Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery*
|
|
|
- Roger Davidson
- 9 years ago
- Views:
Transcription
1 Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery* I. Introduction A. Definition and Scope of Subspecialty Fellowship training requires more in depth education about the pathophysiology and management than can usually be obtained in residency training in ophthalmology. Fellowships include a continuous period of intense and focused training in developing and maintaining knowledge, skills, scholarship and professionalism. Subspecialty Fellowship training should include: The diagnosis and medical management of diseases of the lids, conjunctiva, cornea/sclera and anterior ocular segment, as well as recognition and treatment of posterior segment disease that may affect the anterior segment. Surgery of the conjunctiva, cornea/sclera, anterior segment, lens, and anterior vitreous, with special emphasis on corneal transplantation and related procedures. Principles and practice of keratorefractive surgery. * Principles of contact lens fitting and management of complications of contact lens wear. (* Programs wishing to list Refractive Surgery on their Fellowship listing and certificate must also follow the additional Refractive Surgery guidelines listed with an asterisk (*)) B. Duration and Scope of Education 1. Any fellow entering AUPO FCC compliant program must be able to fully comply with the clinical requirements of the program and have completed an appropriate residency program for that sub specialty fellowship. 2. A minimum of 12 months of clinical training is required, including appropriate short periods for vacation or special assignments. In special circumstances the 12 months do not have to be continuous as long as the aggregate training is equal to 12 months or longer. 3. Prior to entry in the program, each fellow must be notified of the required length of the program, policies regarding vacation, duties, stipends, other forms of support and any restrictions associated with the training (e.g. restrictive covenant).
2 II. Institutional Organization 1. Fellowship programs are often in institutions that sponsor ACGME accredited residency programs in ophthalmology. Whenever possible, there should be coordination of the fellowship and residency programs. Affiliation of the fellowship with an ACGMEaccredited residency is not required. 2. The number of fellowship positions that may be offered will contingent on the adequacy of both clinical and surgical volume, number of faculty, and other resources. 3. All of a program s clinical positions should be offered through the San Francisco Fellowship Matching Program (SF FMP). Positions may be filled out of the Match only for unfilled positions after the Match results. The AUPO FCC must be notified at the time of initial application of any non clinical fellowship positions. Prior arrangements with applicants (e.g. notifying them of their rank) is against the spirit of the Match and considered a violation. 4. Where applicable, the fellowship program, as much as possible should complement, support, and enhance the residency program. Where applicable, the department chair, fellowship program director and residency program director should work together and periodically meet to assure that the presence of the subspecialty fellowship does not unduly draw cases, learning opportunities or funding from the residency program. III. Faculty Qualifications and Responsibilities A. Fellowship Program Director There must be a single program director responsible for the program. 1. Qualifications of the fellowship program director: a. Be certified by the American Board of Ophthalmology, or possess appropriate educational qualifications if outside of the United States. b. Have at least five years of clinical subspecialty experience following his/her training of which at least 50% is dedicated to the subspecialty. c. Be engaged in ongoing academic endeavors in the area of subspecialty training, as demonstrated by regular publications in refereed journals, presentation of research material at national meetings, appointments to national or international committees in the recognized specialty and should be a recognized expert in the field d. Clinical practice at least 50% of which is dedicated to the area of subspecialty practice.
3 e. Have an academic appointment on the faculty of a recognized JCAHO / AHA accredited institution. f. Be licensed to practice medicine in the state(s) where the program is located. g. Practice greater than 50% of the time in the institution(s) where the Fellow receives his training. 2. Responsibilities of the fellowship program director: a. Prepare a written statement outlining the educational goals of the program with respect to knowledge, skills and other attributes, and educational goals for each major rotation or other program assignment. b. Develop and maintain documentation of the fellow selection process, patient care statistics, evaluations of faculty and the program, and assessment of the fellow s performance. c. Have prior approval by the AUPO FCC for the following: i. A change in the number of fellow positions in the training program, including any non clinical positions. ii. iii. A change in the duration of the training period. Extension of individual period of training greater than three months. d. Select fellows in accordance with guidelines established by the San Francisco Fellowship Matching Program and where applicable any institutional and departmental policies and procedures. e. Designate and supervise the faculty through explicit descriptions of supervisory lines of responsibility for the care of patients. f. Ensure the implementation of fair procedures and due process regarding academic discipline and fellow complaints or grievances. g. Monitor fellow stress, including mental or emotional conditions inhibiting performance or learning, and drug or alcohol related dysfunction. Program directors and faculty should be sensitive to the need for timely provision of confidential counseling and psychological support services to fellows. Training situations that consistently produce undesirable stress on fellows must be evaluated and modified. h. Prepare an accurate statistical and narrative description of the program.
4 3. Any change in the Fellowship Director MUST be communicated to the AUPO FCC in writing within 30 days. B. Faculty Faculty members must: 1. Be highly qualified and possess appropriate clinical and teaching skills. The faculty must devote adequate time to the education of fellows. 2. Demonstrate a strong interest in the education of fellows, sound clinical and teaching abilities, support of the goals and objectives of the program, commitment to their own continuing medical education, and participation in scholarly activities. 3. Have regularly scheduled, documented meetings in order to review the program s goals and objectives, as well as the program s effectiveness in achieving them. 4. While the fellowship director will be the principal preceptor, one or more additional clinical faculty is required. Minimally, one additional faculty should have completed a year of cornea and external disease fellowship training, be certified by the ABO (or Canadian or foreign equivalent) and have at least two years of practice experience in that specialty. These additional instructors may have part time or voluntary faculty appointments. Additional (non clinical) faculty may include non ophthalmologists, and non physician doctorates. The expertise of the director and/or the additional instructors must include keratorefractive surgery for fellowships desiring to list Refractive Surgery in addition to Cornea & External Disease in their postings and certificates. C. Other Program Personnel Programs must be provided with the additional professional, technical and clerical personnel needed to support the administrative and educational activities of the program. IV. FACILITIES AND RESOURCES 1. Outpatient Examination Facilities The outpatient area of each participating program must have a minimum of one fully equipped examination lane for each fellow. There must be access to current diagnostic equipment. 2. Inpatient Facilities Inpatient facilities must be available with sufficient space and beds for good patient care.
5 3. Library Fellows must have ready access to a major medical library and facilities for electronic retrieval of information from medical databases V. EDUCATIONAL PROGRAM The program director is responsible for the structure and content of the educational program and must provide objectives, methods of implementation, and procedures for assessment of the program. The educational experience must be designed and supervised by the program director. The program requirements for cornea/external disease fellowship are a continuation, in depth, of the general ophthalmology residency program but extend beyond the normal requirements of a general program. A wider variety of diseases and more patients in each disease category are encountered. Fellowships may be offered in Cornea and External Disease alone or Cornea, External Disease and Refractive Surgery. (Programs wishing to list Refractive Surgery on their Fellowship certificate must also follow the additional Refractive Surgery guidelines listed with an asterisk (*)) A. Clinical Components The goal of the fellowship is to produce an ophthalmologist with subspecialty skills that allow independent medical and surgical management of cornea and external disease. The subspecialist should be able to use all of these skills in order to diagnose and treat disorders relevant to the subspecialty. The subspecialist should at a minimum be able to: 1. take a complete patient s history for relevant review of systems and the social history including the details of the onset and course of their ocular condition with special emphasis on anterior segment disease. 2. complete a detailed examination of the eyelids, orbits, conjunctiva, cornea, anterior chamber, iris, anterior chamber angle, lens, vitreous, retina and choroid. 3. evaluate a patient with acute or chronic redness of the eye. 4. diagnose acute or chronic loss of vision due to structural changes or anomalies of the anterior segment. 5. be able to create a differential diagnosis for the typical corneal findings for the specific anterior segment effects of various systemic and ocular medications. 6. recognize the various tests that are available to aid in the diagnosis of external disease patients including measurement of the tear film, use of the microbiology laboratory, information available from genetic analysis, special ophthalmic examination techniques (e.g. ultrasound, corneal topography/tomography, specular and confocal microscopy, optical coherence tomography and other anterior segment imaging devices). 7. for surgery of the cornea and conjunctiva, to delineate the risks and benefits for medical therapy and surgical procedures of the anterior segment.
6 The fellow should see and be responsible for approximately 2000 patients to allow experience in the following specific areas: 1. Acute and chronic blepharitis to include both infectious and non infectious etiologies, with emphasis on microbial blepharitis, meibomian gland dysfunction, and rosacea. 2. Acute and chronic conjunctivitis, neonatal conjunctivitis, Chlamydial disease, adenoviral conjunctivitis, allergic conjunctivitis, and bacterial conjunctivitis. 3. Acute and chronic infectious keratitis including bacterial, viral, fungal and parasitic, with emphasis on herpes simplex, herpes zoster, adenovirus, acanthamoeba, and contact lensassociated problems. 4. Non infectious keratitis including marginal keratitis, central ulcerative keratitis, epitheliopathies, endotheliopathies, and interstitial keratitis. 5. Anterior segment anomalies, including various anomalies associated with specific genetic abnormalities, corneal dystrophies, and corneal degenerations. 6. Benign and malignant adnexal, conjunctival and corneal neoplasias, including corneal/conjunctival intraepithelial neoplasia, melanocytic tumors, lymphocytic tumors, papillomatous lesions and congenital or developmental lesions. 7. Autoimmune and immunologic diseases of the anterior segment including allergy, corneal graft rejection, and cicatrizing conjunctivitis; and familiarity with oral and topical immunosuppression and anti allergy medications. 8. Fundamentals of anterior segment anatomy, chemistry, physiology and wound healing including tear formation and function, corneal topography/tomography, endothelial cell function and maintenance of corneal clarity. 9. Fundamentals of refractive surgery* and its complications, with special emphasis on forms of keratorefractive surgery including incisional, excisional (such as stromal removal by mechanical and laser ablation), thermal keratoplasty, and alloplastic inserts. 10. Principles of anterior segment pharmacology including antimicrobial, anti inflammatory, ocular hypotensive, topical/systemic chemotherapeutic and immunosuppressive agents, with emphasis on bioavailability, mechanism of actions, relative efficacy, safety, and potential complications. 11. Skill in anterior segment surgery including eyelid, conjunctival, scleral and corneal procedures, with emphasis on corneal protective procedures (such as tarsorrhaphy), reconstruction of the ocular surface, surgical management of corneal erosions, surgical management of ocular surface tumors and phototherapeutic keratectomy. 12. Skill in penetrating and lamellar keratoplasty, with emphasis on patient selection,
7 surgical technique, and postoperative care including recognition and management of graft rejection and endophthalmitis and advanced techniques for lamellar and penetrating keratoplasty including full-thickness transplants and endothelial keratoplasty. The fellow should have knowledge of different techniques of Keratoprosthesis surgery. 13. Knowledge of the diagnosis, medical management and surgical treatment of anterior segment trauma. 14. Fundamental knowledge of contact lens physiology, design and materials, and complications for both cosmetic and therapeutic use. 15. Understanding the role of diagnostic techniques including biomicroscopy, specular microscopy, corneal topography/tomography, vital stains of the ocular surface, corneal biopsy techniques and interpretation, and corneal pachymetry. 16. Medical and surgical management of corneal thinning and perforation, including techniques of pharmacological manipulation, office procedures such as application of tissue glue and therapeutic contact lenses. 17. Medical and surgical management of complications of IOLs including, but not exclusive to; dislocated IOLs, suturing IOLs, iris suturing and visual aberrations and complications related to single vision and multifocal IOLs 18. An understanding of cornea and conjunctival pathology results and interpretation of ocular cultures; 19. An eye banking curriculum including a review of specific eye banking functions (recovery, processing, storage, evaluation and distribution of tissue; and donor eligibility), and at least one on-site visit during the fellowship to an EBAA-accredited eye bank. 20. Skill in use of reference material, including electronic searching and retrieval of relevant articles, monographs, and abstracts. B. Didactic Components Demonstrate scholarly activity by participating in research and clinical conferences or their equivalent for a minimum of 100 hours per year of which 25 hours should be of didactic instruction, including seminars, lectures, basic science courses and hands on skill courses. Each fellow should be actively engaged in at least one research project during the fellowship year or be lead author of one peer reviewed publication or presentation at a nationally recognized meeting in corneal and external disease within one year of fellowship completion. Directly evaluate and provide diagnosis and recommended plan in the care of a minimum of 2,000 patients under direct supervision during the course of the year. These patients must have
8 corneal or external diseases as described in the main body of paragraph 5. The fellow must demonstrate that appropriate history was obtained, he examination was accurate, the use of the laboratory was directed by the history and physical examination, and that the differential diagnosis and management are logical. When applicable, corneal fellows will participate in the teaching programs of the cornea service and of the institution if the fellowship is affiliated with a teaching institution. Examples of such include the following: 1. Attendance at weekly grand rounds. The fellow is to actively participate in case presentations and discussions of patients with corneal and external disease. 2. Attendance at monthly morbidity, pathology, and complications conferences. 3. Attendance at lectures on corneal topics given by the faculty during the resident teaching program. These must include at least 6 lecture hours per year. The fellow must prepare and present at least one of these lectures. 4. Attendance and participation in courses on anterior segment surgery, corneal transplantation, external disease and refractive surgery. 5. The fellow must actively participate, along with the cornea faculty, in a journal club at least quarterly. The fellow and faculty should present and critically discuss selections from the current literature. 6. The fellow should attend local and regional conferences relevant to corneal and external disease surgery. C. Supervision 1. Faculty should be available to supervise fellows as they examine and treat outpatients and inpatients. They should be available for contemporary consultation, assistance, and review of the patients. The supervision should be direct for the majority of encounters. Direct faculty supervision occurs when the faculty reviews the findings with the fellow prior to the patient s leaving the clinic or being discharged from the hospital. 2. The faculty must participate as primary surgeon or assistant surgeon to the fellow in a sufficient number of surgical procedures to confirm the fellow s surgical judgment and skill. The fellow should receive instruction and develop surgical proficiency in both full thickness penetrating keratoplasty and selective endothelial keratoplasty. The fellow should participate as either primary or primary assistant in at least 70 endothelial replacement corneal transplant case with the fellow acting as primary surgeon in at least 10 endothelial keratoplasty cases and 10 penetrating keratoplasty cases. The fellow should actively participate in the postoperative management in the majority of grafts where he/she is part of the surgical team. The fellow should have sufficient experience
9 with other surgical procedures including pterygium excision with graft, corneal and conjunctival biopsies, astigmatic keratotomies, and phototherapeutic keratectomy. The fellow should participate in the surgery of more complex conditions, including extensive conjunctival reconstruction, amniotic membrane transplantation, lamellar keratoplasties, and limbal stem cell transplantation. The fellow should be certified for photorefractive keratectomy (PRK) and laser assisted stromal in situ keratomileusis (LASIK) for programs listing Refractive Surgery*. The fellow should participate in the planning and implementation of other astigmatic correcting techniques including toric IOLs, surgical wound revisions and laser enhancements. * 3. The faculty must make a determination that the fellow uses sound clinical judgment in making recommendations for surgery that is in patients best interests. The faculty is responsible to determine that the fellow has sufficient surgical skill to practice independently. 4. In programs offering training in refractive surgery, they will perform at least 8 laser refractive procedures (e.g. LASIK, PRK, LASEK) and assist and/or observe in at least 50 other cases. * D. Duty Hours and Conditions of Work Duty hours and night and weekend call for fellows must reflect the concept of responsibility for patients and provide for adequate patient care. Salary is left up to the discretion of the Program. It is strongly suggested that individual health benefits be included in any compensation package (even in the absence of salary). A minimum of one week vacation and one week of approved conference time should be allotted. A signed agreement between the Program Director (or institution, practice or department) and the fellow should be in place outlining the salary and benefits prior to any formal patient contact. The Fellow must be made aware of any restrictive covenant prior to accepting the fellowship. E. Scholarly Activity The fellowship must take place in a scholarly atmosphere where resources are available that allow the fellow to participate in scholarly activities, such as research. Fellows should participate in the development of new knowledge and evaluate research findings. The responsibility for establishing and maintaining an environment of inquiry and scholarship rests with the faculty. While not all members of the faculty must be involved in research, the staff as a whole must demonstrate broad involvement in scholarly activity. This activity should include: 1. Active participation of the faculty in clinical discussions, rounds and conferences in a manner that promotes a spirit of inquiry and scholarship. Scholarship implies an in depth understanding of basic mechanisms of normal and abnormal states and the application of current knowledge to practice.
10 2. Participation in journal clubs and research conferences. 3. Participation as a critical reviewer for journal articles either as primary reviewer or compiling a review for an faculty reviewer. 4. Active participation in regional or national professional and scientific societies, particularly through presentations at their meetings and publications in refereed journals. 5. Participation in research leading to peer review publications or presentations at regional and national scientific meetings. 6. Offering of guidance and technical support (e.g. research design, statistical analysis) for fellows involved in research. 7. Provision of support for fellow participation in scholarly activities. 8. Adherence by faculty and fellows, who participate in research, to the Declaration of Helsinki on Rights of Research Human Subjects and to the Association for Research in Vision and Ophthalmology s Guidelines for Use of Research Animals. F. Fellow s Research Activities The fellow should be exposed to opportunities to develop research skills. A specific block of time may be set aside for clinical or laboratory research. When the research component exceeds 20% of the total time it may be necessary that the fellowship be extended beyond [12] months. VI. EVALUATION A. Program and Faculty Evaluation The educational effectiveness of a program must be evaluated in a systematic manner. In particular, the quality of the curriculum and the extent to which the educational goals have been met by fellows must be assessed. Teaching faculty must be evaluated on a regular basis. Documentation of faculty evaluation should include teaching ability and commitment as well as clinical knowledge. There must be a formal mechanism by which fellows participate in this evaluation. Written evaluations by fellows, through mechanisms that promote candor and maintain confidentiality, as much as possible, should be utilized in the evaluation of both the program and faculty.
11 B. Fellow Evaluation There must be regular evaluation of the fellow s knowledge, skills, and overall performance, including the development of professional attitudes consistent with being a physician The program director, with the participation of members of the faculty, shall: 1. At least quarterly review the surgical log, evaluate the knowledge, skills and professional growth of the fellow(s). 2. Communicate each evaluation to the fellow in a timely manner. 3. Advance fellows to positions of higher responsibility on the basis of evidence of their progressive development of knowledge, skills and professionalism. 4. Maintain a permanent record of evaluation for each fellow and have it accessible to the fellow and other authorized personnel. 5. Participate with and allow the Fellow to participate in any program evaluations and/or reviews performed by or authorized by the AUPO FCC. C. The program director must provide a written, final evaluation for each fellow who completes the program. The evaluation must include a review of the fellow s performance during the period of training and should verify that the fellow has demonstrated sufficient professional ability to practice competently and independently. This final evaluation should be part of the fellow s permanent record maintained by the Program Director. ACCEPTED 01/26/05 REVISED 04/26/07 REVISED 11/11/08 REVISED 11/20/09 REVISED 04/11/11 ACCEPTED 10/23/11 REVISED 10/10/15 ACCEPTED 5/3/16
Program Requirements for Fellowship Education in Neuro- Ophthalmology
 Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Program Requirements for Fellowship Education in Surgical Retina & Vitreous
 Program Requirements for Fellowship Education in Surgical Retina & Vitreous I. Introduction A Definition and Scope of the Subspecialty The goal of the fellowship is to provide an advanced level of training
Program Requirements for Fellowship Education in Surgical Retina & Vitreous I. Introduction A Definition and Scope of the Subspecialty The goal of the fellowship is to provide an advanced level of training
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY SUPERVISION OF RESIDENTS POLICY Applies to: All Ophthalmology Residents, including those in ACGME- and non-acgme-accredited specialty
Medicare and Corneal Surgery: Cosmetic versus Functional
 Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE
 BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family Physicians
BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family Physicians
BSM Connection elearning Course
 BSM Connection elearning Course Scope of the Eye Care Practice 2008, BSM Consulting All Rights Reserved. Table of Contents OVERVIEW...1 THREE O S IN EYE CARE...1 ROUTINE VS. MEDICAL EXAMS...2 CONTACT LENSES/GLASSES...2
BSM Connection elearning Course Scope of the Eye Care Practice 2008, BSM Consulting All Rights Reserved. Table of Contents OVERVIEW...1 THREE O S IN EYE CARE...1 ROUTINE VS. MEDICAL EXAMS...2 CONTACT LENSES/GLASSES...2
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH)
 Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
Educational Goals & Objectives for Ophthalmology Residents at Parkland Memorial Hospital (PMH) Competencies addressed: PC = Patient care MK = Medical knowledge Pr = Professionalism PBLI = Practice-based
Managing Post-Operative Complications for LASIK and PRK
 Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
VISION PATTERN. What Can you Expect from the ReSTOR procedure?
 RESTOR Presbyopia is the normal aging process that everyone experiences over the age of 40 which affects near vision. This usually results in the need for reading glasses or bifocals. The crystalline lens
RESTOR Presbyopia is the normal aging process that everyone experiences over the age of 40 which affects near vision. This usually results in the need for reading glasses or bifocals. The crystalline lens
WHAT IS A CATARACT, AND HOW IS IT TREATED?
 4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
4089 TAMIAMI TRAIL NORTH SUITE A103 NAPLES, FL 34103 TELEPHONE (239) 262-2020 FAX (239) 435-1084 DOES THE PATIENT NEED OR WANT A TRANSLATOR, INTERPRETOR OR READER? YES NO TO THE PATIENT: You have the right,
THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY.
 THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY. EVERYBODY WANTS TO SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we rely on it to guide us through our day-to-day
THE GUIDE TO REFRACTIVE LENS EXCHANGE SEE CLEARLY. EVERYBODY WANTS TO SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we rely on it to guide us through our day-to-day
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments
 Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Corporate Medical Policy Implantation of Intrastromal Corneal Ring Segments File Name: Origination: Last CAP Review: Next CAP Review: Last Review: implantation_of_intrastromal_corneal_ring_segments 8/2008
Basic Standards for Residency Training in Ophthalmology
 Basic Standards for Residency Training in Ophthalmology American Osteopathic Association and American Osteopathic Colleges of Ophthalmology and Otolaryngology Head and Neck Surgery BOT Oct 2015, Effective
Basic Standards for Residency Training in Ophthalmology American Osteopathic Association and American Osteopathic Colleges of Ophthalmology and Otolaryngology Head and Neck Surgery BOT Oct 2015, Effective
Explanation of the Procedure
 Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
Informed Consent Cataract Surgery with Intraocular Lens Implant Please initial below indicating that you have read and understand each section Introduction The internal lens of the eye can become cloudy
PLASTIC SURGERY RESIDENTS HANDBOOK
 PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
MEDICAL POLICY No. 91529-R2 REFRACTIVE KERATOPLASTY / LASIK
 REFRACTIVE KERATOPLASTY / LASIK Effective Date: August 18, 2010 Review Dates: 7/07, 6/08, 6/09, 6/10, 8/10, 8/11, 8/12, 8/13, 8/14 Date Of Origin: July 2007 Status: Current I. POLICY/CRITERIA Keratoplasty
REFRACTIVE KERATOPLASTY / LASIK Effective Date: August 18, 2010 Review Dates: 7/07, 6/08, 6/09, 6/10, 8/10, 8/11, 8/12, 8/13, 8/14 Date Of Origin: July 2007 Status: Current I. POLICY/CRITERIA Keratoplasty
Call today at 1 877 702 2020
 Call today at 1 877 702 2020 VISIAN ICL LASIK is a well known, successful, and accurate laser vision correction procedure which has been FDA approved in the U.S. for 15 years. The majority of patients
Call today at 1 877 702 2020 VISIAN ICL LASIK is a well known, successful, and accurate laser vision correction procedure which has been FDA approved in the U.S. for 15 years. The majority of patients
International Guidelines for Specialty Training and Education in Oral and Maxillofacial Surgery
 International Guidelines for Specialty Training and Education in Oral and Maxillofacial Surgery International Guidelines for Specialty Training and Education in Oral and Maxillofacial Surgery International
International Guidelines for Specialty Training and Education in Oral and Maxillofacial Surgery International Guidelines for Specialty Training and Education in Oral and Maxillofacial Surgery International
Residency Program in Ocular Disease and. Refractive and Ocular Surgery
 Mission Statement: Residency Program in Ocular Disease and Refractive and Ocular Surgery The mission of the Eye Center of Texas (ECT) residency program is to provide qualified postdoctoral optometry graduates
Mission Statement: Residency Program in Ocular Disease and Refractive and Ocular Surgery The mission of the Eye Center of Texas (ECT) residency program is to provide qualified postdoctoral optometry graduates
I have read and understood this page. Patient Initials
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
Curriculum Vitae. Irwin Y. Cua, M.D. Present Positions:
 Curriculum Vitae Name: Irwin Y. Cua, M.D. Present Positions: Affiliate Consultant, Vision Laser Center, St. Luke s Medical Center Affiliate Consultant, Section of Cornea and External Disease, St. Luke
Curriculum Vitae Name: Irwin Y. Cua, M.D. Present Positions: Affiliate Consultant, Vision Laser Center, St. Luke s Medical Center Affiliate Consultant, Section of Cornea and External Disease, St. Luke
Ocular Surface Diseases Course 2016 MIAMI,FLORIDA. Bascom Palmer Eye Institute. Sponsored by the University of Miami Miller School of Medicine
 Ocular Surface Diseases Course 2016 Bascom Palmer Eye Institute Sponsored by the University of Miami Miller School of Medicine MIAMI,FLORIDA April 16, 2016 BASCOM PALMER EYE INSTITUTE Ocular Surface Diseases
Ocular Surface Diseases Course 2016 Bascom Palmer Eye Institute Sponsored by the University of Miami Miller School of Medicine MIAMI,FLORIDA April 16, 2016 BASCOM PALMER EYE INSTITUTE Ocular Surface Diseases
Cornea and Refractive Surgery Update
 Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
NP/PA Clinical Hepatology Fellowship Summary of Year-Long Curriculum
 OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery
 Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 INTRODUCTION A university wishing to have an accredited program in Orthopedic Surgery must also sponsor an accredited
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 INTRODUCTION A university wishing to have an accredited program in Orthopedic Surgery must also sponsor an accredited
Master of Physician Assistant Studies Course Descriptions for Year I
 FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
FALL TERM COURSES: Master of Physician Assistant Studies Course Descriptions for Year I PHAC 7230 Fundamentals in Pharmacology for Health Care I Credit Hrs: 3 This course will build on foundational knowledge
Descemet s Stripping Endothelial Keratoplasty (DSEK)
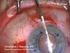 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
How To Treat Eye Problems With A Laser
 1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
Basic Standards for Residency Training in Ophthalmology
 RES. NO. 0 COPT 0/ For Public Comment Page Basic Standards for Residency Training in Ophthalmology American Osteopathic Association and American Osteopathic Colleges of Ophthalmology and Otolaryngology
RES. NO. 0 COPT 0/ For Public Comment Page Basic Standards for Residency Training in Ophthalmology American Osteopathic Association and American Osteopathic Colleges of Ophthalmology and Otolaryngology
RESIDENCY IN PRIMARY EYE CARE William V. Chappell Jr. Veterans Multi-Specialty Outpatient Clinic
 RESIDENCY IN PRIMARY EYE CARE William V. Chappell Jr. Veterans Multi-Specialty Outpatient Clinic Mission of the Residency Program Daytona Beach, Florida Program Coordinator: Ian D. Raden, O.D., M.B.A.
RESIDENCY IN PRIMARY EYE CARE William V. Chappell Jr. Veterans Multi-Specialty Outpatient Clinic Mission of the Residency Program Daytona Beach, Florida Program Coordinator: Ian D. Raden, O.D., M.B.A.
ATTACHMENT I TO APPENDIX B OF UNOS BYLAWS
 ATTACHMENT I TO APPENDIX B OF UNOS BYLAWS Designated Transplant Program Criteria XIII. Transplant Programs. A. In order to qualify for membership, a transplant program must utilize, for its histocompatibility
ATTACHMENT I TO APPENDIX B OF UNOS BYLAWS Designated Transplant Program Criteria XIII. Transplant Programs. A. In order to qualify for membership, a transplant program must utilize, for its histocompatibility
2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1
 Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1 INTRODUCTION A university wishing to have an accredited program in Orthopedic
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1 INTRODUCTION A university wishing to have an accredited program in Orthopedic
two years (as part-time fellows) will need discuss and receive approval from the relevant certifying Board. instead of one?
 Frequently Asked Questions: Sports Medicine Review Committees for Emergency Medicine, Family Medicine, Pediatrics, and Physical Medicine & Rehabilitation ACGME Question Scope and Duration of Program/Distance
Frequently Asked Questions: Sports Medicine Review Committees for Emergency Medicine, Family Medicine, Pediatrics, and Physical Medicine & Rehabilitation ACGME Question Scope and Duration of Program/Distance
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine
 Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
Medicine in Osteopathic Family Practice and Manipulative Treatment
 0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical,
 sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
sight see OLYMPIA EYE & LASER CENTRE Your one stop vision centre Our ophthalmic centre offers comprehensive eye management, which includes medical, At the Olympia Eye & Laser Centre, our vision is to improve
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques
 Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
Minimally Invasive Surgery: Femtosecond Lasers and Other Innovative Microsurgical Techniques Julio Narváez MD Associate Professor of Ophthalmology Loma Linda University Non-Refractive Applications of Femtosecond
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME
 Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
Frequently Asked Questions: Physical Medicine and Rehabilitation Review Committee for Physical Medicine and Rehabilitation ACGME Questions Program Personnel and Resources Does the Review Committee grant
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL
 REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES
 Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Vision Correction Surgery Patient Information
 Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Eye Surgery. Laser Eye Surgery and Refractive Surgery
 Eye Surgery Laser Eye Surgery and Refractive Surgery Traditional LASIK (Laser-In-Situ-Keratomileusis) Technique is the most practiced surgical procedure for resolving of the eyesight problems with dominating
Eye Surgery Laser Eye Surgery and Refractive Surgery Traditional LASIK (Laser-In-Situ-Keratomileusis) Technique is the most practiced surgical procedure for resolving of the eyesight problems with dominating
Frequently Asked Questions: Ophthalmology Review Committee for Ophthalmology ACGME
 Frequently Asked Questions: Ophthalmology Review Committee for Ophthalmology ACGME Question Introduction What is the process to follow when a resident needs additional time beyond the 36-month program
Frequently Asked Questions: Ophthalmology Review Committee for Ophthalmology ACGME Question Introduction What is the process to follow when a resident needs additional time beyond the 36-month program
COS Statement on Values for Uninsured Services in Canada
 COS Statement on Values for Uninsured Services in Canada Introduction A number of eye health services provided by physicians are not considered medically necessary and are therefore not insured under provincial
COS Statement on Values for Uninsured Services in Canada Introduction A number of eye health services provided by physicians are not considered medically necessary and are therefore not insured under provincial
Refractive Surgery. Common Refractive Errors
 Refractive Surgery Over the last 25 years developments in medical technology and Refractive Surgery allow almost all need for glasses and contact lenses to be eliminated. Currently there are a number of
Refractive Surgery Over the last 25 years developments in medical technology and Refractive Surgery allow almost all need for glasses and contact lenses to be eliminated. Currently there are a number of
Mastering the Techniques of LASIK, EPILASIK and LASEK (Techniques and Technology with DVD-ROM)
 440 Kerala Journal of Ophthalmology Vol. XX, No. 4 B O O K REVIEW Mastering the Techniques of LASIK, EPILASIK and LASEK (Techniques and Technology with DVD-ROM) Edited by Ashok Garg, Jorge L Alio, Bojan
440 Kerala Journal of Ophthalmology Vol. XX, No. 4 B O O K REVIEW Mastering the Techniques of LASIK, EPILASIK and LASEK (Techniques and Technology with DVD-ROM) Edited by Ashok Garg, Jorge L Alio, Bojan
Basic Standards for Residency Training in Child and Adolescent Psychiatry
 Basic Standards for Residency Training in Child and Adolescent Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Adopted 1980 Revised, 1984
Basic Standards for Residency Training in Child and Adolescent Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Adopted 1980 Revised, 1984
Excimer Laser Eye Surgery
 Excimer Laser Eye Surgery This booklet contains general information that is not specific to you. If you have any questions after reading this, ask your own physician or health care worker. They know you
Excimer Laser Eye Surgery This booklet contains general information that is not specific to you. If you have any questions after reading this, ask your own physician or health care worker. They know you
Consent for Bilateral Simultaneous Refractive Surgery PRK
 Consent for Bilateral Simultaneous Refractive Surgery PRK Please sign and return Patient Copy While many patients choose to have both eyes treated at the same surgical setting, there may be risks associated
Consent for Bilateral Simultaneous Refractive Surgery PRK Please sign and return Patient Copy While many patients choose to have both eyes treated at the same surgical setting, there may be risks associated
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION
 NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
NC DIVISION OF SERVICES FOR THE BLIND POLICIES AND PROCEDURES VOCATIONAL REHABILITATION Section: E Revision History Revised 01/97; 05/03; 02/08; 04/08; 03/09; 05/09; 12/09; 01/11; 12/14 An individual is
RESIDENCY IN PRIMARY EYE CARE/LOW VISION REHABILITATION VA BOSTON HEALTHCARE SYSTEM
 RESIDENCY IN PRIMARY EYE CARE/LOW VISION REHABILITATION VA BOSTON HEALTHCARE SYSTEM PROGRAM DIRECTOR: Jennifer A. Gustafson, OD, FAAO PROGRAM SITES: VA Boston Healthcare System and local affiliated sites
RESIDENCY IN PRIMARY EYE CARE/LOW VISION REHABILITATION VA BOSTON HEALTHCARE SYSTEM PROGRAM DIRECTOR: Jennifer A. Gustafson, OD, FAAO PROGRAM SITES: VA Boston Healthcare System and local affiliated sites
There must be an appropriate administrative structure for each residency program.
 Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State
 Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State University Columbus, Ohio Refractive Errors Myopia (nearsightedness)
Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State University Columbus, Ohio Refractive Errors Myopia (nearsightedness)
How To Choose An Implantable Contact Lens
 The Guide to Implantable Contact Lenses LOOK GREAT. SEE GREAT. Laser Refractive Cosmetic Eyelid Premium Cataract SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we
The Guide to Implantable Contact Lenses LOOK GREAT. SEE GREAT. Laser Refractive Cosmetic Eyelid Premium Cataract SEE CLEARLY Many of us take our sight for granted, whether it s forgetting how often we
refractive surgery a closer look
 2011-2012 refractive surgery a closer look How the eye works Light rays enter the eye through the clear cornea, pupil and lens. These light rays are focused directly onto the retina, the light-sensitive
2011-2012 refractive surgery a closer look How the eye works Light rays enter the eye through the clear cornea, pupil and lens. These light rays are focused directly onto the retina, the light-sensitive
LASER VISION C ORRECTION REFRACTIVE SURGERY CENTER
 LASER VISION C ORRECTION REFRACTIVE SURGERY CENTER W e l c o m e Throughout our history, physicians at Mass. Eye and Ear have led clinical advances and research that have resulted in the discovery of disease-causing
LASER VISION C ORRECTION REFRACTIVE SURGERY CENTER W e l c o m e Throughout our history, physicians at Mass. Eye and Ear have led clinical advances and research that have resulted in the discovery of disease-causing
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Maximizing Your Cataract Surgery Outcomes in Corneal Disease
 Maximizing Your Cataract Surgery Outcomes in Corneal Disease W. Barry Lee, M.D., F.A.C.S. Cornea & Refractive Surgery Eye Consultants of Atlanta Piedmont Hospital Co-Medical Director Georgia Eye Bank Atlanta,
Maximizing Your Cataract Surgery Outcomes in Corneal Disease W. Barry Lee, M.D., F.A.C.S. Cornea & Refractive Surgery Eye Consultants of Atlanta Piedmont Hospital Co-Medical Director Georgia Eye Bank Atlanta,
IMAGE ASSISTANT: OPHTHALMOLOGY
 IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
IMAGE ASSISTANT: OPHTHALMOLOGY Summary: The Image Assistant has been developed to provide medical doctors with a software tool to search, display, edit and use medical illustrations of their own specialty,
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK)
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
LICENSURE TO PRACTICE: California (Expired 1980) 1976-1980 Washington 1979-present California 1987-present
 Richard D. Grutzmacher, MD EDUTION: University of California, Berkeley, BA, Physiology, 1972 Northwestern University School of Medicine, Chicago, Illinois, Medical School 1976 PROFESSIONAL TRAINING and
Richard D. Grutzmacher, MD EDUTION: University of California, Berkeley, BA, Physiology, 1972 Northwestern University School of Medicine, Chicago, Illinois, Medical School 1976 PROFESSIONAL TRAINING and
Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model.
 TRAINING REQUIREMENTS Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model. A plastic surgery program director may choose to
TRAINING REQUIREMENTS Introduction There are two approved residency training models for plastic surgery, the Independent Model and the Integrated Model. A plastic surgery program director may choose to
Managing Challenging Cases in Refractive Surgery
 Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
The cataract laser technology of tomorrow is here for you today.
 The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options Thanks to new advancements, this is a great time to have cataract surgery Laser
The cataract laser technology of tomorrow is here for you today. See inside to learn about all your exciting new options Thanks to new advancements, this is a great time to have cataract surgery Laser
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM
 1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
Welcome to our Office!
 Randy Burks, MD, FACS Raymond Gailitis, MD, FACS Northwest Medical Plaza 5800 Colonial Drive, Suite 100-103 Margate, Florida 33063 954-977-8770 Comprehensive Eye Care 954-969-0090 LASIK 954-977-8774 Fax
Randy Burks, MD, FACS Raymond Gailitis, MD, FACS Northwest Medical Plaza 5800 Colonial Drive, Suite 100-103 Margate, Florida 33063 954-977-8770 Comprehensive Eye Care 954-969-0090 LASIK 954-977-8774 Fax
Congratulations! You have just joined the thousands of people who are enjoying the benefits of laser vision correction.
 Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology
 Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology INTRODUCTION 2009 A university wishing to have an accredited program in Pediatric Hematology/Oncology must also
Specific Standards of Accreditation for Residency Programs in Pediatric Hematology/Oncology INTRODUCTION 2009 A university wishing to have an accredited program in Pediatric Hematology/Oncology must also
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels
 iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
iocutouchtm for ipad Contents of Videos and Still Images Anatomy 906. Normal Eye and Orbit - no labels 907. Normal Eye and Orbit - with labels Normal Eye 474. Normal Eye overview 476. Cornea - overview
Refractive Surgery. Evolution of Refractive Error Correction
 Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Some of the ophthalmic surgeries performed at the DMV Center.
 Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary center as well as the equipment
Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary center as well as the equipment
Oregon Eye Specialists, PC YOUR GUIDE CATARACT SURGERY. Improving VISION. Improving LIFE.
 Oregon Eye Specialists, PC YOUR GUIDE TO CATARACT SURGERY Dinelli M. Monson, M.D. Comprehensive Ophthalmology Physician and Surgeon Tualatin Clinic: 19250 SW 65 th Ave, Ste 215 503.692.3630 Newberg Clinic:
Oregon Eye Specialists, PC YOUR GUIDE TO CATARACT SURGERY Dinelli M. Monson, M.D. Comprehensive Ophthalmology Physician and Surgeon Tualatin Clinic: 19250 SW 65 th Ave, Ste 215 503.692.3630 Newberg Clinic:
CLINICAL DEPARTMENTS STATEMENT OF FACULTY ORGANIZATION, STANDARDS AND CRITERIA FOR RANK (Approved 9/27/94) (Revised 10/13/04, 12/20/05, 12/2007)
 CLINICAL DEPARTMENTS STATEMENT OF FACULTY ORGANIZATION, STANDARDS AND CRITERIA FOR RANK (Approved 9/27/94) (Revised 10/13/04, 12/20/05, 12/2007) INTRODUCTION Each Clinical Department 1 will develop the
CLINICAL DEPARTMENTS STATEMENT OF FACULTY ORGANIZATION, STANDARDS AND CRITERIA FOR RANK (Approved 9/27/94) (Revised 10/13/04, 12/20/05, 12/2007) INTRODUCTION Each Clinical Department 1 will develop the
VASDHS MEDICAL CENTER
 VASDHS MEDICAL CENTER The General Practice Residency Program at the Veterans Affairs San Diego Healthcare System, Medical Center is a one year advanced training program accredited by the Commission on
VASDHS MEDICAL CENTER The General Practice Residency Program at the Veterans Affairs San Diego Healthcare System, Medical Center is a one year advanced training program accredited by the Commission on
INFORMED CONSENT LASER IN SITU KERATOMILEUSIS (LASIK)
 Edward C. Wade, M. D Christopher D. Allee, O. D. Ting Fang-Suarez, M. D. Jill Autry, O. D. Mark L. Mayo, M. D. Amanda Bachman, O. D. Randall N. Reichle, O. D Julie Ngo, O. D. INFORMED CONSENT LASER IN
Edward C. Wade, M. D Christopher D. Allee, O. D. Ting Fang-Suarez, M. D. Jill Autry, O. D. Mark L. Mayo, M. D. Amanda Bachman, O. D. Randall N. Reichle, O. D Julie Ngo, O. D. INFORMED CONSENT LASER IN
Our Commitment To You
 SYSTEM SUPPORT Quality-crafted, the system boasts dependability with high efficiency and low gas usage. We provide responsive service and maintenance contract options, supported by our nationwide direct
SYSTEM SUPPORT Quality-crafted, the system boasts dependability with high efficiency and low gas usage. We provide responsive service and maintenance contract options, supported by our nationwide direct
LASIK. Cornea. Iris. Vitreous
 LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
LASIK Introduction LASIK surgery is a procedure that improves vision and can decrease or eliminate the need for eyeglasses or contact lenses. If you and your doctor decide that LASIK surgery is right for
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
To date, several million patients have been treated worldwide. So why not discover the benefits The Eye Hospital can bring to your life.
 L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT
 TLC The Laser Center (Northeast) Inc. TLC Laser Eye Centers (Charlotte) TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT Informed Consent. The purpose of this Informed Consent is to help
TLC The Laser Center (Northeast) Inc. TLC Laser Eye Centers (Charlotte) TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT Informed Consent. The purpose of this Informed Consent is to help
Refractive errors are caused by an imperfectly shaped eyeball, cornea or lens, and are of three basic types:
 Tips on Lasik Eye Surgery If you re tired of wearing glasses or contact lenses, you may be considering Lasik eye surgery one of the newest procedures to correct vision problems. Before you sign up for
Tips on Lasik Eye Surgery If you re tired of wearing glasses or contact lenses, you may be considering Lasik eye surgery one of the newest procedures to correct vision problems. Before you sign up for
Prosthetic Replacement of the Ocular Surface Ecosystem PROSE. Information for Patients and Doctors
 Prosthetic Replacement of the Ocular Surface Ecosystem PROSE Information for Patients and Doctors Treatment Description PROSE (prosthetic replacement of the ocular surface ecosystem) is a pioneering treatment
Prosthetic Replacement of the Ocular Surface Ecosystem PROSE Information for Patients and Doctors Treatment Description PROSE (prosthetic replacement of the ocular surface ecosystem) is a pioneering treatment
Curriculum Vitate. Name: Mohamed Mostafa Hantera Profile: Male, 40 years, Married and father for 2 Kids. Current location: Jeddah, Saudi Arabia.
 1 Curriculum Vitate SUMMARY: Name: Mohamed Mostafa Hantera Profile: Male, 40 years, Married and father for 2 Kids. Current location: Jeddah, Saudi Arabia. Current position(s): Chief of Cornea and Refractive
1 Curriculum Vitate SUMMARY: Name: Mohamed Mostafa Hantera Profile: Male, 40 years, Married and father for 2 Kids. Current location: Jeddah, Saudi Arabia. Current position(s): Chief of Cornea and Refractive
How To Become A Chiropractor
 CCEI The Councils On Chiropractic Education International INTERNATIONAL CHIROPRACTIC ACCREDITATION STANDARDS FOREWORD To master its future, the chiropractic profession must contribute to and thereby influence
CCEI The Councils On Chiropractic Education International INTERNATIONAL CHIROPRACTIC ACCREDITATION STANDARDS FOREWORD To master its future, the chiropractic profession must contribute to and thereby influence
