Patellar Dislocation Conservative and Operative Rehabilitation
|
|
|
- Julia McKinney
- 7 years ago
- Views:
Transcription
1 1 Patellar Dislocation Conservative and Operative Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Patellar stability is dependent upon two components: bony (trochlear groove) and soft tissue structures. There are multiple soft tissue layers that surround the patellofemoral joint. Medially, the superficial layer is consists of the fascia over the sartorius muscle, the second layer contains the medial patellofemoral ligament (MPFL) and the retinaculum, and the third layer contains the medial collateral ligament and joint capsule. The MPFL provides 50-80% of total restraining force medially. Fascial interconnections between fibers of the iliotibial band, lateral hamstrings, lateral collateral ligament, and lateral quadriceps comprise the lateral retinaculum. Pathogenesis: Patellar instability can be correlated with one or more of the following anatomical risk factors: tightness of lateral structures, patella alta, patella or femoral dysplasia, increased Q-angle, increased sulcus angle, generalized laxity, increased femoral anteversion, increased external tibial torsion, lateral position of the tibial tuberosity, abnormal foot pronation, and a vertical vastus medialis oblique (VMO) insertion. Patella dislocation can occur from indirect, twisting or rapid change of direction with the foot planted, or direct trauma to patella. Epidemiology: A higher incidence of patellar dislocations occur in females ages 10 to 17 years of age and the athletically active, with less incidence over age 30. Lateral dislocations are very common and will be the topic of discussion in this guideline. Medially dislocations are typically rare and result from direct trauma, an excessive lateral release or overcorrection of a realignment procedure. Redislocations occur more frequently in patients younger than 20 and tend to decrease with advancing age. Diagnosis History of dislocation with giving way Effusion Positive apprehension test (Fairbank sign) Medial retinacular tenderness Other clinical findings may include: Patellar mobility (Sage test for lateral retinacular tightness positive if medial patellar excursion is less than ¼ of greatest patellar width) Patellar maltracking Abnormal Q angle (normal = males 8-10 degrees, females degrees) Abnormal sulcus angle (normal = <150 degrees) Imaging studies help confirm the diagnosis
2 2 Nonoperative Versus Operative Management: Conservative treatment includes bracing and taping to restore proper patellar alignment and physical therapy to regain strength and range of motion. Conservative treatment is most often attempted first, especially with a first-time dislocation. Operative treatment is recommended in the presence of anatomical abnormalities or osteochondral fractures. It is more effective in preventing recurrence of dislocations and is often only considered after conservative treatment has been unsuccessful. Surgical Procedure: Many different procedures are performed to correct patellar instability. Proximal realignment procedures include lateral release, medial reefing, advancement of the vastus medialis oblique (VMO), and Galleazzi s procedure. Lateral release involves an incision of the lateral retinaculum. Medial reefing involves tightening the medial structures and is often done in conjunction with a lateral release. VMO realignment involves reattaching the VMO insertion more distally and laterally on the patella. The Galeazzi procedure is seldom performed however involves attaching the semitendinosus tendon to the medial side of the patella. Distal realignment consists of transferring the patellar tendon and tibial tubercle medially. Soft tissue distal realignment involves transferring the medial 1/3 of the patellar tendon to the tibial collateral ligament. Evidence has shown that lateral release is more effective when combined with another procedure (i.e. proximal or distal realignment) and for many investigators would only be used it there was a residual patellar tilt after repair/reconstruction of the medial retinacular structures. CONSERVATIVE REHABILITATION (Acute) Note: The following rehabilitation progression after a first-time acute lateral patellar dislocation is a summary of the guidelines provided by D Amato and Bach, published in Clinical Orthopaedic Rehabilitation by S. Brent Brotzman and Kevin E. Wilk. Phase I Goals: Decrease pain and swelling Limit range of motion and weight-bearing to protect healing tissues Return muscle function Avoid overaggressive therapy that may lead the patient into a patellofemoral pain syndrome Bracing: set at 0 degrees initially with ambulation, lateral buttress pad in brace Ice McConnell taping; light compressive bandage Instruction in partial weight-bearing with crutches Electrical stimulation for activation of the VMO
3 3 Supine straight leg raise (SLR) with minimal to no pain Ankle pumps if edema is present Isometric hamstrings Phase II Criteria: no significant joint effusion, no quadriceps extension lag, minimal to no pain with activities of daily living Goals: Full ROM pain-free Improve quadriceps strength Low-level functional activities Initiate conditioning Avoid patellofemoral symptoms or instability Continue patellar bracing or taping Weight-bearing as tolerated; discard crutches when extension lag is no longer present Continue electrical stimulation and modalities as needed Continue supine SLR and add adduction and abduction SLRs Toe raises with equal weight bearing Closed kinetic chain exercises Low-level endurance and pool exercises Phase III Criteria: full active ROM, good to normal quadriceps strength, full weight-bearing with normal gait pattern Goals: Improve function Gradual return to high-level activities Bracing: wean from bracing and taping as quadriceps function improves Four-way hip exercises Pool therapy walking with progression to running Sport and skill-specific training Proprioceptive training Patient education Criteria for Return to Full Activity (8-12 weeks)
4 4 Equal ROM between lower extremities No pain or edema 85% strength compared with uninvolved limb Satisfactory 1-minute single leg hop test, two-legged hop test Patellar stability with clinical tests Preoperative Rehabilitation: Acute Phase: PRICE - protection, rest, ice, compression, elevation (if acute) Maintain quadriceps strength and flexibility of the hamstrings Patellar bracing and taping to restore proper alignment POSTOPERATIVE REHABILITATION Distal and/or Proximal Realignment Procedures Note: The following rehabilitation progression is a summary of the guidelines after a distal and/or proximal realignment procedure provided by D Amato and Bach, published in Clinical Orthopaedic Rehabilitation by S. Brent Brotzman and Kevin E. Wilk. The same rehabilitation protocol is used for both distal and proximal realignment procedures, with a few exceptions noted below. For a combined distal and proximal realignment, the protocol for distal realignment is used. Phase I for Immediate Postoperative Weeks 1-6 Goals: Control inflammation Protect fixation Activation of quadriceps and VMO Full knee extension and minimize adverse effects of immobilization ROM: 0-2 wks 0-30 degrees of flexion, 2-4 wks 0-60 degrees, 4-6 wks 0-90 degrees Brace: 0-4 wks locked in full extension 24 hours 7 days a week except for therapeutic exercises and continuous passive motion use, 4-6 wks unlocked for sleeping, locked for ambulation Weight-bearing: Proximal realignment as tolerated with two crutches, Distal realignment 50% with two crutches Quadriceps sets and isometric adduction with electrical stimulation for VMO (* no electrical stimulation for 6 wks with proximal realignment procedure)
5 5 Heel slides 0-60 degrees (proximal), 0-90 degrees (distal) Non-weight bearing gastrocnemius/soleus, hamstring stretches 4-way SLR with brace locked in full extension Resisted ankle ROM Patellar mobilization (when tolerable) Aquatic therapy at 3-4 wk gait training Phase II Weeks 6-8 Criteria for progression: Good quadriceps set, ~90 degrees of flexion, no signs of active inflammation Goals: Increase flexion Avoid overstressing fixation Control of quadriceps and VMO for proper patellar tracking Brace: discontinue use for sleeping, unlock for ambulation as per physician's orders Weight bearing: As tolerated with crutches Progress to weight-bearing gastrocnemius/soleus stretching, full flexion with heel slides Aquatic therapy Balance exercises Stationary bike low-resistance, high seat Wall slides 0-45 degrees of flexion progress to mini squats Phase III Week 8-4 months Criteria for progression: No quadriceps extensor lag with SLR, nonantalgic gait, no evidence of lateral patellar tracking or instability Discontinue crutches when: no extensor lag with SLR, full extension, nonantalgic gait pattern Step-ups - 2 inches progress to 8 inches Stationary bike moderate resistance Endurance swimming, Stairmaster Gait training 4-way hip exercise Leg press 0-45 degrees of flexion Toe raises, hamstring curls Continue balance activities
6 6 Hamstrings, gastrocnemius/soleus, add quadriceps and iliotibial band stretches Phase IV 4-6 months Criteria for progression: Good to normal quadriceps strength, no soft tissue complaints, no evidence of patellar instability, clearance from physician to progress closed-chain exercises and resume full or partial activity. Progression of closed-kinetic chain exercises Jogging/running in pool with resistance Functional progression, sport-specific training Selected References: Aglietti P, Buzzi R, De Biase P, Giron F. Surgical treatment of recurrent dislocation of the patella. Clin Orthop. 1994;308:8-17. Brotzman SB, Wilk KE. Clinical Orthopaedic Rehabilitation. Philadelphia, Mosby, Inc. pp Fithian DC, Paxton EW, Stone ML, Silva P, Davis D, Elias D, White LM. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med. 2004;32: Garth WP, Pomphrey M, Merrill K. Functional treatment of patellar dislocation in an athletic population. Am J Sports Med. 1996;24: Maenpaa H, Lehto MUK. Surgery in acute patellar dislocation evaluation of the effect of injury mechanism and family occurrence on the outcome of treatment. Br J Sports Med. 1995;29: Myers P, Williams A, Dodds R, Bulow J. The three-in-one proximal and distal soft tissue patellar realignment procedure. Am J Sports Med. 1999;27: Scuderi G. Surgical treatment for patellar stability. Orthop Clin N Am. 1992;23: Vainionpaa S, Laasonen E, Silvennoinen T, Vasenius J, Rokkanen P. Acute Dislocation of the patella. J Bone Joint Surg. 1990;72:366-9.
How To Treat A Patella Dislocation
 Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Rehabilitation Guidelines for Patellar Realignment The knee consists of four bones that form three joints. The femur is the large bone in your thigh, and attaches by ligaments and a capsule to your tibia,
Lateral Retinacular Release of the Patella. and its relation with proximal and distal realignment procedures
 1 Lateral Retinacular Release of the Patella and its relation with proximal and distal realignment procedures Surgical Indications and Considerations Anatomical Considerations: Two components of knee extensor
1 Lateral Retinacular Release of the Patella and its relation with proximal and distal realignment procedures Surgical Indications and Considerations Anatomical Considerations: Two components of knee extensor
PREOPERATIVE: POSTOPERATIVE:
 PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
PREOPERATIVE: ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL Reconstruction Post Operative Rehabilitation Protocol
 ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
ACL Reconstruction Post Operative Rehabilitation Protocol The following is a generalized outline for rehabilitation following ACL reconstruction. The protocol may be modified if additional procedures,
William J. Robertson, MD UT Southwestern Orthopedics 1801 Inwood Rd. Dallas, TX 75390-8882 Office: (214) 645-3300 Fax: (214) 3301 billrobertsonmd.
 Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Anterior Cruciate Ligament Reconstruction Postoperative Rehab Protocol You will follow-up with Dr. Robertson 10-14 days after surgery. At this office visit you will also see one of his physical therapists.
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW Health Sports Rehabilitation Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
Cincinnati Sportsmedicine and Orthopaedic Center
 Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
Cincinnati Sportsmedicine and Orthopaedic Center Total Knee Replacement: Rehabilitation Protocol This rehabilitation protocol was developed for patients who have had a cemented total knee arthroplasty.
MEDIAL PATELLA FEMORAL LIGAMENT RECONSTRUCTION Rehab Protocol
 Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Rehab Protocol This rehabilitation protocol has been designed for patients who have undergone an MPFL reconstruction. Dependent upon the particular procedure, this protocol also may be slightly deviated
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol
 Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
Post-Operative ACL Reconstruction Functional Rehabilitation Protocol Patient Guidelines Following Surgery The post-op brace is locked in extension initially for the first week with the exception that it
POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL
 Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Corey A. Wulf, MD POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POSTOPERATIVE REHABILITATION PROTOCOL The range of motion allowed after posterior cruciate ligament reconstructive surgery is dependent upon
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon
 Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
Make sure you check with the surgeon before you start using any protocol. Also, obtain a copy of the post-operative report from the surgeon Knee Arthroscopy Physical Therapy Protocol This rehabilitation
Theodore B. Shybut, M.D. 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521. Sports Medicine
 Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Anterior Cruciate Ligament Reconstruction Accelerated Rehab This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning to a high level of activity as quickly
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction
 Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Noyes Knee Institute Rehabilitation Protocol: Medial Ligament Repair or Reconstruction Brace: Long-leg postoperative Custom unloading if required minimum goals: 0-90 0-110 0-120 0-130 Weight bearing: Toe
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe
 Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Knee Arthroscopy/Lateral Release Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol is designed for patients who have undergone knee arthroscopy or arthroscopic lateral release. The intensity
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Walter R. Lowe This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Introduction: This rehabilitation protocol is designed for patients with ACL injuries who anticipate returning early to a high
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION Hamstring Graft/PTG-Accelerated Rehab
 The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
The rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning early to a high level of activity postoperatively. The ACL Rehabilitation protocol for all three
AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY
 Frisbie Memorial Hospital Marsh Brook Rehabilitation Services Wentworth-Douglass Hospital AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY FREQUENCY: 2-3 times per week. DURATION: 4-6 weeks
Frisbie Memorial Hospital Marsh Brook Rehabilitation Services Wentworth-Douglass Hospital AQUATIC/LAND BASED CLINICAL PROTOCOL FOR GRADE I/II MCL INJURY FREQUENCY: 2-3 times per week. DURATION: 4-6 weeks
Anterior Cruciate Ligament Reconstruction. ACL Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Anterior Cruciate Ligament Reconstruction Rehab Protocol This rehabilitation protocol has been designed for patients following ACL reconstruction who anticipate returning to a high level of activity as
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities
 Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Noyes Knee Institute Rehabilitation Protocol for Primary ACL Reconstruction: Early Return to Strenuous Activities 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: immobilizer for patient comfort () minimum goals:
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol GENERAL CONSIDERATIONS * This handout serves as a general outline for you as a patient to better understand guidelines and time frames
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
The Insall Scott Kelly Center for Orthopaedics and Sports Medicine 210 East 64th Street, 4 th Floor, New York, NY 10065
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE REHABILITATION PROTOCOL 2003 AUTOGRAFT BONE-PATELLA TENDON-BONE and ALLOGRAFT PROTOCOL PHASE I-EARLY FUNCTIONAL (WEEKS 1-2) Goals: 1. Educate re:
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
GALLAND/KIRBY ACL RECONSTRUCTION WITH MENISCUS REPAIR POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered,
Progression to the next phase is based on Clinical Criteria and/or Time Frames as appropriate.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Phyp Physical Therapy Total Hip Arthroplasty/ Hemiarthroplasty Protocol: The intent of this protocol is to provide the clinician with
REHABILITATION PROTOCOL
 COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
COSM REHAB ANOTHER SERVICE PROVIDED BY THE CENTER FOR ORTHOPAEDICS & SPORTS MEDICINE REHABILITATION PROTOCOL KNEE ACL Reconstruction Protocol Please contact us with any questions. www.pacosm.com Indiana
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Post Surgery Rehabilitation Program
 Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Post Surgery Rehabilitation Program Medial Patellofemoral Ligament Reconstruction and Imbrication This protocol is designed to assist you with your rehabilitation after surgery and should be followed under
Medial Collateral Ligament (MCL) Rehabilitation Protocol
 Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Introduction: This rehabilitation protocol is designed for patients with Medial Collateral Ligament (MCL) Rehabilitation Protocol MCL injuries who require an early return to high level activity following
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees
 Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
Noyes Knee Institute Rehabilitation Protocol for ACL Reconstruction: Revision Knees, Allografts, Complex Knees 1-2 3-4 5-6 7-8 9-12 4 5 6 7-12 Brace: postoperative & functional () minimum goals: 0-90 0-120
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING. Minni Titicula
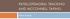 PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
Inland Orthopaedic Surgery & Sports Medicine
 Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Inland Orthopaedic Surgery & Sports Medicine Dr. Ed Tingstad 825 SE Bishop Blvd., Suite 120 Pullman, WA 99163 (509)332-2828 ACL Rehabilitation Guidelines General Guidelines: The following ACL rehabilitation
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Posterior Cruciate Ligament Reconstruction and Rehabilitation
 1 Posterior Cruciate Ligament Reconstruction and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Many authors describe the posterior cruciate ligament (PCL) as the primary
1 Posterior Cruciate Ligament Reconstruction and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: Many authors describe the posterior cruciate ligament (PCL) as the primary
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY
 B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
B. TED MAURER, MD POSTOPERATIVE REHABILITATION PROTOCOL TOTAL KNEE ARTHROPLASTY Goals addressed prior to discharge from hospital setting: Independence with bed mobility, transfers (supine to sit and sit
Meniscus Repair Rehabilitation Dr. Walter R. Lowe
 Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Meniscus Repair Rehabilitation Dr. Walter R. Lowe This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Meniscal repairs located in the vascular zones of the periphery
Post Surgery Rehabilitation Program for Knee Arthroscopy
 Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Post Surgery Rehabilitation Program for Knee Arthroscopy This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist May
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes
 Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
Meniscus Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol was developed for patients who have isolated meniscal repairs. Depending upon the complexity of the tear
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella)
 EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Knee Arthroscopy (Meniscectomy)
 Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Knee Arthroscopy (Meniscectomy) Anatomy and Biomechanics The knee is a hinge joint at the connection point between the femur and tibia bones. It is held together by several important ligaments. The knee
Cincinnati SportsMedicine and Orthopaedic Center
 Cincinnati SportsMedicine and Orthopaedic Center Medial Collateral Ligament Reconstruction Rehabilitation Protocol* This rehabilitation protocol was developed for patients who have had medial collateral
Cincinnati SportsMedicine and Orthopaedic Center Medial Collateral Ligament Reconstruction Rehabilitation Protocol* This rehabilitation protocol was developed for patients who have had medial collateral
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
ACL Non-Operative Protocol
 ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
ACL Non-Operative Protocol Anatomy and Biomechanics The knee is a hinge joint connecting the femur and tibia bones. It is held together by several important ligaments. The most important ligament to the
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Eastern Suburbs Sports Medicine Centre
 Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
Eastern Suburbs Sports Medicine Centre ACCELERATED ANTERIOR CRUCIATE LIGAMENT REHABILITATION PROGRAM Alan Davies Diane Long Mark Kenna (APA Sports Physiotherapists) The following ACL reconstruction rehabilitation
HIPABDUCTOR REPAIR PROTOCOL (Gluteus Medius/Minimus Repair)
 R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
R. JOHN ELLIS, JR., M.D. LAWRENCE A. SCHAPER, M.D. MARK G. SMITH, M.D. G. JEFFREY POPHAM, M.D. AKBAR NAWAB, M.D. MICHAEL SALAMON, M.D. MATTHEW PRICE, M.D. DANIEL RUEFF, M.D. ELLIS & BADENHAUSEN ORTHOPAEDICS,
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth)
 Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
Dr Doron Sher MB.BS. MBiomedE, FRACS(Orth) Knee, Shoulder, Elbow Surgery ACL REHABILITATION PROGRAM (With thanks to the Eastern Suburbs Sports Medicine Centre) The time frames in this program are a guide
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Rehabilitation after ACL Reconstruction: From the OR to the Playing Field. Mark V. Paterno PT, PhD, MBA, SCS, ATC
 Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Objectives Rehabilitation after ACL Reconstruction: From the OR to the Playing Field Mark V. Paterno PT, PhD, MBA, SCS, ATC Coordinator of Orthopaedic and Sports Physical Therapy Cincinnati Children s
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Post-Operative Exercise Program
 785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
785 E. Holland Spokane, WA 99218 (877) 464-1829 (509) 466-6393 Fax (509) 466-3072 Knee Joint Replacement Surgery Weeks 1 through 6 The goal of knee replacement surgery is to return you to normal functional
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Steps to Success: A Guide to Knee Rehabilitation
 Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Steps to Success: A Guide to Knee Rehabilitation Indications Carticel (autologous cultured chondrocytes) is indicated for the repair of symptomatic, cartilaginous defects of the femoral condyle (medial,
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
Anterior Knee Pain: Patellofemoral Pain a review
 Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
What is petellofemoral Pain syndrome?
 Jackie Davis What is petellofemoral Pain syndrome? Patellofemoral Syndrome can be defined as retropatellar or peripatellar pain resulting from physical and biochemical changes in the patellofemoral joint.
Jackie Davis What is petellofemoral Pain syndrome? Patellofemoral Syndrome can be defined as retropatellar or peripatellar pain resulting from physical and biochemical changes in the patellofemoral joint.
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair
 Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
Rehabilitation Guidelines for Posterior Shoulder Reconstruction with or without Labral Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a
ACL Reconstruction Protocol
 ACL Reconstruction Protocol The primary emphasis of this ACL rehab protocol is on functional weight bearing exercises with a focus on restoring the balance between the quadriceps and hamstrings muscles,
ACL Reconstruction Protocol The primary emphasis of this ACL rehab protocol is on functional weight bearing exercises with a focus on restoring the balance between the quadriceps and hamstrings muscles,
Rehabilitation Guidelines for Autologous Chondrocyte Implantation. Ashley Conlin, PT, DPT, SCS, CSCS
 Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation Guidelines for Autologous Chondrocyte Implantation Ashley Conlin, PT, DPT, SCS, CSCS Objectives Review ideal patient population Review overall procedure for Autologous Chondrocyte Implantation
Rehabilitation After Knee Meniscus Repair
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Rehabilitation After Knee Meniscus Repair Phase One: The first week after surgery Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Charles C. Lind, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation
ChondroCelect Rehabilitation Program
 ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
ChondroCelect Rehabilitation Program Rehabilitation differs depending on the type and site of the lesion and the patient personal profile. Grouping of the lesions and patient profiles is helpful to ensure
Radial Head Fracture Repair and Rehabilitation
 1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
1 Radial Head Fracture Repair and Rehabilitation Surgical Indications and Considerations Anatomical Considerations: The elbow is a complex joint due to its intricate functional anatomy. The ulna, radius
Cincinnati SportsMedicine and Orthopaedic Center
 Cincinnati SportsMedicine and Orthopaedic Center Anterior Cruciate Ligament Reconstruction: Accelerated Rehabilitation Protocol* This rehabilitation protocol was developed for patients who have anterior
Cincinnati SportsMedicine and Orthopaedic Center Anterior Cruciate Ligament Reconstruction: Accelerated Rehabilitation Protocol* This rehabilitation protocol was developed for patients who have anterior
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee.
 Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando ANTERIOR CRUCIATE
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hamstring Apophyseal Injuries in Adolescent Athletes
 Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
ORTHOPAEDIC KNEE CONDITIONS AND INJURIES
 11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
Patella Realignment Tibial Tuberosity Transfer with Lateral Release
 Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Patella Realignment Tibial Tuberosity Transfer with Lateral Release Alan M. Reznik, M.D. The Orthopaedic Group, LLC The knee is made of three bones, the kneecap (patella), the shin bone (tibia) and thigh
Indications for Treatment: Indications for treatment include pain, swelling, instability, loss of mobility and function.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy ICD 9 Codes: 844.1 Case Type / Diagnosis: The anatomy of the medial knee has been divided into 3 layers, consisting of
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy ICD 9 Codes: 844.1 Case Type / Diagnosis: The anatomy of the medial knee has been divided into 3 layers, consisting of
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
UW Health Sports Rehabilitation Rehabilitation Guidelines for Posterior Cruciate Ligament Reconstruction The knee has three joints--the patellofemoral joint (knee cap), the tibiofemoral joint and the tibiofibular
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Total Knee Arthroplasty. TKA - Indications. Technical Goals - TKA. Prosthesis parallel to Floor/Stance. Mechanical Axis/Center of Joint
 Total Knee Arthroplasty TKA - Indications Osteoarthritis Rheumatoid Arthritis Post Traumatic Arthritis Osteonecrosis Tumor Technical Goals - TKA Prosthesis parallel to Floor/Stance Mechanical Axis/Center
Total Knee Arthroplasty TKA - Indications Osteoarthritis Rheumatoid Arthritis Post Traumatic Arthritis Osteonecrosis Tumor Technical Goals - TKA Prosthesis parallel to Floor/Stance Mechanical Axis/Center
Anterior Cruciate Ligament Reconstruction
 1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL
 REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
REHABILITATION GUIDELINES AUTOLOGOUS CHONDROCYTE IMPLANTATION USING CARTICEL Michael M. Reinold, PT, ATC Kevin E. Wilk, PT Jeffrey R. Dugas, MD E. Lyle Cain, MD Scott D. Gillogly, MD The following has
Rehabilitation. Modalities and Rehabilitation. Basics of Injury Rehabilitation. Injury Rehabilitation. Vocabulary. Vocabulary
 Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Modalities and Rehabilitation Rehabilitation Chapter 12: Basics of Injury Rehabilitation Vocabulary Balance: ability to maintain our center of gravity over a base of support Kinesthesia: the ability to
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair
 Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Rotator Cuff Surgery: Post-Operative Protocol for Mini-Open or Arthroscopic Rotator Cuff Repair Considerations: 1. Mini-Open - shoulder usually assessed arthroscopically and acromioplasty is usually performed.
Goals. Our Real Goals. Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas. Perform a basic, logical, history and physical exam
 Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
