Stoma Care for Health Care Assistants
|
|
|
- Christian May
- 9 years ago
- Views:
Transcription
1 Stoma Care for Health Care Assistants
2 Introduction Contents To the Healthcare Assistant The role of the Healthcare Assistant (HCA), also known as the Healthcare Support worker (HCSW), is increasingly recognised and valued in a variety of healthcare settings. As HCAs take on a wider range of activities, they require the knowledge, understanding and skills to become competent practitioners. Skills for Health (SfH), the Sector Skills Council for UK health care, has developed a range of workforce competencies including one for stoma care Unit CHS10, Undertake stoma care (level 3). Stoma Care for Healthcare Assistants has been designed to reflect the performance criteria and knowledge detailed in CHS10. Working through this booklet and the accompanying workbook, together with practical experience in your workplace, will help you to become competent in caring for patients with a stoma. Although the booklet is aimed at healthcare assistants who work in hospitals, most of the knowledge it contains may be applied in a variety of settings, including primary care. Learning outcomes. On completion of the booklet the reader should be able to: Identify the different types of stoma, why they are formed and their normal function. Recognise stoma abnormalities. Discuss the importance of effective communication in stoma care, including cultural and religious considerations. Describe the role of the Stoma Care Nurse and the HCA in caring for patients with a stoma. Describe care of the stoma patient in the immediate post-operative period. Describe the support a patient may need to become independent with stoma care. Demonstrate an understanding of the general dietary requirements for the 3 types of stoma. Demonstrate an understanding of products used in stoma care. Describe requirements for the safe discharge from hospital of a patient with a stoma. What is a stoma? 4 How the digestive system usually works 5 Stoma operations 6 Colostomy 7 Ileostomy 8 Urostomy 9 Role of the Stoma Care Nurse Specialist 10 Role of the SCN and HCA in the patient pathway 11 Effective communication verbal 12 Effective communication written 13 Cultural and religious considerations 14 Post-operative care 15 Stoma management recognising abnormalities 17 Products used in the management of stomas 19 Teaching the patient self care 22 Basic dietary advice for patients with stomas 26 Safe discharge 28 Bibliography 29 Useful Contact Details & Acknowledgements 30 Notes 31
3 What is a Stoma? How the digestive system usually works The word stoma is from the Greek word for mouth and is a surgically created opening in the body. There are three main types of stoma u Colostomy a stoma formed in the colon (large intestine or bowel). u Ileostomy a stoma formed in the ileum (small intestine or bowel). u Urostomy different from the other two types of stoma because it is not formed in the digestive system but in the urinary tract (see page 9). Common reasons why a stoma may be necessary include: Obstruction or blockage of the bowel/bladder Perforation of the bowel Removal of severely diseased bowel or bladder Common conditions which may sometimes require a stoma include: Bowel or bladder cancer Formation of a stoma Diverticular disease Ulcerative colitis Crohn s disease Birth abnormalities of the bowel or bladder in children A colostomy and an ileostomy may be carried out as a temporary measure (while, for example, another area of the bowel is being allowed to heal), or as a permanent measure. A urostomy is usually carried out as a permanent measure. With all three types of stoma, the patient has no control over the output and so will have to wear a pouch or bag on their abdomen to collect either faeces (colostomies and ileostomies) or urine (urostomy). End Stoma An end stoma is when just one end of the bowel is formed into a stoma. Digestion begins in the mouth where food is chewed. Swallowed food passes down the oesophagus (1) into the stomach (2). The stomach acts like a liquidizer, churning the food in digestive juices until it is reasonably liquid and passing it into the ileum (3) also known as the small intestine or small bowel. The small intestine is the longest portion of the digestive system it is more than 6 metres long. The food passes along the small intestine (the walls of the intestines contain muscles that expand and contract to move the food onwards this is called peristalsis). During its journey through the small intestine most of the nutrients in the food are absorbed into the body, leaving a fairly liquid mixture of indigestible matter and water. This matter passes into the large intestine, or colon (4), which is about 1.5 metres long. The colon s main job is to take water back into the body, maintaining the body s fluid balance. This leaves the indigestible or waste matter (faeces) in a semi-solid form. At the end of the colon, waste material is stored in the rectum (5) before being expelled through the anus (6). å ç è é ê ë å Oesophagus ç Stomach é Small intestine - Ileum è Large intestine Colon ê Rectum ë Anus Loop Stoma A loop of bowel is brought out through the abdomen. The opened edges are then sutured to the skin. The stoma has two different openings, a functioning opening (proximal loop) and a non-functioning end (distal loop). A loop is sometimes supported by a bridge in the early stages. 4 5
4 Stoma operations Colostomy Abdominoperineal Excision of Rectum Colostomy Hartmann s Procedure Right Transverse Colostomy (Defunctioning) Sometimes a part of the rectum and/or colon has to be removed completely (or temporarily bypassed). This means the faeces produced by the body can no longer leave the body via the anus in the usual way. The surgeon therefore needs to create a new outlet for waste material to be passed and this is done by making an opening onto the abdomen at the front of the body. Resected bowel Panproctocolectomy Sigmoid Colostomy Resected bowel Sigmoid Colostomy Proximal loop Distal loop Ileostomy Total Colectomy Anterior Resection with defunctioning ileostomy How it is formed A colostomy is a surgically created opening in the large intestine or colon. The colon (bowel) is brought through the abdominal wall and sutured to the skin. A colostomy can be formed anywhere in the colon but is commonly positioned on the left side of the abdomen. It may be either a temporary or permanent measure. Appearance A colostomy looks like a small spout, deep pink in colour similar to the inside of the mouth. Although it looks raw, it has no feeling. Waste matter (faeces) comes out of the stoma and is collected in a special stoma pouch fitted over it. End colostomy Loop colostomy Normal output The colon usually absorbs water from the waste as it moves along towards the rectum. So the further along the colon the stoma is sited, the thicker and more formed the waste matter or faeces coming out of the stoma will be. å ç The opened part of the colon (1) Transverse or (2) Sigmoid is brought through the abdominal wall and stitched to the skin on the surface of the abdomen. Appliance A closed stoma pouch is generally used and is attached over the stoma. A colostomate usually changes their appliance once, twice or up to three times a day. Resected bowel End Ileostomy Resected Rectum End Loop Rectal stump Resected bowel Ileostomy ileostomy bowel 6 7
5 Ileostomy Urostomy An ileostomy is a similar type of procedure to a colostomy, except that the stoma is created in the ileum (small intestine) rather than in the colon (large intestine). An ileostomy may be created as a temporary or permanent measure. How it is formed An ileostomy is a surgically created opening in the small bowel, the ileum. The end part of the ileum (terminal ileum) is brought through the abdominal wall and sutured to the skin. An ileostomy is generally formed on the right side of the abdomen, usually with a slightly longer spout than a colostomy (because the output is more liquid). Appearance The stoma looks like a spout, deep pink in colour similar to the inside of the mouth. Although it looks raw, it has no feeling. Waste matter (faeces) comes out of the stoma and is collected in a special stoma pouch affixed over it. Normal Output Because the waste matter has not travelled round the colon, little water is absorbed from it and the faeces that comes out of an ileostomy is usually more liquid and in greater amounts than that from a colostomy. The average volume of output is between ml in 24 hours. An abnormal output would be more than a litre of liquid passed. Mucous Fistula Sometimes, if the rectum has not been removed but is left in place, the cut end of that may also be brought to the surface to make a small opening called a mucous fistula. Initially after surgery, excess mucus will drain through the mucous fistula and sometimes, especially when surgery is undertaken as an emergency procedure, retained faeces may pass through. At first, a small drainable pouch will be used; usually after two weeks or so a stoma cap or small dressing is adequate All or part of the colon (1) is removed and sometimes the rectum (4) too. The end part of the ileum (2) is brought through an opening made in the abdomen (3) and stitched in place. 2 4 Appliance An ileostomate usually needs to wear a drainable pouch, so that the pouch may be easily emptied several times a day, on average between 4-6 times in twenty-four hours. The pouch itself is generally changed every day or every other day, according to choice. How the urinary system usually works In carrying out its functions, the body naturally produces waste chemicals that pass into the blood. The kidneys continuously filter the blood to remove the waste matter. The resulting urine travels from the kidneys through the ureters to the bladder, where it is stored. It is then passed or excreted out of the body via the urethra. What happens with a urostomy With a urostomy, urine is no longer passed in the usual way. Instead of being excreted via the bladder and urethra, the urine passes down the ureters from the kidneys and is then diverted out to the surface via an opening (a stoma) on the abdomen. The stoma is usually situated on the right hand side of the abdomen. How is the stoma formed? To create the stoma that opens onto the abdomen, the surgeon usually removes a short piece of the ileum (small intestine) and uses it to fashion a kind of tube or spout known as an ileal conduit. (The rest of the ileum is rejoined so that the digestive system functions just the same as before.) The two ureters are plumbed in to the ileal conduit which opens on to the abdomen as a stoma. Normal Output The normal output from a urostomy is a continuous flow of urine, which sometimes contains mucus. Appliance Urostomates use a urostomy pouch with a tap which will require emptying several times in twenty-four hours. Urostomates often use a continuous drainable bag at night. The pouch is usually changed every day or every other day. Right Kidney Right Ureter The ileal conduit opens on to the surface of the skin as the urostomy Bladder Urethra A section of the ileum is used to form the ileal conduit Urostomy night drainage system Left Kidney Left Ureter The ureters are diverted from the bladder into the new ileal conduit 9
6 Role of the Stoma Care Nurse Specialist Role of the SCN and HCA in the patient pathway Patients who have a stoma formed have particular needs for specialist information, technical skills to manage their stoma and also emotional support. The Stoma Care Nurse (SCN) is responsible for providing a service which meets these needs. The specific role of the Stoma Care Nurse Specialist varies between localities but many see patients both in the hospital and the community as well as holding nurse led clinics. There are several components to the role of the stoma care nurse as detailed below. Pathway Stoma Nurse activities HCA activities Pre-operatively Before admission: Patient referred to SCN if stoma surgery indicated Elective patients normally referred prior to admission Emergency patients should be referred to SCN at earliest opportunity Patient admitted Gives detailed stoma information Demonstrates pouch change Provides psychological support Arranges voluntary visitor if required Marks stoma site Check that patient has been referred to SCN Provide reassurance Inform SCN of admission Check stoma sited prior to theatre Component Clinical Resource Education Management Example Manages a clinical caseload - provides direct patient care and guides management of stoma care for new and established patients. Provides specialist advice on stoma care as member of hospital Multi-Disciplinary Team (MDT). Liaises with community team. Resource for other parties concerned, e.g. voluntary groups, appliance manufacturers. Provides formal stoma care teaching e.g. study days. Informal ward based teaching. One-to-one & shadowing. Develops educational resources. Management and administration of Stoma Care Service in hospital and primary care. Post-operatively All HCA actions to be carried out on each shift Discharge Assesses stoma & output regularly for any abnormalities Selects appropriate pouch & reviews according to individual needs Teaches patient self care of stoma Provides ongoing psychological support to patient Liaises with MDT & community team to enable safe discharge Arranges appropriate supplies for home Provides home visit within 1 week of discharge Monitor and record stoma function. Report any abnormalities Assist patient with diet to maintain stoma function Carry out stoma care according to care plan; record activity Report any problems Ensure adequate supply of appliances available at patient s bedside at all times Provide active support for patient in learning self care, maintaining privacy and dignity Record progress & report any problems Encourage patient to communicate feelings and concerns Report as required to enable needs to be met Check patient understands arrangements made for discharge and knows how to contact SCN Check patient has adequate (2 weeks) supplies to take home Change agent Development of stoma service in line with medical advances and changes in healthcare provision. Rehabilitation Regular follow up at nurse-led community stoma clinic (or home visits) for 3-6 months Liaises with community team Research/Audit May be involved in formal stoma care research, product trials. Audit of stoma care service. Ongoing support Telephone support as required Stoma clinic appointments as required Annual Stoma check-up offered 10 11
7 Effective Communication Verbal Effective Communication Written A stoma has a great impact on a patient s body image and self esteem. Take a moment to consider how you would feel if you were told you had to wear a pouch on your abdomen to collect faeces or urine and how this would affect the way you thought about your body. In communicating with patients with regard to stoma care, you need to take account of both their practical and emotional needs. Practical needs how the stoma is managed/looked after particularly when the patient has just undergone major surgery and/or is elderly or frail. Emotional needs how the patient feels about their condition. Sensitive communication includes using the right kind of language and being aware of your facial expressions. Dealing with a stoma is a very intimate and personal subject. Consider how you can ensure a private, confidential and safe environment when you are communicating with a stoma patient. Listen to the patient let them talk about their concerns and worries. These might include: worry about the appearance of the stoma, whether it shows under clothing, is there any odour, how will they manage their stoma, fear of leakage, reaction from other people, effect on work or social activities. You may feel that the SCN or other nursing staff should be informed so that the patient s concerns can be dealt with and their needs met. There are also patient booklets that give information and support. On the practical side, when helping patients with stoma management/care, you need to support them in a manner which promotes dignity, privacy and self-respect. You can do this by: Obtaining consent before proceeding. Agree the best place for pouch changing, e.g. the bathroom. Assist patients to retain their modesty during the procedure. Recognise any concerns about odour, e.g. by using a special deodorant spray. Effective communication also includes written communication recording events in writing. It is important to have accurate and timely recording and reporting in order to maintain the continuity of stoma care, so that everyone knows what is going on and what has been done. You should know how and when to refer to the SCN for advice and information. When stoma patients are admitted, promptly notify the Stoma Care Nurse. Have you got the contact details of the SCN readily available? When does the SCN routinely visit your ward/department? On every shift, record all stoma care procedures in the appropriate documentation, e.g. Care Plan, Care Pathway, Fluid Balance Chart. You need to record: any procedure being carried out and why. e.g. pouch emptying routine pouch change routine pouch change because of leakage stoma output record the amount (volume), colour and consistency. stoma condition/colour and report any changes or problems, e.g. sudden swelling, stoma unusually pale or dark, sore skin around the stoma. the patient s progress towards independence with self-care of stoma; note anything which the patient finds difficult. When stoma patients are due for discharge, promptly notify the Stoma Care Nurse of the planned discharge date. (See also further information on discharge on page 28 Safe Discharge). You can help stoma patients to achieve independence in looking after their stoma by encouraging them to participate in stoma care (according to their stage in the care pathway). Observe their technique and give guidance accordingly. Use a step-by-step changing guide to assist the patient through the process. Consider what factors affect the amount of assistance they require, e.g. medical condition, age, disability, level of dexterity, confidence and etc
8 Cultural and religious considerations Post-operative care Religious and cultural influences may affect how a patient and their family reacts to a stoma and have implications for stoma care. For example, in certain cultures, having a stoma may be regarded as unclean, adding to the difficulties for the patient in adjusting. Ritual washing before prayer is required within some faiths, such as Islam or Hinduism. This may mean changing the stoma pouch more frequently; they may also wish to use running water. The siting of the stoma above or below the level of the umbilicus may be important to a devout Muslim who may also be reluctant to use their right hand when cleaning their stoma (the right hand being used for eating, the left hand for cleaning and hygiene). Particular dietary requirements or the need for fasting can affect the frequency and consistency of the stoma output and therefore how often the pouch needs emptying or changing. Caring holistically for a patient means you need to be sensitive to the religious and cultural issues which may affect them and ask for further information when you are unfamiliar with particular requirements. However, there can be wide variety of different beliefs and practices even within the same religious group. How strictly practices are observed can also vary, so it is important not to make assumptions but to make sure you understand the needs of each patient as a unique individual. In the immediate post-operative period the patient relies on nursing staff to provide care. In addition to general nursing care, the patient with a stoma has specific care needs at this stage. Monitor and record the condition of the stoma (colour/size/surrounding skin). It should be checked daily, or more frequently if there is cause for concern. Report any abnormality immediately. (see section Stoma Management recognising abnormalities pages 17 & 18). Monitor, measure and record the stoma output Empty the pouch frequently as a pouch which is allowed to become too full may leak. Leakage can contaminate a wound leading to infection. It is also very unpleasant and demoralising for the patient, causing them unnecessary anxiety which may make it more difficult for them to come to terms with having a stoma. You should report any leakage so that the cause can be assessed and remedied. Sometimes, certain types of stoma may pass large amounts of very watery output (more than 1 litre of fluid in a day), especially during the first week or so after surgery. In this case, a urostomy pouch and continuous drainage bag may be fitted as a temporary measure to contain the high output. As soon as the patient returns to the ward after their operation, make sure that a stock of the correct stoma equipment is available in the patient s locker. Check their supplies every day so that they do not run out of any item. 14 Typical contents of patient s individual stock holdall (these may vary according to individual patient needs and your unit s own procedures) o Pouches (clear, drainable pouches for first few days after surgery; then the type may change according to individual needs) o Pouch clips (if required) o Small bowl for water o Disposal bags o Wipes/swabs (non sterile) to clean and dry skin o Adhesive remover o Ostomy deodorant spray o Barrier wipes to protect skin o Additional accessories as specified in care plan o Template/measuring guide o Paper towel/pad to protect clothing 15
9 Post-operative care Ensure that the patient is fitted with suitable, leak proof appliance at all times. A clear drainable pouch should be used in the first few days postoperatively. This allows for frequent emptying of the pouch when the output is very fluid; the clear plastic enables the colour and condition of the stoma to be checked more easily. If the patient has a colostomy or ileostomy, you need to monitor that they start passing wind (flatus) from their stoma. Therefore, for the first few days post-operatively, the flatus filter on the pouch should be sealed with a special filter cover (these are provided by the manufacturer in each box of pouches). Alternatively, a pouch without a filter may be used. Once the stoma has begun to work, a routine for emptying and changing the pouch should be adopted. You should record every pouch change in the care plan, stating whether it was a routine procedure or due to an untoward event, such as leakage. Encourage the patient to assist with pouch emptying and changing as soon as their condition allows. Bridges and Stents Stoma Management recognising abnormalities It is important to be able to recognise the normal from the abnormal in order to monitor, record and report any problems. Stoma colour Normal pink/red/warm to touch. Abnormal black/dusky/pale/sloughy. Skin Normal Skin surrounding the stoma should be intact. Abnormal Any soreness/ulceration/inflammation or broken skin. Normal colour Normal skin Abnormal colour Abnormal skin Oedema (swelling) Normal In the post-operative period the stoma can be quite swollen. It may reduce in size for about 6 weeks after surgery. Abnormal Any sudden or unexplained swelling of the stoma. Bleeding Stoma Normal A slight smear of blood on the wipe when washing or drying the stoma. Abnormal Excessive bleeding when cleaning the stoma/blood in the pouch/bleeding from inside the stoma. Bridges The purpose of a bridge or rod is to support a loop colostomy or loop ileostomy following surgery. The rod or bridge is usually external and prevents the loop of bowel which forms the stoma from retracting into the abdomen. Bridges can be made of plastic, rubber or glass. Sometimes they are sutured at each end to the skin surface which may make fitting a pouch more difficult. A bridge usually remains in place for 5-8 days after which time it is gently removed by the stoma nurse, once medical permission has been obtained. Bridge Ureteric Stents When a urostomy is first formed the ureters are plumbed into the piece of bowel which forms the stoma. The join is temporarily protected by using fine bore plastic tubes or ureteric stents. The stents pass along the ureters and out through the urostomy, where the ends of the tubes should be visible at all times. They remain in place for 7-10 days then are gently removed by the stoma nurse, once medical permission has been obtained. Type of stoma Colostomy Ileostomy Urostomy Rectal discharge Normal output Passing flatus (wind) is the first sign that the bowel has started to work again after surgery. Soft/formed stool 1-3 times daily (may take a few days to work and can be fluid in the post-operative period). Fluid to soft faeces consistency may vary between porridge and watery. [Haemo-serous fluid (pink, clear fluid) and flatus (wind) is normal during the first 48 hours after surgery]. In a 24 hour period output should be approximately 500/800ml. Continuous flow of urine, should be clear, strawcoloured. Sometimes contains mucus. Mucus, and sometimes a small amount of faeces may be passed via the rectum when this has been left in place after bowel surgery. Abnormal output Constipation - hard stool/no output for over 2 days. Obstruction - no output associated with pain/vomiting/distended abdomen. Diarrhoea. Blood mixed with output. Should never be constipated. Excessive watery/bile stained output (common in the first few days after surgery). No output for longer than 12 hours. Blood mixed with output. Cloudy/offensive/dark/concentrated urine. Increased mucus production/blood in urine. No urine. Blood/pus
10 Stoma Management recognising abnormalities Products used in the management of stomas Complications The following events can cause problems with stoma management and/or leakage from the pouch. You should report if any of these problems occur. Prolapse Where an excessive length of bowel protrudes through the stomal opening. The types of pouches used include: One-piece, drainable or closed; Two-piece, drainable or closed. Drainable pouches are generally used when the output will need to be drained frequently, e.g. ileostomies. Special drainable pouches with a tap outlet are used for urostomies. Retraction Where the stoma shrinks back below the level of the skin. Closed pouches are generally used for the firmer, less frequent motions of colostomies. One-piece pouches, as the name suggests, are all in one piece, i.e. the whole thing is removed when the pouch is changed. One-piece drainable pouch Skin creases Creases in the skin radiating from the stoma. Sometimes only evident when sitting. Stenosis Where the opening of the bowel has become narrowed. Two-piece pouches available for all types of stoma have a separate baseplate flange to which a pouch is fitted. The baseplate flange is left in place on the abdomen, with a new pouch fitted when necessary. Every 2-4 days the baseplate flange will need to be changed too. One-piece closed pouch Parastomal hernia Abnormal swelling around the stoma due to a weakness of the muscle wall. 18 Muco-cutaneous separation Partial or total breakdown of the sutures joining the stoma to the skin edge. This can be caused by local infection or by a stoma that has been formed under tension. Sore skin One-piece urostomy pouch Two-piece drainable pouch 19
11 Products used in the management of stomas Products used in the management of stomas Product How to use Purpose Product How to use Purpose Adhesive remover Aerosol spray or wipes. Barrier wipes/ sprays/creams Sachet wipes, sprays or sticks. Protective paste Hydrocolloid powder Washers Discs, varying in size, made from the same hydrocolloid material as pouch flanges. Filler paste In a tube or strips. Apply to flange prior to removing pouch. Apply to the skin around the stoma before fitting the pouch. Some versions contain alcohol avoid use of these on sore or sensitive skin. Apply to broken skin, especially around edge of stoma. Apply to sore peristomal skin. Use sparingly, too much may prevent flange adhesion. Position around stoma/on sore skin. Alternatively place on the pouch prior to positioning over stoma. Apply to uneven skin prior to fitting the pouch. Softens flange adhesive, makes flange easier to remove, preventing trauma to skin. Protects the skin from the corrosive effects of stoma output. Healing of sore, broken skin. Healing of wet, excoriated (sore) skin. Assists in skin protection and management of flush and recessed stomas. Management of leaking pouch caused by uneven skin areas and crease. Convex pouches/ baseplates Belts Narrow elasticated material. Ostomy Deodorant Spray or Drops Perfumed sprays or drops. Thickening agents Sachets, capsules or strips of special absorbent granules. Filter covers Adhesive patches. Has a flange/baseplate with a noticeable raised area. This puts pressure on the skin around the stoma and encourages faeces/urine to flow into the pouch. Attach to belt hooks on flange/ baseplate. Spray into the air or drop into pouch. Insert into pouch before fitting and after emptying. Thickening agents should not be used immediately post-operatively for at least two weeks, as it gives a false observation of the stoma output. Apply over pouch filter to seal it. Management of flush and recessed stomas, prevention of leaks. Only to be used when instructed by SCN. Assists in the management of flush/recessed stomas Disperses odour after emptying and changing pouch. Absorbs moisture from output. Reduces likelihood of leakage. Reduces frequency of pouch emptying. Useful for excessive and watery output. Prevents filter becoming wet and ineffective during bathing or showering. Also used to prevent faeces pancaking. Flange extenders Semi circles or strips of hydrocolloid/ microporous adhesive. Apply around the edge of the flange. Extra adhesion to flange and increased security for patient. Stoma Measurement guides Cards displaying holes of various mm sizes. Apply over stoma to gauge correct aperture of flange. Ensures correct size of aperture, prevents sore skin/or damage to stoma from incorrect fit
12 Teaching the patient self care Teaching the patient self care The process of teaching the patient to care for their stoma starts as soon as possible. When the patient is having a planned (elective) operation, the Stoma Care Nurse will normally have begun the teaching process prior to the patient s admission to hospital. If the patient has undergone an emergency operation, they will have had little or no pre-operative preparation and so they are likely to take longer to adjust to having a stoma. Some patients resist taking part in their care in an effort to avoid confronting the reality of having a stoma. Until the patient has recovered sufficiently for them to learn self care, the procedure for stoma care will be as below, except that the HCA or nurse carries out the actions listed under Patient Action. Explaining each stage helps to familiarise the patient with the process. Preparation Explain the procedure to the patient. Apply standard infection control precautions for handling body fluids. Assess the patient s level of competence and confidence so that supervision and guidance can be given where needed. Encourage the patient to wash their hands before and after the procedure. Encourage the patient to think through each step for themselves. Report any situation which may prevent you carrying out the procedure. The importance of good hygiene The bowel is inhabited by a variety of organisms generally called coliforms; Escherichia coli, Enterococci, Klebsiella and Enterobacters are a few of the more common ones. These can become pathogens (which means capable of causing disease) when they enter other areas of the body such as the urinary tract and wounds. The Urinary Tract is supposed to be free from any organisms, however if hand hygiene or stoma hygiene is not good then either infection or colonisation can occur. The skin has many organisms that are natural to it such as Staphylococcus epidermidis and Staphylococcus aureus which are potential pathogens if they get in to the body via wounds, catheters, drain sites etc. In order to minimise the possibility of such organisms causing infection, it is important that you observe standard precautions for infection control when emptying or changing a stoma pouch. These will include hand washing/cleansing before and after the activity, using disposable gloves and aprons, appropriate handling of soiled pouches and equipment and disposing of waste safely. 22 Teaching the patient to empty their pouch Learning to empty their pouch is often the first step towards self care which the patient will undertake. This gives the patient some control over their stoma management. Empty pouch when half full (the possibility of leaks is reduced if a pouch is not allowed to overfill). Steps for emptying the pouch Wash hands. If output is being measured, drain into a suitable container. Or To empty directly into the toilet: patient sits on toilet as far back as possible, with legs apart, alternatively they can stand over or kneel by the toilet if they prefer. Toilet paper placed in the bowl will reduce splashing. Hold the bottom of the pouch upwards and release the fastening. Direct contents into the toilet (or container). Clean the opening of the pouch using tissue. Fasten closure securely. Wash hands. Patient Action HCA Action Rationale Encourage the patient to wash their hands. Hold container for patient if necessary. Help patient to find a suitable position. Observe patient technique. Observe patient technique. Observe patient technique. Check fastening secure. Encourage the patient to wash their hands. Good hygiene. Patient has both hands free to control pouch emptying. Patient is in comfortable position for emptying pouch. Prevent accidental spillage of contents. Prevent spillage. Prevent soiling of outside of pouch. Prevent accidental leakage. Good hygiene. 23
13 Teaching the patient self care Teaching the patient self care Changing a pouch (N.B. The HCA or nurse carries out the whole procedure until the patient is able to take part in self-care) Set out the following equipment in the area to be used, preferably in the bathroom: Bowl or basin of warm water Disposal bag Adhesive remover Wipes/swabs to clean and dry skin Barrier wipe to protect skin Prepared appliance (and clip if required) Template/measuring guide Ostomy deodorant spray Paper towel /cloth to protect clothing Additional accessories as specified in care plan (items may vary according to individual patient needs and your unit s own procedures) Steps for changing a pouch Patient Action HCA Action Rationale Prepare equipment. Use towel or pad to protect clothing. Empty drainable pouch. Remove pouch. Explain product usage. Encourage patient to empty pouch into the toilet whenever possible. Encourage the patient to gently remove pouch using an adhesive remover. (If changing a urostomy pouch, use swab over stoma). Familiarises the patient with the procedure. Prevents spillage when pouch is removed. Promotes normality (this is what they ll do at home). Prevents trauma to the skin. (Soaks up urine that comes constantly through the stoma). Steps for changing a pouch (contd) Patient Action HCA Action Rationale Check stoma size. Encourage patient to measure A well fitting pouch prevents stoma using either a prepared leakage and minimises the risk of template or a measuring guide. skin damage. Prepare new appliance. Apply skin barrier to skin around stoma. Leave for a few seconds to dry. Remove the protective cover from the adhesive flange. Apply pouch. Dispose of pouch safely. Wash hands. If the pouch flange needs adjusting, encourage patient to cut the hole to the required size (using a template if required). Observe patient technique. Check the appliance is well adhered with no creases around the flange. For drainable pouches, ensure the outlet is closed! Ensure patient is aware of how to dispose of soiled waste bag. When the patient is at home, the used (emptied) pouch and the used swabs are put in a disposal bag, sealed and put into the domestic refuse bin. If the patient is using a flushable pouch, manufacturer s instructions for disposal should be followed. Encourage the patient to wash their hands. As above. Skin barrier helps prevent skin damage and aids adherence of the new pouch. Prevents leakage and odour. Adhere to Trust guidelines for the disposal of soiled waste. Good hygiene. Remove excess soiling on the stoma and surrounding skin with dry swab. Wash stoma and surrounding area with water and dry thoroughly. Observe patient technique. Note any abnormalities with the stoma and surrounding skin. Promotes good standard of hygiene minimising the risk of sore skin. Aids adherence of new pouch. Record activity in care plan and report findings. Maintain continuity of care. You can view the Securicare pouch changing video on our website or visit our site on Youtube. SecuriCare also produce a DVD on pouch changing
14 Basic dietary advice for patients with stomas Basic dietary advice for patients with stomas The aim for all patients who have a new stoma is to return to a normal diet as soon as possible. After stoma surgery, a patient s appetite may be poor, but they may be encouraged to eat small meals at regular intervals until their appetite returns. New stoma patients may experience excessive wind and odour after eating certain foods, but things often settle down. Precise dietary advice is impossible to give as everybody reacts differently to various foods. Patients with stomas need to experiment with each food several times before excluding it from their diet. The most important advice is to relax and enjoy their food! Dietary advice for colostomates General advice: There are no dietary restrictions, but individuals vary and some foods may cause a problem, especially in the first few weeks after surgery. Eat regular meals. Drink a variety of fluids, e.g. water, squash, tea, coffee, milk. Aim for 8-10 large cups or mugs per day. To prevent constipation: Increase fibre intake by gradually increasing the amount of fruit and vegetables eaten to at least 5 portions a day. Add Bran to a meal (about 2 teaspoons). Increase fluid intake, especially water, squash, fruit juice. Gentle exercise helps the bowel to function. If the colostomy functions fewer than two or three times a week, the patient may be constipated. Medical advice should be sought. Dietary advice for ileostomates General advice: Because the output is quite fluid, ileostomates should have a good fluid and salt intake to prevent dehydration. Aim for 8-10 large cups or mugs per day (e.g. water, squash, tea, coffee, milk). Certain foods, e.g. spicy foods may cause diarrhoea. High fibre foods may cause a blockage. Foods to be cautious with include: celery, dried fruit, nuts, coconut, mushrooms, fruit skins, sweetcorn. Chew food well and peel fruit before eating. If an ileostomy has not functioned for twelve hours medical advice must be sought. Dietary advice for urostomates General advice: There are no dietary restrictions. Drink plenty of fluids to help prevent urinary infections. A urostomate can be prone to constipation for the first few weeks after surgery due to disturbance caused by a small piece of bowel being used to form the urostomy. Some foods and medicines may discolour the urine. Patient leaflets giving nutritional advice are available Nutritional advice For the well ostomist All SecuriCare information leaflets are available as downloadable PDF files on our website
15 Safe Discharge Bibliography Is the patient ready for discharge? The patient, or their carer, must be able to manage stoma care when at home. Having helped in teaching the patient self care, do you think he or she (or the carer) is ready to safely manage stoma care? Has the SCN assessed them? If you think by the date of discharge that the patient or their carer cannot manage stoma care, you should alert the appropriate member of the hospital team. When a patient is ready for discharge: Notify the Stoma Care Nurse of the planned discharge date. Provide the patient with contact details for the SCN. Advise the patient who to contact outside normal hours if problems arise following discharge (normally their GP or District Nurse). Has the patient been provided with 2 weeks supplies to take home, according to their type of stoma? (This will allow time for the patient s first prescription to be processed and delivered). Check that the patient can explain how they will safely dispose of used stoma pouches at home. Generally, the patient may dispose of used pouches with domestic refuse. Used pouches should be emptied and wrapped securely before disposal. Local regulations vary and may sometimes require that a special waste collection service is used. Check with the stoma care nurse that you know what regulations apply in the patient s area. Flushable pouches have a liner which can be flushed down the toilet. Black, P. & Stuchfield, B (2006). Multicultural stoma care. In: Caring for stoma patients, best practice guidelines. CliniMed Ltd., High Wycombe. Dean, J. et al (2004). Ostomy Glossary. Dansac Ltd., Cambridge. Fulham, J (2006). Nutritional concerns for patients with a stoma. In: Caring for stoma patients, best practice guidelines. CliniMed Ltd., High Wycombe. Gibson, P. & Hardy, L (2007). Cumbria Competence and Training: Assisting clients with stoma management. Cumbria Changing Workforce Project. Lyon, C. & Smith, A (2001). Abdominal stomas and their skin disorders - an atlas of diagnosis and management. Dunitz Ltd., London NHS Modernisation Agency (2003). Essence of care: communication. Department of Health, London. Perrin, A. et al (2004). Stoma Care District Nurse Resource Pack. 2nd edition. Salts Healthcare. Porrett, T. & McGrath, A. eds. (2005). Stoma Care. Blackwell Publishing, Oxford. SecuriCare (Medical) Ltd (2006). Stoma Care at a Glance. SecuriCare (Medical) Ltd., High Wycombe. Skills for Health (2004). Health competence CHS10, Undertake Stoma care. Skills for Health, Bristol. Skills for Health (2004). Health competence Gen 14, Provide advice and information to individuals on how to manage their own condition. Skills for Health, Bristol. Skills for Health (2004). Health competence HSC31, Promote effective communication for and about individuals. Skills for Health, Bristol. Stephenson, N (2008). Self-directed learning: communication. British Journal of Healthcare Assistants, 2(6), p
16 Useful contact details Notes SecuriCare (Medical) Ltd Compass House Knaves Beech Way Loudwater High Wycombe Buckinghamshire HP10 9QY Freephone: CliniMed Ltd Cavell House Knaves Beech Way Loudwater High Wycombe Buckinghamshire HP10 9QY Freephone: Colostomy Association Celia Waters General Manager 15 Station Road, Reading Berkshire RG1 1LG Freephone: ia the Ileostomy and Internal Pouch Support Group Anne Demick National Secretary Peverill House 1-5 Mill Road, Ballyclare Co. Antrim BT39 9DR Freephone: Urostomy Association Mrs Hazel Pixley National Secretary 18 Foxglove Avenue Uttoxeter, Staffordshire ST14 8UN Telephone: Acknowledgements Authors: Denise Carter RGN, Diploma in Professional Studies Stoma Care Nursing. Stoma Care Sister, County Durham and Darlington NHS Foundation Trust. Gillian Harker RGN, ENB 998, Stoma Care Nurse, North Cumbria University Hospitals NHS Trust. Siobhan Shallow RGN, DipN, Stoma/Colorectal Nurse Specialist, Leicester Royal Infirmary. Sylvia Waller RGN, DipN, ENB 216. Clinical Quality Manager, SecuriCare (Medical) Ltd. This booklet sets out the authors understanding of best practice according to knowledge and experience current at the time of publication. What is best practice in this field is constantly developing and evolving. Readers are advised to assess the advice contained in the booklet against the most current information available and in context. Neither SecuriCare (Medical) Ltd., nor the authors assume any liability for any injury and/or damage, save as caused by any negligence on their part
17 SecuriCare (Medical) Ltd, Compass House, Knaves Beech Way, Loudwater, High Wycombe, Bucks HP10 9QY Freephone Careline: SecuriCare (Medical) Ltd 959/0708
However, each person may be managed in a different way as bowel pattern is different in each person.
 Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
How do I evaluate my skin condition? What causes sore skin?
 skin care Taking good care of your peri-stomal skin is of utmost importance. Your skin is the base, on which all of your stoma products will be placed, so it is vital that it is kept in good condition.
skin care Taking good care of your peri-stomal skin is of utmost importance. Your skin is the base, on which all of your stoma products will be placed, so it is vital that it is kept in good condition.
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
NHS Northamptonshire Comprehensive Stoma Care Guidelines. Information for General Practitioners
 NHS Northamptonshire Comprehensive Stoma Care Guidelines Information for General Practitioners Appendix 1 Stoma Care Department, Northampton General Hospital Lorraine Batty, Angie Dillon, Melissa Downing
NHS Northamptonshire Comprehensive Stoma Care Guidelines Information for General Practitioners Appendix 1 Stoma Care Department, Northampton General Hospital Lorraine Batty, Angie Dillon, Melissa Downing
Stoma Care Clinical Nursing Standards
 Stoma Care Clinical Nursing Standards Introduction A standard is a level of quality against which performance can be measured. It can be described as essential - the absolute minimum to ensure safe and
Stoma Care Clinical Nursing Standards Introduction A standard is a level of quality against which performance can be measured. It can be described as essential - the absolute minimum to ensure safe and
Ileostomy. A practical guide to stoma care. Putting you first
 Ileostomy A practical guide to stoma care Putting you first Foreword Contents Having ileostomy surgery can be a life-changing experience. For some, it is relief from a debilitating illness and for others
Ileostomy A practical guide to stoma care Putting you first Foreword Contents Having ileostomy surgery can be a life-changing experience. For some, it is relief from a debilitating illness and for others
Having a supra pubic urinary catheter
 Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a supra pubic urinary catheter Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A guide to common stoma problems
 A guide to common stoma problems www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 A guide to common stoma problems
A guide to common stoma problems www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 A guide to common stoma problems
Looking after your urinary catheter at home. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Looking after your urinary catheter at home An information guide Looking after your urinary catheter at home This leaflet is provided for
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Looking after your urinary catheter at home An information guide Looking after your urinary catheter at home This leaflet is provided for
Looking after your urinary catheter at home
 Looking after your urinary catheter at home Information for patients and carers Useful contacts to keep: Name and title of community nurse Single point of access (SPA) for community nursing 24 hour service
Looking after your urinary catheter at home Information for patients and carers Useful contacts to keep: Name and title of community nurse Single point of access (SPA) for community nursing 24 hour service
A Guide to Help You Manage Your Catheter and Drainage Bags
 A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence
 Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
Having a urinary catheter information for men
 Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Managing your bladder with a suprapubic catheter at home
 Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
After care following insertion of a suprapubic catheter
 Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Understanding Laparoscopic Colorectal Surgery
 Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Patient Information:
 Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis)
 Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Ilioinguinal dissection (removal of lymph nodes in the groin and pelvis) This sheet answers common questions about ilio-inguinal dissection. If you would like further information, or have any particular
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Infection Prevention & Control Team. Your urinary catheter & how to care for it 0151 430 2452 / 0151 430 1384. Patient Information Leaflet
 Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Indwelling urinary catheter. Information for patients and carers. RDaSH. Doncaster Community Integrated Services
 Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
Living life to the full with an indwelling catheter
 Living life to the full with an indwelling catheter www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 Living with and
Living life to the full with an indwelling catheter www.fittleworth.com Opening hours: 8am 8pm Monday to Friday 9am 1pm on Saturday Freephone National 0800 378 846 Scotland 0800 783 7148 Living with and
Colonic Stenting Your Procedure Explained
 Colonic Stenting Your Procedure Explained Patient Information Introduction This leaflet tells you about the procedure known as colonic stenting. It explains what is involved and some of the common complications
Colonic Stenting Your Procedure Explained Patient Information Introduction This leaflet tells you about the procedure known as colonic stenting. It explains what is involved and some of the common complications
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
online version Understanding Indwelling Urinary Catheters and Drainage Systems Useful information When to call for help
 When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
PATIENT URINARY CATHETER PASSPORT
 n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
PROCEDURE FOR CATHETER AFTERCARE
 PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
RECOVERY AFTER STOMA REVERSAL
 RECOVERY AFTER STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction Surgery to reverse a stoma is basically to reconnect the bowel and is a successful surgical procedure
RECOVERY AFTER STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction Surgery to reverse a stoma is basically to reconnect the bowel and is a successful surgical procedure
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Information for Patients having a Colonic Stent Placement
 Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
Colorectal Surgery Koch pouch operation. Information for patients
 Colorectal Surgery Koch pouch operation Information for patients What is a Koch pouch operation? Your consultant has discussed with you an operation called a Koch pouch. The Koch pouch is also known as
Colorectal Surgery Koch pouch operation Information for patients What is a Koch pouch operation? Your consultant has discussed with you an operation called a Koch pouch. The Koch pouch is also known as
Having a Mitrofanoff continent urinary diversion
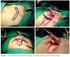 Having a Mitrofanoff continent urinary diversion Your surgeon has recommended that you need a continent urinary diversion. This leaflet aims to answer your questions about having a Mitrofanoff continent
Having a Mitrofanoff continent urinary diversion Your surgeon has recommended that you need a continent urinary diversion. This leaflet aims to answer your questions about having a Mitrofanoff continent
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE
 GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE Reference Date approved Nov 2012 Approving Body Matrons Forum Supporting Policy/ Working in New Ways (WINW) Package Implementation date Supersedes
GUIDELINE FOR CARE OF A PATIENT WITH A NEPHROSTOMY TUBE Reference Date approved Nov 2012 Approving Body Matrons Forum Supporting Policy/ Working in New Ways (WINW) Package Implementation date Supersedes
Management of urinary catheters
 Information for patients and relatives This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Corp/326.2 (2012)
Information for patients and relatives This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Corp/326.2 (2012)
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
HOW TO CARE FOR YOUR CATHETER (FEMALE)
 HOW TO CARE FOR YOUR CATHETER (FEMALE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What is a catheter? A catheter is a narrow flexible soft tube inserted into the bladder for the purpose
HOW TO CARE FOR YOUR CATHETER (FEMALE) Information Leaflet Your Health. Our Priority. Page 2 of 6 What is a catheter? A catheter is a narrow flexible soft tube inserted into the bladder for the purpose
Percutaneous Nephrostomy. Care of your Nephrostomy. Department of Urology
 Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
Information and advice following placement of seton for anal fistula
 Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Patient Information Leaflet Anal Fistula operation
 Patient Information Leaflet Anal Fistula operation SM07/04 Anal Fistula operation What is a fistula? An anal fistula is a track between the skin on the outside of the buttock/anal area and the anal canal
Patient Information Leaflet Anal Fistula operation SM07/04 Anal Fistula operation What is a fistula? An anal fistula is a track between the skin on the outside of the buttock/anal area and the anal canal
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Intermittent Self Catheterisation for Women
 ISCW Intermittent Self Catheterisation for Women National Service, Locally Based www.fittleworth.com Opening hours: 8am - 8pm Monday to Friday 9am - 1pm on Saturday Freephone National 0800 378 846 Scotland
ISCW Intermittent Self Catheterisation for Women National Service, Locally Based www.fittleworth.com Opening hours: 8am - 8pm Monday to Friday 9am - 1pm on Saturday Freephone National 0800 378 846 Scotland
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Going home with a urinary cathether
 Going home with a urinary cathether A patient s guide 1 Your doctor has advised that you require a urinary catheter so that urine can be drained from your bladder. This leaflet provides advice to help
Going home with a urinary cathether A patient s guide 1 Your doctor has advised that you require a urinary catheter so that urine can be drained from your bladder. This leaflet provides advice to help
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Excision or Open Biopsy of a Breast Lump Your Operation Explained
 Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Aids and Appliances for Urinary Incontinence
 Aids and Appliances for Urinary Incontinence Alison Stubbs, RGN, Clinical Specialist for WyMedical Ltd Tel. 01404 44088 e-mail: [email protected] Abstract Functional incontinence, where toileting
Aids and Appliances for Urinary Incontinence Alison Stubbs, RGN, Clinical Specialist for WyMedical Ltd Tel. 01404 44088 e-mail: [email protected] Abstract Functional incontinence, where toileting
Vesico-Vaginal Fistula
 Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Saint Mary s Hospital The Warrell Unit Vesico-Vaginal Fistula Information For Patients Contents Page What is a vesico-vaginal fistula? 3 How does a fistula develop? 3 What tests will I need? 3 How can
Transurethral Resection of Bladder Tumour (T.U.R.B.T)
 Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
Transurethral Resection of Bladder Tumour (T.U.R.B.T) Patient Information Introduction This booklet has been written to help you understand the surgery you are about to undergo. It will give you information
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION
 SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
URETEROSCOPY (AND TREATMENT OF KIDNEY STONES)
 URETEROSCOPY (AND TREATMENT OF KIDNEY STONES) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
URETEROSCOPY (AND TREATMENT OF KIDNEY STONES) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
The Children s Hospital Treatment for Hypospadias Information for parents
 The Children s Hospital Treatment for Hypospadias Information for parents What is hypospadias and what is the cause? Hypospadias is a congenital (since birth) abnormality of a boy s penis. Hypospadias
The Children s Hospital Treatment for Hypospadias Information for parents What is hypospadias and what is the cause? Hypospadias is a congenital (since birth) abnormality of a boy s penis. Hypospadias
Maintaining Proper Bowel Elimination
 Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the nursing assistant should be able to: 1. Describe the normal
Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the nursing assistant should be able to: 1. Describe the normal
Overactive bladder syndrome (OAB)
 Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: [email protected] www.ms-society.ie
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
WHAT IS INCONTINENCE?
 CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
High output stomas and their impact on Quality of Life. Carolyn Swash Community Stoma Care Nurse Hollister Limited
 High output stomas and their impact on Quality of Life Carolyn Swash Community Stoma Care Nurse Hollister Limited Aims of presentation What is quality of life Define High output stoma Look at reasons why
High output stomas and their impact on Quality of Life Carolyn Swash Community Stoma Care Nurse Hollister Limited Aims of presentation What is quality of life Define High output stoma Look at reasons why
Recovery plan: radical cystectomy Information for patients
 Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
Recovery plan: radical cystectomy Information for patients Help for you following a bereavement 5 This leaflet will help you know what to expect during your time with us. Please take some time to read
DIETARY ADVICE FOR CONSTIPATION
 Leicestershire Nutrition and Dietetic Services DIETARY ADVICE FOR CONSTIPATION What is constipation? Constipation is one of the most common digestive complaints. Normal bowel habits vary between people.
Leicestershire Nutrition and Dietetic Services DIETARY ADVICE FOR CONSTIPATION What is constipation? Constipation is one of the most common digestive complaints. Normal bowel habits vary between people.
After your gastric banding
 After your gastric banding Exceptional healthcare, personally delivered 2 Please call J Ward at Southmead Hospital on 0117 323 5132 if you have any questions or concerns soon after discharge. You may be
After your gastric banding Exceptional healthcare, personally delivered 2 Please call J Ward at Southmead Hospital on 0117 323 5132 if you have any questions or concerns soon after discharge. You may be
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
How To Care For A Stoma
 People who have a stoma often share many of the same questions and concerns. This best practice document provides answers to some of the common questions that people ask about the day to day care of the
People who have a stoma often share many of the same questions and concerns. This best practice document provides answers to some of the common questions that people ask about the day to day care of the
Learning Resource Guide. Understanding Incontinence. 2000 Prism Innovations, Inc. All Rights Reserved
 Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Learning Resource Guide Understanding Incontinence 2000 Prism Innovations, Inc. All Rights Reserved ElderCare Online s Learning Resource Guide Understanding Incontinence Table of Contents Introduction
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
Clinical Guideline for: Aseptic Technique
 Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
After Your Abdominal Surgery
 UW MEDICINE PATIENT EDUCATION After Your Abdominal Surgery Self-care and follow-up You recently had abdominal surgery. This handout explains what to expect during your recovery. Please read these instructions
UW MEDICINE PATIENT EDUCATION After Your Abdominal Surgery Self-care and follow-up You recently had abdominal surgery. This handout explains what to expect during your recovery. Please read these instructions
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed
 Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Epigastric Hernia Repair
 Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
ANTERIOR RESECTION YOUR OPERATION EXPLAINED
 ANTERIOR RESECTION YOUR OPERATION EXPLAINED Information Leaflet Your Health. Our Priority. Page 2 of 10 Introduction This leaflet explains the procedure known as an Anterior Resection. It includes what
ANTERIOR RESECTION YOUR OPERATION EXPLAINED Information Leaflet Your Health. Our Priority. Page 2 of 10 Introduction This leaflet explains the procedure known as an Anterior Resection. It includes what
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Individualized Care Plans Fully Developed
 Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Problems of the Digestive System
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
Spigelian Hernia Repair
 Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
