EMERGENCY & TRAUMA CARE TRAINING COURSE
|
|
|
- Scarlett Summers
- 10 years ago
- Views:
Transcription
1 EMERGENCY & TRAUMA CARE TRAINING COURSE Basic Trauma, Anesthesia and Surgical Skills for Frontline Health Providers Including management of injuries in women, children, elderly and humanitarian emergencies Emergency & Essential Surgical Care Clinical Procedures Unit Department of Health Systems Policies & Workforce World Health Organization Geneva, Switzerland 1
2 Objectives: INTRODUCTION This course is about managing trauma, from minor injury to humanitarian emergencies, including injuries in women, children and the elderly, with the principal goal of improving quality of care and patient safety. Introduction of instructors and participants Presentation of WHO Integrated Management for Emergency and Essential Surgical Care (IMEESC) toolkit [] 2
3 This is a compilation of all WHO documents relevant to Emergency and Trauma Care Training Course Resources Integrated Management for Emergency and Essential Surgical Care (IMEESC) toolkit Surgical Care at the District Hospital Pratique Chirurgicale de Base 3
4 Additional links to WHO Resources: 1. Guidelines for Essential Trauma Care 2. Hospital Care for Children 3. Integrated Management of Adult Illnesses, District Clinician Manual: Hospital Care for Adolescents and Adults a) Quick Check and emergency treatments for adolescents and adults 4. Emergency Triage Assessment and Treatment 5. Guidelines on Emergency Health Care 6. Integrated Management of Childhood Illnesses 7. Integrated Management of Pregnancy and Childbirth a) Managing Complication in Pregnancy and Childbirth: a guide for midwives and doctors b) Pregnancy, Childbirth, Postpartum and Newborn Care: a guide for essential practice 8. Oxygen Therapy for Acute Respiratory Infections in Young Children in Developing Countries 9. Mass Casualty Management Systems Prevention and Management of Wound infections ion.pdf 11. Safe Surgery Patient Safety Pulse Oximetry Project Tetanus Vaccination Clinical Management of Rape Survivors tml 15. Guidelines for Medico-legal Care for Victims of Sexual Violence index.html 4
5 MODULE 1 Principles and Techniques of Trauma Care 5
6 OBJECTIVES OF MODULE 1 Learn basic techniques of triage and emergency care within the first, most critical hour, of a patient s arrival at the hospital Basic emergency resuscitation skills in adults and children open and maintain airway perform life-saving procedures manage active bleeding place intravenous lines learn shock management 6
7 SIX PHASES OF TRAUMA CARE MANAGEMENT Phase I Phase II Triage Primary Survey Resuscitation Phase III Secondary Survey Phase IV Stabilization Phase V Transfer Phase VI Definitive Care Patient care timeline 7
8 MANAGEMENT GOALS Primary survey Examine, diagnose, treat life-threatening injuries as soon as they are diagnosed Use simplest treatment possible to stabilize patient s condition Secondary survey Perform complete, thorough patient examination to ensure no other injuries are missed 8
9 TRAUMA CARE MANAGEMENT Phase I Phase II Triage Primary Survey Resuscitation Phase III Secondary Survey Start resuscitation at the same time as performing primary survey Do not start secondary survey until completing primary survey Constantly reassess patient for response to treatment; if condition deteriorates, reassess ABC 9
10 TRAUMA CARE MANAGEMENT Phase IV Phase V Stabilization Transfer Phase VI Definitive Care Do not start definitive treatment until secondary survey is completed unless required as life-saving measure When definitive treatment is not available, have a plan for safe transfer of patient to another centre 10
11 MAJOR TRAUMA Trauma mechanism: A fall >3 meters Road traffic accident: net speed >30 km/h Thrown from or trapped in a vehicle Pedestrian or cyclist hit by a car Unrestrained occupant of a vehicle Injury from high or low velocity weapon 11
12 MAJOR TRAUMA Physical findings: Airway or respiratory distress Blood pressure <100 mmhg Glasgow Coma Scale <13/15 Penetrating injury More than 1 area injured Make a full primary and secondary survey of any patient who is injured, especially if major trauma 12
13 PHASE I: TRIAGE Triage: sorting and treating patients according to priority; identify, treat patients with life-threatening conditions first Priority may be determined by: Medical necessity Personnel skills Available equipment Vital signs Pulse rate Blood pressure Respiratory rate SpO2% Temperature AVPU (Alert, verbal, pain or unresponsive) Urine output 13
14 PHASE II: THE PRIMARY SURVEY Airway Breathing Circulation Disability or neurologic Damage Expose the patient Purpose is to identify and treat life threatening injuries: Airway obstruction Breathing difficulties Severe external or internal haemorrhage 14
15 AIRWAY Always assess the airway Talk to the patient A patient speaking freely and clearly has an open airway Look and listen for signs of obstruction Snoring or gurgling Stridor or noisy breathing Foreign body or vomit in mouth If airway obstructed, open airway and clear obstruction 15
16 TECHNIQUES FOR OPENING THE AIRWAY No trauma Position patient on firm surface Tilt the head Lift the chin to open the airway Remove foreign body if visible Clear secretions Give oxygen 5 L/min obstructed airway chin lift jaw thrust 16
17 TECHNIQUES FOR OPENING THE AIRWAY Modified jaw thrust In case of trauma Stabilize cervical spine Do not lift head! Open airway using jaw thrust Remove foreign body if visible Clear secretions Give oxygen 5 L/min 17
18 AIRWAY DEVICES Oropharyngeal airway Use if patient unconscious Use correct size - measure from front of ear to corner of mouth Slide airway over tongue If patient resists, gags or vomits, remove immediately! Nasopharyngeal airway Better tolerated if patient is semi-conscious Pass well lubricated into one nostril Direct posteriorly, towards the throat 18
19 AIRWAY Before attempting intubation the answer to these questions should be YES: Is there an indication? - Failure to maintain or protect the airway (risk of aspiration) or - Failure to oxygenate or ventilate or - Impending airway failure (inhalation injury, angioedema) Do you have working equipment? - Functioning laryngoscope with working light - Appropriate endotracheal tube size - Bag-valve mask - Working oxygen source - Suction Do you have a post-intubation plan? - Is a mechanical ventilator available? (unless only short-term need) - Are sedative drugs available? 19
20 BREATHING Assess ventilation - Is the patient in respiratory distress? Look - For cyanosis, wounds, deformities, ecchymosis, amplitude, paradoxical movement Feel - Painful areas, abnormal movement Percuss - Dullness Listen - Reduced breath sounds 20
21 INDICATIONS FOR CHEST DECOMPRESSION Signs and Symptoms Absent or diminished breath sounds on one side Evidence of chest trauma or rib fracture Open or "sucking" chest wound Diagnoses Pneumothorax Tension pneumothorax Hemothorax Hemo-pnemothorax 21
22 OPEN CHEST WOUND "Sucking" sound Requires very prompt treatment Apply an occlusive "plastic pack" dressing to wound, tape down on three sides, leaving one side open for air to escape Place a chest drain Never insert chest tube through wound Give high flow oxygen Give antibiotics Debride wound and consider closure 22
23 TENSION PNEUMOTHORAX Air from lung puncture enters pleural space, cannot escape Progressive increase in intrathoracic pressure causes mediastinal shift and hypotension due to reduced venous return Patient becomes short of breath and hypoxic Diminished breath sounds on side of pneumothorax Requires urgent needle decompression, then chest drain as soon as possible compression of increasing superior intrapleural vena cava pressure compression of inferior Vena Cava mediastinal shift 23
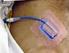
24 TENSION PNEUMOTHORAX 2 nd intercostal space at mid-clavicular line Give high flow oxygen After aseptic skin preparation Insert a large bore needle over rib: 2 nd intercostal space Over 3 rd rib at mid-clavicular line Listen for hissing sound of air escaping Insert chest drain 24
25 INSERTION OF CHEST DRAIN NAV A B C D Mark incision just above rib in mid-axillary line; use nipple as a landmark so incision not too low (A) Prepare area with antiseptic; inject local anaesthetic in area of incision down to pleura Make small transverse incision just above rib to avoid vascular injury; (A, B) Using a pair of large curved artery forceps, go over top of rib, penetrate pleura bluntly, enlarge opening (C, D) 25
26 Insertion of Chest Drain and Underwater Seal Drainage E F Use same forceps, grasp tube at tip, introduce into chest (E), advancing tube well past holes at end of tube Close incision with interrupted skin sutures; use one stitch to anchor tube in place (F) Leave additional stitch untied adjacent to tube for closing wound after tube removal (G) Apply gauze dressing Connect tube to underwater-seal drainage system, mark initial level of fluid in drainage bottle (G) G 26
27 CIRCULATION: HAEMORRAGHIC SHOCK Assess the circulation Signs of hypoperfusion Confusion, lethargy or agitation Pallor or cold extremities Weak or absent radial and femoral pulses Tachycardia Hypotension Examine the abdomen for tenderness or guarding Carefully assess pelvic stability 27
28 CIRCULATION: HAEMORRAGHIC SHOCK Large volumes of blood may be hidden in thoracic, abdominal and pelvic cavities, or from femoral shaft fractures. To decrease bleeding: Apply pressure to external wounds Apply splint to possible femur fracture Apply pelvic binder to possible pelvic fracture If patients is pregnant, she should not be on her back, put her on her left side. Send blood for type and crossmatch 28
29 CIRCULATION Obtain two large bore IV catheters If systolic BP <90 mmhg or pulse >110 bpm Give 500 ml bolus of Ringer s Lactate or NS Keep patient warm Reassess vitals If still hypotensive after 2L of crystalloids, transfuse blood 29
30 STOP THE BLEEDING Apply direct pressure to the wound, then put on compression dressing. Apply only enough pressure to stop the bleeding. Direct pressure ONLY if bleeding is life-threatening and cannot be controlled, apply a tourniquet. Use a blood pressure cuff or wide elastic band over padded skin. Transfer urgently! 30
31 DISABILITY or DAMAGE Checking for neurological damage: vital part of primary survey Abbreviated neurological examination: ALERT VERBAL - responsive to verbal stimulus PAIN - responsive to painful stimulus UNRESPONSIVE 31
32 GLASGOW COMA SCORE (GCS) Eyes Score Verbal Score Motor Score Open spontaneously 4 Oriented 5 Obeys commands 6 Open to command 3 Confused talk 4 Localizes to pain 5 Open to pain 2 Inappropriate words 3 Withdraws to pain 4 None 1 Incomprehensible sounds 2 Flexor (decorticate) 3 None 1 Extensor (decerebrate) 2 None 1 Total Score = Eye + Verbal + Motor Scores 32
33 GLASGOW COMA SCORE Eyes +Verbal + Motor Scores = GCS Severe head injury: GCS 8 or less Moderate head injury: GCS 9-12 Mild head injury: GCS GCS is to be repeated and recorded frequently. It is the best way to determine deterioration 33
34 HEAD INJURY Deterioration Unequal or dilated pupils may indicate increased intracranial pressure Avoid sedation or analgesics as it interferes with neurologic examinations, reduces breathing (increased CO 2 causes increased intracranial pressure) Bradycardia, hypertension may indicate worsening condition 34
35 EXPOSURE Remove all patient's clothing Examine whole patient Front and back; log roll carefully Do not allow patient to get cold (especially children) 35
36 IMAGING X-Rays - Chest - Pelvis - Cervical spine Ultrasound - FAST scan 36
37 PHASE III: SECONDARY SURVEY Head Exam Scalp, eyes, ears Soft tissues Neck Exam Penetrating injuries Swelling or crepitus Neurological Exam Glasgow Coma Score Motor examination Sensory examination Reflexes Chest Exam Clavicles, ribs Breath, heart sounds Abdominal Exam Penetrating injury Blunt injury: nasogastric tube Rectal exam Urinary catheter Pelvis and Limbs Fractures Pulses Lacerations, ecchymosis 37
38 URINARY CATHETER PLACEMENT 1. Wash area with soap and water, retract prepuce 2. Put on sterile gloves, apply bland antiseptic 3. Check integrity of catheter balloon 4. Lubricate catheter generously 5. Hold penis vertically, slightly stretched 6. Introduce catheter gently-don't force 7. Urine in catheter confirms placement 8. Inflate balloon slowly 9. Replace prepuce 38
39 REASSESSMENT Always perform an ABCDE primary survey if patient deteriorates Signs of adequate resuscitation Slowing of tachycardia Urine output normalizes Blood pressure increases 39
40 MONITORING EKG monitoring if available Pulse oximeter Most widely used physiological monitoring device for heart rate, oxygenation Especially useful in anaesthesia, ICU Simple to use Should be minimum standard of monitoring in every surgical theatre Blood pressure Manually or automated machine 40
41 Patient Referral and Transport 41
42 STABILIZATION AND TRANSFER Resuscitation completed Analgesia administered Laboratory specimen sent Fractures immobilized Documentation completed Transfer Ward Operating theatre Higher level of care centre 42
43 DECISION MAKING Can we do procedure here? Is operating theatre safe, ready to use? Are necessary equipment, drugs, supplies available? Are team members available? Do I have knowledge and skill to perform necessary procedure safely? Is there back-up or extra support available if needed? Can we manage potential complications if problems arise? Do we have facilities for good post-operative care? If the answer to any of these questions is "NO" it is inadvisable to proceed with surgery! 43
44 TRANSFER OF TRAUMA PATIENT Patient transfer carries inherent risk Patients must be stabilized prior to departure: Effectively resuscitated Controlled airway Normalized circulation Immobilized fractures Appropriate analgesia Functioning intravenous lines Patients should be transported only to facilities offering higher level of care 44
45 TRANSFER OF TRAUMA PATIENT Planning and preparation: Mode of transport Accompanying personnel, including family Supplies needed for any possible treatment Identifying possible complications Communicate with all involved in transfer including receiving hospital Be prepared: if anything can go wrong, it will and at the worst possible time! 45
46 PATIENT SAFETY: Consent Informed consent means that patient and patient s family understand What is to take place Potential risks, complications of both proceeding and not proceeding Have given permission for intervention Be attentive to legal, religious, cultural, linguistic, family norms and differences Our job is not to judge, but to provide care to all without regard to social status or any other considerations 46
47 PATIENT SAFETY: Consent With invasive, surgical procedures important to fully explain : What are you proposing to do? What are reasons for recommending procedure? What are expectations, goals? Communicate effectively: Use language that can be understood Draw pictures, use an interpreter if necessary Allow patient, family members, elders to ask questions and consider what has been discussed 47
48 RECORD KEEPING Essential that patients receive written note describing diagnosis, procedure performed All records should be clear, accurate, complete, signed 48
49 RECORD KEEPING Admission note/preoperative note Preoperative assessment, management plan, patient consent should be clearly documented Delivery book Chronological list of deliveries, procedures, interventions, complications, outcomes for mother and baby 49
50 RECORD KEEPING Operating theatre records Patient identity Procedure performed: both major and minor Personnel involved Complications Blood loss Standardized forms save time, encourage staff to record required information Postoperative notes All patients assessed at least once after surgery Vital signs, patient s condition accurately recorded 50
51 RECORD KEEPING Progress note Need not be long, must comment on patient s condition, note any changes in management plan Should be signed by person writing note Discharge note Admitting and definitive diagnoses Summary of patient s course in hospital Outpatient instructions: medication details planned follow-up suture removal, special wound care 51
52 Emergency procedures 52
53 OXYGEN SUPPLEMENTATION Reliable oxygen supply is essential for anaesthesia or any seriously ill patient Oxygen concentrators are the most suitable, economical way to provide oxygen; few cylinders in case of power failure Whichever source of oxygen, an effective system is needed for maintenance and repairs Clinical staff need training in how to use oxygen safely, effectively, economically 53
54 OXYGEN SUPPLEMENTATION Cylinder System Oxygen Concentrator Inexpensive to buy Expensive to operate Needs year-round supply of cylinders Training and maintenance needed Can store oxygen More expensive to buy Inexpensive to operate Requires only electricity Training and maintenance needed Cannot store oxygen; provides only when power supply is on 54
55 OXYGEN SUPPLEMENTATION Start oxygen at 5 L/min If no improvement, increase to: 6-10 L/min via facemask or L/min via facemask with reservoir When improving, titrate down 1-2 L/min, allowing at least 2-3 minutes to evaluate effect. Strive to maintain saturation >90% 55
56 INTRAVENOUS ACCESS Cannula should be placed in arm vein, not over joint, easy fixation. Comfortable and convenient for drug administration and care Best veins in emergencies: - Antecubital fossa - Femoral - External jugular Do not attempt subclavian vein due to high risk of pleural puncture Cephalic Vein Basilic Vein Superficial veins 56
57 INTRAVENOUS ACCESS: Central veins Femoral Vein Lateral to medial: Nerve, Artery, Vein, Empty space, Ligament (NAVEL) Femoral vein If right handed, stand on patient s right, palpate femoral artery Prep area carefully; site is contaminated Use a 14, 16 or 18 G (20 G in child) cannula mounted on 5 ml syringe Avoid injured extremities, if possible 57
58 A VENOUS CUTDOWN B C Equipment Small scalpel Artery forceps Scissors Large catheter (or sterile infant feeding tube) Transverse incision 2 finger breadths above, anterior to medial malleolus (A); (use patient's own finger breadths to define incision) Place two sutures under vein (B) Once catheter in place, tie sutures (C) Use closing sutures to secure catheter 58
59 FLUIDS AND MEDICINES Avoid fluids containing dextrose during resuscitation Use Saline or Ringer's lactate For shocked patient: give fluids as fast as drip runs until blood pressure responds May need a pressure infusion bag to push fluids Monitor response carefully; look at vital signs, urine output Always give medicines intravenously during resuscitation 59
60 SURGICAL CRICOTHYROIDOTOMY Hyperextend neck, if possible Identify groove between cricoid and thyroid cartilages just below "Adam's apple" Clean area, infiltrate with local anaesthetic 1 Incise through skin vertically, use blunt dissection to clearly see membrane between thyroid and cricoid Using small scalpel, stab through membrane into trachea 2 60
61 SURGICAL CRICOTHYROIDOTOMY 4 Rotate blade, use curved forceps to widen opening Pass thin introducer or nasogastric tube into trachea if small access Run #4-6 size endotracheal tube over introducer, pass into trachea (D) Remove introducer, if used Do not attempt surgical cricothyroidotomy in children < 10 years 61
62 LARGE NEEDLE CRICOTHYROIDOTOMY A B - Puncture the crico-thyroid membrane with a large bore catheter attached to syringe filled with water or saline. - Aspirate as you insert. When entering the trachea, air bubbles will appear in the syringe. - Advance the catheter and retract the needle - Secure the catheter - Connect the catheter to oxygen source, set to 15 L/min - Use I:E ration 1:4 sec (Inspiration:Expiration ratio) C D 62
63 Trauma in Children 63
64 TRAUMA IN CHILDREN Trauma is the leading cause of death in all children Most common surgical problem affecting children Proper treatment can prevent death and life-long disability Infants and children differ from adults in significant physiological and anatomical ways - smaller physiological reserves - increased risk of: dehydration hypoglycaemia hypothermia 64
65 TRAUMA IN CHILDREN Airway Breathing Circulation Disability Exposure of child without losing heat Principles of managing paediatric trauma patients are essentially same as for adult 65
66 MANAGING THE AIRWAY IN A CHILD WITH OBSTRUCTED BREATHING 66
67 MANAGING THE AIRWAY IN A CHILD WITH SUSPECTED NECK TRAUMA 67
68 STABILIZE SUSPECTED NECK TRAUMA 68
69 LOGROLL IN SUSPECTED NECK TRAUMA Avoid rotation, extremes of flexion and extension of neck One person should assume responsibility for neck: Stand at top of patient and hold head Place fingers at edge of mandible with palm over ears Maintain gentle traction to keep neck straight and in line with body 69
70 BREATHING If child not breathing, ventilate with self-inflating bag and mask Connect mask to oxygen if available Must have correct size and position of facemask to prevent leakage 70
71 OROPHARYNGEAL AIRWAYS Can improve airway opening Come in different sizes Appropriate sized airway goes from centre of teeth (incisors) to angle of jaw when laid on face with raised curved (convex) side up Take particular care in children because of possibility of soft tissue damage 71
72 INSERTION OF OROPHARYNGEAL AIRWAY Select appropriate sized airway Position child to open airway Use tongue depressor, insert airway Convex side up in infant Concave side up in older child until tip reaches soft palate, then rotate 180 and slide back over tongue Recheck airway opening, use different size or reposition if necessary Give oxygen 72
73 HOW TO GIVE OXYGEN 73
74 CIRCULATION The radial pulse at the wrist should be felt. If strong and not obviously fast, pulse is adequate If radial pulse is difficult to find, try brachial pulse in middle of upper arm 74
75 INTRAVENOUS ACCESS IN CHILDREN Select suitable vein to place 22 or 24 gauge cannula Have assistant keep limb steady, use rubber glove or tubing as tourniquet Clean surrounding skin with antiseptic solution Introduce cannula into vein and fix securely with tape Apply a splint with elbow extended, wrist slightly flexed. 75
76 INTRAOSSEOUS ACCESS Intraosseous puncture provides quick access to circulation in shocked child if venous cannulation impossible Fluids, blood, medicines may be given Fluids may need to be given under pressure If intraosseous needles unavailable, use spinal or bone marrow biopsy needle Intraosseous needle normally sited in upper tibia at junction of upper and middle third, avoiding growth plate 76
77 TRAUMA IN CHILDREN Most sensitive indicator of fluid status in a child is urine output Infants are unable to concentrate urine as well as adults, thus more susceptible to electrolyte abnormalities Dosage calculation (based on weight), for fluids, transfusions, drugs is crucial to correct management Normal Urine output: (ml/kg/hour) Infants 1-2 ml/kg/h Children 1 ml/kg/h Adults 0.5 ml/kg/h How much urine would you expect a 20 kg child to produce in 24 hours? 77
78 TRAUMA IN CHILDREN Monitor fluid status, electrolytes, haemoglobin diligently Maintenance fluid requirements must be supplemented to compensate for all losses Tachycardia is an earlier sign than hypotension Events happen quickly in babies; monitor closely 78
79 TRAUMA IN CHILDREN Malnutrition can impair response of children to injury, ability to heal and recover Good nutrition promotes healing - poor nutrition prevents it Avoid hypothermia. Infants and young children, especially those with little subcutaneous fat, are unable to maintain normal body temperature when there are wide variations in ambient temperature or when anaesthetized 79
80 SHOCK RESUSCITATION PROTOCOL IN CHILDREN 80
81 TRAUMA IN THE ELDERLY Injury risk increases due to slower reflexes, reduced visual acuity, diminished strength Even though appearing minor, injuries should be given higher severity scores simply based on age Clinician's index of suspicion should be increased 81
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Enables MDA Medical Teams to categorize victims in mass casualty scenarios, in order to be able to triage and treat casualties
 MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
PRACTICE GUIDELINE TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL
 PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
TRANSPORT OF CRITICALLY ILL PATIENTS
 TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Vascular Access. Chapter 3
 Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Basic ATLS. The Primary Survey. Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon
 Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
PARAMEDIC TRAINING CLINICAL OBJECTIVES
 Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Patient Assessment/Management Trauma
 Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Chapter 6. Hemorrhage Control UNDER FIRE KEEP YOUR HEAD DOWN
 Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES
 QTP4N0X1C-9 02 July 2015 AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES Volume 9 TOTAL FORCE, TOTAL CARE EVERYTIME, ANYWHERE 383d TRAINING SQUADRON/XUFB
QTP4N0X1C-9 02 July 2015 AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES Volume 9 TOTAL FORCE, TOTAL CARE EVERYTIME, ANYWHERE 383d TRAINING SQUADRON/XUFB
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services
 State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care. Clinical Management Guideline: Standard Trauma Resuscitation
 Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma
 Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma Deakin, C. D. MA, MRCP, FRCA; Davies, G. MRCP; Wilson, A. FRCS Author Information From the Helicopter Emergency Medical Service, Royal
Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma Deakin, C. D. MA, MRCP, FRCA; Davies, G. MRCP; Wilson, A. FRCS Author Information From the Helicopter Emergency Medical Service, Royal
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
Emergency Medical Responder Mid-Course Knowledge Evaluation
 Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
Percutaneous Abscess Drainage
 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT
 CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Obstetric Emergencies
 Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Package for Emergency Resuscitation and Intensive Care Unit
 Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit
Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
Guidelines for Transport of the Critically Ill
 Page 1 of 16 Guidelines for Transport of the Critically Ill Version Effective Date 1 May 1994 2 Feb 2002 3 Apr 2014 Document Number Prepared by College Guidelines Committee Endorsed by HKCA Council Next
Page 1 of 16 Guidelines for Transport of the Critically Ill Version Effective Date 1 May 1994 2 Feb 2002 3 Apr 2014 Document Number Prepared by College Guidelines Committee Endorsed by HKCA Council Next
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM
 Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
N26 Chest Tubes 5/9/2012
 Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
 XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
Seven steps to patient safety The full reference guide. Second print August 2004
 Seven steps to patient safety The full reference guide Second print August 2004 National Patient Safety Agency Seven steps to patient safety 113 Appendix Four F Examples of events according to severity
Seven steps to patient safety The full reference guide Second print August 2004 National Patient Safety Agency Seven steps to patient safety 113 Appendix Four F Examples of events according to severity
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
ADMINISTERING EMERGENCY OXYGEN
 FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
RP0807 - PERFORM SPLINTING TECHNIQUES
 RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Patient Information. Anterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Injury Law Center OTHER INJURIES
 Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. OTHER INJURIES
Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. OTHER INJURIES
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION
 A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
A PROCEDURAL GUIDE TO MIDLINE CATHETER INSERTION See Also CPG midline catheters for indications, contraindications and post insertion management What is a midline A midline catheter is an 8-12 cm catheter
Anaesthesia tutorial of the week 112: Prone Positioning
 Anaesthesia tutorial of the week 112: Prone Positioning Dr D G Hovord Specialist Trainee Registrar - Anaesthetics University Hospitals of Coventry and Warwick [email protected] Self-assessment Before
Anaesthesia tutorial of the week 112: Prone Positioning Dr D G Hovord Specialist Trainee Registrar - Anaesthetics University Hospitals of Coventry and Warwick [email protected] Self-assessment Before
Human Capital Development & Education Program Proposal
 Human Capital Development & Education Program Proposal Cardiology & Cardiovascular Surgery Emergency Medicine Respiratory Medicine Infection Control HMIS 1 (15 Courses) Module 1/2 1/15 Course Title : Management
Human Capital Development & Education Program Proposal Cardiology & Cardiovascular Surgery Emergency Medicine Respiratory Medicine Infection Control HMIS 1 (15 Courses) Module 1/2 1/15 Course Title : Management
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains)
 NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains) Date of First Issue 12/12/2012 Approved 12/12/2012 Current Issue Date 12/12/2012 Review Date 12/12/2014 Version 1 EQIA Yes 14/12/2012
NHS FORTH VALLEY Chest Drain Insertion by Seldinger Method (Pigtail drains) Date of First Issue 12/12/2012 Approved 12/12/2012 Current Issue Date 12/12/2012 Review Date 12/12/2014 Version 1 EQIA Yes 14/12/2012
Procedure -8. Intraosseous Infusion Adult and Pediatric EZIO. Page 1 of 7 APPROVED:
 Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
Frontline First Aid EMR Scenario Examples
 Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Airway and Breathing Skills Levels Interpretive Guidelines
 Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma
 Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Licensed Vocational Nurse Scope of Practice Standards Health Care Services
 1BCHAPTER 5 2BLicensed Vocational Nurse Scope of Practice Standards I. POLICY: Licensed Vocational Nurses (LVNs) are NOT independent practitioners. It is not within the scope of LVN practice to function
1BCHAPTER 5 2BLicensed Vocational Nurse Scope of Practice Standards I. POLICY: Licensed Vocational Nurses (LVNs) are NOT independent practitioners. It is not within the scope of LVN practice to function
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]
![SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]](/thumbs/27/9667060.jpg) SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Objective of This Lecture
 Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
Component 2: The Culture of Health Care Unit 3: Health Care Settings The Places Where Care Is Delivered Lecture 5 This material was developed by Oregon Health & Science University, funded by the Department
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
New 7/1/2015 MCFRS 1
 New 7/1/2015 MCFRS 1 The providers will summarize the need for this change from an epinephrine auto injector The provider will define the proper dosage of epinephrine for the adult and pediatric patient
New 7/1/2015 MCFRS 1 The providers will summarize the need for this change from an epinephrine auto injector The provider will define the proper dosage of epinephrine for the adult and pediatric patient
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Placement of an indwelling urinary catheter in female dogs
 Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Inferior Vena Cava Filter Placement and Removal
 Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
DELINEATION OF PRIVILEGES - EMERGENCY MEDICINE
 KALEIDA HEALTH Name: Date DELINEATION OF PRIVILEGES - EMERGENCY MEDICINE LEVEL I (CORE) PRIVILEGES Physicians with these privileges are expected to have training and/or experience and competence on a level
KALEIDA HEALTH Name: Date DELINEATION OF PRIVILEGES - EMERGENCY MEDICINE LEVEL I (CORE) PRIVILEGES Physicians with these privileges are expected to have training and/or experience and competence on a level
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Measuring central venous pressure
 Elaine Cole Senior lecturer ED/Trauma, City University Barts and the London NHS Trust 1 Learning outcomes That the clinician can: Describe the sites of central venous catheterisation Understand why central
Elaine Cole Senior lecturer ED/Trauma, City University Barts and the London NHS Trust 1 Learning outcomes That the clinician can: Describe the sites of central venous catheterisation Understand why central
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g.
 How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
