Headache: Is it a migraine? Think again
|
|
|
- Horace Payne
- 10 years ago
- Views:
Transcription
1 Techniques in Regional Anesthesia and Pain Management (2005) 9, : Is it a migraine? Think again Andrea Trescot, MD, FIPP From The Pain Center, Orange Park, Florida. KEYWORDS: Migraine; ; Cephalgia; management For many years, headaches or migraines have been felt to be intracranial in nature. However, recently a large number of migraines have been found to be due to extracranial causes which are amenable to interventional pain techniques. Recognition of the causes of extracranial headaches will result in effective and rewarding headache treatment Elsevier Inc. All rights reserved. If you would test the skill of a young physician, give him a patient with a headache to treat. William Sunderham, MD University of Michigan 1935 Interventional pain physicians have traditionally focused on spinal pain as their area of interest. Despite the fact that many back pain patients develop chronic headaches as part of their disease process, most interventionalists have had neither the training nor the interest in treating headache patients. Since headaches are felt to be primarily a female disease, there has been little interest in the diagnosis and treatment, much in the same way as premenstrual syndrome has been largely ignored. s appear to be considered the property of neurologists, and because headaches (especially migraines ) are felt to be primarily intracranial, they have been of little interest to an interventionalist. However, as the pathophysiology of extracranial headaches becomes better known, it becomes clear that there is a role as well as a need for interventional treatment of this potentially debilitating condition. This treatise is an attempt to introduce the pain physician to a practical approach to the diagnosis and treatment of headaches and migraines. I have deliberately used the term migraine in quotes, because much of the confusion regarding headache management has come from the use of this term. The International Society (HIS) has defined migraine as an intracranial headache, unilateral and throbbing, associated with photophobia, phonophobia, and nausea. Unfortunately, extracranial headaches can present symptoms in exactly the same way, and patients usually use the term migraine to mean Address reprint requests and correspondence: Andrea Trescot, MD, FIPP, The Pain Center, 1564 Kingsley Ave., Orange Park, FL address: [email protected] X/$ -see front matter 2005 Elsevier Inc. All rights reserved. doi: /j.trap a sick headache. As a result, the term is meaningless and confusing, and I will use the term headache instead. In the evaluation of headache patients, the same principles of history, physical examination, and diagnostic studies apply. However, the diagnostic studies are primarily to identify secondary causes of headaches, such as tumors. The true diagnosis is best made at the time of the patient s headache by the use of a diagnostic injection. It is amazing and gratifying (as well as diagnostic) to be able to provide nearly instant relief to a patient with an acute headache, by performing a diagnostic (as well as therapeutic) injection. Almost before the needle is out of the head, the headache, nausea, and photophobia start to rapidly resolve. Within a few minutes, the patient will start to feel normal. As with all diagnostic injections, an injection of a structure with a small volume of local anesthetic that gives at least temporary relief of the pain is considered diagnostic of a pain generator. If the patient does not get relief, that structure is not considered to be the source of the pain. However, that assumes that the patient gets numb from that local anesthetic. As was reported in Pain Physician, 1 skin testing with lidocaine, bupivicaine, and mepivicaine revealed that 7.5% of the studied patients only got numb from mepivicaine, and another 4% only get numb from lidocaine. In these patients, bupivicaine (the most commonly used local anesthetic because of its long-lasting effect) would be either very slow in onset or totally ineffective, potentially even resulting in increased pain. In my practice, therefore, all patients are skin tested to evaluate the most effective local anesthetic before any injections. As with every disease, once a diagnosis is made, the long-term treatment plan can be formulated. Practitioners must realize that the term headache is not a diagnosis, but rather a symptom; just as is the way that low back pain must
2 Trescot 69 be viewed. Treating a patient with low back pain by using epidural steroids for sacroiliac pathology will give no greater long-term relief than treating an occipital neuralgia patient with triptans. The pertinent history of a headache patient centers on the site of the initial pain sensation, the referral pattern, and the contributing factors. For example, a patient complaining of unilateral or bilateral temple pain (triggered by talking, chewing, and menses), which awakens the patient at 3 or 4 o clock AM, should immediately bring to mind auriculotemporal neuralgia (ATN), as I will describe later. A confirmatory physical examination of the ATN region showing tenderness of the region would be supportive of this diagnosis. However, similarly presenting pathologies, such as temporomandibular joint (TMJ), sternocleitomastoid muscle (SCM), supraorbital, and occipital, may also be supported or refuted by the physical examination. The diagnosis is then confirmed by a small-volume injection of the presumed pathology, such as the ATN. If local anesthetic (as well as deposteroid if indicated) gave excellent but only temporary relief, more long-term therapies such as cryoneuroablation, radiofrequency lesioning, botulism toxin, regenerative injection therapy, or subcutaneous stimulation, in addition to rational drug therapy (anticonvulsants for nerve pathology, muscle relaxants for muscle pathology, etc.) could then be offered. The dictum You can not treat what you can not diagnose has never been truer than in the treatment of headaches. On physical examination, there is marked tenderness over the supraorbital notch, and/or over the supratrochlear nerve at the lateral border of the nasal bone. This area is very sensitive, and a 30-gauge needle is appropriate. Less than 1 cc of total volume should be used, and care must be taken to avoid directing the needle into the foramen itself, since injection of a large volume in the foramen could cause increased entrapment of the nerve. Supraorbital neuralgia usually responds well to cryoneuroablation, with a dramatic and sustained relief of the headache. It is interesting that Botulin toxin, first used by plastic surgeons to treat frown lines, was noted to relieve certain types of headaches. Also a retrograde effect on the DRG has been proposed as a potential mechanism of the headache relief from Botulin toxin. I think it is much more likely and logical that this represents a decrease in pressure on the supraorbital nerve with frowning, which is then released with the relaxation of the muscle. Pulsed radiofrequency has not been described, but theoretically might be appropriate. Early experience with subcutaneous electrical stimulation suggests that there may be a role for this therapy in intractable cases. Supraorbital neuralgia The headache of supraorbital neuralgia is often confused with frontal sinusitis, cluster headaches, and menstrual migraines. The headache may have been preceded by trauma recently, or many years later, as a cicatrix forms around the nerve over time. The nerve can become entrapped by fluid retention such as during the perimenstrual time frame or by salt intake. The nerve can also be injured by poorly fitting glasses or entrapped by frowning or squinting. The supratrochlear nerve, which is present medially, may also have pathology, and may need to be treated concurrently or sequentially. The patient will complain of a frontal headache, either dull or throbbing, unilaterally or bilaterally. There may be severe nausea and emesis. Triptans will help but only temporarily. There can be lacrimation, scleral injection, and sudden stabbing pain that can mimic cluster headaches. The patient will often self-treat with sinus medications without relief. The supraorbital nerve is the termination of the first division of the trigeminal nerve. Irritation of the nerve occurs primarily at the supraorbital notch. A small ligament completes the inferior border of a foramen through which the nerve passes before passage through the orbicularis oculi. Auriculotemporal neuralgia Auriculotemporal neuralgia (ATN) is probably the most common of the trigeminal headaches. The pain is primarily in the temple, with radiation to the retro-orbital region, and may be unilateral or bilateral. There may be associated ear and lower jaw pain. The headache is often throbbing in nature, probably due to its proximity to the temporal artery, and can be associated with severe nausea and vomiting. This is the headache that wakes the patient up at 3 or 4 AM, presumably due to clenching or bruxing during this lightest stage of sleep. It is misdiagnosed as TMJ pathology (though the auriculotemporal nerve gives innervation to the joint). The auriculotemporal nerve derives from the third division of the trigeminal nerve. It runs inferiorly under the pterygoid muscle to the neck of the mandible and then turns cephalad to travel with the temporal artery between the external ear and the condyle of the jaw, giving branches to the TMJ and the anterior ear as it passes cephalad to the temporalis muscle. There are two sites of pathology and therefore two potential injection sites. The most common is the distal en-
3 70 Techniques in Regional Anesthesia and Pain Management, Vol 9, No 2, April 2005 trapment that occurs at the temporalis muscle. This spot is usually identified as an exquisitely tender area at the apex of an isosceles triangle with the base composed of lines connecting the tragus and the corner of the eye. This is usually in close proximity to the artery. One cc of local anesthetic and depot steroid are then injected in a cephalad direction, parallel to the path of the nerve. The artery is usually slightly more posterior, so, if the pulsations of the artery are not obvious, I usually try to place the injection slightly anteriorly to avoid a hematoma. Careful evaluation will confirm that the artery itself is not tender, therefore decreasing the likelihood of a missed diagnosis of temporal arteritis. The second site is more proximal and less common. It is located as the nerve passes anterior to the TMJ, just inferior to the zygoma. This is close to the facial nerve, and the patient must be warned of the possibility of temporary facial weakness. For that reason, small volumes (less than 0.5 cc) and meticulous needle placement are important. There is occasionally a double crush syndrome with the nerve trapped at both sites, and both would then need to be treated. The distal ATN entrapment is very amenable to cryoneuroablation. However, because of the proximity of the facial nerve to the proximal ATN, special care and meticulous motor stimulation are advisable for the proximal technique. The use of clonazepam or tizanidine at night will keep the patient in a deeper plain of sleep, decreasing the bruxing and therefore decreasing the entrapment. Standard bite blocks are usually ineffective, but an anterior occlusion splint, which places the front teeth in opposition and prevents clenching, may be useful. (You may wish to try this yourself. First, place your finger on your temple and clench, feeling the temporalis contraction under your finger. Then, place your front teeth together and try again. Neither the masseter nor temporalis can contract.) Facial neuralgia Although the facial nerve is primarily a motor nerve, it does carry sensory fibers to the face and can be a cause of headaches. The most common entrapment is the zygomatic branch at the coronoid notch. This headache usually occurs in the morning after the dentures have been out all night, with the loss of the dentition height leading to a narrowing of the coronoid notch, which results in entrapment. Other less common entrapment sites include the temporal branch, lateral to the orbicularis oculi. The facial nerve exits the cranium at the stylo-mastoid foramen. The nerve runs within the body of the parotid gland and then splits into five branches to supply five areas of the face: temporal, zygomatic, buccal, mandibular, and cervical. The zygomatic branch of the facial nerve lies just inferior to the zygoma. A small volume of local and deposteroid (total volume less than 2 ml) can give nearly instant relief. Most of the small branches of the facial nerve are amenable to cryoneuroablation. However, it is important to remind the patient of the risk of motor weakness. Luckily, the motor function is the first to return, usually long before sensory function, and many desperate patients would gladly exchange a small amount of facial weakness in exchange for relief of intractable headaches. Posterior auricular neuralgia Pathology of the posterior auricular nerve (also called the greater auricular nerve) will cause a parietal headache associated with ear pain. This nerve is injured by trauma to the mastoid such as seen with blows to the head. For that reason, these headaches are more common on the left, since most male abusers are right handed. Flexion/extension injuries, especially with the head turned, will also traumatize the nerve. The entrapment may be seen many years after the trauma as a cicatrix of scar tissue forms around the nerve. Palpation of the posterior auricular area will reveal a palpable groove just posterior to the SCM attachment, which will be tender and will replicate the pain. The posterior auricular nerve is a branch of the superficial cervical plexus, and runs along the posterior border of the SCM muscle, superficially and immediately posterior to the mastoid. The tissues of the posterior auricular region are very thin, and the nerve is usually easy to identify. The apparent entrapment is just posterior to the SCM attachment, and the diagnostic injection should enter just at the base of the skull, aiming cephalad and slightly anteriorly. The injection should be of a small volume (less than 1 cc) of a depot steroid and local anesthetic, taking care that the needle remains on bone. Cryoneuroablation of the posterior auricular nerve can be very successful. Care, however, must be used to avoid frostbite of the superficial tissues since the skin can be quite thin at this region.
4 Trescot 71 Occipital neuralgia Occipital neuralgia is probably one of the most recognized of the extracranial pathologies. These headaches usually start at the base of the skull, and radiate anteriorly, often to behind the eyes. However, as noted earlier, the presentation may be first in a trigeminal distribution, often described as an ice pick in the retro-orbital region with pain then radiating to the occipital region. Alternatively, the pain may start as a tension headache in the upper cervical region and then center at the base of the skull. The headache can be sharp, dull, or throbbing, and may be unilateral or bilateral, with nausea and photophobia. The nerve can be entrapped by the trapezius muscle, and is commonly seen in flexion/extension injuries. There are actually three occipital nerves. The largest, the greater occipital nerve, is the dorsal ramus of C2. It originates lateral to the lateral atlantoaxial joint, deep to the inferior oblique muscle, where it may receive a communicating branch from C3. It then ascends up the neck over the rectus capitus and then pierces the semispinalis capitus muscle, deep to the trapezius. It then exits the neck through an aponeurotic sling composed of the insertions of the trapezius and sternocleidomastoid muscles, close to the occipital artery. The lesser occipital nerve is also a branch of C2, but travels more laterally, and exits the neck just lateral to the occipital prominence. The third occipital nerve also comes from C2 and C3, running medially to the occiput, innervating the suboccipital region. The classic description of the occipital nerve was for surgical anesthesia of the posterior scalp. Ten cc of local anesthetic was injected subcutaneously from lateral to medial across the nuchal ridge. This would usually effectively anesthetize all three nerves, but not at the site of the entrapment. In addition, because the tissue is so adherent to the scalp at this level, large volumes could potentially create an entrapment of the nerves. Two alternative techniques are being described here. For my technique, the injection site (in this case describing the right side) is identified by placing the thumb of the right hand at the foramen magnum (which identifies midline and avoids the cisternal injection); the index finger is then placed at the conjoined tendon attachment, and the second finger will then identify the injection site at the base of the skull. The needle is directed cephalad and slightly medially until contact is made with bone. Small volumes (less than 2 ml) of local and steroid are thereby injected underneath the tendon where the nerve pierces the tendon attachment. Dr. Gabor Racz (personal communication) instead recommends a cephalad to caudad approach to reach the potential space anterior to the splenius muscles, using large volumes to decompress the nerve proximal to the fascia piercing. A specialized curved blunt-tipped stealth needle has been developed to facilitate this approach. Cryoneuroablation of the occipital nerve is probably for most practitioners the most familiar of the cryoablation techniques. If the small volume technique described above gives good but only temporary relief, the cryo probe can be advanced from a caudad to cephalad direction to the occipital bone, and the nerve frozen at that site. Pulsed RF is being used, but I would strongly caution against heat RF or surgical resection of the nerve because of the high incidence of neuroma formation. However, if the pathology is more proximal, the C2 or C3 nerve root may need to be addressed. There has also been a good deal of interest in the use of occipital subcutaneous stimulation for intractable occipital headaches. Myofascial pathology (masseter, SCM, trapezius) Myofascial pain or trigger points can present as a variety of headache conditions. Chronic stress leading to teeth clenching, bruxism, dental malocclusion, and TMJ pathology can all cause spasm of the masseter muscle, which will refer pain to the temples, jaw, and over the eye. The SCM muscle will refer pain to the ear, temple, and face, especially over the eye. Patients often complain of fullness in the ear with decreased hearing, leading to unnecessary ENT evaluations. There can also be tinnitus and vertigo, mimicking vestibulitis. Since flexion/extension injuries will traumatize the SCM, what have been considered coup-contra coup brain injuries are now being recognized as myofascial pain. Tension headaches is a term that seems to trivialize the intractable occipital and retro orbital headaches that are caused by trapezius spasm. The pain can be caused by stress, chronic postural problems (for instance with prolonged neck flexion for reading), or flexion/extension injuries. The anatomy of these muscles is well described in Travell. 2 Trigger point injections such as described in Travell can give immediate, dramatic, and sustained relief. Injections with botulin toxin has been shown to give long-term relief, up to 3 to 4 months. This provides a window of opportunity for neuromuscular reeducation.
5 72 Techniques in Regional Anesthesia and Pain Management, Vol 9, No 2, April 2005 Cervical ligament pathology In 1954, Feinstein 3 followed up on work done by Kellgren, 4 which showed that irritation of the cervical ligaments can refer pain to the head and face as well as the extremities. These cervical ligaments are traumatized in flexion/extension injuries but also can occur with chronic low-grade trauma. The subsequent ligament laxity no longer allows support of the 30-pound head, and the cervical muscles will go into spasm to hold the head up. This ligament pathology results in a straightening of the cervical lordosis. Thus, the common x-ray diagnosis of loss of cervical lordosis secondary to spasm is actually the reverse contraction of a muscle above and below the lordosis must cause more lordosis if the muscles are the pathology. On physical examination, palpable defects in the ligament can be observed, and patients often describe the sensation that their head is too heavy to hold up. The dorsal median branch of the dorsal median nerve innervates the interspinous ligament, as well as the facets and paravertebral muscles. Then, it enters the spinal column at the level of the cervical nerve roots. Whereas facet pathology will give a unilateral referred pain, interspinous ligament pathology will give bilateral pain. Pain can be referred to the face or occipital region, as well as down the shoulder or arm, just as is seen with facet pathology. In fact, there is an argument that facet pathology (as well as disc pathology) cannot occur without ligamentous disruption. The interspinous ligament injection is performed by injecting 1 cc of local and depo-steroid into the superficial ligament, dorsal to the level of the lamina. To decrease the risk of entering the epidural or intrathecal space, the needle should be directed inferiorly, ideally contacting the spinous process to confirm depth. If the diagnostic injection gives good but only temporary relief, Regenerative Injection Therapy (RIT), formally known as prolotherapy, may give long-term relief. An old technique that fell out of favor but has gradually returned into mainstream therapy, RIT relies on the injection of deliberately irritating material at the fibro-osseous junction to stimulate the proliferation of fibroblasts, causing the production of new tissue at the area. Typical solutions are based on high concentrations of dextrose with local anesthetic. Not only is there symptomatic relief, but also the reinforcement of the ligament can be palpated as a decrease in the ligament defect. However, patients on chronic antiinflammatory agents or anticoagulants, as well as smokers, do not usually respond well, probably due to suppression of the fibroblast activity. In addition, this technique is currently not approved by Medicare. An alternative therapy may be to use heat radiofrequency lesioning at the same fibro-osseous junction. This results in a denervation of the painful periosteum, but may also create a thermal stimulus for fibroblastic activity. Conclusion Aggressive treatment of headaches and migraines can be gratifying and technically satisfying for the interventional pain physician with the knowledge and skill to provide injection therapy to patients with these pain problems. References 1. Trescot AM: management in an interventional pain practice. Pain Physician 3: , Travell JC, Simons DC: Myofascial Pain and Dysfunction: The Trigger Point Manual (vol. 1). Baltimore, MD, Williams & Wilkins, Feinstein MD: Experiments on pain referred from deep somatic tissues. J Bone Joint Surg 36A: , Kellgren JH: On the distribution of pain rising from deep somatic structures with charts of segmental pain areas. Clin Sci 4:35-46, 1939
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies
 Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
by joseph e. muscolino, DO photography by yanik chauvin
 by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE
 TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Headaches + Facial pain
 Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Headaches + Facial pain Introduction: Each of us experienced sporadically/ chronically headache 40% worldwide population suffers with severe, disabling headache at least annually Common ailment Presenting
Toothaches of Non-dental Origin
 Toothaches of Non-dental Origin This brochure is produced by the American Academy of Orofacial Pain The American Academy of Orofacial Pain is an organization of health care professionals dedicated to alleviating
Toothaches of Non-dental Origin This brochure is produced by the American Academy of Orofacial Pain The American Academy of Orofacial Pain is an organization of health care professionals dedicated to alleviating
Careful Coding: Headaches
 Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Lateral pterygoid muscle Medial pterygoid muscle
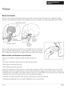 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
X-Plain Temporomandibular Joint Disorders Reference Summary
 X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
It is a syndrome characterized by chronic pain caused by multiple trigger points and
 1 WHAT IS MYOFASCIAL PAIN SYNDROME? It is a syndrome characterized by chronic pain caused by multiple trigger points and myofascial tightening. The term fascial pertains to the muscle, and it is a lining
1 WHAT IS MYOFASCIAL PAIN SYNDROME? It is a syndrome characterized by chronic pain caused by multiple trigger points and myofascial tightening. The term fascial pertains to the muscle, and it is a lining
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Headaches. This chapter will discuss:
 C H A P T E R Headaches 1 1 Almost everyone gets an occasional headache at some time or another. Some people get frequent headaches. Most people do not worry about headaches and learn to live with them
C H A P T E R Headaches 1 1 Almost everyone gets an occasional headache at some time or another. Some people get frequent headaches. Most people do not worry about headaches and learn to live with them
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
THE TMJ TREATMENT CENTER
 THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
Laser Treatment Policy
 Laser Treatment Policy Pursuant to federal law 21 CFR 812.2(c)7 and 812.3(b), physician(s) at this pain center may advise and use unapproved laser s on patients under one or more of the following conditions:
Laser Treatment Policy Pursuant to federal law 21 CFR 812.2(c)7 and 812.3(b), physician(s) at this pain center may advise and use unapproved laser s on patients under one or more of the following conditions:
Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy
 Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Pain Physician 2007; 10:313-318 ISSN 1533-3159 Case Series Case Series on Chronic Whiplash Related Neck Pain Treated with Intraarticular Zygapophysial Joint Regeneration Injection Therapy R. Allen Hooper
Oh, 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8
 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
Colossus Important Diagnoses. Instructions for How to List Diagnoses
 1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
The Neck: Whiplash & Central Ligament Sprains. Presented by Dr. Ben Benjamin
 Debilitating Orthopedic Injury Sampler #1 The Neck: Whiplash & Central Ligament Sprains Presented by Dr. Ben Benjamin Instructor: Ben Benjamin, Ph.D. 2 1 Instructor: Ben Benjamin, Ph.D. [email protected]
Debilitating Orthopedic Injury Sampler #1 The Neck: Whiplash & Central Ligament Sprains Presented by Dr. Ben Benjamin Instructor: Ben Benjamin, Ph.D. 2 1 Instructor: Ben Benjamin, Ph.D. [email protected]
A Case of Occipital Neuralgia
 A Case of Occipital Neuralgia Abstract Occipital Neuralgia (ON) is a rare form of headache characterised by paroxysms of stabbing pain in the distribution of the Greater or Lesser Occipital Nerves. Because
A Case of Occipital Neuralgia Abstract Occipital Neuralgia (ON) is a rare form of headache characterised by paroxysms of stabbing pain in the distribution of the Greater or Lesser Occipital Nerves. Because
Post Traumatic and other Headache Syndromes. Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA
 Post Traumatic and other Headache Syndromes Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA Over 45 million Americans have chronic, recurring headaches 62% of these
Post Traumatic and other Headache Syndromes Danielle L. Erb, MD Brain Rehabilitation Medicine, LLC Brain Injury Rehab Center, PRA Over 45 million Americans have chronic, recurring headaches 62% of these
THORACIC OUTLET SYNDROME
 THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
HEADACHE. as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D.
 HEADACHE as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D. Dpt. of Neurology Charles University in Prague, 2nd Faculty of Medicine Motol University Hospital History of headache 1200 years B.C.
HEADACHE as. MUDr. Rudolf Černý, CSc. doc. MUDr. Petr Marusič, Ph.D. Dpt. of Neurology Charles University in Prague, 2nd Faculty of Medicine Motol University Hospital History of headache 1200 years B.C.
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 [email protected] DISCLAIMER: The information in this booklet is compiled from a
A Patient s Guide to Carpal Tunnel Syndrome 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 [email protected] DISCLAIMER: The information in this booklet is compiled from a
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California.
 Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
Welcome to the July 2012 edition of Case Studies from the files of the Institute for Nerve Medicine in Santa Monica, California. In this issue, we focus on a 23-year-old female patient referred by her
The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches
 Cosmetic The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches Scott W. Mosser, M.D., Bahman Guyuron, M.D., Jeffrey E. Janis, M.D., and Rod J. Rohrich, M.D. Cleveland,
Cosmetic The Anatomy of the Greater Occipital Nerve: Implications for the Etiology of Migraine Headaches Scott W. Mosser, M.D., Bahman Guyuron, M.D., Jeffrey E. Janis, M.D., and Rod J. Rohrich, M.D. Cleveland,
Objectives AXIAL SKELETON. 1. Frontal Bone. 2. Parietal Bones. 3. Temporal Bones. CRANIAL BONES (8 total flat bones w/ 2 paired)
 Objectives AXIAL SKELETON SKULL 1. On a skull or diagram, identify and name the bones of the skull 2. Identify the structure and function of the bones of the skull 3. Describe how a fetal skull differs
Objectives AXIAL SKELETON SKULL 1. On a skull or diagram, identify and name the bones of the skull 2. Identify the structure and function of the bones of the skull 3. Describe how a fetal skull differs
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT
 C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT N u rten Inan, Aysegul Ceyhan, Levent Inan*, Ozlem Kavaklioglu, Alp Alptekin, Nurten Unal Ministry
C 2 / C 3 N E RVE BLOCKS AND GREATER OCCIPITAL NERVE BLOCK IN CERV I C O G E N I C HEADACHE TREATMENT N u rten Inan, Aysegul Ceyhan, Levent Inan*, Ozlem Kavaklioglu, Alp Alptekin, Nurten Unal Ministry
Whiplash and Cervical Spine Disorders: Evaluation and Management
 Whiplash and Cervical Spine Disorders: Evaluation and Management Dr. Corrie Graboski Definition by Quebec Task Force Pain Generators an acceleration-deceleration mechanism of energy transfer to the neck
Whiplash and Cervical Spine Disorders: Evaluation and Management Dr. Corrie Graboski Definition by Quebec Task Force Pain Generators an acceleration-deceleration mechanism of energy transfer to the neck
The Axial Skeleton Eighty bones segregated into three regions
 The Axial Skeleton Eighty bones segregated into three regions Skull Vertebral column Bony thorax Bones of the Axial Skeleton Figure 7.1 The Skull The skull, the body s most complex bony structure, is formed
The Axial Skeleton Eighty bones segregated into three regions Skull Vertebral column Bony thorax Bones of the Axial Skeleton Figure 7.1 The Skull The skull, the body s most complex bony structure, is formed
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Diagnosis of TMD and Associated Head Pain. Cortex Thalamus C 1 C 2 C 3. A Peer-Reviewed Publication Written by Steven R.
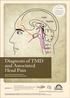 Cortex Thalamus Earn 3 CE credits This course was written for dentists, dental hygienists, and assistants. C 1 C 2 C 3 Diagnosis of TMD and Associated Head Pain A Peer-Reviewed Publication Written by Steven
Cortex Thalamus Earn 3 CE credits This course was written for dentists, dental hygienists, and assistants. C 1 C 2 C 3 Diagnosis of TMD and Associated Head Pain A Peer-Reviewed Publication Written by Steven
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011
 Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Chapter Thirteen MIGRAINE & PERIPHERAL NERVES
 Chapter Thirteen MIGRAINE & PERIPHERAL NERVES MIGRAINE HEADACHE!!!!!!. MIGRAINE & PHERIPERAL NERVES INTRODUCTION MIGRAINE HEADACHE!!!!!! You know what it is. That is not why you are reading this. You have
Chapter Thirteen MIGRAINE & PERIPHERAL NERVES MIGRAINE HEADACHE!!!!!!. MIGRAINE & PHERIPERAL NERVES INTRODUCTION MIGRAINE HEADACHE!!!!!! You know what it is. That is not why you are reading this. You have
WHIPLASH! Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT. Helpful and effective treatment with Neuromuscular Therapy. What does Whiplash mean?
 WHIPLASH! Helpful and effective treatment with Neuromuscular Therapy Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT What does Whiplash mean? Whiplash is a non-medical term used to describe neck pain
WHIPLASH! Helpful and effective treatment with Neuromuscular Therapy Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT What does Whiplash mean? Whiplash is a non-medical term used to describe neck pain
Whiplash injuries can be visible by functional magnetic resonance imaging. Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp.
 Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
SpineFAQs. Whiplash. What causes this condition?
 SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
Trigeminal Neuralgia. U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health
 Trigeminal Neuralgia U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Trigeminal Neuralgia What is trigeminal neuralgia? Trigeminal neuralgia (TN), also
Trigeminal Neuralgia U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Trigeminal Neuralgia What is trigeminal neuralgia? Trigeminal neuralgia (TN), also
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
A fresh, new, effective holistic approach to the age-old problem of treating headaches. Dr Prue King
 A fresh, new, effective holistic approach to the age-old problem of treating headaches Dr Prue King Just how big a problem are headaches? Headache disorders are among the most common disorders of the nervous
A fresh, new, effective holistic approach to the age-old problem of treating headaches Dr Prue King Just how big a problem are headaches? Headache disorders are among the most common disorders of the nervous
Notice of Independent Review Decision DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE:
 Notice of Independent Review Decision DATE OF REVIEW: 08/15/08 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for physical
Notice of Independent Review Decision DATE OF REVIEW: 08/15/08 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for physical
Temporo-Mandibular Joint Complex Exercise Suggestions
 Temporo-Mandibular Joint Complex Exercise Suggestions I. Exercise Generalizations: A. Patients with post-traumatic TMJ problems or with recent-onset dysfunction that is largely posture-related will generally
Temporo-Mandibular Joint Complex Exercise Suggestions I. Exercise Generalizations: A. Patients with post-traumatic TMJ problems or with recent-onset dysfunction that is largely posture-related will generally
Image-guided Spine Procedures for Relief of Severe Lower Back Pain:
 Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Image-guided Spine Procedures for Relief of Severe Lower Back Pain: A Guide to Epidural Steroid Injection, Facet Joint Injection, and Selective Nerve Root Block. PETER H TAKEYAMA MD HENRY WANG MD PhD SVEN
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Cervicogenic Headaches
 Cervicogenic Headaches Definition/Description Cervicogenic headaches refer to headache type sensations felt in the head and/face that originates from the neck, most commonly the upper cervical zygapophyseal
Cervicogenic Headaches Definition/Description Cervicogenic headaches refer to headache type sensations felt in the head and/face that originates from the neck, most commonly the upper cervical zygapophyseal
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Differential Diagnosis of Craniofacial Pain
 1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Hand Injuries and Disorders
 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
The Trigeminal and Facial Nerves The Facial and Blink
 The Trigeminal and Facial Nerves The Facial and Blink Introduction We commonly perform nerve conduction studies on three cranial nerves. Two of these, the trigeminal nerve (CN V) and the facial nerve (CN
The Trigeminal and Facial Nerves The Facial and Blink Introduction We commonly perform nerve conduction studies on three cranial nerves. Two of these, the trigeminal nerve (CN V) and the facial nerve (CN
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Selective Nerve Root Block
 Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons
 Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Low Back: Sacroiliac Dysfunction. Presented by Dr. Ben Benjamin
 Debilitating Orthopedic Injury Sampler #1 Low Back: Sacroiliac Dysfunction Presented by Dr. Ben Benjamin 1 Instructor: Ben Benjamin, Ph.D. 2 Instructor: Ben Benjamin, Ph.D. [email protected] 3 1 Thank
Debilitating Orthopedic Injury Sampler #1 Low Back: Sacroiliac Dysfunction Presented by Dr. Ben Benjamin 1 Instructor: Ben Benjamin, Ph.D. 2 Instructor: Ben Benjamin, Ph.D. [email protected] 3 1 Thank
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
WORKERS COMPENSATION BOARD APPEAL TRIBUNAL. [Personal information] CASE I.D. #[personal information]
![WORKERS COMPENSATION BOARD APPEAL TRIBUNAL. [Personal information] CASE I.D. #[personal information] WORKERS COMPENSATION BOARD APPEAL TRIBUNAL. [Personal information] CASE I.D. #[personal information]](/thumbs/25/6156167.jpg) WORKERS COMPENSATION BOARD APPEAL TRIBUNAL BETWEEN: [personal information] CASE I.D. #[personal information] PLAINTIFF AND: WORKERS COMPENSATION BOARD OF PRINCE EDWARD ISLAND DEFENDANT DECISION #41 [Personal
WORKERS COMPENSATION BOARD APPEAL TRIBUNAL BETWEEN: [personal information] CASE I.D. #[personal information] PLAINTIFF AND: WORKERS COMPENSATION BOARD OF PRINCE EDWARD ISLAND DEFENDANT DECISION #41 [Personal
Joint Pain: Wrist, Knee, Shoulder, Ankle, Elbow, TMJ
 Joint Pain: Wrist, Knee, Shoulder, Ankle, Elbow, TMJ 6 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Your wrist hurts when you bend
Joint Pain: Wrist, Knee, Shoulder, Ankle, Elbow, TMJ 6 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Your wrist hurts when you bend
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report
 Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
PAIN MANAGEMENT AT UM/SYLVESTER
 PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
PAIN MANAGEMENT AT UM/SYLVESTER W HAT IS THE PURPOSE OF THIS BROCHURE? We created this brochure for patients receiving care from the University of Miami Sylvester Comprehensive Cancer Center and their
Eastman Dental Hospital. Temporomandibular disorder. Facial Pain Team
 Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
WHIPLASH INJURIES By Prof RP Grabe, Department of Orthopaedics, University of Pretoria
 1 WHIPLASH INJURIES By Prof RP Grabe, Department of Orthopaedics, University of Pretoria In a recent publication in Spine the Quebec task force mentions that very little is available in the literature
1 WHIPLASH INJURIES By Prof RP Grabe, Department of Orthopaedics, University of Pretoria In a recent publication in Spine the Quebec task force mentions that very little is available in the literature
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
How To Find Out If You Can Get A Medical Expense Benefit From A Car Accident
 CASE NO. 18 Z 600 01641 03 2 A M E R I C A N A R B I T R A T I O N A S S O C I A T I O N NO-FAULT/ACCIDENT CLAIMS In the Matter of the Arbitration between (Claimant) AAA CASE NO.: 18 Z 600 01641 03 v.
CASE NO. 18 Z 600 01641 03 2 A M E R I C A N A R B I T R A T I O N A S S O C I A T I O N NO-FAULT/ACCIDENT CLAIMS In the Matter of the Arbitration between (Claimant) AAA CASE NO.: 18 Z 600 01641 03 v.
National Hospital for Neurology and Neurosurgery. Migraine associated dizziness Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
Any rapid head movement can cause a Whiplash. ALTERNATIVE CARE CHIROPRACTIC Reston, Virginia
 ALTERNATIVE CARE CHIROPRACTIC Reston, Virginia P ROV E N R E L I E F F RO M W H I P L A S H Any rapid head movement can cause a Whiplash injury. Although whiplash is commonly associated with car accidents
ALTERNATIVE CARE CHIROPRACTIC Reston, Virginia P ROV E N R E L I E F F RO M W H I P L A S H Any rapid head movement can cause a Whiplash injury. Although whiplash is commonly associated with car accidents
Pain Syndromes Acute Neck and Back Pain with or without arm or leg pain Chronic Neck and Back Pain with or without arm or leg pain
 Pain Syndromes The most common and best understood type of pain is acute pain. Acute pain will result when tissue is injured by trauma, surgery, illness, or infection. This type of pain is generally understood
Pain Syndromes The most common and best understood type of pain is acute pain. Acute pain will result when tissue is injured by trauma, surgery, illness, or infection. This type of pain is generally understood
TMJ Dysfunction & Pain
 TMJ Dysfunction & Pain The temporomandibular joints (TMJs) are two of the most functionally important and frequently used joints in the body. It is with these joints that important processes such as chewing,
TMJ Dysfunction & Pain The temporomandibular joints (TMJs) are two of the most functionally important and frequently used joints in the body. It is with these joints that important processes such as chewing,
A Look at Two Syndromes:
 TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
Neurovascular Orofacial Pain. Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that
 Neurovascular Orofacial Pain Introduction Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that a large population of patients with migraine and trigeminal autonomic
Neurovascular Orofacial Pain Introduction Orofacial pain of potential neurovascular origin may mimic odontogenic pain to the extent that a large population of patients with migraine and trigeminal autonomic
Neck Pain. www.physiofirst.org.uk
 Neck Pain www.physiofirst.org.uk Neck pain is common. The cause can be obvious like an accident or more subtle when related to a repetitive task or prolonged position. There are many triggers for neck
Neck Pain www.physiofirst.org.uk Neck pain is common. The cause can be obvious like an accident or more subtle when related to a repetitive task or prolonged position. There are many triggers for neck
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Upper Arm. Shoulder Blades R L B R L B WHICH SIDE IS MORE PAINFUL? (CERVICAL PAIN SIDE) RIGHT LEFT EQUAL NOT APPLICABLE (N/A) CERVICAL.
 1 NECK PAIN Patient Name In order to properly assess your condition, we must understand how much your NECK/ARM problems has affected your ability to manage everyday activities. For each item below, please
1 NECK PAIN Patient Name In order to properly assess your condition, we must understand how much your NECK/ARM problems has affected your ability to manage everyday activities. For each item below, please
