Methotrexate versus Azathioprine in Chronic Plaque Type Psoriasis: A Comparative Study
|
|
|
- Betty May
- 9 years ago
- Views:
Transcription
1 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: , p-issn: Volume 15, Issue 5 Ver. IX (May. 2016), PP Methotrexate versus Azathioprine in Chronic Plaque Type Psoriasis: A Comparative Study Atishay Bukharia 1, Nidhi Jain 2, Shyam Sundar Chaudhary 3 1 M.D.(Derm) Resident, Rajendra Institute Of Medical Sciences, Ranchi, Jharkhand, India 2 Psychiatry Senior Resident, Central Institute Of Psychiatry, Ranchi, Jharkhand, India 3 Prof & Head, Department Of Dermatology, Venereology And Leprosy, Rajendra Institute Of Medical Sciences, Ranchi, Jharkhand, India Abstract Introduction: Psoriasis is chronic disease where treatments are often needed throughout life. Since 1806, when Thomas girdlestone used potassium arsenate for Psoriasis to present era, we are still in search of drug which can cure this disease. Azathioprine is a relatively safe drug which has not been tested vigourously for chronic plaque type Psoriasis. Aims and objectives: To evaluate and compare the effect of Methotrexate and Azathioprine in chronic plaque type Psoriasis. Material and methods: this study was a randomized, double blind control hospital based study, conducted over 100 Psoriasis patients, divided into two groups of 50 each. Group A which Methotrexate in a dose of 15 mg weekly for 12 weeks. Group B Azathioprine in a dose of 2-3 mg/kg/day for 12 weeks. Severity of Psoriasis was assessed by PASI on 0,4,8 and 12 weeks and relapse was seen within 8 weeks of stopping the medication. Results: Statistically significant difference found after 8 and 12 weeks of treatment, with significantly higher PASI Clearnace by Methotrexate in comparison to Azathioprine. Conclusion: Although azthioprine is effective but Methotrexate is more effective than Azathioprine in chronic plaque type Psoriasis. I. Introduction Psoriasis is a common, chronic, disfiguring, inflammatory and proliferative condition of unknown etiology. The disease is enormously variable in duration, periodicity of flares and extent. It has a bimodal age of onset affecting both males and females equally. 1 Although rarely fatal but it has significant impact on quality of life because of its chronicity and relapsing tendency. Its prevalence is about 2%. 2 At some places prevalence of 4.8% has also been reported. 3 Various studies have shown a serious impairment in quality of life 47,48 and patients also feel that current available treatment do not provide long term relief 4,5,6. Psoriasis patients have a higher financial burden due to absenteeism in addition to the cost of treating their disease 7,8. We are still unable to comment over the prognosis of disease, how long the disease will last, whether a relapse will occur, or for what period of time the patient will remain free from Psoriasis 1 All forms of therapies have their own merits and demerits, often no single treatment is ideal. Treatment of Psoriasis remains a challenging and often frustrating experience for dermatologists where cure is not ensured. The management includes relevant investigations and treatment of the disease. The treatment depends upon age, sex, occupation, general health, intelligence of the patient, clinical type, extent and duration of the disease. Reassurance and emotional support are valuable. In general, therapy should be simpler, potentially less toxic and more effective. The therapeutic tools available to combat this disease are numerous, as are their untoward effects. 12 Local therapy include Tar, Dithranol, Topical corticosteroid, topical calcineurin inhibitors, intralesional corticosteroids, calcitriols, retinoid. 1 Systemic therapies for Psoriasis which are in common use include psoralen photochemotherapy, biologicals, retinoids, Methotrexate and cyclosporine. 13 Of these the equipment required for psoralen photochemotherapy is not easily available, also there is always a risk of basal cell carcinoma and squamous cell carcinoma. 14 This carcinogenic property is further compounded by its use with immunosuppressive like cyclosporine. 9 Hydroxycarbamide (hydroxyurea) carries significant side effect of bone marrow suppression and leucopenia in most treated patients. 10 Systemic retinoids can not be used in females of child bearing age, children below 12 years of age, in patients with existing hyperlipidemia. 15,1. Cyclosporine is effective but nephrotoxicity, hypertension, and malignancy potential raises a concern about its use. 11,32 Biologicals like infliximab and Adalimumab is FDA approved for chronic plaque type Psoriasis 16,17,18. but the cost, side effects like infusion reactions, anti-drug antibodies and inadequate experience DOI: / Page
2 in using these limits its use in developing countries like ours. 19 Methotrexate is quite effective but is toxic to liver and its side effect are difficult to monitor. 16 Azathioprine has a long history of being safely used by rheumatologist, gastroenterologist and dermatologist. Azathioprine not only have immunosuppressive effect but also possess anti inflammatory properties and in dermatology it is primarily used for immunobullous disorders like pemphigus. 14 Azathioprine is easy to monitor and carries less side effects in comparison to Methotrexate. 49,50 So, in view of availability of many modalities of treatment it is worthwhile to study and compare the effects of Methotrexate and Azathioprine in chronic plaque type Psoriasis, which would add to the future trends in the management of Psoriasis and would help the suffering patients. Aims and Objectives: To evaluate the effect of Methotrexate and Azathioprine and to know the comparative effect of Methotrexate against Azathioprine in chronic plaque type Psoriasis II. Materials And Methods The study was a randomised double blind control hospital based study conducted in Department of Dermatology, Venereology & Leprosy, Rajendra Institute of Medical Sciences (RIMS), Ranchi. The subjects were recruited for the study by simple random sampling technique. The treatment trial was of 20 weeks which include 12 weeks of hospitalization and 8 weeks of follow up between December 2013 to December with 18 to 60 years age of either sex and who were diagnosed as chronic plaque type Psoriasis were included and patients with History of any current or previous malignancy, pregnant or lactating women, history of diabetes mellitus, Epilepsy, HIV positive patients, known hypersensitivity to Methotrexate and Azathioprine, patients taking any systemic therapy with steroids, immunomodulators and cytotoxic drugs in previous 2 months, patients using topical treatment with formulations containing active agents as steroids, tar or dithranol in previous 2 weeks, TLC less than 3x10 9 /l, platelets count less than 50,000/mm3 and hemoglobin less than 9 gm/dl were excluded from the study. A special designed semi structured Performa, included various socio-demographic variables (age, sex, education, religion, marital status, socioeconomic status) and clinical variables (clinical diagnosis, age of onset, duration of illness, treatment details) was applied. Psoriasis Area and Severity Index (PASI) 46 is used to assess the skin area involved and the severity of the dermatological illness. Severity assessment is done along a 0-4 scale (0-no lesion, 4-severest possible lesion) for the three target symptoms of erythema, infiltration and desquamation. The total PASI score, ranging from 0.0 to 72. PASI is considered an objective measure and it is widely used in research purpose. Though Psoriasis Area and Severity Index (PASI) has limitations, it remains the gold standard. 20,39 Limitations of the PASI system includes expression of very different aspects of Psoriasis in one single figure and inter-observer variability. Complete blood count, liver functions tests, blood urea and creatinine levels, ECG and chest X-RAY were done before start of treatment. Screening for hepatitis B and C was also done. were randomized using block randomization method into either: Group A which Methotrexate in a dose of 15 mg weekly for 12 weeks. Group B Azathioprine in a dose of 2-3 mg/kg/day for 12 weeks. Severity of Psoriasis was assessed by measurement scores according to PASI scale. The PASI was scored on 0, 4, 8 and 12 weeks.clearance of PASI from the base line levels were taken as percentage of clearance and interpretation of the results was done as follows: excellent response = 80% clearance; good response = 70 to 79 % clearance; fair response = 50 to 69 % clearance; and poor response = 49 % clearance. Group A patients receiving Methotrexate had their complete blood counts weekly for first two weeks and thereafter fortnightly. Liver and Renal function tests were done weekly for the first 2 weeks and then fortnightly thereafter until the completion of the study. Group B patients receiving Azathioprine had their complete blood counts were done weekly for the first 2 weeks then fortnightly for another 10 weeks Liver function test was done fortnightly till the completion of study. Data was analyzed using Statistical Packages for Social Sciences (SPSS Version 22). Descriptive statistics was used to define the sample characteristics. For testing the variance among socio demographic and clinical variables, chi square test was applied for discrete variables and independent t-test was applied for continuous variables. III. Observation And Results The data gathered were consolidated, coded and subjected to appropriate statistical analysis. According to table 1 majority of patients belongs to 36 to 60 years of age i.e. 60 % and 64% in patients Methotrexate and Azathioprine respectively. Majority of patients were male in both the groups i.e. 70% and 74% respectively. 58% and 46% patients were educated above 12 th standard in patients Methotrexate and Azathioprine respectively. Majority of the patients were hindu, married and of lower socioeconomic status in both groups. The difference was not statistically significant between between both the groups in DOI: / Page
3 sociodemographic profile. Mean duration of illness was 10.84±6.70 and 13.04±5.75 in Methotrexate and Azathioprine groups respectively. This difference was not statistically significant (P= 0.08). Mean PASI score was 17.47±8.84 and 15.90±8.97 in Methotrexate and Azathioprine groups respectively. It also showed no statistically significant difference (p=0.38). (Table 2). After 4 weeks of Methotrexate treatment, 70% patients showed PASI clearance less than 49%, and 6% patient showed more than 70%. After 4 weeks of Azathioprine treatment, 88% patients showed PASI clearance less than 49%, and 2% patient showed more than 70% response. After 8 weeks of Methotrexate treatment, 26% patients showed PASI clearance less than 49%, and 32% patient showed more than 70% PASI clearance. After 8 weeks of Azathioprine treatment, 58% patients showed PASI clearance less than 49%, and 10% patient showed more than 70% PASI clearance. After 12 weeks of Methotrexate treatment, 14% patients showed PASI clearance less than 49%, and 54% patient showed more than 70% PASI clearance. After 12 weeks of Azathioprine treatment, 40% patients showed PASI clearance less than 49%, and 28% patient showed more than 70% PASI clearance.there was no statistically significant difference (p=0.09) found in PASI clearance after 4 weeks while this difference was significant after 8 weeks (p=0.01) and 12 weeks (p=0.02 ) of treatment. After 12 weeks of therapy with Methotrexate, 31 (62%) cases were relapsed within 8 weeks of stopping Methotrexate while 37 (74 %) cases were relapsed within 8 weeks of stopping Azathioprine but this difference was not statistically significant (p=0.20).(table 4) Side effects were present in 34% of the patient who had Methotrexate and 30% of the patients who had Azathioprine which include nausea, vomiting, diarrhea, abdominal pain, fatigue, headache, arthralgia, elevated liver enzymes, thrombocytopenia and leucopenia. Most common side effects were of gastrointestinal type in both the group and nausea vomitting constitute the majority.(table 5) IV. Discussion Azathioprine has been widely used for various autoimmune and inflammatory disorders. Azathioprine is very safe to use and with Thio Purine Methyl Transferase (TPMT) discovery and its available testing, we can avoid dreaded side effects like myelosuppression. 14 Routine examination like complete blood count and liver function test provide aids to monitor hepatotoxicity and myelosuppression during the course of study. Azathioprine acts by inhibiting purine metabolism and cell division through incorporation of its metabolite into the DNA and RNA. 15 But exactly it is not clear, how this mechanism leads to immunosuppression. Other reason for using Azathioprine is its easy availability and relatively cheap, considering the need of developing countries. There had been very few trial of Azathioprine use in Psoriasis. The socio-demographic parameters were assessed in the two study groups. There was no significant difference between patients Methotrexate and Azathioprine in terms of age, sex and education which was in accordance to our study plan. In our study majority of patients belongs to years of age (Table 1), which was in concordance with study of Haider et al 21 which showed majority of patients belong to age group of 40±12 years. Another study of Yui Yi 22, largest study in china which showed age of onset was 36 years. Dhir et al 23 also found the age range 35 to 67 years in their study. In Karn et al 24 study the mean age of Psoriasis patients was also ± In present study 72% of patients were male (Table 1), which is also similar to Haider et al. 21 findings where 61.6% were males. Dhir et al 23 also reported majority of patients were male (75%). Karibasappa and George 25 also found majority of patients were male in his study (60%). In Dayal et al 26 and Icen m et al 27 studies also showed overall incidence was higher in males than in females. Current findings of Mean duration of illness of 10.84±6.70 and 13.04±5.75 years in Methotrexate and Azathioprine groups respectively are supported by Dhir et al 23 in which mean duration of illness was 11.6 years (1-25 years) and Karisappa et al 25 study in which duration of illness was 2-23 years. It is also supported by Singh and Rai 28 study. Current findings of Mean PASI score of 17.47±8.84 and 15.90±8.97 in Methotrexate and Azathioprine group respectively, supported by Haider et al 21 study, where mean PASI was 14.8±4.2, it is also supported by Singh and rai 28 study where mean PASI was ± 10.64, ± and ± 9.80 for three different groups. Dayal et al 26 also found mean PASI ± 3.90 SD and 21.6 ± 4.42 SD in two different groups. Also In Karn et al 24 study mean PASI score at base line was ± 1.12 and ± 1.07 for 2 different groups. After 4 weeks of Methotrexate treatment, 70% patients showed PASI clearance less than 49%, and 6% patient showed more than 70%. In Karn et al 24 study, mean baseline PASI was ±1.12 and after 4 weeks it was 15.60±0.72 which showed less than 40 percent clearance while in another study by Masuria et al 29 complete clearance of Psoriasis was seen in 40% of patients in 4 weeks. In another study by Flystrom et al 35 baseline PASI of 14.1±7 changed to 9.3±6.1. Vijayshree and Kumar 44 who also gave similar results in which % patients showed PASI clearance less than 60. After 4 weeks of Azathioprine treatment, 88% patients showed PASI clearance less than 49%, and 2% patient showed more than 70% response. Comparing with the study done by Vijayshree and Kumar 44 who also gave similar results in which more than 80% improvement was seen in only 2.4% patients and they also found DOI: / Page
4 64.26% patients show reduction less than 60% of patients which was again consistent with our findings. Greeves and Dawber 30 showed improvement of only 25% in PASI clearance, in half of the patients after 6 weeks of Azathioprine treatment. After 8 weeks of Methotrexate treatment, 26% patients showed PASI clearance less than 49%, and 32% patient showed more than 70% PASI clearance, which was comparable to Haider et al 21 study in which 60 percent of patient showed PASI-75 after 8 week of treatment and twenty nine (40%) patients had an almost complete remission during the 8 weeks of treatment i.e. showed >90% PASI clearance. In another study by Opmeer BC et al 31, mean baseline PASI score before treatment was 14.8±4.2 and at the end of 8 weeks of treatment was 4.9±4.3. In Karn et al., 24 study, mean baseline PASI was ±1.12. and after 8 weeks it was 9.45 ± In 2015 study of Singh and Rai 28 PASI-75 achieved after 8 weeks. In Malik & ejaz 32 study, 73% patients had PASI clearance >80% and 45% had >60% clearance in 8 week. Vijayshree and Kumar 44 who also gave similar results in which 35.6% patients showed PASI clearance less than 60%. After 8 weeks of Azathioprine treatment, 58% patients showed PASI clearance less than 49%, and 10% patient showed more than 70% PASI clearance. Comparing with the study done by Vijayshree and Kumar 44 who also gave similar results in which 42.8 % patients showed PASI clearance less than 60% and 9.5% patient showed PASI clearance more than 80% after 8 weeks of Azathioprine treatment. After 12 weeks of Methotrexate treatment, 14% patients showed PASI clearance less than 49%, and 54% patient showed more than 70% PASI clearance. In Karn et al 24 study, the mean percent reduction of PASI score from base week to 12 weeks of treatment, was found to be 76.63± 1.79 for Methotrexate. In a similar study done by Opmeer BC et al. 31 base line PASI score was 13.4 ± 3.6 and at the end of 16 weeks it was 5.0± 4.5. Akhyani et al 34 also found that PASI -75 was achieved in 73.3% of patients on Methotrexate. Flystrom I et al 35 also found change from baseline at 12 weeks was 58% in the Methotrexate group. In the study by Sandhu et al 36, the mean PASI change at 12 weeks was 98% in the Methotrexate group. After 12 weeks of Azathioprine treatment, 40% patients showed PASI clearance less than 49%, and 28% patient showed more than 70% PASI clearance. Du Vivier et al 37 gave the Azathioprine upto a dose of 300 mg per day and 66% of the patients were responded. In the study of Hewitt et al 38 complete remission was reported in 20% of the subjects, almost complete remission in 30%, good response but incomplete remission in 45% and no response in 5%. Greaves and Dawber 3 used reduction in area of involvement as outcome assessment. In 50% of the subjects there was 0-25% reduction, in 20% there was 25-50% reduction, in 10% there was 50-75% reduction and in 20% there was % reduction. Reduction of Psoriasis efflorescences was the outcome assessment by Weitgasser et al 40. Forty subjects (60%) had complete remission, 20 (30%) had partial reduction and 6 (10%) had no significant reduction. In the series of Le Quintrec et al. 41 complete remission was found in 80% of the subjects, incomplete remission in 10% and in 10% of the subjects there was a relapse of the Psoriasis. Complete remission was attained in 91% of the subjects in the study of Baum et al 42 and 9% had marked improvement. After 12 weeks of therapy with Methotrexate 31 (62%) cases were relapsed within 8 weeks of stopping Methotrexate while 19 (38%) were not relapsed. After 12 weeks of therapy with Azathioprine, 37 (74%) cases were relapsed within 8 weeks of stopping Azathioprine while 13 (26%) cases were not relapsed. There was no statistically significant difference (p=0.20) found in relapse within 8 weeks of stopping Methotrexate and Azathioprine. Our findings are supported by Singh and Rai 28 who observed relapse in 36.5 % of cases after 12 weeks of stopping Methotrexate. In another study by Karibasappa et al 25 Methotrexate in the dose of 15mg/week was given to 20 patients with chronic plaque Psoriasis, till remission (4-12 weeks), followed by a maintenance dose (5mg/week) for 8 weeks. All patients were found to have relapsed within 6-12 weeks of stopping Methotrexate. Kravetz and Balsam 53 for first time used Azathioprine in Psoriasis; they used 2 mg/kg daily in 12 patients, 1-4 courses with improvement. In majority of the patients, it relapsed within months after the last dose. Greaves and Dawber 30 used 2.5 mg/kg/day for 6 weeks in 10 patients with 25% clearance of the lesions in 5 patients within 2-6 weeks duration. Relapse was seen 1 month after stoppage of Azathioprine. Feldges and Barnes 54 used 2.5 mg/kg/day in 10 patients for 4 ½ months to 5 ½ years with almost complete clearance of skin lesions in 6 patients. Azathioprine was discontinued after remission lasting for 1 year. However, the lesions relapsed after stoppage of treatment. In 1974, Du Vivier et al. 37 used mg Azathioprine daily for 2-24 weeks with % clearance of Psoriasis lesions with maintenance dose of mg daily in 13 out of 29 patients. One patient who was free of the lesions developed relapse 6 months after complete stoppage of Azathioprine. Side effects were present in 34% of the patients who had Methotrexate and 30% of the patients who had Azathioprine, which include nausea, vomiting, diarrhea, abdominal pain, fatigue, headache, arthralgia, elevated liver enzymes, thrombocytopenia and leucopenia. Most common side effects were of gastrointestinal type in both the groups and nausea,vomiting constitute the majority. Fatigue and elevated liver enzymes were more common in Methotrexate group. Transient thorombocytopenia and leucopenia were seen in DOI: / Page
5 2% of the patients receiving Methotrexate but revert back to normal after receiving folinic acid supplement which the patient missed during the therapy. Serious side effects like Pulmonary fibrosis and Secondary leukemia was not seen and is probably due to their low dose usage in dermatology in contrast with other branches where they are primarily given in higher doses for various transplantation and cancers. Our findings has been supported by Karn et al 24 who also reported that gastrointestinal side effects were the most common to occur with Methotrexate. In his study he found about 30.43% of the patients of Methotrexate group were suffered from elevated liver enzymes, while in our study it is limited to only 10%. This difference can be attributed to patients selection criteria in our study. Trivedi et al 51 and Sturdevant et al 52 reported most common adverse effects of Azathioprine were gastrointestinal including nausea, vomiting, and diarrhea. There was no significant difference in PASI clearance after 4 weeks of Methotrexate and Azathioprine treatment but statistically significantly difference found after 8 weeks (p=0.01) and 12 weeks (p=0.02) of treatment, i.e. patients Methotrexate shown significantly higher PASI clearance (better response) in comparison to patients azathioprone. There was no statistically significant difference (p=0.20) found in relapse within 8 weeks of stopping Methotrexate and Azathioprine. Similar findings were also seen in studies by Malik and ejaz 32 who found at the end of week 8, the Methotrexate-treated group had a significantly greater percentage reduction in the PASI compared with that of the Azathioprine treated Group. In another study by Mezzadara et al. 43 who gave Azathioprine in very high doses to their patients i.e. 6 gram over a period of 18 days and then followed their patients for further ten weeks. They found Azathioprine to be comparable to Methotrexate in Psoriasis. Du vivier et al 37 concluded that patients showed poorer tolerance and clinical response to Azathioprine than to Methotrexate, and the drug will therefore represent an advance in therapy only if the long-term complications are significantly less. Vijayshree and Kumar 44 also observed that at the end of 8 week it was Methotrexate group that have shown better response in the form of reduction in PASI score in comparison to Azathioprine. Strength of our study is that we have taken a drug naive population, it was a prospective study which included 3 months of hospitalization at a tertiary health care centre. Weakness of our study is that we could not remove the confounding facors like stress, effect of cold and infection. Sample size was also modest and futher clinical trial are needed over large sample size in order to find out the best drug which could maintain the long term remission and carries least side effect in management of this incurable disease. References [1]. Griffiths CEM, Camp RDR, Barker JNWN. Psoriasis. In: Burns D, Breathnach S, Cox N, Griffiths C, editors. Rook s textbook of dermatology. Oxford: Blackwell Science; pp [2]. Christopher E.Psoriasis Epidemiology and clinical spectrum. Clin Exp Dermatol 2001; 26: [3]. Kavli G, Færde OH, Arnesen E et al. Psoriasis: familial predisposition and environmental factors. BMJ 1985; 291: [4]. Krueger G, Koo J, Lebwohl M, Menter A, Stern RS, Rolstad T. The impact of Psoriasis on quality of life: results of a 1998 National Psoriasis Foundation patient-membership survey. Arch Dermatol.2001;137: [5]. Pearce DJ, Singh S, Balkrishnan R, Kulkarni A, Fleischer AB, Feldman SR. The negative impact of Psoriasis on the workplace. J Dermatolog Treat. 2006;17: de Arruda LH, De Moraes AP. The impact of Psoriasis on quality of life. Br J Dermatol. 2001;144: [6]. Feldman SR, Fleischer AB, Jr, Reboussin DM, Rapp SR, Bradham DD, Exum ML, Clark AR. The economic impact of Psoriasis increases with Psoriasis severity. J Am Acad Dermatol. 1997;37: doi: /S (97) [7]. Finlay AY, Coles EC. The effect of severe Psoriasis on the quality of life of 369 patients. Br J Dermatol. 1995;132: [8]. Paul CF, Ho VC, McGeown C et al. Risk of malignancies in Psoriasis patients treated with cysclosporine: a 5 year cohort study. J Invest Dermatol 2003; 120: [9]. Hunter GA, Simmons IJ, Thomas BM. A clinical trial of hydroxyurea for Psoriasis. Australas J Dermatol 1972; 13: [10]. Bos JD, Meinardi MMHM, van Joost T et al. Use of cyclosporin in Psoriasis. Lancet 1989; ii: [11]. Spuls PI, Witkamp L, Bossuyt PM, Bos JD.A systematic review of five systemic treatments for severe Psoriasis. Br J Dermatol 1997; 137: [12]. Boztepe G, Karaduman A, Sahin S et al. The effect of maintenance narrow-band ultraviolet B therapy on the duration of remission for Psoriasis: a prospectiverandomized clinical trial. Int J Dermatol 2006; 45: [13]. Badalamenti,S.S.,Kerdel,F.A. Azathioprine. in: S.E.Wolverton(Ed.) ComprehensiveDermatologicTherapy. Saunders, Edinburgh, Scotland; 2013: [14]. Loo TL, Luce JK, Sullivan MP, et al. Clinical pharmacologic observations of 6-mercaptopurine and 6-methythipurine ribonucleoside. Clin Pharmacol Ther 1968;14: [15]. O Quinn RP, Miller JL. The effectiveness of tumor necrosis factor alpha antibody (infliximab) in treating recalcitrant Psoriasis: A report of 2 cases. Arch Dermatol 2002;138(5): [16]. Oh CJ, Das KM, Gottlieb AB. Treatment with anti-tumor necrosis factor alpha (TNF-alpha) monoclonal antibody dramatically decreases the clinical activity of Psoriasis lesions. J Am Acad Dermatol 2000;42(5): [17]. Gordon KB, Langley RG, Leonardi C, et al. Clinical response to adalimumab treatment in patients with moderate to severe Psoriasis: Double-blind, randomized controlled trial and open-label extension study. J Am Acad Dermatol 2006;55(4): [18]. Mehlis S, Gordon KB. Tumor necrosis factor (TNF) inhibitors. in: S.E. Wolverton (Ed.) Comprehensive Dermatologic Therapy. Saunders, Edinburgh, Scotland; 2013: [19]. Puzenat E, Bronsard V, Prey S, Gourraud PA, Aractingi S, Bagot M, Cribier B, DOI: / Page
6 [20]. Joly P, Jullien D, Le Maitre M, Paul C, Richard-Lallemand MA, Ortonne JP, Aubin F. What are the best outcome measures for assessing plaque Psoriasis severity? A systematic review of the literature. J Eur Acad Dermatol Venereol Apr;24 Suppl 2:10-6. [21]. Haider S, Wahid Z, Najam-us-Saher, Riaz F. Efficacy of Methotrexate in patients with plaque type Psoriasis. Pak J Med Sci 2014;30(5): [22]. Yui Yip S. The prevalence of Psoriasis in the mongoloid race. J Am Acad Dermatol 1984; 10: [23]. Dhir R, Tutakne MA, Chari KVR. Relapse in Psoriasis after Methotrexate Indian J Dermatol Venereol Leprol 1992;58: Karn D, Amatya A, Khatri R. Comparative study of Methotrexate and Cyclosporine in the treatment of Psoriasis. Nepal journal of dermatology venereology and leprosy 2010; vol 9,1: [24]. Karibasappa NA, George A. Relapse in Psoriasis after Methotrexate. Indian J Dermatol Venereol Leprol 1997;63: [25]. Dayal S, Mayanka, Jain V K. Comparative evaluation of NBUVB phototherapy and PUVA photochemotherapy in chronic plaque Psoriasis. Indian J Dermatol Venereol Leprol 2010;76: [26]. Icen M, Crowson CS, McEvoy MT, Dann FJ, Gabriel SE, Maradit Kremers H. Trends in incidence of adult-onset Psoriasis over three decades: a population- based study. J Am Acad Dermatol Mar;60(3): [27]. Singh SK, Rai T. Relapse in Psoriasis with two different tapering regimens of Methotrexate: A randomized open-label controlled study. Indian J Dermatol Venereol Leprol 2015;81: [28]. Masuria B L, Bansal N K, Sharma M, Singhi M K, Mittal. A clinico histopathological outcome of 4 weeks Methotrexate pluse therapy in Psoriasis. Indian J Dermatol Venereol Leprol 1999;65: [29]. Greaves MW, Dawber W. Azathioprine in Psoriasis. Br Med J 1970; 2 (5703): [30]. Opmeer BC, Heydendael VM, De Borgie CA, Spuls PI, Bossuyt PM, Bos JD, et al. Costs of treatment in patients with moderate to severe plaque Psoriasis: economic analysis in a randomized controlled comparison of Methotrexate and cyclosporine. Arch Dermatol. 2004;140(6): [31]. Malik T, Ejaz A. Comparison of Methotrexate and Azathioprine in the treatment of Psoriasis: A randomized controlled trial. J Pakistan Association of Dermatologists 2010; 20: [32]. Heydendael VM, Spuls PI, Opmeer BC, de Borgie CA, Reitsma JB, Goldschmidt WF, Bossuyt PM, Bos JD, de Rie MA. Methotrexate versus cyclosporine in moderate-to-severe chronic plaque Psoriasis. N Engl J Med Aug 14;349(7): [33]. Akhyani M, Chams-Davatchi C, Hemami MR, Fateh S. Efficacy and safety of mycophenolate mofetil vs. Methotrexate for the treatment of chronic plaque Psoriasis. J Eur Acad Dermatol Venereol Dec;24(12): [34]. Flyström I, Stenberg B, Svensson A, Bergbrant IM. Methotrexate vs.ciclosporin in Psoriasis: effectiveness, quality of life and safety. A randomized controlled trial. Br J Dermatol. 2008; 158(1): [35]. Sandhu K, Kaur I, Kumar B, et al. Efficacy and safety of cyclosporine versus Methotrexate in severe Psoriasis: a study form north India. J Dermatol. 2003;30: [36]. Du Vivier A, Munro DD, Verbov J. Treatment of Psoriasis with Azathioprine. Br Med J 1974; 1(5897): [37]. Hewitt J, Escande JP, Leibowitch M et al. [Trial therapy of Psoriasis with Azathioprine]. [French]. Bull Soc Fr Dermatol Syphiligr 1970; 77: [38]. Feldman SR, Fleischer AB Jr, Reboussin DM, Rapp SR, Exum ML, Clark AR, NurreL. The self-administered Psoriasis area and severity index is valid and reliable. J Invest Dermatol Jan;106(1): [39]. Weitgasser H, Weitgasser H. [Experiences with an ambulatory immunosuppressive therapy of generalized Psoriasis]. [German]. Hautarzt 1972; 23: [40]. Le Quintrec JL, Menkes CJ, Amor B. Severe psoriatic rheumatism. Treatment with Azathioprine. report of 11 cases. Rev Rhum Mal Osteoartic 1990; 57: [41]. Baum J, Hurd E, Lewis D et al. Treatment of psoriatic artthritis with 6-mercaptopurine. Arthritis Rheum 1973; 16: [42]. Mezzadra G. Therapeutic experience with Azathioprine in Psoriasis. G Ital Dermatol Minerva Dermatol 1972; 47: [43]. Vijayashree J, Kumar JS. Study of Effect of Methotrexate on Psoriasis in Comparison with Azathioprine. Journal of Evidence based Medicine and Healthcare; Volume 2, Issue 41, October 12, 2015: [44]. Fredriksson T, Pettersson U. Severe Psoriasis oral therapy with a new retinoid. Dermatologica 1978; 157: [45]. Mattoo SK, Handa S, Kaur I, Gupta N, Malhotra R. Psychiatric morbidity in Psoriasis: Prevalence and correlates in India. Ger J Psychiatry. 2005;8: [46]. Kumar V, Mattoo SK, Handa S. Psychiatric morbidity in pemphigus and Psoriasis: A comparative study from India. Asian J Psychiatr. 2013;6: [47]. Patel AA, Swerlick RA, McCall CO. Azathioprine in dermatology: The past, the present, and the future. J Am Acad Dermatol 2006; 55: [48]. Wolverton SE. Optimizing clinical use of Azathioprine with newer pharmacogenetic data. Arch Dermatol 2009; 145: [49]. Trivedi CD, Pitchumoni CS. Drug-induced pancreatitis: an update. J Clin Gastroenterol 2005;39: [50]. Sturdevant RAL, Singleton JW, Deren JJ, et al. Azathioprine-related pancreatitis in patients with Crohn s disease. Gastroenterology 1979;77: [51]. Kravetz RE, Balsam T. Treatment of Psoriasis with mercaptopurine. Arch Dermatol. 1961;84: [52]. Feldges DH, Barnes CG. Treatment of psoriatic arthropathy with either Azathioprine or Methotrexate.Rheumatol Rehabil. 1974;13: Table 1: Comparing sociodemographic profile among patients Methotrexate and Azathioprine. DOI: / Page
7 Fischer s exact test was applied, where cell count was less than 5. Variables Methotrexate / Mean(±SD) Received Azathioprine / Mean(±SD) t/χ2 /fisher s exact test df P Age 18-35yrs 20(40%) 18(36%) yrs 30(60%) 32(64%) Sex Male 35(70%) 37 (74%) Female 15 (30%) 13 (26%) Education <12 th 21(42%) 27(54%) th 29 (58%) 23 (46%) Religion Hindu 31 (62%) 34 (68%) Others 19 (38%) 16 (32%) Marital status Married 37 (74%) 38 (76%) Single 13 (26%) 12 (24%) Socioeconomic status Upper 4 (8%) 4 (8%) Middle 10 (20%) 8 (16%) Lower 36(72%) 38 (76%) Table 2: Comparing duration of illness and baseline PASI among patients Methotrexate and Azathioprine. Variables Duration of illness Mean(±SD) Baseline PASI Methotrexate 10.84± ±8.84 Azathioprine 13.04± ±8.97 P Value df *indicates p <.05 **indicates p<.01 Table 3: Comparing PASI clearance at week 4, 8 and 12 among patients Methotrexate and Azathioprine. PASI clearance After 4 weeks After 8 weeks After 12 weeks Methotrexate Azathioprine Methotrexate Azathioprine Methotrexate *indicates p <.05 **indicates p<.01 Fischer s exact test was applied, where cell count was less than 5. Table 4: Comparing relapse 8 weeks after stopping drugs. *indicates p <.05 **indicates p<.01 Azathioprine 80% (12%) 1(2%) 13(26%) 6(12%) 70-79% 3(6%) 1(2%) 10(20%) 4(8%) 14(28%) 8(16%) 50-69% 12(24%) 5(10%) 21(42%) 16(32%) 16(32%) 16(32%) 49% 35(70%) 44(88%) 13(26%) 29(58%) 7(14%) 20(40%) χ Df P.09.01*.02* Methotrexate Azathioprine Relapsed 31 (62%) 37 (74%) Not relapsed 19 (38%) 13 (26%) χ2 df P value DOI: / Page
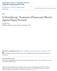
8 Side effects Table 5: Showing side effects of Methotrexate and Azathioprine. Methotrexate present 17 (34%) 15 (30%) Absent 33 (66%) 35 (70%) Nausea and Vomitting 14 (28%) 10 (20%) Diarrhea 3 (6%) - Abdominal pain 1 (2%) 2 (4%) Fatique 12 (24%) 4 (8%) Headache 5 (10%) 1 (2%) Arthralgia 3 (6%) 2 (4%) Elevated liver enzymes 5 (10%) 1 (2%) Thrombocytopenia 1 (2%) - Leucopenia 1 (2%) 3 (6%) A Methotrexate DOI: / Page
Azathioprine pulse therapy in the treatment of psoriasis
 Original Article Azathioprine pulse therapy in the treatment of psoriasis Ramji Gupta Department of Dermatology, Indraprastha Apollo Hospital Sarita Vihar, New Delhi, 110076 India Abstract Objective To
Original Article Azathioprine pulse therapy in the treatment of psoriasis Ramji Gupta Department of Dermatology, Indraprastha Apollo Hospital Sarita Vihar, New Delhi, 110076 India Abstract Objective To
Is Monotherapy Treatment of Etanercept Effective Against Plaque Psoriasis?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 Is Monotherapy Treatment of Etanercept
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 Is Monotherapy Treatment of Etanercept
Preetha selva et al. / International Journal of Phytopharmacology. 6(1), 2015, 42-46. International Journal of Phytopharmacology
 International Journal of Phytopharmacology Journal homepage: www.onlineijp.com 42 e- ISSN 0975 9328 Print ISSN 2229 7472 IJP A CLINICAL STUDY TO EVALUATE THE EFFECT OF TOPICAL TAZAROTENE IN THE TREATMENT
International Journal of Phytopharmacology Journal homepage: www.onlineijp.com 42 e- ISSN 0975 9328 Print ISSN 2229 7472 IJP A CLINICAL STUDY TO EVALUATE THE EFFECT OF TOPICAL TAZAROTENE IN THE TREATMENT
The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis
 1 The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis ผ ว จ ย Rutsanee Akaraphanth MD, Yotsinee Kittipavara MD, Nataya Voravutinon MD, Usa Wachiratarapadorn
1 The efficacy of a far erythemogenic dose of narrow- band UVB phototherapy in chronic plaque type psoriasis ผ ว จ ย Rutsanee Akaraphanth MD, Yotsinee Kittipavara MD, Nataya Voravutinon MD, Usa Wachiratarapadorn
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Original Policy Date
 MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
MP 5.01.20 Tysabri (natalizumab) Medical Policy Section Prescription Drug Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local Policy/12:2013 Return to Medical Policy Index Disclaimer
CLINICAL BRIEFS. Considerations for the Clinical Assessment of the Patient With Plaque Psoriasis. By Amy Krajacic
 CLINICAL BRIEFS Considerations for the Clinical Assessment of the Patient With Plaque Psoriasis By Amy Krajacic Senior Medical Editor, Custom Publications MediMedia USA, Yardley, Pa. A review of recently
CLINICAL BRIEFS Considerations for the Clinical Assessment of the Patient With Plaque Psoriasis By Amy Krajacic Senior Medical Editor, Custom Publications MediMedia USA, Yardley, Pa. A review of recently
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Psoriasis Treatment Transition Pathway
 Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
EVIDENCE BASED TREATMENT OF CROHN S DISEASE. Dr E Ndabaneze
 EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
EVIDENCE BASED TREATMENT OF CROHN S DISEASE Dr E Ndabaneze PLAN 1. Case presentation 2. Topic on Evidence based Treatment of Crohn s disease - Introduction pathology aetiology - Treatment - concept of
MEDICAL ASSISTANCE HANDBOOK PRIOR AUTHORIZATION OF PHARMACEUTICAL SERVICES `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists
 MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
MEDICAL ASSISTANCE HBOOK `I. Requirements for Prior Authorization of Cytokine and CAM Antagonists A. Prescriptions That Require Prior Authorization All prescriptions for Cytokine and CAM Antagonists must
to Part of Dossier: Name of Active Ingredient: Title of Study: Quality of life study with adalimumab in rheumatoid arthritis. ESCALAR.
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Individual Study Table Referring to Part of Dossier: Adalimumab (HUMIRA) (For National Authority Use Only) Name of Active Ingredient: Adalimumab Title
2.0 Synopsis Abbott Laboratories Name of Study Drug: Individual Study Table Referring to Part of Dossier: Adalimumab (HUMIRA) (For National Authority Use Only) Name of Active Ingredient: Adalimumab Title
Sponsor Novartis. Generic Drug Name Secukinumab. Therapeutic Area of Trial Psoriasis. Approved Indication investigational
 Clinical Trial Results Database Page 2 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Psoriasis Approved Indication investigational Clinical Trial Results Database Page 3 Study
Clinical Trial Results Database Page 2 Sponsor Novartis Generic Drug Name Secukinumab Therapeutic Area of Trial Psoriasis Approved Indication investigational Clinical Trial Results Database Page 3 Study
Rheumatoid Arthritis monitoring of DMARDs
 www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
www.bpac.org.nz keyword: DMARDS Rheumatoid Arthritis monitoring of DMARDs Key reviewers: Professor John Highton, Head of Section, Department of Medical and Surgical Sciences, Dunedin School of Medicine,
Psoriasis. Psoriasis. Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine
 Psoriasis Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine Psoriasis Psoriasis is a chronic skin disorder resulting from a polygenic predisposition combined with
Psoriasis Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine Psoriasis Psoriasis is a chronic skin disorder resulting from a polygenic predisposition combined with
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac
 PUBLIC SUMMARY DOCUMENT Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac Sponsor: Genepharm Australasia Ltd Date of PBAC Consideration: July 2007 1. Purpose
PUBLIC SUMMARY DOCUMENT Product: Tazarotene, cream, 500 micrograms per g (0.05%) and 1.0 mg per g (0.1%), 30 g, Zorac Sponsor: Genepharm Australasia Ltd Date of PBAC Consideration: July 2007 1. Purpose
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists
 Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Current Rheumatoid Arthritis Treatment Options: Update for Managed Care and Specialty Pharmacists 1. Which of the following matches of biologic targets that contribute to rheumatoid arthritis (RA) and
Drug Therapy Guidelines: Humira (adalimumab)
 Drug Therapy Guidelines: Humira (adalimumab) Effective Date: 5/1/08 Committee Review Date: 1/6/01, 9/18/01, 1/15/02, 1/7/03, 1/20/04, 1/18/05, 12/7/05, 10/15/06, 7/2/07, 11/5/07, 3/25/08 Policy Statements:
Drug Therapy Guidelines: Humira (adalimumab) Effective Date: 5/1/08 Committee Review Date: 1/6/01, 9/18/01, 1/15/02, 1/7/03, 1/20/04, 1/18/05, 12/7/05, 10/15/06, 7/2/07, 11/5/07, 3/25/08 Policy Statements:
GP Symposium Dermatology Dr Seow Hoong Foo Dr Shireen Velangi March 6th 2014
 Psoriasis : It s not just skin de eep NICE Guidelines and Quality Standards: a collaboration to deliver quality care GP Symposium Dermatology y p gy Dr Seow Hoong Foo Dr Shireen Velangi March 6th 2014
Psoriasis : It s not just skin de eep NICE Guidelines and Quality Standards: a collaboration to deliver quality care GP Symposium Dermatology y p gy Dr Seow Hoong Foo Dr Shireen Velangi March 6th 2014
Psoriasis Co-morbidities: Changing Clinical Practice. Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology. Psoriatic Arthritis
 Psoriasis Co-morbidities: Changing Clinical Practice Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology Psoriatic Arthritis Psoriatic Arthritis! 11-31% of patients with psoriasis have psoriatic
Psoriasis Co-morbidities: Changing Clinical Practice Theresa Schroeder Devere, MD Assistant Professor, OHSU Dermatology Psoriatic Arthritis Psoriatic Arthritis! 11-31% of patients with psoriasis have psoriatic
Available online www.jocpr.com. Research Article
 Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research, 2014, 6(2):736-741 Research Article ISSN : 0975-7384 CODEN(USA) : JCPRC5 A comparative study of efficacy and safety of combination
Available online www.jocpr.com Journal of Chemical and Pharmaceutical Research, 2014, 6(2):736-741 Research Article ISSN : 0975-7384 CODEN(USA) : JCPRC5 A comparative study of efficacy and safety of combination
Disclosures. Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
 Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
Psoriasis, Incidence, Quality of Life, Psoriatic Arthritis, Prevalence
 1.0 Abstract Title Prevalence and Incidence of Articular Symptoms and Signs Related to Psoriatic Arthritis in Patients with Psoriasis Severe or Moderate with Adalimumab Treatment (TOGETHER). Keywords Psoriasis,
1.0 Abstract Title Prevalence and Incidence of Articular Symptoms and Signs Related to Psoriatic Arthritis in Patients with Psoriasis Severe or Moderate with Adalimumab Treatment (TOGETHER). Keywords Psoriasis,
TNF-α Antagonists in the Treatment of Nail Psoriasis
 Review DOI: 10.6003/jtad.1264r1 TNF-α Antagonists in the Treatment of Nail Psoriasis Zekayi Kutlubay, MD, Burhan Engin, MD, Abdullah Songür, MD, Yalçın Tüzün, MD Address: Istanbul University, Cerrahpaşa
Review DOI: 10.6003/jtad.1264r1 TNF-α Antagonists in the Treatment of Nail Psoriasis Zekayi Kutlubay, MD, Burhan Engin, MD, Abdullah Songür, MD, Yalçın Tüzün, MD Address: Istanbul University, Cerrahpaşa
New Evidence reports on presentations given at EULAR 2012. Rituximab for the Treatment of Rheumatoid Arthritis
 New Evidence reports on presentations given at EULAR 2012 Rituximab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Long-term safety of rituximab: 10-year follow-up in the
New Evidence reports on presentations given at EULAR 2012 Rituximab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Long-term safety of rituximab: 10-year follow-up in the
Rheumatoid Arthritis. Outline. Treatment Goal 4/10/2013. Clinical evaluation New treatment options Future research Discussion
 Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
Rheumatoid Arthritis Robert L. Talbert, Pharm.D., FCCP, BCPS University of Texas at Austin College of Pharmacy University of Texas Health Science Center at San Antonio Outline Clinical evaluation New treatment
Immune modulation in rheumatology. Geoff McColl University of Melbourne/Australian Rheumatology Association
 Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Treatments for severe psoriasis
 Treatments for severe psoriasis John R Sullivan, Dermatologist and Clinical Pharmacologist, Southderm Kogarah, Skin and Cancer Foundation Australia, St Vincent s Hospital, and University of New South Wales,
Treatments for severe psoriasis John R Sullivan, Dermatologist and Clinical Pharmacologist, Southderm Kogarah, Skin and Cancer Foundation Australia, St Vincent s Hospital, and University of New South Wales,
Adalimumab for the treatment of psoriasis
 DOI: 10.3310/hta13suppl2/07 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Adalimumab for the treatment of psoriasis D Turner, J Picot,* K Cooper and E Loveman Southampton Health Technology Assessments
DOI: 10.3310/hta13suppl2/07 Health Technology Assessment 2009; Vol. 13: Suppl. 2 Adalimumab for the treatment of psoriasis D Turner, J Picot,* K Cooper and E Loveman Southampton Health Technology Assessments
New and Emerging Immunotherapies for Multiple Sclerosis: Oral Agents
 New and Emerging Immunotherapies for Multiple Sclerosis: Oral Agents William Tyor, M.D. Chief, Neurology Atlanta VA Medical Center Professor, Department of Neurology Emory University School of Medicine
New and Emerging Immunotherapies for Multiple Sclerosis: Oral Agents William Tyor, M.D. Chief, Neurology Atlanta VA Medical Center Professor, Department of Neurology Emory University School of Medicine
The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma
 The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma 11 th Annual National Leadership Summit on Health Disparities Innovation Towards Reducing Disparities Congressional Black
The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma 11 th Annual National Leadership Summit on Health Disparities Innovation Towards Reducing Disparities Congressional Black
Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice
 Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice Gu NY 1, Huang XY 2, Globe D 2, Fox KM 3 1 University of Southern California,
Methods for Measuring Dose Escalation in TNF Antagonists for Rheumatoid Arthritis Patients Treated in Routine Clinical Practice Gu NY 1, Huang XY 2, Globe D 2, Fox KM 3 1 University of Southern California,
Autoimmune Diseases More common than you think Randall Stevens, MD
 Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
Guideline for the use of Biological Therapies in the Treatment of Psoriasis
 1 Date of Production: March1 st 2011 Date of 1 st review: July 10 th 2015 Date for next review: March1 st 2018 Local Contact Dermatology Consultant Shanti Ayob Patient group to which this applies: Patients
1 Date of Production: March1 st 2011 Date of 1 st review: July 10 th 2015 Date for next review: March1 st 2018 Local Contact Dermatology Consultant Shanti Ayob Patient group to which this applies: Patients
Key words: Psoriasis, Calcipotriol, Tazarotene. tazarotene. 16 ( 4 ) tazarotene calcipotriol ( 22 : 23-34, 2004)
 In the treatment of plaque psoriasis, tazarotene was known to be effective, but its efficacy in a Taiwanese population has not been reported. Our purpose was to compare the efficacy, side effects and the
In the treatment of plaque psoriasis, tazarotene was known to be effective, but its efficacy in a Taiwanese population has not been reported. Our purpose was to compare the efficacy, side effects and the
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
How To Choose A Biologic Drug
 North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
North Carolina Rheumatology Association Position Statements I. Biologic Agents A. Appropriate delivery, handling, storage and administration of biologic agents B. Indications for biologic agents II. III.
Phenotypes and Classification of Psoriasis
 Rheumatology 2010 Birmingham 21 April 2010 Phenotypes and Classification of Psoriasis Christopher E.M. Griffiths Abbott Centocor Incyte Galderma Janssen-Cilag Leo Pharma Lynxx Novartis Pfizer Schering-Plough
Rheumatology 2010 Birmingham 21 April 2010 Phenotypes and Classification of Psoriasis Christopher E.M. Griffiths Abbott Centocor Incyte Galderma Janssen-Cilag Leo Pharma Lynxx Novartis Pfizer Schering-Plough
subcutaneous initially every 4 weeks then every 12 weeks Coverage Criteria: Express Scripts, Inc. monograph dated 02/24/2010
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Humira (adalimumab subcutaneous injection) Commercial HMO/PPO/CDHP
TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY. Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine
 TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine AUTOIMMUNE DISEASES An autoimmune disorder occurs when the body s immune
TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine AUTOIMMUNE DISEASES An autoimmune disorder occurs when the body s immune
Systematic Review of UV-Based Therapy for Psoriasis
 Am J Clin Dermatol (2013) 14:87 109 DOI 10.1007/s40257-013-0015-y EVIDENCE-BASED REVIEW ARTICLE Systematic Review of UV-Based Therapy for Psoriasis Fahad Almutawa Naif Alnomair Yun Wang Iltefat Hamzavi
Am J Clin Dermatol (2013) 14:87 109 DOI 10.1007/s40257-013-0015-y EVIDENCE-BASED REVIEW ARTICLE Systematic Review of UV-Based Therapy for Psoriasis Fahad Almutawa Naif Alnomair Yun Wang Iltefat Hamzavi
Summary of the risk management plan (RMP) for Otezla (apremilast)
 EMA/741412/2014 Summary of the risk management plan (RMP) for Otezla (apremilast) This is a summary of the risk management plan (RMP) for Otezla, which details the measures to be taken in order to ensure
EMA/741412/2014 Summary of the risk management plan (RMP) for Otezla (apremilast) This is a summary of the risk management plan (RMP) for Otezla, which details the measures to be taken in order to ensure
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Multiple Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Multiple Technology Appraisal Infliximab, adalimumab and golimumab for treating moderately to severely active ulcerative colitis after the failure of conventional
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Multiple Technology Appraisal Infliximab, adalimumab and golimumab for treating moderately to severely active ulcerative colitis after the failure of conventional
Psoriasis; a new marker for Hepatitis C among Egyptian Patients
 ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 761-767 http://www.ijcmas.com Original Research Article Psoriasis; a new marker for Hepatitis C among Egyptian Patients Asmaa E Mohamed 1, Samaa A Taha 2, Amal
ISSN: 2319-7706 Volume 4 Number 6 (2015) pp. 761-767 http://www.ijcmas.com Original Research Article Psoriasis; a new marker for Hepatitis C among Egyptian Patients Asmaa E Mohamed 1, Samaa A Taha 2, Amal
IMPORTANT DRUG WARNING Regarding Mycophenolate-Containing Products
 Dear Healthcare Provider: Mycophenolate REMS (Risk Evaluation and Mitigation Strategy) has been mandated by the FDA (Food and Drug Administration) due to postmarketing reports showing that exposure to
Dear Healthcare Provider: Mycophenolate REMS (Risk Evaluation and Mitigation Strategy) has been mandated by the FDA (Food and Drug Administration) due to postmarketing reports showing that exposure to
Dermatologica Sinica
 DERMATOLOGICA SINICA 31 (2013) 49e53 Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com ORIGINAL ARTICLE Efficacy and safety of etanercept
DERMATOLOGICA SINICA 31 (2013) 49e53 Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com ORIGINAL ARTICLE Efficacy and safety of etanercept
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC)
 BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
SYNOPSIS. 2-Year (0.5 DB + 1.5 OL) Addendum to Clinical Study Report
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier (For National Authority Use
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier (For National Authority Use
påçííáëü=jéçáåáåéë=`çåëçêíáìã==
 påçííáëü=jéçáåáåéë=`çåëçêíáìã== adalimumab 40mg pre-filled syringe for subcutaneous injection (Humira ) No. (218/05) Abbott New indication: treatment of active and progressive psoriatic arthritis in adults
påçííáëü=jéçáåáåéë=`çåëçêíáìã== adalimumab 40mg pre-filled syringe for subcutaneous injection (Humira ) No. (218/05) Abbott New indication: treatment of active and progressive psoriatic arthritis in adults
Patient Input Information Clinical Trials Outcomes Common Drug Review
 CDEC FINAL RECOMMENDATION USTEKINUMAB (Stelara Janssen Inc.) Indication: Psoriatic Arthritis Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that ustekinumab not be listed at the submitted
CDEC FINAL RECOMMENDATION USTEKINUMAB (Stelara Janssen Inc.) Indication: Psoriatic Arthritis Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that ustekinumab not be listed at the submitted
5.07.09. Aubagio. Aubagio (teriflunomide) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd
 ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd 07 February 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the
ustekinumab 45mg solution for injection in pre-filled syringe (Stelara ) SMC No. (944/14) Janssen-Cilag Ltd 07 February 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Version History. Previous Versions. Policy Title. Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author
 Version History Policy Title Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields
Version History Policy Title Drugs for MS.Drug facts box Glatiramer Acetate Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields
PREVALENCE AND RISK FACTORS FOR PSYCHIATRIC COMORBIDITY IN PATIENTS WITH ALCOHOL DEPENDENCE SYNDROME Davis Manuel 1, Linus Francis 2, K. S.
 PREVALENCE AND RISK FACTORS FOR PSYCHIATRIC COMORBIDITY IN PATIENTS WITH ALCOHOL DEPENDENCE SYNDROME Davis Manuel 1, Linus Francis 2, K. S. Shaji 3 HOW TO CITE THIS ARTICLE: Davis Manuel, Linus Francis,
PREVALENCE AND RISK FACTORS FOR PSYCHIATRIC COMORBIDITY IN PATIENTS WITH ALCOHOL DEPENDENCE SYNDROME Davis Manuel 1, Linus Francis 2, K. S. Shaji 3 HOW TO CITE THIS ARTICLE: Davis Manuel, Linus Francis,
GT-020 Phase 1 Clinical Trial: Results of Second Cohort
 GT-020 Phase 1 Clinical Trial: Results of Second Cohort July 29, 2014 NASDAQ: GALT www.galectintherapeutics.com 2014 Galectin Therapeutics inc. Forward-Looking Statement This presentation contains, in
GT-020 Phase 1 Clinical Trial: Results of Second Cohort July 29, 2014 NASDAQ: GALT www.galectintherapeutics.com 2014 Galectin Therapeutics inc. Forward-Looking Statement This presentation contains, in
TREATING INFLAMMATORY BOWEL DISEASE (IBD) BACKGROUNDER
 Press information for journalists only TREATING INFLAMMATORY BOWEL DISEASE (IBD) BACKGROUNDER Why treat IBD? IBD describes a range of chronic diseases of the gastrointestinal system, encompassing Ulcerative
Press information for journalists only TREATING INFLAMMATORY BOWEL DISEASE (IBD) BACKGROUNDER Why treat IBD? IBD describes a range of chronic diseases of the gastrointestinal system, encompassing Ulcerative
9/16/2014. Anti-Immunoglobulin E (IgE) Omalizumab (Xolair ) Dosing Guidance
 Disclosure Statement of Financial Interest New Therapies for Asthma Including Omalizumab and Anti-Cytokine Therapies Marsha Dangler, PharmD, BCACP Clinical Pharmacy Specialist James H. Quillen VA Medical
Disclosure Statement of Financial Interest New Therapies for Asthma Including Omalizumab and Anti-Cytokine Therapies Marsha Dangler, PharmD, BCACP Clinical Pharmacy Specialist James H. Quillen VA Medical
Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment.
 1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
1 Low dose capecitabine is effective and relatively nontoxic in breast cancer treatment. John T. Carpenter, M.D. University of Alabama at Birmingham NP 2508 1720 Second Avenue South Birmingham, AL 35294-3300
CHAPTER V DISCUSSION. normal life provided they keep their diabetes under control. Life style modifications
 CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
CHAPTER V DISCUSSION Background Diabetes mellitus is a chronic condition but people with diabetes can lead a normal life provided they keep their diabetes under control. Life style modifications (LSM)
Science > MultiClear. How the MultiClear works?
 Science > MultiClear How the MultiClear works? Treatment of Psoriasis by UVB is a common, effective and respected therapy for more than 100 years.[1] Narrow band UVB light (peak 296-313 nm) has been clinically
Science > MultiClear How the MultiClear works? Treatment of Psoriasis by UVB is a common, effective and respected therapy for more than 100 years.[1] Narrow band UVB light (peak 296-313 nm) has been clinically
LEFLUNOMIDE (Adults)
 Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Shared Care Guideline DRUG: Introduction: LEFLUNOMIDE (Adults) Indication: Disease modifying drug for rheumatoid arthritis and psoriatic arthritis Licensing Information: Disease modifying drug for active
Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy
 Media Release Basel, 6 June 2012 Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy Roche (SIX: RO, ROG; OTCQX: RHHBY) today announced
Media Release Basel, 6 June 2012 Roche s RoACTEMRA improved rheumatoid arthritis signs and symptoms significantly more than adalimumab as single-agent therapy Roche (SIX: RO, ROG; OTCQX: RHHBY) today announced
Activity of pemetrexed in thoracic malignancies
 Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden
 Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden Collaborators: Primary investigators Dr Lars Erik Kristensen,
Effectiveness and Drug Adherence in Rheumatoid Arthritis Patients on Biologic Monotherapy: A prospective observational study in Southern Sweden Collaborators: Primary investigators Dr Lars Erik Kristensen,
EMEA PUBLIC STATEMENT ON LEFLUNOMIDE (ARAVA) - SEVERE AND SERIOUS HEPATIC REACTIONS -
 The European Agency for the Evaluation of Medicinal Products Post-authorisation evaluation of medicines for human use London, 12 March 2001 Doc. Ref: EMEA/H/5611/01/en EMEA PUBLIC STATEMENT ON LEFLUNOMIDE
The European Agency for the Evaluation of Medicinal Products Post-authorisation evaluation of medicines for human use London, 12 March 2001 Doc. Ref: EMEA/H/5611/01/en EMEA PUBLIC STATEMENT ON LEFLUNOMIDE
Managing Relapsing Remitting MS Risks & benefits of emerging therapies. Dr Mike Boggild The Walton Centre
 Managing Relapsing Remitting MS Risks & benefits of emerging therapies Dr Mike Boggild The Walton Centre MS: Facts and figures Affects 1 in 800 in the UK Commonest cause of acquired neurological disability
Managing Relapsing Remitting MS Risks & benefits of emerging therapies Dr Mike Boggild The Walton Centre MS: Facts and figures Affects 1 in 800 in the UK Commonest cause of acquired neurological disability
National MS Society Information Sourcebook www.nationalmssociety.org/sourcebook
 National MS Society Information Sourcebook www.nationalmssociety.org/sourcebook Chemotherapy The literal meaning of the term chemotherapy is to treat with a chemical agent, but the term generally refers
National MS Society Information Sourcebook www.nationalmssociety.org/sourcebook Chemotherapy The literal meaning of the term chemotherapy is to treat with a chemical agent, but the term generally refers
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
CLINICAL MANIFESTATIONS OF PSORIATIC NAIL AT THE NATIONAL HOSPITAL OF DERMATOLOGY AND VENEREOLOGY (NHDV)
 Southeast-Asian J. of Sciences: Vol. 2, No 1 (2013) pp. 101-107 CLINICAL MANIFESTATIONS OF PSORIATIC NAIL AT THE NATIONAL HOSPITAL OF DERMATOLOGY AND VENEREOLOGY (NHDV) Nguyen Huu Sau and Nguyen Minh Thu
Southeast-Asian J. of Sciences: Vol. 2, No 1 (2013) pp. 101-107 CLINICAL MANIFESTATIONS OF PSORIATIC NAIL AT THE NATIONAL HOSPITAL OF DERMATOLOGY AND VENEREOLOGY (NHDV) Nguyen Huu Sau and Nguyen Minh Thu
The Psoriasis Area and Severity Index Is the Adequate Criterion to Define Severity in Chronic Plaque-Type Psoriasis
 Clinical and Laboratory Investigations Dermatology 2005;210:194 199 DOI: 10.1159/000083509 Received: June 3, 2004 Accepted: October 4, 2004 The Psoriasis Area and Severity Index Is the Adequate Criterion
Clinical and Laboratory Investigations Dermatology 2005;210:194 199 DOI: 10.1159/000083509 Received: June 3, 2004 Accepted: October 4, 2004 The Psoriasis Area and Severity Index Is the Adequate Criterion
A prospective study on drug utilization pattern of anti-diabetic drugs in rural areas of Islampur, India
 Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 2015, 7 (5):33-37 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-5071 USA CODEN: DPLEB4
Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 2015, 7 (5):33-37 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-5071 USA CODEN: DPLEB4
Arthritis and Rheumatology Clinics of Kansas Patient Education. Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis
 Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Professor Andrew Wright,
 Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Professor Andrew Wright, Systemic treatments are drugs taken as tablets or injections that travel through the bloodstream, dampening down the immune system to reach and treat eczema all over the body.
Version History. Previous Versions. Drugs for MS.Drug facts box fingolimod Version 1.0 Author
 Version History Policy Title Drugs for MS.Drug facts box fingolimod Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields as required
Version History Policy Title Drugs for MS.Drug facts box fingolimod Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further fields as required
Articles Presented. Journal Presentation. Dr Albert Lo. Dr Albert Lo
 * This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
* This presentation is prepared by the author in one s personal capacity for the purpose of academic exchange and does not represent the views of his/her organisations on the topic discussed. Journal Presentation
Laquinimod Polman, C. et al. Neurology 2005;64:987-991
 Laquinimod Polman, C. et al. Neurology 2005;64:987-991 Multicenter, double-blind, randomized trial, patients with RR MS received 0.1 mg or 0.3 mg laquinimod or placebo as three daily tablets for 24 weeks
Laquinimod Polman, C. et al. Neurology 2005;64:987-991 Multicenter, double-blind, randomized trial, patients with RR MS received 0.1 mg or 0.3 mg laquinimod or placebo as three daily tablets for 24 weeks
How To Treat Psoriasis With Omega 3 Fatty Acids
 CAN PSORIASIS TREATMENT BE AIDED BY OMEGA-3 FATTY ACIDS? Brittney Urban Psoriasis Chronic skin disease Cell life cycle build up Can be disabling Symptoms: Red patches with silvery scales Dry, cracked skin
CAN PSORIASIS TREATMENT BE AIDED BY OMEGA-3 FATTY ACIDS? Brittney Urban Psoriasis Chronic skin disease Cell life cycle build up Can be disabling Symptoms: Red patches with silvery scales Dry, cracked skin
