Yue Zhu, Nader Hanna, Cherif Boutros, H. Richard Alexander Jr. Background
|
|
|
- Felicia Rich
- 8 years ago
- Views:
Transcription
1 Review Article Assessment of clinical benefit and quality of life in patients undergoing cytoreduction and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) for management of peritoneal metastases Yue Zhu, Nader Hanna, Cherif Boutros, H. Richard Alexander Jr Division of Surgical Oncology, Department of Surgery and the Marlene and Stewart Greenebaum Cancer Center, University of Maryland School of Medicine, Baltimore, Maryland, USA Corresponding to: Yue Zhu, M.D, M.S. Department of Surgery, University of Maryland School of Medicine, 22 S. Greene Street Room S4B10, Baltimore, Maryland 21201, USA. Abstract: Peritoneal metastases is a significant clinical challenge; life expectancy following diagnosis is usually very short. Surgical cytoreduction with HIPEC is being used with increasing frequency in selected patients; most outcome data have shown that prolonged median survivals can be observed in selected patients. This review summarizes the published data related to outcome and quality of life after cytoreduction and HIPEC to provide insights into its use in patients with peritoneal carcinomatosis. Key Words: Cytoreduction surgery (CRS); Hyperthermic Intraperitoneal Chemotherapy (HIPEC); peritoneal metastases Submitted Aug 17, Accepted for publication Sep 28, doi: /j.issn Scan to your mobile device or view this article at: Background Once peritoneal metastases occur from gastrointestinal cancers or mesothelioma, morbidity and mortality are almost always secondary to disease progression within the abdominal cavity. Patients experience progressive abdominal distention due to tumor growth and malignant ascites, pain, early satiety, and ultimately experience profound cachexia and inanition (1). The condition is characterized grossly by diffuse tumor nodules on the peritoneal surfaces; the omentum is a favored site for development of extensive bulky metastases which is typically referred to as omental caking on preoperative imaging studies. Tissue is usually obtained by laparoscopic or percutaneous biopsy and the histologic features of the tumor combined with other clinical, laboratory, or imaging findings can successfully identify the tumor site of origin. According to the multicenter EVOCAPE I study (2), the median survival in patients with peritoneal metastases was 5.2 months for those with advanced colorectal cancer (n=118) and 3.1 months for those with advanced gastric cancer (n=125). Despite significant advances in the development of more efficacious systemic chemotherapy for many GI cancers, most notably colorectal cancer; systemic treatment is associated with potentially severe toxicity in many patients and median survival is still less than two years (Table 1). Mesothelioma is very rare with new cases diagnosed annually in US, its incidence is increasing and expected to reach a peak in 2020 in Europe (3). Systemic chemotherapy for advanced GI cancers and mesothelioma It is important to briefly review the efficacy and toxicity of various systemic chemotherapy regimens commonly used for patients with advanced GI cancers or mesothelioma to provide context and better understand the potential role of cytoreduction surgery (CRS) and HIPEC. Over the past 6 years there have been several new chemotherapeutic and biological agents that have been approved by the FDA for treatment of patients with advanced colorectal cancer. One common regimen is 5-fluorouracil, leucovorin, and oxaliplatin (FOLFOX) combined with bevacizumab. Saltz et al. reported results of a 2 2 factorial design random assignment trial comparing capcitebine and oxaliplatin to FOLFOX with or without bevacizumab (4). A response rate greater than 50% and a median actuarial survival longer than 20 months were reported for those treated with
2 Journal of Gastrointestinal Oncology, Vol 4, No 1 March Table 1 Survival in patients with peritoneal dissemination secondary to various cancers based on variability in tumor biology Histology in order of decreasing biological aggressiveness Estimated median survival (months) Pancreatic adenocarcinoma ~6 Gastric adenocarcinoma ~6-12 High-grade appendiceal adenocarcinoma Colorectal adenocarcinoma Peritoneal mesothelioma Low grade appendiceal neoplasms >60 Table 2 Early and late signs and symptoms related to peritoneal metastases Early Late Mild distention/bloating Massive ascites/distention/dyspnea Crampy intermittent pain High grade obstruction Early satiety Weight loss/malnutrition Decreased energy Inanition, cachexia, death FOLFOX and bevacizumab; however, less than half of all patients completed the full course of planned therapy. In addition to the toxicities associated with chemotherapy, a recent study showed that the fatal adverse events (FAEs) associated with bevacizumab and chemotherapy was 2.9% (5). Compared with chemotherapy alone, the addition of bevacizumab was associated with an increased risk of FAEs, with a relative risk of This association varied significantly with chemotherapeutic agents, such as taxanes or platinum agents, but not with tumor types or bevacizumab doses. The most common causes of FAEs were hemorrhage (23.5%), neutropenia (12.2%), and gastrointestinal tract perforation (7.1%). In patients with malignant peritoneal mesothelioma the use of pemetrexed and cisplatin has been widely used; however, the overall response rate is approximately 20% and the duration of response is less than 12 months (6). In a Phase III clinical study of chemotherapy in malignant peritoneal mesothelioma patients, pemetrexed and cisplatin resulted in grade 3 or 4 neutropenia in 27.9% and grade 3 or 4 leukopenia in 17.7%) (7). The incidence of grade 3/4 neutropenia was significantly higher among none or partial vitamin supplementation patients (41.4%) compared with full supplementation patients. Fourteen patients who received pemetrexed/cisplatin died while on study therapy or within 30 days of the last dose of study drug, compared with eight patients who received cisplatin alone (6.2% vs. 3.6%). The incidence of nausea, vomiting, fatigue, diarrhea, dehydration and stomatitis were significantly higher in the pemetrexed and cisplatin group. Taken together, these data show that systemic chemotherapy and biological therapy regimens commonly accepted as standard of care for patients with advanced GI cancers and MPM have considerable toxicity and mortality. Toxicities can be cumulative as in the case of oxaliplatin and severe as noted with bevacizumab. Patients typically receive protracted courses of therapy in order to enjoy continued clinical benefit and not systemic regimens have been shown to be curative in the setting of metastatic disease. CRS and HIPEC In the past, the role of operation in the management of patients with cancer has been mainly to cure localized cancers, to provide staging information, and for palliation in patients with pain, bleeding or obstruction (Table 2). Pseudomyxoma peritonei, malignant mesothelioma and peritoneal carcinomatosis from gastrointestinal cancers have been considered incurable conditions for which the role of surgical intervention was limited (1). However, over the last two decades, multi-modality treatments have evolved for patients with peritoneal carcinomatosis and the utilization of cytoreduction combined with hyperthermic intraperitoneal chemotherapy (HIPEC) has been increasingly used with therapeutic intent (Figure 1). Most data regarding its efficacy and morbidity have been derived from single center reviews or more recently from combined institutional databases (8-11). CRS requires a combination of standard surgical maneuvers designed to completely resect or ablate all gross disease in the peritoneum (Table 3). The various operative procedures may include parietal and visceral peritonectomy, greater omentectomy, splenectomy, cholecystectomy, ablation of tumor deposits on the liver capsule, small bowel
3 64 Zhu et al. CRS and HIPEC for patients with peritoneal metastases A B Figure 1 A. Operative photograph shows a massive omental metastasis and smaller volume peritoneal metastases in a patient with a high grade appendiceal carcinoma; B. A complete CRS was possible resulting in a good quality of life for over one year after operation Table 3 Advantages and rationale for the use of CRS and HIPEC Disease Features Limited to local/ regional spread Symptomatic ascites, mucin production Clinically relevant distant metastases infrequent Death due to local/regional complications Peritoneal dissemination is a common mode of metastases for: Colorectal cancer Appendiceal cancer Malignant peritoneal mesothelioma Resection Features Tumors are surface metastases Multiple in number and small in size Can usually be resected or ablated Can palliate symptoms of obstruction Can control ascites HIPEC Features Provides intensive regional treatment to the site of micrometastases Delivers chemotherapy and hyperthermia to all serosal surfaces Applies clinical useful levels of regional hyperthermia: Has direct lethal effects on tumor Potentiates the cytotoxicity of chemotherapy Limits systemic exposure and unnecessary toxicity: Well established pharmacokinetic advantage Therapeutic benefit established in ovarian cancer patients resection, colonic and rectal resection, partial gastrectomy, lesser omentectomy, hysterectomy, ovariectomy, and urinary bladder or ureteral resection (Figure 2). The aim of CRS is to obtain a complete macroscopic cytoreduction; after resection a score estimating the completeness of cytoreduction or CCR is used and defined as: CCR-0, no residual peritoneal tumor nodules; CCR-1, residual tumor nodules <2.5 mm; CCR-2, residual tumor nodules between 2.5 mm and 2.5 cm; or CCR-3 residual tumor nodules >2.5 cm or a confluence of unresectable tumor nodules at any site (12). For the performance of HIPEC a circuit pump consisting of a reservoir heat exchanger and roller pump is necessary to circulate the perfusate via several drains place into the peritoneal cavity. The intraperitoneal temperature should reach C by using leading to an inflow temperature of about 43. HIPEC can be performed in open or closed abdomen technique. One of the leading advantages of the open technique is a better control of the intraperitoneal
4 Journal of Gastrointestinal Oncology, Vol 4, No 1 March circulation and uniform distribution of the cytostatic agents (Table 3). However, the disadvantage is the increased risk of exposure to health care personnel when compared with the closed abdomen technique. Mitomycin-c is the most common agent used during HIPEC in the treatment of peritoneal carcinomatosis patients from appendiceal and colorectal cancers. It is an antitumor antibiotic, with approximately 90% of the drug absorbed within the 90 minutes intraperitoneal irrigation. Cisplatin is an alkylating agent used in treating gastric cancer, ovarian cancer and diffuse malignant peritoneal mesothelioma (13). In selected patients with minimal disease burden or in those undergoing staging laparoscopy, laparoscopic HIPEC can be performed. The benefit of such approach is based on avoiding inherent complications related to major abdominal incision. Laparoscopy is usually associated with less postoperative pain, hospital stay and an earlier capacity to return to work. Mortality and mrbidity of CRS and HIPEC Figure 2 Operative photograph shows diffuse small volume peritoneal metastases in a patient with malignant peritoneal mesothelioma. Note the relative sparing of the small bowel serosa which is a favorable finding; the mesenteric implants were treated primarily with argon beam electrofulguration The morbidity and mortality after CRS and HIPEC range from 12% to 41% and from 0% to 8%, respectively (12-24) (Table 4, Figure 3). Morbidity can be divided into surgery-related and chemotherapy-related events. Common surgical complications are bleeding, postoperative bowel obstruction, anastomotic leakage, wound infection, pulmonary embolism and venous thrombosis. Morbidity related with cytostatic agents used in HIPEC is rare but includes leucopenia, anemia, thrombocytopenia, and liver or renal toxicity. Numerous reports over the past 20 years indicate that mortality and morbidity following cytoreduction with HIPEC is decreasing because of improvements of surgical technique and patient selection criteria (Table 5). Two recent publications addressing mortality and morbidity provide Table 4 Selected series showing morbidity and mortality associated with CRS and HIPEC Authors, year Patients (n) Origin Agents Mortality (%) Median survival (months) Overall morbidity (%) Major morbidity Stephens et al., 1999 (19) 200 Mixed MMC Glenhen et al., 2003(12) 216 Mixed MMC CDDP CDDP/MMC Gusani et al., 2008 (15) 124 Mixed MMC Kusamura et al., 2006 (16) 209 Mixed CDDP+MMC Verwaal et al., 2003 (25) 105 CRC MMC Glehen et al., 2004 (18) 506 CRC MMC/LOHP Yonemura et al., 2005 (20) 105 GC MMC/DDP Feldmann et al., 2003 (22) 49 DMPM DDP Deraco et al., 2006 (23) 49 DMPM DDP/DXR DDP/MMC Yan et al., 2007 (17) 70 DMPM MMC/DDP Cotte et al., 2007 (24) 81 OC DDP DI Glorgio et al. (21) 47 OC CDDP CRC, colorectal cancer; GC, gastric cancer; PMP, pseudomyxoma peritonei; OC, Ovarian cancer; DMPM, diffuse malignant peritoneal mesothelioma; MMC, mitomycin C; DDP, cisplatin; LOHP, oxaliplatin; DXR, doxorubicin
5 66 Zhu et al. CRS and HIPEC for patients with peritoneal metastases A B Figure 3 A. CT scan shows a patient with symptomatic ascites secondary to peritoneal mesothelioma before CRS and HIPEC; B. The patient underwent a successful CRS and HIPEC and remained asymptomatic and free of imageable disease based on CT scan for over 18 months Table 5 Summary of features associated with HRQoL questionnaires Sub scales Items Data collection Scores FACT-C PWB, SWB, EWB, Treatment Outcome 37 Self-administered, Higher, better Index interview SF-36 Physical functioning, role physical, role 36 Self-administered Higher, better emotional, bodily pain, general health, vitality and mental health Interview CES-D Depressive disorder 20 Self-administered >=17 indicates significant depressive symptoms BPI Intensity of pain, reactive dimension 14 Self- administered Higher, more interference EORTC C-30 Role, physical, cognitive, emotional and 30 Self-administered Higher, better social functioning EORTC QLQ-CR 38 CRC specific supplement of QLQ-C30 38 Self-adminstered Higher, better FACT-C, Functional Assessment of Cancer Therapy Colon; PWB, Physical well-being; SWB, Social/family well-being; EWB, Emotional well-being; SF-36, Medical Outcomes Study Health Survey, short form; CES-D scale, Center for Epidemiologic Studies Depression; BPI, Brief Pain Inventory; EORTC QLQ-C30, European Organization for Research and Treatment of Cancer Quality of Life Questionnaire Core; EORTC QLQ-CR38, Colorectal Cancer Module 38, the CRC-specific supplementation of the QLQ-C30 informative data. Glehen and et al. conducted a retrospective multicenter cohort study in French-speaking institutions to evaluate toxicity and principal prognostic factors after cytoreduction surgery and HIPEC (14). One thousand two hundred ninety patients from 25 institutions who underwent 1,344 procedures between 1989 and 2007 were included; HIPEC was performed in 1,154 procedures. Colorectal adenocarcinoma (40.5%), pseudomyxoma peritonei (23.3%), gastric adenocarcinoma (12.3%), peritoneal mesothelioma (6.8%), and appendiceal adenocarcinoma (3.9%) were the principal origins of carcinomatosis. The overall morbidity and mortality rates were 33.6% and 4.1%, respectively. The median survival was 30 months for patients with colorectal cancer, 9 months for patients with gastric cancer, 41 months for patients with peritoneal mesothelioma, and 77 months for patients with cancer from appendiceal adenocarcinoma. Gusani et al. reported low mortality in patients treated at a single institution (15). A total of 122 patients underwent 124 cytoreduction and HIPEC procedures. R-0 resection was achieved in 28.7% of cases, R-1 in 54.9%, and R-2 in 16.4%. Median operative time was 460 minutes (range, minutes) and median blood loss was 1,150 ml (range, 10-14,000 ml). Grade 3 or 4 morbidity was seen in 29.8% of cases, with overall morbidity 56.5%. Two-year survival was 66.7% for appendiceal cancer patients; however, 5-year survival was 36.7%. The number of anastomoses and extent
6 Journal of Gastrointestinal Oncology, Vol 4, No 1 March 2013 of cytoreduction were independent prognostic variables for major morbidity. In-hospital and 30-day mortality rates were 0% and 1.6%, respectively. Survival following CRS and HIPEC In 2003, Verwaal et al. reported results of a small prospective randomized controlled trial from the Netherlands Cancer Institute including 105 colorectal cancer patients who had peritoneal metastases or positive cytology from ascites who were treated with CRS and HIPEC versus intravenous 5-fluorouracil (Table 4). This trial was updated with a minimal follow-up of 6 years in 2008 (25,26). The study showed a disease-specific survival of 22.2 months after CRS and HIPEC that was significantly better than the survival of 12.6 months after standard systemic chemotherapy. Elias et al. reported a cohort controlled study that compared outcomes of 48 patients treated with systemic chemotherapy to 48 who underwent CRS and HIPEC for peritoneal metastases for colorectal cancer (27). Most clinical and pathological variables were well matched; the median actuarial overall survivals were 23.9 months in the chemotherapy treated group and 62.7 months in the CRS and HIPEC group. The differences were statistically significant; the outcome of the CRS and HIPEC treated group was better than most other reports of this treatment approach in this patient population. The largest single study providing outcomes in patients following CRS and HIPEC in patients with colorectal cancer was reported by Glehen and et al. That study included 506 patients treated at 28 institutions operated between 1987 and 2002 (18). The morbidity and mortality rates were 22.9% and 4%, respectively. The overall median survival was 19.2 months compared to the 62.7 months median survival reported by Elias et al. Patients in whom CRS was complete had a median survival of 32.4 months compared with 8.4 months for patients in whom complete CRS was not possible. Survival is only marginally improved by CRS and HIPEC in selected patients with peritoneal metastases from gastric cancer and is approximately 9 months (18,20). Patients with ovarian cancer who have undergone CRS and HIPEC had median survival rates ranging from 28 to 46 months and 5-year survival rates from 15% to 50% (21,24). For patients with diffuse malignant peritoneal mesothelioma (DMPM), a rare disease with relatively low incidence, median overall survivals between 34 and 92 months and 5-year survival rates from 33% to 59%, respectively, have been reported (17,23). Since patients with peritoneal metastases have a poor prognosis and limited longevity, measuring quality of life (QoL) endpoints for patients after CRS and HIPEC is very important. Health related quality of life after CRS and HIPEC 67 The concept of health-related quality of life (HRQOL) and its determinants have evolved since the 1980s to encompass those aspects of overall quality of life that can be clearly shown to affect health either physical or mental (28-30). HRQoL is a broad multi-dimensional concept that usually includes self-reported measures of physical and mental health. Several measures have been used to assess HRQoL and related concepts of functional status. However, there is no substitute for a standard QOL questionnaire properly administered. The HRQoL construct is measurable in that its dimensions can be assessed reliably over time and have been shown to be valid with reference to other validated instruments (Table 5). There are at least four areas can be measured in quality of life assessment: physical wellbeing, social/family well-being, functional well-being and emotional well-being. There are other important factors in patient s life that may modify how they experience their overall QOL, such as spirituality, financial and support resources, psychological resilience and sexuality. FACT-C and SF-36 are the mostly used questionnaires to estimate QoL in patients after CRS and HIPEC. The FACT-C scale (Functional Assessment of Cancer Therapy Colon) is a self-reported questionnaire, consisting of the FACT-G general version with 28 items plus 9 items for the colon subscale (31). It consists of subscales measuring physical well-being (PWB), functional well-being (FWB), social/ family well-being (SWB), emotional well-being (EWB), and a Treatment Outcome Index (TOI). The TOI is calculated by adding PWB, FWB, and the colon cancer subscale. The FACT can be either self-administered or used in an interview format and is easily completed in 5 to 10 minutes. A higher score indicates a better QoL. The SF-36 (Medical Outcomes Study Health Survey, short form) is a 36-item generic health measure. It assesses the physical functioning, role physical, role emotional, bodily pain, general health, vitality and mental health (32). Scores range from 0 to 100. A higher score indicates better functioning. While these measures have been widely used and extensively validated in clinical settings and special population studies, their length often makes them impractical to use in population surveillance. In addition to the FACT-C and SF-36, there are other instruments to evaluate patient s QoL. The CES-D scale (Center for Epidemiologic Studies Depression) is a 20-item self-report measure having a high sensitivity
7 68 Zhu et al. CRS and HIPEC for patients with peritoneal metastases Table 6 Outcomes of published studies in quality of life following CRS and HIPEC Author Patients (n) Follow-up time Questionnaire used Primary tumor site Schmidt et al. (43) years EORTC QLQ-C30 Appendix Tuttle et al. (45) months FACT-C, TOI Mixed Hill et al. (42) months FACT-C, SF-36, BPI, CES-D, ECOG Colonic Per Jess et al. (44) months SF-36, EORTC QLQ-C30, CR38 McQuellon et al. (37) months FACT-C, SF-36 Mixed McQuellon et al. (39) months FACT-C, SF-36, CES-D, BPI, ECOG Mixed McQuellon et al. (40) months FACT-C, SF-36,CES-D, PSRS, LAS, SCCQ, Mixed McQuellon et al. (41) months FACT-C, SF-36, CES-D, ECOG Appendiceal and positive predictive value for detecting depressive disorders (33). A score of >=17 indicates that the patients has significant depressive symptoms and would be categorized as a possible case of depression. Brief Pain Inventory (BPI) is a 14-item, self-report questionnaire used to provide information on the intensity of pain (the sensory dimension) as well as the degree to which pain interferes with function (the reactive dimension) (34). The Eastern Cooperative Oncology Group (ECOG) performance status are used by doctors and researchers to assess how a patient s disease is progressing, assess how the disease affects the daily living abilities of the patient, and determine appropriate treatment and prognosis (35). The score runs from 0 to 5, with 0 denoting perfect health and 5 denoting death. European Organization for Research and Treatment of Cancer Quality of Life Questionnaire Core 30 (EORTC QLQ-C30) is a 30-item self-reporting questionnaire developed to assess the quality of life of cancer patients. It is grouped into five functional subscales (role, physical, cognitive, emotional and social functioning). The Colorectal Cancer Module 38 (EORTC QLQ-CR38) is the CRC-specific supplementation of the QLQ-C30. Its 38 items cover symptoms and side effects from different treatment modalities, body image, sexuality, and future perspective. It was tested in 117 Dutch colorectal patients and was found to yield good reliability and validity (36). The amount of data published relating to the HRQoL in patients after CRS and HIPEC are very limited (37-45) (Table 6). Ideally, data should be derived from a prospectively designed study in which patients receive a pre-surgery assessment of QoL as the baseline. Postoperative assessments are then conducted at various time points ranges and compared with the baseline score. With each patient serving as their own control relatively small studies can be used to identify statistically significant differences in HRQoL over time. The research group at Wake Forest University has published results of several studies relating to the QoL in patients after CRS and HIPEC. Their initial study was in 64 patients treated by CRS and HIPEC in 2001 (37). The authors used FACT-C to assess QoL and they found significant decrease of physical, emotional and functional, and well-being scores with an increase relative to baseline levels during follow-up at 3,6 and 12 months. Most patients returned to baseline or better levels of functioning within 3 months post-treatment. Seventy-four percent of patients resumed greater than 50% of their normal activities one year after surgery. Depressive symptoms were observed at base line and different time points. The patterns were similar to those of patients following bone marrow transplantation (38). The same research group subsequently published the largest HRQoL study in patients treated by CRS and HIPEC from 1998 to 2005 which included 96 patients (39). Patients completed a questionnaire before and after surgery at 3, 6 and 12 months. Similar assessment instruments were used (FACT-C, SF-36, CES-D, BPI, ECOG). Quality of life and pain scores improved from baseline to 12 months. Physical functioning changed over the 12-month study period with improvement recorded at 6 months. Depressive symptoms were common as 25% of patients had symptoms. The authors concluded that acceptable QoL, return of functional status, and reduced pain can be attained between 3 and 6 months following treatment although some deficits in general health remains. The highest scores on general health subscale are lower than the scores in general population. McQuellon et al. also studied long term survivor ship in 17 patients (40). They were interviewed from 3.1 to 8.0 years after treatment. Sixty-two percent described their health as excellent or very good. No limitations on moderate activity were reported in 94% of cases. Functional well-being, physical well-being and FACT total were significantly improved and demonstrated that long-term survivors of peritoneal carcinomas after CRS and HIPEC can return to a good life of quality. Appendiceal cancer is also research interest for
8 Journal of Gastrointestinal Oncology, Vol 4, No 1 March 2013 investigators. QoL for patients with disseminated peritoneal cancer of appendiceal cancer were studied by McQuellon et al. Fifty-eight patients with a mean age 52.4 years were assessed before surgery. Overall survival at 1 year was 78.7%. Emotional well-being improved over the study period, while physical well-being and physical functioning declined at 3 months and then improved to near baseline levels at 6 and 12 months. Depressive symptoms and some physical limitations remain in surviving patients. Percentage of patients with depressive symptoms ranges from 24% to 33% in baseline, 3, 6, and 12 months (41). The authors conclude survival in appendix cancer patients with peritoneal cancer is good, although complications may affect short-form recovery. However, half of patients dropped out of the study. In Hill et al. s recently published paper a total 62 patients who underwent HIPEC for peritoneal carcinomatosis of colonic origin were studied (42). Questionnaires were completed preoperatively and after surgery at 3, 6, and 12 months. The authors used FACT-C, Brief Pain Inventory (BPI), SF-36, CES-D, and the ECOG Performance Status Rating to estimate their QoL. Median overall survival was 18 months, with 71.3 % survival at 1 year. Emotional well-being scores significantly improved after HIPEC. Social/family wellbeing and the colon subscale of the FACT worsened at 3 months, but recovered at 6 months. CES-D scores showed 33%-50% of patients reported depressive symptom. Pain scores increased above base line at 3 months, but decreased below base line at 6 and 12 months. 47% of patients reported normal activity according to their performance status. Long-term functioning in patients following CRS and HIPEC has also been studied by Schmidt et al. who evaluated QoL in 67 patients using the EORTC QLQ-C30 questionnaire with an average post-treatment time of 4 years (range 1-8 years) (43). The mean score for global health status of long-term survivors was 62.6, which was significantly decreased when compared with the general Norwegian population (73.3). The authors showed functional status, particularly the role and the social functioning, were impaired because of presence of ostomies, fatigue, insomnia, or pain. These data indicated that QoL may be adversely affected following CRS and HIPEC. Per Jess et al. reported a clinical study of 23 patients underwent CRS and early postoperative intraperitoneal chemotherapy for pseudomyxoma peritonei (44). Patients were followed in clinic 3, 6, 12, 18, and 24 months after surgery. Short Form-36, together with the two symptomspecific instruments-- EORTC-C30, and EORTC-CR38 were used to assess the quality of life. Seventy percent of 69 patients had one or more complications during or after surgery, but all had recovered; 14% had an asymptomatic recurrence detected within two years. No significant decrease was observed in the scores on the Short Form-36 Questionnaire scales of physical dimension and role physical three months after surgery, only returning to normal after six months. No measurable decrease in QoL was found after 12 and 18 months. Tuttle et al. studied 35 consecutive patients with peritoneal metastases enrolled in a prospective trial from 2001 to Before treatment and then at 4-month postoperative intervals, the authors used the FACT-C, FACT-G and TOI instrument to assess the patients quality of life (45). Quality of life measurements returned to baseline 4 months after treatment and were significantly improved at 8 and 12 months. Functional well being scores and emotional well being scores improved significantly at 8 and 12 months when compared to baseline. Patients treated by MMC dose >30 mg were significantly more likely to have an adverse event compared to low dose MMC treated patients. In their study, many patients were still receiving systemic chemotherapy 4 months after CRS and HIPEC which decreased their quality of life scores. The authors found the QoL of patients after CRS and HIPEC at 12 months is similar to the QoL of colorectal cancer patients who underwent curative resection of primary tumors. Summary Peritoneal metastases from cancer are a common and unfortunate pattern of recurrent metastatic disease for many cancers arising from the gastrointestinal tract or the peritoneal lining. Despite advance in chemotherapy survival is limited; many patients suffer from a marked morbidity from tumor progression in the abdominal cavity. CRS and HIPEC provide a promising and potentially therapeutic option for selected patients with peritoneal surface metastases. Short term mortality and morbidity have been reduced in recent years because of better patient selection and improvements in operative technique and postoperative management. Because CRS and HIPEC have associated morbidity it is important to assess the success of treatment in terms of both quality and longevity of life. In most clinical studies, patient HRQoL status returns to baseline and is generally improve for up to a year after treatment. Acknowledgements Disclosure: The authors declare no conflict of interest.
9 70 Zhu et al. CRS and HIPEC for patients with peritoneal metastases References 1. Glockzin G, Ghali N, Lang SA, et al. Peritoneal carcinomatosis. Surgical treatment, including hyperthermal intraperitoneal chemotherapy. Chirurg 2007;78:1100, , Rusch VW. A proposed new international TNM staging system for malignant pleural mesothelioma. From the International Mesothelioma Interest Group. Chest 1995; 108: Neumann V, Muller KM, Fischer M. Peritoneal mesothelioma--incidence and etiology. Pathologe 1999;20: Saltz LB, Clarke S, Diaz-Rubio E, et al. Bevacizumb in combination with oxaliplatin-based chemotherapy as firstline therapy in metastatic colorectal cancer: a randomized phase III study. J Clin Oncol 2008;26: Ranpura V, Hapani S, Wu S. Treatment-related mortality with bevacizumab in cancer patients: a meta-analysis. JAMA 2011;305: Obasaju CK, Ye Z, Wozniak AJ, et al. Single-arm, open label study of pemetrexed plus cisplatin in chemotherapy naive patients with malignant pleural mesothelioma: outcomes of an expanded access program. Lung Cancer 2007;55: Vogelzang NJ, Rusthoven JJ, Symanowski J, et al. Phase III study of pemetrexed in combination with cisplatin versus cisplatin alone in patients with malignant pleural mesothelioma. J Clin Oncol 2003;21: Sugarbaker PH, Cunliffe WJ, Belliveau J, et al. Rationale for integrating early postoperative intraperitoneal chemotherapy into the surgical treatment of gastrointestinal cancer. Semin Oncol 1989;16: Loggie BW, Fleming RA, McQuellon RP, et al. Cytoreduction surgery with intraperitoneal hyperthermic chemotherapy for disseminated peritoneal cancer of gastrointestinal origin. Am Surg 2000;66: Stewart JH 4th, Shen P, Levine EA. Intraperitoneal hyperthermic chemotherapy for peritoneal surface malignancy: current status and future directions. Ann Surg Oncol 2005;12: Sugarbaker PH. Cytoreduction surgery and peri-operative intraperitoneal chemotherapy as a curative approach to pseudomyxoma peritonei syndrome. Eur J Surg Oncol 2001;27: Glehen O, Osinsky D, Cotte E, et al. Intraperitoneal chemohyperthermia using a closed abdominal procedure and cytoreduction surgery for the treatment of peritoneal carcinomatosis: morbidity and mortality analysis of 216 consecutive procedures. Ann Surg Oncol 2003;10: Yan TD, Cao CQ, Munkholm-Larsen S. A pharmacological review on intraperitoneal chemotherapy for peritoneal malignancy. World J Gastrointest Oncol 2010;2: Glehen O, Gilly FN, Boutitie F, et al. Toward curative treatment of peritoneal carcinomatosis from nonovarian origin by cytoreduction surgery combined with perioperative intraperitoneal chemotherapy: a multi-institutional study of 1,290 patients. Cancer 2010;116: Gusani NJ, Cho SW, Colovos C, et al. Aggressive surgical management of peritoneal carcinomatosis with low mortality in a high-volume tertiary cancer center. Ann Surg Oncol 2008;15: Kusamura S, Younan R, Baratti D, et al. Cytoreduction surgery followed by intraperitoneal hyperthermic perfusion: analysis of morbidity and mortality in 209 peritoneal surface malignancies treated with closed abdomen technique. Cancer 2006;106: Yan TD, Welch L, Black D, et al. A systematic review on the efficacy of cytoreduction surgery combined with perioperative intraperitoneal chemotherapy for diffuse malignant peritoneal mesothelioma. Ann Oncol 2007;18: Glehen O, Kwiatkowski F, Sugarbaker PH, et al. Cytoreduction surgery combined with perioperative intraperitoneal chemotherapy for the management of peritoneal carcinomatosis from colorectal cancer: a multiinstitutional study. J Clin Oncol 2004;22: Stephens AD, Alderman R, Chang D, et al. Morbidity and mortality analysis of 200 treatments with cytoreduction surgery and hyperthermic intraoperative intraperitoneal chemotherapy using the coliseum technique. Ann Surg Oncol 1999;6: Yonemura Y, Kawamura T, Bandou E, et al. Treatment of peritoneal dissemination from gastric cancer by peritonectomy and chemohyperthermic peritoneal perfusion. Br J Surg 2005;92: Di Giorgio A, Naticchioni E, Biacchi D, et al. Cytoreduction surgery (peritonectomy procedures) combined with hyperthermic intraperitoneal chemotherapy (HIPEC) in the treatment of diffuse peritoneal carcinomatosis from ovarian cancer. Cancer 2008;113: Feldman AL, Libutti SK, Pingpank JF, et al. Analysis of factors associated with outcome in patients with malignant peritoneal mesothelioma undergoing surgical debulking and intraperitoneal chemotherapy. J Clin Oncol 2003;21: Deraco M, Nonaka D, Baratti D, et al. Prognostic analysis of clinicopathologic factors in 49 patients with diffuse malignant peritoneal mesothelioma treated with cytoreduction surgery and intraperitoneal hyperthermic
10 Journal of Gastrointestinal Oncology, Vol 4, No 1 March perfusion. Ann Surg Oncol 2006;13: Cotte E, Glehen O, Mohamed F, et al. Cytoreduction surgery and intraperitoneal chemo-hyperthermia for chemo-resistant and recurrent advanced epithelial ovarian cancer: prospective study of 81 patients. World J Surg 2007;31: Verwaal VJ, van Ruth S, de Bree E, et al. Randomized trial of cytoreduction and hyperthermic intraperitoneal chemotherapy versus systemic chemotherapy and palliative surgery in patients with peritoneal carcinomatosis of colorectal cancer. J Clin Oncol 2003;21: Verwaal VJ, Bruin S, Boot H, et al. 8-year follow-up of randomized trial: cytoreduction and hyperthermic intraperitoneal chemotherapy versus systemic chemotherapy in patients with peritoneal carcinomatosis of colorectal cancer. Ann Surg Oncol 2008;15: Mahteme H, Hansson J, Berglund A, et al. Improved survival in patients with peritoneal metastases from colorectal cancer: a preliminary study. Br J Cancer 2004;90: Centers for Disease Control: Measuring healthy days: Population assessment of health related quality of life Gandek B, Sinclair SJ, Kosinski M, et al. Psychometric evaluation of the SF-36 health survey in Medicare managed care. Health Care Financ Rev 2004;25: McHorney CA. Health status assessment methods for adults: past accomplishments and future challenges. Annu Rev Public Health 1999;20: Cella DF, Tulsky DS, Gray G, et al. The Functional Assessment of Cancer Therapy scale: development and validation of the general measure. J Clin Oncol 1993;11: Ware JE, Snow KK, Kosinski M, et al. SF-36 Health Survey Manual and Interpretation Guide. Boston: New England Medical Center, Radloff LS. The CES-D Scale. Applied Psychological Measurement 1977;1: Cleeland CS, Ryan KM. Pain assessment: global use of the Brief Pain Inventory. Ann Acad Med Singapore 1994;23: Zubrod CG, Schneiderman M, Frei E, et al. Appraisal of methods for the study of cancer in man: Comparative therapeutic trial of nitrogen mustard and triethylene thiophoramide. J Chron Dis 1960;11: Sprangers MA, te VA, Aaronson NK. The construction and testing of the EORTC colorectal cancer-specific quality of life questionnaire module (QLQ-CR38). European Organization for Research and Treatment of Cancer Study Group on Quality of Life. Eur J Cancer 1999;35: McQuellon RP, Loggie BW, Fleming RA, et al. Quality of life after intraperitoneal hyperthermic chemotherapy (IPHC) for peritoneal carcinomatosis. Eur J Surg Oncol 2001;27: McQuellon RP, Russell GB, Rambo TD. Quality of life and psychological distress of bone marrow transplant recipients: The time trajectory to recovery over the first year. Bone Marrow Transplant 1998;21: McQuellon RP, Danhauer SC, Russell GB, et al. Monitoring health outcomes following cytoreduction surgery plus intraperitoneal hyperthermic chemotherapy for peritoneal carcinomatosis. Ann Surg Oncol 2007;14: McQuellon RP, Loggie BW, Lehman AB, et al. Longterm survivorship and quality of life after cytoreduction surgery plus intraperitoneal hyperthermic chemotherapy for peritoneal carcinomatosis. Ann Surg Oncol 2003;10: McQuellon RP, Russell GB, Shen P, et al. Survival and health outcomes after cytoreduction surgery with intraperitoneal hyperthermic chemotherapy for disseminated peritoneal cancer of appendiceal origin. Ann Surg Oncol 2008;15: Hill AR, McQuellon RP, Russell GB, et al. Survival and Quality of Life Following Cytoreduction Surgery Plus Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Carcinomatosis of Colonic Origin. Ann Surg Oncol 2011;18: Schmidt U, Dahlke MH, Klempnauer J, et al. Perioperative morbidity and quality of life in longterm survivors following cytoreduction surgery and hyperthermic intraperitoneal chemotherapy. Eur J Surg Oncol 2005;31: Jess P, Iversen LH, Nielsen MB, et al. Quality of life after cytoreduction surgery plus early intraperitoneal postoperative chemotherapy for pseudomyxoma peritonei: a prospective study. Dis Colon Rectum 2008;51: Tuttle TM, Zhang Y, Greeno E, et al. Toxicity and quality of life after cytoreduction surgery plus hyperthermic intraperitoneal chemotherapy. Ann Surg Oncol 2006;13: Cite this article as: Zhu Y, Hanna N, Boutros C, Alexander HR Jr. Assessment of clinical benefit and quality of life in patients undergoing cytoreduction and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) for management of peritoneal metastases.. doi: /j.issn
Cytoreduction and hyperthermic intraperitoneal chemotherapy for the treatment of pseudomyxoma
 Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
Medical Policy Cytoreduction and Hyperthermic Intraperitoneal Chemotherapy for the Treatment of Pseudomyxoma Peritonei and Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal Mesothelioma
Peritoneal Surface Malignancies. Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA
 Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Peritoneal Surface Malignancies Ira Allen Jacobs, MD, FACS Surgical Oncology San Diego, CA Cancer dissemination routes Hematogenous metastases Lymphatic metastases Implants on peritoneal surfaces Surgically
Luis D. Carcorze Soto, MD PGY-3
 Luis D. Carcorze Soto, MD PGY-3 Peritoneal Surface Malignancies Peritoneum Patient Selection Operative Technique HIPEC EPIC Primary: Primary Peritoneal Carcinoma Malignant Peritoneal Mesothelioma Metastatic:
Luis D. Carcorze Soto, MD PGY-3 Peritoneal Surface Malignancies Peritoneum Patient Selection Operative Technique HIPEC EPIC Primary: Primary Peritoneal Carcinoma Malignant Peritoneal Mesothelioma Metastatic:
Comments: Policy Accepted during 2013 Annual Review with no changes.
 Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 09/18/2013 Title: Cytoreduction Surgery with Hyperthermic Intraperitoneal Chemotherapy Comments: Policy
Health Plan Coverage Policy ARBenefits Approval: 01/01/2012 Effective Date: 01/01/2012 Revision Date: 09/18/2013 Title: Cytoreduction Surgery with Hyperthermic Intraperitoneal Chemotherapy Comments: Policy
Intraoperative Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Volodymyr Labinskyy MD
 Intraoperative Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Volodymyr Labinskyy MD KCHC 8/29/13 52 y.o. F presented with severe pain in the right back and right flank, sharp, 8 out of 10, for 7 days.
Intraoperative Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Volodymyr Labinskyy MD KCHC 8/29/13 52 y.o. F presented with severe pain in the right back and right flank, sharp, 8 out of 10, for 7 days.
Laparoscopic Hyperthermic Intraperitoneal Chemotherapy: Indications, Aims, and Results: A Systematic Review of the Literature
 Ann Surg Oncol DOI 10.1245/s10434-012-2360-0 ORIGINAL ARTICLE REVIEW ARTICLE Laparoscopic Hyperthermic Intra Chemotherapy: Indications, Aims, and Results: A Systematic Review of the Literature Enrico Facchiano,
Ann Surg Oncol DOI 10.1245/s10434-012-2360-0 ORIGINAL ARTICLE REVIEW ARTICLE Laparoscopic Hyperthermic Intra Chemotherapy: Indications, Aims, and Results: A Systematic Review of the Literature Enrico Facchiano,
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAOPERATIVE HYPERTHERMIC INTRAPERITONEAL CHEMOTHERAPY (HIPEC)
 MEDICAL POLICY INTRAOPERATIVE HYPERTHERMIC INTRAPERITONEAL CHEMOTHERAPY (HIPEC) Policy Number: CS141.A Effective Date: September 1, 2015 Table of Contents COVERAGE RATIONALE DEFINITIONS... APPLICABLE CODES..
MEDICAL POLICY INTRAOPERATIVE HYPERTHERMIC INTRAPERITONEAL CHEMOTHERAPY (HIPEC) Policy Number: CS141.A Effective Date: September 1, 2015 Table of Contents COVERAGE RATIONALE DEFINITIONS... APPLICABLE CODES..
Chirurgia Avanzata Del Carcinoma Ovarico Nuove Strategie A Confronto Ovarian Cancer Advanced Surgery New Strategies in Comparison
 Peritoneal dissection and intraperitoneal chemotherapy under hyperthermic conditions. If you select the right patients long-term survival can be achieved. Chirurgia Avanzata Del Carcinoma Ovarico Nuove
Peritoneal dissection and intraperitoneal chemotherapy under hyperthermic conditions. If you select the right patients long-term survival can be achieved. Chirurgia Avanzata Del Carcinoma Ovarico Nuove
Rachel E. Kirby, Jing Zhao, Terence Chua, Winston Liauw and David L. Morris *
 Send Orders for Reprints to reprints@benthamscience.net The Open Surgical Oncology Journal, 2014, 5, 1-5 1 Open Access Avoidance of Early Post-Operative Intraperitoneal Chemotherapy (EPIC) Following Peritonectomy
Send Orders for Reprints to reprints@benthamscience.net The Open Surgical Oncology Journal, 2014, 5, 1-5 1 Open Access Avoidance of Early Post-Operative Intraperitoneal Chemotherapy (EPIC) Following Peritonectomy
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Now and the Future
 Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Now and the Future Mazin Al-kasspooles, MD Associate Professor of Surgery Division of Surgical Oncology Director, Regional Therapy
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy (HIPEC): Now and the Future Mazin Al-kasspooles, MD Associate Professor of Surgery Division of Surgical Oncology Director, Regional Therapy
Corporate Medical Policy
 Corporate Medical Policy Hyperthermic Intraperitoneal Chemotherapy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hyperthermic_intraperitoneal_chemotherapy 5/19/2005 3/2016 3/2017
Corporate Medical Policy Hyperthermic Intraperitoneal Chemotherapy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hyperthermic_intraperitoneal_chemotherapy 5/19/2005 3/2016 3/2017
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): July 22, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): July 22, 2014 Effective Date: October 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland School of Medicine Baltimore, Md
 Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
Major Advances in Cancer Prevention, Diagnosis and Treatment~ Why Mesothelioma Leads the Way H. Richard Alexander, Jr., M.D. Department of Surgery and The Greenebaum Cancer Center University of Maryland
A succesfull case of HIPEC in a peritoneal mesothelioma patient
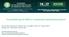 A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
A succesfull case of HIPEC in a peritoneal mesothelioma patient Firmino, NLJ¹²; Miranda, E¹³; Oliveira, DA ²; Lima, MBA ¹²; Diniz, AF ¹²; Gomes, GES ¹²; Azevedo, LW ¹²; Soares,MC¹²; Gomes, ASA³. ¹Pernambuco
Columbia University Mesothelioma Applied Research Foundation - 2009 - www.curemeso.org. Mesothelioma Center www.mesocenter.org
 Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
Columbia University Mesothelioma Center www.mesocenter.org Multimodal clinical trials, treatment (surgery, radiation, chemotherapy) Peritoneal mesothelioma program Immunotherapy translational, experimental
National Medical Policy
 National Medical Policy Subject: Policy Number: Intraperitoneal Hyperthermic Chemotherapy for Abdominopelvic Cancers NMP346 Effective Date*: June 2007 Updated: November 2014 This National Medical Policy
National Medical Policy Subject: Policy Number: Intraperitoneal Hyperthermic Chemotherapy for Abdominopelvic Cancers NMP346 Effective Date*: June 2007 Updated: November 2014 This National Medical Policy
Post-operative intrapleural chemotherapy for mesothelioma
 Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Post-operative intrapleural chemotherapy for mesothelioma Robert Kratzke, MD John Skoglund Chair for Lung Cancer Research Section of Heme-Onc-Transplant University of Minnesota Medical School Efficacy
Population Pharmacokinetics and Pharmacodynamics of Cisplatinum During Intraperitoneal Chemohyperthermia Using a Closed Abdominal Procedure
 Population Pharmacokinetics and Pharmacodynamics of Cisplatinum During Intraperitoneal Chemohyperthermia Using a Closed Abdominal Procedure Eddy Cotte, Brigitte Tranchand, Annie-Claude Beaujard, François-Noël
Population Pharmacokinetics and Pharmacodynamics of Cisplatinum During Intraperitoneal Chemohyperthermia Using a Closed Abdominal Procedure Eddy Cotte, Brigitte Tranchand, Annie-Claude Beaujard, François-Noël
Clinical Commissioning Policy: Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma
 Clinical Commissioning Policy: Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma Reference: NHS England B03/P/a 1 Information Reader Box (IRB) to be inserted
Clinical Commissioning Policy: Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma Reference: NHS England B03/P/a 1 Information Reader Box (IRB) to be inserted
Clinical Commissioning Policy: Cytoreductive surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma
 Clinical Commissioning Policy: Cytoreductive surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma Reference: NHS England A08/P/c 2 NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Cytoreductive surgery and Hyperthermic Intraperitoneal Chemotherapy for Peritoneal Mesothelioma Reference: NHS England A08/P/c 2 NHS England INFORMATION READER BOX Directorate
Activity of pemetrexed in thoracic malignancies
 Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Management of Peritoneal Metastases (PM) from colorectal cancers: New Perspectives. Dominique ELIAS
 Management of Peritoneal Metastases (PM) from colorectal cancers: New Perspectives Dominique ELIAS Declaration of interest BOARDS Congress and teaching 0 Merck 0 Ipsen Novartis Sanofi Trials The peritoneum
Management of Peritoneal Metastases (PM) from colorectal cancers: New Perspectives Dominique ELIAS Declaration of interest BOARDS Congress and teaching 0 Merck 0 Ipsen Novartis Sanofi Trials The peritoneum
Cytoreduction and Intraperitoneal Chemotherapy for the Management of Non-Gynecological Peritoneal Surface
 J. Exp. Clin. Cancer Res., 22, 4, 2003 - Supplement Cytoreduction and Intraperitoneal Chemotherapy for the Management of Non-Gynecological Peritoneal Surface Malignancy Yan T.D., Esquivel J., Carmignani
J. Exp. Clin. Cancer Res., 22, 4, 2003 - Supplement Cytoreduction and Intraperitoneal Chemotherapy for the Management of Non-Gynecological Peritoneal Surface Malignancy Yan T.D., Esquivel J., Carmignani
Peritoneal Carcinomatosis: Pathophysiology, Prevention, and Treatment
 Peritoneal Carcinomatosis: Pathophysiology, Prevention, and Treatment Wim Ceelen, MD, PhD, FACS GI Surgery, UZ Gent KAGB 27/4/2013 Overview What is peritoneal carcinomatosis? Rationale for IP drug delivery
Peritoneal Carcinomatosis: Pathophysiology, Prevention, and Treatment Wim Ceelen, MD, PhD, FACS GI Surgery, UZ Gent KAGB 27/4/2013 Overview What is peritoneal carcinomatosis? Rationale for IP drug delivery
Cigna Medical Coverage Policy
 Cigna Medical Coverage Policy Subject Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Table of Contents Coverage Policy... 1 General Background... 1 Coding/Billing Information... 8 References... 8 Effective
Cigna Medical Coverage Policy Subject Hyperthermic Intraperitoneal Chemotherapy (HIPEC) Table of Contents Coverage Policy... 1 General Background... 1 Coding/Billing Information... 8 References... 8 Effective
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
O. Glehen 1,2, E. Cotte 1,2, J. C. Lifante 1,2, C. Arvieux 2,3, N. Moles 1, C. Brigand 2,4, A. C. Beaujard 1,2, Y. François 1,2, F. N.
 Acta chir belg, 2006, 106, 285-290 Peritoneal Carcinomatosis in Digestive Cancers : Cytoreductive Surgery Combined with Intraperitoneal Chemohyperthermia. The Experience in Centre Hospitalier et Universitaire
Acta chir belg, 2006, 106, 285-290 Peritoneal Carcinomatosis in Digestive Cancers : Cytoreductive Surgery Combined with Intraperitoneal Chemohyperthermia. The Experience in Centre Hospitalier et Universitaire
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Scottish Medicines Consortium
 Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Scottish Medicines Consortium pemetrexed 500mg infusion (Alimta ) No. (192/05) Eli Lilly 8 July 2005 The Scottish Medicines Consortium has completed its assessment of the above product and advises NHS
Peritoneal Carcinosis
 Peritoneal Carcinosis What is it and how to cure it Peritoneum Peritoneum is a thin and transparent membrane that covers the internal part of the abdominal and pelvic cavity and all the viscera contained
Peritoneal Carcinosis What is it and how to cure it Peritoneum Peritoneum is a thin and transparent membrane that covers the internal part of the abdominal and pelvic cavity and all the viscera contained
Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases
 I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma
 The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
J Clin Oncol 27:6237-6242. 2009 by American Society of Clinical Oncology INTRODUCTION
 VOLUME 27 NUMBER 36 DECEMBER 20 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Malignant Peritoneal Mesothelioma:
VOLUME 27 NUMBER 36 DECEMBER 20 2009 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Malignant Peritoneal Mesothelioma:
PRODYNOV. Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI. Image Assisted Laser Therapy for Oncology
 PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
PRODYNOV Targeted Photodynamic Therapy of Ovarian Peritoneal Carcinomatosis ONCO-THAI Image Assisted Laser Therapy for Oncology Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Gastrointestinal Oncology Peritoneal Mesothelioma
 Gastrointestinal Oncology Two Decades of Progress in the Management of a Rare Disease Paul H Sugarbaker, MD, FACS, FRCS Medical Director, Center for Gastrointestinal Malignancies, MedStar Washington Hospital
Gastrointestinal Oncology Two Decades of Progress in the Management of a Rare Disease Paul H Sugarbaker, MD, FACS, FRCS Medical Director, Center for Gastrointestinal Malignancies, MedStar Washington Hospital
Cytoreductive Surgery (CRS) and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) for Peritoneal Mesothelioma
 Original Article 291 Cytoreductive Surgery (CRS) and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) for Peritoneal Mesothelioma Grace HC Tan, 1 MBBS (London), MRCS (Edinburgh), Michelle Cheung, 1 MBBCh
Original Article 291 Cytoreductive Surgery (CRS) and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) for Peritoneal Mesothelioma Grace HC Tan, 1 MBBS (London), MRCS (Edinburgh), Michelle Cheung, 1 MBBCh
IN MANY PATIENTS WITH ABDOMINAL OR PELVIC MALIGNANCIES, surgical treatment
 Sugarbaker, Cancerología 3 (2008): 119-124 1 Washington Cancer Institute, Washington, DC, USA Overview of Peritoneal Carcinomatosis Paul H. Sugarbaker 1 Abstract IN MANY PATIENTS WITH ABDOMINAL OR PELVIC
Sugarbaker, Cancerología 3 (2008): 119-124 1 Washington Cancer Institute, Washington, DC, USA Overview of Peritoneal Carcinomatosis Paul H. Sugarbaker 1 Abstract IN MANY PATIENTS WITH ABDOMINAL OR PELVIC
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality. Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006
 The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
Cytoreductive surgery and perioperative intraperitoneal chemotherapy for peritoneal carcinomatosis in the elderly
 Huang et al. World Journal of Surgical Oncology (2015) 13:262 DOI 10.1186/s12957-015-0682-7 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Cytoreductive surgery and perioperative intraperitoneal chemotherapy
Huang et al. World Journal of Surgical Oncology (2015) 13:262 DOI 10.1186/s12957-015-0682-7 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Cytoreductive surgery and perioperative intraperitoneal chemotherapy
Protocol. Cytoreductive Surgery and Perioperative Intraperitoneal Chemotherapy for Select Intra-Abdominal and Pelvic Malignancies
 Chemotherapy for Select Intra-Abdominal and Pelvic Malignancies (20307) (Formerly Chemotherapy for the Treatment of Pseudomyxoma Peritonei, Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal
Chemotherapy for Select Intra-Abdominal and Pelvic Malignancies (20307) (Formerly Chemotherapy for the Treatment of Pseudomyxoma Peritonei, Peritoneal Carcinomatosis of Gastrointestinal Origin, and Peritoneal
Ching-Yao Yang, Yu-Wen Tien
 Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Ching-Yao Yang, Yu-Wen Tien Division of General Surgery, Department of Surgery, National Taiwan University Hospital Oct-30-2010 Pancreatic NET have poorer prognosis when presence of liver metastases at
Avastin: Glossary of key terms
 Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Avastin: Glossary of key terms Adenocarcinoma Adenoma Adjuvant therapy Angiogenesis Anti-angiogenics Antibody Antigen Avastin (bevacizumab) Benign A form of carcinoma that originates in glandular tissue.
Selection of patients and staging of peritoneal surface malignancies
 Online Submissions: http://www.wjgnet.com/1948-5204office wjgo@wjgnet.com doi:10.4251/wjgo.v2.i1.31 World J Gastrointest Oncol 2010 January 15; 2(1): 31-35 ISSN 1948-5204 (online) 2010 Baishideng. All
Online Submissions: http://www.wjgnet.com/1948-5204office wjgo@wjgnet.com doi:10.4251/wjgo.v2.i1.31 World J Gastrointest Oncol 2010 January 15; 2(1): 31-35 ISSN 1948-5204 (online) 2010 Baishideng. All
New strategies in anticancer therapy
 癌 症 診 療 指 引 簡 介 及 臨 床 應 用 New strategies in anticancer therapy 中 山 醫 學 大 學 附 設 醫 院 腫 瘤 內 科 蔡 明 宏 醫 師 2014/3/29 Anti-Cancer Therapy Surgical Treatment Radiotherapy Chemotherapy Target Therapy Supportive
癌 症 診 療 指 引 簡 介 及 臨 床 應 用 New strategies in anticancer therapy 中 山 醫 學 大 學 附 設 醫 院 腫 瘤 內 科 蔡 明 宏 醫 師 2014/3/29 Anti-Cancer Therapy Surgical Treatment Radiotherapy Chemotherapy Target Therapy Supportive
Pseudomyxoma Peritonei Where are we in 2014?
 Pseudomyxoma Peritonei Where are we in 2014? Santiago González-Moreno, MD, PhD Head, Department of GI Surgical Oncology Peritoneal Surface Oncology Program Medical Director * * * * * * * * * * * * French
Pseudomyxoma Peritonei Where are we in 2014? Santiago González-Moreno, MD, PhD Head, Department of GI Surgical Oncology Peritoneal Surface Oncology Program Medical Director * * * * * * * * * * * * French
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
MALIGNANT MESOTHELIOMA: A TYPICAL PRESENTATION IN AN ATYPICAL PATIENT
 MALIGNANT MESOTHELIOMA: A TYPICAL PRESENTATION IN AN ATYPICAL PATIENT Written by: Karyn Varley MS, SCT(ASCP) The donating laboratory would like to remain anonymous. PATIENT HISTORY 28 year old female Lived
MALIGNANT MESOTHELIOMA: A TYPICAL PRESENTATION IN AN ATYPICAL PATIENT Written by: Karyn Varley MS, SCT(ASCP) The donating laboratory would like to remain anonymous. PATIENT HISTORY 28 year old female Lived
J of Evidence Based Med & Hlthcare, pissn- 2349-2562, eissn- 2349-2570/ Vol. 2/Issue 33/Aug. 17, 2015 Page 5063
 PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
PERITONEAL MALIGNANT MESOTHELIOMA: A RARE S. R. Dhamotharan 1, S. Shanthi Nirmala 2, F. Celine Foustina Mary 3, M. Arul Raj Kumar 4, R. Vinothprabhu 5 HOW TO CITE THIS ARTICLE: S. R. Dhamotharan, S. Shanthi
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Colorectal cancer. A guide for journalists on colorectal cancer and its treatment
 Colorectal cancer A guide for journalists on colorectal cancer and its treatment Contents Contents 2 3 Section 1: Colorectal cancer 4 i. What is colorectal cancer? 4 ii. Causes and risk factors 4 iii.
Colorectal cancer A guide for journalists on colorectal cancer and its treatment Contents Contents 2 3 Section 1: Colorectal cancer 4 i. What is colorectal cancer? 4 ii. Causes and risk factors 4 iii.
January 2013 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW. Summary. Contents
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Paclitaxel albumin (Abraxane ) as a substitute for docetaxel/paclitaxel for cancer Paclitaxel albumin (Abraxane ) as a substitute for docetaxel/ paclitaxel for
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Paclitaxel albumin (Abraxane ) as a substitute for docetaxel/paclitaxel for cancer Paclitaxel albumin (Abraxane ) as a substitute for docetaxel/ paclitaxel for
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases.
 Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
Metastatic Renal Cell Carcinoma: Staging and Prognosis of Three Separate Cases. Abstract This paper describes the staging, imaging, treatment, and prognosis of renal cell carcinoma. Three case studies
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Oncologist. The. Clinical Pharmacology. Update on Chemotherapeutic Agents Utilized for Perioperative Intraperitoneal Chemotherapy
 The Oncologist Clinical Pharmacology Update on Chemotherapeutic Agents Utilized for Perioperative Intraperitoneal Chemotherapy PAUL H. SUGARBAKER, a JORGE TORRES MORA, b PABLO CARMIGNANI, a O. ANTHONY
The Oncologist Clinical Pharmacology Update on Chemotherapeutic Agents Utilized for Perioperative Intraperitoneal Chemotherapy PAUL H. SUGARBAKER, a JORGE TORRES MORA, b PABLO CARMIGNANI, a O. ANTHONY
Surgical Staging of Endometrial Cancer
 Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
Surgical Staging of Endometrial Cancer I. Endometrial Cancer Surgical Staging Overview Uterine cancer types: carcinomas type I and type II, sarcomas, carcinosarcomas Hysterectomy with BSO Surgical Staging
MesoPDT. Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI. Image Assisted Laser Therapy for Oncology
 MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
MesoPDT Photodynamic Therapy for malignant pleural mesothelioma ONCO-THAI Image Assisted Laser Therapy for Oncology Unité Inserm ONCO-THAI «Image Assisted Laser Therapy for Oncology» Inserm ONCO-THAI "Image
Avastin in Metastatic Breast Cancer
 Non-interventional study Avastin in Metastatic Breast Cancer ML 21165 / 2007 Clinical Study Report Synopsis ROCHE ML21165 / WiSP Project RH09 / V. 1.0 / 24.06.2013 ROCHE ML21165-2 - Name of Sponsor Roche
Non-interventional study Avastin in Metastatic Breast Cancer ML 21165 / 2007 Clinical Study Report Synopsis ROCHE ML21165 / WiSP Project RH09 / V. 1.0 / 24.06.2013 ROCHE ML21165-2 - Name of Sponsor Roche
MR Imaging of Peritoneal Malignancy Russell N. Low, MD
 MR Imaging of Peritoneal Malignancy Russell N. Low, MD From: Sharp and Children's MRI Center and Sharp HealthCare, 7901 Frost Street, San Diego, California, 92123. Phone: (858) 939-3600. Email: rlow@ucsd.edu
MR Imaging of Peritoneal Malignancy Russell N. Low, MD From: Sharp and Children's MRI Center and Sharp HealthCare, 7901 Frost Street, San Diego, California, 92123. Phone: (858) 939-3600. Email: rlow@ucsd.edu
Omental mesothelioma as a diagnostic and therapeutic challenge: A case report
 www.edoriumjournals.com Case in Images OPEN ACCESS Omental mesothelioma as a diagnostic and therapeutic challenge: A case report Cihan Akgul Ozmen, Yekta Tuzun, Hatice Ozturkmen Akay, Hasan Nazaroglu ABSTRACT
www.edoriumjournals.com Case in Images OPEN ACCESS Omental mesothelioma as a diagnostic and therapeutic challenge: A case report Cihan Akgul Ozmen, Yekta Tuzun, Hatice Ozturkmen Akay, Hasan Nazaroglu ABSTRACT
Report on New Patented Drugs - Alimta
 Report on New Patented Drugs - Alimta Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the PMPRB s Excessive
Report on New Patented Drugs - Alimta Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the PMPRB s Excessive
Hospital: IRB #: Principal Phone Fax Email Investigator: Dr. A. Co-investigators: Dr. C Dr. D Dr. E Dr. F
 Title: Protocol for the Implementation of Treatment of Patients with Peritoneal Surface Malignancy with Hyperthermic Intraoperative Intraperitoneal Chemotherapy and Normothermic Early Postoperative Intraperitoneal
Title: Protocol for the Implementation of Treatment of Patients with Peritoneal Surface Malignancy with Hyperthermic Intraoperative Intraperitoneal Chemotherapy and Normothermic Early Postoperative Intraperitoneal
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Evidence-Based Medicine in the Treatment of Peritoneal Carcinomatosis: Past, Present, and Future
 2009;100:335 344 Evidence-Based Medicine in the Treatment of Peritoneal Carcinomatosis: Past, Present, and Future AVIRAM NISSAN, MD, 1,2 * ALEXANDER STOJADINOVIC, MD, 3,4 ALFREDO GAROFALO, MD, 5{ JESUS
2009;100:335 344 Evidence-Based Medicine in the Treatment of Peritoneal Carcinomatosis: Past, Present, and Future AVIRAM NISSAN, MD, 1,2 * ALEXANDER STOJADINOVIC, MD, 3,4 ALFREDO GAROFALO, MD, 5{ JESUS
Clinical Policy Bulletin: Hyperthermia in Cancer Therapy
 Hyperthermia in Cancer Therapy Page 1 of 28 Aetna Better Health 2000 Market Street, Suite 850 Philadelphia, PA 19103 AETNA BETTER HEALTH Clinical Policy Bulletin: Hyperthermia in Cancer Therapy Number:
Hyperthermia in Cancer Therapy Page 1 of 28 Aetna Better Health 2000 Market Street, Suite 850 Philadelphia, PA 19103 AETNA BETTER HEALTH Clinical Policy Bulletin: Hyperthermia in Cancer Therapy Number:
Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment.
 1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT
 1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
Advances In Chemotherapy For Hormone Refractory Prostate Cancer. TAX 327 study results & SWOG 99-16 study results presented at ASCO 2004
 Ronald de Wit Rotterdam Cancer Institute The Netherlands Advances In Chemotherapy For Hormone Refractory Prostate Cancer TAX 327 study results & SWOG 99-16 study results presented at Slide 1 Prostate Cancer
Ronald de Wit Rotterdam Cancer Institute The Netherlands Advances In Chemotherapy For Hormone Refractory Prostate Cancer TAX 327 study results & SWOG 99-16 study results presented at Slide 1 Prostate Cancer
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES.
 PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
POLICY A. INDICATIONS
 Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
Alimta (pemetrexed) Line(s) of Business: HMO; PPO; QUEST Integration Akamai Advantage Original Effective Date: 09/01/2007 Current Effective Date: 10/01/2015 POLICY A. INDICATIONS The indications below
COMMISSIONING. for ULTRA-RADICAL SURGERY ADVANCED OVARIAN CANCER
 COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
COMMISSIONING for ULTRA-RADICAL SURGERY in ADVANCED OVARIAN CANCER WHY THIS MUST HAPPEN PERSPECTIVE COMMISSIONING FOR WHO, FOR WHAT? Biological Basis Surgical Basis International and national standards
Clinical Trial Design. Sponsored by Center for Cancer Research National Cancer Institute
 Clinical Trial Design Sponsored by Center for Cancer Research National Cancer Institute Overview Clinical research is research conducted on human beings (or on material of human origin such as tissues,
Clinical Trial Design Sponsored by Center for Cancer Research National Cancer Institute Overview Clinical research is research conducted on human beings (or on material of human origin such as tissues,
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
the standard of care 2009 5/1/2009 Mesothelioma: The standard of care take home messages PILC 2006 Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009
 Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Primary Care Management of Colorectal Cancer
 Primary Care Management of Colorectal Cancer Dr. Dan Renouf, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Primary Care Management of Colorectal Cancer Survivors Daniel
Primary Care Management of Colorectal Cancer Dr. Dan Renouf, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Primary Care Management of Colorectal Cancer Survivors Daniel
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
MEDICAL POLICY SUBJECT: HYPERTHERMIA AS A CANCER TREATMENT. POLICY NUMBER: 2.01.25 CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: HYPERTHERMIA AS A CANCER PAGE: 1 OF: 7 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: HYPERTHERMIA AS A CANCER PAGE: 1 OF: 7 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Multicystic Peritoneal Mesothelioma Treated by Surgical Cytoreduction and Hyperthermic Intra-peritoneal Chemotherapy (HIPEC)
 Multicystic Peritoneal Mesothelioma Treated by Surgical Cytoreduction and Hyperthermic Intra-peritoneal Chemotherapy (HIPEC) D. BARATTI 1, S. KUSAMURA 1, A. SIRONI 2, A. CABRAS 3, L. FUMAGALLI 4, B. LATERZA
Multicystic Peritoneal Mesothelioma Treated by Surgical Cytoreduction and Hyperthermic Intra-peritoneal Chemotherapy (HIPEC) D. BARATTI 1, S. KUSAMURA 1, A. SIRONI 2, A. CABRAS 3, L. FUMAGALLI 4, B. LATERZA
Clinical Management Guideline Management of locally advanced or recurrent Renal cell carcinoma. Protocol for Planning and Treatment
 Protocol for Planning and Treatment The process to be followed in the management of: LOCALLY ADVANCED OR METASTATIC RENAL CELL CARCINOMA Patient information given at each stage following agreed information
Protocol for Planning and Treatment The process to be followed in the management of: LOCALLY ADVANCED OR METASTATIC RENAL CELL CARCINOMA Patient information given at each stage following agreed information
Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer
 Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer David Josephson, MD FACS Fellowship Director, Urologic Oncology and Robotic Surgery Program Staging Most important in risk assessment and
Treatment and Surveillance of Non- Muscle Invasive Bladder Cancer David Josephson, MD FACS Fellowship Director, Urologic Oncology and Robotic Surgery Program Staging Most important in risk assessment and
Evidence tabel Lokaal palliatieve behandelingen
 Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
Auteurs, jaartal Mate van bewijs Studie type Follow-up Populatie (incl. steekproef-grootte) Patienten kenmerken Interventie Controle Resultaten Conclusie Opmerkingen, commentaar Hartgrink, 2002 The Netherlands
INTRODUCTION. Abstract Background. 3 Centre hospitalier Lyon Sud Hospices Civils de Lyon, Pierre-Bé
 Childbearing after hyperthermic intraperitoneal chemotherapy: results from an international survey Pablo Ortega-Deballon 1 2 *, Olivier Glehen 3, Edward Levine 4, Pompiliu Piso, Paul H. Sugarbaker 6, Andrea
Childbearing after hyperthermic intraperitoneal chemotherapy: results from an international survey Pablo Ortega-Deballon 1 2 *, Olivier Glehen 3, Edward Levine 4, Pompiliu Piso, Paul H. Sugarbaker 6, Andrea
2nd International Symposium on Pressurized IntraPeritoneal Aerosol Chemotherapy (PIPAC)
 2nd International Symposium on Pressurized IntraPeritoneal Aerosol Chemotherapy (PIPAC) Wednesday Oct 7th, 2015 Congress Center (Hörsaal 1 3) Marien Hospital Herne Accreditation by the Medical Chamber
2nd International Symposium on Pressurized IntraPeritoneal Aerosol Chemotherapy (PIPAC) Wednesday Oct 7th, 2015 Congress Center (Hörsaal 1 3) Marien Hospital Herne Accreditation by the Medical Chamber
Tricia Cox on 7/18/2012 at Oncology Center. Sarah Randolf. Female
 SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Carcinoma of the vagina is a relatively uncommon disease, affecting only about 2,000 women in
 EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition, 2001 Vagina Jeffrey L. Stern, MD Carcinoma of the vagina is
EVERYONE S GUIDE FOR CANCER THERAPY Malin Dollinger, MD, Ernest H. Rosenbaum, MD, Margaret Tempero, MD, and Sean Mulvihill, MD 4 th Edition, 2001 Vagina Jeffrey L. Stern, MD Carcinoma of the vagina is
Peritoneal Mesothelioma: The Columbia Experience
 48 Peritoneal Mesothelioma: The Columbia Experience Jennifer A. Wagmiller, Mary-Louise Keohan, John A. Chabot, Karen Fountain, Mary Hesdorffer, and Robert N. Taub Malignant peritoneal mesothelioma is a
48 Peritoneal Mesothelioma: The Columbia Experience Jennifer A. Wagmiller, Mary-Louise Keohan, John A. Chabot, Karen Fountain, Mary Hesdorffer, and Robert N. Taub Malignant peritoneal mesothelioma is a
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
How To Treat Lung Cancer At Cleveland Clinic
 Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Treatment Guide Lung Cancer Management The Chest Cancer Center at Cleveland Clinic, which includes specialists from the Respiratory Institute, Taussig Cancer Institute and Miller Family Heart & Vascular
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer
 Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer Review Article [1] December 01, 2003 By George W. Sledge, Jr, MD [2] Gemcitabine (Gemzar) and paclitaxel show good activity as single
Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer Review Article [1] December 01, 2003 By George W. Sledge, Jr, MD [2] Gemcitabine (Gemzar) and paclitaxel show good activity as single
Malignant pleural mesothelioma P/D vs. EPP
 3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
3 rd International Thoracic Oncology Congress Dresden, September 13 15, 2012 Malignant pleural mesothelioma P/D vs. EPP Walter Weder, MD Professor of Surgery Dokumentenname Datum Seite 1 Extrapleural Pneumonectomy
