Computer-Guided Planning and Placement of Dental Implants
|
|
|
- Sophie Harrison
- 10 years ago
- Views:
Transcription
1 Atlas Oral Maxillofacial Surg Clin N Am 20 (2012) Computer-Guided Planning and Placement of Dental Implants Gary Orentlicher, DMD a, *, Douglas Goldsmith, DDS a, Marcus Abboud, DMD b a Private Practice, New York Oral, Maxillofacial, and Implant Surgery, 495 Central Park Avenue, Suite 201, Scarsdale, NY, USA b Department of Prosthodontics and Digital Technology, School of Dental Medicine, State University of New York at Stony Brook, Stony Brook, NY 11794, USA The goal of dental implant therapy is the accurate and predictable restoration of a patient s dentition. These goals are best achieved when all members of the surgical and restorative team are working together on diagnosis, planning, and reconstruction. The recent introduction of new 3- dimensional (3D) diagnostic and treatment planning technologies in implant dentistry have created an environment for the team approach to the planning and placement of dental implants, according to a restoratively driven treatment plan. The team can now start with the end result, the planned tooth, and then place an implant into the correct position according to the restorative plan. The accurate and predictable placement of implants according to a computer-generated virtual treatment plan is now a reality, transferring the virtual plan from the computer to operative treatment. Third-party proprietary implant software and associated surgical instrumentation, in combination with 3D imaging technologies, has revolutionized dental implant diagnosis and treatment. This development has created an interdisciplinary environment in which communication between the team members leads to better patient care and outcomes. Historical overview Standard dental diagnosis involves evaluating and diagnosing patients using 2-dimensional radiographic images (ie, periapical, bitewing, panoramic, and cephalometric radiographs). Clinician acceptance of the limitations of these technologies was required in the evaluation of actual 3D problems, because few options were available. Oral and maxillofacial surgeons, because of their hospital training, have long used computed tomography (CT) scans for the 3D evaluation of facial trauma and pathologic lesions. These CT evaluations were commonly viewed in 2 dimensions as axial or reformatted frontal or coronal slices through the area of interest of a patient s anatomy, viewed as sheets of printed films or on a computer screen. The remainder of the dental community had little if any exposure to 3D image evaluation. The first medical-grade helical CT scanners were all slower, single-slice machines, typically based in hospitals or private radiology facilities. Today s medical multislice CT scanners are capable of performing an upper and/or lower jaw scan in a few seconds. However, radiation exposure, the lack of familiarity and training among dentists, the size and cost of the machines, and the perceived costbenefit ratio in patient care made them inappropriate for a dental office setting. In 1998, with the development and introduction of the New Tom 9000 (Quantitative Radiology, Verona, Italy), conebeam volumetric tomography (CBVT/CBCT) was introduced to the dental community [1]. Although the early machines were large, the advantages were that they produced good 3D images at lower * Corresponding author. address: [email protected] /12/$ - see front matter Ó 2012 Elsevier Inc. All rights reserved. doi: /j.cxom oralmaxsurgeryatlas.theclinics.com
2 54 ORENTLICHER et al radiation doses [2 4]. The newer machines of today have a much smaller footprint and are small enough to fit into a dental office. The disadvantages were that although the radiation was less than medical-grade CT, it was larger than conventional dental radiographs and because of the reduced radiation, the images produced had somewhat less definition than medical CT. Medical-grade CT remains the gold standard for accurate 3D diagnosis [5,6]. Adaptive statistical iterative reconstruction (ASIR) software has recently been reported to allow up to a 50% reduction in radiation dose in medical CT scans, without diminishing image quality [7 10]. There are different average deviations and percentage error measurements for all CBCT scanners [11,12]. In the late 1980s articles discussing the use of Dentascans to evaluate the bone of the maxilla and mandible in preparation for placement of dental implants began to appear in the professional literature [13 16]. Columbia Scientific (CSI) introduced the 3D Dental software in This software converted CT axial slices into reformatted cross-sectional images of the alveolar ridges for diagnosis and evaluation. In 1991, a combination software named ImageMaster-101 was introduced by CSI, which added the ability to place graphic dental implants on the cross-sectional images. The first version of Sim/Plant was introduced by CSI in This software allowed the placement of virtual implants of exact dimensions, on CT images, in cross-sectional, axial, and panoramic views. In 1999 SimPlant 6.0 was introduced, adding the creation of 3D reformatted image surface-rendering images to the software [17]. Soon after Materialise (Leuven, Belgium) purchased CSI in 2001, the technology for drilling osteotomies to exact depth and direction through a surgical guide was introduced. SimPlant was designed as an open system to perform osteotomies for the placement of straightwalled implants from all implant manufacturers. It was not designed for the final placement of implants to depth, through a surgical guide, or for tapered implant systems. NobelBiocare (Zurich, Switzerland) introduced the NobelProcera/NobelGuide technology in This technology was introduced as a complete implant planning and placement system, for both straight-walled and tapered NobelBiocare implants. Instrumentation was developed to create osteotomies of accurate depth and direction, as well as the ability to place implants flaplessly, to accurate depth, through a guide. The system was designed for typical postimplant insertion treatment (cover screws or healing abutments), immediate loading of implants, and the fabrication of partial-arch or full-arch restorations before implant placement. In 2011, NobelClinician, a completely redesigned upgrade of the NobelGuide software, was introduced. Software from other manufacturers, such as EasyGuide (Keystone Dental, Burlington, MA, USA), Straumann codiagnostix (Straumann, Basel, Switzerland), VIP Software (BioHorizons, Birmingham, AL, USA), Implant Master (IDent, Foster City, CA, USA), and others are now available as well. Other implant manufacturers have developed instrument trays for the guided placement of their implants using the SimPlant software for implant planning (ie, Facilitate [AstraTech Dental, Molndal, Sweden], Navigator [Biomet 3i, Palm Beach Gardens, FL, USA], ExpertEase [Dentsply Friadent, Mannheim, Germany]). General technology concepts Using CT/CBCT scanners, the visualization of the height and width of available bone for implant placement, soft tissue thicknesses, proximity and root anatomy of adjacent teeth, the exact location of the maxillary sinuses, sinus septae, and other pertinent vital structures such as the mandibular canal, mental foramen, and incisive canal are possible [18 20]. Variations and aberrations of normal anatomy are also easily visualized. Once images are imported into proprietary software programs (SimPlant, NobelClinician, and so forth), the clinician can then virtually plan treatment for the placement of implants according to an individual patient s anatomy and case plan. The type and size of the planned implant, its position within the bone, its relationship to the planned restoration and adjacent teeth and/or implants, and its proximity to vital structures can be determined before performing surgery on a patient [18 22]. Surgical drilling guides can then be fabricated from the virtual treatment plan. These surgical guides are used by the clinician to place the planned implants in the same positions as those of the virtual treatment plan, allowing for more accurate and predictable implant placement [23 27] and reduced patient morbidity [28 31]. All of the current systems have similar restorative and surgical protocols. Upper and lower arch impressions are made, and a bite registration is obtained. Poured models are mounted on an articulator. Guided surgery requires reverse planning. The prosthodontist or restorative dentist first creates an ideal
3 COMPUTER-GUIDED DENTAL IMPLANTATION 55 restorative treatment plan, determining the planned tooth position by creating a diagnostic wax-up that indicates the exact anatomy and position of the teeth to be replaced. This ideal diagnostic wax-up is then incorporated, by a dental laboratory, into an acrylic prosthesis, referred to as a radiographic guide, scan prosthesis or scan appliance. Depending on the system to be used, this scan prosthesis can be a partial or full denture (Figs. 1 3.) Most systems, other than NobelClinician, require that the planned restorations contain a 20% to 30% barium sulfate mixture in the acrylic to allow for radiopacity of the planned restorations in the CT/CBCT images. NobelClinician uses a double-scan technique with a hard acrylic scan prosthesis and gutta percha markers as reference points, with no barium sulfate. According to the individual system protocols, the CT/CBCT scan is then taken with the patient wearing the scan prosthesis. The CT scan DICOM (Digital Imaging and Communication in Medicine) images are then imported into the various proprietary software programs (SimPlant, NobelClinician, EasyGuide, and so forth). The software programs are then used to virtually place implants into their ideal position related to the planned restoration and the underlying bony anatomy (Figs. 4 6.) The digital treatment plan is then downloaded to the manufacturer for fabrication of a surgical guide (Figs. 7 9). The surgical guide is used, with implant-specific drilling instrumentation, to precisely place the implants in the positions, depths, and angulations as planned virtually. Many CT-guided implant planning technologies require radiopaque fiducial reference markers to be placed in the scan prosthesis that the patient wears during the CT/CBCT scan. The software uses these reference markers to virtually position the scan appliance, and with it the parameters of the planned restoration(s), to the patient s jaw. The accurate assessment of these geometric markers can be difficult for some CBCT scanners and has the potential to add error into a precise planning system, ultimately leading to inaccurate fitting of surgical guides and error in implant placement. It is advisable to make every effort to investigate which CBCT scanners have high levels of accuracy or to use medical CT scanners when using these technologies [32]. Fig. 1. NobelGuide Radiographic Guide, fully edentulous. Modification of a patient s well-fitting existing denture. Fig. 2. SimPlant radiographic barium stent, partially edentulous.
4 56 ORENTLICHER et al Fig. 3. EZ Guide radiographic appliance, partially edentulous. Fig. 4. NobelGuide virtual treatment plan, fully edentulous. Fig. 5. SimPlant virtual treatment plan, partially edentulous.
5 COMPUTER-GUIDED DENTAL IMPLANTATION 57 Fig. 6. EZ Guide virtual treatment plan, partially edentulous. Fig. 7. NobelBiocare NobelGuide fabricated from treatment plan in Fig. 4. Fig. 8. SimPlant SurgiGuide fabricated from treatment plan in Fig. 5.
6 58 ORENTLICHER et al Fig. 9. EZ Guide fabricated from treatment plan in Fig. 6. Indications for use Because of its precision and accuracy in implant placement, an argument could be made for the use of CT-guided implant surgery in almost all cases. As with anything in medicine, a cost/time/ benefit determination must be made by the clinician, based on the circumstances of an individual case. In certain cases the increased patient and treatment planning time, the additional expense, and the additional radiation exposure to the patient may outweigh the clinical benefits. The authors have found that these technologies are most beneficial to the patient and the dental team in the following clinical circumstances. Three or more implants in a row Proximity to vital anatomic structures Problems related to the proximity of adjacent teeth Questionable bone volume Implant position that is critical to the planned restoration Flapless implant placement Multiple unit or full-arch immediate restorations, with or without extractions and immediate placement Significant alteration of the soft tissue or bony anatomy by prior surgery or trauma Patients with physical, medical, and psychiatric comorbidities. Conventional surgical guides to aid in implant positioning have been used in implant dentistry for many years. Guides of these types can be simple (ie, vacuform shells with the buccal or palatal/ lingual facings of the planned restorations) or more complex (ie, dental laboratory fabricated guides with 2-mm drill holes or metal tubes). The problem in their use is that there is no correlation in these appliances between the planned restoration and the underlying bony anatomy. This anatomic relationship can be predictably established and considered before surgery only with the use of 3D visualization and the use of computer-guided implant surgical guides. The fabrication of a surgical guide, used in implant treatment, is determined by the patient s anatomy and local references, such as the numbers and locations of teeth in the arch to be treated or in the opposing arch. Fewer anatomic references are present for the predictable accurate placement of implants as the length of the edentulous area increases. In a fully edentulous case, all local references are lost other than the soft tissue ridge and palate. Bone and soft tissue loss from periodontal disease and atrophy, long-term denture wear, and sinus pneumatization can make it difficult to predictably use a traditional surgical guide. In cases for which 3 or more implants in a row are planned, concepts of implant spacing and angulations, implant parallelism in all dimensions, proximity of implants to anatomic structures, and relationships between implant positions and the planned restorations are all significant considerations for the clinician. CT/CBCT-guided surgery allows for the ideal placement of multiple dental implants according to the planned restoration(s), the relationships of implants to surrounding anatomy, and principles of ideal prosthodontic implant positioning and spacing (Figs ).
7 COMPUTER-GUIDED DENTAL IMPLANTATION 59 Fig. 10. Lower right mandible, 3 implants in a row, virtual treatment plan. Fig. 11. Three implants in a row, NobelGuide in place. Note Implant Mounts with attached implants placed to depth. Fig. 12. Final posteroanterior radiograph. Note implant parallelism, different diameters and lengths, and spacing corresponding to the implant site and the planned restorations. Fig. 13. Final individual restorations, 3 implants in a row.
8 60 ORENTLICHER et al Differences in x-ray machines and radiographic techniques commonly lead to distortion of anatomic structures on conventional 2-dimensional images, such as elongation, shortening, stretching, and contraction. Accurate 3D evaluations and measurements of the relationship between a planned implant and the position of the mental nerve, inferior alveolar nerve (Figs. 14 and 15), nasopalatine/incisive nerve (Fig. 16), maxillary sinuses, and nasal floor (Fig. 17) are best visualized, evaluated, and measured using CT-generated images. In cases for which there are questions of nerve or sinus proximity related to the patient s available bone, implants are most accurately placed using computer-generated surgical guides. These technologies minimize potential patient morbidities. All proprietary implant planning software has the functionality to isolate the roots of teeth adjacent to the edentulous areas to aid in the accurate placement of implants between and adjacent to tooth roots in the planned sites. Some software will use virtual dots or lines to outline tooth roots (Fig. 18), whereas others have the ability to alter the software s sensitivity to Hounsfield units or isovalues to virtually remove bone from around tooth roots (known as segmentation) (Fig. 19). These technologies are most beneficial when implants must be placed in tight spaces because of close root proximities, or when tooth roots are in extremely divergent or convergent relationships. Surgical dilemmas that require implant placement in only one possible location or implant depth are common. Clinical scenarios frequently require the placement of implants into tight spaces with minimal bony leeway either mesial-distally, buccal-lingually, or both (see Fig. 16; Fig. 20). Tooth root proximities can require threading the needle with implant placement, a common problem with congenitally missing teeth. Scenarios of limited bone volume often leave situations in which the patient s anatomy dictates where the implant can be placed. Some of the most complex restorative and surgical cases treated in implant dentistry involve single and multiple implants in the esthetic zone. Thicknesses of crestal and buccal soft tissues and buccal and palatal cortical plates, buccal-lingual ridge dimensions, proximity to adjacent teeth, implant-toroot relationships, gingival and papilla support and contours, gingival exposure, smile lines, and implant angulations and emergence are just a few of the many complex considerations. Knowledge of the appropriate implant position based on the type of restoration planned (ie, cement or screw retained) is an important prosthetic-based consideration. Small variations in implant positions can lead to difficult restorative dilemmas in these cases. Proper implant position can be critical to the esthetic and functional success of the planned restoration. CT/CBCT-guided implant planning and placement allows for the evaluation and visualization of the ideal restoration for a site based on the surrounding bony and soft tissue anatomy. The virtual placement of implants based on the planned Fig. 14. Severe atrophy of posterior mandible, implant placement planned lingual to the inferior alveolar nerve.
9 COMPUTER-GUIDED DENTAL IMPLANTATION 61 Fig. 15. Three-dimensional reformation of Fig. 14. Note appearance of proximity between implant and inferior alveolar nerve in lateral view. Fig. 16. Implant placement planned in close proximity to enlarged nasopalatine canal. Fig. 17. Severe maxillary atrophy. Implant planned in the anterior nasal spine, in close proximity to the nasal floor.
10 62 ORENTLICHER et al Fig. 18. Outlining of tooth roots with virtual treatment planning. restoration related to the underlying bone is then performed. Surgical guides are then used to position the implants accurately and predictably into the optimal position for the planned restoration (Figs ). The time required from implant placement to loading has been dramatically reduced by implant technologies and surface characteristics in use today. Immediate placement and immediate loading of implants are now commonly performed. In some cases teeth can be extracted, implants can be placed immediately, and temporary crowns can be placed at the time of implant insertion. Concepts of crossarch stabilization and loading of multiple implants have changed the way cases are planned for treatment. Depending on the clinical circumstances and the experience and comfort level of the clinician, these technologies can be used to place single units, multiple units, or full arches of implants, with a tissue incision or flaplessly. Implants can be placed as a 2-stage, a single-stage with healing abutments, or as an immediate-placement/immediate-load case. Patients experience less surgical trauma, pain, and swelling while their recovery time is reduced and the ability to return to their normal lives is expedited [22 29]. Taking CT-guided technology to the next step involves the accurate fabrication of a restoration before implant insertion, with its immediate insertion at the time of surgery. After the virtual treatment plan is created by the clinician (Figs. 26 and 36), computer-generated stereolithographic surgical guides are fabricated by the manufacturer from the virtual treatment plan (Figs. 27 and 37). Using Fig. 19. Segmentation of images with virtual treatment planning.
11 COMPUTER-GUIDED DENTAL IMPLANTATION 63 Fig. 20. Implant virtually placed in location with limited buccal-palatal width. the fabricated surgical guide along with patient models, a dental laboratory then fabricates temporary, and in some cases final, restorations, before implant placement surgery (see Figs. 27, 28, 41, 42). The surgical guide can then be used to place implants flaplessly, only removing a core of tissue in the planned implant sites. Once the surgical guide is accurately secured in the patient s mouth it rarely is removed until all implants are inserted to the proper depth and direction (Figs. 29 and 38). Abutments can then be immediately placed on the implants, and temporary, or in some cases final, restorations can be inserted (see Figs and 32 49). In most circumstances, placing the implants where the bone is has become a concept from the past. Large and small soft tissue and connective tissue grafts, as well as sinus-lift grafts, block-bone grafts, ridge splitting, and alveolar distraction procedures are a few of the procedures routinely performed to prepare the recipient jaw sites before placing implants. Previous surgical procedures, including the prior placement of different types of dental implants (ie, blade and subperiosteal implants) can leave patients with challenging reconstructive bony defects (Figs ). Traumatic injuries or benign or malignant pathology can result in the loss of bone, teeth, and soft tissue, with resultant defects of varying sizes. Reconstructive procedures to treat these defects can leave areas of abnormal bony anatomy and scarred soft tissue. Bone and soft tissue volumes can be Fig. 21. A 17-year-old female patient with overretained, maxillary right primary canine and lateral incisors, and congenitally missing right canine and bilateral lateral incisors and second premolars. Preoperative grafting procedures were necessary to prepare each site for dental implants. Preoperative photo.
12 64 ORENTLICHER et al Fig. 22. Virtual treatment plan for the patient described in Fig. 21. Fig. 23. Virtual treatment plan, occlusal view, for the patient described in Fig. 21. Note implant planned in the right canine site for 2-unit cantilever bridge anteriorly. Fig. 24. Final restorations for the patient described in Fig. 21.
13 COMPUTER-GUIDED DENTAL IMPLANTATION 65 Fig. 25. A 20-year-old man with bilateral maxillary central incisors avulsed traumatically. Treatment was done using Astra- Tech Dental Facilitate technology. 20 year old male, preoperative photo. Fig. 26. Treatment of the patient described in Fig. 25. Facilitate virtual treatment plan. Fig. 27. Treatment of the patient described in Fig. 25. Presurgical laboratory placement of implant analogs into the Facilitate surgical guide, before pouring stone into the guide for fabrication of a master model. Fig. 28. Treatment of the patient described in Fig. 25. Presurgical fabrication of provisional restorations on the poured master model.
14 66 ORENTLICHER et al Fig. 29. Treatment of the patient described in Fig. 25. Guided osteotomy preparation using the Facilitate instrumentation. Fig. 30. Treatment of the patient described in Fig. 25. Implants inserted, temporary restoration placed at the time of surgery. Fig. 31. Treatment of the patient described in Fig. 25. Final restorations in place, 5 months later. Fig year old male, partially edentulous mandible. Case treatment planned for immediate extraction, immediate implant placement, and immediate loading with a provisional restoration. Preoperative panoramic radiograph.
15 COMPUTER-GUIDED DENTAL IMPLANTATION 67 Fig. 33. Treatment of the patient described in Fig. 32. Preoperative clinical photo, mandibular ridge. Fig. 34. Treatment of the patient described in Fig. 32. Multiple piece Radiographic Guide. Fig. 35. Treatment of the patient described in Fig. 32. Mandibular Radiographic Guide and Radiographic Index in place at time of CT scan.
16 Fig. 36. Treatment of the patient described in Fig. 32. Virtual treatment plan, immediate extraction, 8 implant placement planned. Fig. 37. Treatment of the patient described in Fig. 32. NobelGuide planned from virtual treatment plan in Fig. 36. Fig. 38. Treatment of the patient described in Fig. 32. Osteotomy drilling through the NobelGuide, using NobelGuide for NobelActive surgical instrumentation.
17 COMPUTER-GUIDED DENTAL IMPLANTATION 69 Fig. 39. Treatment of the patient described in Fig. 32. Clinical photo, minimally traumatic extractions with implants in place. Fig. 40. Treatment of the patient described in Fig. 32. Postoperative panoramic radiograph. Fig. 41. Treatment of the patient described in Fig. 32. Master cast fabricated from NobelGuide, Quick Temp abutments with nylon pick up sleeves in place. Fig. 42. Treatment of the patient described in Fig. 32. Fabrication of provisional restoration on master cast.
18 70 ORENTLICHER et al Fig. 43. Treatment of the patient described in Fig. 32. Provisional restoration, pick up of nylon Quick Temp sleeves. Six implants incorporated in provisional restoration. Fig. 44. Treatment of the patient described in Fig. 32. Provsional restoration in place, occlusal view. Fig. 45. Treatment of the patient described in Fig. 32. Master cast, planned occlusion with provisional restoration, frontal view. Fig. 46. Treatment of the patient described in Fig. 32. Provisional restoration in place at time of surgery, frontal view.
19 COMPUTER-GUIDED DENTAL IMPLANTATION 71 Fig. 47. Treatment of the patient described in Fig. 32. Final restoration, frontal view. Fig. 48. Treatment of the patient described in Fig. 32. Final restoration, right side. Fig. 49. Treatment of the patient described in Fig. 32. Final restoration, left side. Fig. 50. Preoperative panoramic radiograph of a 45-year-old woman who had a blade implant placed in the left mandible in 2003, resulting in multiple infections and implant and bridge loosening. After implant removal, osseointegrated implants were planned for mandibular right and left sides.
20 72 ORENTLICHER et al Fig. 51. Treatment of the patient described in Fig. 50. Defect of the left mandible after removal of blade implant and restoration. Fig. 52. Treatment of the patient described in Fig. 50. Virtual treatment plan, 3 implants in the left mandible. Fig. 53. A 68-year-old woman with prior full-arch maxillary subperiosteal implant. Note severe atrophy and distorted anatomy.
21 COMPUTER-GUIDED DENTAL IMPLANTATION 73 Fig. 54. Virtual treatment plan for the patient described in Fig. 53. Four implants were planned for overdenture restoration. unpredictable after healing, graft maturation, and settling of graft materials. Lateral block-onlay grafts can resorb a portion of their bone volume during healing and maturation [33 35]. CT/ CBCT-guided technologies allow the surgeon to predict the volume of sinus-lift graft material necessary to augment an area of the maxilla to a desired height of bone [36]. Newer technologies are being investigated and developed in which customized block-bone grafts can be created after evaluating bony defects from CT/CBCT data. Using these technologies allows for the visualization and evaluation of a patient s distorted anatomy without making an incision or removing any soft tissue or bone [37]. Implants can be placed accurately and predictably with knowledge of the patient s underlying distorted bony anatomy, without making an incision and removing the periosteal blood supply from the areas (Figs ). Compromised patients Preoperative and postoperative radiation therapy potentially alters healing capacity in head and neck cancer patients. To increase bone vascularity before implant placement, the literature advocates Fig. 55. A 32-year-old man with severe atrophy of anterior maxilla resulting from a sports injury. Preoperative cross-sectional image in area of the right lateral incisor (SimPlant). Note measurements revealing deficiencies of bone in all dimensions.
22 74 ORENTLICHER et al Fig. 56. Postgrafting cross-sectional image of the patient described in Fig. 55. Area of right lateral incisor after maxillary anterior distraction osteogenesis and lateral block grafts (NobelGuide). Note measurements of 13.0 mm (height) and 9.6 mm (width). preoperative and postoperative courses of hyperbaric oxygen therapy in these patients [38 41]. Minimizing flap elevation and hard and soft tissue trauma is indicated in these patients to minimize the likelihood of the development of osteoradionecrosis of the jaws [38,42]. Bleeding, swelling, and alteration of the blood supply to the bone and soft tissue are limited by using CT Guided implant placement technologies [43]. Fig. 57. Cross-sectional view after sinus-lift graft. Note bone graft placement primarily laterally, virtual implant placed in image.
23 COMPUTER-GUIDED DENTAL IMPLANTATION 75 Fig. 58. Three-dimensional reconstruction of left mandible, after Ameloblastoma resection and iliac crest reconstruction. Virtual treatment plan, 4 implants. Patients with medical problems such as bleeding dyscrasias, anticoagulation issues, or significant cardiovascular disease may necessitate specific medication protocols that cannot be altered presurgically. Minimizing bleeding by limiting surgical trauma to the soft and hard tissues is indicated in patients with difficult medical management issues. 3D implant evaluation and planning with CT-guided implant placement allows for flapless, minimally traumatic, accurate implant placement, an indication for use in patients with these challenging medical management problems. Procedures that require long periods in a dental chair can prevent some patients from seeking treatment because of extreme levels of anxiety, stress, and phobias. The amount of time a patient can sit in a dental chair can be limited by orthopedic and spinal disorders. Wheelchair-bound patients pose another set of logistical treatment problems. These types of patients can require extensive planning and preparation before treatment. Without compromising quality, treatment must be performed quickly and efficiently. Computer-generated implant planning allows for the preoperative visualization of most of the potential planning and anatomic issues that may be encountered during surgery, all before the patient sits in the dental chair. By using surgical guides to place the implants, implants can be placed quickly and predictably, thus minimizing the patient s stress, pain, and time in the dental chair. Discussion Three types of computer-generated surgical guides are currently available: tooth supported, mucosa supported, and bone supported. Tooth-supported guides are used in partially edentulous cases. The surgical guide is designed to rest on other teeth in the arch for accuracy of guide fit. Mucosal-supported guides are designed to rest on the mucosa and are primarily used in fully edentulous cases. Accurate interarch bite registrations are of utmost importance when using these guides to assure accurate surgical guide positioning and placement of securing screws or pins before the placement of implants (see Figs. 37 and 38). Bone-supported guides can be used in partially or fully edentulous cases, but are used primarily in fully edentulous cases when significant ridge atrophy is present and good seating of a mucosa-supported guide will be questionable. An extensive fullthickness flap is necessary when using bone-supported guides to expose the bone in the planned implant sites and in the adjacent areas for full stable seating of the guide over the bony ridge. At this time, only SimPlant (Materialise) manufactures bone-supported surgical guides. Dental implant placement using CT-guided surgery with drill guides is known to enhance safety compared with the freehand technique [44,45] while being compatible with conventional flap elevation surgery or flapless procedures [46] According to the NobelGuide protocol, when using the Guided Abutment to secure the immediate restoration, the accuracy should be sufficient for inserting a prefabricated final restoration at the time of implant surgery. No available CT-guided drill guide technology exists today that has absolute precision. All articles on stereolithographic guides show error in all dimensions between virtual planning and actually obtained implant positions [47]. According to the literature, implants placed by mucosa-supported guides have the lowest mean deviations whereas implants placed by bone-supported guides have higher deviations [48]. Toothsupported guides have been found to have the lowest measured deviation, likely because there are
24 76 ORENTLICHER et al teeth present in the arch acting as accurate stops for guide placement [49]. A single guide, using metal guide sleeves and rigid screw or pin fixation with specific drilling instrumentation, further minimizes error. Most systems use these fixation techniques to stabilize mucosal-supported guides; some use them to stabilize all guides. A reduction in treatment time is the main advantage of inserting a final restoration immediately after implant placement. Clinicians who are using these technologies more commonly place temporary restorations after implant placement for many reasons. An accurate prediction of the contours and anatomy of the healed gingiva is impossible, whether a procedure is flapless or not. This issue is a significant one for a laboratory technician fabricating a final restoration. The patient s aesthetic demands can sometimes be great. Observation of the tissue response to the temporary restoration can give the restorative dentist invaluable information regarding the gingival contours and aesthetics in preparation for the final restoration. In addition, a small number of implant failures occur, regardless of whether an implant is placed guided or nonguided. Most surgery-related implant failures typically occur within the first 3 to 4 months after placement. Management of an implant failure, both surgically and restoratively, is best done before insertion of the final restoration. According to Abrahamsson and colleagues [50], changing from a healing abutment to a permanent abutment did not result in a change in the dimension and quality of the transmucosal attachment that developed, and did not differ from the mucosal barrier that formed to a permanent abutment placed after surgery. In addition, an acrylic occlusal surface or a composite restoration has been found to have better shock-absorbing behavior and to reduce the forces of impact when compared with ceramic materials [51]. These factors are all additional reasons to place immediate acrylic temporary restorations rather than immediate final porcelain restorations. SimPlant (Materialise) and NobelGuide/NobelClinician (NobelBiocare) are the 2 major systems currently in use. Clinically the NobelGuide system is a more comprehensive one, with full sets of specific instrumentation for the fully guided placement of all NobelBiocare implants to accurate position, depth, and angulation, and the components to immediately load implants if desired. NobelGuide and 3i Navigator are the only systems currently available with instrumentation for the placement of tapered implants. The NobelGuide technology and instrumentation can be used for performing osteotomies for a straight-walled implant from any implant manufacturer. In these cases, the system can only be used for depth and direction of osteotomies. Because the NobelGuide Implant Mounts are designed only for NobelBiocare implants, implants from other manufacturers cannot be accurately placed and fully guided. In these cases, the depth of implant placement should be evaluated with the guide off, usually after an incision and tissue-flap elevation. SimPlant is designed as an open system for all implant systems. Although this feature increases its functionality, it is also a limitation because it is not perfectly adapted to one implant system in a comprehensive manner. Some clinicians believe that the SimPlant software currently is more intuitive and easier to learn. Several implant manufacturers have recently developed and marketed instrumentation specific for the placement of their straight-walled implants, flapless and fully guided, using the SimPlant software for planning (eg, Facilitate [AstraTech Dental], ExpertEase [Dentsply Friadent], Navigator [3i/Biomet]). Other manufacturers have developed nonstereolithographic model technologies for the fabrication of surgical guides as well (eg, IDent [Foster City, CA, USA], EZ Guide [Keystone Dental, Burlington, MA, USA], Straumann codiagnostix [Straumann, Basel, Switzerland]). In these technologies, the surgical guide is created by scanning the patient while he or she is wearing a barium radiographic appliance, the implant position(s) are then planned virtually, and then the surgical guide is created by milling the radiographic appliance according to the digital CT-based treatment plan. Guide sleeves are then added to the guide to accomodate the instrumentation for osteotomies and guided implant placement. Maximizing patient comfort by minimizing traumatic injury to the tissues is the rationale for using minimally invasive procedures. Flapless insertion of dental implants has been found to have success rates comparable with conventional implant placement, while minimizing potential complications from soft tissue elevation such as infection, dehiscence, and soft and hard tissue necrosis [30,52,53]. Surgical guidance for drill depth and angulation, in combination with a flapless technique, minimizes the potential injury to underlying anatomic structures during the implant osteotomy preparation. Fully flapless surgery is not advised in most SimPlant cases because fully guided instrumentation for implant insertion is not available. Depth and angulation guidance of all osteotomies is possible, but accurate implant platform placement will require direct visualization of the bone, necessitating an incision and elevation of a flap. If using Navigator, ExpertEase, Facilitate, or SimPlant-fabricated NobelGuide compatible
25 COMPUTER-GUIDED DENTAL IMPLANTATION 77 surgical guides, fully guided and flapless placement of implants is possible because of available instrumentation. CT-based technologies available today have limitations and questions that require further investigation regarding their effect on guided surgery outcomes. The resolution and accuracy of specific CBCT machines compared with the gold standard of medical-grade CT scanners has been questioned [54]. A calibration object is marketed by NobelBiocare, which calibrates an individual CBCT/CT machine to an acrylic object of a known contour and density specifically for the NobelGuide protocol. This object adds to the precision of the stereolithographic fabrication of the NobelGuide [55]. The manufacture of a stereolithographic surgical guide or model involves reproducing the digitally planned dimensions of the surgical guide or model by using a laser beam to selectively solidify an ultraviolet-sensitive liquid resin. Stereolithographic materials have inherent potential problems that can lead to light sensitivity and expansion and/or shrinkage of the material. Leaving them exposed to light for extended periods of time, as well as sterilization in high-temperature autoclaves, will distort stereolithographic materials. The literature concludes that preparation of the implant site using surgical drill guides generates more heat than classic implant-site preparation, regardless of the irrigation system used [56]. Summary New technologies based on the 3D evaluation of patients for dental implants have opened new avenues to clinicians for accurate and predictable diagnosis, planning, and treatment in a multidisciplinary patient-based approach. Communication between clinicians and understanding these technologies are key components of improved case results and clinical outcomes. Analyzing, understanding, and possibly adopting future technologies will not only benefit and open new doors for the dental team but will benefit patients, with more improved predictable outcomes. The use of CT-guided implant planning and placement does not separate the surgical and restorative team from diligent adherence to the basic principles of oral and implant surgery and prosthetic implant dentistry. Well-established concepts of implant spacing, depth and angulation, case planning and engineering, minimally traumatic manipulation of soft and hard tissues, soft tissue and bone grafting, osseointegration times, soft and hard tissue healing, heat generation, dental materials, ideal occlusion, and many others must be maintained and adhered to. CT-guided implant surgery facilitates the placement of dental implants into an ideal position according to a restoratively driven treatment plan. Essentially, the final tooth position is determined first. The implant position is then planned and placed into that ideal position related to the restoration, with accuracy and precision. Treatment plans should be created according to the requirements of an individual case and the comfort level of the surgical and restorative team. Cases can be treated with implants buried with cover screws and staged, with healing abutments, or immediately loaded with temporary, or in some circumstances, final restorations. Proper case selection and patient awareness, education, and compliance are all critical factors for success. It must be understood that a steep learning curve is necessary for the successful integration of CT technology and CT-guided surgery into dental implant practice. Clinicians interested in these technologies are strongly encouraged to pursue continuing education on the technologies before their clinical use. CT-guided implant surgery is not conventional implant surgery. Knowledge of CT scans, proprietary treatment planning software, the complete treatment process protocols, and guidedsurgery instrumentation and techniques are all instrumental to successful treatment outcomes. In addition, clinicians should take into consideration the inherent additional costs involved in the use of the proprietary software and computer-aided design and manufacturing processing technologies. Of primary importance, good patient selection and diagnosis, pretreatment planning, knowledge of the technology, and adherence to surgical and prosthetic principles will strongly affect clinical outcomes. References [1] Mozzo P, Procacci C, Tacconi A, et al. A new volumetric CT machine for dental imaging based on the cone beam technique: preliminary results. Eur Radiol 1998;8:1558.
26 78 ORENTLICHER et al [2] Mah J, Hatcher D. Three dimensional craniofacial imaging. Am J Orthod Dentofacial Orthop 2004;126:308. [3] Hashimoto K, Yoshinori A, Kazui I, et al. A comparison of a new, limited cone beam computed tomography machine for dental use with a multi-detector row helical CT machine. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005;95:371. [4] Sukovic P. Cone beam computed tomography in craniofacial imaging. Orthod Craniofac Res 2003;6(Suppl 1):31. [5] Yu L, Vrieze TJ, Bruesewitz MR, et al. Dose and image quality evaluation of a dedicated cone-beam CT system for highcontrast neurologic applications. Am J Roentgenol 2010;194:W193. [6] Yamashina A, Tanimoto K, Sutthiprapaporn P, et al. The reliability of computed tomography (CT) values and dimensional measurements of the oropharyngeal region using cone beam CT: comparison with multidetector CT. Dentomaxillofac Radiol 2008;37:245. [7] Flicek K, Hara A, Silva A, et al. Reducing the radiation dose for CT colonography using adaptive statistical iterative reconstruction: a pilot study. Am J Roentgenol 2010;195: [8] Silva A, Lawder H, Hara A, et al. Innovations in CT dose reduction strategy: application of the adaptive statistical iterative reconstruction algorithm. Am J Roentgenol 2010;194: [9] Leipsic J, LaBounty T, Heilbron B, et al. Estimated radiation dose reduction using adaptive statistical iterative reconstruction in coronary CT angiography: the ERASIR study. Am J Roentgenol 2010;195: [10] Sagara Y, Hara A, Pavlicek W, et al. Abdominal CT: comparison of low-dose CT with adaptive statistical iterative reconstruction and routine-dose CT with filtered back projection in 53 patients. Am J Roentgenol 2010;195: [11] Liang X, Lambrichts I, Sun Y, et al. A comparative evaluation of cone beam computed tomography (CBCT) and multislice CT (MSCT). Part II: on 3D model accuracy. Eur J Radiol 2010;75: [12] Loubele M, Maes F, Schutyser F, et al. Assessment of bone segmentation quality of cone beam CT versus multislice spiral CT: a pilot study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006;102: [13] Rothman SL, Chaftez N, Rhodes ML, et al. CT in the preoperative assessment of the maxilla and mandible for endosseous implant surgery. Radiology 1988;169(2):581. [14] Casselman JW, Deryckere F, Hermans R, et al. Denta Scan: CT software program used in the anatomic evaluation of the mandible and maxilla in the perspective of endosseous implant surgery. Rofo 1991;155(1):4 10. Available at: Accessed December 31, [15] Villari N, Fanfani F. Diagnostic contribution of CT in implantology: use of a new Denta-Scan reconstruction program. Radiol Med 1992;83(5): [16] Tal H, Moses O. A comparison of panoramic radiography with computed tomography in the planning of implant surgery. Dentomaxillofac Radiol 1991;20(1):40 2. [17] Available at: Web history-about CSI. Accessed December 31, [18] Ramez J, Donazzan M, Chanavaz M, et al. The contribution of scanner imagery in implant surgery and sinus overflow using frontal oblique orthogonal reconstruction. Rev Stomatol Chir Maxillofac 1992;93: [19] Pattijn V, van Cleynenbreugel T, vander Sloten J, et al. Structural and radiological parameters for the nondestructive characterization of trabecular bone. Ann Biomed Eng 2001;29: [20] Sonick M, Abrahams J, Faiella R. A comparison of the accuracy of periapical, panoramic, and computerized tomographic radiographs in locating the mandibular canal. Int J Oral Maxillofac Implants 1994;9(4): [21] Todd A, Gher M, Quintero G, et al. Interpretation of linear and computed tomograms in the assessment of implant recipient sites. J Periodontol 1993;64: [22] Gehr ME, Richardson AC. The accuracy of dental radiographic techniques used for evaluation of implant fixture placement. Int J Periodontics Restorative Dent 1995;15: [23] vansteenberghe D, Glauser R, Blombäck U, et al. A computed tomographic scan derived customized surgical template and fixed prosthesis for flapless surgery and immediate loading of implants in fully edentulous maxillae. A prospective multicenter study. Clin Implant Dent Relat Res 2005;7(Suppl 1):S [24] Tardieu P, Vrielinck L. Implantologie assistée par ordinateur: le propramme SimPlant/SurgiCaseÔ et le SAFE SystemÔ mis en charge immediate d un bridge mandibulaire avec des impalt transmuqueux. Implant 2003;9: [25] Rosenfeld AL, Mandelaris GA, Tardieu PB. Prosthetically directed implant placement using computer software to ensure precise placement and predictable prosthetic outcomes. Part 3: stereolithographic drilling guides that do not require bone exposure and the immediate delivery of teeth. Int J Periodontics Restorative Dent 2006;26:493. [26] Vrielinck L, Politis C, Schepers S, et al. Image-based planning and clinical validation of zygoma and pterygoid implant placement in patients with severe bone atrophy using customized drill guides. Preliminary results from a prospective clinical follow-up study. Int J Oral Maxillofac Surg 2003;32:7 14. [27] Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants 2003;18: [28] Hahn J. Single stage, immediate loading, and flapless surgery. J Oral Implantol 2000;26: [29] Campelo LD, Dominguez Camara JR. Flapless implant surgery: a 10 year clinical retrospective analysis. J Oral Maxillofac Implants 2002;17: [30] Becker W, Goldstein M, Becker BE, et al. Minimally invasive flapless implant surgery: a prospective multicenter study. Clin Implant Dent Relat Res 2005;7(Suppl 1):S21 7. [31] Becker W, Wikesjo UM, Sennerby L, et al. Histologic evaluation of implants following flapless and flapped surgery: a study in canines. J Periodontol 2006;77: [32] Abboud M, Wahl G. Clinical benefits, risks, accuracy of cone beam CT based guided implant placement. Clin Oral Implants Res 2009;20:909. [33] Johansson B, Grepe A, Wannfors K, et al. A clinical study of changes in the volume of bone grafts in the atrophic maxilla. Dentomaxillofac Radiol 2001;30(3):
27 COMPUTER-GUIDED DENTAL IMPLANTATION 79 [34] Verhoeven JW, Ruijter J, Cune MS, et al. Onlay grafts in combination with endosseous implants in severe mandibular atrophy; one year s results of a prospective, quantitative radiological study. Clin Oral Implants Res 2000;11(6): [35] Smolka W, Eggensperger N, Carollo V, et al. Changes in the volume and density of calvarial split bone grafts after alveolar ridge augmentation. Clin Oral Implants Res 2006;17(2): [36] Krennmair G, Krainhofner M, Maier H, et al. Computerized tomography-assisted calculation of sinus augmentation volume. Int J Oral Maxillofac Implants 2006;21(6): [37] Orentlicher GP, Goldsmith DH, Horowitz A. Thinking out of the box the use of virtual implant treatment planning and surgery in challenging cases. Inside Dentistry 2008;4(6): [38] Marx RE. Osteoradionecrosis: a new concept of its pathophysiology. J Oral Maxillofac Surg 1983;41:283. [39] Marx RE, Ames JR. The use of hyperbaric oxygen therapy in bony reconstruction of the irradiated and tissue-deficient patient. J Oral Maxillofac Surg 1982;40: [40] Granstrom G. Placement of dental implants in irradiated bone: the case for using hyperbaric oxygen. J Oral Maxillofac Surg 2006;64: [41] Granstrom G. Radiotherapy, osseointegration, and hyperbaric oxygen therapy. Periodontol ;33:245. [42] Koga DH, Salvajoli JV, Alves FA. Dental extractions and radiotherapy in head and neck oncology: review of the literature. Oral Dis 2008;14:40 4. [43] Horowitz AD, Orentlicher GP, Goldsmith DH. Case report computerized implantology: for the irradiated patient. J Oral Maxillofac Surg 2009;67: [44] Komiyama A, Pettersson A, Hultin M, et al. Virtually planned and template-guided implant surgery: an experimental model matching approach. Clin Oral Implants Res 2010;22: [45] Wagner A, Wanschitz F, Birkfellner W, et al. Computer-aided placement of endosseous oral implants in patients after ablative tumour surgery: assessment of accuracy. Clin Oral Implants Res 2003;14: [46] Casap N, Tarazi E, Wexler A, et al. Intraoperative computerized navigation for flapless implant surgery and immediate loading in the edentulous mandible. Int J Oral Maxillofac Implants 2005;20:92 8. [47] D Haese J, Van De Velde T, Komiyama A, et al. Accuracy and complications using computer-designed stereolithographic surgical guides for oral rehabilitation by means of dental implants: a review of the literature. Clin Implant Dent Relat Res [Epub ahead of print]. DOI: /j x. [48] Arisan V, Karabuda ZC, Ozdemir T. Accuracy of two stereolithographic guide systems for computer-aided implant placement: a computed tomography-based clinical comparative study. J Periodontol 2010;81: [49] Ozan O, Turkyilmaz I, Ersoy AE, et al. Clinical accuracy of 3 different types of computed tomography-derived stereolithographic surgical guides in implant placement. J Oral Maxillofac Surg 2009;67: [50] Abrahamsson I, Berglundh T, Sekino S, et al. Tissue reactions to abutment shift: an experimental study in dogs. Clin Implant Dent Relat Res 2003;5:82 8. [51] Gracis SE, Nicholls JI, Chalupnik JD, et al. Shock-absorbing behavior of five restorative materials used on implants. Int J Prosthodont 1991;4: [52] Arisan V, Karabuda CZ, Ozdemir T. Implant surgery using bone- and mucosa-supported stereolithographic guides in totally edentulous jaws: surgical and post-operative outcomes of computer-aided vs. standard techniques. Clin Oral Implants Res 2010;21: [53] Cannizzaro G, Torchio C, Leone M, et al. Immediate versus early loading of flapless-placed implants supporting maxillary full-arch prostheses: a randomised controlled clinical trial. Eur J Oral Implantol 2008;1: [54] Van Assche N, van Steenberghe D, Guerrero ME, et al. Accuracy of implant placement based on pre-surgical planning of three-dimensional cone-beam images: a pilot study. J Clin Periodontol 2007;34: [55] Wouters V, Mollemans W, Schutyser F. Calibrated segmentation of CBCT for digitization of dental prostheses. Int J Comput Assist Radiol Surg 2011;6(5): Doi: /s [Epub 2011 May 3]. [56] Misir AF, Sumer M, Yenisey M, et al. Effect of surgical drill guide on heat generated from implant drilling. J Oral Maxillofac Surg 2009;67:
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
How To Plan A Dental Implant With A 3D Image Based Program
 J Oral Maxillofac Surg 62:41-47, 2004, Suppl 2 Interactive Imaging for Implant Planning, Placement, and Prosthesis Construction Stephen M. Parel, DDS,* and R. Gilbert Triplett, DDS, PhD Purpose: This review
J Oral Maxillofac Surg 62:41-47, 2004, Suppl 2 Interactive Imaging for Implant Planning, Placement, and Prosthesis Construction Stephen M. Parel, DDS,* and R. Gilbert Triplett, DDS, PhD Purpose: This review
Luigi Vito Stefanelli,D.Eng.,DDS
 LYON, 27-28/09/2013 Luigi Vito Stefanelli,D.Eng.,DDS Assistant Researcher, Department of Oral Sciences, Sapienza University of Rome, Italy, School of Dentistry. Private practitioner dental office Stasi
LYON, 27-28/09/2013 Luigi Vito Stefanelli,D.Eng.,DDS Assistant Researcher, Department of Oral Sciences, Sapienza University of Rome, Italy, School of Dentistry. Private practitioner dental office Stasi
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
While the prosthetic rehabilitation of
 Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT
 Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT Introduction A 58 year old male had been missing teeth #7=12 for approximately 28 years. During
Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT Introduction A 58 year old male had been missing teeth #7=12 for approximately 28 years. During
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Accelerated Patient Rehabilitation
 Accelerated Patient Rehabilitation Providing The Tools Necessary For An Immediate Solution: NanoTite Implants QuickBridge Provisional Components Navigator System For CT Guided Surgery Initial Patient Presentation
Accelerated Patient Rehabilitation Providing The Tools Necessary For An Immediate Solution: NanoTite Implants QuickBridge Provisional Components Navigator System For CT Guided Surgery Initial Patient Presentation
VOL. XX, NO. X. Dr. Leo Malin Erases Challenges of Implant Dentistry
 Xxxxxxx Wisconsin xxxxx Edition Edition Xxxxxx 2004 VOL. XX, NO. X Dr. Leo Malin Erases Challenges of Implant Dentistry Dr. Leo Malin Brings Cutting-Edge CT Technology Right to Dentists Doorsteps By Jeff
Xxxxxxx Wisconsin xxxxx Edition Edition Xxxxxx 2004 VOL. XX, NO. X Dr. Leo Malin Erases Challenges of Implant Dentistry Dr. Leo Malin Brings Cutting-Edge CT Technology Right to Dentists Doorsteps By Jeff
Dr. Little received his doctorate degree in dentistry from UT Health at San Antonio Dental
 Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
All-on-4 treatment concept with NobelSpeedy Groovy
 All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
Cone Beam Implant Planning Manual
 Cone Beam Implant Planning Manual (Everything you want to know about CBCT planning) Page 2 Overview & Guide Selection Criteria Page 3 Scan Appliance basics When are they required? Page 4 Scan Appliance
Cone Beam Implant Planning Manual (Everything you want to know about CBCT planning) Page 2 Overview & Guide Selection Criteria Page 3 Scan Appliance basics When are they required? Page 4 Scan Appliance
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Abutment fracture in a bridge supported by natural teeth and implants
 Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
 Users Group Meeting 2011 Northeastern Society of Orthodontists 89th Annual Meeting November 11-14, 2010 Hilton Montréal Bonaventure Montréal, Quebec, Canada 14 Lecture Schedule Saturday continued w Doctor
Users Group Meeting 2011 Northeastern Society of Orthodontists 89th Annual Meeting November 11-14, 2010 Hilton Montréal Bonaventure Montréal, Quebec, Canada 14 Lecture Schedule Saturday continued w Doctor
A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading
 A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading Fredrik Ahlgren, DDS, MSc 1 / Kjell Størksen, DDS 2 /Knut Tornes, DDS, PhD 3 Purpose: The purpose of this study was
A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading Fredrik Ahlgren, DDS, MSc 1 / Kjell Størksen, DDS 2 /Knut Tornes, DDS, PhD 3 Purpose: The purpose of this study was
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Prosthodontist s Perspective
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANTS IN FOCUS. Endosseous dental implant restorations PLANNING FOR IMPLANT RESTORATIONS
 IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
E. Richard Hughes, D.D.S.
 E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 [email protected] Diplomate,
E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 [email protected] Diplomate,
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Full Mouth Restoration with Screw-Retained Zirconia Bridges
 Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
 Step-by-Step Virtual Implant Planning MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed
Step-by-Step Virtual Implant Planning MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed
Nobel Clinician - Quick Guide
 1220 E. Birch St. #201 Brea, CA 92821 (800)750-5004 Haupt Dental Lab Inc. Nobel Clinician - Quick Guide Step #1 - Diagnostics Make impressions of both the upper and lower arches using custom trays. Care
1220 E. Birch St. #201 Brea, CA 92821 (800)750-5004 Haupt Dental Lab Inc. Nobel Clinician - Quick Guide Step #1 - Diagnostics Make impressions of both the upper and lower arches using custom trays. Care
BioHorizons Education Programme 2015
 BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
CAD/CAM technology supporting successful implant therapy
 CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Single anterior tooth replacement: clinical approaches
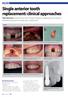 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation
 Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
forrest avenue d e n t a l c e n t r e
 Implant Treatment FAQ IMPLANT TREATMENT: FREQUENTLY ASKED QUESTIONS WHAT ARE DENTAL IMPLANTS? Dental implants are titanium rods that are surgically placed in your jaw bone which will subsequently support
Implant Treatment FAQ IMPLANT TREATMENT: FREQUENTLY ASKED QUESTIONS WHAT ARE DENTAL IMPLANTS? Dental implants are titanium rods that are surgically placed in your jaw bone which will subsequently support
Implant rehabilitation in the edentulous jaw: the All-on-4 immediate function concept
 Implant rehabilitation in the edentulous jaw: the All-on-4 immediate function concept By Christopher CK Ho, BDS (Hons), Grad.Dip.Clin.Dent (Implants), M.Clin.Dent (Pros) The All-on-4 technique involves
Implant rehabilitation in the edentulous jaw: the All-on-4 immediate function concept By Christopher CK Ho, BDS (Hons), Grad.Dip.Clin.Dent (Implants), M.Clin.Dent (Pros) The All-on-4 technique involves
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration
 Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Ando A., Nakamura Y., Kanbara R., Kumano H., Miyata T., Masuda T., Ohno Y. and Tanaka Y.
 11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
ATLANTIS abutments design guide CAD/CAM patient-specific abutments
 ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software
 Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software XCPT Patient Engagement System was developed and engineered to combine scientific research relating to the brain s ability
Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software XCPT Patient Engagement System was developed and engineered to combine scientific research relating to the brain s ability
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
SURGICAL MANUAL. Step By Step Techniques
 SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
Virtual Planning for Dental Implant Placement Using Guided Surgery
 18 Virtual Planning for Dental Implant Placement Using Guided Surgery Vinicius Nery Viegas, Celso Gustavo Schwalm Lacroix, Rogério Miranda Pagnoncelli and Marília Gerhardt de Oliveira Pontifícia Universidade
18 Virtual Planning for Dental Implant Placement Using Guided Surgery Vinicius Nery Viegas, Celso Gustavo Schwalm Lacroix, Rogério Miranda Pagnoncelli and Marília Gerhardt de Oliveira Pontifícia Universidade
GUIDELINES. Educational Requirements & Professional Responsibilities for Implant Dentistry CONTENTS. The Guidelines of the Royal College of
 Educational Requirements & Professional GUIDELINES Approved by Council May 2013 This is replacing the document last published in August 2002. Educational Requirements & Professional The Guidelines of the
Educational Requirements & Professional GUIDELINES Approved by Council May 2013 This is replacing the document last published in August 2002. Educational Requirements & Professional The Guidelines of the
The definitive implant restoration
 CASE REPORT Implant Bone Rings. One-Stage Three-Dimensional Bone Transplant Technique: A Case Report Mark R. Stevens, DDS 1 * Hany A. Emam, MS 2 Mahmoud E. L. Alaily, MS 3 Mohamed Sharawy, PhD 4 A variety
CASE REPORT Implant Bone Rings. One-Stage Three-Dimensional Bone Transplant Technique: A Case Report Mark R. Stevens, DDS 1 * Hany A. Emam, MS 2 Mahmoud E. L. Alaily, MS 3 Mohamed Sharawy, PhD 4 A variety
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
CAD/CAM Technology in Implant Dentistry
 Chapter 7 CAD/CAM Technology in Implant Dentistry Ilser Turkyilmaz, Caroline Corrigan Eskow and Gokce Soganci Additional information is available at the end of the chapter http://dx.doi.org/10.5772/59322
Chapter 7 CAD/CAM Technology in Implant Dentistry Ilser Turkyilmaz, Caroline Corrigan Eskow and Gokce Soganci Additional information is available at the end of the chapter http://dx.doi.org/10.5772/59322
The Mandibular Two-Implant Overdenture First-Choice. Standard of Care for the Edentulous Denture Patient
 The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
B978-0-443-06895-9.00005-8,
 B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
Surgical Planning and Prosthesis Construction Using Computed Tomography, CAD/CAM Technology, and the Internet for Immediate Loading of Dental Implants
 Surgical Planning and Prosthesis Construction Using Computed Tomography, CAD/CAM Technology, and the Internet for Immediate Loading of Dental Implants STEPHEN F. BALSHI, MBE* GLENN J. WOLFINGER, DMD, FACP
Surgical Planning and Prosthesis Construction Using Computed Tomography, CAD/CAM Technology, and the Internet for Immediate Loading of Dental Implants STEPHEN F. BALSHI, MBE* GLENN J. WOLFINGER, DMD, FACP
Dental Implant Treatment after Improvement of Oral Environment by Orthodontic Therapy
 Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
IMPLANT DENTISTRY CLINICAL SYLLABUS
 IMPLANT DENTISTRY CLINICAL SYLLABUS RESD 535 MATS H. KRONSTROM, DDS, PhD Course Director DEPARTMENT OF RESTORATIVE DENTISTRY SCHOOL OF DENTISTRY UNIVERSITY OF WASHINGTON 2008 2009 RD 535 - SCHEDULE FALL
IMPLANT DENTISTRY CLINICAL SYLLABUS RESD 535 MATS H. KRONSTROM, DDS, PhD Course Director DEPARTMENT OF RESTORATIVE DENTISTRY SCHOOL OF DENTISTRY UNIVERSITY OF WASHINGTON 2008 2009 RD 535 - SCHEDULE FALL
In 1999, more than 1 million people in
 Clinical SHOWCASE Slip-and-Fall Injuries Causing Dental Trauma Morley S. Rubinoff, DDS, Cert Prosth Clinical Showcase is a series of pictorial essays that focus on the technical art of clinical dentistry.
Clinical SHOWCASE Slip-and-Fall Injuries Causing Dental Trauma Morley S. Rubinoff, DDS, Cert Prosth Clinical Showcase is a series of pictorial essays that focus on the technical art of clinical dentistry.
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016
 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 About the Program Implants
USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 About the Program Implants
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
THE MANAGEMENT OF A COMPLEX IMPLANT CASE USING CAD-CAM TECHNOLOGY: A CLINICAL REPORT
 CSE REPORT DOI:10.4047/jkap.2008.46.6.634 THE MNGEMENT OF COMPLEX IMPLNT CSE USING CD-CM TECHNOLOGY: CLINICL REPORT Eun-Jin Park*, DDS, MMSc, PhD ssistant Professor, Department of Dentistry School of Medicine,
CSE REPORT DOI:10.4047/jkap.2008.46.6.634 THE MNGEMENT OF COMPLEX IMPLNT CSE USING CD-CM TECHNOLOGY: CLINICL REPORT Eun-Jin Park*, DDS, MMSc, PhD ssistant Professor, Department of Dentistry School of Medicine,
How To Use Nobelbiocare'S Integrated Treatment Workflow
 The key to successful treatments NobelClinician Software Visualize what you need to see with the unique SmartFusion technique. Increase efficiency with the integrated treatment workflow. Collaborate more
The key to successful treatments NobelClinician Software Visualize what you need to see with the unique SmartFusion technique. Increase efficiency with the integrated treatment workflow. Collaborate more
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Flapless Implant Surgery for Replacement of Posterior Teeth
 Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Dental Implants and Esthetics
 Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Attachment S: Benefits Covered - ADULTS - AGE 21 AND OVER
 Diagnostic services include the oral examinations and selected radiographs needed to assess the oral health, diagnose oral pathology and develop an adequate treatment plan for the Participant s oral health.
Diagnostic services include the oral examinations and selected radiographs needed to assess the oral health, diagnose oral pathology and develop an adequate treatment plan for the Participant s oral health.
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION
 PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION Derived from patient CT Data Customizable design features Strength with low profile This publication is not intended
PATIENT SPECIFIC PLATES FOR MANDIBLE: CUSTOM MADE PLATES FOR TRAUMA AND RECONSTRUCTION Derived from patient CT Data Customizable design features Strength with low profile This publication is not intended
General Dentist Fees
 General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Renaissance of One-Piece Implants
 2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE
 IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
Implant Bar Overdenture Utilizing Locator Attachments
 Utilizing Locator Attachments Step-by-Step Restorative Protocol Implant Bar Overdentures offer a removable implant solution for edentulous patients desiring a stable and esthetic prosthesis that improves
Utilizing Locator Attachments Step-by-Step Restorative Protocol Implant Bar Overdentures offer a removable implant solution for edentulous patients desiring a stable and esthetic prosthesis that improves
ADA Insurance Codes for Laboratory Procedures:
 ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
BICON DENTAL IMPLANTS
 BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
A Review of Implant Abutments - Abutment Classification to Aid Prosthetic Selection
 A Review of Implant Abutments - Abutment Classification to Aid Prosthetic Selection Sanjay Karunagaran, B.D.S., D.D.S., M.S.D., Gregory J. Paprocki, D.D.S., Russell Wicks, D.D.S., M.S., Sony Markose, B.D.S.,
A Review of Implant Abutments - Abutment Classification to Aid Prosthetic Selection Sanjay Karunagaran, B.D.S., D.D.S., M.S.D., Gregory J. Paprocki, D.D.S., Russell Wicks, D.D.S., M.S., Sony Markose, B.D.S.,
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Eastman Dental Hospital. Dental implants - general information for patients. Department of Restorative Dentistry
 Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Dentalworkers JOB DESCRIPTIONS Great Team Members make your Office function!
 Dentalworkers JOB DESCRIPTIONS Great Team Members make your Office function! Dental Assistant Registered Dental Assistant with Expanded Function: RDAEF Sterilization Assistant Dental Hygienist General
Dentalworkers JOB DESCRIPTIONS Great Team Members make your Office function! Dental Assistant Registered Dental Assistant with Expanded Function: RDAEF Sterilization Assistant Dental Hygienist General
