHIFTING Gary G., Michigan Gary thought he had his financial assistance grant set up to cover his out-of-pocket
WHITE PAPER REVISING SPECIALTY TIERS PROTECTING MEDICARE PART D BENEFICIARIES FROM BURDENSOME COST SHIFTING Gary G., Michigan Gary thought he had his financial assistance grant set up to cover his out-of-pocket
Drugs Requiring Prior Authorization. Olysio. Subsys. Prolia. Tecfidera
 Abstral Acthar Hp Adcirca Adempas Affinitor Amitiza Amitriptyline Ampyra Androgel Androderm Androxy Aranesp Arcalyst Aubagio Avonex Bosulif Bydureon Byetta Cimzia Cinryze Clomipramine Cometriq Copaxone
Abstral Acthar Hp Adcirca Adempas Affinitor Amitiza Amitriptyline Ampyra Androgel Androderm Androxy Aranesp Arcalyst Aubagio Avonex Bosulif Bydureon Byetta Cimzia Cinryze Clomipramine Cometriq Copaxone
Prescription Drug Benefit Description
 Prescription Drug Benefit Description Herein called Description Prescription Drug Program For State of Kansas Employees Health Plan This booklet describes the Prescription Drug benefits available through
Prescription Drug Benefit Description Herein called Description Prescription Drug Program For State of Kansas Employees Health Plan This booklet describes the Prescription Drug benefits available through
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
CONNECTICARE, INC. & AFFILIATES
 CONNECTICARE, INC. & AFFILIATES INSERT PAGE FOR PRE-CERTIFICATION AND PRE- AUTHORIZATION LISTS UPDATE Applies to all ConnectiCare health plans, except the ConnectiCare Network USA-PPO Plan and as otherwise
CONNECTICARE, INC. & AFFILIATES INSERT PAGE FOR PRE-CERTIFICATION AND PRE- AUTHORIZATION LISTS UPDATE Applies to all ConnectiCare health plans, except the ConnectiCare Network USA-PPO Plan and as otherwise
April 30, 2009. The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate
 United States Government Accountability Office Washington, DC 20548 April 30, 2009 The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate Subject:
United States Government Accountability Office Washington, DC 20548 April 30, 2009 The Honorable Edward M. Kennedy Chairman Committee on Health, Education, Labor, and Pensions United States Senate Subject:
Specialty Pharmacy. Business Plan. July 8, 2013. 2013 RUSH University Medical Center
 Specialty Pharmacy Business Plan July 8, 2013 Specialty Pharmaceuticals What are they? Biotech/gene-based therapy Require special handling Newer products oral or self- administered One third have REMS
Specialty Pharmacy Business Plan July 8, 2013 Specialty Pharmaceuticals What are they? Biotech/gene-based therapy Require special handling Newer products oral or self- administered One third have REMS
Humana 2015 Autorización previa
 Humana 2015 Autorización previa Los medicamentos a continuación requerirán autorización previa en 2015. Para información sobre el nivel de copago, visite Humana.com. Abstral 100 mcg sublingual tablet Abstral
Humana 2015 Autorización previa Los medicamentos a continuación requerirán autorización previa en 2015. Para información sobre el nivel de copago, visite Humana.com. Abstral 100 mcg sublingual tablet Abstral
Medications most likely to be seen in primary care
 Hazardous Medicines The majority of medicines are not classed as hazardous. The only medicinal products that are automatically deemed to be hazardous are cytotoxic and cytostatic medicines. There is no
Hazardous Medicines The majority of medicines are not classed as hazardous. The only medicinal products that are automatically deemed to be hazardous are cytotoxic and cytostatic medicines. There is no
Hydration, IV Infusions, Injections and Vaccine Charge Process
 There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
There are a number of items to be considered when billing for the Nursing service to perform drug therapy, the charge process is divided into three specific groups of codes and processes. 1. Hydration
Safety Policy Manual Policy No. 106
 Safety Policy Manual Policy No. 106 Policy: Hazardous Drugs (Including Chemotherapeutic) Page 1 of 11 APPLICATION NYU Langone Medical Center (NYULMC) PURPOSE To protect employees from exposure to hazardous
Safety Policy Manual Policy No. 106 Policy: Hazardous Drugs (Including Chemotherapeutic) Page 1 of 11 APPLICATION NYU Langone Medical Center (NYULMC) PURPOSE To protect employees from exposure to hazardous
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS
 MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
Great-West s Drug Prior Authorization
 Great-West s Drug Prior Authorization Great-West Life s prior authorization process is designed to provide an effective approach to managing claims for specific prescription drugs. Approval for coverage
Great-West s Drug Prior Authorization Great-West Life s prior authorization process is designed to provide an effective approach to managing claims for specific prescription drugs. Approval for coverage
ACTEMRA. Cigna Medicare Rx (PDP) 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary. Products Affected Actemra. Prior Authorization Criteria
 Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Cigna Medicare Rx (PDP) Medicare Part D Prescription Drug Plans 2014 Cigna Medicare Rx Secure Plan (PDP) Formulary Prior Authorization ACTEMRA Products Affected Actemra PA Details Age Other Authorization
Specialty drug trend
 2 0 0 8 Specialty drug trend r e p o r t Specialty Pharmacy A n E x p r e s s S c r i p t s C o m p a n y Lead Authors Emily Cox, PhD, RPh Yakov Svirnovskiy, MA Chris Peterson, PharmD Aimee Tharaldson,
2 0 0 8 Specialty drug trend r e p o r t Specialty Pharmacy A n E x p r e s s S c r i p t s C o m p a n y Lead Authors Emily Cox, PhD, RPh Yakov Svirnovskiy, MA Chris Peterson, PharmD Aimee Tharaldson,
LTC Pharmacy Setting B/D Coverage. Because most LTC facilities are not considered a beneficiary s home 3
 Medicare Parts Issues This table provides a reference guide for the most frequent B/D coverage determination scenarios facing Part D plans and Part D pharmacy providers. It does not address all potential.
Medicare Parts Issues This table provides a reference guide for the most frequent B/D coverage determination scenarios facing Part D plans and Part D pharmacy providers. It does not address all potential.
Prior Authorization FID 16157 VER.7 UPDATED 8/2015
 Prior Authorization FID 16157 VER.7 UPDATED 8/2015 Prior Authorization 2016 MAPD Leon 3 Tier Last Updated: 10/22/2015 ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Other 1 ACTIMMUNE Products
Prior Authorization FID 16157 VER.7 UPDATED 8/2015 Prior Authorization 2016 MAPD Leon 3 Tier Last Updated: 10/22/2015 ACTEMRA Products Affected Actemra INJ 162MG/0.9ML PA Details Other 1 ACTIMMUNE Products
ACTEMRA. Step Therapy Criteria HEALTH CHOICE EXCHANGE 2016 Effective Date: 01/01/2016. PRODUCT(s) AFFECTED ACTEMRA
 ACTEMRA ACTEMRA Claim will pay automatically for Actemra if enrollee has a paid claim for at least a 1 days supply of Enbrel and Humira in the past 365 days. Otherwise, Actemra requires a step therapy
ACTEMRA ACTEMRA Claim will pay automatically for Actemra if enrollee has a paid claim for at least a 1 days supply of Enbrel and Humira in the past 365 days. Otherwise, Actemra requires a step therapy
Coverage and Pricing. of Drugs That Can Be Covered Under. Part B and Part D
 Coverage and Pricing Elizabeth Hargrave NORC at the University of Chicago Jack Hoadley of Drugs That Can Be Covered Under Part B and Part D Jennifer Thompson Georgetown University MedPAC A study conducted
Coverage and Pricing Elizabeth Hargrave NORC at the University of Chicago Jack Hoadley of Drugs That Can Be Covered Under Part B and Part D Jennifer Thompson Georgetown University MedPAC A study conducted
Filtration Guidelines for the Administration of Intravenous Medications UK Pharmacy Services Revised 8/2010
 iltration Guidelines for the Administration of Intravenous Medications UK Pharmacy Services Revised 8/2010 SUMMARY O CHANGES: Green = Added from literature (Lexi-Comp, Micromedex, pkg inserts) Yellow =
iltration Guidelines for the Administration of Intravenous Medications UK Pharmacy Services Revised 8/2010 SUMMARY O CHANGES: Green = Added from literature (Lexi-Comp, Micromedex, pkg inserts) Yellow =
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information
 Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Effective Date: 6/3/14
 North Shore-Long Island Jewish Health System, Inc. Long Island Jewish Medical Center PATIENT CARE SERVICES POLICY TITLE: ORDERING, ADMINISTRATION AND DISPOSAL OF ORAL CHEMOTHERAPEUTIC AGENTS Prepared by:
North Shore-Long Island Jewish Health System, Inc. Long Island Jewish Medical Center PATIENT CARE SERVICES POLICY TITLE: ORDERING, ADMINISTRATION AND DISPOSAL OF ORAL CHEMOTHERAPEUTIC AGENTS Prepared by:
The Basics of Pharmacy Benefits Management (PBM) 2009
 The Basics of Pharmacy Benefits Management (PBM) 2009 Andrew Kingery Pharmacy Account Management Virginia CE Forum 2009 Course# 201719 Objectives & Introduction Provide basic components of a PBM Define
The Basics of Pharmacy Benefits Management (PBM) 2009 Andrew Kingery Pharmacy Account Management Virginia CE Forum 2009 Course# 201719 Objectives & Introduction Provide basic components of a PBM Define
Drugs covered under Medicare Part B or Part D
 LABEL_NAME GENERIC_NAME MESSAGE GEMZAR INJ 1 GM GEMCITABINE HCL FOR INJ 1 GM ALIMTA INJ 500MG PEMETREXED DISODIUM FOR IV SOLN 500 MG (BASE EQUIV) FUNGIZONE INJ 50MG AMPHOTERICIN B FOR INJ 50 MG KYTRIL
LABEL_NAME GENERIC_NAME MESSAGE GEMZAR INJ 1 GM GEMCITABINE HCL FOR INJ 1 GM ALIMTA INJ 500MG PEMETREXED DISODIUM FOR IV SOLN 500 MG (BASE EQUIV) FUNGIZONE INJ 50MG AMPHOTERICIN B FOR INJ 50 MG KYTRIL
Medical School for Actuaries. June 12, 2013. Baltimore, Maryland
 Medical School for Actuaries June 12, 2013 Baltimore, Maryland Developments in the Treatment of Conditions Treated with Specialty Mediations (Cancer, MS, RA, Hemophilia) Mark S. Matusik, PharmD Developments
Medical School for Actuaries June 12, 2013 Baltimore, Maryland Developments in the Treatment of Conditions Treated with Specialty Mediations (Cancer, MS, RA, Hemophilia) Mark S. Matusik, PharmD Developments
Winter 2013. Changing landscapes, pipeline products and plan sponsor impact
 Winter 2013 Changing landscapes, pipeline products and plan sponsor impact Changing landscapes, pipeline products and plan sponsor impact The pharmaceutical landscape is changing as is the profile of blockbuster
Winter 2013 Changing landscapes, pipeline products and plan sponsor impact Changing landscapes, pipeline products and plan sponsor impact The pharmaceutical landscape is changing as is the profile of blockbuster
encourages correct prescription drug use for a particular diagnosis, promotes the safe use of prescription drugs, and helps reduce drug costs.
 Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
Prior Authorization Your health plan participates in a Prior Authorization (PA) program for specific prescription drugs. This means that Caremark must review certain information provided by your doctor
Multiple Sclerosis Center of Nebraska
 Multiple Sclerosis Center of Nebraska Date: Initial Visit Patient Information (Multiple Sclerosis) To be Completed Before Appointment Patient Name: DOB: Address: Social Security Number: Power of Attorney
Multiple Sclerosis Center of Nebraska Date: Initial Visit Patient Information (Multiple Sclerosis) To be Completed Before Appointment Patient Name: DOB: Address: Social Security Number: Power of Attorney
United Healthcare Medicare Solutions
 United Healthcare Medicare Solutions Part B Specialty Drug Prior Authorization Program Provider Training Agenda Program Mission Program Description Implementation Timeline Program Resources Prior Authorization
United Healthcare Medicare Solutions Part B Specialty Drug Prior Authorization Program Provider Training Agenda Program Mission Program Description Implementation Timeline Program Resources Prior Authorization
NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only
 Updated 5.5.14 NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only 68152-0103-03 A9543 YTTRIUM Y-90 IBRITUMOMAB TIUXETAN ZEVALIN Y-90 VIAL 9/1/2013 12/31/2013 50419-0320-05
Updated 5.5.14 NDC HCPCS HCPCS Description NDC Description Effective Date End Date X-Over Only 68152-0103-03 A9543 YTTRIUM Y-90 IBRITUMOMAB TIUXETAN ZEVALIN Y-90 VIAL 9/1/2013 12/31/2013 50419-0320-05
for Extended Stability Parenteral Drugs Third Edition Caryn M. Bing, R.Ph., M.S., FASHP Editor
 Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
University of Nebraska Prescription Drug Program 2014
 University of Nebraska Prescription Drug Program 2014 The University of Nebraska s prescription benefit program is administered by CVS Caremark, a leading national provider of prescription drug benefit
University of Nebraska Prescription Drug Program 2014 The University of Nebraska s prescription benefit program is administered by CVS Caremark, a leading national provider of prescription drug benefit
How Breast Cancer Treatment affects Massage Therapy
 How Breast Cancer Treatment affects Massage Therapy A Webinar with Tracy Walton, MS, LMT Part 4 of the More about Cancer Care and Massage Webinar Series 11 Background Tracy Walton Author Educator Researcher
How Breast Cancer Treatment affects Massage Therapy A Webinar with Tracy Walton, MS, LMT Part 4 of the More about Cancer Care and Massage Webinar Series 11 Background Tracy Walton Author Educator Researcher
4Precertification. and Referrals. Precertification...59 Referrals (Gated Plans Only)...73
 4Precertification and Referrals Precertification.....................59 Referrals (Gated Plans Only)............73 Section 4 Precertification and Referrals 58 www.oxfordhealth.com Precertification and
4Precertification and Referrals Precertification.....................59 Referrals (Gated Plans Only)............73 Section 4 Precertification and Referrals 58 www.oxfordhealth.com Precertification and
A guide to cancer types and chemotherapy medications
 A guide to cancer types and chemotherapy medications This guides lists words that mean cancer, cancer types and intravenous chemotherapy medications. If you have any questions, see page 10 for details
A guide to cancer types and chemotherapy medications This guides lists words that mean cancer, cancer types and intravenous chemotherapy medications. If you have any questions, see page 10 for details
Original Policy Date
 MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
Authorized by the U.S. District Court for the District of Massachusetts
 Authorized by the U.S. District Court for the District of Massachusetts If you made a Cash Payment or Percentage Co-Payment for Certain Drugs, from January 1, 1991 to March 1, 2008, you may be able to
Authorized by the U.S. District Court for the District of Massachusetts If you made a Cash Payment or Percentage Co-Payment for Certain Drugs, from January 1, 1991 to March 1, 2008, you may be able to
PATIENT ASSISTANCE PROGRAMS
 PATIENT ASSISTANCE PROGRAMS Definitions SAP Class I Class II BC Cancer Agency Health Canada Special Access Program Reimbursed for active cancer or approved treatment or approved indication only Reimbursed
PATIENT ASSISTANCE PROGRAMS Definitions SAP Class I Class II BC Cancer Agency Health Canada Special Access Program Reimbursed for active cancer or approved treatment or approved indication only Reimbursed
Outpatient Prescription Drug Benefit
 Outpatient Prescription Drug Benefit GENERAL INFORMATION This supplemental Evidence of Coverage and Disclosure Form is provided in addition to your Member Handbook and Health Plan Benefits and Coverage
Outpatient Prescription Drug Benefit GENERAL INFORMATION This supplemental Evidence of Coverage and Disclosure Form is provided in addition to your Member Handbook and Health Plan Benefits and Coverage
Cardiac Procedure: Outpatient Office Inpatient Emergent/Urgent Diagnostic Catheterization Required Required Not Not required
 Important Changes In Notification and Prior Authorization Procedures (This is revised from the article that was posted in the September 2012 Network Bulletin. Changes are in Section 3, Standardization
Important Changes In Notification and Prior Authorization Procedures (This is revised from the article that was posted in the September 2012 Network Bulletin. Changes are in Section 3, Standardization
Prescription Drug Benefit
 Prescription Drug Benefit The Cleveland Clinic Employee Health Plan (EHP) Total Care Prescription Drug Benefit is administered through CVS Caremark. CVS Caremark has a dedicated, toll-free Customer Service
Prescription Drug Benefit The Cleveland Clinic Employee Health Plan (EHP) Total Care Prescription Drug Benefit is administered through CVS Caremark. CVS Caremark has a dedicated, toll-free Customer Service
Specialty Drug Management Solutions You Haven t Heard Before
 Specialty Drug Management Solutions You Haven t Heard Before Sarah Martin, ASA, MAAA, CEBS Vice President, Senior Pharmacy Consultant Lockton Kansas City, Missouri The opinions expressed in this presentation
Specialty Drug Management Solutions You Haven t Heard Before Sarah Martin, ASA, MAAA, CEBS Vice President, Senior Pharmacy Consultant Lockton Kansas City, Missouri The opinions expressed in this presentation
Specialty drug program. Save time. Save money. Feel good.
 Specialty drug program Save time. Save money. Feel good. What are specialty drugs? Specialty drugs are used to treat serious or ongoing medical conditions such as multiple sclerosis, hemophilia, hepatitis
Specialty drug program Save time. Save money. Feel good. What are specialty drugs? Specialty drugs are used to treat serious or ongoing medical conditions such as multiple sclerosis, hemophilia, hepatitis
Cost Differences in Cancer Care Across Settings
 Cost Differences in Cancer Care Across Settings August 2013 THE MORAN COMPANY 1 Cost Differences in Cancer Care Across Settings In a prior memorandum, we presented evidence documenting the growing share
Cost Differences in Cancer Care Across Settings August 2013 THE MORAN COMPANY 1 Cost Differences in Cancer Care Across Settings In a prior memorandum, we presented evidence documenting the growing share
RIDER ADDING PRESCRIPTION DRUG COVERAGE
 Group Health Incorporated (hereinafter referred to as GHI ) 441 Ninth Avenue New York, NY 10001 RIDER ADDING PRESCRIPTION DRUG COVERAGE RETAIL DRUG PROGRAM Deductible: Generic Drugs: Brand Name Preferred
Group Health Incorporated (hereinafter referred to as GHI ) 441 Ninth Avenue New York, NY 10001 RIDER ADDING PRESCRIPTION DRUG COVERAGE RETAIL DRUG PROGRAM Deductible: Generic Drugs: Brand Name Preferred
TABLE OF CONTENTS. Home Infusion Therapy Guidelines... 2
 TABLE OF CONTENTS Home Infusion Therapy Guidelines... 2 Services normally considered eligible for benefits... 2 Description... 2 Pre-certification Requirements... 3 Billing Guidelines... 3 Home Infusion
TABLE OF CONTENTS Home Infusion Therapy Guidelines... 2 Services normally considered eligible for benefits... 2 Description... 2 Pre-certification Requirements... 3 Billing Guidelines... 3 Home Infusion
The definition of the small business market is changing to 1-100 employees. FAQs for brokers and employers.
 The definition of the small business market is changing to 1-100 employees. FAQs for brokers and employers. On January 1, 2016, as a result of health reform, the definition of a small business will increase
The definition of the small business market is changing to 1-100 employees. FAQs for brokers and employers. On January 1, 2016, as a result of health reform, the definition of a small business will increase
Drugs Used to Treat Nausea and Vomiting
 Evaluating the Oral 5-HT3 Antagonists: Drugs Used to Treat Nausea and Vomiting Comparing Effectiveness, Safety, and Price Our Recommendations A Summary The 5-HT3 antagonists are a class of drugs often
Evaluating the Oral 5-HT3 Antagonists: Drugs Used to Treat Nausea and Vomiting Comparing Effectiveness, Safety, and Price Our Recommendations A Summary The 5-HT3 antagonists are a class of drugs often
PATIENT / VISIT INFORMATION PATIENT INFORMATION
 PATIENT / VISIT INFORMATION PATIENT INFORMATION Name of Patient: Date of Birth: Date of Visit: VISIT INFORMATION Please complete this form in its entirety, and present it to the registration desk when
PATIENT / VISIT INFORMATION PATIENT INFORMATION Name of Patient: Date of Birth: Date of Visit: VISIT INFORMATION Please complete this form in its entirety, and present it to the registration desk when
BREAST CANCER - METASTATIC & LOCALLY ADVANCED CHEMOTHERAPY REGIMENS Capecitabine. Capecitabine + Docetaxel. Capecitabine + Vinorelbine
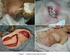 Capecitabine Capecitabine 1000-1250mg/m 2 oral TWICE daily for 14 days Until disease progression Capecitabine + Docetaxel Capecitabine 750-1000mg/m 2 oral TWICE daily for 14 days Up to 6 cycles Capecitabine
Capecitabine Capecitabine 1000-1250mg/m 2 oral TWICE daily for 14 days Until disease progression Capecitabine + Docetaxel Capecitabine 750-1000mg/m 2 oral TWICE daily for 14 days Up to 6 cycles Capecitabine
Drugs That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS
 That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS ACNE Approve for those 12 years of age and older AVITA, RETIN-A MICRO, TRETINOIN ACTHAR HP All FDA-approved
That Require Prior Authorization (PA) Before Being Approved for Coverage PRIOR AUTHORIZATION MEDICATIONS ACNE Approve for those 12 years of age and older AVITA, RETIN-A MICRO, TRETINOIN ACTHAR HP All FDA-approved
Treating Recurrent Metastatic Breast Cancer
 BREAST CANCER Treating Recurrent Metastatic Breast Cancer Presented by Julie Gralow, MD Fred Hutchinson Cancer Research Center Generosa Grana, MD UMDNJ/Robert Wood Johnson School of Medicine Patricia Spicer,
BREAST CANCER Treating Recurrent Metastatic Breast Cancer Presented by Julie Gralow, MD Fred Hutchinson Cancer Research Center Generosa Grana, MD UMDNJ/Robert Wood Johnson School of Medicine Patricia Spicer,
Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines
 Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines Survey Finds Private Sector Negotiations Provide Both Savings and Choice, Making Government Interference Unnecessary
Medicare Part D Plans Deliver Significant Savings on Innovative, Breakthrough Medicines Survey Finds Private Sector Negotiations Provide Both Savings and Choice, Making Government Interference Unnecessary
REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans
 Moda Health Referral/Authorization Guidelines Oregon updated September 2014 Page 1 of 7 REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans Referral & Authorization Information Referral and authorization
Moda Health Referral/Authorization Guidelines Oregon updated September 2014 Page 1 of 7 REFERRAL/AUTHORIZATION GUIDELINES Commercial Plans Referral & Authorization Information Referral and authorization
Cytokine and CAM Antagonists
 Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
Texas Prior Authorization Program Clinical Edit Criteria Drug/Drug Class Clinical Edit Information Included in this Document Actemra (Tocilizumab) Drugs requiring prior authorization: the list of drugs
HealthPartners, Inc. 2013 Medicare Part D Formulary ID 13142, Version 22 Prior Authorization Criteria. Last Updated: 11/01/2013
 ACTEMRA Actemra (1) DIAGNOSIS OF MODERATELY TO SEVERELY ACTIVE RHEUMATOID ARTHRITIS, OR (2) JUVENILE IDIOPATHIC ARTHRITIS, AND (3) DOCUMENTATION OF MEDICAL CONTRAINDICATIONS OR FAILURE WITH ENBREL OR HUMIRA.
ACTEMRA Actemra (1) DIAGNOSIS OF MODERATELY TO SEVERELY ACTIVE RHEUMATOID ARTHRITIS, OR (2) JUVENILE IDIOPATHIC ARTHRITIS, AND (3) DOCUMENTATION OF MEDICAL CONTRAINDICATIONS OR FAILURE WITH ENBREL OR HUMIRA.
UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 RA05/15.654
 UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 1PU 2PU 3PU 4PU UPU UPU UPU UPU P P P P P Tier Master List (PDL) (Drug Formulary) Effective July 1, 2015 THE BLUEGRASS FAMILY HEALTH
UMASTER PREFERRED DRUG LIST (DRUG FORMULARY) Effective July 1, 2015 1PU 2PU 3PU 4PU UPU UPU UPU UPU P P P P P Tier Master List (PDL) (Drug Formulary) Effective July 1, 2015 THE BLUEGRASS FAMILY HEALTH
ACNE PRODUCTS. Affected Drugs: Epiduo Retin-A Tretinoin. Covered Uses: All FDA-approved indications not otherwise excluded from Part D
 ACNE PRODUCTS Epiduo Retin-A Tretinoin Exclusion Criteria: Esthetic purposes N/A N/A TSA 2015 Royal, Classic, Vital and Vital Plus Formulary Page 1 of 148 ACTEMRA Actemra Exclusion Criteria: 1) Active
ACNE PRODUCTS Epiduo Retin-A Tretinoin Exclusion Criteria: Esthetic purposes N/A N/A TSA 2015 Royal, Classic, Vital and Vital Plus Formulary Page 1 of 148 ACTEMRA Actemra Exclusion Criteria: 1) Active
P&T Committee Meeting Minutes (GHP Family Business) March 18, 2014
 P&T Committee Meeting Minutes (GHP Family Business) March 18, 2014 Present: Bret Yarczower, MD, MBA Chair Peter Mikhail, Pharm.D., MBA Secretary Charles Baumgart, MD, MBA Keith Boell, DO Kimberly Clark,
P&T Committee Meeting Minutes (GHP Family Business) March 18, 2014 Present: Bret Yarczower, MD, MBA Chair Peter Mikhail, Pharm.D., MBA Secretary Charles Baumgart, MD, MBA Keith Boell, DO Kimberly Clark,
MEDICAL CENTER ADMINISTRATIVE POLICY AND PROCEDURES SCOPE KFH Hospital, City Section No.
 of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
of 22 I. Purpose To establish safe medication practices for High Alert medications to maximize the safety of the medication processes associated with these medications. II. Policy. High alert medications
Non-Hodgkin Lymphoma Richard Orlowski, MD
 Non-Hodgkin Lymphoma Richard Orlowski, MD The American Cancer Society (ACS) estimates that 69,740 Americans will be diagnosed with non-hodgkin lymphoma (NHL) in 2013. Excluding non-melanoma skin cancers,
Non-Hodgkin Lymphoma Richard Orlowski, MD The American Cancer Society (ACS) estimates that 69,740 Americans will be diagnosed with non-hodgkin lymphoma (NHL) in 2013. Excluding non-melanoma skin cancers,
Medicines for Rheumatoid. Arthritis. A Review of the Research for Adults
 Medicines for Rheumatoid Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this summary is for you if: Your doctor* has told you that you have rheumatoid (pronounced
Medicines for Rheumatoid Arthritis A Review of the Research for Adults Is This Information Right for Me? Yes, this summary is for you if: Your doctor* has told you that you have rheumatoid (pronounced
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES I. Requirements for Prior Authorization of Tysabri
 MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF I. Requirements for Prior Authorization of Tysabri A. Prescriptions That Require Prior Authorization All prescriptions for Tysabri must be prior authorized.
MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF I. Requirements for Prior Authorization of Tysabri A. Prescriptions That Require Prior Authorization All prescriptions for Tysabri must be prior authorized.
An Economic Assessment of ANCO Member Practices Roberta Buell, M.B.A. OnPoint Oncology LLC. Patricia Falconer, M.B.A.
 An Economic Assessment of ANCO Member Practices Roberta Buell, M.B.A. OnPoint Oncology LLC Patricia Falconer, M.B.A. Health Options José Luis González Association of Northern California Oncologists Abstract
An Economic Assessment of ANCO Member Practices Roberta Buell, M.B.A. OnPoint Oncology LLC Patricia Falconer, M.B.A. Health Options José Luis González Association of Northern California Oncologists Abstract
Prior Authorization, Pharmacy and Health Case Management Information. Prior Authorization. Pharmacy Information. Health Case Management
 Prior Authorization, Pharmacy and Health Case Management Information The purpose of this information sheet is to provide you with details on how Great-West Life will be assessing and managing your claim
Prior Authorization, Pharmacy and Health Case Management Information The purpose of this information sheet is to provide you with details on how Great-West Life will be assessing and managing your claim
Transitioning to Express Scripts
 Transitioning to Express Scripts Welcome to Express Scripts. We re pleased to announce that, beginning 1/1/2015 the City of Frisco prescription benefit will be managed by Express Scripts. Express Scripts
Transitioning to Express Scripts Welcome to Express Scripts. We re pleased to announce that, beginning 1/1/2015 the City of Frisco prescription benefit will be managed by Express Scripts. Express Scripts
COVERAGE MANAGEMENT PROGRAMS
 COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
FREQUENTLY ASKED QUESTIONS ABOUT THE CVS CAREMARK PRESCRIPTION DRUG PROGRAM
 FREQUENTLY ASKED QUESTIONS ABOUT THE CVS CAREMARK PRESCRIPTION DRUG PROGRAM ABBVIE EMPLOYEES WANT TO KNOW What s New in 2015? AbbVie is making changes in its pharmacy benefit program to ensure our medical
FREQUENTLY ASKED QUESTIONS ABOUT THE CVS CAREMARK PRESCRIPTION DRUG PROGRAM ABBVIE EMPLOYEES WANT TO KNOW What s New in 2015? AbbVie is making changes in its pharmacy benefit program to ensure our medical
BreastCancerTrials.org History Form: Metastatic Breast Cancer ABOUT ME
 BreastCancerTrials.org History Form: Metastatic Breast Cancer This form is for patients with metastatic breast cancer who were: Were recently diagnosed with metastatic breast cancer (cancer that has spread
BreastCancerTrials.org History Form: Metastatic Breast Cancer This form is for patients with metastatic breast cancer who were: Were recently diagnosed with metastatic breast cancer (cancer that has spread
Contents General Information... 1. General Information
 Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
Contents General Information... 1 Preferred Drug List... 2 Pharmacies... 3 Prescriptions... 4 Generic and Preferred Drugs... 5 Express Scripts Website and Mobile App... 5 Specialty Medicines... 5 Prior
Implications of dose rounding intravenous chemotherapy at a community based hospital
 Implications of dose rounding intravenous chemotherapy at a community based hospital 1 2 ABSTRACT OBJECTIVES: To quantify and evaluate the total number of pharmacist interventions completed for dose rounding
Implications of dose rounding intravenous chemotherapy at a community based hospital 1 2 ABSTRACT OBJECTIVES: To quantify and evaluate the total number of pharmacist interventions completed for dose rounding
FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS
 FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS Money is tight for everyone these days. Many families work hard to stay within a budget, and, if they are lucky, they are also able to
FREE PRESCRIPTION DISCOUNT CARD AVAILABLE TO WELD COUNTY RESIDENTS Money is tight for everyone these days. Many families work hard to stay within a budget, and, if they are lucky, they are also able to
this 7^ day of September 2014 by Randall S. Gregg Special Deputy Director
 r STATE OF MICHIGAN DEPARTMENT OF INSURANCE AND FINANCIAL SERVICES Before the Director of Insurance and Financial Services In the matter of: Petitioner, v File No. 143525-001 Health Alliance Plan of Michigan,
r STATE OF MICHIGAN DEPARTMENT OF INSURANCE AND FINANCIAL SERVICES Before the Director of Insurance and Financial Services In the matter of: Petitioner, v File No. 143525-001 Health Alliance Plan of Michigan,
Overview of the Specialty Drug Trend
 WHITE PAPER Overview of the Specialty Drug Trend Succeeding In The Rapidly Changing U.S. Specialty Market 1 Specialty drugs are prescribed to treat complex conditions such as cancer, HIV and inflammatory
WHITE PAPER Overview of the Specialty Drug Trend Succeeding In The Rapidly Changing U.S. Specialty Market 1 Specialty drugs are prescribed to treat complex conditions such as cancer, HIV and inflammatory
5.07.09. Aubagio. Aubagio (teriflunomide) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
GENERAL INFORMATION. With Express Scripts, you have access to:
 CONTENTS GENERAL INFORMATION... 1 PREFERRED DRUG LIST....2 PHARMACIES... 3 PRESCRIPTIONS... 4 GENERIC AND PREFERRED DRUGS... 5 EXPRESS SCRIPTS WEBSITE AND MOBILE APP... 5 SPECIALTY MEDICATIONS... 6 PRIOR
CONTENTS GENERAL INFORMATION... 1 PREFERRED DRUG LIST....2 PHARMACIES... 3 PRESCRIPTIONS... 4 GENERIC AND PREFERRED DRUGS... 5 EXPRESS SCRIPTS WEBSITE AND MOBILE APP... 5 SPECIALTY MEDICATIONS... 6 PRIOR
Bayer HealthCare, LLC Sharps Disposal Submission to CalRecycle July 1, 2014
 Bayer HealthCare, LLC Sharps Disposal Submission to CalRecycle July 1, 2014 1. A pharmaceutical manufacturer that sells or distributes a medication in California that is usually intended to be self-injected
Bayer HealthCare, LLC Sharps Disposal Submission to CalRecycle July 1, 2014 1. A pharmaceutical manufacturer that sells or distributes a medication in California that is usually intended to be self-injected
Prescription Drug Plan
 Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
Provider Manual. This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc.
 2014 Provider Manual This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc. We hope you find this information and the enclosed documents
2014 Provider Manual This manual is to help you learn more about The Ohio State University s medical plans, administered by OSU Health Plan Inc. We hope you find this information and the enclosed documents
Novel Opportunities for Engagement Utilizing in House Pharmacy Services
 Novel Opportunities for Engagement Utilizing in House Pharmacy Services Ray Bailey, BSPharm RPh Director of Pharmacy, FCS Rx to Go Pharmacy rbailey@flcancer.com Angel Aslo, Pharm.D. Director of Pharmacy,
Novel Opportunities for Engagement Utilizing in House Pharmacy Services Ray Bailey, BSPharm RPh Director of Pharmacy, FCS Rx to Go Pharmacy rbailey@flcancer.com Angel Aslo, Pharm.D. Director of Pharmacy,
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE May 11, 2015 SUBJECT EFFECTIVE DATE May 18, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of Multiple Sclerosis Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
ISSUE DATE May 11, 2015 SUBJECT EFFECTIVE DATE May 18, 2015 MEDICAL ASSISTANCE BULLETIN NUMBER *See below BY Prior Authorization of Multiple Sclerosis Agents Pharmacy Service Leesa M. Allen, Deputy Secretary
New York State Auto Dealers Association Group Insurance Trust (GIT) Prescription Drug Coverage Summary
 New York State Auto Dealers Association Group Insurance Trust (GIT) Prescription Drug Coverage Summary Effective January 1, 2014, all pharmacy coverage will be administered by Express Scripts and its affiliates.
New York State Auto Dealers Association Group Insurance Trust (GIT) Prescription Drug Coverage Summary Effective January 1, 2014, all pharmacy coverage will be administered by Express Scripts and its affiliates.
THE HAZARDOUS WASTE (ENGLAND AND WALES) REGULATIONS 2005
 THE HAZARDOUS WASTE (ENGLAND AND WALES) REGULATIONS 2005 Interim Guidance for the NHS Hospital Sector for England and Wales and Information for Scotland Additional paper copies may be requested by contacting:
THE HAZARDOUS WASTE (ENGLAND AND WALES) REGULATIONS 2005 Interim Guidance for the NHS Hospital Sector for England and Wales and Information for Scotland Additional paper copies may be requested by contacting:
Local Coverage Article: Self-Administered Drug Exclusion List (A51866)
 Local Coverage Article: Self-Administered Drug Exclusion List (A51866) Contractor Information Contractor Name Novitas Solutions, Inc. Article Information General Information Article ID A51866 General Article
Local Coverage Article: Self-Administered Drug Exclusion List (A51866) Contractor Information Contractor Name Novitas Solutions, Inc. Article Information General Information Article ID A51866 General Article
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES. I. Requirements for Prior Authorization of Hepatitis C Agents
 MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF PHARMACEUTICAL SERVICES I. Requirements for Prior Authorization of Hepatitis C Agents A. Prescriptions That Require Prior Authorization Prescriptions for Interferon,
MEDICAL ASSISTANCE HBOOK PRI AUTHIZATION OF PHARMACEUTICAL SERVICES I. Requirements for Prior Authorization of Hepatitis C Agents A. Prescriptions That Require Prior Authorization Prescriptions for Interferon,
BreastCancerTrials.org History Form: Completed Treatment for Breast Cancer ABOUT ME
 BreastCancerTrials.org History Form: Completed Treatment for Breast Cancer This form is for patients with DCIS or early stage invasive cancer who are: On hormone therapy after breast cancer surgery Or
BreastCancerTrials.org History Form: Completed Treatment for Breast Cancer This form is for patients with DCIS or early stage invasive cancer who are: On hormone therapy after breast cancer surgery Or
Excluded Drug Criteria. Coverage Duration. Age Restrictions. Prescriber Restrictions. Prior Authorization Type Description.
 2015 Cigna-HealthSpring - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna- HealthSpring Preferred Plus (HMO) (Updated December 2015) Name Other ABELCET ABRAXANE
2015 Cigna-HealthSpring - H0354 - Cigna-HealthSpring Preferred (HMO), Cigna-HealthSpring Achieve Plus (HMO SNP), Cigna- HealthSpring Preferred Plus (HMO) (Updated December 2015) Name Other ABELCET ABRAXANE
