trust clinical guideline
|
|
|
- Stephen Woods
- 10 years ago
- Views:
Transcription
1 CG25 VERSION 1.0 1/20 Guideline ID CG25 Version 1.0 Title Approved by Urinary Catheterisation Clinical Effectiveness Group Date Issued 01/10/2014 Review Date 31/09/2017 Directorate Authorised Staff Medical Ambulance Care Assistant Emergency Care Assistant Student Paramedic Advanced Technician Paramedic (non-ecp) Nurse (non-ecp) ECP Doctor Clinical Publication Category Guidance (Green) - Deviation permissible; Apply clinical judgement 1. Introduction 1.1 Urinary Catheterisation is defined as the passage of a catheter into the urinary bladder. A catheter is a thin hollow flexible tube which can be inserted in the bladder either through the urethra (urethral) or suprapubic channel to drain the urine. 1.2 Catheterisation is a core skill for Emergency Care Practitioners. However, as the provision of catheterisation is normally well managed within primary care, only those ECP localities with an identified need shall be deemed to require this skill. 2. Indications 2.1 Primary catheterisation is now supported by the Trust where the individual ECP skill set and competencies allow. 2.2 Urethral re-catheterisation is indicated for those patients in acute urinary retention whose catheter is currently blocked.
2 CG25 VERSION 1.0 2/20 3. Competence 3.1 All ECPs who are required to catheterise must achieve and maintain clinical competence in urinary catheterisation. Initial training and sign off may be achieved through the use of training aids. 3.2 Competence to undertake primary catheterisation for male patients in retention should also be maintained for those ECPs who undertake catheterisation as a regular feature of their clinical workload. 4. Assessment of Acute Retention Requiring Primary Intervention 4.1 Classically, acute urinary retention affects men with prostatic hypertrophy (enlarged prostate). When obstruction occurs the patient will experience pain and may become agitated. Inserting a urinary catheter into the bladder will generally relieve the symptoms. 4.2 History taking will aid diagnosis of the type of retention: Acute retention is defined by sudden inability to void with a tender, palpable bladder. Chronic retention is long standing incomplete bladder emptying with an over-distended, non-tender bladder and very large residual, with possible renal impairment. Acute chronic retention is the sudden inability to void, with a background of chronic retention and possible overflow or night-time incontinence. 4.3 Detailed abdominal assessment must be undertaken prior to primary insertion, which must also cover: Check blood pressure as a possible indicator of renal impairment. Abdominal and genitourinary examination. Patients with significant urinary retention should have a palpable enlarged bladder, which will usually be non-tender. Check for enlargement of kidneys, via bimanual palpation. Examine external genitalia to seek evidence of urethral abnormalities causing urinary flow obstruction, e.g. urethral stricture, phimosis or meatal stenosis. Neurological examination should exclude cord compression and look for evidence of other relevant neurological conditions.
3 CG25 VERSION 1.0 3/ Where available consider onward referral and engagement with urology nurses and District Nurses for consideration of catheter care, particularly over the out of hours period. Those patients with suspected chronic or acute exacerbation of chronic retention of urine will need admission to hospital (for close fluid balance monitoring, fluid replacement and investigations). All uncomplicated patients should be referred back to their GP for determination of the cause of retention and consideration of definitive management. 4.5 If after primary catheterisation the residual volume drained initially exceeds 1200mls, then a follow up visit must be arranged in two to four hours. If at this revisit there is evidence of a urinary output of 200mls per hour or more then there is severe risk of dehydration and potentially fatal hypovolaemia. If due to service demands a revisit is impossible then a referral to another health care provider is essential i.e. GP, out of hours clinician or community nursing. If this cannot be arranged, then the patient must be referred to secondary care. A telephone call to the patient could be indicative but must not replace verification 4.6 Initial drainage of the residual volume depends on catheter size: 12ch = Approximately 1 hour 14ch = Approximately 20 minutes 16ch = Approximately 6-7 minutes 5. Catheters 5.1 When consideration is given to the type of catheter used for re-catheterisation following assessment and determination of acute urinary retention, the choice should be based on the patient s current catheter. Where possible the patient s own supplies should be used. 5.2 Silicone The silicone catheter (100% silicone) is very gentle for the tissue and is hypoallergenic. Because it is uncoated it has a relatively large lumen and has a reduced tendency for encrustation. While silicone causes less tissue irritation and potential damage, the catheter balloon has a tendency to lose fluid which increases the risk of displacement. Silicone catheters also have a greater risk for developing a cuff when deflated, which can result in uncomfortable catheter removal or urethral trauma.
4 CG25 VERSION 1.0 4/ A Cochrane review from 2007 did not find sufficient evidence to determine the best type of indwelling urinary catheter for long-term bladder drainage in adults. However, silicone catheters might be preferable to other catheter materials to reduce the risk of encrustation in long-term catheterised patients. 5.3 Hydrogel-coated Hydrogel coated catheters are soft and highly biocompatible. Because they are hydrophilic, they absorb fluid to form a soft cushion around the catheter, and reduce friction and urethral irritations. 5.4 Silicone-coated/Silicone Elastomer-coated Silicone elastomer coated catheters are latex catheters coated inside and out with silicone. The catheter has the strength and flexibility of latex and the durability and reduced encrustation typical of 100% silicone catheters. 5.5 Silver-coated Catheter One type of coating combines a thin layer of silver alloy with hydrogel which is antiseptic. Silver-hydrogel coated catheters are available in latex and silicone. Silver alloy coated catheters significantly reduce the incidence of asymptomatic bacteriuria, but only for less than a week. There is some evidence of reduced risk in the case of symptomatic UTIs. Therefore, they may be useful in some settings. Another type, silver oxide coated catheters are not associated with a statistically significant reduction in bacteriuria. 5.6 PTFE (Polytetrafluoroethylene) PTFE-coated latex catheters or Teflon has been developed to protect the urethra against latex. The absorption of water is reduced due to the Teflon coating. It is smoother than plain latex, which helps to prevent encrustation and irritation. Do not use this catheter for patients who are sensitive to latex. 5.7 Latex Latex, made from natural rubber is a flexible material but it has some disadvantages. Because of the potential discomfort due to high surface friction, vulnerability to rapid encrustation by mineral deposits from the urine and the implication of latex allergic reactions in the development of urethritis and urethral stricture or anaphylaxis, the use of latex catheters is restricted to short-term indwelling catheterisation and should be avoided if possible.
5 CG25 VERSION 1.0 5/ Catheter Gauge Foley catheters are sized in Charrieres, also known as French Grade (FG): 1 Ch = 1/3 mm diameter. Selection of the right catheter size will increase patient comfort and allow adequate drainage (a 12 Ch catheter has a drainage capacity of 100 litres in 24 hours) The smallest size of catheter allowing drainage should be used, as larger gauges are more likely to cause trauma and mucosal irritation. However, where there is infection or postoperative bleeding, a larger bore minimises the risk of obstruction Catheters sizes are labelled using the colour code below. The following provides an approximate guide to which size of catheter to insert in specific circumstances: Catheterisation (female), with clear urine, containing no grit (encrustation), debris or haematuria Ch/3.3-4mm. Catheterisation (male), with clear urine, containing no grit, debris or haematuria Ch/4-4.7mm. Male and female with debris or mild haematuria 16 ch/5.3mm Length The standard male catheter length of cm can be used for males and females, but a shorter female length of 25 cm can be more comfortable and discrete for some women. However, a female catheter can be too short if the woman is severely obese and then a male size is preferred. The female length catheter must not be used for males as inflation of the balloon within the urethra can result in severe trauma.
6 CG25 VERSION 1.0 6/ Closed Drainage System When the catheter has been inserted using aseptic technique, it is directly connected to the sterile bag, because an aseptic closed drainage system minimises the risk of catheter associated urinary tract infections (CAUTI). Unnecessary disconnection of a closed drainage system should be avoided, but if it occurs the catheter and collecting system have to be replaced using aseptic technique and sterile equipment. There are several different bags available. Selection of the bag depends on whether it is for short-term drainage or for long-term use, taking into consideration the patient s mobility, cognitive function, daily life routine. Leg bags can be used for 5-7 days before needing changing, unless single use only, night bags used in the community should be single use only Leg Bag/Body Worn Bag If the patient is mobile a leg bag can be preferable. The leg bags allow maximum freedom and movement and can be concealed beneath the clothes. Leg bags are available in different sizes, designs and qualities and it is important to select a bag according to the patient s preference, mobility and the intended duration The following factors must be considered when selecting a bag: Capacity: Ranges from 120 to 800 ml and the size depends on how often the bag has to be emptied according to the patient s daily routines. Chamber: Bags are available with a single or several chambers. Several chambers flatten the bags profile and are therefore more discreet. Materials: Bags are produced in different materials with different backings for comfort. Some of the bags are PVC-free as well. Tube: Range from about 4 cm to 45 cm. Some can be cut to length. In addition some tubes are kinking-free, which reduces the risk for obstruction. Suspension System: Leg bags can be attached to the leg with straps (elasticated), nets, bags/pocket of cotton, etc Overnight Bedside Bag Patients normally require a 2 litre drainage bag that is connected to the leg bag at night or if they are immobile or bedbound. The outlet tap on the leg bag is left open so that the urine collects in the larger bag without breaking the closed drainage system. The night bag requires a stand for support, to reduce the risk of dislodging the link system and is available in different designs and materials.
7 CG25 VERSION 1.0 7/ Catheter Valves Valves are small devices connected to the catheter outlet instead of a bag and are available in a variety of designs. These are only suitable for patients with the dexterity and cognitive ability to open the valve 5 6 times/day; they are not suitable for patients with chronic retention or renal impairment. 6. Preparation 6.1 Consent Catheterisation is an invasive procedure that can cause embarrassment, physical and psychological discomfort and impact on the patient s self-image. To ensure the patient is fully prepared for catheterisation it is the responsibility of the clinician to inform the patient of the reasons and necessity for the procedure, and obtain the patient s permission. It is a necessity that verbal consent and agreement is reached and the relevant information is recorded in the patient s clinical records. Informed consent requires the patient to understand the reason for catheterisation, possible complications and what is required to manage the catheter. 6.2 Information and Support Explaining the procedure to the patient can help reduce patient anxiety and embarrassment and help the patient to report any problems that may occur while the catheter is in-situ. Relaxing the patient by offering reassurance and support will help for smoother insertion of the catheter and assist in avoiding unnecessary discomfort and the potential of urethral trauma during the insertion. 6.3 Equipment and Preparation The clinician should take a brief medical patient history, especially about urological conditions before the procedure. Catheterisation is a sterile procedure as it involves instrumentation of a sterile tract. It is imperative that the clinician has a good understanding of the principles of the aseptic procedure as this will help to reduce the risk of UTI.
8 CG25 VERSION 1.0 8/ Lubricating Gel Catheterisation can be painful in both males and females. The use of anaesthetic lubricating gels is well recognised for male catheterisation. An appropriate sterile single-use syringe with lubricant should be used before catheter insertion of a non-lubricated catheter to minimise urethral trauma, discomfort and infection. However, it is essential to ask the patient if they have any sensitivity to lignocaine/lidocaine, chlorhexidine or latex before commencing the procedure. There have been reported cases of anaphylaxis attributed to the chlorhexidine component in lubricating gel. Ten to fifteen ml of the gel is instilled directly into the urethra, until this volume reaches the sphincter/bladder neck region. Blandy and Colley recommend a 3 to 5 minute gap before starting the catheterisation after instilling the gel, but it is important to follow manufacturer s guidance A maximised anaesthetic effect will help the patient to relax and the insertion of the catheter should be easier if the lubricant contains lignocaine/lidocaine or chlorhexidine. Care should be taken if the patient has an open wound, severe damaged mucous membranes or infections in the regions where the lubricant will be used. Caution is advised in patients with severe disorders of the impulse conduction system or epilepsy as well as women in the first three months of pregnancy or breast feeding, prior using a lignocaine/lidocaine containing lubricant. 7. Procedures 7.1 Removal of a Urethral Catheter Equipment Checklist: Non-sterile Disposable gloves. Syringe for deflating balloon. Disposable pad (to protect bed). Plastic disposable apron or protective clothing. Gauze swabs disposable wipes.
9 CG25 VERSION 1.0 9/ Procedure Action 1. Explain procedure to patient. 2. Check volume of water in balloon (refer to patient documentation if available). 3. Attach the syringe to catheter valve to deflate the balloon. Do not use suction on the syringe but allow the solution to come back spontaneously. 4. Ask patient to breathe in and then out: as patient exhales, gently remove the catheter. Male patients should be warned of discomfort as the deflated balloon passes through the prostatic urethra. 5. Clean meatus using gauze / disposable wipe, clear away equipment, and make the patient comfortable. 6. Used equipment should be placed in a clinical waste bag and disposed of in line with Trust policy. 7.2 Male Urethral Catheterisation Equipment Checklist: Sterile catheterisation pack containing gallipots, receiver, low-linting swabs, disposable towels. Disposable pad for bed protection. 2 pairs of sterile gloves, in order to maintain asepsis. Selection of appropriate catheters; it is advisable to take a spare catheter in addition to the one you want, and one of a different/smaller size. Sterile anaesthetic lubricating jelly (1-2 tubes). Universal specimen container, if required. Cleansing solution. Bactericidal alcohol hand disinfection. 10ml sterile water (inflation of balloon) or as recommended by the manufacturer. Syringe and needle to draw up sterile water and inflate balloon Disposable plastic apron/protective clothing. A closed urinary drainage system, e.g. a night bag, leg bag or catheter valve. A catheter drainage bag stand, if required Procedure Action and Rationale 1. Check patient file/history for past problems, allergies etc. 2. Before the procedure explain the process to the patient, to ensure that they are able to give informed consent. 3. Undertake procedure on the patient s bed or in clinical treatment area using screens/curtains to promote and maintain dignity.
10 CG25 VERSION /20 4. Assist the patient to get into the supine position to ensure the penis is accessible. Do not expose the patient at this stage of the procedure. 5. Wash hands using soap and water or bactericidal alcohol hand rub to reduce risk of infection. 6. Place all equipment required on a clean working surface. 7. Open the outer cover of the catheterisation pack then open the sterile field, handling the outer corners only. Using aseptic non-touch technique open/place all other equipment onto sterile field. 8. Remove cover that is maintaining the patient s privacy and position a disposable pad under the patient s buttocks and thighs, to ensure urine does not leak onto bed. 9. Clean hands again with a bactericidal alcohol hand rub, as they may have become contaminated by handling the outer packs. Put on first pair sterile gloves. 10. Using an aseptic technique, connect the bag to the catheter at this stage. 11. Place dressing/protective towel across the patient s thighs and under penis. To create a protective sterile field. 12. Lift the penis and if present, retract the foreskin, using a gauze swab. Clean the glans penis with the solution. Beginning with the foreskin, the glans and urethral meatus at the end, using a new swab for each part. 13. Still with the first pair of sterile gloves on, hold the penis in an upright position (to straighten out the penile urethra and facilitate catheterisation). Slowly instill ml of the (anaesthetic) lubricating gel into the urethra holding firmly below the glans with thumb and fingers and with the tip of the syringe firmly in the meatus to prevent the gel from leaking out. Adequate lubrication helps to prevent urethral trauma. Use of a local anaesthetic minimises the discomfort experienced by the patient and can aid success of the procedure. 14. Remove the syringe tip from the urethra and keep the urethra closed. 15. Wait as recommended by the manufacturer (normally 3 to 5 minutes) to maximise the anaesthetic effect. 16. Now remove gloves, decontaminate hands and put on second sterile pair 17. Insert the catheter into meatus and advance the catheter gently to the bifurcation. Hold the penis all the time in the upright position, with traction of the other hand. If no urine drains gently apply pressure over the symphysis pubis area or ask the patient to cough. Advancing the catheter ensures that it is correctly positioned in the bladder. 18. Slowly inflate the balloon according to the manufacturer s instructions, having ensured that the catheter is draining urine beforehand. Inadvertent inflation of the balloon in the urethra causes pain and urethral trauma.
11 CG25 VERSION / Withdraw the catheter slightly to ensure that the balloon sits at the bladder base ensuring optimal urine drainage. 20. Secure the catheter using a support strap. Ensure that the catheter does not become taut when patient is mobilising, to maintain patient comfort and to reduce the risk of urethral and bladder neck trauma. 21. Ensure that the glans penis is cleansed after the procedure and reposition the foreskin if present. Retraction and constriction of the foreskin behind the glans penis resulting in paraphimosis may occur if this is not done. 22. Help the patient into a comfortable position. Ensure that the patient s skin and the bed are both dry. If the area is left wet or moist, secondary infection and skin irritation may occur. 23. Measure the amount of urine. Be aware of bladder capacity for patients with previous episodes of urinary retention and to assess for chronic retention. 24. Consider taking a urine specimen for examination, if required. 25. Dispose of equipment in a plastic clinical waste bag and seal the bag. 7.3 Female Urethral Catheterisation Procedure 1. Check patient file for past problems, allergies etc. 2. Prior to the procedure explain the process to the patient, ensure that they are able to give informed consent. 3. Undertake procedure on the patient s bed or in clinical treatment area using screens/curtains to promote and maintain dignity. 4. Assist the patient to get into the supine position. Do not expose the patient at this stage of the procedure. 5. Wash hands using soap and water or bactericidal alcohol hand rub to reduce risk of infection. 6. Prepare all equipment required on a clean working surface. 7. Open the outer cover of the catheterisation pack then open the sterile field, handling the outer corners only. Using aseptic non-touch technique open/place all other equipment onto sterile field. 8. Using an aseptic technique, connect the bag to the catheter. 9. Remove cover that is maintaining the patient s privacy and position a disposable pad under the patient s buttocks and thighs. To ensure urine does not leak onto bed. 10. Clean hands with a bactericidal alcohol hand rub, as hands may have become contaminated by handling the outer packs. 11. Put on non-sterile gloves. 12. Place dressing / protective towel across the patient s thighs, to create a protective sterile field.
12 CG25 VERSION / Clean the meatus: labia majora, labia minor and finally the urethral meatus. One swab one wipe anterior to posterior, to avoid wiping any bacteria from the perineum and anus forwards towards the urethra. 14. Replace existing gloves with a sterile pair. 15. Separate the labia with one hand and give traction upwards. In order to have a good view on the meatus and to minimise the risk of contamination of the urethra. 16. Apply a little lubrication to the meatus and then insert the conus of the syringe with (anaesthetic) lubrication in the meatus and slowly instill 6ml of the gel into the urethra. Remove the nozzle from the urethra. Adequate lubrication helps to prevent urethral trauma. Use of a local anaesthetic minimises the discomfort experienced by the patient and can add to the success of the procedure. 17. Pick up the catheter with the hand with the sterile glove. Insert the catheter in the meatus and gently advance the catheter along the urethra until it reaches the bladder and urine flows out. Then insert the catheter 2cm deeper, to confirm that the balloon is in the bladder. Inadvertent inflation of the balloon in the urethra causes pain and urethral trauma. 18. Withdraw the catheter slightly to ensure that the balloon sits at the bladder base ensuring optimal urine drainage. 19. If the patient wishes, secure the catheter using a support strap. Ensure that the catheter does not become taut when patient is mobilising. To maintain patient comfort and to reduce the risk of urethral and bladder neck trauma. 20. Ensure that the labia are cleaned after the procedure to avoid skin irritation. 21. Help the patient into a comfortable position. Ensure that the patient s skin and the bed are both dry. If the area is left wet or moist, secondary infection and skin irritation may occur. 22. Measure the amount of urine. Be aware of bladder capacity for patients with previous occurrences of urinary retention. To monitor renal function and fluid balance. 23. Consider taking a urine specimen for examination, if required. 24. Dispose of equipment in a plastic clinical waste bag and seal the bag. 25. Record information in relevant documents, as detailed in section 7.8.
13 7.4 Removal of a Suprapubic Catheter Equipment Checklist: Non-sterile disposable gloves. Syringe for deflating balloon. Disposable pad (to protect bed). Plastic disposable apron or protective clothing. Gauze swabs / disposable wipes. Sterile absorbing dressing and tape. CG25 VERSION / Procedure 1. Maintain patient dignity. 2. Prior to the procedure explain the process to the patient, to ensure that they are able to give informed consent. 3. Decontaminate hands and put on non-sterile gloves. 4. Check volume of water in balloon (refer to patient documentation), then attach the syringe to catheter valve to deflate the balloon. Do not use suction on the syringe but allow the solution to come back spontaneously. 5. Ask patient to breathe in and then out; as patient exhales, gently remove the catheter. 6. Clean suprapubic fistula using gauze/disposable wipe, clear away equipment, put on an occlusive absorbent dressing and make the patient comfortable. 7. Used equipment should be placed in clinical waste bag and disposed of in line with local Trust policy. 8. Document procedure and note any difficulties / problems experienced as detailed in section Insertion of a Suprapubic Balloon Catheter Any clinician who undertakes suprapubic re-catheterisation must have undergone a programme of training and clinical supervision and be assessed as competent to undertake this procedure. 7.6 Changing a Suprapubic Catheter Checklist equipment: Sterile catheterisation pack. Disposable pad for bed protection. Two pairs of gloves, one of which must be sterile for handling new catheter. Appropriate catheter; it is advisable to take a spare catheter in addition to the one you want. Sterile anaesthetic lubricating gel (5-6mls).
14 CG25 VERSION /20 Universal specimen container, if required. Cleansing solution (sodium chloride 0.9% is sufficient). Bactericidal alcohol hand rub. 10ml sterile water (inflation of balloon) or as recommended by manufacturer. Syringe and drawing up needle to draw up sterile water and inflate balloon, 10ml syringe to deflate existing balloon. Disposable plastic apron/protective clothing. A closed urinary drainage system, e.g. a night bag, leg bag or catheter valve. A catheter drainage bag stand, if required. Dressing and wound care set (supplementary pack) Procedure 1. Check patient file for past problems, allergies etc. 2. Prior to the procedure explain the process to the patient, to ensure that they are able to give informed consent. 3. Undertake procedure on the patient s bed or in clinical treatment area using screens/curtains to promote and maintain dignity. Assist the patient to get into a comfortable supine position to ensure the suprapubic tract is accessible. Do not expose the patient at this stage of the procedure. 4. Wash hands using soap and water or bactericidal alcohol hand rub. 5. Put on a disposable plastic apron or protective clothing. 6. Prepare all equipment required. Assemble all of the necessary equipment. The catheter size and amount of water instilled in the balloon should be the same as the existing suprapubic catheter. 7. Open the outer cover of the catheterisation pack then open the sterile field, handling the outer corners only using an aseptic non-touch technique, open the supplementary packs. 8. Using an aseptic technique, connect the bag to the catheter at this stage. 9. Remove cover that is maintaining the patient s privacy and position a disposable pad under the patient s buttocks and thighs, to ensure urine does not leak onto bed. 10. Clean hands with an bactericidal alcohol hand rub. 11. Put on sterile gloves. 12. Observe the current suprapubic site for the lie of the catheter, angle of insertion and mark the existing catheter with tape at the point of entry to the skin. This will act as a guide for the insertion length and angle for the new catheter. 13. Place dressing/protective towel across the patient s abdomen.
15 CG25 VERSION / Using a gauze swab clean the cystostomy site. 15. Remove existing gloves, decontaminate hands and put on sterile pair of gloves and place new sterile towel at the cystostomy site. 16. Deflate balloon (without suction) of existing catheter and remove catheter. Ensure you have sterile gauze at hand, to put on the Supra Pubic Catheter insertion site to prevent leakage. 17. Insert 5ml to 10ml of water-soluble lubricant or local anaesthetic gel into the suprapubic tract. 18. Remove gloves decontaminate hands with bactericidal alcohol hand rub and put on sterile pair. 19. Insert the catheter and advance the same length as the previous one. Ensure urine draining. Apply gentle pressure over symphysis pubis area if no urine draining. 20. Slowly inflate the balloon according to the manufacturer s instructions. 21. Withdraw the catheter slightly; the catheter should be able to slide up and down the cystostomy slightly. 22. Secure the catheter using a support strap, ensure that the catheter does not become taut when patient mobilises. 23. Help the patient into a comfortable position to ensure that the patient s skin and the bed are both dry. 24. Measure and document the amount of urine. 25. Take a urine specimen for laboratory examination, if required. 26. Dispose of equipment in a plastic clinical waste bag and seal the bag. 27. Record information in relevant documents, as detailed in section Obtaining a Urine Sample From an Indwelling Catheter 1. Prior to the procedure explain the process to the patient, to ensure that they are able to give informed consent. 2. Wash your hands with soap and water and put on an apron. Clean hands with bactericidal alcohol hand rub and put on sterile gloves. 3. If there is no urine visible in the catheter tubing then a clamp may be placed a few centimetres distal to the sampling port. 4. Once there is sufficient urine visible in the drainage tube above the clamp, then wipe the sampling port with a 2% Chlorhexidine in 70% alcohol swab and allow to dry. 5. Insert a sterile syringe into the needle-free sampling port. Aspirate the required amount of urine. 6. Remove the syringe and transfer specimen into sterile specimen pot. 7. Wipe the sampling port with a 2% Chlorhexidine in 70% alcohol swab and allow to dry. 8. Unclamp the drainage tubing.
16 CG25 VERSION /20 9. Dispose of all waste materials as clinical waste according to Trust policy. 10. Wash hands with soap and water or bactericidal alcohol hand rub. 11. Complete documentation as detailed in section Documentation It is important that all aspects of catheter management are documented thoroughly, including: Reasons for catheterisation. Date and time of catheterisation. Catheter type, length and size. Amount of water instilled into the balloon. Batch number and manufacturer (catheter packaging may have include stickers for this purpose which can be peeled off and placed on clinical record). Drainage system used. Problems negotiated during the procedure. Follow up arrangements as required.
17 CG25 VERSION /20 8. Complications 8.1 Catheter Bypassing Catheter bypassing occurs in up to 40% of patients with indwelling catheters, and may occur as a consequence of various aetiologies including catheter blockage, bladder spasm, constipation, pulling on the catheter or a too large diameter of the catheter. In itself, catheter bypassing is not a diagnosis but rather a symptom; treatment of which should be aimed at the underlying cause. 8.2 Iatrogenic Trauma Iatrogenic trauma during urethral catheterisation may result in either the formation of a false passage, usually at the level of the prostate or bladder neck, urethral stricture disease or traumatic cleaving in the male, with sphincteric disruption in the female. Such trauma is rare, with an overall incidence of 0.3%. Paraphimosis may occur when an uncircumcised male is catheterised and the prepuce is not replaced. Care and continued patient and carer education will reduce the incidence of such a complication. 11% of urethral strictures requiring urethroplasty arise following urethral catheterisation Suprapubic catheterisation is associated with a potential for visceral injury which although difficult to reliably quantify due to under-reporting, is in the region of 2-3% for bowel perforation, carrying a 30-day mortality rate in the region of 2%. Visceral trauma is more common amongst patients with previous lower abdominal surgery and in those with neurological disease. The patient should always be observed for persistence or worsening of lower abdominal pain, pain spreading away from cystostomy, change in bowel habit, poor or no urine output or becoming unexpectedly unwell all signs of visceral bowel injury requiring urgent admission to hospital The incidence of visceral trauma during SPC insertion may be reduced by ensuring the existing catheter is marked with tape at point of entry to skin (to act as a guide for length of re-insertion) or there is some urine (300 ml) in the bladder and that the new catheter is draining freely.
18 CG25 VERSION / Bladder Spasm/Bladder Pain Bladder spasm is common in patients with indwelling catheters, causing pain and by-passing. It usually settles spontaneously. Chronic constipation may cause bladder spasm. Maintaining regular bowel function with a highfibre and high-fluid intake helps prevent constipation. Sometimes a different catheter (smaller lumen and balloon size) can also reduce the spasm caused by constipation. Hydrogel catheters are more biocompatible and may reduce bladder spasm. Persistent bladder spasm pain and symptoms can be relieved with antimuscarinic medication. 8.4 Haematuria Haematuria may occur following catheterisation and is usually self limiting. During urethral catheterisation, prostatic trauma may be the underlying cause, although decompression of high pressure chronic retention may also result in haematuria. The patient should be reassured and oral fluids encouraged. Hospitalisation is not necessary unless frank haematuria or clots are present or the patient is haemodynamically unstable. 8.5 Inability to Remove Catheter Catheters may occasionally prove impossible to remove via balloon deflation. This may be as a consequence of balloon calcific encrustation or a faulty deflation mechanism. 8.6 Catheter Washout People requiring long-term bladder draining with an indwelling catheter can often experience catheter blockage. As there are quite a few causes of catheter blockage (e.g. kinks in a tube, constipation, catheter against bladder wall, encrustation, debris) it is important to diagnose the exact reason for the blockage in order to decide on the correct course of treatment. Whilst catheter maintenance solutions exist, these should be used to maintain the catheter in situ i.e. prevent blockage and should not be used to try to unblock a catheter that is already blocked. Using maintenance solution to unblock a catheter is then an incorrect use of the product and product licence. If a catheter is blocked it needs to be changed, any form of washout or catheter manipulation must not be used.
19 CG25 VERSION /20 9. Patient Wellbeing 9.1 Fluid intake Drinking sufficient fluid dilutes the urine and helps reduce the risk of catheter encrustation and blockage. A good fluid intake also ensures a constant downward drainage and flushing effect. There is no standard amount of advised fluid intake and the type of fluid consumed appears to be insignificant as long as the volume is sufficient to prevent concentration of urine. The amount of fluid needed varies and depends on patient s size (25-35 ml/kg/day), amount of fluid loss, patient s food intake and patients circulatory and renal status. Regular fluid intake maintains the urinary flow and reduces the risk of infection and catheter blockage As a general rule, patients with indwelling catheters should not be given prophylactic antibacterial therapy and the treatment of bacteriuria with antibiotics should be carefully considered. Misuse of antibacterial therapy is likely to produce antibiotic resistance. The bowel and the bladder then become a reservoir for antibiotic resistant organisms. To avoid this complication, antibiotics should not be given in an attempt to prevent bacteriuria in long term catheterisation but rather reserved for treatment of acute episodes of clinical infection indicated by fever > 38 C, pus in urine, suprapubic or loin pain or sudden onset of confusion.
20 CG25 VERSION /20 References Harrison. C.W., et al. (2010). British Association of Urological Surgeons (BAUS), Suprapubic catheter practice guidelines. BJUI available online at baus.org.uk. The Health and Social Care Act Code of Practice on the prevention and control of infections and related guidance. London: Department of Health. Belfield P, (1988). Urinary catheters. British Medical Journal. 296, 6625, pp Blandy J et al, (1989). Catheters and catheterisation. In Blandy J et al (Eds). Urology for Nurses. First Edition. Oxford, Blackwell Scientific Publications Ltd. Britton R et al, (1990). Catheters: making an informed choice. Professional Nurse. 5, 4, pp Department of Health (2006) Essential steps to safe, clean care. Reducing healthcareassociated infections in Primary Care Trusts; Mental health trusts; Learning disability organisations; Independent healthcare; Care Homes; Hospices: GP practices and Ambulance Services. DoH, London. Getliffe K, (1993). Care of urinary catheters. Nursing Standard. 7, 44, pp Horgan A et al, (1992). Acute urinary retention: comparison of suprapubic and urethral catheterisation. British Journal of Urology. 70, 2, pp McGill S, (1982). Catheter management: it s the size that s important. Nursing Mirror. 154, April 7, pp Norton C, (1986). Catheterisation. In Norton C (Ed). Nursing for Continence. Beaconsfield Publishers, Beaconsfield. Pomfret I, (2000). Catheter care in the community. Nursing Standard. 14, 27, pp The Royal Marsden NHS Trust (2001) Manual and Clinical Nursing Procedures, London: Blackwell Science. Winn C, (1998). Complications with urinary catheters. Professional Nurse. 13, 5 (Suppl), pp7-10. Woodward S, (1997). Complications of allergies to latex urinary catheters. British Journal of Nursing. 6, 14, pp
Male Urethral Catheterisation Education Package
 Male Urethral Catheterisation Education Package TABLE OF CONTENTS 1. Accountability 2. Introduction 3. Types of Catheters 4. Guidelines for catheter selection 5. Patient Preparation 6. Equipment 7. Procedure
Male Urethral Catheterisation Education Package TABLE OF CONTENTS 1. Accountability 2. Introduction 3. Types of Catheters 4. Guidelines for catheter selection 5. Patient Preparation 6. Equipment 7. Procedure
Location: Clinical Practice Manual
 Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Male Urinary Catheterisation & Catheter Care
 Male Urinary Catheterisation & Catheter Care Mark Jones, Martin Steggall & Marsh Gelbart City University, London. Good practice Consent gain informed consent. Who can catheterise any Registered Nurse who
Male Urinary Catheterisation & Catheter Care Mark Jones, Martin Steggall & Marsh Gelbart City University, London. Good practice Consent gain informed consent. Who can catheterise any Registered Nurse who
online version Understanding Indwelling Urinary Catheters and Drainage Systems Useful information When to call for help
 When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
Fact Sheet. Caring for and Changing your Supra-Pubic Catheter (SPC) Queensland Spinal Cord Injuries Service
 and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
CATHETERISATION. East Lancashire Hospitals NHS Trust Eileen Whitehead 2010
 CATHETERISATION East Lancashire Hospitals NHS Trust Eileen Whitehead 2010 1 Indications for catheterisation: A person is unable to void naturally due to injury or a disease process Diagnostic or therapeutic
CATHETERISATION East Lancashire Hospitals NHS Trust Eileen Whitehead 2010 1 Indications for catheterisation: A person is unable to void naturally due to injury or a disease process Diagnostic or therapeutic
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Male Catheterisation
 1 Prepare your equipment, put what you need on to the trolley, choose catheter appropriate for urethral size and check the volume of water needed to inflate the balloon. All this information is written
1 Prepare your equipment, put what you need on to the trolley, choose catheter appropriate for urethral size and check the volume of water needed to inflate the balloon. All this information is written
Foley Catheter Placement
 Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
PATIENT URINARY CATHETER PASSPORT
 n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
Indwelling urinary catheter. Information for patients and carers. RDaSH. Doncaster Community Integrated Services
 Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER
 URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
PROCEDURE FOR URINARY CATHETERISATION
 PROCEDURE FOR URINARY CATHETERISATION First Issued Issue Version One Purpose of Issue/Description of Change Planned Review Date To promote safe and effective urinary catheterisation for patients in a community
PROCEDURE FOR URINARY CATHETERISATION First Issued Issue Version One Purpose of Issue/Description of Change Planned Review Date To promote safe and effective urinary catheterisation for patients in a community
Infection Prevention & Control Team. Your urinary catheter & how to care for it 0151 430 2452 / 0151 430 1384. Patient Information Leaflet
 Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
Catheter Care. What you need to know. Jacinta Stewart Continence Nurse
 Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed
 Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER PROBLEMS
 PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One Outlines the process for staff
PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One Outlines the process for staff
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care
 Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Patient Information:
 Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES
 ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
Managing your bladder with a suprapubic catheter at home
 Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
ATI Skills Modules Checklist for Urinary Catheter Care
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Looking after your urinary catheter at home. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Looking after your urinary catheter at home An information guide Looking after your urinary catheter at home This leaflet is provided for
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Looking after your urinary catheter at home An information guide Looking after your urinary catheter at home This leaflet is provided for
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
Bladder Catheterization
 Approved by: Bladder Catheterization Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Ensenat Medical Director, Neonatology Neonatal Nursery Policy & Procedures
Approved by: Bladder Catheterization Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Ensenat Medical Director, Neonatology Neonatal Nursery Policy & Procedures
Self Catheterization Guide
 Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
PROCEDURE FOR CLEAN INTERMITTENT CATHETERIZATION MALE
 PROCEDURE FOR CLEAN INTERMITTENT CATHETERIZATION MALE 1. Wash hands. PROCEDURE POINTS TO REMEMBER 2. Assemble equipment. Water-soluble lubricant, such as K-Y Jelly, Lubrifax, Surgel Catheter, plastic or
PROCEDURE FOR CLEAN INTERMITTENT CATHETERIZATION MALE 1. Wash hands. PROCEDURE POINTS TO REMEMBER 2. Assemble equipment. Water-soluble lubricant, such as K-Y Jelly, Lubrifax, Surgel Catheter, plastic or
Policies & Procedures. Care of
 Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
Guidelines for the Insertion, Ongoing Care and Removal of Indwelling Urethral Catheters
 Derby Hospitals NHS Foundation Trust Guidelines for the Insertion, Ongoing Care and Removal of Indwelling Urethral Catheters Aim Reference No: CG-T/2011/140 These evidence based guidelines seek to provide
Derby Hospitals NHS Foundation Trust Guidelines for the Insertion, Ongoing Care and Removal of Indwelling Urethral Catheters Aim Reference No: CG-T/2011/140 These evidence based guidelines seek to provide
PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014
 PICU Urinary Catheter & Care Guideline September 2014 Introduction PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014 Background: Urinary catheterisation
PICU Urinary Catheter & Care Guideline September 2014 Introduction PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014 Background: Urinary catheterisation
Looking after your urinary catheter at home
 Looking after your urinary catheter at home Information for patients and carers Useful contacts to keep: Name and title of community nurse Single point of access (SPA) for community nursing 24 hour service
Looking after your urinary catheter at home Information for patients and carers Useful contacts to keep: Name and title of community nurse Single point of access (SPA) for community nursing 24 hour service
Having a urinary catheter information for men
 Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Percutaneous Nephrostomy. Care of your Nephrostomy. Department of Urology
 Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
Catheterisation Insertion and Management Protocol (Whole Healthcare Economy)
 Catheterisation Insertion and Management Protocol (Whole Healthcare Economy) NHFT policy ICP 013 Version: June11 v2 Ratified by: Trust Policy Board Date ratified: 21 st June 2011 Implementation date: 1
Catheterisation Insertion and Management Protocol (Whole Healthcare Economy) NHFT policy ICP 013 Version: June11 v2 Ratified by: Trust Policy Board Date ratified: 21 st June 2011 Implementation date: 1
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Intermittent Self Catheterisation for Women
 ISCW Intermittent Self Catheterisation for Women National Service, Locally Based www.fittleworth.com Opening hours: 8am - 8pm Monday to Friday 9am - 1pm on Saturday Freephone National 0800 378 846 Scotland
ISCW Intermittent Self Catheterisation for Women National Service, Locally Based www.fittleworth.com Opening hours: 8am - 8pm Monday to Friday 9am - 1pm on Saturday Freephone National 0800 378 846 Scotland
Going home with a urinary cathether
 Going home with a urinary cathether A patient s guide 1 Your doctor has advised that you require a urinary catheter so that urine can be drained from your bladder. This leaflet provides advice to help
Going home with a urinary cathether A patient s guide 1 Your doctor has advised that you require a urinary catheter so that urine can be drained from your bladder. This leaflet provides advice to help
Having a supra pubic urinary catheter
 Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
After care following insertion of a suprapubic catheter
 Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
PROCEDURE FOR CATHETER AFTERCARE
 PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
A Guide to Help You Manage Your Catheter and Drainage Bags
 A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
Care of the Catheterised Patient and Urinalysis
 Care of the Catheterised Patient and Urinalysis Male Pelvic Anatomy Female Pelvic Anatomy What does a urinary catheter do? Urinary Catheters Urinary Catheters Urinary Catheters Why do patients have catheters?
Care of the Catheterised Patient and Urinalysis Male Pelvic Anatomy Female Pelvic Anatomy What does a urinary catheter do? Urinary Catheters Urinary Catheters Urinary Catheters Why do patients have catheters?
INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline
 INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline TITLE: Insertion of a curved tip Urinary Catheter (Coude/Tiemann) NUMBER: CC 50-013 Effective Date: August 2015 Page 1 of 5 Applies To: All Preamble:
INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline TITLE: Insertion of a curved tip Urinary Catheter (Coude/Tiemann) NUMBER: CC 50-013 Effective Date: August 2015 Page 1 of 5 Applies To: All Preamble:
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
SAMPLE Policy and Procedure Insertion, Removal and Care of an Indwelling Foley Catheter
 SAMPLE Policy and Procedure Insertion, Removal and Care of an Indwelling Foley Catheter Approved by: Policy and Procedure Committee Effective: x/xx Revised: x/xx Description: This policy provides the procedure
SAMPLE Policy and Procedure Insertion, Removal and Care of an Indwelling Foley Catheter Approved by: Policy and Procedure Committee Effective: x/xx Revised: x/xx Description: This policy provides the procedure
Living life to the full with an indwelling catheter
 Living life to the full with an indwelling catheter www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 Living with and
Living life to the full with an indwelling catheter www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 Living with and
Achieving Independence
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
How to Change a Foley Catheter Step-by-step instructions for the caregiver
 Patient Education How to Change a Foley Catheter Step-by-step instructions for the caregiver This handout gives stepby-step instructions for changing a Foley catheter, a tube in the bladder to drain urine.
Patient Education How to Change a Foley Catheter Step-by-step instructions for the caregiver This handout gives stepby-step instructions for changing a Foley catheter, a tube in the bladder to drain urine.
SECTION 12.1 URINARY CATHETERS
 SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
Appropriate Urinary Catheter Use and Management
 Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION
 SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE. Author: GRCS Date: 20/06/09 Catalogue No: 712438
 CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE Author: GRCS Date: 20/06/09 Catalogue No: 712438 What is a urinary catheter? A urinary catheter is a hollow tube which drains urine
CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE Author: GRCS Date: 20/06/09 Catalogue No: 712438 What is a urinary catheter? A urinary catheter is a hollow tube which drains urine
Intermittent Self Dilatation (ISD) for Men
 Welcome to Fittleworth Intermittent Self Dilatation (ISD) for Men Simply... a secure home delivery service Freephone Freephone National: National: 0800 378 0800 846 378 846 Freephone Freephone Scotland:
Welcome to Fittleworth Intermittent Self Dilatation (ISD) for Men Simply... a secure home delivery service Freephone Freephone National: National: 0800 378 0800 846 378 846 Freephone Freephone Scotland:
You have been sent home with. Suprapubic Catheter
 You have been sent home with Suprapubic Catheter 1 SUPRAPUBIC CATHETER 1.- What is a suprapubic catheter? 2.- What do you need on discharge. 3.- Basic care 4.- Choosing your bag and bag care 5.- Possible
You have been sent home with Suprapubic Catheter 1 SUPRAPUBIC CATHETER 1.- What is a suprapubic catheter? 2.- What do you need on discharge. 3.- Basic care 4.- Choosing your bag and bag care 5.- Possible
Clinical Guideline for: Aseptic Technique
 Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
NHS Professionals. CG8 Guidelines for Continence and Catheter Care. Introduction
 NHS Professionals CG8 Guidelines for Continence and Catheter Care Introduction Continence has been defined as control of bladder and bowel function and continence care is the name given to the total care
NHS Professionals CG8 Guidelines for Continence and Catheter Care Introduction Continence has been defined as control of bladder and bowel function and continence care is the name given to the total care
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
PATIENT CARE MANUAL PROCEDURE
 PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
Looking after your bladder
 Looking after your bladder A guide for women after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who
Looking after your bladder A guide for women after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who
Urinary tract and perineum
 9 Urinary tract and perineum Key Points 9.1 9.1 THE URINARY BLADDER URINARY RETENTION Acute retention of urine is an indication for emergency drainage of the bladder The common causes of acute retention
9 Urinary tract and perineum Key Points 9.1 9.1 THE URINARY BLADDER URINARY RETENTION Acute retention of urine is an indication for emergency drainage of the bladder The common causes of acute retention
Bard. Guide for Patients. Comprehensive Care Managing Urinary Catheters and Drainage Systems. Useful information. Useful organisations
 Useful information Your catheter and bags may be obtained on prescription from your doctor To register to Prescription Xpress Free Home Delivery service simply contact the Prescription Xpress Support Team
Useful information Your catheter and bags may be obtained on prescription from your doctor To register to Prescription Xpress Free Home Delivery service simply contact the Prescription Xpress Support Team
CLINICAL GUIDELINES Urinary Catheterisation Guidelines
 Reference Date approved Approving Body CLINICAL GUIDELINES Urinary Catheterisation Guidelines Matron s Forum Supporting Policy/ Working in Male Urethral Catheterisation New Ways (WINW) Package Implementation
Reference Date approved Approving Body CLINICAL GUIDELINES Urinary Catheterisation Guidelines Matron s Forum Supporting Policy/ Working in Male Urethral Catheterisation New Ways (WINW) Package Implementation
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Clean Intermittent Catheterization (CIC) For Males
 The Emily Center Clean Intermittent Catheterization (CIC) For Males Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 male patient
The Emily Center Clean Intermittent Catheterization (CIC) For Males Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 male patient
POLICY FOR CATHETER MANAGEMENT
 POLICY FOR CATHETER MANAGEMENT 1 Document Control Sheet Name of document: Version: 6 Status: Owner: File location / Filename: Policy for catheter management Infection Prevention & Control Team Date of
POLICY FOR CATHETER MANAGEMENT 1 Document Control Sheet Name of document: Version: 6 Status: Owner: File location / Filename: Policy for catheter management Infection Prevention & Control Team Date of
HOW TO CARE FOR YOUR CATHETER (FEMALE)
 HOW TO CARE FOR YOUR CATHETER (FEMALE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What is a catheter? A catheter is a narrow flexible soft tube inserted into the bladder for the purpose
HOW TO CARE FOR YOUR CATHETER (FEMALE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What is a catheter? A catheter is a narrow flexible soft tube inserted into the bladder for the purpose
Management of urinary catheters
 Information for patients and relatives This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Corp/326.2 (2012)
Information for patients and relatives This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Corp/326.2 (2012)
Urinary Indwelling Catheter. The Urinary System
 Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Clean Intermittent Catheterization (CIC) For Females What it is:
 The Emily Center Clean Intermittent Catherterization (CIC) for Females Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 female
The Emily Center Clean Intermittent Catherterization (CIC) for Females Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 female
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Canterbury Continence Forum Health Professionals Working in Partnership CATHETER CARE GUIDELINES 2013
 Canterbury Continence Forum Health Professionals Working in Partnership CATHETER CARE GUIDELINES 2013 Contents ACKNOWLEDGEMENTS... 3 THE CONTINENCE REFERRERS AND PROVIDERS FORUM... 3 CATHETER CARE GUIDELINES...
Canterbury Continence Forum Health Professionals Working in Partnership CATHETER CARE GUIDELINES 2013 Contents ACKNOWLEDGEMENTS... 3 THE CONTINENCE REFERRERS AND PROVIDERS FORUM... 3 CATHETER CARE GUIDELINES...
GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE
 GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE Reference Date approved Nov 2012 Approving Body Matrons Forum Supporting Policy/ Working in New Ways (WINW) Package Implementation date Supersedes
GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE Reference Date approved Nov 2012 Approving Body Matrons Forum Supporting Policy/ Working in New Ways (WINW) Package Implementation date Supersedes
SARI. Guidelines for the Prevention of Catheterassociated Urinary Tract Infection
 Guidelines for the Prevention of Catheterassociated Urinary Tract Infection Published on behalf of SARI by HSE Health Protection Surveillance Centre 2011 SARI A Strategy for the Control of Antimicrobial
Guidelines for the Prevention of Catheterassociated Urinary Tract Infection Published on behalf of SARI by HSE Health Protection Surveillance Centre 2011 SARI A Strategy for the Control of Antimicrobial
Instruction Guide to Sterile Self-Catheterization for Women Using the Cure Catheter Closed System
 Cure Medical donates 10% of net income to medical research in pursuit of a cure for spinal cord injuries and central nervous system disorders. For information on scientific advancements, visit www.curemedical.com.
Cure Medical donates 10% of net income to medical research in pursuit of a cure for spinal cord injuries and central nervous system disorders. For information on scientific advancements, visit www.curemedical.com.
Urinary Catheter Policy for Community Health Services, Inpatient Facilities and Primary Care
 1 Urinary Catheter Policy for Community Health Services, Inpatient Facilities and Primary Care The document describes the processes and procedures for insertion and management of urinary catheters for
1 Urinary Catheter Policy for Community Health Services, Inpatient Facilities and Primary Care The document describes the processes and procedures for insertion and management of urinary catheters for
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Intermittent Clean Catheterization for Women
 2014 Intermittent Clean Catheterization for Women Intermittent Clean Catheterization for Women What is intermittent catheterization? Intermittent catheterization is a way to drain urine (pee) from your
2014 Intermittent Clean Catheterization for Women Intermittent Clean Catheterization for Women What is intermittent catheterization? Intermittent catheterization is a way to drain urine (pee) from your
Intermittent Self-Catheterization. A Step by Step Guide for Men and Women
 Inside this book Intermittent Self-Catheterization A Step by Step Guide for Men and Women 1986 2005 St. Joseph s Healthcare Hamilton Hamilton, Ontario Contributors: Jennifer Skelly Paula Eyles Linda Hilts
Inside this book Intermittent Self-Catheterization A Step by Step Guide for Men and Women 1986 2005 St. Joseph s Healthcare Hamilton Hamilton, Ontario Contributors: Jennifer Skelly Paula Eyles Linda Hilts
RATIFIED BY NNPDG SEPTEMBER 2006 FOR REVIEW 2009
 NOTTINGHAM UNIVERSITY HOSPTIALS/RUSHCLIFFE PCT NURSING PRACTICE GUIDELINES GUIDELINES FOR CARE OF A PATIENT WITH A WOUND DRAINAGE SYSTEM CONTENTS PAGE Introduction and Types of Drains 1 Procedure for Applying
NOTTINGHAM UNIVERSITY HOSPTIALS/RUSHCLIFFE PCT NURSING PRACTICE GUIDELINES GUIDELINES FOR CARE OF A PATIENT WITH A WOUND DRAINAGE SYSTEM CONTENTS PAGE Introduction and Types of Drains 1 Procedure for Applying
Catheter Care How to Care for a Urinary Catheter
 Catheter Care How to Care for a Urinary Catheter Ensure patient/client is provided with any available product specific instructions along with this booklet. About Your Catheter Your urinary catheter allows
Catheter Care How to Care for a Urinary Catheter Ensure patient/client is provided with any available product specific instructions along with this booklet. About Your Catheter Your urinary catheter allows
Discussions about having a Supra pubic catheter
 Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
Discussions about having a Supra pubic catheter What is a supra pubic catheter? A supra pubic catheter is used to drain urine from the bladder by inserting a catheter (narrow hollow drainage tube) directly
University College Hospital
 University College Hospital Caring for your urinary catheter Urology Directorate for men 2 3 If you require a large print, audio or translated version of this leaflet, please contact us on 0845 155 5000
University College Hospital Caring for your urinary catheter Urology Directorate for men 2 3 If you require a large print, audio or translated version of this leaflet, please contact us on 0845 155 5000
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
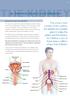 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
A Child s guide to Clean Intermittent Catheterization. Boys
 A Child s guide to Clean Intermittent Catheterization Boys Introduction Probably you have just heard that you have to learn to catheterize your bladder. Most children are worried, frightened or scared
A Child s guide to Clean Intermittent Catheterization Boys Introduction Probably you have just heard that you have to learn to catheterize your bladder. Most children are worried, frightened or scared
Care of a Foley Catheter
 Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Placement of an indwelling urinary catheter in female dogs
 Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Female Dog Urinary Catheterization 1 of 6 Placement of an indwelling urinary catheter in female dogs Bernie Hansen DVM MS North Carolina State University College of Veterinary Medicine Materials Needed
Catheterisation. Indwelling catheters in adults. Evidence-based Guidelines for Best Practice in Urological Health Care. Urethral and Suprapubic
 Evidence-based Guidelines for Best Practice in Urological Health Care Catheterisation Indwelling catheters in adults Urethral and Suprapubic 2012 European Association of Urology Nurses 2 Catheterisation:
Evidence-based Guidelines for Best Practice in Urological Health Care Catheterisation Indwelling catheters in adults Urethral and Suprapubic 2012 European Association of Urology Nurses 2 Catheterisation:
4. Infection control measures
 4. Infection control measures Apart from general hygienic practices and vaccination, staff of institutions should also adopt specific infection control measures against communicable diseases. The measures
4. Infection control measures Apart from general hygienic practices and vaccination, staff of institutions should also adopt specific infection control measures against communicable diseases. The measures
Intermittent Self Catheterization for Males
 Intermittent Self Catheterization for Males CEAC 0371 January 2016 Intermittent Self Catheterization This involves inserting a catheter (small tube) into your bladder at regular intervals to help empty
Intermittent Self Catheterization for Males CEAC 0371 January 2016 Intermittent Self Catheterization This involves inserting a catheter (small tube) into your bladder at regular intervals to help empty
Catheter Associated Urinary Tract Infection (CAUTI) Prevention. System CAUTI Prevention Team
 Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Urinary Catheter Care and Prostate Cancer Treatment
 Urinary Catheter Care and Prostate Cancer Treatment The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions
Urinary Catheter Care and Prostate Cancer Treatment The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions
Learning Resource Guide. Understanding Incontinence. 2000 Prism Innovations, Inc. All Rights Reserved
 Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
