Hip Replacement Surgery
|
|
|
- Frederica Tate
- 8 years ago
- Views:
Transcription
1 Hip Replacement Surgery Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures. Since the 1970 s, while total joint techniques and methodologies have evolved and improved, one thing at DMOS has remained the same: the commitment to specialized, compassionate orthopaedic care for every patient. As the largest and most comprehensive total joint center in Iowa, you can be assured that your surgeon and their colleagues experience in the science and techniques of total joint replacement is at the forefront of exceptional care. In addition to the thousands of total joints performed, DMOS surgeons have published hundreds of articles explaining and exploring the science of total joint replacements. As a result, the Joint Replacement Center at DMOS is second to none in the area. We thank you for choosing DMOS and look forward to helping you gain mobility and get back to life with your total joint.
2 INTRODUCTION TO HIP REPLACEMENT
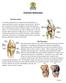
3 TYPES OF HIP ARTHRITIS INTRODUCTION The hip joint is commonly called a ball and socket joint. The ball of the hip joint, the femoral head, rests within a socket called the acetabulum (Figure #1). The femoral head and acetabulum are covered by a specialized surface, articular cartilage, which allows smooth and painless motion of the joint. With hip Fig. 1 injury or disease, articular cartilage undergoes degeneration and wears away. The joint surfaces become rough and irregular resulting in pain and stiffness. This is commonly known as arthritis but it has many causes. The onset of pain is gradual and, initially, it occurs only after higher levels of physical activity. Pain gradually increases and may become present at rest as well. Physical disability includes a limp, muscle spasm, and increasing stiffness. DAMAGED HIPS Osteoarthritis (figure #2) As we age, normal wear and tear can add up. Injuries and hereditary factors can predispose a patient to this wear. Cartilage may begin to crack and roughen. As the surfaces rub together, the cartilage is worn away. This leads to a bone on bone joint, which is stiff and painful. Fracture (figure #3) A bad fall or blow to the hip can break (fracture) the bone. Sometimes hip replacement is immediately performed after a fracture; at other times, it is not indicated until much later. Inflammatory Arthritis (figure #4) An inflammatory disease, such as rheumatoid arthritis or gout, can cause swelling and heat (inflammation) in the joint lining. As the disease progresses, cartilage may be worn away and the joint will become painful. Osteonecrosis (figure #5) Long-term use of alcohol or steroids or a bad injury can reduce blood supply to the bone. If the bone dies (necrosis), the ball will collapse, leading to hip pain. DAMAGED HIPS Fig. 2 Fig. 3 Fig. 4 Fig. 5
4 TYPES OF HIP JOINT REPLACEMENT There are many different operations used to treat the damaged hip joint. By far, the most common operation is total hip replacement. This operation involves taking the hip apart and removing the scar tissue (capsule) from around the hip, cutting off the bony ball on the upper end of the thighbone, and deepening the bony socket in the pelvic bone. A socket prosthesis (acetabular component) is then fixed into the pelvic bone, and a stem prosthesis (femoral component) is inserted into the maroon cavity of the upper thighbone. The metal ball on the end of the stem fits into the socket. It is then held in place by your muscles and by the scar tissue (capsule) that reforms during the healing process. The three most common types of total hip replacement (THR) are: Cemented THR Hybrid THR Uncemented THR Currently, uncemented THR is the most common of the three. Hip resurfacing is also a type of total hip replacement, where the bony ball is capped (resurfaced) instead of removed. CEMENTED THR Cemented THR has been used extensively in the past, with generally excellent results. This operation involves fixing both the socket and the stem to bone with acrylic cement. We still do a fully cemented THR in selected cases, but in general, the most common types of THR done in the United States today are Hybrid THR and Uncemented THR. At this time, the most common metals used in total hip replacements are titanium, chrome, cobalt, and stainless steel. Fig. 6 HYBRID THR (FIGURE #6) Hybrid THR involves fixing the socket to the pelvis with uncemented fixation, and the stem to the thighbone with cemented fixation. The socket prosthesis is made of metal and has a special porous surface with microscopic holes that allows the growth of bone into the holes, much like a fracture healing. This metal socket is wedged into the bony socket of the pelvis after the bone is prepared by reaming (deepening and shaping of the bone). Screws can then be placed through holes in the socket to further stabilize the metal socket. Some surgeons use screws all the time, and some surgeons use screws only occasionally. After the metal socket is fixed to the bony pelvis, a liner is then snapped into the metal socket. This liner is usually made out of polyethylene (a very durable plastic). In hybrid THR, the stem is fixed to the thighbone with acrylic cement. This type of cement has been used for over 35 years. It has proven to be durable in many patients for well over 35 years. Fig. 7 UNCEMENTED THR (FIGURE #7) In uncemented THR, the metal socket and plastic liner are placed in the same fashion noted above for hybrid THR. The stem is then inserted tightly into the marrow cavity of the thighbone. The stem prosthesis also usually has a porous surface that allows bone ingrowth. In some cases, the stem will have a surface that is coated with hydroxypetite (a chemical that induces bone ingrowth).
5 In summary, the choice of an uncemented socket has largely replaced that of a cemented socket throughout the United States. On the other hand, both cemented fixation (for hybrid THR) and uncemented fixation (for uncemented THR) of the stem remain popular. Currently over 95% of our THR procedures are performed with uncemented fixation of the stem. The choice at this time is based primarily on surgeon preference and bone quality. In hip resurfacing, the metal socket is made out of chromium cobalt and is placed without screws. The inner surface of this socket is polished and matches the femoral head prosthesis that is used to cap the bony ball (figure 8). This procedure is Fig. 8 less common now in the U.S. Treatment options, prior to THR, include reducing stress on the hip, physical therapy, and medication. Weight reduction is highly desirable, since one pound of weight loss equals three pounds in stress reduction on the hip while walking! The use of a cane or walking stick is also a very effective means of reducing stress on the hip. Physical therapy and exercises are directed at preserving muscle strength and range of motion within the limits of pain. Recommended medications include antiinflammatory agents, such as aspirin, Indocin, Motrin or Advil (ibuprofen), Feldene, Naprosyn or Aleve (naproxen), Voltaren, Mobic, Lodine, Celebrex, and others. Selection of the optimal treatment plan should be consistent with the degree of pain, the amount of hip disability, and the nonsurgical and surgical alternative. The individual s anticipated life span will also influence the selection of treatment. ALTERNATIVES TO STANDARD TOTAL JOINT REPLACEMENT At this time, there are numerous alternatives to standard total hip replacement. Some of these alternatives are new, and some have been used for many years. Although the plastic liners that have been used in the past have been shown to be durable over periods of greater than 25 years, this part of the hip replacement (the bearing surface) has been found to be the weak link in many cases of THR failure. Therefore the polyethylene in almost all plastic liners has been improved by the implant companies throughout the 2000s. A newer type of plastic, called highly cross-linked polyethylene, is used in almost all total hips now. This polyethylene has been shown to wear at a rate that is less than 10% of the old polyethylene. In addition, other bearing surfaces such as ceramic and metal-on-metal are being used in some centers. All these options are available to us here, but for many reasons we still reserve them for patients with extraordinary needs. In young patients, we often use a ceramic ball on a highly cross-linked polyethylenic liner. This can reduce the wear rate even further but has the disadvantage of being slightly more fragile.
6 Minimal Incision THR is also preferred at our center. Potential advantages of this technology are possible lower blood loss and more rapid recovery. Potential disadvantages include decreased surgical visualization, which could lead to complications or decreased durability. Another operation, hip resurfacing, or total hip resurfacing, where both the ball and the socket are resurfaced with metal coverings only (metal-on-metal), is now commonly performed at our center. This operation has been performed extensively in Europe and Australia. The primary advantage of this operation compared to total hip replacement is that it saves bone. Some surgeons believe that patients with surface replacement can be more active, but that is unproven. Another advantage is that it allows a very large femoral ball, so dislocation is rare. Disadvantages include the fact that the operation is technically more difficult than THR, increased femoral neck fracture risk, and the fact that metal-to-metal implants can t be used in certain patients, such as those with renal disease and females of childbearing age. There is a rare metal-on-metal allergic-type reaction after this operation, and the femoral neck fracture risk is increased in patients with small bones (usually females). Because of the femoral neck fracture risk, hip resurfacing is usually done in patients with strong bones. traditional option is not likely to work that we will suggest an alternative or experimental option. In general, you want what works, not what s new. TO DO BEFORE SURGERY: Pre-Op History & Physical Find Family Member or Coach to Accompany Me to Total Joint Class and to Assist Home Starting Post-Op Day #1 Attend Total Joint Class The most important information we can give you about all of these alternatives to standard THR is that we do our best to attend meetings, talk to colleagues, and study the literature. We are involved in research and societies that study the hip. We will always do our best to help you choose the best operation for you. In general, our philosophy is that most patients would prefer an operation that is proven to work over one that is experimental. It is primarily in cases where the
7 PREDICTED RESULTS OF SURGERY Following your surgery, you can expect to be up walking the night of surgery and will be in the hospital 1-3 days after surgery. You will leave the hospital walking with a walker or on crutches and you can plan to use these for about 4 weeks. At that time, you will begin walking with a cane or single crutch and you will do this until you walk well without support. Most patients are walking without support by 5-6 weeks, but this varies from patient to patient. Patients who limped longer before the surgery tend to limp longer after. During the next 12 months, you will continue to gain strength and endurance. This means you will be able to walk with minimal or no limp, minimal or no pain, without cane or crutches, as far as you want to walk. You should have enough motion to sit and stand normally and very likely bend to tie your shoes. You can also expect to do pretty much what you want to do. You will not have a normal hip. The purpose of the operation is not to give you a hip that functions normally, but one that functions significantly better than your hip functioned prior to surgery. However, with reasonable common sense, you should be able to live a normal life. You can expect that your reflexes have slowed, therefore it is recommended that you do not drive a car for 4-6 weeks following surgery. Most people are able to return to light work for limited periods of time at about 4-6 weeks following the surgery. Most people can return to a full day s work at a desk job at 4-6 weeks and heavy labor at about 3 months. Some examples of expected workload are listed below for your benefit: Farming: Most farmers can return to tractor driving in about 2-3 months. Heavier farm work is usually resumed in 3-6 months following surgery. Golf/Tennis: Most people can play golf at 3-4 months postoperative or light tennis at 4-6 months postoperative. Other Recreational Sports: Bike/Horse Riding: You may be able to ride a horse or a bicycle at 4-6 months following the surgery. Most patients are able to return to recreational and fitness activities such as skiing, swimming and weightlifting, but running for exercise is generally not recommended after total hip replacement. Based on our results to date, you have a 98% chance of having what we call a good result.
8 LONG-TERM OUTCOMES Based on the results of the first 1,000 operations performed by DMOS and monitored for 20 years, you may expect the following: HIP DISLOCATION You have one chance in 300 of your hip dislocating (ball coming out of the socket). The need for another operation to correct this problem is very rare. With new technology, since the year 2000, this complication has been reduced to less than 1% of our patients. WEAR OF THE ARTIFICIAL PARTS Wear of the artificial parts has not been a major problem in the first 20 years for our patients. There are, however, extensive reports of bone destruction (osteolysis) caused by wear of the artificial parts. Because of this concern, we recommend that you discuss with your surgeon an appropriate time period to be X-rayed. this concern or loosening of the products over time, we recommend this operation to young people only after failure of conservative measures. It should be pointed out that these are the results of the operation as we performed it 30 years ago. We have made a number of improvements in the way the operation is performed which should reduce the chances of the artificial pieces coming loose from the bone. New artificial pieces have been developed which are much more durable with lab testing. We have also learned a little more about preparing the bone for either cemented or uncemented parts. All of these changes should reduce the chances of loosening or failure of your prosthesis. Of course, only time will tell how much difference these improvements will make. LOOSENING Loosening of the metal ball from the thighbone or of the socket from the pelvic bone has been found to be the major long-term problem. This is most likely due to wear debris causing bone destruction or the plastic cement beginning to crumble because of fatigue due to higher levels of mechanical stress than the cement will tolerate repetitively. While reoperation for this problem has been reported to be needed in as many as 25% of patients, our own experience has been much more favorable. In our own experience, if you have a good result at one year you have only one chance in 100 of needing additional surgery to replace a loose ball or socket during the first 10 years. After 20 years, only 5% total of our patients had either a loose ball or socket. However, because of
9 RISKS AND COMPLICATIONS No surgery is without risk. Understanding the risks is necessary in order for you to make an informed decision about your desire for surgery. MEDICAL COMPLICATIONS. Anesthesia and surgery-related complications, such as heart attack, stroke, death, or loss of limb (less than 1 in 10,000 chance), may occur. Fortunately, these events occur extremely rarely. A thorough medical examination prior to surgery minimizes these risks. INFECTION. Infection is a very serious complication of any joint replacement surgery. Many precautions are taken to avoid infection, and as a result, the risk of infection is very low (less than half of a percent). These precautions include the use of antibiotics at the time of surgery. Use of designated operating rooms with special air-handling filters, and in some instances, the use of space suits by the surgeons and nurses. Further surgery would be necessary if an infection should occur, and the successful treatment of infection could require many months of treatment. DISLOCATION. There is a less than 1% chance of your hip dislocating (ball coming out of socket). This can usually be managed by simply pulling on the leg while you are under anesthesia. The ball snaps back into the socket and is unlikely to come out again if you are reasonably careful. Occasionally, another operation is necessary. BLOOD LOSS. Following hip replacement surgery, a blood transfusion may be required. Patients undergoing a single joint replacement have a less than a 5% risk of requiring a transfusion. Patients undergoing bilateral (right and left) replacements, however, have a greater than 10% chance of requiring blood transfusion. Bloodborne diseases (AIDS, hepatitis, etc.) and adverse allergic reactions are the major hazards of blood transfusions. Our blood bank screening is as modern and thorough as possible, and therefore, the risks are exceedingly small. In fact, the risk of dying from a blood transfusion is hundreds of times lower than that of driving your car for one day. There are many options available to lower your chance of needing a blood transfusion. OBESITY. Excessive weight can make the actual surgical procedure more difficult and increases your risk of complications, such as wound healing and infection. Expectations following hip replacement surgery in obese patients are diminished. Patients of large size generally will not be able to walk as far; stair climbing and rising from a chair will remain more difficult. Excessive weight may also shorten the life of the prosthesis. However, patients with excessive weight generally are pleased with their joint replacement. BLOOD CLOTS. Blood clots or deep vein thromboses may occur following any lower extremity surgery, including hip joint replacement. These clots cause increased swelling in the legs and although rare, can travel to the lung and cause more severe illness or even sudden death. The risks of these events are minimized by several important treatments. All patients are given appropriate blood thinner soon after surgery. Generally, you will be required to take small injections of blood thinner (Lovenox or Fragmin) daily or you will use an oral blood thinner (Coumadin or Pradaxa). Adult-strength aspirin is becoming the preferred protection from blood clots. Either of these medications will be continued after your discharge from the hospital. In addition to these medications, we minimize the risk of blood clots by the use of foot pumps, used while in bed, or by getting you up and moving very soon after surgery. NERVE, ARTERY, OR BONE INJURY. Though rare, other complications could include artery or nerve damage or fractures of the bones near the hip.
10 BILATERAL SURGERY Many of the diseases that cause disabling hip problems affect both hips. The hips may be affected at the same time or at different times and to different degrees. We only operate on the hip if and when it becomes a major problem. However, we have found that if both hips are a major problem, it is reasonable to do the operations close together. The advantage is convenience for the patient, while the disadvantage is a possible slight increase in risk. We have found that recovery from the first operation is sufficient to safely do the second operation after two to seven days and then rehabilitation can proceed properly. REVISION (REDO) SURGERY Increasing numbers of patients are undergoing revision surgery. The most frequent cause of failure of a total hip replacement is loosening of the implant in bone, which may be caused or aggravated by the wear process. The magnitude of the surgery depends on the complexity of prosthetic removal and restoration of bone deficiency. Revision surgery may require bone grafts from your pelvic area and/or from the bone bank. Custom prostheses may be needed. Like primary surgery, the durability is dependent upon the techniques utilized. Revision surgery is technically more difficult, though quality results can be achieved. Third, fourth, and even tenth revisions have also been performed. Once again, each revision may have special and more difficult challenges for the surgeon and the patient. Special precautions are often necessary following these types of procedures. implants and tissue and reinserting a new implant at the same operation. While the success of these procedures has continued to increase, special precautions are recommended. These include careful monitoring and close observation in the postoperative period because there is a risk for the recurrence of infection. All of the complications mentioned for the original operation apply to the reoperation. The results of the reoperation are nearly as good as the original operation. Due to the fact that the operation is much more extensive and bone may have been destroyed, the chances of complications are greater than with the original operation. In cases where infection is detected, we may need to remove all of the artificial components and leave them out. Patients who have had infections of hip joints may be advised to have delayed reinsertion of a total hip replacement (two operations: one for removal and one for reinsertion of the implants); or direct exchange, which involves thoroughly removing the infected,
11 PREPARATIONS FOR SURGERY ROUTINE LABORATORY TESTS are generally performed with your pre-surgical medical exam prior to surgery. These include necessary blood tests, possibly X-rays, and an EKG. PRE-SURGERY JOINT REPLACEMENT PROGRAM. The hospital offers a Pre-Surgery Joint Replacement Program class for you and a family member to attend. It is necessary that all joint replacement patients attend this pre-surgery class. The program will provide useful information concerning your hospitalization for your total hip replacement and will answer many of your questions. In addition to your attendance, we strongly encourage a family member to attend the program with you as well. Your surgeon and his/her staff will provide you with more information about the Pre-Surgery Joint Replacement Program class. Once you have made the decision to proceed with hip replacement surgery, a number of necessary events will be scheduled. A DATE FOR SURGERY will be determined and scheduled at the hospital by your surgeon. If you need to contact the program coordinator or would like more information about the class, the contact information is below: METHODIST WEST: (515) IOWA LUTHERAN HOSPITAL: (515) ST. ANTHONY REGIONAL HOSPITAL: (712) A PRE-SURGICAL MEDICAL EXAMINATION will be scheduled. This examination should be carried out in the weeks prior to the scheduled surgery. In most cases, your age and medical condition will require a complete medical exam by an internal medicine specialist and/or a cardiologist, who will then be available to assist in your care during your post-operative hospital stay. We will provide additional information concerning these exams and schedule your evaluation.
12 HOSPITAL ADMISSION AND CARE PREPARATION FOR SURGERY The following directions are important to follow in preparation for your surgery and to facilitate an effective recovery. 1. NO FOOD OR BEVERAGE OF ANY KIND AFTER MIDNIGHT THE NIGHT BEFORE YOUR SURGERY. This includes gum, chewing tobacco, and cigarettes. The day before your surgery, eat a regular breakfast and lunch. After lunch drink only clear liquids for the rest of the day (until midnight). 2. Due to the fact that your digestive system slows for a few days following surgery, it is recommended that you consider an enema the night before surgery, especially if you have a history of constipation. A Fleets Enema, which can be purchased at any drugstore, is recommended. 3. If you take blood pressure, heart or diabetes medication, please be sure to bring specific instructions regarding your dosages with you to your surgery. Stop all aspirin, Motrin and antiinflammatories 7 days before surgery. Tylenol is acceptable to use in place of these if necessary. 4. Take time to read the materials provided to you in this packet and the materials provided by the hospital. You are encouraged to bring the materials with you to the hospital for reference during your hospital stay. 5. If you are on a blood thinner (Coumadin, Warfarin, Plavix, Xarelto, etc.), discuss this with your surgeon at the time of scheduling your surgery. DAY OF SURGERY METHODIST WEST, IOWA METHODIST MEDICAL CENTER AND IOWA LUTHERAN HOSPITAL Patients are admitted to the hospital the day of surgery. You will be contacted the day before your surgery to confirm the time of your surgery and what time to arrive. If you have not received a call by 3 p.m. please call your surgeons office. If your surgery is scheduled on a Monday, you will be contacted on the Friday before your surgery. ST. ANTHONY REGIONAL HOSPITAL Patients will be contacted two to three days before your surgery to notify you of the time of your surgery and what time you need to arrive at the hospital. LODGING IOWA METHODIST MEDICAL CENTER ONLY Patients that live a distance from the hospital or prefer to stay close by on the preoperative night can stay at the Care Inn, just south of Iowa Methodist Medical Center, for a fee. To reach the Care Inn, please call (515) to make a reservation. The Care Inn is located on the Iowa Methodist campus. HOTELS There are several hotels available near each hospital campus, many of which offer a medical/patient discount. If you or your family require a hotel room, this expense is your responsibility, not your insurance company s or the hospital s responsibility. Please contact your surgeon s office for a list of discounted hotels.
13 DISCHARGE / COMMON QUESTIONS AT HOME Determination for discharge from the hospital is based on your medical condition and your ability to walk and get up and down independently. Most patients will be discharged at 1 3 days after a routine total hip replacement. Many patients will not be able to do their own cooking, cleaning, laundry, etc. The level of assistance that you will need is related in a large part to the abilities you had prior to your surgery. If you need further assistance with your rehabilitation, you may go to a Skilled Nursing Facility (SNF). Most patients would go to an SNF if on post-op day #3 if they are not able to get out of bed and walk independently. While there, you are given assistance with normal daily activities as well as physical therapy. Your length of stay there is determined by your progress. Most people are there less than two weeks. These arrangements are completed at the hospital with a Social Worker. The Social Worker will often make arrangements for a Skilled Nursing Facility several days before your anticipated discharge, and we can always cancel this if necessary. Whenever possible, the Social Worker will take your facility preferences into consideration. Transportation to the skilled facility is generally not covered by insurance companies and is the responsibility of the patient and their family. If you have assistance at home and are able to transfer and walk independently, you can plan to be discharged to your own home. Most insurance companies will cover a visiting nurse or therapist who can come to your home if necessary. COMMON QUESTIONS AT HOME There are always questions that arise once you are home. Listed below are some of the most common questions. 1. SWELLING. Once you are home, it is likely that you will be more active and up for longer periods than you were at the hospital. You may notice increasing swelling in your entire leg on the operative side. Swelling is normal and may occur for several months. There are guidelines to follow that should minimize your problems with swelling. Throughout the day plan for periods to lie down with your leg elevated above your heart, usually in bed with your leg on a pillow. Continue your exercises including foot pumps and ankle circles. These help with circulation. Alternate periods of sitting and standing, avoid either for extended periods of time. Avoid long periods of sitting. Your swelling should be decreased in the morning. Following discharge from either the hospital or a skilled care facility, you should arrange for further assistance with family and friends.
14 2. INFECTION. It is important to check your incision daily. Normally you will notice swelling along with slight redness and bruising. There may be drainage that is light yellow to pink in color. All of these things are normal and should improve. Contact our office if you develop: An increase in drainage that is purulent (pus like) or green tinged An elevation in your temperature (over 102 ) A general feeling of malaise-chills, sweats, aches, accompanied by a loss of energy If you develop a secondary illness such as urinary tract infection, upper respiratory infection, toothache, or an open wound, contact a medical doctor without a delay. Contact your surgeon for any of these developments even if you have seen your family physician for treatment! 3. BLOOD THINNERS. After surgery, most patients will be managed on a blood thinner to lower the risk of blood clots. The growing trend in this country is to treat most patients with aspirin only for blood clot prevention. This has been found safe when combined with early activity and foot or leg compression devices. Some patients will receive Coumadin, which is sometimes monitored with a blood test (PT/INR). Those that receive Coumadin will usually continue the medication for 3 or 4 weeks after leaving the hospital. Other patients will receive low molecular weight heparin like Fragmin or Lovenox. These drugs are given by small injections under the skin. Those that receive Fragmin or Lovenox will usually continue the medication for a few days after leaving the hospital, and will be taught how to give the medication while in the hospital. Some patients are discharged on over-the-counter aspirin treatments. It is very important that you know the name and dosage of the blood thinner you will be using when you leave the hospital. If you are on Coumadin, it is important that you understand who will monitor the medication after you leave (your Surgeon, Internist, or Family Physician). If the dose of Coumadin is low, it may not require monitoring. 4. DISLOCATION PRECAUTIONS. Following your total hip replacement, it is advised to sit in high, firm chairs. Avoid couches and low or overstuffed chairs. It is also important to not cross your legs and to keep your knees apart for six weeks. Avoid quick movements, especially those that involve bending and twisting. Our restrictions following a total hip replacement are not numerous due to the surgical approach we use, which is associated with a very low risk of dislocation. However, revisions and complex cases may have more specific restrictions. 5. PHYSICAL THERAPY. Supervised physical therapy following discharge after total hip replacement is generally not warranted. Patients have been found to do just as well with a home exercise program (in other words, in multiple studies, patients who have had routine total joint replacement have equal results with or without supervised physical therapy). We do want you to do the exercises you are taught at class and in the hospital, and we will arrange outpatient physical therapy in cases of special need. After a total hip replacement, the most beneficial exercise is walking. ASSISTANCE FOLLOWING DISCHARGE It is recommended that the family be prepared to be available to help at the time of discharge. The patient will require transportation. In addition, family or a friend will need to be available to assist the patient at home for home for 3 to 7 days. Insurance companies do not authorize additional days of hospitalization due to a lack of transportation or assistance at home.
15 DENTAL CARE AFTER TOTAL JOINT REPLACEMENT SURGERY The American Association of Orthopaedic Surgeons and the American Dental Association have active interest in antibiotic coverage after total joint replacement surgery. Although controversial, we currently recommend lifetime use of oral antibiotics one hour before dental work. Most dentists are happy to provide this prescription and we are also happy to provide one if necessary. UNSOLICITED ADVICE AFTER TOTAL JOINT REPLACEMENT SURGERY It is quite common after total hip replacement for patients to receive extensive advice from their friends and family. Some of these friends have had a joint replacement themselves, and some have known someone who has. Please realize that very few of these people have performed a total joint replacement, and very few have seen hundreds of patients who have undergone total joint replacement. You may hear comments like: You re not getting enough therapy I didn t have that much pain after my surgery You shouldn t be limping still Why are you still swollen, using crutches, etc. We suggest that you listen to the positive and encouraging comments and ignore the negative ones. Realize that all patients are different, and that some will recover rapidly while others will recover slowly. Recovery rate depends on multiple factors, including patient age, patient physical condition, complexity of the operation, and others. We will do our best to give you the best care possible and to help you recover from surgery as rapidly as possible.
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Total Knee Replacement
 Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
PALM BEACH ORTHOPAEDIC INSTITUTE, P.A. FAQ: OUT-PATIENT SURGERY
 DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
 Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery
 Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Patient Labeling Information System Description
 Patient Labeling Information System Description The Trident Ceramic Acetabular System is an artificial hip replacement device that features a new, state-of-the-art ceramic-on-ceramic bearing couple. The
Patient Labeling Information System Description The Trident Ceramic Acetabular System is an artificial hip replacement device that features a new, state-of-the-art ceramic-on-ceramic bearing couple. The
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT Total Hip replacement is usually needed when the normally smooth, slippery soft joint surface cartilage wears down to rough bone (degenerative arthritis or osteoarthritis). One or
TOTAL HIP REPLACEMENT Total Hip replacement is usually needed when the normally smooth, slippery soft joint surface cartilage wears down to rough bone (degenerative arthritis or osteoarthritis). One or
Anterior Approach. to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Dr. Anseth s Frequently Asked Questions about Hip Replacement
 Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Lumbar or Thoracic Fusion +/- Decompression
 Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Why an Exactech Hip is Right for You
 Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments. For Knee Replacement Surgery
 No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments For Knee Replacement Surgery Table of Contents Here s how it works....2 Why does my knee
No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments For Knee Replacement Surgery Table of Contents Here s how it works....2 Why does my knee
BIRMINGHAM HIP Resurfacing (BHR ) System PATIENT INFORMATION
 BIRMINGHAM HIP Resurfacing (BHR ) System PATIENT INFORMATION Table of Contents 1.0 What is the BHR Device? 2.0 What is the Purpose of the BHR Device? 3.0 When Should the BHR Device Not Be Used? (Contraindications)
BIRMINGHAM HIP Resurfacing (BHR ) System PATIENT INFORMATION Table of Contents 1.0 What is the BHR Device? 2.0 What is the Purpose of the BHR Device? 3.0 When Should the BHR Device Not Be Used? (Contraindications)
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Treatment Guide Hip Pain. Choosing Your Care
 Treatment Guide Hip Pain Choosing Your Care The good news is that there are more effective treatment options available today than ever before. At Cleveland Clinic s Orthopaedic & Rheumatologic Institute,
Treatment Guide Hip Pain Choosing Your Care The good news is that there are more effective treatment options available today than ever before. At Cleveland Clinic s Orthopaedic & Rheumatologic Institute,
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Total Hip Replacement
 Total Hip Replacement INTRODUCTION T he following information is a guide to your upcoming surgery. It describes what is likely to happen at the time of surgery. This is a guide only and there may be some
Total Hip Replacement INTRODUCTION T he following information is a guide to your upcoming surgery. It describes what is likely to happen at the time of surgery. This is a guide only and there may be some
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP
 TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so that
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so that
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
Total Hip Joint Replacement. A Patient s Guide
 Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Total Hip Joint Replacement A Patient s Guide Don t Let Hip Pain Slow You Down What is a Hip Joint? Your joints are involved in almost every activity you do. Simple movements such as walking, bending,
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
.org. Shoulder Joint Replacement. Anatomy
 Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Total Hip Replacement
 Total Hip Replacement 1. What are the surgical options for the arthritic hip? When non-operative treatments for hip pain due to arthritis fail to work, surgery may be indicated. The surgical options include
Total Hip Replacement 1. What are the surgical options for the arthritic hip? When non-operative treatments for hip pain due to arthritis fail to work, surgery may be indicated. The surgical options include
.org. Total Knee Replacement. Anatomy
 Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Cormet Hip Resurfacing System
 Cormet Hip Resurfacing System Patient Product Information 325 Corporate Drive Mahwah, NJ 07430 t: 1-888-STRYKER www.aboutstryker.com The information presented in this brochure is for educational purposes
Cormet Hip Resurfacing System Patient Product Information 325 Corporate Drive Mahwah, NJ 07430 t: 1-888-STRYKER www.aboutstryker.com The information presented in this brochure is for educational purposes
Patient Education Manual. Total Hip Replacement
 Patient Education Manual Total Hip Replacement Table of Contents Total Hip Replacement Patient Education Manual Welcome Letter... 1 Overview OrthoVirginia and Joint Replacement Capabilities... 4 Medical
Patient Education Manual Total Hip Replacement Table of Contents Total Hip Replacement Patient Education Manual Welcome Letter... 1 Overview OrthoVirginia and Joint Replacement Capabilities... 4 Medical
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE
 TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so
TOTAL KNEE REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE KNEE John T. Dearborn, M.D. and Alexander P. Sah, M.D. The Center for Joint Replacement Please read this pamphlet before you see me so
Should I have a knee replacement?
 Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Total Knee Replacement. Patient Information
 Total Knee Replacement Patient Information Introduction: We would like to thank you for choosing The Institute for Advanced Bone and Joint Surgery at St. Joseph s/ Candler for your Total Joint Replacement
Total Knee Replacement Patient Information Introduction: We would like to thank you for choosing The Institute for Advanced Bone and Joint Surgery at St. Joseph s/ Candler for your Total Joint Replacement
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Total Knee Replacement
 Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Answers to commonly asked questions from patients with metal-on-metal hip replacements / resurfacings. Contents
 Answers to commonly asked questions from patients with metal-on-metal hip replacements / resurfacings John Skinner 1 and Alister Hart 2, Consultant Orthopaedic Surgeons and Directors of the London Implant
Answers to commonly asked questions from patients with metal-on-metal hip replacements / resurfacings John Skinner 1 and Alister Hart 2, Consultant Orthopaedic Surgeons and Directors of the London Implant
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
PERIACETABULAR OSTEOTOMY SURGERY
 1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
1 PERIACETABULAR OSTEOTOMY SURGERY It is important to us that all of our patients know what to expect before surgery, during their hospitalization and after surgery. Office Visits Planning begins with
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Treatment with Rivaroxaban
 UW MEDICINE PATIENT EDUCATION Treatment with Rivaroxaban Xarelto This handout explains the medicine rivaroxaban, a drug that helps prevent blood clots. What is rivaroxaban? Rivaroxaban (brand name Xarelto)
UW MEDICINE PATIENT EDUCATION Treatment with Rivaroxaban Xarelto This handout explains the medicine rivaroxaban, a drug that helps prevent blood clots. What is rivaroxaban? Rivaroxaban (brand name Xarelto)
Total Hip Arthroplasty (Hip Replacement) PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
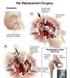 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
Robotic-Arm Assisted Surgery
 Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
Mako TM Robotic-Arm Assisted Surgery for Total Hip Replacement A Patient s Guide Causes of Your Hip Pain Your joints are involved in almost every activity you do. Movements such as walking, bending and
Orthopaedic Stem Cell Treatment
 Orthopaedic Stem Cell Treatment Stem Cell Injections Surgically Implanted Stem Cells Learn about the treatment option that is best for you. Emory Healthcare patients can benefit from surgical implantation
Orthopaedic Stem Cell Treatment Stem Cell Injections Surgically Implanted Stem Cells Learn about the treatment option that is best for you. Emory Healthcare patients can benefit from surgical implantation
This information is for patients who are considering having a hip replacement.
 Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Hip Replacement Discharge Instructions
 Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
TOTAL HIP REPLACEMENT FOR A LIFETIME: THE CEMENTLESS METAL ON METAL RECONSTRUCTION
 Richard A. Sweet, M.D. Louisville Orthopaedic Clinic Louisville, KY TOTAL HIP REPLACEMENT FOR A LIFETIME: THE CEMENTLESS METAL ON METAL RECONSTRUCTION INTRODUCTION Total hip replacement surgery (THR) has
Richard A. Sweet, M.D. Louisville Orthopaedic Clinic Louisville, KY TOTAL HIP REPLACEMENT FOR A LIFETIME: THE CEMENTLESS METAL ON METAL RECONSTRUCTION INTRODUCTION Total hip replacement surgery (THR) has
Low Back Surgery. Remember to bring this handout to the hospital with you.
 Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
Remember to bring this handout to the hospital with you. Table of contents Page Why do I need low back surgery?... 1 What kinds of low back surgeries are there?... 2 Before your surgery... 3 After your
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Selective Nerve Root Block
 Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
Selective Nerve Root Block What is a selective nerve root block? Selective nerve root blocks is similar to epidural injections, as the preparation and approach is identical. Epidural refers to the space
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
Total Joint Replacement
 Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Total Hip Replacement. University Hospital Ahuja Medical Center
 Total Hip Replacement University Hospital Ahuja Medical Center Total Hip Replacement Whether you have just begun exploring treatment options or have already decided to undergo hip replacement surgery,
Total Hip Replacement University Hospital Ahuja Medical Center Total Hip Replacement Whether you have just begun exploring treatment options or have already decided to undergo hip replacement surgery,
Treatment with Apixaban
 UW MEDICINE PATIENT EDUCATION Treatment with Apixaban Eliquis This handout explains the medicine apixaban, a drug that helps prevent blood clots. What is apixaban? Apixaban (brand name Eliquis) is an anticoagulant
UW MEDICINE PATIENT EDUCATION Treatment with Apixaban Eliquis This handout explains the medicine apixaban, a drug that helps prevent blood clots. What is apixaban? Apixaban (brand name Eliquis) is an anticoagulant
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
P REPLACEMENT SURGERY
 P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
