Erectile Function, Incontinence, and Other Quality of Life Outcomes Following Proton Therapy for Prostate Cancer in Men 60 Years Old and Younger
|
|
|
- Janice Patrick
- 8 years ago
- Views:
Transcription
1 Erectile Function, Incontinence, and Other Quality of Life Outcomes Following Proton Therapy for Prostate Cancer in Men 60 Years Old and Younger Bradford S. Hoppe, MD, MPH 1 ; Romaine C. Nichols, MD 1 ; Randal H. Henderson, MD, MBA 1 ; Christopher G. Morris, MS 1 ; Christopher R. Williams, MD 2 ; Joseph Costa, DO 2 ; Robert B. Marcus, Jr, MD 1 ; William M. Mendenhall, MD 1 ; Zuofeng Li, PhD 1 ; and Nancy P. Mendenhall, MD 1 BACKGROUND: This study sought to evaluate patient-reported health-related quality of life following proton therapy for prostate cancer in men 60 years old. METHODS: Between August 2006 and January 2010, 262 hormone-naive men 60 years old were treated with definitive proton therapy for prostate cancer. Before treatment and every 6 months after treatment, patients filled out the Expanded Prostate Index Composite (EPIC) and the International Index of Erectile Function (IIEF) questionnaires. Potency was defined as successful sexual intercourse in the prior month or an EPIC sexual summary (SS) score 60. RESULTS: Median follow-up was 24 months; 90% of men completed follow-up EPIC forms within the last year. For EPIC urinary, bowel, and hormone subscales, the average decline from baseline to 2 years was 5 points, except for bowel function (5.2 points). SS scores declined 12.6 points after 2 years. Potency rates declined by 11% from baseline at 2 years, but 94% of men were potent with a baseline IIEF > 21, body mass index < 30, and no history of diabetes. At 2 years after treatment, only 1.8% of men required a pad for urge incontinence. On multivariate analysis, factors associated with a significant decline in SS score were mean penile bulb dose 40 cobalt Gy equivalents (P ¼.012) and radiation dose 80 cobalt Gy equivalents (P ¼.017); only diabetes was significantly associated with impotence (P ¼.015). CONCLUSIONS: Young men undergoing proton therapy for treatment of prostate cancer have excellent outcomes with respect to erectile dysfunction, urinary incontinence, and other health-related quality of life parameters during the first 2 years after treatment. Longer follow-up is needed to confirm these findings. Cancer 2012;000: VC 2012 American Cancer Society. KEYWORDS: prostate cancer, proton therapy, radiation therapy, outcomes, toxicity. Erectile dysfunction (ED) is a critical health-related quality of life (HRQoL) outcome in men treated for prostate cancer and has been associated with depression and significant distress. 1,2 Many effective treatment options are available to men with prostate cancer, including surgery, external-beam radiotherapy (EBRT), and brachytherapy, and some men select treatment based on perceived side effect profiles, frequently focusing on urinary incontinence and ED. Several studies have investigated and compared HRQoL factors following various treatments for prostate cancer. 3-6 These studies have consistently found a more significant decline in ED following surgery than after EBRT. The median age of patients receiving surgery is typically significantly lower than that of patients who receive EBRT; in addition, the EBRT population also includes less healthy men who are not candidates for surgery. 3,6 Thus, reported ED outcomes following EBRT are generally based on an older, less healthy cohort with lower baseline sexual function and may not reflect outcomes attainable with EBRT in a younger, healthier population of patients with prostate cancer. Proton therapy (PT) is a highly conformal radiotherapy modality that delivers much less radiation dose to nontargeted normal tissues, such as the bladder and rectum, than conventional radiation therapy. Moreover, comparative dosimetry studies have documented lower doses to nontargeted tissues with PT compared with intensity-modulated radiotherapy, 7 providing a rationale for the very low rates of genitourinary and rectal toxicity that have been observed in clinical studies 8 and the expectation of a lower rate of second malignancy in younger men with prostate cancer Although patient-reported ED and urinary incontinence following PT have been studied, 11,12 none have investigated outcomes using the more commonly used Expanded Prostate Cancer Index Composite (EPIC) questionnaire, which can easily be compared with outcomes after other prostate cancer treatments. Furthermore, no study has evaluated Corresponding author: Bradford S. Hoppe, MD, MPH, University of Florida Proton Therapy Institute, 2015 North Jefferson Street, Jacksonville, FL 32206; Fax: (904) ; bhoppe@floridaproton.org 1 University of Florida Proton Therapy Institute, Jacksonville, Florida; 2 University of Florida Department of Surgery, Jacksonville, Florida We thank Jessica Kirwan and the editorial staff at the University of Florida Department of Radiation Oncology for editorial support. Presented at the American Society for Radiation Oncology (ASTRO) 53rd Annual Meeting; October 2-6, 2011; Miami Beach, FL. DOI: /cncr.27398, Received: September 16, 2011; Revised: October 20, 2011; Accepted: November 16, 2011, Published online in Wiley Online Library (wileyonlinelibrary.com) Cancer Month 00,
2 ED in a cohort of young men treated with EBRT, where interactions from medical comorbidities are less likely to influence ED outcomes and for whom baseline sexual function would be similar to typical surgical patients. This study investigates patient-reported HRQoL outcomes (with an emphasis on sexual outcomes) through use of the EPIC questionnaire in a young cohort of patients (60 years old) who received definitive treatment with PT alone. MATERIALS AND METHODS Patients This study was approved by the University of Florida Institutional Review Board (IRB) and included men aged 60 years or less who were treated with definitive PT alone for prostate cancer. These men were all treated on an IRBapproved outcome tracking protocol and may also have been enrolled on 1 of 3 IRB-approved treatment protocols open between August 2006 and January Patients were excluded if they received hormone therapy (n ¼ 28) or had less than 6 months of follow-up (n ¼ 7). In total, 262 patients were included in the study. HRQoL parameters were captured prospectively before the start of definitive treatment, every 6 months for the first year, and then every 6 to 12 months annually following treatment, using the 50-item EPIC questionnaire, 13 the 5-item International Index of Erectile Function (IIEF), and the International Prostate Symptom Score. If a patient was unable to return for follow-up to fill out the questionnaire, the questionnaire was mailed to the patient or the patient filled out the questionnaire through a secure online medical records portal. For the purposes of this study, if a patient did not have 12-month follow-up, his 18-month HRQoL was used instead for assessment at 1 year. If a patient did not have 24-month follow-up, his 30-month or 36-month HRQoL was used. The EPIC summaryandsubscaleswerethencalculatedandreportedusing a scale of 0 to 100, with higher scores indicating better outcomes. IIEF scores were calculated and reported by a scale of 5 to 25, with higher scores indicating better outcomes. For the purposes of this study, a strict definition of potency was defined as having successfully engaged in sexual intercourse at least once in the past month or an EPIC sexual summary score of Patient baseline characteristics and medical comorbidities that could impact ED were extracted from the patient s initial history at consultation. Simulation, Planning, and Treatment The University of Florida Proton Therapy Institute simulation, planning, and treatment guidelines for prostate cancer have previously been published. 15 In brief, after having 3 to 4 visicoil fiducial markers placed within the prostate by transrectal ultrasound guidance, patients were simulated on a Philips Brilliance computed tomography (CT) big-bore simulator (Philips Healthcare, Andover, Mass). Thirty minutes before simulation, patients voided, then drank 420 cm 3 (15 ounces) of water. Patient position was secured with a vacuum-locked body mold. Supine positioning was typically used. Saline ( ml) was instilled into the rectum or a rectal balloon was used to stabilize the prostate position. Immediately after CT simulation, a magnetic resonance imaging (MRI) scan was obtained on a Philips Panorama 0.23T open-mri system. The CT and MRI images were fused using the Philips Pinnacle AcQSim3 virtual simulation workstation, and imported into the Varian Eclipse treatment planning system (Varian Medical Systems, Palo Alto, Calif). Prostate and seminal vesicle targets along with the penile bulb were contoured by the treating physicians. Normal tissues, including the bladder, rectum, bowel, and femoral heads, were manually contoured by dosimetrists and confirmed by the treating physician. A planning target volume (PTV) was constructed from the prostate and/or seminal vesicles with margins of 4 mm in the antero-posterior and lateral directions, and 6 mm in the superior-inferior direction. Dosimetric specifications required that 95% of the PTV receive 100% of the prescribed dose and 100% of the PTV receive at least 95% of the prescribed dose. Patients were treated with double-scatter PT with right and left lateral (or slightly oblique) field arrangements with customized brass apertures and compensators. Image-guided treatment was performed by using orthogonal kilovolt imaging for fiducial localization. Depending on protocol, patients were treated either with 2 cobalt Gy equivalents (CGE) per fraction to a total dose of CGE or at 2.5 CGE per fraction to a total dose of CGE. Statistics SAS and JMP software were used for all statistical computation (SAS Institute, Cary, NC). A repeated-measures analysis of variance was used to determine whether there was a statistically significant average increase or decrease in EPIC scores between baseline and 24 months after treatment. A likelihood ratio chi-squared test provided the same repeated measures assessment of potency frequencies between baseline and 24 months after treatment. The nonparametric version of the chi-squared test (Fisher exact test) was used for the analysis of the categorical endpoints of potency and 2 dichotomized versions of delta 2 Cancer Month 00, 2012
3 Proton Therapy for Young Prostate Cancer Patients/Hoppe et al change from baseline EPIC sexual summary score. The 2 dichotomized EPIC sexual summary scores were accomplished by comparing each patient s last available sexual summary score to values equivalent to 0.5 standard deviation (considered clinically relevant in other HRQoL studies) 16,17 and 1 standard deviation lower than the baseline sexual summary mean. The last available follow-up was also used to determine potency. RESULTS The median follow-up for the entire cohort was 24 months (range, 6-53 months). Thus far, only one patient has developed a biochemical recurrence; he had high-risk prostate cancer (stage ct3a, Gleason score of 8, and pretreatment prostate-specific antigen level of 33) and refused hormone therapy as part of definitive treatment. A separate patient died from an asthma attack 9 months after treatment. A total of 90% of patients contributed follow-up within 1 year of analysis. The proportion of responses at baseline, 6 months, 1 year, and 2 years for the EPIC questionnaire were available for 97%, 96%, 91%, and 87% of patients, respectively. Patient-, disease-, and treatment-specific details for the patient cohort are summarized in Table 1. The median age was 56 years (range, years) and 87% were caucasian. The median height, weight, and body mass index (BMI) were 180 cm (range, cm), 87.7 kg (range, kg), and 27.7 kg/m 2 (range, kg/m 2 ), respectively. At baseline, 41 men (16%) admitted to using phosphodiesterase-5 inhibitor. Mean EPIC scores with standard deviations over the first 2 years and at last follow-up are listed by subscale in Table 2. For urinary, bowel, and hormone categories, the average absolute reduction from baseline to 2 years was 5 points, except for bowel function (5.2 points). Urinary subscores did not substantially change. Urinary incontinence scores only declined from 95.8 at baseline to 92.2 at 2 years. In response to the specific urinary incontinence questions from the EPIC at 2 years, 1.8% of men used a pad to manage urge incontinence. The sexual summary, sexual function, and sexual bother scores reported over time are presented in Figure 1. The largest decline in the EPIC sexual summary score occurred within the first year after treatment, with a mean drop of 11.1 points, whereas the mean drop was 12.6 points from baseline to 2 years. The incidence of potency (defined earlier) is depicted for all patients (Fig. 2). Potency rates declined by 11% from baseline over 2 years. In a subgroup of men Table 1. Patient, Disease, and Treatment Characteristics Characteristic N % Marital status Married Divorced/separated Single 21 8 Widowed 2 1 Unknown 6 2 Mood disorder Depression 20 8 Anxiety 19 7 None Diabetes Yes 17 6 No High cholesterol Yes No Hypertension Yes No Cardiac disease Yes 22 8 No T classification T1c T2a T2b 10 4 T2c/T3a 3 1 Gleason score Prostate-specific antigen < to > Risk group Low Intermediate High 6 2 Radiation dose CGE at 2.5 CGE/fraction CGE at 2 CGE/fraction CGE at 2 CGE/fraction without diabetes, BMI < 30, and a baseline IIEF > 21, 94% were potent 2 years after treatment. The degree of ED as defined by the IIEF-5 score (none, >21; mild, 17-21; mild-moderate, 12-16; moderate, 8-11; severe, 5-7) at baseline and at last follow-up is shown in Table 3. The rates of no ED or mild ED remained high 2 years after treatment (73%) compared with baseline levels Cancer Month 00,
4 Table 2. Expanded Prostate Cancer Index Composite (EPIC) Scores Over Time in Our Patient Population (and Standard Deviations in Parentheses) Baseline 6 mo 1 y 2 y Last Follow-Up P Urinary summary 91.6 (8.5) 88.9 (11.6) 87.3 (12.4) 88.5 (11.6) 88.6 (11.5) <.001 Urinary function 97 (6.9) 94.5 (9.5) 93.4 (10.3) 94.2 (9.5) 94 (9.9).0006 Urinary bother 87.7 (11.9) 84.9 (14.7) 82.9 (15.8) 84.4 (15.0) 84.7 (14.7).0002 Urinary incontinence 95.8 (9.2) 93.8 (11) 92.5 (13.2) 92.2 (13.0) 92 (12.9).0418 Urinary irritative/obstructive 90.2 (9.6) 87 (13.6) 85.6 (14.7) 87.5 (12.7) 87.8 (12.7).0002 Bowel summary 95.1 (5.8) 91.7 (10.4) 89.0 (11.7) 90.3 (10.8) 90.8 (10.3) <.0001 Bowel function 96 (6.9) 91.9 (12.5) 88.9 (14.6) 90.8 (9.3) 90.9 (12.5) <.0001 Bowel bother 94.1 (6.4) 91.7 (9.5) 89.3 (10.3) 89.7 (13.7) 91 (9.4) <.0001 Sexual summary 75.5 (17.8) 67.7 (20) 64.4 (22.0) 62.9 (22.6) 62.7 (22.1) <.0001 Sexual function 71.9 (17.1) 64.2 (18.3) 61.7 (20.7) 60.6 (20.5) 59.7 (20.5) <.0001 Sexual bother 84.3 (22.1) 75.2 (26.9) 71.0 (27.8) 69.1 (30.2) 70 (28.4) <.0001 Hormone summary 92.6 (9.2) 90.7 (10.2) 91.7 (9.7) 91.8 (9.2) 91.1 (9.7).7673 Hormone function 89.9 (11.3) 88.2 (12) 89.2 (11.3) 89.8 (10.9) 88.9 (11.5).9567 Hormone bother 94.5 (8.8) 92.9 (9.9) 93.8 (9.3) 93.6 (8.6) 93 (9.3).8169 Number of potential patients Number of patients with data Percent of patients with data 97% 93% 91% 87% 100% Figure 1. EPIC sexual scores over time are shown. SB indicates sexual bother; SF, sexual function; SS, sexual summary. (86%). The number of patients actively engaging in sexual intercourse at least weekly only dropped by 11% at 2 years. In addition, answers to selected questions from the EPIC at baseline through last follow-up are also listed in Table 3. The results of univariate and multivariate analyses are listed in Table 4 for sexual summary score and also for potency. On multivariate analysis, no factor was significant for a decline of 50% of baseline standard deviation. Two factors were significant for a decline by baseline standard deviation or greater, including penile bulb mean dose 40 CGE (P ¼ 0.012) and PT dose 80 CGE (P ¼ 0.017). Multivariate analysis for potency was significant for only diabetes (P ¼ 0.015). DISCUSSION Men undergoing EBRT as definitive treatment for prostate cancer have traditionally been older and have had more medical comorbidities (precluding surgery) than men undergoing prostatectomy. Considering the comparatively favorable cure rates emerging from long-term studies of radiotherapy in patients with prostate cancer, younger men are considering radiotherapy as an option due to concerns about urinary incontinence and ED following prostatectomy. The present study investigated HRQoL outcomes with an emphasis on urinary incontinence and erectile function in younger men (60 years old) following definitive PT and found only mild changes 4 Cancer Month 00, 2012
5 Proton Therapy for Young Prostate Cancer Patients/Hoppe et al Figure 2. Incidence of potency over time is shown. Table 3. Distribution of Answers to Specific IIEF and EPIC Questions Over 2 Years Quality of Life Question Baseline 6 mo 1 y 2 y Erectile dysfunction determined by IIEF score No Problem 69% 57% 48% 45% Mild ED 17% 21% 25% 28% Mild to Mod ED 9% 10% 10% 12% Moderate ED 1% 3% 7% 4% Severe ED 0% 3% 4% 4% Not sexually active 5% 6% 4% 8% How many pads per day did you use to control leakage during the last month? None 100.0% 99.6% 99.2% 98.2% One or more pads 0.0% 0.4% 0.8% 1.8% During the last month, how often did you have sexual intercourse? Not at all 14% 14% 18% 18% <Weekly 23% 28% 29% 30% Weekly 63% 58% 53% 52% Overall, how big a problem has your sexual function been for you over the last month? No problem 65% 48% 37% 39% Very small problem 19% 21% 22% 20% Small problem 7% 14% 17% 15% Moderate or big problem 10% 17% 24% 26% ED indicates erectile dysfunction; EPIC, Expanded Prostate Cancer Index Composite; IIEF, International Index of Erectile Function. in the urinary, bowel, hormone, and sexual scores following treatment. Although erectile function appeared to be affected by PT, the EPIC sexual summary scores demonstrated an average decline of only 12.6 points over a 2-year period. Furthermore, potency rates as defined in this study remained high, with 90% of all men and 94% of patients with high pretreatment potency, no obesity, and no diabetes remaining potent 2 years following treatment. Urinary continence levels were also well maintained, including only a 3.6-point decline over 2 years and only 1.8% of men requiring a pad at 2 years (no diapers). HRQoL studies that evaluated the various prostate cancer treatments through use of the EPIC questionnaire have recently gained in popularity. In the landmark study, Sanda et al 3 administered the shortened EPIC-26 questionnaire to patients at 0, 2, 6, 12, and 24 months after treatment for prostate cancer with either surgery, EBRT, or brachytherapy. The study demonstrated a substantial decline from baseline sexual summary score and urinary incontinence score in patients at 2 years after undergoing surgery, but only a mild to moderate decline in sexual score and a minimal decline in urinary incontinence score in patients who received either EBRT alone or Cancer Month 00,
6 Table 4. Univariate and Multivariate Analysis for Decline in SS Score and Potency SS Decline 50% SD SS Decline SD Potency Factor UVA MVA UVA MVA UVA MVA Age Body mass index Marital status Mood disorder Dose 80 CGE Dose/fraction 2.5 CGE vs Risk (low vs intermediate/high) Smoker 10 pack years Drinks > 7/wk Bulb mean dose 40 CGE Diabetes High cholesterol Hypertension Cardiac disease Alpha blocker Pretreatment IIEF < Testosterone < CGE indicates cobalt Gy equivalent; IIEF, International Index of Erectile Function; MVA, univariate analysis; SD, standard deviation; SS, sexual summary; UVA, univariate analysis. brachytherapy alone. Brachytherapy and radiotherapy alone did, however, lead to mild increases in urinary irritation or obstructive symptoms and bowel symptoms not seen with surgery. Pardo et al demonstrated similar outcomes after evaluating EPIC scores 3 years after treatment of prostate cancer with surgery, brachytherapy, or EBRT in a cohort of patients from Spain. 6 Despite the higher radiation doses delivered with PT in our study, the results seen with the EBRT groups in the studies of Sanda et al and Pardo et al are similar with respect to urinary incontinence, urinary irritation/ obstructive score, bowel score, and hormonal score. Importantly, Sanda et al reported the use of pads for the management of incontinence at 2 years in 20% of patients following prostatectomy, 5% following EBRT, and 8% following brachytherapy. The outcomes after EBRT are similar to those that were found in our study with a rate of 1.8%. Although the sexual outcomes were better with PT in the present study compared with the other radiation modalities reported in the studies by Sanda et al and Pardo et al, this finding may be due to selection bias. The PT group was made up of younger men with higher baseline sexual function and, thus, we might expect corresponding higher sexual summary scores in follow-up as well. Nevertheless, the data is valuable for prediction of important HRQoL outcomes in younger men facing treatment decisions. Although the sexual data is hard to compare to other radiotherapy data sets, due to both the high baseline function in this study and young age of the patients, comparisons with surgical data are reasonable. In fact, in the study by Sanda et al, the baseline sexual score was 80, but it dropped to 40 at 2 years following nerve-sparing surgery (and declined to 20 after non nerve-sparing surgery). Similarly, in the study by Pardo et al, the EPIC sexual summary score of the prostatectomy patients dropped from 67 at baseline to 40 at 2 years after nerve-sparing surgery and 18 after non nerve-sparing surgery. This contrasts considerably with the results from our study with PT, where baseline function only declined from 75.5 to 62.9 at 2 years. In addition, the number of men engaging in sexual intercourse at least weekly only dropped by 11% (from 63% at baseline to 52% at 2 years) in the 2 years following PT. Thus, preservation of sexual function after PT compares favorably with reported surgical experiences in the first 2 years following treatment. Despite the excellent outcomes at 2 years, there does appear to be some clinically relevant decline in sexual function and potency following PT, potentially attributable to factors other than increasing age. The multivariate analysis suggests a possible dose-related injury to the penile bulb, because mean dose to the penile bulb 40 CGE was associated with a decline by greater than the standard deviation in sexual summary scores. Other studies of penile bulb dose with standard EBRT and ED have yielded mixed results. The study by van der Wielen et al 18 found no correlation between ED at 2 years and dose to either the crura or the penile bulb in a study of 96 patients treated with doses of 68 to 78 Gy. However, Mangar et al 19 reported a significant correlation at 2 years between 6 Cancer Month 00, 2012
7 Proton Therapy for Young Prostate Cancer Patients/Hoppe et al the penile bulb dose-volume histogram (DVH) and ED in 51 men with baseline potency who had received 3 to 6 months of hormonal treatment and 64 or 74 Gy of radiotherapy. Dose received by 90% of the penile bulb (D90) > 50 Gy was significantly associated with ED (P ¼ 0.006). Likewise, in a study by Wenicke et al 20 of 29 men who received 66.6 to 79.2 Gy of 3-dimensional conformal radiotherapy, higher penile bulb doses (D30, D45, D60, and D75) were associated with an increased risk of ED. Finally, in an analysis of the Radiation Therapy Oncology Group 9406 trial, men who were potent at the start of treatment were evaluated in follow-up, and those who received a penile dose of >52.5Gy had a greater risk of impotence (P ¼.039). The data from these different studies are not entirely consistent but suggestive of doserelated penile bulb injury as a mechanism for radiationinduced ED. More prospective studies with penile bulb dose tracking will be required to determine how reliable this parameter is for predicting preservation of sexual function. The outcomes reported here are similar to those reported by investigators from the Massachusetts General Hospital, Boston, Massachusetts, in men receiving PT. 12 Coen et al demonstrated small increases in bowel dysfunction and incontinence with more pronounced changes in sexual dysfunction. Their study, however, used the Prostate Cancer Symptom Indices, which cannot be directly compared with the EPIC data available from contemporary surgery and brachytherapy series and included a much older patient cohort with poorer baseline erectile function. A major limitation of studies on sexual potency is that ED function is subjective, defined differently in various studies, and clearly affected by non treatment-related factors. Many studies have included patients who received hormone therapy, which can have a negative effect on ED. Other medical comorbidities, such as diabetes, obesity, and cardiac disease, may not have been assessed, and baseline sexual function may not have been considered. One strength of the present study is in its highly selected cohort of younger patients (60 years old) with known baseline function and comorbidities at the time of treatment. In addition, only a small fraction (10%) of patients in the current study have not completed a followup in the last 12 months, so the potential impact on outcomes from missing data is minimal. Furthermore, the percentage of patients who responded at 1 year (91%) and 2 years (87%) are similar to the response rate from Sanda et al (92% at 1 year and 87% at 2 years) 3 and Pardo et al (88% at 1 year and 85% at 2 years). Conclusions Young men undergoing PT for definitive treatment of prostate cancer have excellent outcomes with respect to ED and urinary incontinence. Attempting to keep the mean penile bulb dose to <40 CGE may further improve outcomes. PT may offer young men an excellent treatment option, with a lower risk of ED and urinary incontinence than with surgery. Further follow-up of this cohort of patients is needed to confirm long-term outcomes. FUNDING SOURCES No specific funding was disclosed. CONFLICT OF INTEREST DISCLOSURE The authors made no disclosure. REFERENCES 1. Nelson CJ, Mulhall JP, Roth AJ. The association between erectile dysfunction and depressive symptoms in men treated for prostate cancer. J Sex Med. 2011;8: Helgason AR, Adolfsson J, Dickman P, Fredrikson M, Arver S, Steineck G. Waning sexual function the most important diseasespecific distress for patients with prostate cancer. Br J Cancer. 1996;73: Sanda MG, Dunn RL, Michalski J, et al. Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med. 2008;358: Ferrer M, Suárez JF, Guedea F, et al; Multicentric Spanish Group of Clinically Localized Prostate Cancer. Health-related quality of life 2 years after treatment with radical prostatectomy, prostate brachytherapy, or external beam radiotherapy in patients with clinically localized prostate cancer. Int J Radiat Oncol Biol Phys. 2008;72: Rice K, Hudak J, Peay K, et al. Comprehensive quality-of-life outcomes in the setting of a multidisciplinary, equal access prostate cancer clinic. Urology. 2010;76: Pardo Y, Guedea F, Aguiló F, et al. Quality-of-life impact of primary treatments for localized prostate cancer in patients without hormonal treatment. J Clin Oncol. 2010;28: Vargas C, Fryer A, Mahajan C, et al. Dose-volume comparison of proton therapy and intensity-modulated radiotherapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2008;70: Fontenot JD, Lee AK, Newhauser WD. Risk of secondary malignant neoplasms from proton therapy and intensity-modulated x-ray therapy for early-stage prostate cancer. Int J Radiat Oncol Biol Phys. 2009;74: Vargas C, Mahajan C, Fryer A, et al. Rectal dose-volume differences using proton radiotherapy and a rectal balloon or water alone for the treatment of prostate cancer. Int J Radiat Oncol Biol Phys. 2007;69: Zietman AL, Bae K, Slater JD, et al. Randomized trial comparing conventional-dose with high-dose conformal radiation therapy in early-stage adenocarcinoma of the prostate: long-term results from proton radiation oncology group/american college of radiology J Clin Oncol. 2010;28: Talcott JA, Rossi C, Shipley WU, et al. Patient-reported long-term outcomes after conventional and high-dose combined proton and photon radiation for early prostate cancer. JAMA. 2010;303: Coen JJ, Paly JJ, Niemierko A, et al. Long-term quality of life outcome after proton beam monotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys May 26. [Epub ahead of print]. 13. Wei JT, Dunn RL, Litwin MS, Sandler HM, Sanda MG. Development and validation of the expanded prostate cancer index Cancer Month 00,
8 composite (EPIC) for comprehensive assessment of health-related quality of life in men with prostate cancer. Urology. 2000;56: Schroeck FR, Donatucci CF, Smathers EC, et al. Defining potency: a comparison of the International Index of Erectile Function short version and the Expanded Prostate Cancer Index Composite. Cancer. 2008;113: Mendenhall NP, Li Z, Hoppe BS, et al. Early outcomes from three prospective trials of image-guided proton therapy for prostate cancer. Int J Radiat Oncol Biol Phys. 2012;82: Barry MJ. Quality of life and prostate cancer treatment. J Urol. 1999;162: Norman GR, Sloan JA, Wyrwich KW. Interpretation of changes in health-related quality of life: the remarkable universality of half a standard deviation. Med Care. 2003;41: van der Wielen GJ, Hoogeman MS, Dohle GR, van Putten WL, Incrocci L. Dose-volume parameters of the corpora cavernosa do not correlate with erectile dysfunction after external beam radiotherapy for prostate cancer: results from a dose-escalation trial. Int J Radiat Oncol Biol Phys. 2008;71: Mangar SA, Sydes MR, Tucker HL, et al; MRC RT01 Trial Management Group. Evaluating the relationship between erectile dysfunction and dose received by the penile bulb: using data from a randomised controlled trial of conformal radiotherapy in prostate cancer (MRC RT01, ISRCTN ). Radiother Oncol. 2006;80: Wernicke AG, Valicenti R, Dieva K, Houser C, Pequignot E. Radiation dose delivered to the proximal penis as a predictor of the risk of erectile dysfunction after three-dimensional conformal radiotherapy for localized prostate cancer. Int J Radiat Oncol Biol Phys. 2004;60: Roach M, Winter K, Michalski JM, et al. Penile bulb dose and impotence after three-dimensional conformal radiotherapy for prostate cancer on RTOG 9406: findings from a prospective, multi-institutional, phase I/II dose-escalation study. Int J Radiat Oncol Biol Phys. 2004;60: Cancer Month 00, 2012
Comparative Effectiveness Study of Patient-Reported Outcomes After Proton Therapy or Intensity-Modulated Radiotherapy for Prostate Cancer
 Comparative Effectiveness Study of Patient-Reported Outcomes After Proton Therapy or Intensity-Modulated Radiotherapy for Prostate Cancer Bradford S. Hoppe, MD, MPH 1 ; Jeff M. Michalski, MD 2 ; Nancy
Comparative Effectiveness Study of Patient-Reported Outcomes After Proton Therapy or Intensity-Modulated Radiotherapy for Prostate Cancer Bradford S. Hoppe, MD, MPH 1 ; Jeff M. Michalski, MD 2 ; Nancy
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引
 馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
Proton Therapy for Prostate Cancer
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Proton Therapy for Prostate Cancer
 BRADFORD HOPPE, MD, MPH 1 RANDAL HENDERSON, MD, MBA 1 WILLIAM M. MENDENHALL, MD 1 ROMAINE C. NICHOLS, MD 1 ZUOFENG LI, PhD 1 NANCY P. MENDENHALL, MD 1 Proton Therapy for Prostate Cancer Abstract: Proton
BRADFORD HOPPE, MD, MPH 1 RANDAL HENDERSON, MD, MBA 1 WILLIAM M. MENDENHALL, MD 1 ROMAINE C. NICHOLS, MD 1 ZUOFENG LI, PhD 1 NANCY P. MENDENHALL, MD 1 Proton Therapy for Prostate Cancer Abstract: Proton
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results. Alan Katz MD JD Flushing, NY USA
 CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
1 of 6 6/13/11 12:40 PM
 ONCOLOGY. Vol. 25 No. 7 REVIEW ARTICLE Proton Therapy for Prostate Cancer By Bradford Hoppe, MD, MPH 1, Randal Henderson, MD, MBA 1, William M. Mendenhall, MD 1, Romaine C. Nichols, MD 1, Zuofeng Li, PhD
ONCOLOGY. Vol. 25 No. 7 REVIEW ARTICLE Proton Therapy for Prostate Cancer By Bradford Hoppe, MD, MPH 1, Randal Henderson, MD, MBA 1, William M. Mendenhall, MD 1, Romaine C. Nichols, MD 1, Zuofeng Li, PhD
Proton Therapy for Prostate Cancer: Your Questions, Our Answers.
 Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Proton Therapy for Prostate Cancer: Your Questions, Our Answers. When you re looking for the right treatment for your prostate cancer, nothing s more important than accurate information. Read on, and learn
Implementation Date: April 2015 Clinical Operations
 National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
Cyberknife Information Guide. Prostate Cancer Treatment
 Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
LATE MORBIDITY PROFILES IN PROSTATE CANCER PATIENTS TREATED TO 79 84 GY BY A SIMPLE FOUR-FIELD COPLANAR BEAM ARRANGEMENT
 PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
PROTON THERAPY FOR PROSTATE CANCER: THE INITIAL LOMA LINDA UNIVERSITY EXPERIENCE
 doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
Ryan C. Hedgepeth,* Jessica Labo, LingLing Zhang and David P. Wood, Jr.
 Expanded Prostate Cancer Index Composite Versus Incontinence Symptom Index and Sexual Health Inventory for Men to Measure Functional Outcomes After Prostatectomy Ryan C. Hedgepeth,* Jessica Labo, LingLing
Expanded Prostate Cancer Index Composite Versus Incontinence Symptom Index and Sexual Health Inventory for Men to Measure Functional Outcomes After Prostatectomy Ryan C. Hedgepeth,* Jessica Labo, LingLing
Prostate Cancer Patients Report on Benefits of Proton Therapy
 Prostate Cancer Patients Report on Benefits of Proton Therapy Dobson DaVanzo & Associates, LLC Vienna, VA 703.260.1760 www.dobsondavanzo.com Prostate Cancer Patients Report on Benefits of Proton Therapy
Prostate Cancer Patients Report on Benefits of Proton Therapy Dobson DaVanzo & Associates, LLC Vienna, VA 703.260.1760 www.dobsondavanzo.com Prostate Cancer Patients Report on Benefits of Proton Therapy
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
The Science behind Proton Beam Therapy
 The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
The Science behind Proton Beam Therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School Principles underlying Radiotherapy Radiation related
Subject: Proton Beam Therapy for Prostate Cancer
 Subject: Proton Beam Therapy for Prostate Cancer Guidance Number: MCG-153 Revision Date(s): Original Effective Date: 10/30/13 Medical Coverage Guidance Approval Date: 10/30/13 PREFACE This Medical Guidance
Subject: Proton Beam Therapy for Prostate Cancer Guidance Number: MCG-153 Revision Date(s): Original Effective Date: 10/30/13 Medical Coverage Guidance Approval Date: 10/30/13 PREFACE This Medical Guidance
TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software.
 SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
Prostate Cancer. What is prostate cancer?
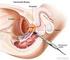 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma
 1773 Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma Leslie R. Schover, Ph.D. 1 Rachel T. Fouladi, Ph.D. 1 Carla L. Warneke, M.S. 1 Leah Neese, M.A. 1 Eric A. Klein, M.D. 2 Craig
1773 Defining Sexual Outcomes after Treatment for Localized Prostate Carcinoma Leslie R. Schover, Ph.D. 1 Rachel T. Fouladi, Ph.D. 1 Carla L. Warneke, M.S. 1 Leah Neese, M.A. 1 Eric A. Klein, M.D. 2 Craig
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021
 Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
How To Know If You Should Get A Brachytherapy Or Radioactive Seed Implantation
 MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
Radiation Therapy for Prostate Cancer: Treatment options and future directions
 Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Erectile function and quality of life after interstitial radiation therapy for prostate cancer
 (2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
(2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
Prostate Cancer Treatment Comparison
 Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Historical Basis for Concern
 Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate
 Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
Prostatectomy, pelvic lymphadenect. Med age 63 years Mean followup 53 months No other cancer related therapy before recurrence. Negative.
 Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Protons vs. CyberKnife. Protons vs. CyberKnife. Page 1 UC SF. What are. Alexander R. Gottschalk, M.D., Ph.D.
 Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
LONG-TERM URINARY TOXICITY AFTER 3-DIMENSIONAL CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER IN PATIENTS WITH PRIOR HISTORY OF TRANSURETHRAL RESECTION
 PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
PROTON BEAM THERAPY FOR PROSTATE CANCER. A Technology Assessment
 PROTON BEAM THERAPY FOR PROSTATE CANCER A Technology Assessment INTRODUCTION The California Technology Assessment Forum is requested to review the scientific evidence for the use of proton therapy for
PROTON BEAM THERAPY FOR PROSTATE CANCER A Technology Assessment INTRODUCTION The California Technology Assessment Forum is requested to review the scientific evidence for the use of proton therapy for
2/14/09. Long Term Risk of Radiation Therapy for Clinically Localized Prostate Cancer. Radiation Therapy: Various Forms of Radiation Treatment
 Radical ctomy (surgery) Mack Roach III MD Professor & Chair Department of Radiation Oncology Long Term Risk of Radiation Therapy for Clinically Localized Cancer Radiation Therapy: Hormonal Therapy Cryotherapy
Radical ctomy (surgery) Mack Roach III MD Professor & Chair Department of Radiation Oncology Long Term Risk of Radiation Therapy for Clinically Localized Cancer Radiation Therapy: Hormonal Therapy Cryotherapy
SRO Tutorial: Prostate Cancer Treatment Options
 SRO Tutorial: Prostate Cancer Treatment Options May 7th, 2010 Daniel M. Aebersold Klinik und Poliklinik für Radio-Onkologie Universität Bern, Inselspital Is cure necessary in those in whom it may be possible,
SRO Tutorial: Prostate Cancer Treatment Options May 7th, 2010 Daniel M. Aebersold Klinik und Poliklinik für Radio-Onkologie Universität Bern, Inselspital Is cure necessary in those in whom it may be possible,
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
PROSTATE CANCER WITH LARGE GLANDS TREATED WITH 3- DIMENSIONAL COMPUTERIZED TOMOGRAPHY GUIDED PARARECTAL BRACHYTHERAPY: UP TO 8 YEARS OF FOLLOWUP
 0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
Proton Beam Therapy. Methods Literature for this article was obtained using the Touro College Online library, in particular PubMed.
 Is Proton Beam Therapy more Effective than Intensity- Modulated Radiotherapy in Prostate Cancer Treatment? Daniel Zelefsky Daniel will graduate in June 2015 with an Honors Biology B.S. degree. Abstract
Is Proton Beam Therapy more Effective than Intensity- Modulated Radiotherapy in Prostate Cancer Treatment? Daniel Zelefsky Daniel will graduate in June 2015 with an Honors Biology B.S. degree. Abstract
Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director Stuart Klein, MHA Executive Director Zuofeng Li, DSc Physics Director
 Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director A University of Florida College of Medicine faculty member since 1985, Dr. Mendenhall served as the chair of the Department
Key Staff Members EXECUTIVE TEAM Nancy Price Mendenhall, MD Medical Director A University of Florida College of Medicine faculty member since 1985, Dr. Mendenhall served as the chair of the Department
Beyond the PSA: Genomic Testing in Localized Prostate Cancer
 Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
NATURAL HISTORY OF CLINICALLY STAGED LOW- AND INTERMEDIATE-RISK PROSTATE CANCER TREATED WITH MONOTHERAPEUTIC PERMANENT INTERSTITIAL BRACHYTHERAPY
 doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15.
 Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward
 Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy
 Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Does my patient need more therapy after prostate cancer surgery?
 Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
855-DRSAMADI or 212-241-8779
 SMART SURGERY NEWS MARCH 2013 Dr. David Samadi 855-DRSAMADI or 212-241-8779 YOUR PROSTATE CANCER NEWS PREVENTION DIAGNOSIS TREATMENT LIFE AFTER PROSTATE CANCER PREVENTION Prostate Cancer Need-to-Knows
SMART SURGERY NEWS MARCH 2013 Dr. David Samadi 855-DRSAMADI or 212-241-8779 YOUR PROSTATE CANCER NEWS PREVENTION DIAGNOSIS TREATMENT LIFE AFTER PROSTATE CANCER PREVENTION Prostate Cancer Need-to-Knows
A new score predicting the survival of patients with spinal cord compression from myeloma
 A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
A new score predicting the survival of patients with spinal cord compression from myeloma (1) Sarah Douglas, Department of Radiation Oncology, University of Lubeck, Germany; sarah_douglas@gmx.de (2) Steven
Thomas A. Kollmorgen, M.D. Oregon Urology Institute
 Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Particle Therapy for Lung Cancer. Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org
 Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy and Howard Amols
 Long-Term Outcome of High Dose Intensity Modulated Radiation Therapy for Patients With Clinically Localized Prostate Cancer Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy
Long-Term Outcome of High Dose Intensity Modulated Radiation Therapy for Patients With Clinically Localized Prostate Cancer Michael J. Zelefsky,*, Heather Chan, Margie Hunt, Yoshiya Yamada, Alison M. Shippy
DOCTOr. Doctor to HIGHLIGHTS. issue NO. 3 VOLuMe NO. 1
 Doctor to DOCTOr issue NO. 3 VOLuMe NO. 1 PROSTATE CANCER is the most common cancer in men, with 233,000 new cases diagnosed per year. Although prostate cancer remains the second leading cause of cancer
Doctor to DOCTOr issue NO. 3 VOLuMe NO. 1 PROSTATE CANCER is the most common cancer in men, with 233,000 new cases diagnosed per year. Although prostate cancer remains the second leading cause of cancer
TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples
 AD Award Number: W81WH-07-1-0069 TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples PRINCIPAL INVESTIGATOR: Sally L. Maliski, Ph.D., R.N. CONTRACTING ORGANIZATION:
AD Award Number: W81WH-07-1-0069 TITLE: The Impact Of Prostate Cancer Treatment-Related Symptoms On Low-Income Latino Couples PRINCIPAL INVESTIGATOR: Sally L. Maliski, Ph.D., R.N. CONTRACTING ORGANIZATION:
IBA Proton Therapy. Biomed days 2015. Vincent Bossier. System Architect Vincent.bossier@iba-group.com. Protect, Enhance and Save Lives
 Vincent Bossier System Architect Vincent.bossier@iba-group.com IBA Proton Therapy Biomed days 2015 Protect, Enhance and Save Lives 1 Agenda AN INTRODUCTION TO IBA WHY PROTON THERAPY CLINICAL WORKFLOW TREATMENT
Vincent Bossier System Architect Vincent.bossier@iba-group.com IBA Proton Therapy Biomed days 2015 Protect, Enhance and Save Lives 1 Agenda AN INTRODUCTION TO IBA WHY PROTON THERAPY CLINICAL WORKFLOW TREATMENT
Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer
 Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer Whoon J. Kil, MD 1 ; Nancy P. Mendenhall, MD 1 ; Christopher G. Morris, MS 1 ;R. Charles Nichols, MD 1 ; Randal
Patient-reported Hip Symptoms following Treatment with Proton Therapy for Prostate Cancer Whoon J. Kil, MD 1 ; Nancy P. Mendenhall, MD 1 ; Christopher G. Morris, MS 1 ;R. Charles Nichols, MD 1 ; Randal
Prostate Cancer Treatment Comparison
 Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Prostate Cancer Treatment Comparison Treatment Comparative Data Outcome Comparison: Surgery vs. Radiotherapy Outcome Radical Prostatectomy* Radiation** Survival duration compared to conservative disease
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds
 Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Forum. Advances in radiation therapy for prostate. cancer. Abstract. Radiation therapy for localised prostate. cancer
 Advances in radiation therapy for prostate cancer Nitya Patanjali 1 and Scott Williams 2 1. Radiation Oncology, Sydney Cancer Centre, Royal Prince Alfred Hospital, Sydney. 2. Radiation Oncology, Peter
Advances in radiation therapy for prostate cancer Nitya Patanjali 1 and Scott Williams 2 1. Radiation Oncology, Sydney Cancer Centre, Royal Prince Alfred Hospital, Sydney. 2. Radiation Oncology, Peter
Dosimetric and radiobiological impact of intensity modulated proton therapy and RapidArc planning for high-risk prostate cancer with seminal vesicles
 ORIGINAL ARTICLE Dosimetric and radiobiological impact of intensity modulated proton therapy and RapidArc planning for high-risk prostate cancer with seminal vesicles Suresh Rana, MS, 1,2 ChihYao Cheng,
ORIGINAL ARTICLE Dosimetric and radiobiological impact of intensity modulated proton therapy and RapidArc planning for high-risk prostate cancer with seminal vesicles Suresh Rana, MS, 1,2 ChihYao Cheng,
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT
 MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Therapies for Prostate Cancer and Treatment Selection
 Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
Focal therapy for prostate cancer: seriously or seriously? Disclosures
 Focal therapy for prostate cancer: seriously or seriously? Mitchell Kamrava, MD Assistant Clinical Professor Department of Radiation Oncology University of California Los Angeles Disclosures Speaking honorarium
Focal therapy for prostate cancer: seriously or seriously? Mitchell Kamrava, MD Assistant Clinical Professor Department of Radiation Oncology University of California Los Angeles Disclosures Speaking honorarium
Neoadjuvant hormonal therapy in prostate cancer impact of PSA level before radiotherapy
 JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
JBUON 2013; 18(4): 949-953 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Neoadjuvant hormonal therapy in prostate cancer impact of PSA level
Transition from 2D to 3D Brachytherapy in Cervical Cancers: The Vienna Experience. Richard Pötter MD. BrachyNext, Miami, 2014.
 Transition from 2D to 3D Brachytherapy in Cervical Cancers: The Vienna Experience Richard Pötter MD BrachyNext, Miami, 2014 Disclosures Richard Pötter, MD, does not have any financial relationships or
Transition from 2D to 3D Brachytherapy in Cervical Cancers: The Vienna Experience Richard Pötter MD BrachyNext, Miami, 2014 Disclosures Richard Pötter, MD, does not have any financial relationships or
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer
 Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Use of Androgen Deprivation Therapy (ADT) in Localized Prostate Cancer Adam R. Kuykendal, MD; Laura H. Hendrix, MS; Ramzi G. Salloum, PhD; Paul A. Godley, MD, PhD; Ronald C. Chen, MD, MPH No conflicts
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
4/8/13. Pre-test Audience Response. Prostate Cancer 2012. Screening and Treatment of Prostate Cancer: The 2013 Perspective
 Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Prostate cancer is the second most
 Treatment Options for Localized Prostate Cancer RAVINDER MOHAN, MD, PhD, and PAUL F. SCHELLHAMMER, MD Eastern Virginia Medical School, Norfolk, Virginia In the United States, more than 90 percent of prostate
Treatment Options for Localized Prostate Cancer RAVINDER MOHAN, MD, PhD, and PAUL F. SCHELLHAMMER, MD Eastern Virginia Medical School, Norfolk, Virginia In the United States, more than 90 percent of prostate
Current and Future Trends in Proton Treatment of Prostate Cancer
 Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm
 NAACCR Conference, Austin, TX June 13, 2013 In Collaboration with: Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm John W. Morgan, DrPH, CPH, Brice Jabo,
NAACCR Conference, Austin, TX June 13, 2013 In Collaboration with: Does Radiation Treatment of Prostate Cancer Increase Risk for Rectal Cancer? The Perfect Storm John W. Morgan, DrPH, CPH, Brice Jabo,
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
FIVE-YEAR BIOCHEMICAL OUTCOME FOLLOWING PERMANENT INTERSTITIAL BRACHYTHERAPY FOR CLINICAL T1 T3 PROSTATE CANCER
 PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
Understanding the. Controversies of. testosterone replacement. therapy in hypogonadal men with prostate cancer. controversies surrounding
 Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Summary ID# 13614. Clinical Study Summary: Study F3Z-JE-PV06
 CT Registry ID# Page 1 Summary ID# 13614 Clinical Study Summary: Study F3Z-JE-PV06 INSIGHTS; INSulin-changing study Intending to Gain patients insights into insulin treatment with patient-reported Health
CT Registry ID# Page 1 Summary ID# 13614 Clinical Study Summary: Study F3Z-JE-PV06 INSIGHTS; INSulin-changing study Intending to Gain patients insights into insulin treatment with patient-reported Health
GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision
 RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
IGRT. IGRT can increase the accuracy by locating the target volume before and during the treatment.
 DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD
 MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Official reprint from UpToDate www.uptodate.com 2013 UpToDate
 Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
Precise, Minimally Invasive Prostate Cancer Removal
 Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
[Insuree] Page 1 Letter of Appeal
![[Insuree] Page 1 Letter of Appeal [Insuree] Page 1 Letter of Appeal](/thumbs/24/3356957.jpg) - - - - - - - - - - - - - - - - - - - - From: [Insuree]- - - 8/16/09 Board of Trustees - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - -
- - - - - - - - - - - - - - - - - - - - From: [Insuree]- - - 8/16/09 Board of Trustees - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - - -
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER
 2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
Robotic Radical Prostatectomy: What s s the Advantage? Matthew T. Gettman, M.D. Associate Professor Department of Urology
 Robotic Radical Prostatectomy: What s s the Advantage? Matthew T. Gettman, M.D. Associate Professor Department of Urology Prostate Cancer Epidemiology: 2009 Estimated new cases: 230,000 Estimated deaths:
Robotic Radical Prostatectomy: What s s the Advantage? Matthew T. Gettman, M.D. Associate Professor Department of Urology Prostate Cancer Epidemiology: 2009 Estimated new cases: 230,000 Estimated deaths:
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
