Procedure 17: Cardiopulmonary Resuscitation
|
|
|
- Violet Watts
- 7 years ago
- Views:
Transcription
1 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually begins as a primary respiratory arrest. This is in contrast to adults, in whom CPA or sudden death is almost always a primary cardiac event that occurs with onset of ventricular fibrillation and an abrupt change in the heart s electrical activity. Because cessation of effective breathing is the precipitating factor in pediatric CPA, airway management and ventilation are to children in CPA what defibrillation is to adults. Cardiopulmonary resuscitation (CPR) refers to basic airway management, artificial ventilation, and chest compressions to provide oxygen and circulation to Indications Newly born, neonate, infant, or child of any age who is apneic and pulseless Newly born with a heart rate less than 60 beats/min and not improving after standard newborn care Neonate, infants and children with a heart rate less than 60 beats/min and poor perfusion. Contraindication Newly born, infant, or child with effective perfusion (palpable central or peripheral pulse) Equipment Mouth-to-mask device Bag-mask device, infant or child Airway adjuncts Appropriate mask sizes core organs: the heart, brain, and lungs. In children, CPR has been shown to improve survival from drowning, and it may also benefit patients in CPA from other causes. Rationale CPR encompasses the basic procedures for sustaining critical oxygenation, ventilation, and perfusion recommended by the American Heart Association. The pediatric techniques are slightly modified from the adult techniques to reflect the known differences in CPA between age groups. Furthermore, there are specific differences between infants and children, including number of rescuers, placement of hands and fingers, rates of ventilation, and rates and depth of chest compressions. Preparation 1. Position a child on a hard surface. Position a neonate or infant on a hard surface or on the forearm of the rescuer with the hand supporting the head Assess Responsiveness Assess responsiveness. If unresponsive, assess breathing.
2 350 Cardiopulmonary Resuscitation 17-2 Assess Breathing Open airway using either the headtilt/chin-lift maneuver (medical patient) or modified jaw thrust maneuver (trauma patient) to achieve a neutral position. If spinal injury is possible, have a second rescuer maintain manual spinal stabilization. Remove any obvious obstructions, such as loose teeth or vomitus. Look, listen, and feel for signs of breathing. Manipulation of the head to keep the airway in a neutral position is essential for effective ventilation. A towel roll under the shoulders of the infant or small child may help maintain neutral head position. Compression Rates These are the timing rates for single rescuers, not the actual number of compressions delivered each minute because of pauses for ventilations and reassessments. Newly born: At least 120 events/min Neonate and infant: 100 compressions/min Child 1 8 years: 100 compressions/min Child over 8 years: 100 compressions/min Possible Complications Coronary vessel injury Diaphragm injury Hemopericardium Hemothorax Interference with ventilation Liver injury Myocardial injury Pneumothorax Rib fractures Spleen injury Sternal fracture
3 Cardiopulmonary Resuscitation Ventilation Rate If not breathing, begin mouth-to-mask ventilation, or perform bag-mask ventilation with 100% oxygen. Give two initial breaths at a rate of 1 second per breath. If breaths now expand the chest, assess pulse. Take no more than 10 seconds. Slowly repeat squeeze-release-release to time bag-mask ventilation rate. If first breath does not expand the chest, reposition the head and attempt again. If breaths are still ineffective, suction the mouth with a bulb syringe or flexible suction catheter (newly born) or a large-bore rigid suction catheter (neonates, infants, and children) and attempt breaths again. If pulse is present ( 60 beats/min), but the victim is still not breathing, continue ventilations. Give one every 2 seconds in newly born and rescue breaths at a rate of 12 to 20 breaths per minute (every 3 to 5 seconds) until spontaneous breathing resumes. Use the E-C clamp technique to achieve a good mask seal and watch for adequate chest rise to ensure effective ventilation. Continuously assess effectiveness of CPR by ensuring chest rise and feeling for a palpable pulse every 2 minutes.
4 352 Cardiopulmonary Resuscitation 17-4 Compression Rate Check central pulse. Newly born: umbilical cord stump or listen to precordium. Neonate and infant: brachial pulse or femoral pulse. Child: carotid pulse. If pulse is absent or if heart rate is less than 60 beats/min, with shock or poor peripheral perfusion, begin chest compressions. Newly born: 3 compressions: 1 ventilation. Neonate, infant, and child: one rescuer 30 compressions: 2 ventilations, two rescuers 15 compressions: 2 ventilations. Use proper compression technique, compression-ventilation ratio, depth of compression, and compression-release ratio (Tables P17-1 and P17-2). Table P17-1 Compression and Ventilation Rates per Minute* Rate of Rescue Breaths per Minute Rescue Breaths per Minute Age Compressions (min) without Compressions with Compressions (mouth to mouth or mask) with Advanced Airway Newly born (<1 day) Neonate (1 28 days) and infant (1 12 months) Child 1 8 years Child over 8 years One or two rescuers *The rate of compressions and the actual number of compressions delivered per minute are different. The rate of compressions refers to the timing of compressions when they are being performed, and the rate does not account for pauses for breathing. Delivered compressions are the actual number of compressions delivered per minute after accounting for breathing. The ratios are calculated from the timing rates, not the delivered rates. Table P17-2 Parameters for BLS Resuscitation for Health Care Providers Compressions Compression to Depth Hand Placement Age (min) Ventilation Ratio (in) for Compression Newly born 120 3:1 1 /3 depth of chest 2 fingers at lower 1 / 3 of sternum, 1 finger (< 1 day) below nipple line, or 2 thumbs at midsternum with hands encircling chest Neonate (1 28 days) /3 to 1 / 2 depth of chest One rescuer 30:2 2 or 3 fingers at lower 1 / 3 of sternum, 1 finger below nipple line Two rescuers 15:2 2 thumbs at midsternum with hands encircling chest Infant (1 12 months) /3 to 1 / 2 depth of chest One rescuer 30:2 2 fingers at midsternum, 1 finger below nipple line Two rescuers 15:2 2 thumbs at lower 1 / 2 of sternum with hands encircling chest Child 1 8 years /3 to 1 / 2 depth of chest Heel of 1 or 2 hands at lower 1 / 2 of sternum One rescuer 30:2 (do not push on xiphoid process) Two rescuers 15:2 Child over 8 years : inches Heel of one hand, other hand on top, One or two at lower 1 / 2 of sternum between nipples rescuers
5 Cardiopulmonary Resuscitation Finger or Hand Placement Newly born: Use the two thumb encircling chest method for the newborn. The two finger method is acceptable, but should be used when the two thumb method is not easily accomplished. Compression depth should be one third of chest depth. Two thumb technique: encircle the chest and use thumbs just below the intermammary line with the fingers supporting the spine. Two finger technique: Use two fingers on the lower 1 / 3 of the sternum just below the intermammary line, with the other hand supporting the spine. Child (1 to 8 years old): Use the heel of one hand on the sternum above the xiphoid process. Compression depth should be one third to one half the depth of the chest. Child (> 8 years): Use the heel of both hands on the sternum above the xiphoid process. Lay rescuers and lone health care providers use two finger technique. Two health care providers use two thumbs encircling hands technique Compressions The depth of chest compressions should be approximately one third to one half the depth of the chest. Compressions should be deep enough to produce a palpable brachial, femoral, or carotid pulse. Push hard and fast and release completely to allow chest to fully rise. Use the two-rescuer technique when possible. Reassessment: Check pulse after approximately every 5 compressionventilation cycles. A common problem in the transition from one-rescuer to two-rescuer child CPR is the lack of coordination between ventilations and compressions.
6 354 AED and Defibrillation Procedure 18: AED and Defibrillation Introduction Synchronized cardioversion for tachydysrhythmias has long been part of adult emergency care and is one of the most effective treatments for sudden cardiac arrest from ventricular dysrhythmias. However, ventricular dysrhythmias are rare in children, especially in infants, and pediatric supraventricular tachycardia (SVT) is usually treatable with medical therapy. For these reasons, pediatric synchronized cardioversion is not often indicated. However, when a child develops ventricular fibrillation or pulseless ventricular tachycardia, defibrillation (unsynchronized cardioversion) may be lifesaving. Also, synchronized cardioversion may resuscitate a child in shock with SVT. Use the Indications Ventricular fibrillation Pulseless ventricular tachycardia SVT with shock and no vascular access rapidly available (synchronized) Ventricular tachycardia with shock and unresponsiveness with pulse and no vascular access rapidly available Atrial fibrillation or atrial flutter with shock Contraindication Conscious patient with good perfusion Equipment Automatic external defibrillator Standard defibrillator Newer models feature lower power outputs to deliver lower energy countershocks synchronized mode when there is SVT or ventricular tachycardia with a pulse, and the asynchronized (defibrillation) mode for ventricular fibrillation or ventricular tachycardia without a pulse. Rationale When a child s heart deteriorates into ventricular tachycardia or fibrillation, there is usually a severe systemic insult such as profound hypoxia, ischemia, electrocution, or myocarditis. Death may result if treatment is delayed. SVT, in contrast, is usually a more stable cardiac rhythm. When the child is pulseless and has ventricular fibrillation or ventricular tachycardia, perform defibrillation as quickly as possible with the appropriate technique. If a child has SVT or ventricular tachycardia and shock, use synchronized cardioversion. Do not attempt to perform synchronized cardioversion on a child with SVT who is well perfused. Preparation 1. Open airway and ventilate with bag-mask device with 100% oxygen while assembling equipment for cardioversion or defibrillation. 2. If child is pulseless, begin closed-chest compressions, until automatic external defibrillator (AED) or conventional defibrillator is available. Do not deliver synchronized cardioversion to a conscious child with SVT or ventricular tachycardia unless the child is in shock and has no IV or IO access rapidly available for medical treatment. For a child with ventricular fibrillation or pulseless ventricular tachycardia, use the asynchronized (defibrillation) mode.
7 AED and Defibrillation Conventional Defibrillator Use Apply the paddles directly to the skin. Place one paddle on the anterior chest wall on the right side of the sternum inferior to the clavicle and the other paddle on the left midclavicular line at the level of the xiphoid process. As another option, use the anterior-posterior position. Begin recording rhythm. Deliver the electrical countershock with firm pressure. per EMS protocol. Treat bradycardia or other dysrhythmias. Assess the patient for evidence of reperfusion and check the monitor for the rhythm. Clear the nearby area to avoid shocking someone. Announce, I am going to shock on three. One, I am clear. Two, you are clear. Three, everybody is clear. If the first electrical shock is unsuccessful, deliver additional electrical countershocks as per EMS protocol. Give specific dysrhythmia treatment with epinephrine or other drugs, as The preferred paddle location in children is controversial and no study in humans has compared the two techniques. Anterior chest wall placement has the advantage of a supine child and easier airway management. Anterior-posterior placement may allow larger paddles and more effective delivery of the charge. Preparation Conventional Defibrillator Use 1. Select the proper paddle size. Use the 8-cm adult paddles if these will fit on the chest wall; otherwise, use the 4.5-cm pediatric paddles (Table P18-1). 2. Prep paddles or skin electrodes with electrode jelly, paste, or saline-soaked gauze pads, or use self-adhesive defibrillator pads. Do not let jelly or paste from one site touch the other and form an electrical bridge between sites, which could result in ineffective defibrillation or skin burns. 3. Establish appropriate electrical charge (Table P18-2). 4. Select synchronized or asynchronized mode. 5. Properly charge pack and stop chest compressions. Table P18-1 Paddle Size 8-cm adult paddles (Use in children over 12 months of age or weighing more than 10 kg) On anterior chest wall, OR Anterior-posterior 4.5-cm pediatric paddles (Use in infants up to 12 months of age or weighing less than 10 kg) on the anterior chest wall Failure to firmly apply paddles to the chest wall will decrease effective delivery of charge.
8 356 AED and Defibrillation 18-2 One Rescuer with an AED For children under 8 years of age use a child-pad cable system if available. There are inadequate data to recommend AED use for the child less than 1 year of age. Verify unresponsiveness. Check for signs of circulation. If there are no signs of circulation, attach the AED and proceed with the AED treatment algorithm. The AED operator should take the following actions. ATTACH the AED. Select the correct pads for victim s size and age (adult vs. child). Peel the backing from the pads. Attach the adhesive pads to the victim as shown on the pads. (If only adult pads are available, and they overlap when placed on the chest, use an anterior [chest] and posterior [back] placement.) Attach the electrode cable to the AED (if not preconnected). Open the airway, and check for breathing. POWER ON the AED and follow voice prompts. Some devices will turn on when the AED lid or carrying case is opened. Allow the AED to ANALYZE the victim s rhythm ( clear victim during analysis). Deliver a SHOCK if needed ( clear victim before shock). If the victim is not breathing effectively, give two ventilations. Reasonable variations in this sequence are acceptable. Table P18-2 Appropriate Electrical Charge for Countershock Dysrhythmia Mode Charge Ventricular fibrillation Defibrillation 2 J/kg, then 4 J/kg, then 4 J/kg, Ventricular tachycardia (asynchronized) as needed. without a pulse Then 4 J/kg after CPR and each dose of medication. Ventricular tachycardia Synchronized J/kg. Repeat as needed. with pulse SVT Atrial fibrillation and atrial flutter with shock Possible Complications Ineffective delivery of countershock because of failure to charge, improper positioning on the chest, incorrect paddle size, or improper conduction medium Burns on the chest wall Failure to clear before voltage discharge, leading to electrical shock of a team member or bystander Tachydysrhythmia Bradycardia Myocardial damage or necrosis Cardiogenic shock Embolic phenomena
9 AED and Defibrillation Two Rescuer AED Sequence of Action Adapted from Circulation 2005: 112: IV Verify unresponsiveness. If victim is unresponsive, have partner call Get AED. Open airway: head-tilt/chin-lift (or jaw thrust if trauma is suspected). Check for effective breathing: provide breathing if needed. Check for breathing (look, listen, and feel). If not breathing, give two slow breaths. A mouthto-mask device should be available in the AED carrying case. Check for signs of circulation: if no signs of circulation are present, perform these steps. Perform chest compressions and prepare to attach the AED. If there is any doubt that the signs of circulation are present, the first rescuer initiates chest compressions while the second rescuer prepares to use the AED. Remove clothing covering the victim s chest to provide chest compressions and apply the AED electrode pads. Attempt defibrillation with the AED if no signs of circulation are present. Place the AED near the rescuer who will be operating it. The AED is usually placed on the side of the victim opposite the rescuer who is performing CPR. The rescuer begins performing CPR while the rescuer who was performing CPR prepares to operate the AED. (It is acceptable to reverse these roles.) ATTACH the AED to the victim. Select correct pads for the victim s size and age. Peel the backing from the pads. Ask the rescuer performing CPR to stop chest compressions. Attach the adhesive pads to the victim as shown on the pads. (If only adult pads are available, and they overlap when placed on the chest, use an anterior [chest] and posterior [back] placement.) Attach the AED connecting cables to the AED (if not preconnected). ANALYZE rhythm. Clear the victim before and during analysis. Check that no one is touching the victim. Press the ANALYZE button to start rhythm analysis (some brands of AEDs do not require this step). Shock Indicated message. Resume CPR until AED is charged and ready to deliver shock. Clear the victim once more before pushing the SHOCK button (I m clear, you re clear, everybody s clear ). Check that no one is touching the victim. Press the SHOCK button (victim may display muscle contractions). No Shock Indicated message. Check for signs of circulation (including a pulse). If signs of circulation are present, check breathing. If breathing is inadequate, assist breathing. If breathing is adequate, place the victim in the recovery position, with the AED attached. The AED operator takes the following actions. POWER ON the AED first (some devices will turn on automatically when the AED lid or carrying case is opened). If no signs of circulation are present, resume CPR for 5 cycles, then recheck for signs of circulation. If there are still no signs of circulation, analyze rhythm, repeat the analyze rhythm step, then follow the shock indicated or no shock indicated steps as appropriate.
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
BLS for Healthcare Providers Study Guide and Pretest
 BLS for Healthcare Providers Study Guide and Pretest Adult CPR 1-Rescuer CPR Sequence check for responsiveness if no response, activate 911 and get the AED open the airway look, listen, & feel for breathing
BLS for Healthcare Providers Study Guide and Pretest Adult CPR 1-Rescuer CPR Sequence check for responsiveness if no response, activate 911 and get the AED open the airway look, listen, & feel for breathing
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED)
 EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Heart of America Medical Center EMR, EMT, EMT-Intermediate & AEMT Protocols
 USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
USE OF THE LUCAS DEVICE TO PROVIDE EXTERNAL CHEST COMPRESSIONS IN PATIENTS SUFFERING CARDIAC ARREST Purpose This procedure describes the appropriate methods to apply, operate, and discontinue the LUCAS
BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID)
 BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID) 1. THIS BLS FOR HEALTHCARE PROVIDERS COURSE IS GIVEN TO: a. Nurses, Doctors, Paramedics, & Healthcare Workers.
BLS PRETEST BASIC LIFE SUPPORT FOR HEALTHCARE PROVIDERS (CREATED BY LAST MINUTE CPR & FIRST AID) 1. THIS BLS FOR HEALTHCARE PROVIDERS COURSE IS GIVEN TO: a. Nurses, Doctors, Paramedics, & Healthcare Workers.
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Allina Emergency Medicine Education Healthcare Provider. CPR Study Guide. American Heart Association 2010 Guidelines
 Allina Emergency Medicine Education Healthcare Provider CPR Study Guide American Heart Association 2010 Guidelines The American Heart Association strongly promotes knowledge and proficiency in BLS< ACLS
Allina Emergency Medicine Education Healthcare Provider CPR Study Guide American Heart Association 2010 Guidelines The American Heart Association strongly promotes knowledge and proficiency in BLS< ACLS
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest ANNOTATED ANSWER KEY February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses
American Heart Association Basic Life Support for Healthcare Providers Pretest ANNOTATED ANSWER KEY February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses
Heart information. CPR cardiopulmonary resuscitation
 Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Basic life support (BLS) Techniques
 module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
The purpose of this course is to outline the American Heart Association s guidelines for CPR, the use of AEDs, and the Heimlich maneuver.
 CPR Cardiopulmonary Resuscitation WWW.RN.ORG Reviewed May, 2016, Expires May, 2018 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2016 RN.ORG, S.A., RN.ORG,
CPR Cardiopulmonary Resuscitation WWW.RN.ORG Reviewed May, 2016, Expires May, 2018 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2016 RN.ORG, S.A., RN.ORG,
Infant CPR Skills Testing Checklist
 Infant CPR Skills Testing Checklist Student Name Date of Test Scenario: While you are pushing a baby in a stroller at the park, you notice something is wrong with the baby. You do not have a phone nearby.
Infant CPR Skills Testing Checklist Student Name Date of Test Scenario: While you are pushing a baby in a stroller at the park, you notice something is wrong with the baby. You do not have a phone nearby.
In-hospital resuscitation. Superseded by
 6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
BASIC LIFE SUPPORT - ADULT
 BASIC LIFE SUPPORT - ADULT First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised 12 months
BASIC LIFE SUPPORT - ADULT First Issued by/date BKW PCT May 2003 Issue Version Purpose of Issue/Description of Change 3 Policy reviewed. No changes in procedure or legislation since policy revised 12 months
HOW TO USE THE LIFEPAK 1000 DEFIBRILLATOR 3
 3 How to Use the LIFEPAK 1000 Defibrillator HOW TO USE THE LIFEPAK 1000 DEFIBRILLATOR 3 This section provides an overview of information and instructions for using the LIFEPAK 1000 defibrillator. Modes
3 How to Use the LIFEPAK 1000 Defibrillator HOW TO USE THE LIFEPAK 1000 DEFIBRILLATOR 3 This section provides an overview of information and instructions for using the LIFEPAK 1000 defibrillator. Modes
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
American Heart Association. BLS Instructor Course. Written Examination. July 2003
 American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
Cardiac and Pulmonary Issues in the Elite Athlete. Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015
 Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Cardiac and Pulmonary Issues in the Elite Athlete Keep Your Edge Hockey Sports Medicine 2015 Toronto August 28-30 2015 THORACIC EMERGENCIES Hockey related thoracic trauma is blunt Injury to the boney
Orientation Guide www.lucas-cpr.com a product by JOLIFE 900080-00 RevB JOLIFE 2012
 Orientation Guide www.lucas-cpr.com a product by JOLIFE 900080-00 RevB JOLIFE 2012 Refer to the Instructions for Use for complete directions for use, indications, contraindications, warnings, precautions
Orientation Guide www.lucas-cpr.com a product by JOLIFE 900080-00 RevB JOLIFE 2012 Refer to the Instructions for Use for complete directions for use, indications, contraindications, warnings, precautions
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Use of the A-B-C basic life support sequence.
 Basic Life Support A change in the basic life support (BLS) sequence of steps for trained rescuers from A-B-C (Airway, Breathing, Chest compressions) to C-A-B (Chest compressions, Airway, Breathing) for
Basic Life Support A change in the basic life support (BLS) sequence of steps for trained rescuers from A-B-C (Airway, Breathing, Chest compressions) to C-A-B (Chest compressions, Airway, Breathing) for
EMBARGOED FOR RELEASE
 Systems of Care and Continuous Quality Improvement Universal elements of a system of care have been identified to provide stakeholders with a common framework with which to assemble an integrated resuscitation
Systems of Care and Continuous Quality Improvement Universal elements of a system of care have been identified to provide stakeholders with a common framework with which to assemble an integrated resuscitation
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
CPR /AED for Professional Rescuers
 CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100
 U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100 DEVELOPMENT This subcourse is approved for resident and correspondence
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 CARDIAC IMPAIRMENT SUBCOURSE MD0571 EDITION 100 DEVELOPMENT This subcourse is approved for resident and correspondence
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
R Series Quick Reference Guide
 R Series Quick Reference Guide 2010 ZOLL Medical Corporation. All rights reserved. CPR Index, OneStep, R Series, Real CPR Help, See-Thru CPR, statpadz, and ZOLL are trademarks or registered trademarks
R Series Quick Reference Guide 2010 ZOLL Medical Corporation. All rights reserved. CPR Index, OneStep, R Series, Real CPR Help, See-Thru CPR, statpadz, and ZOLL are trademarks or registered trademarks
Adult Basic Life Support
 2 Adult Basic Life Support Introduction This chapter contains the guidelines for out-of-hospital, single rescuer, adult basic life support (BLS). Like the other guidelines in this publication, it is based
2 Adult Basic Life Support Introduction This chapter contains the guidelines for out-of-hospital, single rescuer, adult basic life support (BLS). Like the other guidelines in this publication, it is based
19.109 AUTOMATED EXTERNAL DEFIBRILLATOR
 19.109 AUTOMATED EXTERNAL DEFIBRILLATOR References: American Heart Association Healthcare Provider (CPR/AED) Ohio Revised Code Chapter 2305.235 Immunity of Person Involved with Providing Automated External
19.109 AUTOMATED EXTERNAL DEFIBRILLATOR References: American Heart Association Healthcare Provider (CPR/AED) Ohio Revised Code Chapter 2305.235 Immunity of Person Involved with Providing Automated External
How you can help save lives
 How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
2015 AHA /ECC updates for BLS: Compression rate and depth - how to perform and monitor
 2015 AHA /ECC updates for BLS: Compression rate and depth - how to perform and monitor 范 文 林 醫 師 2016/04/10 Reinforced Chest compressions are the key component of effective CPR. Characteristics of chest
2015 AHA /ECC updates for BLS: Compression rate and depth - how to perform and monitor 范 文 林 醫 師 2016/04/10 Reinforced Chest compressions are the key component of effective CPR. Characteristics of chest
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
Infant CPR. What You Need to Know. How to Do Infant CPR
 Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
Guidelines for CPR and ECC
 H i g h l i g h t s o f t h e 2010 American Heart Association Guidelines for CPR and ECC Contents Major Issues Affecting All Rescuers 1 Lay Rescuer Adult CPR 3 Healthcare Provider BLS 5 Electrical Therapies
H i g h l i g h t s o f t h e 2010 American Heart Association Guidelines for CPR and ECC Contents Major Issues Affecting All Rescuers 1 Lay Rescuer Adult CPR 3 Healthcare Provider BLS 5 Electrical Therapies
Department of Emergency and Disaster Medicine Medical University of LODZ
 Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
(Organization s Name)
 2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT
 Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
EMR Medical Directives and Guidelines
 EMR Medical Directives and Guidelines Central East Prehospital Care Program, May 1, 2009 Section One 1 USE OF MEDICAL DIRECTIVES / GUIDELINES These medical directives and guidelines are not intended to
EMR Medical Directives and Guidelines Central East Prehospital Care Program, May 1, 2009 Section One 1 USE OF MEDICAL DIRECTIVES / GUIDELINES These medical directives and guidelines are not intended to
www.nanoomtech.co.kr ( (
 ( www.nanoomtech.co.kr ( 4 minutes start brain damage 6 minutes brain death begins 10 minutes biological death Resuscitate within 5 Minutes do we need AEDs? Sudden Cardiac Arrest (SCA) is the leading cause
( www.nanoomtech.co.kr ( 4 minutes start brain damage 6 minutes brain death begins 10 minutes biological death Resuscitate within 5 Minutes do we need AEDs? Sudden Cardiac Arrest (SCA) is the leading cause
Instructions For Use AED Trainer
 Instructions For Use AED Trainer PART NUMBER Copyright 2007 Cardiac Science Corporation. All rights reserved. The Automated External Defibrillator (AED) Trainer is a device for teaching basic AED rescue
Instructions For Use AED Trainer PART NUMBER Copyright 2007 Cardiac Science Corporation. All rights reserved. The Automated External Defibrillator (AED) Trainer is a device for teaching basic AED rescue
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
Presenters Alison Ellison Children s Healthcare of Atlanta Georgina Howard Therese McGuire Michael Tenoschok Georgia Department of Education
 CPR (Cardio Pulmonary Resuscitation) and AED (Automated External Defibrillator) Information August 29, 2013 Today s Session will begin at 3:30 PM While you are waiting, please do the following: Configure
CPR (Cardio Pulmonary Resuscitation) and AED (Automated External Defibrillator) Information August 29, 2013 Today s Session will begin at 3:30 PM While you are waiting, please do the following: Configure
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
American Heart Association. Pediatric Advanced Life Support. Written Precourse Self-Assessment. Questions and Answer Key for Students.
 E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
CARDIOPULMONARY RESUSCITATION (CPR)
 Alert the Emergency Team Algorithm ABC Assess & Manage Defibrillation Medications Disability Exposure Secondary Survey Emergency Team Roles Medical Emergency Team Roles - Nursing Role in Wards Post-Resuscitation
Alert the Emergency Team Algorithm ABC Assess & Manage Defibrillation Medications Disability Exposure Secondary Survey Emergency Team Roles Medical Emergency Team Roles - Nursing Role in Wards Post-Resuscitation
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Training Manikin Requirements for American Red Cross Certification Courses
 Training Manikin Requirements for American Red Cross Certification Courses Introduction We are pleased to announce the release of the requirements for training manikins. These requirements apply to all
Training Manikin Requirements for American Red Cross Certification Courses Introduction We are pleased to announce the release of the requirements for training manikins. These requirements apply to all
Journal of American Science 2014;10(5) http://www.jofamericanscience.org
 Effect of Frequent Application of Code Blue Training Program on the Performance of Pediatric Nurses Ghada Saeed AL-Ghamdi 1 ; Magda Aly Essawy 2 and Dr. Mohammad Al-Qahtani 3 1 College of Nursing, University
Effect of Frequent Application of Code Blue Training Program on the Performance of Pediatric Nurses Ghada Saeed AL-Ghamdi 1 ; Magda Aly Essawy 2 and Dr. Mohammad Al-Qahtani 3 1 College of Nursing, University
LIFE SUPPORT TRAINING CENTER
 LIFE SUPPORT TRAINING CENTER (LSTC) Contents Preface Page 1 Basic Life Support Page 3 Advanced Cardiovascular Life Support Page 5 Pediatric Advanced Life Support Page 7 Neonatal Resuscitation Program
LIFE SUPPORT TRAINING CENTER (LSTC) Contents Preface Page 1 Basic Life Support Page 3 Advanced Cardiovascular Life Support Page 5 Pediatric Advanced Life Support Page 7 Neonatal Resuscitation Program
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE
 October 22, 2015 Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE Summary: Expand Naloxone down to the Emergency Medical Technician (EMT)
October 22, 2015 Summary of State Emergency Medical Control Committee (SEMCC) Approved Protocol Revisions September 1, 2015 NALOXONE Summary: Expand Naloxone down to the Emergency Medical Technician (EMT)
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
11 Newborn Life Support
 11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
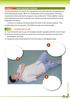 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
Armstrong Medical Little Joe. 1 Manikin 1 Red Cross-branded Carrying Case
 Category Ambu CPR Pal Trainer Ambu Multi Man Armstrong Medical Actar D-Fib Armstrong Medical Little Joe Laerdal Little Anne Laerdal Resusci Anne Prestan Professional Adult Manikin Retail Price $257.89/each
Category Ambu CPR Pal Trainer Ambu Multi Man Armstrong Medical Actar D-Fib Armstrong Medical Little Joe Laerdal Little Anne Laerdal Resusci Anne Prestan Professional Adult Manikin Retail Price $257.89/each
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Percent pulseless cardiac events monitored or witnessed (pediatric patients): Percent of pulseless cardiac events monitored or witnessed
 RESUSCITATION RFACT SHEET Get With The Guidelines -Resuscitation is the American Heart Association s collaborative quality improvement program demonstrated to improve adherence to evidence-based care of
RESUSCITATION RFACT SHEET Get With The Guidelines -Resuscitation is the American Heart Association s collaborative quality improvement program demonstrated to improve adherence to evidence-based care of
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
