GPsi - A Case Study in Substance Misuse
|
|
|
- Stella Woods
- 5 years ago
- Views:
Transcription
1 The safe implementation of a prison-based methadone maintenance programme: 7 year time-series analysis of primary care prescribing data Nat MJ Wright HMP Leeds Healthcare Department 2 Gloucester Terrace Armley Leeds LS12 2TJ [email protected] (corresponding author) Charlotte French HMP Leeds Healthcare Department 2 Gloucester Terrace Armley Leeds LS12 2TJ [email protected] Victoria Allgar John Hughlings Jackson Building University of York Heslington York YO10 5DD [email protected] 1
2 Abstract Aims: To evaluate the impact and safety of the introduction of a general practitioner with a special interest (GPsi) in substance misuse led methadone prescribing service into a UK prison between 2003 and Methods: Time series analysis of secondary prescribing data pertaining to opiate maintenance therapies, opiate detoxification therapies and opiate related deaths for the time period 2003 to Results: Results show that following introduction of a GPsi in substance misuse there was a statistically significant increase in both methadone maintenance and detoxification treatments. Over time the rate of methadone maintenance prescribing plateaued with a corresponding decrease in the rate of methadone detoxification prescribing. There were no methadone related deaths in prison over the study period. Conclusion: The phased introduction of opiate replacement therapies into a busy remand prison did not result in any deaths within the prison for which opiate replacement was identified as the cause. GPsi led opiate prescribing programmes can be introduced safely into secure environments. Keywords: methadone maintenance, prison medicine, opiates, dependence, 2
3 Background Recently published statistics show that the prison population for England and Wales was 84,586 at the end of August 2010 [1]. This figure represents an increase in the prison population of approximately 30 per cent since The increase was due to a combination of tougher sentencing and enforcement outcomes, and a more serious mix of offence groups coming before the courts. It equates to a prison population rate of 153/100,000 of the national population. Internationally there are countries with a higher proportion of the population imprisoned. For example the United States has the highest prison population rate in the world with 714 per 100,000 of the national population in prison and Russia 629/100,000 of the national population, [2]. Upon reception into prison up to 80% of offenders test positive for either heroin or cocaine [3]. A cross-sectional survey of a sample of the UK prison population conducted in 1998 revealed that 38% of male remand prisoners and 48% of sentenced prisoners admitted to using drugs during their current period of imprisonment. The survey was conducted at a time when there was very little drug treatment available in the UK prison setting. The practice of coerced detoxification from opiate maintenance was commonplace upon reception into prison leading to a class action brought against the Home Office for negligent drug treatment provision whilst in prison [4]. An out of court compensation settlement led to a growing pressure to develop prison based drug treatment services. Compensation was provided as it was acknowledged that opiate maintenance and detoxification therapies had significant potential to reduce harms associated with illicit drug withdrawal. 3
4 There was an established evidence base that opiate maintenance reduced rates of crime, illicit drug use, and injecting practice yet prisoners were not routinely provided this treatment. Also there was an emerging UK evidence base that rates of self-harm and suicides were markedly increased in the week following reception into prison and that uncontrolled symptoms of opiate withdrawal were a contributory factor [5]. At that time the vast majority of primary care services were provided by doctors employed by the Home Office and not the National Health Service (NHS). Not all practitioners offering primary care services held a certificate of accreditation in general practice. Nevertheless some drug users were able to become abstinent whilst in prison. However in the absence of safe prison based primary care prescribing of opiate maintenance there is an increased risk of drug related death upon release from prison. This is due to accidental overdose in the community if similar drug misuse practices are re-commenced upon release following a period of enforced abstinence in prison leading to a loss of tolerance to prescribed opiates. An analysis of almost 50,000 newly released prisoners in England and Wales during the period 1998 to 2000 highlighted over 440 deaths, of which over 250 (59%) were drug-related [6]. In the year following release, the drug-related mortality rate was 5.2 per 1000 per annum among men and 5.9 per 1000 per annum among women. However, all-cause mortality in the first and second weeks following prison release for men was 37 and 26 deaths per 1000 per annum, respectively. In total, 95% of these deaths were drug-related. All-cause mortality in the first and second weeks following prison release for women was 47 and 38 deaths per 1000 per 4
5 annum, respectively, all of which were drug-related [6]. These data highlights the period of the first two weeks post-release from prison as a time of high risk for opioid-related deaths. In June 2004, in such a context of litigation and drug related death post prison-release, an opiate maintenance programme was introduced into a remand prison in the North of England with a population of approximately 1200 prisoners. The introduction was phased and preceded the widespread introduction of such programmes across both the national and international prison estate. Examples of the international context at that time are that in the Australian penal system, a prison based randomised controlled trial evaluating the effectiveness of methadone maintenance had just been published [7]. Key findings were that at five-month follow-up in prison, those receiving methadone maintenance reported significant reductions in heroin use, drug injection and syringe sharing. Four years later, a USA randomised controlled trial evaluating the effectiveness of prison based opiate maintenance therapy was published. The researchers randomly allocated two hundred and eleven users prisoners to either counselling in prison, with passive referral to treatment upon release; counselling and transfer (counselling in prison with transfer to methadone maintenance treatment upon release); or counselling and methadone (methadone maintenance and counselling in prison, continued in a community-based methadone maintenance program upon release). Key findings were at one-month follow-up post release a higher engagement in treatment and lower proportion of individuals testing positive for illicit opiates in the group who received prison based methadone 5
6 maintenance [8]. However neither of these two trials specifically mentioned GP involvement in the provision of opiate maintenance to prisoner populations. We are unaware of any published empirical research pertaining to core competencies required by GPs in prescribing that has traditionally been viewed as high risk. In response to such a gap in the evidence base this paper reports the findings from a time series analysis of seven years prescribing data for opiate maintenance which took place at a time of increasing international research activity evaluating the introduction of such maintenance therapy into prison settings. Methods The introduction of a methadone maintenance programme was undertaken by a general practitioner with special interest (GPsi) in substance misuse who commenced prison based drug treatment in December 2003 in Her Majesty s Prison (HMP) Leeds, a remand prison with a capacity for 1283 prisoners, where the average length of stay for each prisoner was thirteen weeks. A consensus document between the UK Royal College of General Practitioners (RCGP) and Royal College of Psychiatrists, supported by the National Treatment Agency for Substance Misuse defined the competencies of a GPsi as having received specific higher-level training in the management of substance misusers in primary care, usually the Royal College of General Practitioners Certificate in the management of drug misuse in primary care, Part 2. The document recommended that such practitioners can deliver a fuller range of drug treatment services and, as a result of additional ongoing higher-level training and professional development activity, are able to work 6
7 more autonomously, accepting referrals from generic GP colleagues, and take responsibility for more complex cases in substance misuse [9]. For the first six months from January to June 2004 methadone was not prescribed but organisational changes were made to facilitate the introduction of a methadone maintenance programme. Such changes included writing a policy containing guidelines for safe prescribing, dispensing and administration; and stock requisition. In June 2004 the GPsi commenced a weekly prescribing clinic for opiate maintenance. Fifteen months later the number of clinics was increased to five per week. All new treatment inductions (new commencements) were seen in this clinic. However over the following two years patients stable on methadone maintenance treatment were followed up in generic (ie not substance misuse specific) prison GP clinics. Over time new inductions (commencements) onto maintenance treatment and methadone detoxification regimes were initiated in clinics run by prison GPs who had acquired core competencies to work as a GPsi in substance misuse. New treatment inductions included those who were initiated on methadone for the first time following a clinical history consistent with opioid dependence and a urine sample positive for either opiates, methadone or buprenorphine. It included new treatment inductions in either normal prison working hours or evening clinics for patients newly received into prison. It also included those assessed in such evening clinics where community prescribed opiate maintenance had been disrupted due to an absence of methadone prescribing in police custody at the time the study was taking place. Repeat treatment inductions were excluded from analysis. Such patients included 7
8 those who were re-imprisoned during the study period who had previously been included as a new treatment induction. Methadone prescribing for both maintenance and detoxification was initiated at a dose of 30mg daily if the patient was assessed on first night reception, and at a dose of 20mg daily if the patient was assessed in the routine prison clinic. The rationale for such prescribing regimes was that compared to patients presenting in routine clinics, patients presenting at first night prison reception typically both reported and exhibited more severe symptoms and signs of withdrawal. Subsequently for those receiving a detoxification regime at an initial dose of 20mg od (once daily), the dose would be increased the following day to 30mg od for a period of six days prior to a reducing regime from 30mg od to zero over a two week period. In total such a prescribing regime would be of three weeks duration. For those receiving a maintenance prescribing regime at an initial dose of 20mg od, the dose would be increased the following day to 30mg od. Any subsequent increases would only take place following review by a GP. Subsequently published national guidelines for prison recommend that to ensure patient safety within this context, methadone treatment programmes should be established through a process of dose induction. Initial doses of five to ten milligrams of methadone (1mg in 1ml mixture) are to be given, at least six hours apart [10]. National guidelines published in 2007 pertaining to drug treatment recommended in general, the initial daily dose will be in the range of mg. If tolerance is low or uncertain then mg is more appropriate. With heavily dependent misusers who are tolerant, and where the clinician is experienced or competent, a first dose can be up to 40 mg but it is unwise to exceed this dose [11]. 8
9 Anonymised secondary data for both maintenance and detoxification treatments was retrieved from the Pharmacy Manager prison pharmacy dispensing databases for the period covering the start of January 2003 to end March Once retrieved, the data was aggregated into discrete three month time periods according to the date of first receipt of a methadone prescription. Methadone prescribing was introduced into the prison in May Therefore by obtaining data at equally- spaced time intervals (ie. three month time periods) both pre and post-intervention, it was possible to analyse by an interrupted time-series methodology.. Durbin-Watson statistics were used to test for serial correlation (a relationship between values separated from each other by a given time lag). The trend component of this time-series is examined to determine the long-term variation of the trends in prescribing methadone maintenance and detoxification therapies in the prison and community. The basic model: Yt = bo + b1t + b2d + b3p + et, where T is time from the start of the observational period, D is a dummy variable for pre or post intervention and P is time since the intervention; et is the random variation at time t not explained by the model. Ordinary Least Squares regression was undertaken to analyse prescribing trends over time, with 3 independent variables: T time, D dummy for pre-post intervention and P time since the intervention. The model can determine the change over time before the intervention was implemented, change in the outcome measure from the last time point before the intervention to the first time point after the intervention, and the difference in the slope of the time period before the intervention and the slope of the time period after the intervention. Ordinary 9
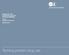
10 least squares regression assumes that the error terms associated with each observation (time point) are uncorrelated. Results Over the study period a total of 4551 patients were inducted onto methadone maintenance and 3181 patients received a detoxification treatment. For methadone maintenance, the numbers of individuals receiving maintenance prescriptions rise steadily from its introduction in 2004, to 282 in April - June Subsequently, prescriptions remain within the range of until October - December 2009, where they fall to 216 before rising slightly at the beginning of 2010 to 232. Figure 1 shows the number of inductions new commencements maintenance and detoxification episodes between the time period start of January 2003 to end of March 2010 and this is displayed in table format in appendix 1. <<<<Figure 1 here>>>> Ordinary least squares regression was undertaken to analyse prescribing trends over time. Durbin-Watson statistics to test for serial correlation of the error terms was not significant (p=0.556), meaning that there was no autocorrelation. The trend prior to intervention was flat (p=.978), as would be expected. Following the intervention of GPsi prescribing there was an increase in patients receiving maintenance (Graph 1), but this was not 10
11 significant (p=0.085). Also there was no significant change in trend immediately after the intervention (0.494). However over time post the intervention of a GPsi there is a statistically significant increase for methadone maintenance treatment episodes (p=0.002). As regards the results for detoxification treatments, prior to the time-point April - July 2006, detoxification treatments appear to have been preferred to maintenance. The number of detoxification prescriptions rose dramatically from 18 (April-June 2005) to 255 (October December 2005), staying higher than those for methadone until the end of 2006, when they fell to 161. There then appears to be a rapid increase in detoxification therapies prescribed in January-March 2007, reaching 277. However after this increase, methadone detoxification prescriptions have remained lower than those for methadone maintenance and have decreased steadily from 277 at the beginning of 2007 to 67 in January March Ordinary least squares regression was undertaken to analyse prescribing trends over time. Durbin-Watson statistics to test for serial correlation of the error terms was not significant (p=0.597), meaning that there was no autocorrelation. The trend prior to intervention was flat (p=0.935), as would be expected. Following the intervention of GPsi prescribing there was an increase in patients receiving detoxification (Graph 1), which was significant (p=0.016). There was no significant change in trend after the intervention (p=0.864). However over time post the intervention of a GPsi there was no statistically significant increase in detoxification treatment episodes (p=0.619). 11
12 Drug-related deaths There were no opioid related deaths in the prison over the study period prior to the introduction of methadone maintenance treatment. During the time period of there was one death of a patient receiving methadone treatment at the time of death. His death occurred in 2006 one week after initiation of methadone at a daily dose of 30mg. However toxicology investigations highlighted the illicit use of mirtazapine, a sedative antidepressant [12]. At inquest the coroner reported that the prescribing of methadone maintenance was appropriate in this case and therefore, this patient s death was not attributed to his methadone treatment. Thus, there are no methadone related deaths recorded at HMP Leeds since its introduction in Discussion Following the intervention of a GPsi led prescribing service for substance misuse there was a steady increase over the following four and half years in patients being initiated onto methadone maintenance. The fact that the increase only became statistically significant over time is evidence that the implementation was phased to ensure that the system was safe. From the time-point April-June 2008 a further increase in the number of patients being initiated onto methadone maintenance is evidence of a second prison based GPsi receiving the core competencies to work with substance misuse and the practice of methadone induction therefore becoming normalised in the prison healthcare department. 12
13 Following the introduction of a GPsi led prescribing service there was an immediate statistically significant increase in patients receiving detoxification regimes. However two years after the introduction there was a decline in detoxification prescribing, the decline starting in the time-point April-June This can be explained by the fact that the local prescribing protocol changed. Initially due to pressure on the service a patient could only be initiated onto opiate maintenance if they had failed to become abstinent upon completion of a detoxification regime. However as over 80% of drug users in the prison failed to achieve abstinence [13], the protocol was changed to permit patients to be inducted onto methadone maintenance where appropriate. In the time-point January -March 2007 there was a further increase in methadone detoxification treatments. This can be explained by the recruitment of a new GP who at the time of recruitment did not possess the core competencies of a GPsi. Therefore the prescribing interventions of the GP were limited to offering detoxification (and not maintenance) regimes. As the GP acquired the core competencies to practice as a GPsi, the number of maintenance treatments continued to rise and over time a corresponding fall in detoxification treatments. In 2001, a UK based taskforce highlighted that the prison environment can be a difficult and complex one in which to work as a doctor. It highlighted that the nature of the prisoner population meant that prison based doctors would require particular skills in dealing with alcohol and substance misuse. It also highlighted the inherent risks of professional isolation working in prison settings and recommended that the priority should be in developing a robust 13
14 structure of primary care provision in prison settings [14]. A key clinical governance concern was that not all doctors providing primary care services in the UK prison estate at that time were trained in the skills of general practice. In 2001 the UK Royal College of General Practitioners commenced a training unit dedicated to training general practitioners in the knowledge and skills required to competently offer treatment to drug users. At the time of writing, since the inception of this course 14,137 individuals have been trained in the basics of drug treatment and 2016 have received training to confer the competencies required to practice as a GPsi in substance misuse [15]. We would suggest that the RCGP has learned lessons that can be disseminated internationally. The RCGP through the Membership of Royal College of General Practitioners International academic examination currently has a successful formula for internationally conferring generic primary care core competencies. The challenge for the RCGP will be how it can replicate this successful generic international primary care model in the field of primary care drug treatment. We would suggest that networking with international policy leads, and international marketing of training programmes are key to disseminating best training practice. International data pertaining to the background of doctors providing primary care based drug treatment in prison settings is lacking. It is possible that other countries are facing similar clinical governance concerns regarding the safety of prison primary care based drug treatment. There is evidence from research conducted in the Belgian prison healthcare service of prisoners consulting the GP 3.8 times more than a demographically equivalent population in the community [16]. The high consultation rate was explained in part by health concerns relating to drug 14
15 misuse. However there is a paucity of research evaluating primary care based drug treatment provision. Clearly if internationally prisoners are high users of primary care services then general practitioners who have received training in the provision of safe drug treatment will be key to increasing the international provision of prison based drug treatment. It would not be our aspiration that such general practitioners would necessarily adopt the UK title of general practitioner with a special interest. Rather the purpose of this paper has been in describing the core competencies to ensure safe primary care provision. It is the competencies rather than the terminology that we would wish to share with the international readership. The main strength of this research is in highlighting that such primary care development is possible and that methadone replacement therapies can safely be introduced into prison settings providing such a practice is by GPs possessing a GPsi level of core competency. Additionally generic GPs are able to safely offer detoxification regimes within clear prescribing protocols. This is an important message to the GP field. The burden of investigation upon GPs practicing in secure environments is intense. In the UK, every death in custody is by statute subject to scrutiny by Coroner s Inquiry [17] and investigation by the Prisons and Probation Ombudsman [18]. Therefore GPs seeking to provide opiate maintenance therapies in the prison setting should only do so having undertaken either further training or supervision in the management of substance misuse. In 2007, the World Health Organisation through its Health in Prisons Project recommended opiate maintenance therapies are made more widely available across the international prison 15
16 estate [19]. Our research has provided a primary care workforce model which will be able to facilitate the safe and effective implementation of this key international policy recommendation. A primary care workforce is critical to increasing availability of drug treatment. Indeed in 1978 the WHO endorsed the critical importance of primary care organisations as the central focus for promoting improvements in population health [20]. The main limitation of this research is that it is limited to prescribing data collated at one remand prison and therefore we would be confident that our findings could be generalised with confidence only to remand prisons with similar health needs relating to substance misuse. Also it was not possible to cross-check our data against coronial records to evaluate the impact of the programme upon opioid related deaths post release from prison. We suggest this is an area for future research activity. Also our research did not collect data pertaining to buprenorphine medication as this was not routinely prescribed in the prison at the time of initiating data collection. The reason for this was that the UK prisons at that time had widespread problems regarding buprenorphine abuse and therefore prescribing of such medication was not encouraged [21]. Our research has shown that a GPsi led prison drug treatment service is safe if on first night reception the first induction dose of methadone does not exceed 30mg and if in routine outpatient prison clinics the first induction dose of methadone does not exceed 20mg. This provides evidence for future reviews of current UK national prison clinical guidelines which currently 16
17 recommend a more cautious approach of initial induction at doses of methadone 5-10mg given at least six hours apart [10]. Not every prison will have access to a GPsi. However increasingly clinical leads in prisons are practicing at a GPsi level of competency and our findings would support higher initial induction doses being prescribed in prison first night reception centres. In demonstrating that methadone maintenance prescribing can be safely introduced into prison settings, our findings raise questions regarding longterm outcomes of patients receiving such maintenance treatment. The outcomes of survival, re-offending, abstinence and retention in treatment postrelease are all areas that merit future research activity. Also comparing prescribing data between prisons internationally would facilitate the comparing of clinical standards and frameworks and lead to enhanced sharing of international best practice. Future research activity should also analyse prescribing data for buprenorphine as this is increasingly being used for both maintenance and detoxification in prison settings. In summary our research has highlighted that a GPsi led phased implementation of methadone maintenance into prisons does not compromise patient safety. Competing Interests None. 17
18 Author contributions NW provided access to the prescribing data from HMP Leeds and participated in the design of the project and drafted the manuscript. CF gathered and processed the data required to analyse the number of individuals commenced on methadone and also assisted in drafting the manuscript. VA conducted the statistical analysis and drafted this into the methods and results sections. All authors read and approved the final manuscript. Authors Information Nat Wright is the Associate Medical Director for Specialist Services and Vulnerable Groups, Leeds Community Healthcare. This role entails providing medical leadership to a cluster of prisons. Charlotte French undertook this work whilst completing a BSc in primary health care. Victoria Allgar is Senior Lecturer in Medical Statistics at Hull and York Medical School/Health Sciences, University of York. Acknowledgements We wish to acknowledge Chris Rowlands, head of pharmacy and clinical lead for HMP Leeds, for her help in retrieving the data from the pharmacy dispensing system. We also wish to acknowledge Sophie Wilkinson, Rose Kennedy, Nadia Hendrickse-Welsh and Matthew Limm, all of whom gathered some of the initial data in a project whilst at HMP Leeds. 18
19 Appendix 1 Table 1: Numbers of Methadone Maintenance and Detoxification new treatments issued from Time period Methadone Maintenance New Treatment Induction episodes Methadone New Detoxification Treatment episodes Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar Apr-Jun Jul-Sep Oct-Dec Jan-Mar TOTAL
20 References [1] Ministry of Justice Population in custody monthly tables August 2010 England and Wales: Ministry of Justice Statistics bulletin (accessed 11/06/2013). [2] Walmsley R. World Prison Population List (eighth edition). London: International Centre for Prison Studies, [3] National Offender Management Service (2005) Strategy for the Management and Treatment of Problematic Drug Users within the Correctional Facilities, London, National Offender Management Service. [4] Silverman J Prisoners who take on the system. (accessed 11/06/13). [5] Shaw J, Appleby L and Baker D. Safer Prisons: A National Study of Prison Suicides by the National Confidential Inquiry into Suicides and Homicides by People with Mental Illness. London: Department of Health, [6] Farrell M and Marsden J. Drug related mortality among newly released offenders London: Home Office, ce.gov.uk/rds/pdfs05/rdsolr4005.pdf (Accessed: 11/06/13). [7] Dolan K, Shearer J, MacDonald M, Mattick RP, Hall W and Wodak A. A randomised controlled trial of methadone maintenance treatment versus wait list control in an Australian prison system. Drug and Alcohol Dependence 2003; 72: [8] Kinlock TW, Gordon MS, Schwartz RP, O Grady K, Fitzgerald TT and Wilson M. A randomized clinical trial of methadone maintenance for prisoners: results at 1-month post-release. Drug and Alcohol Dependence 2007; 91: [9] Royal College of General Practitioners and Royal College of Psychiatrists. Roles and responsibilities of doctors in the provision of treatment for drug and alcohol misusers Council Report CR131 London: Royal College of Psychiatrists, [10] Department of Health, National Treatment Agency for Substance Misuse, Royal College of General Practitioners, Royal College of Psychiatrists and Royal Pharmaceutical Society of Great Britain. Clinical Management of Drug Dependence in the Adult Prison Setting, including psychosocial treatment as a core part. London: Department of Health,
21 [11] Department of Health (England) and the devolved administrations. Drug misuse and Dependence: UK guidelines on Clinical Management. London: Department of Health (England), the Scottish Government, Welsh Assembly Government and Northern Ireland Executive, [12] Shaw S, Report by the Prisons and Probation Ombudsman for England and Wales (April 2007). Investigation into the circumstances surrounding the death of a man at HMP Leeds in July (Accessed 11/06/13). [13] Wright NMJ, Sheard L, Adams CE, Rushforth B, Harrison W, Bound N, Hart R, Tompkins CNE. The Leeds Evaluation of Efficacy of Detoxification Study (LEEDS) Prisons Project: A randomised controlled trial comparing methadone and buprenorphine for opiate detoxification. British Journal of General Practice 2011; 61 (593): [14] Prison Health Task Force and Policy Unit Report of the Working Group on Doctors Working in Prisons. et/dh_ pdf. (Accessed 11/06/2013). [15] Schwarz M. Numbers completing RCGP certificate in substance misuse courses. Personal Communications, 11/1/13. [16] Feron JM, Paulus D, Tonglet R, Lorant V and Pestiaux D. Substantial use of primary health care by prisoners: epidemiological description and possible explanations. Journal of Epidemiology and Community Health 2005;59: [17] Coroner s Act (Accessed 11/06/2013). [18] Prisons and Probation Ombudsman (Accessed 11/06/2013). [19] World Health Organisation Health in prisons: A WHO guide to the essentials in prison health. data/assets/pdf_file/0009/99018/e90174.pdf (Accessed 11/06/2013). [20] WHO Primary Healthcare: Report of the International Conference on Primary Healthcare at Alma-Ata, USSR, September Geneva: WHO/UNICEF, [21] Ministry of Justice. A Survey of Buprenorphine Misuse in Prison. London: HM Prison Service, National Offender Management Service. Strategy for the Management and Treatment of Problematic Drug Users within the 21
22 Correctional Facilities. London: National Offender Management Service,
23 Timepoint at which GPsi prescribing commenced Number of individuals commenced on Methadone Treatment Jan-Mar 03 Apr-Jun 03 Jul-Sep 03 Oct-Dec 03 Jan-Mar 04 Apr-Jun 04 Jul-Sep 04 Oct-Dec 04 Jan-Mar 05 Apr-Jun 05 Jul-Sep 05 Oct-Dec 05 Jan-Mar 06 Apr-Jun 06 Jul-Sep 06 Oct-Dec 06 Jan-Mar 07 Time Apr-Jun 07 Jul-Sep 07 Oct-Dec 07 Jan-Mar 08 Apr-Jun 08 Jul-Sep 08 Oct-Dec 08 Jan-Mar 09 Apr-Jun 09 Jul-Sep 09 Oct-Dec 09 Jan-Mar 10 Figure 1: Number of individuals commenced on Methadone for either Maintenance or Detoxification at HMP Leeds from Maintenance Detox Figure 1
POWDER COCAINE: HOW THE TREATMENT SYSTEM IS RESPONDING TO A GROWING PROBLEM
 Effective treatment is available for people who have a powder-cocaine problem seven in ten of those who come into treatment either stop using or reduce their use substantially within six months POWDER
Effective treatment is available for people who have a powder-cocaine problem seven in ten of those who come into treatment either stop using or reduce their use substantially within six months POWDER
SCOTTISH PRISON SERVICE DRUG MISUSE AND DEPENDENCE OPERATIONAL GUIDANCE
 SCOTTISH PRISON SERVICE DRUG MISUSE AND DEPENDENCE OPERATIONAL GUIDANCE 1 P a g e The following Operational Guidance Manual has been prepared with input from both community and prison addictions specialists
SCOTTISH PRISON SERVICE DRUG MISUSE AND DEPENDENCE OPERATIONAL GUIDANCE 1 P a g e The following Operational Guidance Manual has been prepared with input from both community and prison addictions specialists
drug treatment in england: the road to recovery
 The use of illegal drugs in England is declining; people who need help to overcome drug dependency are getting it quicker; and more are completing their treatment and recovering drug treatment in ENGlaND:
The use of illegal drugs in England is declining; people who need help to overcome drug dependency are getting it quicker; and more are completing their treatment and recovering drug treatment in ENGlaND:
Support to Primary Care from Derbyshire Substance Misuse Service for prescribed / OTC drug dependence
 Support to Primary Care from Derbyshire Substance Misuse Service for prescribed / OTC drug dependence SUMMARY 1) Derbyshire Substance misuse service provides Psycho-social treatment interventions for ALL
Support to Primary Care from Derbyshire Substance Misuse Service for prescribed / OTC drug dependence SUMMARY 1) Derbyshire Substance misuse service provides Psycho-social treatment interventions for ALL
Reducing Drug Use, Reducing Reoffending Are programmes for problem drug-using offenders in the UK supported by the evidence?
 Bringing evidence and analysis together to inform UK drug policy Reducing Drug Use, Reducing Reoffending Are programmes for problem drug-using offenders in the UK supported by the evidence? Summary Over
Bringing evidence and analysis together to inform UK drug policy Reducing Drug Use, Reducing Reoffending Are programmes for problem drug-using offenders in the UK supported by the evidence? Summary Over
The Government's Drug Strategy
 Report by the Comptroller and Auditor General HC 297 SesSIon 2009 2010 march 2010 Tackling problem drug use Report by the Comptroller and Auditor General Tackling problem drug use HC 297 Session 2009-2010
Report by the Comptroller and Auditor General HC 297 SesSIon 2009 2010 march 2010 Tackling problem drug use Report by the Comptroller and Auditor General Tackling problem drug use HC 297 Session 2009-2010
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT ALCOHOL MISUSE
 SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
SPECIFICATION FOR THE LOCAL COMMISSIONED SERVICE FOR THE MANAGEMENT OF ALCOHOL MISUSE Date: March 2015 1 1. Introduction Alcohol misuse is a major public health problem in Camden with high rates of hospital
DMRI Drug Misuse Research Initiative
 DMRI Drug Misuse Research Initiative Executive Summary Dexamphetamine Substitution as a Treatment of Amphetamine Dependence: a Two-Centre Randomised Controlled Trial Final Report submitted to the Department
DMRI Drug Misuse Research Initiative Executive Summary Dexamphetamine Substitution as a Treatment of Amphetamine Dependence: a Two-Centre Randomised Controlled Trial Final Report submitted to the Department
Getting help for a drug problem A guide to treatment
 Getting help for a drug problem A guide to treatment Who we are The National Treatment Agency for Substance Misuse is part of the National Health Service. We were set up in 2001 to increase the numbers
Getting help for a drug problem A guide to treatment Who we are The National Treatment Agency for Substance Misuse is part of the National Health Service. We were set up in 2001 to increase the numbers
Alcohol and Re-offending Who Cares?
 January 2004 Alcohol and Re-offending Who Cares? This briefing paper focuses on the high level of alcohol misuse and dependence within the prison population. In recent years a great deal of time and money
January 2004 Alcohol and Re-offending Who Cares? This briefing paper focuses on the high level of alcohol misuse and dependence within the prison population. In recent years a great deal of time and money
The story of drug treatment
 EFFECTIVE TREATMENT CHANGING LIVES www.nta.nhs.uk www.nta.nhs.uk 1 The story of drug treatment The use of illicit drugs is declining in England; more and more people who need help with drug dependency
EFFECTIVE TREATMENT CHANGING LIVES www.nta.nhs.uk www.nta.nhs.uk 1 The story of drug treatment The use of illicit drugs is declining in England; more and more people who need help with drug dependency
The Federation of State Medical Boards 2013 Model Guidelines for Opioid Addiction Treatment in the Medical Office
 The Federation of State Medical Boards 2013 Model Guidelines for Opioid Addiction Treatment in the Medical Office Adopted April 2013 for Consideration by State Medical Boards 2002 FSMB Model Guidelines
The Federation of State Medical Boards 2013 Model Guidelines for Opioid Addiction Treatment in the Medical Office Adopted April 2013 for Consideration by State Medical Boards 2002 FSMB Model Guidelines
The National Community Detoxification Pilot
 The National Community Detoxification Pilot Aoife Dermody, Progression Routes Initiative NDCI, 2011 Community Detoxification Protocols Guidelines for outpatient detoxification from methadone or benzodiazepines
The National Community Detoxification Pilot Aoife Dermody, Progression Routes Initiative NDCI, 2011 Community Detoxification Protocols Guidelines for outpatient detoxification from methadone or benzodiazepines
Statistics from the National Drug Treatment Monitoring System (NDTMS) Statistics relating to young people England, 1 April 2010 31 March 2011
 Statistics from the National Drug Treatment Monitoring System (NDTMS) Statistics relating to young people England, 1 April 2010 31 March 2011 8 December 2011 Executive Summary 21,955 young people accessed
Statistics from the National Drug Treatment Monitoring System (NDTMS) Statistics relating to young people England, 1 April 2010 31 March 2011 8 December 2011 Executive Summary 21,955 young people accessed
Resources for the Prevention and Treatment of Substance Use Disorders
 Resources for the Prevention and Treatment of Substance Use Disorders Table of Contents Age-standardized DALYs, alcohol and drug use disorders, per 100 000 Age-standardized death rates, alcohol and drug
Resources for the Prevention and Treatment of Substance Use Disorders Table of Contents Age-standardized DALYs, alcohol and drug use disorders, per 100 000 Age-standardized death rates, alcohol and drug
Guidelines for the Prescribing, Supply and Administration of Methadone and Buprenorphine on Transfer of Care
 Hull & East Riding Prescribing Committee Guidelines for the Prescribing, Supply and Administration of Methadone and Buprenorphine on Transfer of Care 1. BACKGROUND Patients who are physically dependent
Hull & East Riding Prescribing Committee Guidelines for the Prescribing, Supply and Administration of Methadone and Buprenorphine on Transfer of Care 1. BACKGROUND Patients who are physically dependent
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SPECIAL HEALTH AUTHORITY TENTH WAVE WORK PROGRAMME DRUG MISUSE. Psychosocial interventions in drug misuse
 Attachment B NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SPECIAL HEALTH AUTHORITY TENTH WAVE WORK PROGRAMME DRUG MISUSE Psychosocial interventions in drug misuse On 16 th June 2004 the Department of Health
Attachment B NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SPECIAL HEALTH AUTHORITY TENTH WAVE WORK PROGRAMME DRUG MISUSE Psychosocial interventions in drug misuse On 16 th June 2004 the Department of Health
Adult drug treatment plan 2009/10. Part 1: Strategic summary, needs assessment and key priorities
 Birmingham Drug and Alcohol Action Team Adult drug treatment plan 2009/10 Part 1: Strategic summary, needs assessment and key priorities The strategic summary incorporating the findings of the needs assessment,
Birmingham Drug and Alcohol Action Team Adult drug treatment plan 2009/10 Part 1: Strategic summary, needs assessment and key priorities The strategic summary incorporating the findings of the needs assessment,
Evaluating OST programmes MMT and drug treatment in the Maldives
 Evaluating OST programmes MMT and drug treatment in the Maldives Prof Gerry Stimson Based on A PROCESS AND SYSTEMS EVALUATION OF THE DRUG TREATMENT AND REHABILITATION SERVICES IN THE MALDIVES. Gordon Mortimore
Evaluating OST programmes MMT and drug treatment in the Maldives Prof Gerry Stimson Based on A PROCESS AND SYSTEMS EVALUATION OF THE DRUG TREATMENT AND REHABILITATION SERVICES IN THE MALDIVES. Gordon Mortimore
Treatments for drug misuse
 Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Understanding NICE guidance Information for people who use NHS services Treatments for drug misuse NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and
Opioid Addiction & Corrections
 Opioid Addiction & Corrections Medication Assisted Treatment in the Connecticut Department of Correction April 30, 2015--CJPAC Kathleen F. Maurer, MD, MPH, MBA Medical Director and Director of Health and
Opioid Addiction & Corrections Medication Assisted Treatment in the Connecticut Department of Correction April 30, 2015--CJPAC Kathleen F. Maurer, MD, MPH, MBA Medical Director and Director of Health and
Addressing Alcohol and Drugs in the Community. Cabinet member: Cllr Keith Humphries - Public Health and Protection Services
 Wiltshire Council Cabinet 17 April 2012 Subject: Addressing Alcohol and Drugs in the Community Cabinet member: Cllr Keith Humphries - Public Health and Protection Services Key Decision: Yes Executive Summary
Wiltshire Council Cabinet 17 April 2012 Subject: Addressing Alcohol and Drugs in the Community Cabinet member: Cllr Keith Humphries - Public Health and Protection Services Key Decision: Yes Executive Summary
Criminal Justice Integrated Drug Teams and treatment interventions. Clinical guidance to maximise access to drug treatment
 Criminal Justice Integrated Drug Teams and treatment interventions Clinical guidance to maximise access to drug treatment November 2003 NTA Clinical Guidance to CJIP Teams Nov O3 Page 1 of 17 1. Introduction
Criminal Justice Integrated Drug Teams and treatment interventions Clinical guidance to maximise access to drug treatment November 2003 NTA Clinical Guidance to CJIP Teams Nov O3 Page 1 of 17 1. Introduction
How To Treat Anorexic Addiction With Medication Assisted Treatment
 Medication Assisted Treatment for Opioid Addiction Tanya Hiser, MS, LPC Premier Care of Wisconsin, LLC October 21, 2015 How Did We Get Here? Civil War veterans and women 19th Century physicians cautious
Medication Assisted Treatment for Opioid Addiction Tanya Hiser, MS, LPC Premier Care of Wisconsin, LLC October 21, 2015 How Did We Get Here? Civil War veterans and women 19th Century physicians cautious
Neurobiology and Treatment of Opioid Dependence. Nebraska MAT Training September 29, 2011
 Neurobiology and Treatment of Opioid Dependence Nebraska MAT Training September 29, 2011 Top 5 primary illegal drugs for persons age 18 29 entering treatment, % 30 25 20 15 10 Heroin or Prescription Opioids
Neurobiology and Treatment of Opioid Dependence Nebraska MAT Training September 29, 2011 Top 5 primary illegal drugs for persons age 18 29 entering treatment, % 30 25 20 15 10 Heroin or Prescription Opioids
Research Note RN 00/91 1 November 2000 DRUG COURTS
 Research Note RN 00/91 1 November 2000 DRUG COURTS There will be a Scottish National Party debate on Drug Courts on Thursday 2 November 2000. This brief research note gives information on the background
Research Note RN 00/91 1 November 2000 DRUG COURTS There will be a Scottish National Party debate on Drug Courts on Thursday 2 November 2000. This brief research note gives information on the background
DRUG AND ALCOHOL DETOXIFICATION: A GUIDE TO OUR SERVICES
 01736 850006 www.bosencefarm.co.uk DRUG AND ALCOHOL DETOXIFICATION: A GUIDE TO OUR SERVICES An environment for change Boswyns provides medically-led drug and alcohol assessment, detoxification and stabilisation.
01736 850006 www.bosencefarm.co.uk DRUG AND ALCOHOL DETOXIFICATION: A GUIDE TO OUR SERVICES An environment for change Boswyns provides medically-led drug and alcohol assessment, detoxification and stabilisation.
Adult drug treatment plan 2007/08 Part 1 Section A: Strategic summary Section B: National targets Section C: Partnership performance expectations
 name Adult drug treatment plan Part 1 Section A: Strategic summary Section B: National targets Section C: expectations Published by NTA: 2 October This strategic summary incorporating national targets
name Adult drug treatment plan Part 1 Section A: Strategic summary Section B: National targets Section C: expectations Published by NTA: 2 October This strategic summary incorporating national targets
REVIEW OF DRUG TREATMENT AND REHABILITATION SERVICES: SUMMARY AND ACTIONS
 REVIEW OF DRUG TREATMENT AND REHABILITATION SERVICES: SUMMARY AND ACTIONS 1. INTRODUCTION 1.1 Review Process A Partnership for a Better Scotland committed the Scottish Executive to reviewing and investing
REVIEW OF DRUG TREATMENT AND REHABILITATION SERVICES: SUMMARY AND ACTIONS 1. INTRODUCTION 1.1 Review Process A Partnership for a Better Scotland committed the Scottish Executive to reviewing and investing
The Government propose to take a zero tolerance approach to the following 8 controlled drugs which are known to impair driving:
 Drug-Driving: Proposed New Law New law on drug driving to be introduced in the near future The new law on drug driving is designed, in part, to reduce the number of failed prosecutions under the existing
Drug-Driving: Proposed New Law New law on drug driving to be introduced in the near future The new law on drug driving is designed, in part, to reduce the number of failed prosecutions under the existing
Treatment System 101
 Treatment System 101 A brief overview for courtroom decision-makers and people working in criminal justice sectors March 11, 2015 West Toronto Human Services & Justice Coordinating Cttee. Agenda Introduction
Treatment System 101 A brief overview for courtroom decision-makers and people working in criminal justice sectors March 11, 2015 West Toronto Human Services & Justice Coordinating Cttee. Agenda Introduction
THE DRUG DETOX UNIT AT MOUNTJOY PRISON A REVIEW
 1 THE DRUG DETOX UNIT AT MOUNTJOY PRISON A REVIEW By Dr. Des Crowley, General Practitioner INTRODUCTION The Drug Detox Unit was opened in July 1996 at Mountjoy Prison in response to the escalating drug
1 THE DRUG DETOX UNIT AT MOUNTJOY PRISON A REVIEW By Dr. Des Crowley, General Practitioner INTRODUCTION The Drug Detox Unit was opened in July 1996 at Mountjoy Prison in response to the escalating drug
Substance misuse among young people in England 2012-13
 Substance misuse among young people in England December 2013 About Public Health England Public Health England s mission is to protect and improve the nation s health and to address inequalities through
Substance misuse among young people in England December 2013 About Public Health England Public Health England s mission is to protect and improve the nation s health and to address inequalities through
EPIDEMIOLOGY OF OPIATE USE
 Opiate Dependence EPIDEMIOLOGY OF OPIATE USE Difficult to estimate true extent of opiate dependence Based on National Survey of Health and Mental Well Being: 1.2% sample used opiates in last 12 months
Opiate Dependence EPIDEMIOLOGY OF OPIATE USE Difficult to estimate true extent of opiate dependence Based on National Survey of Health and Mental Well Being: 1.2% sample used opiates in last 12 months
Directory for Substance Misuse Services in Caerphilly
 Directory for Substance Misuse s in Caerphilly Background Substance Misuse services use a tiered approach in their approach and delivering of drug/alcohol services. These are as follows: Tier 1 Interventions
Directory for Substance Misuse s in Caerphilly Background Substance Misuse services use a tiered approach in their approach and delivering of drug/alcohol services. These are as follows: Tier 1 Interventions
Why invest? How drug treatment and recovery services work for individuals, communities and society
 Why invest? How drug treatment and recovery services work for individuals, communities and society What is drug addiction? Drug addiction is a complex but treatable condition Those affected use drugs compulsively,
Why invest? How drug treatment and recovery services work for individuals, communities and society What is drug addiction? Drug addiction is a complex but treatable condition Those affected use drugs compulsively,
Substance Misuse. See the Data Factsheets for more data and analysis: http://www.rbkc.gov.uk/voluntaryandpartnerships/jsna/2010datafactsheets.
 Substance Misuse See the Data Factsheets for more data and analysis: http://www.rbkc.gov.uk/voluntaryandpartnerships/jsna/2010datafactsheets.aspx Problematic drug use Kensington and Chelsea has a similar
Substance Misuse See the Data Factsheets for more data and analysis: http://www.rbkc.gov.uk/voluntaryandpartnerships/jsna/2010datafactsheets.aspx Problematic drug use Kensington and Chelsea has a similar
Specialist Alcohol & Drug Services in Lanarkshire
 Specialist Alcohol & Drug Services in Lanarkshire This brochure describes what help is available within Lanarkshire s specialist treatment services. These include the North Lanarkshire Integrated Addiction
Specialist Alcohol & Drug Services in Lanarkshire This brochure describes what help is available within Lanarkshire s specialist treatment services. These include the North Lanarkshire Integrated Addiction
Trends in deaths related to drug misuse in England and Wales, 1993 2004
 Trends in deaths related to drug misuse in, 1993 24 Oliver Morgan, Office for National Statistics and Imperial College London, Clare Griffiths, Barbara Toson and Cleo Rooney, Office for, Azeem Majeed,
Trends in deaths related to drug misuse in, 1993 24 Oliver Morgan, Office for National Statistics and Imperial College London, Clare Griffiths, Barbara Toson and Cleo Rooney, Office for, Azeem Majeed,
TRENDS IN HEROIN USE IN THE UNITED STATES: 2002 TO 2013
 2013 to 2002 States: United the in Use Heroin in Trends National Survey on Drug Use and Health Short Report April 23, 2015 TRENDS IN HEROIN USE IN THE UNITED STATES: 2002 TO 2013 AUTHORS Rachel N. Lipari,
2013 to 2002 States: United the in Use Heroin in Trends National Survey on Drug Use and Health Short Report April 23, 2015 TRENDS IN HEROIN USE IN THE UNITED STATES: 2002 TO 2013 AUTHORS Rachel N. Lipari,
Drug and Alcohol Agency Action Plan 2010 2014
 Drug and Alcohol Agency Action Plan 2010 2014 Making a positive difference. CONTENTS INTRODUCTION...3 OBJECTIVES...4 STRATEGY 1: FOCUSING ON PREVENTION...5 STRATEGY 2: INTERVENING BEFORE PROBLEMS BECOME
Drug and Alcohol Agency Action Plan 2010 2014 Making a positive difference. CONTENTS INTRODUCTION...3 OBJECTIVES...4 STRATEGY 1: FOCUSING ON PREVENTION...5 STRATEGY 2: INTERVENING BEFORE PROBLEMS BECOME
Phoenix Futures Prison Treatment programmes
 Phoenix Futures Prison Treatment programmes Karen Biggs Chief Executive, Phoenix Futures Overview of Presentation Political and Strategic context in England Overview of some of our programmes. Outcomes
Phoenix Futures Prison Treatment programmes Karen Biggs Chief Executive, Phoenix Futures Overview of Presentation Political and Strategic context in England Overview of some of our programmes. Outcomes
The National Study of Psychiatric Morbidity in New Zealand Prisons Questions and Answers
 The National Study of Psychiatric Morbidity in New Zealand Prisons Questions and Answers How have prisons dealt with mental illness in the past? Regional forensic psychiatric services were established
The National Study of Psychiatric Morbidity in New Zealand Prisons Questions and Answers How have prisons dealt with mental illness in the past? Regional forensic psychiatric services were established
DEVELOPING MANUFACTURING SUPPLYING. Naltrexone Implants. Manufactured by NalPharm Ltd WWW.NALPHARM.COM
 DEVELOPING MANUFACTURING SUPPLYING Naltrexone Implants Background to Nalpharm NalPharm is a specialist pharmaceutical company supplying proprietary branded medications and generic drugs in the area of
DEVELOPING MANUFACTURING SUPPLYING Naltrexone Implants Background to Nalpharm NalPharm is a specialist pharmaceutical company supplying proprietary branded medications and generic drugs in the area of
SUMMARY INFORMATION ON PROBATION IN ENGLAND AND WALES
 SUMMARY INFORMATION ON PROBATION IN ENGLAND AND WALES General Information Number of inhabitants: 54.98 million at December 2009. 1 Prison population rate per 100,000 inhabitants: 153. Link to Probation
SUMMARY INFORMATION ON PROBATION IN ENGLAND AND WALES General Information Number of inhabitants: 54.98 million at December 2009. 1 Prison population rate per 100,000 inhabitants: 153. Link to Probation
IN THE GENERAL ASSEMBLY STATE OF. Ensuring Access to Medication Assisted Treatment Act
 IN THE GENERAL ASSEMBLY STATE OF Ensuring Access to Medication Assisted Treatment Act 1 Be it enacted by the People of the State of Assembly:, represented in the General 1 1 1 1 Section 1. Title. This
IN THE GENERAL ASSEMBLY STATE OF Ensuring Access to Medication Assisted Treatment Act 1 Be it enacted by the People of the State of Assembly:, represented in the General 1 1 1 1 Section 1. Title. This
THE STORY OF DRUG TREATMENT
 THE STORY OF DRUG TREATMENT EFFECTIVE TREATMENT CHANGING LIVES The story of drug treatment The goal of all treatment is for drug users to achieve abstinence from their drug or drugs of dependency. For
THE STORY OF DRUG TREATMENT EFFECTIVE TREATMENT CHANGING LIVES The story of drug treatment The goal of all treatment is for drug users to achieve abstinence from their drug or drugs of dependency. For
THE BASICS. Community Based Medically Assisted Alcohol Withdrawal. World Health Organisation 2011. The Issues 5/18/2011. RCGP Conference May 2011
 RCGP Conference May 2011 Community Based Medically Assisted Alcohol Withdrawal THE BASICS An option for consideration World Health Organisation 2011 Alcohol is the world s third largest risk factor for
RCGP Conference May 2011 Community Based Medically Assisted Alcohol Withdrawal THE BASICS An option for consideration World Health Organisation 2011 Alcohol is the world s third largest risk factor for
Simon Community Northern Ireland welcomes the opportunity to respond to the Alcohol and Drug Commissioning Framework for Northern Ireland 2013-2016
 Simon Community Northern Ireland welcomes the opportunity to respond to the Alcohol and Drug Commissioning Framework for Northern Ireland 2013-2016 About the Simon Community Simon Community Northern Ireland
Simon Community Northern Ireland welcomes the opportunity to respond to the Alcohol and Drug Commissioning Framework for Northern Ireland 2013-2016 About the Simon Community Simon Community Northern Ireland
TITLE: REVIEW OF DRUG USE IN HARLOW (PART 2 OF 2) LYNN SEWARD, HEAD OF COMMUNITY WELLBEING (01279) 446119 TEAM MANAGER (01279) 446115
 REPORT TO: SCRUTINY COMMITTEE DATE: 22JANUARY 2014 TITLE: REVIEW OF DRUG USE IN (PART 2 OF 2) LEAD OFFICER: CONTRIBUTING OFFICER: LYNN SEWARD, HEAD OF COMMUNITY WELLBEING (01279) 446119 MARYSIA RUDGLEY,
REPORT TO: SCRUTINY COMMITTEE DATE: 22JANUARY 2014 TITLE: REVIEW OF DRUG USE IN (PART 2 OF 2) LEAD OFFICER: CONTRIBUTING OFFICER: LYNN SEWARD, HEAD OF COMMUNITY WELLBEING (01279) 446119 MARYSIA RUDGLEY,
ABOUT THE COMMUNITY PAYBACK ORDER
 ABOUT THE COMMUNITY PAYBACK ORDER Introduction 1. The Criminal Justice and Licensing (Scotland) Act 2010 (the 2010 Act) is the largest piece of legislation introduced into the Scottish Parliament by the
ABOUT THE COMMUNITY PAYBACK ORDER Introduction 1. The Criminal Justice and Licensing (Scotland) Act 2010 (the 2010 Act) is the largest piece of legislation introduced into the Scottish Parliament by the
Women in the penal system
 All Party Parliamentary Group on Women in the Penal System Chaired by Baroness Corston Women in the penal system Second report on women with particular vulnerabilities in the criminal justice system Women
All Party Parliamentary Group on Women in the Penal System Chaired by Baroness Corston Women in the penal system Second report on women with particular vulnerabilities in the criminal justice system Women
(Health Scrutiny Sub-Committee 9 March 2009)
 Somerset County Council Health Scrutiny Sub-Committee 9 March 2009 Drug and Alcohol Treatment Services Author: Amanda Payne Somerset DAAT Co-ordinator Contact Details: [email protected] Paper
Somerset County Council Health Scrutiny Sub-Committee 9 March 2009 Drug and Alcohol Treatment Services Author: Amanda Payne Somerset DAAT Co-ordinator Contact Details: [email protected] Paper
Adviceguide Advice that makes a difference
 Health in prison Getting medical treatment in prison If you re in prison, you should get the same health services as you'd get from the NHS. This includes mental health services. Qualified doctors, dentists,
Health in prison Getting medical treatment in prison If you re in prison, you should get the same health services as you'd get from the NHS. This includes mental health services. Qualified doctors, dentists,
10.7 Undertake the substance testing of parents
 10.7 Undertake the substance testing of parents Purpose This procedure outlines the process for facilitating the substance testing of parents in cases where there are indicators that parents are engaging
10.7 Undertake the substance testing of parents Purpose This procedure outlines the process for facilitating the substance testing of parents in cases where there are indicators that parents are engaging
Rapid Access Protocol Bradford and Airedale Drug Services
 Rapid Access Protocol Bradford and Airedale Drug Services Responsible Head Of Service: Name of responsible committee: Name of Author: Contact for further details: Simon Long Professional Advisory Sub Committee
Rapid Access Protocol Bradford and Airedale Drug Services Responsible Head Of Service: Name of responsible committee: Name of Author: Contact for further details: Simon Long Professional Advisory Sub Committee
HOSC Report Integrated community drugs and alcohol service retendering options beyond April 2016
 HOSC Report Integrated community drugs and alcohol service retendering options beyond April 2016 Meeting Date Sponsor Report author Purpose of report (summary) 12 th May 2015 Margaret Willcox Steve O Neill
HOSC Report Integrated community drugs and alcohol service retendering options beyond April 2016 Meeting Date Sponsor Report author Purpose of report (summary) 12 th May 2015 Margaret Willcox Steve O Neill
Patient Group Directions. Guidance and information for nurses
 Patient Group Directions Guidance and information for nurses Patient Group Directions Guidance and information for nurses Contents Introduction 4 What is a patient group direction (PGD)? 4 When can PGDs
Patient Group Directions Guidance and information for nurses Patient Group Directions Guidance and information for nurses Contents Introduction 4 What is a patient group direction (PGD)? 4 When can PGDs
Milton Keynes Drug and Alcohol Strategy 2014-17
 Health and Wellbeing Board Milton Keynes Drug and Alcohol Strategy 2014-17 www.milton-keynes.gov.uk 2 Contents Foreword 4 Introduction 5 National context 6 Local context 7 Values and principles 9 Priorities
Health and Wellbeing Board Milton Keynes Drug and Alcohol Strategy 2014-17 www.milton-keynes.gov.uk 2 Contents Foreword 4 Introduction 5 National context 6 Local context 7 Values and principles 9 Priorities
Fairfax-Falls Church Community Services Board
 LOB #267: ADULT RESIDENTIAL TREATMENT SERVICES Purpose Adult Residential Treatment Services provides residential treatment programs for adults with severe substance use disorders and/or co occurring mental
LOB #267: ADULT RESIDENTIAL TREATMENT SERVICES Purpose Adult Residential Treatment Services provides residential treatment programs for adults with severe substance use disorders and/or co occurring mental
GP-led services for alcohol misuse: the Fresh Start Clinic
 London Journal of Primary Care 2011;4:11 15 # 2011 Royal College of General Practitioners GP Commissioning GP-led services for alcohol misuse: the Fresh Start Clinic Johannes Coetzee GP Principle, Bridge
London Journal of Primary Care 2011;4:11 15 # 2011 Royal College of General Practitioners GP Commissioning GP-led services for alcohol misuse: the Fresh Start Clinic Johannes Coetzee GP Principle, Bridge
Substance Misuse Treatment Framework (SMTF) Guidance for the Provision of Evidence Based Tier 4 Services in the Treatment of Substance Misuse
 Substance Misuse Treatment Framework (SMTF) Guidance for the Provision of Evidence Based Tier 4 Services in the Treatment of Substance Misuse ISBN 978 0 7504 6273 0 Crown copyright 2011 WG-12567 F9161011
Substance Misuse Treatment Framework (SMTF) Guidance for the Provision of Evidence Based Tier 4 Services in the Treatment of Substance Misuse ISBN 978 0 7504 6273 0 Crown copyright 2011 WG-12567 F9161011
TESTIMONY. March 17, 2014. Rutland, VT
 Community Solutions to Breaking the Cycle of Heroin & Opioid Addiction TESTIMONY Harry Chen, MD, Commissioner of Health March 17, 2014 Senate Committee on the Judiciary Franklin Conference Center at the
Community Solutions to Breaking the Cycle of Heroin & Opioid Addiction TESTIMONY Harry Chen, MD, Commissioner of Health March 17, 2014 Senate Committee on the Judiciary Franklin Conference Center at the
Brighton and Hove Dual Diagnosis Needs Assessment 2012 1
 Brighton and Hove Dual Diagnosis Needs Assessment 2012 1 Brighton and Hove Dual Diagnosis Needs Assessment 2012 2 Contents RECOMMENDATIONS 6 EXECUTIVE SUMMARY 10 1. INTRODUCTION 16 1.1 Scope and definition
Brighton and Hove Dual Diagnosis Needs Assessment 2012 1 Brighton and Hove Dual Diagnosis Needs Assessment 2012 2 Contents RECOMMENDATIONS 6 EXECUTIVE SUMMARY 10 1. INTRODUCTION 16 1.1 Scope and definition
LONG-TERM TREATMENT OUTCOME: WHAT ARE THE 11 YEAR OUTCOMES OF TREATMENT FOR HEROIN DEPENDENCE?
 AUSTRALIAN T R E A T M E N T OU T C O M E STUDY - N S W Funded by the National Health and Medical Research Council and the Australian Government Department of Health. ATOS NSW is a project of the Centre
AUSTRALIAN T R E A T M E N T OU T C O M E STUDY - N S W Funded by the National Health and Medical Research Council and the Australian Government Department of Health. ATOS NSW is a project of the Centre
Testimony of The New York City Department of Health and Mental Hygiene. before the
 Testimony of The New York City Department of Health and Mental Hygiene before the New York City State Assembly Committee on Alcoholism and Drug Abuse on Programs and Services for the Treatment of Opioid
Testimony of The New York City Department of Health and Mental Hygiene before the New York City State Assembly Committee on Alcoholism and Drug Abuse on Programs and Services for the Treatment of Opioid
The Recovery Pathway Service forms a key component of the Sunderland Integrated Substance Misuse Service, as illustrated below:
 SERVICE SPECIFICATION LOT 1 RECOVERY PATHWAY 1.0 SERVICE MODEL The Recovery Pathway Service forms a key component of the Sunderland Integrated Substance Misuse Service, as illustrated below: Recovery Outcomes
SERVICE SPECIFICATION LOT 1 RECOVERY PATHWAY 1.0 SERVICE MODEL The Recovery Pathway Service forms a key component of the Sunderland Integrated Substance Misuse Service, as illustrated below: Recovery Outcomes
National Assembly for Wales: Health and Social Care Committee
 2 Ashtree Court, Woodsy Close Cardiff Gate Business Park Cardiff CF23 8RW Tel: 029 2073 0310 [email protected] www.rpharms.com 18 th October 2011 Submission to: Call for Evidence: Response from: National
2 Ashtree Court, Woodsy Close Cardiff Gate Business Park Cardiff CF23 8RW Tel: 029 2073 0310 [email protected] www.rpharms.com 18 th October 2011 Submission to: Call for Evidence: Response from: National
Minimum Insurance Benefits for Patients with Opioid Use Disorder The Opioid Use Disorder Epidemic: The Evidence for Opioid Treatment:
 Minimum Insurance Benefits for Patients with Opioid Use Disorder By David Kan, MD and Tauheed Zaman, MD Adopted by the California Society of Addiction Medicine Committee on Opioids and the California Society
Minimum Insurance Benefits for Patients with Opioid Use Disorder By David Kan, MD and Tauheed Zaman, MD Adopted by the California Society of Addiction Medicine Committee on Opioids and the California Society
WHAT WE KNOW. Collective Action Issue Brief #2 Updated June 2014 PRESCRIPTION PAIN MEDICATION MISUSE
 Collective Action Issue Brief #2 Updated June 2014 PRESCRIPTION PAIN MEDICATION MISUSE WHAT WE KNOW The misuse and abuse of prescription drugs has become a leading cause of harm among New Hampshire adults,
Collective Action Issue Brief #2 Updated June 2014 PRESCRIPTION PAIN MEDICATION MISUSE WHAT WE KNOW The misuse and abuse of prescription drugs has become a leading cause of harm among New Hampshire adults,
