ORIGINAL ARTICLE. Mirja Sargent & Stefan Boeck & Volker Heinemann & Karl-Walter Jauch & Thomas Seufferlein & Christiane J. Bruns
|
|
|
- Merilyn Peters
- 8 years ago
- Views:
Transcription
1 Langenbecks Arch Surg (2011) 396: DOI /s ORIGINAL ARTICLE Surgical treatment concepts for patients with pancreatic cancer in Germany results from a national survey conducted among members of the Chirurgische Arbeitsgemeinschaft Onkologie (CAO) and the Arbeitsgemeinschaft Internistische Onkologie (AIO) of the Germany Cancer Society (DKG) Mirja Sargent & Stefan Boeck & Volker Heinemann & Karl-Walter Jauch & Thomas Seufferlein & Christiane J. Bruns Received: 6 May 2010 /Accepted: 12 July 2010 /Published online: 15 August 2010 # Springer-Verlag 2010 Abstract Background To date, only limited data are available regarding the routine surgical management of patients with exocrine pancreatic cancer (PC) in German community and university hospitals. Methods With the use of a standardized questionnaire, a national survey on surgical and oncological treatment concepts for PC in Germany was conducted on behalf of the Chirurgische Arbeitsgemeinschaft Onkologie and Arbeitsgemeinschaft Internistische Onkologie. The surgical part of that questionnaire contained 25 questions on criteria regarding resectability, surgical techniques, perioperative Mirja Sargent and Stefan Boeck contributed equally. M. Sargent : S. Boeck : V. Heinemann Department of Internal Medicine III, Klinikum Grosshadern, Ludwig Maximilian University of Munich, Munich, Germany S. Boeck stefan.boeck@med.uni-muenchen.de K.-W. Jauch Department of Surgery, Klinikum Grosshadern, Ludwig Maximilian University of Munich, Marchioninistr. 15, Munich, Germany T. Seufferlein : C. J. Bruns (*) Department of Internal Medicine I, University of Halle, Halle, Germany christiane.bruns@med.uni-muenchen.de patient management, and palliative surgical procedures in advanced PC. Data were collected centrally and analyzed using the SPSS software. Additionally, predefined subgroup analyses, classifying the results by the professional site of the responding physician and the local annual number of treated patients, were carried out. Results One-hundred and two questionnaires on the surgical survey section were returned. For the majority of the survey respondents, arterial infiltration is the most important criterion for non-resectability of PC (common hepatic artery, 69.9%; superior mesenteric artery, 85.3%; celiac trunk, 86.3%), whereas only 17.6% would define nonresectability based on portal vein infiltration; 69.9% consider extrapancreatic tumor manifestations as a criterion of surgical non-resectability. Of the survey participants, 53.9% perform a biliary drainage in case of preoperative cholestasis, whereas 43.1% reject this preoperative endoscopic-interventional approach. For cancers of the pancreatic head, 24.5% of surgical units recommend a classical Kausch Whipple procedure, 52.9% prefer the pylorus-preserving partial pancreatoduodenectomy, and 20.6% use both procedures; 74.5% routinely perform a standard lymphadenectomy, whereas 16.7% prefer an extended procedure. A radical pancreatic resection would be performed by 63.7% of survey respondents also if a single liver metastasis would be found intraoperatively. Conclusion Surgical treatment of PC in Germany is heterogeneous; future efforts to implement an evidence-based and standardized surgical management will be necessary.
2 224 Langenbecks Arch Surg (2011) 396: Keywords Pancreatic cancer. Surgery. Survey Introduction In Germany each year, approximately 12,800 patients are newly diagnosed with exocrine pancreatic cancer (PC). The 5-year survival rate of PC currently is below 5%. This is among the lowest in malignant diseases. According to its high malignancy, incidence and mortality are nearly identical in PC, and long-term survival unfortunately is a rare exception [1 3]. To date, radical surgical tumor resection is regarded as the only viable option for any long-term survival or even cure [2]. The biology and prognosis of PC is significantly affected by its early dissemination [4]. Due to the absence of early symptoms and the resulting late detection, in over 90% of patients the cancer has, at the time of diagnosis, spread beyond the boundaries of the pancreatic tissue [2]. However, as any oncosurgical intervention should be performed with curative intent [5], several questions arise regarding the daily management of patients with PC; for instance, how to uniformly define surgical resectability in PC or how to establish standard surgical procedures for optimal treatment outcome in this patient population. Currently, several fields in the surgical management of patients with PC may be regarded as a matter of scientific debate. These include the value of interventions like preoperative biliary drainage [6 10], the perioperative use of somatostatin analogs [11, 12], the standardization of pathological work-up of resected PC specimens [13, 14], surgical techniques in PC surgery (i.e., lymph node dissection) [15 18], and the importance of surgical treatment options in patients with advanced disease (e.g., palliative surgery, resection of PC metastases) [19 22]. Based on a national survey with standardised questionnaires, this study aimed to evaluate the current daily clinical practise in PC surgery at German community and university hospitals. The results obtained from this multicenter survey were also interpreted within the context of the recently published multidisciplinary S3 guideline on exocrine pancreatic cancer, which was generated as a result of an evidence-based consensus conference, including recommendations for prevention/screening, diagnosis, and treatment of PC [2]. Material and methods Survey design and questionnaire The methods of this multicenter survey have already been published previously [3]. On behalf of the CAO ( Chirurgische Arbeitsgemeinschaft Onkologie ) and AIO ( Arbeitsgemeinschaft Internistische Onkologie ) working groups of the German Cancer Society (DKG), questionnaires regarding the current surgical treatment of PC were sent to members of the CAO and AIO at German community and university hospitals. Responsible for the design of the questionnaire were C. J. Bruns and K. W. Jauch (surgical section) and S. Boeck, T. Seufferlein and V. Heinemann (section for medical oncology). This paper describes the results of the surgical part only, the data regarding the oncological part of the survey have been published separately in 2009 [3]. The questionnaires asked for statistical information about the participating physicians, their respective centers/surgical units (professional site, number of annual patients with PC, and number of PC surgeries per year), local criteria for resectability, pre- and perioperative measures, as well as detailed information about actual surgical procedures. That includes the preferred type of surgical intervention (e.g., extent of lymph node dissection, use of laparoscopy). The surgical section of the study questionnaire consisted of 25 questions, with 6 multiple-choice, 14 yes/no-questions, and 5 open questions. Its main objective was to illustrate the current surgical standard of care for patients with PC in Germany. Participating physicians Between February 2007 and March 2008, 1,130 standardized questionnaires were sent out to all members of the AIO GI cancer study group and all members of the CAO. All participating CAO/AIO physicians were contacted via e- mailing lists. Additionally, members of the project group Gastrointestinal Tumors (chair: C. J. Bruns) of the Tumorzentrum München were contacted via mail and fax, and a participation in the national CAO/AIO survey was offered to each physician registered in this local project group. Furthermore, the questionnaire was published in the journal Z Gastroenterol (2007; 45: ) of the DGVS ( Deutsche Gesellschaft für Verdauungs- und Stoffwechselkrankheiten ) encouraging readers to fill out the questionnaire and return it by fax to the study center at the University of Munich. Statistical analyses All returning questionnaires were collected centrally at the University of Munich, and data were entered into an electronic database by one person (M. Sargent). Study data were analyzed using SPSS software (version 16.0) and the Microsoft Office package (Excel database). Pre-defined subgroup analysis was performed by grouping the results of each question with regard to the professional site of the
3 Langenbecks Arch Surg (2011) 396: responding physician (university hospital vs. community hospital) and to the local number of patients treated by year (<5 patients vs patients vs. >30 patients). Results Participants of the survey From the 1,130 questionnaires that were sent out, 102 questionnaires concerning the surgical part of the survey were completed and returned; 32.4% of the responding surgeons/surgical units were located at university hospitals, and 67.6% at community hospitals. Regarding the annual number of patients seen with PC, 6 respondents (5.9%) replied to see less than 5 patients per year; 20.6% see between patients, 18.6% see patients, 14.7% have annual PC patient contacts, 9.8% see between 41 and 50, and 30.4% treat more than 50 patients with PC every year. The number of surgical resections of PC per year was specified by nine surgical units with less than five (8.8%) resections. Of the 42 resections between 11 and 20 patients per year (41.2%), 16 perform resections (15.7%) and 9 survey participants perform resections (8.8 %). Further, 7 respondents (6.9%) carried out resections, and 18 (17.6%) perform more than 50 pancreatic resections annually at their institution. Surgical criteria for resectability Only 7 (6.9%) of the responding surgeons define a pancreatic tumor as non-resectable if imaging modalities suggests a possible regional lymph node infiltration (cn1). An infiltration of the common hepatic artery equals nonresectability in the opinion of 71 (69.9%) respondents. A pancreatic tumor infiltrating the portal vein is regarded as non-resectable by 18 (17.6%), infiltration of the superior mesenteric artery by 87 (85.3%), and infiltration of the celiac trunk by 88 (86.3%). Extrapancreatic manifestations of the tumor are regarded as a criterion for surgical nonresectability by 71 (69.9%) survey participants (see Fig. 1). Perioperative medical procedures Fifty-five surgeons (53.9%) would decide to perform a biliary drainage in case of a significant preoperative cholestasis (defined for this survey as a bilirubin level of 15 mg/dl), whereas 44 (43.1%) reject this preoperative endoscopic-interventional approach. Eighty-three (81.4%) of the respondents would select to place a biliary stent by endoscopic retrograde cholangiopancreatography (ERCP) in order to treat a preoperative malignant bile duct stenosis, whereas 10 (9.8%) would recommend a percutaneous transhepatic cholangio drainage (PTCD). Fifty-two survey participants (51.8%) apply the somatostatin analog octreotide perioperatively; in contrast, 49 (48.0%) do not use octreotide in the perioperative setting in PC surgery. Surgical procedures Resectable pancreatic tumors Carcinomas of the head of the pancreas are treated by 25 survey respondents (24.5%) with a classical Kausch Whipple procedure (partial pancreatoduodenectomy, PPD); 54 (52.9%) prefer the pylorus-preserving partial pancreatoduodenectomy technique according to Traverso/Longmire (PPPD), and 21 (20.6%) use both procedures, depending on the individual case. Seventy-one surgeons (69.6%) support Fig. 1 Selected criteria of surgical non-resectability in PC cn1 by imaging criteria 6,9% Infiltration common hepatic artery 69,6% Portal vein infiltration 17,6% Infiltration superior mesenteric artery 85,3% Celiac trunk infiltration 86,3% Extrapancreatic tumor manifestations 69,6%
4 226 Langenbecks Arch Surg (2011) 396: the statement that the PPPD shows relevant advantages compared to the classical PPD. Explicitly named (free text answer) were the shorter operation time as well as a better digestive passage and less reflux. Twenty-seven participants (26.5%) do not see a superiority of a PPPD compared to the classical Kausch Whipple procedure. Seventy-six physicians (74.5%) routinely perform a standard lymphadenectomy, whereas 17 (16.7%) prefer an extended procedure; 7 colleagues (6.9%) decide the extent of lymphadenectomy individually based on each single case. Adenocarcinomas of the body of the pancreas are treated by 81 surgeons (79.4%) with a distal pancreatectomy, 10 (9.8%) perform an extended Kausch Whipple procedure. In patients with pancreatic tail carcinomas, 98 survey participants (96.1%) would perform a distal pancreatectomy. In both scenarios (pancreatic body and tail tumors), the removal of local lymph nodes and the spleen is performed within an individual case-by-case decision (free text answer). Forty-two respondents (41.2%) use laparoscopic surgical techniques in pancreatic surgery, most of them for staging (45.6%) or diagnostic (21.7%) procedures, i.e., to exclude peritoneal metastasis (15.2%). Fifty-nine centers (57.8%) never apply laparoscopy within their standard procedures. Intraoperative histological evaluation of the resection margins is a mandatory step for 97 (95.1%) of the survey respondents. Only three surgeons (2.9%) do not perform intraoperative frozen section exams to determine the resection margin status. Eighty-six surgeons (84.3%) would also perform multivisceral resections if the tumor infiltrates surrounding organs, whereas 13 (12.7%) would not perform multivisceral surgical resections. Advanced pancreatic tumors If a preoperatively unknown, but technically resectable distant metastasis (e.g., single liver mass) would be found during the surgical exploration and pancreatic resection, 67 surgeons (65.7%) would remove them, whereas 34 colleagues (33.3%) would not resect these metastases. Sixty-five of the responding survey participants (63.7%) would perform a radical pancreatic resection if a single liver metastasis would be found intraoperatively, whereas 30 surgeons (29.4%) would in this case scenario not resect the primary tumor in the pancreas. Palliative surgical procedures, specifically bypass gastroenterostomy and biliodigestive anastomosis, are performed by 51 survey participants (50.0%) in case of jaundice or pyloric/duodenal stenosis. However, 5 colleagues (4.9%) would also perform such palliative surgical procedures in asymptomatic patients (e.g., no bowel obstruction or malignant bile duct stenosis) with non-resectable PC. In asymptomatic PC patients with distant metastases, 16 surgeons (15.7%) would recommend to perform the above-named palliative surgical procedures. Subgroup analyses In PC surgery, large volume centers (defined by >50 patients/year) are mainly located at German university hospitals (72.7% of university surgical units state to see more than 50 PC patients per year, and 54.5% of university centers perform more than 50 pancreatic resections each year, respectively). Most surgical units localized at community hospitals (53.6%) consult with between 11 and 30 patients with PC annually. Influence of the professional site of the responding surgeon on treatment decisions Figure 2 summarizes the criteria for surgical nonresectability split by the professional site of the responding surgeon. Surgeons (53.6%) working in community hospitals use perioperative octreotide treatment, whereas at university centers, 45.5% of survey surgeons apply this somatostatin analog. Standard lymphadenectomy is performed by 73.9% of community-based surgeons and by 75.8% of the university physicians. As shown in Fig. 3, the opinion on surgical removal of intraoperatively detected, technically resectable distant metastasis differed significantly between surgeons at community and university hospitals (resection rate, 58.0% vs. 81.8%). For the other above-named variables, no significant differences were apparent when analyzing the data with regard to the professional site of the responding surgeon (data not shown). Influence of the number of patients treated per year on treatment decisions Figure 4 illustrates the different assessment of nonresectability criteria in PC surgery with regard to the number of patients treated per year. A PPPD approach is, compared to the classical Kausch Whipple procedure, performed more often at high-volume centers (rate of PPPD; <5 patients/year, 16.7%; patients/year, 47.5%; >30 patients/year, 60.7%). The PPPD is also regarded as more advantageous at hospitals with more than 30 patients per year compared to lower volume centers (see Fig. 5). Discussion Radical surgical resection is still regarded as the only valid option for long-term survival in patients with PC. Although
5 Langenbecks Arch Surg (2011) 396: surgical techniques have improved during the last 10 years, the rate of resections in curative intent is still low. It remains unclear as to how many PC patients in Germany are actually treated according to the consensus-based recommendations suggested by the current S3 guidelines [2]. For this national survey, 102 German surgeons from university and community hospitals completed and returned a questionnaire regarding their local standard surgical management of PC. A return rate of 9% (102/1,130) may be regarded as low for a national survey; however, one must consider that most contacted physicians (mainly via the AIO mailing list) were medical oncologists or gastroenterologists [3]. The available CAO mailing list contained 261 surgeons; thus, a theoretical response rate of 102 (39%) may be regarded as more representative. In fact, we cannot rule out that also surgical oncologists that were contacted via the AIO mailing list responded to the survey; however, the authors would assume that this did not confound the results significantly. Moreover, a main limitation of this national CAO/AIO survey arises from the fact that we contacted only physicians that were registered within the CAO or AIO, respectively. This approach may have resulted in a significant selection bias, which also could have influenced the findings obtained from this national survey. Thus, when interpreting the data, one should be aware of these possible confounders. As many low-volume centers (<5 to 10 PC patients per year) were potentially not contacted for this survey, a possible pre-selection of university and higher-volume community hospitals was performed. Therefore, the results may not necessarily reflect the actual surgical treatment of PC in Germany. This national CAO/AIO survey, however, suggests that several aspects of surgical PC management are heterogeneous in Germany. As shown in Figs. 1 and 2, no standardized definitions for a technically unresectable pancreatic tumor exist. On the one hand, this may be based on the fact that the currently available radiological imaging methods (spiral CT, MRI scan, PET-CT) still have several limitations in the preoperative assessment of resectability; on the other hand, the decision for a radical surgical resection may also correlate with the experience of the operating surgeon. However, only 70% of the survey respondents regard extrapancreatic tumor manifestations as an (imaging) criterion for non-resectability. Regarding the perioperative management of PC patients, the role of the endoscopic-interventional treatment (by ERCP or PTCD) of preoperative jaundice is a matter of debate. Based on previous studies, the S3 guideline from 2007 recommends the use of biliary drainage only in case of cholangitis or if surgical resection needs to be delayed [2, 6 8]. Two recently published studies showed that the routine use of preoperative biliary drainage may increase the rate of postpancreatectomy (infectious) complications [9, 10]. However, the authors are aware of the fact that these data were not available when the survey was conducted. Based on our data, the participants could be divided into two nearly equal groups with regard to the use of preoperative biliary drainage (54% vs. 43%). During the last years, several clinical studies and also a meta-analysis have suggested that the use of a PPPD may be at least as effective as the classical Kausch Whipple procedure in carcinomas of the pancreatic head [2, 15]. Our national data show that the majority of German surgical centers (53%) prefer the PPPD, and we also found a correlation between the number of PC patients treated per year and the use of PPPD (Fig. 5). The role of surgical treatment options in patients with advanced PC is currently a matter of scientific debate. The S3 guideline clearly states that in patients with non- Fig. 2 Criteria of surgical non-resectability in PC grouped by professional site of the responding surgeon cn1 by imaging criteria Infiltration common hepatic artery 3,0% 8,7% 75,8% 66,7% Portal vein infiltration 15,2% 18,8% Infiltration superior mesenteric artery 78,8% 88,4% Celiac trunk infiltration 78,8% 89,9% Extrapancreatic tumor manifestations 57,58% 75,4% Community hospital University hospital
6 228 Langenbecks Arch Surg (2011) 396: ,0% Resection yes 81,8% Community hospital 42,0% Resection no University hospital 15,2% Fig. 3 Resection of technically removable distant metastases during PC surgery (grouped by professional site of the responding surgeon) ,3% 67,5% Yes 75,0% < >30 66,7% 27,5% 21,4% Fig. 5 Response to the survey question Does the pylorus-preserving procedure (PPPD) offer advantages compared to the classical Kausch Whipple operation? grouped by number of patients treated per year resectable disease, systemic gemcitabine-based chemotherapy is the treatment of choice [2]. Nevertheless, there is preliminary evidence in surgical literature, provided by high-volume specialized centers, which supports the possible benefit of palliative surgical intervention in (highly) selected patients with locally advanced or metastatic PC [19, 21, 22]. Surprisingly, a significant proportion of survey respondents (66%) would already resect intraoperatively detected and technically resectable distant metastases during a radical PC operation. However, this rate may differ significantly based on the professional site of the responding surgeon (Fig. 3). Based on current scientific evidence, one must clearly state that such an experimental approach is not recommended and should be offered to PC patients only within controlled clinical trials [2]. Furthermore, 64% of the responding physicians would proceed with the radical surgical resection of a pancreatic tumor if they detect a single liver metastasis intraoperatively. Palliative surgical interventions like bypass gastroenterostomy or biliodigestive anastomosis are recommended by 50% of survey participants only in a symptomatic patient (e.g., malignant bowel obstruction or bile duct stenosis). The benefit of a pre-emptive medical treatment with somatostatin analogs is also controversial in PC surgery. A meta-analysis of ten studies suggested a reduction in complications and morbidity [11], whereas another recent meta-analysis with eight studies concluded that there is no significant decrease in postoperative complications [12]. The participants of this survey are equally split in this aspect; 51% do and 48% do not apply octreotide or one of its analogs prior to their surgical intervention. The S3 guideline does not give a clear recommendation in this point and states that a specific group of patients who would benefit from this prophylaxis has not yet been identified [2]. No Fig. 4 Criteria of surgical non-resectability in PC grouped by number of patients per year cn1 by imaging criteria Infiltration common hepatic artery Portal vein infiltration 1,8% 12,5% 16,7% 8,9% 22,5% 50,0% 75,0% 65,0% 66,7% Infiltration superior mesenteric artery Celiac trunk infiltration Extrapancreatic tumor manifestations 80,4% 90,0% 100% 83,9% 87,5% 100% 66,1% 72,5% 83,3% < >30
7 Langenbecks Arch Surg (2011) 396: In conclusion, the results from the surgical section of the national CAO/AIO survey clearly illustrate that the surgical management of PC patients at German community and university hospitals is heterogeneous and that as expected both the professional site and the number of patients treated per year may have an influence on local treatment decisions. Future efforts should focus on the implementation of evidence-based and standardized surgical management procedures at German hospitals which treat patients with PC. Acknowledgements The authors would like to thank all members of the CAO, AIO, DGVS, and of the GI group of the Tumorzentrum München for their active support of this survey. This work is part of the doctoral thesis of Mirja Sargent. Conflicts of interest References None. 1. Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics. CA Cancer J Clin 59: Adler G, Seufferlein T, Bischoff SC, Brambs HJ, Feuerbach S, Grabenbauer G, Hahn S, Heinemann V, Hohenberger W, Langrehr JM, Lutz MP, Micke O, Neuhaus H, Neuhaus P, Oettle H, Schlag PM, Schmid R, Schmiegel W, Schlottmann K, Werner J, Wiedenmann B, Kopp I (2007) S3 guidelines exocrine pancreatic cancer Z Gastroenterol 45: Boeck S, Bruns CJ, Sargent M, Schafer C, Seufferlein T, Jauch KW, Heinemann V (2009) Current oncological treatment of patients with pancreatic cancer in germany: results from a national survey on behalf of the Arbeitsgemeinschaft Internistische Onkologie and the Chirurgische Arbeitsgemeinschaft Onkologie of the Germany Cancer Society. Oncology 77: Schneider G, Hamacher R, Eser S, Friess H, Schmid RM, Saur D (2008) Molecular biology of pancreatic cancer new aspects and targets. Anticancer Res 28: Wagner M, Redaelli C, Lietz M, Seiler CA, Friess H, Büchler MW (2004) Curative resection is the single most important factor determining outcome in patients with pancreatic adenocarcinoma. Br J Surg 91: Sewnath ME, Birjmohun RS, Rauws EA, Huibregtse K, Obertop H, Gouma DJ (2001) The effect of preoperative biliary drainage on postoperative complications after pancreaticoduodenectomy. J Am Coll Surg 192: Schwarz RE (2002) Technical considerations to maintain a low frequency of postoperative biliary stent-associated infections. J Hepatobiliary Pancreat Surg 9: Jagannath P, Dhir V, Shrikhande S, Shah RC, Mullerpatan P, Mohandas KM (2005) Effect of preoperative biliary stenting on immediate outcome after pancreaticoduodenectomy. Br J Surg 92: Mezhir JJ, Brennan MF, Baser RE, D'Angelica MI, Fong Y, Dematteo RP, Jarnagin WR, Allen PJ (2009) A matched case control study of preoperative biliary drainage in patients with pancreatic adenocarcinoma: routine drainage is not justified. J Gastrointest Surg 13: van der Gaag NA, Rauws EA, van Eijck CH, Bruno MJ, van der Harst E, Kubben FJ, Gerritsen JJ, Greve JW, Gerhards MF, de Hingh IH, Klinkenbijl JH, Nio CY, de Castro SM, Busch OR, van Gulik TM, Bossuyt PM, Gouma DJ (2010) Preoperative biliary drainage for cancer of the head of the pancreas. N Engl J Med 362: Connor S, Alexakis N, Garden OJ, Leandros E, Bramis J, Wigmore SJ (2005) Meta-analysis of the value of somatostatin and its analogues in reducing complications associated with pancreatic surgery. Br J Surg 92: Zeng Q, Zhang Q, Han S, Yu Z, Zheng M, Zhou M, Bai J, Jin R (2008) Efficacy of somatostatin and its analogues in prevention of postoperative complications after pancreaticoduodenectomy: a meta-analysis of randomized controlled trials. Pancreas 36: Lüttges J, Zamboni G, Klöppel G (1999) Recommendation for the examination of pancreaticoduodenectomy specimens removed from patients with carcinoma of the exocrine pancreas. A proposal for a standardized pathological staging of pancreaticoduodenectomy specimens including a checklist. Dig Surg 16: Verbeke CS, Leitch D, Menon KV, McMahon MJ, Guillou PJ, Anthoney A (2006) Redefining the R1 resection in pancreatic cancer. Br J Surg 93: Diener MK, Knaebel HP, Heukaufer C, Antes G, Büchler MW, Seiler CM (2007) A systematic review and meta-analysis of pylorus-preserving versus classical pancreaticoduodenectomy for surgical treatment of periampullary and pancreatic carcinoma. Ann Surg 245: Siriwardana HP, Siriwardena AK (2006) Systematic review of outcome of synchronous portal-superior mesenteric vein resection during pancreatectomy for cancer. Br J Surg 93: Farnell MB, Aranha GV, Nimura Y, Michelassi F (2008) The role of extended lymphadenectomy for adenocarcinoma of the head of the pancreas: strength of the evidence. J Gastrointest Surg 12: Michalski CW, Kleeff J, Wente MN, Diener MK, Büchler MW, Friess H (2007) Systematic review and meta-analysis of standard and extended lymphadenectomy in pancreaticoduodenectomy for pancreatic cancer. Br J Surg 94: Sasson AR, Hoffman JP, Ross EA, Kagan SA, Pingpank JF, Eisenberg BL (2002) En bloc resection for locally advanced cancer of the pancreas: is it worthwhile? J Gastrointest Surg 6: Hüser N, Michalski CW, Schuster T, Friess H, Kleeff J (2009) Systematic review and meta-analysis of prophylactic gastroenterostomy for unresectable advanced pancreatic cancer. Br J Surg 96: Michalski CW, Erkan M, Hüser N, Müller MW, Hartel M, Friess H, Kleeff J (2008) Resection of primary pancreatic cancer and liver metastasis: a systematic review. Dig Surg 25: Shrikhande SV, Kleeff J, Reiser C, Weitz J, Hinz U, Esposito I, Schmidt J, Friess H, Büchler MW (2007) Pancreatic resection for M1 pancreatic ductal adenocarcinoma. Ann Surg Oncol 14:
Preoperative drainage is always indicated in malignant CBD strictures PRO. Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany
 Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
Preoperative drainage is always indicated in malignant CBD strictures PRO Horst Neuhaus Evangelisches Krankenhaus Düsseldorf, Germany Background Jaundice is associated with high perioperative morbidity
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY. Dr. Shailesh V. Shrikhande
 PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality. Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006
 The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
David R. DeHaas, Jr. MD Sacred Heart Medical Center at RiverBend
 David R. DeHaas, Jr. MD Sacred Heart Medical Center at RiverBend 1. To review the surgical history of the Whipple procedure for periampullary tumors. 2. To review the differential diagnosis for patients
David R. DeHaas, Jr. MD Sacred Heart Medical Center at RiverBend 1. To review the surgical history of the Whipple procedure for periampullary tumors. 2. To review the differential diagnosis for patients
Cancer of the Pancreas
 Cancer of the Pancreas James H. North Jr., M.D., F.A.C.S. It is estimated that in 2007, 37,170 patients will be diagnosed with cancer of the pancreas and 33,370 patients will die of this disease. 1 The
Cancer of the Pancreas James H. North Jr., M.D., F.A.C.S. It is estimated that in 2007, 37,170 patients will be diagnosed with cancer of the pancreas and 33,370 patients will die of this disease. 1 The
To Whipple or Not to Whipple, that is the Question: Evaluating the Resectability of Pancreatic Adenocarcinoma
 August 2009 To Whipple or Not to Whipple, that is the Question: Evaluating the Resectability of Pancreatic Adenocarcinoma Christina Ramirez, Harvard Medical School Year III Gillian Lieberman, MD Agenda
August 2009 To Whipple or Not to Whipple, that is the Question: Evaluating the Resectability of Pancreatic Adenocarcinoma Christina Ramirez, Harvard Medical School Year III Gillian Lieberman, MD Agenda
Ching-Yao Yang, Yu-Wen Tien
 Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Diagnosis and Prognosis of Pancreatic Cancer
 Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Main Page Risk Factors Reducing Your Risk Screening Symptoms Diagnosis Treatment Overview Chemotherapy Radiation Therapy Surgical Procedures Lifestyle Changes Managing Side Effects Talking to Your Doctor
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
J Clin Oncol 24:2897-2902. 2006 by American Society of Clinical Oncology INTRODUCTION
 VOLUME 24 NUMBER 18 JUNE 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Perioperative CA19-9 Levels Can Predict Stage and Survival in Patients With Resectable Pancreatic Adenocarcinoma
VOLUME 24 NUMBER 18 JUNE 20 2006 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Perioperative CA19-9 Levels Can Predict Stage and Survival in Patients With Resectable Pancreatic Adenocarcinoma
Surgical Treatment of Various GI Tract Cancers
 Surgical Treatment of Various GI Tract Cancers By James Ouellette, DO, FACS, Surgical Oncology, Hepatobiliary Surgery Surgical treatment for most gastrointestinal (GI) cancers requires multidisciplinary
Surgical Treatment of Various GI Tract Cancers By James Ouellette, DO, FACS, Surgical Oncology, Hepatobiliary Surgery Surgical treatment for most gastrointestinal (GI) cancers requires multidisciplinary
restricted to certain centers and certain patients, preferably in some sort of experimental trial format.
 Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Pancreatic Cancer. The Killer that must be discovered early. Dr Alfred Kow Wei Chieh
 Pancreatic Cancer The Killer that must be discovered early 27 th June 2015 Dr Alfred Kow Wei Chieh Consultant Department of Surgery Division of HPB Surgery & Liver Transplantation & Assistant Dean (Education)
Pancreatic Cancer The Killer that must be discovered early 27 th June 2015 Dr Alfred Kow Wei Chieh Consultant Department of Surgery Division of HPB Surgery & Liver Transplantation & Assistant Dean (Education)
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives
 Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Evidence tabel Lokaal palliatieve behandelingen
 Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Pancreatic Cancer Basics. Meghan McGurk, PA-C, MMSc Physician Assistant Department of Medical Oncology Yale Cancer Center
 Pancreatic Cancer Basics Meghan McGurk, PA-C, MMSc Physician Assistant Department of Medical Oncology Yale Cancer Center Case Study Mr.T is a 36 yo male who presented in the fall of 2003, at the age of
Pancreatic Cancer Basics Meghan McGurk, PA-C, MMSc Physician Assistant Department of Medical Oncology Yale Cancer Center Case Study Mr.T is a 36 yo male who presented in the fall of 2003, at the age of
Understanding. Pancreatic Cancer
 Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
The Royal Marsden. Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum
 The Royal Marsden Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum Any surgeon can cure Surgeon - dependent No surgeon can cure EMR D2 GASTRECTOMY H N SN. WEDGE
The Royal Marsden Surgery for Gastric and GE Junction Cancer: primary palliative where and when? William Allum Any surgeon can cure Surgeon - dependent No surgeon can cure EMR D2 GASTRECTOMY H N SN. WEDGE
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
How to treat early gastric cancer. Surgery
 How to treat early gastric cancer Surgery Mark I. van Berge Henegouwen Department of Surgery, AMC, Amsterdam Director upper GI surgical unit Academic Medical Center Upper GI surgery at AMC 100 oesophagectomies
How to treat early gastric cancer Surgery Mark I. van Berge Henegouwen Department of Surgery, AMC, Amsterdam Director upper GI surgical unit Academic Medical Center Upper GI surgery at AMC 100 oesophagectomies
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
CEU Update. Pancreatic Cancer
 CEU Update A semi-annual publication of the National Association for Health Professionals June 2015 Issue #0615 Pancreatic Cancer The Pancreatic Cancer Action Network, Inc. (PanCAN), established in 1999,
CEU Update A semi-annual publication of the National Association for Health Professionals June 2015 Issue #0615 Pancreatic Cancer The Pancreatic Cancer Action Network, Inc. (PanCAN), established in 1999,
CLINICAL MANAGEMENT OF INTRADUCTAL PAPILLARY MUCINOUS NEOPLASMS OF THE PANCREAS
 1 CLINICAL MANAGEMENT OF INTRADUCTAL PAPILLARY MUCINOUS NEOPLASMS OF THE PANCREAS Carlos Fernández-del Castillo, M.D. Associate Professor of Surgery Massachusetts General Hospital Harvard Medical School,
1 CLINICAL MANAGEMENT OF INTRADUCTAL PAPILLARY MUCINOUS NEOPLASMS OF THE PANCREAS Carlos Fernández-del Castillo, M.D. Associate Professor of Surgery Massachusetts General Hospital Harvard Medical School,
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES.
 PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
NP/PA Clinical Hepatology Fellowship Summary of Year-Long Curriculum
 OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
Vascular resection during pancreaticoduodenectomy. Ryan Turley, MD Research Fellow, Duke University
 Vascular resection during pancreaticoduodenectomy. Ryan Turley, MD Research Fellow, Duke University Vascular Resection during PD Outline Review of pancreatic adenocarcinoma Role of PD in treatment of pancreatic
Vascular resection during pancreaticoduodenectomy. Ryan Turley, MD Research Fellow, Duke University Vascular Resection during PD Outline Review of pancreatic adenocarcinoma Role of PD in treatment of pancreatic
A Patient s Guide to. Pancreatic Cysts. University of Michigan Comprehensive Cancer Center
 A Patient s Guide to Pancreatic Cysts University of Michigan Comprehensive Cancer Center Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for
A Patient s Guide to Pancreatic Cysts University of Michigan Comprehensive Cancer Center Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
A Brief Guide to Pancreatic Cancer
 A Brief Guide to Pancreatic Cancer Contributing authors; Dr. Michele Molinari MD Dr. Mark Walsh MD Dr. Ian Beauprie MD Dr. Daniel Rayson MD Elizabeth Reid P.Dt Sarah De Coutere, RN Craig s Cause Pancreatic
A Brief Guide to Pancreatic Cancer Contributing authors; Dr. Michele Molinari MD Dr. Mark Walsh MD Dr. Ian Beauprie MD Dr. Daniel Rayson MD Elizabeth Reid P.Dt Sarah De Coutere, RN Craig s Cause Pancreatic
HEALING AND SUPPORT FOR PEOPLE WITH PANCREATIC, LIVER, COLORECTAL, AND BILE DUCT CANCERS
 HEALING AND SUPPORT FOR PEOPLE WITH PANCREATIC, LIVER, COLORECTAL, AND BILE DUCT CANCERS ONLY THE FOREMOST EXPERTS Our multidisciplinary team includes specialists in gastroenterology, hepatology, oncology,
HEALING AND SUPPORT FOR PEOPLE WITH PANCREATIC, LIVER, COLORECTAL, AND BILE DUCT CANCERS ONLY THE FOREMOST EXPERTS Our multidisciplinary team includes specialists in gastroenterology, hepatology, oncology,
Hepatocellular Carcinoma (HCC)
 Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
Abhishek Vadalia Introduction Chemoembolization is being used with increasing frequency in the treatment of solid hepatic tumors such as Hepatocellular Carinoma (HCC) & rare Cholangiocellular Carcinoma
Pancreatic Carcinoma Recurrence in the Remnant Pancreas after a Pancreaticoduodenectomy
 CASE REPORT Pancreatic Carcinoma Recurrence in the Remnant Pancreas after a Pancreaticoduodenectomy Raffaele Dalla Valle 1, Cristina Mancini 2, Pellegrino Crafa 2, Rodolfo Passalacqua 3 1 Department of
CASE REPORT Pancreatic Carcinoma Recurrence in the Remnant Pancreas after a Pancreaticoduodenectomy Raffaele Dalla Valle 1, Cristina Mancini 2, Pellegrino Crafa 2, Rodolfo Passalacqua 3 1 Department of
Preliminary Program 9th EDS Postgraduate Course Riga, Latvia May 14-16, 2015
 Preliminary Program 9th May 14-16, 2015 Venue: Riga city Bellevue Park Hotel Riga, Slokas iela 1, Rīga, Latvia Thursday, May 14, 2015 Time 14:00-14:20 Workshop: Evidence Based Medicine (limited to 35 participants)
Preliminary Program 9th May 14-16, 2015 Venue: Riga city Bellevue Park Hotel Riga, Slokas iela 1, Rīga, Latvia Thursday, May 14, 2015 Time 14:00-14:20 Workshop: Evidence Based Medicine (limited to 35 participants)
A Patient s Guide to. Pancreatic Cancer
 A Patient s Guide to Pancreatic Cancer Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for this handbook GI Oncology Program, Patient Education
A Patient s Guide to Pancreatic Cancer Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for this handbook GI Oncology Program, Patient Education
What you need to know. JAMES L. ABBRUZZESE, MD Chairman, Gastrointestinal Medical Oncology The University of Texas M. D. Anderson Cancer Center
 Myths & Facts about pancreatic cancer What you need to know JAMES L. ABBRUZZESE, MD Chairman, Gastrointestinal Medical Oncology The University of Texas M. D. Anderson Cancer Center BEN EBRAHIMI, MD Fellow,
Myths & Facts about pancreatic cancer What you need to know JAMES L. ABBRUZZESE, MD Chairman, Gastrointestinal Medical Oncology The University of Texas M. D. Anderson Cancer Center BEN EBRAHIMI, MD Fellow,
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases
 I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL HEPATOCELLULAR CARCINOMA GI Site Group Hepatocellular Carcinoma Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL HEPATOCELLULAR CARCINOMA GI Site Group Hepatocellular Carcinoma Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION
Surgery for Advanced and Metastatic Pancreatic Cancer Current State and Perspectives
 Review Surgery for Advanced and Metastatic Pancreatic Cancer Current State and Perspectives OLIVER MANN, TIM STRATE, CLAUS SCHNEIDER, EMRE F. YEKEBAS and JAKOB R. IZBICKI Department of General, Visceral
Review Surgery for Advanced and Metastatic Pancreatic Cancer Current State and Perspectives OLIVER MANN, TIM STRATE, CLAUS SCHNEIDER, EMRE F. YEKEBAS and JAKOB R. IZBICKI Department of General, Visceral
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
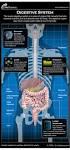 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
Abdominal Surgery Rotation Section 7- Whipple resection. 1. Surgical considerations
 Abdominal Surgery Rotation Section 7- Whipple resection 1. Surgical considerations The Whipple resection consists of a pancreaticoduodenectomy followed by anastamosis of the pancreas, liver and stomach
Abdominal Surgery Rotation Section 7- Whipple resection 1. Surgical considerations The Whipple resection consists of a pancreaticoduodenectomy followed by anastamosis of the pancreas, liver and stomach
Cancer: Pancreatic (Adult)
 A02/S/b 2013/14 NHS STANDARD CONTRACT FOR CANCER: PANCREATIC (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review A02/S/b
A02/S/b 2013/14 NHS STANDARD CONTRACT FOR CANCER: PANCREATIC (ADULT) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review A02/S/b
Cancer of the Cardia/GE Junction: Surgical Options
 Cancer of the Cardia/GE Junction: Surgical Options Michael A Smith, MD Associate Chief Thoracic Surgery Center for Thoracic Disease St Joseph s Hospital and Medical Center Phoenix, AZ Michael Smith, MD
Cancer of the Cardia/GE Junction: Surgical Options Michael A Smith, MD Associate Chief Thoracic Surgery Center for Thoracic Disease St Joseph s Hospital and Medical Center Phoenix, AZ Michael Smith, MD
Hepatocellular Carcinoma Treatment Decision Tree
 Treatment Decision Tree Derek DuBay, MD Assistant Professor of Surgery Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery 1 UAB Liver Tumor Clinic Referrals: 205 996 5970 (phone) 205
Treatment Decision Tree Derek DuBay, MD Assistant Professor of Surgery Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery 1 UAB Liver Tumor Clinic Referrals: 205 996 5970 (phone) 205
Clinical Practice Assessment Robotic surgery
 Clinical Practice Assessment Robotic surgery Background: Surgery is by nature invasive. Efforts have been made over time to reduce complications and the trauma inherently associated with surgery through
Clinical Practice Assessment Robotic surgery Background: Surgery is by nature invasive. Efforts have been made over time to reduce complications and the trauma inherently associated with surgery through
Phase 1 Trial of Preoperative, Short-Course Carbon-Ion Radiotherapy for Patients With Resectable Pancreatic Cancer
 Phase 1 Trial of Preoperative, Short-Course Carbon-Ion Radiotherapy for Patients With Resectable Pancreatic Cancer Makoto Shinoto, MD 1,2 ; Shigeru Yamada, MD, PhD 1 ; Shigeo Yasuda, MD, PhD 1 ; Hiroshi
Phase 1 Trial of Preoperative, Short-Course Carbon-Ion Radiotherapy for Patients With Resectable Pancreatic Cancer Makoto Shinoto, MD 1,2 ; Shigeru Yamada, MD, PhD 1 ; Shigeo Yasuda, MD, PhD 1 ; Hiroshi
Carbohydrate antigen 19 9 (CA 19 9) (serum, plasma)
 Carbohydrate antigen 19 9 (CA 19 9) (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Carbohydrate antigen 19 9 (CA 19 9) 1.2 Alternative names Cancer antigen 19 9, cancer antigen GI
Carbohydrate antigen 19 9 (CA 19 9) (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Carbohydrate antigen 19 9 (CA 19 9) 1.2 Alternative names Cancer antigen 19 9, cancer antigen GI
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Gastrointestinal Cancer
 Surgical Treatment of Pancreatic Cancer Magnus Bergenfeldt 1 and Åke Andrén-Sandberg 2 1. Associate Professor of Surgery, Department of Surgical Gastroenterology, Herlev Hospital; 2. Professor of Surgery,
Surgical Treatment of Pancreatic Cancer Magnus Bergenfeldt 1 and Åke Andrén-Sandberg 2 1. Associate Professor of Surgery, Department of Surgical Gastroenterology, Herlev Hospital; 2. Professor of Surgery,
Peritoneal Surface Malignancies. Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA
 Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50
 General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
General Data Seton Medical Center Hepatocellular Carcinoma Patterns of Care Study Rate of Treatment with Chemoembolization 2007 2012 N = 50 The vast majority of the patients in this study were diagnosed
Oxford University Hospitals
 Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Journal Name: International Journal of Hepatobiliary and Pancreatic Diseases (IJHPD)
 ACCEPTED MAN U SCRIPT EARLY VIEW ARTICLE Early View Article: Online published version of an accepted article before inclusion in an issue of International Journal of Hepatobiliary and Pancreatic Diseases
ACCEPTED MAN U SCRIPT EARLY VIEW ARTICLE Early View Article: Online published version of an accepted article before inclusion in an issue of International Journal of Hepatobiliary and Pancreatic Diseases
Extended Radical Whipple Resection for Cancer of the Pancreatic Head: Operative Procedure and Results
 How I Do It Dig Surg 1998;15:299 307 Received: February 17, 1997 Accepted: March 20, 1997 T. Imaizumi F. Hanyu N. Harada T. Hatori A. Fukuda Department of Gastroenterological Surgery, Tokyo Women s Medical
How I Do It Dig Surg 1998;15:299 307 Received: February 17, 1997 Accepted: March 20, 1997 T. Imaizumi F. Hanyu N. Harada T. Hatori A. Fukuda Department of Gastroenterological Surgery, Tokyo Women s Medical
Version 1.2012. Also available at NCCN.com. Pancreatic Cancer. NCCN Guidelines for Patients. Dedicated to the memory of Randy Pausch
 Pancreatic Cancer NCCN Guidelines for Patients Dedicated to the memory of Randy Pausch Also available at NCCN.com About this booklet Its purpose Learning that you have cancer can be overwhelming. The goal
Pancreatic Cancer NCCN Guidelines for Patients Dedicated to the memory of Randy Pausch Also available at NCCN.com About this booklet Its purpose Learning that you have cancer can be overwhelming. The goal
Locally advanced and bordeline forms of pancreatic cancer
 19 May 2011 Locally advanced and bordeline forms of pancreatic cancer P r Pascal Hammel Pôle des Maladies de l Appareil Digestif Hôpital Beaujon, 92110 Clichy Université Paris VII, Denis Diderot pascal.hammel@bjn.aphp.fr
19 May 2011 Locally advanced and bordeline forms of pancreatic cancer P r Pascal Hammel Pôle des Maladies de l Appareil Digestif Hôpital Beaujon, 92110 Clichy Université Paris VII, Denis Diderot pascal.hammel@bjn.aphp.fr
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
WallFlex Biliary RX Stent. Fully, Partially and Uncovered Self-Expanding Metal Stents
 WallFlex Biliary RX Stent Fully, Partially and Uncovered Self-Expanding Metal Stents WallFlex Biliary RX Stent Fully, Partially and Uncovered Self-Expanding Metal Stents The WallFlex Biliary RX Stent is
WallFlex Biliary RX Stent Fully, Partially and Uncovered Self-Expanding Metal Stents WallFlex Biliary RX Stent Fully, Partially and Uncovered Self-Expanding Metal Stents The WallFlex Biliary RX Stent is
Treatment Advances for Liver Cancer
 Treatment Advances for Liver Cancer Guest Expert: Wasif, MD Associate Professor of Medical Oncology Mario Strazzabosco, MD Professor of Internal Medicine, Digestive Diseases www.wnpr.org www.yalecancercenter.org
Treatment Advances for Liver Cancer Guest Expert: Wasif, MD Associate Professor of Medical Oncology Mario Strazzabosco, MD Professor of Internal Medicine, Digestive Diseases www.wnpr.org www.yalecancercenter.org
Cytoreduction and hyperthermic intraperitoneal chemotherapy for the treatment of pseudomyxoma
 Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
Gallbladder Cancer. What is gallbladder cancer? About the gallbladder
 Gallbladder Cancer What is gallbladder cancer? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other areas of
Gallbladder Cancer What is gallbladder cancer? Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other areas of
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Cancer of the Exocrine Pancreas, Ampulla of Vater and Distal Common Bile Duct Proforma
 Cancer of the Exocrine, Ampulla of Vater and Distal Coon Bile Duct Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Sex Male Female Intersex/indeterminate
Cancer of the Exocrine, Ampulla of Vater and Distal Coon Bile Duct Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Sex Male Female Intersex/indeterminate
Borderline Resectable Pancreatic Cancer: The Importance of This Emerging Stage of Disease
 Borderline Resectable Pancreatic Cancer: The Importance of This Emerging Stage of Disease Matthew HG Katz, MD, Peter WT Pisters, MD, FACS, Douglas B Evans, MD, FACS, Charlotte C Sun, DrPH, MPH, Jeffrey
Borderline Resectable Pancreatic Cancer: The Importance of This Emerging Stage of Disease Matthew HG Katz, MD, Peter WT Pisters, MD, FACS, Douglas B Evans, MD, FACS, Charlotte C Sun, DrPH, MPH, Jeffrey
UCLA Asian Liver Program
 CLA Program Update Program Faculty Myron J. Tong, PhD, MD Professor of Medicine Hepatology Director, Asian Liver Program Surgery Ronald W. Busuttil, MD, PhD Executive Chair Department of Surgery Director,
CLA Program Update Program Faculty Myron J. Tong, PhD, MD Professor of Medicine Hepatology Director, Asian Liver Program Surgery Ronald W. Busuttil, MD, PhD Executive Chair Department of Surgery Director,
Surgery and other procedures to control symptoms
 Surgery and other procedures to control symptoms This fact sheet is for people diagnosed with inoperable pancreatic cancer who will be having surgery or another interventional procedure to relieve symptoms
Surgery and other procedures to control symptoms This fact sheet is for people diagnosed with inoperable pancreatic cancer who will be having surgery or another interventional procedure to relieve symptoms
Pancreatic resectional surgery: An evidencebased
 Review Article Free full text available from www.cancerjournal.net Pancreatic resectional surgery: An evidencebased perspective Melroy A D souza, Shailesh V Shrikhande Department of Gastrointestinal and
Review Article Free full text available from www.cancerjournal.net Pancreatic resectional surgery: An evidencebased perspective Melroy A D souza, Shailesh V Shrikhande Department of Gastrointestinal and
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
Treatment Guide Pancreatic Disease CHOOSING YOUR CARE
 Treatment Guide Pancreatic Disease The pancreas is one of the body s great multi-taskers this dual-purpose organ is also a gland. Some people may not give much thought to the pancreas, especially those
Treatment Guide Pancreatic Disease The pancreas is one of the body s great multi-taskers this dual-purpose organ is also a gland. Some people may not give much thought to the pancreas, especially those
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
What is pancreatic cancer?
 Pancreatic Cancer What is pancreatic cancer? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines PANCREATIC CANCER:
Pancreatic Cancer What is pancreatic cancer? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines PANCREATIC CANCER:
Bile Leaks After Laparoscopic Cholecystectomy. Kings County Hospital Center Eliana A. Soto, MD
 Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Long-Term Survival After Multidisciplinary Management of Resected Pancreatic Adenocarcinoma
 Ann Surg Oncol DOI 10.1245/s10434-008-0295-2 ORIGINAL ARTICLE HEPATOBILIARY AND PANCREATIC TUMORS Long-Term Survival After Multidisciplinary Management of Resected Pancreatic Adenocarcinoma Matthew H.
Ann Surg Oncol DOI 10.1245/s10434-008-0295-2 ORIGINAL ARTICLE HEPATOBILIARY AND PANCREATIC TUMORS Long-Term Survival After Multidisciplinary Management of Resected Pancreatic Adenocarcinoma Matthew H.
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
GENERAL CODING. When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis.
 GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma. Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma
 New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma Riccardo Lencioni Author s Affiliation: Division of Diagnostic
New Data Supporting Modified RECIST (mrecist) for Hepatocellular Carcinoma Running Title: Modified RECIST (mrecist) for Hepatocellular Carcinoma Riccardo Lencioni Author s Affiliation: Division of Diagnostic
and Helicobacter pylori
 Family Practice Oncology Network Upper Gastrointestinal Cancer (Suspected) Part 2 External Review Effective Date: TBD SCOPE: Part 2 of this guideline outlines recommendations for the prevention, screening,
Family Practice Oncology Network Upper Gastrointestinal Cancer (Suspected) Part 2 External Review Effective Date: TBD SCOPE: Part 2 of this guideline outlines recommendations for the prevention, screening,
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Treatment of Hepatic Neoplasm
 I. Policy University Health Alliance (UHA) will reimburse for treatment of hepatic neoplasm outside of systemic chemotherapy alone when determined to be medically necessary and within the medical criteria
I. Policy University Health Alliance (UHA) will reimburse for treatment of hepatic neoplasm outside of systemic chemotherapy alone when determined to be medically necessary and within the medical criteria
Gallstone Ileus. Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005
 Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Survival Predictors of Patients With Primary Duodenal Adenocarcinoma
 Int Surg 2011;96:111 116 Survival Predictors of Patients With Primary Duodenal Adenocarcinoma Hiroshi Kawahira 1,2, Fumihiko Miura 3, Kenichi Saigo 4, Akinao Matsunaga 1, Toshiyuki Natsume 1, Takashi Akai
Int Surg 2011;96:111 116 Survival Predictors of Patients With Primary Duodenal Adenocarcinoma Hiroshi Kawahira 1,2, Fumihiko Miura 3, Kenichi Saigo 4, Akinao Matsunaga 1, Toshiyuki Natsume 1, Takashi Akai
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases
 Sarcoma (2002) 6, 69 73 ORIGINAL ARTICLE The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases JOHN M. KANE III, J. WILLIAM FINLEY, DEBORAH DRISCOLL, WILLIAM G. KRAYBILL
Sarcoma (2002) 6, 69 73 ORIGINAL ARTICLE The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases JOHN M. KANE III, J. WILLIAM FINLEY, DEBORAH DRISCOLL, WILLIAM G. KRAYBILL
Pancreaticoduodenectomy (PD) is being performed in
 AGING & SURGERY Pancreaticoduodenectomy in Elderly Adults: Is It Justified in Terms of Mortality, Long-Term Morbidity, and Quality of Life? Fabian Gerstenhaber, MD,* Julie Grossman, MD,* Nir Lubezky, MD,*
AGING & SURGERY Pancreaticoduodenectomy in Elderly Adults: Is It Justified in Terms of Mortality, Long-Term Morbidity, and Quality of Life? Fabian Gerstenhaber, MD,* Julie Grossman, MD,* Nir Lubezky, MD,*
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Pancreatic Cancer and Pre Cancer: A Diagnosis and Treatment Update Webcast October 6, 2010 Joo Ha Hwang, M.D. Dorothy Snyder
 Pancreatic Cancer and Pre Cancer: A Diagnosis and Treatment Update Webcast October 6, 2010 Joo Ha Hwang, M.D. Dorothy Snyder Please remember the opinions expressed on Patient Power are not necessarily
Pancreatic Cancer and Pre Cancer: A Diagnosis and Treatment Update Webcast October 6, 2010 Joo Ha Hwang, M.D. Dorothy Snyder Please remember the opinions expressed on Patient Power are not necessarily
Surgical Staging of Endometrial Cancer
 Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
The TV Series. www.healthybodyhealthymind.com INFORMATION TELEVISION NETWORK
 The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
The TV Series www.healthybodyhealthymind.com Produced By: INFORMATION TELEVISION NETWORK ONE PARK PLACE 621 NW 53RD ST BOCA RATON, FL 33428 1-800-INFO-ITV www.itvisus.com 2005 Information Television Network.
Current Status and Perspectives of Radiation Therapy for Breast Cancer
 Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Pancreatic cancer An overview of diagnosis and treatment
 Pancreatic cancer An overview of diagnosis and treatment Introduction This booklet is for anyone who has recently been diagnosed with pancreatic cancer. Partners, family members and friends may also find
Pancreatic cancer An overview of diagnosis and treatment Introduction This booklet is for anyone who has recently been diagnosed with pancreatic cancer. Partners, family members and friends may also find
9 TUMORS OF THE PANCREAS, BILIARY TRACT, AND LIVER
 9 Tumors of the Pancreas, Biliary Tract, and Liver 1 9 TUMORS OF THE PANCREAS, BILIARY TRACT, AND LIVER Steven M. Strasberg, M.D., F.A.C.S., and David C. Linehan, M.D., F.A.C.S. Numerous types of tumors
9 Tumors of the Pancreas, Biliary Tract, and Liver 1 9 TUMORS OF THE PANCREAS, BILIARY TRACT, AND LIVER Steven M. Strasberg, M.D., F.A.C.S., and David C. Linehan, M.D., F.A.C.S. Numerous types of tumors
