Knee Replacement Surgery Patient Information Manual
|
|
|
- Melinda Alberta Spencer
- 10 years ago
- Views:
Transcription
1 Knee Replacement Surgery Patient Information Manual Maximizing Your New Knee(s) UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute
2
3 INTRODUCTION Congratulations! You have chosen a premier orthopaedic team to conduct your knee replacement! The University of Florida Orthopaedic Surgery program first began in 1960 as a division of the Department of Surgery. In 1975 the Division of Orthopaedic Surgery achieved full departmental status. From our beginning in 1960, the University of Florida Orthopaedics and Rehabilitation program has earned a reputation for excellence in research, teaching and clinical care. Our commitment to patient health care motivates every aspect of our efforts, from the bedside, to the classroom, to the research lab. The foundation of our department is built on two outstanding institutions: the University of Florida, a top 20 public university and UF Health Shands Hospital, one of the Southeast s premier health systems. Your doctor has explained your procedure, and what to expect post surgery. The purpose of this guide is to provide you with more information as to what to expect along the road to recovery, and what you can do to prevent any complications and maximize your outcomes. Although the healthcare team will assist you in your recovery, YOU AND YOUR FAMILY are the most important members of the team. We believe knowledge and preparation as to what to expect pre- and post-operatively will make your recovery easier. If you have questions along the way, be sure to ask them. We are here to help you achieve your goals and want you to be satisfied with your entire experience. Our goal is EXCELLENT service, from start to finish. So, let s begin.
4 YOUR NEW KNEE Your doctor has explained how your painful knee will be replaced with an artificial knee joint called a prosthesis. The prosthesis is designed to work in the same way as your natural knee. There are two types of knee arthroplasty. The total knee arthroplasty and the unicompartmental arthroplasty. You need to ask your orthopaedic surgeon the difference between the two and who qualifies for the different types. Your surgeon will carefully choose the best type of prosthesis for you. Some patients will need a total knee arthroplasty or a partial knee replacement while others may have both knees operated on at the same time. The pictures below show the parts of the prosthetic knee. Total Knee Replacement Partial Knee Replacement Femur (thigh bone) Metal Surface Plastic Bearing Metal Surface Screws Tibia (shin bone) Your new knee will function like a door hinge. Like the natural knee, the prosthesis will give you smooth, pain-free movement. A prosthesis will be inserted to replace your deteriorated joint areas. The prosthesis is custom fit to you by your surgeon. You will need to do exercises to strengthen your muscles and give your knee time to heal. In addition, you will be taught exercises that make all of the muscles surrounding your knee stronger and will increase the movement of your knee. You should not attempt to kneel for at least 6 weeks following surgery. The amount of discomfort will be the guide for how much kneeling you can do after that time.
5 ANSWERS TO SOME FREQUENTLY ASKED QUESTIONS ABOUT TOTAL KNEE SURGERY Are there any major risks? Most surgeries go well with no complications. There are two serious complications that are most concerning infection and blood clots. To avoid these, antibiotics are used during and after surgery as well as blood thinners. Special precautions are taken in the operating room to reduce the risk of infection. Will I need blood? You may need to receive a blood transfusion after surgery. The blood bank is very safe, but if you want to use your own blood, please discuss this with your surgeon months before surgery. For more information about blood transfusions, please read the section in this booklet. How long will I be in the hospital? Most knee patients are in the hospital 2-3 days after their surgery. There are several goals that must be met before you go home. What if I live alone? Will I need help at home? Where will I go after I am discharged from the hospital? You can t stay alone after you leave the hospital due to risk of falls while on pain medication, as well as your recent anesthesia and surgery. Most patients are able to go home directly after discharge from the hospital with assistance from family or friends. You may also have a home health nurse and physical therapist assist you at home several times a week, but you still need family or friends to be there to help with meal preparation, bathing and other household activities for several days or weeks depending on your progress. Case management will follow you in the hospital and help you with this decision and make the necessary arrangements. You may go to a rehab facility (inpatient rehab hospital or skilled nursing facility that specializes in rehab). You need to know ahead of time what your insurance will pay for and also you need to meet criteria to be admitted into a facility; not everyone meets the criteria. Please remember if your insurance doesn t pay, you will be responsible for payment for a facility or home care, not the hospital or the physician. The case manager, physician and hospital can t make insurance companies pay for anything that is not in your contract. Will I need equipment before I go home? YES. You will either be using a walker or crutches when you go home. The physical therapist (PT), physician and case manager will help you decide which is safest and how long to use each device. A three-in-one bedside commode might be needed. Whatever equipment is needed for your home, your case manager will make sure it is delivered to your hospital room or your home before discharge. A tub bench and grab bars in the tub or shower may be helpful, but most insurance companies will not pay for them or the installation. Those items would be best purchased and installed before your surgery.
6 ANSWERS TO SOME FREQUENTLY ASKED QUESTIONS ABOUT TOTAL KNEE SURGERY (continued) Will I need physical therapy (PT) when I go home? YES. Home care PT or outpatient PT will have already been discussed with you and arranged for by the case manager while you are in the hospital. In most cases, home care PT is set up for two weeks for three times a week visits. Then, you will likely go to outpatient PT. Outpatient PT is also usually three times a week. The length of time required for therapy varies with each patient. Outpatient PT is desirable if you have transportation to your appointments and insurance benefits for Outpatient Physical therapy, as this encourages you to get up and get moving and gets you out into the community. You can choose the clinic you would like to attend, so be looking for one in your home town that you feel would provide the excellent outpatient care you require for your rehabilitation. When will I be able to drive? The ability to drive depends on whether surgery was on your right or left leg, the type of car you drive. If you had your left knee operated on and have an automatic transmission, you could be driving after three weeks if you are not taking narcotic pain medication. You cannot drive while taking pain medication, it is against the law. If you had your right knee operated on, it could be 5-6 weeks before you can drive. Do you recommend any restrictions following surgery? YES. High impact activities such as running, tennis and basketball are not recommended. Kneeling on your new knee is strongly discouraged. Will I notice anything different about my knee after surgery? YES. Your knee could be swollen for 3-6 months after surgery. You may notice some clicking noise when you walk; this is normal and is the result of the artificial surfaces coming together. You may have some numbness on the outside of your scar which may last for a year or more and is not serious. You may also have soreness in your knee up to 3-6 months after surgery; this will go away.
7 WEIGHT-BEARING PRECAUTIONS Follow your weight-bearing instructions from your surgeon and physical therapist. You will be instructed and educated about how much weight you may place on your operated leg. Weight-bearing as tolerated (WBAT) indicates that you may place as much weight as you are comfortable with on your operated leg. Your physical therapist will also instruct you on proper techniques. Partial weight-bearing (PWB) allows you to place pounds of pressure on your operated leg. Touchdown weight-bearing (TDWB) allows you to place 5-10 pounds of pressure on your operated leg. Non-weight-bearing (NWB) indicates that you may not place any weight at all on your operated leg. During your hospitalization, physical therapy will teach you how to do this properly with specific instructions for you. Please maintain your weight-bearing status as instructed until your surgeon tells you otherwise. SAFETY PRECAUTIONS: WALKER AND CRUTCHES Beware of potential hazards! Remove all throw rugs and plastic runners from walkways in your home. Remove or tape down extension cords. Stay off wet or waxed floors, ice, and grass all of which can be slick and dangerous. Wipe off wet crutch tips or wet walker tips. If you must travel over a slick surface, take short and purposeful steps. Use the elevator when possible; avoid escalators. If you have pets, be careful that you don t trip over them. If you must use the stairs, use stairs with sturdy handrails. If your home has stairs, specifically discuss this with your PT during your hospital stay for problem solving and practice if needed. Walker tips: When getting up from a chair or toilet, do not use the walker for support. Push off of the armrest or seat with your hands. Once standing, place both hands onto the walker handles. Keep your head up and look straight ahead. Stand up straight! When walking, use the wheels on the front of the walker to move you forward. Remember if it has wheels, glide it like a grocery cart.
8 ACTIVITIES AND EXERCISE You will be expected to learn and follow your exercises as you recover. The successful outcome of your surgery will depend on how much you take responsibility for your own care and rehabilitation. The goal is to return to as much independence as possible and perform your own daily activities. Here are some general rules to follow: Let pain be your guide when moving your leg or hip. Use chairs with arms to help you stand up and sit down. Always push up from the surface you are coming from, do not lean and pull on walker. Avoid waterbeds Avoid low, soft sofas and chairs. If necessary, add firmness to low or soft chairs by using pillows or folded blankets. Use your walker or crutches as instructed. DO NOT DRIVE until you are cleared by your surgeon s office. You may ride in a car but try to keep the trips to less than one hour. If longer trips are necessary, you may need to take breaks each hour. Under no circumstances are you to drive while on pain medication. DO complete safe transfers as instructed by physical therapy. DO NOT kneel on your operated knee until your surgeon says it s okay. DO NOT participate in any sports for the first six weeks. CPM NOTE: We currently only occasionally use a CPM machine. Depending on your surgeon s post-op orders, the physical therapist (PT) may apply a continuous passive motion machine (CPM) to your knee while you are in the recovery room or after you get to the floor following your surgery. Your operative leg will be supported in this machine which slowly bends and straightens your knee. The purpose of this machine is to aid in gaining motion of the new knee joint. The CPM helps improve the motion of your new knee in the first couple of days after surgery. The motion will be increased on a daily basis by the PT and he/she will show you how to increase the range of motion (ROM) as approved by your surgeon. The machine is often used for 6-8 hours in a 24 hour period. The machine does not get sent home with you; we want you to move your knee yourself without relying on a machine. Exercises Your physical therapist (PT) will also teach you and your family exercises to strengthen your muscles and increase your knee motion. It is very important that you do these exercises at least twice a day. This will start by the second day after your surgery and will continue for six weeks. A copy of these exercises is provided in this booklet so you can become familiar with them prior to your surgery. If you knee is not too painful, you may begin the exercises before surgery. It will help in your recovery after surgery.
9 ACTIVITIES AND EXERCISE (continued) Control of Swelling Another important factor in your recovery will be controlling any swelling you might have. The better the swelling is controlled, the easier it will be for you to move and strengthen your knee. You should also have less pain. Placing your leg on a pillow under your calf (NOT UNDER YOUR KNEE) helps to keep the swelling down. There are two other ways to help: Apply a cold pack/wrap to your knee for twenty minutes following all exercise and every four hours if you are in a lot of pain. Wrap your leg with an Ace wrap or wear the TED hose you received at the hospital. Use of ice at home: The use of ice after knee surgery has the following purposes: To decrease swelling and the sensation of warmth in your knee To relieve pain, especially following exercise To relieve muscle spasms Tips for applying ice: Apply ice in a warm, comfortable environment. Even though you are only icing your knee, your whole body can feel colder. DO NOT APPLY ICE FOR MORE THAN 20 minutes. Different ways to apply ice: Fill a large sealable freezer bag halfway with ice, and then add water to cover the ice. Close the bag securely to prevent leaking. Wrap the bag in the towel and apply to knee. Use a commercially available gel cold pack. Wrap in a towel and apply to knee. To make your own reusable cold pack, take a sealable freezer bag and fill with one part water and two parts rubbing alcohol. Do not fill bag to its maximum. Place in freezer and wait until it forms a gel-like consistency. Wrap in a towel and apply to knee. To use the commercial cold wraps (if one was sent home with you from the hospital), fill the container with ice and water to the fill line inside the container. Connect the wrap to the unit by snapping the connectors together. Then plug the connector into the unit and then into the wall. Precautions Care must be taken when using ice to avoid freezing the skin. Keep the incision dry by never putting the ice bag/wrap directly against the skin, always use a washcloth or towel first against the skin. Ambulation The physical therapist will teach you to walk properly with a walker or potentially crutches depending on your needs. The assistive device will help you walk and take weight off your operative leg so that your muscles can recover. It is important that you do not plant your leg and then twist or turn your knee joint; this could damage your muscles and the stability of the joint. You will learn to walk on flat surfaces and then steps. Also, your PT will instruct you in the proper method for moving up/down a step and/or stairs.
10 ACTIVITIES AND EXERCISE (continued) Crutch Walking: Posture Keep your head up, with eyes focused about ten feet in front of you and your weight on your hands (NOT on your armpits) Your elbows should press the crutch tops against your ribs. When turning on crutches, keep the crutches in front of you and take small steps. DO NOT turn with your foot on the floor Stairs: The phrase Good goes to heaven, bad goes down will help you remember which leg goes first. Going up Balance on crutches, weight on your hands Push on crutches Start up the step with the non-operative leg ( good goes to heaven ) Step up with the operated leg Once balanced, bring crutches up to step Going down Hold operated leg out in front of you Position toes of the non-operative foot over the edge of the top step Lower crutches down to next step keeping your weight on your hands Step down with operated leg ( bad goes down ) Step down on the heel of your non-operative foot, lowering your body between the crutches and bending the hip and knee of your non-operative leg Come to a firm balance after each move! Avoid quick moves to prevent falling. After Knee Surgery, your physician may request a special dressing be placed on your leg. The Robert Jones Dressing For some physicians, the Jones dressing is used post-operatively for 2 days to apply gentle pressure to the limb to help control swelling and bleeding. If you have this type of wrap on your leg, you will not be doing as much bending of your knee, as the dressing will restrict this. You can work on straightening and lifting your operative leg, and you should be doing isometrics and other exercises that your therapist will show you. The use of a Jones dressing is based on physician preference. Please note that both with and without have very positive outcomes in regards to motion and edema management. Usually the Jones dressing is removed within 48 hrs, and you can perform Range of Motion as able within the dressing until removal.
11 HOSPITAL CARE This section is just a brief summary of what your hospital stay will be like. There are always exceptions! SURGERY DAY You will have remained NPO (no food or water allowed) before surgery. You will be taken to an area called pre-op holding or to the block room. Your family will be shown where the waiting room is, where the doctor will find them after your surgery. In the pre-op area or block room the following may occur: An IV line will be started to replace fluids during the surgery. A Foley catheter will be inserted into your bladder in the operating room after you are asleep. This will remain inserted for approximately 24 hours. Sticky patches, called electrodes, will be placed on your body to monitor your heart rhythm and function. In the operating room: The anesthesiologist will be right there monitoring your vital signs, and will give you medication to make you sleep and forget your surgery. When you are asleep, a breathing tube will be inserted into your throat. This is breathing for you during surgery. The anesthesiologist will be monitoring this and will remove the tube as soon as your lungs wake up and you are breathing on your own. This tube may leave your throat a little sore. DAY OF SURGERY Depending on your surgeon, you may be fitted with a device called a CPM which provides continuous passive motion. Your surgeon determines length of time and range of motion. DAY 1 AFTER SURGERY Your Foley catheter will be taken out. You will be up and moving quite a bit today, so be ready! Moving your knee actively throughout the day is very important if this allowed for you. You will start taking oral pain medication. Make sure you communicate your pain levels and do not wait until the pain has worsened before asking for medication. You will be working with Physical Therapy several times today. But your out-of-bed activity should not stop there. You should be getting up for your meals with nursing and moving to the bathroom with assistance. Sit up as much as possible. You will need assistance whenever you move from the bed, chair, or toilet. The physical therapist will teach you any special precautions and teach you specific exercises for your knee. You are expected to work on seated Knee bending while up. The goal is 90 degrees of bend!
12 HOSPITAL CARE (continued) DAY 2 AFTER SURGERY You will work with PT twice today, and Occupational Therapy as well should you have a need. Most of your IV lines and blocks are gone by today. You can walk with nursing staff as well as family, if you have been cleared to do so... make sure you ask what your mobility goals are for the day! The more you walk and the more time you spend out of bed, the faster your recovery will be. Therapy will be working with you to determine any additional equipment needs you might have, as well as practicing going up and down uneven surfaces such as curbs or steps in preparation for the outside world. You could be discharged home today if you are medically stable and have met your rehab goals. Strive to get home day 2. Work hard and stay active. DAY 3 AFTER SURGERY This day s events are similar to day 2, but you should be up, hopefully dressed in regular clothes, and moving about in your room. This is discharge day for a majority of our knee patients. You may go home directly, to a rehab facility, or a skilled nursing facility. The case manager and the health team will have discussed where a safe and appropriate discharge will be for you to maximize your function and safety. Your follow up care will be established and information will be provided to you at time of discharge. IF YOU ARE GOING DIRECTLY HOME Someone responsible needs to drive you. You cannot drive yourself home! Before you arrive and are admitted to the hospital, please arrange for someone who will drive you home. It is not the hospital s responsibility to get you home. You will receive written discharge instructions from the nurse and possibly the case manager concerning medications, therapy, activity, precautions, etc. Take this information home with you. IF YOU ARE GOING TO A REHAB FACILITY The decision to go to a rehab facility will be made in collaboration with you, the case manager, your surgeon, physical therapist and your insurance company. Every attempt will be made to have this decision finalized prior to your discharge day, but sometimes this gets delayed until the day of discharge. Someone responsible needs to drive you or we can help you arrange for transportation if needed. Transfer papers will be completed by nursing staff and the case manager. A physician from the rehab facility will be caring for you in consultation with your surgeon. Your length of stay is determined by your progress. Upon discharge, home instructions will be given to you by the rehab staff.
13 DISCHARGE INFORMATION KNOW the discharge language... Patients, family caregivers and healthcare providers all play roles in planning for discharge. It is a significant part of the overall care plan that many patients and care givers do not understand. Careful attention to the discharge plan and post hospital care ensures your successful surgery. Many types of post hospital care are not covered under insurance. Here are the basics. Insurance type and medical recommendations both play a role in the type of final discharge plan. Medical staff, Case Managers and Physical Therapists can recommend the appropriate level of care, insurance policies direct care based on coverage and contracts with companies. This can impact your choice of facility and amount of care you are eligible to receive. After joint surgery, patients are discharged to a variety of locations based on their general state of health, how will they recover from surgery, their assistance at home, and their insurance policies. Inpatient Rehab Hospitals are facilities such as UF Health Shands Rehab, or Brooks Rehabilitation in Jacksonville, Florida. To be admitted to these types of facilities, you need a recommendation from physical therapy for intensive therapeutic management of three or more hours per day and have medical needs that require ongoing doctor s supervision. This is most like residing in a hospital. Most orthopedics-planned joint replacements do not discharge to these types of facilities. Medicare, Medicaid and some private insurances cover this type of care. Many private insurances have a very limited benefit for this type of care. Skilled facility, Subacutes, SNF or sometimes skilled nursing facilities or extended care facilities To be admitted to these types of facilities, you need a recommendation from the physical therapist for sub-acute rehab. These facilities have both short-term recovery areas and longterm residential areas where patients receive care. These facilities have physical therapists, occupational therapists, separate therapy gyms to assist with rehabilitation; they also provide nursing care, custodial care, and can accommodate a longer stay for patients. Many orthopedics-planned joint replacements do discharge to these types of facilities. Patients that need additional assistance with walking, more time to recover from surgery, have steps or live in a difficult to reach area, or live alone, often discharge to a sub-acute facility. Is this covered by my insurance? Medicare and private insurances cover this expense; however, most private insurances or Medicare advantage plans require you to go to a facility in their network and a copayment.
14 Home Care DISCHARGE INFORMATION (continued) Home care is a visit by a medical professional including a visit by a nurse to assess, physical therapist or occupational therapist. All planned joint replacements receive some type of homecare to assist with mobility. You will be asked to choose a Home Care agency. Medicare and private insurances cover this expense, there are restrictions on the company that your insurance allows you to choose from, and you will be provided with a list of companies that are available within your network. DME This stands for durable medical equipment and includes walkers, wheelchairs, crutches, bedside commodes, and other items to assist with your mobility and care. Most insurances cover the above items, however, they do not carry specialty items such as shower chairs, slide boards or hand rails. Outpatient Rehab This is therapy that you will receive in an outpatient clinic. Most insurances cover this service, although you may have a limited choice or area that you must choose from.
15 PAIN CONTROL Many patients are concerned about pain after surgery and how well it will be controlled. There are many factors, in addition to the surgery, that affect how much pain you will have. For example, the temperature of the room, how tired you are, and how worried you are. Everyone is different when it comes to pain. Your pain will be controlled to a level that is tolerable for you. Orthopaedic staff are experienced in helping patients in pain to be more comfortable. What kind of pain medications will be used? There are many different ways to take pain medication; pills, intravenously, PCA pump or through a special catheter placed in your back (epidural) or leg (femoral nerve sheath). If you are going to have an epidural or femoral nerve sheath, your doctor and anesthesiologist will explain it to you and will provide you with an information sheet. It is important you tell us any time you feel you are not getting enough pain relief. BE AWARE that we cannot get rid of all your pain; you will have some discomfort. When you switch to pain pills, they will be ordered PRN. PRN means as needed, so you must ask the nurse for pills. The doctor s order for pain medication states a time limit. For example, patient may have pills every three or four hours. It is important for you to plan on taking your pain medications around your physical therapy schedule. Most patients prefer to take the pills about 30 minutes before PT. Although pain medications are necessary, they sometimes cause bothersome side effects. Be alert for any of these side effects and tell your nurse right away. Dry mouth Itching Nausea and/or vomiting Constipation Decreased appetite Urinary retention (trouble urinating) Pain medications can cause severe drowsiness or confusion. Although this is rare, we will be watching for these side effects and your medication will be changed if they are seen. Comfort Measures There are many other ways that you can control pain and feel more comfortable. We will remind you of these when you are in the hospital.
16 PAIN CONTROL (continued) If you have a backache: Raise the head of your bed about halfway Ask us to roll a towel and place it under your lower back Shift your weight or move your legs Use the trapeze on your bed to move around If you feel spasms in your leg: Tighten and release thigh and buttock muscles. Your physical therapist will show you how to do these isometric exercises. You may have ice bags placed over your dressing or a cold wrap incorporated into your total knee dressing. It is important not to get your incision wet, so ask us to help you do this. Don t lie in a wet bed if the ice bag leaks. Please tell your nurse or personal care attendant so your bed can be changed. Let us know how you are feeling! We will help you find a more comfortable position as best we can.
17 ANESTHESIA AND YOU You will see an anesthesiologist and/or an anesthesia nurse practitioner before your surgery. He/she will review your medical history and perform a brief physical exam. The anesthesiologist will discuss with you the options you have for anesthesia during your surgery. Keep in mind your anesthesiologist, based on your history, physical exam, type of surgery and other factors, may suggest one particular anesthetic technique. The most common is General Anesthesia, where you are unconscious during the procedure by a variety of drugs and gases. Spinal Anesthesia is where a small needle is used to inject an anesthetic solution into your back. This medication should take away all pain sensation and movement from the abdomen down to your toes. You also will be sedated so that you are comfortable and relatively unaware of your surroundings (light sleep). Another technique similar to a spinal is Epidural Anesthesia. It also involves using a needle to inject the medication into the lower back. With the epidural, a small catheter is placed through the epidural needle and used to have continuous analgesic medication while in surgery and for a few days after surgery. The anesthesiologist might suggest a combination of the above techniques. Pain relief after surgery can be done in a variety of ways. This is discussed more in depth later in this booklet.
18 MANAGING SURGICAL PAIN WITH NERVE BLOCKS Discuss with your physician what he/she feels is the right choice of analgesia for you! Leg Surgery: Femoral nerve blocks Femoral nerve blocks are used for surgery on the thigh and knee. The block numbs the nerve that transmits signals from much of the front and sides of the thigh and knee. This nerve is relatively close to the skin in the groin area and runs down the leg. A separate block of the sciatic nerve is usually required to fully numb the back of the thigh and lower leg. The sciatic block will be done in much the same way as the femoral nerve block. Here s how the femoral nerve block is typically given: The skin around entry site is cleaned and numbed Anesthesiologist locates the nerve painlessly with nerve stimulator and needle you may feel a slight tingling sensation or muscle twitch He or she then delivers nerve-blocking anesthesia If continuous infusion is planned for long-term pain control, catheter is inserted and connected to a small portable pump Numbness lasts up to 12 hours with a single dose or until continuous infusion catheter is removed Following surgery, you ll need to take special care of your leg until sensation fully returns. When will I be given a nerve block, and how is it done? It s usually done just before surgery in a patient examination room. First, the anesthesiologist numbs the skin with local anesthesia, inserts a stimulating needle, then uses a small hand-held machine called a nerve stimulator. The nerve stimulator sends a low-level electrical signal into your tissue below the skin that helps pinpoint the precise nerve location. The signal will cause a painless muscle twitch, and possibly a tingling sensation. Next, the anesthesiologist gently inserts a very thin catheter (as small as a piece of angel hair pasta) to the nerve location and injects the precise amount of anesthetic needed. Given just before surgery The anesthesiologist locates the nerve painlessly with nerve stimulator He or she then numbs the skin and gently inserts a thin catheter The catheter sends anesthetic directly to nerve Your anesthesiologist can give more details about getting a peripheral nerve block.
19 CARE OF YOUR INCISION During surgery, your incision will be closed with metal clips called staples or a special type of glue depending on your surgeon. You will have a large bulky dressing or your knee will be wrapped from toes to upper thigh with an Ace wrap for two days (the day of surgery and the first day post-op). The bulky dressing will be taken down on the second day post-op and then a lighter gauze dressing will be applied. We will watch for any signs of bleeding or infection and keep your incision dry by changing the dressing as needed. You may have a drain called a Hemovac/Autovac. It will be pulled the first day after your surgery. You may feel a brief burning sensation when the drain is pulled out. You will receive antibiotics through your IV as long as the drain is in to prevent infection. Your dressing should be changed whenever it has drainage on it. The nurse will show your family or caregiver how to change the dressing before you leave the hospital. Hands should be washed before changing the dressing! Avoid touching your incision until it is healed. If home care is set up for you by the case manager, the home care nurse will also reinforce how to change the dressing. If you have staples, they are removed days after surgery and pieces of special tape called Steristrips will be put over your incision. Your staples will be taken out either by a home care nurse or by a nurse at the rehab or skilled nursing facility. You may shower 2 days after the staples come out NOT BEFORE THEN! Pat your incision dry after you shower. The Steristrips may fall off after a few days. If they don t, you can gently peel them off in 5-7 days. Your incision may itch, feel numb or drain a little clear fluid. This is normal. Your incision also may be closed with special surgical super-glue or sutures depending on your surgeon. If closed by glue, you may shower in 72 hours (3 days) but no soaking or scrubbing the incision line. Also, you are not to clean the incision line with anything; there is a possibility of dissolving the glue. Use nothing! If you have sutures, they will either be taken out in the clinic or by a home health nurse. You still can t shower until the day after the sutures are removed. SHOWERING: IF your wound is clean and dry, your physician may allow you to shower at home after discharge. Showering requires physician approval in the immediate post operative period, and he or she will advise you whether you can or cannot shower immediately post-op. MAKE SURE you ask your physician this question before discharge! NEVER SOAK or immerse your incision site until the physician gives authorization. Look at your incision everyday for signs of infection. If you can t see your incision, look in a mirror or have someone else look at it. If you see any signs of infection, call your doctor s office. Signs of infection are: Swelling Increased pain or tenderness Redness and heat Drainage (other than clear reddish yellow) Fever When your incision has no open areas or scabs, you can massage with a water-based lotion (approximately 4 weeks after surgery).
20 PREVENTION OF BLOOD CLOTS Patients who have hip surgery or knee surgery are at risk for developing blood clots in their legs. Blood clots can be dangerous if they break away and travel to your lungs. There are several things you can do to decrease the chances of blood clots forming. When you are lying in bed after surgery and not moving around like you normally would, it is very important that you begin leg exercises (see examples in booklet). These are done by pressing the backs of both knees into the bed, tightening your calf and thigh muscles and moving your ankles up and down. Your physical therapist (PT) will show you how to do these exercises properly. It is important that you get up into the chair and start walking as soon as possible with assistance. You will wear special elastic stockings that help to circulate the blood in your legs. They are white or brown stockings called TED hose. They will be placed on your legs right after surgery in the recovery room and you will need to wear them the entire time that you are in the hospital. We will remove them to wash your legs every day and check to make sure your skin is alright. In order for the stockings to help, it is important they fit properly. They should feel a little tight and smooth without wrinkles or creases. They should not be cut or rolled down. Wear them after you go home until there is no tendency for your legs to swell, usually around 10 days. You will be wearing another special type of machine called a sequential compression device that helps circulate the blood in your legs. These are cloth sleeves attached to a pump. The pump hooks onto the end of your bed and the hoses are attached to the sleeves. Air is pumped into the sleeve through the hoses and then released. There are also medications that help prevent blood clots. Your doctor may order one of these medications for you, especially if you have had blood clots in the past. Coumadin is one drug that may be prescribed. If you are taking Coumadin, it is important that your blood is checked everyday (while in the hospital) until the desired blood lab value is obtained. If your doctor has you continue to take Coumadin after you go home, you will need to have your blood values checked once or twice a week. These tests will be planned for you before your discharge from the hospital. In addition, you will receive dietary instructions from the dietician because some foods may affect your Coumadin level. Aspirin, heparin, Lovenox (enoxaparin) are other drugs that help prevent blood clots. If your doctor orders one of these drugs, we will give you information at that time. Blood clots can be a very serious complication after having knee surgery. It is important that you stick to your prescribed medication in order to decrease your chances of blood clots. It is important to get up and move often. You should not sit longer than one hour at a time. Although blood clots are rare, it is important to know the signs and symptoms to look for: Pain in your lower legs or swelling not relieved by lying down and putting your legs up Heat and redness in the calf muscle area You should notify your doctor immediately if you have any of these symptoms! If you become short of breath or develop chest pain, you need to call 911. It is important that you see a doctor as soon as possible!
21 DIET Good nutrition is essential for proper wound healing. Good nutrition includes eating a balanced diet high in protein and calories. Do not diet while you are healing from your surgery. If you are diabetic, you will be put on a diabetic diet to keep your blood sugar under control. People with diabetes take longer to heal. The more your blood sugar is kept under good control, the better you will heal. If you have allergies to food or are a strict vegetarian, please let the doctor know at pre-op. If you have questions about your diet, please ask your nurse or doctor. At your request, a dietician can speak with you. Depending on your dietary restrictions, your family may bring food into the hospital for you to eat. PREVENTION OF CONSTIPATION Pain medication and anesthesia can be very constipating. The doctors put you on stool softeners and laxatives after surgery but you still may have difficulty. Passing gas is normal and lets us know that your bowel function is starting to come back; don t be embarrassed by this. If you haven t had a bowel movement (pooped) by the second day post-op, please ask your nurse to give you a laxative. If you normally have problems with constipation, let the doctors know what works at home to resolve the issue and hopefully we can do the same for you here in the hospital. BLOOD TRANSFUSIONS Your doctor will talk to you about blood transfusions. Your blood values will be closely monitored after surgery. If they fall too low, your doctor may order a blood transfusion. You may have already donated your own blood at the local blood bank. If needed, this blood will be used for you after surgery. Your own blood (autologous donation) is the safest type of blood transfusion. However, all donated blood is thoroughly tested for many things including hepatitis and HIV. Sometimes it is not safe for you to store your own blood up for surgery. Discuss this with your surgeon. Autotransfusion is another type of blood transfusion. This means that blood, draining from your surgical wound, is collected in a special drain and given back to you through your IV the day of surgery. PREVENTION OF PNEUMONIA Coughing and deep breathing exercises are very important to help prevent pneumonia. Your nurses will ask you take long, deep breaths several times each hour and to cough up any mucous. You will be taught to use a device called an incentive spirometer that will help you with your deep breathing exercises. A nurse will show you how to use this before surgery or right after surgery. Also, getting up in a chair as soon as possible with assistance helps prevent lung problems. If you smoke, quitting before surgery will help your recovery and decrease your chances of getting pneumonia. Smoking is not allowed after surgery while you are in the hospital. PREVENTION OF INFECTION You have a special need to protect yourself from infection after you have surgery. Antibiotics will be needed before you have dental work, surgery or other procedures such as colonoscopy. It is important that you tell your dentist and other health care providers that you have a knee prosthesis.
22 A PATIENT S PERSPECTIVE Surgery will hurt; but it doesn t compare to the 24 hour pain you have been dealing with that led you to have this surgery in the first place. Our health care team is dedicated to helping you recover and maximize your new joint! Your patient experience with us important, so please let us help you make your stay a satisfying one. You will be up and moving right after surgery, perhaps the same day of surgery, so be ready! You will be using an assistive device, such as a walker or crutches initially, so expect that when you are getting up. You need to increase your activity, exercise bouts, and be out of bed more than in it while staying with us. Getting dressed is allowed, so feel free to bring loose fitting clothes that can easily be donned over a bulky knee dressing or immobilizer. EXPECT to go home day 2 or 3 of your stay with us. This is normal. You will have continued therapy outside of the hospital if your insurance offers this benefit. You will need to continue your exercises at home, walking frequently, and staying active. You will have pain medicine to help should you need it. YOU ARE YOUR BEST COACH. STAY ACTIVE. BE FIT!
23 GETTING READY FOR SURGERY What should I expect prior to surgery? When your surgery was scheduled, you received a packet that included this booklet, and a general information sheet about surgery at Shands. You will also be asked to get a clearance letter from your family doctor or internist. This clearance is very important. It is up to you to make sure this is done and that we get the clearance before your pre-op day at the clinic. If you have lab tests, EKGs, or chest x-rays, we need to have those results in the clinic on the day of your pre-op. If you wait and do not get the clearance, your surgery will be cancelled. We want to make sure you are at minimum risk for this elective surgery. If you have a cardiac condition, you must have your cardiac doctor clear you for surgery. Please bring all your medications that you take with you to the pre-op clinic. If you don t bring them, make sure you have a list of all medications that you take both over-the-counter (such as aspirin, Motrin, vitamins, and herbal remedies) and prescribed medications with dosages and how often you take them. The correct medication and dosages are important so we can maintain your health throughout your hospital experience. You will be talking to a nurse case manager either pre-op or post-op who will assist you in obtaining any equipment or services needed after discharge from the hospital. They follow you while you are an inpatient and also as an outpatient. Please be aware that not all insurance pays for inpatient rehab, outpatient rehab, homecare rehab, etc. If you have questions or concerns about where you will be discharged to after leaving the hospital, call the clinic and ask to speak to the case manager for your doctor. If you get the case manager s voice mail, please leave your name, your doctor s name, your phone number and what type of surgery you will be having and when. A case manager will call you back and talk to you about discharge plans. What happens on the pre-op testing day? Prior to your surgery date, you will be scheduled to come to the orthopaedic clinic and the preoperative anesthesia clinic. At this time, a complete history and physical will be done to be sure you are in the best condition for surgery. A chest x-ray and EKG may be done and blood may be drawn. The surgeon and anesthesiologist will explain the surgery and the anesthesia plan to you and your family, answer any questions, and have you sign the operative and anesthesia permits. Be sure to ask all of your questions!
24 WHAT SHOULD I BRING TO THE HOSPITAL? Sturdy slip-on shoes with rubber soles or bedroom slippers with closed toe and heel A copy of your Living Will if you have one Comfortable loose fitting clothing Your personal hygiene items Red ID bracelet received in anesthesia pre-op clinic (if given to you) This booklet Questions to ask before having surgery! List of questions: Bring this sheet with your questions to pre-op so you can remember to ask the doctor, nurse, anesthesiologist what you want to know and address any concerns you may have. Please DO NOT bring valuables (money, watch, jewelry, cell phones) with you. If you wear a wedding ring or band, it will have to be removed before surgery. Please leave your valuables at home; the hospital cannot be responsible for your items.
25 INFORMATION SHEET Welcome to UF Health! You are scheduled to have an elective knee replacement in the near future, and the Rehabilitation Department wanted to give you some information on what to expect day by day in regards to your post-operative care. Nursing and Rehab follow a specific care plan established by your physician for elective joint patients. This guideline standardizes how we offer care to our elective joint patients and allows all stakeholders to know what to expect each day in regards to your care progression. Day 0, or day of surgery Mobility Goals: Edge of bed sitting or out of bed as able Walking as able with assistive device Begin circulation exercises Ankle pumps Quad sets Gluteal sets You will be up and moving if your physician orders it as early as today. Nursing or Therapy can help with this. You will be instructed on any specific precautions you have following this surgery. You can begin circulation exercises as soon as you are alert to do so. You will not have your knee propped on a pillow, it will lay flat on the bed. This keeps your knee in the best alignment. You should see signs in your room that give information on your mobility status, and call don t fall - which means, ask for help and don t get up alone! You likely have a trapeze bar on your bed, you can use this to off load pressure on your bottom, but don t rely on it for mobility - you won t have a bar at home so we practice out of bed without it! You may have ice or a cooling unit for your knee. You will have a catheter for a short time after surgery, but it will be removed first thing in the morning so you can start walking to the bathroom.
26 INFORMATION SHEET (continued) Day 0, or day of surgery (continued) Day 1 after surgery Mobility Goals: Ambulate at least 20 feet with assistive device Sitting up in chair for meals Ambulate to bathroom as able for toileting with assist Bend your knee in sitting at least 60 degrees Active motion or active assisted motion ideal Day 2 after surgery Mobility Goals: Walking increased distances, out of bed for all meals, step training You will have a knee immobilizer on your knee if you have a nerve block. Once the block is gone the immobilizer is not used. You will have a device on your calves that will that will help maintain adequate circulation to the legs. Catheter should be removed. If you have an epidural, you may still have the catheter a little longer. You will be out of bed with therapy and multiple times today. You will be sitting up in the chair for all your meals. You are expected to walk 20 feet with your walker or crutches. You will have help for out-of-bed activity. You will start working on exercises designed to strengthen your new knee. Do these both in and outside of your therapy sessions. You should be bending your knee at least 60 degrees today, and working hard to get your knee as straight as possible when you extend it. Exercises should be done at least twice daily, 1 time with your therapist and another with your family member or on your own. Discharge today is possible. Motion of the knee should approach 80 degrees of flexion. Extension should be close to full. Walking in the hallway for 50 plus feet with a walker or crutches.
27 INFORMATION SHEET (continued) Day 2 after surgery (continued) You will practice going up and down uneven surfaces (steps). Exercises at least twice today. Day 3 after surgery Mobility Goals: Ambulation in hallway and bathroom Get dressed Stay out of bed Discharge note Discharge today is likely. Knee motion should be approaching or at 90 degrees of flexion. Walking in the hallway should exceed 100 feet with an assistive device. Exercises should be done independent of therapy and family member assisting if present. Master uneven surfaces. Out of bed should be independent of trapeze. Getting dressed if able. You will likely have some form of followup therapy. You should perform your home exercise program at least twice a day on your own or with family assistance. You should be trying to bend and straighten your knee as much as possible. You should not be wearing the immobilizer at home unless instructed to do so. You should be walking often. Monitor for clinical signs of infection: fever, swelling, increased pain, redness, etc. (call MD) Thank you for choosing UF Health for your elective surgery. We appreciate your business, and wish you years of comfortable mobility!
28 BILATERAL KNEE SURGERY Simultaneous Bilateral Total Knee Replacement: If you have both knees equally painful and stiff, it is possible to have both knees replaced with total knee prostheses during one operative procedure, under one anesthesia. The operations are followed by a single rehabilitation period within one hospital stay. Such simultaneous surgeries are called Simultaneous Bilateral Total Knee Replacement. Why do the surgeries together? You will have only one surgical event, single anesthesia, shorter hospital stay. Risks of performing a bilateral procedure There can be complications to any procedure. A bilateral knee operation can increase your need for blood transfusion, has a higher rate of post-operative complication the single knee surgery, and will likely require an inpatient rehab stay versus going home directly. If you are overweight, get short of breath easily, and are not physically fit prior to a bilateral knee, you may have difficulty with your post-operative recovery. Discuss the pros and cons with your physician before choosing a Bilateral TKA. What can I expect? Be ready to work hard. We usually place knee immobilizers on both legs for support and stability on the first day post-op. If you have a nerve block, you will have immobilizers on regardless until the block is discontinued. You will Typical knee need help getting up with two knee braces on, as functionally we need to immobilizer have our knees bent to shift our weight forward for leverage. No worries. You can still walk or get up to a chair with knee braces on. Rehab will likely ask you to lead with your weaker, or more painful limb, to initiate mobility. The immobilizers, or at least one, are usually removed once the block is gone. As mentioned above, your anesthesiologist will place femoral nerve catheters into both legs. A pain relieving drug will be pumped into each catheter by a special pump that regulates the amount of drug you receive. These catheters will stay in place until several days after your surgery and the dosing will be determined by the anesthesia pain management team. Your pain will not be totally relieved by the femoral nerve blocks but they will they will make your pain much more controllable with oral or intravenous (IV) medications. Since pain medications are given as needed it is up to the patient to request pain medications when needed and in anticipation of therapy. Nerve Blocks: A side effect of the femoral nerve pain block is the temporary loss of quadriceps muscle control. The quadriceps muscle is the muscle that allows you to extend your knees and stand. After surgery you will be fitted with knee braces to enable you to stand with your walker for the first few post-op days. It is very important for your safety that you not try to walk or stand without these braces or without the help of therapy or nursing staff until the femoral nerve block is removed.
29 BILATERAL KNEE SURGERY? (continued) Local anesthesia (bupivacaine) injected onto femoral nerve Femoral Nerve Block Signal transmission through femoral nerve dampened Single injection or continuous catheter may be used Single injection lasts hours Physical therapy will be ordered twice a day after surgery in order to begin your return to normal movement. But your therapy is not just happening during these sessions. Your nurses are trained to assist you out of bed, and your family can help you with the exercises included in this packet. Rehab after surgery is hard work; patients are expected to participate in exercises and training designed to speed recovery and limit complications. If your physician chooses CPMs for your rehab, you will be required equal wear time on both knees. That may mean on/off cycles, or alternating flexion (while one knee is bending, the other is straightening) simultaneous wear (your therapist will work with you on this). If your knee is having difficulty extending all the way, you may have a pillow placed under your ankle (NEVER UNDER THE KNEE) to allow gravity to passively stretch the area. We do not allow pillows under the knee for comfort as this can cause your knee to get stiff with a slight bend in it. Acute goals for bilateral total knee replacement are: 1. Early mobilization with out of bed activities designed to overcome the effects of anesthesia and improve circulation. It is expected that every patient will spend some time out of bed in a chair on post-op day Training in the use of an assistive device for transfers, walking and steps. 3. Training the patient and caregiver in range of motion and strengthening exercises that will speed your recovery. A day by day summary of what to expect is included in this packet.
30 GENERAL THERAPY TIPS REHAB BECOME A REHAB STAR! Remember to get up and MOVE! Your post-surgical pain is temporary. You have been dealing with joint pain for a long time, so you know that you can get through the post-operative period. Your new knee is waiting for you! You can do it! Ask for help to get up as often as you can Exercise outside of therapy to maximize outcomes Do not place a pillow under your knee. Always promote a straight leg by putting the support under the calf. Strive to achieve your daily goals. Be safe, get help, and prevent falls Get your family involved
31 TOTAL KNEE ARTHROPLASTY HOME EXERCISE PROGRAM Do the following exercises 2-3 times a day. Do 10 or more repetitions of each. 1. ANKLE PUMPS: Make up and down motions with your feet, or point and flex your foot. 2. QUAD SETS: Keep your legs out straight and toes pointed up. Tighten the muscles in the front of your thigh and press your knee down. Hold for a count of 5, then relax. 3. GLUT SETS: Tighten your buttocks by squeezing together, hold for a count of 5, then relax. 4. BRIDGING: Place a roll under your knees. Press down on the roll with your thigh and lift your buttocks. Lower slowly. 5. TERMINAL KNEE EXTENSION: With the roll under your knees, lift your foot until your leg is straight; hold and lower slowly. 6. HEEL SLIDES: Bend hip and knees, bringing heel towards buttocks, then push out until leg is straight. Remember not to bend the hip past 70 degrees.
32 TOTAL KNEE ARTHROPLASTY HOME EXERCISE PROGRAM(continued) Do the following exercises 2-3 times a day. Do 10 or more repetitions of each. 7. ABDUCTION: With leg out straight, slide the leg out away from your body, then pull leg back in. 8. STRAIGHT LEG RAISES: Bend the opposite knee. Do a quad set, then lift leg 12 without letting your knee bend, then lower slowly. 9. Sit in a chair with your foot propped in another chair and knee unsupported for 15 minutes to maintain knee extension. 10. KNEE EXTENSIONS (Very important! Work hard at seated flexion): While sitting in a chair, bend involved leg back as far as you can; use unaffected leg to assist for more knee flexion, then kick out straight. For more flexion, scoot bottom edge of chair with foot planted. 11. After exercises, ice knee for 15 minutes, observing incisional precautions. 12. Ambulate with your observing a weight-bearing of.
33 ON THE MOVE! How many times have you gotten up today? FACT: Staying in bed does not get you home more quickly, and it DOES NOT make you stronger! FACT: Prolonged bed rest can cause: Increased risk of bed sores, blood clots, and pulmonary embolism Pneumonia Exercise intolerance, weakness, and changes in blood pressure Decreased bone density, decreased muscle mass Constipation Depression, a sense of helplessness SO, WHAT CAN I DO TO HELP MYSELF OR MY LOVED ONE? Get out of bed for meals Walk with or without assistance as directed by your physician / nurse / therapist Have slippers with good grips and backs on them for out of bed mobility and activities Make sure you have your glasses and hearing aids Avoid daytime sleeping so a normal sleep cycle is maintained Keep blinds open during the day Encourage use of incentive spirometer for deep breathing... what s this? Ask your nurse! Do any exercises assigned to you outside of your therapy sessions. GET MOVING!
34 FOUR THINGS YOU CAN DO TO PREVENT FALLS Begin a regular exercise program Exercise is one of the most important ways to lower your chances of falling. It makes you stronger and helps you feel better. Exercises that improve balance and coordination (like Tai Chi) are the most helpful. Lack of exercise leads to weakness and increases your chances of falling. Ask your doctor or health care provider about the best type of exercise program for you. Have your health care provider review your medications Have your doctor or pharmacist review all of the medications you take, even over-the-counter medications. As you get older, the way medicines work in your body can change. Some medications, or combinations of medications, can make you sleepy or dizzy and can cause you to fall. Have your vision checked Have your eyes checked by an eye doctor at least once a year. You may be wearing the wrong glasses and need your prescription updated or have a condition such as glaucoma or cataracts that limits your vision. Poor vision can increase your chances of falling. Make your home safer About half of all falls happen at home. To make your home safer: Remove things you trip over (like papers, books, clothes, and shoes) from stairs and places where you walk. Remove small throw rugs or use double-sided tape to keep the rugs from slipping. Keep items you use often in cabinets you can reach easily without using a step stool. Have grab bars put in next to your toilet and in the tub or shower. Use non-slip mats in the bathtub and on shower floors. Improve the lighting in your home. As you get older, you need brighter lights to see well. Hang light-weight curtains or shades to reduce glare. Have handrails and lights put in on all staircases. Wear shoes both inside and outside the house. Avoid going barefoot or wearing slippers.
35 Ask your nurse or therapist to help you up as much as possible PUBLIC PROGRESS REPORT Record your progress and track your accomplishments You can track your progress each day in the hospital with this SAT UP IN CHAIR GOT UP TO THE COMMODE WALKED 30 FEET WITH ASSISTANCE WALKED GREATER THAN 30 FEET DID MY EXERCISES Breakfast Breakfast Breakfast Breakfast Breakfast DAY 1 Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Extras? (time) Extras? (time) Extras? (time) Extras? (time) Extras? (time) Breakfast Breakfast Breakfast Breakfast Breakfast DAY 2 Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Extras? (time) Extras? (time) Extras? (time) Extras? (time) Extras? (time) Breakfast Breakfast Breakfast Breakfast Breakfast DAY 3 Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Extras? (time) Extras? (time) Extras? (time) Extras? (time) Extras? (time) Breakfast Breakfast Breakfast Breakfast Breakfast DAY 4 Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Lunch Dinner Extras? (time) Extras? (time) Extras? (time) Extras? (time) Extras? (time)
36 NOTES /QUESTIONS
37 NOTES /QUESTIONS
38 NOTES /QUESTIONS
39
40 Rev. 12/4/13 PS99228
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Endovascular Abdominal Aortic Aneurysm Repair Surgery
 Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Hip Replacement Discharge Instructions
 Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Knee Replacement Discharge Instructions
 Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Shoulder Replacement Surgery Patient Information Manual
 Shoulder Replacement Surgery Patient Information Manual Maximizing Your New Shoulder UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute www.rehabcenters.ufhealth.org
Shoulder Replacement Surgery Patient Information Manual Maximizing Your New Shoulder UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute www.rehabcenters.ufhealth.org
AFTER TOTAL KNEE REPLACEMENT. Living with Your New Knee
 AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM
 ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
Lumbar Spine Surgery What to Expect
 Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program
 Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery
 Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Low Back Surgery. Remember to bring this handout to the hospital with you.
 Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you.
 Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Dr. Anseth s Frequently Asked Questions about Hip Replacement
 Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Total Knee Replacement
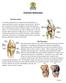 Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
You and your doctor will talk about your condition and the treatment that is best for you.
 PATIENT EDUCATION patienteducation.osumc.edu It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your surgery. If
PATIENT EDUCATION patienteducation.osumc.edu It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your surgery. If
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Knee / Hip Replacement Orientation Class
 THIS IS YOUR GUIDE FOR YOUR HIP OR KNEE REPLACEMENT PATIENT NAME DATE OF SURGERY Physicians Location Phone Christian H. Bean, MD Green Mountain Orthopaedic Surgery (802) 229-2663 Mahlon A. Bradley, MD
THIS IS YOUR GUIDE FOR YOUR HIP OR KNEE REPLACEMENT PATIENT NAME DATE OF SURGERY Physicians Location Phone Christian H. Bean, MD Green Mountain Orthopaedic Surgery (802) 229-2663 Mahlon A. Bradley, MD
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Lumbar or Thoracic Fusion +/- Decompression
 Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Laser of the Vulva. This is a surgery where your doctor will use a laser light to remove unhealthy tissue.
 What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
My Spinal Surgery: Going Home
 My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
PERIACETABULAR OSTEOTOMY SURGERY
 1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
TOTAL KNEE REPLACEMENT
 PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION
 www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
AFTER TOTAL HIP REPLACEMENT. Living with Your New Hip
 AFTER TOTAL HIP REPLACEMENT Living with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step is rehabilitation
AFTER TOTAL HIP REPLACEMENT Living with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step is rehabilitation
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Preoperative Education: LUMBAR SPINE SURGERY
 Preoperative Education: LUMBAR SPINE SURGERY 1 Dear Patient, In order to make your hospital stay as comfortable as possible, we have prepared this informational packet for you designed to outline and explain
Preoperative Education: LUMBAR SPINE SURGERY 1 Dear Patient, In order to make your hospital stay as comfortable as possible, we have prepared this informational packet for you designed to outline and explain
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Total Hip or Knee Joint Replacement
 Preparing for your Total Hip or Knee Joint Replacement Pre-operative education for patients St. Clair Hospital Center for Orthopedics Copyright 2011 by St. Clair Hospital The Orthopedic Team Physicians
Preparing for your Total Hip or Knee Joint Replacement Pre-operative education for patients St. Clair Hospital Center for Orthopedics Copyright 2011 by St. Clair Hospital The Orthopedic Team Physicians
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
TOTAL HIP REPLACEMENT
 PENN ORTHOPAEDICS TOTAL HIP REPLACEMENT Home Exercise Program Maintain Your 3 HIP PRECAUTIONS! The purpose of your hip precautions is to allow for the best healing and the most successful outcomes from
PENN ORTHOPAEDICS TOTAL HIP REPLACEMENT Home Exercise Program Maintain Your 3 HIP PRECAUTIONS! The purpose of your hip precautions is to allow for the best healing and the most successful outcomes from
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Going home after an AV Fistula or AV Graft
 Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
