How To Treat Lung Cancer
|
|
|
- Corey Jenkins
- 5 years ago
- Views:
Transcription
1 The Lung Cancer Program at St. Joseph Hospital takes a comprehensive and individualized approach to patient care. We offer a wide range of services that include cancer prevention, CT lung cancer screening, diagnosis and treatment, research and supportive care. Our program was nationally recognized at the 2005 Advisory Board Company s Oncology Round Table annual symposium as a best practice model for our comprehensive program planning and our CT Screening approach to early diagnosis. At St. Joseph Hospital we stress patient-centered care. Interdisciplinary treatment management conferences are held weekly; participants include expert thoracic surgeons, pulmonologists, medical and radiation oncologists, pathologists, radiologists, and nursing and research staff. As a team, these specialists evaluate and provide treatment recommendations for newly diagnosed lung cancer patients. Using evidence-based medicine, these healthcare professionals strive to achieve the best patient care outcomes possible tailored to the individual needs of each patient. Lung cancer is a complicated disease that requires many combined modalities for treatment, such as radiation therapy, surgery, chemotherapy and biotherapy. Within the past five years many new treatment options have been discovered and researched that provide better outcomes and survival benefits for lung cancer patients. At St. Joseph Hospital we utilize the most recent medical developments and clinical trials to produce the best prognosis and outcome for our patients. We have found that patients want the most aggressive treatment with the least side effects producing the best/longest overall survival. Our survival rates are considerably greater than the state or national average. We are continually incorporating the most up-to-date evidence-based practice into our treatment plans. We utilize the National Cancer Center Institute (NCCN) guidelines when appropriating treatment. However, each patient s treatment plan is designed to meet the individual needs of the patient and family. Lung Cancer Program 1
2 Meet the Team Raymond Casciari, MD Co-Medical Director Lung Cancer Program Chief Medical Officer, St. Joseph Hospital Board Certifications: Internal Medicine and Pulmonary Disease Medical School: Temple University School of Medicine, Philadelphia, PA Residency: University of California at Irvine Medical Center Fellowship: University of California at Irvine Medical Center (714) Brian Palafox, MD Co-Medical Director Lung Cancer Program Board Certifications: General and Thoracic Surgery Medical School: University of California, Irvine Residency: University of California Irvine Medical Center Fellowship: University of California Irvine Medical Center Expertise: Minimally Invasive General Thoracic Surgery (VATS) Pam Matten, RN Lung Nurse Navigator Education: B.S.N. Degree, Azusa Pacific University Certifications: Registered Nurse, Chemotherapy, Public Health Nurse, Oncology Nurse Experience: St. Joseph Hospital Cancer Center nurse since Lung Cancer Program 2
3 What is Lung Cancer? Cancer is a condition in which cells multiply uncontrollably to form growths (tumors) that invade and destroy normal tissue. Lung cancer is a malignant tumor that can grow in one or both of your lungs. The cells that line your airways and nearby glands are what typically form the tumor. These are the cells that come in contact with the air you breathe, which may contain carcinogens. In lung cancer, the changing of normal cells into cancer transpires over a period of several years. While smoking is the number one cause of lung cancer, there are many people with lung cancer who have never smoked. There are other factors that can contribute to lung cancer, such as exposure to an airborne chemical, such as asbestos or radon. Genetics also plays a role, as people with a family history of lung cancer are at a higher risk of developing the disease. Age is also a factor, as this disease typically occurs in people over 65. If you ve had other lung diseases that have blocked your lung air flow such as chronic obstructive pulmonary disease (COPD) or tuberculosis you are at an increased risk for developing lung cancer. Cigarette smoke contains more than 43 different carcinogens (cancer causing chemicals) and is associated with many cancers such as: esophagus, mouth, stomach, pancreatic, bladder and liver cancer. Smoking accounts for about 30% of all cancer-related deaths and 87% of lung cancer deaths. Second-hand smoke also contains carcinogens; each year in the U.S., 5,000 to 10,000 people are diagnosed with lung cancer from having breathed in second-hand smoke. Smoking cigars and pipe tobacco also increase the risk for developing lung cancer. If you are/were a smoker and have been diagnosed with lung cancer you may experience a range of emotions, including anger, guilt, blame and hopelessness. Whatever the cause of your lung cancer it is helpful to try and forgive your body so you can invest your energy in the healing process. If you have lung cancer from smoking you can make a difference in your treatment and healing by quitting smoking. It is never too late to quit smoking. Also, people who are diagnosed with cancer have a higher chance of developing a second cancer. Quitting smoking can help decrease your risk of a second cancer. If you need help with smoking cessation, St. Joseph Hospital has free Quit Smoking classes that are held every eight weeks. Please see your Nurse Navigator for more information.
4 Types of Lung Cancer There are several types of lung cancer, but most fall into two main categories: small-cell lung cancer (SCLC) and non-small cell lung cancer (NSCLC). These two types of lung cancer act differently and are treated differently. Non-Small Cell Lung Cancer Non-small cell lung cancer (NSCLC) is the most common form of lung cancer, comprising 80-85% of all lung cancers. It is divided into four major subtypes: adenocarcinoma, bronchioloalveolar carcinoma, squamous cell carcinoma and large cell carcinoma. Adenocarcinoma Represents up to 60% of the non-small cell lung cancer cases in the United States Is the most common lung cancer among women Usually starts on the outer edges of the lungs May spread to other parts of the body Is the type that occurs in non-smokers as well as smokers Bronchioloalveolar carcinoma Is a rare sub-type of adenocarcinoma and represents only 3% of all lung cancers Increase is on the rise because of the increase in adenocarcinoma Typically presents in younger patients, women and non-smokers Initially spreads through tiny sacs in the lungs called alveoli rather than in solid tumors Squamous cell carcinoma Represents about 30% of NSCLC lung cancers in the United States Usually starts centrally in one of the bronchi Frequently spreads to regional lymph nodes but tumors are slow growing Is strongly associated with smoking Large cell undifferentiated carcinoma Represents about 10% of NSCLC lung cancers in the United States May occur in any part of the lung Frequently a diagnosis of exclusion Is strongly associated with smoking Small Cell Lung Cancer (SCLC) Represents 15% to 20% of all lung cancers in the United States Typically grows more rapidly than NSCLC Spreads to the lymph nodes and other organs more quickly than NSCLC Is seen predominantly in smokers or former smokers (about 98% of cases are attributed to smoking) Usually starts in one of the large bronchi At the time of diagnosis, usually has spread and is considered a systemic disease Is more responsive to a variety of chemotherapy drugs than NSCLC SCLC was previously called oat cell cancer because the cells are small and oval like oat grains
5 Mesothelioma Mesothelioma is a rare type of cancer often beginning in the outer lining of the cells surrounding the mesothelium of the lungs Occurs most often after many years of asbestos exposure Family members can develop mesothelioma by secondary exposure through inhalation, i.e. doing the laundry of an asbestos worker Smoking and asbestos exposure together greatly increase the risk How is Lung Cancer Diagnosed? Early diagnosis of lung cancer is difficult because noticeable symptoms don t usually show up until the disease is more advanced. You may have felt fine, and your diagnosis was a surprise to you and your doctor. Or you may have had signs or symptoms of lung cancer during a routine physical examination, and your doctor ordered tests that found the cancer. Many lung cancers are found coincidently with a chest X-ray following work up for an unrelated surgery or illness. There are certain tests that must be performed to confirm the diagnosis of lung cancer. Diagnostic Tests In addition to a history and physical examination, there are diagnostic tests for people with suspected lung cancer. These tests consist of laboratory testing, radiology tests, tissue biopsies and/or sampling of pleural fluid. The understanding of all test results helps the lung cancer team determine tumor type, clinical stage and individual treatment planning. Here are some of the tests your clinical team may order: Chest X-ray. The most common test used when lung cancer is suspected is the chest X-ray, which uses small amounts of radiation to take a picture of inside your chest, including your lungs. Some tumors around your lungs can be visible with chest X-ray. However it should be noted that a chest x-ray cannot detect small tumors only visible on CT scan. CT and MRI scans. CT (computed tomography) and MRI (magnetic resonance imaging) use computers to produce detailed, three-dimensional images that help diagnose lung cancer and can determine the size, shape, and location of the tumor. If symptoms of lung cancer are present, a contrast-enhanced CT scan is recommended. Both CT and MRI scans are useful in determining if lung cancer has spread to other areas of the body. PET scans. PET (positive emission tomography) scans may give a more accurate picture of the stage of NSCLC, often as a follow-up to other tests or to diagnose recurrent disease. However there is no evidence that PET scan can replace pathological staging of lymph nodes through biopsy. PET/CT. Most recently PET/CT scans have become valuable in restaging of NSCLC lung cancer following treatment. PET captures images of miniscule changes in the body s metabolism caused by the growth of abnormal cells. These abnormal cells will reveal
6 hot spots that may be abnormal growth of tumors. It should be noted that hot spots could be reflective of other conditions such as inflammation or infection. CT images simultaneously allow physicians to pinpoint the exact location, size and shape of the diseased tissue or tumor. The PET and the CT images are fused together. The CT scan shows anatomical detail and the PET scan provides the metabolic activity of the tumor. Sputum Cytology. In this test your sputum, which is the mucus you cough up, is collected and examined under the microscope to look for cancer cells. The most accurate way to do this is to collect and analyze early morning mucus for 3 days. Biopsy. The previously mentioned tests allow your treatment team to view the inside of your body. However, they do not test the tumor for the presence of cancer cells. Therefore these tests do not provide absolute proof that you have cancer. To confirm the presence of cancer, a sample of tissue from the tumor is needed. A biopsy is the term used for the removal and examination of a tissue sample to determine if it is cancerous. Biopsies are performed in different ways depending on the location and size of the tumor. Procedures for Biopsy Bronchoscopy. A bronchoscopy allows the doctor to see inside of the lungs and airways using a hollow tube (called a bronchoscope) and inserting it into the mouth, down the trachea and into the lungs. A small camera on the end of the bronchoscope takes pictures and sends them back to a monitor so the doctor can see the tissue. A small tool at the end of the scope is then used to remove a sample of the tissue from the tumor. In addition, bronchial lavage or washing is a technique used with bronchoscopy. Direct brushing or washing of the abnormalities is used to determine a diagnosis. Transthoracic needle aspiration. The doctor uses a needle to penetrate the chest wall to take a sample of tissue within the lung. This procedure is used for tumors close to the chest wall. Cervical Mediastinoscopy. A small tube is passed through an incision at the top of the breastbone, in front of the trachea and into the mediastinum. A small camera at the end of the tube allows the doctor to see the tissues. This procedure determines whether cancer has spread to lymph nodes near the trachea one of the first places lung cancer is likely to spread. This procedure requires a local and general anesthesia but can usually be done on an outpatient basis. Thoracentesis. If fluid is collecting between the lungs and the chest wall, this procedure is used to extract some of the fluid through a needle to see if cancerous cells are present. This procedure can be performed with local anesthesia. Video-assisted thoracoscopy. A tube containing a small television camera is inserted between the ribs through a small incision in the skin, so the doctor can see the tumor. This procedure removes a larger portion of the tumor rather than taking a small tissue sample. General anesthesia is used and can result in a short hospital stay.
7 Understanding Treatment for Lung Cancer Standard Therapies-This section provides an overview of the general types of therapy used to treat lung cancer. Standard treatment for NSCLC usually involves surgery, radiation therapy, chemotherapy, or a combination of these approaches. In some cases, it also involves novel targeted therapies. For SCLC, it involves chemotherapy and frequently radiation therapy. (For more specific information: see Treating NSCLC, and Treating SCLC.) Surgery Surgical removal of the tumor is a common choice when the cancer has not spread to other tissues in the chest or beyond. The following types of surgery are used to treat lung cancer: Wedge or segmental resection removal of a small part of the lung Lobectomy removal of an entire section (lobe) of the lung Bilobectomy removal of more than one lobe Pneumonectomy removal of the entire lung Surgery may be the first type of treatment used, or it may be used after chemotherapy, radiation or both have been given to shrink the tumor. Generally surgery is not used as first-line treatment if the lung cancer has: Spread from the lung into other parts of the chest (e.g., the heart, or the plural luid which is fluid between the lung and chest wall) Spread to lymph nodes in the neck, mediastinum (area located in the center of the chest, but outside the lungs) or to other organs (e.g., the liver, adrenal glands, or brain) Made it difficult to breathe Developed in a part of the lung that can t be removed Been diagnosed as SCLC Surgery is not recommended when the person has other health-related problems that would make surgery risky (e.g., heart or vascular problems, severe emphysema, diabetes, and certain other chronic conditions). To find out whether your lungs are healthy enough for surgery, the doctor may give you several tests (e.g., pulmonary function tests and a quantitative ventilation/perfusion scan). Pulmonary rehabilitation programs may be recommended, both before and after surgery especially for people who do not have a regular exercise program. Sometimes bronchodilators, like those used to treat asthma, can also help improve breathing function enough for surgery. VATS may be used as a less-invasive surgical option in some situations (see Newer Therapies for more information). Chemotherapy Chemotherapy uses drugs to destroy or damage cancer cells so they cannot reproduce. It can be used to shrink tumors, slow cancer s growth, keep the cancer from spreading, relieve disease-related symptoms or prolong survival. In addition to destroying cancer cells, chemo-
8 therapy also affects some normal cells which leads to commonly experienced side effects. (See information about managing symptoms and side effects.) Chemotherapy is given as a single drug or in a combination of drugs; combination chemotherapy may significantly increase the amount of cancer cells that are destroyed. Most chemotherapy drugs are given intravenously (through a vein.) Because the drugs continue to work for days or weeks after they are taken, a period of rest and recovery follows each dose. Radiation Radiation therapy, also called radiotherapy, is another common treatment option for some types of lung cancer. With radiation therapy, high-energy X-rays are used to shrink tumors, relieve pain and pressure, decrease symptoms, and improve quality of life. Radiation can be effective when used alone or in combination with surgery or chemotherapy. Cancer specialists called radiation oncologists provide this specialized treatment. Radiation treatments are given to a specific area of the body called a radiation field during a series of outpatient hospital visits. The amount of radiation used to treat lung cancer varies, based on the size and location of the tumor and the sensitivity of the normal tissue that surrounds it. Side effects of radiation depend on where the radiation field is located. Newer Therapies Cancer treatments are improving constantly. Although many of these newer drugs and techniques are still under investigation, there are treatment options that may hold hope for controlling the disease and improving quality of life for people with lung cancer. The following section is an overview of some major areas of discovery. Talk with your doctor about new cancer treatments in development, to determine what might be most appropriate for you. Targeted Therapies One of the most exciting approaches to cancer treatment today is the expanding area of targeted therapies. Unlike chemotherapy, targeted therapies are designed to work through specific pathways involved in cancer growth to attack cancer cells directly, with less effect on healthy tissues. Targeted therapies aim to interfere with the growth of cancer cells and the molecular pathways that signal the cancer development process, without disrupting the functions of normal cells and tissues. The result is to improve symptoms, shrink tumors or stabilize the disease. New Ways to Stop Cancer as It Grows Targeted therapies include agents that: Prevent cell growth Inhibit the invasive nature of tumor cells to control the spread of cancerous cells and metastasises Cause apoptosis (spontaneous cell death) of cancer cells Are angiogenesis inhibitors, which block the growth of new blood vessels and interfere with growth and metastases from solid tumors
9 Some of the more common targeted therapy types are defined below: Epidermal growth factor receptor (EGFR) inhibitors. Epidermal growth factor receptors (EGFR) are naturally occurring cell proteins that sit on the surface of cells that appear to aid in the growth of cancer cells, thereby causing lung tumors to grow. A compound designed to cut off that aid by blocking EGF receptors is Tarceva (erlotinib). This drug seems to work best in people who have never smoked or who have certain genetic characteristics. Researchers are studying ways to identify the people who will benefit most from this treatment. Tarceva has been approved by the FDA for the treatment of advanced non-small cell lung cancer as a second-line and third-line therapy (after initial treatment). Anti-angiogenesis therapy. Cancerous tumors create new blood vessels through a process called angiogenesis. New blood vessels help cancer cells grow and spread. Anti-angiogenesis is a new treatment approach to prevent the growth of blood vessels to tumors, thus stopping the growth of the tumor. Various clinical trials are evaluating different anti-angiogenesis drugs to assess their impact on the disease. AvastinTM (bevacizumab) is an angiogenesis inhibitor, and a monoclonal antibody. It was approved by the FDA in combination with carboplatin and paclitaxel for the treatment of patients with advanced metastatic NSCLC, who have not received prior chemotherapy. Monoclonal antibodies. Substances designed to attach themselves to a specific protein (antigen), which means that they are laboratory produced and can be tailored to attack and destroy only certain tumor cells. In addition to AvastinTM, other monoclonal antibodies being investigated in patients with NSCLC are ABX-EGF, and Erbitux (certuximab). Ablation therapy. Radiofrequency or laser therapy, which involves a thermal energy is applied to destroy the cancer cells. This is only an option on small lesions. (See also: Treatment for NSCLC by Stage IA and IB.) Another option which can have a curative-intent is sterotactic radiosurgery for lung lesions in medically inoperable patients or those who refuse surgery with Stage I disease. This uses a focused beam of radiotherapy to destroy the tumor cells but is dependent upon size of the tumor for feasibility purposes. This is planned to be available at St. Joseph Hospital in the near future. Some other targeted therapies currently available in clinical trials include: Vascular endothelial growth factor receptor (VEGFr) inhibitors, such as the drugs sorafenib, sunitinib and others, which work by preventing the ability of cancer cells to stimulate the growth of blood vessels, thereby slowing or stopping cancer cell growth. TS, DHFR and GARFT Enzyme inhibitors, such as AlimtaTM(pemetrexed for injection), which is approved for the first-line treatment of mesothelioma and second-line treatment of NSCLC. This drug helps to inhibit the three enzymes (TS, DHFR, and GARFT) which are needed to increase the number of cancer cells and growth of the lesion. Other, similar agents are available through clinical trials.
10 Vaccine Therapy Several new cancer vaccines are being evaluated for lung cancer treatment. These are used as treatment to help the person s immune system recognize a tumor as foreign and push the body s normal defense mechanisms to destroy tumor cells. Vaccines have many theoretical advantages, such as greater specificity in targeting cancer cells with fewer toxic side effects. Some of the new approaches have clear clinical efficacy as well. Vaccines come in a wide variety of types, but can be made from an individual s tumor cells that have been removed and made into a vaccine, or consist of a synthesized tumor-specific antigen. For more information on our lung vaccine clinical trial MAGE-A3 please contact your Nurse Navigator or the St. Joseph Hospital Research team. Surgical Techniques Surgery remains the standard treatment for Stage I or II NSCLC, but some people have health problems that make surgery inappropriate. For people with poor lung function who cannot tolerate major surgery, a new technique called video-assisted thoracic surgery (VATS) may be helpful. VATS: Uses a tiny video camera to guide the surgeon Makes it possible to remove a section of a lung though a small incision May reduce surgical trauma and shorten hospital stays by avoiding large incisions. However, with VATS, a surgeon cannot see the entire lung and may not obtain adequate lymph node samples to check for the spread of cancer. Other surgical techniques being investigated include nerve-sparing surgery, computerenhanced imaging tools and stereotactic radiologic surgical tools that use high-energy X-rays (e.g., a gamma knife) to destroy deep-seated tumors for brain metastases. Radiation Techniques Three-dimensional conformal radiation therapy uses computers to shape radiation beams to match the tumor s size and shape, so the radiation dose can be intensified over a shorter time period without harming the surrounding tissue. Fractionated stereotactic radiosurgery uses a CT scanner to target tumors using radiation with high accuracy. Accelerated hyper-fractionation varies the dose and duration between radiation treatments, giving smaller doses of radiation more often. Brachytherapy delivers high doses of radiation from very short distances by placing a radioactive source, sealed inside a container, on the surface of the body near the tumor or the affected area. Radiation modifiers drugs that improve the way cancer cells respond to radiation. Radiation sensitizers drugs that make cells more sensitive to the effects of radiation.
11 Treatment Decision-Making Tool This tool is designed to help you discuss treatment options with your doctor. Bring this with you to appointments and use it as a guide to help you with discussions. Medical Background Questions Answers What type of lung cancer do I have? (The type of cancer will determine the types of treatment you will receive) What is the stage of my lung cancer? (The stage of cancer will also determine the types of treatment available) What is my current health status? (Is this the first time you are receiving treatment? Your overall health can affect the types of treatments you can tolerate) What should be the goal of my treatment? (The goal of treatment determined by you and your doctor [cure, symptom control, prolonged remission] may affect the type of treatment available to you) How can I prepare for side effects? (By preparing for common side effects before starting treatment, you can improve your quality of life and stay on-course throughout your treatment schedule)
12 Treatment Decision-Making Tool - Part Two Treatment Options: Things to consider when making a treatment decision As you discuss treatment options with your doctor, take notes in the columns below. Potential side effects (i.e., hospitalization, hair loss, fatigue, neuropathy, etc.) Quality of Life/Treatment Convenience (i.e., required clinic visits to receive treatments, monitoring blood counts, restricted activity, etc.) Effectiveness (i.e., what are the chances that this treatment will work for me?) Surgery (Can the tumor be removed?) Pre- or post-surgery chemotherapy Pre- or post-surgery radiation Targeted therapy Investigational therapy in clinical trials Combination treatments (from above) Best supportive care
13 Lung Cancer Staging and Treatment Staging lung cancer looks at where the cancer is located and whether it has spread to other parts of the body. This is very important in order to determine best options for treatment. There is no one treatment for lung cancer. Your treatment will be as individual as you are and will adapt to your changing needs and side effects. The stage of cancer is the major focus in determining a treatment plan. It is important to understand the concept of stage for lung cancer, as it classifies you into a group of patients with comparable outcomes who are eligible for similar treatment. The following review of treatments by stage of NSCLC and small cell lung cancer provides only general descriptions of the usual approaches. There are many variations of existing options, and many new treatments are emerging that provide additional treatment options. Please note that non-small and small cell lung cancer are treated differently. Non Small Cell Lung Cancer (NSCLC) Staging Stage IA and IB In Stage IA, the cancer is smaller than three centimeters (slightly less than 1 1/4 inches), has not spread to the membranes that surround the lungs, lymph nodes or other distant organs, and does not affect the main branches of the bronchi. Stage IB means the tumor is either larger than three centimeters or may involve a portion of the main bronchus or the visceral pleura (sac surrounding the lung). However, stage IB tumors do not involve lymph nodes or extend to the center of the chest outside of the lung and do not involve more than one area in the lung. NSCLC Stage IIA and IIB in stage IIA, the tumor is no larger than three centimeters, has not spread to the membranes that surround the lungs, and does not affect the main branches of the bronchi. However, it has spread to the lymph nodes within the cancerous lung but not to distant sites. Stage IIB means the cancer is either larger than three centimeters. It has spread to the membranes that surround the lung and/or the lymph nodes within the same cancerous lung or has spread to the chest wall, the diaphragm and/or the membranes that surround the lungs. It does not affect the main branches of the bronchi. However, it has spread to the lymph nodes within the cancerous lung but not to distant sites. Stage IIB means the cancer is either larger than three centimeters and has spread to the membranes that surround the lung and/ or the lymph nodes within the same cancerous lung, or has spread to the chest wall, the diaphragm, the membranes that surround the space between the lungs, or the membranes that surround the sac of the heart without involving lymph nodes around the heart and trachea (mediastinal lymph nodes) or distant organs. Stage IIIA Stage IIIA is confined to the lung and the lymph nodes around the windpipe or in the mediastinum (the place behind the chest bone and in front of the heart) on the same side as the cancerous lung. Stage IIIB Stage IIIB can be a tumor of any size that may involve the bronchus, trachea (main airway), esophagus, backbone, or the fluid in the space surrounding the lung and, most importantly, has spread to the lymph nodes near the collarbone on either side and/or the lymph
14 nodes within the lung or mediastinal lymph nodes on the side that is opposite the cancerous lung. Sometimes Stage IIIB tumors are referred to as wet or dry. Wet means the cancer has spread into the fluid that fills the space surrounding each lung (pleural fluid) or around the heart (pericardial fluid). Stage IV Stage IV is the most advanced form because the cancer has spread from the lungs to distant parts of the body such as the liver, adrenal glands, brain or bone. Treatment for NSCLC by Stage Stages IA and IB People diagnosed at these early stages have the best chance of recovery. Surgery. Surgery alone is the standard of care for patients with Stage I lung cancer. Surgery is the gold standard of curative treatment for localized lung cancer. Traditionally, lung cancer surgery has been performed as a thoracotomy. This involves a 6- to 8-inch-long incision across the patient s side, cutting numerous muscles in the chest wall and separating the ribs. The hospital stay for a thoracotomy is usually one week or longer. However, at St. Joseph Hospital our thoracic surgeons are trained in a recently developed, minimally invasive lung surgery called Video-Assisted Thoracic Surgery (VATS). This is a minimally invasive surgical procedure that allows surgeons to view the inside of the chest wall cavity with a video-assisted camera. Only very small incisions are needed and the recovery time is shorter, with patients usually leaving the hospital in three to four days. It should be noted that there are instances when a traditional thoracotomy is the only option for the patient. People diagnosed with Stage IA or IB NSCLC are usually treated with a VATS surgery and a lobectomy is performed. This is when a whole section, or lobe of the lung is removed. Lobectomies are considered superior to a wedge resection, which removes only a small portion of a lobe. In some cases, it might be necessary to remove an entire lung (pneumonectomy) if tumors are found in more than one lobe or one side of the chest. During lung surgery, the surgeon should definitely perform a complete examination of the lymph nodes in the chest cavity, including the mediastinum. One of the biggest problems with surgeries performed by non-cancer specialists is inadequate assessment of the mediastinal lymph nodes. Ask your surgeon specifically if he/she plans to remove these lymph nodes for examination. Additional therapy. It is possible, but unproven, that chemotherapy after surgery improves survival in people with Stage IB disease. You might want to discuss with a medical oncologist the possibility of chemotherapy in addition to surgery. This therapy will usually consist of a platinum-based drug (cisplatin or carboplatin) and one of several other chemo agents (gemcitabine, taxol, docetaxel, or vinorelbine).
15 Radiofrequency Ablation (RFA) In some cases, lung tumors can not be removed with traditional surgery or individuals are unable to withstand surgery. At St. Joseph Hospital, we have successfully used RFA - a method by which electrodes are used to heat and destroy abnormal tissue. It is a promising new technique to safely and effectively treat patients who have inoperable lung tumors. This method can also be used in very specific tumors of later stage lung cancer. NCI-recommended standard treatment options for Stage I lung cancers: Surgical removal of a wedge, segment or lobe of one lung, possibly with removal of part of a bronchial tube Radiation therapy (if the person has other health conditions that would make surgery inadvisable) Clinical trials of adjuvant chemotherapy after surgical resection Prevention trials to reduce the risk of a second lung cancer. Stages IIA and IIB If you are diagnosed with Stage IIA or IIB NSCLC, it is recommended that you meet with a surgeon, a medical oncologist and a radiation oncologist to discuss possible therapeutic options, including clinical trials for your stage of disease. Surgery. Surgery has been the standard of treatment for Stage IIA and IIB and selected stage IIIA disease (such as a lobectomy, bilobectomy, or pneumonectomy) if the person can medically tolerate the procedure. Chemotherapy. Recent studies have shown that chemotherapy after surgery improves survival in people with Stage IIA and IIB lung cancer and consists of a platinum-based regimen. If the chest is involved with the IIB cancer you may benefit from treatment with radiation and/or chemotherapy before surgery. The hope is to shrink the tumor to improve the chances that the surgical procedure will be successful in removing all of the tumor. Ask your doctor if chemotherapy would be a good option for you. Radiation Therapy. If you have a stage IIB tumor that involves the chest wall, radiation may be given prior to surgery to improve the chances of removing all the cancer cells with surgery. NCI-recommended standard treatment option: Surgical removal of the whole lung, one lobe, a wedge or segment, or part of a bronchial tube Radiation therapy for people who could have surgery but have other health problems that make surgery impossible Clinical trials of adjuvant chemotherapy with or without other therapies after curative surgery Clinical trials of radiation therapy after surgery Clinical trials of a novel targeted therapy, with or without other modalities after curative surgery
16 Stage IIIA Stage IIIA NSCLC is a somewhat complex stage of lung cancer to manage. Several treatment options are potentially effective. However, there is not enough evidence to determine which treatment is best in any one individual. Treatment at this stage is determined by whether the tumor can be operated on or not. Operable Stage IIIA NSCLC The standard of care for potentially operable Stage IIIA NSCLC is controversial. Recent data from clinical trials has been inconclusive as to which treatment is most effective. Depending on the details of your case, options may include: Surgery followed by chemotherapy Chemotherapy and/or radiation followed by surgery Chemotherapy and radiation alone Surgery followed by chemotherapy, with or without radiation Surgery. Surgery without chemotherapy may be possible in some cases if the tumor can be easily removed, especially when the lymph nodes were found to be involved only at the time of surgery. When mediastinal lymph nodes are involved, most commonly chemotherapy with or without radiation is given before or after surgery. Radiation. Radiation is sometimes used for Stage IIIA NSCLC either with chemotherapy or in combination with surgery. Radiation combined with chemotherapy may be used instead of surgery to eliminate the tumor, and is probably the most common form of therapy at this stage. NCI-recommended standard treatment options: Surgery followed by chemotherapy in people with operable tumors and minimal lymph node involvement Radiation alone for those who cannot physically tolerate chemotherapy and surgery Chemotherapy combined with radiation Inoperable Stage IIIA NSCLC Surgery. Stage IIIA NSCLC is considered inoperable when the tumor is too large, in a location that is difficult for the surgeon to reach, or the patient has other complicating factors that put him or her at risk for surgery. Chemotherapy. The standard of care for inoperable Stage IIIA is chemotherapy combined with radiation therapy in a fit patient. Commonly used chemotherapy drugs include a platinum drug together with one of several non-platinum based drugs. Delivery of chemotherapy and radiation therapy concurrently (at the same time) appears to be superior to the sequential administration of chemotherapy and radiation treatments. Radiation therapy. Radiation therapy is often used as part of the treatment for this stage of cancer. Several clinical trials are evaluating different types and timing of chemotherapy. NCI-recommended standard treatment options: Chemotherapy together with radiation therapy.
17 Stage IIIB and Stage IV The treatment for Stage IIIB and Stage IV NSCLC depends on whether the stage III tumor is associated with pleural effusion (leakage of fluid between the lungs and chest wall). If there is a pleural effusion, the tumor is often referred to as a wet IIIB. A stage IIIB tumor without pleural effusion (a dry IIIB) is generally treated much different than wet tumors. People who have Stage IIIB NSCLC without a pleural effusion are usually offered the same treatment options as those patients with inoperable Stage IIIA NSCLC, though surgery may be an option based on the tumor location. People with Stage IIIB NSCLC who also have a pleural effusion are usually treated with similar therapies as patients with Stage IV. Most people with Stage IIIB wet and Stage IV NSCLC are treated with radiation therapy only for areas of cancer that cause specific symptoms, such as pain or obstruction of a vital organ. Cure is rarely achieved in patients with stage IIIB wet or IV lung cancer, so the goal of treatment is to improve quality of life and prolong survival. Surgery. Surgery is rarely indicated for people with Stage IIIB wet or Stage IV NSCLC. Chemotherapy. Chemotherapy improves survival and quality of life when compared to best supportive care (to relieve symptoms only) in some people with Stage IIIB (with pleural effusion) and Stage IV NSCLC who are healthy enough to tolerate the side-effects. Current clinical trials have shown that a combination of different drugs, is superior to giving one drug alone. AvastinTM (bevacizumab) combined with chemotherapy may be used in select patients. Approximately 50-60% of people with advanced NSCLC who receive chemotherapy achieve some clinical benefit. Approximately 25% achieve a partial response (tumor shrinkage of 50% or more). A small percentage will experience a disappearance of the entire disease, while others have a stabilization of their disease. NCI-recommended standard treatment options: Chemotherapy consisting of carboplatin plus paclitaxel with the anti-angiogenesis agent Avastin (bevacizumab), in patients without contradictions (such as: squamous cell history, brain metastases, coughing up blood). Chemotherapy combinations: Gemzar (gemcitabine) + platinum agent Taxol (paclitaxel) + platinum agent Navelbine (vinorelbine) + platinum agent Taxotere (docetaxel) + platinum agent
18 Radiation. Radiation therapy is often used to shrink the tumor size and relieve symptoms to improve a person s quality of life. Targeted Therapy. Targeted therapies continue to be studied in clinical trials with recurrent NSCLC. Tarceva (erlotinib) found to be superior to supportive care as a second or third line treatment. AvastinTM (bevacizumab) is an antibody approved in combination with chemotherapy for patients with newly diagnosed NSCLC, but may also be used in second-line therapy. If you choose not to take chemotherapy or a targeted therapy, supportive care treatment that helps relieve symptoms but does not affect the growth of the cancer may be recommended. Supportive care may include pain control measures, radiation or laser therapy to relieve symptoms. Whatever you and your oncologist decide, there is hope. Even if a cure is not possible, there is hope that effective treatment can maintain or improve your quality of life and even slow or control the disease itself. It is now more possible to treat advanced lung cancer as a chronic condition in some patients, keeping the disease stable until new drugs and treatments are discovered. As mentioned many times in this handbook, it is important for you to talk with your doctor about all of your treatment options, weighing the potential side effects with the possible benefits. Treating Small Cell Lung Cancer Current treatment for SCLC involves a combination of different chemotherapy drugs with or without radiation therapy. Because new therapies for cancer are always in development, you should discuss the latest treatments with your oncologist, including the possibility of finding a clinical trial that might be good for you. Clinical trials generally represent state-of-the-art treatment for SCLC. Treatment is determined by the stage of your disease, your overall health, the possible side effects of specific therapies and your preferences. Members of your healthcare team have expertise that can be helpful as you weigh treatment options. No matter what choices you make, it is important that you get the information you need to understand the potential impact of those decisions for your health and for your future.
19 Staging of SCLC Small cell lung cancer is generally categorized as either limited-stage or extensive-stage disease: Limited stage tumors typically are on one side of the chest in one lung and within the surrounding area that can be treated by radiation. Extensive stage tumors have spread outside one lung to the other lung or to other areas of the body. SCLC is an aggressive type of lung cancer. By the time it is diagnosed, it often has spread to the lymph nodes in the chest or to other organs. Nevertheless, it is curable in some cases and there are many people who live meaningful and productive lives with good quality of life in the face of a serious illness such as SCLC. Treatment of SCLC by Stage Newly Diagnosed Limited-Stage SCLC According to the NCI, the current standard treatment for patients with newly diagnosed limited-stage SCLC should be four cycles of combination chemotherapy containing VP-16 (etoposide) and cisplatin concurrently with chest irradiation. Prophylactic cranial irradiation preventive radiation therapy to the brain is used to protect against brain metastases, and it is recommended for some people with limited-stage SCLC who are in remission after initial chemotherapy. Newly Diagnosed Extensive-Stage SCLC While extensive-stage SCLC is defined by more advanced disease, it usually responds to chemotherapy initially. The most common treatment is the same chemotherapy without additional radiation therapy. Frequently used first-line chemotherapy drugs include: VP-16 (etoposide) plus a platinum agent like cisplatin or carboplatin Camptosar (irinotecan/cpt-11) plus a platinum agent (not approved at this stage but is often used because it generated promising results in clinical trials) Cytoxan (cyclophosphamide) plus doxorubicin plus vincristine (older regimen less widely used in the U.S.) Treatment of Recurrent SCLC If your small cell lung cancer does not respond to initial therapy or returns within two years of successful treatment, it is considered to be resistant or recurrent SCLC. The goal of therapy at this stage is to improve quality of life and prolong survival. The National Cancer Institute states that while no single chemotherapy regimen should be considered standard, several treatment options have shown promise.
20 Treatment for Mesothelioma What is Mesothelioma? The National Cancer Institute (NCI) states that: Malignant mesothelioma, a rare form of cancer, is a disease in which cancer (malignant) cells are found in the sac lining the chest (the pleura), the lining of the abdominal cavity (the peritoneum) or the lining around the heart (the pericardium). How do you get Mesothelioma? Most people with malignant mesothelioma have worked on jobs where they breathed asbestos. Others have been exposed to asbestos in a household environment, often unaware. There is some evidence that family members and others living with asbestos workers have an increased risk of developing mesothelioma, and possibly other asbestos related diseases. This risk may be the result of exposure to asbestos dust brought home on the clothing of asbestos workers. This worker is spreading asbestos on the boiler of a locomotive. This man is working with asbestos without any breathing protection. The asbestos can also be seen on his hat and coveralls. People began to suspect there may be an association with asbestos exposure and illness in the 1940 s.
21 How much exposure does it take to get the disease? An exposure of as little as one or two months can result in mesothelioma 30 or 40 years later. How long does it take after exposure for the disease to show up? People exposed in the 1940s, 50s, 60s, and 70s are now being diagnosed with mesothelioma because of the long latency period of asbestos disease. What are the stages of mesothelioma? Malignant mesothelioma stages are divided into two groups: localized and advanced disease. In localized malignant mesothelioma (stage I) cancer is found in the lining of the chest wall and may also be found in the lining of the lung, the lining of the diaphragm, or the lining of the sac that covers the heart on the same side of the chest. Advanced malignant mesothelioma includes stage II, stage III, and stage IV. Stage II-cancer is found in the lining of the chest wall and the lymph nodes on the same side of the chest. Cancer may also be found in the lining of the lung, the lining of the diaphragm, or the lining of the sac that covers the heart on the same side of the chest. Stage III-cancer has spread to any of the following areas: the chest wall, the mediastinum, the heart, beyond the diaphragm and the peritoneum. Cancer may have also spread to to lymph nodes on the other side of the chest or outside the chest. Stage IV-cancer has spread to distant organs or tissues. How is mesothelioma treated? Traditionally malignant mesothelioma is treated with multi-modality therapy including surgery, radiation therapy and chemotherapy. Are there any potential curative procedures for mesothelioma? The procedures listed below are performed for curative intent. The goal is removal of gross disease, with the knowledge that microscopic disease will most likely remain. For this reason many patients are given chemotherapy and/or radiation therapy after surgery to remove any cancer cells that remain. In the past St. Joseph Hospital has traditionally referred patients to the East Coast for mesothelioma surgery. Most recently, the extrapleural pneumonectomy surgery has been made available through St. Joseph Hospital Lung Program by our expertly trained thoracic surgeons. We are proud of the fact that West Coast residents can have these potentially curative procedures for Mesothelioma. Please call for a surgical consultation to find out if you may be a candidate for these procedures.
22 For Pleural Mesothelioma: Pleurectomy/decortication is usually performed on patients with early stage disease (Stage I and selected Stage II), and attempts to remove all gross tumor. If it is found that all tumor can not be removed without removing the lung, a pneumonectomy (removal of lung) may be performed at the same time. Extrapleural pneumonectomy surgery is an option for a select few. Early-stage malignant pleural mesothelioma patients with respectable cancer formation (capable of being removed) are the best candidates for extrapleural pneumonectomy surgery. Extrapleural Pneumonectomy -- The Procedure Extrapleural pneumonectomy surgeries are incredibly invasive, requiring a great deal of preoperative and postoperative treatment. Patients are given a general anesthesia to limit preoperative pain and discomfort. For management of postoperative pain, a thoracic epidural catheter is inserted before the operation. Extrapleural pneumonectomy surgery itself begins by entering the chest over the unrestricted sixth rib (occasionally the sixth rib is removed). Extrapleural dissection follows, during which the surgeon takes great care to avoid entering the pleural cavity, as this could cause spillage of malignant cells within the operative field. The parietal pleura (lining of the lung) is removed along with the pericardium (lining of the heart), the diaphragm (the muscle that assists with breathing) and the appropriate lung (dependent on affected side of the chest). Extrapleural Pneumonectomy - Postoperative Care Postoperative care of extrapleural pneumonectomy patients is similar to that of patients recovering from a standard pneumonectomy procedure. Postoperative patients are at risk of developing dangerously low blood pressure (hypotension) resulting from reconstruction of the pericardium. If a postoperative extrapleural pneumonectomy patient experiences hypotension, immediate follow-up surgery is needed. Managing a patient s pain is the most important postoperative concern. If pain is not controlled, it could lead to the collapse of the remaining lung (called postoperative atelectasis). On the second day following extrapleural pneumonectomy, patients begin pulmonary rehabilitation to restore heart function to normal levels. Postoperative treatment can require a hospital stay of five to ten days. After the patient goes home from the hospital a three to four week course of outpatient respiratory and physical therapy is ordered. This helps strengthen the remaining lung, increases ventilation, improves healing and promotes exercise tolerance. The patient is closely followed by the Lung Program treatment team.
23 Considerations after Initial Lung Cancer Treatment Recurrence After treatment is completed, there is still a high risk that lung cancer will recur in the original site or spread to another site. The risk for recurrence increases when the disease is in an advanced stage. It is important that people with lung cancer work closely with their healthcare team to be sure that their condition is monitored regularly. Treatment guidelines suggest that people who have been treated for lung cancer should see their oncologist: Every three months for the first two years Every six months for two more years, and Annually after four years Many people continue to see their oncologists or primary care doctor every three months so that any recurrence can be detected as early as possible. At these visits, your doctor will check your general health status, probably do blood work and other tests, and may schedule a CT or other scan depending on your health history. Palliative Therapy In most cases, treatment of advanced, metastatic lung cancer is considered to be palliative rather than curative. The goal of palliative therapy is to prolong survival, shrink the tumor if possible, reduce/alleviate symptoms and improve your quality of life. Palliative therapy can include surgery, radiation therapy, chemotherapy and targeted cancer therapies, as well as pain management and oxygen therapy. As with any treatment, make sure you understand the goals and possible benefits and negative aspects of any palliative therapy before you make a decision about it.
24 Resources American College of Chest Physicians Toll Free: Offers suggestions for lung cancer specialists and second opinions. American Cancer Society (ACS) Toll Free: ACS Provides local support, resources, and information for all cancer types, including lung cancer. American Lung Association (ALA) Toll Free: LUNGUSA Provides free interactive decision support tools to answer the question, What does the clinical information mean to me? You will receive a personalized treatment options report tailored to your diagnosis. Your report will provide the pros and cons of each treatment, side effects, questions to ask your physician, plus access to relevant summaries of clinical studies. Focus on Lung Cancer Toll free: HOPE (4673) Call the Lung Cancer Toll-Free Information Line for lung cancer support. The Lung Cancer Alliance (LCA) Toll Free: Provides patient support and advocacy to people affected by lung cancer. Also maintains a website on risk and screening at The National Cancer Institute (NCI) Toll Free: CANCER Provides comprehensive and up-to-date information about lung cancer, treatment options a nd more. The Wellness Center Toll Free: WELL A non-profit organization dedicated to providing free support, education and hope to people with cancer and their loved ones.
25 The national organizations listed below can provide additional information and support. Clinical Trials National Cancer Institute (NCI) Toll Free: CANCER Provides comprehensive information about cancer clinical trials and access to NCI-sponsored trials. If you have questions or cannot find a clinical trial, call to speak with a Cancer Information Service specialist who can help you (in English or Spanish). National Library of Medicine, National Institutes of Health Toll Free: Provides a thorough and searchable listing of federally sponsored clinical trials and general information. The Wellness Community Toll Free: WELL In collaboration with Emergingmed.com this site provides general information about cancer trials and an online search engine to find a clinical trial for your cancer. Complementary and Alternative Medicine National Center for Complementary and Alternative Medicine (NCCAM) Toll Free: Provides information about and conducts research and training on complementary and alternative medicine. The National Cancer Institute s Office of Cancer Complementary and Alternative Medicine (OCCAM) Toll Free: CANCER OCCAM s goal is to increase the amount of quality information and cancer research conducted on complementary and alternative medicine (CAM) therapies. The American Cancer Society (ACS) Toll Free: ACS The ACS Guide to Complementary and Alternative Cancer Methods and the booklet Making Treatment Decisions: Complementary and Alternative Therapy can be ordered on their website or by calling.
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Non-Small Cell Lung Cancer About Your Lungs and Lung Cancer How do your lungs work? To understand lung cancer it is helpful to understand your lungs. Your lungs put oxygen into the blood, which the heart
Surgery. Wedge resection only part of the lung, not. not a lobe, is removed. Cancer Council NSW
 The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
The treatment you receive will depend on your lung cancer type, for example, whether you have a non-small cell lung cancer Adenocarcinoma or Squamous cell carcinoma, and if this is a sub-type with a mutation.
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
SMALL. 1-800-298-2436 LungCancerAlliance.org
 UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
UNDERSTANDING Non- SMALL CELL LUNG CANCER 1-800-298-2436 LungCancerAlliance.org A guide for the patient I ANATOMY OF THE LUNGS The following image shows different parts that make up the lungs. Please use
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Lung Cancer Understanding your diagnosis
 Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
People Living with Cancer
 Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Patient Guide ASCOInformation for People Living with Cancer ADVANCED LUNG CANCER TREATMENT Recommendations of the American Society of Clinical Oncology Welcome The American Society of Clinical Oncology
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
Lung Cancer Treatment
 Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
Scan for mobile link. Lung Cancer Treatment Lung cancer overview More than one in four of all diagnosed cancers involve the lung, and lung cancer remains the most common cancer-related cause of death among
The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options
 Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Why We re Here The lungs What is lung cancer? How common is it? Risks & symptoms Diagnosis & treatment options What Are Lungs? What Do They Do? 1 Located in the chest Allow you to breathe Provide oxygen
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
How To Understand How Cancer Works
 Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Lung Cancer. Understanding your diagnosis
 Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
About lung cancer. Contents. The lungs
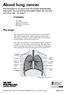 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
This factsheet aims to outline the characteristics of some rare lung cancers, and highlight where each type of lung cancer may be different.
 There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
There are several different kinds of lung cancer, often referred to as lung cancer subtypes. Some of these occur more often than others. In this factsheet we will specifically look at the subtypes of cancers
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE
 Providing the best in cancer care for Veterans TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE VA Pittsburgh s state-of-the-art TomoTherapy machine, which delivers radiation to patients.
Providing the best in cancer care for Veterans TREATING LUNG CANCER AT VA PITTSBURGH HEALTHCARE SYSTEM A HERO S GUIDE VA Pittsburgh s state-of-the-art TomoTherapy machine, which delivers radiation to patients.
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
YOUR LUNG CANCER PATHOLOGY REPORT
 UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
UNDERSTANDING YOUR LUNG CANCER PATHOLOGY REPORT 1-800-298-2436 LungCancerAlliance.org A GUIDE FOR THE PATIENT 1 CONTENTS What is a Pathology Report?...3 The Basics...4 Sections of a Pathology Report...7
Lung Carcinoid Tumor
 Lung Carcinoid Tumor What are lung carcinoid tumors? Lung carcinoid tumors (also known as lung carcinoids) are a type of lung cancer, which is a cancer that starts in the lungs. Cancer starts when cells
Lung Carcinoid Tumor What are lung carcinoid tumors? Lung carcinoid tumors (also known as lung carcinoids) are a type of lung cancer, which is a cancer that starts in the lungs. Cancer starts when cells
Malignant Mesothelioma
 Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant Mesothelioma
 Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Malignant mesothelioma is a tumour originating from mesothelial cells. 85 95% of mesotheliomas are caused by asbestos exposure. It occurs much more commonly in the chest (malignant pleural mesothelioma)
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer.
 Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer. The Condition: Lung Cancer The lung is the organ that moves oxygen through your body. You have two lungs
Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer. The Condition: Lung Cancer The lung is the organ that moves oxygen through your body. You have two lungs
Lung cancer (non-small-cell)
 Patient information from the BMJ Group Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important decisions about
Patient information from the BMJ Group Lung cancer (non-small-cell) It can be devastating to find out that you or someone close to you has lung cancer. You will have to make some important decisions about
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Understanding Lung Cancer
 Lung Understanding Lung Cancer Information for individuals with lung cancer and their families Your Primary Team at the JCC Medical Oncologist Primary Nurse Radiation Oncologist Primary Nurse Other Oncology
Lung Understanding Lung Cancer Information for individuals with lung cancer and their families Your Primary Team at the JCC Medical Oncologist Primary Nurse Radiation Oncologist Primary Nurse Other Oncology
Asbestos and your lungs
 This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
This information describes what asbestos is and the lung conditions that are caused by exposure to it. It also includes information about what to do if you have been exposed to asbestos, and the benefits
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
HEALTH EFFECTS. Inhalation
 Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
Health Effects HEALTH EFFECTS Asbestos can kill you. You must take extra precautions when you work with asbestos. Just because you do not notice any problems while you are working with asbestos, it still
THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR:
 central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
Understanding. Pancreatic Cancer
 Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
What is Mesothelioma?
 What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
What is Mesothelioma? Mesothelioma is a rare type of cancer that develops in the mesothelial cells found in one s body. These cells form membranous linings that surround and protect the body s organs and
PRIMARY LUNG CANCER TREATMENT
 PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
PRIMARY LUNG CANCER TREATMENT Cancer Care Pathways Directorate Tailored Information in Cancer Care (TICC) Sir Anthony Mamo Oncology Centre December 2014 Contents About this booklet 1 Types of Lung Cancer
Asbestos Related Diseases
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Mesothelioma and Asbestos
 CANCER INFORMATION FACTSHEET Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
CANCER INFORMATION FACTSHEET Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
The following information is only meant for people who have been diagnosed with advanced non-small cell
 Important information for people with advanced non-small cell lung cancer The following information is only meant for people who have been diagnosed with advanced non-small cell lung cancer (NSCLC). NSCLC
Important information for people with advanced non-small cell lung cancer The following information is only meant for people who have been diagnosed with advanced non-small cell lung cancer (NSCLC). NSCLC
Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too.
 Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Lung cancer. A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment
 Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Lung cancer A guide for journalists on Non-Small Cell Lung Cancer (NSCLC) and its treatment Contents Contents 2 3 Section 1: Lung Cancer 4 i. Types of lung cancer 4 ii. Causes and risk factors 5 iii. Symptoms
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Asbestos Related Diseases. Asbestosis Mesothelioma Lung Cancer Pleural Disease. connecting raising awareness supporting advocating
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
Emphysema. Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Breast Cancer. CSC Cancer Experience Registry Member, breast cancer
 ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
Multiple Myeloma. This reference summary will help you understand multiple myeloma and its treatment options.
 Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Lung Cancer. Know how to stay strong
 Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
Lung Cancer Know how to stay strong What is cancer? 2 Cancer is a disease when some cells in the body grow out of control Normal cells Your body has many tiny cells and keeps making new cells to keep you
Mesothelioma and Asbestos
 Cancer information factsheet Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
Cancer information factsheet Mesothelioma and Asbestos The information in this factsheet will help you to understand more about mesothelioma. It is an agreed view on this cancer by medical experts. We
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
Lung cancer case study
 Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Change Presentation title and date in Footer dd.mm.yyyy Lung cancer case study Dr Jaishree Bhosle Consultant Medical Oncologist Change Presentation title and date in Footer dd.mm.yyyy 1 2 Part One Initial
Brain Tumor Center. A Team Approach to Treating Brain Tumors
 Brain Tumor Center A Team Approach to Treating Brain Tumors Introducing Our Brain Tumor Center Making an appointment with the Brain Tumor Center at the Center for Advanced Medicine is the important first
Brain Tumor Center A Team Approach to Treating Brain Tumors Introducing Our Brain Tumor Center Making an appointment with the Brain Tumor Center at the Center for Advanced Medicine is the important first
Basic Radiation Therapy Terms
 Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
Malignant Pleural Mesothelioma. NCCN Guidelines for Patients
 Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
Malignant Pleural Mesothelioma NCCN Guidelines for Patients Presented with support from the national law firm of Baron & Budd Also available at NCCN.com About this booklet Its purpose Learning that you
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
