EMR Medical Directives and Guidelines
|
|
|
- Joseph Barton
- 8 years ago
- Views:
Transcription
1 EMR Medical Directives and Guidelines Central East Prehospital Care Program, May 1, 2009 Section One 1
2 USE OF MEDICAL DIRECTIVES / GUIDELINES These medical directives and guidelines are not intended to be all encompassing of the complex medical and trauma situations that may be encountered in the field. Since patients do not always fit into a cook book approach, these medical directives and guidelines are not a substitute for good judgment. As a Firefighter / First Responder, it is your responsibility to assess the situation and use your knowledge and skills to benefit the patient while remaining within your scope of practice. We would strongly recommend that if you are involved in a situation that does not fall within a specific directive and/or guideline as outlined for your level of certification, that you contact the Central East Prehospital Care Program (CEPCP) as soon as possible. DELEGATION The Firefighter / First Responder is the extension of the physician in the field and provides care under the direction of the Base Hospital Medical Directors of the CEPCP. The Firefighter / First Responder receives delegation from the Medical Director through written medical directives. The Firefighter / First Responder does not receive delegation from an on-scene physician, nor should the Firefighter / First Responder delegate to another defibrillation provider or citizen. The medical directives that are associated with the use of a Semi-Automated External Defibrillator (SAED) fall under the auspices of delegation. RESPONSIBILITY With the development of SARS (Severe Acute Respiratory Syndrome), the Firefighter / First Responder must recognize their obligation to protect themselves and others while providing patient care. It is strongly recommended that the Firefighter / First Responder utilize all available personal protective equipment (PPE) precautions to limit personal exposure and disease transmission. It is important to note that not all victims of infectious respiratory illnesses are febrile, and some prehospital interventions may increase the risk of contamination. The Firefighter / First Responder must use their judgment and investigative skills to identify situations of risk and take appropriate protective steps. Central East Prehospital Care Program, May 1, 2009 Section One 2
3 CARDIAC ARREST GENERAL MEDICAL DIRECTIVE When the following indications and conditions exist, a Firefighter / First Responder may treat victims of cardiac arrest according to the following: Indications Conditions Patient is in cardiac arrest (Vital Signs Absent - VSA). Patient is 1 year old for application of an SAED. Contraindications Procedure 1. Patients who meet the criteria for obvious death. 2. Patients who have a valid and completed Ministry of Health (MOH) DNR Confirmation form or a York / Durham Base Hospital approved DNR form. 1. Confirm VSA by the absence of spontaneous respirations and palpable pulses. 2. Initiate airway management, oxygen, ventilation, and CPR. 3. Initiate therapy outlined in a directive according to the causative agent and based upon SAED prompts received. Central East Prehospital Care Program, July 1, 2009 Section One 3
4 MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE Indication: Patient who is in a medical cardiac arrest Procedure: 1. Ensure Scene Safety 2. Establish Unresponsiveness (AVPU) 3. Open airway and check breathing for 3 6 seconds 4. If no breathing, insert an oral airway and ventilate x 2 with a BVM to ascertain airway patency 5. Check for signs of circulation including carotid pulse 6. If the arrest was unwitnessed, initiate 2 min of dedicated CPR. (If the arrest is witnessed, apply the cardiac monitor and proceed with an immediate analysis). 7. Attach the SAED and turn it on and follow the prompt to: Stop CPR and analyze Stand clear 8. a) If the rhythm is shockable, defibrillate according to the following chart Defibrillator standard AHA 2005 compliant # shocks delivered 1 CPR interval Reanalyze 2 minutes After 2 min of CPR b) If the rhythm is non-shockable, proceed to the next step. 9. Initiate 2 min of dedicated CPR followed by an assessment of signs of circulation and carotid pulse. 10. Continue the cycle of analysis defibrillation (if shockable) CPR circulation assessment. 11. Provide a report of patient care on arrival of EMS. Notes N/A Central East Prehospital Care Program, July 1, 2009 Section One 4
5 HYPOTHERMIA CARDIAC ARREST DIRECTIVE Indication: Patient who is in a medical cardiac arrest due to hypothermia. Procedure: 1. Ensure Scene Safety 2. Establish Unresponsiveness (AVPU) 3. Open airway and check breathing for 3 6 seconds 4. If no breathing, ventilate x 2 with a BVM to ascertain airway patency 5. Assess the patient s core temperature by feeling the abdomen 6. Check for signs of circulation including carotid pulse (minimum seconds) 7. If no pulse, initiate 2 minutes of dedicated CPR. 8. Attach the SAED and turn it on and follow the prompt to: Stop CPR and analyze Stand clear. 9. a) If the rhythm is shockable, defibrillate according to the following chart Defibrillator standard AHA 2005 compliant # shocks delivered 1 CPR interval Reanalyze b) If the rhythm is non-shockable, proceed to the next step. 2 minutes NONE 10. Initiate 2 min of dedicated CPR followed by an assessment of signs of circulation and carotid pulse. 11. Resume CPR and ignore subsequent defibrillator prompts to analyze. 12. Provide a report of patient care on arrival of EMS. Notes An oral airway should only be used if a patent airway cannot be maintained using manual airway management procedures. After the first analysis is complete, subsequent defibrillator prompts are to be ignored when following this directive. The Base Hospital recommends that you unplug your SAED pads if you have an SAED that analyzes automatically. Central East Prehospital Care Program, July 1, 2009 Section One 5
6 TRAUMA ARREST MEDICAL DIRECTIVE Indication: Patient is in cardiac arrest due to multiple system trauma: Procedure: 1. Ensure Scene Safety 2. Establish Unresponsiveness (AVPU) 3. Open airway and check breathing for 3 6 seconds 4. If no breathing, insert an oral airway and ventilate x 2 with a BVM to ascertain airway patency 5. Check for signs of circulation including carotid pulse 6. If no pulse, rapidly extricate the patient using C-spine precautions and initiate 2 minutes of CPR 7. a) If the cause of the cardiac arrest is PENETRATING trauma, continue to perform CPR until EMS arrives and DO NOT attach the SAED. b) If the cause of cardiac arrest is BLUNT trauma, attach the SAED and continue with the following steps; 8. Turn the SAED on and follow the prompt to: Stop CPR and analyze - Stand clear 9. a) If the rhythm is shockable, defibrillate according to the following chart Defibrillator standard AHA 2005 compliant # shocks delivered 1 CPR interval Reanalyze b) If the rhythm is non-shockable, proceed to the next step. 2 minutes NONE 10. Initiate 2 min of dedicated CPR followed by an assessment of signs of circulation and carotid pulse. 11. Resume CPR and ignore subsequent defibrillator prompts to analyze. 12. Provide a report of patient care on arrival of EMS. Notes If the cardiac arrest patient (regardless of cause) is trapped, or in a rescue situation where paramedics cannot safely enter, you should provide immediate extrication while attempting CPR for two minutes. Nothing should delay extrication, but if the patient is still trapped, or in a rescue situation after two minutes, then attempt to attach the SAED. If prompted, deliver one shock and upon completion of the shock all efforts should be put towards extricating the patient. After the first analysis is complete, subsequent defibrillator prompts are to be ignored when following this directive. The Base Hospital recommends that you unplug your SAED pads if you have an SAED that analyzes automatically. Central East Prehospital Care Program, July 1, 2009 Section One 6
7 NEONATAL RESUSCITATION MEDICAL DIRECTIVE When the following indications and conditions exist, a Firefighter / First Responder may treat pediatric victims of cardiac arrest/cardio-respiratory distress according to the following: Indications: Conditions: Patient is in cardiac arrest (Vital Signs Absent - VSA) or in severe cardio-respiratory distress. Patient is < 29 days of age Procedure: 1. Ensure Scene Safety 2. Establish level of responsiveness (AVPU). In the newly born: dry, warm, position, suction and stimulate as necessary 3. Open airway and check breathing for 3 6 seconds If not breathing: Insert an oral airway Ventilate x 2 with BVM to ascertain airway patency If breathing Administer blow-by oxygen (O 2 ) 4. Check for signs of circulation* including carotid/brachial pulse Assess the newly born using the APGAR scale If no pulse, start CPR: 120 compressions/min 3 compressions : 1 vent If pulse < 100 bpm: Secure the airway Ventilate with BVM at 40 breaths/min x 1 min 5. Reassess If no pulse and no breathing: Continue CPR If pulse < 60 bpm, start CPR: 120 compressions/min 3 compressions : 1 vent 6. Continue to reassess frequently 7. Provide a report of patient care on arrival of EMS. Notes If meconium is present in the airway of the newborn, the meconium must be suctioned prior to positive pressure ventilation. The mouth, nose and posterior (back) area of the oral cavity should be suctioned following delivery of head, or as soon as possible. *Signs of poor circulation include unresponsiveness, agonal or no breathing, cool skin temperature that is centrally cyanotic or mottled with delayed capillary refill. Central East Prehospital Care Program, July 1, 2009 Section One 7
8 RECOGNITION OF DEATH MEDICAL DIRECTIVE The medical directives for patients that have are Vital Signs Absent (VSA) should be followed, except in the following circumstances: 1. OBVIOUSLY DEAD The Firefighter / First Responder may presume death, and not initiate resuscitation, when one or more of the following gross signs of obvious death is present: Decapitation Transection Visible decomposition Putrefaction (smell) Otherwise (see below) Otherwise is delineated as: Grossly charred body Open head or torso wounds with gross outpouring of cranial or visceral contents Gross rigor mortis in a pulseless, apneic, warm patient In such cases, no treatment is required, but Central Communications contact is required to notify the Emergency Medical Services and the Police Department. Documentation Guidelines for the Firefighter / First Responder You need to complete a Medical Assist Report (MAR) for any cardiac arrest including: Date and time of the call Patient s name, address and date of birth Incident history, and assessment findings Names and/or I.D. numbers of EMS paramedics in attendance 2. EXPECTED DEATH DO NOT RESUSCITATE (DNR) Upon arrival at a scene a Firefighter / First Responder may be presented with a request NOT to initiate resuscitation. In order to consider the request, one of the following must be present: A. An appropriately completed Ministry of Health (MOH) DNR CONFIRMATION FORM (a sample is provided on page 12). OR B. A York/Durham Region recognized DO NOT RESUSCITATE MEDICAL DIRECTIVE AND FUNERAL HOME TRANSFER FORM order document clearly identifying the patient, the physician and any substitute decision-maker involved (a sample is provided on page 11). OR C. The attending physician is present and he/she indicates that he/she is the patient s physician and that resuscitation is not indicated. Central East Prehospital Care Program, July 1, 2009 Section One 8
9 If no physician is present, the Firefighter / First Responder will: Contact Central Communications: o stating the patient s condition o verifying the presence of valid documentation o ensure that Emergency Medical Services is responding o ensure that the Police department is responding Complete a MAR, leaving the white copy on-scene and retaining the others for distribution. Remain at the scene until EMS has arrived. If the family/attending physician is on scene, the Firefighter / First Responder will: Contact Central Communications: o stating the patient s condition o identifying the name of the physician on scene o ensure that Emergency Medical Services is responding Complete a MAR, leaving the white copy on scene and retaining the others for distribution. Documentation Guidelines for the Firefighter / First Responder Do NOT document anything on the DO NOT RESUSCITATE MEDICAL DIRECTIVE AND FUNERAL HOME TRANSFER FORM. You need to complete a MAR as for any other cardiac arrest including: NOTES Date and time of the call Patient s name, address and date of birth That the appropriate DNR was seen by responders Names of witnesses at the scene (person assuming responsibility for the victim or on-scene physician Names and / or numbers of EMS paramedics in attendance In the event of a disagreement on scene between family members regarding the resuscitation, the firefighter / first responder on scene will consider the DNR null and void and initiate a resuscitation, until otherwise directed by EMS. Central East Prehospital Care Program, July 1, 2009 Section One 9
10 DO NOT RESUSCITATE MEDICAL DIRECTIVE & FUNERAL HOME TRANSFER FORM I, have discussed and understand my health status and (Client s name-print) prognosis with my physician,. I request that, in the event my (Physician name-print) heart stops beating and/or my breathing stops, Emergency Medical Responders (Nurses, Paramedics, Police or Firefighters) shall not attempt to resuscitate me. In the event that the above named person is incapable of making, or understanding their own health care decisions, has been appointed as the substitute (Substitute Decision-makername-print) decision-maker and agrees to the preceding information. (Client s signature, date) (Client s name-print) (Substitute Decision-maker signature, date) (Relationship and/or Power of Attorney for Care) (Physician signature, date) (Alternate Physician name/ Physician Group) Tel # After Hr # Pager/cell (Physician contact no. in event of death) Tel # After Hr # Pager/cell (alternate Physician/Group contact no. in event of death) Pronounced at home on at (date) (time) by (Nurse/Paramedic) (Agency) Dr. notified at (Doctor s name) (date & time) Funeral Home contacted at (Funeral Home name) (date & time) Once death has been pronounced, this form will enable a funeral home to remove the deceased prior to signature of the Medical Certificate of Death. The Funeral director will arrange with the Attending Physician for completion of the Medical Certificate of Death. The Paramedics/Nurse or Coroner s agent will notify the Attending Physician as soon as possible. In the event that the Attending Physician is not immediately available, his/her Alternate will be contacted. It is requested, that a partially completed Medical Certificate of Death be left attached to this form (not yet completed and unsigned by physician). The Do Not Resuscitate Medical Directive and Funeral Home Transfer Form must be completed in full, and signed, to be acted upon by Emergency Responders This document has been authored conjointly by the Coroner s office, Palliative care Physician group, Durham Access To Care, Funeral Director s group and the Base Hospital Paramedic Program for York / Durham Region. Nov 2006 Central East Prehospital Care Program, July 1, 2009 Section One 10
11 Central East Prehospital Care Program, July 1, 2009 Section One 11
12 CARDIAC ARREST REFERENCE PAGE Witnessed refers to a cardiac arrest that occurs in front of the firefighter / first responder. Unwitnessed refers to the situation in which the firefighter / first responder arrives to find the patient in cardiac arrest. If effective CPR is being performed by a bystander upon your arrival, you may credit the bystander s CPR into your 2 minutes of CPR to be done before the SAED is applied. CPR should be performed according to the Heart and Stroke Foundation of Canada Guidelines for PATIENT AGE SINGLE RESCUER MULTIPLE RESCUERS COMPRESSION RATE Adult ( 8 years of age) Child/Infant (30 days to 8 years of age) Neonate (< 29 days of age) 30 : 2 30 : / min 30 : 2 15 : / min 3 : 1 3 : / min If the Firefighter / First Responder encounters a citizen with an SAED on scene, allow the citizen to complete the shock sequence safely. Once the citizen SAED prompts to commence CPR, the Firefighter / First Responder should switch over to their defibrillator and continue the resuscitation. Make sure that treatment provided by the citizen provider is reported to the EMS paramedic, as well as documented on the Medical Assist Report (MAR). It is the responsibility of the citizen responder to download the information from their SAED. The Firefighter / First Responder is only responsible for the information transfer from their own SAED. In the event of return of spontaneous circulation and then re-arrest, the rhythm should be reanalyzed immediately and the directive resumed (this may necessitate turning the defibrillator off and back on). If the SAED fails to operate, continue CPR. A second rescuer should attempt to trouble shoot the SAED problem (i.e. change battery, examine cables/pads, improve pad adherence to the chest etc.). You should update EMS of the situation and consider calling for a second SAED from your service if it will be faster than EMS. After the call is complete, you should remove the SAED from service and ensure it is flagged for maintenance. You should also document the SAED and details of your management of the patient and SAED situation on the MAR. Should exceptional conditions (water rescue, long distance difficult access, etc.) warrant the need for patient movement to facilitate a rendezvous with EMS, the patient may be moved as long as appropriate patient care is continued and safety precautions taken. Pad placement the preferred pad placement in cardiac arrest is the sternum apex position. In the event that the pads cannot be placed in this position without overlapping, as In the smaller patient, including the pediatric patient, the bi-axillary (armpit) position is next in order of preference. If due to curvature of the chest wall, this position cannot be used, the anterior posterior position may be used. Central East Prehospital Care Program, July 1, 2009 Section One 12
13 RAPID TRAUMA EXTRICATION GUIDELINE When the following indications and conditions exist, a Firefighter / First Responder may treat victims of cardiac arrest according to the following: Indications 1. Environmental situations that place the patient s life in imminent danger. 2. Primary Survey findings that place the victim s life in imminent danger: a) no breathing with the inability to ventilate in the position found, and/or b) no pulse with the inability to provide chest compressions in the position found and/or c) serious gross bleeding with the inability to control it in the position found Conditions N/A Contraindications Firefighter / First Responder safety is at risk Procedure 1. Maintain the patient s head and neck in neutral alignment. 2. Remove the patient to a safe place and reassess beginning with the primary survey. 3. If available, an appropriately sized cervical collar and a backboard may be applied to the patient. Notes Immobilization with a collar and backboard is typically undertaken under the direction of an EMS crew. Central East Prehospital Care Program, July 1, 2009 Section One 13
14 ADDITIONAL GUIDELINES FOR THE EMR IMMOBILIZATION When the following indications and conditions exist, an EMR firefighter may immobilize patients according to the following: Indications 1. Rescue situation that paramedics can t safely enter (e.g. high angle rescue or confined space, etc.) 2. Under the direction of an on-scene paramedic Conditions N/A Contraindications Procedure Notes: Firefighter / First Responder safety is at risk 1. Apply manual stabilization of the head & neck in a neutral position 2. Size and apply cervical collar 3. Log-roll patient supine onto backboard (using 3 rescuers) holding: a. The head b. The shoulder area c. The pelvic area 4. Apply head blocks on each side of head 5. Secure the head, chest and pelvis (straps and tape) to the backboard Always ensure ABCs are being assessed and treated. Example - oxygen 100% - ventilation - cardiac compression - AED - control severe bleeding Firefighters need to protect the neck and spine of stable patients by holding their head and preventing movement. Immobilization is typically undertaken under the direction of EMS. Central East Prehospital Care Program, July 1, 2009 Section One 14
15 ADDITIONAL GUIDELINES FOR THE EMR BURN TREATMENT When the following indications and conditions exist, an EMR firefighter may treat patients with burns according to the following: Indications Primary assessment indicates that the patient has been burned. This includes burns caused by thermal, chemical, radiation and electrical sources. Conditions N/A Contraindications Procedure Notes Firefighter / First Responder safety is at risk 1. Manage the scene safely, especially when removing the patient from the source of the burn. 2. Assess and manage the airway, ventilation and oxygenation. 3. Treat burn patients as trauma patients, and perform a rapid trauma assessment. 4. Properly cool thermal burns if you reach the patient early, but be careful not to induce hypothermia. 5. Initiate therapy according to the appropriate guideline (i.e. thermal, radiation, electrical and chemical). These guidelines are found on the next few pages. Patients do not die quickly from burns. It is the injuries and trauma that are associated with the burns (i.e. potential airway problems, altered levels of consciousness, major injuries) that cause rapid death. Therefore, manage the life threatening injuries before the burns. Remember that any victim exposed to smoke and/or fire should be assumed to have carbon monoxide poisoning, airway swelling and/or airway compromise due to the heat and smoke from the fire. The upper and lower airways could have burns that will not appear serious until the victim s condition suddenly changes. Physical findings to alert you are: Unresponsive or semi-responsive victim Facial burns Soot on face and/or in mouth Difficulty swallowing or talking Shortness of breath Use of accessory muscles to breathe (neck, shoulders, in-drawing of chest, JVD, etc.) Central East Prehospital Care Program, July 1, 2009 Section One 15
16 ADDITIONAL GUIDELINES FOR THE EMR THERMAL & RADIATION BURNS Procedure 1. Ensure the area is safe and you can remove the patient from the hazard safely. 2. Ensure airway, breathing and circulation is adequate. Provide oxygen (high concentration) and ventilation support if required. 3. If burns involve the face/airway, and the patient is unresponsive to pain, ensure an oropharyngeal airway is inserted. 4. Complete a rapid trauma assessment. 5. Remove burned clothing that is not stuck to the burn. 6. Remove rings, watches, or other jewelry if that area is involved (i.e. hands, wrists, or toes). 7. Cover partial thickness burns with a BSA (Body Surface Area) of less than 10% with clean/sterile dressings. You may cool with water/saline or use a manufactured dressing like a Water Jel if the blisters are not broken and the tissue is still hot. 8. Cover partial or full thickness burns with a BSA of 10% or greater with a dry sterile dressing only. Apply water only to extinguish fire/smoldering clothes or flesh. Central East Prehospital Care Program, July 1, 2009 Section One 16
17 ADDITIONAL GUIDELINES FOR THE EMR ELECTRICAL BURNS Procedure 1. Ensure the area is safe and you can remove the patient from the hazard safely. Special training is required to safely handle energized electrical equipment. Ensure appropriate personal protective equipment is worn to protect yourself. 2. Ensure airway and breathing are adequate. Provide oxygen (high concentration) and ventilation support if required. 3. Assess circulation. (A common result of electrical contact is ventricular fibrillation. Therefore, check cardiac status and ensure the SAED is readily available. Continue to monitor pulse. With high voltages and lightning strikes, assume spinal injuries as well.) 4. If burns involve the face/airway, and the patient is unresponsive to pain, ensure an oropharyngeal airway is inserted. 5. Complete a rapid trauma assessment 6. Remove burned clothing that is not stuck to the burn. 7. Remove rings, watches, or other jewelry if that area is involved (i.e. hands, wrists, or toes). 8. Cover partial thickness burns with a BSA of less than 10% with sterile dressings. You may cool with water/saline or use a manufactured dressing like a Water Jel if the blisters are not broken. 9. Cover partial or full thickness burns with a BSA of 10% or greater with a dry sterile dressing only. Apply water only to extinguish fire/smoldering clothes or flesh. 10. Additional information will be required by the treating hospital. If possible and without delaying patient transfer inquire about the following: a. The type and amount of current b. Path of current flow (through the body) c. How long the patient was in contact with the current 11. Industrial EMR should also ensure that the appropriate management supervisor follows up with any additional information on the nature of the electrical contact to the treating hospital. Notes N/A Central East Prehospital Care Program, July 1, 2009 Section One 17
18 ADDITIONAL GUIDELINES FOR THE EMR CHEMICAL BURNS Procedure 1. Identify the chemical. Ensure the area is safe and you can remove the patient from the hazard safely. Special training is required to safely handle hazardous materials like corrosive chemicals. Ensure appropriate personal protective equipment is worn. 2. Ensure the area is safe and you can remove the patient from the hazard safely. 3. Remove any contaminated clothing from the patient. This will protect both the patient and the responder from the chemical. Brush off any dry powder chemicals from the patient before flushing the burn area. Flush the affected area with water for 15 minutes. If it is a liquid chemical, flush immediately before removing the clothing and continue for 15 minutes. Remove the clothing from the liquid contaminated casualty while flushing. 4. Ensure airway, breathing and circulation is adequate. Provide ventilation support if required. 5. If burns involve the face/airway, and the patient is unresponsive to pain, ensure an oropharyngeal airway is inserted. 6. Complete a rapid trauma assessment. 7. Remove burned clothing that is not stuck to the burn. 8. Remove rings, watches, or other jewelry if that area is involved (i.e. hands, wrists, or toes). 9. Cover burns with a dry sterile dressing. 10. Industrial EMR should also ensure that the appropriate management supervisor follows up communicating any additional information on the chemical to the treating hospital. Notes In some circumstances, steps 3 and 4 may need to be completed at the same time as Step 2, but remember to protect yourself from the chemical. Central East Prehospital Care Program, July 1, 2009 Section One 18
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
State of Indiana EMR Psychomotor Skills Examination
 SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
Patient Assessment/Management Trauma
 Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT
 Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED)
 EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
Objectives. Burn Assessment and Management. Questions Regarding the Case Study. Case Study. Patient Assessment. Patient Assessment
 Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Types of electrical injuries
 Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Frontline First Aid EMR Scenario Examples
 Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
CHAPTER 32 QUIZ. Handout 32-1. Write the letter of the best answer in the space provided.
 Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services
 State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
Emergency Medical Technician Basic. Practical Skills Examination Sheets
 New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
3/24/2014. Waubonsee Community College Safety Day 2014. Why do we need a First Aid Program?
 Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
EMR EMERGENCY MEDICAL RESPONDER Course Syllabus
 6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum
 EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Procedure 17: Cardiopulmonary Resuscitation
 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Scenario 2 Is it ever safe enough?
 IRECA BLS Competition 2011 Scenario 2 Is it ever safe enough? Team Name Captain Name Judge 1 Judge 2 The Event: You are dispatched to a shooting for two injured at a local bar. Witnesses have told police
IRECA BLS Competition 2011 Scenario 2 Is it ever safe enough? Team Name Captain Name Judge 1 Judge 2 The Event: You are dispatched to a shooting for two injured at a local bar. Witnesses have told police
Training Bulletin. December 2010. Emergency Health Services Branch Ministry of Health and Long-Term Care. Issue Number 111 version 1.
 Training Bulletin Deceased Patient Standard December 2010 Issue Number 111 version 1.0 Emergency Health Services Branch Ministry of Health and Long-Term Care Training Bulletin, Issue Number 111 version
Training Bulletin Deceased Patient Standard December 2010 Issue Number 111 version 1.0 Emergency Health Services Branch Ministry of Health and Long-Term Care Training Bulletin, Issue Number 111 version
Emergency Medical Responder Safety and Wellness
 Chapter 2 Emergency Medical Responder Safety and Wellness OBJECTIVES DIRECTORY 1. Define key terms introduced in this chapter. 55-56 2. List indications of the potential for danger to yourself or others
Chapter 2 Emergency Medical Responder Safety and Wellness OBJECTIVES DIRECTORY 1. Define key terms introduced in this chapter. 55-56 2. List indications of the potential for danger to yourself or others
Heart of America Medical Center EMR, EMT, EMT-Intermediate & AEMT Protocols
 USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
Emergency Medical Services Division. DNR Guidelines Draft
 Emergency Medical Services Division Draft Ross Elliott EMS Director Robert Barnes, M.D. Medical Director 1 Revision Log 01/01/1992 Initial draft 08/01/2013 POLST Addition Kern County Public Health Services
Emergency Medical Services Division Draft Ross Elliott EMS Director Robert Barnes, M.D. Medical Director 1 Revision Log 01/01/1992 Initial draft 08/01/2013 POLST Addition Kern County Public Health Services
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Health Science Career Cluster Emergency Medical Responder Course Number: 25.45000
 Health Science Career Cluster Emergency Medical Responder Course Number: 25.45000 Course Description: The Emergency Medical Responder (EMR) course prepares the student to provide initial stabilizing care
Health Science Career Cluster Emergency Medical Responder Course Number: 25.45000 Course Description: The Emergency Medical Responder (EMR) course prepares the student to provide initial stabilizing care
(Organization s Name)
 2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
19.109 AUTOMATED EXTERNAL DEFIBRILLATOR
 19.109 AUTOMATED EXTERNAL DEFIBRILLATOR References: American Heart Association Healthcare Provider (CPR/AED) Ohio Revised Code Chapter 2305.235 Immunity of Person Involved with Providing Automated External
19.109 AUTOMATED EXTERNAL DEFIBRILLATOR References: American Heart Association Healthcare Provider (CPR/AED) Ohio Revised Code Chapter 2305.235 Immunity of Person Involved with Providing Automated External
TN Emergency Medical Services
 TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
1st Responder to Emergency Medical Responder Transition Course
 1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
Emergency Action Plans
 Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Regional Medical Response Technician Protocols. Region V Medical Advisory Committee 2009 05 MAR 2009
 Regional Medical Response Technician Protocols Region V Medical Advisory Committee 2009 05 MAR 2009 Charlotte Hungerford Hospital Danbury Hospital New Milford Hospital Sharon Hospital Saint Mary s Hospital
Regional Medical Response Technician Protocols Region V Medical Advisory Committee 2009 05 MAR 2009 Charlotte Hungerford Hospital Danbury Hospital New Milford Hospital Sharon Hospital Saint Mary s Hospital
Emergency Medical Technician
 Emergency Medical Technician 2!! " " New for 2015-2016 Clarification has been added about competitors competing in the highest level of their training. Rating sheets have been updated to include a possible
Emergency Medical Technician 2!! " " New for 2015-2016 Clarification has been added about competitors competing in the highest level of their training. Rating sheets have been updated to include a possible
Chapter 31 Obstetrics and Neonatal Care 1137. Scene Size-up. Primary Assessment
 Chapter 31 Obstetrics and Neonatal Care 1137 Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and safe access to the patient. Standard precautions should
Chapter 31 Obstetrics and Neonatal Care 1137 Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and safe access to the patient. Standard precautions should
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH DATE: December 30, 2011 TO: FROM: REF: All EMS-Instructors Kevin Scott Brown, MS, NREMTP, EMS-I State Education and Training Coordinator CHANGES IN THE
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH DATE: December 30, 2011 TO: FROM: REF: All EMS-Instructors Kevin Scott Brown, MS, NREMTP, EMS-I State Education and Training Coordinator CHANGES IN THE
CENTRAL TEXAS COLLEGE EMSP 1305 EMERGENCY CARE ATTENDANT. Semester Hours Credit: 3
 CENTRAL TEXAS COLLEGE EMERGENCY CARE ATTENDANT INSTRUCTOR: Semester Hours Credit: 3 OFFICE HOURS: I. INTRODUCTION Course Description: First responder course in emergency medical care. Emphasis on requirements
CENTRAL TEXAS COLLEGE EMERGENCY CARE ATTENDANT INSTRUCTOR: Semester Hours Credit: 3 OFFICE HOURS: I. INTRODUCTION Course Description: First responder course in emergency medical care. Emphasis on requirements
How To Manage A Catastrophic Injury
 Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
Ohio s Do-Not-Resuscitate Law
 Ohio s Do-Not-Resuscitate Law Copied from Choices: Living Well at the End of Life developed in collaboration with the Ohio Hospice and Palliative Care Organization, the Ohio State Medical Association,
Ohio s Do-Not-Resuscitate Law Copied from Choices: Living Well at the End of Life developed in collaboration with the Ohio Hospice and Palliative Care Organization, the Ohio State Medical Association,
EMS Patient Care Report Navigation Logic for Record Creation
 EMS Patient Report Navigation Logic for Record Creation This document serves to provide specifications regarding data entry and data element completion requirements for PreMIS Version 2 web-based application
EMS Patient Report Navigation Logic for Record Creation This document serves to provide specifications regarding data entry and data element completion requirements for PreMIS Version 2 web-based application
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Automated External Defibrillators (AED) Program Oversight
 Automated External Defibrillators (AED) Program Oversight DISTRICT AED/HEALTH COORDINATOR 1. Coordinate school/district CPR/AED training 2. Work with schools to select and maintain CPR/AED trained personnel
Automated External Defibrillators (AED) Program Oversight DISTRICT AED/HEALTH COORDINATOR 1. Coordinate school/district CPR/AED training 2. Work with schools to select and maintain CPR/AED trained personnel
At Elite Ambulance, we are always here to serve you.
 FAQ Important Disclaimer: The following FAQ section includes information regarding health provider decisions, health and payment matters not financial matters. None of the following questions or answers
FAQ Important Disclaimer: The following FAQ section includes information regarding health provider decisions, health and payment matters not financial matters. None of the following questions or answers
EMS POLICIES AND PROCEDURES
 EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
INFORMATION ON DO-NOT-RESUSCITATE (DNR) REQUESTS IN EMERGENCY MEDICAL SERVICES
 INFORMATION ON DO-NOT-RESUSCITATE (DNR) REQUESTS IN EMERGENCY MEDICAL SERVICES This summary provides information about the types of Do-Not-Resuscitate (DNR) requests that will be honored in the field by
INFORMATION ON DO-NOT-RESUSCITATE (DNR) REQUESTS IN EMERGENCY MEDICAL SERVICES This summary provides information about the types of Do-Not-Resuscitate (DNR) requests that will be honored in the field by
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Intermedix Inc. EMR 2006 Data Element Name. Compliant. Data Number. Elements
 D01_01 EMS Agency X D01_02 EMS Agency D01_03 EMS Agency State X D01_04 EMS Agency County X D01_05 Primary Type of Service D01_06 Other Types of Service D01_07 Level of Service X D01_08 Organizational Type
D01_01 EMS Agency X D01_02 EMS Agency D01_03 EMS Agency State X D01_04 EMS Agency County X D01_05 Primary Type of Service D01_06 Other Types of Service D01_07 Level of Service X D01_08 Organizational Type
How you can help save lives
 How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
California Correctional Health Care Services
 RN Protocol: I. POLICY A. Function: To facilitate and guide the Registered Nurse (RN) in the assessment and treatment of patients presenting with burns. B. Circumstances under which the RN may perform
RN Protocol: I. POLICY A. Function: To facilitate and guide the Registered Nurse (RN) in the assessment and treatment of patients presenting with burns. B. Circumstances under which the RN may perform
EMR Instructional Guidelines. Preparatory
 EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
notes Video User s s Guide Accident Involving Radioactive Material
 Emergency Response to a Transportation Accident Involving Radioactive Material DISCLAIMER Viewing this video and completing the enclosed printed study material do not by themselves provide sufficient skills
Emergency Response to a Transportation Accident Involving Radioactive Material DISCLAIMER Viewing this video and completing the enclosed printed study material do not by themselves provide sufficient skills
National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs
 National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs National Association of Emergency Medical Services Directors (NASEMSD) 1 and the National Association of Emergency
National Guidelines for Statewide Implementation of EMS "Do Not Resuscitate" (DNR) Programs National Association of Emergency Medical Services Directors (NASEMSD) 1 and the National Association of Emergency
Snohomish County Fire Chiefs Association
 Snohomish County Fire Chiefs Association DOCUMENT 60-06-09 ON SCENE REHABILITATION GUIDELINE Adopted December 2009 County Chiefs Meeting INTENT To provide standard operating guidelines to implement and
Snohomish County Fire Chiefs Association DOCUMENT 60-06-09 ON SCENE REHABILITATION GUIDELINE Adopted December 2009 County Chiefs Meeting INTENT To provide standard operating guidelines to implement and
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
Emergency procedures instructions to farm staff
 Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
MRC Medical Jeopardy Feud List of Treatments for Possible Injuries/Conditions
 List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION. ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements
 TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
Emergency Medical Responder Course Syllabus
 Emergency Medical Responder Course Syllabus Instructor: Assistant Instructor: Instructor Office Hours and Location: One half hour before and after class or by appointment Course Meeting Days and Times:
Emergency Medical Responder Course Syllabus Instructor: Assistant Instructor: Instructor Office Hours and Location: One half hour before and after class or by appointment Course Meeting Days and Times:
(ISBN:9781449604103) Preferred Package Digital Supplement
 College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: gregl@tcdupage.org Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: gregl@tcdupage.org Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
NUCLEARINSTALLATIONSAFETYTRAININGSUPPORTGROUP DISCLAIMER
 NUCLEARINSTALLATIONSAFETYTRAININGSUPPORTGROUP DISCLAIMER Theinformationcontainedinthisdocumentcannotbechangedormodifiedinanywayand shouldserveonlythepurposeofpromotingexchangeofexperience,knowledgedissemination
NUCLEARINSTALLATIONSAFETYTRAININGSUPPORTGROUP DISCLAIMER Theinformationcontainedinthisdocumentcannotbechangedormodifiedinanywayand shouldserveonlythepurposeofpromotingexchangeofexperience,knowledgedissemination
First Aid as a Life Skill. Training Requirements for Quality Provision of Unit Standard-based First Aid Training
 First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015
 2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015 Introduction This document provides the statewide
2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015 Introduction This document provides the statewide
Occupational Health and Safety. Bulletin. Quality Management Plan Requirements for First Aid Training in Alberta Workplaces
 Occupational Health and Safety Bulletin Quality Management Plan Requirements for First Aid Training in Alberta Workplaces FA010 First Aid 1 Table of Contents Introduction... 3 Quality Management Plan (QMP)...
Occupational Health and Safety Bulletin Quality Management Plan Requirements for First Aid Training in Alberta Workplaces FA010 First Aid 1 Table of Contents Introduction... 3 Quality Management Plan (QMP)...
Emergency Medical Technician - Basic
 Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
ALLOW NATURAL DEATH/WITHHOLDING AND/OR WITHDRAWING L I F E - S U S T A I N I N G T R E A T M E N T / NON-BENEFICIAL CARE AND RESUSCITATION POLICY
 PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
PURPOSE SUPPORTIVE DATA To specify the parameters within which decisions regarding the withholding and/or withdrawing of life-sustaining treatment/non beneficial care and/or no initiation of cardiopulmonary
Chapter Review Questions
 1 Chapter Review Questions Chapter 1 1. True or false: As an Emergency Medical Responder, your first priority when responding to any emergency scene is patient care. 2. True or false: The first step in
1 Chapter Review Questions Chapter 1 1. True or false: As an Emergency Medical Responder, your first priority when responding to any emergency scene is patient care. 2. True or false: The first step in
Electrical Safety Health Worker Safety Training Module 6
 Electrical Safety Health Worker Safety Training Module 6 Topics Introduction Key definitions Causes of electric shock Dangers of electric shock Electrical burns The Electrical Safety Model Introduction
Electrical Safety Health Worker Safety Training Module 6 Topics Introduction Key definitions Causes of electric shock Dangers of electric shock Electrical burns The Electrical Safety Model Introduction
EMSPIC State NEMSIS Datasets
 E01_01 Patient Care Report Number X X E01_02 Software Creator X X E01_03 Software Name X X E01_04 Sofware Version X X E02_01 EMS Agency Number X X E02_02 Incident Number X E02_03 EMS Unit (Vehicle) Response
E01_01 Patient Care Report Number X X E01_02 Software Creator X X E01_03 Software Name X X E01_04 Sofware Version X X E02_01 EMS Agency Number X X E02_02 Incident Number X E02_03 EMS Unit (Vehicle) Response
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector
 OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
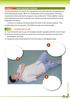 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Automated External Defibrillator
 Automated External Defibrillator 1. INTRODUCTION An automated external defibrillator (AED) is used to treat victims who experience sudden cardiac arrest. It must only be applied to victims who are unconscious,
Automated External Defibrillator 1. INTRODUCTION An automated external defibrillator (AED) is used to treat victims who experience sudden cardiac arrest. It must only be applied to victims who are unconscious,
Confined Space Rescue
 Both the Building Code and Fire Code require us to have a suitable emergency response plan to get our workers to safety. The confined space legislation puts confined space rescue squarely on the shoulders
Both the Building Code and Fire Code require us to have a suitable emergency response plan to get our workers to safety. The confined space legislation puts confined space rescue squarely on the shoulders
MABAS DIVISION XII REHABILITATION POLICY
 MABAS DIVISION XII REHABILITATION POLICY Purpose To ensure that the physical and mental condition of employees operating at the scene of an emergency, training exercise, or other fire department activity
MABAS DIVISION XII REHABILITATION POLICY Purpose To ensure that the physical and mental condition of employees operating at the scene of an emergency, training exercise, or other fire department activity
EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS
 Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
