Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting
|
|
|
- Griselda Barton
- 8 years ago
- Views:
Transcription
1 Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting March 2015
2 Contents Purpose of this Document... 2 Basic Facts about Type 1 Diabetes... 3 Supportive Environment... 3 Supporting Independence... 4 Emergency Management... 5 Nutritional Management and Physical Activity... 6 Blood Glucose Monitoring... 6 Insulin Administration... 7 Roles and Responsibilities... 7 Parents/guardians:... 7 Boards of Education:... 8 Health Authorities:... 9 Glossary Appendices: Diabetes Support Plan and Medical Alert Administration Diabetes Medication Administration Form Websites and Links to Provincial Diabetes Information Materials Page 1 of 17
3 Provincial Standards: Supporting Students with Type 1 Diabetes In the School Setting Purpose of this Document The purpose of this document is to provide information about type 1 diabetes 1 (T1D), outline the provincial standards to support students with T1D in the school setting, and articulate the roles and responsibilities of parents/guardians, the school administrator and the Health Authorities. The overarching goal is to work together to ensure students with type 1 diabetes are provided with a safe and positive learning environment and have equitable access to learning, opportunities for achievement and the pursuit of excellence in all aspects of their educational program. Provincial standards provide the foundation upon which individual boards of education develop policies and procedures that address the unique needs of the student population and characteristics of the communities they serve. Local policies outline, more specifically, the procedures and processes unique to each school district. Further guidelines about roles and responsibilities can be found under Planning and Coordinating of Community Services in Section C of Special Education Services: A Manual of Policies, Procedures and Guidelines. Individual board policies can be viewed at the British Columbia School Trustees Association (BCSTA) or by contacting the local school board office. These provincial standards also inform applicable policies developed by health authorities and MCFD and align with the Inter- Ministerial Protocols for the Provision of Support Services to School Age Children and the Children and Youth with Special Needs Framework for Action. This document was developed by the Ministries of Health, Education and Children and Family Development. It was informed by Diabetes Care in the School Setting: Evidence-Informed Key Components, Care Elements and Competencies developed by Child Health BC. Sections have also been adapted from Kids with Diabetes in Your Care produced by the Canadian Diabetes Association. 1 The focus of this document is school-aged children and youth with T1D. Students with type 2 diabetes usually use oral medications and rarely experience emergency episodes of high or low blood sugar. In very rare circumstances, some students will have other conditions necessitating emergency planning for low blood sugar and those cases will involve individual planning. Page 2 of 17
4 Basic Facts about Type 1 Diabetes Type 1 diabetes (T1D) is one of the most common chronic diseases of childhood. Appropriate diabetes care in the school setting is important for the child s immediate safety, long term wellbeing and optimal academic performance. T1D occurs when the pancreas is unable to produce insulin. The exact cause of this condition is unknown; however, genetic and environmental factors both play a part. Insulin is a hormone produced by the pancreas. Carbohydrate (starch and sugar) from food eaten is broken down into glucose and enters the bloodstream. Insulin enables the body to use the glucose from the bloodstream for energy. Without insulin, glucose builds up in the bloodstream (high blood sugar), and the body s cells are deprived of their energy source. Diabetes management has advanced in recent years, changing the way children and youth manage their diabetes. Intensive insulin therapies (multiple daily injections or use of insulin pumps) are being recommended to improve blood glucose control and decrease long term health complications. With appropriate planning, a student with diabetes can participate in all school activities, and in most cases well managed diabetes will have little or no negative impact on a student s education or school experience. However, all students with diabetes will have occasional high or low blood glucose. Students whose diabetes is more challenging to manage may experience some disruption of their education. Teachers and school staff should discuss concerns regarding diabetes and its impact on a student s education with parents/guardians. Additional resources about T1D can be found in the Appendices. Supportive Environment A safe and supportive environment for students with T1D depends on regular and ongoing communication and coordinated planning and documentation among all parties. Regular and ongoing communication is established between schools, the student, and the parents/guardians to support a safe learning environment. A Diabetes Support Plan and Medical Alert Information from is required for every student with T1D enrolled in the BC Public Education System and participating Independent Schools. All school staff are familiar with the Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting and access General Information about Diabetes for School Personnel Page 3 of 17
5 The Diabetes Support Plan and Medical Alert Information includes: Names and contact information for parents, Diabetes Care Team, other involved health professionals, principal, and all involved school staff; Emergency plan; Student s self-management plan outlining the student s level of independence; Plan for nutrition, physical education, insulin and blood glucose monitoring; and Location of all supplies. The Diabetes Support Plan and Medical Alert Information is readily accessible to school staff and is developed in collaboration with the student s Diabetes Care Team (see glossary), the parents/guardians, and the school. Students requiring additional assistance in the form of delegated care will have a Nursing Support Services Delegated Care Plan. Both plans are updated annually or more frequently as needed. Students are permitted to contact their parents/guardians as needed regarding diabetes management. Supporting Independence Students are supported to work towards independence in managing their diabetes care in the school setting, to the extent that is appropriate for their functional and cognitive ability, maturity and experience with their diabetes. Goals toward independence will be developed in consultation between the parent/guardian, school personnel, diabetes care team and student. Delegation: Students who are not able to perform blood glucose monitoring and/or insulin administration can have these tasks performed or supervised by school staff through a process called delegation. Nursing Support Services (NSS) is available to delegate these nursing tasks when it is deemed to be in the best interest of the student. Delegation occurs when the required task is performed primarily by Registered Nurses (RN) and is outside the role description and training of an unregulated care provider, such as a school staff member. The delegating RN is responsible and accountable for the decision to delegate and the process of delegation including the ongoing supervision/monitoring to assess the ability of the school staff member to perform the delegated task. The designated school staff member is accountable to the RN for the performance of the delegated task. The delegated task is childspecific and may only be performed by the school staff member who is trained by the RN. If delegation is deemed appropriate for an individual student, the NSS Coordinator completes a NSS Delegated Care Plan in consultation with the parent, the child s Diabetes Care Team and the school administrator. The NSS Delegated Care Plan is updated annually at a minimum or whenever there is a change in the student s diabetes care as determined by the diabetes care team and parent. Page 4 of 17
6 Students are supported to work towards independence in managing their diabetes care in the school setting, to the extent that is appropriate for their functional and cognitive ability, maturity and experience with their diabetes. For students requiring NSS Delegated Care, the ongoing monitoring of school staff is provided by NSS Coordinators in accordance of the College of Registered Nurses Practice Standard Delegating Tasks to Unregulated Care Providers. The NSS Delegated Care Plan is updated annually at a minimum or whenever there is a change in the student s care as determined by the Diabetes Care Team and the parent. When a student is discharged from the NSS program, he or she may still require support from school staff in the form of reminders or confirmation that a task is completed until the student is fully independent in their diabetes management in the school setting. The level of support needed by the student can be documented in the Diabetes Support Plan and Medical Alert Information form. Emergency Management Emergency management of T1D involves the rapid and effective treatment of low blood glucose (hypoglycemia). 2 Low blood glucose is usually the result of too much insulin, missed or delayed meals or snacks, not eating enough food, engaging in extra intense or unplanned physical activity, or being ill, particularly with gastrointestinal illness. Hypoglycemia can range from mild to severe and in rare cases can be life threatening. Mild to moderate hypoglycemia is treated with fast-acting sugar while severe hypoglycemia is treated with an injection of glucagon. Glucagon is a hormone that allows the body to release the stored sugar in the liver and raise the blood glucose from dangerous low levels. Parents who wish to have glucagon administered at school need to have a Diabetes Medication Administration Form completed and signed by the student s physician. Every student with T1D will have an emergency plan as part of their Diabetes Support Plan and Medical Alert Information. School staff will know how to respond to a diabetes emergency. The poster Managing Low Blood Sugar is posted in visible locations in the school. Designated school staff will be trained to administer injectable glucagon in the event of a severe low blood glucose if requested by the parent. 2 Hyperglycemia, or high blood sugar, is not usually an emergency. Symptoms and management of hyperglycemia are included in the Diabetes Support Plan. Page 5 of 17
7 For planning and support for students in the event of a disaster or earthquake, consult BC Children's Hospital Earthquake Kit for Schools Nutritional Management and Physical Activity Children with diabetes should follow a healthy diet as recommended for all children in Eating Well with Canada s Food Guide. The maintenance of a proper balance of food, insulin and physical activity is important to achieving good blood glucose control in students with diabetes. Schools provide supportive and inclusive environments for students with diabetes. Students have unrestricted access to food and opportunities to participate in physical activities. Students with diabetes: Require unrestricted access to snacks and water anywhere, including the classroom, on field trips or the school bus, as necessary to prevent or treat low blood glucose; Require meal and snack times to be regular and predictable; Require adequate time to finish meals; Should be given the opportunity to participate fully and freely in physical activity and on sports teams; Be allowed to participate in classroom and school activities in a safe and inclusive manner; and Be allowed unrestricted access to use the washroom. Blood Glucose Monitoring Monitoring blood glucose is an essential component of diabetes management as it indicates whether insulin, food intake and activity are appropriately balanced. In the school setting, blood glucose monitoring is recommended at midmorning, lunchtime, two hours after lunch (midafternoon), before sport or exercise, and if there are concerns regarding low blood glucose or high blood glucose. More frequent blood glucose monitoring is not usually indicated. Special considerations regarding blood glucose monitoring may be required for students that have long commutes to and from school. Schools provide opportunities for students to check their blood glucose levels and to respond to the results when and where needed. For students not able to perform the task, NSS Coordinators are available to delegate to school staff the task of blood glucose monitoring or the supervision of the student. Students with diabetes: Are permitted to check blood glucose levels and respond to the results in the classroom, at every school location or at any school activity; Must be given access to all necessary supplies; and Page 6 of 17
8 If preferred by the student, a private location to do blood glucose monitoring must be provided unless low blood glucose is suspected. Insulin Administration Increasingly, intensive insulin therapies, either by multiple daily injections or via insulin pumps, are being recommended in the management of T1D in children and youth to improve blood glucose control and decrease long term health complications. Both therapies require insulin to be given during the school day. Conventional insulin regimes in which long-acting insulin is given outside of school hours are also being used and these regimes require regular and consistent food intake. The choice of insulin regime depends on many factors, including the child s age, duration of diabetes, lifestyle, targets of diabetes control, and family and student factors. Daily insulin dosage varies greatly between individuals and changes over time. Schools provide opportunities for students to administer insulin when and where it is needed. For students not able to perform the task, NSS Coordinators are available to delegate to school staff the task of insulin administration (via pump or pen) or the supervision of the student. School staff delegated in tasks related to insulin administration will follow the NSS Delegated Care Plan. Delegated school staff will not be permitted to, or allow a student in their care to: (1) override the calculated dose on the insulin pump, (2) change the number of carbohydrates from that actually consumed, (3) change the settings on the pump, (4) not follow the NSS Delegated Care Plan. Students who have insulin given by a school staff person need to have a Diabetes Medication Administration Form completed and signed by the student s physician. Roles and Responsibilities Parents/guardians: Parental consent and involvement is required for the child specific supports to be provided. Notify the school of their child s diabetes at the onset of his/her enrolment or upon diagnosis, and arrange a meeting with the school principal; Participate in the development of the Diabetes Support Plan and Medical Alert Information in collaboration with their health care provider and where applicable the Nursing Support Services Delegated Care Plan; Review the student s Diabetes Support Plan and Medical Alert Information annually with the school; If the student receives NSS Delegated Care, review and sign the NSS Delegated Care Plan annually or in the event of changes in the student s health status or diabetes regime; Page 7 of 17
9 Ensure the student wears medical identification; Inform the school of any relevant changes to the students lifestyle, health or diabetes management; Provide all snacks and lunches, as well as an ongoing supply of recommended fast-acting glucose for treating hypoglycemia (see examples in glossary). For students participating in a school breakfast or lunch program, parents work with the school to ascertain the carbohydrate content of menu items potentially consumed; For students using an intensive insulin regime who require assistance with carbohydrate counting: o Clearly and consistently label all snacks and meals with the correct carbohydrate number; and o If a student does not routinely consume an entire food item (such as a sandwich), the item should be provided in divided portions with carbohydrates clearly labeled for each portion. For young children, parents provide instructions for food provided during school parties and other activities; Provide all necessary supplies and equipment in full working order for blood glucose monitoring and insulin administration and replace supplies as needed; Provide adequate insulin to last the school day; For students using an insulin pump, trouble shoot all pump malfunctions and alarms and ensure the insertion site is functioning and be available for re insertion of infusion set if it becomes dislodged and the student is not able to self-manage; Provide an emergency glucagon kit with a clearly labelled expiration date and replace as needed; Provide supplies to be used in the event of a natural disaster; and Be available (or arrange for a delegate) to respond either by phone or in person at all times. Boards of Education: Ensure district policies and procedures are aligned with the Provincial Standards of Diabetes Care in the School Setting document. Ensure that schools are familiar with the Provincial Standards of Diabetes Care in the School Setting document and district policies and procedures related to supports for students with T1D, and that these policies are communicated to the public. Ensure that all school staff attend or review the General Information about Diabetes for School Personnel presentation. Ensure the poster Managing Low Blood Sugar is posted in visible locations in the school; Coordinate and ensure that two designated school personnel receive training on the administration of injectable glucagon if requested by parents. Support the completion the Diabetes Support Plan and Medical Alert Information and support staff to carry out the directions within that plan; Ensure schools have established a process by which all staff, including teachers on call, can identify student(s) with T1D enrolled in the school; For students approved to receive Delegated Care through NSS, the School Administrator will: Page 8 of 17
10 o Identify school staff to be trained and monitored in delegated nursing tasks. This includes situations in which there is staff turnover or when a staff person is not competent in performing the task as determined by the delegating nurse; o Ensure that assigned staff are fully available to attend all necessary initial and ongoing training provided by NSS; o Ensure that a NSS Delegated Care Plan is accessible to appropriate staff; o Ensure that only staff trained by the NSS Coordinator perform delegated tasks; and o Notify parents whenever trained staff are unavailable on a given day. Ensure schools policies address the storage of insulin and all other related supplies including the emergency glucagon kits; Ensure schools have policies and procedures for safe disposal of sharps; aligned with principles of universal precautions ; and Ensure timely notice is provided to parents/guardians of relevant changes in school district or school policies or of upcoming special events. Health Authorities: Provide glucagon administration training annually (or more frequently if required) to designated school staff in a school where a child or youth with T1D attends, and if glucagon administration is requested by the parent; Support the NSS Coordinator s role in determining that delegating the task of insulin administration and/or blood glucose monitoring is in the best interest of the student. This role includes assessing the care needs of the student, the complexity of the task, the environment in which the task will be performed, and the suitability of the school staff person(s) to carry out the task. There may be situations when delegation is not possible; Support the NSS Coordinator s role in developing and implementing the NSS Delegated Care Plan in consultation with the parent/guardian; and Support the NSS Coordinator s role in training and monitoring delegated school staff. Page 9 of 17
11 Glossary Blood glucose: The amount of glucose (sugar) in the blood at a given time. Blood glucose monitoring, or self-monitoring of blood glucose: People with diabetes must monitor their blood glucose regularly as part of the process for achieving their target blood glucose level. Levels will change depending on food consumption, physical activity, stress, illness, problems with the insulin delivery system and many other unknown factors. To test blood glucose, the individual pricks his or her finger with a lancing device and places a drop of blood on a blood glucose strip, which is inserted into a blood glucose meter to obtain a reading. Carbohydrate: One of the main sources of energy (calories). All forms of carbohydrate are broken down into glucose during digestion and increase blood glucose. Carbohydrates are found in fruits, vegetables, milk and grains/starches such as rice, potatoes, corn and legumes, and refined sugars. Delegation: Occurs when the required task is performed primarily by registered nurses and is outside the role description and training of an unregulated care provider, such as a school staff member. The delegated task is client-specific and the delegation is determined to be in the client s best interests The delegating Registered Nurse is responsible and accountable for the decision to delegate and the process of delegation including the ongoing supervision to assess the ability of the unregulated care provider to perform the delegated task. The unregulated care provider is accountable to the Registered Nurse for the performance of the delegated task. Diabetes Care Team: The team of health professionals who work with the student and family to manage the student s diabetes. This may include: Pediatric Endocrinologists, Pediatricians, Family Physicians, Diabetes Clinic Nurses, Dietitians, Social Workers, or Pharmacists. Diabetic ketoacidosis (DKA): An acute and severe complication of diabetes that is the result of high levels of blood glucose and ketones. It is often associated with poor control of diabetes or occurs as a complication of other illnesses. It can be life threatening and requires emergency treatment. Signs and symptoms include fruity odour on the breath, shortness of breath, confusion, nausea, vomiting and weight loss. Page 10 of 17
12 Fast-acting carbohydrate: (or fast-acting sugar) A carbohydrate to eat or drink for the treatment of mild to moderate hypoglycemia (e.g. juice, glucose tablets) to quickly raise the blood glucose level. Because of the importance of preventing severe hypoglycemia, the following items are recommended, depending on the weight of the student: 10 grams OR 15 grams Glucose tablets as labelled Glucose tablets as labelled 1/2 cup of juice or regular soft drink 3/4 cup of juice or regular soft drink 10 ml (2 teaspoons) or 2 packets of table sugar dissolved in water 15 ml (1 tablespoon) or 3 packets of table sugar dissolved in water 2 teaspoons of honey 1 tablespoon of honey 10 skittles 15 skittles OR: Other items as recommended by the students diabetes care team Glucagon: A hormone that raises blood glucose. An injectable form of glucagon is used to treat severe hypoglycemia. Glucose: The fuel that the body needs to produce energy. Glucose (sugar) comes from carbohydrates such as breads, cereal, fruit and milk. Hyperglycemia, or high blood glucose: A situation that occurs when the amount of blood glucose (sugar) is higher than an individual s target range. Hypoglycemia, or low blood glucose: Occurs when the amount of blood glucose (sugar) is lower than 4.0 mmol/l. Hypoglycemia can be mild, moderate or severe. It is often preventable and is the greatest immediate danger to students with type 1 diabetes. Severe Hypoglycemia: Occurs when a student with hypoglycemia is unconscious, having a seizure, or so uncooperative that the student is unable to consume oral fast-acting sugar. Caregivers should administer glucagon, if trained and if parents have consented. Always call and parents. Insulin: A hormone that facilitates the conversion of glucose to energy. Since people with type 1 diabetes cannot produce their own insulin, glucose builds up in the blood instead of being used for energy. They must therefore administer insulin by syringe, insulin pen or insulin pump. Insulin pen: A cartridge pen-like device used to inject insulin into the body. The pen is preloaded with insulin. Insulin pump: A computerized device that is programmed to deliver small, steady doses of insulin throughout the day. Additional doses are given when needed to cover food intake and to lower high blood glucose levels. The insulin is delivered through a system of plastic tubing (infusion set). Medical Alert Identification: An identification card, necklace, or bracelet indicating a student has diabetes and listing emergency numbers to call for help. Page 11 of 17
13 Sharps: Used syringes, insulin pen needles, and lancets. These items must be carefully disposed of in appropriate containers. Target blood glucose range: Acceptable blood glucose levels based on the 2013 Canadian Diabetes Association s Clinical Practice Guidelines and personalized for the student, by their diabetes care team and their parent or guardian. Type 1 diabetes: An autoimmune disease that occurs when the pancreas no longer produces any insulin or produces very little insulin. Type 1 diabetes usually develops in childhood or adolescence and affects approximately 10% of people with diabetes. There is no cure. It is usually treated with lifelong insulin injections and careful attention to diet and physical activity. Type 2 diabetes: A disease that occurs when the pancreas does not produce enough insulin to meet the body s needs and/or the body is unable to respond properly to the actions of insulin (insulin resistance). Type 2 diabetes usually occurs later in life (although it can occur in children) and affects approximately 90% of people with diabetes. There is no cure. It is treated with careful attention to diet and exercise and usually requires medication (oral antihyperglycemic agents) and/or insulin. Page 12 of 17
14 Appendices: Provincial Standards: Supporting Students with Type 1 Diabetes in the School Setting Diabetes Support Plan and Medical Alert Information Instructions: This form is a communication tool for use by parents to share information with the school. Students who are receiving Nursing Support Services (NSS) Delegated Care do not need to complete page 3. This form does NOT need to be completed by Diabetes Clinic staff, Nursing Support Service Coordinators or Public Health Nurses. Name of Student: Date of Birth; School: Grade: Teacher/Div: Care Card Number: Date of Plan: CONTACT INFORMATION Parent/Guardian 1: Name: Call First Phone Numbers: Cell Work Home Other Parent/Guardian 2: Name: Call First Phone Numbers: Cell: Work: Home: Other: Other/Emergency: Name: Able to advise on diabetes care: Yes No Relationship: Phone Numbers: Cell: Work: Home: Other: Have emergency supplies been provided in the event of a natural disaster? Yes No If yes, location of emergency supply of insulin: STUDENTS RECEIVING NSS DELEGATED CARE NSS Coordinator: Phone: School staff providing delegated care: Parent Signature: Name: Date: Page 13 of 17
15 MEDICAL ALERT - TREATING MILD TO MODERATE LOW BLOOD GLUCOSE NOTE: PROMPT ATTENTION CAN PREVENT SEVERE LOW BLOOD GLUCOSE SYMPTOMS Shaky, sweaty Hungry Pale Dizzy Irritable Tired/sleepy Blurry vision Confused Poor coordination Difficulty speaking Headache Difficulty concentrating Other: TREATMENT FOR STUDENTS NEEDING ASSISTANCE (anyone can give sugar to a student): Location of fast acting sugar: 1. If student able to swallow, give one of the following fast acting sugars: 10 grams glucose tablets 1/2 cup of juice or regular soft drink 2 teaspoons of honey 10 skittles 10 ml (2 teaspoons) or 2 packets of table sugar dissolved in water Other (ONLY if 10 grams are labelled on package): 2. Contact designated emergency school staff person OR 15 grams glucose tablets 3/4 cup of juice or regular soft drink 1 tablespoon of honey 15 skittles 15 ml (1 tablespoon) or 3 packets of table sugar dissolved in water Other (ONLY if 15 grams are labelled on package): 3. Blood glucose should be retested in 15 minutes. Retreat as above if symptoms do not improve or if blood glucose remains below 4 mmol/l 4. Do not leave student unattended until blood glucose 4 mmol/l or above 5. Give an extra snack such as cheese and crackers if next planned meal/snack is not for 45 minutes. MEDICAL ALERT GIVING GLUCAGON FOR SEVERE LOW BLOOD GLUCOSE SYMPTOMS PLAN OF ACTION Unconsciousness Having a seizure (or jerky movements) So uncooperative that you cannot give juice or sugar by mouth Place on left side and maintain airway Call 911, then notify parents Manage a seizure: protect head, clear area of hard or sharp objects, guide arms and legs but do not forcibly restrain, do not put anything in mouth Administer glucagon Medication Dose & Route Directions Glucagon (GlucaGen or Lilly Glucagon) Frequency: Emergency treatment for severe low blood glucose 0.5 mg =0.5 ml. (for students 5 years of age and under) OR 1.0 mg = 1.0 ml. (for students 6 years of age and over) Give by injection: Intramuscular Remove cap Inject liquid from syringe into dry powder bottle Roll bottle gently to dissolve powder Draw fluid dose back into the syringe Inject into outer mid-thigh (may go through clothing) Once student is alert, give juice or fast acting sugar Page 14 of 17
16 LEVEL OF SUPPORT REQUIRED FOR STUDENTS NOT RECEIVING NSS DELEGATED CARE Requires checking that task is done (child is proficient in task): Blood glucose testing Carb counting/adding Administers insulin Eating on time if on NPH insulin Act based on BG result Requires reminding to complete: Blood glucose testing Carb counting/adding Insulin administration Eating on time if on NPH insulin Act based on BG result Student is completely independent MEAL PLANNING: The maintenance of a proper balance of food, insulin and physical activity is important to achieving good blood glucose control in students with diabetes. In circumstances when treats or classroom food is provided but not labelled, the student is to: Call the parent for instructions Manage independently BLOOD GLUCOSE TESTING: Students must be allowed to check blood glucose level and respond to the results in the classroom, at every school location or at any school activity. If preferred by the student, a private location to do blood glucose monitoring must be provided, unless low blood glucose is suspected. Frequency of Testing: midmorning lunchtime mid afternoon before sport or exercise With symptoms of hyper/hypoglycemia Before leaving school Location of equipment: With student In classroom In office Other Time of day when low blood glucose is most likely to occur: Instructions if student takes school bus home: PHYSICAL ACTIVITY: Physical exercise can lower the blood glucose level. A source of fast-acting sugar should be within reach of the student at all times (see page 2 for more details). Blood glucose monitoring is often performed prior to exercise. Extra carbohydrates may need to be eaten based on the blood glucose level and the expected intensity of the exercise. Comments: INSULIN: All students with type 1 diabetes use insulin. Some students require insulin during the school day, most commonly before meals. Is insulin required at school on a daily basis? Yes No Insulin delivery system: Pump Pen Needle and syringe (at home or student fully independent) Frequency of insulin administration: Location of insulin: with student In classroom In office Other Insulin should never be stored in a locked cupboard. Page 15 of 17
17 Diabetes Medication Administration Form Instructions: This form is updated annually to document physician approval regarding the following: Administration of glucagon by school staff Administration of insulin by school staff for a student not able to complete the task (NSS Delegated Care) Supervision by school staff of a student self-administering insulin who is not yet fully independent in the task (NSS Delegated Care) Student Name: Date of Birth: School: Care Card Number: Parent/Guardians Name(s): Home Phone: Cell Phone: Glucagon (GlucaGen or Lilly Glucagon ) For severe low blood glucose, give by intramuscular injection: 0.5 mg = 0.5 ml for students 5 years of age and under 1.0 mg = 1.0 ml for students 6 years of age and over Insulin (rapid acting insulin only) Insulin delivery device: insulin pump insulin pen Note: The following cannot be accommodated when insulin administration is being delegated to a school staff person via pump or pen: Overriding the calculated dose Entering an altered carbohydrate count for foods in order to change the insulin dose Changing the settings on the pump Deviating from the NSS Delegated Care Plan For students using an insulin pen, insulin may be administered at lunchtime only (due to the inability to accurately calculate insulin on board). The method of calculating the dose is as follows: Bolus Calculator Sheet Variable dose insulin scale for blood glucose for consistent carbohydrates consumed InsuLinx Meter Parent/guardian authority to adjust insulin dose for bolus calculator sheet or sliding scale: Yes No For students using an insulin pump, insulin can be given if needed at recess, lunch and two hours after lunch (as there is an ability to know the insulin on board). I agree the student s diabetes can be safely managed at school within the above parameters Physician Signature: Date: Physician Name: Clinic Phone Number: Page 16 of 17
18 Websites and Links to Diabetes Information Materials General Information About Diabetes for School Personnel Narrated Presentation Glucagon Administration Presentation with Speaking Notes Managing Low Blood Sugar - Poster Ministry of Education - Ministry of Children and Family Development - Canadian Diabetes Association - Child Health BC - Page 17 of 17
OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN
 PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
PART I OFFICE OF CATHOLIC SCHOOLS DIOCESE OF ARLINGTON DIABETES MEDICAL MANAGEMENT PLAN Page 1 of 5 TO BE COMPLETED BY PARENT OR GUARDIAN Student School Date of Birth Date of Diagnosis Grade/ Teacher Physical
Riley Hospital for Children General Diabetes Medical Management Information- Injections
 Riley Hospital for Children General Diabetes Medical Management Information- Injections 1. HEALTH CARE SUPERVISION All school support staff, including: secretaries, cafeteria staff, custodians and bus
Riley Hospital for Children General Diabetes Medical Management Information- Injections 1. HEALTH CARE SUPERVISION All school support staff, including: secretaries, cafeteria staff, custodians and bus
Diabetes Management and Treatment Plan for School (For the insulin pump student)
 Lafayette School Corporation Health Services Diabetes Management and Treatment Plan for School (For the insulin pump student) Effective Dates: This plan should be complete by the student s personal health
Lafayette School Corporation Health Services Diabetes Management and Treatment Plan for School (For the insulin pump student) Effective Dates: This plan should be complete by the student s personal health
Diabetes Health Care Plan
 The Public Schools of Brookline School Health Services of Plan: Diabetes Health Care Plan To be completed by the student s health care team and parents/guardian. Plan will be kept with the school nurse
The Public Schools of Brookline School Health Services of Plan: Diabetes Health Care Plan To be completed by the student s health care team and parents/guardian. Plan will be kept with the school nurse
Diabetes Medical Management Plan
 Diabetes Medical Management Plan 1 School District: School: School Year: Grade: Student Name: DOB: Provider Name: Phone #: Fax #: Blood Glucose Monitoring at School Blood Glucose Target Range: - mg/dl
Diabetes Medical Management Plan 1 School District: School: School Year: Grade: Student Name: DOB: Provider Name: Phone #: Fax #: Blood Glucose Monitoring at School Blood Glucose Target Range: - mg/dl
Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106
 EMPOW ERING A COMMUNITY OF LEARNERS AND LEADERS Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106 Student DOB School Grade Doctor Phone School Year
EMPOW ERING A COMMUNITY OF LEARNERS AND LEADERS Diabetes Insulin Pump Health Care Plan District Nurse Phone: 262-560-2104 District Nurse Fax: 262-560-2106 Student DOB School Grade Doctor Phone School Year
School Year 20 / 20. Diabetes Health Care Plan for Southgate Schools
 School Year 20 / 20 Diabetes Health Care Plan for Southgate Schools Diabetes Medical Management Plan, Initialized Healthcare Plan and Physician Orders Part A: Contact Information must be completed by the
School Year 20 / 20 Diabetes Health Care Plan for Southgate Schools Diabetes Medical Management Plan, Initialized Healthcare Plan and Physician Orders Part A: Contact Information must be completed by the
Section 504 Plan (pg 1 of 8)
 Section 504 Plan (pg 1 of 8) of Birth School Today s Section 504 Plan for: Disability: Diabetes School Year: Grade: Homeroom Teacher: Bus Number: Background Objectives The student has type diabetes. Diabetes
Section 504 Plan (pg 1 of 8) of Birth School Today s Section 504 Plan for: Disability: Diabetes School Year: Grade: Homeroom Teacher: Bus Number: Background Objectives The student has type diabetes. Diabetes
ALVIN INDEPENDENT SCHOOL DISTRICT Diabetes Medical Management Plan
 ALVIN INDEPENDENT SCHOOL DISTRICT Diabetes Medical Management Plan of Plan: School Year (must be current): This plan should be completed by the student s personal health care team and parents/guardian.
ALVIN INDEPENDENT SCHOOL DISTRICT Diabetes Medical Management Plan of Plan: School Year (must be current): This plan should be completed by the student s personal health care team and parents/guardian.
Telephone: Home Work Cell E-mail Address Father/Guardian: Address:
 SAMPLE Diabetes Medical Management Plan/Individualized Healthcare Plan Part A: Contact Information must be completed by the parent/guardian. Part B: Diabetes Medical Management Plan (DMMP) must be completed
SAMPLE Diabetes Medical Management Plan/Individualized Healthcare Plan Part A: Contact Information must be completed by the parent/guardian. Part B: Diabetes Medical Management Plan (DMMP) must be completed
Diabetes. Emergency Checklists. From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed.
 Diabetes Emergency Checklists From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed. Hyperglycemia High Blood Sugar * Hyperglycemia occurs when the blood
Diabetes Emergency Checklists From A Child in Your Care Has Diabetes. A Collection of Information. Copyright 2005 by Elisa Hendel, M.Ed. Hyperglycemia High Blood Sugar * Hyperglycemia occurs when the blood
Diab.etes Me.dic.al-Ma-nage-me-n-t -P-la-n -.
 Date of Plan: Diab.etes Me.dic.al-Ma-nage-me-n-t -P-la-n -. Effective Dates: WJ Student's Name: Date of Birth:,-..,,;... Date of Diabetes Diagnosis: Grade: Homeroom Teacher: Physical Condition: 0 Diabetes
Date of Plan: Diab.etes Me.dic.al-Ma-nage-me-n-t -P-la-n -. Effective Dates: WJ Student's Name: Date of Birth:,-..,,;... Date of Diabetes Diagnosis: Grade: Homeroom Teacher: Physical Condition: 0 Diabetes
Diabetes Medical Management Plan (DMMP)
 Diabetes Medical Management Plan (DMMP) This plan should be completed by the student s personal diabetes health care team, including the parents/guardian. It should be reviewed with relevant school staff
Diabetes Medical Management Plan (DMMP) This plan should be completed by the student s personal diabetes health care team, including the parents/guardian. It should be reviewed with relevant school staff
Guidelines for the Care *
 Guidelines for the Care * Purpose: To acknowledge and help clarify the essential roles and responsibilities among the Diabetes Care Team (DCT), which is comprised of the student living with diabetes, his
Guidelines for the Care * Purpose: To acknowledge and help clarify the essential roles and responsibilities among the Diabetes Care Team (DCT), which is comprised of the student living with diabetes, his
SCHOOL DISTRICT #22 VERNON DIABETES POLICY
 SCHOOL DISTRICT #22 VERNON DIABETES POLICY A student with diabetes does not automatically qualify for additional support. The student may qualify as a temporary D category (chronic health) after diagnosis
SCHOOL DISTRICT #22 VERNON DIABETES POLICY A student with diabetes does not automatically qualify for additional support. The student may qualify as a temporary D category (chronic health) after diagnosis
Acknowledgements. The working group consists of the following individuals:
 Acknowledgements This document is based largely on the New Brunswick Department of Education and Early Childhood Development Handbook for Type 1 Diabetes Management in Schools. We are indebted to New Brunswick
Acknowledgements This document is based largely on the New Brunswick Department of Education and Early Childhood Development Handbook for Type 1 Diabetes Management in Schools. We are indebted to New Brunswick
Anchor Bay School District Diabetic Medical Care Plan. Student Name Date Grade Teacher
 Rev: 4/2009 Anchor Bay School District Diabetic Medical Care Plan Place Child s Picture Here Student Name Date Grade Teacher Emergency Contact information (Please list in order to be called) #1 Parent
Rev: 4/2009 Anchor Bay School District Diabetic Medical Care Plan Place Child s Picture Here Student Name Date Grade Teacher Emergency Contact information (Please list in order to be called) #1 Parent
Dear Parent/Guardian and Physician of
 DIABETIC MANAGEMENT PLAN Parent Consent and Physician Authorization POWAY UNIFIED SCHOOL DISTRICT HEALTH SERVICES 15250 Avenue of Science San Diego CA 92128 Dear Parent/Guardian and Physician of California
DIABETIC MANAGEMENT PLAN Parent Consent and Physician Authorization POWAY UNIFIED SCHOOL DISTRICT HEALTH SERVICES 15250 Avenue of Science San Diego CA 92128 Dear Parent/Guardian and Physician of California
TYPE 2 DIABETES PROCEDURES AND FORMS ELEMENTARY SECONDARY SCHOOL ADMINISTRATOR
 TYPE 2 DIABETES PROCEDURES AND FORMS ELEMENTARY SECONDARY SCHOOL ADMINISTRATOR 2013 SCHOOL ADMINISTRATOR TYPE 2 DIABETES PROCEDURES and FORMS: Parent/guardian informs school administrator child/youth has
TYPE 2 DIABETES PROCEDURES AND FORMS ELEMENTARY SECONDARY SCHOOL ADMINISTRATOR 2013 SCHOOL ADMINISTRATOR TYPE 2 DIABETES PROCEDURES and FORMS: Parent/guardian informs school administrator child/youth has
Guidelines for the Care Needed for Students with Diabetes
 Guidelines for the Care Needed for Students with Diabetes for the implementation of State Board of Education Rule 160-4-8-.18 Diabetes Medical Management Plans Version 1.0 Table of Contents (1) DEFINITIONS:...
Guidelines for the Care Needed for Students with Diabetes for the implementation of State Board of Education Rule 160-4-8-.18 Diabetes Medical Management Plans Version 1.0 Table of Contents (1) DEFINITIONS:...
Name Date. Doctor. Usual times to test glucose at school Extra tests (check those that apply) before exercise after exercise other (explain)
 Appendix A SAMPLE IHP Name Date Phone numbers Blood glucose Hypoglycemia Hyperglycemia Insulin Parent/guardian#1 Work Home Parent/guardian#2 Work Home Other emergency contact Doctor Usual times to test
Appendix A SAMPLE IHP Name Date Phone numbers Blood glucose Hypoglycemia Hyperglycemia Insulin Parent/guardian#1 Work Home Parent/guardian#2 Work Home Other emergency contact Doctor Usual times to test
FHUSD Diabetic Management Plan
 This plan should be completed by the student s personnel Physician or Licensed Healthcare Provider and parent/guardian. It should be reviewed with relevant school staff and copies should be kept in a place
This plan should be completed by the student s personnel Physician or Licensed Healthcare Provider and parent/guardian. It should be reviewed with relevant school staff and copies should be kept in a place
THE MOLLY CENTER FOR CHILDREN WITH DIABETES AND ENDOCRINE DISORDERS DIABETES-HEALTH CARE PLAN
 THE MOLLY CENTER FOR CHILDREN WITH DIABETES AND ENDOCRINE DISORDERS DIABETES-HEALTH CARE PLAN (To be completed by parent and school nurse) DATE: SCHOOL: GRADE: STUDENT: BIRTHDATE: HOME ADDRESS: PARENT/GUARDIAN:
THE MOLLY CENTER FOR CHILDREN WITH DIABETES AND ENDOCRINE DISORDERS DIABETES-HEALTH CARE PLAN (To be completed by parent and school nurse) DATE: SCHOOL: GRADE: STUDENT: BIRTHDATE: HOME ADDRESS: PARENT/GUARDIAN:
Diabetes Hypoglycemia/Hyperglycemia Reaction
 Diabetes Hypoglycemia/Hyperglycemia Reaction Hypoglycemic Reaction (Insulin Shock) A. Hypoglycemic reactions (insulin reactions) should be treated according to current nursing and medical recommendations.
Diabetes Hypoglycemia/Hyperglycemia Reaction Hypoglycemic Reaction (Insulin Shock) A. Hypoglycemic reactions (insulin reactions) should be treated according to current nursing and medical recommendations.
BLOOD GLUCOSE MONITORING MEDICATION
 DIABETES CARE FOR SCHOOL MEDICAL MANAGEMENT PLAN Most Recent A1C and Date: BLOOD GLUCOSE MONITORING Meter Type: Testing Independently: yes no Testing times: Before meals Two hours after insulin dosing
DIABETES CARE FOR SCHOOL MEDICAL MANAGEMENT PLAN Most Recent A1C and Date: BLOOD GLUCOSE MONITORING Meter Type: Testing Independently: yes no Testing times: Before meals Two hours after insulin dosing
Section 6: Diabetes Emergencies
 Section 6: Diabetes Emergencies SECTION OVERVIEW General Overview Low Blood Glucose (Hypoglycemia) Glucagon High Blood Glucose (Hyperglycemia) Diabetic Ketoacidosis Monitoring Ketones Emergency Medical
Section 6: Diabetes Emergencies SECTION OVERVIEW General Overview Low Blood Glucose (Hypoglycemia) Glucagon High Blood Glucose (Hyperglycemia) Diabetic Ketoacidosis Monitoring Ketones Emergency Medical
Diabetes Education Information for Teachers and School staff
 Diabetes Education Information for Teachers and School staff The information below is intended to educate school staff on the basics of diabetes care. If you have a student in your classroom or you will
Diabetes Education Information for Teachers and School staff The information below is intended to educate school staff on the basics of diabetes care. If you have a student in your classroom or you will
LOW BLOOD Glucose with TYPE 1 DIABETES
 LOW BLOOD Glucose with TYPE 1 DIABETES Hypoglycemia is the medical term for low blood glucose or low blood sugar. It occurs when blood glucose (sugar) drops below the normal range (i.e below 4 mmol/l).
LOW BLOOD Glucose with TYPE 1 DIABETES Hypoglycemia is the medical term for low blood glucose or low blood sugar. It occurs when blood glucose (sugar) drops below the normal range (i.e below 4 mmol/l).
INSULIN-DEPENDENT DIABETES HEALTH CARE PLAN: II
 INSULIN-DEPENDENT DIABETES HEALTH CARE PLAN: II DATE: SCHOOL: GRADE: STUDENT: BIRTHDATE: HOME ADDRESS: PARENT/GUARDIAN: PARENT S PHONE: Home: Mom s work: Dad s work: EMERGENCY CONTACT (NAME, NUMBER and
INSULIN-DEPENDENT DIABETES HEALTH CARE PLAN: II DATE: SCHOOL: GRADE: STUDENT: BIRTHDATE: HOME ADDRESS: PARENT/GUARDIAN: PARENT S PHONE: Home: Mom s work: Dad s work: EMERGENCY CONTACT (NAME, NUMBER and
Helping you help students manage their diabetes. Canadian Diabetes Association s website at diabetes.ca. More information
 Kids with diabetes in your care management Helping you help students manage their diabetes This resource kit provides basic information to people who provide care to students with diabetes, including parents/guardians,
Kids with diabetes in your care management Helping you help students manage their diabetes This resource kit provides basic information to people who provide care to students with diabetes, including parents/guardians,
Blood Sugar and How to Manage It
 PO Box 70735, SW Station Washington, DC 20024-0735 800-717-0060 office / 202-889-0502 fax Young Marines Diabetes Care Plan Child s Name: Date of Birth: Age: Unit: Event: (Drill, Encampment, SPACES, NDSP,
PO Box 70735, SW Station Washington, DC 20024-0735 800-717-0060 office / 202-889-0502 fax Young Marines Diabetes Care Plan Child s Name: Date of Birth: Age: Unit: Event: (Drill, Encampment, SPACES, NDSP,
Student Name: Date of Birth:
 Place Photo Here ITASCA DISTRICT 10 DIABETES CARE PLAN Student Name: Date of Birth: Date of Conference: School Nurse: Health Data: has diabetes. This is a condition in which the pancreas is unable to make
Place Photo Here ITASCA DISTRICT 10 DIABETES CARE PLAN Student Name: Date of Birth: Date of Conference: School Nurse: Health Data: has diabetes. This is a condition in which the pancreas is unable to make
SAMPLE SECTION 504 PLAN
 SAMPLE SECTION 504 PLAN The attached sample Section 504 Plan was developed by the American Diabetes Association (ADA) and the Disability Rights Education and Defense Fund, Inc. (DREDF). 0 MODEL 504 PLAN
SAMPLE SECTION 504 PLAN The attached sample Section 504 Plan was developed by the American Diabetes Association (ADA) and the Disability Rights Education and Defense Fund, Inc. (DREDF). 0 MODEL 504 PLAN
Equipment and Supplies Checklist for Parents Student: DOB: School: Grade: Equipment and Supplies to be Provided by Parent. Parent Signature Date
 Equipment and Supplies Checklist for Parents Student: DOB: School: Grade: Equipment and Supplies to be Provided by Parent Parent Signature Date Daily Snacks (for AM/PM snack times): Specify: Extra Snacks
Equipment and Supplies Checklist for Parents Student: DOB: School: Grade: Equipment and Supplies to be Provided by Parent Parent Signature Date Daily Snacks (for AM/PM snack times): Specify: Extra Snacks
Green Brook Township School District DIABETES- Insulin Pump IHP/IEHP
 Green Brook Township School District DIABETES- Insulin Pump IHP/IEHP 1. Personal Information: I. STUDENT INFORMATION NAME: Grade HR.- Teacher: Address Home Phone #: Birth date Bus: # N/A Gender Male Female
Green Brook Township School District DIABETES- Insulin Pump IHP/IEHP 1. Personal Information: I. STUDENT INFORMATION NAME: Grade HR.- Teacher: Address Home Phone #: Birth date Bus: # N/A Gender Male Female
See, Think, and Act! Diabetes
 See, Think, and Act! Diabetes California After School Resource Center (CASRC) Administered for the California Department of Education (C.D.E.) Hello. My name is Joan Edelstein. I am a health trainer for
See, Think, and Act! Diabetes California After School Resource Center (CASRC) Administered for the California Department of Education (C.D.E.) Hello. My name is Joan Edelstein. I am a health trainer for
2. What Should Advocates Know About Diabetes? O
 2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
DIABETES PACKET. To ensure your child s well-being, please provide the school with the following supplies:
 NSG-203A NORTH ROYALTON CITY SCHOOLS 6579 Royalton Road North Royalton, Ohio 44133 DIABETES PACKET Dear Parent/Guardian: You have indicated that your child has Diabetes. Please complete the attached SCHOOL
NSG-203A NORTH ROYALTON CITY SCHOOLS 6579 Royalton Road North Royalton, Ohio 44133 DIABETES PACKET Dear Parent/Guardian: You have indicated that your child has Diabetes. Please complete the attached SCHOOL
Glucagon Training Standards for School Personnel: Providing Emergency Medical Assistance to Pupils with Diabetes
 Glucagon Training Standards for School Personnel: Providing Emergency Medical Assistance to Pupils with Diabetes Performance Standards for the Training and Supervision of School Personnel in Providing
Glucagon Training Standards for School Personnel: Providing Emergency Medical Assistance to Pupils with Diabetes Performance Standards for the Training and Supervision of School Personnel in Providing
The Nursing Department of Central CUSD 301 provides nursing services that promote students ability to learn. Our goals are to:
 Date Dear (Parent / Guardian), The Nursing Department of Central CUSD 301 provides nursing services that promote students ability to learn. Our goals are to: o Assist students in learning how to take care
Date Dear (Parent / Guardian), The Nursing Department of Central CUSD 301 provides nursing services that promote students ability to learn. Our goals are to: o Assist students in learning how to take care
Managing Diabetes in the School Setting. Alabama State Department of Education Alabama Board of Nursing
 Managing Diabetes in the School Setting Alabama State Department of Education Alabama Board of Nursing Diabetes Mellitus: Type I Diabetes Previously called Insulin-dependent or Juvenile Onset Diabetes
Managing Diabetes in the School Setting Alabama State Department of Education Alabama Board of Nursing Diabetes Mellitus: Type I Diabetes Previously called Insulin-dependent or Juvenile Onset Diabetes
Diabetes in School. Interior Health. March 2010
 Diabetes in School Interior Health March 2010 What is Diabetes? Diabetes is a chronic health condition in which the body cannot use the glucose (sugar) found in food Not contagious Without glucose the
Diabetes in School Interior Health March 2010 What is Diabetes? Diabetes is a chronic health condition in which the body cannot use the glucose (sugar) found in food Not contagious Without glucose the
Management of the Student with Diabetes in Schools
 Michigan Department of Education Michigan Department of Community Health Management of the Student with Diabetes in Schools MODEL SCHOOL NURSE GUIDELINE Original Date of Issue: 2013 Foreword These guidelines
Michigan Department of Education Michigan Department of Community Health Management of the Student with Diabetes in Schools MODEL SCHOOL NURSE GUIDELINE Original Date of Issue: 2013 Foreword These guidelines
High blood sugars caused by steroids
 High blood sugars caused by steroids Your blood sugars are high because you are taking a medication called steroids. Steroids are used to: decrease swelling decrease the natural response of your immune
High blood sugars caused by steroids Your blood sugars are high because you are taking a medication called steroids. Steroids are used to: decrease swelling decrease the natural response of your immune
Procedure for the Management of. when unwell. To be completed at the start of each academic year and reviewed regularly.
 The student/parents should provide the teacher/school with: Sufficient oral and written information to allow the school to have a safe and appropriate environment for their child Supplies to treat low
The student/parents should provide the teacher/school with: Sufficient oral and written information to allow the school to have a safe and appropriate environment for their child Supplies to treat low
Insulin pump: advice for schools
 Insulin pump: advice for schools Information for school staff Dr Gray s Hospital Your pupil.. has Type 1 insulin dependent diabetes. This means that the pancreas has stopped making the hormone insulin.
Insulin pump: advice for schools Information for school staff Dr Gray s Hospital Your pupil.. has Type 1 insulin dependent diabetes. This means that the pancreas has stopped making the hormone insulin.
A Training Program for Diabetes Management in the School Setting: The Role of Unlicensed School Staff. Virginia Department of Education 2015
 A Training Program for Diabetes Management in the School Setting: The Role of Unlicensed School Staff Virginia Department of Education 2015 Objectives To understand legal authorization and protection for
A Training Program for Diabetes Management in the School Setting: The Role of Unlicensed School Staff Virginia Department of Education 2015 Objectives To understand legal authorization and protection for
My Sick Day Plan for Type 1 Diabetes on an Insulin Pump
 My Sick Day Plan for Type 1 Diabetes on an Insulin Pump When you are sick, your blood sugar levels may be harder to keep under control. Your blood sugar may go too high or too low. Use this guide to help
My Sick Day Plan for Type 1 Diabetes on an Insulin Pump When you are sick, your blood sugar levels may be harder to keep under control. Your blood sugar may go too high or too low. Use this guide to help
Getting the Big Picture
 About Diabetes This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding your health. Please consult
About Diabetes This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding your health. Please consult
Insulin pen start checklist
 Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Your Road Map to Diabetes Medication Administration Record (Part 1)
 Your Road Map to Diabetes Medication dministration Record (Part 1) Ohio Revised ode (3313.713) is the education law that addresses prescriptive medication administration in Ohio schools. This OR lists
Your Road Map to Diabetes Medication dministration Record (Part 1) Ohio Revised ode (3313.713) is the education law that addresses prescriptive medication administration in Ohio schools. This OR lists
Introduction. We hope this guide will aide you and your staff in creating a safe and supportive environment for your students challenged by diabetes.
 Introduction Diabetes is a chronic disease that affects the body s ability to metabolize food. The body converts much of the food we eat into glucose, the body s main source of energy. Glucose is carried
Introduction Diabetes is a chronic disease that affects the body s ability to metabolize food. The body converts much of the food we eat into glucose, the body s main source of energy. Glucose is carried
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
Starting Insulin Injections
 Starting Insulin Injections A Gestational Diabetes Information Booklet Supported by What does insulin do? insulin Insulin is made by your pancreas. pancreas Insulin is released into the blood when you
Starting Insulin Injections A Gestational Diabetes Information Booklet Supported by What does insulin do? insulin Insulin is made by your pancreas. pancreas Insulin is released into the blood when you
Diabetes Information
 Diabetes Information Your diabetes team includes: Consultant Paediatric Endocrinologist Paediatric Diabetes Clinical Nurse Specialists Senior Clinical Nutritionists/Dietitians Senior Clinical Psychologist
Diabetes Information Your diabetes team includes: Consultant Paediatric Endocrinologist Paediatric Diabetes Clinical Nurse Specialists Senior Clinical Nutritionists/Dietitians Senior Clinical Psychologist
Diabetes Management. Managing Diabetes in our Schools
 Diabetes Management Managing Diabetes in our Schools 2010 The Toronto District School Board has a primary responsibility to ensure the safety of students and staff inside our schools and on Board property.
Diabetes Management Managing Diabetes in our Schools 2010 The Toronto District School Board has a primary responsibility to ensure the safety of students and staff inside our schools and on Board property.
Section 2: Quick Tip Sheets
 Section 2: Quick Tip Sheets SECTION OVERVIEW Diabetes: The Basic Facts Blood Glucose Monitor Use Signs and Symptoms of Low Blood Glucose (Hypoglycemia) Low Blood Glucose (Hypoglycemia) Action Plan Signs
Section 2: Quick Tip Sheets SECTION OVERVIEW Diabetes: The Basic Facts Blood Glucose Monitor Use Signs and Symptoms of Low Blood Glucose (Hypoglycemia) Low Blood Glucose (Hypoglycemia) Action Plan Signs
Hypoglycemia and Diabetes
 My Doctor Says I Should Avoid Low Blood Glucose Reactions... How Can I Prevent Them? BD Getting Started Hypoglycemia and Diabetes What You Should Know About Low Blood Glucose Reactions If you are taking
My Doctor Says I Should Avoid Low Blood Glucose Reactions... How Can I Prevent Them? BD Getting Started Hypoglycemia and Diabetes What You Should Know About Low Blood Glucose Reactions If you are taking
Blood Glucose Management
 Blood Glucose Management What Influences Blood Sugar Levels? There are three main things that influence your blood sugar: Nutrition Exercise Medication What Influences Blood Sugar Levels? NUTRITION 4 Meal
Blood Glucose Management What Influences Blood Sugar Levels? There are three main things that influence your blood sugar: Nutrition Exercise Medication What Influences Blood Sugar Levels? NUTRITION 4 Meal
You and Your Child s Rights. What is a 504 Plan? Who Qualifies for a 504? 3/11/2014. Speak Softly and Carry a Big Stick!
 Practical Tips for Helping Your Child with Diabetes Succeed in School By Kathy Spain RN, BSN, CDE, CPT You and Your Child s Rights Your child has the right to a free, appropriate public education without
Practical Tips for Helping Your Child with Diabetes Succeed in School By Kathy Spain RN, BSN, CDE, CPT You and Your Child s Rights Your child has the right to a free, appropriate public education without
Form 9: School Health Care Plan for Insulin Pump Page 1 of 10
 Form 9: School Health Care Plan for Insulin Pump Page 1 of 10 of Birth CHI Photograph of pupil Address School Once completed, the parent/carer is responsible for taking a copy of this School Health Care
Form 9: School Health Care Plan for Insulin Pump Page 1 of 10 of Birth CHI Photograph of pupil Address School Once completed, the parent/carer is responsible for taking a copy of this School Health Care
School Nurse Diabetes Resource Guide
 School Nurse Diabetes Resource Guide Table of Contents Introduction.....1 Insulin Pump Basics....2 Safe at School...4 Diabetes Care Plan: Blood glucose monitoring and management...6 Insulin and glucagon
School Nurse Diabetes Resource Guide Table of Contents Introduction.....1 Insulin Pump Basics....2 Safe at School...4 Diabetes Care Plan: Blood glucose monitoring and management...6 Insulin and glucagon
Steroid Induced Diabetes
 What is high blood sugar (hyperglycemia)? Hyperglycemia is a high level of sugar in the blood. Blood sugar is also called glucose. Some people are unable to process the sugar that is found in food and
What is high blood sugar (hyperglycemia)? Hyperglycemia is a high level of sugar in the blood. Blood sugar is also called glucose. Some people are unable to process the sugar that is found in food and
SCHOOL DISTRICT #43 (COQUITLAM) MEDICAL ALERT FORMS FORM(S) MUST BE COMPLETED AT THE START OF EACH SCHOOL YEAR
 SCHOOL DISTRICT #43 (COQUITLAM) MEDICAL ALERT FORMS FORM(S) MUST BE COMPLETED AT THE START OF EACH SCHOOL YEAR Please read instructions below carefully. Feel free to contact your school if you need any
SCHOOL DISTRICT #43 (COQUITLAM) MEDICAL ALERT FORMS FORM(S) MUST BE COMPLETED AT THE START OF EACH SCHOOL YEAR Please read instructions below carefully. Feel free to contact your school if you need any
High Blood Sugar, Low Blood Sugar. Let s Check our Blood Sugar
 High Blood Sugar, Low Blood Sugar Testing your blood sugar Check with your provider to see if and when he/she wants you to check your blood sugar. Keep a record of your blood sugar numbers, the date and
High Blood Sugar, Low Blood Sugar Testing your blood sugar Check with your provider to see if and when he/she wants you to check your blood sugar. Keep a record of your blood sugar numbers, the date and
Type 1 Diabetes. Pennington Nutrition Series. Overview. About Insulin
 Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 32 Type 1 Diabetes Overview Type 1 Diabetes (DM) is usually diagnosed in children and young adults.
Pennington Nutrition Series Healthier lives through education in nutrition and preventive medicine Pub No. 32 Type 1 Diabetes Overview Type 1 Diabetes (DM) is usually diagnosed in children and young adults.
Myths About Type 2 Diabetes and Insulin
 About Diabetes This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding your health. Please consult
About Diabetes This health information is being provided for general educational purposes only. Your health care provider is the single best source of information regarding your health. Please consult
Diabetes Mellitus: Type 1
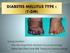 Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
Diabetes Mellitus: Type 1 What is type 1 diabetes mellitus? Type 1 diabetes is a disorder that happens when your body produces little or no insulin. The lack of insulin causes the level of sugar in your
DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY
 DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY First Edition September 17, 1997 Kevin King R.N., B.S., C.C.R.N. Gregg Kunder R.N., B.S.N., C.C.T.C. 77-120 CHS UCLA Medical Center
DIABETIC EDUCATION MODULE ONE GENERAL OVERVIEW OF TREATMENT AND SAFETY First Edition September 17, 1997 Kevin King R.N., B.S., C.C.R.N. Gregg Kunder R.N., B.S.N., C.C.T.C. 77-120 CHS UCLA Medical Center
A Guide for Families: Diabetes Care for Children and Teens with Type 1 Diabetes
 A Guide for Families: Diabetes Care for Children and Teens with Type 1 Diabetes A Guide for Families: Diabetes Care for Children and Teens with Type 1 Diabetes Overwaitea Food Group banners including
A Guide for Families: Diabetes Care for Children and Teens with Type 1 Diabetes A Guide for Families: Diabetes Care for Children and Teens with Type 1 Diabetes Overwaitea Food Group banners including
School Nurse Role in Care and Management of the Child with Diabetes in Colorado Schools and Child Care Settings Position Statement 1 POSITION It is
 Schools and Child Care Settings Position Statement 1 POSITION It is the position of the Colorado Diabetes Resource Nurses that the school nurse is the only school staff member who has the skills, knowledge
Schools and Child Care Settings Position Statement 1 POSITION It is the position of the Colorado Diabetes Resource Nurses that the school nurse is the only school staff member who has the skills, knowledge
MAKING CARBS COUNT Why totting up totals can help your control
 ISSUE 17 MAGAZINE MAKING CARBS COUNT Why totting up totals can help your control WINTER FEET Seasonal care to avoid sore paws PLUS New Products roovy giveaways News (for T1 and T2) ELEANA PAPADOPOULOU,
ISSUE 17 MAGAZINE MAKING CARBS COUNT Why totting up totals can help your control WINTER FEET Seasonal care to avoid sore paws PLUS New Products roovy giveaways News (for T1 and T2) ELEANA PAPADOPOULOU,
Management of Diabetes
 Management of Diabetes Blood Glucose Monitoring MANAGEMENT OF DIABETES Once someone is told they have diabetes, they are usually asked to check their blood glucose at home with a home blood glucose meter
Management of Diabetes Blood Glucose Monitoring MANAGEMENT OF DIABETES Once someone is told they have diabetes, they are usually asked to check their blood glucose at home with a home blood glucose meter
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993
 N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
N E B R A S K A JAIL BULLETIN NUMBER 102 OCTOBER 1993 The Jail Bulletin is a monthly feature of the Crime Commission Update. The Bulletin may be used as a supplement to your jail in-service training program
Section 5: Type 2 Diabetes
 SECTION OVERVIEW Definition and Symptoms Blood Glucose Monitoring Healthy Eating Physical Activity Oral Medication Insulin Sharps Disposal Definition and Symptoms Type 2 diabetes is occurring more frequently
SECTION OVERVIEW Definition and Symptoms Blood Glucose Monitoring Healthy Eating Physical Activity Oral Medication Insulin Sharps Disposal Definition and Symptoms Type 2 diabetes is occurring more frequently
THE INS AND OUTS OF INSULIN. Mary Beth Wald, RN,BSN,CDE
 THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
The Basics of Insulin Pump Therapy
 The Basics of Insulin Pump Therapy Table of Contents The Basics of Insulin Pump Therapy Introduction Welcome... 3 Chapter 1 Balancing Glucose and Insulin............................. 10 Section 1: Glucose,
The Basics of Insulin Pump Therapy Table of Contents The Basics of Insulin Pump Therapy Introduction Welcome... 3 Chapter 1 Balancing Glucose and Insulin............................. 10 Section 1: Glucose,
Administrative Procedures Memorandum
 Administrative Procedures Memorandum DATE OF ISSUE: September 2004 Revised: January 2014, September 2015 MEMO TO: FROM: Principals, Vice-Principals, Supervisory Officers Director of Education PURPOSE The
Administrative Procedures Memorandum DATE OF ISSUE: September 2004 Revised: January 2014, September 2015 MEMO TO: FROM: Principals, Vice-Principals, Supervisory Officers Director of Education PURPOSE The
Managing Type 1 Diabetes with Multiple Daily Injections (MDI)
 with Multiple Daily Injections (MDI) Diabetes Care and Research Program Important telephone numbers Diabetes Clinic: Diabetes Specialist: Nurse Practitioner/Nurse: Registered Dietitian: Pharmacist: Family
with Multiple Daily Injections (MDI) Diabetes Care and Research Program Important telephone numbers Diabetes Clinic: Diabetes Specialist: Nurse Practitioner/Nurse: Registered Dietitian: Pharmacist: Family
Do children with diabetes need a special diet?
 Do children with diabetes need a special diet? No! The basic nutritional needs of a child or adolescent with diabetes is the same as their peers Healthy eating is important for all children Children with
Do children with diabetes need a special diet? No! The basic nutritional needs of a child or adolescent with diabetes is the same as their peers Healthy eating is important for all children Children with
Low Blood Sugar. What is low blood sugar? What else is low blood sugar called? Why does low blood sugar occur?
 Low Blood Sugar What is low blood sugar? Low blood sugar means there is not enough glucose (sugar) in the body. Glucose is the major fuel needed to feed the body's cells. A normal glucose level will vary
Low Blood Sugar What is low blood sugar? Low blood sugar means there is not enough glucose (sugar) in the body. Glucose is the major fuel needed to feed the body's cells. A normal glucose level will vary
Chapter 23 The School/ Work and Diabetes
 Chapter 23 The School/ Work and Diabetes Susie Owen, RN, CDE H. Peter Chase, MD INTRODUCTION The first and main job of parents in relation to school is to educate those who will be working with the child
Chapter 23 The School/ Work and Diabetes Susie Owen, RN, CDE H. Peter Chase, MD INTRODUCTION The first and main job of parents in relation to school is to educate those who will be working with the child
Pediatric Diabetic Teaching Guidelines/Checklist
 Pediatric Diabetic Teaching Guidelines/Checklist This teaching guideline contains the essential elements for teaching pediatric inpatients with diabetes. All teaching and patient/family responses should
Pediatric Diabetic Teaching Guidelines/Checklist This teaching guideline contains the essential elements for teaching pediatric inpatients with diabetes. All teaching and patient/family responses should
Department of Health Commencing insulin therapy
 Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration
 of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org
 written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
Diabetes and exercise
 Diabetes and exercise Summary Symptoms of hypoglycaemia are caused by low blood sugar. Hypoglycaemia can occur if you take your diabetes medication and then do not eat enough or exercise more than usual.
Diabetes and exercise Summary Symptoms of hypoglycaemia are caused by low blood sugar. Hypoglycaemia can occur if you take your diabetes medication and then do not eat enough or exercise more than usual.
Guidelines for Training School Employees who are not Licensed Healthcare Professionals
 Guidelines for Training School Employees who are not Licensed Healthcare Professionals to implement House Bill 984 (79 th Legislature) related to the Care of Elementary and Secondary School Students with
Guidelines for Training School Employees who are not Licensed Healthcare Professionals to implement House Bill 984 (79 th Legislature) related to the Care of Elementary and Secondary School Students with
Causes, incidence, and risk factors
 Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Causes, incidence, and risk factors Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both. To understand diabetes,
Glucagon Emergency Adminis. ningng Tool A Resource for School Nurses and School Personnel
 Glucagon Emergency Adminis nistration Traini ningng Tool A Resource for School Nurses and School Personnel Please note: Speakers notes are intended to be read by the school nurse to the volunteers in training.
Glucagon Emergency Adminis nistration Traini ningng Tool A Resource for School Nurses and School Personnel Please note: Speakers notes are intended to be read by the school nurse to the volunteers in training.
how to control blood glucose during PREGNANCY?
 how to control blood glucose during PREGNANCY? one HOW THE BODY WORKS DURING PREGNANCY During all pregnancies, the placenta makes a called human placental lactogen which allows the baby to grow and develop.
how to control blood glucose during PREGNANCY? one HOW THE BODY WORKS DURING PREGNANCY During all pregnancies, the placenta makes a called human placental lactogen which allows the baby to grow and develop.
Training for Volunteer Health Aides Care of Students With Diabetes
 Training for Volunteer Health Aides Care of Students With Diabetes You are a KEY player in contributing to the student s Academic Performance & keeping the student Safe at School Attention: Volunteer Health
Training for Volunteer Health Aides Care of Students With Diabetes You are a KEY player in contributing to the student s Academic Performance & keeping the student Safe at School Attention: Volunteer Health
Starting insulin treatment for people with type 2 diabetes. What you need to know
 Starting insulin treatment for people with type 2 diabetes What you need to know Contents Information 3 Any questions? 3 Glossary of terms 3 Why do I need insulin? 4 What does insulin do? 5 Why are there
Starting insulin treatment for people with type 2 diabetes What you need to know Contents Information 3 Any questions? 3 Glossary of terms 3 Why do I need insulin? 4 What does insulin do? 5 Why are there
Starting insulin for people with type 2 diabetes
 Starting insulin for people with type 2 diabetes What you need to know Contents Page Why do I need insulin? 3 What does insulin do? 4 Why are there different types of insulin? 4 How do I take insulin?
Starting insulin for people with type 2 diabetes What you need to know Contents Page Why do I need insulin? 3 What does insulin do? 4 Why are there different types of insulin? 4 How do I take insulin?
ACH DIABETES TEAM CONTACT INFORMATION
 DIABETES 101 PHYSICIANS: DR. JON ODEN SECTION CHIEF DR. PAUL FRINDIK DR. Y. ANNIE WANG DR. ABHA CHOUDHARY ADVANCED PRACTICE NURSES: HEATHER CANTRELL, APRN, MNSC, CPNP AC, CDE LINDLEY ABRAMS, APRN, MNSC,
DIABETES 101 PHYSICIANS: DR. JON ODEN SECTION CHIEF DR. PAUL FRINDIK DR. Y. ANNIE WANG DR. ABHA CHOUDHARY ADVANCED PRACTICE NURSES: HEATHER CANTRELL, APRN, MNSC, CPNP AC, CDE LINDLEY ABRAMS, APRN, MNSC,
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Diabetes Management in School. Signs and Symptoms of Hypo and Hyper glycemia Blood Glucose Testing Glucagon Injections
 ONLINE TRAINING FOR Diabetes Management in School This training will cover the following Diabetic Care Tasks: Signs and Symptoms of Hypo and Hyper glycemia Blood Glucose Testing Glucagon Injections Ketone
ONLINE TRAINING FOR Diabetes Management in School This training will cover the following Diabetic Care Tasks: Signs and Symptoms of Hypo and Hyper glycemia Blood Glucose Testing Glucagon Injections Ketone
VA/DoD Clinical Practice Guideline for Management of Diabetes TOOLKIT
 VA/DoD Clinical Practice Guideline for Management of Diabetes TOOLKIT VA/DoD Clinical Practice Guideline for Management of Diabetes TOOLKIT For the Provider/Educator Teaching Tips Consider patient readiness
VA/DoD Clinical Practice Guideline for Management of Diabetes TOOLKIT VA/DoD Clinical Practice Guideline for Management of Diabetes TOOLKIT For the Provider/Educator Teaching Tips Consider patient readiness
Glucagon Education for School Nurses in Tennessee. by Mary Kornguth PhD, RN, NCSN
 Glucagon Education for School Nurses in Tennessee by Mary Kornguth PhD, RN, NCSN Objectives: At the end of this module the school nurse will be able to: 1. State what glucagon is and describe its action
Glucagon Education for School Nurses in Tennessee by Mary Kornguth PhD, RN, NCSN Objectives: At the end of this module the school nurse will be able to: 1. State what glucagon is and describe its action
HOW TO RECOGNIZE IT AND WHAT DO TO
 Low blood glucose HOW TO RECOGNIZE IT AND WHAT DO TO L ipoglicemia Lilly What is low blood glucose? Low blood glucose, or hypoglycemia, occurs when the level of sugar in the blood is 70mg/dl or less. Low
Low blood glucose HOW TO RECOGNIZE IT AND WHAT DO TO L ipoglicemia Lilly What is low blood glucose? Low blood glucose, or hypoglycemia, occurs when the level of sugar in the blood is 70mg/dl or less. Low
