Dynamic prostate brachytherapy
|
|
|
- Rhoda Powell
- 9 years ago
- Views:
Transcription
1 Dynamic prostate brachytherapy a single visit treatment for prostate cancer This leaflet aims to answer your questions about having brachytherapy to treat your prostate cancer. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital. If you have any further questions or want more detailed information, please speak to your nurse specialist contact details are at the end of this leaflet. What is radiotherapy? Radiotherapy is the use of radiation to treat cancer. It is called deep x-ray therapy (DXT) or external beam radiotherapy (EBRT). Radiotherapy uses high-energy x-rays to destroy cancer cells by preventing them from dividing and growing larger. Although normal cells in the treatment area are also affected by the radiation, they can repair themselves better than the cancer cells. Treatment can be given either as external or internal radiotherapy. External beam radiotherapy is where a machine produces beams of radiation targeted at the cancerous area. These beams travel through your body to destroy the cancer cells and are stronger than those used for taking x-rays. Internal radiotherapy is where solid radioactive material (material that gives off radiation) is placed in your body to destroy the cancer cells. It is placed within or near to your cancer, as the radiation does not travel very far. What is brachytherapy? Prostate brachytherapy is a form of internal radiotherapy for cancer that has not spread outside of your prostate gland (known as localised cancer ). It involves implanting (inserting) seeds or pellets of radioactive material directly into your prostate gland under a general or spinal anaesthetic. For more information about anaesthetic, please see our leaflet, Having an anaesthetic. page 1 of 9
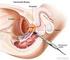
2 These seeds are about the size of a grain of rice and, using ultrasound for guidance, are implanted with a long, thin, hollow needle. See figure 1 below. prostate needle rectum probe Figure 1. Inserting radioactive seeds. Image supplied by the Prostate Cancer Charity. Brachytherapy is an established procedure for treating prostate cancer and is recognised as an alternative to traditional, external beam radiotherapy. It can be given as a single treatment or used in combination with a course of external beam radiotherapy (Brachytherapy Boost) for men with more significant cancers. Brachytherapy has been available in the UK for a number of years and several centres now offer this treatment. Our service uses the most modern treatment approach, in which both the planning stage of the procedure and the procedure itself is done in one visit. Most other centres do these separately, needing two hospital visits and anaesthetics. What are the benefits of brachytherapy? It is a simple, one day procedure compared to external beam radiotherapy, which involves six weeks of daily hospital visits. You can return to normal life much quicker than with other treatments. Because the radioactivity only travels a few millimetres to kill nearby cancer cells, a higher dose of radiation can be given than with external beam radiotherapy. As the radiation dose is targeted at the area needing treatment, the tissues surrounding the prostate, such as the bowel and bladder are less affected than with external beam radiotherapy. Although there is only limited follow-up data on the effectiveness of brachytherapy in treating prostate cancer so far, evidence from American studies suggests it is just as effective at 8-10 years after treatment compared to external beam radiation and radical surgery to remove the prostate (prostatectomy). Brachytherapy is associated with a lower risk of erectile dysfunction, urgency (an urgent need to pass urine), and radiation proctitis (pain or inflammation of the back passage) when compared to external beam radiotherapy. Please see the risk section below for more information about this. 2 of 9
3 Who will carry out the procedure? This procedure is carried out by Mr Popert, Mr Challacombe, Dr Beaney and Dr Morris who have all undergone specialist training in this procedure with experts in America and Europe. What are the alternatives? Brachytherapy is just one of the available options to treat localised prostate cancer. Your doctor will discuss with you any other treatments that are appropriate for your grade and extent of cancer. Please read our other leaflets for more information on these specific treatments: external beam radiotherapy, beams of radiation to destroy the cancer cells open radical prostatectomy, surgery to remove your prostate though an incision (cut) in your abdomen robotic radical prostatectomy, surgery to remove your prostate using robotic instruments and several keyholes active surveillance/monitoring. In some cases it may be an option not to treat your cancer. This is referred to as active surveillance or monitoring. Some cancers need to be treated more urgently than others, depending on how aggressive they are. If a very aggressive cancer is not treated, it may spread to other parts of the body. Your doctor will tell you if active surveillance is an option for you, but please do not make any decisions before speaking to your doctor or specialist nurse. How does brachytherapy compare to other treatments? Recently published data has suggested that brachytherapy is as successful as external beam radiotherapy and surgery in curing small, slow growing prostate cancers. You will already have had a PSA (prostate specific antigen) blood test to help diagnose your cancer. PSA tests are also used to monitor the effectiveness of any treatment you receive. American studies have shown that 17 out of 20 men had no rise in their PSA in the 10 years following brachytherapy. These results mirror studies of patients who have surgery to remove the prostate. As with any form of radiotherapy to the prostate, you are at risk of incontinence and impotence or sexual dysfunction. However, studies have shown that the risks of these side-effects are significantly lower for brachytherapy than for external beam radiotherapy or surgery. Also, unlike other treatments, brachytherapy does not affect your fertility or ability to ejaculate. There are no clear long-term disadvantages to brachytherapy in comparison to external beam radiotherapy. The short term side-effects of lower urinary tract symptoms, such as urgency to urinate, frequency (the need to pass urine often) and discomfort when urinating, are more common with brachytherapy. This is due to the radiation, which is released over a period of months. 3 of 9
4 What are the risks? Your consultant will discuss the following possible complications with you in more detail. Urinary frequency and urgency. About 1 out of 50 men experience some urgency for up to three months after brachytherapy. These symptoms are mild in 4 out of 5 patients and moderately severe in 1 out of 5 patients. The symptoms usually peak 6-12 weeks after brachytherapy and improve after this. They can be controlled by making sure you drink plenty of clear fluids and avoiding caffeine and alcohol. We can also give you medication if needed, to improve your urine flow and reduce irritation to your urethra (tube through which you pass urine). These symptoms have usually resolved within six months of your implant. This risk is lower for brachytherapy than external beam radiotherapy where 2-3 out of 10 men experience urge incontinence (where you leak urine before reaching a toilet) and surgery where 1 out 2 men experience stress incontinence (when you leak urine without the urge to the toilet, for example when you sneeze or laugh). Urinary retention (the inability to pass urine). This is unusual, but can occur particularly if your prostate is large and swells further after treatment. If we think you are at risk, we will discuss the options for managing this with you before your treatment. Erectile dysfunction. About 1 out of 5 men may have a temporary reduction in the quality of their erections in the six months after brachytherapy. This is less than the 6-7 out of 10 men treated with external beam radiotherapy and almost all of the men who have had a radical prostatectomy. Erectile dysfunction can be helped by medicine if needed. Your erections normally return to pretreatment level within a year. In the longer term (several years), there may be a further reduction in erectile function, but again this can be helped by medicines. The risk of erectile dysfunction is greater for patients who have combination treatment, with hormones or external beam radiation with brachytherapy. Compared to radical surgery and hormone radiation, erectile function is much better maintained with brachytherapy. Fertility. Although other radical treatments will usually leave you sterile, this is not the case after brachytherapy. If your partner is of childbearing age she should be aware of this fact. Because the seeds remain radioactive for about a year after implantation, we recommend that you and your partner use contraception for a year after your treatment to avoid pregnancy. Rectal bleeding/ proctitis (pain/inflammation of the back passage). 1 to 2 out of 50 patients may experience this after brachytherapy, compared to 5-10 out of 50 men treated with external beam radiotherapy If you have rectal bleeding you must contact us so we can advise you what to do. Bowel irritation. This can occur as late as two to three years after brachytherapy, but medicines can often treat this. If your GP refers you to a bowel specialist, they must be told that you have had brachytherapy. They should speak to your consultant before you have any biopsies of your bowel, as this can lead to further problems. 4 of 9
5 Seed migration (where the radioactive seeds are carried in the blood vessels to the lungs). You will not experience any specific symptoms if you have seed migration. It is generally picked up during investigations for other unrelated problems. When you first have your implant the risk is around 1 in 100 patients although up to 30 in 100 patients may experience some seed migration in the long-term. However, studies that have followed up seed migration cases have not reported any long-term harmful effects. Anaesthetic. Modern anaesthesia is very safe and serious problems are uncommon. Your anaesthetist (a specially trained doctor who gives anaesthetics) will use specialist equipment to monitor you closely throughout the procedure. However, risk cannot be removed completely and some people may have side effects or complications. Our leaflet, Having an anaesthetic, has more information about this. Please ask for a copy from a member of staff. How can I prepare for the procedure? Prostate assessment and symptom score Before brachytherapy, the size of your prostate has to be measured to estimate the number of seeds needed for the procedure. You may hear this assessment called a trans rectal ultrasound. Images from an ultrasound probe (rather like the one that was used during your biopsies) are taken to allow the size and volume of your prostate to be carefully measured. If your prostate biopsy was carried out at Guy s and St Thomas Hospital a prostate assessment will have been done at this time. If not, your prostate size and symptoms will be assessed a few weeks or months before the brachytherapy. To make sure that your risk of urinary retention is low, we will also carry out: a prostate symptom score (questionnaire which helps us monitor how many urinary symptoms you have and how severe you think they are); and a flow rate (where you pass urine into a special machine that measures how strong your urine flow is). Many centres are unable to carry out brachytherapy on large prostates (greater than 50cc) and patients are given medicine to reduce the size of their prostate before treatment. We have found this to be unnecessary and have treated prostates up to 80cc in size. However, the risk of urinary symptoms and retention is greater if you have a large prostate. You may need to learn how to pass a small tube (catheter) into your bladder to drain off any excess urine. This will prevent you from needing to come into hospital if you can t pass urine properly at first. If your prostate is too large, we may discuss alternative treatments with you or offer hormone therapy for three months. We may also offer an operation to core out the middle of your prostate to reduce its size. If you need this, your prostate will be reassessed before the brachytherapy treatment. We will give you a prescription for a type of medicine called an alpha blocker (tamsulosin or alfuzosin hydrochloride), which you will need to start taking 48 hours before you come to hospital for your implant. This medicine helps to ease the flow of your urine over the coming months, while your prostate is swollen from the implants. It will also help to reduce the risk of urinary retention. 5 of 9
6 If you do not get a prescription, please contact your specialist nurse to organise this. You will need to continue taking this medicine until one of the doctors looking after you tells you otherwise. To do this, you will need to get repeat prescriptions from your GP. You may need to take the medicine for up to 18 months after the implant. We will give you a prescription for an enema. This is to clear your bowels either on the morning of your procedure or the night before if you are travelling from some distance away. Your doctor/nurse will give you instructions on when you should give this. You will be given a prescription for an antibiotic called ciprofloxacin. You should start this after your implant (the evening of the implant). Make sure that you have this prescription before you leave the hospital. Pre-admission clinic You will need to attend a pre-admission clinic before you have your treatment. We will check your suitability for a spinal or general anaesthetic at this appointment. A spinal anaesthetic is where your body is numbed below the waist and a general anaesthetic is where you are put to sleep for the whole procedure. This will be discussed with you in more detail at your clinic appointment. We will carry out a number of tests to make sure that your heart, lungs and kidneys are working properly. You may have a chest x-ray, ECG or electrocardiogram (recording of the electrical activity of your heart) and some blood taken. Your doctor will explain any further tests you need. Please let us know if you are taking any antiplatelet medicines (for example, aspirin, clopidogrel) or any medicines that thin the blood (for example, warfarin), as these may need to be withheld temporarily before the procedure. We will give you more advice about this. Do not make any changes to your usual medicines and continue to take them unless you are told otherwise. Please remember to bring them with you to the pre-admission clinic and on the day of your procedure. If you smoke, you may be asked to stop smoking, as this increases the risk of developing a chest infection or deep vein thrombosis or DVT (blood clot developing in a deep vein). Smoking can also delay wound healing because it reduces the amount of oxygen that reaches the tissues in your body. If you would like to give up smoking, please speak to your nurse or call the NHS Smoking Helpline on You must not eat or drink anything for at least six hours before the procedure is carried out. This will be explained to you in the pre-admission clinic. If you do not follow these instructions, your procedure may have to be cancelled. What should I expect when I come to hospital? When you arrive at hospital, you will be seen by a nurse who will take some of your details and prepare you for theatre. A doctor from your consultant s team will ask your permission to perform the procedure. You will be asked to sign a consent form that says you have agreed to the procedure and that you understand the benefits, risks and alternatives. If there is anything you don t understand or you need more time to think about it, please tell the staff caring for you. 6 of 9
7 Remember, it is your decision. You can change your mind at any time, even if you have signed the consent form. Let staff know immediately if you change your mind. Your wishes will be respected at all times. If you would like to read our consent policy, please tell a member of staff. The anaesthetist will also see you to discuss your anaesthetic. If you have any further questions or concerns, your specialist nurse will be available to answer them. The procedure The procedure itself takes between one and a half and two hours. In the technique used here at Guys and St Thomas, between 40 and 120 radioactive seeds are placed inside the prostate. These gradually release their radiation dose over a few months. Once you are anaesthetised, the doctor will insert an ultrasound probe into your rectum, to help see where the needles are to be placed. When your doctor can clearly see your prostate on the ultrasound, needles are inserted into your prostate through your perineum - the area of skin beneath your scrotum. Once the needles have been positioned, the doctor will make careful measurements of your prostate and use a computer to determine the exact placing, and number of seeds. The seeds are then inserted into your prostate through these needles. Implanting the seeds will take about 45 minutes to an hour. The seeds will be permanently left in your prostate, although they will have released 95% of their radiation a year after being implanted. Your doctor will carefully work out the dose of radiation you are given so that the size and shape of your prostate is covered by the radiation, as well as a small area of surrounding tissue. We will reduce unnecessary radiation to the bladder and bowel and reduce the dose to your urethra as much as possible. After the implant After the seeds have been implanted you will be taken to the recovery room. You will stay here until you awake from the anaesthetic, which usually takes about an hour. After this, you will be taken back to your ward or day surgery unit. When you wake up you will have a drip (a bag of fluid connected to a small tube in a vein in your arm) to keep you well hydrated until you are able to drink fluids. Passing urine may be a little uncomfortable at first. If you have problems with this you may need a catheter inserted, although most patients do not need this. If you are coming in as a day surgery patient you will need a relative or friend to help you home afterwards. If you are staying on the ward and your friends and family members come to visit you in hospital, they can wait in the ward day room and visit you afterwards. You will stay on the main ward with other patients, which shows just how safe the radiation levels are. There are a few special precautions to follow because of the radiation. Please do not allow any young children to sit on your lap and do not cuddle them or anyone who is pregnant. This is because young children and foetuses (babies before they are born) are more vulnerable to even low levels of radiation and it could impact on their development. For this reason, we recommend that you avoid close contact (<0.5m) with young children and pregnant women for the first two months after the implant. Also you must wear a condom during sexual intercourse due to the very small risk of passing a seed, again only for the first two months after the implant. Please speak to your nurse specialist if you have any questions or concerns regarding these precautions. 7 of 9
8 Your consultant or a member of his team will come and see you after you have returned to the ward and your nurse has settled you in. There is not usually much pain from this procedure; although you may be a little sore. We can give you painkillers if you need them, so please let us know if you are in pain. We will usually give you oral painkillers such as paracetamol or ibuprofen, which you can take as soon as you are able to eat and drink. This is usually within hours of returning to the ward. When can I go home? You should be able to leave hospital within 12 hours of the procedure. Before leaving the hospital you will be given a Radionuclide Instruction card, which is about the size of a credit card. The card has details of who to contact in an emergency and information on the special radiation precautions we should follow after your implant. You should keep the card with you at all times, especially if you are travelling abroad as the implants can set off security alarms in airports in much the same way as hip/knee replacements and pacemakers can. You will be given one week course of antibiotics to start the evening of your implant. You must complete the course as it will reduce the risk of urinary infection. Your nurses will also give you a set of reminder instructions when you leave the hospital. If you have any questions between your implant and follow-up appointment please contact one of the prostate cancer nurses contact details are at the end of this leaflet. When you go home, please drink plenty of clear fluids each day. We recommend two to three litres, but do not drink any caffeine (tea or coffee) or fizzy drinks. You should be able to return to normal activities within about three days. Please take things gently at first and build up your activities slowly. You should be able to go back to work about five days after the implant. What side-effects can I expect after getting home? You may experience the following symptoms in the first two to three days: discomfort around your bottom when you sit down blood-stained urine bruising under your scrotum difficulty passing urine needing to pass urine frequently and having to rush to the toilet to pass urine. Please let us know if you have problems passing urine, as you may need additional treatment for a few days such as a catheter to drain your urine. One in 10 patients will need catheterisation after having brachytherapy. These symptoms should get better with time. Four to eight weeks after your implant you might have: pain when you ejaculate, less forceful ejaculation or a reduced amount of ejaculate. This is related to the medication (tamsulosin) and the effect of the radiotherapy urinary frequency (going many times to pass small amounts of urine) pain on passing urine (this is the most common time to experience this) complete loss of erections this is rare, but if it does happen, there is a variety of treatments to help, which we can discuss with you. 8 of 9
9 If you continue to have problems around eight weeks after your implant, you may need further treatment from your specialist. When will I have a follow-up appointment? You will be closely followed-up after the implant. You will have a CT scan of your prostate four to six weeks after having your implant, to check the positioning of the seeds, particularly if you have needed a Transurethral resection of the prostate (TURP) before the brachytherapy treatment. This is part of a quality control assessment, to check the implant quality and compare this to the assessment made at the time of the procedure. It is not used to see whether the cancer has gone. Testing your PSA You will have your first PSA test two to four months after the implant and again at six to eight months after implantation. We expect your PSA to fall in the months following the implant and most patients will have a PSA of less than 0.5 three to five years after brachytherapy. However, you should be aware that for some patients, their PSA rises months after the implant and then starts to fall again. This is called PSA bounce. It is not a sign of treatment failure, but occurs more commonly in patients under 70 and those with larger prostates. PSA bounce occurs in up to 30 out of 100 of patients, but this has not been shown to have any negative impact on the treatment outcome. Contact us If you have any questions or concerns, please contact Netty Kinsella (prostate cancer advanced nurse practitioner) or Sharon Clovis (prostate nurse specialist) on Monday to Friday, 8am to 5pm. Alternatively call the hospital switchboard on and ask for the bleep desk. Ask the operator to bleep 2393 or 1005 respectively and wait for a response. If you need medical advice outside of these hours, please contact your GP, NHS Direct (details below) or if it is urgent go to your nearest Accident and Emergency (A&E) Department. Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: am to 5pm, Monday to Friday NHS Direct Offers health information and advice from specially trained nurses over the phone 24 hours a day. t: w: Leaflet number: 0123/VER4 Date published: July 2013 Review date: July Guy s and St Thomas NHS Foundation Trust 9 of 9
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate)
 Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
University College Hospital. Prostate high dose rate (HDR) brachytherapy. Radiotherapy Department Patient information series
 University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
University College Hospital Prostate high dose rate (HDR) brachytherapy Radiotherapy Department Patient information series 18 2 If you need a large print, audio or translated copy of the document, please
Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT)
 Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
Treatment for bladder tumours - transurethral resection of a bladder tumour (TURBT) You have had a cystoscopy or other examination that has shown that you have an abnormal area (tumour) in your bladder.
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
GreenLight laser prostatectomy
 Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Ambulatory Care & Local Networks GreenLight laser prostatectomy Information for day surgery patients This information sheet answers some of the questions you may have about having a GreenLight laser prostatectomy.
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet
 Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Transrectal Ultrasound (Trus) Guided Prostate Biopsies Urology Patient Information Leaflet Page 1 What is the purpose of my appointment? Your doctor has informed us that you have an elevated Prostate Specific
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer This information sheet has been given to you to explain the use of maintenance
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Maintenance BCG for nonmuscle invasive bladder cancer This information sheet has been given to you to explain the use of maintenance
Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy
 6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
6 Pages, English Information sheet: Robotic-Assisted Laparoscopic Radical Prostatectomy This information sheet is to provide you and your family with information regarding your treatment and recovery from
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH)
 GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
GreenLight Laser Therapy for Treating Benign Prostatic Hyperplasia (BPH) To learn about this procedure it helps to know these words: The prostate is the sexual gland that makes a fluid which helps sperm
Radioactive Seed Implants for Prostate Cancer information for patients and their families
 UROLOGICAL CANCER Radioactive Seed Implants for Prostate Cancer information for patients and their families The Alvin J. Siteman Cancer Center 660 South Euclid Avenue, Box 8100 St. Louis, MO 63110-1093
UROLOGICAL CANCER Radioactive Seed Implants for Prostate Cancer information for patients and their families The Alvin J. Siteman Cancer Center 660 South Euclid Avenue, Box 8100 St. Louis, MO 63110-1093
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
SUPRAPUBIC CATHETER INSERTION INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Macroplastique injection for stress urinary incontinence
 Macroplastique injection for stress urinary incontinence Information for patients This information sheet answers some of the questions you may have about having a Macroplastique injection. It explains
Macroplastique injection for stress urinary incontinence Information for patients This information sheet answers some of the questions you may have about having a Macroplastique injection. It explains
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife
 Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Specific Antigen (PSA) Blood Test
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
Treating Mesothelioma - A Quick Guide
 Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Treating Mesothelioma - A Quick Guide Contents This is a brief summary of the information on Treating mesothelioma from CancerHelp UK. You will find more detailed information on the website. In this information
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Rivaroxaban for the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE)
 Rivaroxaban for the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) This leaflet aims to answer your questions about rivaroxaban that may be prescribed for you when you are diagnosed
Rivaroxaban for the treatment of deep vein thrombosis (DVT) and pulmonary embolism (PE) This leaflet aims to answer your questions about rivaroxaban that may be prescribed for you when you are diagnosed
How prostate cancer is diagnosed
 How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
AMPUTATION OF THE PENIS (PARTIAL OR COMPLETE) FOR CANCER INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] AMPUTATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] AMPUTATION
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Periurethral bulking agent for stress urinary incontinence (macroplastique)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
A Patient s Guide to TURP Your Prostate Operation
 A Patient s Guide to TURP Your Prostate Operation Mr John Davies BSc FRCS(Urol) Mr Christopher Eden MS FRCS(Urol) Mr Simon Bott FRCS Professor Stephen Langley MS FRCS(Urol) Prostate Cancer Centre, Guildford
A Patient s Guide to TURP Your Prostate Operation Mr John Davies BSc FRCS(Urol) Mr Christopher Eden MS FRCS(Urol) Mr Simon Bott FRCS Professor Stephen Langley MS FRCS(Urol) Prostate Cancer Centre, Guildford
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
Patient Information Sheet
 TRANSURETHRAL RESECTION OF PROSTATE (TURP) Patient Information Sheet Department of Urology Homerton University Hospital NHS Foundation Trust Homerton Row, London, E9 6SR Reviewed: June 2012 Next date:
TRANSURETHRAL RESECTION OF PROSTATE (TURP) Patient Information Sheet Department of Urology Homerton University Hospital NHS Foundation Trust Homerton Row, London, E9 6SR Reviewed: June 2012 Next date:
Headache after an epidural or spinal injection What you need to know. Patient information Leaflet
 Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Headache after an epidural or spinal injection What you need to know Patient information Leaflet April 2015 We have produced this leaflet to give you general information about the headache that may develop
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
PATIENT INFORMATION. Brachytherapy for Cancer of the Cervix
 PATIENT INFORMATION Brachytherapy for Cancer of the Cervix Cancer Therapy Centre Locked Mailbag 7103, Liverpool BC, NSW 1871 Telephone: 8738 5180 Facsimile: 8738 5188 August 2013 1. Introduction Radiotherapy
PATIENT INFORMATION Brachytherapy for Cancer of the Cervix Cancer Therapy Centre Locked Mailbag 7103, Liverpool BC, NSW 1871 Telephone: 8738 5180 Facsimile: 8738 5188 August 2013 1. Introduction Radiotherapy
Botox treatment for an overactive bladder in women. Information for patients Gynaecology
 Botox treatment for an overactive bladder in women Information for patients Gynaecology What is bladder overactivity (OAB)? Bladder overactivity is a common condition, affecting around one in five people.
Botox treatment for an overactive bladder in women Information for patients Gynaecology What is bladder overactivity (OAB)? Bladder overactivity is a common condition, affecting around one in five people.
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
External beam radiotherapy
 Treatment Helpline 0800 074 8383 prostatecanceruk.org 1 External beam radiotherapy In this fact sheet: Who can have radiotherapy? How does radiotherapy treat prostate cancer? What are the advantages and
Treatment Helpline 0800 074 8383 prostatecanceruk.org 1 External beam radiotherapy In this fact sheet: Who can have radiotherapy? How does radiotherapy treat prostate cancer? What are the advantages and
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE
 VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
VAGINAL TAPE PROCEDURES FOR THE TREATMENT OF STRESS INCONTINENCE AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k
CONTENTS: WHAT S IN THIS BOOKLET
 Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
University College Hospital. Hormone therapy for prostate cancer. Radiotherapy Department Patient information series
 University College Hospital Hormone therapy for prostate cancer Radiotherapy Department Patient information series 10 2 If you need a large print, audio or translated copy of the document, please contact
University College Hospital Hormone therapy for prostate cancer Radiotherapy Department Patient information series 10 2 If you need a large print, audio or translated copy of the document, please contact
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
The PSA Test for Prostate Cancer Screening:
 For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
UCLH. Transurethral resection of bladder tumour (TURBT) Urology Directorate
 UCLH Transurethral resection of bladder tumour (TURBT) Urology Directorate 2 3 If you require a large print, audio or translated version of this leaflet, please contact us on 0845 155 5000 ext 79280. We
UCLH Transurethral resection of bladder tumour (TURBT) Urology Directorate 2 3 If you require a large print, audio or translated version of this leaflet, please contact us on 0845 155 5000 ext 79280. We
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER. How Will I Know If My Prostate Cancer Returns?
 WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
Having a urinary catheter information for men
 Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Understanding the PSA test. A guide for men concerned about prostate cancer
 Understanding the PSA test A guide for men concerned about prostate cancer Introduction This booklet is for men who want to know more about having a blood test, called a PSA test, that can help diagnose
Understanding the PSA test A guide for men concerned about prostate cancer Introduction This booklet is for men who want to know more about having a blood test, called a PSA test, that can help diagnose
Enhanced recovery after laparoscopic surgery (ERALS) programme: patient information and advice 2
 This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
This booklet is funded by, and developed in collaboration between University Hospital Southampton NHS Foundation Trust and Pfizer Limited. NPKAM0198 March 2014 Enhanced recovery after laparoscopic surgery
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
However, each person may be managed in a different way as bowel pattern is different in each person.
 Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Prostate Cancer. What is prostate cancer?
 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
What to Expect While Receiving Radiation Therapy for Prostate Cancer
 What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
Having denervation of the renal arteries for treatment of high blood pressure
 Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
Having denervation of the renal arteries for treatment of high blood pressure The aim of this information sheet is to help answer some of the questions you may have about having denervation of the renal
What should I expect before the procedure?
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
Primary and revision lumbar discectomy. (nerve root decompression)
 Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Primary and revision lumbar discectomy (nerve root decompression) The aim of this leaflet is to help answer some of the questions you may have about having a lumbar discectomy. It explains the benefits,
Information for men considering a male sling procedure
 Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Colposuspension for stress urinary incontinence
 Colposuspension for stress urinary incontinence Information for patients This leaflet sheet answers some of the questions you may have about colposuspension. It explains the benefits, the risks and the
Colposuspension for stress urinary incontinence Information for patients This leaflet sheet answers some of the questions you may have about colposuspension. It explains the benefits, the risks and the
Short Course, Pre-operative Radiotherapy for Bowel Cancer
 Short Course, Pre-operative Radiotherapy for Bowel Cancer Patient Information Introduction This leaflet tells you about short course, pre-operative radiotherapy for the treatment of bowel cancer. It explains
Short Course, Pre-operative Radiotherapy for Bowel Cancer Patient Information Introduction This leaflet tells you about short course, pre-operative radiotherapy for the treatment of bowel cancer. It explains
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer
 Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
Information for Men Receiving Radiation and Hormone Treatments for Prostate Cancer Treatment Plan Stage of prostate cancer: RADIATION THERAPY Radiation Treatments: Date for planning CT: Date to start radiation
An operation for prolapse Colpocleisis
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
The following document includes information about:
 Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
V03 Varicose Veins Surgery
 V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
150640_Brochure_B 4/12/07 2:58 PM Page 2. Patient Information. Freedom From an Enlarged Prostate
 150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Vasectomy Services Patient Information
 Vasectomy Services Patient Information Vasectomy Vasectomy Please read this information leaflet and consent form carefully, and bring it with you to your appointment. Please ask the doctor any questions
Vasectomy Services Patient Information Vasectomy Vasectomy Please read this information leaflet and consent form carefully, and bring it with you to your appointment. Please ask the doctor any questions
Breast reduction surgery
 Pan Manchester Patient Information Service July 2007 Plastic Surgery Department Issue 2 BSBR Pan Manchester Plastic Surgery Services Department of Plastic Surgery Acknowledgement: Written by Mr P Kumar,
Pan Manchester Patient Information Service July 2007 Plastic Surgery Department Issue 2 BSBR Pan Manchester Plastic Surgery Services Department of Plastic Surgery Acknowledgement: Written by Mr P Kumar,
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Transobturator tape sling Female sling system
 Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
The Children s Hospital Treatment for Hypospadias Information for parents
 The Children s Hospital Treatment for Hypospadias Information for parents What is hypospadias and what is the cause? Hypospadias is a congenital (since birth) abnormality of a boy s penis. Hypospadias
The Children s Hospital Treatment for Hypospadias Information for parents What is hypospadias and what is the cause? Hypospadias is a congenital (since birth) abnormality of a boy s penis. Hypospadias
Drinking fluids and how they affect your bladder
 Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS. Ask a member of
Drinking fluids and how they affect your bladder Contact us Patient Advice and Liaison Service (PALS) To make comments or raise concerns about the Trust s services, please contact PALS. Ask a member of
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Contents. Overview. Removing the womb (hysterectomy) Overview
 This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
This information is an extract from the booklet Understanding womb (endometrial) cancer. You may find the full booklet helpful. We can send you a free copy see page 9. Overview Contents Overview Removing
