Dry Eye After LASIK. Clinical. Factors adversely affecting the ocular surface and tear film before LASIK
|
|
|
- Hillary Lewis
- 8 years ago
- Views:
Transcription
1 Clinical Dry Eye After LASIK Dr. Sivakami, MS Resident, Aravind Eye Hospital, Madurai LASIK has now become the standard of care in cornea - based refractive surgery. An increasing number of patients are undergoing this procedure. This has led to an increasing interest in our attempts to understand the post LASIK changes in the ocular surface health. There has been much interest in dry eye symptoms affecting patients who have undergone LASIK. Dry eye is considered as the most common complication of LASIK. Ocular surface and tear film before LASIK Complications during LASIK and even after LASIK can be influenced by the state of the ocular surface and tear film before surgery. Implications of pre-existing dry eye symptoms and ocular surface and tear film disorders on LASIK outcomes Dry eye and associated contact lens intolerance motivate individuals to consider refractive surgery. Pre-existing ocular surface and tear film disorders can have a negative impact on the outcome of keratorefractive surgery in a number of ways. Dry eye symptoms and signs before LASIK are a significant risk factor for experiencing dry eye after LASIK. Poor tear secretion before surgery (Schirmer test value less than 10mm) is a significant risk factor for experiencing dry eye symptoms after surgery. In addition, patients diagnosed with dry eye before surgery have, prolonged recovery of corneal sensation, and more severe and sustained dry eye symptoms after surgery compared to those without dry eye before LASIK. Ocular surface and tear film disorders before surgery may adversely affect LASIK refractive outcome. Disorders of the ocular surface and tear film before LASIK have been implicated in increasing the risk of complications during and after LASIK, including epithelial defects and epithelial in growth, flap folds, wrinkles and displacement, diffuse lamellar keratitis, and infectious keratitis. Factors adversely affecting the ocular surface and tear film before LASIK Contact lens wear Contact lens wear before LASIK can reduce the predictability of refractive surgical outcome by inducing corneal warpage, and altering tear proteins, ocular surface morphology, corneal physiology, barrier function, pachymetry and sensation. These factors may increase the potential for complications during and after refractive surgery. In LASIK studies, tear secretion and corneal sensitivity before and 6 months after LASIK were significantly more depressed in long-term contact lens wearers, compared to non-contact lens wearers. A history of contact lens intolerance can serve as a red flag for the potential exacerbation of dry eye problems after LASIK. Eyelid disease Anterior blepharitis and Meibomian gland dysfunction must be managed before LASIK to minimize the risk of complications after surgery. Staphylococcus aureus has been isolated in appreciable frequency from patients with anterior blepharitis and was reported to be the most prevalent causative microorganism for microbial keratitis after LASIK. Ocular allergy Ocular allergy has the potential to impact on surgical outcomes due to increased incidence of toxicity reactions to medications and their preservatives. Increased mucous in the tear film may lodge in the microkeratome gears and cause incomplete flaps.
2 2 AECS Illumination Also, there is potential for inflammation after surgery due to increased levels of cytokines and chemical mediators released from the inflamed conjunctival and subconjunctival tissues. Herpetic keratitis Patients with a history of actual or suspected herpetic keratitis are advised not to have elective refractive surgery. Epithelial basement membrane dystrophy Patients with epithelial basement membrane disorders before surgery have an increased risk of incurring epithelial defects during and after LASIK. LASIK should not be performed in eyes with this condition due to the increased risk of epithelial in growth and loss of best spectacle - corrected visual acuity. Lid-related anomalies Several disorders of lid aperture, lid/globe congruity, and blinking can pose a problem for the LASIK surgeon and must be recognized and managed before LASIK can be considered. Conjunctivochalasis, large fleshy pterygia, exophthalmos, lagophthalmos, and incomplete blinking should be managed prior to LASIK. Age, gender and medical conditions Old age is one of the risk factors for epithelial defects during surgery. This has been attributed to both decreased epithelial adhesion and increased friction from drier eyes in the older patients. In terms of gender, there is some evidence to suggest that females may have inferior outcomes after LASIK compared to males. Although further research is required, clinical experience suggests that the hormonal changes (particularly the reduction in androgen levels) experienced by older females contribute to the dry eye symptoms, abnormal healing, and less than optimal LASIK results observed in this demographic group. In terms of medical conditions, patients with Diabetes require particular attention. Diabetes has been associated with reductions in tear quality, tear volume, ocular surface epithelial health, goblet cell density, and corneal sensation. Ocular surface and tear film during LASIK Use of topical anaesthetics Excessive and / or repeated dosing of anaesthetic can be toxic to the corneal epithelium and stromal keratocytes. Overuse of topical anaesthetic can result in epithelial toxicity, epithelial defects, diffuse lamellar keratitis, and epithelial in growth. Topical anaesthetic should be used just before surgery to minimize epithelial damage during surgery. Flap reference marking Gentian violet dye used for flap reference marking is toxic to the corneal epithelium and stroma and it has been implicated in causing diffuse lamellar keratitis. Signs of LASIK-induced dry eye Myopic LASIK can cause punctate epitheliopathy, elevated tear osmolarity, decrease in tear secretion, tear volume, tear clearance, tear film stability, goblet cell density, and blink rate. Mechanisms of LASIK-induced dry eye Surgical trauma to the ocular surface All ocular surgical procedures disrupt the ocular surface and tear film. Trauma to the ocular surface that occurs during LASIK has been proposed as a cause of tear film instability, punctate epitheliopathy, and recurrent corneal erosions after LASIK. Trauma from the suction ring could be a contributing factor to the loss of perilimbal conjunctival goblet cells after LASIK. The shearing forces of the traversing microkeratome and excessive drying and wiping of the ocular surface during surgery could damage the microvilli of the superficial epithelium. Ocular surface sensory denervation LASIK disrupts the normal organization of corneal innervation and induces a corneal anaesthesia or hypoaesthesia, lasting up to 6 months. However, in patients with dry eye before LASIK, patients who have worn contact lenses long-term before surgery, or patients who have superior hinged flaps or deeper
3 Vol. XII, No.2, April - June ablations, the return of corneal sensation to levels observed before surgery appears to take longer than 6 months and is associated with more persistent dry eye signs and symptoms. Another study reports that corneal sensation after LASIK recovers within 6 months and that nasally hinged flaps were associated with a significantly greater decrease in corneal sensation than superior hinged flaps. Investigative studies have suggested that this loss of sensory denervation is one of the leading causes of tear film anomalies and punctate epitheliopathy after LASIK. Reduced corneal and conjunctival sensitivity results in reduced tear secretion, tear clearance, goblet cell density, and blink frequency, as well as increased tear osmolarity and ocular surface staining. All of these anomalies are features of the eye after LASIK and support neurotrophic mechanisms as a main cause for dry eye after LASIK. As sensory denervation can mask symptoms of ocular surface irritation, patients who have LASIKinduced tear film and ocular surface problems may only become aware of symptoms as the damaged nerves regenerate. This temporal feature of sensory denervation makes it difficult to correlate symptoms and signs after LASIK. Inflammation The inflammatory changes observed after LASIK may contribute to chronic dry eye symptoms and signs after LASIK. Reduction in tear secretion and tear clearance in eyes after LASIK have been proposed to cause an increase in the concentration of pro-inflammatory cytokines and matrix degrading enzymes in the tear film. This could stimulate up regulation of other inflammatory mediators, leading to further inflammation and damage to the ocular surface. Increased cytokine levels in the tear film may exacerbate the LASIK induced corneal nerve damage, thus further decreasing corneal sensation and further impairing lacrimal gland function. These theories are yet to be verified in experimental studies. Alterations to surface topography and corneal curvature A number of studies have linked changes in corneal profile after LASIK to symptoms and signs of dry eye. Irregularities within the interface, together with the gutter of the flap and the irregular shape of the cornea after LASIK, have the potential to alter the normal relationship between the lids and the corneal surface and hence, change the spreading of the tear film across the ocular surface. A reduction in the spread of tears during blinking could create areas of non wetting or stagnation of tears. This could result in increased tear evaporation and areas of ocular surface desiccation. Type of correction, characteristics of the flap and ablation profile Evidence suggests that tear film and ocular surface problems and dry eye symptoms after LASIK may be affected by the type of correction performed, the characteristics of the flap, and the ablation profile. LASIK for hyperopia appears to induce more severe and more sustained dry eye symptoms and greater adverse effects on the ocular surface and tear film, compared to LASIK for myopia. This may reflect greater corneal sensory denervation effects with hyperopic LASIK due to the larger flap and midperipheral ablation. Also, an increased number of older patients, who are more likely to experience dry eye, have hyperopic LASIK. Management of the ocular surface and tear film after LASIK Artificial tears are a critical component of the ocular surface and tear film management strategy after LASIK. Carboxymethyl cellulose-based, hydroxypropyl methylcellulose-based, and sodium hyaluronate-based artificial tears have been recommended to protect and regenerate the ocular surface and tear film.
4 Vol. XII, No.2, April - June Reference 1. Golas L, Manche EE. Dry eye after laser in situ keratomileusis with femtosecond laser and mechanical keratome. J Cataract Refract Surg Aug;37(8): Shoja MR, Besharati MR. Dry eye after LASIK for myopia: Incidence and risk factors. Eur J Ophthalmol Feb;17(1): Salomão MQ, Ambrósio R Jr, Wilson SE. Dry eye associated with laser in situ keratomileusis: Mechanical microkeratome versus femtosecond laser. J Cataract Refract Surg Oct;35(10): Mian SI, Li AY, Dutta S, Musch DC, Shtein RM. Dry eyes and corneal sensation after laser in situ keratomileusis with femtosecond laser flap creation Effect of hinge position, hinge angle, and flap thickness. J Cataract Refract Surg Dec;35(12): Toda I. LASIK and dry eye. Compr Ophthalmol Update Apr;8(2):79 85; discussion Ambrósio R Jr, Tervo T, Wilson SE. LASIK-associated dry eye and neurotrophic epitheliopathy: pathophysiology and strategies for prevention and treatment. J Refract Surg Apr;24(4): Shtein RM. Post-LASIK dry eye. Expert review of ophthalmology Oct;6(5): Nettune GR, Pflugfelder SC. Post-LASIK tear dysfunction and dysesthesia. Ocul Surf Jul;8(3): Toda I, Yoshida A, Sakai C, Hori-Komai Y, Tsubota K. Visual performance after reduced blinking in eyes with soft contact lenses or after LASIK. J Refract Surg Jan;25(1):69-73.
5 Clinical Pneumatic Retinopexy Dr.R.Ramakrishnan,Chief Medical Officer, Aravind Eye Hospital, Tirunelveli Definition Pneumatic retinopexy consists of an intravitreal gas injection with retinochroidal adhesive procedure (e.g. transconjunctival cryopexy) and appropriate head positioning. Indications 1. Isolated break of less than one clock hour in the superior 8 clock hours of retina 2. Multiple breaks within one clock hour of retina in the superior 9 clock hours 3. Mascular breaks and other posterior retinal breaks 4. Redetachment after scleral buckling due to superior open break 5. Fish mouthing after RD surgery. Contraindications 1. Multiple breaks extending over more than one clock hour of retina 2. Single break larger than one clock hour 3. Breaks in the inferior 4 clock hour of retina 4. Presence of PVR of grade C or more 5. Mental retardation 6. Physical disability precluding maintenance of the required positioning 7. Uncontrolled glaucoma 8. Difficulty in assessment of retina due to media haze. Important notes 1. The selected gas is drawn through a Milipore filter (0.22µm). 2. A few ml.of gas drawn into the syringe is discarded and the syringe is refilled. 3. A disposable 30 gauge, ½ inch needle should be used for gas injection. 4. Gas should be injected moderately briskly, not too briskly nor too slowly. 5. Air travel is contraindicated for longer period of time with C3F8 due to risk of increased IOP during the ascent of the airplane. 6. Proper positioning after gas injection is a must 7. IOP should be checked of the selected gas and thereafter 8. Paracentasis may be done if required to lower the IOP 9. I/O should be done after gas injection to evaluate central retinal artery Possible complications 1. New or missed breaks 2. PVR 3. Redetachment 4. Persistent SRF 5. Macular pucker formation 6. ERM formation 7. Incarceration of Vitreous 8. Vitreous haze 9. Reopening of original break 10. Subconjunctival / subretinal gas 11. Increase IOP / Glaucoma 12. Lens Opacities 13. Dislocation of IOL 14. Bulbous Keratopathy 15. Subretinal pigment migration 16. Uveitis Geometry of intraocular gas bubble Arc of bubble contact (Degrees) Vitreous Diameter 21 mm 24 mm ml 0.42 ml ml 1.13 ml ml 2.24 ml ml 3.62 ml
6 6 AECS Illumination Different types of gases used for PR Gas Dose (%) Max.rate of expansion Max expansion Average time Average time of expansion Longevity Total Duration Air 0.8ml. No expansion No expansion No expansion 5-7 days SF6 0.5ml. 6 hours hours times days C3F8 0.3ml. 6-8 hours hours 4 times days C2F6 0.3ml 6-8 hours hours 3.3 times days Reference 1. Hutter J, Luu H, Schroeder L. A biological model of tamponade gases following pneumatic retinopexy. Curr. Eye Res Oct;25(4): Friberg TR. Inverted pneumatic retinopexy. Ophthalmology Nov;110(11):2261; author reply Schechter RJ. Inverted pneumatic retinopexy. Ophthalmology Nov;110(11): ; author reply Chang TS, Pelzek CD, Nguyen RL, Purohit SS, Scott GR, Hay D. Inverted pneumatic retinopexy: a method of treating retinal detachments associated with inferior retinal breaks. Ophthalmology Mar;110(3): Greenberg PB, Baumal CR. Laser therapy for rhegmatogenous retinal detachment. Curr Opin Ophthalmol Jun;12(3): Georgalas I, Papaconstantinou D, Karagiannis D, Ladas I. Pneumatic displacement of acute submacular hemorrhage with and without the use of tpa. Eur J Ophthalmol Apr;21(2):220; author reply Coe RP, Eller AW, Friberg TR. Pneumatic retinopexy. Arch. Ophthalmol Aug;129(8): ; author reply McGimpsey SJ, Cooke CA, Best RM. Pneumatic retinopexy. Ophthalmology Feb;114(2): Mansour AM. Pneumatic retinopexy for inferior retinal breaks. Ophthalmology Oct;112(10): Yeung L, Kokame GT, Brod RD, Lightman DA, Lai JC. Pneumatic retinopexy for retinal detachment associated with severe choroidal detachment. Retina (Philadelphia, Pa.) Jan;31(1): Chan CK, Lin SG, Nuthi ASD, Salib DM. Pneumatic retinopexy for the repair of retinal detachments: a comprehensive review ( ). Surv Ophthalmol Oct;53(5): Ross WH, Lavina A. Pneumatic retinopexy, scleral buckling, and vitrectomy surgery in the management of pseudophakic retinal detachments. Can. J. Ophthalmol Feb;43(1): Kleinmann G, Rechtman E, Pollack A, Schechtman E, Bukelman A. Pneumatic retinopexy: results in eyes with classic vs relative indications. Arch. Ophthalmol Nov;120(11): Zaidi AA, Alvarado R, Irvine A. Pneumatic retinopexy: success rate and complications. Br J Ophthalmol Apr;90(4): Schaal S, Sherman MP, Barr CC, Kaplan HJ. Primary retinal detachment repair: comparison of 1-year outcomes of four surgical techniques. Retina (Philadelphia, Pa.) Sep;31(8): Sharma T, Gopal L. Recent developments in vitreoretinal surgery. J Indian Med Assoc Dec;98(12):754 8,
7 Clinical Retinal Vasculitis Approach to Diagnosis and Management Retinal vasculitis is a sight threatening inflammatory eye disease which involves the retinal blood vessels, predominantly retinal veins. Clinically, it presents as fluffy white perivascular infiltrates in the retina with aqueous and vitreous inflammatory cells. Fluorescein angiogram shows staining and diffuse leakage from the retinal blood vessels with or without cystoid macular odema. The etiology of the disease is varied. It may occur as an isolated ocular condition, as a manifestation of infectious, or neoplastic disorders or in association with systemic inflammatory diseases. Hence, it is essential that a complete history, ocular and systemic examination and a detailed laboratory work up is done in all patients with retinal vasculitis. Classification The causes of Retinal vasculities can be classified as follows 1. Systemic diseases 2. Infectious diseases 3. Ocular diseases 4. Malignancies 5. Drug Induced Systemic diseases Sarcoidosis, Behcet s disease, Multiple sclerosis, Systemic lupus erythematosus, Wegeners granulomatosis, Polyarteritis nodosa, Relapsing polychondroitis, Seronegative arthropathies, Polymyositis, Dermatomyositis, Antiphospholipid antibody syndrome, Takayasu arteritis Crohn s disease. Infectious disease Tuberculosis, Toxoplasmosis, Syphilis, Herpes, Cytomegalovirus, Leptospirosis, Cat scratch disease, Candidiasis, Rickettsia, Amoebiasis, Brucellosis. Ocular disease Idiopathic, Intermediate uveitis, Eales disease, Birdshot retinochoroidopathy, Frosted branch angitis, Serpiginous choroiditis, Idiopathic retinal Vasculitis, aneurysms and neuroretinitis. Masquerades Leukemia, Lymphoma, Retinoblastoma Drug induced Immunoglobulins, Ripabutin methamphetamines Systemic disease associated with retinal vasculitis Behcet s disease It is a multisystem inflammatory disease which is diagnosed by the clinical triad of recurrent orogenital ulcers, skin lesions and uveitis. Erythema nodosum arthralgia and meningoencephalitis are also commonly seen. Ocular involvement is seen in 70% of patients. It usually presents as recurrent vasoocclusive retinopathy which affects both arterioles and veins in the posterior pole. Fundus examination shows retinal hemorrhages, Yellow, White retinal infiltrates, retinal odema and optic disc odema with hyperemic in the acute stage. Chronic stage of the disease shows macular ischemia neovascularization of retina and disc sheathed vessels and optic atrophy. Sarcoidosis This disease typically affects young adults and presents with bilateral hilar lymphadenopathy and ocular and skin lesions. Retinal vasculitis is a characteristic feature and mainly involves retinal veins. These venules are usually mid peripheral or peripheral in location and show short segments
8 8 AECS Illumination of perivascular cuffing associated with retinal infiltrates, Sarcoid nodules and snow ball vitreous opacities. Yellow perivenous exudates, classically described candle wax drippings (taches de bougie) may also be seen. Wegeners granulomatosis It is a granulomatous necrotizing vasculitic condition that primarily affects upper and lower respiratory tracts and kidneys. In addition to retinal vasculitis, other clinical findings include necrotizing scleritis, peripheral ulcerative keratitis, dacryocystitis and proptosis. Systemic lupus erythematosus Patients present with malaise, fatigue, anorexia and low grade fever. They may also have arthritis, Facial rash, alopecia and pleurisy. Fundus examination shows multiple cotton wool spots; dilated, tortuous arterioles and intraretinal haemorrhages. Retinal vasculitis is usually uncommon but very devastating. It causes severe vaso-occlusive diseases leading to retinal ischemia and proliferative retinopathy. Infectious diseases associated with retinal vasculitis Tuberculosis Though choroiditis is the most common ocular feature of tuberculosis, periphlebitis is also commonly present. It occurs either by direct infection or by hypersensitivity reaction to Mycobacterial antigens. It is associated with vitritis and retinal hemorrhages and may lead to branch or central retinal vein occlusion leading to neovascularization and vitreous hemorrhage. Toxoplasmosis Toxoplasmic retinochoroiditis is commonly associated with retinal periphlebitis. Retinal veins show continuous sheathing with narrowing near acute lesions. Perivasculitis is believed to be caused by an Arthus-type reaction. Locally produced antigens diffuse into the vessel walls and react with circulating antibodies, activate complement and recruit inflammatory cells that form a perivascular cuff. Focal periarterial exudates or plaques, called kyrieleis arterialitis are also seen near the active focus and these lesions do not cause vascular obstruction or leakage. Syphilis Syphilis can have protean ocular manifestations. Retinal vasculitis is rare and has been described in secondary and tertiary syphilis causing venous or arterial occlusion. Other clinical findings can be vitritis, chorioretinitis, neuro retinitis, optic neuritis, subretinal neovascularization and exudative retinal detachment. Herpes virus Retinal infections with herpes group of viruses cause necrotizing retinits, vasculitis, and retinal hemorrhages. Acute retinal necrosis caused by herpes simplex and varicella zoster viruses is a fulminant peripheral necrotizing retinitis with severe vitritis and occlusive vasculitis affecting arterioles in the retina and choroids. Cytomegalovirus in immunocompromised patients causes fluffy white necrotic lesions along the vascular arcades of the posterior pole with retinal hemorrhages and vasculitis. The vasculitis is caused by perivascular neutrophilic infiltration of both arteries and veins. Ocular diseases associated with retinal vasculitis Intermediate Uveitis is characterized by vitritis, snowball exudates, peripheral retinal periphlebitis and pars plana exudates. Eales disease is an idiopathic obliterative periphlebitis which commonly occurs in healthy young males between years of age. It starts anterior to the equator and progresses posteriorly and ultimately involves multiple quadrants of the retina. This inflammation induced vascular occlusion leads to proliferative vascular retinopathy with sequelae as recurrent vitreous hemorrhage and tractional retinal detachment. The etiology of this disease is still unknown however it is believed to be due to hypersensitivity to tuberculoprotein.
9 Vol. XII, No.2, April - June Birdshot Retinochoroidopathy is a bilateral panuveitis where fundus examination shows cream colored, deep, round lesions, retinal vasculitis and cystoid macular odema. Frosted branch angiitis is a rare vasculitis where thick inflammatory infiltrates surround the retinal arterioles and venules creating an appearance of frosted tree branches. The sheathing of the blood vessels is so extensive that the underlying vessels are obscured. Mostly it is idiopathic, but cases have been reported in herpes, rubella, cytomegalovirus infections and malignancies. Pathogenesis Retinal vasculitis is presumed to be an immunologically medicated condition. It is an autoimmune phenomenon and various studies have shown the presence of CD4+ve T cells within and surrounding the retinal vessels in patients with retinal vasculitis. Thus, cell medicated immunity plays a major role in the pathogenesis, however humoral immunity and immune complex formation can also be involved. Symptoms Patients usually complain of gradual painless loss of vision except where vasculitis involved the macular and there is sudden loss of vision. Presence of floaters is due to inflammatory exudates in the vitreous cavity. Scotomas, photopsias, Color vision alterations metamorphopsia may also be profound. Slit lamp examination may show-aqueous or vitreous vells, aqueous flare, keratic precipitates, posterior synechiae and posterior subcapsular cataract. Fundus examination reveals fluffy white exudates around retinal vessels in the form of either continuous skip lesions. Vascular sheathing, retinal hemorrhage retinal odema and anterior - venous anastomoses are seen in cases where venules are the site of inflammation. Cotton - wool spots which represent nerve fibre layer infarcts are mainly seen in systemic vasculitic diseases. Intra-retinal infiltrates are characteristic of infectious causes of retinal vasculitis except for Behcet s disease. Vitreous snow ball exudates and cystoid macular odema are seen in intermediate uveitis, sarcoidosis and tuberculosis. Chronic stage of the disease shows vascular occlusion, neovascularization of the disc or retina, vitreous hemorrhage, branch retinal vein occlusion, sclerosed vessels and optic atrophy. Involvement of retinal venules is more common in conditions like Behcet s disease, tuberculosis, sarcoidosis, Eales disease, multiple sclerosis, inflammatory bowel disease and sero negative arthropathies. Retinal arterioles are involved in systemic vasculitis and viral retinitis. Retinal capillary involvement occurs commonly in syphilis and whipples disease. Management Investigation As retinal vasculitis is associated with various systemic, ocular and infectious disease, a detailed laboratory work up is always essential. A thorough medical history and physical examination should be the basis for a focused diagnostic evaluation. The initial evaluation should include complete blood count, erythrocyte sedimentation rate, C-reactive protein, VDRL, FTA-ABS, mantoux test, angiotensin converting enzyme, rheumatoid factor (RA), antinuclear antibody (ANA) and chest x-ray. If an infectious etiology is suspected, especially in retinal vasculitis associated with dense vitritis investigations should include ocular fluid cultures, serological tests and polymerase chain reaction. Serological tests are done for toxoplasma, syphilis, lyme disease and cat-scratch disease. Polymerase chain reaction in ocular fluid specimens has been extremely useful in identifying herpes simplex, varicella zoster, cytomegalovirus, Mycobacterium tuberculosis and toxoplama gondii. In patients with non-infectious systemic diseases, diagnostic tests should be focused on systemic vasculitic syndromes. Laboratory work up includes rheumatoid factor, antinuclear antibody, anti-double stranded DNA antibodies, anti-neutrophil cytoplasmic antibodies, anticardiolipin antibodies, complement levels, and imaging studies.
10 10 AECS Illumination Human leukocyte antigen (HLA) testing is another useful technique in certain diseases. These HLA associations include Behcet s disease and HLA-B51, birdshot retinochoroidopathy and HLA-A29 and systemic lupus erythematosus and HLA-DR3, Finally, MRI and CT scan can be considered in patients with multiple sclerosis and primary central nervous system lymphoma. Fluorescein angiography can be done in active or healed vasculitis. It shows staining and leakage of retinal veins, areas of capillary non-perfusion, retinal neovascularization, sclerosis of vessels, optic disc leakage, cystoid macular odema, vascular occlusion and macular ischemia. Optical coherence tomography may also be done in cases of refractory macular odema to follow them and see the response of treatment when it is not clinically apparent. Treatment The main goal of treatment in retinal vasculitis is suppression of intraocular inflammation in order to prevent visual loss and long-term complications. The mainstay of therapy is corticosteroids and immuno suppressives. In case of an infective lesion, specific therapy against the infective agent with or without corticosteroids may be required. Corticosteroids may be given either systemically or by posterior subtenon s injection. Periocular steroids are useful in patients with unilateral and mild inflammation. Though this route avoids the systemic side effects, it carries a risk of raised intraocular pressure and globe perforation. Oral corticosteroids are given in patients with moderate to severe bilateral inflammation and a marked decrease in visual acuity. Severe cases of sight threatening retinal vasculitis involving the posterior pole may require intravenous methyl prednisolone followed by oral corticosteroids and immunosuppressives. Intravitreal steroid injections can also be given in cases of refractory macular odema. In cases, where retinal vasculitis does not respond or shows inadequate control to oral corticosteroids, steroid sparing immunosuppressive agents are useful. These drugs are also used in patients who develop intolerable side effects to oral steroids. Various immunosuppressive agents used for treatment of retinal vasculitis include azathioprine, cyclosporine, cyclophosphamide, methotrexate, mycophenolate mofetil and infliximab. The choice of immunosuppressive agent should be individualized for each patient with a specific systemic disease. Azathioprine, cyclosporine and inflicimab are used in-behcets disease. Alkylating agents like cyclophosphamide are often used with systemic corticosteroids in vasculitis associated with systemic autoimmune diseases like Wegeners granulomatosis and systemic lupus erythematosus. Topical steroids with cycloplegics are given in cases with co-existing iridocyclitis. Other modalities of treatment in retinal vasculitis are laser photocoagulation and vitrectomy. Laser photocoagulation is indicated in patients with retinal neovascularization with recurrent or non clearing vitreous hemorrhage and neovascular glaucoma. As photocoagulation may induce cystoid macular odema, intraocular inflammation must be adequately controlled prior to laser treatment. Vitrectomy is useful in patients with non-clearing vitreous hemorrhage, tractional retinal detachment and epiretinal membrane removal. Conclusion In summary, retinal vasculitis is not only a potentially blinding intraocular inflammatory condition, it can also be the first sign of a lethal systemic disease. A detailed history, ocular and physical examination with a focuses laboratory work up can help in prompt diagnosis and appropriate management of the disease.
11 Vol. XII, No.2, April - June Reference 1. Biswas J, Sharma T, Gopal L, Madhavan HN, Sulochana KN, Ramakrishnan S. Eales disease--an update. Surv Ophthalmol Jun;47(3): Natarajan S. From the editor s desk - vasculitis my brief synopsis. Indian J Ophthalmol Aug;59(4): Nourinia R, Montahai T, Amoohashemi N, Hassanpour H, Soheilian M. Idiopathic retinal vasculitis, aneurysms and neuroretinitis syndrome associated with positive perinuclear antineutrophil cytoplasmic antibody. J Ophthalmic Vis Res Oct;6(4): Pantanelli SM, Khalifa YM. Retinal manifestations of autoimmune and inflammatory disease. Int Ophthalmol Clin. 2012;52(1): Levy-Clarke GA, Nussenblatt R. Retinal vasculitis. Int Ophthalmol Clin. 2005;45(2): Sanders MD, Graham EM. Retinal vasculitis. Postgrad Med J Jul;64(753): Shrestha JK, Khadka D, Lamichhane G, Khanal S. Retinal vasculitis. Nepal J Ophthalmol Jun;1(1): Rahi AH, Tabbara KF. Retinal vasculitis: pathogenesis and laboratory investigations. Int Ophthalmol Clin. 1995;35(3): Brydak-Godowska J, Dróbecka-Brydak E. [Retinal vasculitis--causes, diagnosis, treatment]. Klin Oczna. 2007;109(1-3): Stanford MR, Graham EM. Systemic associations of retinal vasculitis. Int Ophthalmol Clin. 1991;31(3):23 33.
1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors
 Golden eye rules Examination techniques 1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors Snellen chart (6 metre)
Golden eye rules Examination techniques 1 Always test and record vision wearing distance spectacles test each eye separately A 1mm pinhole will improve acuity in refractive errors Snellen chart (6 metre)
TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM
 1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
Managing Post-Operative Complications for LASIK and PRK
 Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Eye Manifestations of Lupus And Sjogren s Syndrome
 Eye Manifestations of Lupus And Sjogren s Syndrome Based on a presentation by Dr. N. Kevin Wade at the BC Lupus Society Symposium held October 22, 2005. Background Dr. Wade completed his MD in 1998 at
Eye Manifestations of Lupus And Sjogren s Syndrome Based on a presentation by Dr. N. Kevin Wade at the BC Lupus Society Symposium held October 22, 2005. Background Dr. Wade completed his MD in 1998 at
Cataract Testing. What a Patient undergoes prior to surgery
 Cataract Testing What a Patient undergoes prior to surgery FINANCIAL DISCLOSURE I have no financial interest or relationships to disclose What do most Technicians find to be the most mundane yet very important
Cataract Testing What a Patient undergoes prior to surgery FINANCIAL DISCLOSURE I have no financial interest or relationships to disclose What do most Technicians find to be the most mundane yet very important
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels
 iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL
 REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS
 RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS FEHMA TUFAIL M.D Case Report A 77-year-old white male presented with a history of painful, red right eye. The patient was diagnosed with mild iritis in the right
RHEUMATOID ARTHRITIS ASSOCIATED SCLERITIS FEHMA TUFAIL M.D Case Report A 77-year-old white male presented with a history of painful, red right eye. The patient was diagnosed with mild iritis in the right
Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D.
 Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D. What is a retinal detatchment? The retina is the light sensitive layer covering the inside of the back of the eye. It is
Retinal Detachments Mark E. Hammer, M.D. Ivan J. Suñer, M.D. Marc C. Peden, M.D. What is a retinal detatchment? The retina is the light sensitive layer covering the inside of the back of the eye. It is
How To Know If You Can See Without Glasses Or Contact Lense After Lasik
 The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
Systemic Lupus Erythematosus
 Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES
 Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH)
 Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
Ocular Surface Syndrome after LASIK
 Alaa Atef Ghaith, MD Professor of Ophthalmology Alexandria University Ocular Surface Syndrome after LASIK Up to 33% of eyes Multifactorial entity which causes distress to the patients and physicians 1
Alaa Atef Ghaith, MD Professor of Ophthalmology Alexandria University Ocular Surface Syndrome after LASIK Up to 33% of eyes Multifactorial entity which causes distress to the patients and physicians 1
PATIENT CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
The pinnacle of refractive performance.
 Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
PSORIATIC ARTHRITIS. Chryssanthie Kafkala, M.D. INTRODUCTION:
 PSORIATIC ARTHRITIS Chryssanthie Kafkala, M.D. INTRODUCTION: Psoriatic arthritis is a disease with generally good prognosis. Both ocular and systemic involvement is usually benign, however, the following
PSORIATIC ARTHRITIS Chryssanthie Kafkala, M.D. INTRODUCTION: Psoriatic arthritis is a disease with generally good prognosis. Both ocular and systemic involvement is usually benign, however, the following
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report
 Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
Risks and Limitations of LASIK Procedure
 Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
C-30078 Diagnosis and Management of Dry Eyes Part 1. Dr Colm McAlinden, BSc (Hons), MSc, PhD and Dr Eirini Skiadaresi, MD.
 C-30078 Diagnosis and Management of Dry Eyes Part 1 Dr Colm McAlinden, BSc (Hons), MSc, PhD and Dr Eirini Skiadaresi, MD January 11 2013 Detailed Answers IMAGE A Image Courtesy of Professor Giuseppe Ravalico
C-30078 Diagnosis and Management of Dry Eyes Part 1 Dr Colm McAlinden, BSc (Hons), MSc, PhD and Dr Eirini Skiadaresi, MD January 11 2013 Detailed Answers IMAGE A Image Courtesy of Professor Giuseppe Ravalico
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions
 Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Vitreo-Retinal and Macular Degeneration Frequently Asked Questions What is a Vitreo-Retinal specialist? Retinal specialists are eye physicians and surgeons who focus on diseases in the back of the eye
Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy
 Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
Medical Care for the Elderly Visual Disorders in Middle-Age and Elderly Patients with Diabetic Retinopathy JMAJ 46(1): 27 32, 2003 Shigehiko KITANO Professor, Department of Ophthalmology, Diabetes Center,
Refractive Surgery - Correcting Eye Problems
 What is LASIK? The eye and vision errors The cornea is a part of the eye that helps focus light to create an image on the retina. It works in much the same way that the lens of a camera focuses light to
What is LASIK? The eye and vision errors The cornea is a part of the eye that helps focus light to create an image on the retina. It works in much the same way that the lens of a camera focuses light to
Managing Challenging Cases in Refractive Surgery
 Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
Lanoma - Research in Vision & Ophthalmology
 Denise L. Kayser, MD, MPH&TM Curriculum Vitae Work Address: 3536 Mendocino Avenue, Suite 380 Santa Rosa, CA 95403 Telephone: (707) 575-5353 Premedical Education Aug 1988 May 1992 Jan 1991 Aug 1991 Medical
Denise L. Kayser, MD, MPH&TM Curriculum Vitae Work Address: 3536 Mendocino Avenue, Suite 380 Santa Rosa, CA 95403 Telephone: (707) 575-5353 Premedical Education Aug 1988 May 1992 Jan 1991 Aug 1991 Medical
Principles of Diagnosis MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE. Medical Decision-Making. Medical Decision-Making.
 MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Principles of Diagnosis The study of the art and science of
MEDICAL DECISION-MAKING IN OPTOMETRIC PRACTICE Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com Principles of Diagnosis The study of the art and science of
Retinal Vasculitis REVIEW INTRODUCTION. Clinical Findings
 Ocular Immunology and Inflammation, 13:415 433, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591003828 REVIEW Retinal Vasculitis Ahmed M. Abu El-Asrar
Ocular Immunology and Inflammation, 13:415 433, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591003828 REVIEW Retinal Vasculitis Ahmed M. Abu El-Asrar
Guideline for the Management of Acute Peripheral Facial nerve palsy. Bells Palsy in Children
 Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
IMAGE ASSISTANT: OPHTHALMOLOGY
 IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE?
 24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
24. Glaucoma: Imaging EFFECT OF MYOPIC LASIK ON RETINAL NERVE FIBER LAYER THICKNESS- IS IT SAFE OR UNSAFE? Chief Author: Dr. Amit porwal 1 Co-Authors: Dr. Kavita Porwal 2, Dr. Puja Rai 1 1. Choithram Netralaya,
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Ophthalmic Consultants of Long Island
 Case History Improving Cataract and Refractive Surgery Outcomes Through Ocular Surface Optimization 59 year old healthy white female History increased IOP Mother has history of glaucoma Presents for refractive
Case History Improving Cataract and Refractive Surgery Outcomes Through Ocular Surface Optimization 59 year old healthy white female History increased IOP Mother has history of glaucoma Presents for refractive
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D.
 PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
Laser Vision Correction: A Tutorial for Medical Students
 Laser Vision Correction: A Tutorial for Medical Students Written by: Reid Turner, M4 Reviewed by: Anna Kitzmann, MD Illustrations by: Steve McGaughey, M4 November 29, 2011 1. Introduction Laser vision
Laser Vision Correction: A Tutorial for Medical Students Written by: Reid Turner, M4 Reviewed by: Anna Kitzmann, MD Illustrations by: Steve McGaughey, M4 November 29, 2011 1. Introduction Laser vision
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
ON NOT Associated with MS
 ON NOT Associated with MS Neuromyelitis optica (NMO, Devic s disease) Acute disseminated encephalomyelitis (ADEM) Chronic relapsing inflammatory optic neuropathy (CRION) Post-vaccination-associated optic
ON NOT Associated with MS Neuromyelitis optica (NMO, Devic s disease) Acute disseminated encephalomyelitis (ADEM) Chronic relapsing inflammatory optic neuropathy (CRION) Post-vaccination-associated optic
SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic
 SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic Many roads can lead to glaucoma. With the exception of primary open-angle glaucoma (POAG) and
SECONDARY GLAUCOMA: Pseudoexfoliation (PXF), Pigmentary Dispersion Syndrome (PDS), Neovascular (NV), Uveitic Many roads can lead to glaucoma. With the exception of primary open-angle glaucoma (POAG) and
INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE DETAILED TABLE
 Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
Proposed Disease Severity Level No apparent Mild Non- Proliferative Moderate Nonproliferative Severe Non- Proliferative Proliferative INTERNATIONAL CLINICAL DIABETIC RETINOPATHY DISEASE SEVERITY SCALE
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling.
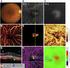 Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
Spectral domain OCT used to view and quantify choroidal vascular congestion in new subretinal fluid following scleral buckling. Robert Gizicki MD, Mohamed Haji, Flavio Rezende Retina Service, Hôpital Maisonneuve-Rosemont,
Management of Epithelial Ingrowth after LASIK. Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA
 Management of Epithelial Ingrowth after LASIK Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA Acknowledgements IOP Ophthalmics Staar Surgical Case Presentation 46
Management of Epithelial Ingrowth after LASIK Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA Acknowledgements IOP Ophthalmics Staar Surgical Case Presentation 46
Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years
 Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years Hassan Hashemi, MD 1,2 Mehrdad Mohammadpour, MD 3 Abstract Purpose: To describe a case of successful laser in situ
Retreatment by Lifting the Original Laser in Situ Keratomileusis Flap after Eleven Years Hassan Hashemi, MD 1,2 Mehrdad Mohammadpour, MD 3 Abstract Purpose: To describe a case of successful laser in situ
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION
 NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
IntraLase and LASIK: Risks and Complications
 No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
Vision Correction Surgery Patient Information
 Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Descemet s Stripping Endothelial Keratoplasty (DSEK)
 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Refractive Errors & Correction
 Super Vision 6 Chapter Lasik is currently the most sophisticated procedure for correction of refractive errors. Lasik is an acronym for Laser Assisted Insitu Keratomileusis. In Lasik, Excimer laser is
Super Vision 6 Chapter Lasik is currently the most sophisticated procedure for correction of refractive errors. Lasik is an acronym for Laser Assisted Insitu Keratomileusis. In Lasik, Excimer laser is
Ocular manifestations of HIV infection
 Ocular manifestations of HIV infection Introduction AIDS is an infectious disease caused by the gradual decrease in CD4+ T lymphocytes causing subsequent opportunistic infections and neoplasia. It is a
Ocular manifestations of HIV infection Introduction AIDS is an infectious disease caused by the gradual decrease in CD4+ T lymphocytes causing subsequent opportunistic infections and neoplasia. It is a
Corporate Medical Policy
 Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2015 6/2016 6/2015 Description of Procedure or Service
Corporate Medical Policy Intravitreal Implant File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intravitreal_implant 11/2010 6/2015 6/2016 6/2015 Description of Procedure or Service
INFORMED CONSENT FOR LASER ASSISTED SUBEPITHELIAL KERATOMILEUSIS (LASEK)/PHOTO-REFRACTIVE KERATECTOMY (PRK)
 INFORMED CONSENT FOR LASER ASSISTED SUBEPITHELIAL KERATOMILEUSIS (LASEK)/PHOTO-REFRACTIVE KERATECTOMY (PRK) Please read the following consent form very carefully. Please initial each page where indicated.
INFORMED CONSENT FOR LASER ASSISTED SUBEPITHELIAL KERATOMILEUSIS (LASEK)/PHOTO-REFRACTIVE KERATECTOMY (PRK) Please read the following consent form very carefully. Please initial each page where indicated.
Getting Ready for ICD-10. Dianna Hoskins, OCS Cincinnati Eye Institute
 Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
Dianna Hoskins, OCS Cincinnati Eye Institute Chart Documentation: Will your documentation stand up to ICD-10? Do you always mark which eye, severity or status of the disease (chronic or acute), site, etiology
Institute of Ophthalmology. Thyroid Eye Disease. aka Thyroid Associated Ophthalmopathy
 Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Associated Eye Surgeons
 Associated Eye Surgeons 45 Resnik Road, Suite 301 Plymouth, MA 02360 Henry J Kriegstein MD, FACS Board Certified Lois M. Townshend, MD, FRCSC Board Certified Kristin S. Kenney, OD LASIK CONSENT FORM I.
Associated Eye Surgeons 45 Resnik Road, Suite 301 Plymouth, MA 02360 Henry J Kriegstein MD, FACS Board Certified Lois M. Townshend, MD, FRCSC Board Certified Kristin S. Kenney, OD LASIK CONSENT FORM I.
What is Refractive Error?
 Currently, about 55% of the civilian pilots in the United States must utilize some form of refractive correction to meet the vision requirements for medical certification. While spectacles are the most
Currently, about 55% of the civilian pilots in the United States must utilize some form of refractive correction to meet the vision requirements for medical certification. While spectacles are the most
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY
 INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INFORMED CONSENT FOR PHAKIC IMPLANT SURGERY INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
How To See With An Cl
 Deciding on the vision correction procedure that s right for you is an important one. The table below provides a general comparison of the major differences between Visian ICL, LASIK and PRK. It is NOT
Deciding on the vision correction procedure that s right for you is an important one. The table below provides a general comparison of the major differences between Visian ICL, LASIK and PRK. It is NOT
Multiple Sclerosis. Ellen Yu, M.D. Case Report
 Multiple Sclerosis Ellen Yu, M.D. Case Report A 44 white female presented with a complaint of floaters on both eyes. There was no blurring of vision, flashes, pain nor photophobia. Past medical and family
Multiple Sclerosis Ellen Yu, M.D. Case Report A 44 white female presented with a complaint of floaters on both eyes. There was no blurring of vision, flashes, pain nor photophobia. Past medical and family
DIABETIC RETINOPATHY. Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered
 DIABETIC RETINOPATHY Diabetes mellitus Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered insulin production or activity. There are two types diabetes mellitus- Insulin
DIABETIC RETINOPATHY Diabetes mellitus Diabetes mellitus is an abnormality of the blood glucose metabolism due to altered insulin production or activity. There are two types diabetes mellitus- Insulin
Slide 4. Slide 5. Slide 6
 Slide 1 High Risk LASIK Patients Do you feel lucky? Slide 4 Derek N. Cunningham, OD, FAAO Slide 2 Traditional Risk Assessment Slide 5 Randelman Scale What s the point Topography (unilateral keratoconics?)
Slide 1 High Risk LASIK Patients Do you feel lucky? Slide 4 Derek N. Cunningham, OD, FAAO Slide 2 Traditional Risk Assessment Slide 5 Randelman Scale What s the point Topography (unilateral keratoconics?)
Guide to Eye Surgery and Eye-related Claims
 If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
If you or a loved one have suffered because of a negligent error during eye treatment or surgery, you may be worried about how you will manage in the future, particularly if your eyesight has been made
To: all optometrists and billing staff
 Number: Opto 27 Date: September 29, 2011 Page: 1 of 1 Subject: Schedule of Optometric Benefits amendments October 1, 2011/New explanatory code list Reference: Schedule of Optometric Benefits To: all optometrists
Number: Opto 27 Date: September 29, 2011 Page: 1 of 1 Subject: Schedule of Optometric Benefits amendments October 1, 2011/New explanatory code list Reference: Schedule of Optometric Benefits To: all optometrists
THE EYES IN MARFAN SYNDROME
 THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
THE EYES IN MARFAN SYNDROME Marfan syndrome and some related disorders can affect the eyes in many ways, causing dislocated lenses and other eye problems that can affect your sight. Except for dislocated
Ophthalmology Department,Tanta University, Egypt
 Moataz M. Sabry, MD, PhD. Ophthalmology Department,Tanta University, Egypt 1 SHOULD WE ABONDONE MECHANICAL MICROKERATOMES? 2 With Mechanical, LASIK is a one-laser procedure, there s no moving of patient
Moataz M. Sabry, MD, PhD. Ophthalmology Department,Tanta University, Egypt 1 SHOULD WE ABONDONE MECHANICAL MICROKERATOMES? 2 With Mechanical, LASIK is a one-laser procedure, there s no moving of patient
Eye Diseases. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com otf30101 Last reviewed: 05/21/2014 1
 Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Eye Diseases Introduction Some eye problems are minor and fleeting. But some lead to a permanent loss of vision. There are many diseases that can affect the eyes. The symptoms of eye diseases vary widely,
Macular Hole. James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D.
 Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
Macular Hole James L. Combs, M.D. Eleanore M. Ebert, M.D. Byron S. Ladd, M.D. George E. Sanborn, M.D. Jeffrey H. Slott, M.D. (804) 285-5300 or (804) 287-4200 www.vaeye.com Macular Hole In order to maintain
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition?
 There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
Introduction Houston Retina Associates
 1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
1 2 Introduction This book was written by Houston Retina Associates to provide our patients with basic knowledge about retinal anatomy, an introduction to some of the diagnostic tests and treatments used
WHAT SHOULD TREATMENT ACHIEVE?
 Uveitis Information Group Factsheet The Treatment of Uveitis (2) Drug Treatments Please use these factsheets as background information to help discussion with your doctors. Individual cases may vary enormously
Uveitis Information Group Factsheet The Treatment of Uveitis (2) Drug Treatments Please use these factsheets as background information to help discussion with your doctors. Individual cases may vary enormously
Pre-Operative Laser Surgery Information
 Pre-Operative Laser Surgery Information Contact 1800 10 20 20 Our Facility The Canberra Eye Laser Centre has always been at the forefront of refractive technology employing the most up to date equipment
Pre-Operative Laser Surgery Information Contact 1800 10 20 20 Our Facility The Canberra Eye Laser Centre has always been at the forefront of refractive technology employing the most up to date equipment
CATARACT AND LASER CENTER, LLC
 CATARACT AND LASER CENTER, LLC Patient Information Date: Patient Name: M F Address: Street City State Zip Home Phone: Work Phone: Cell Phone: E-Mail : Referred by: Medical Doctor: Who is your regular eye
CATARACT AND LASER CENTER, LLC Patient Information Date: Patient Name: M F Address: Street City State Zip Home Phone: Work Phone: Cell Phone: E-Mail : Referred by: Medical Doctor: Who is your regular eye
To date, several million patients have been treated worldwide. So why not discover the benefits The Eye Hospital can bring to your life.
 L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939
 Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939 INFORMED CONSENT FOR LASIK (LASER IN SITU KERATOMILEUSIS) and PRK (PHOTOREFRACTIVE KERATECTOMY)
Daniel F. Goodman, M.D. 2211 Bush Street, 2nd Floor San Francisco, CA 94115 Phone: 415-474-3333 Fax: 415-474-3939 INFORMED CONSENT FOR LASIK (LASER IN SITU KERATOMILEUSIS) and PRK (PHOTOREFRACTIVE KERATECTOMY)
INFORMED CONSENT FOR LASIK SURGERY
 IMPORTANT: READ EVERY WORD! This information is to help you make an informed decision about having laser assisted in-situ keratomileusis (LASIK) surgery to treat your nearsightedness, farsightedness and/or
IMPORTANT: READ EVERY WORD! This information is to help you make an informed decision about having laser assisted in-situ keratomileusis (LASIK) surgery to treat your nearsightedness, farsightedness and/or
LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY
 Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE TECHNOLOGY
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) USING INTRALASE TM BLADE-FREE
Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery*
 Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery* I. Introduction A. Definition and Scope of Subspecialty Fellowship training requires more in depth education
Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery* I. Introduction A. Definition and Scope of Subspecialty Fellowship training requires more in depth education
THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY.
 THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY. EVERYBODY WANTS TO SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we rely on it to guide us through our day-to-day
THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY. EVERYBODY WANTS TO SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we rely on it to guide us through our day-to-day
The cataract laser technology of tomorrow is here for you today.
 The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options Thanks to new advancements, this is a great time to have cataract surgery Laser
The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options Thanks to new advancements, this is a great time to have cataract surgery Laser
Cataracts. Cataract and Primary Eye Care Service...215-928-3041. Main Number...215-928-3000. Physician Referral...1-877-AT-WILLS 1-877-289-4557
 Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Main Number...215-928-3000 Physician Referral...1-877-AT-WILLS 1-877-289-4557 Emergency Service...215-503-8080 Cataract and Primary Eye Care Service...215-928-3041 Retina Service... 215-928-3300 Cataract
Avastin (Bevacizumab) Intravitreal Injection
 Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
Avastin (Bevacizumab) Intravitreal Injection This handout describes how Avastin may be used to treat wet age related macular degeneration (AMD) or macular edema due to retinal vascular disease such as
Vision Glossary of Terms
 Vision Glossary of Terms EYE EXAMINATION PROCEDURES Eyeglass Examinations: The standard examination procedure for a patient who wants to wear eyeglasses includes at least the following: Case history; reason
Vision Glossary of Terms EYE EXAMINATION PROCEDURES Eyeglass Examinations: The standard examination procedure for a patient who wants to wear eyeglasses includes at least the following: Case history; reason
INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY
 INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
INTRODUCTION INFORMED CONSENT FOR PHAKIC LENS IMPLANT SURGERY This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness.
WAKE FOREST BAPTIST HEALTH EYE CENTER. LASIK Consent Form
 1 WAKE FOREST BAPTIST HEALTH EYE CENTER LASIK Consent Form 1. GENERAL INFORMATION The following information is intended to help you make an informed decision about having Laser In-Situ Keratomileusis (LASIK).
1 WAKE FOREST BAPTIST HEALTH EYE CENTER LASIK Consent Form 1. GENERAL INFORMATION The following information is intended to help you make an informed decision about having Laser In-Situ Keratomileusis (LASIK).
Registered Charity No: 326679 Caring for those with a rare, complex and lifelong disease www.behcets.org.uk
 Registered Charity No: 326679 Caring for those with a rare, complex and lifelong disease www.behcets.org.uk Behçet s Disease and the Kidneys How are the kidneys affected by Behçet s disease? Kidney disease
Registered Charity No: 326679 Caring for those with a rare, complex and lifelong disease www.behcets.org.uk Behçet s Disease and the Kidneys How are the kidneys affected by Behçet s disease? Kidney disease
Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical,
 sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
 THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
THE EYES IN CHARGE: FOR THE OPHTHALMOLOGIST Roberta A. Pagon, M.D. Division of Medical Genetics, CH-25, Children's Hospital /Medical Center, Box C5371, Seattle, WA 98105-0371 bpagon@u.washington.edu (206)
Accelerated Refractive Performance
 Accelerated Refractive Performance Get There at the Speed of WaveLight Designed to accommodate your refractive technology goals now and into the future, the WaveLight Workstation is a faster way to get
Accelerated Refractive Performance Get There at the Speed of WaveLight Designed to accommodate your refractive technology goals now and into the future, the WaveLight Workstation is a faster way to get
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Rheumatology Labs for Primary Care Providers. Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine
 Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment
 Shinagawa LASIK Center OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment Minoru Tomita, MD, Ph.D 1) Executive Medical Director at Shinagawa LASIK Center, Tokyo, Japan 2) Clinical Professor
Shinagawa LASIK Center OCT-guided Femtosecond Laser for LASIK and Presbyopia Treatment Minoru Tomita, MD, Ph.D 1) Executive Medical Director at Shinagawa LASIK Center, Tokyo, Japan 2) Clinical Professor
SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC)
 SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC) PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU
SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC) PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU
Explanation of the Procedure
 Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
DISTANCE LEARNING COURSE. Anatomy of the Patient Exam. 2008 2012, BSM Consulting All rights reserved.
 DISTANCE LEARNING COURSE Anatomy of the Patient Exam 2008 2012, BSM Consulting All rights reserved. Table of Contents OVERVIEW... 1 PRELIMINARY WORK-UP... 1 OTHER DIAGNOSTIC TESTING... 3 DIAGNOSIS... 4
DISTANCE LEARNING COURSE Anatomy of the Patient Exam 2008 2012, BSM Consulting All rights reserved. Table of Contents OVERVIEW... 1 PRELIMINARY WORK-UP... 1 OTHER DIAGNOSTIC TESTING... 3 DIAGNOSIS... 4
How To Diagnose And Treat Retinal Vasculitis
 Central Retinal Vein Occlusion due to retinal vasculitis Priyanka Doctor, M.S.(Ophth.) MERSI Case A 53 year old male presenting to us with sudden unilateral visual loss History Approximately two weeks
Central Retinal Vein Occlusion due to retinal vasculitis Priyanka Doctor, M.S.(Ophth.) MERSI Case A 53 year old male presenting to us with sudden unilateral visual loss History Approximately two weeks
Informed Consent for Refractive Lens Exchange (Clear Lens Replacement)
 Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
Mark Packer, M.D. Informed Consent for Refractive Lens Exchange (Clear Lens Replacement) This surgery involves the removal of the natural lens of my eye, even though it is not a cataract. The natural lens
Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps
 Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps Lingo Y. Lai, MD William G. Zeh, MD Clark L. Springs, MD The authors
Comparison of Residual Stromal Bed Thickness and Flap Thickness at LASIK and Post-LASIK Enhancement in Femtosecond Laser-Created Flaps Lingo Y. Lai, MD William G. Zeh, MD Clark L. Springs, MD The authors
