Proton Pump Inhibitors vs. Histamine 2 -Receptor Antagonists for Stress Ulcer Prophylaxis Battle of the Acid Suppressants
|
|
|
- Imogen Hannah Walton
- 8 years ago
- Views:
Transcription
1 Proton Pump Inhibitors vs. Histamine 2 -Receptor Antagonists for Stress Ulcer Prophylaxis Battle of the Acid Suppressants Andrew J. Burris, Pharm.D. PGY1 Pharmacy Resident University Health System, San Antonio, Texas Division of Pharmacotherapy, The University of Texas at Austin College of Pharmacy Pharmacotherapy Education and Research Center, University of Texas Health Science Center at San Antonio February 7, 2014 Learning Objectives: 1. Describe the pathophysiology associated with stress-related mucosal disease 2. Identify appropriate indications for stress ulcer prophylaxis 3. Identify when stress ulcer prophylaxis should be discontinued 4. Evaluate the safety and efficacy associated with histamine 2 -receptor antagonists and proton pump inhibitors
2 Stress-Related Mucosal Disease I. What is stress-related mucosal disease (SRMD)? 1-3 A. Acute superficial inflammatory lesions of the gastric mucosa B. Occurs during critical illness C. Continuum of manifestations Stress-Related Injury Involves superficial mucosal damage Primarily erosions Stress Ulcer Involve focal deep mucosal damage High risk for bleeding Figure 1. Stress-Related Mucosal Disease Progression 2 II. Definitions of gastrointestinal (GI) bleeding A. Occult bleeding 4 i. Not visible to naked eye ii. Detected via guaiac test B. Overt bleeding 4 i. Visible to naked eye ii. Examples include hematemesis, hematochezia, and coffee ground aspiration C. Clinically-significant bleeding 5 i. Overt bleeding complicated by: 1. Hemodynamic instability 2. Decreased hemoglobin requiring blood transfusion ii. Should be used as outcome measure for all trials iii. Increased morbidity and mortality 6 1. Increase intensive care unit (ICU) length of stay by 11 days 2. Mortality increased seven-fold III. What is the incidence of SRMD in the ICU? 1 A % of patients have endoscopically detectable mucosal damage within 24 hours 6,7 B. Up to 25% of patients develop overt gastric bleeding 6 D. Clinically-significant GI bleeding ranges from 0.6-5% 6 Burris AJ Page 2
3 IV. Pathophysiology of SRMD 1,3 Critical Illness Cardiac output Catecholamines vasoconstriction Proinflammatory cytokine release Splanchnic hypoperfusion GI motility Mucosal ischemia Acid back diffusion Reduced HCO 3 secretion Impaired mucous production Acute stress ulcer Figure 2. Pathophysiology of Stress Ulcers 3 V. What are the risk factors associated with SRMD? 1-4,7 A. Cook et al. 5 prospective, multicenter cohort study i. 2,252 ICU patients evaluated for potential risk factors for stress ulceration ii. Two independent risk factors 1. Respiratory failure 2. Coagulopathy iii. Low incidence of clinically-significant bleeding 1. Patients with one or both independent risk factor(s) 3.7% 2. Patients with neither risk factor 0.1% B. Hastings et al. 8 randomized 100 patients at risk for stress ulcers to prophylaxis vs. no prophylaxis i. Increased risk of bleeding with increasing number of risk factors Burris AJ Page 3
4 Table 1. Risk Factors for SRMD 5 Mechanical ventilation >48 hours* Coagulopathy* INR >1.5 PTT >2 times control value Platelet count <50,000 Hypotension Severe sepsis Hepatic failure Spinal cord injury Hepatic or renal transplantation Thermal injury (>35% body surface area) Multiple trauma with Injury Severity Score 16 General (medical, surgical, respiratory) ICU populations Head injury (GCS 10) or inability to obey simple commands History of gastric ulceration or bleeding during the year before admission Presence of at least 2 of the following: Sepsis ICU stay >1 week Occult bleeding for 6 days Corticosteroid therapy (>250 mg of hydrocortisone or equivalent daily) *Independent risk factors; INR, International Normalized Ratio; PTT, Partial Thromboplastin Time; GCS, Glasgow Coma Scale Stress Ulcer Prophylaxis I. What are the indications for stress ulcer prophylaxis (SUP) in ICU patients? 1 A. Prophylaxis only recommended for subset of ICU patients (Table 1) B. Discontinue when risk factors have resolved II. What is the role for SUP in the non-icu setting? 1 A. Qadeer et al. 9 (n=17,707 patients admitted to general medicine service) i. Incidence of hospital-acquired GI bleeding 0.4% ii. No protective benefit seen with prophylactic use iii. Rates of bleeding and all-cause mortality similar between two groups B. SUP not routinely indicated in this population st reported case series of SRMD 1983 FDA approved ranitidine CSB ranged from % 2000 FDA approved omeprazole & pantoprazole 2010 s CSB reported incidence 5% 6% 1970 s CSB ranged from 5.3% - 33% 1977 FDA approved cimetidine 1986 FDA approved famotidine 1995 FDA approved lansoprazole Figure 3. Stress Ulcer Prophylaxis Timeline 10, FDA approved esomeprazole CSB: clinically significant bleeding; FDA: Food and Drug Administration Burris AJ Page 4
5 III. Why did the incidence of bleeding change over time? 1,4 A. Enteral feeding B. Low tidal volume ventilation C. Prompt and adequate fluid resuscitation IV. What are the options for SUP? 1-4 A. Antacids i. Mechanism of action (MOA) 1. Directly buffer or neutralize acid contents of stomach ii. Efficacy 1. Hastings et al. 8 randomized 100 patients at risk for stress ulcers a. Prophylaxis with antacids vs. no prophylaxis b. Decreased bleeding rate when antacid therapy titrated to ph >3.5 (p<0.005) iii. Limitations 1. Administered every 1-2 hours for adequate acid neutralization 2. High dose antacids increase risk of aspiration pneumonia and toxicity a. Highest risk in patients with renal dysfunction B. Sucralfate i. MOA 1. Adheres to epithelial cells and forms protective barrier 2. No acid-neutralizing activity ii. Efficacy 1. Cook et al. 12 randomized 1,200 ICU patients to intravenous (IV) ranitidine vs. sucralfate a. Clinically significant GI bleeding higher in the sucralfate group (3.8%) vs. ranitidine (1.7%) group (p=0.02) b. No significant difference in the incidence of pneumonia iii. Limitations 1. Constipation 2. Hypophosphatemia 3. Nasogastric tube occlusion 4. Aluminum toxicity (chronic renal insufficiency) 5. Decreased absorption of concomitantly administered oral medications C. Histamine 2 -receptor antagonists (H 2 RAs) i. MOA (Figure 4) 1. Inhibit histamine-stimulated acid secretion by blocking H 2 -receptor 2. Highly selective with little or no effect on other histamine receptors ii. Efficacy 1. H 2 RAs are significantly better than placebo, antacids and sucralfate 9 2. Proton pump inhibitors vs. H 2 RAs to be determined (TBD) iii. Adverse effects 1. Tolerance 2. Drug Interactions a. Cimetidine = primary offender b. Inhibition of cytochrome P450s 3. Thrombocytopenia 4. Renal dysfunction requires dose adjustment Burris AJ Page 5
6 iv. Agents 1. Ranitidine (Zantac ) 2. Famotidine (Pepcid ) 3. Cimetidine (Tagamet ) D. Proton pump inhibitors (PPIs) i. MOA (Figure 4) 1. Inhibit gastric acid secretion by inhibition of H + /K + ATPase pump ii. Efficacy 1. PPIs vs. H 2 RAs TBD iii. Adverse effects 1. Drug interactions 2. Hypomagnesemia 3. Increased risk of infection 4. Acute interstitial nephritis iv. Warnings/Precautions 1. Bone fracture 2. Hypomagnesemia 3. Vitamin B 12 deficiency 4. Clostridium difficile-associated diarrhea v. Agents 1. Omeprazole (Prilosec ) 2. Pantoprazole (Protonix ) 3. Esomeprazole (Nexium ) 4. Lansoprazole (Prevacid ) 5. Rabeprazole (Aciphex ) ACh M 3 Gastrin Histamine CCK 2 + K H+/K+ ATPase H + Proton pump inhibitors H 2 receptorantagonists H 2 Parietal cell Gastric lumen ph 2 Figure 4. Mechanism of Action for H 2 RAs & PPIs 13 Burris AJ Page 6
7 Discontinuation of Stress Ulcer Prophylaxis I. Is SUP used appropriately in the inpatient setting? 1 A. Patients who are critically-ill with zero risk factors 70% receive SUP B. Original risk factors resolve SUP is continued after ICU downgrade C. SUP often used in medicine patients and continued on hospital discharge II. What is the economic impact of the inappropriate use of SUP? 1 A. Substantial economic impact on the overuse of SUP i. Heidelbaugh et al. 14 (n=1,769 general medicine patients) 1. Inappropriate SUP use increased annual inpatient and outpatient costs $111,791 ii. Managed care organization ,000 patients prescribed PPI inappropriately at hospital discharge 2. Inappropriate continuation for 30 days associated with cost of US $3 million over four years iii. Neither study accounted for costs incurred from complications of SUP III. What strategies can reduce the overuse of SUP? 1 A. Few studies have explored potential solutions B. Interventions that improve prescribing patterns i. Educational materials ii. Daily medication reconciliation iii. Pharmacist participation on rounds C. Additional strategies i. Reevaluate use of H 2 RAs and PPIs on standardized order sets ii. Integrate decision-making prompts into the electronic medical record D. Quality improvement studies are needed Burris AJ Page 7
8 What is the efficacy associated with PPIs and H 2 RAs? Table 2. Meta-Analyses Evaluating Safety and Efficacy of PPIs vs. H 2 RAs for SUP Lin PC et al Barkun AN et al Alhazzani W et al Objective To examine the efficacy and safety of PPIs vs. H 2 RAs for stress-related upper GI bleeding Study Selection Published Articles - 5 Powell 1993 Levy 1997 Kantorova 2004 Conrad 2005 Somberg 2008 Abstracts - 2 Phillips 1998 Azevedo 1999 Published Articles 8 Powell 1993 Levy 1997 Kantorova 2004 Conrad 2005 Somberg 2008 Hata 2005 Solouki 2009 Brophy 2010 Abstracts - 5 Phillips 1998 De Azevedo 2000 Morris 2001 Fink 2003 Pan 2004 Published Articles - 10 Powell 1993 Levy 1997 Kantorova 2004 Conrad 2005 Somberg 2008 Hata 2005 Solouki 2009 Azevedo 2000 Pan 2004 Risaliti 1993 Abstracts 4 Phillips 1998 Morris 2001 Fink 2003 Kotlyanskaya 2007 N 936 1,587 1,720 Inclusion Studies directly comparing any PPIs vs. any H 2 RAs (any drug, dose, or route of administration) Exclusion Primary Outcome Secondary Outcome Statistics Results Studies using placebo, antacids or sucralfate rather than H 2 RAs for comparator Incidence of stress-related upper GI bleeding Pneumonia ICU mortality Random effect model I 2 statistic to assess heterogeneity Pre-planned sensitivity & subgroup analysis Funnel plot to assess publication bias No difference in 1 o or 2 o outcomes (Pooled risk difference 0.04; 95% CI, to 0.01; p=0.08; I 2 =66%) Trials comparing different dosing regimens of the same molecule Rate of clinically significant upper GI bleeding Nosocomial Pneumonia All-cause mortality ICU LOS Fixed effect model I 2 statistic to assess heterogeneity Pre-planned sensitivity analysis Funnel plot to assess publication bias PPIs>H 2 RAs for 1 o outcome (OR 0.30; 95% CI, ) No difference in 2 o outcomes NNT N/A I. Critique of meta-analyses A. Low quality studies i. Levy et al. 19 compared omeprazole to ranitidine 1. Included in all three meta-analyse 2. Clinically-significant bleeding appropriately defined 3. Differing number of risk factors between groups a. Ranitidine (2.7) vs. omeprazole (1.9) (p<0.05) Other interventions Pediatric population Observational studies Clinically important GI bleeding Overt upper GI bleeding Nosocomial pneumonia All-cause mortality ICU LOS Clostridium difficile infection Random effect model I 2 statistic to assess heterogeneity Pre-planned sensitivity & subgroup analysis Funnel plot to assess publication bias PPIs>H 2 RAs for 1 o outcome (RR 0.36; 95% CI, ; p=0.002; I 2 =0%) No difference in 2 o outcomes No trials reported on C. difficile Burris AJ Page 8
9 4. High incidence of bleeding a. Ranitidine (31%) vs. omeprazole (6%) (p<0.05) b. Higher than reported rate (0-16%) from other studies c. Barkun et al. reported overall incidence of 1.3% 5. Study accounted for 20% of weight ii. Brophy et al. 20 compared lansoprazole to famotidine 1. Only included in meta-analysis by Barkun et al. 2. Clinically-significant bleeding appropriately defined a. Only overt bleeding reported 3. Clinically-significant bleeding is secondary outcome a. Study not powered for outcome B. Definitions of bleeding i. Variable from study to study ii. Few studies appropriately define clinically-significant bleeding iii. In Barkun et al studies have no definition C. Data quality i. Positives 1. Funnel plot performed 2. All assessed heterogeneity 3. Sensitivity and subgroup analysis preformed 4. Trial quality assessed a. Higher quality studies showed smaller treatment effect ii. Negatives 1. Heterogeneity seen in Lin et al. a. No heterogeneity seen in Barkun et al. 17 and Alhazzani et al. 18 b. Five studies and one abstract included in all three meta-analysis 2. 40% of patients included low risk of clinically significant bleeding 3. Publication/language bias seen via funnel plots II. Take home points A. Majority of studies included in meta-analyses did not appropriately define clinicallysignificant bleeding B. Significant heterogeneity among studies with regard to risk difference C. Superior efficacy of PPIs compared to H 2 RAs is difficult to support with current available evidence What are the risks associated with PPIs and H 2 RAs? I. PPIs are one of the most commonly prescribed classes of drugs worldwide 21 A. Sales totaling US $26.9 billion dollars in B. Experts generally view PPIs as safe C. Potential complications ( risk of infection) have caused concern II. Community-acquired pneumonia (CAP) 22 A. Proposed mechanisms i. Increase in gastric ph bacterial overgrowth and colonization 1. Subsequent translocation to lungs by aspiration Burris AJ Page 9
10 ii. H + /K + ATPase also present in the respiratory tract 1. PPIs may alter ph of seromucinous secretions bacterial growth iii. Acid-suppressive drugs may impair function of neutrophils and natural killer cells 23 Table 3. Studies Evaluating the Risk of CAP with PPIs & H 2 RAs 24,25 Laheij RJ et al Gulmez SE et al Objective To examine the association between the use of acid-suppressive drugs and the risk of PNA Study Design Nested case-control Case-control N 364,683 34,176 Patient Population Primary care setting, data collected via IPCI Inpatient setting, data collected via County of Funen Inclusion One year history of valid database history No use of acid suppression before enrollment Cases defined by first admission with CAP Index date = first registered date of CAP diagnosis Exclusion Diagnosis of PNA in preenrollment period (1 year) Statistics Nested case-control analysis preformed to confounders o 10 controls from cohort matched with each case of PNA o Matched on sex, year of birth, & index date (date of first PNA) RR of PNA estimated with OR & adjusted for all covariates Results 19,459* received 1 st Rx for acid-suppression o H 2 RAs: n=10,177 o PPIs: n=2,337 Pneumonia risk o PPIs & H 2 RAs: adjusted OR, 1.27 (95% CI, ) o PPIs alone: adjusted OR, 2.2 (95% CI, ) Significant dose response observed o H 2 RAs alone: adjusted OR, 1.7 (95% CI, ) No dose response observed NNH PPIs = 226 H 2 RAs = 508 Critique Large case-control study o Appropriate for study on adverse effect Nested analysis conducted to confounders Higher risk when evaluating only laboratoryconfirmed PNA risk most pronounced with PPI use o Dose-response relationship NNH calculated for H 2 RAs with no statistical significance Diagnosis of malignancy, recent d/c in last 7 days Controls randomly extracted from population Matched by age & sex to the cases with a 4:1 ratio Logistic regression to estimate crude & adjusted ORs Stratified analyses were conducted by: o Age o Dose of PPI o Recency of PPI 7,642 cases met inclusion/exclusion criteria o H 2 RAs: n=161 o PPIs: n=817 Pneumonia risk o PPIs alone: adjusted OR, 1.5 (95% CI, ) Associating current use with CAP Highest risk in first 7 days (OR, 5.0; 95% CI, ) o H 2 RAs alone: adjusted OR, 1.1 (95% CI, ) No definite association found PPIs = 6 H 2 RAs = N/A Large case-control study o Appropriate for study on adverse effect risk of CAP with PPI use Highest risk seen in first seven days No association observed in H 2 RA users PNA, pneumonia; IPCI, Integrated Primary Care Information; RR, relative risk; OR, odds ratio; Rx, prescription; CI, confidence interval; d/c, discharge; N/A, not applicable; *Some patients used both H 2RAs plus PPIs Burris AJ Page 10
11 B. Take home points i. Increased risk of CAP observed with PPI use and no risk observed in H 2 RA users ii. Most pronounced risk seen in current users of PPIs and higher doses iii. Case-control study and meta-analysis report consistent results 26,27 III. Nosocomial pneumonia (PNA) A. Proposed mechanisms i. Same proposed mechanisms as CAP Table 4. Studies Evaluating the Risk of Nosocomial Pneumonia with PPIs & H 2 RAs 22,28 Miano TA et al Eom CS et al Objective To determine whether SUP with PPI PNA risk compared with H 2 RA To examine the association between acid-suppressive medication and PNA Study Design Retrospective cohort analysis Meta-analysis 31 studies o 5 case-control o 3 cohort studies o 23 randomized controlled trials N 834 Observational studies: n=1,965,358 RCTs: n=4,168 Patient Population Inclusion Exclusion Statistics Critically ill patients Cardiothoracic surgery patients All patients receiving acid-suppressive therapy Age > 18 years Admitted to cardiothoracic surgery service Received either pantoprazole or ranitidine without crossover Documented aspiration during hospital admission Diagnosis of PNA within preceding 3 months History of immunosuppression Diagnosis of HIV infection Recent SOT Propensity score analysis to balance the distribution of covariates Multivariate logistic regression model to control for selection bias Mixed Eight observational studies o Five evaluating risk of CAP o Three evaluating risk of HAP o Evaluating risk of PNA with PPIs RCTs o ICU setting o Evaluating risk of HAP with H 2 RAs Case-control study, cohort study or RCT; investigating the association between acid- suppressive drugs and risk of PNA Study did not include data about risk of PNA Results for PPIs and H 2 RAs not reported separately Observational studies o Pooled OR & 95% CI from the adjusted ORs & 95% CIs reported in studies RCTs o Summary relative risk from the relative risks of individual trials Higgins I 2 used to assess heterogeneity Random-effects model for overall effect Burris AJ Page 11
12 Table 4. (Continued) Studies Evaluating the Risk of Nosocomial Pneumonia with PPIs & H 2 RAs Miano TA et al Eom CS et al Results 834 patients o PPIs: n=377 o H 2 RAs: n=457 Nosocomial PNA incidence o Pantoprazole: n=35 (9.3%) o Ranitidine: n=7 (1.5%) Unadjusted OR, 6.6 (95% CI, ) o Propensity adjusted, multivariable linear regression found pantoprazole to be independent risk factor Adjusted OR, 2.7 ( 95% CI, ; p=0.034) Observational studies o PPI use risk of PNA o Adjusted OR, 1.27 (95% CI, ) RCTs o H 2 RA use risk of HAP o RR 1.22 (95% CI, ) Subgroup analysis o Higher dose of PPIs more strongly associated with PNA o Highest risk seen in first seven days Adjusted OR, 3.95 (95% CI, ) o Among high-quality RCTs no risk of PNA seen with H 2 RAs RR 0.96 (95% CI, ) NNH PPIs = 13 Acid-suppression = 200 Critique Large comparison of PPIs & H 2 RAs in critical care population Propensity sore methodology was used to balance covariate distribution Results may not apply to other populations Large meta-analysis including RCTs & observational studies When looking at high quality RCTs no risk observed with H 2 RA use Risk of PNA still seen in high quality observational studies Use of acid-suppressive drugs associated with risk of PNA SUP, stress ulcer prophylaxis; PPI, proton pump inhibitor; PNA, pneumonia; H 2RA, histamine 2-receptor antagonist; CAP, community-acquired pneumonia; HAP, hospital-acquired pneumonia; RCTs, randomized controlled trials; HIV, human immunodeficiency virus; SOT, solid organ transplant; OR, odds ratio; CI, confidence interval; RR, relative risk B. Take home points i. PPI use associated with increased risk of nosocomial PNA in ICU setting ii. Results echo CAP studies with highest risk in recent users and higher doses iii. Results of high-quality RCTs did not find an increased risk of PNA with H 2 RAs IV. Clostridium difficile infection (CDI) 21 A. Proposed mechanism i. gastric ph > 4 allows 50% of ingested bacteria to escape acid barrier ii. Disruption in natural gut bacteria 1. Lack of destruction of ingested microorganism 2. ascending bacterial colonization from the intestine Burris AJ Page 12
13 Table 5. Studies Evaluating the Risk of Clostridium difficile Infection with PPIs & H 2 RAs 29,30 Objective Study Design Beaulieu M et al Kwok CS et al To determine if PPIs & H 2 RAs are risk factors for CDAD in hospitalized ICU patients Cohort study C. difficile (+) MICU patients To evaluate risk of CDI with PPI use To evaluate risk of CDI with PPI use + abx To evaluate risk of CDI with H 2 RAs Meta-analysis 42 observational studies o 30 case-control o 12 cohort N ,000 Inclusion MICU admission 24 hours CDAD (+) o Diarrhea 24 hours o Enzyme immunoassay (+) for C. difficile toxins A & B Studies that reported OR/RR for CDI with PPI use or Reported sufficient raw data to calculate OR/RR Exclusion CDAD diagnosed before study period Studies not evaluating PPI use and risk of CDI Statistics Results Kaplan-Meier curves constructed o Day 0 = day of MICU admission Multivariate logistic regression model 335 (40.5%) patients received PPI 470 (56.8%) patients received H 2 RA 182 (22%) patients received no acid suppression Kaplan-Meier analysis o Clindamycin HR, 2.06 (95% CI, ) p 0.05 o Macrolide HR, 1.85 (95% CI, ) p 0.05 Independent risk factors o Age 65 years HR, 2.33 (95% CI, ) p 0.01 o Female sex HR, 1.68 (95% CI, ) p 0.01 No significant difference in PPIs & H 2 RAs o PPIs HR, 0.90 (95% CI, ) o H 2 RAs HR, 0.78 (95% CI, ) NNH N/A PPIs = 67 H 2 RAs = 121 PPIs + abx = 22 NNT N/A PPIs H 2 RAs = 69 Critique Risk of CDAD assessed in the ICU setting o Limited data in this setting where SUP is mostly indicated No significant difference between no prophylaxis & PPI/H 2 RA use Identified risk factors for developing CDAD o Women o Older age ( 65 years) o Clindamycin/macrolide exposure Random effect model I 2 statistic to assess heterogeneity o 30-60% moderate Prespecified subgroup analysis Rothman synergy index o Assessing PPI + antibiotic risk Risk of CDI with PPI use o 39 studies o OR 1.74 (95% CI, ; p<0.001; I 2 = 85%) Risk of recurrent CDI with PPI use o 3 studies o OR 2.51 (95% CI, ; p = 0.02; I 2 = 78%) Risk of CDI with PPI use & abx o 6 studies o OR 1.96 (95% CI, ) o Rothman s synergy index 1.36 o Attributable proportion of risk 19% Risk of CDI with H 2 RAs* o 15 studies o OR 0.71 (95% CI, ) Large meta-analysis of observational studies o Appropriate for study on adverse effects PPI use associated with a 74% risk of CDI Pooled analysis showed risk of recurrent CDI Unexplained significant heterogeneity among studies No asymmetry testing performed to assess publication bias CDAD, Clostridium difficile-associated disease; MICU, medical ICU; CDI, Clostridium difficile infection; PPI, proton pump inhibitor; abx, antibiotic; H 2RAs, histamine 2-receptor antagonists; OR, odds ratio; RR, risk ratio; CI, confidence interval; *In comparison to PPIs Burris AJ Page 13
14 B. Take home points i. Conflicting results ii. Significant unexplained heterogeneity also observed in Janarthanan et al Janarthanan et al. 31 conducted a meta-analysis (n=288,620) to summarize the association between CDAD and PPIs 2. Included similar studies as Kwok et al. 30 and heterogeneity unexplained by subgroup analysis 3. Results showed a 65% increase in incidence of CDAD among PPI users iii. PPI use may be associated with an increase risk of CDI and recurrent CDI 1. Quality of evidence is low interpret cautiously V. Summary of risks A. Studies have demonstrated association but not causality B. All associated risks were greater with PPIs as compared to H 2 RAs C. PPIs have also been linked to potential long-term side effects or complications 21 i. Fracture risk ii. Iron deficiency iii. Hypomagnesaemia iv. Vitamin B 12 deficiency D. Many evaluations did not find a risk with H 2 RAs Table 6. Potential Adverse Effects with PPIs 21 Adverse effect Underlying mechanism Strength of association CAP Plausible Weak to moderate OR > 2 Nosocomial Plausible Weak to PNA moderate OR > 2 C. difficile Infection Plausible Weak to moderate OR > 2 Consistency of association Inconsistent results Inconsistent results Inconsistent results CAP, community-acquired pneumonia; PNA, pneumonia; CDI, Clostridium difficile infection; OR, odds ratio Summary and Recommendations Clinical implications PPI therapy should only be used for appropriate indications PPI therapy should only be used for appropriate indications Consider potential alternative therapy in patients with concurrent CDI risk factors I. Summary A. SUP is important in preventing clinically significant bleeding B. Acid suppressive therapy is not indicated in everyone C. Discontinuation of SUP is warranted when original risk factors resolve D. Limitations of current available evidence make it difficult to claim PPIs as the superior agent E. Increases in gastric ph are associated with an increase risk of infection i. CAP Management of an uncomplicated case of PNA costs approximately US $7,000 dollars 2. 40% attributable mortality in patients requiring admission to an ICU Burris AJ Page 14
15 ii. Nosocomial pneumonia Hospital-acquired pneumonia (HAP) has an associated cost of more than US $40,000 dollars 2. Overall mortality attributed to HAP may be as high as 50% iii. Clostridium difficile infection % attributable mortality in critically ill patients Table 7. Comparison of Number Needed to Harm with PPIs and Attributable Mortality in ICU Patients CAP Nosocomial PNA Clostridium difficile Infection NNH N=6 Attributable Mortality NNH N=13 Attributable Mortality NNH N=22 Attributable Mortality II. Recommendations A. With advancements in medicine SUP may no longer be required B. Healthcare professionals should weigh the risks and benefits when choosing an agent for SUP C. If SUP is indicated, histamine 2 -receptor antagonists are the preferred agent of choice Burris AJ Page 15
16 References 1. Anderson ME. Stress Ulcer Prophylaxis in Hospitalized Patients. Hosp Med Clin. 2013;2:e32-e Spirt MJ. Stress-related mucosal disease: risk factors and prophylactic therapy. Clin Ther. 2004;26: Stollman N, Metz DC. Pathophysiology and prophylaxis of stress ulcer in intensive care unit patients. J Crit Care. 2005;20: Laine L. Chapter 41. Gastrointestinal Bleeding. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson J, Loscalzo J. eds. Harrison's Principles of Internal Medicine, 18e. New York: McGraw- Hill; id= Accessed January 03, Cook DJ, Fuller HD, Guyatt GH, et al. Risk factors for gastrointestinal bleeding in critically ill patients. Canadian Critical Care Trials Group. N Engl J Med. 1994;330: Mutlu GM, Mutlu EA, Factor P. GI complications in patients receiving mechanical ventilation. Chest. 2001;119: Grube RR, May DB. Stress ulcer prophylaxis in hospitalized patients not in intensive care units. Am J Health-Syst Pharm. 2007;64: Hastings PR, Skillman JJ, Bushnell LS, Silen W. Antacid titration in the prevention of acute gastrointestinal bleeding: a controlled, randomized trial in 100 critically ill patients. N Engl J Med. 1978;298: Qadeer MA, Richter JE, Brotman DJ. Hospital-acquired gastrointestinal bleeding outside the critical care unit: risk factors, role of acid suppression, and endoscopy findings. J Hosp Med. 2006;1: ASHP Therapeutic Guidelines on Stress Ulcer Prophylaxis. ASHP Commission on Therapeutics and approved by the ASHP Board of Directors on November 14, Am J Health-Syst Pharm. 1999;56: Lucas CE, Sugawa C, Riddle J, Rector F, Rosenberg B, Walt AJ. Natural history and surgical dilemma of "stress" gastric bleeding. Arch Surg. 1971;102: Cook D, Guyatt G, Marshall J, et al. A comparison of sucralfate and ranitidine for the prevention of upper gastrointestinal bleeding in patients requiring mechanical ventilation. Canadian Critical Care Trials Group. N Engl J Med. 1998;338: Wallace JL, Sharkey KA. Chapter 45. Pharmacotherapy of Gastric Acidity, Peptic Ulcers, and Gastroesophageal Reflux Disease. In: Brunton LL, Chabner BA, Knollmann BC. eds. Goodman & Gilman's The Pharmacological Basis of Therapeutics, 12e. New York: McGraw-Hill; id= Accessed January 30, Heidelbaugh JJ, Inadomi JM. Magnitude and economic impact of inappropriate use of stress ulcer prophylaxis in non-icu hospitalized patients. Am J Gastroenterol. 2006;101: Thomas L, Culley EJ, Gladowski P. Longitudinal analysis of the costs associated with inpatient initiation and susbsequent outpatient continuation of proton pump inhibitor therapy for stress ulcer prophylaxis in a large managed care organization. J Manag Care Pharm. 2010;16: Lin PC, Chang CH, Hsu PI, Tseng PL, Huang YB. The efficacy and safety of proton pump inhibitors vs histamine-2 receptor antagonists for stress ulcer bleeding prophylaxis among critical care patients: a meta-analysis. Crit Care Med. 2010;38: Burris AJ Page 16
17 17. Barkun AN, Bardou M, Pham CQ, Martel M. Proton pump inhibitors vs. histamine 2 receptor antagonists for stress-related mucosal bleeding prophylaxis in critically ill patients: a metaanalysis. Am J Gastroenterol. 2012;107:507-20; quiz Alhazzani W, Alenezi F, Jaeschke RZ, Moayyedi P, Cook DJ. Proton pump inhibitors versus histamine 2 receptor antagonists for stress ulcer prophylaxis in critically ill patients: a systematic review and meta-analysis. Crit Care Med. 2013;41: Levy MJ, Seelig CB, Robinson NJ, Ranney JE. Comparison of omeprazole and ranitidine for stress ulcer prophylaxis. Dig Dis Sci. 1997;42: Brophy GM, Brackbill ML, Bidwell KL, Brophy DF. Prospective, randomized comparison of lansoprazole suspension, and intermittent intravenous famotidine on gastric ph and acid production in critically ill neurosurgical patients. Neurocrit Care. 2010;13: Reimer C. Safety of long-term PPI therapy. Best Pract Res Clin Gastroenterol. 2013;27: Eom CS, Jeon CY, Lim JW, Cho EG, Park SM, Lee KS. Use of acid-suppressive drugs and risk of pneumonia: a systematic review and meta-analysis. CMAJ. 2011;183: Zedtwitz-Liebenstein K, Wenisch C, Patruta S, Parschalk B, Daxbock F, Graninger W. Omeprazole treatment diminishes intra- and extracellular neutrophil reactive oxygen production and bactericidal activity. Crit Care Med. 2002;30: Laheij RJ, Sturkenboom MC, Hassing RJ, Dieleman J, Stricker BH, Jansen JB. Risk of communityacquired pneumonia and use of gastric acid-suppressive drugs. JAMA. 2004;292: Gulmez SE, Holm A, Frederiksen H, Jensen TG, Pedersen C, Hallas J. Use of proton pump inhibitors and the risk of community-acquired pneumonia: a population-based case-control study. Arch Intern Med. 2007;167: Sarkar M, Hennessy S, Yang YX. Proton-pump inhibitor use and the risk for community-acquired pneumonia. Ann Intern Med. 2008;149: Johnstone J, Nerenberg K, Loeb M. Meta-analysis: proton pump inhibitor use and the risk of community-acquired pneumonia. Aliment Pharmacol Ther. 2010;31: Miano TA, Reichert MG, Houle TT, MacGregor DA, Kincaid EH, Bowton DL. Nosocomial pneumonia risk and stress ulcer prophylaxis: a comparison of pantoprazole vs ranitidine in cardiothoracic surgery patients. Chest. 2009;136: Beaulieu M, Williamson D, Pichette G, Lachaine J. Risk of Clostridium difficile-associated disease among patients receiving proton-pump inhibitors in a Quebec medical intensive care unit. Infect Control Hosp Epidemiol. 2007;28: Kwok CS, Arthur AK, Anibueze CI, Singh S, Cavallazzi R, Loke YK. Risk of Clostridium difficile infection with acid suppressing drugs and antibiotics: meta-analysis. Am J Gastroenterol. 2012;107: Janarthanan S, Ditah I, Adler DG, Ehrinpreis MN. Clostridium difficile-associated diarrhea and proton pump inhibitor therapy: a meta-analysis. Am J Gastroenterol. 2012;107: Tejerina E, Frutos-Vivar F, Restrepo MI, et al. Prognosis factors and outcome of communityacquired pneumonia needing mechanical ventilation. J Crit Care. 2005;20: American Thoracic S, Infectious Diseases Society of A. Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005;171: Kenneally C, Rosini JM, Skrupky LP, et al. Analysis of 30-day mortality for clostridium difficileassociated disease in the ICU setting.[erratum appears in Chest Nov;132(5):1721 Note: McKenzie, Wendi [corrected to McKinzie, Wendi E]]. Chest. 2007;132: Burris AJ Page 17
18 Appendix Appendix A. Summary of Individual Studies Included in Meta-Analyse Study N Intervention Definition of Bleeding Outcomes Powell et al Omeprazole 80 mg IV bolus, then 40 mg IV bolus TID (n=10); omeprazole 80 mg IV bolus then 40 mg IV infusion TID (n=10); ranitidine 50 mg IV TID (n=11); placebo (n=10) Bloody nasogastric tube aspirate Clinically important bleeding; mortality Levy et al Kantorova et al Conrad et al Somberg et al Hata et al Solouki et al Azevedo et al Omeprazole 40 mg NG daily (n=32); ranitidine 50 mg IV bolus, then 150 mg IV daily (n=35) 287 Omeprazole 40 mg IV daily (n=72); famotidine 40 mg IV BID (n=71); sucralfate 1 g NG QID (n=69); placebo (n=75) 359 Omeprazole suspension 40 mg NG BID loading, then 40 mg NG daily (n=178); cimetidine 300 mg IV bolus, then infusion at 50 mg/hr (n=181) 202 Pantoprazole 40 mg IV daily (n=32); pantoprazole 40 mg IV BID (n=38); pantoprazole 80 mg IV daily (n=23); pantoprazole 80 mg IV BID (n=39); pantoprazole 80 mg IV TID (n=35); cimetidine 300 mg IV bolus, then 50 mg/hr infusion (n=35) 210 Rabeprazole PO 10 mg daily (n=70); ranitidine PO 30 mg daily (n=70); teprenone 150 mg NG daily (n=70) 129 Omeprazole 20 mg NG BID (n=61); ranitidine 50 mg IV BID (n=68) 108 Omeprazole 40 mg IV BID (n=38); ranitidine 150 mg/day infusion (n=38); sucralfate 1 g NG QID (n=32) Gross bleeding as manifest by hematemesis, aspiration of coffee ground material from the NG tube, or melena, or a Hgb of > 2 g/dl complicated by either the need for transfusion or hemodynamic instability Overt bleeding with one of the following: a) Drop in SBP >20 mm Hg or rise in HR >20 beats/min within 24 hrs of the onset of bleeding not explained by other causes; or b) Drop in Hgb by 2 g/dl or more not explained by other causes a) Bright right blood not clearing after tube adjustment and lavage with saline for 5-10 mins; b) 8 hrs of persistent gastro-occult positive coffee ground material with aspirates every 2 hrs not clearing with lavage; or c) Persistent gastro-occult positive coffee ground material over 2-4 hrs on d 3-14 in three consecutive aspirates not clearing with lavage a) Hematemesis or bright red blood in gastric aspirate that did not clear after adjustment of NG or OG tube and a 5- to 10-min lavage with iced water or saline; b) Persistent coffee ground material for 8 consecutive hrs that did not clear with a 100 ml lavage, or was accompanied by a 5% in Hct; c) A in Hct requring one or more transfusions that occurred in the absence of any obvious source and required further diagnostic studies; or d) Melena or frank bloody stools from an upper GI source Upper GI bleeding (hematemesis, coffe ground emesis, or melena) confirmed with gastrodudenoscopy Overt bleeding associated with one of the following: a) A 20 mm Hg in SBP or DBP during the first 24 hrs after bleeding; b) A 20 beat/min HR or 10 mm Hg in SBP in a standing position; c) A 2 g/dl of Hgb or 6% decrease in Hct during the first 24 hrs after bleeding; d) Lack of in Hgb after infusing two units of packed cells Upper GI bleeding including hematemesis, bright red blood, coffee ground emesis or melena Clinically important bleeding; nosocomial PNA; mortality; ICU LOS Clinically important bleeding; nosocomial PNA; mortality; ICU LOS; adverse events Clinically important bleeding; overt bleeding; PNA; mortality Clinically important bleeding; PNA; mortality; adverse events Overt bleeding; adverse events Clinically important bleeding; nosocomial PNA; mortality; ICU LOS Overt bleeding; nosocomial PNA; mortality; ICU LOS
19 Appendix A. (Continued) Summary of Individual Studies Included in Meta-Analyse Study N Intervention Definition of Bleeding Outcomes Pan et al. 30 Rabeprazole PO 20 mg once daily (n=20); Melena or hematemesis Overt bleeding 2004 famotidine IV 40 mg BID (n=10) Risaliti et al No clear definition Phillips et al Fink et al Morris et al Kotlyanskaya et al Brophy et al Omeprazole 40 mg daily IV, then 20 mg PO daily (n=14); ranitidine 150 mg IV daily, then 300 mg PO daily (n=14) 58 Omeprazole 40 mg NG loading, then 20 mg NG daily (n=33); ranitidine 50 mg IV loading, then mg/day infusion (n=25) 189 (4:1) Randomization as follows: IV pantoprazole 40 mg daily, 40 mg BID, 80 mg daily, or 80 mg BID (n=158); IV cimetidine 300 mg bolus, then 50 mg/hr infusion (n=31) 202 (5:1) Randomization as follows: IV pantoprazole 40 mg daily, 40 mg BID, 80 mg daily, 80 mg BID, or 80 mg TID (n=169); IV cimetidine 300 mg IV loading, then 50 mg/hr (n=33) 66 Lansoprazole (suspension) NG (n=22); lansoprazole (tablet) NG (n=23); ranitidine (n=21) (dose and frequency not reported) 51 Lansoprazole (suspension) 30 mg NG daily (n=23); famotidine 20 mg IV BID (n=23) No clear definition No clear definition No clear definition Overt bleeding associated with change in hemodynamics or drop in the Hgb Endoscopic evidence of stress-related mucosal bleeding, bright red blood per NG tube that did not clear after lavage, or overt bleeding (hematemesis, bloody gastric aspirate, melana, or hematochezia) plus either a in BP of 20 mm Hg, or a of 2 g/dl in Hg and two units of blood transfused within 24 hrs Clinically important bleeding; overt bleeding; adverse events Clinically important bleeding; PNA; adverse events UGI bleeding; mortality UGI bleeding; nosocomial PNA Clinically important bleeding; overt bleeding; nosocomial PNA; drug adverse events Time ph 4; percentage of time gastric residuals < 28 ml; clinically significant bleeding IV, intravenous; BID, twice daily; TID, three times daily; QID, four times daily; NG, nasogastric; OG, orogastric; Hgb, hemoglobin; Hct, hematocrit; PNA, pneumonia; LOS, length of stay; BP, blood pressure; SBP, systolic blood pressure; DBP, diastolic blood pressure; HR, heart rate; GI, gastrointestinal; hrs, hours; d, day
Inhibit terminal acid secretion from parietal cells by blocking H + /K + - ATPase pump
 Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Association between Proton Pump Inhibitors and Clostridium difficile
 Association between Proton Pump Inhibitors and Clostridium difficile Lauren Petrik and Nicholas Hellebusch, Pharm.D. Candidates 2013, Tatum Mead, Pharm.D. UMKC School of Pharmacy Clostridium difficile,
Association between Proton Pump Inhibitors and Clostridium difficile Lauren Petrik and Nicholas Hellebusch, Pharm.D. Candidates 2013, Tatum Mead, Pharm.D. UMKC School of Pharmacy Clostridium difficile,
Awareness of the inappropriate use of GI prophylaxis and its cost. Adverse effects of proton pump inhibitor
 Understand the indication for stress ulcer/gi prophylaxis Awareness of the inappropriate use of GI prophylaxis and its cost Adverse effects of proton pump inhibitor A. 65yo w/ HTN and ESRD on HD p/w left
Understand the indication for stress ulcer/gi prophylaxis Awareness of the inappropriate use of GI prophylaxis and its cost Adverse effects of proton pump inhibitor A. 65yo w/ HTN and ESRD on HD p/w left
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting
 Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
Improving Appropriate Use of Proton Pump Inhibitors as Gastrointestinal Prophylaxis in the Hospital Setting DATE Educating for Quality Improvement & Patient Safety 1 The Team Division CS&E Participants
A. Ketorolac*** B. Naproxen C. Ibuprofen D. Celecoxib
 1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
1. A man, 66 years of age, with a history of knee osteoarthritis (OA) is experiencing increasing pain at rest and with physical activity. He also has a history of depression and coronary artery disease.
Gloucestershire Hospitals
 TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
TRUST GUIDELINE In the case of hard copies of this policy the content can only be assured to be accurate on the date of issue marked on the document. The Policy framework requires that the policy is fully
Digestive System (continued) Digestive System. Stomach. Peptic Ulcer Disease
 Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
Digestive System Digestive System (continued) Responsible for breaking down food, absorbing nutrients, eliminating wastes Alimentary canal Also known as gastrointestinal tract Reaches from mouth to anus
Presented by: Jean Yoo-Campbell, Matthew Konerman, Monica Konerman, Jean Yoo Campbell, Christian Gocke, Eunpi Cho Donald Lynch
 Bass N.M., et. al. N Engl J Med 2010; 362:1071-1081 Presented by: Jean Yoo-Campbell, Matthew Konerman, Monica Konerman, Jean Yoo Campbell, Christian Gocke, Eunpi Cho Donald Lynch Faculty Advisor: Dr. Fred
Bass N.M., et. al. N Engl J Med 2010; 362:1071-1081 Presented by: Jean Yoo-Campbell, Matthew Konerman, Monica Konerman, Jean Yoo Campbell, Christian Gocke, Eunpi Cho Donald Lynch Faculty Advisor: Dr. Fred
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE)
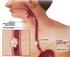 Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
National Digestive Diseases Information Clearinghouse
 Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
Gastritis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is gastritis? Gastritis is a condition in which the stomach
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
CDEC FINAL RECOMMENDATION
 CDEC FINAL RECOMMENDATION RIVAROXABAN (Xarelto Bayer Inc.) New Indication: Pulmonary Embolism Note: The Canadian Drug Expert Committee (CDEC) previously reviewed rivaroxaban for the treatment of deep vein
CDEC FINAL RECOMMENDATION RIVAROXABAN (Xarelto Bayer Inc.) New Indication: Pulmonary Embolism Note: The Canadian Drug Expert Committee (CDEC) previously reviewed rivaroxaban for the treatment of deep vein
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
The author has no disclosures
 Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
Mary Bradbury, PharmD, BCPS Clinical Pharmacy Specialist, Cardiac Surgery September 18, 2012 Mary.bradbury@inova.org This presentation will discuss unlabeled and investigational use of products The author
GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
Clostridium Difficile Colitis: Treatments, Guidelines, and Challenges
 Clostridium Difficile Colitis: Treatments, Guidelines, and Challenges Brian S. Zuckerbraun, MD, FACS Henry T. Bahnson Professor of Surgery University of Pittsburgh Chief, Trauma and Acute Care Surgery
Clostridium Difficile Colitis: Treatments, Guidelines, and Challenges Brian S. Zuckerbraun, MD, FACS Henry T. Bahnson Professor of Surgery University of Pittsburgh Chief, Trauma and Acute Care Surgery
Upper Endoscopy (EGD)
 Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
Upper Endoscopy (EGD) Appointment Information: Patient Name: MRN: Physician Name: Location: _ For information on Directions, please visit: http://www.brighamandwomens.org/general/directions/directions.aspx
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Vasopressors. Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco
 Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Big data size isn t enough! Irene Petersen, PhD Primary Care & Population Health
 Big data size isn t enough! Irene Petersen, PhD Primary Care & Population Health Introduction Reader (Statistics and Epidemiology) Research team epidemiologists/statisticians/phd students Primary care
Big data size isn t enough! Irene Petersen, PhD Primary Care & Population Health Introduction Reader (Statistics and Epidemiology) Research team epidemiologists/statisticians/phd students Primary care
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
GI Bleeding. Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics
 GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
GI Bleeding Thomas S.Foster,Pharm.D. PHR 961 Integrated Therapeutics Overview Because GI bleeding is internal, it is possible for a person to have GI bleeding without symptoms. Important to recognize
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
Summary and general discussion
 Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
Chapter 7 Summary and general discussion Summary and general discussion In this thesis, treatment of vitamin K antagonist-associated bleed with prothrombin complex concentrate was addressed. In this we
4/18/14. Background. Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients. Background. Signs and Symptoms of Withdrawal
 Background 1 Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients Alyssa Cavanaugh, PharmD PGY1 Pharmacy Resident Children s Hospital of Michigan **The speaker has no actual or
Background 1 Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients Alyssa Cavanaugh, PharmD PGY1 Pharmacy Resident Children s Hospital of Michigan **The speaker has no actual or
Inpatient Anticoagulation Safety. To provide safe and effective anticoagulation therapy through a collaborative approach.
 Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Inpatient Anticoagulation Safety Purpose: Policy: To provide safe and effective anticoagulation therapy through a collaborative approach. Upon the written order of a physician, Heparin, Low Molecular Weight
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
New Oral Anticoagulants
 New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
New Oral Anticoagulants Tracy Minichiello, MD Associate Professor of Medicine Chief, San FranciscoVA Anticoagulation and Thrombosis Service Ansell, J. Hematology Copyright 2010 American Society of Hematology.
Research funding was provided by TAP Pharmaceutical Products, Inc.
 DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
DOES THE DOSING FREQUENCY OF PROTON PUMP INHIBITORS (PPIs) AFFECT SUBSEQUENT RESOURCE UTILIZATION AND COSTS AMONG PATIENTS DIAGNOSED WITH GASTROESOPHAGEAL REFLUX DISEASE (GERD)? Boulanger L 1, Mody R 2,
If several different trials are mentioned in one publication, the data of each should be extracted in a separate data extraction form.
 General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
Nursing 113. Pharmacology Principles
 Nursing 113 Pharmacology Principles 1. The study of how drugs enter the body, reach the site of action, and are removed from the body is called a. pharmacotherapeutics b. pharmacology c. pharmacodynamics
Nursing 113 Pharmacology Principles 1. The study of how drugs enter the body, reach the site of action, and are removed from the body is called a. pharmacotherapeutics b. pharmacology c. pharmacodynamics
Decreasing Sepsis Mortality at the University of Colorado Hospital
 Decreasing Sepsis Mortality at the University of Colorado Hospital Maureen Dzialo, RN, BSN - Nurse Manager, Cardiac Intensive Care Unit Olivia Kerveillant, RN Clinical Nurse III, Medical Intensive Care
Decreasing Sepsis Mortality at the University of Colorado Hospital Maureen Dzialo, RN, BSN - Nurse Manager, Cardiac Intensive Care Unit Olivia Kerveillant, RN Clinical Nurse III, Medical Intensive Care
Omega-3 fatty acids improve the diagnosis-related clinical outcome. Critical Care Medicine April 2006;34(4):972-9
 Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
STROKE PREVENTION IN ATRIAL FIBRILLATION. TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: ABBREVIATIONS: BACKGROUND:
 STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
STROKE PREVENTION IN ATRIAL FIBRILLATION TARGET AUDIENCE: All Canadian health care professionals. OBJECTIVE: To guide clinicians in the selection of antithrombotic therapy for the secondary prevention
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Tapered Withdrawal of a Proton Pump Inhibitor to Prevent Rebound Acid-Related Symptoms
 Akin Oyalowo CRC Rotation IRB Proposal August 8, 2012 Tapered Withdrawal of a Proton Pump Inhibitor to Prevent Rebound Acid-Related Symptoms A. Study Purpose and Rationale Proton pump inhibitors (PPIs)
Akin Oyalowo CRC Rotation IRB Proposal August 8, 2012 Tapered Withdrawal of a Proton Pump Inhibitor to Prevent Rebound Acid-Related Symptoms A. Study Purpose and Rationale Proton pump inhibitors (PPIs)
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
Oral Zinc Supplementation as an Adjunct Therapy in the Management of Hepatic Encephalopathy: A Randomized Controlled Trial
 Oral Zinc Supplementation as an Adjunct Therapy in the Management of Hepatic Encephalopathy: A Randomized Controlled Trial Marcus R. Pereira A. Study Purpose Hepatic encephalopathy is a common complication
Oral Zinc Supplementation as an Adjunct Therapy in the Management of Hepatic Encephalopathy: A Randomized Controlled Trial Marcus R. Pereira A. Study Purpose Hepatic encephalopathy is a common complication
Gastroesophageal Reflux Disease
 3702 Timberline Rd 2555 East 13th St Suite 220 Ft.Collins, CO 80525 Loveland, CO 80537 82001 7251 W. 20th St Greeley, CO 80634 4108 Laramie Cheyenne, WY Gastroesophageal Reflux Disease Author(s): Peter
3702 Timberline Rd 2555 East 13th St Suite 220 Ft.Collins, CO 80525 Loveland, CO 80537 82001 7251 W. 20th St Greeley, CO 80634 4108 Laramie Cheyenne, WY Gastroesophageal Reflux Disease Author(s): Peter
IMPORTANT DRUG WARNING Regarding Mycophenolate-Containing Products
 Dear Healthcare Provider: Mycophenolate REMS (Risk Evaluation and Mitigation Strategy) has been mandated by the FDA (Food and Drug Administration) due to postmarketing reports showing that exposure to
Dear Healthcare Provider: Mycophenolate REMS (Risk Evaluation and Mitigation Strategy) has been mandated by the FDA (Food and Drug Administration) due to postmarketing reports showing that exposure to
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Medication Error. Medication Errors. Transitions in Care: Optimizing Intern Resources
 Transitions in Care: Optimizing Intern Resources DeeDee Hu PharmD, MBA Clinical Specialist Critical Care and Cardiology PGY1 Program Director Memorial Hermann Memorial City Medical Center Medication Error
Transitions in Care: Optimizing Intern Resources DeeDee Hu PharmD, MBA Clinical Specialist Critical Care and Cardiology PGY1 Program Director Memorial Hermann Memorial City Medical Center Medication Error
A list of FDA-approved testosterone products can be found by searching for testosterone at http://www.accessdata.fda.gov/scripts/cder/drugsatfda/.
 FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
Guide to Biostatistics
 MedPage Tools Guide to Biostatistics Study Designs Here is a compilation of important epidemiologic and common biostatistical terms used in medical research. You can use it as a reference guide when reading
MedPage Tools Guide to Biostatistics Study Designs Here is a compilation of important epidemiologic and common biostatistical terms used in medical research. You can use it as a reference guide when reading
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN
 BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014
 CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
CLINICAL QUALITY MEASURES FINALIZED FOR ELIGIBLE HOSPITALS AND CRITICAL ACCESS HOSPITALS BEGINNING WITH FY 2014 e 55 0495 2 Emergency Department (ED)- 1 Emergency Department Throughput Median time from
High Impact Intervention Care bundle to reduce ventilation-association pneumonia
 High Impact Intervention Care bundle to reduce ventilation-association pneumonia Aim To reduce the incidence of ventilation-associated pneumonia (VAP). Context The aim of the care bundle, as set out in
High Impact Intervention Care bundle to reduce ventilation-association pneumonia Aim To reduce the incidence of ventilation-associated pneumonia (VAP). Context The aim of the care bundle, as set out in
Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points
 372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
372 Gut 2001;49:372 379 Drug treatments in upper gastrointestinal bleeding: value of endoscopic findings as surrogate end points G M Hawkey, A T Cole, A S McIntyre, R G Long, C J Hawkey Division of Gastroenterology,
BYE-BYE, PPI. A toolkit for deprescribing proton pump inhibitors in EMR-enabled primary care settings
 BYE-BYE, PPI. A toolkit for deprescribing proton pump inhibitors in EMR-enabled primary care settings version 1.0 Don t maintain long-term Proton Pump Inhibitor (PPI) therapy for gastrointestinal symptoms
BYE-BYE, PPI. A toolkit for deprescribing proton pump inhibitors in EMR-enabled primary care settings version 1.0 Don t maintain long-term Proton Pump Inhibitor (PPI) therapy for gastrointestinal symptoms
Drug Shortage Alert 11/15/2012
 Drug Shortage Alert 11/15/2012 Recommendations and information provided in Drug Shortage Alerts are compiled by experts in the field. Practitioners always are advised to consult with staff to ensure response
Drug Shortage Alert 11/15/2012 Recommendations and information provided in Drug Shortage Alerts are compiled by experts in the field. Practitioners always are advised to consult with staff to ensure response
A study to Evaluate PPI s effect on vitamin D levels. Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD
 A study to Evaluate PPI s effect on vitamin D levels Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD The sunshine vitamin Existed over 500 million years. Prehormone, not only a vitamin. Two major sources:
A study to Evaluate PPI s effect on vitamin D levels Rani Hanna M.D., M.S. PGY-3 Joseph Grisanti, MD The sunshine vitamin Existed over 500 million years. Prehormone, not only a vitamin. Two major sources:
DVT/PE Management with Rivaroxaban (Xarelto)
 DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
DVT/PE Management with Rivaroxaban (Xarelto) Rivaroxaban is FDA approved for the acute treatment of DVT and PE and reduction in risk of recurrence of DVT and PE. FDA approved indications: Non valvular
1.1. (Es)omeprazole and vitamin B12 deficiency
 1.1. (Es)omeprazole and Introduction Omeprazole, a substituted benzimidazole, and esomeprazole, the S-isomere of omeprazole belong to the class of proton pump inhibitors (PPIs) which strongly reduce gastric
1.1. (Es)omeprazole and Introduction Omeprazole, a substituted benzimidazole, and esomeprazole, the S-isomere of omeprazole belong to the class of proton pump inhibitors (PPIs) which strongly reduce gastric
Proton Pump Inhibitors (PPIs) and Histamine-2 Antagonists (H2As)
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119
American Journal of Gastroenterology ISSN 0002-9270
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00399.x Published by Blackwell Publishing Role of Intravenous Omeprazole in Patients
Clostridium Difficile Colitis. Presented by Mark Skains August 2003
 Clostridium Difficile Colitis Presented by Mark Skains August 2003 What is Clostridium Difficile Gram positive rod Produces spores (hang out in diverticula) Forms Endotoxin A + B which cause diarrhea.
Clostridium Difficile Colitis Presented by Mark Skains August 2003 What is Clostridium Difficile Gram positive rod Produces spores (hang out in diverticula) Forms Endotoxin A + B which cause diarrhea.
Drug Class Review Proton Pump Inhibitors
 Drug Class Review Proton Pump Inhibitors Final Report Update 5 May 2009 Update 4: May 2006 Update 3: May 2005 Update 2: April 2004 Update 1: April 2003 Original Report: November 2002 The literature on
Drug Class Review Proton Pump Inhibitors Final Report Update 5 May 2009 Update 4: May 2006 Update 3: May 2005 Update 2: April 2004 Update 1: April 2003 Original Report: November 2002 The literature on
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses
 WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses 20 August 2009 Table of contents EXECUTIVE SUMMARY... i Other recommendations...iii 1. INTRODUCTION...
WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses 20 August 2009 Table of contents EXECUTIVE SUMMARY... i Other recommendations...iii 1. INTRODUCTION...
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department!
 Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Plumbing 101:! TXA and EMS! Jay H. Reich, MD FACEP! EMS Medical Director! City of Kansas City, Missouri/Kansas City Fire Department! EMS Section Chief! Department of Emergency Medicine! University of Missouri-Kansas
Appendix G - Identification and Selection of Studies
 FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
FINAL Emergency framework for rationing of blood for massively bleeding patients during a red phase of a Appendix G - Identification and Selection of Studies Inclusion/Exclusion Criteria We included studies
GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION
 GUIDELINES GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION Preamble The purpose of this document is to provide guidance for the pharmacist
GUIDELINES GUIDELINES ON PREVENTING MEDICATION ERRORS IN PHARMACIES AND LONG-TERM CARE FACILITIES THROUGH REPORTING AND EVALUATION Preamble The purpose of this document is to provide guidance for the pharmacist
Public Assessment Report. Pharmacy to General Sales List Reclassification. Nexium Control 20mg Gastro-Resistant Tablets.
 Public Assessment Report Pharmacy to General Sales List Reclassification Nexium Control 20mg Gastro-Resistant Tablets (Esomeprazole) EMA Agency number: Pfizer Consumer Healthcare Ltd TABLE OF CONTENTS
Public Assessment Report Pharmacy to General Sales List Reclassification Nexium Control 20mg Gastro-Resistant Tablets (Esomeprazole) EMA Agency number: Pfizer Consumer Healthcare Ltd TABLE OF CONTENTS
Advanced Heart Failure & Transplantation Fellowship Program
 Advanced Heart Failure & Transplantation Fellowship Program Curriculum I. Patient Care When on the inpatient Heart Failure and Transplant Cardiology service, the cardiology fellow will hold primary responsibility
Advanced Heart Failure & Transplantation Fellowship Program Curriculum I. Patient Care When on the inpatient Heart Failure and Transplant Cardiology service, the cardiology fellow will hold primary responsibility
Treatments for Barrett s Oesophagus
 Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with Heartburn Cancer UK (HCUK), a
Treatments for Barrett s Oesophagus Introduction This leaflet describes the various ways in which Barrett s Oesophagus is treated. It has been produced in association with Heartburn Cancer UK (HCUK), a
in the Elderly Thomas Robinson, MD Surgery Grand Rounds March 10 th, 2008
 Post- Operative Delirium in the Elderly Thomas Robinson, MD Surgery Grand Rounds March 10 th, 2008 What is the most common post-operative complication in elderly patients? What is the most common post-operative
Post- Operative Delirium in the Elderly Thomas Robinson, MD Surgery Grand Rounds March 10 th, 2008 What is the most common post-operative complication in elderly patients? What is the most common post-operative
Figure 3: Dysphagia. 14 meets. esophageal. esophageal manometry +/- +/- impedance measurement. structural lesion? no. 19 yes
 Figure 3: Dysphagia 1 patient with dysphagia 2 history and physical exam. suggestive of nesophageal etiology? 3 evaluate and treat as as indicated 4 upper GI GI endoscopy with biopsies 15 achalasia, absent
Figure 3: Dysphagia 1 patient with dysphagia 2 history and physical exam. suggestive of nesophageal etiology? 3 evaluate and treat as as indicated 4 upper GI GI endoscopy with biopsies 15 achalasia, absent
Hematologic Malignancies/Stem Cell Transplantation Program Clinical Section UCLA Health System Los Angeles, CA 90095
 Clinical Section UCLA Health System Los Angeles, CA 90095 CS 6.2 DIAGNOSIS AND MANAGEMENT OF INTERSTITIAL PNEUMONIA Location: Clinical Section Supersedes/Replaces: B3.421g Document drive\path\name Effective
Clinical Section UCLA Health System Los Angeles, CA 90095 CS 6.2 DIAGNOSIS AND MANAGEMENT OF INTERSTITIAL PNEUMONIA Location: Clinical Section Supersedes/Replaces: B3.421g Document drive\path\name Effective
convey the clinical quality measure's title, number, owner/developer and contact
 CMS-0033-P 153 convey the clinical quality measure's title, number, owner/developer and contact information, and a link to existing electronic specifications where applicable. TABLE 20: Proposed Clinical
CMS-0033-P 153 convey the clinical quality measure's title, number, owner/developer and contact information, and a link to existing electronic specifications where applicable. TABLE 20: Proposed Clinical
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Gastrointestinal bleeding
 Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
Gastrointestinal bleeding..is the reason in 2 % of all admissions to hospital 85.000 cases/year in the US. The incidence of urgent upper GI bleeding: 145/100.000 inhabitant/year in Hungary ( Nagy Gy. MBA
BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN ADMINISTRATION OF DRUGS. SUMMARY.
 BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN ADMINISTRATION OF DRUGS. SUMMARY. Bibliographical review on cost of Patient Safety Failings in administration of drugs. Summary This has been
BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN ADMINISTRATION OF DRUGS. SUMMARY. Bibliographical review on cost of Patient Safety Failings in administration of drugs. Summary This has been
BRITTANY N. HARRIS; DONNA S. WEST, RPh, PhD; JILL JOHNSON, PharmD; SONG HEE HONG, PhD; and CINDY D. STOWE, PharmD
 CONTEMPORARY SUBJECT Effects on the Cost and Utilization of Proton Pump Inhibitors From Adding Over-the Counter Omeprazole to Drug Benefit Coverage in a State Employee Health Plan BRITTANY N. HARRIS; DONNA
CONTEMPORARY SUBJECT Effects on the Cost and Utilization of Proton Pump Inhibitors From Adding Over-the Counter Omeprazole to Drug Benefit Coverage in a State Employee Health Plan BRITTANY N. HARRIS; DONNA
Endoscopy & ACS. 8/1/2014 Dr. Whang
 Endoscopy & ACS 8/1/2014 Dr. Whang Outline I. Antiplatelets II. Coronary Artery Disease in U.S. III. GI Bleeding in ACS IV. ACC/AHA guidelines: Dual Antiplatelet Therapy in CAD V. PPI and Plavix Controversy
Endoscopy & ACS 8/1/2014 Dr. Whang Outline I. Antiplatelets II. Coronary Artery Disease in U.S. III. GI Bleeding in ACS IV. ACC/AHA guidelines: Dual Antiplatelet Therapy in CAD V. PPI and Plavix Controversy
Medication error is the most common
 Medication Reconciliation Transfer of medication information across settings keeping it free from error. By Jane H. Barnsteiner, PhD, RN, FAAN Medication error is the most common type of error affecting
Medication Reconciliation Transfer of medication information across settings keeping it free from error. By Jane H. Barnsteiner, PhD, RN, FAAN Medication error is the most common type of error affecting
Committee Approval Date: September 12, 2014 Next Review Date: September 2015
 Medication Policy Manual Policy No: dru361 Topic: Pradaxa, dabigatran Date of Origin: September 12, 2014 Committee Approval Date: September 12, 2014 Next Review Date: September 2015 Effective Date: November
Medication Policy Manual Policy No: dru361 Topic: Pradaxa, dabigatran Date of Origin: September 12, 2014 Committee Approval Date: September 12, 2014 Next Review Date: September 2015 Effective Date: November
Riociguat Clinical Trial Program
 Riociguat Clinical Trial Program Riociguat (BAY 63-2521) is an oral agent being investigated as a new approach to treat chronic thromboembolic pulmonary hypertension (CTEPH) and pulmonary arterial hypertension
Riociguat Clinical Trial Program Riociguat (BAY 63-2521) is an oral agent being investigated as a new approach to treat chronic thromboembolic pulmonary hypertension (CTEPH) and pulmonary arterial hypertension
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation. Joy Wahawisan, Pharm.D., BCPS April 25, 2012
 New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
New Anticoagulation Options for Stroke Prevention in Atrial Fibrillation Joy Wahawisan, Pharm.D., BCPS April 25, 2012 Stroke in Atrial Fibrillation % Stroke 1991;22:983. Age Range (years) CHADS 2 Risk
Active centers: 2. Number of patients/subjects: Planned: 20 Randomized: Treated: 20 Evaluated: Efficacy: 13 Safety: 20
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinialTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClinialTrials.gov
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Sponsor Novartis. Generic Drug Name Secukinumab. Therapeutic Area of Trial Psoriasis. Approved Indication investigational
 Clinical Trial Results Database Page 2 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Psoriasis Approved Indication investigational Clinical Trial Results Database Page 3 Study
Clinical Trial Results Database Page 2 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Psoriasis Approved Indication investigational Clinical Trial Results Database Page 3 Study
What can I eat? Peptic ulcers. What are peptic ulcers? What tests are needed? Will the ulcer come back? What causes a peptic ulcer?
 In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
In association with: INFORMATION ABOUT Peptic ulcers www.corecharity.org.uk What are peptic ulcers? What causes a peptic ulcer? How are NSAIDs and aspirin involved? How do I know if I ve got an ulcer?
HSE Health Protection Surveillance Centre. Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection
 Clostridium difficile Sub-Committee Health Protection Surveillance Centre Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection Version 3, January 2016 This document has
Clostridium difficile Sub-Committee Health Protection Surveillance Centre Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection Version 3, January 2016 This document has
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs
 Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs Problem: Use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) in clients with any one of the following risk
Medication Management Improvement System Protocol #4 Potentially Inappropriate Use of NSAIDs Problem: Use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) in clients with any one of the following risk
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
There may be up to 5 to 6 million cases of. Treatment Costs of Community- Acquired Pneumonia in an Employed Population*
 Treatment Costs of Community- Acquired Pneumonia in an Employed Population* Gene L. Colice, MD, FCCP; Melissa A. Morley, MA; Carl Asche, PhD; and Howard G. Birnbaum, PhD Background: Community-acquired
Treatment Costs of Community- Acquired Pneumonia in an Employed Population* Gene L. Colice, MD, FCCP; Melissa A. Morley, MA; Carl Asche, PhD; and Howard G. Birnbaum, PhD Background: Community-acquired
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Oral Bisphosphonate and Risk of Esophageal Cancer: A Nationwide Claim Study
 J Bone Metab 2015;22:77-81 http://dx.doi.org/10.11005/jbm.2015.22.2.77 pissn 2287-6375 eissn 2287-7029 Original Article Oral Bisphosphonate and Risk of Esophageal Cancer: A Nationwide Claim Study Gi Hyeon
J Bone Metab 2015;22:77-81 http://dx.doi.org/10.11005/jbm.2015.22.2.77 pissn 2287-6375 eissn 2287-7029 Original Article Oral Bisphosphonate and Risk of Esophageal Cancer: A Nationwide Claim Study Gi Hyeon
Learning Objectives. Introduction to Reconciling Medication Information. Background. Elements of Performance NPSG.03.06.01
 Pharmacy Evaluation of Medication Reconciliation Initiated in the Emergency Department Manuel A. Calvin, Pharm.D. PGY1 Pharmacy Resident Saint Francis Hospital, Tulsa, OK OSHP Annual Meeting Residency
Pharmacy Evaluation of Medication Reconciliation Initiated in the Emergency Department Manuel A. Calvin, Pharm.D. PGY1 Pharmacy Resident Saint Francis Hospital, Tulsa, OK OSHP Annual Meeting Residency
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
John E. O Toole, Marjorie C. Wang, and Michael G. Kaiser
 Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
Hypothermia and Human Spinal Cord Injury: Updated Position Statement and Evidence Based Recommendations from the AANS/CNS Joint Sections on Disorders of the Spine & Peripheral Nerves and Neurotrauma &
American Gastroenterological Association Institute Technical Review on the Management of Gastroesophageal Reflux Disease
 GASTROENTEROLOGY 2008;135:1392 1413 American Gastroenterological Association Institute Technical Review on the Management of Gastroesophageal Reflux Disease Learning Objectives At the end of this activity,
GASTROENTEROLOGY 2008;135:1392 1413 American Gastroenterological Association Institute Technical Review on the Management of Gastroesophageal Reflux Disease Learning Objectives At the end of this activity,
