CORNEAL NERVES IN REFRACTIVE SURGERY AND DRY EYE
|
|
|
- Rafe Ball
- 10 years ago
- Views:
Transcription
1 Department of Ophthalmology University of Helsinki Helsinki, Finland CORNEAL NERVES IN REFRACTIVE SURGERY AND DRY EYE ILPO S. TUISKU Academic Dissertation To be publicly discussed, with the permission of the Medical Faculty of the University of Helsinki, in Lecture Hall 2 of Biomedicum, Haartmaninkatu 8, Helsinki, on February 22 nd, 2008, at 12 noon. Helsinki
2 Supervised by: Professor Timo Tervo Department of Ophthalmology University of Helsinki FINLAND Reviewed by: Professor Hannu Uusitalo Department of Ophthalmology University of Tampere FINLAND and Professor Marja Liisa Vuori Department of Ophthalmology University of Turku FINLAND Opponent: Professor Friedrich Kruse Department of Ophthalmology University of Erlangen Nürnberg GERMANY Ilpo S. Tuisku ISBN (paperback) ISBN (PDF) Yliopistopaino Helsinki
3 3 To Johanna, Tom, and Matias
4 CONTENTS LIST OF ORIGINAL PUBLICATIONS 6 ABBREVIATIONS 7 ABSTRACT 9 INTRODUCTION 10 REVIEW OF THE LITERATURE Corneal structure Corneal innervation and sensitivity Neurosecretorial regulation of tearing Tear fluid cytokines Corneal wound healing Antigen presenting cells Excimer laser Photorefractive keratectomy PRK Nerve regeneration after PRK Corneal sensitivity after PRK Laser in situ keratomileusis LASIK Nerve regeneration after LASIK Corneal sensitivity after LASIK Dry eye Dry eye after refractive surgery Sjögren s syndrome Neurological manifestations in Sjögren s syndrome 31 AIMS OF THE STUDY 32 SUBJECTS AND METHODS Subjects PRK patients LASIK patients and controls Primary Sjögren s syndrome patients and controls 34 4
5 2. Methods Clinical examination Tear fluid analysis In vivo confocal microscopy IVCM Noncontact esthesiometry PRK LASIK Statistical analyses 41 RESULTS Tear fluid cytokines, haze, and nerve regeneration after PRK Tear fluid cytokines after PRK IVCM three months after PRK Correlations between IVCM data and cytokines Dry eye and corneal sensitivity after high myopic LASIK Subjective symptoms Objective dry eye tests Corneal sensitivity Corneal morphology and sensitivity in primary Sjögren s syndrome Subjective symptoms Objective dry eye tests Corneal sensitivity IVCM in primary Sjögren s syndrome 46 DISCUSSION Tear fluid cytokines and haze after PRK Nerve regeneration after PRK Corneal sensitivity after high myopic LASIK Corneal sensitivity in primary Sjögren s syndrome Corneal nerves in primary Sjögren s syndrome 53 SUMMARY AND CONCLUSIONS 57 ACKNOWLEDGMENTS 58 REFERENCES 60 ORIGINAL PUBLICATIONS 74 5
6 LIST OF ORIGINAL PUBLICATIONS This dissertation is based on the following original publications, which are referred to in the text by Roman numerals I IV: I Ilpo S. J. Tuominen, Timo M. T. Tervo, Anna Maija Teppo, Tuuli U. Valle, Carola Grönhagen Riska and Minna H. Vesaluoma. Human tear fluid PDGF BB, TNF and TGF 1 vs corneal haze and regeneration of corneal epithelium and subbbasal nerve plexus after PRK. Exp. Eye Res. 2001;72: II Ilpo S. Tuisku, Nina Lindbohm, Steven E. Wilson, Timo M. Tervo. Dry eye and corneal sensitivity after high myopic LASIK. J. Refract. Surg. 2007;23: III Ilpo S. J. Tuominen, Yrjö T. Konttinen, Minna H. Vesaluoma, Jukka A.O. Moilanen, Maaret Helintö, Timo M. T. Tervo. Corneal innervation and morphology in primary Sjögren s syndrome. Invest. Ophthalmol. Vis. Sci. 2003;44: IV Ilpo S. Tuisku, Yrjö T. Konttinen, Liisa M. Konttinen, Timo M. Tervo. Alterations in corneal sensitivity and nerve morphology in patients with primary Sjögren s syndrome. Submitted These publications have been reprinted with the kind permission of their copyright holders. In addition, some unpublished material is presented. 6
7 ABBREVIATIONS APC Antigen presenting cell Ar F Argon fluoride ARVO Association for Research in Vision and Ophthalmology BSCVA Best spectacle corrected visual acuity BM Basal membrane BUT Tear break up time CCK Cholecystokinin CGRP Calsitonin gene related peptide CMTF Confocal microscopy through focusing D Diopter DC Dendritic cell DLK Diffuse lamellar keratitis ECM Extracellular matrix EGF Epidermal growth factor Excimer Excited dimer Fas Fas (Apo 95) receptor Fas L Fas ligand FML Fluorometholone GAL Galanin HGF Hepatinocyte growth factor IGF Insulin like growth factor IL Interleukin IVCM In vivo confocal microscopy kda kilodalton KGF Keratinocyte growth factor LASIK Laser assisted in situ keratomileusis LINE LASIK induced neurotrophic epitheliopathy M ENK Methionine enkephalin NCE Noncontact esthesiometer NFB Nerve fiber bundle NGF Nerve growth factor NPY Neuropeptide Y OSDI Ocular surface disease index PACAP Pituitary adenylate cyclase activating polypeptide PDGF Platelet derived growth factor PRK Photorefractive keratectomy pss Primary Sjögren s syndrome SP Substance P SS Sjögren s syndrome sss Secondary Sjögren s syndrome TGF Transforming growth factor TNF Tumor necrosis factor Trk Tyrosine kinase TSCM Tandem scanning confocal microscopy UCVA Uncorrected visual acuity VAS Visual analog scale VIP Vasoactive intestinal polypeptide 7
8 8
9 ABSTRACT This study aimed to investigate the morphology and function of corneal sensory nerves in 1) patients after corneal refractive surgery and 2) patients with dry eye due to Sjögren s syndrome. A third aim was to explore the possible correlation between cytokines detected in tears and development of post PRK subepithelial haze. The main methods used were tear fluid ELISA analysis, corneal in vivo confocal microscopy, and noncontact esthesiometry. The results revealed that after PRK a positive correlation exists between the regeneration of subbasal nerves and the thickness of regenerated epithelium. Pre or postoperative levels of the tear fluid cytokines TGF 1, TNF, or PDGF BB did not correlate with the development of corneal haze objectively estimated by in vivo confocal microscopy 3 months after PRK. After high myopic LASIK, a discrepancy between subjective dry eye symptoms and objective signs of dry eye was observed. The majority of patients reported ongoing dry eye symptoms even 5 years after LASIK, although no objective clinical signs of dry eye were apparent. In addition, no difference in corneal sensitivity was observed between these patients and controls. Primary Sjögren s syndrome patients presented with corneal hypersensitivity, although their corneal subbasal nerve density was normal. However, alterations in corneal nerve morphology (nerve sprouting and thickened stromal nerves) and an increased number of antigen presenting cells among subbasal nerves were observed, implicating the presence of an ongoing inflammation. Based on these results, the relationship between nerve regeneration and epithelial thickness 3 months after PRK appears to reflect the trophic effect of corneal nerves on epithelium. In addition, measurement of tear fluid cytokines may not be suitable for screening patients for risk of scar (haze) formation after PRK. Presumably, at least part of the symptoms of LASIKassociated dry eye are derived from aberrantly regenerated and abnormally functioning corneal nerves. Thus, they may represent a form of corneal neuropathy or phantom pain rather than conventional dry eye. Corneal nerve alterations and inflammatory findings in Sjögren s syndrome offer an explanation for the corneal hypersensitivity or even chronic pain or hyperalgesia often observed in these patients. In severe cases of disabling chronic pain in patients with dry eye or after LASIK, when conventional therapeutic possibilities fail to offer relief, consultation of a physician specialized in pain treatment is recommended. 9
10 INTRODUCTION The cornea is an avascular and delicate optically transparent tissue. Its transparency is maintained by metabolically active pump systems located mainly in the endothelium. Corneal sensory nerves also have a crucial role in maintaining corneal architecture and transparency. The cornea is one of the most densely innervated peripheral tissues in humans. Corneal nerves interfere with epithelial mitotic activity and proliferation, and presumably also with the regulation of keratocyte function. Secretion of tear fluid is also regulated by the corneal nerves forming the afferent loop of the cornea lacrimal gland reflex arc. Several systemic and corneal disorders as well as ocular surgery may damage the corneal nerves and impair their function. Consequently, the regulation of epithelial cell and keratocyte metabolism and also tear formation and corneal sensitivity are disturbed until innervation is restored. Corneal refractive surgery (PRK and LASIK) severs corneal sensory nerves, impairing corneal sensitivity and function. Corneal nerve regeneration begins shortly, but the original fine nerve architecture may never be completely restored. Patients experience varying degrees of dry eye symptoms for a 1 to 6 month period following refractive surgery. Occasionally, extensive dry eye symptoms or even ocular pain may persist for years, with or without dry eye signs. On the other hand, patients may have clinical signs compatible with dry eye, but present with minimal or no symptoms. Dry eye is a common external eye disease that arises from a wide variety of etiologies. Sjögren s syndrome (SS) is a systemic autoinflammatory disorder of unknown etiology, and dry eye is one of its major manifestations. Primary Sjögren s syndrome (pss) occurs without any association with other rheumatological diseases. Consequently, it represents a relatively homogeneous group of patients. Patients presenting with symptoms compatible with dry eye, but with minimal or no dry eye signs found on ocular examination are relatively frequently seen after refractive surgery. The goal of this thesis was to explore the reasons behind this clinical discrepancy by investigating corneal nerves and sensitivity in patients after refractive surgery and in patients with SS. 10
11 REVIEW OF THE LITERATURE 1. Corneal structure The cornea is an avascular tissue accounting for most of the refractive power of the human eye. Due to its transparency, it allows light to enter the eye and to be projected to the retina. According to a recent meta analysis, the average thickness of the central cornea is 534 µm centrally, although values are affected by measurement techniques: for slit lamp based optical pachymetry, the mean central corneal thickness is 530 m, and for ultrasonic pachymetry 544 m (Doughty and Zaman 2000). The normal cornea is thinnest in the center and thickest peripherally, measuring approximately 650 m. Anatomically, the cornea can be divided into five sublayers: 1. epithelium, 2. Bowman s layer, 3. stroma or substantia propria, 4. Descemet s membrane, and 5. endothelium. The epithelium consists of 5 7 layers of nonkeratinized squamous epithelial cells, measuring m in thickness. Three morphological cell types are present in human corneal epithelium: superficial epithelial cells, intermediate wing cells, and the innermost basal epithelial cells (Ehlers 1970). The corneal epithelium is a dynamic tissue in which cells are constantly renewed and lost; nevertheless, the total mass is kept steady by mechanisms not yet fully elucidated. A strong body of evidence suggests that corneal epithelial cells arise from limbal stem cells (reviewed by Tseng 1989 and Dua et al. 2000). Once inside the cornea, cells slowly move towards the apex in a centripetal fashion; this is supported by the XYZ theory by Thoft and Friend (1983) as well as by various clinical observations (Bron 1973, Kaye 1980, Lemp and Mathers 1989). Evidence for the XYZ theory has also been gained from in vivo confocal microscopy studies (Auran et al. 1995) and experimental in vivo studies on transgenic mice (Nagasaki and Zhao 2003). Superficial epithelial cells, which form a barrier against foreign substances, are connected to each other by tight junctions and desmosomes. They have numerous microvilli and microplicae on their surfaces that increase the adherence of tear fluid mucins. The life span of surface epithelial cells is only a few days, after which they are shed in tear fluid. The intermediate wing cells form 2 3 layers beneath the surface epithelium and have wing like extensions. The basal epithelial cells form a monolayer of cells anchored tightly to the basement membrane with the aid of hemidesmosomes and different anchoring fibrils (Gipson et al. 1989). Basal epithelial cells have limited capacity to divide before terminal differentiation, thus being partly 11
12 responsible for the excellent capability of the epithelium to regenerate (Hanna and O Brien 1960, Kruse et al. 1990, reviewed by Li et al. 2007). Bowman s layer was first described by Sir William Bowman at the London Ophthalmic Hospital (Moorfields) in Bowman s layer separates the epithelium from the stroma, acting as an anterior limiting membrane and giving tensile strength to the cornea. In Bowman s layer, individual collagen fibrils are interwoven densely to form a felt like sheet. The thickness of this acellular layer is 8 12 m (Komai and Ushiki 1991). The stroma, or substantia propria, consists of keratocytes, extracellular matrix, and nerve fibers. The stroma constitutes the largest portion of the cornea; its thickness is approximately 470 m. Three hundred to five hundred collagen lamellae running from limbus to limbus are oriented at precise angles with respect to adjacent lamellae, contributing to corneal transparency and strength (Komai and Ushiki 1991, reviewed by Ihanamäki et al. 2004). Stromal collagen lamellae (consisting of types I, III, V, XII, and XIII) are surrounded by several proteoglycans responsible for proper spacing of collagen and stromal hydration (reviewed by Ihanamäki et al. 2004). Descemet s membrane dividing the stroma from the endothelium acts as a basement membrane for the endothelium. The thickness of Descemet s membrane gradually increases from birth (3 µm) to adulthood (8 10 m) (Johnson et al. 1982). The endothelium is a monolayer of 5 mthick cells and is the innermost layer of the cornea, functioning in fluid pumping and regulation of corneal hydration. Endothelial cells are not known to be capable of dividing, thus lacking mitotic activity (Nishida 2005) Figure 1. Schematic drawing of cornea: 1) epithelium, 2) subbasal nerve plexus and Bowman s layer, 3) stromal nerves, 4) stroma, and 5) Descemet s membrane and endothelium. 12
13 2. Corneal innervation and sensitivity Corneal afferent sensory neurons are derived from the Gasserian ganglion and enter the eye ball via long ciliary nerves, which are branches of the nasociliary portion of the ophthalmic division of the trigeminal nerve. In some cases, the inferior cornea receives additional innervation from the maxillary branch of the trigeminal nerve (Zander and Weddel 1951, Ruskell 1974, Rozsa and Beuerman 1982). Long ciliary nerves are myelinated until they penetrate the limbus and form nerve bundles surrounded only by the Schwann s cells (Zander and Weddel 1951). The absence of myelin on central corneal axons is essential for maintaining corneal transparency. In the human cornea, thick nerve trunks move from the periphery below the anterior third of the stroma due to organization of collagen lamellae (Muller et al. 2001, Radner and Mallinger 2002). Nerve fibers run forward in a radial fashion towards the center of the cornea and penetrate Bowman s layer, then turning abruptly and continuing parallelly to the corneal surface, simultaneously losing their Schwann s cell ensheathment (Schimmelpfennig 1982, Muller et al. 1996). Nerve fibers form a network by branching both vertically and horizontally between Bowman s layer and basal epithelial cells; this network is called the subbasal nerve plexus (Muller et al. 1997). Nerve terminals are then sent between epithelial cells (Rozsa and Beuerman 1982), electromicroscopic studies have shown evidence that nerve terminals invaginate both basal epithelial cells and wing cells (Muller et al. 1996). Beaded nerve fibers, with a diameter of approximately 2 µm, contain many mitochondria and glycogen, indicating active metabolism, and are thought to also contain neuropeptides (Muller et al. 1996). Most of the corneal neurons are classified as C type, with a conducting velocity less than 2 m/s, and the rest are myelinated A type axons, typically with conduction velocities between 2 and 15 m/s (Belmonte and Tervo 2005) Figure 2. After the stromal nerves have penetrated Bowman s layer, they run parallel to the corneal surface between the basal epithelium and Bowman s layer, forming a neural network called the subbasal plexus. 1) Wing cells 2) basal epithelial cells, and 3) Bowman s layer. 13
14 Several neural transmitters and neuropeptides have been demonstrated in the corneal nerves. Substance P (SP) (Tervo et al. 1982), calcitonin gene related peptide (CGRP) (Stone et al. 1986), and galanin (GAL) (Jones and Marfurt 1998) are of sensory origin. Catecholamines (Toivanen et al. 1987) and neuropeptide Y (NPY) (Jones and Marfurt 1998) are of sympathetic origin, and galanin (GAL) (Jones and Marfurt 1998), cholecystokinin (CCK) (Stone et al. 1984), vasoactive intestinal peptide (VIP) (Jones and Marfurt 1998), and methionine enkephalin (M ENK) (Jones and Marfurt 1998) are of parasympathetic origin. Development of modern corneal imaging techniques, such as in vivo confocal microscopy (IVCM), has enabled corneal nerves in living corneas to be analyzed. IVCM allows visualization of the subbasal nerve plexus, and is also used in imaging normal corneas (Oliveira Soto and Efron 2001, Grupcheva et al and Patel et al. 2005), patients after PRK (Heinz et al. 1996, Kauffmann et al. 1996, Linna and Tervo 1997, Bohnke et al. 1998, Frueh et al. 1998, Moilanen et al. 2003, Erie et al. 2005b), patients after LASIK (Kauffmann et al. 1996, Linna et al. 2000, Lee et al. 2002, Calvillo et al. 2004, Bragheeth and Dua 2005, Erie et al. 2005b), patients with herpetic keratitis (Rosenberg et al. 2002), patients with keratoconus (Patel and McGhee 2006), patients with diabetes mellitus (Rosenberg et al. 2000b), and patients with various corneal dystrophies, e.g. epithelial basement membrane dystrophy (Rosenberg et al 2000a), lattice dystrophy type II (Rosenberg et al. 2001), cornea plana (Vesaluoma et al. 2000), and Fuchs dystrophy (Mustonen et al. 1998). Patel et al. (2005) have developed a novel technique to elucidate the overall distribution of subbasal nerves in the human cornea by laser scanning in vivo confocal microscopy. Multiple images are obtained from several locations in the cornea, and overlapping images are later reconstructed to confluent montages. With the aid of this novel technique, they observed that subbasal nerves were settled in a whorl like pattern, similar to that seen in the epithelium in corneal verticillata. On the basis of their observations, they hypothesized that epithelial cells and nerves would migrate centripetally in tandem (Patel et al. 2005). Normal corneal sensitivity is higher in the center of the cornea than at the periphery (Millodot and Larson 1969). Accordingly, the central cornea is 5 6 times more densely innervated than the peripheral cornea (Muller et al. 1997). The cornea is one of the most densely innervated peripheral tissues in humans; the nerve density is estimated to be times higher than in, for example, the human finger (Rozsa and Beurman 1982, reviewed by Muller et al. 2003). Based on electrophysiological studies, different functional types of sensory nerve fibers exist in the cornea. The majority of corneal nerves are polymodal nociceptors (70%), which are activated by near noxious mechanical energy, heat, chemical irritants, and a large variety of endogenous chemical mediators. Mechano nociceptors, accounting for 15 20% of corneal peripheral axons, respond only to coarse mechanical forces in the order of magnitude close to that required to damage corneal epithelial cells. Cold sensitive thermal axons accounting for the 14
15 remaining 10 15% of corneal peripheral axons, respond by increasing their firing rate when the corneal temperature falls below normal levels (reviewed by Belmonte et al. 2004, Belmonte and Tervo 2005). Several corneal diseases, corneal dystrophies, and ocular surgery may cause a decline in corneal sensitivity (reviewed by Muller et al. 2003). In addition, corneal sensitivity has been reported to diminish with increasing age (Millodot 1977), although the density and orientation of the subbasal nerves seem to be unaffected (Erie et al. 2005a). Corneal sensitivity can be tested in the clinical setting by gently touching the ocular surface with a wisp of cotton and observing the blink reflex or by comparing the subjective sensation with that evoked from the other eye. This information is easily obtained in clinical settings. However, the results are not quantified and represent only an approximation of the functional status of corneal nerves. The Cochet Bonnet esthesiometer represents a more quantitative approach and uses a calibrated nylon hair of variable length. It measures mainly coarse mechanical sensation and cannot discriminate between mechanical, thermal and chemical sensations. Moreover, it has a limited ability to accurately measure corneal sensitivity at low stimulus thresholds compared with modern noncontact gas esthesiometers (Murphy et al. 1998). The noncontact gas esthesiometer uses an air jet of adjustable flow and temperature that may contain CO 2 in a variable concentration to reduce local ph. This allows mechanical, thermal, or chemical stimulation of a specific limited area of the cornea (Belmonte et al. 1999). The noncontact gas esthesiometer is more accurate and has better repeatability than the Cochet Bonnet esthesiometer (Murphy et al. 1998). 3. Neurosecretorial regulation of tearing Main lacrimal glands are innervated by parasympathetic and sympathetic nerves (Botelho et al. 1966, Sibony et al. 1988). In addition, scarce sensory nerves have been identified in lacrimal glands (Botelho et al. 1966). Nerves are located in close proximity to acinar, ductal, and myoepithelial cells as well as to blood vessels (Botelho et al. 1966, Sibony et al. 1988). Stimulation of the lacrimal gland and secretion occur via the cornea trigeminal nerve brainstem facial nerve lacrimal gland reflex arc. Afferent sensory nerves of the cornea and conjunctiva are activated by stimuli to the ocular surface. Efferent parasympathetic and sympathetic nerves are then activated to stimulate secretion from acinary and tubular cells (Botelho 1964). Neurotransmitters and neuropeptides released by lacrimal gland nerves include acetylcholine (Botelho 1964), vasoactive intestinal peptide (VIP) (Uddman et al. 1980), neuropeptide Y (NPY) (Tsukahara and Jacobowitz 1987), substance P (Nikkinen et al. 1984), and calcitonin gene related peptide (CGRP) (Tsukahara and Jacobowitz 1987). 15
16 While regulation of tearing is under tight neural control, a loss of innervation in the inflamed lacrimal gland has been suggested to explain associated decreased secretory function in SS dry eye (Hakala and Niemelä 2000). Accordingly, lymphocytic infiltration of lacrimal glands was associated with decreased reflex tearing (Schirmer s test II with nasal stimulation) in dry eye (Tsubota et al. 1996). However, several studies have shown that viable nerves do exist in nonfibrotic areas of lacrimal glands, while they are absent in fibrotic areas (Zoukhri et al. 1998a and Zoukhri et al. 1998b). Hence, the lack of lacrimal gland secretion in SS cannot be explained by a loss of neural support. Zoukhri and Kublin (2001) found that remaining nerves were unable to release their neurotransmitters and this also correlated with the lack of lacrimal gland protein secretion. In conclusion, autonomic nerves in the lacrimal gland are not lost in SS dry eye, but the inability to release their neurotransmitters seems to play an important role in impaired lacrimal gland secretion. 4. Tear fluid cytokines Corneal cells are known to express different cytokines and/or their receptors potentially modulating wound healing (Wilson et al. 1992, 1994a, 1994b, 1996a, Li and Tseng 1996). The transforming growth factor (TGF) family, consisting of TGF β1, TGF β2, and TGF β3, are polypeptides of approximately 25 kda (Kokawa et al. 1996). TGF is generally thought to inhibit epithelial, endothelial, and leukocyte cell growth and to stimulate proliferation of fibroblasts (Song et al. 2002). TGF β2 seems to be the major isoform present in all types of corneal cells (Nishida et al. 1995), but TGF β1 has also been detected in small amounts in all corneal layers (Wilson et al. 1992, Nishida et al. 1995). In addition, TGF β1 and 2 have been shown to be present in human tear fluid (Gupta et al. 1996, Kokawa et al. 1996, Vesaluoma et al. 1997a). TGF β1 and 2 are produced and TGF β1 secreted by the human lacrimal gland, suggesting that the lacrimal gland may be one source of TGF β in human tear fluid (Yoshino et al. 1996). TGF β 1 is involved in the regulation of keratocyte activation, myofibroblast transformation, proliferation, chemotaxis, and wound healing after refractive surgery, and it is strongly associated with excessive scarring (Jester et al. 1996, 1999, Andresen et al. 1997, Myers et al. 1997, Andresen and Ehlers 1998, Moller Pedersen et al. 1998b, Jester et al. 2003). Platelet derived growth factor (PDGF) is a cysteine knot containing dimer of 35 kda composed of an A and B chain. It exists as isomers PDGF AA, PDGF AB, and PDGF BB (reviewed by Jones and Kazlauskas 2001). PDGF BB is produced by corneal epithelial cells and is bound at high levels in the epithelial basement membrane (reviewed by Wilson et al. 2001). PDGF receptors are found in corneal fibroblasts (Li and Tseng 1996). PDGF BB has also been shown 16
17 to have mitogenic, chemotactic, and migratory effects on corneal fibroblasts in vitro (Hoppenreijs et al. 1993, Andresen et al. 1997, Andresen and Ehlers 1998, Kamiyama et al. 1998, Kim et al. 1999, Jester et al. 2002). Tumor necrosis factor α (TNF α), on the other hand, is an inducer of apoptosis, which is supposed to play an important role in the first steps of corneal wound healing after PRK (Wilson et al. 1996a, 1996b, Helena et al. 1998). TGF β1, TNF α, and PDGF BB are present in low concentrations in human tear fluid, and PRK induces an increased release of TGF β1, TNFα, and PDGF BB during the early days of wound healing (Gupta et al. 1996, Vesaluoma et al. 1997a, 1997b, 1997c). 5. Corneal wound healing Corneal wound healing is a complex physiologic sequence of events that contributes to reestablishment of normal function and clarity of the cornea. Interindividual variations in the wound healing process after all keratorefractive procedures are the major determinants of surgical outcome. The wound healing process plays a critical role in overcorrection, undercorrection, regression, and other complications as well as in corneal haze and refractive instability. Major challenges of corneal refractive surgery are to control the wound healing process more precisely and to promote more tissue regeneration than tissue fibrosis (Stramer et al. 2003, reviewed by Fini and Stramer 2005). Interaction between the corneal epithelium and stroma is a well known phenomenon and a critical step in corneal wound healing. Removal of the epithelium induces disturbances in ATP content of anterior keratocytes (Herrman and Lebeau 1962), and the anterior stroma beneath the epithelial wound becomes acellular within the following 24 h (Nakayasu 1988, Campos et al. 1994). Initially, the keratocyte loss was thought to be the result of mechanical trauma or osmotic changes (Dohlman et al. 1968). However, more recently, the loss of keratocytes following epithelial removal has been shown to be mediated primarily by apoptosis (Wilson et al. 1996a, 1996b, Gao et al. 1997, Helena et al. 1998, Kim et al. 1999). Among others, interleukin 1 (IL 1 ) and TNF are released from the injured corneal epithelium and induce autocrine suicide in keratocytes by activating the Fas / Fas ligand system (Wilson et al. 1996b, Mohan et al. 1997, reviewed by Wilson et al. 2001). After stromal keratocyte loss due to apoptosis, stromal cells adjacent to the wound area become activated and proliferate. The activated keratocytes migrate to the wound area (Hanna et al. 1989, Del Pero et al. 1990, Zieske et al. 2001), and five days after wounding, these migrated 17
18 keratocytes in the wound area undergo subsequent rounds of cell division and repopulate the wound area (Zieske et al. 2001). Table 1. Characteristic differences in activated keratocytes. Fibroblasts Myofibroblasts / Altered keratocytes Presence in epithelial abrasions + Presence in wounds penetrating Bowman s layer + + Association with wound fibrosis + Biomechanical activity less active active Expression of smooth muscle actin + Expression of collagens, fibronectin, and other matrix proteins + Expression of MMPs upregulated downregulated The extent of the initial wound, especially whether or not the epithelial basement membrane is disrupted, results in different phenotypes of activated keratocytes: fibroblasts or myofibroblasts/ altered keratocytes (Table 1). Wounds that penetrate the basement membrane, such as keratectomy, lead to the presence of myofibroblasts in the wound area, while after pure epithelial abrasions with an intact basement membrane, myofibroblast are not present (Moller Pedersen et al. 1998b, Zieske et al. 2001). Fibroblasts are less biomechanically active, synthesize matrix metalloproteinases (West Mays et al. 1997, Bargagna Mohan et al. 1999), and are associated with corneal ulceration (Riley et al. 1995, Hargrave et al. 2002). Myofibroblasts, by contrast, are associated with wound fibrosis, synthesize collagen, fibronectin, and other matrix proteins (Ohji et al. 1993, Jester et al. 1996), and have downregulated matrix metalloproteinase production (Girard et al. 1991, Fini et al. 1995, West Mays et al. 1999). Myofibroblasts express smooth muscle actin and have well developed focal adhesions, while fibroblasts do not express smooth muscle actin and have poor focal adhesions (Jester et al. 1995, 1996, Petridou et al. 2000). Myofibroblasts have strong biomechanical involvement in matrix organization and wound contraction. Excess proliferation of stromal fibroblasts and myofibroblasts results in stromal hyperplasia and clinical haze, affecting optical transparency of the cornea (Moller Pedersen et al. 1998a, 1998b). TGF seems to be the most essential cytokine in orchestrating the transformation process of myofibroblasts (Jester et al. 1997, 2003). However, in the cornea, the synergistic function of 18
19 TGF and PDGF via integrin signaling pathways is needed for myofibroblast transformation (Jester et al. 2002). The epithelial healing process requires epithelial cell proliferation, migration, and differentiation. The combination of cytokines and growth factors present in corneal cells and tear fluid regulates the early epithelial wound healing cascades. Paracrine cytokine trafficking in the human cornea presents a unique stromal / epithelial interaction (Wilson et al. 1994a). Cytokines responsible for epithelial proliferation are keratinocyte growth factor (KGF), hepatocyte growth factor (HGF), and epidermal growth factor (EGF) (Wilson et al. 1993, 1994b, 1994c, Tervo et al. 1997). Epithelial proliferation is further stimulated by increased levels of PDGF BB (Li and Tseng 1997). Elevated production of KGF and HGF by keratocytes is present up to 7 days after corneal injury (Wilson et al. 1999a). In addition, increased reflex tear fluid production results in higher availability of HGF (Tervo et al. 1997), PDGF BB (Vesaluoma et al. 1997c), and EGF (van Setten 1990). Enhanced expression of mrna for EGF and HGF is present in the lacrimal gland after wounding, contributing to greater availability in tear fluid (Wilson et al. 1999b). In addition, mrnas for EGF and HGF receptors are concurrently upregulated in the epithelium and keratocytes (Wilson et al. 1999a). Migration of epithelial cells at the wound periphery is induced by HGF (Li and Tseng 1997) and EGF (Wilson et al. 1994c) on a provisional fibronectin matrix that accumulates around the wound (Maldonado and Furcht 1995). Fibronectin is not present in the normal corneal epithelial basement membrane, but 8 h after wound healing it is detected in the epithelium (Fujikawa et al. 1984). Endogenously produced fibronectin by corneal epithelial cells promotes cell adhesion (Ohji et al. 1993). Elevated levels of fibronectin are also found in human tear fluid after PRK, promoting epithelial cell migration and attachment (Virtanen et al. 1995). Once epithelial confluence is achieved, the epithelial cells are triggered to proliferate and sequentially differentiate to form a normal corneal stratified epithelium (Wilson et al. 1994c). Normal composition of the basement membrane is achieved by restoring collagens and laminins, which occurs when the fibronectin matrix disappears (reviewed by Suzuki et al. 2003). 19
20 6. Antigen presenting cells In 1867, Engelman noted dendritic or polygonal cells in the corneal epithelium. One year later, a medical student Paul Langerhans observed dendritic cells in the skin epidermis. Similarities between corneal dendritic cells and Langerhans cells of the skin have since been proposed. The cornea is an immune privileged tissue and has long been considered to lack antigen presenting cells (APC) (Gillette et al. 1982). Today, APCs are known to play a critical role in corneal immunology in both health and disease (Hamrah et al. 2002, Rosenberg et al. 2002, Hamrah et al. 2003a, 2003b, Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). Two distinct phenotypic populations of APCs in the normal cornea have been reported. Immature APCs, which do not express MHC class II antigen on their surface, tend to be located in the central corneal epithelium. Immature APCs have a large cell body with only a few short processes, if any (Hamrah et al. 2003a). These APCs are able to capture the antigen, but are unable to present to lymphocytes. Mature APCs, by contrast, have a slender nucleated cell body from which mazes of long membrane processes extend that resemble dendrites of nerve cells. Mature APCs, expressing MHC class II antigen, are found in the peripheral corneal and limbal epithelium (Hamrah et al. 2002, 2003a, 2003b). The evolution of corneal in vivo imaging techniques has provided new data regarding human corneal APCs in living tissue. The density of APCs declines from the limbus to the center of healthy corneas (Hamrah et al. 2002, Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). In the corneal limbal epithelium, dendritic cells are found in virtually every healthy subject, while only 20 30% of healthy controls show APCs in the central cornea (Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). More often APCs are present in the peripheral cornea, where they show signs of a mature phenotype with long slender dendritic processes, whereas immature APCs without dendrites typically predominate in the central cornea (Zhivov et al. 2005). Most of the APCs are located at the level of subbasal cells or among the subbasal nerve plexus (Zhivov et al. 2005). 7. Excimer laser The excimer laser used to sculpt the cornea has been the single most important advancement in the field of refractive surgery. Excimer laser keratectomy involves remodeling the corneal stroma by tissue removal. The advantage of the excimer laser is its ability to remove tissue with a microscopic precision unattainable with other procedures. 20
21 Excited dimers are molecules with bound upper states and weakly bound ground states. The reaction of an excited rare gas atom with a halogen atom produces excited dimers that emit ultraviolet radiation when decaying from the bound upper state to the rapidly dissociating ground state. Trokel et al. (1983) demonstrated that far UV laser emissions (between 150 and 200 nm) can precisely remove corneal tissue without apparent thermal trauma to the adjacent tissue. According to several experimental studies, the 193 nm UV light from the argon fluoride laser was established as the optimal wavelength with the least corneal transmission. The highenergy UV photons emitted by the argon fluoride laser caused less adjacent thermal trauma and created smoother ablation than longer wavelength lasers (Trokel et al. 1983). 8. Photorefractive keratectomy PRK Photorefractive keratectomy (PRK) is based on the use of excimer laser for accurate removal and resculpturing of corneal tissue in order to change the corneal curvature and refractive power of the cornea. Before excimer laser photoablation, the epithelium must be removed either mechanically with a blunt spatula or brush, or by excimer laser (Trokel et al. 1983, Seiler and Wollensak 1991, Palllikaris et al. 1994, Gimbel et al. 1995). Figure 3. Myopic PRK. After the epithelium is removed either mechanically or by excimer laser, Bowman s layer, subbasal nerves, and the anterior stroma, including stromal nerves, are photoablated by excimer laser. The depth of ablation depends on the magnitude of dioptric correction. Accordingly, stromal nerves are destroyed to a variable extent depending on ablation depth. Clinical studies have shown relatively good safety, predictability, and refractive results in low to moderate myopia (Seiler and Wollensak 1991, Gartry et al. 1992, McDonald et al. 1999). However, deeper ablation depths and higher corrections produce a greater incidence of postoperative haze and regression and less predictable refractive results (Seiler et al. 1992, Shah et al. 1998). 21
22 8.1 Nerve regeneration after PRK PRK photoablates Bowman s layer, subbasal nerves, and anterior stromal nerves in the ablation zone, leaving sharply cut nerve trunks at the base and margin of the wound (Tervo et al. 1994, Trabucchi et al. 1994). The degree of stromal nerve destruction depends on the required ablation depth. Considerable data exists on corneal nerve regeneration after PRK, including both experimental and human studies done by in vivo confocal microscopy (IVCM). Experimental studies using histochemical methods have shown that nerve regeneration after PRK is a biphasic process (Rozsa et al. 1983, Beuerman and Rozsa 1984, Tervo et al. 1994). In the first phase, the reinnervated subbasal plexus is formed by fine neurites that originate from the cut peripheral nerve plexus and extend centrally alongside the migrating epithelial cells (Rozsa et al. 1983, Beuerman and Rozsa 1984, Tervo et al. 1994). Neurofilament immunoreactivity can be observed as early as 24 h after the procedure (Trabucchi et al. 1994). The second phase of nerve regeneration is initiated by the degeneration of wound oriented neurites and the concomitant appearance of a second generation of stromal neurites that ultimately re establish a new subbasal plexus (Rozsa et al. 1983, Beuerman and Rozsa 1984). The second phase neurites originate from the transected stumps of stromal nerves at the wound base and the wound margin (Rosza et al. 1983). The regenerating stromal nerves reach the epithelium and contribute to the formation of a new subbasal plexus 6 months after PRK (Tervo et al. 1994, Trabucchi et al. 1994). Trabucchi et al. (1994) observed a regenerated nerve plexus at 1 4 months after surgery that actually appeared thicker than normal. Ishikawa et al. (1994) noted a transient increase in intraepithelial nerves after PRK, the density returning to normal levels by about 7 months after surgery. Normal density of intraepithelial nerve endings was reached 3 months after PRK (Tervo et al. 1994). However, the morphological alterations in the epithelial nerves persisted for as long as 12 months after the procedure, with stromal nerve alterations also being present (Tervo et al. 1994). In vivo confocal microscopy (IVCM) enables imaging of the living cornea, allowing observation of the regeneration of subbasal nerves after PRK. The first regenerating subbasal nerves have been seen as early as one week after PRK (Linna and Tervo 1997). At one month after PRK, subbasal nerves were observed in only 1 of 18 eyes (Frueh et al. 1998). Partial or in some cases total recovery of subbasal nerves has been reported to occur at 8 12 months after PRK (Corbett et al. 1996, Kauffman et al. 1996). However, even at 5 years after PRK, some corneas do not achieve a normal pattern of subbasal nerve morphology, although the mean subbasal nerve density does not differ from that of normal controls (Moilanen et al. 2003). In a recent prospective longitudinal study, preoperative levels of nerve density were achieved 2 years after myopic PRK, and the levels remained stable during the 5 year follow up (Erie et al. 2005b). 22
23 8.2 Corneal sensitivity after PRK The early postoperative decline in corneal sensitivity is followed by a relatively fast recovery of sensation in the following 3 months, when preoperative levels also in the central cornea are achieved (Perez Santonja et al. 1999, Matsui et al. 2001, Kumano et al. 2003, Lee et al. 2005). Interestingly, in some studies, no decrease in corneal sensitivity after PRK was observed during the follow up (Kumano et al. 2003), while in another study a time period of up to 12 months after PRK was needed to achieve normal sensitivity levels (Nejima et al. 2005). PRK patients are characterized by higher tear fluid NGF levels 3 months postoperatively. Higher NGF levels correlated with faster recovery of corneal sensitivity (Lee et al. 2005). Loss of sensitivity after PRK seems to be less severe than after LASIK, and the overall rate of recovery of sensitivity to preoperative levels is faster after PRK than LASIK (Perez Santonja et al. 1999, Matsui et al. 2001, Kumano et al. 2003, Lee et al. 2005, Nejima et al. 2005). 9. Laser in situ keratomileusis LASIK Ionnis Pallikaris was the first to describe laser in situ keratomileusis (LASIK) in 1990 (Pallikaris et al. 1990). A hinged corneal flap, consisting of the epithelium, the subbasal nerve plexus, and the anterior stroma, is created with a microkeratome. After the flap is lifted, corneal sculpturing is performed on the exposed stromal bed, after which the corneal flap is replaced. The flap adheres spontaneously to the stromal bed, with no suturing required. Figure 4. Myopic LASIK. A hinged flap, consisting of the epithelium, Bowman s layer, subbasal nerves, and the anterior stroma, is created using a microkeratome. After the flap is lifted, the corneal stroma is sculptured using excimer laser. 23
24 LASIK is nowadays the most commonly performed procedure in refractive surgery and the first choice for the correction of refractive errors in the majority of patients (Duffey and Leaming 2005). It is a relatively safe, predictable, and effective method for correcting low to moderately high (up to 15 D) myopia, offering many advantages over other existing procedures such as fast and painless recovery of vision, less regression, and less subepithelial haze (McDonald et al. 2001, Solomon et al. 2002, Sugar et al. 2002). However, patients subjected to LASIK surgery often report dry eye symptoms postoperatively, and tear fluid abnormalities are frequently described (Battat et al. 2001, Hovanesian et al. 2001, Toda et al. 2001, Albietz et al. 2004a, De Paiva et al 2006, Shoja and Besharati 2007). These symptoms are the most common adverse effects of LASIK, causing frustration for both patients and surgeons alike (Sugar et al. 2002). LASIK associated dry eye is believed to be attributable to the severing of the afferent corneal nerves during the flap formation. Subbasal nerve bundles and superficial stromal nerve bundles in the flap interface are cut by the microkeratome, with only nerves entering the flap through the hinge region being spared. Subsequent sculpturing of corneal stroma using excimer laser severs stromal nerve fiber bundles (Linna et al. 1998, 2000, Lee et al. 2002, Brageeth and Dua 2005, Erie et al. 2005b). 9.1 Nerve regeneration after LASIK The regeneration of corneal nerves after LASIK has been investigated in experimental models (Latvala et al. 1996, Linna et al. 1998, Fukiage et al. 2007, reviewed by Tervo and Moilanen 2003). Thin regenerating nerve fibers form connections with neighboring stromal nerve fibers and penetrate the most anterior acellular stromal layer to send subbasal nerve fibers to form the nerve terminals between epithelial cells. Regeneration of anterior stromal, subbasal, and epithelial nerve fibers occurs approximately 3 months after LASIK, while deep stromal nerves may show abnormal morphology even 5 months after the procedure (Latvala et al. 1996, Linna et al. 1998). Topically administered neurotrophic factor pituitary adenylate cyclase activating polypeptide (PACAP) has accelerated neural regeneration after LASIK in an experimental model (Fukiage et al. 2007). Accordingly, topical neurotrophic factors PACAP and NGF seem to enhance the recovery of sensitivity after LASIK (Joo et al. 2004, Fukiage et al. 2007). However, lower tear fluid NGF levels after LASIK compared with PRK in human have been accompanied by slower recovery of sensation (Lee et al. 2005). In vivo confocal microscopy studies have enabled imaging of the living human cornea in four dimensions (x, y, z, and t [time]) and have produced abundant information on regeneration and morphological changes in corneal nerves during the post LASIK healing process (Kauffmann et al. 1996, Slowik et al. 1996, Linna et al. 2000, Lee et al. 2002, Perez Gomez and Efron 2003, Avunduk et al. 2004, Calvillo et al. 2004, Bragheeth and Dua 2005, Erie et al. 2005b). 24
25 Degeneration of cut subbasal nerves manifests during approximately one week after surgery, at which time subbasal nerve density decreases by 90% (Linna et al. 2000, Lee et al. 2002, Calvillo 2004, Erie et al. 2005b). Thereafter, a slow regenerative process occurs and regenerating nerve fibers form connections with neighboring nerve fibers. Prospective studies have shown that during the first year after LASIK, subbasal nerve fiber bundles gradually regenerate, achieving numbers that nevertheless remain more than 50% lower than before LASIK (Lee et al. 2002). Total recovery of the subbasal plexus, especially its morphology, probably never occurs, and a significantly longer period of time than previously assumed seems to be needed. Subbasal nerve density remained < 60% of preoperative levels at 3 years post LASIK (Calvillo et al. 2004), and nerve density near preoperative densities was not reached until 5 years after LASIK (Erie et al. 2005b). 9.2 Corneal sensitivity after LASIK An early loss of corneal sensitivity to coarse mechanical stimulation has been reported after LASIK, followed by progressive recovery of sensitivity during the following postoperative months. Corneal sensitivity seems to be at its lowest 1 2 weeks after LASIK, and by 6 12 months sensitivity has recovered to normal levels (Kim and Kim 1999, Perez Santonja et al. 1999, Linna et al. 2000, Benitez del Castillo et al. 2001, Toda et al. 2001, Donnenfeld et al. 2003, 2004, Michaeli et al. 2004, Bragheeth and Dua 2005, Lee et al. 2005). Recovery periods of over 12 months have also been reported (Nejima et al. 2005). By contrast, the return of nearnormal sensitivity levels by 3 weeks post LASIK has also been described (Chuck et al. 2000). Studies comparing the recovery of corneal sensitivity after PRK and LASIK have utilized the Cochet Bonnet esthesiometer, which measures coarse mechanical sensation, but has certain limitations in sensitivity and reproducibility (Murphy et al. 1998). In any case, after LASIK, the loss of sensitivity seems to be more intense and the time needed for recovery longer (Perez Santonja et al. 1999, Matsui et al. 2001, Kumano et al. 2003, Lee et al. 2005). Interestingly, lower tear fluid NGF levels in humans after LASIK, compared with PRK, have been accompanied by slower recovery of sensation. NGF is known to be a potent neurotrophic factor, and thus, tear fluid NGF is suggested to play a role in recovery of sensitivity as well as in regeneration of corneal nerves (Lee et al. 2005). More recently, noncontact gas esthesiometers, which are more sensitive and reproducible than mechanical esthesiometers, have been utilized in studies exploring the recovery of corneal sensitivity after LASIK (De Paiva and Pflugpfelder 2004, Gallar et al. 2004, Stapleton et al. 2006). In contrast to studies utilizing mechanical esthesiometers, which report the greatest decrease of sensitivity 1 2 weeks post LASIK (Linna et al. 2000, Donnenfeld et al. 2004), in the above study, corneas were observed to be hypersensitive at 1 week post LASIK (Gallar et al. 2004). This was followed by a significant decrease in sensitivity to mechanical stimuli during 3 25
26 5 months after surgery. Corneal sensitivity was close to normal values by 2 years post LASIK (Gallar et al. 2004). Patients without dry eye at 1 40 months after LASIK presented with decreased corneal sensitivity, while patients with LASIK associated dry eye showed corneal hypersensitivity at 3 36 months (De Paiva and Pflugfelder 2004). Corneal hypersensitivity observed in LASIK associated dry eye patients was suggested to result from compromised ocular surface barrier function and hypersensitivity to air jet (De Paiva and Pflugfelder 2004). Several factors influencing the severity of the postoperative decrease in corneal sensitivity and subsequent recovery have been suggested, including ablation depth, hinge orientation (superior or nasal), hinge width, and flap thickness. Deep ablations, thus greater corrections, result in a larger decrease in corneal sensitivity and a longer recovery (Kim and Kim 1999, Nassaralla et al. 2003, Bragheeth and Dua 2005, Shoja and Besharati 2007). Accordingly, ablation depth is a clear risk factor for developing dry eye after LASIK (De Paiva et al. 2006, Shoja and Besharati 2007). Depending on the microkeratome used in LASIK, the hinge is positioned either superiorly or nasally. While long ciliary nerves run and penetrate the cornea at the 3 and 9 o clock positions, it has been suggested that flaps with a superior hinge cause more severe nerve damage than those with a nasal hinge, which spares the medial nerve fibers. Seemingly in agreement with this concept, eyes with a nasal hinge were found to have less dry eye symptoms (Donnenfeld et al. 2003) and better corneal sensitivity than eyes with a superior hinge during a 6 month postoperative period (Donnenfeld et al. 2003, Vroman et al. 2005, Nassaralla et al. 2005). However, a prospective randomized clinical study found no difference in dry eye signs or symptoms between patients treated with superiorly and those with nasally hinged flaps (Ghoreishi et al. 2005). The narrow hinge of the flap resulted in a more pronounced decline in corneal sensitivity and more severe dry eye than flaps with a broader hinge (Donnenfeld et al. 2004). The thickness of the flap has also been suggested to be an important factor in regaining corneal sensitivity; thin flaps with a nasally placed hinge were related to more rapid recovery (Nassaralla et al. 2005). In conclusion, corneal mechanical sensitivity, measured with a Cochet Bonnet esthesiometer, decreases during the first postoperative weeks, and regeneration of nerves coincides with the recovery of sensitivity, with normal sensitivity levels typically being achieved 6 12 months after LASIK. However, studies utilizing more sensitive noncontact gas esthesiometers suggest that alterations in corneal sensitivity may persist for up to 24 months. 26
27 10. Dry eye A definition of dry eye was recently produced by the International Dry Eye WorkShop (DEWS 2007): Dry eye is a multifactorial disease of tears and ocular surface that results in symptoms of discomfort, visual disturbance, and tear film instability with potential damage to the ocular surface. It is accompanied by increased osmolarity of the tear film and inflammation of the ocular surface (Lemp et al. 2007). Large epidemiological studies have revealed the prevalence of dry eye at various ages range from 5% to 34% (Smith et al. 2007). However, the definition of dry eye and the diagnostic tests and criteria varied markedly between these studies, and thus, caution is advised in making direct comparisons between the results. Dry eye is classified into two etiopathogenic categories: 1) aqueous tear deficient dry eye and 2) evaporative dry eye. Aqueous tear deficient dry eye is further divided into SS dry eye and non SS dry eye. Non SS dry eye includes 1) primary lacrimal gland deficiencies, e.g. age related dry eye; 2) secondary lacrimal gland deficiencies such as conditions with lacrimal gland infiltration, e.g. sarcoidosis, lymphoma, acquired immunodeficiency syndrome (AIDS), or graft versus host disease; 3) conditions associated with obstruction of lacrimal gland ducts, e.g. trachoma, cicatrical pemphigoid, erythema multiforme, and chemical and thermal burns; 4) conditions affecting sensory innervation, e.g. herpes simplex keratitis, herpes zoster ophthalmicus, penetrating keratoplasty, PRK, LASIK, diabetes mellitus, and topical anesthetic abuse, as well as secretomotor innervation, e.g. damage to the VII cranial nerve and certain systemic medications (Lemp et al. 2007). Evaporative dry eye may be intrinsic, with regulation of evaporative loss from the tear film being directly affected by, for instance, meibomian lipid deficiency, poor lid congruity, wide lid aperture, and low blink rate. Extrinsic evaporative dry eye embraces those etiologies that increase evaporation by their pathological effects on the ocular surface, including vitamin A deficiency, topical drug preservatives, contact lens wear, and ocular surface disease, e.g. allergy (Lemp et al. 2007). 27
28 Figure 5. Lacrimal gland functional unit. Stimulation of the free nerve endings in the cornea generates afferent nerve impulses that travel through the ophthalmic division of the trigeminal nerve to the superior salivary nucleus in the pons. The nerves synapse and the signal is integrated with cortical and other input in the pons. The efferent branch of the loop passes along the nervus intermedius to the pterygopalatine ganglion. Postganglionic fibers then terminate in the main and accessory (Wolfring and Krause) lacrimal glands. Increasing evidence suggests that nerve endings found around the Meibomian glands and conjunctival Goblet cells travel along the same route (Stern et al. 2004). In the normal situation, the ocular surface, interconnecting nerves, and lacrimal glands form a functional unit (Fig. 5) that controls the major components of the tear film and responds to environmental, endocrinological, and cortical influences. If any portion of this funtional unit is compromised, lacrimal gland support to the ocular surface is impeded (Stern et al. 2004). 28
29 11. Dry eye after refractive surgery All keratorefractive surgical procedures, including PRK and LASIK, cause morphological and functional disturbances of corneal nerves. Dry eye is one of the most common complications after refractive surgery (Hong and Kim 1997, Sugar et al. 2002). It is mainly thought to be attributable to the transection of afferent corneal nerves during the lamellar microkeratome cut in LASIK, and additional damage caused by excimer laser photoablation. The ocular surface, lacrimal glands, and interconnecting nerves form a functional unit (Stern et al. 2004), and impairment of corneal nerves interrupts the cornea trigeminal nerve brain stem facial nerve lacrimal gland reflex arc, influencing both reflex and basal tear production. The diagnostic criteria and treatment strategies for dry eye vary widely among ophthalmologists, and among cornea and dry eye specialists. Some clinicians consider clinical signs more essential than symptoms. Conversely, other clinicians value symptoms more highly as early evidence of ocular disease. On the other hand, little correlation exists between the symptoms and clinical test results in dry eye patients (reviewed by Pflugfelder et al and Bron 2001, Dogru et al. 2005). The clinical signs of LASIK dry eye include evaluation of tear film stability with application of fluorescein to the tear film to measure tear film break up time and positive vital staining of the ocular surface with lissamine green, fluorescein or rose bengal. Schirmer s test with or without anesthesia is considered an important parameter at least for use in studies where statistical trends can be monitored. However, there is no consensus as to which method is most useful or regarding diagnostic cut offs (reviewed by Bron 2001). Symptoms can be monitored using different validated questionnaires such as the ocular surface disease index (OSDI) questionnaire (Schiffman et al. 2000). Punctate epithelial keratopathy detected with rose bengal or fluorescein staining has been noted in 2 6% of eyes that have undergone LASIK (reviewed by Ang et al. 2001, Wilson 2001), but symptoms of ocular dryness and irritation were noted in approximately half of the LASIK patients (Hovanesian et al. 2001). In addition to decreased reflex and basal tear production, impairment of corneal nerves may lead to LASIK induced neurotrophic epitheliopathy (LINE) (Wilson 2001, Wilson and Ambrosio 2001), where punctate epithelial microerosions are present on the corneal surface. However, LASIK patients who developed symptoms and signs of dry eye after the procedure had no significant difference in tear production detected by Schirmer s test with anesthesia from patients with no symptoms or signs of dry eye at time points from 1 month to 6 months after surgery (Wilson 2001). Soreness of the eye to touch was observed at 6 months more often after PRK than LASIK, affecting 26.8% and 6.7% of patients, respectively (Hovanesian et al. 2001). This was suggested to be related to symptoms of recurrent erosions. 29
30 Other issues potentially contributing to dry eye symptoms after LASIK include differences in corneal curvature; while normal corneas show prolate profiles, i.e. steeper in the center, and high conventional myopic LASIK produces oblate corneas. These changes in corneal curvature may interfere with even tear distribution, but the mechanical rubbing due to the anatomical change may also be causative. Moreover, patients who seek refractive surgery are often contact lens intolerant and may have preclinical dry eye before surgery. In addition, mechanical trauma caused by the microkeratome suction ring to limbal Goblet cells has been suggested to play a role in LASIK associated dry eye (Lenton and Albietz 1999). Diminished afferent input also results in a decreased blinking rate, which appears to be involved in the pathogenesis of LASIK associated dry eye (Toda et al. 2001). Risk factors for developing LASIK associated dry eye are: female gender, dry eye before surgery (Albietz et al. 2004a), depth of photoablation, and preoperative refractive error (Nassaralla et al. 2003, Albietz et al. 2004a, De Paiva et al. 2006, Shoja and Besharati 2007). LASIK dry eye has been reported to develop more often in patients of Asian origin than in Caucasians (Albietz et al. 2005). In addition to symptoms of dry eye, blurring of vision, and halos, dry eye has been associated with regression of refractive result in PRK (Corbett et al. 1996), hyperopic LASIK (Albietz et al. 2002), and myopic LASIK (Albietz et al. 2004b). 12. Sjögren s syndrome In 1928, Swedish ophthalmologist Henrik Sjögren ( ) saw a patient complaining of dry eyes, dryness of mouth, and pain in several joints. Henrik Sjögren was not the first to notice the combination of xeroftalmia, xerostomia, and arthralgia. French ophthalmologist Henri Gougerot published similar observations a few years earlier, in In 1933, Henrik Sjögren defended his doctoral thesis Zur Kentniss der Keratoconjunctivitis Sicca, where he carefully described 19 patients with a combination of dry eyes and dry mouth. The eponym Gougerot Sjögren disease appeared in the literature in the 1930s, but a decade later this was shortened to Sjögren s disease, mainly because of Sjögren s ongoing interest in the syndrome. Sjögren s syndrome (SS) is a chronic, generalized autoimmune disease. Dry eye and dry mouth are its major clinical manifestations. In primary Sjögren s syndrome (pss), typical symptoms occur in a pure form without an association with any other underlying autoimmune diseases. Secondary Sjögren s syndrome (sss) is associated with other autoimmune diseases such as rheumatoid arthritis or systemic lupus erythematosus (Fox et al. 2000, Fox and Stern 2002). In addition to sicca syndrome, patients frequently suffer from visceral manifestations, including 30
31 autoimmune thyreoiditis, atrophic gastritis, renal tubular glomerular nephritis, autoimmune hepatitis, and interstitial cystitis Neurological manifestations in Sjögren s syndrome In 1933, Henrik Sjögren described a patient with trigeminal nerve involvement in his doctoral thesis. Since then, the trigeminal nerve has been identified to be the most commonly affected cranial nerve in SS (Kaltreider and Talal 1969, reviewed by Kaplan et al. 1990). The overall prevalence of peripheral neuropathy, most commonly of the distal sensory symmetrical type, ranges from 10% to 30% in pss; fortunately, these neuropathies are often subclinical (Gemignani et al. 1994, Olney 1998, Barendregt et al. 2001). In a Japanese study on pss patients, trigeminal neuropathy was observed in 50% (Tajima et al. 1997), while in a Finnish study only 4% of patients were reported to have trigeminal neuropathy (Hietaharju et al. 1990). Electrophysiological studies of the trigemino facial and trigemino trigeminal reflexes in patients with trigeminal nerve involvement suggest lesions in the neurons of the Gasserian ganglia rather than in the trigeminal axons (Valls Sole et al. 1990). The pathophysiological mechanisms are unknown, but may involve vasculitis (Melgren et al. 1989) or lymphocytic inflammation of nerve cell ganglia (Griffin et al. 1990). Decreased corneal sensitivity in SSrelated dry eye has been observed with the aid of the Cochet Bonnet esthesiometer (Xu et al. 1996). 31
32 AIMS OF THE STUDY The role of corneal innervation in dry eye following corneal refractive surgery and in Sjögren s syndrome related dry eye was investigated. The following goals were set: 1. To examine the role of tear fluid cytokines, regeneration of subbasal nerves, and subepithelial haze after PRK using IVCM (I). 2. To examine the recovery of corneal sensitivity using a novel noncontact esthesiometer in patients who had undergone correction of high myopia by LASIK and to assess the relationship between dry eye symptoms and sensory recovery (II). 3. To examine the alterations in corneal nerve morphology in primary Sjögren s syndrome (III). 4. To examine the relationship between corneal nerve morphology and corneal sensitivity in primary Sjögren s syndrome patients (IV). 32
33 SUBJECTS AND METHODS 1. Subjects These studies were carried out according to the tenets of the Declaration of Helsinki at Helsinki University Eye Hospital. Research protocols were approved by the Ethics Review Committee of Helsinki University Eye Hospital. All patients and controls were informed both orally and with a written brochure about the studies. Informed consent was obtained from all participants. Table 2. Demographic characteristics of subjects enrolled in studies I IV. Patients n Female % Patients age Controls n Female % Controls age I PRK ± 5.9 II LASIK ± ± 10.4 III pss ± ± 14.5 IV pss ± ± 4.6 Data presented as mean ± SD. 1.1 PRK patients (I) The study evaluated 20 eyes of 20 patients (16 females and 4 males, mean age 30.7 ± 5.9 years) scheduled for myopic PRK. The spherical equivalent (SE) of the intended correction was 4.7 ± 1.5 D (range 2.75 D to 9.00 D). Astigmatic correction was performed on 12 patients. The intended cylinder correction was 0.73 ± 0.27 D (range 0.50 to 1.50 D). 1.2 LASIK patients and controls (II) The study evaluated 30 eyes of 30 subjects. Twenty eyes of 20 patients (14 females and 6 males, mean age 34.0 ± 7.4 years) who had undergone > 10 D myopic LASIK 2 5 years earlier were included in the study, and 10 eyes of 10 healthy volunteers (6 females and 4 males, mean age 39.8 ± 10.4 years) served as a control group. The mean follow up time was 44.2 ± 11.3 months (range months). A cohort of patients who met the inclusion criteria was selected from the hospital database. These patients were sent an invitation to an additional follow up examination. The inclusion criteria were 1) high myopic correction (SE > 10D) with or without 33
34 astigmatic correction and 2) time interval of 2 years or more after the last LASIK surgery. Exclusion criteria were 1) re treatments, and 2) patients with a history of any other ophthalmic surgical operations. The first 20 consecutive volunteers were included in the study. 1.3 Primary Sjögren s syndrome patients and controls (III and IV) Study III evaluated 20 eyes of 20 subjects. Ten patients with pss (9 females and 1 male, mean age 50.1 ± 13.5 years) were recruited from the Department of Rheumatology, Helsinki University Central Hospital, where they had been thoroughly examined by a rheumatologist. Ten age and sex matched healthy controls (9 females and 1 male, mean age 48.3 ± 14.5 years) served as a control group. The mean duration of dry eye symptoms was 16.3 ± 8.2 years, but the average time elapsed from diagnosis was only 8.0 ± 4.6 years. Study IV evaluated 30 eyes of 30 subjects. Twenty patients with pss (19 females and 1 male, mean age 54.5 ± 7.0 years) and ten age and sex matched healthy controls (9 females and 1 male, mean age 50.2 ± 4.6 years) participated. The mean duration of dry eye symptoms was 18.3 ± 10.0 years, and the average time interval between first symptoms and diagnosis was 10.3 ± 10.3 years. SS diagnosis in both studies (III and IV) was made according to American European consensus criteria (Vitali et al. 2002). The diagnosis was set when at least 4 of the 6 following criteria were met, with either item 4 (histopathology) or item 6 (serology) being present. Diagnosis was also set if any 3 of the 4 objective criteria were present (i.e. items 3, 4, 5, and 6). 1. Ocular symptoms (daily, persistent, troublesome dry eyes for more than 3 months and/or recurrent sensation of sand or gravel in the eyes and/or use of tear substitutes more than 3 times a day). 2. Oral symptoms (daily feeling of dry mouth for more than 3 months and/or recurrently or persistently swollen salivary glands or the need to frequently drink liquids to aid swallowing of dry food). 3. Ocular signs (Schirmer s I test, performed without anesthesia [< 5 mm in 5 min] and/or Rose bengal score or other ocular dye score [> 4 according to van Bijsterveld s scoring system]). 4. Histopathology (focal lymphocytic sialadenitis in minor salivary glands). 34
35 5. Salivary gland involvement (unstimulated whole salivary flow [< 1.5 ml in 15 min] and/or parotid sialography showing the presence of diffuse sialectasias and/or salivary scintigraphy showing delayed uptake, reduced concentration, and/or delayed excretion of tracer). 6. Autoantibodies (antibodies to Ro [SSA] and/or La [SSB]). Patient were excluded if they had past head and neck radiation treatment, hepatitis C infection, acquired immunodeficiency syndrome (AIDS), pre existing lymphoma, sarcoidosis, graft versus host disease, or if they used anticholinergic drugs. 2. Methods 2.1 Clinical examination Ophthalmic examination All patients were evaluated for uncorrected visual acuity (UCVA) and best spectacle corrected visual acuity (BSCVA) and manifest refractions and underwent tonometry, slit lamp examination, and dilated funduscopic examination. Schirmer s test Schirmer s test was performed using a Schirmer test strip (Clement Clarke International Ltd., Harlow, United Kingdom). Two drops of oxybuprocaine hydrochloride 4 mg/ml (Oftan Obucain, Santen Oy, Tampere, Finland) were then administered to prevent reflex tearing. The strip was positioned at the intersection of the temporal third with the nasal two thirds of the lower eyelid, and the patient waited for 5 min with eyes closed until the strips were removed, and the length of the moistened area was measured. Tear break up time (BUT) To measure BUT, 1 drop of oxybuprocaine hydrochloride 3 mg/ml and sodium fluorescein dye 1.25 mg/ml (Oftan Flurecain, Santen Oy, Tampere, Finland) was instilled in the lower conjunctival sac with a micropipette. The tear film was observed under cobalt blue filtered light. The interval between the last complete blink and the first appearance of randomly distributed dry spots was measured. The average of three measurements was calculated. Grading of corneal fluorescein staining Grading of corneal fluorescein staining was performed as recommended by Lemp (1995). The cornea was divided into five areas: central, upper, temporal, inferior, and nasal. Punctate 35
36 corneal staining was recorded using a standardized grading system of 0 3 for each of the five areas, resulting in a scale of Clinical haze grading Clinical corneal haze was estimated with a slit lamp according to the Fantes scale (Fantes et al. 1990). Criteria for corneal opacity grading were as follows: grade 0, totally clear; grade 0.5, a trace or a faint corneal haze; grade 1, haze of minimal density seen with difficulty with direct and diffuse illumination; grade 2, mild haze easily visible with direct focal slit illumination; grade 3, moderately dense opacity partially obscuring the iris details; and grade 4, severely dense opacity completely obscuring details of intraocular structures. CMTF haze estimate Confocal microscopy through focusing (CMTF) scans were obtained as previously described (Li et al. 1997, Moller Pedersen et al. 1997). Using the custom software, the CMTF data were digitized onto the PC, intensity profile curves were calculated, and a quantitative estimate of the increased back scattering from the subepithelial haze (CMTF haze estimate) was achieved. The thickness of the haze area was also calculated. One to four acceptable CMTF scans were produced for each eye. Mean values of the measurements were used for all statistical calculations. Subjective dry eye symptoms Subjective symptoms were evaluated using ocular surface disease index (OSDI), which is a reliable and validated 12 item questionnaire for assessing subjective symptoms in ocular surface diseases and the impact on visual functioning (Schiffmann et al. 2000). In addition, visual analog scale (VAS) was used to evaluate global severity of ocular discomfort. The subjects were asked to evaluate severity of ocular symptoms during the past month and to place a mark with a pencil on a 100 mm scale, with the left end representing minimal symptoms (0 mm) and right end maximal symptoms (100 mm). 2.2 Tear fluid analysis (I) Tear fluid collection All tear fluid samples were collected with a scaled 5 or 25 µl fire polished microcapillary tube as described previously (van Setten et al. 1989). Tears were collected preoperatively (day 0), on the second postoperative day (day 2) and 3 months postoperatively. The samples were immediately transferred to Eppendorf tubes and stored at 70 o C until assessed. Tear fluid flow in the collection capillary (µl/min) was calculated by dividing the volume of the tear fluid sample by the tear fluid collection time. The tear flow corrected concentration, i.e. rate of release, was calculated by multiplying the concentration in the sample (ng/l) by the tear fluid flow in the collection capillary (µl/min) (Vesaluoma et al. 1997a). As the interindividual variations in the tear fluid cytokine 36
37 concentrations were high, changes (%) in the cytokine concentrations and rates of release in preoperative vs. postoperative samples were also calculated. Cytokine immunoassays The concentrations of TGF 1 in tear fluid were measured by an enzyme immunoassay (Vesaluoma et al. 1997a). Microtiter plates (Maxisorp, Nunc Intermed, Denmark) were coated with monoclonal mouse anti TGF β1, β2, and β3 (Genzyme Diagnostics, Cambridge, MA, USA) 0.1 µg/well in 0.05 M Na 2 CO 3 buffer, ph 9.2, overnight at 4 C. After washing the wells with 0.05 M phosphate buffered saline, ph 7.3, containing 0.05% Tween 20, 100 µl of acid activated and neutralized (0.1 M HCL, 4 C, 1 h) standard dilutions (natural human TGF β1, Code BDP 1, R & D Systems, London, UK) and samples (final dilutions 18 fold) were added to the wells and incubated overnight at 4 C. The unbound material was removed with the above washing buffer, and 100 µl of 1000 fold diluted antibodies to human TGF β1 (Code , Jansen Biochimica, Beerse, Belgium) conjugated with alkaline phosphatase was added and incubated at 37 C for 2 h. After washing, the amount of alkaline phosphatase fixed to the tubes was determined in diethanolamine (1.0 mol/l) magnesium chloride (0.5 mol/l) buffer, ph 10.0, using p nitrophenylphosphate as a substrate for 1 h at room temperature. The absorbance of the p nitrophenolate liberated was measured at 405 nm with a 340 ATC microtitration plate reader (SLT, Lab instruments, Vienna, Austria). The detection limit for the assay was 5 ng/l. PDGF BB concentrations were measured by a sandwich enzyme immunoassay (Vesaluoma et al. 1997b). Microtiter plates (Maxisorp TM, Nunc Instrumed, Denmark) were coated with goat IgGtype antibody to highly purified Escherichia coli derived recombinant human PDGF BB (Code AB 220 Na, R & D Systems Europe Ltd., Abingdon, UK) (0.25 µg/well) in 0.05 M Na 2 CO 3 buffer, ph 9.2, overnight at 4 C. After washing the wells with 350 µl of water, 100 µl of recombinant human PDGF BB homodimer (Code , Genzyme Diagnostics, Cambridge, MA, USA) as a standard (serial dilutions from 1000 to 5 ng/l) or 5 to 20 fold diluted tears were added to the wells and incubated at 24 C for 60 min on a horizontal rotating table (80 rpm). The unbound material was removed and the wells were washed twice with saline containing 0.05% Tween 20. One hundred microliters of 100 fold diluted rabbit antibody to human PDGF BB (Code ZP 215, Genzyme Diagnostics, Cambridge, MA, USA) was added and incubated for 1 h at room temperature as above. After washing, 100 µl of 500 fold diluted alkaline phosphatase conjugated swine antibody to rabbit IgG (Code 67850, Orion Diagnostica, Espoo, Finland) was added and incubated as above. The plates were then washed three times with 350 µl of washing solution. The amount of alkaline phosphatase fixed to the tubes was determined in 1.0 M diethanolamine 0.5 M MgCl 2 buffer, ph 10.0 (Code , Reagena Ltd., Kuopio, Finland) at room temperature for 3 h in the dark, using p nitrophenolphosphate (Code , Sigma Chemical Co., St. Louis, MO, USA) as a substrate. The absorbance of p nitrophenolate liberated was measured at 405 nm with a 37
38 340 ATC microtitration plate reader (SLT Lab Instruments, Vienna, Austria). The absorbance of the 0 ng/l standard was subtracted from all the other absorbances, and the delta absorbances were used for calculations. The detection limit of the assay was 20 ng/l. TNF α concentrations were determined by a double antibody radioimmunoassay developed for measuring of serum TNF as described by Vesaluoma et al. (1997b). A volume of 10 µl of tear fluid samples was first diluted by adding assay buffer to reach a final volume of 100 µl. TNF α from tears competed with a fixed amount of 125 I labeled TNF α ( counts/min for 50 µl) for the binding sites of fold diluted specific rabbit antibodies. The bound TNF α was precipitated with Sepharose bound antirabbit IgG and centrifuged, and the radioactivity of the pellets was then counted. E. coli derived recombinant human TNF α (Code TNF H, Genzyme Diagnostics, Cambridge, MA, USA) was used as a standard. This had a molecular weight of 36 kda, and a specific activity > 1 x 10 7 U/mg of protein, as measured by bioassay with mouse L 929 cells. Rabbit antiserum to human TNF α (Code P 300A, Endogen, MA, USA) showed < 1% crossreaction with lymphotoxins. The detection limit of the assay was 10 ng/l. 2.3 In vivo confocal microscopy IVCM (I, III, and IV) Tandem scanning in vivo confocal microscopy (I and III) A tandem scanning confocal microscope (TSCM, Model 165A, Tandem Scanning Corp., Reston, VA, USA) was used to examine the central cornea. A 24X, 0.6 NA variable working distance objective lens was used. The field of view with this lens is 450 x 360 µm, and the z axis resolution 9 µm. Images were detected by using a low light level camera (model VE1000; Dage MTI, Michigan, IN, USA) and recorded on SVHS tape. Video images of interest were digitized using a PC based imaging system with custom software (University of Texas, Southwestern Medical Center at Dallas, Dallas, TX, USA). In addition, confocal microscopy through focusing (CMTF) scans were obtained. Intensity profile curves for digitized CMTF data were calculated. From each CMTF scan, epithelial, Bowman s layer, and total corneal thicknesses were measured. The mean values of each individual s measurements were used for the statistical analysis. After the layers of the central cornea had been scanned with the confocal microscope, special attention was paid to the morphology of the surface and basal epithelium. The microscope was then focused beneath the basal epithelium to evaluate the subbasal nerve plexus in detail. Afterwards, images were digitized from the SVHS video tape, and the number of nerve fibers in the image was determined using point counting principles. The number of nerve fibers in the 38
39 image with the most subbasal nerve fibers was used as a measure of nerve density. Nerve morphology was assessed from the SVHS video tape and digitized images. The morphology of the nerve fibers was evaluated, with attention being paid to the following aspects: thickness (fine and faint, normal, thick), beading, side branching, and sprouting. It must, however, be noted that resolution of confocal microscopy enables counting of nerve fiber bundles, but not of single fibers or terminals. Scanning slit in vivo confocal microscopy (ConfoScan 3) (IV) Corneal in vivo morphology was evaluated using an in vivo scanning slit confocal microscope (ConfoScan 3, software version 3.4, Nidek Technologies Slr, Vigonza, Italy) equipped with a Achroplan 40 x objective (Carl Zeiss Meditec AG, Jena, Germany). A topical anesthetic was instilled in the lower conjunctival fornix of both eyes before examination (oxybuprocaine hydrochloride 4 mg/ml, Oftan Obucain, Santen Oy, Tampere, Finland). The subject was comfortably seated in front of the microscope with the aid of chin and forehead rests and asked to look straight ahead, while a fixation target was not available. A drop of ophthalmic lubricant gel (2 mg/g carbomere, Viscotears, CIBA Vision Europe Ltd., Southhampton, UK) was applied on the objective tip to serve as a coupling media. The microscope is supplied with automatic alignment software that was used to center the objective. Automated mode was used to obtain full thickness scans from the central cornea. During a scan, the instrument recorded images at 25 frames/s as the focal plane advanced anteriorly µm between frames; scans were repeated until 350 frames were recorded. The best focused confocal microscopic images from the central cornea were used for nerve density calculations with software supplied by the manufacturer. The field size of the microscope was 422 µm 322 µm (0.136 mm 2 ) based on calculations from a calibration slide. 2.4 Noncontact esthesiometry (II) Central corneal mechanical sensitivity was assessed with a modified Belmonte Noncontact esthesiometer developed by the Cooperative Research Center for Eye Research and Technology, Sydney, Australia, and based on an instrument previously designed by Dr. Carlos Belmonte, which has been used extensively to assess corneal sensation in animals and humans (Belmonte et al. 1999, Acosta et al. 2001). The instrument is mounted on the frame of an air tonometer and has a box controller and two gas tanks, containing 100% air and 100% CO 2, respectively. The tip of the esthesiometer is adjusted to a distance of 4 mm in front of the cornea, using a focusing mechanism. Subjects were seated in front of the gas esthesiometer, with their chin placed in a cup and their forehead against a band. An audible click produced by the opening of the gas valve identified 39
40 the onset of the stimulus. After each pulse, the subject was asked to report whether the stimulus was felt independently of the sensation evoked. Sequential stimulus was only performed after the patient reported no sensation from the previous stimulation. Subjects were told to blink freely between stimuli. Mechanical stimulation consisted of a series of pulses of warmed air (constant temperature of 42 C at the tip of the probe), with flow varying from 0 to 160 ml/min, applied to the central corneal surface. Sensation caused by the mechanical stimulation was determined using the visual analog scale. Briefly, a series of 2 s pulses were applied randomly in 20 ml/min steps, from 160 ml/min to 20 ml/min. After a negative answer, the next stimulus was 10 ml/min higher until the lowest positive value was achieved. The lowest airflow that elicited a response, even weakly, was recorded as the mechanical threshold. 2.5 PRK (I) PRK was performed after surgical abrasion of the epithelium (diameter 6.5 mm) using a Beaver Eye Blade (Becton Dickinson, Franklin Lakes, NJ, USA). Six millimeter wide PRKs of varying ablation depths were performed using a VisX 20/20 excimer laser (VisX Co., Sunnyvale, CA, USA) or a NIDEK EC 5000 excimer laser (Nidek, Gamagoni, Aichi, Japan). The mean ablation depth was 60.7 ± 14.1 µm (range µm). Eye patching and postoperative medication Each eye was pressure patched for 3 days following PRK. In the morning of the first and/or second postoperative day, the patch was removed and the lids were gently cleaned with a paper wipe. After waiting for about 30 s, the tear fluid sample was collected, after which chloramphenicol ointment (Oftan Chlora; Santen, Tampere, Finland) was applied and the eye repatched. In addition to the ointment twice a day for 4 days, the postoperative medication included fluorometholone drops (Liquifilm FML; Allergan, Irvine, CA, USA) starting on the fourth postoperative day three times a day for 1 3 months, oral diclofenac sodium 25 mg (Voltaren; Ciba Geigy, Basel, Switzerland) 30 min before the operation and 2 3 times a day for the first days after PRK, and oral diazepam 5 10 mg (Diapam; Orion, Helsinki, Finland) for the first two postoperative nights. 2.6 LASIK (II) The corneal flap was created with an automated Hansatome microkeratome (Hansatome, model HT 230, Chiron Vision, Hansa Research & Developement, Inc., Miami, FL, USA). The intended thickness of the flap was either 160 or 180 µm, with a superiorly located hinge. Subsequent laser ablation was performed using a VisX Star S2 (VisX Co., Sunnyvale, CA, USA) excimer laser. The patients were prescribed topical ofloxacin 3 mg/ml (Exocin ; Allergan 40
41 Pharmaceuticals Ltd., Westport, Ireland) three times a day for 7 days and fluorometholone 1 mg/ml, (Liquifilm FML, Allergan Pharmaceuticals Ltd., Westport, Ireland) two times a day for 7 days starting on day 2. Nonpreserved artificial tears were to be used four times a day for at least 6 months after the operation. 2.7 Statistical analyses Statistical comparisons of the mean between groups were performed either with the t test or with the Mann Whitney U test for normally distributed or skewed data, respectively, using SPSS for Windows (version , SPSS Inc., Chicago, IL, USA). Normality of the data was tested using the Shaphiro Wilk test or the Kolmogorov Smirnov test as appropriate. In addition, histograms were used to help in testing normality of samples. Bonferroni corrections were applied in multivariate analysis. Bivariate correlations were examined using Pearson s (r) or Spearman s (rho) correlation test. All values are given as mean + standard deviation (SD) or median and interquartile range (IQR) for normally distributed or skewed data, respectively. P values of less than 0.05 were considered statistically significant. 41
42 RESULTS 1. Tear fluid cytokines, haze, and nerve regeneration after PRK (I) 1.1 Tear fluid cytokines after PRK The tear fluid flow in the collection capillary was (mean ± SD) 9.6 ± 11.1 µl/min ( µl/min) preoperatively, 43.0 ± 30.7 µl/min ( µl/min; P < 0.001) on day 2, and 8.8± 8.2 µl/min ( µl/min; P = 0.003) at 3 months postoperatively. A weak positive correlation (r = 0.498, P = 0.03) was observed between ablation depth and tear fluid flow on day 2. However, at 3 months postoperatively, no correlation existed between these parameters (rho = 0.285, P = 0.237). Cytokine concentrations and rates of release are given in Table IVCM three months after PRK Confocal images can be found in the original articles (I, III, and IV) at the end of this thesis. Surface epithelial cells, posterior stromal keratocytes, and endothelial cells of all corneas presented with a normal shape and reflectivity (images not shown). The basal epithelial cell area of two corneas showed pathological findings. The basal epithelial cells of a cornea with a history of recurrent erosions presented with presumably intracellular deposits (Rosenberg et al. 2000). Similar deposits could be discerned among subepithelial haze resulting from highly reflective keratocyte nuclei and visible keratocyte processes (I / Fig. 1A). Another cornea showed highly reflective particles, round to oval in shape, in the subepithelial area (I / Fig. 1B). The basal epithelial cells of all other patients appeared normal, and the Bowman s layer was absent in all corneas. The epithelial thickness varied from 25 to 49µm (39 ± 7µm), thus, the epithelium was thinner than in normal corneas (Li et al. 1997). The subbasal nerve plexus was absent in two corneas, and 18 corneas showed 1 5 (2.1 ± 1.4) regenerating nerve fiber bundles (I / Fig. 1C). Subepithelial haze was observed in all corneas, and in two cases it was very highly reflecting and appeared vacuolized (I / Fig. 1D). The first anterior keratocytes exhibited brightly reflecting nuclei and thickened keratocyte processes as signs of ongoing keratocyte activation (I / Fig. 1D). In one of these two corneas, the subbasal nerve plexus was absent (I / Fig. 1D). In the other 18 corneas, haze was more subtle, and subbasal nerve fiber bundles were visible (I / Fig. 1C), except in one case. The mean CMTF haze estimate was 506 ± 402 U, and the thickness of the haze area was 40.9 ± 9.2 µm. With the slit lamp, haze was mild (0.38 ± 0.39; range 0 1, (scale +0 to +4)) in all eyes. In general, the CMTF haze estimates were relatively low, in accordance with the clinical scoring. 42
43 Table 3. Concentrations and releases of PDGF BB, TGF 1, and TNF after PRK (I). Concentration Concentration Concentration Release Release Release Day 0 Day 2 Month 3 Day 0 Day 2 Month 3 PDGF BB Below detection limit (n) (ng /l) (ng/l) (ng/l) (pg/min) (pg/min) (pg/min) (13/19) (7/19) (10/20) (13/19) (7/19) (10/19) Median Mean SD Min Max P value * TGF 1 Below detection limit (n) (12/19) (13/19) (7/20) (12/19) (13/19) (7/19) Median Mean SD Min Max P value TNF Below detection limit (n) (0/19) (0/19) (0/20) (0/19) (0/19) (0/19) Median Mean SD Min ,8 Max P value 0.039* 0.002* 0.000** * = P < 0.05, ** = P <
44 1.3 Correlations between IVCM data and cytokines (I) The number of subbasal nerve fiber bundles was positively correlated with epithelial thickness (r = 0.58, P = 0.007). However, the number of subbasal nerve fiber bundles was not correlated with the CMTF haze estimate (rho = 0.281, P = 0.230) or the thickness of the haze area (r = 0.398, P = 0.082). Ablation depth showed no correlation with nerve count (r = 0.240, P = 0.308), CMTF haze estimate (rho = 0.041, P = 0.865), or thickness of the haze area (r = 0.006, P = 0.979). The CMTF haze estimate, as expected, showed a strong correlation with the thickness of the haze area (rho = 0.783, P = 0.000). No correlations were found between cytokine concentrations or rates of release at any timepoints and the CMTF haze estimate at 3 months. The magnitude of the changes from day 0 to day 2 in the concentrations or rates of release of the three cytokines was not correlated with the CMTF haze estimate at 3 months (data not shown). 2. Dry eye and corneal sensitivity after high myopic LASIK (II) 2.1 Subjective symptoms The majority of patients (55%) reported dry eye symptoms when asked a simple question: Do you have dry eyes? Ocular surface disease index (OSDI) score, indicating degree of dry eye symptoms, was significantly higher in LASIK patients (18.6 ± 6.4%) than in normal controls (7.5 ± 5.7%; P = 0.022). However, almost all LASIK patients (95%) were satisfied with the overall outcome and would have chosen the operation again. The only patient who was not entirely satisfied had undergone epithelial erosion during the surgery and subsequent diffuse lamellar keratitis (DLK) in both eyes. A predisposing factor seemed to be a loose epithelium due to basement membrane dystrophy, although the patient had a negative history of erosions and the preoperative examination revealed no abnormalities. 2.2 Objective dry eye tests We found no difference in objective dry eye tests. Schirmer s test values did not differ significantly between patients and controls (14.4 ± 8.9 mm and 9.0 ± 4.2 mm, respectively, P = 0.066), although LASIK patients showed slightly higher scores contrary to expectations. Tear BUTs were similar in patients and controls (15.9 ± 11.2 s and 14.0 ± 10.0 s, respectively, P = 0.505). None of the patients or controls showed corneal fluorescein staining. 44
45 2.3 Corneal sensitivity The mean corneal sensitivity thresholds did not differ between the groups, being 73.5 ± 29.6 ml/min in LASIK patients and 78.0 ± 18.7 ml/min in controls (P = 0.666). No correlations were present between corneal sensitivity threshold values and OSDI scores. Even when patients were divided into two groups: 1) patients claiming to have dry eyes and 2) patients claiming not to have dry eyes, we found no significant difference between sensitivity threshold values. No significant correlation existed between corneal sensitivity thresholds and objective dry eye signs (Schirmer s test or BUT). 3. Corneal morphology and sensitivity in primary Sjögren s syndrome (III and IV) 3.1 Subjective symptoms (IV) OSDI and VAS scores were significantly higher in pss patients than in controls (Table 5), with a strong positive correlation between these two measures of ocular discomfort (rho 0.92, P < 0.01), suggesting that VAS can be used to assess severity of dry eye symptoms in a relatively time effective manner. 3.2 Objective dry eye tests (III and IV) Objective dry eye test values (Schirmer s test, tbut) were lower in pss patients than in controls (Tables 4 and 5). Corneal fluorescein was observed in the majority of pss patients, while none of the controls showed corneal fluorescein staining (Tables 4 and 5). Table 4. Characteristics of pss patients and controls (III). pss Controls P value Number of patients Nerve count (nerves/frame) 5.4 ± ± Schirmer s test (mm) 3.0 ± ± Corneal fluorescein staining % 60 0 Data presented as mean ± SD, = t test, Corneal fluorescein staining % = percentage of patients showing corneal fluorescein staining. 45
46 Table 5. Characteristics of pss patients and controls (IV). pss Controls P value Number of patients Corneal fluorescein staining 1.5 ( ) Schirmer s test (mm) 2.5 ( ) 9.0 ( ) Tear break up time (s) 5.0 ( ) 7.0 ( ) Mechanical threshold (ml/min) Chemical threshold (% CO2) 29.2 ± ± Nerve count (nerves/frame) 5.9 ± ± Stromal nerve thickness (µm) 7.9 ( ) 5.7 ( ) VAS (0 100 mm) 61.0 ( ) 2.5 ( ) OSDI (0 100 %) 37.5 ( ) 5.3 ( ) Data presented as mean ± SD or median and (interquartile range), Mechanical threshold = Corneal mechanical sensitivity detection threshold, Chemical threshold = Corneal chemical sensitivity detection threshold, OSDI = Ocular Surface Disease Index, VAS = Visual Analog Scale, = t test, = Mann Whitney U test. 3.3 Corneal sensitivity (IV) The mean mechanical sensitivity detection threshold was lower in pss patients, implicating corneal mechanical hypersensitivity in pss dry eye. However, no difference was found in chemical sensitivity detection thresholds (Table 5). 3.4 IVCM in primary Sjögren s syndrome (III and IV) Confocal images can be found in the original articles (III and IV) at the end of this thesis. The surface epithelium was irregular or patchy in the majority of SS corneas (III / Fig. 1A), whereas control corneas showed normal morphology (III / Fig. 1B). Basal epithelial cells appeared normal in all subjects. The subbasal nerve density did not differ between SS and control groups (Tables 4 and 5), as reflected in long nerve fiber bundles per microscopic field. The normal subbasal nerve plexus of 46
47 a healthy control subject is shown in IV / Figure 1. Nerve sprouting or a nerve growth cone like pattern (III / Figs 2A and 2B; IV / Fig. 2), presumably indicating neural regeneration, was found at the level of the subbasal nerve plexus in 20 40% of patients. One SS patient with severe peripheral neuropathy showed very thin subbasal nerve fiber bundles without beading (III / Fig. 2C). Control subjects, by contrast, had relatively thick subbasal nerve fibers. Only a single highly reflective nerve fiber bundle was observed in one of the control subjects. In addition, subbasal nerve fiber bundles showed abnormal tortuosity in 2/10 eyes of the SS group (III / Fig. 3B); no such abnormality was seen in the control group (III / Fig. 3D). Interindividual variation in the density of the subbasal nerve plexus was wide, ranging between 4 and 9 long nerve fiber bundles per microscopic field. Round particles, measuring approximately µm in diameter, possibly cells of inflammatory origin, were found at the level of the subbasal nerve plexus of one SS cornea (III / Fig. 3A). Anterior keratocytes revealed signs of activation, hyperreflectivity, or visible processes in 5/10 SS corneas (III / Fig. 1C). Interestingly, three of these corneas also showed nerve sprouting (III / Figs. 1A and 1B). The stromal nerves appeared significantly thicker in pss (IV / Figs 4 and 5) than in controls (IV / Fig. 3; Table 5), possibly indicating neural regeneration. In one patient, an extremely thick stromal nerve measuring 43 µm in diameter was observed (IV / Fig. 5); this patient also presented with APCs among subbasal nerves and a very low mechanical sensory threshold (10 ml/min), implicating severe corneal hypersensitivity. Mature APCs with typical branching and long dendritic extensions were observed among the subbasal plexus of the central cornea in 35% (7/20) of patients (IV / Fig. 6.) but in only 10% (1/10) of controls. In patients in whom APCs were observed (n = 7), their average density in the central cornea was 174 ± 26 cells/mm 2. The number of mature APCs in the central cornea of these patients displayed a strong positive correlation with the subjective symptom score (r = 0.847, P = 0.016). Patients with APCs and/or nerve growth cones otherwise did not differ from other patients with respect to subjective symptoms, objective signs, or other features of nerve morphology. 47
48 DISCUSSION 1. Tear fluid cytokines and haze after PRK (I) The cytokines TGF 1, TNF, and PDGF BB were chosen to be analyzed in tear fluid for their potential influence on corneal keratocytes and stromal wound healing, including keratocyte repopulation of the ablated area after initial keratocyte apoptosis, keratocyte activation, and subsequent production of the ECM (Ohji et al. 1993, Jester et al. 1996, 2002, Wilson et al. 1996a, Andresen et al. 1997, Myers et al. 1997, Andresen and Ehlers 1998, reviewed by Jester et al. 1999). However, of the measured cytokines, only TNF was readily measurable in all samples at all time points. TGF 1 and PDGF BB were detected in 8/20 and 7/20 preoperative samples, in 6/19 and 13/19 samples on day 2, and in 7/20 and 10/20 samples at 3 months, respectively. Several potential sources exist for tear fluid cytokines, including the main and accessory lacrimal glands, corneal epithelial and stromal cells, conjunctival or inflammatory cells, the ECM, and leakage from conjunctival vessels. Corneal wounding seems to result in increased lacrimal gland mrna levels for TNF, HGF, KGF, and EGF (Thompson et al. 1994, Wilson et al. 1999b). Whether the PRK wound induces cytokine production in the human lacrimal gland is unknown. No correlations were present between pre or postoperative tear fluid levels of TGF 1, TNF, or PDGF BB and subepithelial post PRK haze estimated at 3 months by IVCM. Nor did eyes with elevated in cytokine concentrations present with higher CMTF haze estimates. The clinical healing of all eyes proceeded without problems, and the maximal clinical haze observed at 3 months was scored 1 on a scale from +0 to +4. One of the limitations of the study was the small size of the patient group, with no severe complications, such as dense haze (score +3 or +4) occurring in this group. The CMTF haze estimates were also low, which might have contributed to the result. Nevertheless, the observed high cytokine concentrations, e.g. of TGF 1, in individual eyes without haze formation may suggest that tear fluid analysis is not optimal for screening potential candidates for haze formation even had the patient cohort been more representative in terms of different degrees of subepithelial haze. 2. Nerve regeneration after PRK (I) During PRK the anterior stromal nerve trunks and subbasal nerve plexus are ablated. Proper innervation has long been known to be necessary for normal corneal epithelial regeneration (Beuerman and Schimmelpfennig 1980). In addition, individual epithelial cells and possibly 48
49 also keratocytes are innervated (Muller et al. 1996). It is, therefore, to be expected that proper innervation is important for the physiological status of epithelial cells and quiescent keratocytes. Intriguingly, innervation might have a direct effect on corneal wound healing. To my knowledge, I am the first to demonstrate that the degree of subbasal nerve plexus regeneration after PRK in human in vivo cornea positively correlates with restoration of the thickness of corneal epithelium. This is an additional piece of indirect evidence for the trophic and regulatory functions of corneal innervation. My observation is in line with earlier in vitro or experimental findings showing that innervation has an influence on epithelial proliferation (Araki et al. 1994, Nakamura et al. 1997). Whether nerves also exert an effect on the healing of stromal tissue remains obscure. No significant correlation was observed between the number of subbasal nerve fiber bundles and the CMTF haze estimate or the thickness of the haze area. After the initial anterior keratocyte loss after PRK, the area is repopulated with new migratory keratocytes (reviewed by Fini and Stramer 2005), which will rapidly transform to altered keratocytes that produce ECM (Moller Pedersen et al. 1997). The return of keratocytes to quiescence takes months (Linna and Tervo 1997, Bohnke et al. 1998, Frueh et al. 1998), and the timing coincidences with the gradual disappearance of the subepithelial haze (as observed by slit lamp) and regeneration of innervation. Moller Pedersen et al. (1997) showed delicate subbasal nerve fibers in 9/17 patients at 1 month after PRK, whereas according to Frueh et al. (1998) only 1/18 corneas presented with subbasal nerves at that time. In their study, 7/18 corneas showed nerve regeneration by 4 months and 13/18 corneas by 12 months. Bohnke et al. (1998) examined 15 eyes at 8 43 months postoperatively and found regenerated nerve fibers in all eyes. In my study, only two corneas showed a total absence of a subbasal nerve plexus at 3 months, whereas in the other 18 corneas at least single nerve fiber bundles were observed in the central area, although the branching pattern was not normal by 3 months. However, recovery of corneal nerve density to preoperative levels took 2 years after PRK (Erie et al. 2005b). There are certain limitations in grading of neural regeneration, e.g. dense haze impedes the observation of thin nerve fiber bundles. The resolution of confocal microscopy equipment also has a limited threshold. Regrowth of nerve fibers into the ablated area is also essential for restoration of corneal sensitivity after refractive surgery. After PRK, the central sensitivity, measured using a Cochet Bonnet esthesiometer, returns to the preoperative level by 3 months (Perez Santonja et al. 1999, Matsui et al. 2001, Lee et al. 2005). Until then, the cornea lacrimal gland reflex arc, which regulates tear fluid release from the lacrimal glands, is supposed to be damaged, and several patients complain about dryness of the ocular surface for the first few months after PRK. 49
50 3. Corneal sensitivity after high myopic LASIK (II) Corneal mechanical sensitivity detection thresholds over the long term after high myopic LASIK did not differ from those of control subjects. Accordingly, the results of objective dry eye tests were similar to those of controls. However, the patients reported ongoing ocular discomfort and symptoms resembling dry eye (photophobia, grittiness, foreign body sensation, and ocular irritation) significantly more than age and sex matched control subjects. Loss of sensitivity and recovery of sensitivity after LASIK have been shown to correlate with high corrections (Kim and Kim 1999, Nassaralla et al. 2003, Bragheeth and Dua 2005, Shoja and Besharati 2007). It is therefore logical to presume that corneal nerves are implicated in this process in some way. On the other hand, high correction seems to be one of the risk factors for patients developing so called chronic dry eye syndrome after LASIK (reviewed by Albietz and Lenton. 2004, De Paiva et al. 2006, Shoja and Besharati 2007). De Paiva and Pflugfelder (2004) found decreased corneal sensitivity after LASIK in patients without dry eye. They also observed corneal hypersensitivity in patients with post LASIK dry eye compared with normal controls. The LASIK group consisted of 20 patients 1 40 months after myopic or hyperopic correction; data for refractive corrections were not provided. The post LASIK dry eye group included six patients who reported dry eye symptoms and had ocular signs compatible with dry eye after a mean interval of 12 months (range 3 36 months) following myopic LASIK. The authors suggested that corneal hypersensitivity observed in dry eye patients is due to compromised ocular surface barrier function and hypersensitivity to air jet. Some of the differences between their study and my own may be explained by 1) I included only patients with high myopic corrections, and 2) the mean interval after surgery in my study was longer (44.2 ± 11.3 months, range months). In addition to decreased reflex and basal tear production, impairment of corneal nerves may lead to LASIK induced neurotrophic epitheliopathy (LINE) (Wilson 2001, Wilson and Ambrosio 2001, reviewed by Ambrosio et al. 2007), where punctate epithelial microerosions can be detected on the corneal surface. However, patients who developed symptoms and signs of dry eye after LASIK had no significant difference in tear production detected by Schirmer s test with anesthesia from patients who had no symptoms or signs of dry eye at time points from 1 month to 6 months after surgery (Wilson 2001). LASIK associated dry eye has been suggested to represent a neurotrophic epitheliopathy rather than an actual dry eye syndrome (Wilson 2001). This is supported by the data presented in my study of high myopic LASIK patients. The majority of patients reported ocular discomfort resembling dry eye symptoms, although clinical dry eye tests were normal and corneal sensitivity levels were within normal limits. These symptoms of ocular discomfort could be in part be derived from aberrantly regenerated corneal nerves. 50
51 LASIK DRY EYE HYPOTHESIS LASIK patients complain about ongoing dry eye symptoms ALTHOUGH... Objective clinical dry eye tests are normal? Mechanical sensitivity is normal Some of the symptoms may be caused by aberrantly regenerated nerve fibers Figure 6. LASIK dry eye hypothesis: in the long term (2 5 years) after high myopic LASIK, the majority of patients complain about ongoing dry eye like symptoms. However, clinical dry eye tests are normal, and corneal mechanical sensitivity is comparable with that of normal controls. Some of these symptoms may thus be derived from aberrantly regenerated nerve fibers, representing a form of corneal neuropathy rather than conventional dry eye disease. Other issues possibly contributing to dry eye symptoms after LASIK include differences in corneal curvature; while normal corneas show prolate profiles, i.e. are steeper in the center, high conventional myopic LASIK produces oblate corneas. These changes in corneal curvature may interfere with even tear distribution, but mechanical rubbing due to the actual anatomical change may also be causative. Mechanical trauma caused by the microkeratome suction ring to 51
52 limbal Goblet cells has been suggested to play a role in LASIK dry eye (Shin and Lee 2006). Diminished afferent input from corneal nerves also results in a decreased blinking rate, which may be involved in the pathogenesis of LASIK dry eye (Toda et al. 2001). Moreover, patients who seek refractive surgery are often contact lens intolerant and may have preclinical dry eye before surgery. Unfortunately, my study was cross sectional and I was not able to conduct presurgical examinations. Lay patients are unable to differentiate between symptoms of ocular dryness and "sore eyes" due to other basic conditions. In the end, however, the most important aspect is the subjective symptoms experienced by patients. Interestingly, patients report relief in symptoms when using artificial tears, which may be explained by lowering the frictional forces between lids and the ocular surface, and thus, the corneal afferent nerves being less activated. Some of the symptoms experienced may be derived from aberrantly regenerated corneal nerves after LASIK surgery. LASIK dry eye could in fact be a sort of phantom pain, representing a form of corneal neuropathy rather than conventional dry eye syndrome. This new insight into the pathogenesis of LASIK dry eye syndrome as a form of corneal neuropathy has clinical implications and also offers novel therapeutic possibilities. Patients should be informed of the possibility of developing chronic dry eye symptoms, especially after deep ablations. In severe cases of disabling chronic pain after LASIK, when conventional therapeutic possibilities fail to offer relief, consultation of a physician specialized in pain treatment is recommended. 4. Corneal sensitivity in primary Sjögren s syndrome (IV) Corneal sensitivity detection thresholds to mechanical air jet stimuli were significantly decreased in patients with pss dry eye, implicating corneal hypersensitivity. My finding is in line with earlier observations by De Paiva and Pflugfelder (2004), who also found decreased mechanical sensitivity detection thresholds in dry eye measured using a similar modified Belmonte noncontact gas esthesiometer. By contrast, Bourcier et al. (2005) and Benitez Del Castillo et al. (2007) reported increased corneal sensitivity detection thresholds in dry eye patients, suggesting corneal hypoesthesia. Many variables, such as selection of patients and controls and disease severity, can influence the results. For example, in the Bourcier study, only one third of patients had a diagnosis of pss or sss. I included only patients with a diagnosis of pss and age and sex matched controls. In addition, variability among noncontact gas esthesiometers is inevitable and may explain part of the discrepancy. We and De Paiva and Pflugfelder (2004) used a modified Belmonte esthesiometer, while Bourcier et al. and Benitez Del Castillo et al. utilized the original Belmonte esthesiometer. Differences in the size of the tip, the tip distance to the cornea, and the size of the 52
53 corneal area stimulated by the air jet are important factors. Moreover, therapeutic approaches in treating dry eye obviously differ. For instance, different use of topical and/or systemic antiinflammatory pharmaceuticals during the course of the disease may affect the results. Decreased corneal sensitivity in dry eye utilizing the Cochet Bonnet esthesiometer was observed by Xu et al. (1996) and Villani et al. (2007). Different results in these cases might be explained by different research methodologies, as the Cochet Bonnet esthesiometer uses mechanical contact probe stimulation with some limitations in sensitivity and reproducibility. In addition, a mechanical contact probe and a noncontact air jet stimulate corneal afferent sensory nerve endings differently. De Paiva and Pflugfelder (2004) suggested that the corneal hypersensitivity observed in dry eye is due to compromised ocular surface barrier function. In my study, I found a positive correlation between corneal mechanical sensitivity and increased corneal fluorescein staining, supporting this part of their hypothesis. In addition, I observed a positive correlation between corneal morphology, corneal mechanical (hyper)sensitivity, and subjective symptoms, indicating that in patients with the most severe ocular symptoms weak stimuli are recognized and may even elicit painful sensations. The findings of altered corneal nerve morphology may offer another explanation for the observed corneal mechanical hypersensitivity. 5. Corneal nerves in primary Sjögren s syndrome (II and IV) Corneal subbasal nerve density was similar between pss patients and controls (III and IV), suggesting that this may not per se explain the difference seen in corneal sensation. Previously published data concerning corneal nerve density in dry eye have been conflicting. Increased subbasal nerve counts in aqueous tear deficient patients were observed by Zhang et al. (2005), whereas decreased nerve counts were reported by Benitez Del Castillo et al. (2004), and (2007) and Villani et al. (2007). However, in the Benitez Del Castillo studies, a statistically significant difference was found between the SS group and the control group composed of younger subjects, but not between the SS group and the control group of older subjects. Although corneal nerve density is easily calculated and quantified, other properties of the corneal nerves, such as morphological alterations and inflammatory findings, seem to play a more important role than nerve density, which may be increased, decreased, or similar compared with controls. Although corneal subbasal nerve density showed no difference, several morphological alterations were present in corneal nerves. Nerve growth cone like structures in subbasal nerves were found in 20 40% of our patients (III / Figs. 2A and 2B; IV / Fig. 2). These alterations may implicate ongoing nerve sprouting, and may result from attempts of the inflammation injured 53
54 nerve fibers to regenerate. Inflammation is recognized as a critical factor in the pathogenesis of dry eye, and the upregulation of neurotrophins, e.g. nerve growth factor (NGF), during inflammation has been shown in many studies. NGF is known to induce axonal regeneration, nerve sprouting, and when overexpressed even hypertrophy of the peripheral nervous system (Albers et al. 1994). On the other hand, focally applied neutralizing antibodies to neurotrophic factors reduce collateral axonal branching after peripheral nerve lesion (Streppel et al. 2002). NGF is expressed in alpha smooth muscle actin positive dermal myofibroblasts (Hasan et al. 2000), which are comparable with corneal altered keratocytes. Altered keratocytes develop during the corneal wound healing process (reviewed by Jester et al. 1999), and in various inflammatory conditions (reviewed by Petrol et al. 1998, Rosenberg et al. 2002). I observed altered anterior keratocytes with signs of activation: hyperreflectivity or visible processes, in 5/10 SS corneas (III / Fig. 1C). Interestingly, the majority of these corneas also showed nerve growth cone like structures. Presumably, these altered keratocytes are the source of NGF in SS dry eye. Recently, it has been shown that patients with dry eye present with elevated tear fluid levels of NGF (Lee et al. 2006), and topical anti inflammatory treatment with prednisolone decreases tear fluid NGF levels and markedly alleviates dry eye symptoms (Lee et al. 2006). Stromal nerves appeared significantly thicker in SS patients than in controls. A similar finding was reported by Benitez Del Castillo et al The implication of the thickening of stromal nerves remains unclear. However, it has earlier been shown using immunoelectron microscopy and morphometry that nerve fibers regenerating after an inflammatory insult are significantly thicker than normal healthy nerve fibers (Imai et al. 1997, Niissalo et al. 2002). Possibly, stromal nerves are thickened secondary to chronic ocular surface inflammation or this finding may represent a form of neural regeneration. Antigen presenting cells (APCs) play a critical role in corneal immunology in health and disease (Hamrah et al. 2002, 2003a, 2003b). APCs have been observed in living corneas by modern IVCM (Rosenberg et al. 2000a, 2002, Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). The density of APCs declines from the limbus to the center in healthy corneas (Hamrah et al. 2002, 2003b, Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). In the corneal limbal epithelium, dendritic cells are present in virtually all healthy subjects (Mastropasqua et al. 2006), while in the central cornea only some 20 30% of healthy controls show APCs (Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). APCs are more often found in the peripheral cornea, where they show signs of having a mature phenotype with long slender dendritic processes, while immature APCs without dendrites typically predominate in the central cornea (Zhivov et al. 2005). We focused on the central cornea and observed APCs in 35% of patients and in 10% of controls. The density of the APCs in the central cornea in pss patients was significantly higher than that reported in healthy subjects (Zhivov et al. 2005, 2007, Mastropasqua et al. 2006). The high APC density together with the mature phenotype of these cells in the central 54
55 cornea (IV / Fig. 6) suggest that these cells are actively involved in the local pathomechanism as antigen processing and presenting cells. This may contribute to the perpetuation of dry eye and even lacrimal gland adenitis, as it has recently been shown that desiccating stress exposes antigenic epitopes shared by the ocular surface and lacrimal glands (Niederkorn et al. 2006). Primary Sjögren s syndrome patients presented with corneal mechanical hypersensitivity, although their corneal nerve density did not differ from that of controls. Corneal sensitivity appeared to correlate with subjective symptoms and objective ocular signs, but not with corneal nerve density. However, alterations in corneal nerve morphology (nerve sprouting and thickened stromal nerves) and an increased number of APCs, implicating the role of inflammation, were observed. I hypothesize that chronic inflammation and diminished volume of tear fluid, enriched in pro inflammatory cytokines such as IL 1 and IL 6 (Tishler et al. 1998, Solomon et al. 2001), lead to keratocyte activation, which is followed by synthesis of NGF or other neuronal growth factors. NGF and its high affinity receptor TrkA are expressed in the human corneal stroma and epithelium (Lambiase et al. 2000, You et al. 2000). In addition to hypertrophy of neural tissue (Albers et al. 1994), NGF facilitates transmission of pain (hyperalgesia), possibly due to its effect on ion channels (Lewin et al. 1993, reviewed by Apfel 2000, Gould et al. 2000). Overexpression of neuronal growth factors could explain not only the observed changes in corneal nerves and corneal hypersensitivity but also the tenderness or even chronic pain and ocular hyperalgesia often observed in these patients. 55
56 SJÖGREN S SYNDROME HYPOTHESIS Chronic ocular surface inflammation Langerhan s cells IL 1, IL 6, etc Hyperalgesia Degeneration of epithelium and nerves Keratocyte activation Neurotrophins Nerve sprouting Figure 7. Sjögren s syndrome hypothesis: ongoing ocular surface inflammation along with diminished tear fluid volume, enriched with pro inflammatory cytokines, leads to degeneration of the surface epithelium and subbasal nerves. This results in activation of altered keratocytes, followed by synthesis of NGF or other neuronal growth factors. Overexpression of neuronal growth factors could explain not only the observed changes in corneal nerves and corneal hypersensitivity but also the tenderness or even the chronic pain and ocular hyperalgesia often observed in these patients. 56
57 SUMMARY AND CONCLUSIONS Pre or postoperative levels of the tear fluid cytokines TGF 1, TNF and PDGF BB did not correlate with the development of corneal haze, as estimated by IVCM at 3 months after PRK. However, it is noteworthy that none of our patients showed severe grade 3 or 4 haze. Subbasal nerve fibers were observed in the central cornea in 18/20 eyes. A positive correlation was observed between the regeneration of subbasal innervation (based on the IVCM nerve count at 3 months after PRK) and the thickness of regenerated epithelium, possibly reflecting the trophic effect of corneal nerves on epithelium. However, the CMTF haze estimate did not correlate with regeneration of the subbasal nerve plexus. The majority of patients reported ongoing dry eye symptoms long after high myopic LASIK, although objective clinical signs were not demonstrable. No difference in corneal sensitivity was observed between patients and controls. I assume that at least some of the symptoms may be derived from aberrantly regenerated corneal nerves after LASIK surgery, thus representing a form of corneal neuropathy rather than conventional dry eye. Primary Sjögren s syndrome patients presented with corneal mechanical hypersensitivity, although their corneal subbasal nerve density did not differ from that of controls. Corneal mechanical sensitivity appeared to correlate with subjective symptoms and objective ocular signs, but not with corneal nerve density. However, alterations in corneal nerve morphology (nerve sprouting and thickened stromal nerves) and an increased number of APCs among subbasal nerves, implicating the role of inflammation, were observed. We suggest that these findings offer an explanation for the corneal hypersensitivity or even ocular hyperalgesia often observed in these patients. 57
58 ACKNOWLEDGMENTS This study was carried at the Department of Ophthalmology, Helsinki University Central Hospital, from 2000 to I am sincerely grateful to Professor Leila Laatikainen and her successor, Professor Tero Kivelä, the current head of the Department of Ophthalmology, for providing excellent working facilities. My deepest gratitude goes to my supervisor, Professor Timo Tervo, with whom I have had numerous inspiring conversations on scientific issues as well as on other common subjects of interest. Without his innovative ideas, my thesis would not be the same. I am sincerely grateful to Professor Yrjö T. Konttinen. I have been privileged to be able to collaborate with him and to share thoughts and ideas 24 hours a day, 365 days a year, literally. His consistent enthusiasm and positive thinking were instrumental to the completion of this thesis. I am deeply grateful to Docent Minna Vesaluoma. Without her, I would not have been able to start my scientific career in My thanks also belong to my collaborators and colleagues Carola Grönhagen Riska, Maaret Helintö, Juha Holopainen, Eija Kaila, Sissi Katz, Liisa Konttinen, Maria Lamberg, Nina Lindbohm, Jukka Moilanen, Waldir Neira, Anna Maija Teppo, Tuuli Valle, and Steven Wilson. Professors Hannu Uusitalo and Marja Liisa Vuori, the official reviewers of the thesis, are thanked for constructive criticism that vastly improved the manuscript. I am deeply grateful to my author editor Carol Ann Pelli for editing the language of this manuscript, and also to architect Anna Pakkala for drawing the pictures of my thesis. Special thanks go to my teacher of ophthalmology in medical school in 1997, Docent Paula Summanen. She inspired my interest in ophthalmology at the beginning of my career. I also owe special thanks to Jouko Larinkari, MD and Tapio Stenborg, MD, for their encouragement and for teaching me the basics of ocular surgery and ophthalmology. I am very grateful to Richard C. Troutman, MD, and the International Society of Refractive Surgery of the American Academy of Ophthalmology for the prestigious Troutman Award in I was privileged to meet Dr. Troutman, a pioneer in microsurgery of the eye, and really appreciate his encouragement. 58
59 Scientific work has brought an enormous amount of joy and contentment into my life. I cannot imagine my years as an ophthalmic resident without being involved in academic research. Several interesting congresses around the world and many new friends are but a few examples. Research has opened my eyes in so many ways and given me courage to make my own decisions, not always blindly accepting information written by others. I am deeply grateful to have wonderful parents in law, Arja and Tapani Tuisku, who have always been there for me and lent a helping hand. I have been blessed with loving parents, my mother Marja Leena and my late father Seppo Tuominen. They have always been supportive and understanding and have encouraged me to follow in their footsteps as an MD. I remember discussions between my father and myself as a little boy about the definition of an academic dissertation. It was not easy to understand why people have to argue about things why can t they just agree? It took some thirty years for me to discover the answer. I also wish to thank my sister Anna and my brothers Jouni and Joonas for their interest in my project. This work is dedicated to my family, to whom I owe my warmest thanks, especially to my wonderful wife Johanna, who has encouraged and sometimes even pressured me to finish this thesis. She has always taken such good care of us boys (see below), although it has sometimes required exceptionally long nerve fibers. My two lively sons, Tom (4 years) and Matias (3 years), have brought an enormous amount of energy and joy into my life. Unfortunately, I have not been able to do things with them as much as I would have liked. Thankfully, though, they understand that we are not always able to do our men s jobs, such as fixing things with our different tools, because daddy must sometimes leave to fix eyes... This work was supported by the Mary and Georg C. Ehrnrooths Foundation, the Finnish Eye Foundation, the Finnish Medical Society Duodecim, the Finnish Eye and Tissue Bank Foundation, the Friends of the Blind Foundation, the Paulo Foundation, and State EVO grants. Helsinki, January 2008 Ilpo S. Tuisku 59
60 REFERENCES: Acosta MC, Tan ME, Belmonte C, Gallar J. Sensations evoked by selective mechanical, chemical, and thermal stimulation of the conjunctiva and cornea. Invest Ophthalmol Vis Sci 2001;42: Albers KM, Wright DE, Davis BM. Overexpression of nerve growth factor in epidermis of transgenic mice causes hypertrophy of the peripheral nervous system. J Neurosci 1994;14: Albietz JM, Lenton LM, McLennan SG. Effect of laser in situ keratomileusis for hyperopia on tear film and ocular surface. J Refract Surg 2002;18: Albietz JM, Lenton LM. Management of the ocular surface and tear film before, during, and after laser in situ keratomileusis. J Refract Surg 2004a;20: Albietz JM, Lenton LM, McLennan SG. Chronic dry eye and regression after laser in situ keratomileusis for myopia. J Cataract Refract Surg 2004b;30: Albietz JM, Lenton LM, McLennan SG. Dry eye after LASIK: comparison of outcomes for Asian and Caucasian eyes. Clin Exp Optom 2005;88: Ambrosio R, Tervo T, Wilson SE. LASIK associated dry eye and neurotrophic epitheliopathy: Pathophysiology and strategies to prevention and treatment. J Refract Surg In Press. Andresen JL, Ledet T, Ehlers N. Keratocyte migration and peptide growth factors: the effect of PDGF, bfgf, EGF, IGF I, afgf and TGF beta on human keratocyte migration in a collagen gel. Curr Eye Res 1997;16: Andresen JL, Ehlers N. Chemotaxis of human keratocytes is increased by platelet derived growth factor BB, epidermal growth factor, transforming growth factor alpha, acidic fibroblast growth factor, insulin like growth factor I, and transforming growth factor beta. Curr Eye Res 1998;17: Ang RT, Dartt DA, Tsubota K. Dry eye after refractive surgery. Curr Opin Ophthalmol 2001;12: Apfel SC. Neurotrophic factors and pain. Clin J Pain 2000;16:S7 11. Araki K, Ohashi Y, Kinoshita S, Hayashi K, Kuwayama Y, Tano Y. Epithelial wound healing in the denervated cornea. Curr Eye Res 1994;13: Auran JD, Koester CJ, Kleiman NJ, Rapaport R, Bomann JS, Wirotsko BM, Florakis GJ, Koniarek JP. Scanning slit confocal microscopic observation of cell morphology and movement within the normal human anterior cornea. Ophthalmology 1995;102: Avunduk AM, Senft CJ, Emerah S, Varnell ED, Kaufman HE. Corneal healing after uncomplicated LASIK and its relationship to refractive changes: a six month prospective confocal study. Invest Ophthalmol Vis Sci 2004;45: Barendregt PJ, van den Bent MJ, van Raaij van den Aarssen VJ, van den Meiracker AH, Vecht CJ, van der Heijde GL, Markusse HM. Involvement of the peripheral nervous system in primary Sjogren's syndrome. Ann Rheum Dis 2001;60: Bargagna Mohan P, Strissel KJ, Fini ME. Regulation of gelatinase B production in corneal cells is independent of autocrine IL 1alpha. Invest Ophthalmol Vis Sci 1999;40: Battat L, Macri A, Dursun D, Pflugfelder SC. Effects of laser in situ keratomileusis on tear production, clearance, and the ocular surface. Ophthalmology 2001;108: Belmonte C, Acosta MC, Schmelz M, Gallar J. Measurement of corneal sensitivity to mechanical and chemical stimulation with a CO2 esthesiometer. Invest Ophthalmol Vis Sci 1999;40:
61 Belmonte C, Acosta MC, Gallar J. Neural basis of sensation in intact and injured corneas. Exp Eye Res 2004;78: Belmonte C and Tervo T. Pain in and around the eye. In Wall&Melzack s Textbook of Pain: Kimber T (Ed). Elsevier ISBN Chapter 57, Benitez del Castillo JM, del Rio T, Iradier T, Hernandez JL, Castillo A, Garcia Sanchez J. Decrease in tear secretion and corneal sensitivity after laser in situ keratomileusis. Cornea 2001;20: Benitez del Castillo JM, Acosta MC, Wassfi MA, Diaz Valle D, Gegundez JA, Fernandez C, Garcia Sanchez J. Relation between corneal innervation with confocal microscopy and corneal sensitivity with noncontact esthesiometry in patients with dry eye. Invest Ophthalmol Vis Sci 2007;48: Benitez del Castillo JM, Wasfy MA, Fernandez C, Garcia Sanchez J. An in vivo confocal masked study on corneal epithelium and subbasal nerves in patients with dry eye. Invest Ophthalmol Vis Sci 2004;45: Beuerman RW, Schimmelpfennig B. Sensory denervation of the rabbit cornea affects epithelial properties. Exp Neurol 1980;69: Beuerman RW, Rozsa AJ. Collateral sprouts are replaced by regenerating neurites in the wounded corneal epithelium. Neurosci Lett 1984;44: Bohnke M, Thaer A, Schipper I. Confocal microscopy reveals persisting stromal changes after myopic photorefractive keratectomy in zero haze corneas. Br J Ophthalmol 1998;82: Botelho SY. Tears and the lacrimal gland. Sci Am 1964;211: Botelho SY, Hisada M, Fuenmayor N. Functional innervation of the lacrimal gland in the cat. Origin of secretomotor fibers in the lacrimal nerve. Arch Ophthalmol 1966;76: Bourcier T, Acosta MC, Borderie V, Borras F, Gallar J, Bury T, Laroche L, Belmonte C. Decreased corneal sensitivity in patients with dry eye. Invest Ophthalmol Vis Sci 2005;46: Bragheeth MA, Dua HS. Corneal sensation after myopic and hyperopic LASIK: clinical and confocal microscopic study. Br J Ophthalmol 2005;89: Bron AJ. Vortex patterns of the corneal epithelium. Trans Ophthalmol Soc U K 1973;93: Bron AJ. Diagnosis of dry eye. Surv Ophthalmol 2001;45 Suppl 2:S221 S226. Calvillo MP, McLaren JW, Hodge DO, Bourne WM. Corneal reinnervation after LASIK: prospective 3 year longitudinal study. Invest Ophthalmol Vis Sci 2004;45: Campos M, Szerenyi K, Lee M, McDonnell JM, Lopez PF, McDonnell PJ. Keratocyte loss after corneal deepithelialization in primates and rabbits. Arch Ophthalmol 1994;112: Chuck RS, Quiros PA, Perez AC, McDonnell PJ. Corneal sensation after laser in situ keratomileusis. J Cataract Refract Surg 2000;26: Corbett MC, Prydal JI, Verma S, Oliver KM, Pande M, Marshall J. An in vivo investigation of the structures responsible for corneal haze after photorefractive keratectomy and their effect on visual function. Ophthalmology 1996;103: De Paiva CS, Pflugfelder SC. Corneal epitheliopathy of dry eye induces hyperesthesia to mechanical air jet stimulation. Am J Ophthalmol 2004;137: De Paiva CS, Chen Z, Koch DD, Hamill MB, Manuel FK, Hassan SS, Wilhelmus KR, Pflugfelder SC. The incidence and risk factors for developing dry eye after myopic LASIK. Am J Ophthalmol 2006;141:
62 Del Pero RA, Gigstad JE, Roberts AD, Klintworth GK, Martin CA, L'Esperance FA, Jr., Taylor DM. A refractive and histopathologic study of excimer laser keratectomy in primates. Am J Ophthalmol 1990;109: Dogru M, Stern ME, Smith JA, Foulks GN, Lemp MA, Tsubota K. Changing trends in the definition and diagnosis of dry eyes. Am J Ophthalmol 2005;140: Dohlman CH, Gasset AR, Rose J. The effect of the absence of corneal epithelium or endothelium on the stromal keratocytes. Invest Ophthalmol 1968;7: Donnenfeld ED, Solomon K, Perry HD, Doshi SJ, Ehrenhaus M, Solomon R, Biser S. The effect of hinge position on corneal sensation and dry eye after LASIK. Ophthalmology 2003;110: Donnenfeld ED, Ehrenhaus M, Solomon R, Mazurek J, Rozell JC, Perry HD. Effect of hinge width on corneal sensation and dry eye after laser in situ keratomileusis. J Cataract Refract Surg 2004;30: Doughty MJ, Zaman ML. Human corneal thickness and its impact on intraocular pressure measures: a review and meta analysis approach. Surv Ophthalmol 2000;44: Dua HS, Azuara Blanco A. Limbal stem cells of the corneal epithelium. Surv Ophthalmol 2000;44: Duffey RJ, Leaming D. US trends in refractive surgery: 2004 ISRS/AAO Survey. J Refract Surg 2005;21: Ehlers N. Some comparative studies on the mammalian corneal epithelium. Acta Ophthalmol (Copenh) 1970;48: Erie JC, McLaren JW, Hodge DO, Bourne WM. The effect of age on the corneal subbasal nerve plexus. Cornea 2005a;24: Erie JC, McLaren JW, Hodge DO, Bourne WM. Recovery of corneal subbasal nerve density after PRK and LASIK. Am J Ophthalmol 2005b;140: Fini ME, Girard MT, Matsubara M, Bartlett JD. Unique regulation of the matrix metalloproteinase, gelatinase B. Invest Ophthalmol Vis Sci 1995;36: Fini ME, Stramer BM. How the cornea heals: cornea specific repair mechanisms affecting surgical outcomes. Cornea 2005;24:S2 S11. Fox RI, Stern M, Michelson P. Update in Sjogren syndrome. Curr Opin Rheumatol 2000;12: Fox RI, Stern M. Sjogren's syndrome: mechanisms of pathogenesis involve interaction of immune and neurosecretory systems. Scand J Rheumatol Suppl 2002;3 13. Frueh BE, Cadez R, Bohnke M. In vivo confocal microscopy after photorefractive keratectomy in humans. A prospective, long term study. Arch Ophthalmol 1998;116: Fujikawa LS, Foster CS, Gipson IK, Colvin RB. Basement membrane components in healing rabbit corneal epithelial wounds: immunofluorescence and ultrastructural studies. J Cell Biol 1984;98: Fukiage C, Nakajima T, Takayama Y, Minagawa Y, Shearer TR, Azuma M. PACAP induces neurite outgrowth in cultured trigeminal ganglion cells and recovery of corneal sensitivity after flap surgery in rabbits. Am J Ophthalmol 2007;143: Gallar J, Acosta MC, Moilanen JA, Holopainen JM, Belmonte C, Tervo TM. Recovery of corneal sensitivity to mechanical and chemical stimulation after laser in situ keratomileusis. J Refract Surg 2004;20: Gao J, Gelber Schwalb TA, Addeo JV, Stern ME. Apoptosis in the rabbit cornea after photorefractive keratectomy. Cornea 1997;16: Gartry DS, Kerr Muir MG, Marshall J. Excimer laser photorefractive keratectomy. 18 month follow up. Ophthalmology 1992;99:
63 Gemignani F, Marbini A, Pavesi G, Di VS, Manganelli P, Cenacchi G, Mancia D. Peripheral neuropathy associated with primary Sjogren's syndrome. J Neurol Neurosurg Psychiatry 1994;57: Ghoreishi M, Aidenloo NS, Peyman A, Peyman M, Haghdoustoskoey M. Does hinge position affect dry eye after laser in situ keratomileusis? Ophthalmologica 2005;219: Gillette TE, Chandler JW, Greiner JV. Langerhans cells of the ocular surface. Ophthalmology 1982;89: Gimbel HV, DeBroff BM, Beldavs RA, van Westenbrugge JA, Ferensowicz M. Comparison of laser and manual removal of corneal epithelium for photorefractive keratectomy. J Refract Surg 1995;11: Gipson IK, Spurr Michaud S, Tisdale A, Keough M. Reassembly of the anchoring structures of the corneal epithelium during wound repair in the rabbit. Invest Ophthalmol Vis Sci 1989;30: Girard MT, Matsubara M, Fini ME. Transforming growth factor beta and interleukin 1 modulate metalloproteinase expression by corneal stromal cells. Invest Ophthalmol Vis Sci 1991;32: Gould HJ, III, Gould TN, England JD, Paul D, Liu ZP, Levinson SR. A possible role for nerve growth factor in the augmentation of sodium channels in models of chronic pain. Brain Res 2000;854: Griffin JW, Cornblath DR, Alexander E, Campbell J, Low PA, Bird S, Feldman EL. Ataxic sensory neuropathy and dorsal root ganglionitis associated with Sjogren's syndrome. Ann Neurol 1990;27: Grupcheva CN, Wong T, Riley AF, McGhee CN. Assessing the sub basal nerve plexus of the living healthy human cornea by in vivo confocal microscopy. Clin Experiment Ophthalmol 2002;30: Gupta A, Monroy D, Ji Z, Yoshino K, Huang A, Pflugfelder SC. Transforming growth factor beta 1 and beta 2 in human tear fluid. Curr Eye Res 1996;15: Hakala M, Niemela RK. Does autonomic nervous impairment have a role in pathophysiology of Sjogren's syndrome. Lancet 2000;355: Hamrah P, Zhang Q, Liu Y, Dana MR. Novel characterization of MHC class II negative population of resident corneal Langerhans cell type dendritic cells. Invest Ophthalmol Vis Sci 2002;43: Hamrah P, Liu Y, Zhang Q, Dana MR. The corneal stroma is endowed with a significant number of resident dendritic cells. Invest Ophthalmol Vis Sci 2003a;44: Hamrah P, Liu Y, Zhang Q, Dana MR. Alterations in corneal stromal dendritic cell phenotype and distribution in inflammation. Arch Ophthalmol 2003b;121: Hanna C, O'Brien JE. Cell production and migration in the epithelial layer of the cornea. Arch Ophthalmol 1960;64: Hanna KD, Pouliquen Y, Waring GO, III, Savoldelli M, Cotter J, Morton K, Menasche M. Corneal stromal wound healing in rabbits after 193 nm excimer laser surface ablation. Arch Ophthalmol 1989;107: Hargrave SL, Jung JC, Fini ME, Gelender H, Cather C, Guidera A, Udell I, Fisher S, Jester JV, Bowman RW, McCulley JP, Cavanagh HD. Possible role of the vitamin E solubilizer in topical diclofenac on matrix metalloproteinase expression in corneal melting: an analysis of postoperative keratolysis. Ophthalmology 2002;109: Hasan W, Zhang R, Liu M, Warn JD, Smith PG. Coordinate expression of NGF and alpha smooth muscle actin mrna and protein in cutaneous wound tissue of developing and adult rats. Cell Tissue Res 2000;300: Heinz P, Bodanowitz S, Wiegand W, Kroll P. In vivo observation of corneal nerve regeneration after photorefractive keratectomy with a confocal videomicroscope. Ger J Ophthalmol 1996;5: Helena MC, Baerveldt F, Kim WJ, Wilson SE. Keratocyte apoptosis after corneal surgery. Invest Ophthalmol Vis Sci 1998;39:
64 Herrmann H, Lebeau PL. ATP level, cell injury, and apparent epithelium stroma interaction in the cornea. J Cell Biol 1962;13: Hietaharju A, Yli Kerttula U, Hakkinen V, Frey H. Nervous system manifestations in Sjogren's syndrome. Acta Neurol Scand 1990;81: Hong JW, Kim HM. The changes of tear break up time after myopic excimer laser photorefractive keratectomy. Korean J Ophthalmol 1997;11: Hoppenreijs VP, Pels E, Vrensen GF, Felten PC, Treffers WF. Platelet derived growth factor: receptor expression in corneas and effects on corneal cells. Invest Ophthalmol Vis Sci 1993;34: Hovanesian JA, Shah SS, Maloney RK. Symptoms of dry eye and recurrent erosion syndrome after refractive surgery. J Cataract Refract Surg 2001;27: Ihanamaki T, Pelliniemi LJ, Vuorio E. Collagens and collagen related matrix components in the human and mouse eye. Prog Retin Eye Res 2004;23: Ishikawa T, del Cerro M, Liang FQ, Loya N, Aquavella JV. Corneal sensitivity and nerve regeneration after excimer laser ablation. Cornea 1994;13: Imai S, Tokunaga Y, Konttinen YT, Maeda T, Hukuda S, Santavirta S. Ultrastructure of the synovial sensory peptidergic fibers is distinctively altered in different phases of adjuvant induced arthritis in rats: ultramorphological characterization combined with morphometric and immunohistochemical study for substance P, calcitonin gene related peptide, and protein gene product 9.5. J Rheumatol 1997;24: Jester JV, Petroll WM, Barry PA, Cavanagh HD. Expression of alpha smooth muscle (alpha SM) actin during corneal stromal wound healing. Invest Ophthalmol Vis Sci 1995;36: Jester JV, Barry Lane PA, Cavanagh HD, Petroll WM. Induction of alpha smooth muscle actin expression and myofibroblast transformation in cultured corneal keratocytes. Cornea 1996;15: Jester JV, Barry Lane PA, Petroll WM, Olsen DR, Cavanagh HD. Inhibition of corneal fibrosis by topical application of blocking antibodies to TGF beta in the rabbit. Cornea 1997;16: Jester JV, Huang J, Barry Lane PA, Kao WW, Petroll WM, Cavanagh HD. Transforming growth factor(beta) mediated corneal myofibroblast differentiation requires actin and fibronectin assembly. Invest Ophthalmol Vis Sci 1999;40: Jester JV, Petroll WM, Cavanagh HD. Corneal stromal wound healing in refractive surgery: the role of myofibroblasts. Prog Retin Eye Res 1999;18: Jester JV, Huang J, Petroll WM, Cavanagh HD. TGFbeta induced myofibroblast differentiation of rabbit keratocytes requires synergistic TGFbeta, PDGF and integrin signaling. Exp Eye Res 2002;75: Jester JV, Huang J, Fisher S, Spiekerman J, Chang JH, Wright WE, Shay JW. Myofibroblast differentiation of normal human keratocytes and htert, extended life human corneal fibroblasts. Invest Ophthalmol Vis Sci 2003;44: Johnson DH, Bourne WM, Campbell RJ. The ultrastructure of Descemet's membrane. I. Changes with age in normal corneas. Arch Ophthalmol 1982;100: Jones MA, Marfurt CF. Peptidergic innervation of the rat cornea. Exp Eye Res 1998;66: Jones SM, Kazlauskas A. Growth factor dependent signaling and cell cycle progression. FEBS Lett 2001;490: Joo MJ, Yuhan KR, Hyon JY, Lai H, Hose S, Sinha D, O'Brien TP. The effect of nerve growth factor on corneal sensitivity after laser in situ keratomileusis. Arch Ophthalmol 2004;122:
65 Kaltreider HB, Talal N. The neuropathy of Sjogren's syndrome. Trigeminal nerve involvement. Ann Intern Med 1969;70: Kamiyama K, Iguchi I, Wang X, Imanishi J. Effects of PDGF on the migration of rabbit corneal fibroblasts and epithelial cells. Cornea 1998;17: Kaplan JG, Rosenberg R, Reinitz E, Buchbinder S, Schaumburg HH. Invited review: peripheral neuropathy in Sjogren's syndrome. Muscle Nerve 1990;13: Kauffmann T, Bodanowitz S, Hesse L, Kroll P. Corneal reinnervation after photorefractive keratectomy and laser in situ keratomileusis: an in vivo study with a confocal videomicroscope. Ger J Ophthalmol 1996;5: Kaye DB. Epithelial response in penetrating keratoplasty. Am J Ophthalmol 1980;89: Kim WJ, Mohan RR, Mohan RR, Wilson SE. Effect of PDGF, IL 1alpha, and BMP2/4 on corneal fibroblast chemotaxis: expression of the platelet derived growth factor system in the cornea. Invest Ophthalmol Vis Sci 1999;40: Kim WS, Kim JS. Change in corneal sensitivity following laser in situ keratomileusis. J Cataract Refract Surg 1999;25: Kokawa N, Sotozono C, Nishida K, Kinoshita S. High total TGF beta 2 levels in normal human tears. Curr Eye Res 1996;15: Komai Y, Ushiki T. The three dimensional organization of collagen fibrils in the human cornea and sclera. Invest Ophthalmol Vis Sci 1991;32: Kruse FE, Chen JJ, Tsai RJ, Tseng SC. Conjunctival transdifferentiation is due to the incomplete removal of limbal basal epithelium. Invest Ophthalmol Vis Sci 1990;31: Kumano Y, Matsui H, Zushi I, Mawatari A, Matsui T, Nishida T, Miyazaki M. Recovery of corneal sensation after myopic correction by laser in situ keratomileusis with a nasal or superior hinge. J Cataract Refract Surg 2003;29: Lambiase A, Manni L, Bonini S, Rama P, Micera A, Aloe L. Nerve growth factor promotes corneal healing: structural, biochemical, and molecular analyses of rat and human corneas. Invest Ophthalmol Vis Sci 2000;41: Latvala T, Linna T, Tervo T. Corneal nerve recovery after photorefractive keratectomy and laser in situ keratomileusis. Int Ophthalmol Clin 1996;36: Lee BH, McLaren JW, Erie JC, Hodge DO, Bourne WM. Reinnervation in the cornea after LASIK. Invest Ophthalmol Vis Sci 2002;43: Lee HK, Lee KS, Kim HC, Lee SH, Kim EK. Nerve growth factor concentration and implications in photorefractive keratectomy vs laser in situ keratomileusis. Am J Ophthalmol 2005;139: Lee HK, Ryu IH, Seo KY, Hong S, Kim HC, Kim EK. Topical 0.1% prednisolone lowers nerve growth factor expression in keratoconjunctivitis sicca patients. Ophthalmology 2006;113: Lemp MA, Mathers WD. Corneal epithelial cell movement in humans. Eye 1989;3 ( Pt 4): Lemp MA. Report of the National Eye Institute/Industry workshop on Clinical Trials in Dry Eyes. CLAO J 1995;21: Lemp MA and the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007;5:
66 Lenton LM, Albietz JM. Effect of carmellose based artificial tears on the ocular surface in eyes after laser in situ keratomileusis. J Refract Surg 1999;15:S227 S231. Lewin GR, Ritter AM, Mendell LM. Nerve growth factor induced hyperalgesia in the neonatal and adult rat. J Neurosci 1993;13: Li DQ, Tseng SC. Differential regulation of cytokine and receptor transcript expression in human corneal and limbal fibroblasts by epidermal growth factor, transforming growth factor alpha, platelet derived growth factor B, and interleukin 1 beta. Invest Ophthalmol Vis Sci 1996;37: Li DQ, Tseng SC. Differential regulation of keratinocyte growth factor and hepatocyte growth factor/scatter factor by different cytokines in human corneal and limbal fibroblasts. J Cell Physiol 1997;172: Li HF, Petroll WM, Moller Pedersen T, Maurer JK, Cavanagh HD, Jester JV. Epithelial and corneal thickness measurements by in vivo confocal microscopy through focusing (CMTF). Curr Eye Res 1997;16: Li W, Hayashida Y, Chen YT, Tseng SC. Niche regulation of corneal epithelial stem cells at the limbus. Cell Res 2007;17: Linna T, Tervo T. Real time confocal microscopic observations on human corneal nerves and wound healing after excimer laser photorefractive keratectomy. Curr Eye Res 1997;16: Linna TU, Perez Santonja JJ, Tervo KM, Sakla HF, Sanz JL, Tervo TM. Recovery of corneal nerve morphology following laser in situ keratomileusis. Exp Eye Res 1998;66: Linna TU, Vesaluoma MH, Perez Santonja JJ, Petroll WM, Alio JL, Tervo TM. Effect of myopic LASIK on corneal sensitivity and morphology of subbasal nerves. Invest Ophthalmol Vis Sci 2000;41: Maldonado BA, Furcht LT. Epidermal growth factor stimulates integrin mediated cell migration of cultured human corneal epithelial cells on fibronectin and arginine glycine aspartic acid peptide. Invest Ophthalmol Vis Sci 1995;36: Mastropasqua L, Nubile M, Lanzini M, Carpineto P, Ciancaglini M, Pannellini T, Di NM, Dua HS. Epithelial dendritic cell distribution in normal and inflamed human cornea: in vivo confocal microscopy study. Am J Ophthalmol 2006;142: Matsui H, Kumano Y, Zushi I, Yamada T, Matsui T, Nishida T. Corneal sensation after correction of myopia by photorefractive keratectomy and laser in situ keratomileusis. J Cataract Refract Surg 2001;27: McDonald MB, Deitz MR, Frantz JM, Kraff MC, Krueger RR, Salz JJ, Kraff CR, Maguen E, Matta CS, Nesburn AB, Piebenga LW. Photorefractive keratectomy for low to moderate myopia and astigmatism with a small beam, tracker directed excimer laser. Ophthalmology 1999;106: McDonald MB, Carr JD, Frantz JM, Kozarsky AM, Maguen E, Nesburn AB, Rabinowitz YS, Salz JJ, Stulting RD, Thompson KP, Waring GO, III. Laser in situ keratomileusis for myopia up to 11 diopters with up to 5 diopters of astigmatism with the summit autonomous LADARVision excimer laser system. Ophthalmology 2001;108: Mellgren SI, Conn DL, Stevens JC, Dyck PJ. Peripheral neuropathy in primary Sjogren's syndrome. Neurology 1989;39: Michaeli A, Slomovic AR, Sakhichand K, Rootman DS. Effect of laser in situ keratomileusis on tear secretion and corneal sensitivity. J Refract Surg 2004;20: Millodot M, Larson W. New measurements of corneal sensitivity: a preliminary report. Am J Optom Arch Am Acad Optom 1969;46: Millodot M. The influence of age onthe sensitivity of the cornea. Invest Ophthalmol Vis Sci 1977;16:
67 Mohan RR, Liang Q, Kim WJ, Helena MC, Baerveldt F, Wilson SE. Apoptosis in the cornea: further characterization of Fas/Fas ligand system. Exp Eye Res 1997;65: Moilanen JA, Vesaluoma MH, Muller LJ, Tervo TM. Long term corneal morphology after PRK by in vivo confocal microscopy. Invest Ophthalmol Vis Sci 2003;44: Moller Pedersen T, Vogel M, Li HF, Petroll WM, Cavanagh HD, Jester JV. Quantification of stromal thinning, epithelial thickness, and corneal haze after photorefractive keratectomy using in vivo confocal microscopy. Ophthalmology 1997;104: Moller Pedersen T, Li HF, Petroll WM, Cavanagh HD, Jester JV. Confocal microscopic characterization of wound repair after photorefractive keratectomy. Invest Ophthalmol Vis Sci 1998a;39: Moller Pedersen T, Cavanagh HD, Petroll WM, Jester JV. Neutralizing antibody to TGFbeta modulates stromal fibrosis but not regression of photoablative effect following PRK. Curr Eye Res 1998b;17: Muller LJ, Pels L, Vrensen GF. Ultrastructural organization of human corneal nerves. Invest Ophthalmol Vis Sci 1996;37: Muller LJ, Vrensen GF, Pels L, Cardozo BN, Willekens B. Architecture of human corneal nerves. Invest Ophthalmol Vis Sci 1997;38: Muller LJ, Pels E, Vrensen GF. The specific architecture of the anterior stroma accounts for maintenance of corneal curvature. Br J Ophthalmol 2001;85: Muller LJ, Marfurt CF, Kruse F, Tervo TM. Corneal nerves: structure, contents and function. Exp Eye Res 2003;76: Murphy PJ, Lawrenson JG, Patel S, Marshall J. Reliability of the non contact corneal aesthesiometer and its comparison with the Cochet Bonnet aesthesiometer. Ophthalmic Physiol Opt 1998;18: Mustonen RK, McDonald MB, Srivannaboon S, Tan AL, Doubrava MW, Kim CK. In vivo confocal microscopy of Fuchs' endothelial dystrophy. Cornea 1998;17: Myers JS, Gomes JA, Siepser SB, Rapuano CJ, Eagle RC, Jr., Thom SB. Effect of transforming growth factor beta 1 on stromal haze following excimer laser photorefractive keratectomy in rabbits. J Refract Surg 1997;13: Nagasaki T, Zhao J. Centripetal movement of corneal epithelial cells in the normal adult mouse. Invest Ophthalmol Vis Sci 2003;44: Nakamura M, Ofuji K, Chikama T, Nishida T. The NK1 receptor and its participation in the synergistic enhancement of corneal epithelial migration by substance P and insulin like growth factor 1. Br J Pharmacol 1997;120: Nakayasu K. Stromal changes following removal of epithelium in rat cornea. Jpn J Ophthalmol 1988;32: Nassaralla BA, McLeod SD, Nassaralla JJ, Jr. Effect of myopic LASIK on human corneal sensitivity. Ophthalmology 2003;110: Nassaralla BA, McLeod SD, Boteon JE, Nassaralla JJ, Jr. The effect of hinge position and depth plate on the rate of recovery of corneal sensation following LASIK. Am J Ophthalmol 2005;139: Nejima R, Miyata K, Tanabe T, Okamoto F, Hiraoka T, Kiuchi T, Oshika T. Corneal barrier function, tear film stability, and corneal sensation after photorefractive keratectomy and laser in situ keratomileusis. Am J Ophthalmol 2005;139: Niederkorn JY, Stern ME, Pflugfelder SC, De Paiva CS, Corrales RM, Gao J, Siemasko K. Desiccating stress induces T cell mediated Sjogren's Syndrome like lacrimal keratoconjunctivitis. J Immunol 2006;176:
68 Nishida T. Cornea. In Cornea Volume 1: Fundamentals, diagnosis and management. Eds. Krachmer JH, Mannis MJ and Holland EJ. 2005: Elsevier Mosby, London, UK. Niissalo S, Hukkanen M, Imai S, Tornwall J, Konttinen YT. Neuropeptides in experimental and degenerative arthritis. Ann N Y Acad Sci 2002;966: Nikkinen A, Lehtosalo JI, Uusitalo H, Palkama A, Panula P. The lacrimal glands of the rat and the guinea pig are innervated by nerve fibers containing immunoreactivities for substance P and vasoactive intestinal polypeptide. Histochemistry 1984;81: Nishida K, Sotozono C, Adachi W, Yamamoto S, Yokoi N, Kinoshita S. Transforming growth factor beta 1, beta 2 and beta 3 mrna expression in human cornea. Curr Eye Res 1995;14: Ohji M, Sundarraj N, Thoft RA. Transforming growth factor beta stimulates collagen and fibronectin synthesis by human corneal stromal fibroblasts in vitro. Curr Eye Res 1993;12: Oliveira Soto L, Efron N. Morphology of corneal nerves using confocal microscopy. Cornea 2001;20: Olney RK. Neuropathies associated with connective tissue disease. Semin Neurol 1998;18: Pallikaris IG, Papatzanaki ME, Stathi EZ, Frenschock O, Georgiadis A. Laser in situ keratomileusis. Lasers Surg Med 1990;10: Pallikaris IG, Karoutis AD, Lydataki SE, Siganos DS. Rotating brush for fast removal of corneal epithelium. J Refract Corneal Surg 1994;10: Patel DV, McGhee CN. Mapping of the normal human corneal sub basal nerve plexus by in vivo laser scanning confocal microscopy. Invest Ophthalmol Vis Sci 2005;46: Patel DV, McGhee CN. Mapping the Corneal Sub basal Nerve Plexus in Keratoconus by In Vivo Laser Scanning Confocal Microscopy. Invest Ophthalmol Vis Sci 2006;47: Perez Gomez I, Efron N. Change to corneal morphology after refractive surgery (myopic laser in situ keratomileusis) as viewed with a confocal microscope. Optom Vis Sci 2003;80: Perez Santonja JJ, Sakla HF, Cardona C, Chipont E, Alio JL. Corneal sensitivity after photorefractive keratectomy and laser in situ keratomileusis for low myopia. Am J Ophthalmol 1999;127: Petridou S, Maltseva O, Spanakis S, Masur SK. TGF beta receptor expression and smad2 localization are cell density dependent in fibroblasts. Invest Ophthalmol Vis Sci 2000;41: Petroll WM, Cavanagh HD, Jester JV. Clinical confocal microscopy. Curr Opin Ophthalmol 1998;9: Pflugfelder SC, Solomon A, Stern ME. The diagnosis and management of dry eye: a twenty five year review. Cornea 2000;19: Pflugfelder SC. Antiinflammatory therapy for dry eye. Am J Ophthalmol 2004;137: Radner W, Mallinger R. Interlacing of collagen lamellae in the midstroma of the human cornea. Cornea 2002;21: Riley GP, Harrall RL, Watson PG, Cawston TE, Hazleman BL. Collagenase (MMP 1) and TIMP 1 in destructive corneal disease associated with rheumatoid arthritis. Eye 1995;9 ( Pt 6): Rosenberg ME, Tervo TM, Petroll WM, Vesaluoma MH. In vivo confocal microscopy of patients with corneal recurrent erosion syndrome or epithelial basement membrane dystrophy. Ophthalmology 2000;107: Rosenberg ME, Tervo TM, Immonen IJ, Muller LJ, Gronhagen Riska C, Vesaluoma MH. Corneal structure and sensitivity in type 1 diabetes mellitus. Invest Ophthalmol Vis Sci 2000;41:
69 Rosenberg ME, Tervo TM, Gallar J, Acosta MC, Muller LJ, Moilanen JA, Tarkkanen AH, Vesaluoma MH. Corneal morphology and sensitivity in lattice dystrophy type II (familial amyloidosis, Finnish type). Invest Ophthalmol Vis Sci 2001;42: Rosenberg ME, Tervo TM, Muller LJ, Moilanen JA, Vesaluoma MH. In vivo confocal microscopy after herpes keratitis. Cornea 2002;21: Rozsa AJ, Beuerman RW. Density and organization of free nerve endings in the corneal epithelium of the rabbit. Pain 1982;14: Rozsa AJ, Guss RB, Beuerman RW. Neural remodeling following experimental surgery of the rabbit cornea. Invest Ophthalmol Vis Sci 1983;24: Ruskell GL. Ocular fibres of the maxillary nerve in monkeys. J Anat 1974;118: Schiffman RM, Christianson MD, Jacobsen G, Hirsch JD, Reis BL. Reliability and validity of the Ocular Surface Disease Index. Arch Ophthalmol 2000;118: Schimmelpfennig B. Nerve structures in human central corneal epithelium. Graefes Arch Clin Exp Ophthalmol 1982;218: Seiler T, Wollensak J. Myopic photorefractive keratectomy with the excimer laser. One year follow up. Ophthalmology 1991;98: Seiler T, Derse M, Pham T. Repeated excimer laser treatment after photorefractive keratectomy. Arch Ophthalmol 1992;110: Shah S, Chatterjee A, Smith RJ. Predictability of spherical photorefractive keratectomy for myopia. Ophthalmology 1998;105: Shin SY, Lee YJ. Conjunctival changes induced by LASIK suction ring in a rabbit model. Ophthalmic Res 2006;38: Shoja MR, Besharati MR. Dry eye after LASIK for myopia: Incidence and risk factors. Eur J Ophthalmol 2007;17:1 6. Sibony PA, Walcott B, McKeon C, Jakobiec FA. Vasoactive intestinal polypeptide and the innervation of the human lacrimal gland. Arch Ophthalmol 1988;106: Slowik C, Somodi S, Richter A, Guthoff R. Assessment of corneal alterations following laser in situ keratomileusis by confocal slit scanning microscopy. Ger J Ophthalmol 1996;5: Smith JA and the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007;5: Solomon A, Dursun D, Liu Z, Xie Y, Macri A, Pflugfelder SC. Pro and anti inflammatory forms of Interleukin 1 in the tear fluid and conjunctiva of patients with dry eye disease. Invest Ophthalmol Vis Sci 2001;42: Solomon KD, Holzer MP, Sandoval HP, Vargas LG, Werner L, Vroman DT, Kasper TJ, Apple DJ. Refractive Surgery Survey J Cataract Refract Surg 2002;28: Song QH, Klepeis VE, Nugent MA, Trinkaus Randall V. TGF beta1 regulates TGF beta1 and FGF 2 mrna expression during fibroblast wound healing. Mol Pathol 2002;55: Stapleton F, Hayward KB, Bachand N, Trong PH, Teh DW, Deng KM, Yang EI, Kelly SL, Lette M, Robinson D. Evaluation of Corneal Sensitivity to Mechanical and Chemical Stimuli After LASIK: A Pilot Study. Eye Contact Lens 2006;32:
70 Stern ME, Gao J, Siemasko KF, Beuerman RW, Pflugfelder SC. The role of the lacrimal functional unit in the pathophysiology of dry eye. Exp Eye Res 2004;78: Stone RA, Kuwayama Y, Laties AM, McGlinn AM, Schmidt ML. Guinea pig ocular nerves contain a peptide of the cholecystokinin/gastrin family. Exp Eye Res 1984;39: Stone RA, Kuwayama Y, Terenghi G, Polak JM. Calcitonin gene related peptide: occurrence in corneal sensory nerves. Exp Eye Res 1986;43: Stramer BM, Zieske JD, Jung JC, Austin JS, Fini ME. Molecular mechanisms controlling the fibrotic repair phenotype in cornea: implications for surgical outcomes. Invest Ophthalmol Vis Sci 2003;44: Streppel M, Azzolin N, Dohm S, Guntinas Lichius O, Haas C, Grothe C, Wevers A, Neiss WF, Angelov DN. Focal application of neutralizing antibodies to soluble neurotrophic factors reduces collateral axonal branching after peripheral nerve lesion. Eur J Neurosci 2002;15: Sugar A, Rapuano CJ, Culbertson WW, Huang D, Varley GA, Agapitos PJ, de L, V, Koch DD. Laser in situ keratomileusis for myopia and astigmatism: safety and efficacy: a report by the American Academy of Ophthalmology. Ophthalmology 2002;109: Suzuki K, Saito J, Yanai R, Yamada N, Chikama T, Seki K, Nishida T. Cell matrix and cell cell interactions during corneal epithelial wound healing. Prog Retin Eye Res 2003;22: Tajima Y, Mito Y, Owada Y, Tsukishima E, Moriwaka F, Tashiro K. Neurological manifestations of primary Sjogren's syndrome in Japanese patients. Intern Med 1997;36: Tervo K, Tervo T, Eranko L, Vannas A, Cuello AC, Eranko O. Substance P immunoreactive nerves in the human cornea and iris. Invest Ophthalmol Vis Sci 1982;23: Tervo K, Latvala TM, Tervo TM. Recovery of corneal innervation following photorefractive keratoablation. Arch Ophthalmol 1994;112: Tervo T, Vesaluoma M, Bennett GL, Schwall R, Helena M, Liang Q, Wilson SE. Tear hepatocyte growth factor (HGF) availability increases markedly after excimer laser surface ablation. Exp Eye Res 1997;64: Tervo T, Moilanen J. In vivo confocal microscopy for evaluation of wound healing following corneal refractive surgery. Prog Retin Eye Res 2003;22: Thoft RA, Friend J. The X, Y, Z hypothesis of corneal epithelial maintenance. Invest Ophthalmol Vis Sci 1983;24: Thompson HW, Beuerman RW, Cook J, Underwood LW, Nguyen DH. Transcription of message for tumor necrosis factor alpha by lacrimal gland is regulated by corneal wounding. Adv Exp Med Biol 1994;350: Tishler M, Yaron I, Geyer O, Shirazi I, Naftaliev E, Yaron M. Elevated tear interleukin 6 levels in patients with Sjogren syndrome. Ophthalmology 1998;105: Toda I, sano Kato N, Komai Hori Y, Tsubota K. Dry eye after laser in situ keratomileusis. Am J Ophthalmol 2001;132:1 7. Toivanen M, Tervo T, Partanen M, Vannas A, Hervonen A. Histochemical demonstration of adrenergic nerves in the stroma of human cornea. Invest Ophthalmol Vis Sci 1987;28: Trabucchi G, Brancato R, Verdi M, Carones F, Sala C. Corneal nerve damage and regeneration after excimer laser photokeratectomy in rabbit eyes. Invest Ophthalmol Vis Sci 1994;35: Trokel SL, Srinivasan R, Braren B. Excimer laser surgery of the cornea. Am J Ophthalmol 1983;96: Tseng SC. Concept and application of limbal stem cells. Eye 1989;3 ( Pt 2):
71 Tsubota K, Xu KP, Fujihara T, Katagiri S, Takeuchi T. Decreased reflex tearing is associated with lymphocytic infiltration in lacrimal glands. J Rheumatol 1996;23: Tsukahara S, Jacobowitz DM. Peptidergic innervation of the rat Harderian gland. Histochemistry 1987;87: Uddman R, Alumets J, Ehinger B, Hakanson R, Loren I, Sundler F. Vasoactive intestinal peptide nerves in ocular and orbital structures of the cat. Invest Ophthalmol Vis Sci 1980;19: Valls Sole J, Graus F, Font J, Pou A, Tolosa ES. Normal proprioceptive trigeminal afferents in patients with Sjogren's syndrome and sensory neuronopathy. Ann Neurol 1990;28: van Setten GB. Epidermal growth factor in human tear fluid: increased release but decreased concentrations during reflex tearing. Curr Eye Res 1990;9: Vesaluoma M, Teppo AM, Gronhagen Riska C, Tervo T. Release of TGF beta 1 and VEGF in tears following photorefractive keratectomy. Curr Eye Res 1997a;16: Vesaluoma M, Teppo AM, Gronhagen Riska C, Tervo T. Increased release of tumour necrosis factor alpha in human tear fluid after excimer laser induced corneal wound. Br J Ophthalmol 1997b;81: Vesaluoma M, Teppo AM, Gronhagen Riska C, Tervo T. Platelet derived growth factor BB (PDGF BB) in tear fluid: a potential modulator of corneal wound healing following photorefractive keratectomy. Curr Eye Res 1997c;16: Vesaluoma MH, Sankila EM, Gallar J, Muller LJ, Petroll WM, Moilanen JA, Forsius H, Tervo TM. Autosomal recessive cornea plana: in vivo corneal morphology and corneal sensitivity. Invest Ophthalmol Vis Sci 2000;41: Villani E, Galimberti D, Viola F, Mapelli C, Ratiglia R. The cornea in Sjogren's syndrome: an in vivo confocal study. Invest Ophthalmol Vis Sci 2007;48: Virtanen T, Ylatupa S, Mertaniemi P, Partanen P, Tuunanen T, Tervo T. Tear fluid cellular fibronectin levels after photorefractive keratectomy. J Refract Surg 1995;11: Vitali C, Bombardieri S, Jonsson R, Moutsopoulos HM, Alexander EL, Carsons SE, Daniels TE, Fox PC, Fox RI, Kassan SS, Pillemer SR, Talal N, Weisman MH. Classification criteria for Sjogren's syndrome: a revised version of the European criteria proposed by the American European Consensus Group. Ann Rheum Dis 2002;61: Vroman DT, Sandoval HP, Fernandez de Castro LE, Kasper TJ, Holzer MP, Solomon KD. Effect of hinge location on corneal sensation and dry eye after laser in situ keratomileusis for myopia. J Cataract Refract Surg 2005;31: West Mays JA, Sadow PM, Tobin TW, Strissel KJ, Cintron C, Fini ME. Repair phenotype in corneal fibroblasts is controlled by an interleukin 1 alpha autocrine feedback loop. Invest Ophthalmol Vis Sci 1997;38: West Mays JA, Cook JR, Sadow PM, Mullady DK, Bargagna Mohan P, Strissel KJ, Fini ME. Differential inhibition of collagenase and interleukin 1alpha gene expression in cultured corneal fibroblasts by TGF beta, dexamethasone, and retinoic acid. Invest Ophthalmol Vis Sci 1999;40: Wilson SE, He YG, Lloyd SA. EGF, EGF receptor, basic FGF, TGF beta 1, and IL 1 alpha mrna in human corneal epithelial cells and stromal fibroblasts. Invest Ophthalmol Vis Sci 1992;33: Wilson SE, Walker JW, Chwang EL, He YG. Hepatocyte growth factor, keratinocyte growth factor, their receptors, fibroblast growth factor receptor 2, and the cells of the cornea. Invest Ophthalmol Vis Sci 1993;34: Wilson SE, Lloyd SA, He YG. Glucocorticoid receptor and interleukin 1 receptor messenger RNA expression in corneal cells. Cornea 1994a;13:
72 Wilson SE, Schultz GS, Chegini N, Weng J, He YG. Epidermal growth factor, transforming growth factor alpha, transforming growth factor beta, acidic fibroblast growth factor, basic fibroblast growth factor, and interleukin 1 proteins in the cornea. Exp Eye Res 1994b;59: Wilson SE, He YG, Weng J, Zieske JD, Jester JV, Schultz GS. Effect of epidermal growth factor, hepatocyte growth factor, and keratinocyte growth factor, on proliferation, motility and differentiation of human corneal epithelial cells. Exp Eye Res 1994c;59: Wilson SE, He YG, Weng J, Li Q, McDowall AW, Vital M, Chwang EL. Epithelial injury induces keratocyte apoptosis: hypothesized role for the interleukin 1 system in the modulation of corneal tissue organization and wound healing. Exp Eye Res 1996a;62: Wilson SE, Li Q, Weng J, Barry Lane PA, Jester JV, Liang Q, Wordinger RJ. The Fas Fas ligand system and other modulators of apoptosis in the cornea. Invest Ophthalmol Vis Sci 1996b;37: Wilson SE, Chen L, Mohan RR, Liang Q, Liu J. Expression of HGF, KGF, EGF and receptor messenger RNAs following corneal epithelial wounding. Exp Eye Res 1999;68: Wilson SE, Liang Q, Kim WJ. Lacrimal gland HGF, KGF, and EGF mrna levels increase after corneal epithelial wounding. Invest Ophthalmol Vis Sci 1999;40: Wilson SE. Laser in situ keratomileusis induced (presumed) neurotrophic epitheliopathy. Ophthalmology 2001;108: Wilson SE, Ambrosio R. Laser in situ keratomileusis induced neurotrophic epitheliopathy. Am J Ophthalmol 2001;132: Wilson SE, Mohan RR, Mohan RR, Ambrosio R, Jr., Hong J, Lee J. The corneal wound healing response: cytokine mediated interaction of the epithelium, stroma, and inflammatory cells. Prog Retin Eye Res 2001;20: Xu KP, Yagi Y, Tsubota K. Decrease in corneal sensitivity and change in tear function in dry eye. Cornea 1996;15: Yoshino K, Garg R, Monroy D, Ji Z, Pflugfelder SC. Production and secretion of transforming growth factor beta (TGF beta) by the human lacrimal gland. Curr Eye Res 1996;15: You L, Kruse FE, Volcker HE. Neurotrophic factors in the human cornea. Invest Ophthalmol Vis Sci 2000;41: Zander E, Weddell G. Observations on the innervation of the cornea. J Anat 1951;85: Zhang M, Chen J, Luo L, Xiao Q, Sun M, Liu Z. Altered corneal nerves in aqueous tear deficiency viewed by in vivo confocal microscopy. Cornea 2005;24: Zhivov A, Stave J, Vollmar B, Guthoff R. In vivo confocal microscopic evaluation of Langerhans cell density and distribution in the normal human corneal epithelium. Graefes Arch Clin Exp Ophthalmol 2005;243: Zhivov A, Stave J, Vollmar B, Guthoff R. In vivo confocal microscopic evaluation of langerhans cell density and distribution in the corneal epithelium of healthy volunteers and contact lens wearers. Cornea 2007;26: Zieske JD, Guimaraes SR, Hutcheon AE. Kinetics of keratocyte proliferation in response to epithelial debridement. Exp Eye Res 2001;72: Zoukhri D, Hodges RR, Rawe IM, Dartt DA. Ca2+ signaling by cholinergic and alpha1 adrenergic agonists is upregulated in lacrimal and submandibular glands in a murine model of Sjogren's syndrome. Clin Immunol Immunopathol 1998a;89: Zoukhri D, Hodges RR, Dartt DA. Lacrimal gland innervation is not altered with the onset and progression of disease in a murine model of Sjogren's syndrome. Clin Immunol Immunopathol 1998b;89:
73 Zoukhri D, Kublin CL. Impaired neurotransmitter release from lacrimal and salivary gland nerves of a murine model of Sjogren's syndrome. Invest Ophthalmol Vis Sci 2001;42:
Overview of Refractive Surgery
 Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Overview of Refractive Surgery Michael N. Wiggins, MD Assistant Professor, College of Health Related Professions and College of Medicine, Department of Ophthalmology Jones Eye Institute University of Arkansas
Ocular Surface Syndrome after LASIK
 Alaa Atef Ghaith, MD Professor of Ophthalmology Alexandria University Ocular Surface Syndrome after LASIK Up to 33% of eyes Multifactorial entity which causes distress to the patients and physicians 1
Alaa Atef Ghaith, MD Professor of Ophthalmology Alexandria University Ocular Surface Syndrome after LASIK Up to 33% of eyes Multifactorial entity which causes distress to the patients and physicians 1
Managing Post-Operative Complications for LASIK and PRK
 Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
Managing Post-Operative Complications for LASIK and PRK LASIK Flap Complications Epithelial defects o Cause Basement membrane dystrophy Recurrent erosion syndrome Dry eyes Trauma PRK as alternative Pre-treat
The cornea is richly innervated by nerve fibers of the ophthalmic. Reinnervation in the Cornea after LASIK
 Reinnervation in the Cornea after LASIK Bong Hwan Lee, 1 Jay W. McLaren, 1 Jay C. Erie, 1 David O. Hodge, 2 and William M. Bourne 1 PURPOSE. Nerve fibers in the cornea are disrupted by photorefractive
Reinnervation in the Cornea after LASIK Bong Hwan Lee, 1 Jay W. McLaren, 1 Jay C. Erie, 1 David O. Hodge, 2 and William M. Bourne 1 PURPOSE. Nerve fibers in the cornea are disrupted by photorefractive
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment
 Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
Consent for LASIK (Laser In Situ Keratomileusis) Retreatment Please read the following consent form very carefully. Please initial at the bottom of each page where indicated. Do not sign this form unless
TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM
 1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
1 BoydVision TABLE OF CONTENTS: LASER EYE SURGERY CONSENT FORM Risks and Side Effects... 2 Risks Specific to PRK... 3 Risks Specific to LASIK... 4 Patient Statement of Consent... 5 Consent for Laser Eye
PHOTOREFRACTIVE KERATECTOMY (PRK) HAS BECOME
 Comparison of Corneal Nerve Regeneration and Sensitivity Between LASIK and Laser Epithelial Keratomileusis (LASEK) SEUNG JAE LEE, MD, JIN KUK KIM, MD, KYUNG YUL SEO, MD, EUNG KWEON KIM, MD, PHD, AND HYUNG
Comparison of Corneal Nerve Regeneration and Sensitivity Between LASIK and Laser Epithelial Keratomileusis (LASEK) SEUNG JAE LEE, MD, JIN KUK KIM, MD, KYUNG YUL SEO, MD, EUNG KWEON KIM, MD, PHD, AND HYUNG
Medicare and Corneal Surgery: Cosmetic versus Functional
 Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Medicare and Corneal Surgery: Cosmetic versus Functional Riva Lee Asbell INTRODUCTION With the introduction of several new CPT (Current Procedural Terminology) codes for cornea, corneal coding is in the
Dr. Booth received his medical degree from the University of California: San Diego and his bachelor of science from Stanford University.
 We've developed this handbook to help our patients become better informed about the entire process of laser vision correction. We hope you find it helpful and informative. Dr. Booth received his medical
We've developed this handbook to help our patients become better informed about the entire process of laser vision correction. We hope you find it helpful and informative. Dr. Booth received his medical
The Definition & Classification of Dry Eye Disease
 Issue: April 2008 The Definition & Classification of Dry Eye Disease Guidelines from the 2007 International Dry Eye Workshop BY MICHAEL A. LEMP, M. D. AND GARY N. FOULKS, M. D., F.A.C.S. The diagnosis
Issue: April 2008 The Definition & Classification of Dry Eye Disease Guidelines from the 2007 International Dry Eye Workshop BY MICHAEL A. LEMP, M. D. AND GARY N. FOULKS, M. D., F.A.C.S. The diagnosis
Our Commitment To You
 SYSTEM SUPPORT Quality-crafted, the system boasts dependability with high efficiency and low gas usage. We provide responsive service and maintenance contract options, supported by our nationwide direct
SYSTEM SUPPORT Quality-crafted, the system boasts dependability with high efficiency and low gas usage. We provide responsive service and maintenance contract options, supported by our nationwide direct
To date, several million patients have been treated worldwide. So why not discover the benefits The Eye Hospital can bring to your life.
 L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
L a s e r E y e S u r g e r y I N F O R M A T I O N 1 Welcome Imagine the freedom of being able to do away with glasses and contact lenses. You too, may be suitable for laser eye surgery, freeing you from
Financial Disclosure. LASIK Flap Parameters IntraLase Microkeratome 6/9/2008. Femtosecond LASIK Flaps: What Could We Customize Yesterday?
 Financial Disclosure Arturo Chayet, MD Tijuana, BC Mexico Perry S. Binder, MS, MD San Diego CA USA I have the following financial interests or relationships to disclose: AMO/IntraLase Corporation - C Acufocus
Financial Disclosure Arturo Chayet, MD Tijuana, BC Mexico Perry S. Binder, MS, MD San Diego CA USA I have the following financial interests or relationships to disclose: AMO/IntraLase Corporation - C Acufocus
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL
 REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
REFRACTIVE SURGERY NIGHTMARES Dr.ATHIYA AGARWAL POST LASIK INFECTION Infection occurring after photorefractive keratectomy (PRK) may be 1. Secondary to the defect in the epithelium as well as the use of
ReLEx smile Minimally invasive vision correction Information for patients
 ReLEx smile Minimally invasive vision correction Information for patients Seeing is living Our eyes are our most important sensory organ. The human brain obtains over 80 % of its information via the sense
ReLEx smile Minimally invasive vision correction Information for patients Seeing is living Our eyes are our most important sensory organ. The human brain obtains over 80 % of its information via the sense
MAZAHERI LASIK METHOD FOR VISUAL ENHANCEMENT TECHNICAL FIELD OF THE INVENTION. [0001] The present invention is directed, in general, to
![MAZAHERI LASIK METHOD FOR VISUAL ENHANCEMENT TECHNICAL FIELD OF THE INVENTION. [0001] The present invention is directed, in general, to MAZAHERI LASIK METHOD FOR VISUAL ENHANCEMENT TECHNICAL FIELD OF THE INVENTION. [0001] The present invention is directed, in general, to](/thumbs/26/8162223.jpg) MAZAHERI LASIK METHOD FOR VISUAL ENHANCEMENT TECHNICAL FIELD OF THE INVENTION [0001] The present invention is directed, in general, to a surgical procedure and, more particularly, to surgical procedure
MAZAHERI LASIK METHOD FOR VISUAL ENHANCEMENT TECHNICAL FIELD OF THE INVENTION [0001] The present invention is directed, in general, to a surgical procedure and, more particularly, to surgical procedure
The Evolution of the Optical Zone in Corneal Refractive Surgery. Bruce Drum, Ph.D.
 The Evolution of the Optical Zone in Corneal Refractive Surgery. Bruce Drum, Ph.D. FDA, Division of Ophthalmic and ENT Devices, Rockville, MD Disclaimer This presentation represents the professional opinion
The Evolution of the Optical Zone in Corneal Refractive Surgery. Bruce Drum, Ph.D. FDA, Division of Ophthalmic and ENT Devices, Rockville, MD Disclaimer This presentation represents the professional opinion
LASIK EPILASIK FEMTOSECOND LASER. Advantages
 LASIK EPILASIK FEMTOSECOND LASER Advantages There are many advantages to having laser vision correction. Laser vision correction gives most patients the freedom to enjoy their normal daily activities without
LASIK EPILASIK FEMTOSECOND LASER Advantages There are many advantages to having laser vision correction. Laser vision correction gives most patients the freedom to enjoy their normal daily activities without
Vision Correction Surgery Patient Information
 Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
Vision Correction Surgery Patient Information Anatomy of the eye: The eye is a complex organ composed of many parts, and normal vision requires these parts to work together. When a person looks at an object,
REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES
 Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
Introduction REFRACTIVE ERROR AND SURGERIES IN THE UNITED STATES 150 million wear eyeglasses or contact lenses 2.3 million refractive surgeries performed between 1995 and 2001 Introduction REFRACTIVE SURGERY:
LASIK, Epi LASIK and PRK Past present and future
 LASIK, Epi LASIK and PRK Past present and future Ioannis G. Pallikaris MD, PhD Institute of Vision and Optics University of Crete Medical School Heraklion Crete Greece Photorefractive Keratectomy Kerr-Muir
LASIK, Epi LASIK and PRK Past present and future Ioannis G. Pallikaris MD, PhD Institute of Vision and Optics University of Crete Medical School Heraklion Crete Greece Photorefractive Keratectomy Kerr-Muir
Pre-Operative Laser Surgery Information
 Pre-Operative Laser Surgery Information Contact 1800 10 20 20 Our Facility The Canberra Eye Laser Centre has always been at the forefront of refractive technology employing the most up to date equipment
Pre-Operative Laser Surgery Information Contact 1800 10 20 20 Our Facility The Canberra Eye Laser Centre has always been at the forefront of refractive technology employing the most up to date equipment
Cornea and Refractive Surgery Update
 Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
Cornea and Refractive Surgery Update Fall 2015 Optometric Education Dinner Sebastian Lesniak MD Matossian Eye Associates Disclosures: None Bio: Anterior Segment and Cornea Surgery Fellowship Wills Eye
The pinnacle of refractive performance.
 Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
Introducing! The pinnacle of refractive performance. REFRACTIVE SURGERY sets a new standard in LASIK outcomes More than 98% of patients would choose it again. 1 It even outperformed glasses and contacts
Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report
 Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
Case Reports in Ophthalmological Medicine Volume 2011, Article ID 796463, 4 pages doi:10.1155/2011/796463 Case Report Laser Vision Correction on Patients with Sick Optic Nerve: A Case Report Ming Chen
FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US
 FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US JON DISHLER, MD DENVER, COLORADO, USA INTRODUCTION AND STUDY OBJECTIVES This article summarizes the first US
FIRST EXPERIENCE WITH THE ZEISS FEMTOSECOND SYSTEM IN CONJUNC- TION WITH THE MEL 80 IN THE US JON DISHLER, MD DENVER, COLORADO, USA INTRODUCTION AND STUDY OBJECTIVES This article summarizes the first US
How To See With An Cl
 Deciding on the vision correction procedure that s right for you is an important one. The table below provides a general comparison of the major differences between Visian ICL, LASIK and PRK. It is NOT
Deciding on the vision correction procedure that s right for you is an important one. The table below provides a general comparison of the major differences between Visian ICL, LASIK and PRK. It is NOT
Femto-LASIK. Pulsewidth: Ultrashort-pulse micro- machining can make sub- wavelength holes. micromachining
 All-laser laser LASIK (Femto( Femto-LASIK) Femto-LASIK 台 大 眼 科 王 一 中 IntraLase 2/1 Perfect Vision Ziemer (DaVinci) Carl Zeiss Meditec Pulsewidth: Femtosecond laser (Nd:Glass)) 153 nm (near infrared) Each
All-laser laser LASIK (Femto( Femto-LASIK) Femto-LASIK 台 大 眼 科 王 一 中 IntraLase 2/1 Perfect Vision Ziemer (DaVinci) Carl Zeiss Meditec Pulsewidth: Femtosecond laser (Nd:Glass)) 153 nm (near infrared) Each
Excimer Laser Eye Surgery
 Excimer Laser Eye Surgery This booklet contains general information that is not specific to you. If you have any questions after reading this, ask your own physician or health care worker. They know you
Excimer Laser Eye Surgery This booklet contains general information that is not specific to you. If you have any questions after reading this, ask your own physician or health care worker. They know you
Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State
 Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State University Columbus, Ohio Refractive Errors Myopia (nearsightedness)
Curtin G. Kelley, M.D. Director of Vision Correction Surgery Arena Eye Surgeons Associate Clinical Professor of Ophthalmology The Ohio State University Columbus, Ohio Refractive Errors Myopia (nearsightedness)
Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK
 Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK Javad Amoozadeh, MD; Soheil Aliakbari, MD; Amir-Houshang Behesht-Nejad, MD; Mohammad-Amin Seyedian, MD; Bijan Rezvan, DDS; Hassan
Confocal Microscopy of Corneal Stroma and Endothelium After LASIK and PRK Javad Amoozadeh, MD; Soheil Aliakbari, MD; Amir-Houshang Behesht-Nejad, MD; Mohammad-Amin Seyedian, MD; Bijan Rezvan, DDS; Hassan
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Laser Vision Correction: A Tutorial for Medical Students
 Laser Vision Correction: A Tutorial for Medical Students Written by: Reid Turner, M4 Reviewed by: Anna Kitzmann, MD Illustrations by: Steve McGaughey, M4 November 29, 2011 1. Introduction Laser vision
Laser Vision Correction: A Tutorial for Medical Students Written by: Reid Turner, M4 Reviewed by: Anna Kitzmann, MD Illustrations by: Steve McGaughey, M4 November 29, 2011 1. Introduction Laser vision
LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY
 Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
Thi-Qar Medical Journal (TQMJ): Vol(4) No(4):1(14-21) SUMMARY: LASIK SURGERY IN AL- NASSIRYA CITY A CLINICOSTATISTICAL STUDY Dr. Ali Jawad AL- Gidis (M.B.Ch.B., D.O., F.I.C.O.)* Background: LASIK which
Defense Technical Information Center Compilation Part Notice
 UNCLASSIFIED Defense Technical Information Center Compilation Part Notice ADP020051 TITLE: A Review of Infrared Laser Energy Absorption and Subsequent Healing in the Cornea DISTRIBUTION: Approved for public
UNCLASSIFIED Defense Technical Information Center Compilation Part Notice ADP020051 TITLE: A Review of Infrared Laser Energy Absorption and Subsequent Healing in the Cornea DISTRIBUTION: Approved for public
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
How To Know If You Can See Without Glasses Or Contact Lense After Lasik
 The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
The LASIK experience I WHO CAN HAVE LASIK? To be eligible for LASIK you should be at least 21 years of age, have healthy eyes and be in good general health. Your vision should not have deteriorated significantly
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) John D. Goosey, MD Introduction DSAEK is a corneal transplant technique where the unhealthy, diseased, posterior portion of a patient s cornea
Corneal Collagen Cross-Linking (CXL) With Riboflavin
 Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Refractive Errors & Correction
 Super Vision 6 Chapter Lasik is currently the most sophisticated procedure for correction of refractive errors. Lasik is an acronym for Laser Assisted Insitu Keratomileusis. In Lasik, Excimer laser is
Super Vision 6 Chapter Lasik is currently the most sophisticated procedure for correction of refractive errors. Lasik is an acronym for Laser Assisted Insitu Keratomileusis. In Lasik, Excimer laser is
Applications in Dermatology, Dentistry and LASIK Eye Surgery using LASERs
 Applications in Dermatology, Dentistry and LASIK Eye Surgery using LASERs http://www.medispainstitute.com/menu_laser_tattoo.html http://www.life123.com/bm.pix/bigstockphoto_close_up_of_eye_surgery_catar_2264267.s600x600.jpg
Applications in Dermatology, Dentistry and LASIK Eye Surgery using LASERs http://www.medispainstitute.com/menu_laser_tattoo.html http://www.life123.com/bm.pix/bigstockphoto_close_up_of_eye_surgery_catar_2264267.s600x600.jpg
Alexandria s Guide to LASIK
 Alexandria s Guide to LASIK A Community Service Project sponsored by: Wallace Laser Center Your Guide To A Successful LASIK Procedure The word LASIK is actually an acronym for Laser Assisted In-Situ Keratomileusis.
Alexandria s Guide to LASIK A Community Service Project sponsored by: Wallace Laser Center Your Guide To A Successful LASIK Procedure The word LASIK is actually an acronym for Laser Assisted In-Situ Keratomileusis.
Surgical Advances in Keratoconus. Keratoconus. Innovations in Ophthalmology. New Surgical Advances. Diagnosis of Keratoconus. Scheimpflug imaging
 Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
Surgical Advances in Keratoconus Keratoconus Ectatic disorder 1 in 1,000 individuals Starts in adolescence & early adulthood Uncertain cause 20% require corneal transplant Innovations in Ophthalmology
refractive surgery a closer look
 2011-2012 refractive surgery a closer look How the eye works Light rays enter the eye through the clear cornea, pupil and lens. These light rays are focused directly onto the retina, the light-sensitive
2011-2012 refractive surgery a closer look How the eye works Light rays enter the eye through the clear cornea, pupil and lens. These light rays are focused directly onto the retina, the light-sensitive
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
your bestchoice for Laser Vision Correction www.aucklandeyelaser.co.nz
 your bestchoice for Laser Vision Correction www.aucklandeyelaser.co.nz Auckland Eye is the Centre of Excellence for Laser Eye Surgery in Auckland Welcome to a life of freedom from contact lenses and glasses.
your bestchoice for Laser Vision Correction www.aucklandeyelaser.co.nz Auckland Eye is the Centre of Excellence for Laser Eye Surgery in Auckland Welcome to a life of freedom from contact lenses and glasses.
VISX Wavefront-Guided LASIK for Correction of Myopic Astigmatism, Hyperopic Astigmatism and Mixed Astigmatism (CustomVue LASIK Laser Treatment)
 CustomVue Advantage Patient Information Sheet VISX Wavefront-Guided LASIK for Correction of Myopic Astigmatism, Hyperopic Astigmatism and Mixed Astigmatism (CustomVue LASIK Laser Treatment) Statements
CustomVue Advantage Patient Information Sheet VISX Wavefront-Guided LASIK for Correction of Myopic Astigmatism, Hyperopic Astigmatism and Mixed Astigmatism (CustomVue LASIK Laser Treatment) Statements
IntraLase and LASIK: Risks and Complications
 No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
No surgery is without risks and possible complications and LASIK is no different in that respect. At Trusted LASIK Surgeons, we believe patients can minimize these risks by selecting a highly qualified
Risks and Limitations of LASIK Procedure
 Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
Drs. Fine, Hoffman & Packer, LLC 1550 Oak Street, Suite #5 Eugene, OR 97401 541-687-2110 From Drs. Fine, Hoffman, & Packer Risks and Limitations of LASIK Procedure Infection, serious injury, or even death,
LASIK Eye Surgery Report
 LASIK Eye Surgery Report LASIK eye surgery can be a liberating experience for people hoping to reduce or eliminate their dependence on glasses and contact lenses. Most patients do not realize how evolved
LASIK Eye Surgery Report LASIK eye surgery can be a liberating experience for people hoping to reduce or eliminate their dependence on glasses and contact lenses. Most patients do not realize how evolved
Flap striae after LASIK can be treated successfully
 Flap striae after LASIK can be treated successfully Following a few key rules leads to positive outcomes, surgeons say. by Insun Lee, Miten Vasa, and Emil W. Chynn, MD Special to OCULAR SURGERY NEWS LASIK
Flap striae after LASIK can be treated successfully Following a few key rules leads to positive outcomes, surgeons say. by Insun Lee, Miten Vasa, and Emil W. Chynn, MD Special to OCULAR SURGERY NEWS LASIK
Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology
 Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to
Eye Associates Custom LASIK With IntraLASIK Correction Of Nearsightedness, Farsightedness, and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to
Refractive Surgery. Evolution of Refractive Error Correction
 Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
Refractive Surgery Techniques that correct for refractive error in the eye have undergone dramatic evolution. The cornea is the easiest place to place a correction, so most techniques have focused on modifying
PATIENT CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
INTRODUCTION: You have been diagnosed with myopia (nearsightedness) or hyperopia (farsightedness) with or without astigmatism, or astigmatism alone. Myopia is a result of light entering the eye and focusing
FUNCTIONS OF THE SKIN
 FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery*
 Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery* I. Introduction A. Definition and Scope of Subspecialty Fellowship training requires more in depth education
Program Requirements for Fellowship Education in Cornea, External Diseases & Refractive Surgery* I. Introduction A. Definition and Scope of Subspecialty Fellowship training requires more in depth education
Managing Challenging Cases in Refractive Surgery
 Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
Managing Challenging Cases in Refractive Surgery Missouri Optometric Association Stephen A. Wexler, MD Eric E. Polk, OD, FAAO Outline The presenters will review challenging cases they have managed in refractive
Consumer s Guide to LASIK
 Consumer s Guide to LASIK A Community Service Project brought to you by Price Vision Group Your Guide To A Successful LASIK Procedure The purpose of this educational guide is to help prospective patients
Consumer s Guide to LASIK A Community Service Project brought to you by Price Vision Group Your Guide To A Successful LASIK Procedure The purpose of this educational guide is to help prospective patients
Accelerated Refractive Performance
 Accelerated Refractive Performance Get There at the Speed of WaveLight Designed to accommodate your refractive technology goals now and into the future, the WaveLight Workstation is a faster way to get
Accelerated Refractive Performance Get There at the Speed of WaveLight Designed to accommodate your refractive technology goals now and into the future, the WaveLight Workstation is a faster way to get
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery
 Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Anterior Lamellar Keratoplasty With a Microkeratome: A Method for Managing Complications After Refractive Surgery Farhad Hafezi, MD; Michael Mrochen, PhD; Franz Fankhauser II, MD; Theo Seiler, MD, PhD
Dry eye after LASIK for myopia: Incidence and risk factors
 Shoja:Shoja 30-01-2007 16:32 Pagina 1 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 1-6 Dry eye after LASIK for myopia: Incidence and risk factors M.R. SHOJA, M.R. BESHARATI Department
Shoja:Shoja 30-01-2007 16:32 Pagina 1 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 1-6 Dry eye after LASIK for myopia: Incidence and risk factors M.R. SHOJA, M.R. BESHARATI Department
Femtosecond Lasers in LASIK Surgery
 Femtosecond Lasers in LASIK Surgery Dr Chan Tat Keong Senior Consultant Refractive Surgery Service Singapore National Eye Centre Disclosure Speaker has no financial interest in the products to be discussed
Femtosecond Lasers in LASIK Surgery Dr Chan Tat Keong Senior Consultant Refractive Surgery Service Singapore National Eye Centre Disclosure Speaker has no financial interest in the products to be discussed
Management of Epithelial Ingrowth after LASIK. Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA
 Management of Epithelial Ingrowth after LASIK Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA Acknowledgements IOP Ophthalmics Staar Surgical Case Presentation 46
Management of Epithelial Ingrowth after LASIK Helen K. Wu, MD New England Eye Center Tufts University School of Medicine Boston, MA Acknowledgements IOP Ophthalmics Staar Surgical Case Presentation 46
Rediscover quality of life thanks to vision correction with technology from Carl Zeiss. Patient Information
 Rediscover quality of life thanks to vision correction with technology from Carl Zeiss Patient Information 5 2 It was really w Vision defects: Light that goes astray For clear vision the eyes, cornea and
Rediscover quality of life thanks to vision correction with technology from Carl Zeiss Patient Information 5 2 It was really w Vision defects: Light that goes astray For clear vision the eyes, cornea and
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus
 Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
Complications of Combined Topography-Guided Photorefractive Keratectomy and Corneal Collagen Crosslinking in Keratoconus Michelle Cho, M.D. 1 Anastasios John Kanellopoulos, M.D 1,2 New York University
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition?
 There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
There Are Millions of People at Risk For Dry Eye Who Is Likely to Develop This Irritating Condition? Dry eye can be a temporary or chronic condition and occurs when the eye does not produce tears properly,
Descemet s Stripping Endothelial Keratoplasty (DSEK)
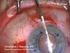 Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
Descemet s Stripping Endothelial Keratoplasty (DSEK) Your doctor has decided that you will benefit from a corneal transplant operation. This handout will explain your options to you. It explains the differences
TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT
 TLC The Laser Center (Northeast) Inc. TLC Laser Eye Centers (Charlotte) TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT Informed Consent. The purpose of this Informed Consent is to help
TLC The Laser Center (Northeast) Inc. TLC Laser Eye Centers (Charlotte) TLC LASER EYE CENTERS VISION CORRECTION SURGERY INFORMED CONSENT Informed Consent. The purpose of this Informed Consent is to help
SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC)
 SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC) PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU
SLADE AND BAKER VISION CENTER INFORMED CONSENT FOR LASER VISION CORRECTION (LVC) PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU
Congratulations! You have just joined the thousands of people who are enjoying the benefits of laser vision correction.
 Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
Dear Valued Patient, Thank you for choosing Shady Grove Ophthalmology for your laser vision correction procedure. Our excellent staff is committed to offering you the highest quality eye care using state
Refractive Errors. Refractive Surgery. Eye Care In Modern Life. Structure of the Eye. Structure of the Eye. Structure of the Eye. Structure of the Eye
 Structure of the Eye Eye Care In Modern Life Dr. Dorothy Fan Department of Ophthalmology & Visual Sciences September 2007 Information age > 90% of sensory input Blindness is one of the most fearful disabilities
Structure of the Eye Eye Care In Modern Life Dr. Dorothy Fan Department of Ophthalmology & Visual Sciences September 2007 Information age > 90% of sensory input Blindness is one of the most fearful disabilities
Original Article Effects of nerve growth factor on nerve regeneration after corneal nerve damage
 Int J Clin Exp Med 2014;7(11):4584-4589 www.ijcem.com /ISSN:1940-5901/IJCEM0002088 Original Article Effects of nerve growth factor on nerve regeneration after corneal nerve damage Ke Ma, Naihong Yan, Yongzhi
Int J Clin Exp Med 2014;7(11):4584-4589 www.ijcem.com /ISSN:1940-5901/IJCEM0002088 Original Article Effects of nerve growth factor on nerve regeneration after corneal nerve damage Ke Ma, Naihong Yan, Yongzhi
SCHWIND CAM Perfect Planning wide range of applications
 SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PALK-CAM PTK-CAM 2 SCHWIND CAM the system solution The latest version of the modular SCHWIND CAM represents an even more efficient
SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PALK-CAM PTK-CAM 2 SCHWIND CAM the system solution The latest version of the modular SCHWIND CAM represents an even more efficient
Intended Benefits. Who Is Not Eligible For the Procedure? (Intralase Sub-Bowman s Keratomileusis)
 PATIENT CONSENT FORM Intralase SBK / WGA SBK (Intralase Sub-Bowman s Keratomileusis) Intralase Sub-Bowman s Keratomileusis (SBK) is a term used to describe a Laser Vision Correction procedure where a laser
PATIENT CONSENT FORM Intralase SBK / WGA SBK (Intralase Sub-Bowman s Keratomileusis) Intralase Sub-Bowman s Keratomileusis (SBK) is a term used to describe a Laser Vision Correction procedure where a laser
Eye Care In Modern Life
 Eye Care In Modern Life Dr. Dorothy Fan Department of Ophthalmology & Visual Sciences November 2009 [email protected] Structure of the Eye Information age > 90% of sensory input Blindness is one of
Eye Care In Modern Life Dr. Dorothy Fan Department of Ophthalmology & Visual Sciences November 2009 [email protected] Structure of the Eye Information age > 90% of sensory input Blindness is one of
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK)
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding Photorefractive Keratectomy (PRK)
Refractive Surgery. Common Refractive Errors
 Refractive Surgery Over the last 25 years developments in medical technology and Refractive Surgery allow almost all need for glasses and contact lenses to be eliminated. Currently there are a number of
Refractive Surgery Over the last 25 years developments in medical technology and Refractive Surgery allow almost all need for glasses and contact lenses to be eliminated. Currently there are a number of
How To Treat Eye Problems With A Laser
 1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
1550 Oak St., Suite 5 1515 Oak St., St Eugene, OR 97401 Eugene, OR 97401 (541) 687-2110 (541) 344-2010 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) This information is to help you make an informed
Neurotrophic factors and Their receptors
 Neurotrophic factors and Their receptors Huang Shu-Hong Institute of neurobiology 1 For decades, scientists believed that brain cells of the central nervous system could not regrow following damage due
Neurotrophic factors and Their receptors Huang Shu-Hong Institute of neurobiology 1 For decades, scientists believed that brain cells of the central nervous system could not regrow following damage due
Laser in situ keratomileusis (LASIK)
 Corneal Stromal Changes Induced by Myopic LASIK Minna Vesaluoma, 1 Juan Pérez Santonja, 2 W. Matthew Petroll, 3 Tuuli Linna, 1 Jorge Alió, 2 and Timo Tervo 1 PURPOSE. Despite the rapidly growing popularity
Corneal Stromal Changes Induced by Myopic LASIK Minna Vesaluoma, 1 Juan Pérez Santonja, 2 W. Matthew Petroll, 3 Tuuli Linna, 1 Jorge Alió, 2 and Timo Tervo 1 PURPOSE. Despite the rapidly growing popularity
Keratoconus. Progressive bilateral ectasia. Onset puberty. Prevalence 1:2000. 20% progress to transplantation. Pathogenesis unclear
 Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Keratoconus Progressive bilateral ectasia Onset puberty Prevalence 1:2000 20% progress to transplantation Pathogenesis unclear Increased pepsin and catalase Decreased collagen crosslinking cf normal Conventional
Chetek-Weyerhaeuser High School
 Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Institute of Ophthalmology. Thyroid Eye Disease. aka Thyroid Associated Ophthalmopathy
 Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
Institute of Ophthalmology Thyroid Eye Disease aka Thyroid Associated Ophthalmopathy Causes TED/TAO is an eye disease associated with disease of the thyroid gland Most commonly, it occurs with an overactive
