Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage
|
|
|
- Rolf McKinney
- 7 years ago
- Views:
Transcription
1 SOGC CLINICAL PRACTICE GUIDELINE SOGC CLINICAL PRACTICE GUIDELINE No. 235 October 2009 (Replaces No. 88, April 2000) Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage This Clinical Practice Guideline has been prepared by the Clinical Practice Obstetrics Committee and approved by the Executive and Council of the Society of Obstetricians and Gynaecologists of Canada. PRINCIPAL AUTHOR Dean Leduc, MD, Ottawa ON Vyta Senikas, MD, Ottawa ON André B. Lalonde, MD, Ottawa ON CLINICAL PRACTICE OBSTETRICS COMMITTEE Dean Leduc (Chair), MD, Ottawa ON Charlotte Ballerman, MD, Edmonton AB Anne Biringer, MD, Toronto ON Martina Delaney, MD, St. John s NL Louise Duperron, MD, Montreal QC Isabelle Girard, MD, Montreal QC Donna Jones, MD, Calgary AB Lily Shek-Yun Lee, MD, Vancouver BC Debra Shepherd, MD, Regina SK Kathleen Wilson, RM, Ilderton ON Disclosure statements have been received from all members of the committee. Abstract Objective: To review the clinical aspects of postpartum hemorrhage (PPH) and provide guidelines to assist clinicians in the prevention and management of PPH. These guidelines are an update from the previous Society of Obstetricians and Gynaecologists of Canada (SOGC) clinical practice guideline on PPH, published in April Evidence: Medline, PubMed, the Cochrane Database of Systematic Reviews, ACP Journal Club, and BMJ Clinical Evidence were searched for relevant articles, with concentration on randomized controlled trials (RCTs), systematic reviews, and clinical practice guidelines published between 1995 and Each article was screened for relevance and the full text acquired if determined to Key Words: Prevention, hemorrhage, obstetrics, obstetric hemorrhage be relevant. Each full-text article was critically appraised with use of the Jadad Scale and the levels of evidence definitions of the Canadian Task Force on Preventive Health Care. Values: The quality of evidence was rated with use of the criteria described by the Canadian Task Force on Preventive Health Care. Sponsor: The Society of Obstetricians and Gynaecologists of Canada. Recommendations Prevention of Postpartum Hemorrhage 1. Active management of the third stage of labour (AMTSL) reduces the risk of PPH and should be offered and recommended to all women. (I-A) 2. Oxytocin (10 IU), administered intramuscularly, is the preferred medication and route for the prevention of PPH in low-risk vaginal deliveries. Care providers should administer this medication after delivery of the anterior shoulder. (I-A) 3. Intravenous infusion of oxytocin (20 to 40 IU in 1000 ml, 150 ml per hour) is an acceptable alternative for AMTSL. (I-B) 4. An IV bolus of oxytocin, 5 to 10 IU (given over 1 to 2 minutes), can be used for PPH prevention after vaginal birth but is not recommended at this time with elective Caesarean section. (II-B) 5. Ergonovine can be used for prevention of PPH but may be considered second choice to oxytocin owing to the greater risk of maternal adverse effects and of the need for manual removal of a retained placenta. Ergonovine is contraindicated in patients with hypertension. (I-A) 6. Carbetocin, 100 g given as an IV bolus over 1 minute, should be used instead of continuous oxytocin infusion in elective Caesarean section for the prevention of PPH and to decrease the need for therapeutic uterotonics. (I-B) 7. For women delivering vaginally with 1 risk factor for PPH, carbetocin 100 g IM decreases the need for uterine massage to prevent PPH when compared with continuous infusion of oxytocin. (I-B) 8. Ergonovine, 0.2 mg IM, and misoprostol, 600 to 800 g given by the oral, sublingual, or rectal route, may be offered as alternatives in vaginal deliveries when oxytocin is not available. (II-1B) 9. Whenever possible, delaying cord clamping by at least 60 seconds is preferred to clamping earlier in premature newborns (< 37 weeks gestation) since there is less intraventricular hemorrhage and less need for transfusion in those with late clamping. (I-A) 10. For term newborns, the possible increased risk of neonatal jaundice requiring phototherapy must be weighed against the This document reflects emerging clinical and scientific advances on the date issued and is subject to change. The information should not be construed as dictating an exclusive course of treatment or procedure to be followed. Local institutions can dictate amendments to these opinions. They should be well documented if modified at the local level. None of these contents may be reproduced in any form without prior written permission of the SOGC. 980 OCTOBER JOGC OCTOBRE 2009
2 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage Table 1. Key to evidence statements and grading of recommendations, using the ranking of the Canadian Task Force on Preventive Health Care Quality of Evidence Assessment* I: Evidence obtained from at least one properly randomized controlled trial II-1: Evidence from well-designed controlled trials without randomization II-2: Evidence from well-designed cohort (prospective or retrospective) or case-control studies, preferably from more than one centre or research group II-3: Evidence obtained from comparisons between times or places with or without the intervention. Dramatic results in uncontrolled experiments (such as the results of treatment with penicillin in the 1940s) could also be included in this category III: Opinions of respected authorities, based on clinical experience, descriptive studies, or reports of expert committees Classification of Recommendations A. There is good evidence to recommend the clinical preventive action B. There is fair evidence to recommend the clinical preventive action C. The existing evidence is conflicting and does not allow to make a recommendation for or against use of the clinical preventive action; however, other factors may influence decision-making D. There is fair evidence to recommend against the clinical preventive action E. There is good evidence to recommend against the clinical preventive action L. There is insufficient evidence (in quantity or quality) to make a recommendation; however, other factors may influence decision-making The quality of evidence reported in these guidelines has been adapted from The Evaluation of Evidence criteria described in the Canadian Task Force on Preventive Health Care. 54 Recommendations included in these guidelines have been adapted from the Classification of Recommendations criteria described in the The Canadian Task Force on Preventive Health Care. 54 physiological benefit of greater hemoglobin and iron levels up to 6 months of age conferred by delayed cord clamping. (I-C) 11. There is no evidence that, in an uncomplicated delivery without bleeding, interventions to accelerate delivery of the placenta before the traditional 30 to 45 minutes will reduce the risk of PPH. (II-2C) 12. Placental cord drainage cannot be recommended as a routine practice since the evidence for a reduction in the duration of the third stage of labour is limited to women who did not receive oxytocin as part of the management of the third stage. There is no evidence that this intervention prevents PPH. (II-1C) 13. Intraumbilical cord injection of misoprostol (800 g) or oxytocin (10 to 30 IU) can be considered as an alternative intervention before manual removal of the placenta. (II-2C) Treatment of PPH 14. For blood loss estimation, clinicians should use clinical markers (signs and symptoms) rather than a visual estimation. (III-B) 15. Management of ongoing PPH requires a multidisciplinary approach that involves maintaining hemodynamic stability while simultaneously identifying and treating the cause of blood loss. (III-C) 16. All obstetric units should have a regularly checked PPH emergency equipment tray containing appropriate equipment. (II-2B) 17. Evidence for the benefit of recombinant activated factor VII has been gathered from very few cases of massive PPH. Therefore this agent cannot be recommended as part of routine practice. (II-3L) 18. Uterine tamponade can be an efficient and effective intervention to temporarily control active PPH due to uterine atony that has not responded to medical therapy. (III-L) 19. Surgical techniques such as ligation of the internal iliac artery, compression sutures, and hysterectomy should be used for the ABBREVIATIONS AMTSL active management of the third stage of labour PPH postpartum hemorrhage RCT randomized controlled trial management of intractable PPH unresponsive to medical therapy. (III-B) Recommendations were quantified using the evaluation of evidence guidelines developed by the Canadian Task Force on Preventive Health Care (Table 1). J Obstet Gynaecol Can 2009;31(10): INTRODUCTION Postpartum hemorrhage is the leading cause of maternal death worldwide, with an estimated mortality rate of per year, or 1 maternal death every 4 minutes. 1 PPH occurs in 5% of all deliveries and is responsible for a major part of maternal mortality. 2,3 The majority of these deaths occur within 4 hours of delivery, which indicates that they are a consequence of the third stage of labour. 4,5 Nonfatal PPH results in further interventions, iron deficiency anemia, pituitary infarction (Sheehan s syndrome) with associated poor lactation, exposure to blood products, coagulopathy, and organ damage with associated hypotension and shock. Since all parturient women are at risk for PPH, care providers need to possess the knowledge and skills to practise active management of the third stage of labour to prevent PPH and to recognize, assess, and treat excessive blood loss. DEFINITION OF PPH Primary PPH is defined as excessive bleeding that occurs in the first 24 hours after delivery. OCTOBER JOGC OCTOBRE
3 SOGC CLINICAL PRACTICE GUIDELINE Table 2. Signs and symptoms of shock resulting from blood loss Degree of shock Blood loss Signs and symptoms Mild 20% Diaphoresis Increased capillary refilling Cool extremities Anxiety Moderate 20% to 40% Above plus Tachycardia Tachypnea Postural hypotension Oliguria Severe 40% Above plus Hypotension Agitation/confusion Hemodynamic instability Traditionally the definition of PPH has been blood loss in excess of 500 ml after vaginal delivery and in excess of 1000 ml after abdominal delivery. For clinical purposes, any blood loss that has the potential to produce hemodynamic instability should be considered PPH. The amount of blood loss required to cause hemodynamic instability will depend on the pre-existing condition of the woman. Hemodynamic compromise is more likely to occur in conditions such as anemia (e.g., iron deficiency, thalassemia) or volume-contracted states (e.g., dehydration, gestational hypertension with proteinuria). Hypovolemic Shock 6 Excessive bleeding, or hemorrhage, results in net loss of intravascular volume and decreased oxygen delivery to tissues and organs. Physiological compensatory mechanisms such as reflex tachycardia, peripheral vasoconstriction, and increased myocardial contractility help to maintain tissue perfusion. Increasing blood loss results in circulatory collapse, end-organ damage, and eventual death. Ideally, care providers should be able to assess the amount of blood loss in order to estimate the volume of fluid that needs to be replaced. However, research has shown that clinicians often underestimate the actual loss. 7 The signs and symptoms listed in Table 2 should be used at the bedside to evaluate the amount of blood loss since, in general, the degree of shock parallels the amount of blood loss that results in these clinical markers. 6 Etiology of PPH In regard to the underlying causes of PPH, it may be helpful to think in terms of the 4 Ts: Tone: uterine atony, distended bladder Tissue: retained placenta and clots Trauma: vaginal, cervical, or uterine injury Thrombin: coagulopathy (pre-existing or acquired) The most common and important cause of PPH is uterine atony. The primary protective mechanism for immediate hemostasis after delivery is myometrial contraction causing occlusion of uterine blood vessels, the so-called living ligatures of the uterus. Thus blood flow from the vascular space to the uterine cavity via the myometrium is impeded. Maternity care providers should recognize the risk factors for PPH due to the 4 Ts, as listed in Table 3, and take appropriate action. PREVENTION OF PPH AMTSL involves interventions to assist in expulsion of the placenta with the intention to prevent or decrease blood loss. Interventions include use of uterotonics, clamping of the umbilical cord, and controlled traction of the cord. In contrast, with expectant, or physiological, management, spontaneous delivery of the placenta is allowed, with subsequent intervention, if necessary, that involves uterine massage and use of uterotonics. Prendiville and colleagues meta-analysis 8 demonstrated the benefits of AMTSL to prevent and reduce PPH after vaginal delivery for women at low risk of PPH. Studies included in the meta-analysis had design methods that involved routine use of uterotonics after delivery of the newborn and before delivery of the placenta, early cord clamping, and controlled cord traction. The primary goal of these interventions was to assist placental delivery, thereby allowing the uterus to contract and reduce blood flow across the myometrium. The meta-analysis concluded that active compared with expectant management significantly reduced the risk in all areas, including mild PPH (estimated blood loss > 500 ml; OR 0.38; 95% CI 0.32 to 0.46), severe PPH (estimated blood loss > 1000 ml; OR 0.32; 95% CI 0.21 to 0.50), low postpartum hemoglobin level (< 9 g/dl; OR 0.38; 95% CI 0.27 to 0.53), need for transfusion (OR 0.33; 95% CI 0.21 to 0.52), and need for additional uterotonic medication (OR 0.17; 95% CI 0.14 to 0.21). There was no difference in the incidence of retained placenta or management of this complication by manual or surgical removal. There was significantly more nausea and hypertension in the actively managed group given ergonovine (OR 1.83; 95% CI 1.51 to 2.23). A review of the data resulted in a joint statement in 2004 by the International Confederation of Midwives and International Federation of Gynaecologists and Obstetricians endorsing the need for all deliveries to be attended by a caregiver trained in AMTSL, which should include routine use of uterotonics, controlled cord traction, and uterine massage. 9 Delaying cord clamping by 1 to 3 minutes was 982 OCTOBER JOGC OCTOBRE 2009
4 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage Table 3. Risk factors for postpartum hemorrhage (PPH) Etiologic category and process Tone: abnormalities of uterine contraction Overdistension of uterus Uterine muscle exhaustion Intra-amniotic infection Functional/anatomic distortion of uterus Uterine-relaxing medications Bladder distension, which may prevent uterine contraction 4 Tissue: retained Retained products of conception Abnormal placentation Retained cotyledon or succenturiate lobe Retained blood clots Trauma: of the genital tract Lacerations of the cervix, vagina, or perineum Extensions, lacerations at cesarean section Uterine rupture Uterine inversion Thrombin: abnormalities of coagulation Pre-existing states Clinical risk factors Polyhydramnios Multiple gestation Macrosomia Rapid labour Prolonged labour High parity Oxytocin use Fever Prolonged rupture of membranes Fibroids Placenta previa Uterine anomalies Halogenated anesthetics Nitroglycerin Incomplete placenta at delivery Previous uterine surgery High parity Abnormal placenta seen on ultrasonography Atonic uterus Precipitous delivery Operative delivery Malposition Deep engagement Previous uterine surgery High parity Fundal placenta Excessive cord traction History of hereditary coagulopathies or liver disease Hemophilia A Von Willebrand s disease History of previous PPH Acquired in pregnancy Idiopathic thrombocytopenic purpura Bruising, elevated blood pressure Thrombocytopenia with preeclampsia Disseminated intravascular coagulation Gestational hypertensive disorder of pregnancy with adverse conditions a) Dead fetus in utero b) Severe infection c) Abruption d) Amniotic fluid embolus Therapeutic anticoagulation Elevated blood pressure Fetal demise Fever, neutrophilia/neutropenia Antepartum hemorrhage Sudden collapse History of thrombotic disease favoured over early cord clamping to reduce anemia in the newborn. A similar review of the literature in 2006 by the World Health Organization 10 highlighted the most common cause of PPH as uterine atony and the fact that most women with PPH have no identifiable risk factors. The review resulted in several recommendations to minimize maternal morbidity and mortality rates. 1. Active management should be offered to all women by skilled care providers. 2. Skilled attendants should offer uterotonics (oxytocin preferred over ergonovine, misoprostol, and carboprost) to prevent PPH. 3. Early cord clamping is recommended only when the newborn needs to be resuscitated. OCTOBER JOGC OCTOBRE
5 SOGC CLINICAL PRACTICE GUIDELINE 4. Despite the lack of evidence to support cord traction, this practice should be continued as part of active management. Uterotonics During the third stage of labour the muscles of the uterus contract downward, causing constriction of the blood vessels that pass through the uterine wall to the placental surface and stopping the flow of blood. This action also causes the placenta to separate from the uterine wall. The absence of uterine contractions, clinically defined as atony, may result in excessive blood loss. Uterotonics promote uterine contractions to prevent atony and speed delivery of the placenta. The uterotonic agents include oxytocin, ergonovine, carbetocin, misoprostol, and Syntometrine (a combination of ergonovine and oxytocin, unavailable in Canada). Oxytocin and ergonovine The 1997 Abu Dhabi study 11 included in Prendiville and colleagues meta-analysis 8 randomly allocated low-risk women who delivered vaginally to receive either 10 IU of oxytocin IM with delivery of the anterior shoulder followed by controlled cord traction upon signs of placental separation or minimal intervention. The results revealed a benefit for the oxytocin group: a lower incidence of blood loss > 500 ml (OR 0.50; CI 0.34 to 0.73) and > 1000 ml (OR 0.22; CI 0.08 to 0.57), fewer retained placentas (OR 0.31; CI 0.15 to 0.63), and less need for additional uterotonics (OR 0.44; CI 0.24 to 0.78). A 2004 Cochrane Review 12 compared the efficacy of Syntometrine and oxytocin alone, both administered IM, in AMTSL. The results showed a small benefit for Syntometrine in preventing blood loss > 500 ml (OR 0.82; 95% CI 0.71 to 0.95) but no difference in preventing losses > 1000 ml. The group receiving Syntometrine were more likely to have elevated diastolic blood pressure (OR 2.40; 95% CI 1.58 to 3.64), nausea (OR 4.07; 95% CI 3.43 to 4.84), and vomiting (OR 4.92; 95% CI 4.03 to 6.00). The authors favoured oxytocin alone on the basis of the lower incidence of maternal side effects. A 2008 meta-analysis 13 included 14 studies assessing the benefits of oxytocin in AMTSL for vaginal deliveries. Seven trials comparing oxytocin and no uterotonics found a lower incidence of blood loss > 500 ml (RR 0.50; 95% CI 0.43 to 0.59) and less need for therapeutic oxytocin (RR 0.5; 95% CI 0.39 to 0.64) in the groups receiving oxytocin. Six trials found no difference between the results with oxytocin and ergonovine except that the groups receiving oxytocin had fewer manual removals of the placenta (RR 0.57; 95% CI 0.41 to 0.79) and a tendency to a lower incidence of raised blood pressure (RR 0.53; 95% CI 0.19 to 1.52) than the groups receiving ergonovine. Five trials showed little evidence of a synergistic effect of adding oxytocin to ergonovine versus ergonovine alone. One double-blind randomized controlled trial 14 compared the efficacy of 10 IU of oxytocin in saline solution with saline solution alone in cephalic vaginal deliveries in low-risk women. The oxytocin group had a lower mean blood loss (407 vs. 527 ml), a lower incidence of blood loss > 800 ml (8.8% vs. 5.2%), and a lower rate of use of additional ergonovine (3.5% vs. 2.3%). Another double-blind RCT 15 found no difference in the incidence of PPH among women with low-risk vaginal deliveries given an IV bolus of oxytocin (20 IU in 500 ml of crystalloid) before or after delivery of the placenta. The use of a slow IV bolus in management of the third stage of labour has been adopted as standard practice although there is little supporting evidence in the literature. The Dublin trial 16 was the only study in Prendiville and colleagues meta-analysis 8 in which a uterotonic (Syntometrine) was administered IV; the result was a lower incidence of PPH but more retained placentas. There has been concern about the safety of such rapid administration of oxytocin in the third stage, although 99 women given 10 IU in an IV push after vaginal delivery did not have significant hemodynamic effects. The study, however, was underpowered to demonstrate a reduction in the incidence of PPH. 17 For women undergoing elective Caesarean section, recent studies have demonstrated adverse maternal effects of an oxytocin IV bolus. One double-blind RCT found hemodynamic changes in 30 patients given 5 IU IV over 30 seconds compared with women who received the same dose over 5 minutes. 18 In another double-blind RCT, 40 patients given 10 IU of oxytocin as an IV bolus manifested electrocardiographic changes consistent with myocardial ischemia when compared with pregnant women who received 0.2 mg of ergonovine and nonpregnant women; the effect was transient, with onset at 1 minute and resolution by 5 minutes after exposure to oxytocin. 19 These studies suggest a potential maternal effect of the rapid administration (within 30 seconds) of oxytocin, and it may be dose-related. Oxytocin given as part of AMTSL has been shown to reduce the need for manual removal of a retained placenta compared with expectant management. 8,13 The greater need for manual removal noted in the Dublin trial 16 was attributed to the use of Syntometrine as an IV bolus. A 2001 Cochrane review 13 of prophylactic IM oxytocin use during the third stage of labour demonstrated a significantly reduced need for manual removal of the placenta compared with ergometrine use (RR 0.57; 95% CI 0.41 to 0.79). 984 OCTOBER JOGC OCTOBRE 2009
6 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage Recommendations Recommendations were quantified using the evaluation of evidence guidelines developed by the Canadian Task Force on Preventive Health Care (Table 1). 1. AMTSL reduces the risk of PPH and should be offered and recommended to all women. (I-A) 2. Oxytocin (10 IU), administered intramuscularly, is the preferred medication and route for the prevention of PPH in low-risk vaginal deliveries. Care providers should administer this medication after delivery of the anterior shoulder. (I-A) 3. Intravenous infusion of oxytocin (20 to 40 IU in 1000 ml, 150 ml per hour) is an acceptable alternative for AMTSL. (I-B) 4. An IV bolus of oxytocin, 5 to 10 IU (given over 1 to 2 minutes), can be used for PPH prevention after vaginal birth but is not recommended at this time with elective Caesarean section. (II-B) 5. Ergonovine can be used for prevention of PPH but may be considered second choice to oxytocin owing to the greater risk of maternal adverse effects and of the need for manual removal of a retained placenta. Ergonovine is contraindicated in patients with hypertension. (I-A) Carbetocin Carbetocin is a long-acting oxytocin studied by Dansereau et al., 20 who performed an RCT comparing the incidence of PPH in women undergoing elective Caesarean section who received either carbetocin as a 100- g IV bolus or oxytocin as a continuous infusion for 8 hours (25 IU of oxytocin in 1000 ml of Ringer s lactate, 125 ml per hour). The carbetocin group had a decreased incidence of PPH and of the need for therapeutic oxytocics (4.7% vs. 10.1%; P < 0.05). The recommended dose of carbetocin is 100 g given either IM or slowly (over 1 minute), the pharmacokinetics of the 2 administration routes being almost the same. 21 Boucher and colleagues double-blind 2003 RCT 22 demonstrated that women with at least 1 risk factor for PPH who were given carbetocin (100 g IM) immediately after placental delivery were less likely to required uterine massage as a uterotonic intervention than those given a continuous infusion of oxytocin over 2 hours: 43.4% of women in the carbocetin group (36/83 [43.4%]; 95%CI, 32.7% to 54% vs. 48/77 [62.3%] of women in the oxytocin group; 95% CI, 51.5% to 73.2%) required the massage (P = 0.02). There was no difference in the requirement for additional uterotonic medication (i.e., oxytocin, ergonovine), estimated blood loss, or difference in hemoglobin level before and after vaginal delivery. There was no significant benefit of carbetocin over oxytocin in the prevention of PPH. The authors commented on the advantage of IM intervention in a setting where IV treatment is unavailable. A 2007 Cochrane Review 23 included 4 RCTs that compared carbetocin with oxytocin for prevention of PPH. The results were consistent with the results of the trials conducted by Dansereau and Boucher and their colleagues. 20,22 Since none of the trials included low-risk women, there was insufficient evidence that 100 g of carbetocin given IV is as effective as oxytocin in the prevention of PPH in low-risk vaginal deliveries. An RCT by Leung et al. 24 compared IM administration of carbetocin and Syntometrine in AMTSL for singleton vaginal deliveries after 34 weeks. The results showed no difference in the incidence of a low hemoglobin level, blood loss > 500 ml, retained placenta, or use of additional uterotonic agents. Carbetocin recipients had less nausea (RR 0.18; 95%CI 0.04 to 0.78), vomiting (RR 0.1; 95% CI 0.01 to 0.74), and hypertension 30 minutes (0 vs. 8 cases, P < 0.01) and 60 minutes (0 vs. 6 cases, P < 0.05) after delivery. There was a higher incidence of maternal tachycardia (RR 1.68; 95% CI 1.03 to 3.57) in the carbetocin group. We did not identify any published reports of trials comparing oxytocin and carbetocin, each administered IM for AMTSL, in low-risk term vaginal deliveries. Recommendations 6. Carbetocin, 100 g given as an IV bolus over 1 minute, should be used instead of continuous oxytocin infusion in elective Caesarean section for the prevention of PPH and to decrease the need for therapeutic uterotonics. (I-B) 7. For women delivering vaginally with 1 risk factor for PPH, carbetocin 100 g IM decreases the need for uterine massage to prevent PPH when compared with continuous infusion of oxytocin. (I-B) Misoprostol Misoprostol is a prostaglandin that has generated considerable interest as an effective uterotonic agent owing to its ease of administration, safety profile, cost, and ease of storage. The first study of misoprostol as a uterotonic agent was an uncontrolled prospective study for prevention of PPH. 25 A systematic review 26 that analyzed the pharmacokinetics of misoprostol concluded the following: There is a shorter time to peak concentration with oral and sublingual administration than with vaginal or rectal administration. Sublingual administration results in the most rapid onset of effects and the highest peak concentration. The initial increase in tonus is more pronounced after oral than after vaginal administration. OCTOBER JOGC OCTOBRE
7 SOGC CLINICAL PRACTICE GUIDELINE The effects have a slower onset but longer duration with rectal and vaginal routes than with oral and sublingual routes. Pyrexia is more common when the dose exceeds 600 g. There have been 3 systematic reviews of the use of misoprostol for the prevention of PPH The WHO multicentre trial 30 and the Cochrane review 27 suggested that the observed lesser efficacy of misoprostol compared with injectable uterotonics may be due to the later achievement of peak plasma levels with oral and sublingual administration of misoprostol: 30 minutes versus 1 to 2 minutes for IM or IV administration of oxytocin. All of the reviews concluded that misoprostol was not as effective as oxytocin for the prevention of PPH and that maternal pyrexia was a significant adverse effect. A 2007 study comparing 800 g of misoprostol administered rectally with 10 IU of oxytocin administered IM in a developing country found these 2 agents to be equally effective in minimizing blood loss during the third stage of labour. 31 There was more pyrexia in the misoprostol group, however. The systematic review by Joy and colleagues 29 compared the efficacy of misoprostol with that of oxytocin, other uterotonic agents, and placebo in preventing PPH in the third stage of labour. Compared with placebo, misoprostol was associated with a decreased need for additional uterotonics (OR 0.64; 95% CI 0.46 to 0.90) and an increased risk of shivering and pyrexia. Oxytocin was superior to misoprostol in preventing blood loss and the need for additional agents, and the patients had less shivering and pyrexia. The authors proposed that misoprostol is a reasonable agent for management of the third stage of labour when other agents are not available for reasons of cost, storage, or difficulty of administration. There have been no studies to determine the benefit of a combination of oxytocin and misoprostol compared with either agent alone. Recommendation 8. Ergonovine, 0.2 mg IM, and misoprostol, 600 to 800 g given by the oral, sublingual, or rectal route, may be offered as alternatives in vaginal deliveries when oxytocin is not available. (II-1B) Management of the Placenta Timing of cord clamping Clamping of the umbilical cord is a necessary part of the third stage of labour. Its timing varies widely throughout the world, early clamping being the predominant practice in Western countries. 32 Physiological studies have shown that 25% to 60% of the fetal placental circulation is found in the placental circulation. 33,34 Early cord clamping in term newborns results in a decrease of 20 to 40 ml/kg of blood, which is equivalent to 30 to 35 mg of iron. A delay in clamping, causing increased neonatal blood volume, may lead to complications such as respiratory distress, neonatal jaundice, and polycythemia. Prendiville and colleagues meta-analysis espousing the benefit of AMTSL 8 included studies that applied early cord clamping, controlled traction, and uterotonics before delivery of the placenta. In these studies, early cord clamping was included as part of controlled traction and was not independently studied to demonstrate a benefit. A 2004 Cochrane Review by Rabe et al. 35 and a prospective study by Ibrahim et al. 36 demonstrated that delaying cord clamping by 30 to 120 seconds resulted in less need for transfusion because of anemia (RR 2.01; 95% CI 1.24 to 3.27) and less intraventricular hemorrhage (RR 1.74; 95% CI 1.08 to 2.81) in nonresuscitated premature infants (< 37 weeks gestation). A systematic review and meta-analysis comparing cord clamping done early (less than 1 minute after delivery of the infant) and late (at least 2 minutes after delivery) showed that late clamping conferred physiological benefit to the newborn that extended up to 6 months into infancy. 37 Advantages included prevention of anemia over the first 3 months of life and enhanced iron stores (weighted mean difference 19.90; 95% CI 7.67 to 32.13) and ferritin concentration (weighted mean difference 17.89; 95% CI to 19.21) for up to 6 months. There was no increase in respiratory distress, defined as tachypnea or grunting. Neonates were at increased risk of asymptomatic polycythemia (RR 3.82; 95% CI 1.11 to 13.21). There was no significant difference between the early and late groups in bilirubin levels and proportions of infants receiving phototherapy. A 2008 Cochrane review included 11 RCTs that compared the effect on maternal and neonatal outcomes of cord clamping done early (up to 60 seconds after delivery) and late (beyond 60 seconds after delivery). 38 The results showed no difference in the incidence of PPH but an increased incidence of neonatal jaundice requiring phototherapy, higher newborn hemoglobin levels up to 6 months of age, and higher ferritin levels at 6 months of age after late clamping. Recommendations 9. Whenever possible, delaying cord clamping by at least 60 seconds is preferred to clamping earlier in premature newborns (< 37 weeks gestation) since there is less intraventricular hemorrhage and less need for transfusion in those with late clamping. (I-A) 986 OCTOBER JOGC OCTOBRE 2009
8 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage 10. For term newborns, the possible increased risk of neonatal jaundice requiring phototherapy must be weighed against the physiological benefit of greater hemoglobin and iron levels up to 6 months of age conferred by delayed cord clamping. (I-C) Timing of placental delivery Placental delivery is essential to allow the uterus to contract and thus reduce blood loss in the third stage of labour. This process is completed within 5 minutes in 50% of deliveries and by 15 minutes in 90%. Failure of the placenta to be delivered in such a timely manner is a well-known risk factor of PPH. 39,40 The traditional definition of retained placenta includes failure of placental delivery within 30 to 45 minutes and a requirement of intervention to assist with delivery. One study published in 2006 concluded that the risk of PPH increases if the placenta has not been delivered by 10 minutes, although research is needed to determine if the risk of PPH can be reduced by intervening at this stage. 41 Recommendation 11. There is no evidence that, in an uncomplicated delivery without bleeding, interventions to accelerate delivery of the placenta before the traditional 30 to 45 minutes will reduce the risk of PPH. (II-2C) Placental cord drainage Drainage of cord blood has been proposed to assist with delivery of the placenta. A 2005 Cochrane review 42 included only 2 studies addressing this intervention, which makes it difficult to draw conclusions. The selection criteria for the review were low-risk vaginal deliveries in which a cord clamped within 30 seconds of delivery and separated was unclamped, which allowed the blood from the placenta to drain freely. The measured outcomes included incidence of retained placenta (at 30 to 45 minutes), manual removal of the placenta, PPH, length of the third stage of labour, need for blood transfusion, decrease in maternal hemoglobin level, and maternal pain. The outcomes reported were a decreased incidence of retained placenta at 30 minutes (RR 0.28; 95% CI 0.10 to 0.73) and a shorter third stage (weighted mean difference 5.46; 95% CI 8.02 to 2.90) after cord drainage. A major confounding factor was the lack of use of uterotonics and the varied definition of a prolonged third stage: from 30 to 45 minutes. Sharma et al. 43 randomly assigned 958 women to either placental cord drainage or controlled traction after administration of 0.2 mg of ergonovine with delivery of the anterior shoulder and immediate cord clamping. Measured outcomes were PPH and length of the third stage. The third stage had a mean duration of 3.24 and 3.20 minutes in the drainage group versus 8.57 and 6.20 minutes in the traction group in primigravid (P < 0.05) and multigravid (P < 0.05) women, respectively. There was no significant difference between the groups in the incidence of blood loss > 500 ml and the need for transfusion (P > 0.05), and none of the women had a retained placenta. The limited number of studies makes it difficult to recommend a change in practice to support routine cord drainage, but this intervention does appear to reduce the length of the third stage of labour and the risk of a retained placenta. More research is required to determine if the length of the third stage is reduced with routine drainage after the use of uterotonics and if this intervention reduces the risk of PPH. Recommendation 12. Placental cord drainage cannot be recommended as a routine practice since the evidence for a reduction in the duration of the third stage of labour is limited to women who did not receive oxytocin as part of the management of the third stage. There is no evidence that this intervention prevents PPH. (II-1C) Injection of the umbilical vein Injection of the umbilical vein has been proposed to assist in uterine contractions and dehiscence of the placenta from the uterine wall to effect delivery. If successful, this intervention would avoid manual removal of the placenta, an invasive procedure with potential complications, including hemorrhage, infection, and trauma. A 2001 Cochrane Review 44 assessed if injection of various agents would reduce the need for manual removal of a retained placenta. The authors derived the following conclusions. Saline versus expectant management: no difference (RR 0.97; 95% CI 0.83 to 1.14). Saline plus oxytocin versus expectant management: nonsignificant reduction in the incidence of manual removal (RR 0.86; 95% CI 0.72 to 1.01) with the use of saline plus oxytocin. Saline plus oxytocin versus saline: significantly lower incidence of manual removal of the placenta (RR 0.79; 95% CI 0.69 to 0.91) (number needed to treat: 8; 95% CI 5 to 20) with the use of saline plus oxytocin. Saline plus oxytocin versus plasma expander: nonsignificantly greater incidence of manual removal of the placenta (RR 1.34; 95% CI 0.97 to 1.85) with the use of saline plus oxytocin. Saline plus prostaglandin versus saline: significantly lower incidence of manual removal of the placenta (RR 0.05; 95% CI 0.00 to 0.73) with the use of saline plus prostaglandin but no difference in the incidence of blood loss, fever, pain, and oxytocin augmentation. OCTOBER JOGC OCTOBRE
9 SOGC CLINICAL PRACTICE GUIDELINE Figure 1. Pipingas technique for injection of the intraumbilical vein if the placenta has not separated or delivered within 45 minutes after delivery of the baby Prepare a syringe of misoprostol (800 g) or oxytocin (50 IU) dissolved in 30 ml of normal saline. Insert a size 10 nasogastric suction catheter along the umbilical vein. If resistance is felt, retract the catheter 1 to 2 cm and advance it further, if possible. If the catheter cannot be advanced further without force, inject the solution in this position. If most of the catheter has been inserted when resistance is felt, indicating that it has reached the placenta, retract it 3 to 4 cm to ensure that the tip is in the umbilical vein and not in a placental branch. Connect the syringe to the catheter and inject the solution. Clamp the catheter in situ and record the time of the injection. Allow 30 minutes for the placenta to deliver before undertaking further intervention. Saline plus prostaglandin versus saline plus oxytocin: no difference (RR 0.10; 95% CI 0.01 to 1.59). This review suggests that umbilical vein injection of uterotonics assists with the third stage of labour but provides no convincing evidence of the benefit; the last 3 conclusions were based on the results of a single small trial. The authors conclude that umbilical vein injection of oxytocin may reduce the need for manual removal of a retained placenta, but further investigation is required. There is an ongoing systematic review to determine if routine injection of the umbilical vein with a uterotonic within 15 minutes of birth will affect perinatal and maternal outcomes. 45 An RCT compared the effect of intraumbilical vein injection of Syntocinon (synthetic oxytocin; 50 IU in 30 ml of normal saline), misoprostol (800 g in 30 ml of normal saline), or normal saline (30 ml) on the need for manual removal of the placenta in a prolonged third stage of labour in 87 low-risk women at term. 46 The Pipingas technique (Figure 1) was used for injection. All the women had AMTSL with either oxytocin or Syntometrine with delivery of the anterior shoulder, early cord clamping, and cord traction when signs of placental separation were observed. The women whose third stage exceeded 30 minutes were randomly assigned to intervention at 45 minutes with 1 of the 3 injections. The trial was stopped when the misoprostol group had many fewer instances of manual removal of the placenta (9 of 21 women) compared with the Syntocinon group (16 of 20 women) and the saline group (7 of 13 women). Recommendation 13. Intraumbilical cord injection of misoprostol (800 g) or oxytocin (10 to 30 IU) can be considered as an alternative intervention before manual removal of the placenta. (II-2C) TREATMENT OF ESTABLISHED PPH Research has shown that care providers poorly estimate blood loss 7 and consistently underestimate the loss of a large volume of blood. 43 Clinical signs and symptoms (Table 2) are useful bedside indicators of ongoing blood loss and will assist clinicians in management. A previously established plan of action is of great value when preventive measures have failed. This plan should include aggressive fluid resuscitation, control of bleeding to minimize loss, and access to a surgical room and support personnel (Table 4). The initial goal of management is to determine the cause of blood loss while instituting resuscitative measures. Evaluation of uterine tone and a complete inspection of the lower genital tract are required. The goal of resuscitative measures is to maintain hemodynamic stability and oxygen perfusion of the tissues. An IV infusion of crystalloid solution should be instituted, using large-bore tubing, along with oxygen supplementation. The ABCs should be observed and vital signs, oxygen saturation, and urinary output monitored. A visual assessment of clotting can be done at the bedside while blood is sent for analysis and matching for transfusion. PPH emergencies often occur unexpectedly and, depending on the volume of deliveries in each institution, may be infrequent. When a situation does not resolve with the usual interventions, there is a need for more equipment that may not be readily available when needed. For these reasons, every obstetric unit should have a readily available tray with all of the necessary equipment. Since clinicians may rarely apply these interventions, this equipment should be accompanied by appropriate diagrams illustrating the relevant anatomy and technique. A previously prepared PPH tray in a large Canadian birthing centre was used in 1 in 250 Caesarean sections and 1 in 1000 vaginal deliveries. 47 Recommendations 14. For blood loss estimation, clinicians should use clinical markers (signs and symptoms) rather than a visual estimation. (III-B) 15. Management of ongoing PPH requires a multidisciplinary approach that involves maintaining hemodynamic stability while simultaneously identifying and treating the cause of blood loss. (III-C) 988 OCTOBER JOGC OCTOBRE 2009
10 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage Table 4. Treatment of PPH Initial assessment and treatment for primary PPH Assess etiology Directed therapy If bleeding continues If bleeding continues If bleeding continues Call for help Resuscitation Assess the ABC Oxygen by mask IV line Crystalloid, isotonic fluid replacement Monitor BP, P, R Empty bladder, monitor urine output Laboratory tests Complete blood count Coagulation screen Blood grouping and cross Uterus soft and relaxed Uterine atony Uterine massage Placenta not separated or partially separated (with or without hemorrhage) Retained placenta Uterotonic drugs Whole placenta in uterus Uterotonics Controlled cord traction Intraumbilical vein injection Nonsurgical uterine compression Bimanual uterine compression External aortic compression Uterine packing Balloon (condom) tamponade Placenta still retained Manual removal Compression sutures B-Lynch Vertical compression Cho square Uterine artery embolization Placenta still retained (placenta accreta) Partial or complete removal of placenta through laparotomy Hysterectomy Artery ligation (uterine, hypogastric) Hysterectomy (subtotal or total) Incomplete separation Manual vacuum aspiration Manual exploration Gentle curettage Hysterectomy Excess bleeding or shock shortly after birth, uterus contracted Low genital tract trauma Repair tears in perineum, vagina and cervix Uterine rupture Laparotomy: Primary repair Hysterectomy Uterine fundus not felt abdominally OR visible vaginally Uterine inversion Correct inversion in theatre under general anaesthesia If nonsurgical correction fails, ensure that uterus remains contracted by continued oxytocin infusion Surgery Correction via laparotomy Hysterectomy Clotting Clotting disorder Treat accordingly with blood products Adapted with permission of the World Health Organization from Postpartum Hemorrhage Technical Consultation Meeting Document 55 OCTOBER JOGC OCTOBRE
11 SOGC CLINICAL PRACTICE GUIDELINE 16. All obstetric units should have a regularly checked PPH emergency equipment tray containing appropriate equipment. (II-2B) Uterine Massage and Additional Uterotonic Administration Since the most common cause of PPH is uterine atony, the clinician s initial efforts should be directed at preventing ongoing blood loss by performing the initial basic maneuvres of uterine massage and administering additional uterotonics, which include the following. 1. Oxytocin 10 IU IM. Consider ability of the medication to reach a uterus with poor tissue perfusion. 5 IU IV push 20 to 40 IU in 250 ml of normal saline, infused IV at an hourly rate of 500 to 1000 ml methyl prostaglandin (carboprost tromethamine [Hemabate]) 250 g IM or intramyometrially Can be repeated every 15 minutes to a maximum of 2 mg (8 doses). Asthma is a relative contraindication. 3. Carbetocin 100 g IM or IV over 1 minute Shown to reduce bleeding due to uterine atony in Caesarean sections but not low-risk vaginal deliveries. 4. Misoprostol (off-label use not approved for PPH by Health Canada) 400 to 800 g. Onset of effects is faster with oral or sublingual than with rectal administration. 800 to 1000 g. Effects are longer lasting with rectal than with oral administration. Higher incidence of pyrexia with oral than with rectal administration. 5. Ergonovine 0.25 mg IM or IV, can be repeated every 2 hours Contraindicated in women with hypertension and those taking certain drugs (e.g., proteases for HIV infection). 6. Recombinant activated factor VII Has been used in women with massive PPH but in a limited number of studies, all without randomization. A review by Franchini et al. 48 suggests a potential role, although further research is required to determine this agent s role and benefit. Recommendation 17. Evidence for the benefit of recombinant activated factor VII has been gathered from very few cases of massive PPH. Therefore this agent cannot be recommended as part of routine practice. (II-3L) Tamponade The quickest method of tamponade is with bimanual compression of the uterus. One hand is placed over the uterus externally; the other is placed in the vagina to apply pressure on the lower segment. Consistent compression with the 2 hands results in external compression of the uterus to reduce blood flow. This can be continued until further measures are taken or assistance arrives. In the case of uterine atony, the following can be placed inside the uterus to provide direct compression of the uterine wall and thus decrease blood loss. Bakri SOS tamponade balloon catheter Sengstaken Blakemore esophageal catheter Foley catheter filled with 60 to 80 ml of sterile solution Rusch hydrostatic urologic balloon Hydrostatic condom catheter Uterine packing All the above have been reported to be successful for the temporary control of active bleeding. The insertion technique for a balloon device is relatively simple and requires the operator to ensure that the entire balloon is positioned past the cervical canal. Once inserted, the balloon is filled with sterile solution until there is no further bleeding. After successful tamponade, continued oxytocin infusion may be required to maintain uterine tone. Prophylactic antibiotic therapy should be considered. The balloon can be left in place for 8 to 48 hours and then gradually deflated and removed. Uterine packing requires greater skill and experience to properly pack the uterus with enough gauze to control bleeding while avoiding trauma to the uterine wall. Other disadvantages include risk of infection, unrecognized bleeding with blood soaking the packing material, and the possible need for another surgical procedure to remove the material. Recommendation 18. Uterine tamponade can be an efficient and effective intervention to temporarily control active PPH due to uterine atony that has not responded to medical therapy. (III-L) 990 OCTOBER JOGC OCTOBRE 2009
12 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage Figure 2. B-Lynch technique for uterine compression sutures Reproduced from B-Lynch et al 52 with permission of the Royal College of Obstetricians and Gynaecologists. Figure 3. Cho technique for uterine compression sutures Reproduced from Cho et al 53 with permission of the Royal College of Obstetricians and Gynaecologists. OCTOBER JOGC OCTOBRE
13 SOGC CLINICAL PRACTICE GUIDELINE Radiologic Methods Percutaneous transcatheter arterial embolization is an option when there is active bleeding in a hemodynamically stable woman and before surgical intervention. 49 A review of the literature found success rates of 100% after 49 vaginal deliveries and 89% after 18 Caesarean sections. This technique preserves the uterus and adnexa and thus fertility. The procedure requires rapid access to imaging technology and interventional radiologists, which is not available to all centres. Surgical Methods Ligation of the internal iliac artery was used to control intraoperative bleeding from cervical cancer before being applied to obstetric cases. 50 A retrospective study found this technique to be useful for preventing PPH in women at high risk of hemorrhage and for treating PPH due to uterine atony or genital tract injury. 51 The timing of this intervention is important: it must be done without delay, before excessive blood loss has occurred. Surgical skill is required to avoid failure and complications such as damage to other vascular structures and the ureters. Uterine compression sutures, described by B-Lynch 52 (Figure 2) and Cho 53 (Figure 3), have the benefit of preserving the uterus. Both techniques involve external compression of the uterus to control bleeding, followed by application of sutures into and over the uterus. The sutures are tied down to maintain uterine compression and control further bleeding. A hysterotomy at the lower segment is required to ensure that there are no retained products that would prevent compression of the uterus and subsequent failure of pregnancy. Peripartum hysterectomy is indicated when massive hemorrhage has not responded to previous interventions and requires a surgical intervention familiar to surgeons. Indications include abnormal placentation (previa, accreta), atony, trauma, rupture, and sepsis. The disadvantage of peripartum hysterectomy is the loss of fertility in women who wish to continue childbearing. Recommendation 19. Surgical techniques such as ligation of the internal iliac artery, compression sutures, and hysterectomy should be used for the management of intractable PPH unresponsive to medical therapy. (III-B) REFERENCES 1. AbouZahr C. Global burden of maternal death and disability. Br Med Bull 2003;67: Reynders FC, Senten L, Tjalma W, Jacquemyn Y. Postpartum hemorrhage: practical approach to a life-threatening complication. Clin Exp Obstet Gynecol 2006;33: Subtil D, Sommé A, Ardiet E, Depret-Mosser S. [Postpartum hemorrhage: frequency, consequences in terms of health status, and risk factors before delivery]. J Gynecol Obstet Biol Reprod (Paris) 2004;33(8 Suppl):4S9 4S Ramanathan G, Arulkumaran S. Postpartum haemorrhage. Curr Obstet Gynaecol 2006;16(1): Kane TT, el-kady AA, Saleh S, Hage M, Stanback J, Potter L. Maternal mortality in Giza, Egypt: magnitude, causes, and prevention. Stud Fam Plann 1992;23: Maier RV. Approach to the patient with shock. In: Kasper DL, Braunwald E, Fauci AS, Hauser SL, Longo DL, Jameson JL, editors. Harrison s principles of internal medicine. 16th ed. New York: McGraw-Hill; 2004: Bose P, Regan F, Paterson-Brown S. Improving the accuracy of estimated blood loss at obstetric haemorrhage using clinical reconstructions. BJOG 2006;113: Prendiville WJ, Elbourne D, McDonald S. Active versus expectant management in the third stage of labour. Cochrane Database Syst Rev 2000;(3):CD International Confederation of Midwives, International Federation of Gynaecologists and Obstetricians. Joint statement: management of the third stage of labour to prevent post-partum haemorrhage. J Midwifery Womens Health 2004;49: World Health Organization. Recommendations for the Prevention of Postpartum Haemorrhage. Geneva: WHO; Khan GQ, John IS, Wani S, Doherty T, Sibai BM. Controlled cord traction versus minimal intervention techniques in delivery of the placenta: a randomized controlled trial. Am J Obstet Gynecol 1997;177(4): McDonald S, Abbott JM, Higgins SP. Prophylactic ergometrine oxytocin versus oxytocin for the third stage of labour. Cochrane Database Syst Rev 2004;(1):CD Cotter A, Ness A, Tolosa J. Prophylactic oxytocin for the third stage of labour. Cochrane Database Syst Rev 2001;(4):CD Nordstrom L, Fogelstam K, Fridman G, Larsson A, Rydhstroem H. Routine oxytocin in the third stage of labour: a placebo controlled randomised trial. Br J Obstet Gynaecol 1997;104: Jackson KW Jr, Allbert JR, Schemmer GK, Elliot M, Humphrey A, Taylor J. A randomized controlled trial comparing oxytocin administration before and after placental delivery in the prevention of postpartum hemorrhage. Am J Obstet Gynecol Oct;185(4): Begley C. A comparison of active and physiological management of the third stage of labour. Midwifery 1990;6: Davies GA, Tessier JL, Woodman MC, Lipson A, Hahn PM. Maternal hemodynamics after oxytocin bolus compared with infusion in the third stage of labor: a randomized controlled trial. Obstet Gynecol 2005;105: Thomas JS, Koh SH, Cooper GM. Hemodynamic effects of oxytocin given as IV bolus or infusion on women undergoing caesarean section. Br J Anaesth 2007;98; Svanström MC, Biber B, Hanes M, Johansson G, Näslund U, Balfors EM. Signs of myocardial ischemia after injection of oxytocin: a randomized double-blind comparison of oxytocin and methylergometrine during caesarean section. Br J Anaesth 2008;100: Dansereau J, Joshi AK, Helewa ME, Doran TA, Lange IR, Luther ER, et al. Double-blind comparison of carbetocin versus oxytocin in prevention of uterine atony after cesarean section. Am J Obstet Gynecol 1999;180(3 Pt 1): Sweeney G, Holbrook AM, Levine M, Yip M, Alfredsson K, Cappi S, et al. Pharmacokinetics of a long-acting oxytocin analogue, in non-pregnant women. Curr Ther Res 1990;47: Boucher M, Nimrod CA, Tawagi GF, Meeker TA, Rennicks White RE, Varin J. Comparison of carbetocin and oxytocin for the prevention of 992 OCTOBER JOGC OCTOBRE 2009
14 Active Management of the Third Stage of Labour: Prevention and Treatment of Postpartum Hemorrhage postpartum hemorrhage following vaginal delivery: a double-blind randomized trial. J Obstet Gynaecol Can 2004;26: Su LL, Chong YS, Samuel M. Oxytocin agonists for preventing postpartum hemorrhage. Cochrane Database Syst Rev 2007;(3):CD Leung SW, Ng PS, Wong WY, Cheung TH. A randomized trial of carbetocin versus Syntometrine in the management of the third stage of labour. BJOG 2006;113: El-Refaey H, O Brien P, Morafa W, Walder J, Rodeck C. Misoprostol for third stage of labour [letter]. Lancet 1996;347: Hofmeyr GJ, Walraven G, Gülmezoglu AM, Maholwana B, Alfirevic Z, Villar J. Misoprostol to treat postpartum haemorrhage: a systematic review. BJOG 2005;112: Gülmezoglu AM, Forna F, Villar J, Hofmeyr GJ. Prostaglandins for prevention of postpartum haemorrhage. Cochrane Database Syst Rev 2004;(1):CD Villar J, Gülmezoglu AM, Hofmeyr GJ, Forna F. Systematic review of randomized controlled trials of misoprostol to prevent postpartum hemorrhage. Obstet Gynecol 2002;100: Joy SD, Sanchez-Ramos L, Kaunitz AM. Misoprostol use during the third stage of labor. Int J Gynaecol Obstet 2003;82: Gülmezoglu AM, Villar J, Ngoc NT, Piaggio G, Carroli G, Adetoro L, et al. WHO multicentre randomised trial of misoprostol in the management of the third stage of labour. Lancet 2001;358: Parsons SM, Walley RL, Crane JMG, Matthews K, Hutchens D. Rectal misoprostol versus oxytocin in the management of the third stage of labour. J Obstet Gynaecol Can 2007;29: Morley G. Cord closure: Can hasty clamping injure the newborn? OBG Manage 1998;July: Dixon LR. The complete blood count: physiologic basis and clinical usage. J Perinat Neonatal Nurs 1997;11: Yao AC, Moinian M, Lind J. Distribution of blood between infant and placenta after birth. Lancet 1969;2: Rabe H, Reynolds G, Diaz-Rossello J. Early versus delayed umbilical cord clamping in preterm infants. Cochrane Database Syst Rev 2004;(4):CD Ibrahim HM, Krouskop RW, Lewis DF, Dhanireddy R. Placental transfusion: umbilical cord clamping and preterm infants. J Perinatol 2000;20: Hutton EK, Hassan ES. Late vs early clamping of the umbilical cord in full-term neonates: systematic review and meta-analysis of controlled trials. JAMA 2007;297: McDonald SJ, Middleton P. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev 2008;(2):CD Dombrowski MP, Bottoms SF, Saleh AA, Hurd WW, Romero R. Third stage of labor: analysis of duration and clinical practice. Am J Obstet Gynecol 1995;172: Combs CA, Laros RK. Prolonged third stage of labor; morbidity and risk factors. Obstet Gynecol 1991;77: Magann EF, Doherty DA, Briery CM, Niederhauser A, Morrison JC. Timing of placental delivery to prevent post-partum haemorrhage: lessons learned from an abandoned randomised clinical trial. Aust NZJObstet Gynaecol 2006;46: Soltani H, Dickinson F, Symonds I. Placental cord drainage after spontaneous vaginal delivery as part of the management of the third stage of labour. Cochrane Database Syst Rev 2005;(4):CD Sharma JB, Pundir P, Malhotra M, Arora R. Evaluation of placental drainage as a method of placental delivery in vaginal deliveries. Arch Gynecol Obstet 2005;271: Carroli G, Bergel E. Umbilical vein injection for management of retained placenta. Cochrane Database Syst Rev 2001;(4):CD Nardin JM, Carroli G, Weeks a.d., Mori R. Umbilical vein injection for the routine management of third stage of labour [Protocol]. Cochrane Database Syst Rev 2006;(4):CD Rogers MS, Yuen PM, Wong S. Avoiding manual removal of placenta: evaluation of intra-umbilical injection of uterotonics using the Pipingas technique for management of adherent placenta. Acta Obstet Gynecol 2007;86: Baskett TF. Surgical management of severe obstetrical hemorrhage: experience with an obstetrical hemorrhage equipment tray. J Obstet Gynaecol Can 2004;26: Franchini M, Lippi G, Franchi M. The use of recombinant activated factor VII in obstetric and gynaecological haemorrhage. BJOG 2007;114: Vedantham S, Goodwin SC, McLucas B, Mohr G. Uterine artery embolization: an underused method of controlling pelvic hemorrhage. Am J Obstet Gynecol 1997;176: Kelly HA. Ligation of both internal iliac arteries for hemorrhage in hysterectomy for carcinoma uteri. Bull Johns Hopkins Hosp 1984;5: Joshi V, Otiv SR, Majumder R, Nikam YA, Shrivastava M. Internal iliac artery ligation for arresting postpartum haemorrhage. BJOG 2007;114: B-Lynch C, Coker A, Lawal AH, Abu J, Cowen MJ. The B-Lynch surgical technique for the control of massive postpartum haemorrhage: An alternative to hysterectomy? Five cases reported. Br J Obstet Gynaecol 1997;104: Cho JH, Jun HS, Lee CN. Hemostatic suturing technique for uterine bleeding during cesarean delivery. Obstet Gynecol 2000;96(1): Woolf SH, Battista RN, Angerson GM, Logan AG, Eel W. Canadian Task Force on Preventive Health Care. New grades for recommendations from the Canadian Task Force on Preventive Health Care. CMAJ 2003;169(3): Mathai M, Gulmezoglu AM. Postpartum haemorrhage and retained placenta. WHO guideline. Geneva: World Health Organization;2009. OCTOBER JOGC OCTOBRE
Sign up to receive ATOTW weekly - email worldanaesthesia@mac.com
 MANAGEMENT OF OBSTETRIC HAEMORRAGE ANAESTHESIA TUTORIAL OF THE WEEK 41 1 ST JANUARY 2007 Dr Kath Davies Specialist Registrar in Anaesthesia Dr Matt Rucklidge Consultant Anaesthetist Royal Devon and Exeter
MANAGEMENT OF OBSTETRIC HAEMORRAGE ANAESTHESIA TUTORIAL OF THE WEEK 41 1 ST JANUARY 2007 Dr Kath Davies Specialist Registrar in Anaesthesia Dr Matt Rucklidge Consultant Anaesthetist Royal Devon and Exeter
Obstetric Emergencies for Every Provider
 Obstetric Emergencies for Every Provider James Bates, PhD, MD Associate Professor Director of the division of OB anesthesia Clinical coordinator MOR Department of Anesthesia University of Iowa College
Obstetric Emergencies for Every Provider James Bates, PhD, MD Associate Professor Director of the division of OB anesthesia Clinical coordinator MOR Department of Anesthesia University of Iowa College
WHO Recommendations for the Prevention of Postpartum Haemorrhage Results from a WHO Technical Consultation October 18-20, 2006
 WHO Recommendations for the Prevention of Postpartum Haemorrhage Results from a WHO Technical Consultation October 18-20, 2006 Panel Presentation: M E Stanton, USAID; R Derman, UM/KC; H Sangvhi, JHPIEGO;
WHO Recommendations for the Prevention of Postpartum Haemorrhage Results from a WHO Technical Consultation October 18-20, 2006 Panel Presentation: M E Stanton, USAID; R Derman, UM/KC; H Sangvhi, JHPIEGO;
G THE GLOBAL LIBRARY OF WOMEN S MEDICINE
 the safer motherhood Knowledge Transfer Program Editor-in-Chief: Professor Sir Sabaratnam Arulkumaran The Active Management of the Third Stage of Labor G THE GLOBAL LIBRARY OF WOMEN S MEDICINE www.glowm.com
the safer motherhood Knowledge Transfer Program Editor-in-Chief: Professor Sir Sabaratnam Arulkumaran The Active Management of the Third Stage of Labor G THE GLOBAL LIBRARY OF WOMEN S MEDICINE www.glowm.com
Management of Postpartum Hemorrhage with the SOS Bakri Tamponade Balloon Catheter
 Management of Postpartum Hemorrhage with the SOS Bakri Tamponade Balloon Catheter 1. Introduction 2. Definitions 3. Indications and Contraindications 4. Steps for Effective Application Catheter Placement
Management of Postpartum Hemorrhage with the SOS Bakri Tamponade Balloon Catheter 1. Introduction 2. Definitions 3. Indications and Contraindications 4. Steps for Effective Application Catheter Placement
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
MANAGEMENT OF OBSTETRIC HAEMORRHAGE ANAESTHESIA TUTORIAL OF THE WEEK 257
 MANAGEMENT OF OBSTETRIC HAEMORRHAGE ANAESTHESIA TUTORIAL OF THE WEEK 257 2 ND APRIL 2012 Dr Adrian Jennings, Anaesthetic Registrar Dr James Brunning, Anaesthetic Registrar Dr Catherine Brennan, Consultant
MANAGEMENT OF OBSTETRIC HAEMORRHAGE ANAESTHESIA TUTORIAL OF THE WEEK 257 2 ND APRIL 2012 Dr Adrian Jennings, Anaesthetic Registrar Dr James Brunning, Anaesthetic Registrar Dr Catherine Brennan, Consultant
Priya Rajan, MD Northwestern University September 13, 2013
 Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
Clinical Interruption of Pregnancy (Medical/Surgical Abortion)
 Clinical Interruption of Pregnancy (Medical/Surgical Abortion) Approximately one fifth of all pregnancies in the United States end in abortion (Ventura et al., 2009). According to the CDC (2011a), there
Clinical Interruption of Pregnancy (Medical/Surgical Abortion) Approximately one fifth of all pregnancies in the United States end in abortion (Ventura et al., 2009). According to the CDC (2011a), there
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
EmONC Training Curricula Comparison
 EmONC Training Curricula Comparison The purpose of this guide is to provide a quick resource for trainers and course administrators to decide which EmONC curriculum is most applicable to their training
EmONC Training Curricula Comparison The purpose of this guide is to provide a quick resource for trainers and course administrators to decide which EmONC curriculum is most applicable to their training
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC)
 CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
CLINICAL GUIDELINE FOR VAGINAL BIRTH AFTER CAESAREAN SECTION (VBAC) 1. Aim/Purpose of this Guideline 1.1. Due to a rise in the caesarean section rate there are increasing numbers of pregnant women who
8/13/2014. Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature. Delayed Cord Clamping
 8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
SAMPLE. UK Obstetric Surveillance System. Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery.
 ID Number: UK Obstetric Surveillance System Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery Case Definition: Study 04/11 Data Collection Form - Please report any woman delivering
ID Number: UK Obstetric Surveillance System Management of Pregnancy following Laparoscopic Adjustable Gastric Band Surgery Case Definition: Study 04/11 Data Collection Form - Please report any woman delivering
Maj Alison Baum. R3, Nellis FMR
 Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM
 COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM PREGNANCY WITH ABORTIVE OUTCOME (630 639.9) 630 HYDATIDIFORM MOLE 631 OTHER ABNORMAL PRODUCT OF CONCEPTION 632 MISSED ABORTION 633 ECTOPIC PREGNANCY
COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM PREGNANCY WITH ABORTIVE OUTCOME (630 639.9) 630 HYDATIDIFORM MOLE 631 OTHER ABNORMAL PRODUCT OF CONCEPTION 632 MISSED ABORTION 633 ECTOPIC PREGNANCY
To outline nursing management of patients receiving epidural anesthesia during labor (Includes walking epidurals and combined spinal-epidurals).
 HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
Uterine Balloon Tamponade
 February 2012 Uterine Balloon Tamponade Technology Opportunity Assessment Prepared for the Merck for Mothers Program MAILING ADDRESS PO Box 900922 Seattle, WA 98109 USA ADDRESS 2201 Westlake Avenue Suite
February 2012 Uterine Balloon Tamponade Technology Opportunity Assessment Prepared for the Merck for Mothers Program MAILING ADDRESS PO Box 900922 Seattle, WA 98109 USA ADDRESS 2201 Westlake Avenue Suite
Cornual ruptured pregnancy with placenta increta CORNUAL RUPTURED PREGNANCY WITH PLACENTA INCRETA A RARE CASE
 142 CORNUAL RUPTURED PREGNANCY WITH PLACENTA INCRETA A RARE CASE Agarwal NR 1, Rani A 1 *, Batra S 1 1. Department of Obststetrics and Gynaecology, Institute of Medical Sciences, Banares Hindu Univarsity.
142 CORNUAL RUPTURED PREGNANCY WITH PLACENTA INCRETA A RARE CASE Agarwal NR 1, Rani A 1 *, Batra S 1 1. Department of Obststetrics and Gynaecology, Institute of Medical Sciences, Banares Hindu Univarsity.
Uterine fibroids (Leiomyoma)
 Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
Uterine fibroids (Leiomyoma) What are uterine fibroids? Uterine fibroids are fairly common benign (not cancer) growths in the uterus. They occur in about 25 50% of all women. Many women who have fibroids
WHO Recommendations for the Prevention of Postpartum Haemorrhage
 WHO Recommendations for the Prevention of Postpartum Haemorrhage Department of Making Pregnancy Safer WHO Recommendations for the Prevention of Postpartum Haemorrhage Department of Making Pregnancy Safer
WHO Recommendations for the Prevention of Postpartum Haemorrhage Department of Making Pregnancy Safer WHO Recommendations for the Prevention of Postpartum Haemorrhage Department of Making Pregnancy Safer
Uterine massage for preventing postpartum haemorrhage (Review)
 Uterine massage for preventing postpartum haemorrhage (Review) Hofmeyr GJ, Abdel-Aleem H, Abdel-Aleem MA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and
Uterine massage for preventing postpartum haemorrhage (Review) Hofmeyr GJ, Abdel-Aleem H, Abdel-Aleem MA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and
Tranexamic Acid. Tranexamic Acid. Overview. Blood Conservation Strategies. Blood Conservation Strategies. Blood Conservation Strategies
 Overview Where We Use It And Why Andreas Antoniou, M.D., M.Sc. Department of Anesthesia and Perioperative Medicine University of Western Ontario November 14 th, 2009 Hemostasis Fibrinolysis Aprotinin and
Overview Where We Use It And Why Andreas Antoniou, M.D., M.Sc. Department of Anesthesia and Perioperative Medicine University of Western Ontario November 14 th, 2009 Hemostasis Fibrinolysis Aprotinin and
WHO recommendations for the prevention and treatment of postpartum haemorrhage
 WHO recommendations for the prevention and treatment of postpartum haemorrhage WHO recommendations for the prevention and treatment of postpartum haemorrhage WHO Library Cataloguing-in-Publication Data
WHO recommendations for the prevention and treatment of postpartum haemorrhage WHO recommendations for the prevention and treatment of postpartum haemorrhage WHO Library Cataloguing-in-Publication Data
A report of 300 cases using vacuum aspiration for the termination of pregnancy
 A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
A report of 300 cases using vacuum aspiration for the termination of pregnancy Wu, Yuantai and Wu, Xianzhen Chinese Journal of Obstetrics and Gynaecology (1958:447-9) More than 100 years after Recamier
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Umbilical cord clamping: influence on newborn iron endowment
 Umbilical cord clamping: influence on newborn iron endowment Source: Chaparro and Lutter, PAHO 2007 Anemia prevalence Overview History of cord clamping practices Placental transfusion and effect of delayed
Umbilical cord clamping: influence on newborn iron endowment Source: Chaparro and Lutter, PAHO 2007 Anemia prevalence Overview History of cord clamping practices Placental transfusion and effect of delayed
SOGC Clinical Practice Guideline. Abstract. Key Words: Induction, labour, cervical ripening, post-dates
 No. 296, September 2013 (Replaces No. 107, August 2001) Induction of Labour This clinical practice guideline has been prepared by the Clinical Practice Obstetrics Committee, reviewed by the Maternal Fetal
No. 296, September 2013 (Replaces No. 107, August 2001) Induction of Labour This clinical practice guideline has been prepared by the Clinical Practice Obstetrics Committee, reviewed by the Maternal Fetal
WHO/RHR/12.29. WHO recommendations for the prevention and treatment of postpartum haemorrhage. Evidence base
 WHO/RHR/12.29 WHO recommendations for the prevention and treatment of postpartum haemorrhage Evidence base Contents Standard criteria for grading of evidence... 5 Box 1: Standard criteria for grading
WHO/RHR/12.29 WHO recommendations for the prevention and treatment of postpartum haemorrhage Evidence base Contents Standard criteria for grading of evidence... 5 Box 1: Standard criteria for grading
Certified Professional Midwives Caring for Mothers and Babies in Virginia
 Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Core Topic 3: Uterotonic drugs
 Reference manual Key definitions Core Topic 3: Uterotonic drugs Tonic or tetanic contractions: Continuous contractions with no relaxation. Uterotonics: Substances that stimulate uterine contractions or
Reference manual Key definitions Core Topic 3: Uterotonic drugs Tonic or tetanic contractions: Continuous contractions with no relaxation. Uterotonics: Substances that stimulate uterine contractions or
CLINICAL PRACTICE GUIDELINE PREVENTION AND MANAGEMENT OF PRIMARY POSTPARTUM HAEMORRHAGE
 CLINICAL PRACTICE GUIDELINE PREVENTION AND MANAGEMENT OF PRIMARY POSTPARTUM HAEMORRHAGE Institute of Obstetricians and Gynaecologists Royal College of Physicians of Ireland and Directorate of Strategy
CLINICAL PRACTICE GUIDELINE PREVENTION AND MANAGEMENT OF PRIMARY POSTPARTUM HAEMORRHAGE Institute of Obstetricians and Gynaecologists Royal College of Physicians of Ireland and Directorate of Strategy
UNMH Certified Nurse-Midwife (CNM) Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 03/27/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
How To Know The Effects Of Cord Clamping
 Delayed Cord Clamping: Worth the Wait? Ryan M. McAdams MD Disclosure Neither I nor any member of my immediate family has a financial relationship or interest with any proprietary entity producing health
Delayed Cord Clamping: Worth the Wait? Ryan M. McAdams MD Disclosure Neither I nor any member of my immediate family has a financial relationship or interest with any proprietary entity producing health
Bladder Injury during Cesarean Section: A Case Control Study for 10 Years
 Bahrain Medical Bulletin, Vol., No., September Bladder Injury during Cesarean Section: A Case Control Study for Years Mesfer Al-Shahrani, MD, FRCSC* Objective: To determine the incidence, risk factors
Bahrain Medical Bulletin, Vol., No., September Bladder Injury during Cesarean Section: A Case Control Study for Years Mesfer Al-Shahrani, MD, FRCSC* Objective: To determine the incidence, risk factors
Assessment of Fetal Growth
 Assessment of Fetal Growth Unit / Trust: 1. INTRODUCTION The aim of this guideline template is to outline the methods used to assess fetal growth and the referral pathways utilising customised antenatal
Assessment of Fetal Growth Unit / Trust: 1. INTRODUCTION The aim of this guideline template is to outline the methods used to assess fetal growth and the referral pathways utilising customised antenatal
FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS
 FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS Presentation to Healthy Mothers, Healthy Babies Conference Perinatal Services BC February 22 nd, 2014 Ivy Fernando, RN BSN, PNC(C)
FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS Presentation to Healthy Mothers, Healthy Babies Conference Perinatal Services BC February 22 nd, 2014 Ivy Fernando, RN BSN, PNC(C)
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS
 UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
Pain Relief during Labour and Delivery: What Are My Options?
 Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Effects of Pregnancy & Delivery on Pelvic Floor
 Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
Effects of Pregnancy & Delivery on Pelvic Floor 吳 銘 斌 M.D., Ph.D. 財 團 法 人 奇 美 醫 院 婦 產 部 婦 女 泌 尿 暨 骨 盆 醫 學 科 ; 台 北 醫 學 大 學 醫 學 院 婦 產 學 科 ; 古 都 府 城 台 南 Introduction Pelvic floor disorders (PFDs) include
From Journal of Midwifery & Women's Health Delayed Clamping of the Umbilical Cord: A Review with Implications for Practice
 www.medscape.com From Journal of Midwifery & Women's Health Delayed Clamping of the Umbilical Cord: A Review with Implications for Practice Gina Eichenbaum-Pikser, CNM, MSN; Joanna S. Zasloff, CNM, MSN
www.medscape.com From Journal of Midwifery & Women's Health Delayed Clamping of the Umbilical Cord: A Review with Implications for Practice Gina Eichenbaum-Pikser, CNM, MSN; Joanna S. Zasloff, CNM, MSN
Carry out vaginal examinations at least once every 4 hours in the first stage of labour and plot the findings on the partograph.
 First stage: Diagnosis of Labour Latent phase - Cervix less than 4 cm dilated. Active phase - Cervix between 4 cm and 10 cm dilated - Rate of cervical dilatation at least 1 cm/hour - Effacement is usually
First stage: Diagnosis of Labour Latent phase - Cervix less than 4 cm dilated. Active phase - Cervix between 4 cm and 10 cm dilated - Rate of cervical dilatation at least 1 cm/hour - Effacement is usually
IMAP Statement on Safe Abortion
 International Planned Parenthood Federation IMAP Statement on Safe Abortion Key points: When performed early in pregnancy by trained health personnel in adequate facilities, abortion is a very safe procedure
International Planned Parenthood Federation IMAP Statement on Safe Abortion Key points: When performed early in pregnancy by trained health personnel in adequate facilities, abortion is a very safe procedure
SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES
 SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES TABLE OF CONTENTS SUBJECT PAGE ADULT CRITERIA Red Blood Cells/Autologous 2 Washed Red Blood Cells 2 Cryoprecipitate
SARASOTA MEMORIAL HOSPITAL BLOOD COMPONENT CRITERIA AND INDICATIONS SCREENING GUIDELINES TABLE OF CONTENTS SUBJECT PAGE ADULT CRITERIA Red Blood Cells/Autologous 2 Washed Red Blood Cells 2 Cryoprecipitate
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Document Classification
 Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Emergency Scenarios with Case Review. Hemorrhage. 1) The person facilitating scenarios can print out the pages below.
 Emergency Scenarios with Case Review Hemorrhage This emergency scenario is about patient with hemorrhage following an abortion, and is set up for role-play and case review with your staff. 1) The person
Emergency Scenarios with Case Review Hemorrhage This emergency scenario is about patient with hemorrhage following an abortion, and is set up for role-play and case review with your staff. 1) The person
4/15/2013. Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net
 Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net List the potential complications associated with diabetes during labor. Identify the 2 most important interventions essential
Maribeth Inturrisi RN MS CNS CDE Perinatal Diabetes Educator mbturris@comcast.net List the potential complications associated with diabetes during labor. Identify the 2 most important interventions essential
Preventing Postpartum Hemorrhage: Managing the Third Stage of Labor
 Maternal and Neonatal Health Special Issue OUT Preventing Postpartum Hemorrhage: Managing the Third Stage of Labor Pregnancy and childbirth involve significant health risks, even for women with no preexisting
Maternal and Neonatal Health Special Issue OUT Preventing Postpartum Hemorrhage: Managing the Third Stage of Labor Pregnancy and childbirth involve significant health risks, even for women with no preexisting
Summa Health System. A Woman s Guide to Hysterectomy
 Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Section Two: Arterial Pressure Monitoring
 Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Birth after previous caesarean. What are my choices for birth after a caesarean delivery?
 Birth after previous caesarean Information for you Published September 2008 What are my choices for birth after a caesarean delivery? More than one in five women (20%) in the UK currently give birth by
Birth after previous caesarean Information for you Published September 2008 What are my choices for birth after a caesarean delivery? More than one in five women (20%) in the UK currently give birth by
Primary postpartum haemorrhage
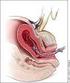 Primary postpartum haemorrhage Document title: Primary postpartum haemorrhage Publication date: December 2012 Document number: Document supplement Amendments: MN12.1-V4-R17 The document supplement is integral
Primary postpartum haemorrhage Document title: Primary postpartum haemorrhage Publication date: December 2012 Document number: Document supplement Amendments: MN12.1-V4-R17 The document supplement is integral
Red Flags that should not be ignored
 Pregnancy that should not be ignored If a pregnant woman tells you she is experiencing any of the following symptoms during pregnancy, assist her to contact her emergency care professional right away.
Pregnancy that should not be ignored If a pregnant woman tells you she is experiencing any of the following symptoms during pregnancy, assist her to contact her emergency care professional right away.
Registered Midwife Clinical Privileges REAPPOINTMENT 2015-2016 Effective from July 1, 2015 to June 30, 2016
 Name: Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the governing body, effective: 04/Jun/2013. Applicant:
Name: Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the governing body, effective: 04/Jun/2013. Applicant:
ALTERNATIVE TREATMENT PLAN AND CONSENT FOR MEDICAL ABORTION WITH MIFEPREX (MIFEPRISTONE) AND MISOPROSTOL
 ALTERNATIVE TREATMENT PLAN AND CONSENT FOR MEDICAL ABORTION WITH MIFEPREX (MIFEPRISTONE) AND MISOPROSTOL The FDA gave its approval status to Mifepristone in 1996 based on research up to that time. Extensive
ALTERNATIVE TREATMENT PLAN AND CONSENT FOR MEDICAL ABORTION WITH MIFEPREX (MIFEPRISTONE) AND MISOPROSTOL The FDA gave its approval status to Mifepristone in 1996 based on research up to that time. Extensive
Facts for Women Termination of pregnancy, abortion, or miscarriage management
 Patient Education Facts for Women Termination of pregnancy, abortion, or miscarriage management This handout answers common questions about miscarriage management and the termination of a pregnancy, also
Patient Education Facts for Women Termination of pregnancy, abortion, or miscarriage management This handout answers common questions about miscarriage management and the termination of a pregnancy, also
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates
 Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse
 Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse Decision support tools are evidenced-based documents used to guide the assessment, diagnosis and
Registered Nurse Initiated Activities Decision Support Tool No. 8A: Obstetrical Emergencies Cord Prolapse Decision support tools are evidenced-based documents used to guide the assessment, diagnosis and
Chapter 14. Board of Certified Direct-Entry Midwives.
 Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
EARLY PREGNANCY LOSS A Patient Guide to Treatment
 EARLY PREGNANCY LOSS A Patient Guide to Treatment You have a pregnancy that has stopped growing, or you have started to miscarry and the process has not completed. If so, there are four ways to manage
EARLY PREGNANCY LOSS A Patient Guide to Treatment You have a pregnancy that has stopped growing, or you have started to miscarry and the process has not completed. If so, there are four ways to manage
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
Birth after Caesarean Choices for delivery
 Birth after Caesarean Choices for delivery page 2 What are my choices for birth after a Caesarean? Currently, approximately 1 in 4 women (25%) in England give birth by Caesarean delivery. Some women have
Birth after Caesarean Choices for delivery page 2 What are my choices for birth after a Caesarean? Currently, approximately 1 in 4 women (25%) in England give birth by Caesarean delivery. Some women have
Coagulation Disorders In Pregnancy
 Coagulation Disorders In Pregnancy Dr Rashmi Sharma, M.D, FRCA SpR Anaesthetics Blackburn Royal Infirmary Dr Anna Bewlay FRCA Consultant Anaesthetist Royal Preston Hospital Physiological changes in pregnancy
Coagulation Disorders In Pregnancy Dr Rashmi Sharma, M.D, FRCA SpR Anaesthetics Blackburn Royal Infirmary Dr Anna Bewlay FRCA Consultant Anaesthetist Royal Preston Hospital Physiological changes in pregnancy
Delayed Cord Clamping
 Delayed Cord Clamping Jeanette Zaichkin RN, MN, NNP-BC Jeanette.zaichkin@outlook.com Washington Section AWHONN Spring Conference May 28, 2015 Learning Objectives Examine the literature regarding early
Delayed Cord Clamping Jeanette Zaichkin RN, MN, NNP-BC Jeanette.zaichkin@outlook.com Washington Section AWHONN Spring Conference May 28, 2015 Learning Objectives Examine the literature regarding early
A Guide to Hysteroscopy. Patient Education
 A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
A Guide to Hysteroscopy Patient Education QUESTIONS AND ANSWERS ABOUT HYSTEROSCOPY Your doctor has recommended that you have a procedure called a hysteroscopy. Naturally, you may have questions about
Uterus myomatosus. 10-May-15. Clinical presentation. Incidence. Causes? 3 out of 4 women. Growth rate vary. Most common solid pelvic tumor in women
 Uterus myomatosus A.J. Henriquez March 14, 2015 Uterus myomatosus Definition, incidence, clinical presentation and diagnosis. New FIGO classification for uterine leiomyomas Brief description on treatment
Uterus myomatosus A.J. Henriquez March 14, 2015 Uterus myomatosus Definition, incidence, clinical presentation and diagnosis. New FIGO classification for uterine leiomyomas Brief description on treatment
PHENYLEPHRINE HYDROCHLORIDE INJECTION USP
 PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
PRESCRIBING INFORMATION PHENYLEPHRINE HYDROCHLORIDE INJECTION USP 10 mg/ml Sandoz Canada Inc. Date of Preparation: September 1992 145 Jules-Léger Date of Revision : January 13, 2011 Boucherville, QC, Canada
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274
 Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
ONTARIO MEDICAL ASSOCIATION. Submission to the Health Professions Regulatory Advisory Council Respecting Issues Related to Midwifery Scope of Practice
 !! " #$% &'()*+, -. /'01'233/ 4'01 '2// &'33453/6 /6/4' 3//340//4 3/'63/ '0// 47/346&'3/8 3/6533/% /6 " / 4'04/34// 34//" 54// 3/ 9$$ ONTARIO MEDICAL ASSOCIATION Submission to the Health Professions Regulatory
!! " #$% &'()*+, -. /'01'233/ 4'01 '2// &'33453/6 /6/4' 3//340//4 3/'63/ '0// 47/346&'3/8 3/6533/% /6 " / 4'04/34// 34//" 54// 3/ 9$$ ONTARIO MEDICAL ASSOCIATION Submission to the Health Professions Regulatory
Pain Relief Options for Labor. Providing You with Quality Care, Information and Support
 Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
WHAT YOU SHOULD KNOW ABOUT ABORTION
 WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
INTRAVENOUS FLUIDS. Acknowledgement. Background. Starship Children s Health Clinical Guideline
 Acknowledgements Background Well child with normal hydration Unwell children (+/- abnormal hydration Maintenance Deficit Ongoing losses (e.g. from drains) Which fluid? Monitoring Special Fluids Post-operative
Acknowledgements Background Well child with normal hydration Unwell children (+/- abnormal hydration Maintenance Deficit Ongoing losses (e.g. from drains) Which fluid? Monitoring Special Fluids Post-operative
How To Test For Fetal Blood
 Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
WHAT YOU SHOULD KNOW ABOUT ABORTION
 WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
WHAT YOU SHOULD KNOW ABOUT ABORTION It is the public policy of the state of Idaho to prefer live childbirth over abortion: "The Supreme Court of the United States having held that the states have a "profound
BEST- Practice Management Guidelines B: BEST Decision E: Evidence-Based S: Simple & Safe T: Team Focused
 OB Excellence: Postpartum Hemorrhage [PPH]-DATA ANALYSIS Perinatal University Speaker/Master Instructor: Carol A. Curran RNC, MS, OGNP CEO & Founder: Clinical Specialists Consulting & Perinatal University
OB Excellence: Postpartum Hemorrhage [PPH]-DATA ANALYSIS Perinatal University Speaker/Master Instructor: Carol A. Curran RNC, MS, OGNP CEO & Founder: Clinical Specialists Consulting & Perinatal University
This Protocol is adapted from the University of Colorado Protocol dated August 26, 2009.
 Protocol for Post-Placental IUD insertion July 14, 2010 This Protocol is adapted from the University of Colorado Protocol dated August 26, 2009. Background Post-placental intrauterine device (IUD) insertion
Protocol for Post-Placental IUD insertion July 14, 2010 This Protocol is adapted from the University of Colorado Protocol dated August 26, 2009. Background Post-placental intrauterine device (IUD) insertion
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Catheter Embolization and YOU
 Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation
 Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
Guideline Statement for the Treatment of Disseminated Intravascular Coagulation Introduction Though a rare occurrence in the perioperative setting, disseminated intravascular coagulation (DIC) is a syndrome
Maternity - Clinical Risk Management Program
 Maternity - Clinical Risk Management Document Number PD2009_003 Publication date 15-Jan-2009 Ministry of Health, NSW 73 Miller Street North Sydney NSW 2060 Locked Mail Bag 961 North Sydney NSW 2059 Telephone
Maternity - Clinical Risk Management Document Number PD2009_003 Publication date 15-Jan-2009 Ministry of Health, NSW 73 Miller Street North Sydney NSW 2060 Locked Mail Bag 961 North Sydney NSW 2059 Telephone
Giving birth in Bronovo. Welcome! Presentatie Verloskunde en Gynaecologie
 Giving birth in Bronovo Welcome! Welcome to Bronovo Content of presentation Preparation The birth When it doesn't go to plan Pain relief Practical information Preparation Medical care from the midwife
Giving birth in Bronovo Welcome! Welcome to Bronovo Content of presentation Preparation The birth When it doesn't go to plan Pain relief Practical information Preparation Medical care from the midwife
NovaSure: A Procedure for Heavy Menstrual Bleeding
 NovaSure: A Procedure for Heavy Menstrual Bleeding The one-time, five-minute procedure Over a million women 1 have been treated with NovaSure. NovaSure Endometrial Ablation (EA) is the simple, one-time,
NovaSure: A Procedure for Heavy Menstrual Bleeding The one-time, five-minute procedure Over a million women 1 have been treated with NovaSure. NovaSure Endometrial Ablation (EA) is the simple, one-time,
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Placenta, Cord, & Fluid
 , Cord, & Fluid Abruption Accreta/Increta/Percreta Chorioangioma Complete Partial Not generally Relevant to U/S Gestational Age (Weeks) Distance from 16-23.9 24 to Internal Os >20 mm No No 11-20 mm 0-10
, Cord, & Fluid Abruption Accreta/Increta/Percreta Chorioangioma Complete Partial Not generally Relevant to U/S Gestational Age (Weeks) Distance from 16-23.9 24 to Internal Os >20 mm No No 11-20 mm 0-10
Vaginal or Cesarean Birth:
 Vaginal or Cesarean Birth: What Is at Stake for Women and Babies? A Best Evidence Review Executive Summary Contributors Henci Goer Amy Romano, MSN, CNM Carol Sakala, PhD, MSPH 2012, Childbirth Connection
Vaginal or Cesarean Birth: What Is at Stake for Women and Babies? A Best Evidence Review Executive Summary Contributors Henci Goer Amy Romano, MSN, CNM Carol Sakala, PhD, MSPH 2012, Childbirth Connection
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
To provide safe and standardized nursing care for the patient requiring induction or augmentation of labor.
 Policy: Guidelines for the Management of Patients Undergoing Induction or Labor & Delivery Effective Date May 2012 Approval Date May 2012 Supersedes September 2011 Applicable to VUH Children s Hospital
Policy: Guidelines for the Management of Patients Undergoing Induction or Labor & Delivery Effective Date May 2012 Approval Date May 2012 Supersedes September 2011 Applicable to VUH Children s Hospital
Women, Children and Sexual Health Division Maternity Services. Guideline: Anti D- Prophylaxis
 Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
Women, Children and Sexual Health Division Maternity Services Guideline: Anti D- Prophylaxis 1. Introduction The National Institute for Clinical Excellence recommend routine antenatal anti-d prophylaxis
The Clinical Content of Preconception Care: Alcohol, Tobacco, and Illicit Drug Exposures
 The Clinical Content of Preconception Care: Alcohol, Tobacco, and Illicit Drug Exposures by R. Louise Floyd, DSN, RN; Brian W. Jack, MD; Robert Cefalo, MD, PhD; Hani Atrash, MD, MPH; Jeanne Mahoney, BSN,
The Clinical Content of Preconception Care: Alcohol, Tobacco, and Illicit Drug Exposures by R. Louise Floyd, DSN, RN; Brian W. Jack, MD; Robert Cefalo, MD, PhD; Hani Atrash, MD, MPH; Jeanne Mahoney, BSN,
MANA Home Birth Data 2004-2009: Consumer Considerations
 MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
Paediatric fluids 13/06/05
 Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Dr Catharine Wilson Consultant Paediatric Anaesthetist Sheffield Children s Hospital. UK Paediatric fluids 13/06/05 Self assessment: Complete these questions before reading the tutorial. Discuss the answers
Using the UN Process Indicators of Emergency Obstetric Services. Questions and Answers
 AMDD Workbook Using the UN Process Indicators of Emergency Obstetric Services Questions and Answers Contributors: Anne Paxton Senior Program Officer Monitoring and Evaluation, AMDD Deborah Maine Program
AMDD Workbook Using the UN Process Indicators of Emergency Obstetric Services Questions and Answers Contributors: Anne Paxton Senior Program Officer Monitoring and Evaluation, AMDD Deborah Maine Program
