Respiratory Issues in the Management of Children With Neuromuscular Disease
|
|
|
- Corey Reed
- 8 years ago
- Views:
Transcription
1 Respiratory Issues in the Management of Children With Neuromuscular Disease Howard B Panitch MD Introduction Physiological Considerations Airway Clearance in Children With Neuromuscular Weakness Secretion-Extraction Maneuvers Mucus Mobilization Devices Mechanical Ventilatory Support NPPV in Young Children Transition to Adult Care Summary Most children with neuromuscular disease eventually require assistance with airway clearance and with breathing, especially during sleep. Techniques and devices for airway clearance and noninvasive ventilation that are commonly used in adults have been successfully adapted for use in infants and young children. Both physiological differences and small size of young patients with neuromuscular disease, however, can limit the applicability of such interventions or require special consideration. Measurements to identify the appropriate time to begin airway clearance assistance are lacking for young children, and the role of early introduction of noninvasive ventilation to preserve or enhance lung growth and chest-wall mobility remains to be elucidated. The paucity of nasal interfaces and headgear commercially made for small patients can reduce patient tolerance of noninvasive ventilation and exacerbate patient-ventilator dyssynchrony. Despite these issues, a greater number of children with neuromuscular diseases are living well past their second decade. Strategies to transition these patients to appropriate adult-care providers, to secure cost-effective health care for them, and to help integrate them into adult society must be developed. Key words: neuromuscular disease, pediatric, mechanical ventilation, noninvasive ventilation. [Respir Care 2006; 51(8): Daedalus Enterprises] Introduction The onset of pulmonary symptoms in children with neuromuscular weakness depends in large part on the type of Howard B Panitch MD is affiliated with the University of Pennsylvania School of Medicine, and with the Division of Pulmonary Medicine, Children s Hospital of Philadelphia, Philadelphia, Pennsylvania. Howard B Panitch MD presented a version of this paper at the 37th RESPIRATORY CARE Journal Conference, Neuromuscular Disease in Respiratory and Critical Care Medicine, held March 17 19, 2006, in Ixtapa, Mexico. underlying disease. For instance, a boy with Duchenne muscular dystrophy may not experience any respiratory problems until mid-adolescence, whereas an infant with spinal muscular atrophy type I is likely to develop respiratory compromise within the first year of life. In either case, there is a typical sequence of events that leads to Correspondence: Howard B Panitch MD, Division of Pulmonary Medicine, Children s Hospital of Philadelphia, 5th Floor Wood Building, 34th Street and Civic Center Boulevard, Philadelphia PA panitch@ .chop.edu. RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 885
2 Table 1. Some Physiological Considerations in Infants and Young Children Regarding the Risk for Mucus Plugging and Atelectasis Smaller absolute airway size Distribution of intrathoracic resistances Higher airway compliance Ineffective collateral ventilation Lower elastic recoil pressure Higher chest-wall compliance respiratory insufficiency and ultimately to respiratory failure. 1,2 Initially, respiratory muscle weakness leads to impaired cough and airway clearance, so these patients are prone to recurrent atelectasis and chest infections. Progressive inspiratory muscle weakness first causes nocturnal respiratory dysfunction, which is manifested by frequent arousals, sleep fragmentation, and sleep-related hypoventilation. Subsequently, hypercapnia extends into the daytime and frank respiratory failure ensues. The duration of this timeline can be expanded by interventions such as assistance with clearance of respiratory secretions and nocturnal mechanical ventilation, or it can be compressed by acute respiratory illnesses. Many of the interventions that have been used in adults with neuromuscular disease to support the respiratory system have also been applied to infants and children. There are, however, unique considerations and limitations of such therapies related to size and to physiological characteristics of the respiratory system of infants and young children. This review will discuss some of those aspects of respiratory care. Physiological Considerations Infants and young children with neuromuscular disease are at higher risk of atelectasis and airway obstruction from mucus plugging, compared with older children and adults (Table 1). Young children s airways are smaller, and a greater proportion of intrathoracic resistance resides in the small airways of children under 5 years of age. 3 Any disease process that affects small airways (eg, viral bronchiolitis), therefore, will cause a greater increase in total respiratory system resistance in young children, compared with older children and adults. There is also a normal maturational reduction in airway wall compliance, so the central airways of infants and young children are more collapsible than are those of adults. 4 The pores of Kohn and other interalveolar pathways are not well developed in infants, so collateral ventilation is not as effective as in older children and adults. 5 Not only do airway characteristics place young children with neuromuscular disease at higher risk for obstruction, but so also do both normal and disease-specific changes in airway/parenchyma interactions. Alveolar multiplication is largely a postnatal event, occurring over the first 2 4 years of life. Thus, infants have fewer alveoli and also fewer alveolar attachments to airway walls than do older children and adults. Elastic recoil of the lung, a force that tethers airways open and is exerted through the alveolar attachments to the airway walls, is also less in infants and increases with age. 6 8 In addition, the chest wall is highly compliant in infants and young children, and it does not become as stiff as the lung until approximately 2 years of age. 9 The chest wall of a young child with neuromuscular disease is even more compliant than that of a healthy child, 10 and it may not achieve the same passive stiffness of the lung until 4 years or more. The outward recoil of the chest wall, coupled via the pleural space to the lung parenchyma, is another important force that helps maintain airway patency. Thus, young children with neuromuscular disease are at higher risk for developing areas of microatelectasis from chronically breathing at low lung volume. Another consideration for pediatric patients with neuromuscular disease is growth, both of the lung and of the body. Chest-wall distortion can lead to acquired pectus excavatum deformity, 2 which can compromise tidal volume further. The degree to which chronic postnatal lowtidal-volume breathing impacts subsequent lung development is not known, but there are concerns that it reduces the potential for lung growth. 11 In addition, because of the compliance characteristics of the chest wall, young children with neuromuscular weakness must expend extra energy, in the form of intercostal muscle contraction, to defend tidal volume and to offset the tendency of the chest wall to deform during inspiration. Thus, some children maintain adequate gas exchange at a much higher energy cost, and can have growth failure as a result. Airway Clearance in Children With Neuromuscular Weakness Cough is the chief mechanism responsible for clearing the central airways of secretions when the mucociliary escalator is made ineffective or is overwhelmed by infection and increased mucus production. A normal cough requires a pre-cough inspiration to 60 90% of total lung capacity, followed by brief glottic closure and simultaneous contraction of expiratory muscles. The glottis then opens and the pressurized thorax forcibly expulses air at a high flow (36 1,000 L/min in healthy adults). 12 Cough in patients with neuromuscular disease can be compromised for several reasons. Inspiratory muscle weakness impairs one s ability to take a deep breath and so dilate intrathoracic airways and increase driving (elastic recoil) pressure. Bulbar weakness or presence of a tracheostomy tube impairs glottic closure so that thoracic pressurization is compromised. Expiratory muscle weakness reduces transmural airway pressure, resulting in a diminu- 886 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8
3 tion of airway compression and a reduction in or absence of supramaximal cough-flow transients. Cough-flow transients accentuate the shearing forces that help propel mucus toward the central airways. The ability to continue to generate these flow spikes during coughing correlates with improved survival among adults with neuromuscular disease, despite the presence of profound respiratory muscle weakness. 13 Assistance with airway clearance is a critical component in the care of children with neuromuscular disease, because of their propensity to develop mucus plugging and atelectasis with chest infections, and their greater exposure to common viral respiratory illnesses. In fact, acute respiratory illness leading to respiratory compromise was found to be the most common cause of unplanned admission to a pediatric intensive care unit among children with neuromuscular disease. 14 Most of the techniques used in adults with neuromuscular disease to enhance secretion clearance have also been successfully used in children. Thus, manual assisted cough, breath stacking, manual and mechanical insufflation, and mechanical exsufflation with negative pressure have all been used to treat pediatric patients with neuromuscular disease. 15 The common goal of all of these interventions, used alone or in combination, is to increase the velocity of expiratory flow during a cough maneuver. Peak cough flow was the single most important factor in determining whether the artificial airway (endotracheal or tracheostomy tube) could be removed in a group of 37 adults with neuromuscular disease who required assistance with secretion removal. 16 Only those patients who, alone or with assistance, could generate peak cough flow 160 L/min were able to have the airway decannulated, independent of their need for ventilatory assistance. Those with peak cough flow 160 L/min required ongoing intrathoracic airway access to facilitate suctioning and removal of secretions. In both healthy subjects 17 and those with neuromuscular disease, 18 acute viral illness can cause a transient reduction in respiratory muscle strength. Thus, using a peak-coughflow cutoff value of 160 L/min to identify those patients at risk for impaired secretion removal may be too stringent. In 2 series, 19,20 when peak cough flow in adults with neuromuscular disease was 270 L/min during periods of wellness, it routinely fell below 160 L/min during acute respiratory illness. In fact, only one patient among these groups who was able to generate an assisted peak cough flow 270 L/min developed pneumonia or respiratory distress. The use of a target peak cough flow 270 L/min to identify patients at risk for lower-respiratory-tract disease, however, may not be appropriate in children. Among healthy 5 18-year-old volunteers studied, the majority of those 13 years of age generated peak cough flow 270 L/ min. 21 Among this group, however, most were able to generate maximum expiratory pressure in excess of 60 cm H 2 O. In another study, involving a group of 22 adolescents and young adults with neuromuscular disease, the ability to generate cough flow transients was associated with generation of maximum expiratory pressure above 60 cm H 2 O. 22 Adequacy of unassisted peak cough flow also correlated with lung function in a group of year-old boys with Duchenne muscular dystrophy, 23 but many children with other types of neuromuscular disease are either too young or may be too intellectually impaired to perform standard spirometry. Aside from this one study, at present there are no established respiratory-muscle or lung-function data to help the practitioner determine which young children are at greater risk for secretion retention, atelectasis, and pneumonia. Secretion-Extraction Maneuvers Among a group of 21 ventilator-assisted adults with neuromuscular disease, breath stacking, manually assisted cough, and use of a mechanical insufflator-exsufflator all significantly increased peak cough flow, compared to the flow during unassisted cough. 24 With all the treatments tested, the patients generated peak cough flow 2.7 L/s (160 L/min). The highest values were achieved with the insufflator-exsufflator. Chatwin et al studied a group of patients with a variety of neuromuscular diseases, eight of whom were years old. 15 As a group, these children had profound respiratory muscle weakness (maximal inspiratory pressure cm H 2 O, maximal expiratory pressure cm H 2 O). Peak cough flow was measured using standard physiotherapy-assisted cough (a component of which included manual assisted cough), in which inspiration was augmented with a noninvasive ventilator, exsufflation-assisted cough, and insufflator-exsufflator-assisted cough. Although the inspiratory and expiratory pressures used with the insufflator-exsufflator were modest ( 15 3 cm H 2 O during insufflation, and 15 9cmH 2 O during exsufflation), the insufflatorexsufflator still generated significantly higher peak cough flow than did unassisted cough. Increases in peak cough flow with the other methods were not statistically higher than those generated without cough assistance. All methods of cough assistance were well tolerated by the patients. Miske et al reported their experience with the use of an insufflator-exsufflator with 62 children and young adults, ranging in age from 3 months to 28.6 years (median 12.6 years). 25 Median insufflation pressure used was 30 cm H 2 O (range cm H 2 O), and median exsufflation pressure was 30 cm H 2 O (range 20 to 50 cm H 2 O). There was no correlation between the pressures used and either age or type of underlying neuromuscular disease. The device was found to be well tolerated RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 887
4 Fig. 1. A: Seven-month old with Prader-Willi syndrome admitted with respiratory distress. There is almost a complete white-out of the left lung, along with absence of air bronchograms and a leftward mediastinal shift. B: After 12 hours of frequent use of a mechanical insufflator-exsufflator, there is dramatic clearing of the left hemithorax, with residual left-lower-lobe atelectasis (arrows). C: After 3 days of mechanical insufflator-exsufflator use the atelectasis has resolved. and safe, the only adverse effect being the appearance of premature ventricular contractions during insufflator-exsufflator use in an adolescent with Duchenne muscular dystrophy and cardiomyopathy. Five patients reported fewer episodes of pneumonia after starting insufflator-exsufflator therapy, and four had demonstrable improvement in chronic atelectasis (Fig. 1). Mucus Mobilization Devices Two techniques that have been used in children and adults with neuromuscular disease to mobilize secretions from more peripheral to central airways are high-frequency chest-wall oscillation and intrapulmonary percussive ventilation. Both techniques result in oscillation of the airways and generation of high-velocity but short-frequency waves of airflow. With high-frequency chest-wall oscillation, energy is applied to the chest wall and transmitted to the airways, whereas with intrapulmonary percussive ventilation, oscillations are applied directly to the airway opening. Critical evaluation of high-frequency chest-wall oscillation in patients with neuromuscular disease has been sparse. In 7 children with quadriplegic cerebral palsy, routine use of high-frequency chest-wall oscillation resulted in fewer episodes of pneumonia and fewer respiratoryrelated hospitalizations in the year after initiating its use, compared with the year before. 26 In addition, among the children with tracheostomies, suctioning was more effective after institution of chest-wall oscillation. Intrapulmonary percussive ventilation is used in conjunction with aerosol therapy. High-frequency mini-bursts of air are applied to the airway opening while liquid (often containing a bronchodilator) is nebulized. Birnkrant et al described the use of intrapulmonary percussive ventilation to treat atelectasis or pneumonia in 4 patients with neuromuscular disease. 27 Two children and one adult experienced rapid improvement in chest radiographic appearance and oxyhemoglobin saturation following institution of intrapulmonary percussive ventilation, after routine chest physiotherapy and manually assisted cough failed to improve their clinical status. The fourth patient also improved, but more slowly. Among 8 ventilator-dependent young adults with Duchenne muscular dystrophy, intrapulmonary percussive ventilation improved secretion removal, but only in those patients considered to be hypersecretors ( 30 ml of secretions per day). 28 Those who did not produce excessive secretions had no significant increase in secretion removal, compared with standard physiotherapy techniques, including manually assisted cough. Intrapulmonary percussive ventilation has also been studied in intubated children without neuromuscular disease who developed atelectasis. 29 In a retrospective review of 46 patients between 1 month and 15 years of age (median 4.2 years), intrapulmonary percussive ventilation significantly improved atelectasis, as quantified by a scoring system. Two patients 3 kg developed hypotension during its use, so subsequent use of the device was limited to patients 3 kg. In a small prospective portion of the study, 7 patients who were treated with intrapulmonary percussive ventilation had greater improvement and more rapid resolution of atelectasis (3.1 d vs 6.2 d, p 0.018) than did 5 patients treated with standard chest physiotherapy. Mechanical Ventilatory Support American 30 and European 31 guidelines suggest that patients with neuromuscular disease should receive ventilatory support when daytime hypercapnia (P CO2 50 mm Hg) exists. Others have instituted nocturnal mechanical ventilation when the patient has sleep hypoventilation (P CO2 50 mm Hg) accompanied by oxyhemoglobin desaturation ( 92%) or a history of recurrent hospitalization for pneumonia or atelectasis. 32 Nocturnal noninvasive positive-pressure ventilation (NPPV) improves survival and reduces the frequency of hospitalization, 32 even in children with progressive neuromuscular diseases. Nocturnal NPPV also improves diurnal gas exchange 34 and normalizes sleep-disordered breathing. 32,36 Nevertheless, the timing of institution of NPPV remains controversial. The role of mechanical ventilation in promoting lung growth, or at least preventing decline in lung 888 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8
5 function, in children with respiratory muscle weakness has not been fully explored. A multicenter study of the role of preventive NPPV in boys with Duchenne muscular dystrophy disappointingly found no evidence for preservation of lung function in those patients treated with NPPV. 37 The patients were randomized to receive NPPV or conventional therapy if vital capacity was 20 50% predicted and gas exchange was normal. Early institution of NPPV failed to halt the progressive loss of lung function or appreciably improve blood-gas abnormalities in the treatment group, compared with controls. Most alarmingly, however, was the finding of greater mortality in the group that received NPPV (n 8) than in the controls (n 2). The majority of deaths resulted from respiratory infection with retention of secretions. The authors speculated that NPPV may have given those patients in the treatment group a false sense of security and perhaps reduced their monitoring of their condition. The study was designed to have patients use NPPV for at least 6 hours per night. Fifteen of the 35 NPPV users, however, used their ventilators for 6 hours per night or not at all. More recently, Ward and coworkers conducted a randomized controlled trial of NPPV in patients with neuromuscular disease who were hypercarbic at night but who had daytime normocapnea. 38 The 12 patients randomized into the experimental cohort were instructed to use their ventilators during sleep and during physiotherapy sessions. A control group of 10 patients received conventional therapies. Another group of 19 patients who had daytime hypercapnia were immediately started on nocturnal NPPV. A priori criteria for instituting ventilatory support were established for the control group. Small differences in nocturnal gas exchange were detected between the experimental and control groups at 6 months, with the NPPV group having a greater decrease in percentage of time with elevated transcutaneously-measured CO 2 from baseline and a statistically greater increase in nocturnal oxygen saturation (measured via pulse oximetry). Importantly, by 12 months, 70% of the control patients met criteria for ventilatory support and so began NPPV, and by 24 months 90% of the control patients were using NPPV. Nightly use of the ventilator among the experimental NPPV group was only hours, and among the control group it was hours. In contrast, those with daytime hypercapnia used their ventilators for hours. These 2 studies highlight both the importance of monitoring adherence to therapy and the need to understand what factors contribute to or detract from acceptance of nocturnal NPPV use in children. Another recent study examined the conditions under which long-term mechanical ventilatory support in children with neuromuscular disease was initiated. Of 73 children, home mechanical ventilation was begun electively in only 21%. 39 The remainder of children were placed on Fig. 2. Standard pediatric nasal interfaces. A: MiniMe nasal mask (SleepNet Corporation, Manchester, New Hampshire). B: Small child s mask (Respironics, Murrysville, Pennsylvania). C: Profile Lite small mask (Respironics, Murrysville, Pennsylvania). D: Small, medium, and large Infant Nasal CPAP (continuous positive airway pressure) Cannulae (Hudson RCI, Temecula, California). home-mechanical-ventilator support nonelectively, usually following failure to wean from support, in association with acute lower-respiratory-tract infection. The authors identified almost 200 missed opportunities to discuss longterm mechanical ventilation and end-of-life issues with these patients during prior hospitalizations, office visits, and after polysomnography. NPPV in Young Children Two important factors in patient adherence with NPPV are patient-ventilator synchrony and the fit and comfort of the interface. Aside from the usual possible complications related to nasal mask ventilation described in adults, including skin irritation or breakdown, sinus and ear pain, eye irritation, gastric distention, and excessive leak leading to inadequate ventilation, 40 certain problems and complications are unique to infants and small children that can undermine adherence with therapy. There is a paucity of nasal interfaces commercially available for infants and toddlers (Fig. 2), and the ability to make custom masks 41 is not as readily available in the United States as it is in Europe. 42 Often, nasal prong systems are adapted for use, but they leak around the prongs, and the resistance across their narrow orifices reduces or eliminates small and weak children s ability to trigger and cycle assisted breaths, so patient-ventilator synchrony is compromised. The resistance across small prongs, coupled with the leak, can also simulate patient effort, causing some bi-level generators to auto-trigger when set in spontaneous/timed mode. For such children, a common practice is to wait for the child to fall asleep and then set the ventilator in a timed or control mode at a rate that overrides the patient s respiratory drive. 35 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 889
6 Fig. 3. Infant wearing a MiniMe nasal mask secured by specifically designed petite headgear (SleepNet Corporation, Manchester, New Hampshire). Fig. 4. A 26-month-old boy with spinal muscular atrophy type I, using standard adult small nasal interface and headgear (SNAPP nasal interface, Tiara Medical Systems, Lakewood, Ohio). Fig. 5. Infant with spinal muscular atrophy type I (left) at time of diagnosis (3 1 2 months of age) and (right) at 18 months of age. She began using bi-level positive airway pressure at 6 months of age, for h/d. Note the flattening of the malar area and erythema from her nasal mask. Even when nasal systems can be created or adapted from setups designed for adults, the headgear used to hold them in place often has to be improvised. 35 Recently, some headgear systems have been adapted for smaller children (Fig. 3), and occasionally toddlers can fit adequately into systems designed for adults (Fig. 4). Often, because of poor-fitting interfaces or inadequate headgear, nasal masks are placed firmly on a child s face, and injury to the underlying skin occurs. The pressure on facial structures from a nasal mask is associated not only with skin injury in children, but also with flattening of facial structures A child s face has achieved only 60% of its adult final growth at 3 4 years of age, and 90% by 12 years of age. 43,44 Forces that are normally responsible for the broadening and outward growth of the face 45 can be counteracted by the inward pressure exerted by a nasal interface. The result is flattening of the face, especially involving the mid-face, 43,44 and malocclusion with retrusion of the maxillary ridge (class III angle malocclusion) (Figs. 5 and 6). 42,44 Recently, mask-related facial injuries were quantified among a group of 40 children using NPPV for obstructive sleep apnea (n 16), neuromuscular disease (n 14), or cystic fibrosis (n 10). 42 For the group, mask ventilation began at 8.8 years (range years), and duration of use was 15 months (range 1 85 months). Importantly, all the children 6 years of age were fitted with custom masks, whereas those older than 6 years were initially given commercially available masks. Older children were given the option of changing to custom masks if the commercial ones were uncomfortable. Global facial flattening was present in 68% of the children, 43% had flattening of the forehead, 38% had flattening of the malar area, and 28% had flattening of the maxilla. Twelve percent were described as having a concave face. Facial flattening was more common among those children with obstructive sleep apnea or neuromuscular 890 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8
7 Fig. 6. This 15-year-old girl with spinal muscular atrophy type II had used nocturnal noninvasive ventilation since the age of years. She developed flattening of the mid-face and a malocclusion that interferes with her ability to chew food. disease (odds ratio 18, 95% confidence interval ), who began using NPPV earlier than the children with cystic fibrosis. Maxillary retrusion was found in 37% and was seen more commonly when the nasal mask was used 10 h/d (odds ratio 6.3, 95% confidence interval ). In this heterogeneous group, facial flattening was not associated with patient age, cumulative use of nasal NPPV, or underlying disease. The same authors also evaluated skin injury related to mask use. Surprisingly, skin injury was much more common in children 10 years of age than in those 10 years old: only 22% of those 10 had skin injury, whereas 82% of those 10 had some degree of skin injury. Notably, however, the use of custom masks was associated with absence of skin injury in 75% of those who used custom masks, whereas some degree of injury was present in 86% of those who used commercially available masks. These data clearly point to the need for a wider variety of nasal interfaces and better availability of custom-made masks for young children. A recent report details how such masks can be made inexpensively from common dental supplies. 41 In addition, young children treated with nasal NPPV should be followed closely by an orthodontist so that necessary mask adjustments can be made or corrective orthotic devices can be employed. 44 Transition to Adult Care Approximately 90% of children born with a disability in the United States will reach age Because of some of the advances in care discussed above, technology-assisted children with neuromuscular disease now routinely live beyond the second decade of life In Pennsylvania s Ventilator Assisted Children s Home Program, for instance, there has been a 360% increase (from 13 to 47) in the number of ventilator-assisted adolescents who reached or were soon to reach adulthood in the years , compared with the period Of that group, 50% require mechanical ventilation for disorders that cause weakness or paralysis. Older adolescents and young adults who began to receive mechanical ventilation in childhood, however, often continue to receive their care in pediatric centers, despite advancing to an age beyond the usual scope of pediatric care. As ventilator-dependent patients with neuromuscular disease age, pediatric care programs may not address issues related to adulthood, and pediatric practitioners may not have the training or resources to address such issues. Some of the challenges for ventilator-assisted young adults with neuromuscular disease include increased reliance on others for activities of daily living, funding for home-care skilled nurses or attendants, coordination of care among multiple subspecialists, and access to transportation, employment, and independent housing. Though various transition models and discussion of obstacles to transition have been described for other specific diseases, no such examples have been published for ventilator-assisted individuals with neuromuscular disease. At a time when achievement of independence and parental separation are paramount, adolescents and young adults with neuromuscular disease typically require more life-sustaining support and assistance with activities of daily living. The requirement for more encompassing personal assistance and the need for parental separation are not necessarily contradictory. Skilled nurses, personal care attendants, or friends can supplant parents in the role of providing basic care needs. The amount of support patients receive through skilled professionals or trained caregivers and assistive technologies relates directly to a better quality of life. 57 How those skilled nurses or trained caregivers are found, and how such services are paid for, however, remain challenges. Presently, home nursing for ventilator-assisted children is funded in part by Medicaid and special waiver programs that exist to support children who require home mechanical ventilation. Similar funding sources are not available for adults who develop chronic respiratory failure and require home ventilation. Furthermore, as patients age and are no longer covered under their parents insurance policies, they suddenly find that home nursing care is no longer a covered benefit. Ventilator-assisted children who grow into adulthood thus find themselves in a double bind: at the same time that concerns arise about aging parents who eventually will not be able to care for the child, the customary support of nonfamily skilled caregivers is threatened by absence of funding. This dilemma can be reversed only by changing the status quo. In addition to lobbying the federal and state governments for long-term funding for nursing or skilled attendant care, 53 alternative ideas, RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 891
8 such as group homes for ventilator-assisted young adults, 58 should be fostered and subsidized. Successful transition of patients from pediatric to adult caregivers has been associated with an orientation toward attaining future goals. 59 Several authors have stressed that older ventilator-dependent patients, including those with progressive neuromuscular weakness, have a positive outlook regarding their quality of life and look to the future with regard to life plans In contrast, Miller et al noted that, in the United States, vocational agencies routinely have minimized the vocational potential of patients with Duchenne muscular dystrophy, because they are perceived to have a poor prognosis. 61 Only continued efforts to educate elected officials and the lay public about the valuable contributions that ventilator-assisted adults can make to their communities will reverse this trend. Summary Children with neuromuscular disease face challenges not only from their underlying medical conditions, but also from limitations in equipment and systems needed to support them. A better understanding of the impact of the developing respiratory system on cough, as well as standards for cough measurement in healthy children and those with neuromuscular disease would allow for earlier detection of children in need of assistance with secretion removal. Devices that mobilize rather than extract secretions are expensive, and their role in the care of infants and children with neuromuscular disease needs to be critically assessed. Pediatric-specific causes for reduced adherence with NPPV must be characterized. A wider variety of commercially available interfaces, and ready access to custom mask fabrication may be important factors in improving adherence and preventing long-term morbidity. Triggering and cycling mechanisms for very weak children and small infants should be developed to improve patientventilator synchrony. Finally, government officials and medical directors of health-care systems must be educated to understand the extraordinary demands of caring for ventilator-assisted children and young adults with neuromuscular disease outside of health-care facilities; the limited options those young adults face regarding access to housing, jobs, education, transportation, and care attendants; and the need to develop rational funding mechanisms and care plans that are humane, helpful, and cost-effective. ACKNOWLEDGMENTS Thanks to Daniel J Weiner MD and Laura J Miske MSN for their critical review of the manuscript. REFERENCES 1. Teague WG. Long-term mechanical ventilation in infants and children. In: Hill NS, editor. Long-term mechanical ventilation. New York: Marcel Dekker; 2001: Simonds AK. Paediatric non-invasive ventilation. In: Simonds AK, editor. Non-invasive respiratory support, 2nd ed. London: Arnold; 2001: Hogg JC, Williams J, Richardson JB, Macklem PT, Thurlbeck WM. Age as a factor in the distribution of lower-airway conductance and in the pathologic anatomy of obstructive lung disease. N Engl J Med 1970;282(23): Croteau JR, Cook CD. Volume-pressure and length-tension measurements in human tracheal and bronchial segments. J Appl Physiol 1961;16: Rosenberg DE, Lyons HA. Collateral ventilation in excised human lungs. Respiration 1979;37(3): Fagan DG. Shape changes in static V-P loops from children s lungs related to growth. Thorax 1977;32(2): Fagan DG. Post-mortem studies of the semistatic volume-pressure characteristics of infants lungs. Thorax 1976;31(5): Zapletal A, Paul T, Samanek M. Pulmonary elasticity in children and adolescents. J Appl Physiol 1976;40(6): Papastamelos C, Panitch HB, England SE, Allen JL. Developmental changes in chest wall compliance in infancy and early childhood. J Appl Physiol 1995;78(1): Papastamelos C, Panitch HB, Allen JL. Chest wall compliance in infants and children with neuromuscular disease. Am J Respir Crit Care Med 1996;154(4 Pt 1): Bach JR, Kang SW. Disorders of ventilation: weakness, stiffness and mobilization. Chest 2000;117(2): Leith DE, Butler JP, Sneddon SL, Brain JD. Cough. In: Macklem PT, Mead J, editors. Section 3: The respiratory system. Bethesda: American Physiological Society; 1986: Chaudri MB, Liu C, Hubbard R, Jefferson D, Kinnear WJ. Relationship between supramaximal flow during cough and mortality in motor neurone disease. Eur Respir J 2002;19(3): Yates K, Festa M, Gillis J, Waters K, North K. Outcome of children with neuromuscular disease admitted to paediatric intensive care. Arch Dis Child 2004;89(2): Chatwin M, Ross E, Hart N, Nickol AH, Polkey MI, Simonds AK. Cough augmentation with mechanical insufflation/exsufflation in patients with neuromuscular weakness. Eur Respir J 2003;21(3): Bach JR, Saporito LR. Criteria for extubation and tracheostomy tube removal for patients with ventilatory failure: a different approach to weaning. Chest 1996;110(6): Mier-Jedrzejowicz A, Brophy C, Green M. Respiratory muscle weakness during upper respiratory tract infections. Am Rev Respir Dis 1988;138(1): Poponick JM, Jacobs I, Supinski G, DiMarco AF. Effect of upper respiratory tract infection in patients with neuromuscular disease. Am J Respir Crit Care Med 1997;156(2 Pt 1): Bach JR, Ishikawa Y, Kim H. Prevention of pulmonary morbidity for patients with Duchenne muscular dystrophy. Chest 1997;112(4): Tzeng AC, Bach JR. Prevention of pulmonary morbidity for patients with neuromuscular disease. Chest 2000;118(5): Airen M, McDonough J, Panitch HB. Cough peak flow measurements in normal school-age children (abstract). Am J Respir Crit Care Med 2004;169:A Szeinberg A, Tabachnik E, Rashed N, McLaughlin FJ, England S, Bryan CA, Levison H. Cough capacity in patients with muscular dystrophy. Chest 1988;94(6): Gauld LM, Boynton A. Relationship between peak cough flow and spirometry in Duchenne muscular dystrophy. Pediatr Pulmonol 2005; 39(5): Bach JR, Smith WH, Michaels J, Saporito L, Alba AS, Dayal R, Pan J. Airway secretion clearance by mechanical exsufflation for post- 892 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8
9 poliomyelitis ventilator-assisted individuals. Arch Phys Med Rehabil 1993;74(2): Miske LJ, Hickey EM, Kolb SM, Weiner DJ, Panitch HB. Use of the mechanical in-exsufflator in pediatric patients with neuromuscular disease and impaired cough. Chest 2004;125(4): Plioplys AV, Lewis S, Kasnicka I. Pulmonary vest therapy in pediatric long-term care. J Am Med Dir Assoc 2002;3(5): Birnkrant DJ, Pope JF, Lewarski J, Stegmaier J, Besunder JB. Persistent pulmonary consolidation treated with intrapulmonary percussive ventilation: a preliminary report. Pediatr Pulmonol 1996;21(4): Toussaint M, De Win H, Steens M, Soudon P. Effect of intrapulmonary percussive ventilation on mucus clearance in Duchenne muscular dystrophy patients: a preliminary report. Respir Care 2003; 48(10): Deakins K, Chatburn RL. A comparison of intrapulmonary percussive ventilation and conventional chest physiotherapy for the treatment of atelectasis in the pediatric patient. Respir Care 2002;47(10): Finder JD, Birnkrant D, Carl J, Farber HJ, Gozal D, Iannaccone ST, et al. Respiratory care of the patient with Duchenne muscular dystrophy: ATS consensus statement. Am J Respir Crit Care Med 2004; 170(4): Rutgers M, Lucassen H, Kesteren RV, Leger P. Respiratory insufficiency and ventilatory support. 39th ENMC International Workshop, Naarden, The Netherlands, January European Consortium on Chronic Respiratory Insufficiency. Neuromuscul Disord 1996;6(6): Katz S, Selvadurai H, Keilty K, Mitchell M, MacLusky I. Outcome of non-invasive positive pressure ventilation in paediatric neuromuscular disease. Arch Dis Child 2004;89(2): Vianello A, Bevilacqua M, Salvador V, Cardaioli C, Vincenti E. Long-term nasal intermittent positive pressure ventilation in advanced Duchenne s muscular dystrophy. Chest 1994;105(2): Simonds AK, Ward S, Heather S, Bush A, Muntoni F. Outcome of paediatric domiciliary mask ventilation in neuromuscular and skeletal disease. Eur Respir J 2000;16(3): Bach JR, Niranjan V, Weaver B. Spinal muscular atrophy type I: a noninvasive respiratory management approach. Chest 2000;117(4): Khan Y, Heckmatt JZ, Dubowitz V. Sleep studies and supportive ventilatory treatment in patients with congenital muscle disorders. Arch Dis Child 1996;74(3): Raphael JC, Chevret S, Chastang C, Bouvet F. Randomized trial of preventative nasal ventilation in Duchenne muscular dystrophy. French Multicentre Cooperative Group on Home Mechanical Ventilation Assistance in Duchenne de Boulogne Muscular Dystrophy. Lancet 1994;343(8913): Ward S, Chatwin M, Heather S, Simonds AK. Randomised controlled trial of non-invasive ventilation (NIV) for nocturnal hypoventilation in neuromuscular and chest wall disease patients with daytime normocapnia. Thorax 2005;60(12): Sritippayawan S, Kun SS, Keens TG, Davidson Ward SL. Initiation of home mechanical ventilation in children with neuromuscular diseases. J Pediatr 2003;142(5): Mehta S, Hill NS. Noninvasive ventilation. Am J Respir Crit Care Med 2001;163(2): Limeres J, Diz P, Vilaboa C, Tomas I, Feijoo JF. Individualized nasal mask fabrication for positive pressure ventilation using dental methods. Int J Prosthodont 2004;17(2): Fauroux B, Lavis JF, Nicot F, Picard A, Boelle PY, Clement A, Vazquez MP. Facial side effects during noninvasive positive pressure ventilation in children. Intensive Care Med 2005;31(7): Li KK, Riley RW, Guilleminault C. An unreported risk in the use of home nasal continuous positive airway pressure and home nasal ventilation in children: mid-face hypoplasia. Chest 2000;117(3): Villa MP, Pagani J, Ambrosio R, Ronchetti R, Bernkopf E. Mid-face hypoplasia after long-term nasal ventilation. Am J Respir Crit Care Med 2002;166(8): Delaire J. Maxillary development revisited: relevance to the orthopaedic treatment of Class III malocclusions. Eur J Orthod 1997; 19(3): Scal P, Evans T, Blozis S, Okinow N, Blum R. Trends in transition from pediatric to adult health care services for young adults with chronic conditions. J Adolesc Health 1999;24(4): Make BJ, Hill NS, Goldberg AI, Bach JR, Criner GJ, Dunne PE, et al. Mechanical ventilation beyond the intensive care unit: report of a consensus conference of the American College of Chest Physicians. Chest 1998;113(5 Suppl):289S 344S. 48. Gozal D. Pulmonary manifestations of neuromuscular disease with special reference to Duchenne muscular dystrophy and spinal muscular atrophy. Pediatr Pulmonol 2000;29(2): Jeppesen J, Green A, Steffensen BF, Rahbek J. The Duchenne muscular dystrophy population in Denmark, : prevalence, incidence and survival in relation to the introduction of ventilator use. Neuromuscul Disord 2003;13(10): Eagle M, Baudouin SV, Chandler C, Giddings DR, Bullock R, Bushby K. Survival in Duchenne muscular dystrophy: improvements in life expectancy since 1967 and the impact of home nocturnal ventilation. Neuromuscul Disord 2002;12(10): Bach J, Alba A, Pilkington LA, Lee M. Long-term rehabilitation in advanced stage of childhood onset, rapidly progressive muscular dystrophy. Arch Phys Med Rehabil 1981;62(7): Gilgoff RL, Gilgoff IS. Long-term follow-up of home mechanical ventilation in young children with spinal cord injury and neuromuscular conditions. J Pediatr 2003;142(5): Downes JJ, Boroughs DS. The transition to adulthood by adolescents with chronic respiratory failure: a growing challenge. Caring 2005; 24(9): Schidlow DV, Fiel SB. Life beyond pediatrics: transition of chronically ill adolescents from pediatric to adult health care systems. Med Clin North Am 1990;74(5): Blum RW, Garell D, Hodgman CH, Jorissen TW, Okinow NA, Orr DP, Slap GB. Transition from child-centered to adult health-care systems for adolescents with chronic conditions: a position paper of the Society for Adolescent Medicine. J Adolesc Health 1993;14(7): Bowes G, Sinnema G, Suris JC, Buhlmann U. Transition health services for youth with disabilities: a global perspective. J Adolesc Health 1995;17(1): Abresch RT, Seyden NK, Wineinger MA. Quality of life. Issues for persons with neuromuscular diseases. Phys Med Rehabil Clin N Am 1998;9(1): Schwerdt M. [Concept of apartment-sharing groups for children and adolescents treated with long-term ventilation]. Med Klin (Munich) 1999;94(1 Spec No): Article in German 59. Reiss J, Gibson R. Health care transition: destinations unknown. Pediatrics 2002;110(6 Pt 2): Gibson B. Long-term ventilation for patients with Duchenne muscular dystrophy : physicians beliefs and practices. Chest 2001;119(3): Miller JR, Colbert AP, Osberg JS. Ventilator dependency: decisionmaking, daily functioning and quality of life for patients with Duchenne muscular dystrophy. Dev Med Child Neurol 1990;32(12): Bach JR, Campagnolo DI, Hoeman S. Life satisfaction of individuals with Duchenne musculardystrophy using long-term mechanical ventilatory support. Am J Phys Med Rehabil 1991;70(3): RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 893
10 Discussion Giordano:* Many pediatric patients on mechanical ventilation are maintained at home. With regard to utilizing noninvasive mechanical ventilation, what level of professionalservices do you think is indispensable to successful management of those patients? Panitch: I ll talk about both invasive and noninvasive ventilation in the same breath. The parents need time to sleep and to go to work, so when it comes to very young children who can t call for help or replace the mask if it becomes displaced, we have to have somebody there, at least to watch for mask displacement or airway obstruction from secretions, so that there can be immediate intervention if necessary. So, at bare minimum, 8 hours, so the parents can work and pay for their health insurance. We typically ask for 16 hours, 18 hours if they have to travel. A lot has to do with how much the child can help out with care, and, luckily, insurance companies recognize that in people under the age of 21 there is a role for skilled care, whether it s nurses or the durablemedical-equipment company or a respiratory therapist who comes in to make assessments. Magically, once you reach adulthood, you re on your own, and it s a huge issue for patients transitioning to adulthood, because they are used to one health-care system. We re lucky in Pennsylvania; we have the Michael Dallas waiver that allows those patients to continue to receive skilled support after the age of 21. The Michael Dallas waiver is a program extension of the Pennsylvania Department of Public Welfare that provides supplemental funding above that provided by Medicaid. Funds can be used * Sam P Giordano MBA RRT FAARC, Executive Director, American Association for Respiratory Care. for nursing care, supplies, and casemanagement services, but office visits and hospitalizations are not covered by the waiver. But in most states, for these patients the financial transition to adulthood is a major problem. Brown: Would you clarify some of the physiology you discussed? I understand that in infants, FRC [functional residual capacity] is determined dynamically. And the airways are more compliant. What is the pleural pressure at FRC in an infant? Panitch: I m not sure, but I think it s about 5 cm H 2 O, which we measure via esophageal catheter. Brown: So, it s the same as in an adult? The transmural pressure of the airway must be the same as in an adult? Panitch: True. Brown: Since the airways are more compliant, they should be bigger in infants than in adults. Panitch: During inspiration. Brown: At FRC, pleural pressure is about 5 cm H 2 O; airway pressure is zero. Panitch: Sure. Brown: But the airways are more compliant and should be pulled open more! But I always Panitch: But elastic recoil is less. Pleural pressure at FRC has actually been measured in healthy infants, and is 1.5 cm H 2 O 1, not 5 cmh 2 O, as was conjectured in the discussion [HBP]. REFERENCE 1. Helms P, Beardsmore CS, Stocks J. Absolute intraesophageal pressure at functional residual capacity in infancy. J Appl Physiol 1981;51(2): Brown: The pressure just outside the airways is the same as pleural pressure, so if the intraluminal pressure is zero and the peribronchial pressure is 5 cm H 2 O, the airway should be pulled open, and they re compliant airways, so they should be larger, not smaller. I ve never been able to understand what I hear my pediatric colleagues say about this. On another subject, all these studies of the Vest [high-frequency chestwall oscillation device] and chest manual therapy and so on need to be controlled for the number of coughs per day. It s cough that clears secretions. Reaching flow limitation and the related dynamic collapse of airways downstream from choke points that s what clears secretions. And all of the studies that I know of have not been properly controlled for the total number of coughs. So you never know whether there s benefit because they re coughing more or because they re using the Vest. King: Just to expand on Sam Giordano s comment, with my 20-plus years in home care, it s unfortunate that I ve never seen a mechanism by the insurance companies to reimburse the respiratory therapist for homeventilator care. There is a nationwide shortage in nursing, particularly nurses experienced in home-ventilator care. There is also a shortage of nurses willing to work the night shift for homeventilator cases. I think it would be helpful if Medicare and Medicaid and the insurance industry would pay for the respiratory therapist to provide some of the care for patients being mechanically ventilated at home. I m not sure why that has never been a viable solution. I wonder how you feel about that as a possibility? Angela King RPFT RRT-NPS, Pulmonetic Systems, Minneapolis, Minnesota. 894 RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8
11 Panitch: I think it s one of a number of creative alternatives, and I think it s a great idea. Hill: Too bad the legislature hasn t acted when this issue comes up, and it s been coming up repeatedly for decades. You commented about problems with adherence to therapy (which used to be called compliance), and you mentioned a couple of studies. In the one by Raphael et al, 1 they didn t describe how they monitored compliance, but presumably they used patient self-reporting, which is notoriously unreliable (tends to overestimate). In the study by Ward et al they used timers to measure patient adherence. 2 Even with the timers the adherence rates were pretty low. In my experience, even in adults, adherence is a major problem, and, as a general rule, if the patient isn t motivated by a desire to alleviate symptoms, you re going to have problems getting them to adhere. Many of them think, This is uncomfortable, it s no fun, and I m not going to put up with the hassle unless I can see some benefit. Of course, there are some patients who don t realize they re symptomatic until they realize how well they feel after succeeding with noninvasive ventilation. And in the pediatric age group the issues are the same. How do you deal with adherence, particularly with very young children, considering that you can t reason with them? As a parent of very young children I know it s very hard to get them to do things they don t want to do. REFERENCES 1. Raphael JC, Chevret S, Chastang C, Bouvet F. Randomised trial of preventive nasal ventilation in Duchenne muscular dystrophy. French Multicentre Cooperative Group on Home Mechanical Ventilation Assistance in Duchenne de Boulogne Muscular Dystrophy. Lancet 1994;343(8913): Ward S, Chatwin M, Heather S, Simonds AK. Randomised controlled trial of noninvasive ventilation (NIV) for nocturnal hypoventilation in neuromuscular and chest wall disease patients with daytime normocapnia. 2005;60(12): Panitch: That s very true, and I guess we put the parent in the middle, and we try either to reason or to explain to them the rationale for what we re doing, and ask them to advocate for us to have their child do something. It s a difficult situation if a child is unwilling. Those little guys can really humble you. RESPIRATORY CARE AUGUST 2006 VOL 51 NO 8 895
SPINAL MUSCULAR ATROPHY (SMA) is an autosomal recessive disorder and the
 SUPPLEMENT ARTICLE Special Considerations in the Respiratory Management of Spinal Muscular Atrophy Mary K. Schroth, MD Department of Pediatrics, University of Wisconsin School of Medicine and Public Health,
SUPPLEMENT ARTICLE Special Considerations in the Respiratory Management of Spinal Muscular Atrophy Mary K. Schroth, MD Department of Pediatrics, University of Wisconsin School of Medicine and Public Health,
Non-Invasive Ventilation Reduces Respiratory Tract Infections in Children With Neuromuscular Disorders
 Pediatric Pulmonology 43:67 71 (2008) Non-Invasive Ventilation Reduces Respiratory Tract Infections in Children With Neuromuscular Disorders C. Dohna-Schwake, MD,* P. Podlewski, MD, T. Voit, MD, and U.
Pediatric Pulmonology 43:67 71 (2008) Non-Invasive Ventilation Reduces Respiratory Tract Infections in Children With Neuromuscular Disorders C. Dohna-Schwake, MD,* P. Podlewski, MD, T. Voit, MD, and U.
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Tests. Pulmonary Functions
 Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Philips Respironics CEU Programs
 Philips Respironics CEU Programs Sleep therapy presentations Interface and Therapy Options Overview Review the selection and fit of three mask categories: minimal contact or pillow masks, nasal masks,
Philips Respironics CEU Programs Sleep therapy presentations Interface and Therapy Options Overview Review the selection and fit of three mask categories: minimal contact or pillow masks, nasal masks,
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
American Thoracic Society Documents
 American Thoracic Society Documents Respiratory Care of the Patient with Duchenne Muscular Dystrophy ATS Consensus Statement This official statement of the American Thoracic Society was approved by the
American Thoracic Society Documents Respiratory Care of the Patient with Duchenne Muscular Dystrophy ATS Consensus Statement This official statement of the American Thoracic Society was approved by the
HLTEN609B Practise in the respiratory nursing environment
 HLTEN609B Practise in the respiratory nursing environment Release: 1 HLTEN609B Practise in the respiratory nursing environment Modification History Not Applicable Unit Descriptor Descriptor This unit addresses
HLTEN609B Practise in the respiratory nursing environment Release: 1 HLTEN609B Practise in the respiratory nursing environment Modification History Not Applicable Unit Descriptor Descriptor This unit addresses
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Non-Invasive Positive Pressure Ventilation in Heart Failure Patients: For Who, Wy & When?
 REUNIÃO CONJUNTA DOS GRUPOS DE ESTUDO DE CUIDADOS INTENSIVOS CARDÍACOS E DE FISIOPATOLOGIA DO ESFORÇO E REABILITAÇÃO CARDÍACA O L H Ã O 2 7 e 2 8 d e J a n e i r o 2 0 1 2 Non-Invasive Positive Pressure
REUNIÃO CONJUNTA DOS GRUPOS DE ESTUDO DE CUIDADOS INTENSIVOS CARDÍACOS E DE FISIOPATOLOGIA DO ESFORÇO E REABILITAÇÃO CARDÍACA O L H Ã O 2 7 e 2 8 d e J a n e i r o 2 0 1 2 Non-Invasive Positive Pressure
Titration protocol reference guide
 Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
06/05/2014. Respiratory Medicine Professor Colin Sullivan
 1 Respiratory Medicine Professor Colin Sullivan 2 3 Modalidade utilizada em 90% dos casos. Thorax 1998 53: 416-18 Lancet 1999 353:2100-05 AJRCCM 2004 169:156-62 AJRCCM 161:857-5-859, 2000 Chest 2005; 128:1304-1309
1 Respiratory Medicine Professor Colin Sullivan 2 3 Modalidade utilizada em 90% dos casos. Thorax 1998 53: 416-18 Lancet 1999 353:2100-05 AJRCCM 2004 169:156-62 AJRCCM 161:857-5-859, 2000 Chest 2005; 128:1304-1309
INTRODUCING RESMED S. Home NIV Solutions. S9 VPAP ST-A with ivaps S9 VPAP ST. Why choose average when you can choose intelligent?
 INTRODUCING RESMED S Home NIV Solutions S9 VPAP ST-A with ivaps S9 VPAP ST Why choose average when you can choose intelligent? Now you can provide intelligent air through ResMed s intelligent Volume-Assured
INTRODUCING RESMED S Home NIV Solutions S9 VPAP ST-A with ivaps S9 VPAP ST Why choose average when you can choose intelligent? Now you can provide intelligent air through ResMed s intelligent Volume-Assured
Respiratory Care. A Life and Breath Career for You!
 Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Care A Life and Breath Career for You! Respiratory Care Makes a Difference At 9:32 am, Lori Moreno brought a newborn baby struggling to breathe back to life What have you accomplished today?
Respiratory Concerns in Children with Down Syndrome
 Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Chapter 17 Medical Policy
 RAD-1 LCD for Respiratory Assist Devices (L11482) Contractor Information Contractor Name Contractor Number 00635 Contractor Type LCD Information LCD Database ID Number L11482 AdminaStar Federal, Inc. DMERC
RAD-1 LCD for Respiratory Assist Devices (L11482) Contractor Information Contractor Name Contractor Number 00635 Contractor Type LCD Information LCD Database ID Number L11482 AdminaStar Federal, Inc. DMERC
Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD)
 Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD) Development of disability in COPD The decline in airway function may initially go unnoticed as people adapt their lives to avoid
Pulmonary Rehabilitation in Chronic Obstructive Pulmonary Disease (COPD) Development of disability in COPD The decline in airway function may initially go unnoticed as people adapt their lives to avoid
MODULE. POSITIVE AIRWAY PRESSURE (PAP) Titrations
 MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
Long Term Acute Care Hospital: Criteria for Admission
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. M issouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Pulmonary Ventilation
 Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
Cardiopulmonary Physical Therapy. Haneul Lee, DSc, PT
 Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
Cardiopulmonary Physical Therapy Haneul Lee, DSc, PT Airway ClearanceTechniques Breathing Exercise SpecialConsiderations for MechanicallyVentilated Exercise Injury Prevention and Equipment provision Patient
For every breath he takes. Trilogy200 ventilator s added sensitivity lets you breathe easier knowing your patients are where they belong home.
 For every breath he takes Trilogy200 ventilator s added sensitivity lets you breathe easier knowing your patients are where they belong home. Sensitive to your patients needs Trilogy200, a portable life-support
For every breath he takes Trilogy200 ventilator s added sensitivity lets you breathe easier knowing your patients are where they belong home. Sensitive to your patients needs Trilogy200, a portable life-support
Alternatives to Endotracheal Intubation for Patients with Neuromuscular Diseases
 Authors: Emilio Servera, MD Jesús Sancho, MD Ma Jesús Zafra, RN Ana Catalá, RN Pedro Vergara, RT Julio Marín, MD Affiliations: From the Rehabilitation and Ventilation Unit, Department of Respiratory Medicine,
Authors: Emilio Servera, MD Jesús Sancho, MD Ma Jesús Zafra, RN Ana Catalá, RN Pedro Vergara, RT Julio Marín, MD Affiliations: From the Rehabilitation and Ventilation Unit, Department of Respiratory Medicine,
Does use of the Cough Assist Machine reduce respiratory morbidity for children with neuromuscular disease?
 RESEARCH REPORT Does use of the Cough Assist Machine reduce respiratory morbidity for children with neuromuscular disease? Rachel Phillips BSc Phys (Hons), PgDip Clin Ed Elizabeth Edwards MB ChB FRACP
RESEARCH REPORT Does use of the Cough Assist Machine reduce respiratory morbidity for children with neuromuscular disease? Rachel Phillips BSc Phys (Hons), PgDip Clin Ed Elizabeth Edwards MB ChB FRACP
Air or oxygen as driving gas for nebulised salbutamol
 Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PROP Acute Care/Rehab Discharge Planning Requirements 1. PROP Medical Criteria 2. PROP Prescription for Services 3
 BC Association for Individualized Technology and Supports for People with Disabilities (BCITS) Proviinciiall Respiiratory Outreach Program ((PROP)) Discharge Planning Guide For ventilator dependent and
BC Association for Individualized Technology and Supports for People with Disabilities (BCITS) Proviinciiall Respiiratory Outreach Program ((PROP)) Discharge Planning Guide For ventilator dependent and
Coding Guidelines for Certain Respiratory Care Services July 2014
 Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
Coding Guidelines for Certain Respiratory Care Services Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line or Coding Listserv.
How To Determine The Number Of Respiratory Therapists
 AARC White Paper November 8, 2012 BEST PRACTICES IN RESPIRATORY CARE PRODUCTIVITY AND STAFFING This paper provides guidance and considerations in the application of the AARC Position Statement: Best Practices
AARC White Paper November 8, 2012 BEST PRACTICES IN RESPIRATORY CARE PRODUCTIVITY AND STAFFING This paper provides guidance and considerations in the application of the AARC Position Statement: Best Practices
Forced vital capacity: maximal volume of air exhaled with maximally forced effort from a maximal inspiration.
 SOP Spirometry 1. General considerations Spirometry serves as a physiological test to quantify pulmonary disease severity and to assess clinical change in respiratory function over time. Standard spirometric
SOP Spirometry 1. General considerations Spirometry serves as a physiological test to quantify pulmonary disease severity and to assess clinical change in respiratory function over time. Standard spirometric
Chapter 26. Assisting With Oxygen Needs. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
BIPAP Synchrony TM AVAPS
 BIPAP Synchrony TM AVAPS Product Presentation V1.6 Contents Home NIV Solution introduction BiPAP Technology and Auto-Trak algorithm Consensus conference, Chest 1999 The AVAPS algorithm The AVAPS settings
BIPAP Synchrony TM AVAPS Product Presentation V1.6 Contents Home NIV Solution introduction BiPAP Technology and Auto-Trak algorithm Consensus conference, Chest 1999 The AVAPS algorithm The AVAPS settings
AT HOME DR. D. K. PILLAI MUG @ UOM
 NON - INVASIVE VENTILATION AT HOME DR. D. K. PILLAI 07.09.2011 MUG @ UOM In the beginning came. OSA (HS) 1. CPAP for OSAHS (Obstructive Sleep Apnoea Hypopnoea Syndrome) 2 NIPPV 2. NIPPV (Non
NON - INVASIVE VENTILATION AT HOME DR. D. K. PILLAI 07.09.2011 MUG @ UOM In the beginning came. OSA (HS) 1. CPAP for OSAHS (Obstructive Sleep Apnoea Hypopnoea Syndrome) 2 NIPPV 2. NIPPV (Non
Improvement in Dyspnea Implementing Pulmonary Rehabilitation in the Home
 Improvement in Dyspnea Implementing Pulmonary Rehabilitation in the Home Mary Cesarz MS, PT Lisa Gorski MS, APRN, BC, FAAN Wheaton Franciscan Home Health & Hospice Milwaukee, WI Objectives To identify
Improvement in Dyspnea Implementing Pulmonary Rehabilitation in the Home Mary Cesarz MS, PT Lisa Gorski MS, APRN, BC, FAAN Wheaton Franciscan Home Health & Hospice Milwaukee, WI Objectives To identify
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
Respiratory Complications of the Muscular Dystrophies
 Respiratory Complications of the Muscular Dystrophies Anita K. Simonds, M.D. 1 ABSTRACT Pulmonary complications including chest infections, atelectasis, pulmonary hypoplasia and ventilatory failure are
Respiratory Complications of the Muscular Dystrophies Anita K. Simonds, M.D. 1 ABSTRACT Pulmonary complications including chest infections, atelectasis, pulmonary hypoplasia and ventilatory failure are
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support
 Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
An Overview of Asthma - Diagnosis and Treatment
 An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
An Overview of Asthma - Diagnosis and Treatment Asthma is a common chronic disorder of the airways that is complex and characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness,
Therapist Multiple-Choice Examination
 Therapist Multiple-Choice Examination Effective: January 2015 Detailed Content Outline Items are linked to open cells. Each scored form will include 20-item pretests. I. PATIENT DATA EVALUATION AND RECOMMENDATIONS
Therapist Multiple-Choice Examination Effective: January 2015 Detailed Content Outline Items are linked to open cells. Each scored form will include 20-item pretests. I. PATIENT DATA EVALUATION AND RECOMMENDATIONS
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
The National Survey of Children s Health 2011-2012 The Child
 The National Survey of Children s 11-12 The Child The National Survey of Children s measures children s health status, their health care, and their activities in and outside of school. Taken together,
The National Survey of Children s 11-12 The Child The National Survey of Children s measures children s health status, their health care, and their activities in and outside of school. Taken together,
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA
 1 ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA There are three documented ways to treat obstructive sleep apnea: 1. CPAP device 2. Oral Appliances 3. Surgical correction of nasal and oral obstructions
1 ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA There are three documented ways to treat obstructive sleep apnea: 1. CPAP device 2. Oral Appliances 3. Surgical correction of nasal and oral obstructions
CPAP titration: PSG technologist or at Home
 CPAP titration: PSG technologist or at Home Carolyn D Ambrosio, MD, MS Associate Professor of Medicine Director, The Center for Sleep Medicine Tufts Medical Center Conflict of Interest No financial interest
CPAP titration: PSG technologist or at Home Carolyn D Ambrosio, MD, MS Associate Professor of Medicine Director, The Center for Sleep Medicine Tufts Medical Center Conflict of Interest No financial interest
Snoring and Obstructive Sleep Apnea (updated 09/06)
 Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
ARTICLE IN PRESS. Neuromuscular Disorders xx (2003) xxx xxx. Workshop report
 Neuromuscular Disorders xx (2003) xxx xxx Workshop report 117th ENMC Workshop: Ventilatory Support in Congenital Neuromuscular Disorders Congenital Myopathies, Congenital Muscular Dystrophies, Congenital
Neuromuscular Disorders xx (2003) xxx xxx Workshop report 117th ENMC Workshop: Ventilatory Support in Congenital Neuromuscular Disorders Congenital Myopathies, Congenital Muscular Dystrophies, Congenital
Nocturnal Oxygenation Using a Pulsed-Dose Oxygen-Conserving Device Compared to Continuous Flow
 Nocturnal Oxygenation Using a Pulsed-Dose Oxygen-Conserving Device Compared to Continuous Robert L Chatburn RRT-NPS FAARC, Joseph S Lewarski RRT FAARC, and Robert W McCoy RRT FAARC BACKGROUND: The pulsed-dose
Nocturnal Oxygenation Using a Pulsed-Dose Oxygen-Conserving Device Compared to Continuous Robert L Chatburn RRT-NPS FAARC, Joseph S Lewarski RRT FAARC, and Robert W McCoy RRT FAARC BACKGROUND: The pulsed-dose
Pulmonary Rehabilitation and Respiratory Therapy Services in the Physician Office Setting* Sam Birnbaum, BBA, CMPE; and Brian Carlin, MD, FCCP
 CHEST Topics in Practice Management Pulmonary Rehabilitation and Respiratory Therapy Services in the Physician Office Setting* Sam Birnbaum, BBA, CMPE; and Brian Carlin, MD, FCCP Pulmonary rehabilitation
CHEST Topics in Practice Management Pulmonary Rehabilitation and Respiratory Therapy Services in the Physician Office Setting* Sam Birnbaum, BBA, CMPE; and Brian Carlin, MD, FCCP Pulmonary rehabilitation
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Breathe With Ease. Asthma Disease Management Program
 Breathe With Ease Asthma Disease Management Program MOLINA Breathe With Ease Pediatric and Adult Asthma Disease Management Program Background According to the National Asthma Education and Prevention Program
Breathe With Ease Asthma Disease Management Program MOLINA Breathe With Ease Pediatric and Adult Asthma Disease Management Program Background According to the National Asthma Education and Prevention Program
Adult Home Oxygen Therapy. Purpose To provide guidance on the requirements for and procedures relating to domiciliary oxygen therapy.
 Contents Purpose... 1 Scope/Audience... 1 Categories for Home Oxygen Therapy... 2 Assessment for Home Oxygen Therapy... 3 Investigations... 3 Requests for home oxygen... 3 Provision of Home Oxygen... 4
Contents Purpose... 1 Scope/Audience... 1 Categories for Home Oxygen Therapy... 2 Assessment for Home Oxygen Therapy... 3 Investigations... 3 Requests for home oxygen... 3 Provision of Home Oxygen... 4
University of Kansas. Respiratory Care Education
 University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
University of Kansas Respiratory Care Education What is Respiratory Care? Respiratory Care is the health profession that specializes in the promotion of optimum cardiopulmonary function and health Respiratory
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Spinal Muscular Atrophy
 Maryam Oskoui, MD, MSc, FRCPC Pediatric Neurologist Spinal Muscular Atrophy Elise Historical Timeline In vitro and animal studies Werdnig and Hoffmann describe SMA 1 (Arch Psych Nervenkrankheiten) Disease
Maryam Oskoui, MD, MSc, FRCPC Pediatric Neurologist Spinal Muscular Atrophy Elise Historical Timeline In vitro and animal studies Werdnig and Hoffmann describe SMA 1 (Arch Psych Nervenkrankheiten) Disease
Titration protocol reference guide
 Titration protocol reference guide Titration protocol reference guide Description Page Patient types 3 Titration protocol goals 4 CPAP CPAP protocol 5-6 auto CPAP auto CPAP protocol 7-8 BiPAP S BiPAP S
Titration protocol reference guide Titration protocol reference guide Description Page Patient types 3 Titration protocol goals 4 CPAP CPAP protocol 5-6 auto CPAP auto CPAP protocol 7-8 BiPAP S BiPAP S
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
Coding & Alan L. Plummer, MD Editor
 Coding & Billing Quarterly march 2014 EDITOR ALAN L. PLUMMER, MD ATS RUC Advisor ADVISORY BOARD MEMBERS: KATINA NICOLACAKIS, MD Chair, ATS Clinical Practice Committee ATS Alternate RUC Advisor STEPHEN
Coding & Billing Quarterly march 2014 EDITOR ALAN L. PLUMMER, MD ATS RUC Advisor ADVISORY BOARD MEMBERS: KATINA NICOLACAKIS, MD Chair, ATS Clinical Practice Committee ATS Alternate RUC Advisor STEPHEN
AVAPS-AE Auto-titration Mode of Noninvasive Ventilation. Monique Hom Sr. Clinical Education Manager HHS
 AVAPS-AE Auto-titration Mode of Noninvasive Ventilation Monique Hom Sr. Clinical Education Manager HHS AVAPS-AE: Why do we need it? 3 AVAPS-AE AVAPS-AE is an Auto-titration Mode of Noninvasive ventilation
AVAPS-AE Auto-titration Mode of Noninvasive Ventilation Monique Hom Sr. Clinical Education Manager HHS AVAPS-AE: Why do we need it? 3 AVAPS-AE AVAPS-AE is an Auto-titration Mode of Noninvasive ventilation
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops
 PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
Using home NIV for the management of hypercapnic COPD
 Home NIV Program for COPD Using home NIV for the management of hypercapnic COPD This program offers COPD treatment guidelines to physicians to help appropriately target and qualify patients for noninvasive
Home NIV Program for COPD Using home NIV for the management of hypercapnic COPD This program offers COPD treatment guidelines to physicians to help appropriately target and qualify patients for noninvasive
Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management
 Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management May 11, 2015 9/25/2013 1 AAMI Foundation Vision: To drive the safe adoption and use of healthcare technology Visit our
Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management May 11, 2015 9/25/2013 1 AAMI Foundation Vision: To drive the safe adoption and use of healthcare technology Visit our
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2
 The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
Pediatric Neuromuscular Disorders: Transitions to Adult Providers
 Pediatric Neuromuscular Disorders: Transitions to Adult Providers 29 th Annual Update in Physical Medicine and Rehabilitation January 29, 2015 Russell Butterfield MD, PhD Assistant Professor, Departments
Pediatric Neuromuscular Disorders: Transitions to Adult Providers 29 th Annual Update in Physical Medicine and Rehabilitation January 29, 2015 Russell Butterfield MD, PhD Assistant Professor, Departments
Arlington Dental Associates Ira Stier DDS PC 876 Dutchess Tpk 2 Lafayette Ct. Poughkeepsie, NY 12603 Fishkill, NY 12524 845-454-7023 845-896-4977
 Home Sleep Test Liability Form Study Equipment Due: @ I, accept responsibility for the sleep monitoring device while it is in rny possession. I understand that if I fail to return the device or I return
Home Sleep Test Liability Form Study Equipment Due: @ I, accept responsibility for the sleep monitoring device while it is in rny possession. I understand that if I fail to return the device or I return
PAGE 1 OF 1 0 REFERENCE CURRENT EFFECT DATE 10/13 ORIGINAL ISSUE DATE 09/12 TITLE: SUBJECT: Patient Care
 PAGE 1 OF 1 0 REFERENCE [ ] All Sharp HealthCare AFFECTED DEPARTMENTS: ACCREDITATION: [ ] System Services Surgery Centers: [ ] SRS [ ] CV-OPS [ ] SCMG [ ] GPSC [ ] SHP [ ] SMH-OPP Hospitals (check all
PAGE 1 OF 1 0 REFERENCE [ ] All Sharp HealthCare AFFECTED DEPARTMENTS: ACCREDITATION: [ ] System Services Surgery Centers: [ ] SRS [ ] CV-OPS [ ] SCMG [ ] GPSC [ ] SHP [ ] SMH-OPP Hospitals (check all
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Pulmonary Function Testing: Coding and Billing Issues
 Pulmonary Function Testing: Coding and Billing Issues Neil R MacIntyre MD FAARC and Catherine M Foss CPFT Introduction Accreditation Developing Coding/Billing Strategies Spirometry Lung Volume Testing
Pulmonary Function Testing: Coding and Billing Issues Neil R MacIntyre MD FAARC and Catherine M Foss CPFT Introduction Accreditation Developing Coding/Billing Strategies Spirometry Lung Volume Testing
Education Goals and Objectives in Physical Medicine and Rehabilitation for the Medical School Graduate
 Education Goals and Objectives in Physical Medicine and Rehabilitation for the Medical School Graduate Medical student education in Physical Medicine and Rehabilitation has been a favored topic for over
Education Goals and Objectives in Physical Medicine and Rehabilitation for the Medical School Graduate Medical student education in Physical Medicine and Rehabilitation has been a favored topic for over
COPD and Asthma Differential Diagnosis
 COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
Provider Type 34 Billing Guide
 Therapy Where to find state policy The Medicaid Services Manual (MSM) Chapter 1700 contains State policy for all therapy services, including respiratory therapy services (not discussed here. See MSM Chapter
Therapy Where to find state policy The Medicaid Services Manual (MSM) Chapter 1700 contains State policy for all therapy services, including respiratory therapy services (not discussed here. See MSM Chapter
PAP Therapy Devices: Delivering the Right Therapy To The Right Patient. Ryan Schmidt, BS,RRT Clinical Specialist Philips Respironics
 PAP Therapy Devices: Delivering the Right Therapy To The Right Patient Ryan Schmidt, BS,RRT Clinical Specialist Philips Respironics Conflict of Interest Disclosure(s) I do not have any potential conflicts
PAP Therapy Devices: Delivering the Right Therapy To The Right Patient Ryan Schmidt, BS,RRT Clinical Specialist Philips Respironics Conflict of Interest Disclosure(s) I do not have any potential conflicts
Critical Care Therapy and Respiratory Care Section
 Category: Section: Title: Critical Care Therapy and Respiratory Care Section Policy #: 03 Revised: 5/02 1.0 DESCRIPTION Clinical Ventilator Management Invasive and Noninvasive Positive Pressure Ventilation
Category: Section: Title: Critical Care Therapy and Respiratory Care Section Policy #: 03 Revised: 5/02 1.0 DESCRIPTION Clinical Ventilator Management Invasive and Noninvasive Positive Pressure Ventilation
CENTER FOR KLINISKE RETNINGSLINJER - CLEARINGHOUSE
 Bilag 2 - Søgematricer Medline Træning amyotrophic lateral upper motor neuron disease Amyotrophic lateral sclerosis [MeSH] physical fitness [MeSH] physical training exercise therapy [MeSH] Rehabilitation
Bilag 2 - Søgematricer Medline Træning amyotrophic lateral upper motor neuron disease Amyotrophic lateral sclerosis [MeSH] physical fitness [MeSH] physical training exercise therapy [MeSH] Rehabilitation
Neuromuscular disorders Development of consensus for diagnosis and standards of care. Thomas Sejersen, Pediatric neurology
 Neuromuscular disorders Development of consensus for diagnosis and standards of care Thomas Sejersen, Pediatric neurology What are neuromuscular disorders? How does the field of neuromuscular disorders
Neuromuscular disorders Development of consensus for diagnosis and standards of care Thomas Sejersen, Pediatric neurology What are neuromuscular disorders? How does the field of neuromuscular disorders
Neurally Adjusted Ventilatory Assist: NAVA for Neonates
 Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
Compliance Issues in Home CPAP Therapy. Joseph Lewarski, BS, RRT, FAARC
 Compliance Issues in Home CPAP Therapy Joseph Lewarski, BS, RRT, FAARC Obstructive Sleep Apnea Syndrome OSA 1 st recognized over 30 years ago 1981 Sullivan publishes small study in Lancet¹ Late 80s, early
Compliance Issues in Home CPAP Therapy Joseph Lewarski, BS, RRT, FAARC Obstructive Sleep Apnea Syndrome OSA 1 st recognized over 30 years ago 1981 Sullivan publishes small study in Lancet¹ Late 80s, early
Guidelines for Medical Necessity Determination for Speech and Language Therapy
 Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
How To Improve Care For Bronchiolitis
 Implementation of an Evidence- Based Care Guideline for Inpatient Bronchiolitis Management J E A N E T T E J O N E S, R N + T H O M A S M A Y E S, M D, M B A * + M A R I S S A M A R T I N E Z, M D + S
Implementation of an Evidence- Based Care Guideline for Inpatient Bronchiolitis Management J E A N E T T E J O N E S, R N + T H O M A S M A Y E S, M D, M B A * + M A R I S S A M A R T I N E Z, M D + S
Diseases and Health Conditions that can Lead to Daytime Sleepiness
 October 21, 2014 Diseases and Health Conditions that can Lead to Daytime Sleepiness Indira Gurubhagavatula, MD, MPH Associate Professor Director, Occupational Sleep Medicine University of Pennsylvania,
October 21, 2014 Diseases and Health Conditions that can Lead to Daytime Sleepiness Indira Gurubhagavatula, MD, MPH Associate Professor Director, Occupational Sleep Medicine University of Pennsylvania,
Key Facts about Influenza (Flu) & Flu Vaccine
 Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Key Facts about Influenza (Flu) & Flu Vaccine mouths or noses of people who are nearby. Less often, a person might also get flu by touching a surface or object that has flu virus on it and then touching
Weaning the Unweanable
 Weaning the Unweanable Gerald W. Staton, Jr, MD Professor of Medicine Pulmonary & Critical Care Medicine Emory University School of Medicine Atlanta, GA gerald.staton@emory.edu Disclosures Pulmonary Program
Weaning the Unweanable Gerald W. Staton, Jr, MD Professor of Medicine Pulmonary & Critical Care Medicine Emory University School of Medicine Atlanta, GA gerald.staton@emory.edu Disclosures Pulmonary Program
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea
 CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
ST. ROSE HOSPITAL Job Description
 ST. ROSE HOSPITAL Job Description JOB TITLE/CLASSIFICATION... REGISTERED RESPIRATORY THERAPIST (RRT) (163) DEPARTMENT... PULMONARY SERVICES STATUS... NON-EXEMPT RELATIONSHIPS Reports to... PULMONARY SUPERVISOR
ST. ROSE HOSPITAL Job Description JOB TITLE/CLASSIFICATION... REGISTERED RESPIRATORY THERAPIST (RRT) (163) DEPARTMENT... PULMONARY SERVICES STATUS... NON-EXEMPT RELATIONSHIPS Reports to... PULMONARY SUPERVISOR
A. Guide to Medicare Coverage
 A. Guide to Medicare Coverage Who qualifies for Medicare benefits? Individuals 65 years of age or older Individuals under 65 with permanent kidney failure (beginning three months after dialysis begins),
A. Guide to Medicare Coverage Who qualifies for Medicare benefits? Individuals 65 years of age or older Individuals under 65 with permanent kidney failure (beginning three months after dialysis begins),
Schedule 3. Services Schedule. Respiratory Therapy
 Respiratory Therapy Services Schedule 20122014 Consolidated Services Version Template Final Version September, 20122014 Schedule 3 Services Schedule Respiratory Therapy Respiratory Therapy Services Schedule
Respiratory Therapy Services Schedule 20122014 Consolidated Services Version Template Final Version September, 20122014 Schedule 3 Services Schedule Respiratory Therapy Respiratory Therapy Services Schedule
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
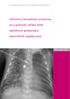 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Respiratory Therapy Program Technical Standards
 Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Respiratory Therapy Program Technical Standards Technical Standards define the observational, communication, cognitive, affective, and physical capabilities deemed essential to complete this program and
Rehabilitation and Lung Cancer Resection. Roberto Benzo MD MS Mindful Breathing Laboratory Division of Pulmonary & CCM Mayo Clinic
 Rehabilitation and Lung Cancer Resection Roberto Benzo MD MS Mindful Breathing Laboratory Division of Pulmonary & CCM Mayo Clinic Disclosure Funded by the National Cancer Institute NIH for Preoperative
Rehabilitation and Lung Cancer Resection Roberto Benzo MD MS Mindful Breathing Laboratory Division of Pulmonary & CCM Mayo Clinic Disclosure Funded by the National Cancer Institute NIH for Preoperative
