Type1DiabetesThroughtheLife Span: A Position Statement of the American Diabetes Association
|
|
|
- Cora Farmer
- 10 years ago
- Views:
Transcription
1 2034 Diabetes Care Type1DiabetesThroughtheLife Span: A Position Statement of the Amerian Diabetes Assoiation Jane L. Chiang, 1 M. Sue Kirkman, 2 Lori M.B. Laffel, 3 and Anne L. Peters, 4 on behalf of the Type 1 Diabetes Sourebook Authors* DOI: /d POSITION STATEMENT Type 1 diabetes is haraterized by an immune-mediated depletion of b-ells that results in lifelong dependene on exogenous insulin. While both type 1 and type 2 diabetes result in hyperglyemia, the pathophysiology and etiology of the diseases are distint and require us to onsider eah type of diabetes independently. As suh, this position statement summarizes available data speifi to the omprehensive are of individuals with type 1 diabetes. The goal is to enhane our ability to reognize and manage type 1 diabetes, to prevent its assoiated ompliations, and to eventually ure and prevent this disease. INCIDENCE AND PREVALENCE OF TYPE 1 DIABETES The exat number of individuals with type 1 diabetes around the world is not known, but in the U.S., there are estimated to be up to 3 million (1). Although it has long been alled juvenile diabetes due to the more frequent and relatively straightforward diagnosis in hildren, the majority of individuals with type 1 diabetes are adults. Most hildren are referred and treated in tertiary enters, where linial data are more readily aptured. The SEARCH for Diabetes in Youth study estimated that, in 2009, 18,436 U.S. youth were newly diagnosed with type 1 diabetes (12,945 non- Hispani white, 3,098 Hispani, 2,070 non-hispani blak, 276 Asian-Paifi Islander, and 47 Amerian Indian) (2). Worldwide, ;78,000 youth are diagnosed with type 1 diabetes annually. Inidene varies tremendously among ountries: East Asians and Amerian Indians have the lowest inidene rates (0.1 8 per 100,000/year) as ompared with the Finnish who have the highest rates (.64.2 per 100,000/year) (3). In the U.S., the number of youth with type 1 diabetes was estimated to be 166,984 (4). The preise inidene of new-onset type 1 diabetes in those over 20 years of age is unknown. This may be due to the prolonged phase of onset and the subtleties in distinguishing the different types of diabetes. In one European study of adults aged years, ;9% tested positive for GAD antibodies (GADA) within 5 years of a diabetes diagnosis, onsistent with other studies (5). Adults with type 1 diabetes often reeive are in primary are settings rather than with an endorinologist. Unlike the onsolidated are seen in pediatri diabetes management, the lak of onsolidated are in adults makes inidene and prevalene rates diffiult to haraterize, and therefore they are often underestimated. The number of adults living with type 1 diabetes is inreasing due to two fators: 1) the rising number of new-onset ases of type 1 diabetes in adults, inluding those diagnosed with latent autoimmune diabetes in adults (LADA), and 2) individuals with hildhood-onset diabetes are living longer (6,7). CLASSIFICATION AND DIAGNOSIS Type 1 diabetes has traditionally been diagnosed based on linial ataboli symptoms suggestive of insulin defiieny: polyuria, polydipsia, weight loss, and marked hyperglyemiathat is nonresponsive to oral agents. It is lassified as an autoimmune disease with progressive b-ell destrution, resultinginaphysiologialdependene on exogenous insulin. Reent studies have broadened our understanding of the disease, but have made diagnosis more omplex. There is tremendous variability in the initial presentation of type 1 diabetes in both youth and adults. Children often present autely, with severe symptoms of polyuria, Diabetes Care Publish Ahead of Print, published online June 16, Amerian Diabetes Assoiation, Alexandria, VA 2 Department of Mediine, University of North Carolina at Chapel Hill, Chapel Hill, NC 3 Pediatri, Adolesent and Young Adult Setion, Joslin Diabetes Center; Department of Pediatris, Harvard Medial Shool, Boston, MA 4 Division of Endorinology, Kek Shool of Mediine of the University of Southern California, Los Angeles, CA Corresponding author: Jane L. Chiang, jhiang@ diabetes.org. The position statement was reviewed and approved by the Professional Pratie Committee in April 2014 and approved by the Exeutive Committee of the Board of Diretors in April *A list of authors of the Amerian Diabetes Assoiation/JDRF Type 1 Diabetes Sourebook an be found in the ACKNOWLEDGMENTS by the Amerian Diabetes Assoiation. See for details.
2 are.diabetesjournals.org Chiang and Assoiates 2035 Figure 1 The perentage of antibody-positive subjets is affeted by the duration of type 1 diabetes for GADA (A)and IA2A(B).Given an inrease in the satter (due to lower numbers of subjets), the x-axis is trunated at a duration of 30 years. Reprodued with permission from Tridgell et al. (16). polydipsia, and ketonemia. However, in adults, type 1 diabetes presents with a more gradual onset, with a linial presentation that may initially appear onsistent with type 2 diabetes. Distinguishing betweentype1andtype2diabetes presents diagnosti hallenges. Traditionally, progressive b-ell destrution has been the hallmark of type 1 diabetes, but residual C-peptide (a surrogate marker for insulin seretion) may be deteted over 40 years after initial diagnosis, regardless of whether the initial diagnosis was made in hildhood or in adulthood (8). Clinial Clues Muh of the diagnosis will depend on linial lues, but the rising inidene of overweight/obesity has also onfounded the diagnosis of type 1 diabetes. A lean individual presenting with linial symptoms without a first-degree relative with diabetes (but often with a history of distant relatives with type 1 diabetes or other autoimmune disease) is generally suggestive of type 1 diabetes. An overweight individual (of any age) with metaboli syndrome and a strong family history of type 2 diabetes may be assessed only for the development of type 2 diabetes, even though type 1 diabetes is on the differential diagnosis. Obesity does not prelude that autoimmunity and hyperglyemia will our even amid the relatively higher levels of endogenous insulin seretion observed in obesity. In young patients aged years with phenotypi type 2 diabetes, 10% have evidene of islet autoimmunity suggesting that type 1 diabetes was the likely diagnosis (9). Thus, although leaner individuals are more likely to be diagnosed as having type 1 diabetes, the potential for type 1 diabetes exists in those who phenotypially appear to have type 2 diabetes. If hyperglyemia persists after treatment with noninsulin agents, whih is unusual in the treatment of newly diagnosed type 2 diabetes, then type 1 diabetes should be onsidered. Panreati Autoantibodies Panreati autoantibodies are harateristi of type 1 diabetes. Highly sensitive laboratory measurements apture ;98% of individuals with autoantibodies at diagnosis (10). Unfortunately, most ommerial laboratories do not have reliably sensitive or speifi assays that measure all five autoantibodies: GADA, islet ell antibodies (ICA), insulin autoantibodies (IAA), protein tyrosine phosphatase antibodies (ICA512 or IA2A), and zin transporter protein (ZnT8). Thus, it may be inappropriate to report a patient as autoantibody negative. Another ause of false-negative autoantibodies is testing far out from diagnosis as antibody titers diminish over time (Fig. 1). It appears that there is an inreased inidene of type 1 diabetes in ethni populations where autoantibody markers may be of variable utility, suh as in Asians where autoantibodies are often negative (11 15). Family History Type 1 diabetes has a geneti prediletion and, in some ases, an be predited in family members. The overall prevalene of type 1 diabetes in the U.S. is ;0.3%, but if a first-degree relative has diabetes, the empiri risk of being affeted is ;5% (17,18), representing a 15-fold inrease among family members. Studies evaluating hildren at risk for developing type 1 diabetes have shown that the presene of more than two autoantibodies was assoiated with a nearly 70% risk for disease development within 10 years and 84% within 15 years (19). Evaluating at-risk individuals in the linial setting is not yet reommended due to limited linial interventions; however, ongoing researh studies are identifying at-risk individuals through geneti testing in both the lowerrisk general population and in the higherrisk population of relatives of people with type 1 diabetes. Diagnosis The Amerian Diabetes Assoiation s (ADA s) diagnosti riteria for type 1 and type 2 diabetes are the same (Table 1). (A) Consider measurement of panreati autoantibodies to onfirm the diagnosis of type 1 diabetes. (B) Identifiation of At-Risk Relatives Inform type 1 diabeti patients of the opportunity to have their relatives tested for type 1 diabetes risk in the setting of a linial researh study. (B) INITIAL EVALUATION AND FOLLOW-UP General Considerations All patients with type 1 diabetes need age-appropriate are, with an understanding of their speifi needs and limitations. Infants and toddlers are approahed quite differently from
3 2036 Position Statement Diabetes Care Table 1 Criteria for the diagnosis of diabetes A1C $6.5%. The test should be performed in a laboratory using a method that is NGSP ertified and standardized to the DCCT assay.* OR FPG $126 mg/dl (7.0 mmol/l). Fasting is defined as no alori intake for at least 8 h.* OR Two-hour plasma gluose $200 mg/dl (11.1 mmol/l) during an oral gluose tolerane test. The test should be performed as desribed by the World Health Organization, using a gluose load ontaining the equivalent of 75 g anhydrous gluose dissolved in water.* OR In a patient with lassi symptoms of hyperglyemia or hyperglyemi risis, a random plasma gluose $200 mg/dl (11.1 mmol/l). *In the absene of unequivoal hyperglyemia, result should be onfirmed by repeat testing. adolesents; the needs of young adults may vary from middle-aged or older adults. Regardless of age, the patient s needs are the same: an individualized are plan with ongoing eduation and support, ongoing assessment for aute and hroni ompliations, and aess to medial providers with type 1 diabetes expertise. Just as patients hange, the therapeuti approah should hange and should be evaluated at eah visit and modified as needed. Type 1 diabetes are must be an iterative proess, adapted as the needs of the individual evolve. Clinial assessments for type 1 diabetes in hildren and adults should inorporate age-appropriate and ompliation-foused evaluations, based on the likelihood that an abnormality will be present. For example, a young adult with low ardiovasular disease (CVD) risk and no ompliations may need more of an assessment of lifestyle adjustment as opposed to an older adult with longer duration of the disease who may need more evaluation of vasular and neurologial issues. Transition of Care From Pediatri to Adult Providers As youth transition into emerging adulthood, the supportive infrastruture often abruptly disappears and glyemi ontrol tends to deteriorate. The ADA reognizes that this is a hallenging time and reommends a strong, pratial transition plan to antiipate the upoming hanges. A suessful transition plan should be initiated early (e.g., early teenage years) and inlude ongoing dialogue between the family and youth. The disussion should inlude finanes, insurane, obtainment of supplies, identifiation of an adult are provider (ideally with ommuniation between the two providers), psyhosoial issues (e.g., depression), and other issues identified by the family/youth. Health are providers, family, and youth should agree to an ahievable diabetes management plan and provide resoures for unantiipated issues. We refer the reader to the ADA s position statement on diabetes are for emerging adults (20). Table 2 provides the hildhood developmental phases and needs. Tables 3, 4, and 5 provide detailed elements of the initial and follow-up evaluation in individuals with type 1 diabetes. Assessing the history of aute ompliations (e.g., severe hypoglyemia/ hyperglyemia and diabeti ketoaidosis [DKA]) is important. Providers should provide ontinuing eduation for the patient/family to prevent ongoing reurrene. For example, it is important to review exerise management to redue hypoglyemia risk and disuss sikday management to redue DKA risk. Risk fator (e.g., ardiovasular) evaluation for prevention and sreening for early evidene of miro- and marovasular ompliations for early intervention should be implemented starting in adolesene and ontinue through adulthood. For hildren, risk fators should be assessed shortly after diagnosis based on family history and initial sreening laboratory test results. Providers should manage risk fators, onsidering age-speifi goals and targets (e.g., blood pressure, lipid, depression, and BMI assessment and management). The frequeny of ongoing sreening for ompliations should be based on age and disease duration. Coexistent Autoimmunity Celia Disease Celia disease is an immune-mediated disorder that ours with inreased frequeny in patients with type 1 diabetes (1 16% of individuals ompared with 0.3 1% in the general population) (21,22). Symptoms of elia disease inlude diarrhea, weight loss or poor weight gain, abdominal pain, bloating, hroni fatigue, malnutrition due to malabsorption, and unexplained hypoglyemia or errati blood gluose levels. Sreening for elia disease with serum levels of tissue transglutaminase or antiendomysial antibodies should be onsidered soon after the diagnosis of diabetes and/or if symptoms develop. Individuals who test positive should be referred to a gastroenterologist for possible small-bowel biopsy to onfirm the diagnosis, although this is not neessary in all ases. Symptomati hildren with strongly positive antibodies and supportive geneti or HLA testing may not require a biopsy, but asymptomati at-risk hildren should have a biopsy (23). In symptomati individuals with type 1 diabetes and onfirmed elia disease, a gluten-free diet redues symptoms and dereases rates of hypoglyemia (24). Thyroid Disease About one-quarter of hildren with type 1 diabetes have thyroid autoantibodies (thyroid peroxidase antibodies or antithyroglobulin antibodies) at the time of diagnosis (25,26). The presene of thyroid autoantibodies is preditive of thyroid dysfuntion, generally hypothyroidism and less ommonly hyperthyroidism (27). Thyroid dysfuntion is more ommon in adults with type 1 diabetes, although the exat prevalene is unknown. Women are more ommonly affeted than men. Sublinial hypothyroidism, hyperthyroidism, or oexistent Addison disease (adrenal insuffiieny) may also deteriorate metaboli ontrol with inreased risk of symptomati hypoglyemia (28) and may redue linear growth in hildren (29). Additional Considerations for Pediatris All hildren require some level of adult supervision in managing their diabetes. Assessments of pediatri patients should address issues speifi to infants/ preshoolers, shool-aged hildren, adolesents, and emerging adults (Table 2). Health are providers should do a thorough assessment of the developmental needs of the youth (and aregiver), fousing on physial and emotional development, family issues, and psyhosoial needs. The diabetes treatment plan
4 are.diabetesjournals.org Chiang and Assoiates 2037 Table 2 Major developmental issues and their effet on diabetes in hildren and adolesents Type 1 diabetes Developmental stages (ages) Normal developmental tasks management priorities Infany (0 12 months) Toddler (13 26 months) Preshooler and early elementary shool (3 7 years) Older elementary shool (8 11 years) Early adolesene (12 15 years) Later adolesene (16 19 years) Developing a trusting relationship or bond with primary aregiver(s) Developing a sense of mastery and autonomy Developing initiative in ativities and onfidene in self Developing skills in athleti, ognitive, artisti, and soial areas Consolidating self-esteem with respet to the peer group Managing body hanges Developing a strong sense of self-identity Establishing a sense of identity after high shool (deisions about loation, soial issues, work, and eduation) Preventing and treating hypoglyemia Avoiding extreme flutuations in blood gluose levels Preventing hypoglyemia Avoiding extreme flutuations in blood gluose levels due to irregular food intake Preventing hypoglyemia Coping with unpreditable appetite and ativity Positively reinforing ooperation with regimen Trusting other aregivers with diabetes management Making diabetes regimen flexible to allow for partiipation in shool or peer ativities Child learning short- and long-term benefits of optimal ontrol Inreasing insulin requirements during puberty Diabetes management and blood gluose ontrol beoming more diffiult Weight and body image onerns Starting an ongoing disussion of transition to a new diabetes team (disussion may begin in earlier adolesent years) Integrating diabetes into new lifestyle Family issues in type 1 diabetes management Coping with stress Sharing the burden of are to avoid parent burnout Establishing a shedule Managing the piky eater Limit-setting and oping with toddler s lak of ooperation with regimen Sharing the burden of are Reassuring hild that diabetes is no one s fault Eduating other aregivers about diabetes management Maintaining parental involvement in insulin and blood gluose management tasks while allowing for independent selfare for speial oasions Continuing to eduate shool and other aregivers Renegotiating parent and teenager s roles in diabetes management to be aeptable to both Learning oping skills to enhane ability to self-manage Preventing and intervening in diabetes-related family onflit Monitoring for signs of depression, eating disorders, and risky behaviors Supporting the transition to independene Learning oping skills to enhane ability to self-manage Preventing and intervening with diabetes-related family onflit Monitoring for signs of depression, eating disorders, and risky behaviors should be individualized and tailored to the needs of individual patients and their families. Efforts to ahieve targetbloodgluoseanda1clevels should be balaned with preservation of quality of life and protet against exessive hypoglyemia. Heightandweightshouldbemeasured at eah visit and traked via appropriate height and weight growth harts. An ageadjusted BMI an be alulated starting at age 2 years. These tools an be found for hildren and teens at Blood pressure measurements should be determined orretly, using the appropriate size uff and with the hild seated and relaxed. Hypertension should be onfirmed on at least 3 separate days. Normal blood pressure levels for age, sex, and height and appropriate methods for determinations are available online at health/prof/heart/hbp/hbp_ped.pdf. Chroni Compliations in Children Retinopathy, nephropathy, and neuropathy rarely have been reported in prepubertal hildren and hildren with diabetes duration of only 1 2 years; however, they may our after the onset of puberty or after 5 10 years of diabetes (30). As sreening reommendations are based on reent evidene, these periodially hange. Therefore, we refer the reader to the ADA Standards of Care for the urrent sreening reommendations for hildren. It is reommended that those with expertise in diabetes management should ondut the assessments. For example, ophthalmologi exams should be performed by those skilled in diabeti retinopathy management and experiened in ounseling pediatri patients and parents on the importane of early prevention/intervention. Another example,
5 2038 Position Statement Diabetes Care Table 3 Medial history Age and harateristis of onset of diabetes (e.g., DKA, asymptomati laboratory finding) Eating patterns, physial ativity habits, nutritional status, and weight history Whether or not patient wears medial alert identifiation Diabetes eduation history; health literay assessment Review of previous insulin treatment regimens and response to therapy (A1C reords), treatment preferenes, and prior diffiulty with therapies Current treatment of diabetes, inluding mediations and mediation adherene, meal plan, physial ativity patterns, and readiness for behavior hange Use of insulin, insulin pumps, arbohydrate ratios, and orretions; knowledge of sik-day rules; ketone testing; pump troubleshooting (if appliable) Results of gluose monitoring, inluding SMBG and CGM and patient s use of data DKA frequeny, severity, and ause Hypoglyemi episodes Hypoglyemia unawareness Any severe hypoglyemia: frequeny and ause Whether or not patient has gluagon available and someone to administer it History of diabetes-related ompliations Mirovasular: retinopathy, nephropathy, and neuropathy (sensory, inluding history of foot lesions; autonomi, inluding sexual dysfuntion and gastroparesis) Marovasular: oronary heart disease, erebrovasular disease, and peripheral artery disease Other: dental disease Psyhosoial issues, inluding urrent or past history of depression, anxiety, eating disorders, and others; assess support systems and need for assistane History of pregnany and any diabetes-related ompliations; desire for future pregnanies Contraeption (if a woman is of hildbearing age) Smoking Alohol use, abuse, and impat on blood gluose levels Illiit drug use Driving nephrologists with experiene with diabeti nephropathy would be aware that intermittent elevations in urinary albumin exretion are ommon in pediatri patients, partiularly in assoiation with exerise. Additional Considerations for Adults Adults with type 1 diabetes now span a very large age spetrumdfrom 18 to 100 years of age and beyond. Unlike the well-haraterized developmental stages of hildren, the life stages traversed through adulthood are often less well doumented and underappreiated. However, an understanding of eah individual s irumstanes is vital. This is true for aging in general, but partiularly true for those with signifiant omorbidities due to long-standing type 1 diabetes. Thus, it is important to assess the linial needs of the patient, setting speifi goals and expetations that may differ signifiantly between a healthy 26-year-old and a frail 84-yearold with CVD and retinopathy. See 2014 ADA Standards of Medial Care for detailed sreening information for CVD, nephropathy, retinopathy, neuropathy, and foot are. Aess to health are should inlude liniians with expertise in type 1 diabetes management, inluding (but not limited to) an endorinologist (or other health are provider with expertise in type 1 diabetes management), a registered dietitian, a diabetes eduator, a mental health professional, an exerise speialist/ physiologist, and speialists required to treat diabetes ompliations. (E) Routine follow-up (generally quarterly) should inlude review of self-monitoring of blood gluose (SMBG), ontinuous gluose monitoring (CGM) and pump data (if appliable), A1C measurement, evidene for aute and/or hroni ompliations of diabetes (partiularly episodes of DKA and mild and/or severe hypoglyemia), measurement of blood pressure and weight (and height in hildren), foot exam, inspetion of injetion/ insertion sites, and disussion of psyhosoial and eduational needs (Tables 4 and 5). (E) Providers should routinely doument the patient s age and disease duration. When linially indiated, laboratory measures suh as lipids, renal funtion measurements, and antibodies for assoiated autoimmune disease (thyroid or elia disease) should be doumented. (E) Parent/guardian involvement in are is required throughout hildhood, with a gradual shift in responsibility of are from the parent/guardian to the youth. (E) Health are for adults should be foused on the needs of the individual throughout the various stages of their life, with age-appropriate evaluation and treatment. (E) Evaluation and treatment of CVD risk should be individualized. (E) Immunizations should be given as reommended by the Centers for Disease Control and Prevention (CDC) for hildren/adults in general and people with diabetes speifially. (C) Consider sreening for elia disease by measuring IgA antitissue transglutaminase or antiendomysial antibodies, with doumentation of normal total serum IgA levels, soon after the diagnosis of diabetes and/or if symptoms develop. Refer the patient to a gastroenterologist if the test is positive. (E) Consider sreening for thyroid peroxidase and thyroglobulin antibodies soon after diagnosis. (E) Sreen for thyroid dysfuntion by measuring thyroid-stimulating hormone (TSH) onentrations soon after type 1 diabetes diagnosis (and after stable metaboli ontrol). If normal, onsider reheking every 1 2 years or more frequently if the patient develops unusual glyemi variation or symptoms of thyroid dysfuntion or thyromegaly. (E) Assess for the presene of additional autoimmune onditions at diagnosis and if symptoms develop. (E) Ongoing nutrition and diabetes selfmanagement eduation (DSME) and support (DSMS) areneededtoaddress hanges in food preferenes, aess to food, daily shedules, ativity patterns, and potential barriers to
6 are.diabetesjournals.org Chiang and Assoiates 2039 Table 4 Children and adolesents* Clinial evaluation Initial Annual Quarterly follow-up Height Weight BMI perentile Blood pressure General physial exam Thyroid exam Injetion/infusion sites (if already on insulin) Comprehensive foot exam If needed, based on age Beginning with older teens with diabetes sine hildhood Visual foot exam If needed, based on high-risk harateristis Retinal exam by eye are speialist In some ases, may be done every 2 years (see ADA Standards of Care) Depression sreen Hypoglyemia assessment Diabetes self-management skills Physial ativity assessment Assess linially relevant issues As needed for teens As needed for teens (e.g., alohol, drug, and tobao use; use of ontraeption; driving) Nutritional knowledge As needed Query for evidene of other As needed As needed autoimmune disease Immunizations as reommended by CDC As needed Laboratory assessments Initial Annual Follow-up A1C Every 3 months Creatinine learane/estimated glomerular filtration rate Lipid panel One glyemia is stable As needed based on treatment TSH As needed based on Frequeny of testing varies based on linial symptoms, presene of antibodies, and/or if on treatment treatment Antithyroid antibodies Repeat as linially indiated (antithyroid peroxidase and antithyroglobulin antibodies) Frequeny of testing is unknown; test if symptoms are present or for periodi sreening Celia antibody panel Repeat as linially indiated Frequeny of testing is unknown; test if symptoms are present or for periodi sreening Urine albumin-to-reatinine ratio Starting 5 years after diagnosis As needed based on treatment Islet ell antibodies: GADA/IA2A/IAA/ZnT8 C-peptide levels May be needed in new-onset patients to establish diagnosis Oasionally needed to establish type 1 diabetes in a patient on insulin or to verify type 1 diabetes for insurane purposesdalways measure a simultaneous blood gluose level *Assumes a patient has a health are provider to manage the nondiabetes-related health assessments and to perform annual evaluations. Patient may opt out of measurement if psyhologially distressing. Foot inspetion should be done at eah visit and self-exams taught if high-risk harateristis are present. Comprehensive foot exam inludes inspetion, palpation of dorsalis pedis and posterior tibial pulses, presene or absene of patellar and Ahilles reflexes, and determination of proprioeption, vibration, and monofilament sensation. Within 5 years after diagnosis. If triglyerides are elevated in a nonfasting speimen, measure a diret LDL holesterol level.
7 2040 Position Statement Diabetes Care Table 5 Adults* Clinial evaluation Initial Annual Follow-up Height Weight BMI Blood pressure General physial exam Thyroid exam If indiated Injetion/infusion sites Comprehensive foot exam Visual foot exam Retinal exam by eye are speialist Starting 5 years after diagnosis; earlier if visual symptoms and/or true date of diagnosis is unknown In some individuals, sreening may be done every 2 years (see ADA Standards of Medial Care) As neededdat eah visit, if high-risk foot Depression sreen Hypoglyemia assessment Diabetes self-management skills Physial ativity assessment Assess linially relevant issues As needed As needed (e.g., alohol, drug, and tobao use; use of ontraeption; driving) Nutritional knowledge As needed Query for evidene of other autoimmune disease As needed based on linial senario As needed based on linial senario Immunizations as reommended by CDC As needed Laboratory assessments Initial Annual Follow-up A1C Every 3 months Creatinine learane/estimated glomerular filtration rate Fasting lipid panel As needed based on treatment TSH As needed based on Frequeny of testing varies based on linial symptoms, presene of antibodies, or if on treatment treatment Antithyroid antibodies Frequeny of testing is unknown; test if symptoms are present or for periodi sreening Celia antibody panel Frequeny of testing is unknown; test if symptoms are present or for periodi sreening Urine albumin-to-reatinine ratio GADA May be needed in new-onset patients to establish diagnosis C-peptide levels Oasionally needed to establish type 1 diabetes in a patient on insulin or to verify type 1 diabetes for insurane purposesdalways measure a simultaneous blood gluose level *Assumes a patient has a health are provider to manage the nondiabetes-related health assessments and to perform annual evaluations. Patient may opt out of measurement if psyhologially distressing. Foot inspetion should be done at eah visit and self-exams taught if high-risk harateristis are present. Comprehensive foot exam inludes inspetion, palpation of dorsalis pedis and posterior tibial pulses, determination of presene or absene of patellar and Ahilles reflexes, and determination of proprioeption, vibration, and monofilament sensation. In some instanes, the test may not need to be done yearly. If a patient is unable to undertake a fasting test due to hypoglyemia, measure a diret LDL holesterol level.
8 are.diabetesjournals.org Chiang and Assoiates 2041 self-are, inluding the risk of an eating disorder. (E) Assess psyhosoial status annually and more often as needed; treat and/or refer to a mental health professional as indiated. (E) DSME AND DSMS DSME and DSMS are the ongoing proesses of failitating the knowledge, skill, and ability neessary for diabetes self-are. These proesses inorporate the needs, goals, and life experienes ofthepersonwithdiabetes.theoverall objetives of DSME and DSMS are to support informed deision making, self-are behaviors, problem solving, and ative ollaboration with the health are team to improve linial outomes, health status, and quality of life in a ost-effetive manner (31). Beause hanges in both treatment and life irumstanes our aross the life span, DSME and DSMS must be a ontinuous proess adapted throughout the life of the person with type 1 diabetes so that self-management an be sustained. No matter how sound the medial regimen, it an only be as suessful as the ability of the individual and/or family to implement it. Family involvement remains an important omponent of optimal diabetes management throughout hildhood and adolesene. Health are providers who are for hildren and adolesents must, therefore, be apable of evaluating the eduational, behavioral, emotional, and psyhosoial fators that impat implementation of a treatment plan and must assist the individual and family to overome barriers or redefine goals as appropriate (Table 6). Diabetes eduation should our at diagnosis and upon transition to adult diabetes are and should be an ongoing proess. The information needs to be individualized and ontinually adaptedtothepatient s needs. Individuals with type 1 diabetes and parents/aregivers (for individuals aged,19 years) should reeive ulturally sensitive and developmentally appropriate individualized DSME and DSMS aording to national standards for DSME and DSMS when their diabetes is diagnosed and routinely thereafter. (B) Table 6 DSME ontent based on life stages Infany (birth 18 months) Period of trust versus mistrust Providing warmth and omfort measures after invasive proedures is important Feeding and sleeping or nap routines Vigilane for hypoglyemia Play age (3 5 years) Reassurane that body is intat, use of Band-Aids and kisses after proedures Identifiation of hypoglyemi signs and symptoms (temper tantrums and nightmares are ommon) Inlude hild in hoosing injetion and finger-prik sites Positive reinforement for ooperation Begin proess for teahing hild awareness of hypoglyemia Shool age (6 12 years) Integrate hild into eduational experiene Determine skill level Identify self-are skills Determine roles and responsibilities Communiation with peers and shool staffdwho and when to tell about diabetes Adolesene (12 18 years) Begin transition are planning Personal meaning of diabetes Determine roles and responsibilities in are Soial situations and dating Who or when to tell about diabetes Driving Sex and preoneption ounseling Alohol and drugs College and areer planning Young adults Personal meaning of diabetes Roles and responsibilities in are Soial situations and dating Who or when to tell about diabetes Geneti risks, oneption, and preoneption Travel Choosing or pursuing a areer Workplae rights Health or life insurane Involving friends and signifiant others in diabetes are Safety Creating a support network Establishing or maintaining independene Middle-aged adults Personal meaning of diabetes Roles and responsibilities in are Involving spouse or signifiant other in are Sexual funtioning Developing a support network Travel Pursuing a areer Workplae rights Health or life insurane Talking with hildren or other family members about diabetes Balaning other responsibilities with diabetes are Safety Faing ompliations Older adults Personal meaning of diabetes Roles and responsibilities in are Maintaining independene Obtaining assistane with diabetes are tasks Involving spouse or signifiant other in are Travel Talking with adult hildren or other family members about diabetes Safety Assessing for delines in ability to perform self-are/ativities of daily living Caring for diabetes along with other hroni illnesses or omorbidities Obtaining health are when living in multiple loations Community resoures Care of type 1 diabetes in long-term or other are failities
9 2042 Position Statement Diabetes Care Additional Considerations for Pediatris Eduation should be provided to appropriate shool personnel as a signifiant portion of a hild s day is spent in shool. (E) The developing teenager must be eduated about the transition to adult health are, beginning in early to midadolesene, with inreasing efforts to establish self-reliane in diabetes are beginning at least 1 year prior to the transition. Even after the transition to adult are is made, support and reinforement are reommended. (E) Additional Considerations for Adults Adult learning theory an be used to tailor DSME and DSMS to the age, life stage, ulture, literay/numeray, knowledge, experiene, and ognitive ability of the patient. (C) PSYCHOSOCIAL: ASSESSMENT AND TREATMENT OF PSYCHOSOCIAL ISSUES Assessment and appropriate management of psyhosoial issues are important throughout the life span of individuals with type 1 diabetes. In pediatris, health are providers should assess the individual hild and the hild s family for their ability to funtion and behave appropriately regarding safe and responsible diabetes are. For adults, the individual is the fous of are. However, family involvement should be strongly enouraged when appropriate. Depression sreening and disussion about psyhosoial issues are important omponents of the diabetes visit. Speial attentionshouldbepaidtodiabetesrelated distress, fear of hypoglyemia (and hyperglyemia), eating disorders, insulin omission, sublinial depression, and linial depression. These fators are signifiantly assoiated with poor diabetes self-management, a lower quality of life, and higher rates of diabetes ompliations. As individuals age, health are providers should evaluate issues related to self-are apaity, mobility, and autonomy. Suh fators are to be promptly addressed, as they make the management of type 1 diabetes ever more problemati. Make age-appropriate sreenings for psyhosoial issues a omponent of most diabetes visits. Any onerns should be pursued through treatment that may inlude referral to a mental health speialist. (E) Additional Considerations for Pediatris Ensure that there is developmentally appropriate parent/family involvement in the management of the hild s/adolesent s diabetesare tasks, avoiding a premature transfer of sole responsibility for diabetes management to the developing hild/ teenager. (B) Diretly ask about diabetes-related family onflit and stress and negotiate an aeptable resolution with the hild/adolesent and parent(s). However, if family onflit is extremely entrenhed and annot be resolved by the diabetes team, referral should be made to a mental health speialist who is knowledgeable about type 1 diabetes in youth and family funtioning. (C) Additional Considerations for Adults Ongoing evaluation of patients general and diabetes-related quality of life, emotional well-being, distress, depression, and resoures is warranted, preferably by a team that inludes a mental health speialist if suh resoures are available. (C) Health are providers should promptly address issues related to self-are apaity, mobility, and autonomy. (E) NUTRITION THERAPY Nutrition therapy is an important omponent of the treatment plan for all individuals with type 1 diabetes. Eah patient should have an individualized food plan based on food preferenes, shedule, and physial ativity. Nutrition therapy aims to ensure that the patient and family understand the impat food has on blood gluose, how food interats with exerise and insulin to prevent hypoand hyperglyemia and to ahieve gluose goals, and how to implement the food plan in a variety of situations. The food plan takes into onsideration the patient s numeray, literay, engagement, and ability to adjust insulin. General diabetes nutrition priniples, as defined in the ADA Standards of Care, apply to people with type 1 diabetes, partiularly in referene to normal growth and development in youth and the maintenane of a healthy body weight at all ages. Speifially, with regards to individuals with type 1 diabetes, topis suh as arbohydrate ounting and meal omposition should be addressed. For seleted individuals who have mastered arbohydrate ounting, eduation on the impat of protein and fat on glyemi exursions should be inorporated into diabetes management (32). Those who are overweight or obese may benefit from weight redution ounseling. Individualized medial nutrition therapy is reommended for all people with type 1 diabetes as an effetive omponent of the overall treatment plan. (A) Monitoring arbohydrate intake, whether by arbohydrate ounting or experiene-based estimation, remains a key strategy in ahieving glyemi ontrol. (B) If adults with type 1 diabetes hoose to drink alohol, they should be advisedtodosoinmoderation(one drink per day or less for adult women and two drinks per day or less for adult men). Disussion with a health are provider is advised to explore potential interations with mediations. Adults should be advised that alohol an lower blood gluose levels and that driving after drinking alohol is ontraindiated. (E) PHYSICAL ACTIVITY AND EERCISE Exerise has many positive health and psyhologial benefits inluding physial fitness, weight management, and enhaned insulin sensitivity. It also provides opportunities for soial interations and builds self-esteem. However, exerise reates hallenges for people with type 1 diabetes due to the inreased risk for both hypoglyemia and hyperglyemia. During exerise, multiple hormones (insulin, gluagon, ateholamines, growth hormone, and ortisol) ontrol fuel metabolism and reate a balane between gluose uptake by exerising musles and hepati gluose prodution (33,34). The equilibrium between insulin seretion and the ounterregulatory hormones varies aording to the exerise type, intensity, and duration (35). Hyperglyemia results from ounterregulatory hormone exess with insuffiient insulin, leading to exessive hepati gluose prodution and limiting
10 are.diabetesjournals.org Chiang and Assoiates 2043 inreased gluose uptake into skeletal musle. Hyperglyemia an our before, during, and after various types of exerise. If the patient feels well, with negative or minimal urine and/or blood ketones, and there is a lear reason for the elevated blood gluose level, suh as underdosing insulin at the preeding meal, it is not neessary to postpone exerise based solely on hyperglyemia. However, when people with type 1 diabetes are deprived of insulin for h and are ketoti, exerise an worsen hyperglyemia and ketosis. Therefore, vigorous ativity should be avoided in the presene of severe hyperglyemia and ketosis, espeially with known insulin omission. Physial ativity inreases hypoglyemia risk during and immediately following exerise, and, again, about 7 11 h postexerise. This delayed suseptibility to hypoglyemia is referred to as the lag effet of exerise (36,37) and is aused by musles replenishing glyogen stores postexerise. Hypoglyemia and fear of hypoglyemia an limit partiipation in exerise. Strategies should be developed to prevent and treat hypoglyemia readily. Individualization is neessary, but linial experiene suggests that it is safest for most patients to have a blood gluose level of 100 mg/dl (5.6 mmol/l) or higher prior to starting exerise. This may be ahieved by reduing the prandial insulin dose for the meal/snak preeding exerise and/or inreasing food intake. Some patients an avoid hypoglyemia by reduing insulin (suh as by lowering pump basal rates) (38) or by onsuming additional arbohydrates during prolonged physial ativity. One study in hildren on pumps suggested that a redution in overnight basal insulin the night following exerise may redue the risk of delayed exerise-indued hypoglyemia (39). Frequent SMBG and/or CGM use are key to exerising safely, as is ready aess to arbohydrates. Basi reommendations for physial ativity are the same as those for all hildren and adults, independent of the diagnosis of diabetes: hildren should be enouraged to engage in at least 60 min of physial ativity daily, and adults should be advised to perform at least 150 min/week of moderateintensity aerobi physial ativity (50 70% of maximum heart rate) or a lesser amount (60 75 min/week) of vigorousintensity ativity (40,41). Exerise should also inlude resistane and flexibility training. Individuals, partiularly adults, should be assessed for ardiovasular risk and the presene of ompliations that might limit exerise as disussed more fully in the ADA Standards of Medial Care in Diabetes (42). Exerise should be a standard reommendation as it is for individuals without diabetes; however, reommendations may need modifiations due to the presene of maro- and mirovasular diabetes ompliations. (E) Patients of all ages (or aregivers of hildren) should be eduated about the prevention and management of hypoglyemia that may our during or after exerise. (E) Patients should be advised about safe preexerise blood gluose levels (typially 100 mg/dl or higher depending on the individual and type of physial ativity). (E) Reduing the prandial insulin dose for the meal/snak preeding exerise and/or inreasing food intake an be used to help raise the preexerise blood gluose level and redue hypoglyemia. (E) A redution in overnight basal insulin the night following exerise may redue the risk for delayed exeriseindued hypoglyemia. (C) SMBG should be performed as frequently as needed (before, during, and after exerise) in order to prevent, detet, and treat hypoglyemia and hyperglyemia. (E) Soure(s) of simple arbohydrate should be readily available before, during, and after exerise to prevent and treat hypoglyemia. (E) TREATMENT TARGETS General Considerations Hyperglyemia defines diabetes and is diretly related to the inidene of ompliations. Therefore, glyemi ontrol is fundamental to diabetes management. The Diabetes Control and Compliations Trial (DCCT) (43) was a prospetive randomized ontrolled study omparing intensive versus standard glyemi ontrol in patients diagnosed with type 1 diabetes relatively reently. The DCCT demonstrated that ahieving an A1C of,7% redued the inidene of mirovasular ompliations of type 1 diabetes ompared with standard ontrol, whih ahieved an A1C of ;9% during the period of the randomized trial. The Epidemiology of Diabetes Interventions and Compliations (EDIC) study (44,45) was a follow-up of the DCCT ohorts. The EDIC study remarkably demonstrated persistent mirovasular and ardiovasular benefits in subjets who had previously reeived intensive treatment, even though their glyemi ontrol had deteriorated over time. While A1C and blood gluose targets are needed, the ADA emphasizes that glyemi targets should be individualized with the goal of ahieving the best possible ontrol while minimizing the risk of severe hyperglyemia and hypoglyemia (Table 7). Goals should be individualized based on duration of diabetes, age/life expetany, omorbid onditions, known CVD or advaned mirovasular ompliations, hypoglyemia unawareness, and individual patient onsiderations. More or less stringent glyemi goals may be appropriate for individual patients. Postprandial gluose may be targeted if A1C goals are not met despite reahing preprandial gluose goals. Reommendation Lifestyle, psyhosoial, and medial irumstanes should be onsidered when reommending glyemi goals for all age-groups. (E) Glyemi Control Goals in Pediatris As the DCCT only inluded pediatri patients aged $13 years (195 adolesents aged years at entry), treatment guidelines for pediatri patients have been based nearly exlusively on professional, expert advie. Furthermore, Table 7 Summary of A1C reommendations for nonpregnant people with diabetes* Youth (,18 years),7.5% Adults,7.0% Older adults Healthy,7.5% Complex/intermediate,8.0% Very omplex/poor health,8.5% *Targets must be individualized based on apatient s irumstanes. No omorbidities, long life expetany.
11 2044 Position Statement Diabetes Care despite the overall A1C goal of,7% for adults with type 1 diabetes, pediatri patients, aged years, had an A1C target of,7.5%. This slightly higher A1C target for adolesents with type 1 diabetes was based on expert reommendations and the linial reality that optimizing glyemi ontrol in adolesent patients with type 1 diabetes is espeially hallenging, given the physiologial and behavioral hallenges that onfront this age-group. The ADA s blood gluose and A1C goals traditionally have been developmentally or age based in the pediatri population, but it is now time to alter the traditional goals based on reent data. The traditional reommendations are an A1C goal of,8.5% for youth under the age of 6 years,,8% for those 6 12 years old, and,7.5% for those years old. Lower blood gluose levels and lower A1C targets should be pursued as long as patients an avoid severe, reurrent hypoglyemia. Thus, the overall reommendation has inluded the goal to ahieve as lose to normal blood gluose and A1C levels as ispossiblewithouttheourreneof severe, reurrent hypoglyemia. Historially, the ADA reommended higher A1C targets for young hildren. This reommendation arose from a ombination of two lines of unsubstantiated evidene. First, an older body of literature, refleting therapy in the premodern era, devoid of insulin analogs, easy-to-use blood gluose monitors, smart pumps, and CGM devies, indiated that severe reurrent hypoglyemia with seizure and/or oma in young hildren was assoiated with neuroognitive ompromise (46). The seond line of evidene arose from literature that questioned what, if any, impat blood gluose and A1C levels prior to puberty have on the risk for the development of future long-term ompliations of diabetes (47,48). With the ombination of these two independent lines of reports, it is not surprising that earlier reommendations regarding glyemi targets foused on the avoidane of severe hypoglyemia in order to redue risk of neuroognitive dysfuntion, espeially in young hildren and even shool-aged hildren. Currently, treatment strategies for hildren reommend physiologial insulin replaement with modern strategies and treatment tools. More reent investigation and ative ongoing researh have dispelled onerns regarding hypoglyemia and neuroognitive dysfuntion (49,50). Studies assessing neuroognitive funtion have failed to identify adverse effets of a past history of hypoglyemia in the young hild; however, as always, further researh needs to be onduted. There are also questions regarding the premise that the years prior to puberty do not impat the future risk of ompliations (51). Many investigators and liniians believe in the importane of ontrolling blood gluose and A1C levels prior to puberty to redue risk for both miro- and marovasular ompliations. Additionally, there is burgeoning evidene that elevated blood gluose levels and glyemi variability in the very young hild with diabetes may produe adverse outomes in the short term on neuroognitive funtion and the entral nervous system (52,53). These reent artiles suggest that hyperglyemia and glyemi variability are assoiated with hanges in the entral nervous system white matter, as observedinmrisans. Taking into aount the ombination of spotty past evidene related to the adverse effets of hypoglyemia on the developing brain and inreasing evidene from more reent investigations foused on the potential risks of hyperglyemia and gluose variability on the entral nervous system, the ADA has deided to alter the reommendations for glyemi targets in pediatri patients with type 1 diabetes and harmonize with other organizations. The International Soiety for Pediatri and Adolesent Diabetes (ISPAD) uses a single A1C goal of,7.5% aross all pediatri age-groups. This reommendation is based on linial studies and expert opinion, as rigorous evidene does not urrently exist. Speifially, the reommendation is derived from a ombination of linial experiene and intensive management strategies that provide opportunities to ahieve as near-normal glyemi ontrol as possible without the ourrene of severe hypoglyemia. In light of the above evidene, the ADA will harmonize its glyemi goals with those of ISPAD (as well as the Pediatri Endorine Soiety and the International Diabetes Federation) by using a single A1C goal of <7.5% aross all pediatri age-groups. However, as mentioned previously, it must be emphasized that the ADA strongly believes that blood gluose and A1C targets should be individualized with the goal of ahieving the best possible ontrol while minimizing the risk of severe hyperglyemia and hypoglyemia and maintaining normal growth and development. Reommendation An A1C goal of,7.5% is reommended aross all pediatri age-groups. (E) Glyemi Control Goals in Adults Similar to in hildren, the are of older adults with diabetes is ompliated by their linial and funtional heterogeneity. Unlike the large older adult population with type 2 diabetes, whih inludes patients with both long-standing and new-onset diabetes, most older adults with type 1 diabetes have longstanding disease. Even so, there is a wide spetrum of health aross older individuals. They may have advaned ompliations, or they may have lived with diabetes for many years without the development of ompliations. Some older patients have multiple omorbid onditions and/or impairments of physial or ognitive funtioning, while others have little omorbidity and high funtional status. Life expetany is highly variable and is defined by omorbidity and funtional status more than it is by age. Health are providers aring for older adults with diabetes must take this heterogeneity into onsideration when setting and prioritizing treatment goals. The benefits of interventions suh as stringent glyemi ontrol may not apply to those with advaned ompliations of diabetes or to those with a life expetany of less than the antiipated time frame of benefit. Conversely, the risks of interventions suh as tight glyemi ontrol (hypoglyemia, treatment burden) may be greater in older patients. Although individualization is ritial, in general, older patients with long life expetany and little omorbidity should have treatment targets similar to those of middle-aged or younger adults. In more frail patients, treatment targets might reasonably be relaxed, while symptomati hyperglyemia or the risk of DKA should still be avoided (54).
12 are.diabetesjournals.org Chiang and Assoiates 2045 Lowering A1C to below or around 7% has been shown to redue mirovasular ompliations of diabetes, and, if ahieved soon after the diagnosis of diabetes, is assoiated with long-term redution in marovasular disease. Therefore, a reasonable A1C goal for many nonpregnant adults with type 1 diabetes is,7%. (B) Providers might reasonably suggest more stringent A1C goals (suh as,6.5%) for selet individual patients, if this an be ahieved without signifiant hypoglyemia or other adverse effets of treatment. Appropriate patients might inlude those with a short duration of diabetes, a long life expetany, hypoglyemia awareness, and no signifiant CVD. (C) Less stringent A1C goals (suh as,8.5%) may be appropriate for patients with a history of severe hypoglyemia, hypoglyemia unawareness, limited life expetany, advaned mirovasular/marovasular ompliations, or extensive omorbid onditions. (B) Glyemi ontrol for those of any age with type 1 diabetes should be assessed based on frequent SMBG levels (and CGM data, if available) in addition to A1C in order to diret hanges in therapy. (B) MONITORING SMBG The DCCT demonstrated the benefits of intensive glyemi ontrol on diabetes ompliations with SMBG as part of a multifatorial intervention, suggesting that SMBG is a ruial omponent of effetive therapy. SMBG allows patients to evaluate their individual response to therapy and assess whether glyemi targets are being ahieved. SMBG results are useful in preventing hypoglyemia, adjusting mediations (partiularly prandial insulin doses), and understanding the impat of appropriate nutrition therapy and physial ativity. More frequent SMBG is orrelated to lower A1C levels (55,56). SMBG frequeny and timing should be ditated by the patient s speifi needs and goals. When presribing SMBG, providers must ensure that patients reeive ongoing instrution and regular evaluation of their SMBG tehnique and their ability to use SMBG data to adjust therapy (insulin and/or food). Furthermore, SMBG results should be downloaded and reviewed at eah visit. SMBG is espeially important for patients with type 1 diabetes to monitor for and prevent asymptomati hypoglyemia and hyperglyemia. Type 1 diabeti patients should perform SMBG prior to, and sometimes after, meals and snaks, at bedtime, before and after exerise, when they suspet low blood gluose, after treating low blood gluose until they are normoglyemi, and prior to ritial tasks suh as driving. For many patients, this will require testing 6 10 times daily, although individual needs may vary. For example, sik hildren may require up to 10 SMBG tests per day or more. A study of hildren and adolesents with type 1 diabetes showed that, after adjustment for multiple onfounders, inreased SMBG frequeny was signifiantly assoiated with lower A1C. In the range of 0 5 testsper day, A1C dereased by 0.46% per additional test per day. Inreased testing wasassoiatedwithsignifiantly less DKA and (probably due to reverse ausality) signifiantly more hypoglyemia (55,56). SMBG auray is dependent on both theinstrumentandtheuser(57),soitis important to evaluate eah patient s monitoring tehnique, both initially and at regular intervals thereafter. Optimal use of SMBG requires a proper review and interpretation of the data by both the patient and the provider. CGM Real-time CGM through the measurement of interstitial gluose (whih orrelates well with plasma gluose) is available. These sensors require alibration with SMBG, and CGM users still require SMBG for making aute treatment deisions. CGM devies have alarms for hypo- and hyperglyemi exursions that inlude absolute level and rate-ofhange alerts. A 26-week randomized trial of 322 type 1 diabeti patients showed that adults aged $25 years using intensive insulin therapy and CGM experiened a 0.5% redution in A1C (from ;7.6% to 7.1%) ompared with usual intensive insulin therapy with SMBG (58). Partiipants aged,25 years (hildren, teenagers, and young adults) randomized to sensor use did not ahieve a signifiant A1C redution. However, these younger patients did not use CGM onsistently. The greatest preditor of A1C lowering for all agegroups was frequeny of sensor use, whih was lowest in 15- to 24-year-old subjets. There was no signifiant differene in hypoglyemia in any age-group. In a smaller randomized ontrolled trial of 129 adults and hildren with baseline A1C,7.0%, outomes ombining A1C and hypoglyemia favored the group using CGM, suggesting that CGM is benefiial for pediatri patients and adults with type 1 diabetes who have already ahieved exellent ontrol (58). Overall, meta-analyses suggest that, ompared with SMBG, CGM use is assoiated with A1C lowering by ;0.26% (59) without an inrease in hypoglyemia, although existing studies have small sample sizes and are of relatively short duration. The tehnology may be partiularly useful in those with hypoglyemia unawareness and/or frequent hypoglyemi episodes, although studies have not onsistently shown signifiant redutions in the ourrene of severe hypoglyemia. A CGM devie equipped with an automati low threshold suspend feature was approved by the U.S. Food and Drug Administration (FDA) in The Automation to Simulate Panreati Insulin Response (ASPIRE) trial of 247 patients showed that sensoraugmented insulin pump therapy with a low gluose suspend feature signifiantly redued noturnal hypoglyemia without inreasing A1C levels for those.16 years of age (60). These devies may offer the opportunity to redue severe hypoglyemia for those with a history of noturnal hypoglyemia, although more linial trials are needed. Patients with type 1 diabetes should perform SMBG prior to meals and snaks, at a minimum, and at other times, inluding postprandially to assess insulin-to-arbohydrate ratios; at bedtime; midsleep; prior to, during, and/or after exerise; when they suspet low blood gluose; after treating low blood gluose until they have restored normoglyemia; when orreting a high blood gluose level; prior to ritial tasks suh as driving; and at more frequent intervals during illness or stress. (B) Individuals with type 1 diabetes need to have unimpeded aess to gluose
13 2046 Position Statement Diabetes Care test strips for blood gluose testing. Regardless of age, individuals may require 10 or more strips daily to monitor for hypoglyemia, assess insulin needs prior to eating, and determine if their blood gluose level is safe enough for overnight sleeping. (B) CGM is a useful tool to redue A1C levels in adults without inreasing hypoglyemia and an redue glyemi exursions in hildren. Glyemi improvements are orrelated with frequeny of CGM use aross all ages. (A) Additional Considerations for Pediatris Children should have additional blood gluose heks if the parent/ aregiver is onerned that the hild s behavior may be due to low/high blood gluose levels. (E) Shool employees and aregivers should be knowledgeable about SMBG and equipped with all neessary supplies. (E) Capable hildren should be permitted to self-manage their diabetes at shool. (E) A1C TESTING A1C reflets average glyemia over 2 3 months (57) and strongly predits diabetes ompliations (43,61). Thus, A1C testing should be performed routinely in all patients with diabetes at initial assessment and as part of ontinuing are. A1C is a onvenient method to trak diabetes ontrol; however, there are disadvantages. Glyation rates, and thus A1C levels, may vary with patients rae/ethniity. However, this is ontroversial. Additionally, anemias, hemoglobinopathies, and situations of abnormal red ell turnover affet A1C (42). A1C measurements approximately every 3 months determine whether a patient s glyemi targets have been reahed and maintained. For any individual patient, the frequeny of A1C testing should be dependent on the linial situation, the treatment regimen used, and the liniian s judgment. Unstable or highly intensively managed patients (e.g., pregnant type 1 diabeti women) may require more frequent testing than every 3 months (62). In patients with hemoglobinopathies that interfere with the A1C assay or with hemolyti anemia or other onditions that shorten the red blood ell life span, the A1C may not aurately reflet glyemi ontrol or orrelate well with SMBG testing results. In suh onditions, frutosamine may be onsidered as a substitute measure of long-term (average over 2 weeks) glyemi ontrol. Perform the A1C test quarterly in most patients with type 1 diabetes and more frequently as linially indiated (i.e., pregnany). (A) Point-of-are A1C testing, using a DCCT standardized assay, may provide an opportunity for more timely treatment hanges. (E) INSULIN THERAPY The DCCT learly showed that intensive insulin therapy, defined as three or more injetions per day of insulin or ontinuous subutaneous insulin infusion (CSII) (or insulin pump therapy), was a key part of improved glyemia and better outomes (43,63). The study was arried out with short- and intermediate-ating human insulins. Despite better mirovasular outomes, intensive insulin therapy was assoiated with a high rate of severe hypoglyemia (62 episodes per 100 patient-years of therapy). Sine the ompletion of the DCCT, a number of rapid-ating and long-ating insulin analogs have been developed. These analogs are assoiated with less hypoglyemia than human insulin while offering thesameamountofa1cloweringin people with type 1 diabetes (64,65). TheSensor-AugmentedPumpTherapy for A1C Redution (STAR 3) study was a large (n 5 485) randomized linial trial omparing insulin pump therapy and CGM with insulin injetions in youth and adults with type 1 diabetes. The two study groups started with the same baseline A1C of 8.3%. After 1 year, the group using insulin pump therapy and CGM had lower A1C levels (7.5% vs. 8.1%, P, 0.001) without signifiant noturnal hypoglyemia ompared with the insulin injetion ohort (66). Reently, a large randomized trial in patients with type 1 diabetes and noturnal hypoglyemia reported that the use of sensor-augmented insulin pump therapy with the threshold-suspend feature redued noturnal hypoglyemia without inreasing glyated hemoglobin values (60). In general, intensive management using pump therapy/cgm should be strongly enouraged, with ative patient/family partiipation enhaning suessful outomes (67 69). Most individuals with type 1 diabetes should be treated with multiple daily insulin injetions (three or more injetions per day of prandial insulin and one to two injetions of basal insulin) or CSII. (A) Most individuals with type 1 diabetes should be eduated in how to math prandial insulin dose to arbohydrate intake, premeal blood gluose, and antiipated ativity. (E) Most individuals with type 1 diabetes should use insulin analogs to redue hypoglyemia risk. (A) All individuals with type 1 diabetes should be taught how to manage blood gluose levels under varying irumstanes, suh as when ill or reeiving gluoortioids or for those on pumps, when pump problems arise. (E) Child aregivers and shool personnel should be taught how to administer insulin based on provider orders when a hild annot self-manage and is out of the are and ontrol of his or her parent/guardian. (E) INTERDICTION Therapy trials to prevent type 1 diabetes development (prevention), to preserve remaining b-ells (preservation), and to replae b-ells (transplantation) are ongoing. Although means are available to sreen and predit family members at risk for developing type 1 diabetes, efforts to delay or prevent disease onset have been largely disappointing. A variety of different immunomodulatory and immune-suppressive agents have been evaluated in patients with reent-onset type 1 diabetes, and the effets have been modest at best: for the subset of drugs that appear to have an effet, not all patients respond; for those who do, the effets are generally transient. Many of the agents tested to date are FDA approved for other indiations, but given the observations to date and potential toxiities, the reommendation is that patients should only reeive these drugs after being enrolled in linial researh protools with appropriate follow-up. Long-term safety and effiay data are sare, espeially in hildren. Investigators ontinue to evaluate promising new agents and ombinations of
14 are.diabetesjournals.org Chiang and Assoiates 2047 drugs or ell-based therapies in an effort to safely and effetively modulate the autoimmune response (70). b-cell REPLACEMENT THERAPY b-cell replaement may be ahieved through panreas or islet transplantation in selet andidates. Panreas transplants are now aepted as a proven therapy, while islet transplants, though signifiantly improving, are still mostly done on an experimental basis. Panreas Transplants Panreas transplants are most often performed in ombination with kidney transplantation, either as a simultaneous panreas-kidney (SPK) transplant or as a panreas-after-kidney (PAK) transplant (71). SPK and PAK transplants may be onsidered for individuals with late-stage kidney disease beause the transplants an normalize gluose levels, whih will prevent hypoglyemia and provide some protetion for the transplanted kidney (72), and provide other benefits, inluding an improvement in quality of life (71). These reipients will already require immunosuppression for their renal transplants, whih means the major additional risk is the operative proedure. SPK transplants funtion for an average of 9 years, ompared with 6 years for PAK transplants (71). There has been debate about panreas transplant alone (PTA) in the absene of an indiation for kidney transplantation beause of the risks of mortality, morbidity, and immunosuppression. Outomes have gradually improved (73), suh that the proedure an be autiously onsidered for individuals without renal failure who have unstable gluose ontrol and hypoglyemia unawareness. Beause of the risks of panreas transplantation ompared with traditional methods for ontrolling blood gluose levels, all available efforts to use exogenous insulin ombined with tehnology, eduation, and gluose follow-up should be exhausted before PTA is performed. The durability of funtion averages 6 years, whih is muh better than islet transplantation but about the same as PAK and not as good as SPK (73). Islet Transplantation A major appeal of islet transplantation is that it does not require major surgery. Moreover, outomes have improved over the past deade suh that normoglyemia without insulin is now maintained for an average of 3 years in speialized protools (74). Even when insulin treatment is reinstituted, residual insulin seretion an help reipients maintain good ontrol with less hypoglyemia and a less ompliated regimen for several more years. At the present time, few islet transplants are being performed and most are experimental. However, they an be onsidered as a treatment option for those who are poor andidates for whole-organ transplants. Importantly, their urrent suess has established a proof of priniple for ellular transplantation. Great progress is being made in finding an abundant soure of healthy insulin-produing ells and in developing better ways to protet transplanted ells from immune destrution (75,76). Potential solutions for the shortage of islets inlude embryoni stem ells, indued pluripotent stem ells, xenogenei tissue, and various other potential souresdall the fous of ongoing researh efforts. Another possible way to replenish the b-ell defiieny of diabetes is through regeneration of the endorine panreas; this too is being worked on intensively. Consider solid organ panreas transplantation simultaneously with kidney transplantation in patients with type 1 diabetes who have an indiation for kidney transplantation and are poorly ontrolled with large glyemi exursions. (B) Consider solid organ panreas transplantation after kidney transplantation in adult patients with type 1 diabetes who have already reeived a kidney transplant. (C) Judiiously onsider solid organ panreas transplantation alone in adults with type 1 diabetes, unstable gluose ontrol, hypoglyemia unawareness, and an inreased risk of diabetesrelated mortality, who have attempted all of the more traditional approahes to glyemi ontrol and have remained unsuessful, yet are judged responsible enough to manage the antirejetion mediation regimen, risks, and follow-up required with an organ transplant. (C) Consider referral to researh enters for protoolized islet ell transplantation in patients with type 1 diabetes and debilitating ompliations of diabetes who are interested in researh possibilities and fit the riteria for the researh protool. (E) ADJUNCTIVE THERAPIES Pramlintide Pramlintide, an amylin analog, is an agent that delays gastri emptying, blunts panreati seretion of gluagon, and enhanes satiety. It is an FDAapproved therapy for use in type 1 diabeti patients and has been shown to redue A1C, indue weight loss, and lower insulin dose. However, it is only indiated for adults. Two 52-week trials of pramlintide (n 5 1,131; age.18 years) showed A1C redutions of ; % (77,78). In both studies, a greater proportion of partiipants ahieved an A1C target of,7% with the therapy than without the therapy. There are a few small, short-term studies of pramlintide use in hildren with type 1 diabetes, with outomes similar to those in the adult studies. Clearly, larger, long-term studies are needed in pediatris. Inretin-Based Therapies Injetable gluagon-like peptide-1 (GLP-1) agonists and oral dipeptidyl peptidase-4 (DPP-4) inhibitors are inreasingly being studied in the type 1 diabeti population, but are not approved by the FDA for this indiation. GLP-1 agonists delay gastri emptying, suppress the postprandial rise in gluagon seretion, and may inrease satiety. Preliminary studies indiate that these agents may also failitate weight loss. Further long-term linial trials in type 1 diabeti patients are needed. Sodium-Gluose Cotransporter 2 Inhibitors Sodium-gluose otransporter 2 (SGLT2) inhibitors work by inhibiting gluose reabsorption in the kidney and are also being tested in individuals with type 1 diabetes. These agents provide insulinindependent gluose lowering by bloking gluose reabsorption in the proximal renal tubule, leading to weight loss and A1C redution in individuals with type 2 diabetes. However, insuffiient data exist to reommend linial use of these agents in type 1 diabetes at this time.
15 2048 Position Statement Diabetes Care Metformin Metformin is a biguanide that dereases hepati gluoneogenesis and is used as first-line therapy in type 2 diabetes. It has been shown to have some benefit in reduing insulin doses and weight in small studies in patients with type 1 diabetes (79) and is now being evaluated more fully for use in patients with type 1 diabetes. Two randomized ontrolled trials are urrently under way evaluating metformin in type 1 diabeti patients. The first study is in adults and is using arotid intima-medial thikness as an outome measure (ClinialTrials.gov identifier: NCT ). The seond study is fousing on overweight or obese youths betweentheagesof12and19yearswho require $0.85 units/kg/day of insulin (ClinialTrials.gov identifier: NCT ). Results are urrently pending. Pramlintide may be onsidered for use as adjuntive therapy to prandial insulin in adults with type 1 diabetes failing to ahieve glyemi goals. (B) Evidene suggests that adding metformin to insulin therapy may redue insulin requirements and improve metaboli ontrol in overweight/ obese patients and poorly ontrolled adolesents with type 1 diabetes, but evidene from larger longitudinal studies is required. (C) Current type 2 diabetes mediations (GLP-1 agonists, DPP-4 inhibitors, and SGLT2 inhibitors) may be potential therapies for type 1 diabeti patients, but require large linial trials before use in type 1 diabeti patients. (E) HYPOGLYCEMIA Hypoglyemia risk is the limiting step in the treatment of type 1 diabetes at any age. Beause urrent methods of blood gluose detetion and insulin replaement are imperfet (though improved from prior eras), hypoglyemia risk is invariably present. Patient eduation (80), frequent SMBG, and CGM an help detet hypoglyemia and allow for adjustments in insulin dosing and arbohydrate intake. Severe hypoglyemia rates inrease with anteedent episodes of hypoglyemia, age, and duration of diabetes; thus, this is an issue that must be reassessed frequently (81). Hypoglyemia unawareness is related to a redued sympathoadrenal response to hypoglyemia; it an our in the setting of reurrent hypoglyemia or autonomi failure and an be reversed by srupulous avoidane of hypoglyemia. Patients should be sreened to determine the threshold at whih hypoglyemia symptoms our; if the threshold is suggestive of hypoglyemia unawareness, the treatment goals and regimen should be revisited and ounseling regarding appropriate self-monitoring before ritial tasks should be reinfored (82). Oral arbohydrate is the treatment of hoie for self-treatment or for the treatment of hypoglyemi adults and hildren who are alert and able to eat. Gluagon is used for severe hypoglyemia. In hildren, small studies have led to the onept of using age-based minidose gluagon if the hild is alert but not able to eat (83). Individuals with type 1 diabetes, or their aregivers, should be asked about symptomati and asymptomati hypoglyemia at eah enounter. (E) Gluose (15 20 g) is the preferred treatment for the onsious individual with hypoglyemia, although any form of arbohydrate may be used. If the SMBG result 15 min after treatment shows ontinued hypoglyemia, the treatment should be repeated. One blood gluose onentration returns to normal, the individual should onsume a meal or snak to prevent reurrene of hypoglyemia. (E) Gluagon should be presribed for all individuals with type 1 diabetes. Caregivers or family members of these individuals should be instruted in its administration. (E) Hypoglyemia unawareness or one or more episodes of severe hypoglyemia should trigger reevaluation of the treatment regimen. (E) Insulin-treated patients with hypoglyemia unawareness or an episode of severe hypoglyemia should be advised to raise their glyemi targets to stritly avoid further hypoglyemia for at least several weeks to partially reverse hypoglyemia unawareness and redue the risk of future episodes. (B) DKA DKA (see ref. 70 for definition) is an aute ompliation of diabetes that an be assoiated with new-onset type 1 diabetes, insulin omission, and inreased levels of ounterregulatory hormones/ytokines assoiated with stress, suh as an infetion. Mild ases an be safely and effetively treated in an aute are setting with appropriate resoures and may not require hospitalization. Eduation must be provided to individuals with type 1 diabetes in order to help prevent DKA, whih an have serious sequelae, partiularly in hildren under 5 years of age. Although DKA and hyperglyemi hyperosmolar state (HHS) may overlap, espeially when dehydration is severe, DKA must be distinguished from HHS (serum gluose.600 mg/dl, serum osmolality.330 mosm/kg, and no signifiant ketosis and aidosis) beause patients with HHS typially are severely dehydrated and require more aggressive fluid management. There are multiple guidelines available for the management of DKA (84). Individuals and aregivers of individuals with type 1 diabetes should be eduated and reminded annually how to prevent DKA, inluding a review of sik-day rules and the ritial importane of always administering insulin and monitoring both gluose and ketone levels. (B) Insulin omission is the major ause of DKA; therefore, individuals with type 1 diabetes must have aess to an uninterrupted supply of insulin. (E) Patients with type 1 diabetes and their families should have around-the-lok aess to medial advie and support to assist with sik-day management. (C) Standard protools for DKA treatment should be available in emergeny departments and hospitals. (E) CVD SCREENING AND TREATMENT Muh of the existing data on the risk of CVD in individuals with diabetes is based on people with type 2 diabetes who often have additional CVD risk fators, suh as metaboli syndrome, hypertension, and dyslipidemia. How muh is appliable to people with type 1 diabetes is unknown. However, people with type 1 diabetes are at inreased risk for CVD, partiularly those with additional risk fators. In type 1 diabetes, standard risk fators apply, suh as hyperlipidemia, hypertension, age, family history, smoking, weight, and presene of albuminuria. As suh,
16 are.diabetesjournals.org Chiang and Assoiates 2049 these should be onsidered when determining the need for evaluation and treatment for CVD. However, even in the absene of lassi risk fators, there may be high CVD risk. An adult with hildhoodonset type 1 diabetes of 20-year duration has a substantially inreased risk of oronary artery disease of 1% per year (83), thus meriting high-intensity statin therapy aording to the new joint Amerian College of Cardiology/Amerian Heart Assoiation guidelines ($7.5% 10-year risk) (85). In some ases, measurement of oronary artery alifiation may be a helpful method for determining CVD risk (86). Here, as with all management issues for people with type 1 diabetes, providers need to individualize assessment and treatment options. With regard to treatment, statin therapy is the preferred treatment for lipid lowering/cvd risk redution (85). The Heart Protetion Study (HPS) did inlude type 1 diabeti partiipants who appeared to experiene the same degree of benefit from statins as others in the study, though the finding was not statistially signifiant due to low numbers (87). Unfortunately, there are no blood pressure intervention trials with CVD end points in type 1 diabetes and only one LDL holesterol lowering trial (85). Statin and aspirin therapy (if not ontraindiated) should be onsidered and used as is individually indiated. Therapy for those under age 40 years with less than a 20-year diabetes duration (or over age 75 years) should be onsidered on an individual basis, though, depending on overall risk, an LDL holesterol,100 mg/dl has been suggested as an appropriate goal with statin intervention for those with LDL holesterol levels of mg/dl. (E) Individuals with type 1 diabetes aged years may benefit from moderateto-intensive statin therapy with onsideration of diabetes duration and CVD risk fators. If 10-year risk is estimated to be $7.5%, then intensive statin therapy should be onsidered. (B) SPECIFIC SETTINGS AND POPULATIONS Pregnany Preoneption Counseling and Care To minimize risks assoiated with pregnany and type 1 diabetes, preoneption ounseling and are are ritial. Preoneption are with tight glyemi ontrol improves outomes inluding lower esarean rates (88), dereased perinatal mortality (89 91), and dereased ongenital malformations (89 97). Although there is some evidene that hildbearing may be redued (98 100), in general, fertility should be assumed to be normal, and all young women with type 1 diabetes should reeive preoneption ounseling overing diabetes and general topis, inluding use of prenatal vitamin, disontinuation of potentially teratogeni mediations, and the importane of glyemi ontrol to redue the risk of ongenital malformations. Pregnany Type 1 diabetes affets approximately % of all pregnanies (101). During pregnany, there are substantial hanges in maternal insulin sensitivity that may ause profound hanges in insulin requirements. Whereas insulin resistane inreases markedly during the seond and third trimesters, a greater proportion of total daily insulin dose must be given prandially and a lower proportion used to over basal metaboli requirements (102). Pregnant women with type 1 diabetes require metiulous glyemi management by experts trained in obstetris, endorinology, and maternal-fetal mediine. Women who are planning pregnany or who are pregnant may need to test blood gluose levels frequently (often 10 or more times daily) to reah and maintain a near-normal A1C level without exessive hypoglyemia. Severe hypoglyemia may our early during pregnany (102). This is followed by periods of insulin resistane and subsequent hyperglyemia if the inreased insulin needs are not met. Therefore, health are providers must be vigilant and frequently adjust insulin dosing throughout gestation. In a pregnany ompliated by diabetes and hroni hypertension, target blood pressure goals of systoli blood pressure mmhg and diastoli blood pressure mmhg are reasonable. Lower blood pressure levels may be assoiated with impaired fetal growth (Table 8). ACE inhibitors and angiotensin reeptor blokers are ontraindiated during pregnany beause they may have adverse effets on the fetus. Antihypertensive drugs known to be effetive and safe in pregnany inlude methyldopa, labetalol, diltiazem, lonidine, and prazosin. Eye examinations should our in the first trimester with lose follow-up throughout pregnany and for 1 year postpartum beause of the risk of rapid retinopathy progression during pregnany. Those with progressive retinopathy should have more frequent sreening by an ophthalmologist experiened in retinopathy management. See the Amerian Diabetes Assoiation/ JDRF Type 1 Diabetes Sourebook (70) for a summary of pregnany reommendations. The prevalene of Hashimoto thyroiditis may be as high as 31% in womenwithtype1diabetes(105). Therefore, all pregnant women with type 1 diabetes should be sreened for thyroid disease early in pregnany. Starting at puberty, preoneption ounseling should be inorporated into routine diabetes lini visits for all adolesents and women of hildbearing potential, and appropriate birth ontrol tehniques should be disussed with women who do not desire pregnany. (C) Table 8 ADA Standards of Care optimal targets in pregnany* Target maternal gluose Fasting mg/dl Peak postprandial mg/dl Mean,100 mg/dl Labor and delivery mg/dl (mean,100) Insulin drips 1 D10 50 /h A1C Preoneption,7% and as lose to normal as possible without signifiant hypoglyemia During pregnany,6% *See refs. 70, 103, and 104. These represent the mean 12 SD for normal. They are targets, but not everyone an ahieve them. There is ertainly marked variability, whih explains why there is greater inidene of large-for-gestational-age infants in patients with type 1 diabetes.
17 2050 Position Statement Diabetes Care As most pregnanies are unplanned, onsider the potential risks and benefits of mediations that are ontraindiated in pregnany in all adolesents and women of hildbearing potential and ounsel women using suh mediations aordingly. (E) Suh mediations should be evaluated prior to oneption, as drugs ommonlyusedtotreatdiabetes and its ompliations may be ontraindiated or not reommended in pregnany, inluding statins, ACE inhibitors, angiotensin reeptor blokers, and most noninsulin therapies. (B) Prenatal vitamins with folate should be started with preoneption planning to redue the risk for birth defets. (B) All pregnant women with type 1 diabetes should be sreened for thyroid disease early in pregnany. (B) Women ontemplating pregnany should be evaluated and, if indiated, treated for diabeti retinopathy, nephropathy, neuropathy, and CVD. (B) A1C levels should be as lose to normal as possible (,7%) before oneption is attempted. (B) Nutritional intake should be optimized and inluded in preoneption planning aording to general pregnany guidelines. (E) Inpatient Management and Outpatient Proedures Management of individuals with type 1 diabetes in the hospital and in preparation for sheduled outpatient proedures often differs from that of individuals with type 2 diabetes. The hallenges inlude diffiulties assoiated with fasting, maintaining a onsistent soure of arbohydrate, and failitating inpatient blood gluose management while modifying sheduled insulin therapy. Outpatient proedures should be performed with the awareness that individuals with type 1 diabetes may have diffiulty fasting for long periods of time (more than 10 h) prior to a proedure. Patients with type 1 diabetes should be prepared with a treatment plan for insulin dose adjustments and oral gluose intake prior to any proedure that requires alterations in dietary intake and/ or fasting. It is imperative that the entire health are team, inluding anesthesiologists and surgeons as well as other speialists who perform proedures, understands type 1 diabetes and how it fators into the omprehensive delivery of are. From a pratial perspetive, this means that people with type 1 diabetes will be at high risk for hypoglyemia during prolonged fasting and are at risk for ketosis if insulin is inappropriately withheld. One under anesthesia, individuals with type 1 diabetes must be arefully monitored for hypoglyemia and hyperglyemia. For some individuals, one the most aute phase of an illness has resolved or improved, patients may be able to self-administer their prior multipledose or CSII insulin regimen under the guidane of hospital personnel who are knowledgeable in glyemi management. Individuals managed with insulin pumps and/or multiple-dose regimens with arbohydrate ounting and orretion dosing may be allowed to manage their own diabetes if this is what they desire, one they are apable of doing so. All patients admitted to the hospital should have type 1 diabetes learly identified in the medial reord. (E) SMBG should be ordered to fit the patient s usual insulin regimen with modifiations as needed based on linial status. (E) Goals for blood gluose levels are the same as for people with type 2 diabetes or hospital-related hyperglyemia. (E) A plan for preventing and treating hypoglyemia should be established for eah patient. (E) Insulin dosing adjustments should be made in the perioperative period and inpatient setting with onsideration of hanges in oral intake, reent blood gluose trends, and the need for uninterrupted basal insulin to prevent hyperglyemia and ketoaidosis, with adjustment of the long-ating insulin or basal insulin requirement to reflet true basal requirements, insofar as they may be antiipated. (B) Child Care and Shools Beause a large portion of a hild s day may be spent in shool and/or in the hild are setting, lose ommuniation with and ooperation of the shool or day are personnel is essential for optimal diabetes management, safety, and maximal aademi opportunities. Child are personnel and shool staff should reeive training to provide diabetes are in the absene of a shool nurse or liensed health are professional. Able and willing shool staff members should be taught the priniples of diabetes management and trained to provide needed are for the hild aording to the ADA s Safe at Shool program (see the ADA position statement on diabetes are in the shool and day are setting [106] for further disussion). Young hildren often lak the motor, ognitive, and ommuniation skills and abilities to manage their diabetes and ompletely depend on adult aregivers. The management priority for younger hildren is the prevention, reognition, and treatment of hypoglyemia and marked hyperglyemia. Students with diabetes should reeive proper diabetes management in shool, with as little disruption to the shool and hild s routineaspossible. Whenever possible, the student should have the opportunity to selfmanage by performing blood gluose monitoring, using CGM (if utilized), administering insulin, having aess to meals/snaks, managing hypoglyemia (with trained personnel prepared to provide gluagon treatment, if required) and hyperglyemia, and partiipating fully in all shool-sponsored ativities (Table 9). Camps A diabetes amp is an ideal plae for hildren and youth to have an enjoyable amp experiene and reeive peer support from other hildren with diabetes under lose medial oversight. The goals for ampers are to learn to ope more effetively with diabetes, learn self-management skills to gain more independene, and share experienes with other young people with diabetes. The amp medial diretor is responsible for the diabetes management of the hildren. A registered dietitian oversees dietary planning at amp. Medial diretors and staff should have expertise in managing type 1 diabetes and must reeive training onerning routine diabetes management and treatment of diabetes-related emergenies at amp. Staff must follow universal preautions inluding Oupational Safety
18 are.diabetesjournals.org Chiang and Assoiates 2051 Table 9 Diabetes are tasks for shool personnel Diabetes are tasks Signs* Treatment Outome if not treated Hypoglyemia reognition and treatment Hyperglyemia reognition and treatment Cateholamine effet (sweating, jitteriness, tahyardia, and palpitations) or neuroglyopenia (behavior hange) Polyuria, polydipsia (most ommon), diffiulty onentrating, headahe, or irritability Gluose, wait 15 min, rehek, give food if blood gluose is adequate (based on DMMP) Know when and how to give gluagon Know when to ontat parents or emergeny medial servies Have all ontat information available on emergeny plan Rapid- or short-ating insulin Dose and frequeny should be learly eluidated on emergeny plan to avoid insulin staking and onsequent hypoglyemia (DMMP) Insulin dosing tehnique (syringe/vial, pens, pumps) Insulin required (DMMP) Ketone heks and when to all parents Corretion fator alulations and insulin for hyperglyemia and ketones DMMP, Diabetes Medial Management Plan. *Varies among individuals but onsistent within a given hild. Seizure or oma Chek for ketones. Follow diretions for ketones if positive to avoid ketoaidosis and Health Administration (OSHA) regulations, Clinial Laboratory Improvement Amendments (CLIA) standards, and state regulations (107). Diabetes in the Workplae There are pratial and legal issues related to diabetes in the workplae. Employers and employees with diabetes should work together to find solutions and eduate themselves about the rights of individuals with diabetes. Individuals with diabetes are responsible for having all neessary diabetes supplies, eating properly, and being aware of safety issues and regulations at work. The Amerians with Disabilities At states that most employers must provide reasonable aommodations to allow an individual with diabetes to safely and suessfully perform a job, unless doing so would plae an undue burden on the employer. We refer the reader to ADA position statement on diabetes and employment for additional information (108) and to the relevant setion of the Amerian Diabetes Assoiation/JDRF Type 1 Diabetes Sourebook (70). Older Adults Older individuals with type 1 diabetes are unique in that they have lived for many years with a omplex disease. Not all older adults are alike: some may ontinue a rigorous regimen, with tighter ontrol, while others may require less stringent targets. Along with age-related onditions, older adults may develop diabetes-related ompliations, whih make managing type 1 diabetes more hallenging. Providers should be aware that insulin dosing errors, meal planning, and physial ativities must be properly managed in older adults. Severe hyperglyemia an lead to symptoms of dehydration and hyperglyemi rises. While hroni hyperglyemia is detrimental, hypoglyemia may be more of a onern in some older adults. Delining ognition may ontribute to hypoglyemia unawareness or the inability to safely manage hypoglyemia when it ours. An individualized approah that inludes the reassessment of prior targets may be warranted. We refer the reader to the ADA onsensus report Diabetes in Older Adults (54). Even though this report fouses primarily on the type 2 diabeti population, there is signifiant overlap in the omorbidities and ompliations experiened by the older type 1 and type 2 diabeti populations. Speial Population Groups Although type 1 diabetes is inreasing in several ethni and raial groups, it remains less ommon in people of non- European desent. A better understanding of the unique pathophysiology of type 1 diabetes is needed. In addition, multidisiplinary diabetes teams should reeive training to properly address the diverse ultural needs of these populations and to optimize health are delivery, improve glyemi ontrol, and prevent ompliations. Additionally, there is a need for approahes to redue health disparities and improve outomes in raial/ethni minorities and in the underserved population with type 1 diabetes (70). Developing Countries: The Global Epidemi Type 1 diabetes is an inreasing global publi health burden. The demands of daily management, hroniity of the disease, potential ompliations, pauity of diabetes speialists, and rising inidene are hallenging in the U.S., but these issues, inluding the onsiderable ost of management, are rippling for those in the developing world. International organizations play a major role in improving are for individuals with type 1 diabetes in the developing world, but implementable, ost-saving, and sustainable strategies are needed to make suh programs suessful (70).
19 2052 Position Statement Diabetes Care Aknowledgments. The authors thank the following ontributors to the Amerian Diabetes Assoiation/JDRF Type 1 Diabetes Sourebook: Nora Algothani, Pamela Allweiss, Barbara J. Anderson, Florene M. Brown, H. Peter Chase, William L. Clarke, Sheri R. Colberg, Kathleen Dungan, Steven Edelman, Martha M. Funnell, Stephen E. Gitelman, Ann E. Goebel- Fabbri, Jeffrey S. Gonzalez, Carla J. Greenbaum, Mihael J. Haller, Kara Hawkins, Laurie A. Higgins, Irl B. Hirsh, William C. Hsu, Heba Ismail, Crystal Crismond Jakson, Tamarra James-Todd, Georgeanna J. Klingensmith, David C. Klonoff, Mary Korytkowski, David Maahs, Hussain Mahmud, Medha N. Munshi, Trevor Orhard, Brue A. Perkins, Jeremy Hodson Pettus, Andrew M. Posselt, Mihael C. Riddell, Elizabeth R. Seaquist, Janet Silverstein, Linda M. Siminerio, Peter Stok, William V. Tamborlane, Guillermo E. Umpierrez, Raynard Washington, Joseph I. Wolfsdorf, Howard Wolpert, Jennifer Ann Wykoff, and Mary Ziotas Zaharatos. The authors aknowledge Gordon Weir and the Steering Committee members: Belinda Childs, Rihard A. Insel, Margaret A. Powers, Rihard Rubin, Desmond Shatz, and Linda M. Siminerio. The authors also thank Erika Gebel Berg (Amerian Diabetes Assoiation) for her invaluable editorial ontribution. Duality of Interest. M.S.K. reeived researh support from Novo Nordisk (to the University of North Carolina) for a study of an investigational drug for type 1 diabetes. In , L.M.B.L. reeived grant support from Bayer Diabetes Care; served as a onsultant/advisory board member for Bristol-Myers Squibb/AstraZenea, Sanofi, Novo Nordisk, and Boehringer Ingelheim; and served as a onsultant for Johnson & Johnson, LifeSan/Animas, Lilly, Menarini, and Dexom. In the past year, A.L.P. onsulted with Abbott Diabetes Care, BD, Janssen, Lilly, Medsape, Medtroni MiniMed, Novo Nordisk, Sanofi, and Takeda; has been on the speaker s bureau for Bristol-Myers Squibb/AstraZenea and Novo Nordisk; and reeived grant funding from the Medtroni MiniMed Foundation. No other potential onflits of interest relevant to this artile were reported. Referenes 1. Prime Group for JDRF. Type 1 Diabetes, JDRF, Lawrene JM, Imperatore G, Pettitt DJ, et al.; SEARCH for Diabetes in Youth Study Group. Inidene of diabetes in U.S. youth by type, rae/ ethniity, and age, Diabetes 2014; 63(Suppl. 1):A Harjutsalo V, Sjöberg L, Tuomilehto J. Time trends in the inidene of type 1 diabetes in Finnish hildren: a ohort study. Lanet 2008; 371: Pettitt DJ, Talton J, Dabelea D, et al.; SEARCH for Diabetes in Youth Study Group. Prevalene of diabetes in U.S. youth in 2009: the SEARCH for Diabetes in Youth study. Diabetes Care 2014; 37: Hawa MI, Kolb H, Shloot N, et al.; Ation LADA onsortium. Adult-onset autoimmune diabetes in Europe is prevalent with a broad linial phenotype: Ation LADA 7. Diabetes Care 2013;36: Miller RG, Serest AM, Sharma RK, Songer TJ, Orhard TJ. Improvements in the life expetany of type 1 diabetes: the Pittsburgh Epidemiology of Diabetes Compliations study ohort. Diabetes 2012;61: Sottish Diabetes Researh Network Epidemiology Group. Life expetany in type 1 diabetes: a Sottish Registry Linkage Study [Internet], Availablefrom resoures/3906. Aessed 9 April Davis A, Haller MJ, Miller K, et al. Residual C-peptide in patients 3-81 years from diagnosis of T1D: A T1D Exhange Study. Diabetes 2013; 62(Suppl. 1):A Klingensmith GJ, Pyle L, Arslanian S, et al.; TODAY Study Group. The presene of GAD and IA-2 antibodies in youth with a type 2 diabetes phenotype: results from the TODAY study. Diabetes Care 2010;33: Wenzlau JM, Juhl K, Yu L, et al. The ation efflux transporter ZnT8 (Sl30A8) is a major autoantigen in human type 1 diabetes. Pro Natl Aad Si USA 2007;104: Todd AL, Ng WY, Lui KF, Thai AC. Low prevalene of autoimmune diabetes markers in a mixed ethni population of Singaporean diabetis. Intern Med J 2004;34: Thai AC, Ng WY, Loke KY, Lee WR, Lui KF, Cheah JS. Anti-GAD antibodies in Chinese patients with youth and adult-onset IDDM and NIDDM. Diabetologia 1997;40: Ly LD, Twigg SM, Tran DT, Nguyen KT. Most type 1 diabetes presenting as diabeti ketoaidosis in Vietnamese people is negative for panreati islet ell autoantibodies. Diabetes Res Clin Prat 2012;96:e63 e Tuomi T, Zimmet P, Rowley MJ, et al. Differing frequeny of autoantibodies to glutami aid dearboxylase among Koreans, Thais, and Australians with diabetes mellitus. Clin Immunol Immunopathol 1995;74: Chan JC, Yeung VT, Chow CC, et al. Panreati beta ell funtion and antibodies to glutami aid dearboxylase (anti-gad) in Chinese patients with linial diagnosis of insulin-dependent diabetes mellitus. Diabetes Res Clin Prat 1996;32: Tridgell DM, Spiekerman C, Wang RS, Greenbaum CJ. Interation of onset and duration of diabetes on the perent of GAD and IA-2 antibody positive subjets in the Type 1 Diabetes Genetis Consortium Database. Diabetes Care 2011;34: Bonifaio E, Ziegler AG. Advanes in the predition and natural history of type 1 diabetes. Endorinol Metab Clin North Am 2010;39: Tuomilehto J. The emerging global epidemi of type 1 diabetes. Curr Diab Rep 2013; 13: Ziegler AG, Rewers M, Simell O, et al. Seroonversion to multiple islet autoantibodies and risk of progression to diabetes in hildren. JAMA 2013;309: Peters A, Laffel L; Amerian Diabetes Assoiation Transitions Working Group. Diabetes are for emerging adults: reommendations for transition from pediatri to adult diabetes are systems: a position statement of the Amerian Diabetes Assoiation, with representation by the Amerian College of Osteopathi Family Physiians, the Amerian Aademy of Pediatris, the Amerian Assoiation of Clinial Endorinologists, the Amerian Osteopathi Assoiation, the Centers for Disease Control and Prevention, Children with Diabetes, The Endorine Soiety, the International Soiety for Pediatri and Adolesent Diabetes, Juvenile Diabetes Researh Foundation International, the National Diabetes Eduation Program, and the Pediatri Endorine Soiety (formerly Lawson Wilkins Pediatri Endorine Soiety). Diabetes Care 2011;34: Holmes GK. Coelia disease and type 1 diabetes mellitus - the ase for sreening. Diabet Med 2001;18: Rewers M, Liu E, Simmons J, Redondo MJ, Hoffenberg EJ. Celia disease assoiated with type 1 diabetes mellitus. Endorinol Metab Clin North Am 2004;33: Husby S, Koletzko S, Korponay-Szabó IR, et al.; ESPGHAN Working Group on Coelia Disease Diagnosis; ESPGHAN Gastroenterology Committee; European Soiety for Pediatri Gastroenterology, Hepatology, and Nutrition. European Soiety for Pediatri Gastroenterology, Hepatology, and Nutrition guidelines for the diagnosis of oelia disease. J Pediatr Gastroenterol Nutr 2012;54: Abid N, MGlone O, Cardwell C, MCallion W, Carson D. Clinial and metaboli effets of gluten free diet in hildren with type 1 diabetes and oelia disease. Pediatr Diabetes 2011;12: Roldán MB, Alonso M, Barrio R. Thyroid autoimmunity in hildren and adolesents with type 1 diabetes mellitus. Diabetes Nutr Metab 1999;12: Triolo TM, Armstrong TK, MFann K, et al. Additional autoimmune disease found in 33% of patients at type 1 diabetes onset. Diabetes Care 2011;34: Kordonouri O, Deiss D, Danne T, Dorow A, Bassir C, Grüters-Kieslih A. Preditivity of thyroid autoantibodies for the development of thyroid disorders in hildren and adolesents with type 1 diabetes. Diabet Med 2002;19: Mohn A, Di Mihele S, Di Luzio R, Tumini S, Chiarelli F. The effet of sublinial hypothyroidism on metaboli ontrol in hildren and adolesents with type 1 diabetes mellitus. Diabet Med 2002;19: Chase HP, Garg SK, Cokerham RS, Wilox WD, Walravens PA. Thyroid hormone replaement and growth of hildren with sublinial hypothyroidism and diabetes. Diabet Med 1990;7: Cho YH, Craig ME, Hing S, et al. Mirovasular ompliations assessment in adolesents with 2- to 5-yr duration of type 1 diabetes from 1990 to Pediatr Diabetes 2011;12: Haas L, Maryniuk M, Bek J, et al. National Standards for Diabetes Self-Management Eduation and Support. Diabetes Care 2014;37 (Suppl.1):S144 S Wolpert HA, Atakov-Castillo A, Smith SA, Steil GM. Dietary fat autely inreases gluose onentrations and insulin requirements in patients with type 1 diabetes: impliations for arbohydrate-based bolus dose alulation and intensive diabetes management. Diabetes Care 2013;36: Riddell MC, Perkins BA. Type 1 diabetes and vigorous exerise: appliations of exerise
20 are.diabetesjournals.org Chiang and Assoiates 2053 physiology to patient management. Can J Diabetes 2006;30: Robertson K, Adolfsson P, Sheiner G, Hanas R, Riddell MC. Exerise in hildren and adolesents with diabetes. Pediatr Diabetes 2009;10(Suppl. 12): Galassetti P, Riddell MC. Exerise and type 1 diabetes (T1DM). In Comprehensive Physiology, John Wiley & Sons, In., Available from phy /abstrat. Aessed 27 Marh MMahon SK, Ferreira LD, Ratnam N, et al. Gluose requirements to maintain euglyemia after moderate-intensity afternoon exerise in adolesents with type 1 diabetes are inreased in a biphasi manner. J Clin Endorinol Metab 2007;92: Tsalikian E, Mauras N, Bek RW, et al.; Diabetes Researh in Children Network DireNet Study Group. Impat of exerise on overnight glyemi ontrol in hildren with type 1 diabetes mellitus. J Pediatr 2005;147: Tsalikian E, Kollman C, Tamborlane WB, et al.; Diabetes Researh in Children Network (DireNet) Study Group. Prevention of hypoglyemia during exerise in hildren with type 1 diabetes by suspending basal insulin. Diabetes Care 2006;29: Taplin CE, Cobry E, Messer L, MFann K, Chase HP, Fiallo-Sharer R. Preventing postexerise noturnal hypoglyemia in hildren with type 1 diabetes. J Pediatr 2010;157: e1 40. U.S. Department of Health and Human Servies Physial Ativity Guidelines for Amerians [Internet], Available from guidelines. Aessed 8 April Garber CE, Blissmer B, Deshenes MR, et al.; Amerian College of Sports Mediine. Amerian College of Sports Mediine position stand. Quantity and quality of exerise for developing and maintaining ardiorespiratory, musuloskeletal, and neuromotor fitness in apparently healthy adults: guidane for presribing exerise. Med Si Sports Exer 2011;43: Amerian Diabetes Assoiation. Standards of Medial Care in Diabetesd2014. Diabetes Care 2014;37(Suppl. 1):S14 S The Diabetes Control and Compliations Trial Researh Group. The effet of intensive treatment of diabetes on the development and progression of long-term ompliations in insulin-dependent diabetes mellitus. N Engl J Med 1993;329: The Diabetes Control and Compliations Trial/Epidemiology of Diabetes Interventions and Compliations Researh Group. Retinopathy and nephropathy in patients with type 1 diabetes four years after a trial of intensive therapy. N Engl J Med 2000;342: Martin CL, Albers J, Herman WH, et al.; DCCT/EDIC Researh Group. Neuropathy among the diabetes ontrol and ompliations trial ohort 8 years after trial ompletion. Diabetes Care 2006;29: Rovet JF, Ehrlih RM. The effet of hypoglyemi seizures on ognitive funtion in hildren with diabetes: a 7-year prospetive study. J Pediatr 1999;134: Krolewski AS, Warram JH, Christlieb AR, Busik EJ, Kahn CR. The hanging natural history of nephropathy in type I diabetes. Am J Med 1985;78: Kostraba JN, Dorman JS, Orhard TJ, et al. Contribution of diabetes duration before puberty to development of mirovasular ompliations in IDDM subjets. Diabetes Care 1989; 12: Cato MA, Mauras N, Ambrosino J, et al.; Diabetes Researh in Children Network (DireNet). Cognitive funtioning in young hildren with type 1 diabetes. J Int Neuropsyhol So 2014;20: Marzelli MJ, Mazaika PK, Barnea-Goraly N, et al.; Diabetes Researh in Children Network (DireNet). Neuroanatomial orrelates of dysglyemia in young hildren with type 1 diabetes. Diabetes 2014;63: Donaghue KC, Fairhild JM, Craig ME, et al. Do all prepubertal years of diabetes duration ontribute equally to diabetes ompliations? Diabetes Care 2003;26: KirhhoffBA,LugarHM,SmithSE,etal. Hypoglyaemia-indued hanges in regional brain volume and memory funtion. Diabet Med 2013;30:e151 e Barnea-Goraly N, Raman M, Mazaika P, et al.; Diabetes Researh in Children Network (DireNet). Alterations in white matter struture in young hildren with type 1 diabetes. Diabetes Care 2014;37: Kirkman MS, Brisoe VJ, Clark N, et al. Diabetes in older adults. Diabetes Care 2012;35: Miller KM, Bek RW, Bergenstal RM, et al.; T1D Exhange Clini Network. Evidene of a strong assoiation between frequeny of selfmonitoring of blood gluose and hemoglobin A1 levels in T1D Exhange lini registry partiipants. Diabetes Care 2013;36: Ziegler R, Heidtmann B, Hilgard D, Hofer S, Rosenbauer J, Holl R; DPV-Wiss-Initiative. Frequeny of SMBG orrelates with HbA1 and aute ompliations in hildren and adolesents with type 1 diabetes. Pediatr Diabetes 2011;12: Saks DB, Arnold M, Bakris GL, et al.; National Aademy of Clinial Biohemistry; Evidene-Based Laboratory Mediine Committee of the Amerian Assoiation for Clinial Chemistry. Guidelines and reommendations for laboratory analysis in the diagnosis and management of diabetes mellitus. Diabetes Care 2011;34:e61 e Tamborlane WV, Bek RW, Bode BW, et al.; Juvenile Diabetes Researh Foundation Continuous Gluose Monitoring Study Group. Continuous gluose monitoring and intensive treatment of type 1 diabetes. N Engl J Med 2008;359: Yeh H-C, Brown TT, Maruthur N, et al. Comparative effetiveness and safety of methods of insulin delivery and gluose monitoring for diabetes mellitus: a systemati review and meta-analysis. Ann Intern Med 2012; 157: Bergenstal RM, Klonoff DC, Garg SK, et al.; ASPIRE In-Home Study Group. Threshold-based insulin-pump interruption for redution of hypoglyemia. N Engl J Med 2013;369: Stratton IM, Adler AI, Neil HAW, et al. Assoiation of glyaemia with marovasular and mirovasular ompliations of type 2 diabetes (UKPDS 35): prospetive observational study. BMJ 2000;321: Jovanovič L, Savas H, Mehta M, Trujillo A, Pettitt DJ. Frequent monitoring of A1C during pregnany as a treatment tool to guide therapy. Diabetes Care 2011;34: Nathan DM, Cleary PA, Baklund JY, et al.; Diabetes Control and Compliations Trial/Epidemiology of Diabetes Interventions and Compliations (DCCT/EDIC) Study Researh Group. Intensive diabetes treatment and ardiovasular disease in patients with type 1 diabetes. N Engl J Med 2005;353: Rosenstok J, Dailey G, Massi-Benedetti M, Fritshe A, Lin Z, Salzman A. Redued hypoglyemia risk with insulin glargine: a meta-analysis omparing insulin glargine with human NPH insulin in type 2 diabetes. Diabetes Care 2005;28: DeWitt DE, Dugdale DC. Using new insulin strategies in the outpatient treatment of diabetes: linial appliations. JAMA 2003;289: Bergenstal RM, Tamborlane WV, Ahmann A, et al.; STAR 3 Study Group. Effetiveness of sensor-augmented insulin-pump therapy in type 1 diabetes. N Engl J Med 2010;363: Wood JR, Miller KM, Maahs DM, et al.; T1D Exhange Clini Network. Most youth with type 1 diabetes in the T1D Exhange lini registry do not meet Amerian Diabetes Assoiation or International Soiety for Pediatri and Adolesent Diabetes linial guidelines. Diabetes Care 2013; 36: Kmietowiz Z. Insulin pumps improve ontrol and redue ompliations in hildren with type 1 diabetes. BMJ 2013;347:f Phillip M, Battelino T, Atlas E, et al. Noturnal gluose ontrol with an artifiial panreas at a diabetes amp. N Engl J Med 2013;368: Peters AL, Laffel L (Eds.). Amerian Diabetes Assoiation/JDRF Type 1 Diabetes Sourebook. Alexandria, VA, Amerian Diabetes Assoiation, Gruessner AC update on panreas transplantation: omprehensive trend analysis of 25,000 ases followed up over the ourse of twenty-four years at the International Panreas Transplant Registry (IPTR). Rev Diabet Stud 2011;8: Fioretto P, Steffes MW, Sutherland DER, Goetz FC, Mauer M. Reversal of lesions of diabeti nephropathy after panreas transplantation. N Engl J Med 1998;339: Gruessner RWG, Gruessner AC. Panreas transplant alone: a proedure oming of age. Diabetes Care 2013;36: Barton FB, Rikels MR, Alejandro R, et al. Improvement in outomes of linial islet transplantation: Diabetes Care 2012;35: Pagliua FW, Melton DA. How to make a funtional b-ell. Development 2013;140: Pepper AR, Gala-Lopez B, Ziff O, Shapiro AJ. Current status of linial islet transplantation. World J Transplant 2013;3: Whitehouse F, Kruger DF, Fineman M, et al. A randomized study and open-label extension evaluating the long-term effiay of pramlintide as an adjunt to insulin therapy
21 2054 Position Statement Diabetes Care in type 1 diabetes. Diabetes Care 2002;25: Ratner RE, Dikey R, Fineman M, et al. Amylin replaement with pramlintide as an adjunt to insulin therapy improves long-term glyaemi and weight ontrol in type 1 diabetes mellitus: a 1-year, randomized ontrolled trial. Diabet Med 2004;21: Vella S, Buetow L, Royle P, Livingstone S, Colhoun HM, Petrie JR. The use of metformin in type 1 diabetes: a systemati review of effiay. Diabetologia 2010;53: Hopkins D, Lawrene I, Mansell P, et al. Improved biomedial and psyhologial outomes 1 year after strutured eduation in flexible insulin therapy for people with type 1 diabetes: the U.K. DAFNE experiene. Diabetes Care 2012; 35: Seaquist ER, Anderson J, Childs B, et al. Hypoglyemia and diabetes: a report of a workgroup of the Amerian Diabetes Assoiation and The Endorine Soiety. Diabetes Care 2013;36: Cryer PE, Davis SN, Shamoon H. Hypoglyemia in diabetes. Diabetes Care 2003;26: Orhard TJ, Costaou T, Kretowski A, Nesto RW. Type 1 diabetes and oronary artery disease. Diabetes Care 2006;29: Kitabhi AE, Umpierrez GE, Miles JM, Fisher JN. Hyperglyemi rises in adult patients with diabetes. Diabetes Care 2009;32: Stone NJ, Robinson J, Lihtenstein AH, et al ACC/AHA guideline on the treatment of blood holesterol to redue atherosleroti ardiovasular risk in adults: a report of the Amerian College of Cardiology/Amerian Heart Assoiation Task Fore on Pratie Guidelines. J Am Coll Cardiol. 7 November 2013 [Epub ahead of print] 86. Cleary PA, Orhard TJ, Genuth S, et al.; DCCT/EDIC Researh Group. The effet of intensive glyemi treatment on oronary artery alifiation in type 1 diabeti partiipants of the Diabetes Control and Compliations Trial/ Epidemiology of Diabetes Interventions and Compliations (DCCT/EDIC) Study. Diabetes 2006;55: Collins R, Armitage J, Parish S, Sleigh P, Peto R; Heart Protetion Study Collaborative Group. MRC/BHF Heart Protetion Study of holesterol-lowering with simvastatin in 5963 people with diabetes: a randomised plaebo-ontrolled trial. Lanet 2003;361: Gunton JE, Morris J, Boye S, Kelso I, MElduff A. Outome of pregnany ompliated by pre-gestational diabetesdimprovement in outomes. Aust N Z J Obstet Gynaeol 2002; 42: Jensen DM, Damm P, Moelsted-Pedersen L, et al. Outomes in type 1 diabeti pregnanies: a nationwide, population-based study. Diabetes Care 2004;27: Steel JM, Johnstone FD, Hepburn DA, Smith AF. Can prepregnany are of diabeti women redue the risk of abnormal babies? BMJ 1990; 301: Willhoite MB, Bennert HW Jr, Palomaki GE, et al. The impat of preoneption ounseling on pregnany outomes. The experiene of the Maine Diabetes in Pregnany Program. Diabetes Care 1993;16: Kitzmiller JL, Gavin LA, Gin GD, Jovanovi- Peterson L, Main EK, Zigrang WD. Preoneption are of diabetes: glyemi ontrol prevents ongenital anomalies. JAMA 1991;265: MElvy SS, Miodovnik M, Rosenn B, et al. A foused preoneptional and early pregnany program in women with type 1 diabetes redues perinatal mortality and malformation rates to general population levels. J Matern Fetal Med 2000;9: Ray JG, O Brien TE, Chan WS. Preoneption are and the risk of ongenital anomalies in the offspring of women with diabetes mellitus: a meta-analysis. QJM 2001;94: Evers IM, de Valk HW, Visser GHA. Risk of ompliations of pregnany in women with type 1 diabetes: nationwide prospetive study in the Netherlands. BMJ 2004;328: Wahabi HA, Alzeidan RA, Bawazeer GA, Alansari LA, Esmaeil SA. Preoneption are for diabeti women for improving maternal and fetal outomes: a systemati review and metaanalysis. BMC Pregnany Childbirth 2010;10: Murphy HR, Roland JM, Skinner TC, et al. Effetiveness of a regional prepregnany are program in women with type 1 and type 2 diabetes: benefits beyond glyemi ontrol. Diabetes Care 2010;33: Jonasson JM, Brismar K, Sparén P, et al. Fertility in women with type 1 diabetes: a populationbased ohort study in Sweden. Diabetes Care 2007;30: Snell-Bergeon JK, Dabelea D, Ogden LG, et al. Reprodutive history and hormonal birth ontrol use are assoiated with oronary alium progression in women with type 1 diabetes mellitus. J Clin Endorinol Metab 2008;93: Whitworth KW, Baird DD, Stene LC, Skjaerven R, Longneker MP. Feundability among women with type 1 and type 2 diabetes in the Norwegian Mother and Child Cohort Study. Diabetologia 2011;54: Amerian Diabetes Assoiation. Medial Management of Type 1 Diabetes. Alexandria, VA, Amerian Diabetes Assoiation, Garía-Patterson A, Gih I, Amini SB, Catalano PM, de Leiva A, Coroy R. Insulin requirements throughout pregnany in women with type 1 diabetes mellitus: three hanges of diretion. Diabetologia 2010;53: Kitzmiller JL, Jovanovi L, Brown F, Coustan D, Reader DM (Eds.). Managing Preexisting Diabetes and Pregnany: Tehnial Reviews and Consensus for Care. Alexandria, VA, Amerian Diabetes Assoiation, Kitzmiller JL, Blok JM, Brown FM, et al. Managing preexisting diabetes for pregnany: summary of evidene and onsensus reommendations for are. Diabetes Care 2008;31: Perros P, MCrimmon RJ, Shaw G, Frier BM. Frequeny of thyroid dysfuntion in diabeti patients: value of annual sreening. Diabet Med 1995;12: Amerian Diabetes Assoiation. Diabetes are in the shool and day are setting. Diabetes Care 2006;29(Suppl. 1):S49 S Amerian Diabetes Assoiation. Diabetes management at amps for hildren with diabetes. Diabetes Care 2012;35(Suppl. 1):S72 S Amerian Diabetes Assoiation. Diabetes and employment. Diabetes Care 2011;34(Suppl. 1):S82 S86
T he American Diabetes Association
 Introdution T he Amerian Diabetes Assoiation (ADA) has been atively involved in the development and dissemination of diabetes are standards, guidelines, and related douments for many years. These statements
Introdution T he Amerian Diabetes Assoiation (ADA) has been atively involved in the development and dissemination of diabetes are standards, guidelines, and related douments for many years. These statements
Diabetes Management in Correctional Institutions
 S104 Diabetes Care Volume 37, Supplement 1, January 2014 Diabetes Management in Corretional Institutions Amerian Diabetes Assoiation POSITION STATEMENT At any given time, over 2 million people are inarerated
S104 Diabetes Care Volume 37, Supplement 1, January 2014 Diabetes Management in Corretional Institutions Amerian Diabetes Assoiation POSITION STATEMENT At any given time, over 2 million people are inarerated
Standards of Medical Care in Diabetes 2015
 January 2015 Volume 38, Supplement 1 Standards of Medial Care in Diabetes 2015 S1 S3 S4 S5 S8 Introdution Professional Pratie Committee Standards of Medial Care in Diabetes 2015: Summary of Revisions 1.
January 2015 Volume 38, Supplement 1 Standards of Medial Care in Diabetes 2015 S1 S3 S4 S5 S8 Introdution Professional Pratie Committee Standards of Medial Care in Diabetes 2015: Summary of Revisions 1.
MEDICATION MANAGEMENT ASSESSMENT
 MEDICATION MANAGEMENT ASSESSMENT The Mediation Management Assessment provides evidene-based reommendations/standards for Minnesota hospitals in the development of a omprehensive mediation safety program.
MEDICATION MANAGEMENT ASSESSMENT The Mediation Management Assessment provides evidene-based reommendations/standards for Minnesota hospitals in the development of a omprehensive mediation safety program.
Henley Business School at Univ of Reading. Pre-Experience Postgraduate Programmes Chartered Institute of Personnel and Development (CIPD)
 MS in International Human Resoure Management For students entering in 2012/3 Awarding Institution: Teahing Institution: Relevant QAA subjet Benhmarking group(s): Faulty: Programme length: Date of speifiation:
MS in International Human Resoure Management For students entering in 2012/3 Awarding Institution: Teahing Institution: Relevant QAA subjet Benhmarking group(s): Faulty: Programme length: Date of speifiation:
State of Maryland Participation Agreement for Pre-Tax and Roth Retirement Savings Accounts
 State of Maryland Partiipation Agreement for Pre-Tax and Roth Retirement Savings Aounts DC-4531 (08/2015) For help, please all 1-800-966-6355 www.marylandd.om 1 Things to Remember Complete all of the setions
State of Maryland Partiipation Agreement for Pre-Tax and Roth Retirement Savings Aounts DC-4531 (08/2015) For help, please all 1-800-966-6355 www.marylandd.om 1 Things to Remember Complete all of the setions
Board Building Recruiting and Developing Effective Board Members for Not-for-Profit Organizations
 Board Development Board Building Reruiting and Developing Effetive Board Members for Not-for-Profit Organizations Board Development Board Building Reruiting and Developing Effetive Board Members for Not-for-Profit
Board Development Board Building Reruiting and Developing Effetive Board Members for Not-for-Profit Organizations Board Development Board Building Reruiting and Developing Effetive Board Members for Not-for-Profit
Henley Business School at Univ of Reading. Chartered Institute of Personnel and Development (CIPD)
 MS in International Human Resoure Management (full-time) For students entering in 2015/6 Awarding Institution: Teahing Institution: Relevant QAA subjet Benhmarking group(s): Faulty: Programme length: Date
MS in International Human Resoure Management (full-time) For students entering in 2015/6 Awarding Institution: Teahing Institution: Relevant QAA subjet Benhmarking group(s): Faulty: Programme length: Date
STANDARDS OF MEDICAL CARE IN DIABETES 2015
 TH E JO U R NA L OF C LI N ICA L A N D A PPL I ED R ESEA RC H A N D EDU CATI O N VOLUME 38 SUPPLEMENT 1 WWW.DIABETES.ORG/DIABETESCARE PP LEME T 1 N SU JANUARY 2015 A M E R I C A N D I A B E T E S A S S
TH E JO U R NA L OF C LI N ICA L A N D A PPL I ED R ESEA RC H A N D EDU CATI O N VOLUME 38 SUPPLEMENT 1 WWW.DIABETES.ORG/DIABETESCARE PP LEME T 1 N SU JANUARY 2015 A M E R I C A N D I A B E T E S A S S
Effectiveness of a law to reduce alcohol-impaired driving in Japan
 Effetiveness of a law to redue alohol-impaired driving in Japan T Nagata, 1,2 S Setoguhi, 3 D Hemenway, 4 M J Perry 5 Original artile 1 Takemi Program, Department of International Health, Harvard Shool
Effetiveness of a law to redue alohol-impaired driving in Japan T Nagata, 1,2 S Setoguhi, 3 D Hemenway, 4 M J Perry 5 Original artile 1 Takemi Program, Department of International Health, Harvard Shool
A Holistic Method for Selecting Web Services in Design of Composite Applications
 A Holisti Method for Seleting Web Servies in Design of Composite Appliations Mārtiņš Bonders, Jānis Grabis Institute of Information Tehnology, Riga Tehnial University, 1 Kalu Street, Riga, LV 1658, Latvia,
A Holisti Method for Seleting Web Servies in Design of Composite Appliations Mārtiņš Bonders, Jānis Grabis Institute of Information Tehnology, Riga Tehnial University, 1 Kalu Street, Riga, LV 1658, Latvia,
Florida Blue has got you covered. Choose your plan. Choose your network.
 overed. Choose your plan. Choose your network. When it omes to your health are overage, you an ount on us. attention and extra support are part of every plan. You hoose features that are most important
overed. Choose your plan. Choose your network. When it omes to your health are overage, you an ount on us. attention and extra support are part of every plan. You hoose features that are most important
A Comparison of Service Quality between Private and Public Hospitals in Thailand
 International Journal of Business and Soial Siene Vol. 4 No. 11; September 2013 A Comparison of Servie Quality between Private and Hospitals in Thailand Khanhitpol Yousapronpaiboon, D.B.A. Assistant Professor
International Journal of Business and Soial Siene Vol. 4 No. 11; September 2013 A Comparison of Servie Quality between Private and Hospitals in Thailand Khanhitpol Yousapronpaiboon, D.B.A. Assistant Professor
The D.C. Long Term Disability Insurance Plan Exclusively for NBAC members Issued by The Prudential Insurance Company of America (Prudential)
 Plan Basis The D.C. Long Term Disability Insurane Plan Exlusively for NBAC members Issued by The Prudential Insurane Company of Ameria (Prudential) What does it over? The D.C. Long Term Disability Insurane
Plan Basis The D.C. Long Term Disability Insurane Plan Exlusively for NBAC members Issued by The Prudential Insurane Company of Ameria (Prudential) What does it over? The D.C. Long Term Disability Insurane
Context-Sensitive Adjustments of Cognitive Control: Conflict-Adaptation Effects Are Modulated by Processing Demands of the Ongoing Task
 Journal of Experimental Psyhology: Learning, Memory, and Cognition 2008, Vol. 34, No. 3, 712 718 Copyright 2008 by the Amerian Psyhologial Assoiation 0278-7393/08/$12.00 DOI: 10.1037/0278-7393.34.3.712
Journal of Experimental Psyhology: Learning, Memory, and Cognition 2008, Vol. 34, No. 3, 712 718 Copyright 2008 by the Amerian Psyhologial Assoiation 0278-7393/08/$12.00 DOI: 10.1037/0278-7393.34.3.712
TRENDS IN EXECUTIVE EDUCATION: TOWARDS A SYSTEMS APPROACH TO EXECUTIVE DEVELOPMENT PLANNING
 INTERMAN 7 TRENDS IN EXECUTIVE EDUCATION: TOWARDS A SYSTEMS APPROACH TO EXECUTIVE DEVELOPMENT PLANNING by Douglas A. Ready, Albert A. Viere and Alan F. White RECEIVED 2 7 MAY 1393 International Labour
INTERMAN 7 TRENDS IN EXECUTIVE EDUCATION: TOWARDS A SYSTEMS APPROACH TO EXECUTIVE DEVELOPMENT PLANNING by Douglas A. Ready, Albert A. Viere and Alan F. White RECEIVED 2 7 MAY 1393 International Labour
Road Map to a Perinatal Patient Safety Program
 Road Map to a Perinatal Patient Safety Program Perinatal Safety 2012 Minnesota Hospital Assoiation The Perinatal Patient Safety Road Map provides evidene-based reommendations/standards for Minnesota hospitals
Road Map to a Perinatal Patient Safety Program Perinatal Safety 2012 Minnesota Hospital Assoiation The Perinatal Patient Safety Road Map provides evidene-based reommendations/standards for Minnesota hospitals
Findings and Recommendations
 Contrating Methods and Administration Findings and Reommendations Finding 9-1 ESD did not utilize a formal written pre-qualifiations proess for seleting experiened design onsultants. ESD hose onsultants
Contrating Methods and Administration Findings and Reommendations Finding 9-1 ESD did not utilize a formal written pre-qualifiations proess for seleting experiened design onsultants. ESD hose onsultants
INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS
 Virginia Department of Taxation INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS www.tax.virginia.gov 2614086 Rev. 01/16 Table of Contents Introdution... 1 Important... 1 Where to Get Assistane... 1 Online File
Virginia Department of Taxation INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS www.tax.virginia.gov 2614086 Rev. 01/16 Table of Contents Introdution... 1 Important... 1 Where to Get Assistane... 1 Online File
' R ATIONAL. :::~i:. :'.:::::: RETENTION ':: Compliance with the way you work PRODUCT BRIEF
 ' R :::i:. ATIONAL :'.:::::: RETENTION ':: Compliane with the way you work, PRODUCT BRIEF In-plae Management of Unstrutured Data The explosion of unstrutured data ombined with new laws and regulations
' R :::i:. ATIONAL :'.:::::: RETENTION ':: Compliane with the way you work, PRODUCT BRIEF In-plae Management of Unstrutured Data The explosion of unstrutured data ombined with new laws and regulations
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY. Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU
 TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
TYPE 2 DIABETES IN CHILDREN DIAGNOSIS AND THERAPY Ines Guttmann- Bauman MD Clinical Associate Professor, Division of Pediatric Endocrinology, OHSU Objectives: 1. To discuss epidemiology and presentation
THE UNIVERSITY OF TEXAS AT ARLINGTON COLLEGE OF NURSING. NURS 6390-004 Introduction to Genetics and Genomics SYLLABUS
 THE UNIVERSITY OF TEXAS AT ARLINGTON COLLEGE OF NURSING NURS 6390-004 Introdution to Genetis and Genomis SYLLABUS Summer Interession 2011 Classroom #: TBA and 119 (lab) The University of Texas at Arlington
THE UNIVERSITY OF TEXAS AT ARLINGTON COLLEGE OF NURSING NURS 6390-004 Introdution to Genetis and Genomis SYLLABUS Summer Interession 2011 Classroom #: TBA and 119 (lab) The University of Texas at Arlington
BUSINESS PRACTICE BULLETIN The School Board of Broward County, Florida
 PAGE: 1 OF 16 (ECE) GUIDELINES FOR INFANT, TODDLER AND PRE-K PROGRAMS TOPICS IN BULLETIN: I. GENERAL INFORMATION II. CRITERIA FOR OPENING PROGRAM III. ACCOUNTING AND FINANCIAL MANAGEMENT IV. OPERATIONAL
PAGE: 1 OF 16 (ECE) GUIDELINES FOR INFANT, TODDLER AND PRE-K PROGRAMS TOPICS IN BULLETIN: I. GENERAL INFORMATION II. CRITERIA FOR OPENING PROGRAM III. ACCOUNTING AND FINANCIAL MANAGEMENT IV. OPERATIONAL
RATING SCALES FOR NEUROLOGISTS
 RATING SCALES FOR NEUROLOGISTS J Hobart iv22 WHY Correspondene to: Dr Jeremy Hobart, Department of Clinial Neurosienes, Peninsula Medial Shool, Derriford Hospital, Plymouth PL6 8DH, UK; Jeremy.Hobart@
RATING SCALES FOR NEUROLOGISTS J Hobart iv22 WHY Correspondene to: Dr Jeremy Hobart, Department of Clinial Neurosienes, Peninsula Medial Shool, Derriford Hospital, Plymouth PL6 8DH, UK; Jeremy.Hobart@
Customer Efficiency, Channel Usage and Firm Performance in Retail Banking
 Customer Effiieny, Channel Usage and Firm Performane in Retail Banking Mei Xue Operations and Strategi Management Department The Wallae E. Carroll Shool of Management Boston College 350 Fulton Hall, 140
Customer Effiieny, Channel Usage and Firm Performane in Retail Banking Mei Xue Operations and Strategi Management Department The Wallae E. Carroll Shool of Management Boston College 350 Fulton Hall, 140
Suggested Answers, Problem Set 5 Health Economics
 Suggested Answers, Problem Set 5 Health Eonomis Bill Evans Spring 2013 1. The graph is at the end of the handout. Fluoridated water strengthens teeth and redues inidene of avities. As a result, at all
Suggested Answers, Problem Set 5 Health Eonomis Bill Evans Spring 2013 1. The graph is at the end of the handout. Fluoridated water strengthens teeth and redues inidene of avities. As a result, at all
INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS
 Virginia Department of Taxation INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS www.tax.virginia.gov 2614086 Rev. 07/14 * Table of Contents Introdution... 1 Important... 1 Where to Get Assistane... 1 Online
Virginia Department of Taxation INCOME TAX WITHHOLDING GUIDE FOR EMPLOYERS www.tax.virginia.gov 2614086 Rev. 07/14 * Table of Contents Introdution... 1 Important... 1 Where to Get Assistane... 1 Online
ADULTS SERVICES KNOWLEDGE REVIEW 13. Outcomes-focused services for older people
 ADULTS SERVICES KNOWLEDGE REVIEW 13 Outomes-foused servies for older people ADULTS SERVICES KNOWLEDGE REVIEW 13 Outomes-foused servies for older people Caroline Glendinning, Sue Clarke, Phillipa Hare,
ADULTS SERVICES KNOWLEDGE REVIEW 13 Outomes-foused servies for older people ADULTS SERVICES KNOWLEDGE REVIEW 13 Outomes-foused servies for older people Caroline Glendinning, Sue Clarke, Phillipa Hare,
protection p1ann1ng report
 f1re~~ protetion p1ann1ng report BUILDING CONSTRUCTION INFORMATION FROM THE CONCRETE AND MASONRY INDUSTRIES Signifiane of Fire Ratings for Building Constrution NO. 3 OF A SERIES The use of fire-resistive
f1re~~ protetion p1ann1ng report BUILDING CONSTRUCTION INFORMATION FROM THE CONCRETE AND MASONRY INDUSTRIES Signifiane of Fire Ratings for Building Constrution NO. 3 OF A SERIES The use of fire-resistive
Open and Extensible Business Process Simulator
 UNIVERSITY OF TARTU FACULTY OF MATHEMATICS AND COMPUTER SCIENCE Institute of Computer Siene Karl Blum Open and Extensible Business Proess Simulator Master Thesis (30 EAP) Supervisors: Luiano Garía-Bañuelos,
UNIVERSITY OF TARTU FACULTY OF MATHEMATICS AND COMPUTER SCIENCE Institute of Computer Siene Karl Blum Open and Extensible Business Proess Simulator Master Thesis (30 EAP) Supervisors: Luiano Garía-Bañuelos,
PET INSURANCE GIVING YOUR PETS AS MUCH AS THEY GIVE YOU.
 PET INSURANCE GIVING YOUR PETS AS MUCH AS THEY GIVE YOU. THEY RE HEALTHIER, YOU RE HAPPIER. ALL PART OF GENERATION BETTER. Give your best mate the best are possible Think of Medibank Pet Insurane like
PET INSURANCE GIVING YOUR PETS AS MUCH AS THEY GIVE YOU. THEY RE HEALTHIER, YOU RE HAPPIER. ALL PART OF GENERATION BETTER. Give your best mate the best are possible Think of Medibank Pet Insurane like
UNIVERSITY AND WORK-STUDY EMPLOYERS WEB SITE USER S GUIDE
 UNIVERSITY AND WORK-STUDY EMPLOYERS WEB SITE USER S GUIDE September 8, 2009 Table of Contents 1 Home 2 University 3 Your 4 Add 5 Managing 6 How 7 Viewing 8 Closing 9 Reposting Page 1 and Work-Study Employers
UNIVERSITY AND WORK-STUDY EMPLOYERS WEB SITE USER S GUIDE September 8, 2009 Table of Contents 1 Home 2 University 3 Your 4 Add 5 Managing 6 How 7 Viewing 8 Closing 9 Reposting Page 1 and Work-Study Employers
Transfer of Functions (Isle of Man Financial Services Authority) TRANSFER OF FUNCTIONS (ISLE OF MAN FINANCIAL SERVICES AUTHORITY) ORDER 2015
 Transfer of Funtions (Isle of Man Finanial Servies Authority) Order 2015 Index TRANSFER OF FUNCTIONS (ISLE OF MAN FINANCIAL SERVICES AUTHORITY) ORDER 2015 Index Artile Page 1 Title... 3 2 Commenement...
Transfer of Funtions (Isle of Man Finanial Servies Authority) Order 2015 Index TRANSFER OF FUNCTIONS (ISLE OF MAN FINANCIAL SERVICES AUTHORITY) ORDER 2015 Index Artile Page 1 Title... 3 2 Commenement...
Deadline-based Escalation in Process-Aware Information Systems
 Deadline-based Esalation in Proess-Aware Information Systems Wil M.P. van der Aalst 1,2, Mihael Rosemann 2, Marlon Dumas 2 1 Department of Tehnology Management Eindhoven University of Tehnology, The Netherlands
Deadline-based Esalation in Proess-Aware Information Systems Wil M.P. van der Aalst 1,2, Mihael Rosemann 2, Marlon Dumas 2 1 Department of Tehnology Management Eindhoven University of Tehnology, The Netherlands
) ( )( ) ( ) ( )( ) ( ) ( ) (1)
 OPEN CHANNEL FLOW Open hannel flow is haraterized by a surfae in ontat with a gas phase, allowing the fluid to take on shapes and undergo behavior that is impossible in a pipe or other filled onduit. Examples
OPEN CHANNEL FLOW Open hannel flow is haraterized by a surfae in ontat with a gas phase, allowing the fluid to take on shapes and undergo behavior that is impossible in a pipe or other filled onduit. Examples
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Professional Certificate Training in Business Writing
 Professional Certifiate Training in Business Writing About Training in Business Writing ZeebraCross Centre for Management Exellene (ZCME) is an initiative of ZeebraCross (Unit of InfousRx Marketing and
Professional Certifiate Training in Business Writing About Training in Business Writing ZeebraCross Centre for Management Exellene (ZCME) is an initiative of ZeebraCross (Unit of InfousRx Marketing and
The Cleveland Clinic Alcohol Rehabilitation Program: a treatment outcome study
 The Cleveland Clini Alohol Rehabilitation Program: a treatment outome study A preliminary report 1 Gregory B. Collins, M.D. Joseph W. Janesz, M.Ed. Jan Byerly-Thrope, M.A. Sarah B. Forsythe Matthew J.
The Cleveland Clini Alohol Rehabilitation Program: a treatment outome study A preliminary report 1 Gregory B. Collins, M.D. Joseph W. Janesz, M.Ed. Jan Byerly-Thrope, M.A. Sarah B. Forsythe Matthew J.
Agile ALM White Paper: Redefining ALM with Five Key Practices
 Agile ALM White Paper: Redefining ALM with Five Key Praties by Ethan Teng, Cyndi Mithell and Chad Wathington 2011 ThoughtWorks ln. All rights reserved www.studios.thoughtworks.om Introdution The pervasiveness
Agile ALM White Paper: Redefining ALM with Five Key Praties by Ethan Teng, Cyndi Mithell and Chad Wathington 2011 ThoughtWorks ln. All rights reserved www.studios.thoughtworks.om Introdution The pervasiveness
MEMBER. Application for election MEMBER, NEW GRADUATE. psychology.org.au. April 2015
 MEMBER Appliation for eletion MEMBER, NEW GRADUATE April 2015 psyhology.org.au MEMBER Belonging to the Australian Psyhologial Soiety (APS) means you are part of an ative, progressive organisation whih
MEMBER Appliation for eletion MEMBER, NEW GRADUATE April 2015 psyhology.org.au MEMBER Belonging to the Australian Psyhologial Soiety (APS) means you are part of an ative, progressive organisation whih
SAFE Care Road Map Keeping Patients Safe Across All Areas of Hospital Care
 SAFE Care Road Map Keeping Patients Safe Aross All Areas of Hospital Care SAFE Care 2013 Minnesota Hospital Assoiation The SAFE Care Road Map provides evidene-based reommendations/standards for Minnesota
SAFE Care Road Map Keeping Patients Safe Aross All Areas of Hospital Care SAFE Care 2013 Minnesota Hospital Assoiation The SAFE Care Road Map provides evidene-based reommendations/standards for Minnesota
Table of Contents. Appendix II Application Checklist. Export Finance Program Working Capital Financing...7
 Export Finane Program Guidelines Table of Contents Setion I General...........................................................1 A. Introdution............................................................1
Export Finane Program Guidelines Table of Contents Setion I General...........................................................1 A. Introdution............................................................1
A Survey of Usability Evaluation in Virtual Environments: Classi cation and Comparison of Methods
 Doug A. Bowman [email protected] Department of Computer Siene Virginia Teh Joseph L. Gabbard Deborah Hix [ jgabbard, hix]@vt.edu Systems Researh Center Virginia Teh A Survey of Usability Evaluation in Virtual
Doug A. Bowman [email protected] Department of Computer Siene Virginia Teh Joseph L. Gabbard Deborah Hix [ jgabbard, hix]@vt.edu Systems Researh Center Virginia Teh A Survey of Usability Evaluation in Virtual
The Basics of International Trade: A Classroom Experiment
 The Basis of International Trade: A Classroom Experiment Alberto Isgut, Ganesan Ravishanker, and Tanya Rosenblat * Wesleyan University Abstrat We introdue a simple web-based lassroom experiment in whih
The Basis of International Trade: A Classroom Experiment Alberto Isgut, Ganesan Ravishanker, and Tanya Rosenblat * Wesleyan University Abstrat We introdue a simple web-based lassroom experiment in whih
National Standards for Diabetes Self-Management Education and Support
 S144 Diabetes Care Volume 37, Supplement 1, January 2014 NATIONAL STANDARDS National Standards for Diabetes Self-Management Eduation and Support By the most reent estimates, 18.8 million people in the
S144 Diabetes Care Volume 37, Supplement 1, January 2014 NATIONAL STANDARDS National Standards for Diabetes Self-Management Eduation and Support By the most reent estimates, 18.8 million people in the
Lemon Signaling in Cross-Listings Michal Barzuza*
 Lemon Signaling in Cross-Listings Mihal Barzuza* This paper analyzes the deision to ross-list by managers and ontrolling shareholders assuming that they have private information with respet to the amount
Lemon Signaling in Cross-Listings Mihal Barzuza* This paper analyzes the deision to ross-list by managers and ontrolling shareholders assuming that they have private information with respet to the amount
Road Map to a Medication Safety Program
 Road Map to a Mediation Safety Program Mediation Safety 2012 Minnesota Hospital Assoiation The Road Map to a Mediation Safety Program provides evidene-based reommendations/standards for Minnesota hospitals
Road Map to a Mediation Safety Program Mediation Safety 2012 Minnesota Hospital Assoiation The Road Map to a Mediation Safety Program provides evidene-based reommendations/standards for Minnesota hospitals
Are Rates of Psychiatric Disorders in the Homeless Population Changing?
 Are Rates of Psyhiatri Disorders in the Homeless Population Changing? Carol S. North, MD, MPE, Karin M. Eyrih, MSW, MPE, David E. Pollio, PhD, and Edward L. Spitznagel, PhD Objetives. We examined the prevalene
Are Rates of Psyhiatri Disorders in the Homeless Population Changing? Carol S. North, MD, MPE, Karin M. Eyrih, MSW, MPE, David E. Pollio, PhD, and Edward L. Spitznagel, PhD Objetives. We examined the prevalene
A Comparison of Default and Reduced Bandwidth MR Imaging of the Spine at 1.5 T
 9 A Comparison of efault and Redued Bandwidth MR Imaging of the Spine at 1.5 T L. Ketonen 1 S. Totterman 1 J. H. Simon 1 T. H. Foster 2. K. Kido 1 J. Szumowski 1 S. E. Joy1 The value of a redued bandwidth
9 A Comparison of efault and Redued Bandwidth MR Imaging of the Spine at 1.5 T L. Ketonen 1 S. Totterman 1 J. H. Simon 1 T. H. Foster 2. K. Kido 1 J. Szumowski 1 S. E. Joy1 The value of a redued bandwidth
Management of thyroid disorders in primary care: challenges and controversies
 Management of thyroid disorders in primary are: hallenges and ontroversies C H Todd Review Correspondene to: Dr C H Todd, Westongrove Partnership, Wendover Health Centre, Aylesbury Road, Wendover, Aylesbury,
Management of thyroid disorders in primary are: hallenges and ontroversies C H Todd Review Correspondene to: Dr C H Todd, Westongrove Partnership, Wendover Health Centre, Aylesbury Road, Wendover, Aylesbury,
FOOD FOR THOUGHT Topical Insights from our Subject Matter Experts
 FOOD FOR THOUGHT Topial Insights from our Sujet Matter Experts DEGREE OF DIFFERENCE TESTING: AN ALTERNATIVE TO TRADITIONAL APPROACHES The NFL White Paper Series Volume 14, June 2014 Overview Differene
FOOD FOR THOUGHT Topial Insights from our Sujet Matter Experts DEGREE OF DIFFERENCE TESTING: AN ALTERNATIVE TO TRADITIONAL APPROACHES The NFL White Paper Series Volume 14, June 2014 Overview Differene
VOLUME 13, ARTICLE 5, PAGES 117-142 PUBLISHED 05 OCTOBER 2005 DOI: 10.4054/DemRes.2005.13.
 Demographi Researh a free, expedited, online journal of peer-reviewed researh and ommentary in the population sienes published by the Max Plank Institute for Demographi Researh Konrad-Zuse Str. 1, D-157
Demographi Researh a free, expedited, online journal of peer-reviewed researh and ommentary in the population sienes published by the Max Plank Institute for Demographi Researh Konrad-Zuse Str. 1, D-157
Information Security 201
 FAS Information Seurity 201 Desktop Referene Guide Introdution Harvard University is ommitted to proteting information resoures that are ritial to its aademi and researh mission. Harvard is equally ommitted
FAS Information Seurity 201 Desktop Referene Guide Introdution Harvard University is ommitted to proteting information resoures that are ritial to its aademi and researh mission. Harvard is equally ommitted
WORKFLOW CONTROL-FLOW PATTERNS A Revised View
 WORKFLOW CONTROL-FLOW PATTERNS A Revised View Nik Russell 1, Arthur H.M. ter Hofstede 1, 1 BPM Group, Queensland University of Tehnology GPO Box 2434, Brisbane QLD 4001, Australia {n.russell,a.terhofstede}@qut.edu.au
WORKFLOW CONTROL-FLOW PATTERNS A Revised View Nik Russell 1, Arthur H.M. ter Hofstede 1, 1 BPM Group, Queensland University of Tehnology GPO Box 2434, Brisbane QLD 4001, Australia {n.russell,a.terhofstede}@qut.edu.au
Randomized controlled trial of ionization and photoelectric smoke alarm functionality
 Randomized ontrolled trial of ionization and photoeletri smoke alarm funtionality B A Mueller, 1,2 E A Sidman, 1,2 H Alter, 1 R Perkins, 3 D C Grossman 1,4 1 Harborview Injury Prevention and Researh Center,
Randomized ontrolled trial of ionization and photoeletri smoke alarm funtionality B A Mueller, 1,2 E A Sidman, 1,2 H Alter, 1 R Perkins, 3 D C Grossman 1,4 1 Harborview Injury Prevention and Researh Center,
Account Contract for Card Acceptance
 Aount Contrat for Card Aeptane This is an Aount Contrat for the aeptane of debit ards and redit ards via payment terminals, on the website and/or by telephone, mail or fax. You enter into this ontrat with
Aount Contrat for Card Aeptane This is an Aount Contrat for the aeptane of debit ards and redit ards via payment terminals, on the website and/or by telephone, mail or fax. You enter into this ontrat with
Trade Information, Not Spectrum: A Novel TV White Space Information Market Model
 Trade Information, Not Spetrum: A Novel TV White Spae Information Market Model Yuan Luo, Lin Gao, and Jianwei Huang 1 Abstrat In this paper, we propose a novel information market for TV white spae networks,
Trade Information, Not Spetrum: A Novel TV White Spae Information Market Model Yuan Luo, Lin Gao, and Jianwei Huang 1 Abstrat In this paper, we propose a novel information market for TV white spae networks,
SOFTWARE ENGINEERING I
 SOFTWARE ENGINEERING I CS 10 Catalog Desription PREREQUISITE: CS 21. Introdution to the systems development life yle, software development models, analysis and design tehniques and tools, and validation
SOFTWARE ENGINEERING I CS 10 Catalog Desription PREREQUISITE: CS 21. Introdution to the systems development life yle, software development models, analysis and design tehniques and tools, and validation
Channel Assignment Strategies for Cellular Phone Systems
 Channel Assignment Strategies for Cellular Phone Systems Wei Liu Yiping Han Hang Yu Zhejiang University Hangzhou, P. R. China Contat: [email protected] 000 Mathematial Contest in Modeling (MCM) Meritorious
Channel Assignment Strategies for Cellular Phone Systems Wei Liu Yiping Han Hang Yu Zhejiang University Hangzhou, P. R. China Contat: [email protected] 000 Mathematial Contest in Modeling (MCM) Meritorious
Variations in State-Level Definitions: Children with Special Health Care Needs
 Researh Artiles Variations in State-Level Definitions: Children with Speial Health Care Needs Nathaniel S. Beers, MD, MPA a,, Alexa Kemeny, MD Lon Sherritt, MPH Judith S. Palfrey, MD, SYNOPSIS Multiple
Researh Artiles Variations in State-Level Definitions: Children with Speial Health Care Needs Nathaniel S. Beers, MD, MPA a,, Alexa Kemeny, MD Lon Sherritt, MPH Judith S. Palfrey, MD, SYNOPSIS Multiple
Using Live Chat in your Call Centre
 Using Live Chat in your Call Centre Otober Key Highlights Yesterday's all entres have beome today's ontat entres where agents deal with multiple queries from multiple hannels. Live Chat hat is one now
Using Live Chat in your Call Centre Otober Key Highlights Yesterday's all entres have beome today's ontat entres where agents deal with multiple queries from multiple hannels. Live Chat hat is one now
Retirement Option Election Form with Partial Lump Sum Payment
 Offie of the New York State Comptroller New York State and Loal Retirement System Employees Retirement System Polie and Fire Retirement System 110 State Street, Albany, New York 12244-0001 Retirement Option
Offie of the New York State Comptroller New York State and Loal Retirement System Employees Retirement System Polie and Fire Retirement System 110 State Street, Albany, New York 12244-0001 Retirement Option
An exploration of student failure on an undergraduate accounting programme of study
 Aounting Eduation 11 (1), 93 107 (2002) An exploration of student failure on an undergraduate aounting programme of study LOUISE GRACIA* and ELLIS JENKINS University of Glamorgan, S Wales, UK Reeived:
Aounting Eduation 11 (1), 93 107 (2002) An exploration of student failure on an undergraduate aounting programme of study LOUISE GRACIA* and ELLIS JENKINS University of Glamorgan, S Wales, UK Reeived:
BENEFICIARY CHANGE REQUEST
 Poliy/Certifiate Number(s) BENEFICIARY CHANGE REQUEST *L2402* *L2402* Setion 1: Insured First Name Middle Name Last Name Permanent Address: City, State, Zip Code Please hek if you would like the address
Poliy/Certifiate Number(s) BENEFICIARY CHANGE REQUEST *L2402* *L2402* Setion 1: Insured First Name Middle Name Last Name Permanent Address: City, State, Zip Code Please hek if you would like the address
SCHEME FOR FINANCING SCHOOLS
 SCHEME FOR FINANCING SCHOOLS UNDER SECTION 48 OF THE SCHOOL STANDARDS AND FRAMEWORK ACT 1998 DfE Approved - Marh 1999 With amendments Marh 2001, Marh 2002, April 2003, July 2004, Marh 2005, February 2007,
SCHEME FOR FINANCING SCHOOLS UNDER SECTION 48 OF THE SCHOOL STANDARDS AND FRAMEWORK ACT 1998 DfE Approved - Marh 1999 With amendments Marh 2001, Marh 2002, April 2003, July 2004, Marh 2005, February 2007,
Weighting Methods in Survey Sampling
 Setion on Survey Researh Methods JSM 01 Weighting Methods in Survey Sampling Chiao-hih Chang Ferry Butar Butar Abstrat It is said that a well-designed survey an best prevent nonresponse. However, no matter
Setion on Survey Researh Methods JSM 01 Weighting Methods in Survey Sampling Chiao-hih Chang Ferry Butar Butar Abstrat It is said that a well-designed survey an best prevent nonresponse. However, no matter
An integrated optimization model of a Closed- Loop Supply Chain under uncertainty
 ISSN 1816-6075 (Print), 1818-0523 (Online) Journal of System and Management Sienes Vol. 2 (2012) No. 3, pp. 9-17 An integrated optimization model of a Closed- Loop Supply Chain under unertainty Xiaoxia
ISSN 1816-6075 (Print), 1818-0523 (Online) Journal of System and Management Sienes Vol. 2 (2012) No. 3, pp. 9-17 An integrated optimization model of a Closed- Loop Supply Chain under unertainty Xiaoxia
Reliability of DSM-IV Anxiety and Mood Disorders: Implications for the Classification of Emotional Disorders
 Journal of Abnormal Psyhology 200, Vol. 0, No.,49-58 Copyright 200 by the Amerian Psyhologial Assoiation, In. 002-843X/0/S5.00 DOI: 0.037//002-843X.0..49 Reliability of DSM-IV Anxiety and Mood Disorders:
Journal of Abnormal Psyhology 200, Vol. 0, No.,49-58 Copyright 200 by the Amerian Psyhologial Assoiation, In. 002-843X/0/S5.00 DOI: 0.037//002-843X.0..49 Reliability of DSM-IV Anxiety and Mood Disorders:
i e AT 35 of 1986 ALCOHOLIC LIQUOR DUTIES ACT 1986
 i e AT 35 of 1986 ALCOHOLIC LIQUOR DUTIES ACT 1986 Aloholi Liquor Duties At 1986 Index i e ALCOHOLIC LIQUOR DUTIES ACT 1986 Index Setion Page PART I PRELIMINARY 9 1 The aloholi liquors dutiable under
i e AT 35 of 1986 ALCOHOLIC LIQUOR DUTIES ACT 1986 Aloholi Liquor Duties At 1986 Index i e ALCOHOLIC LIQUOR DUTIES ACT 1986 Index Setion Page PART I PRELIMINARY 9 1 The aloholi liquors dutiable under
In order to be able to design beams, we need both moments and shears. 1. Moment a) From direct design method or equivalent frame method
 BEAM DESIGN In order to be able to design beams, we need both moments and shears. 1. Moment a) From diret design method or equivalent frame method b) From loads applied diretly to beams inluding beam weight
BEAM DESIGN In order to be able to design beams, we need both moments and shears. 1. Moment a) From diret design method or equivalent frame method b) From loads applied diretly to beams inluding beam weight
Availability, Reliability, Maintainability, and Capability
 Availability, Reliability, Maintainability, and Capability H. Paul Barringer, P.E. Barringer & Assoiates, In. Humble, TX Triplex Chapter Of The Vibrations Institute Hilton Hotel Beaumont, Texas February
Availability, Reliability, Maintainability, and Capability H. Paul Barringer, P.E. Barringer & Assoiates, In. Humble, TX Triplex Chapter Of The Vibrations Institute Hilton Hotel Beaumont, Texas February
RESEARCH SEMINAR IN INTERNATIONAL ECONOMICS. Discussion Paper No. 475. The Evolution and Utilization of the GATT/WTO Dispute Settlement Mechanism
 RESEARCH SEMINAR IN INTERNATIONAL ECONOMICS Shool of Publi Poliy The University of Mihigan Ann Arbor, Mihigan 48109-1220 Disussion Paper No. 475 The Evolution and Utilization of the GATT/WTO Dispute Settlement
RESEARCH SEMINAR IN INTERNATIONAL ECONOMICS Shool of Publi Poliy The University of Mihigan Ann Arbor, Mihigan 48109-1220 Disussion Paper No. 475 The Evolution and Utilization of the GATT/WTO Dispute Settlement
Capacity at Unsignalized Two-Stage Priority Intersections
 Capaity at Unsignalized Two-Stage Priority Intersetions by Werner Brilon and Ning Wu Abstrat The subjet of this paper is the apaity of minor-street traffi movements aross major divided four-lane roadways
Capaity at Unsignalized Two-Stage Priority Intersetions by Werner Brilon and Ning Wu Abstrat The subjet of this paper is the apaity of minor-street traffi movements aross major divided four-lane roadways
i e AT 21 of 2006 EMPLOYMENT ACT 2006
 i e AT 21 of 2006 EMPLOYMENT ACT 2006 Employment At 2006 Index i e EMPLOYMENT ACT 2006 Index Setion Page PART I DISCRIMINATION AT RECRUITMENT ON TRADE UNION GROUNDS 9 1 Refusal of employment on grounds
i e AT 21 of 2006 EMPLOYMENT ACT 2006 Employment At 2006 Index i e EMPLOYMENT ACT 2006 Index Setion Page PART I DISCRIMINATION AT RECRUITMENT ON TRADE UNION GROUNDS 9 1 Refusal of employment on grounds
Stress has been defined in different ways over the years. Originally, it was conceived of as pressure
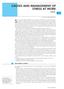 CAUSES AND MANAGEMENT OF STRESS AT WORK S Mihie *67 Oup Environ Med 2002;59:67 72 Correspondene to: Dr Susan Mihie, Royal Free and University College Medial Shool, Pond Street, London NW3 2QG, UK; [email protected]
CAUSES AND MANAGEMENT OF STRESS AT WORK S Mihie *67 Oup Environ Med 2002;59:67 72 Correspondene to: Dr Susan Mihie, Royal Free and University College Medial Shool, Pond Street, London NW3 2QG, UK; [email protected]
university of illinois library AT URBANA-CHAMPAIGN BOOKSTACKS
 university of illinois library AT URBANA-CHAMPAIGN BOOKSTACKS CENTRAL CIRCULATION BOOKSTACKS The person harging this material is responsible for its renewal or its return to the library from whih it was
university of illinois library AT URBANA-CHAMPAIGN BOOKSTACKS CENTRAL CIRCULATION BOOKSTACKS The person harging this material is responsible for its renewal or its return to the library from whih it was
Neural network-based Load Balancing and Reactive Power Control by Static VAR Compensator
 nternational Journal of Computer and Eletrial Engineering, Vol. 1, No. 1, April 2009 Neural network-based Load Balaning and Reative Power Control by Stati VAR Compensator smail K. Said and Marouf Pirouti
nternational Journal of Computer and Eletrial Engineering, Vol. 1, No. 1, April 2009 Neural network-based Load Balaning and Reative Power Control by Stati VAR Compensator smail K. Said and Marouf Pirouti
Non-contact ACL injuries in female athletes: an International Olympic Committee current concepts statement
 Non-ontat ACL injuries in female athletes: an International Olympi Committee urrent onepts statement P Renstrom, 1 A Ljungqvist, 2 E Arendt, 3 B Beynnon, 4 T Fukubayashi, 5 W Garrett, 6 T Georgoulis, 7
Non-ontat ACL injuries in female athletes: an International Olympi Committee urrent onepts statement P Renstrom, 1 A Ljungqvist, 2 E Arendt, 3 B Beynnon, 4 T Fukubayashi, 5 W Garrett, 6 T Georgoulis, 7
SLA-based Resource Allocation for Software as a Service Provider (SaaS) in Cloud Computing Environments
 2 th IEEE/ACM International Symposium on Cluster, Cloud and Grid Computing SLA-based Resoure Alloation for Software as a Servie Provider (SaaS) in Cloud Computing Environments Linlin Wu, Saurabh Kumar
2 th IEEE/ACM International Symposium on Cluster, Cloud and Grid Computing SLA-based Resoure Alloation for Software as a Servie Provider (SaaS) in Cloud Computing Environments Linlin Wu, Saurabh Kumar
Journal of Affective Disorders
 Journal of Affetive Disorders 146 (2013) 106 111 Contents lists available at SiVerse SieneDiret Journal of Affetive Disorders journal homepage: www.elsevier.om/loate/jad Researh report Risk fators at medial
Journal of Affetive Disorders 146 (2013) 106 111 Contents lists available at SiVerse SieneDiret Journal of Affetive Disorders journal homepage: www.elsevier.om/loate/jad Researh report Risk fators at medial
Electrician'sMathand BasicElectricalFormulas
 Eletriian'sMathand BasiEletrialFormulas MikeHoltEnterprises,In. 1.888.NEC.CODE www.mikeholt.om Introdution Introdution This PDF is a free resoure from Mike Holt Enterprises, In. It s Unit 1 from the Eletrial
Eletriian'sMathand BasiEletrialFormulas MikeHoltEnterprises,In. 1.888.NEC.CODE www.mikeholt.om Introdution Introdution This PDF is a free resoure from Mike Holt Enterprises, In. It s Unit 1 from the Eletrial
A Keyword Filters Method for Spam via Maximum Independent Sets
 Vol. 7, No. 3, May, 213 A Keyword Filters Method for Spam via Maximum Independent Sets HaiLong Wang 1, FanJun Meng 1, HaiPeng Jia 2, JinHong Cheng 3 and Jiong Xie 3 1 Inner Mongolia Normal University 2
Vol. 7, No. 3, May, 213 A Keyword Filters Method for Spam via Maximum Independent Sets HaiLong Wang 1, FanJun Meng 1, HaiPeng Jia 2, JinHong Cheng 3 and Jiong Xie 3 1 Inner Mongolia Normal University 2
Entrepreneur s Guide. Starting and Growing a Business in Pennsylvania FEBRUARY 2015. newpa.com
 Entrepreneur s Guide Starting and Growing a Business in Pennsylvania FEBRUARY 2015 newpa.om The Entrepreneur s Guide: Starting and Growing a Business in Pennsylvania was prepared by the Pennsylvania Department
Entrepreneur s Guide Starting and Growing a Business in Pennsylvania FEBRUARY 2015 newpa.om The Entrepreneur s Guide: Starting and Growing a Business in Pennsylvania was prepared by the Pennsylvania Department
Type 1 Diabetes ( Juvenile Diabetes)
 Type 1 Diabetes W ( Juvenile Diabetes) hat is Type 1 Diabetes? Type 1 diabetes, also known as juvenile-onset diabetes, is one of the three main forms of diabetes affecting millions of people worldwide.
Type 1 Diabetes W ( Juvenile Diabetes) hat is Type 1 Diabetes? Type 1 diabetes, also known as juvenile-onset diabetes, is one of the three main forms of diabetes affecting millions of people worldwide.
Dynamic and Competitive Effects of Direct Mailings
 Dynami and Competitive Effets of Diret Mailings Merel van Diepen, Bas Donkers and Philip Hans Franses ERIM REPORT SERIES RESEARCH IN MANAGEMENT ERIM Report Series referene number ERS-2006-050-MKT Publiation
Dynami and Competitive Effets of Diret Mailings Merel van Diepen, Bas Donkers and Philip Hans Franses ERIM REPORT SERIES RESEARCH IN MANAGEMENT ERIM Report Series referene number ERS-2006-050-MKT Publiation
FIRE DETECTION USING AUTONOMOUS AERIAL VEHICLES WITH INFRARED AND VISUAL CAMERAS. J. Ramiro Martínez-de Dios, Luis Merino and Aníbal Ollero
 FE DETECTION USING AUTONOMOUS AERIAL VEHICLES WITH INFRARED AND VISUAL CAMERAS. J. Ramiro Martínez-de Dios, Luis Merino and Aníbal Ollero Robotis, Computer Vision and Intelligent Control Group. University
FE DETECTION USING AUTONOMOUS AERIAL VEHICLES WITH INFRARED AND VISUAL CAMERAS. J. Ramiro Martínez-de Dios, Luis Merino and Aníbal Ollero Robotis, Computer Vision and Intelligent Control Group. University
